Electronic Devices That Identify Individuals with Fever in Crowded Places: A Prototype
Abstract
:Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Lee, C.S.; Lee, J.H. Dynamics of clinical symptoms in patients with pandemic influenza A (H1N1). Clin. Microbiol. Infect. 2010, 16, 389–390. [Google Scholar] [CrossRef] [PubMed]
- Waner, L. Mixed viral infections: Detection and management. Clin. Microbiol. Rev. 1994, 7, 143–151. [Google Scholar] [CrossRef] [PubMed]
- Lin, M.Y.; Trick, W.E. Informatics in infection control. Infect. Dis. Clin. N. Am. 2016, 30, 759–770. [Google Scholar] [CrossRef] [PubMed]
- Boggild, A.K.; Esposito, D.H.; Kozarsky, P.E.; Ansdell, V.; Beeching, N.J.; Campion, D.; Castelli, F.; Caumes, E.; Chappuis, F.; Cramer, J.P.; et al. Differential diagnosis of illness in travelers arriving from Sierra Leone, Liberia, or Guinea: A Cross-sectional Study from the GeoSentinel Surveillance Network. Ann. Intern. Med. 2015, 162, 757–764. [Google Scholar] [CrossRef] [PubMed]
- Ruan, Z.; Wang, C.; Hui, P.M.; Liu, Z. Integrated travel network model for studying epidemics: Interplay between journeys and epidemic. Sci. Rep. 2015, 5, 11401. [Google Scholar] [CrossRef] [PubMed]
- Gibney, E. The inside story on wearable electronics. Nature 2015, 528, 26–28. [Google Scholar] [CrossRef] [PubMed]
- Nouvellet, P.; Garske, T.; Mills, H.L.; Nedjati-Gilani, G.; Hinsley, W.; Blake, I.M.; Van Kerkhove, M.D.; Cori, A.; Dorigatti, I.; Jombart, T.; et al. The role of rapid diagnostics in managing Ebola epidemics. Nature 2016, 528, S109–S116. [Google Scholar] [CrossRef] [PubMed]
- Polanco, C.; Arias Estrada, M.; Castañón González, J.A. Zika virus disease: Electronic devices (Letter to the Editor) The next steps on Zika. Nature 2016, 530, 5. [Google Scholar] [CrossRef]
- Caliò, R.; Rongala, U.B.; Camboni, D.; Milazzo, M.; Stefanini, C.; de Petris, G.; Oddo, C.M. Piezoelectric energy harvesting solutions. Sensors 2014, 14, 4755–4790. [Google Scholar] [CrossRef] [PubMed]
- Koch, N. Organic electronic devices and their functional interfaces. Chemphyschem 2007, 8, 1438–1455. [Google Scholar] [CrossRef] [PubMed]
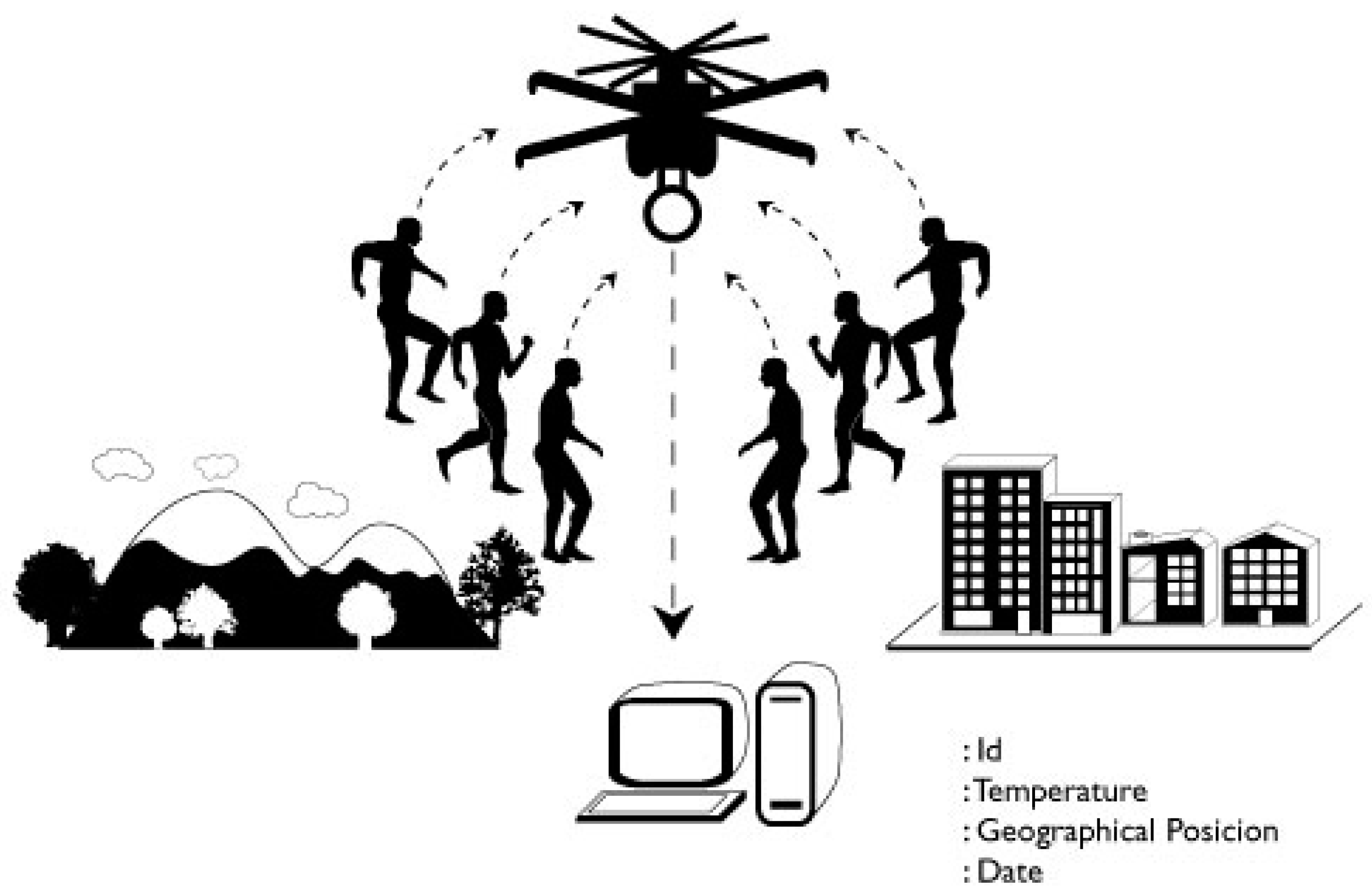
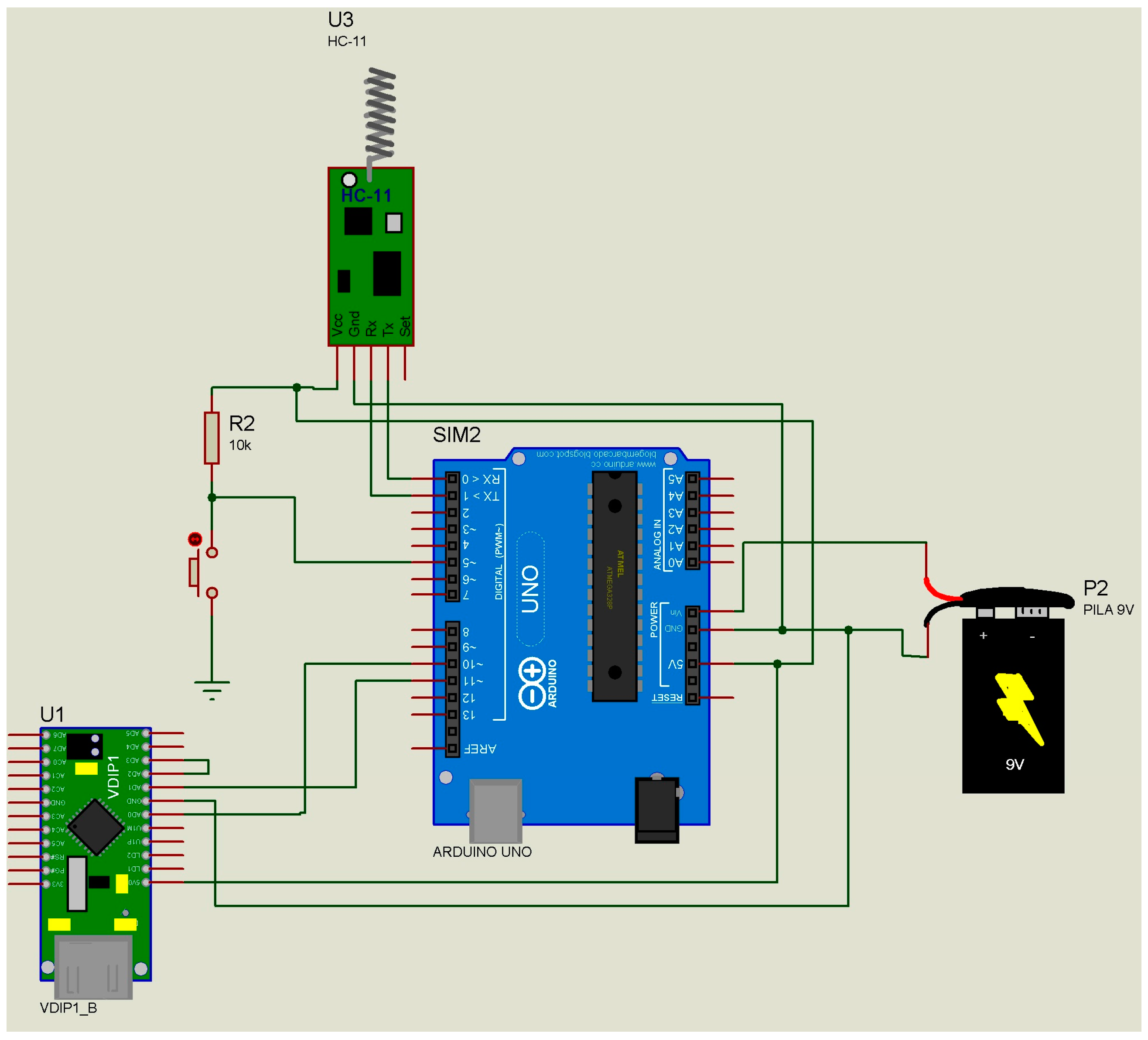
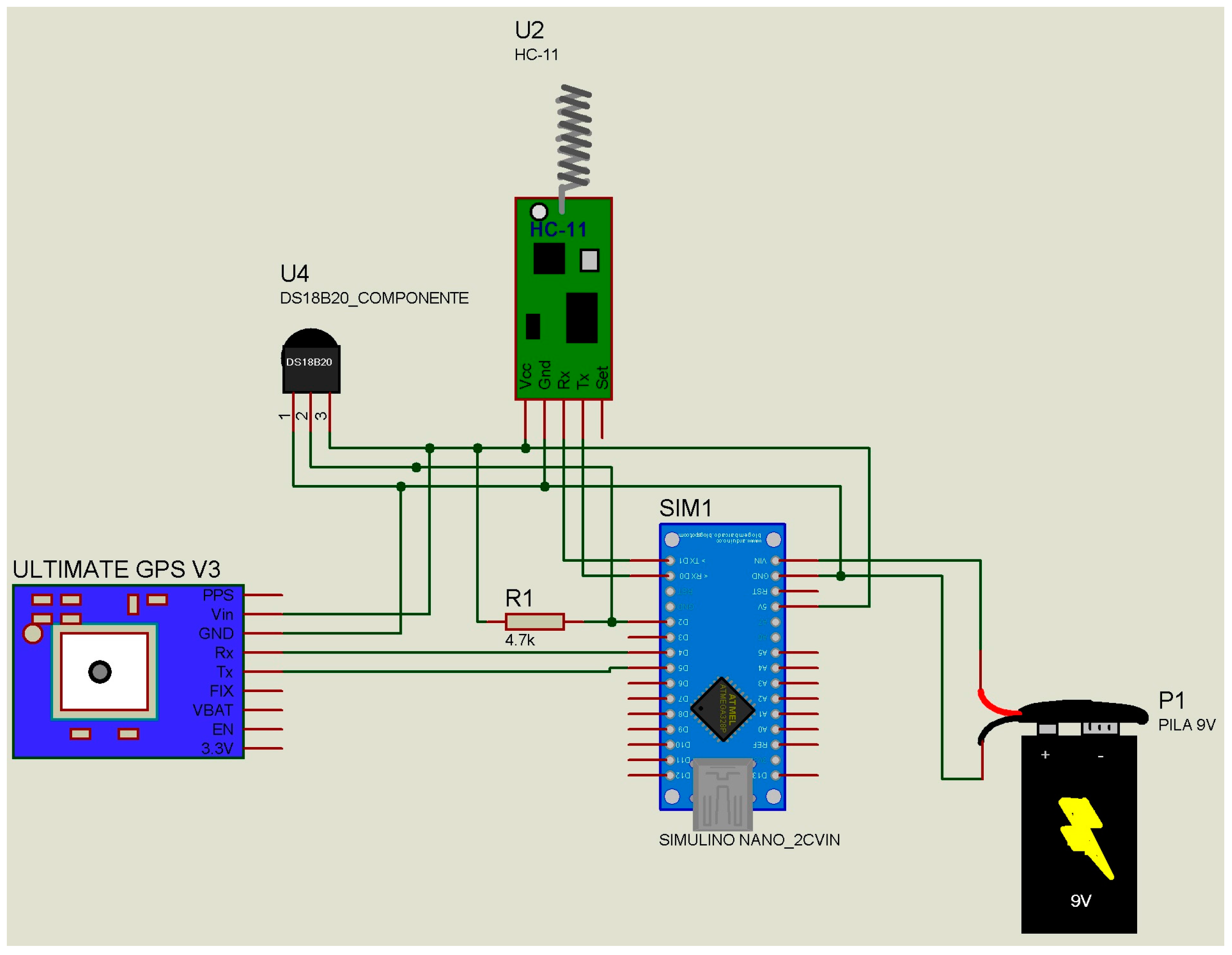
| Start | Id | Temp | Long | Lat | Alt | DD | MM | YYYY | HH | mm | DF | End |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| @ | A | 2637 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 19 | ! | & |
| @ | B | 2512 | 99.1123431 | 19.966522 | 02.92 | 29 | 06 | 16 | 22 | 20 | ! | & |
| @ | A | 2630 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 20 | ! | & |
| @ | B | 2510 | 99.1123431 | 19.966522 | 02.90 | 29 | 06 | 16 | 22 | 20 | ! | & |
| @ | A | 2611 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 20 | ! | & |
| @ | B | 2524 | 99.1123431 | 19.966522 | 02.90 | 29 | 06 | 16 | 22 | 21 | ! | & |
| @ | A | 2636 | 99.1871331 | 19.333145 | 86.15 | 29 | 06 | 16 | 22 | 21 | ! | & |
| @ | B | 2457 | 99.1123431 | 19.966522 | 02.85 | 29 | 06 | 16 | 22 | 21 | ! | & |
| @ | A | 2633 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 21 | ! | & |
| @ | B | 2565 | 99.1123431 | 19.966522 | 02.67 | 29 | 06 | 16 | 22 | 21 | ! | & |
| @ | A | 2337 | 99.1871331 | 19.333145 | 72.84 | 29 | 06 | 16 | 22 | 22 | ! | & |
| @ | B | 2618 | 99.1123431 | 19.966522 | 02.78 | 29 | 06 | 16 | 22 | 22 | ! | & |
| @ | A | 2634 | 99.1871331 | 19.333145 | 86.11 | 29 | 06 | 16 | 22 | 22 | ! | & |
| @ | B | 2573 | 99.1123431 | 19.966522 | 02.88 | 29 | 06 | 16 | 22 | 22 | ! | & |
| @ | A | 2617 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 23 | ! | & |
| @ | B | 2606 | 99.1123431 | 19.966522 | 02.90 | 29 | 06 | 16 | 22 | 23 | ! | & |
| @ | A | 2517 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 23 | ! | & |
| @ | B | 2649 | 99.1123431 | 19.966522 | 02.56 | 29 | 06 | 16 | 22 | 23 | ! | & |
| @ | A | 2410 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 23 | ! | & |
| @ | B | 2586 | 99.1123431 | 19.966522 | 02.89 | 29 | 06 | 16 | 22 | 24 | ! | & |
| @ | A | 2637 | 99.1871331 | 19.333145 | 85.10 | 29 | 06 | 16 | 22 | 24 | ! | & |
| @ | B | 2512 | 99.1123431 | 19.966522 | 02.92 | 29 | 06 | 16 | 22 | 24 | ! | & |
| @ | A | 2630 | 99.1871331 | 19.333145 | 86.10 | 29 | 06 | 16 | 22 | 24 | ! | & |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Polanco González, C.; Islas Vazquez, I.; Castañón González, J.A.; Buhse, T.; Arias-Estrada, M. Electronic Devices That Identify Individuals with Fever in Crowded Places: A Prototype. Micromachines 2017, 8, 202. https://doi.org/10.3390/mi8070202
Polanco González C, Islas Vazquez I, Castañón González JA, Buhse T, Arias-Estrada M. Electronic Devices That Identify Individuals with Fever in Crowded Places: A Prototype. Micromachines. 2017; 8(7):202. https://doi.org/10.3390/mi8070202
Chicago/Turabian StylePolanco González, Carlos, Ignacio Islas Vazquez, Jorge Alberto Castañón González, Thomas Buhse, and Miguel Arias-Estrada. 2017. "Electronic Devices That Identify Individuals with Fever in Crowded Places: A Prototype" Micromachines 8, no. 7: 202. https://doi.org/10.3390/mi8070202
APA StylePolanco González, C., Islas Vazquez, I., Castañón González, J. A., Buhse, T., & Arias-Estrada, M. (2017). Electronic Devices That Identify Individuals with Fever in Crowded Places: A Prototype. Micromachines, 8(7), 202. https://doi.org/10.3390/mi8070202





