Synergistic Interplay between Curcumin and Polyphenol-Rich Foods in the Mediterranean Diet: Therapeutic Prospects for Neurofibromatosis 1 Patients
Abstract
:1. Introduction
2. Materials and Methods
2.1. Methods
2.2. Ethics
2.3. Plasma Sample Preparation
2.4. Chromatographic Analysis of Curcuminoids
2.5. Statistical Analysis
3. Results
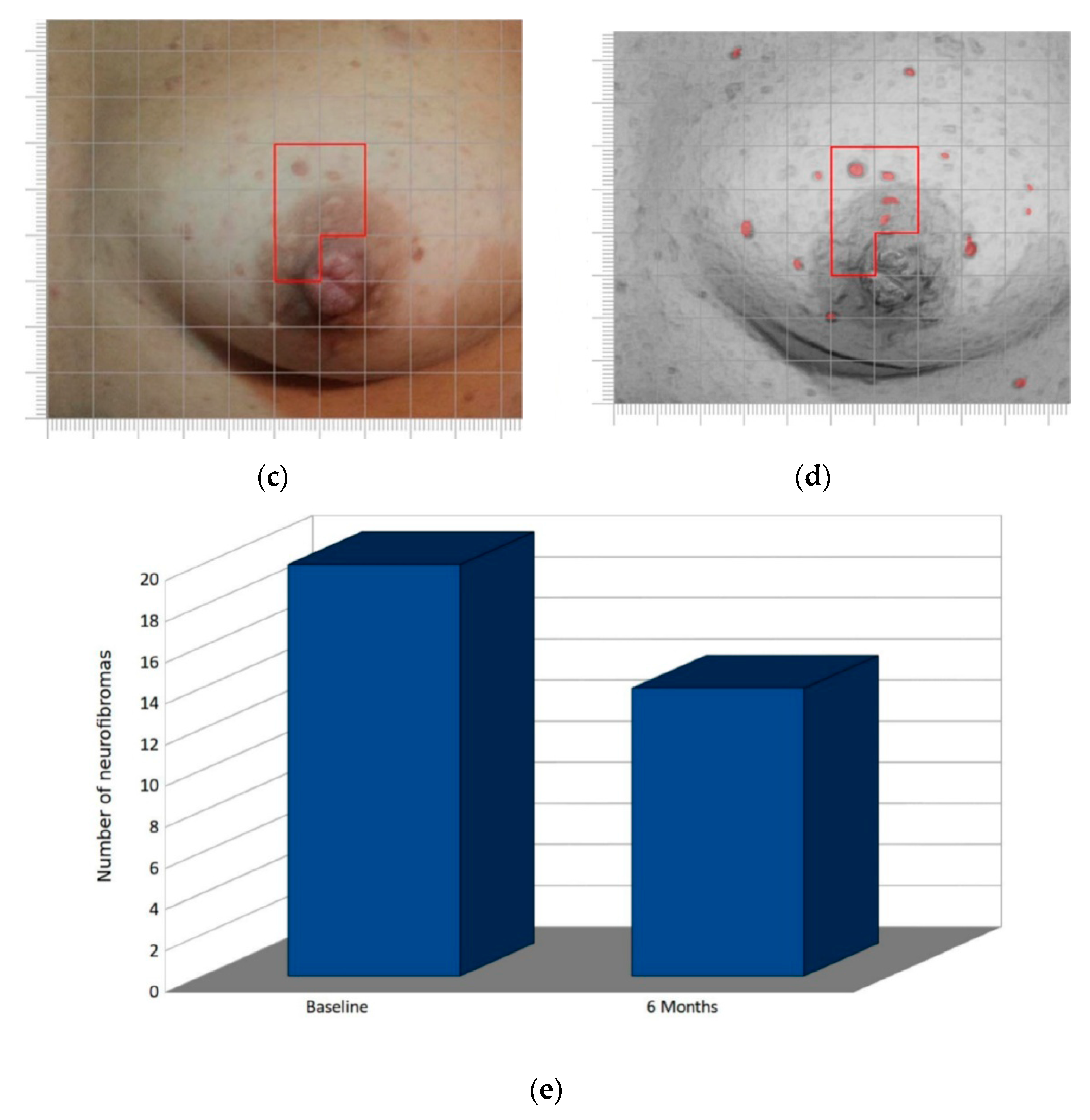
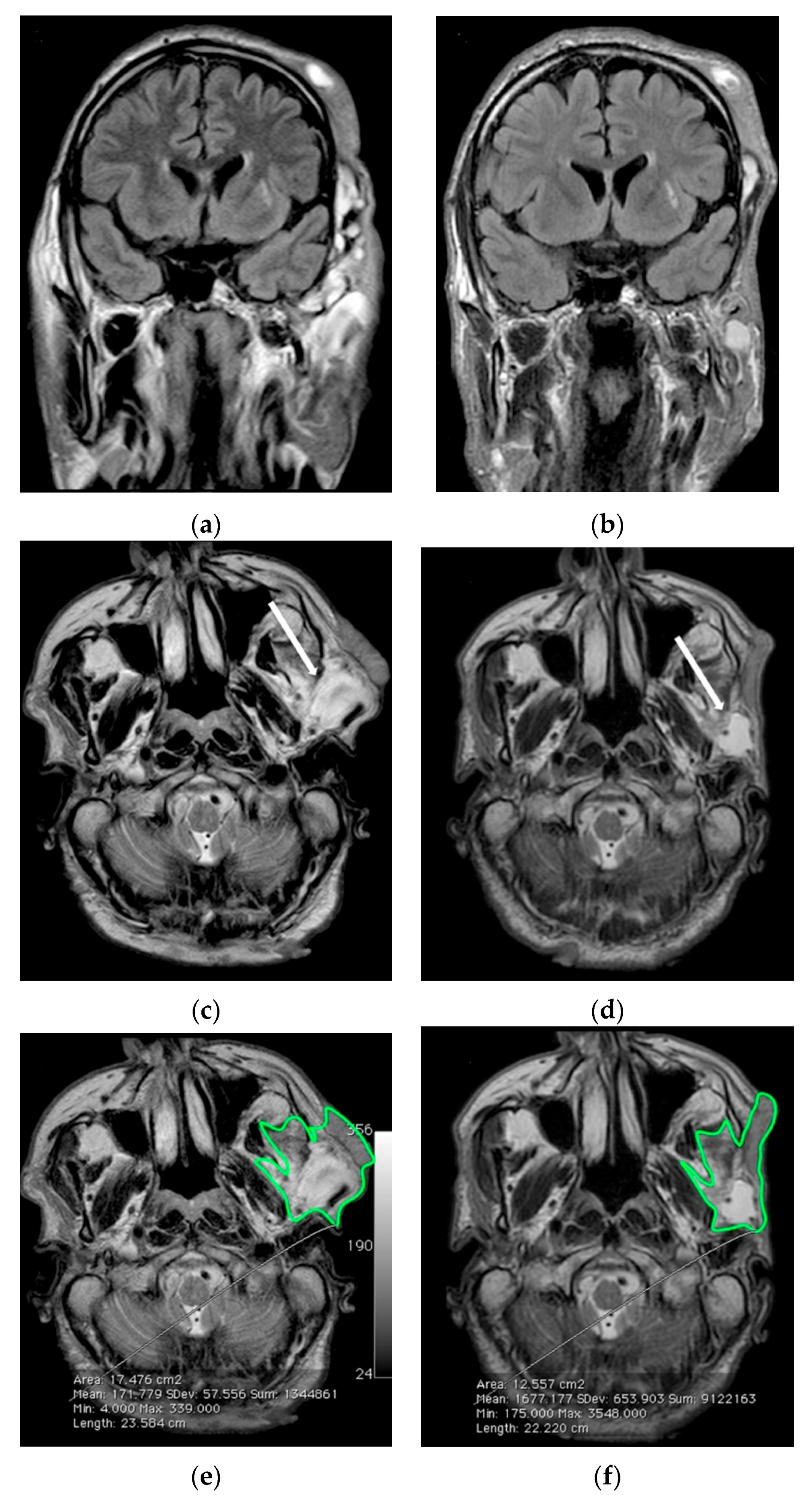
3.1. Follow-Up
3.2. Nutritional and Bioimpedentiometric Data
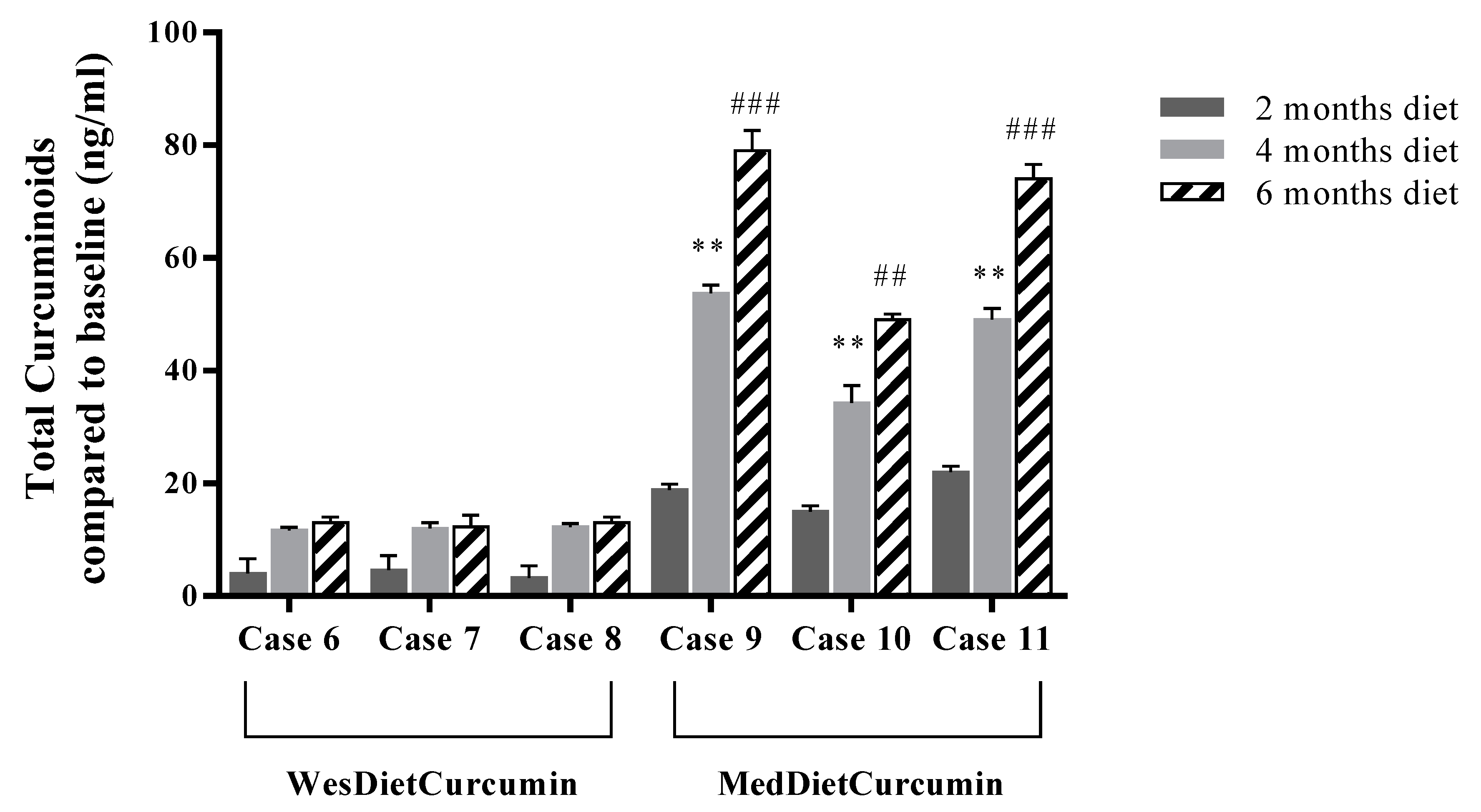
3.3. Plasma Curcuminoid Level
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Conte, R.; De Luca, I.; De Luise, A.; Petillo, O.; Calarco, A.; Peluso, G. New Therapeutic Potentials of Nanosized Phytomedicine. J. Nanosci. Nanotechnol. 2016, 16, 8176–8187. [Google Scholar] [CrossRef]
- Momtazi, A.A.; Derosa, G.; Maffioli, P.; Banach, M.; Sahebkar, A. Role of microRNAs in the Therapeutic Effects of Curcumin in Non-Cancer Diseases. Mol. Diagn. Ther. 2016, 20, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Sahebkar, A.; Cicero, A.F.; Simental-Mendia, L.E.; Aggarwal, B.B.; Gupta, S.C. Curcumin downregulates human tumor necrosis factor-alpha levels: A systematic review and meta-analysis ofrandomized controlled trials. Pharmacol. Res. 2016, 107, 234–242. [Google Scholar] [CrossRef] [PubMed]
- Sahebkar, A. Autophagic activation: A key piece of the puzzle for the curcumin-associated cognitive enhancement? J. Psychopharmacol. 2016, 30, 93–94. [Google Scholar] [CrossRef] [PubMed]
- Sahebkar, A. Curcuminoids for the management of hypertriglyceridaemia. Nat. Rev. Cardiol. 2014, 11, 123. [Google Scholar] [CrossRef] [PubMed]
- Derosa, G.; Maffioli, P.; Simental-Mendia, L.E.; Bo, S.; Sahebkar, A. Effect of curcumin on circulating interleukin-6 concentrations: A systematic review and meta-analysis of randomized controlled trials. Pharmacol. Res. 2016, 111, 394–404. [Google Scholar] [CrossRef] [PubMed]
- Chuang, S.E.; Kuo, M.L.; Hsu, C.H.; Chen, C.R.; Lin, J.K.; Lai, G.M.; Hsieh, C.Y.; Cheng, A.L. Curcumin-containing diet inhibits diethylnitrosamine-induced murine hepatocarcinogenesis. Carcinogenesis 2000, 21, 331–335. [Google Scholar] [CrossRef] [PubMed]
- Casaburi, I.; Puoci, F.; Chimento, A.; Sirianni, R.; Ruggiero, C.; Avena, P.; Pezzi, V. Potential of olive oil phenols as chemopreventive and therapeutic agents against cancer: A review of in vitro studies. Mol. Nutr. Food Res. 2013, 57, 71–83. [Google Scholar] [CrossRef] [PubMed]
- Bayet-Robert, M.; Morvan, D. Metabolomics reveals metabolic targets and biphasic responses in breast cancer cells treated by curcumin alone and in association with docetaxel. PLoS ONE 2013, 8, e57971. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.T.; Lin, Y.W.; Chiu, H.M.; Chiang, B.H. Curcumin Induces Apoptosis of Colorectal Cancer Stem Cells by Coupling with CD44 Marker. J. Agric. Food Chem. 2016, 64, 2247–2253. [Google Scholar] [CrossRef] [PubMed]
- Buhrmann, C.; Kraehe, P.; Lueders, C.; Shayan, P.; Goel, A.; Shakibaei, M. Curcumin suppresses crosstalk between colon cancer stem cells and stromal fibroblasts in the tumor microenvironment: Potential role of EMT. PLoS ONE 2014, 9, e107514. [Google Scholar] [CrossRef] [PubMed]
- Starok, M.; Preira, P.; Vayssade, M.; Haupt, K.; Salome, L.; Rossi, C. EGFR Inhibition by Curcumin in Cancer Cells: A Dual Mode of Action. Biomacromolecules 2015, 16, 1634–1642. [Google Scholar] [CrossRef] [PubMed]
- Jett, K.; Friedman, J.M. Clinical and genetic aspects of neurofibromatosis 1. Genet. Med. 2010, 12, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Lin, A.L.; Gutmann, D.H. Advances in the treatment of neurofibromatosis-associated tumours. Nat. Rev. Clin. Oncol. 2013, 10, 616–624. [Google Scholar] [CrossRef] [PubMed]
- De Souza, M.L.; Jansen, A.K.; Martins, A.S.; Rodrigues, L.O.; De Rezende, N.A. Nutrient intake in neurofibromatosis type 1: A cross-sectional study. Nutrition 2015, 31, 858–862. [Google Scholar] [CrossRef] [PubMed]
- Carotenuto, M.; Esposito, M. Nutraceuticals safety and efficacy in migraine without aura in a population of children affected by neurofibromatosis type I. Neurolog. Sci. 2013, 34, 1905–1909. [Google Scholar] [CrossRef] [PubMed]
- Esposito, T.; Piluso, G.; Saracino, D.; Uccello, R.; Schettino, C.; Dato, C.; Capaldo, G.; Giugliano, T.; Varriale, B.; Paolisso, G.; et al. A novel diagnostic method to detect truncated neurofibromin in neurofibromatosis 1. J. Neurochem. 2015, 135, 1123–1128. [Google Scholar] [CrossRef] [PubMed]
- Conforti, R.; Cirillo, M.; Marrone, V.; Galasso, R.; Capaldo, G.; Giugliano, T.; Scuotto, A.; Piluso, G.; Melone, M.A. Giant thrombosed intracavernous carotid artery aneurysm presenting as Tolosa-Hunt syndrome in a patient harboring a new pathogenic neurofibromatosis type 1 mutation: A case report and review of the literature. Neuropsychiatr. Dis. Treat. 2014, 10, 135–140. [Google Scholar] [CrossRef] [PubMed]
- Cuomo, J.; Appendino, G.; Dern, A.S.; Schneider, E.; Mckinnon, T.P.; Brown, M.J.; Togni, S.; Dixon, B.M. Comparative absorption of a standardized curcuminoid mixture and its lecithin formulation. J. Nat. Prod. 2011, 74, 664–669. [Google Scholar] [CrossRef] [PubMed]
- Burgos-Moron, E.; Calderon-Montano, J.M.; Salvador, J.; Robles, A.; Lopez-Lazaro, M. The dark side of curcumin. Int. J. Cancer 2010, 126, 1771–1775. [Google Scholar] [CrossRef] [PubMed]
- Heath, D.D.; Pruitt, M.A.; Brenner, D.E.; Rock, C.L. Curcumin in plasma and urine: Quantitation by high-performance liquid chromatography. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2003, 783, 287–295. [Google Scholar] [CrossRef]
- Lama, G.; Esposito Salsano, M.; Grassia, C.; Calabrese, E.; Grassia, M.G.; Bismuto, R.; Melone, M.A.; Russo, S.; Scuotto, A. Neurofibromatosis type 1 and optic pathway glioma. A long-term follow-up. Minerva Pediatr. 2007, 59, 13–21. [Google Scholar] [PubMed]
- D’arco, F.; D’amico, A.; Caranci, F.; Di Paolo, N.; Melis, D.; Brunetti, A. Cerebrovascular stenosis in neurofibromatosis type 1 and utility of magnetic resonance angiography: Our experience and literature review. Radiol. Med. 2014, 119, 415–421. [Google Scholar] [CrossRef] [PubMed]
- Perry, A.; Roth, K.A.; Banerjee, R.; Fuller, C.E.; Gutmann, D.H. NF1 deletions in S-100 protein-positive and negative cells of sporadic and neurofibromatosis 1 (NF1)-associated plexiform neurofibromas and malignant peripheral nerve sheath tumors. Am. J. Pathol. 2001, 159, 57–61. [Google Scholar] [CrossRef]
- Korf, B.R. The phakomatoses. Clin. Dermatol. 2005, 23, 78–84. [Google Scholar] [CrossRef] [PubMed]
- Wallace, M.R. Neurofibromatosis: Phenotype, Natural History, and Pathogenesis. Am. J. Hum. Genet. 2000, 67, 264. [Google Scholar]
- Easton, D.F.; Ponder, M.A.; Huson, S.M.; Ponder, B.A. An analysis of variation in expression of neurofibromatosis (NF) type 1 (NF1): Evidence for modifying genes. Am. J. Hum. Genet. 1993, 53, 305–313. [Google Scholar] [PubMed]
- Reuter, S.; Gupta, S.C.; Park, B.; Goel, A.; Aggarwal, B.B. Epigenetic changes induced by curcumin and other natural compounds. Genes Nutr. 2011, 6, 93–108. [Google Scholar] [CrossRef] [PubMed]
- Laycock-Van Spyk, S.; Thomas, N.; Cooper, D.N.; Upadhyaya, M. Neurofibromatosis type 1-associated tumours: Their somatic mutational spectrum and pathogenesis. Hum. Genom. 2011, 5, 623–690. [Google Scholar] [CrossRef]
- Perona, J.S.; Vogler, O.; Sanchez-Dominguez, J.M.; Montero, E.; Escriba, P.V.; Ruiz-Gutierrez, V. Consumption of virgin olive oil influences membrane lipid composition and regulates intracellular signaling in elderly adults with type 2 diabetes mellitus. J. Gerontol. A Biol. Sci. Med. Sci. 2007, 62, 256–263. [Google Scholar] [CrossRef] [PubMed]
- Muriana, F.J.; Vazquez, C.M.; Ruiz-Gutierrez, V. Fatty acid composition and properties of the liver microsomal membrane of rats fed diets enriched with cholesterol. J. Biochem. 1992, 112, 562–567. [Google Scholar] [CrossRef] [PubMed]
- Rahmani, A.H.; Albutti, A.S.; Aly, S.M. Therapeutics role of olive fruits/oil in the prevention of diseases via modulation of anti-oxidant, anti-tumour and genetic activity. Int. J. Clin. Exp. Med. 2014, 7, 799–808. [Google Scholar] [PubMed]
- Goldsmith, C.D.; Vuong, Q.V.; Sadeqzadeh, E.; Stathopoulos, C.E.; Roach, P.D.; Scarlett, C.J. Phytochemical properties and anti-proliferative activity of Olea europaea L. leaf extracts against pancreatic cancer cells. Molecules 2015, 20, 12992–13004. [Google Scholar] [CrossRef] [PubMed]
- Marchetti, C.; Clericuzio, M.; Borghesi, B.; Cornara, L.; Ribulla, S.; Gosetti, F.; Marengo, E.; Burlando, B. Oleuropein-Enriched Olive Leaf Extract Affects Calcium Dynamics and Impairs Viability of Malignant Mesothelioma Cells. Evid. Based Complem. Altern. Med. 2015, 2015, 908493. [Google Scholar] [CrossRef] [PubMed]
- Curic, S.; Wu, Y.; Shan, B.; Schaaf, C.; Utpadel, D.; Lange, M.; Kuhlen, D.; Perone, M.J.; Arzt, E.; Stalla, G.K.; et al. Curcumin acts anti-proliferative and pro-apoptotic in human meningiomas. J. Neurooncol. 2013, 113, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Scoditti, E.; Calabriso, N.; Massaro, M.; Pellegrino, M.; Storelli, C.; Martines, G.; De Caterina, R.; Carluccio, M.A. Mediterranean diet polyphenols reduce inflammatory angiogenesis through MMP-9 and COX-2 inhibition in human vascular endothelial cells: A potentially protective mechanism in atherosclerotic vascular disease and cancer. Arch. Biochem. Biophys. 2012, 527, 81–89. [Google Scholar] [CrossRef] [PubMed]
- Chimento, A.; Casaburi, I.; Rosano, C.; Avena, P.; De Luca, A.; Campana, C.; Martire, E.; Santolla, M.F.; Maggiolini, M.; Pezzi, V.; et al. Oleuropein and hydroxytyrosol activate GPER/ GPR30-dependent pathways leading to apoptosis of ER-negative SKBR3 breast cancer cells. Mol. Nutr. Food Res. 2014, 58, 478–489. [Google Scholar] [CrossRef] [PubMed]
- Aoki, H.; Takada, Y.; Kondo, S.; Sawaya, R.; Aggarwal, B.B.; Kondo, Y. Evidence that curcumin suppresses the growth of malignant gliomas in vitro and in vivo through induction of autophagy: Role of Akt and extracellular signal-regulated kinase signaling pathways. Mol. Pharmacol. 2007, 72, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Yan, C.M.; Chai, E.Q.; Cai, H.Y.; Miao, G.Y.; Ma, W. Oleuropein induces apoptosis via activation of caspases and suppression of phosphatidylinositol 3-kinase/protein kinase B pathway in HepG2 human hepatoma cell line. Mol. Med. Rep. 2015, 11, 4617–4624. [Google Scholar] [CrossRef] [PubMed]
- Yao, J.; Wu, J.; Yang, X.; Yang, J.; Zhang, Y.; Du, L. Oleuropein induced apoptosis in HeLa cells via a mitochondrial apoptotic cascade associated with activation of the c-Jun NH2-terminal kinase. J. Pharmacol. Sci. 2014, 125, 300–311. [Google Scholar] [CrossRef] [PubMed]
- Hassan, Z.K.; Elamin, M.H.; Omer, S.A.; Daghestani, M.H.; Al-Olayan, E.S.; Elobeid, M.A.; Virk, P. Oleuropein induces apoptosis via the p53 pathway in breast cancer cells. Asian Pac. J. Cancer Prev. 2014, 14, 6739–6742. [Google Scholar] [CrossRef] [PubMed]
- Monroe, C.L.; Dahiya, S.; Gutmann, D.H. Dissecting Clinical Heterogeneity in Neurofibromatosis Type 1. Annu. Rev. Pathol. 2017, 12, 53–74. [Google Scholar] [CrossRef] [PubMed]
- Kasi, P.D.; Tamilselvam, R.; Skalicka-Wozniak, K.; Nabavi, S.F.; Daglia, M.; Bishayee, A.; Pazoki-Toroudi, H.; Nabavi, S.M. Molecular targets of curcumin for cancer therapy: An updated review. Tumor Biol. 2016, 37, 13017–13028. [Google Scholar] [CrossRef] [PubMed]
- Cao, A.L.; Tang, Q.F.; Zhou, W.C.; Qiu, Y.Y.; Hu, S.J.; Yin, P.H. Ras/ERK signaling pathway is involved in curcumin-induced cell cycle arrest and apoptosis in human gastric carcinoma AGS cells. J. Asian Nat. Prod. Res. 2015, 17, 56–63. [Google Scholar] [CrossRef] [PubMed]
- Cagnol, S.; Chambard, J.C. ERK and cell death: Mechanisms of ERK-induced cell death—Apoptosis, autophagy and senescence. FEBS J. 2010, 277, 2–21. [Google Scholar] [CrossRef] [PubMed]
- Polivka, J., Jr.; Janku, F. Molecular targets for cancer therapy in the PI3K/AKT/mTOR pathway. Pharmacol. Ther. 2014, 142, 164–175. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.; Shen, G.; Khor, T.O.; Kim, J.H.; Kong, A.N. Curcumin inhibits Akt/mammalian target of rapamycin signaling through protein phosphatase-dependent mechanism. Mol. Cancer Ther. 2008, 7, 2609–2620. [Google Scholar] [CrossRef] [PubMed]
- Hasima, N.; Ozpolat, B. Regulation of autophagy by polyphenolic compounds as a potential therapeutic strategy for cancer. Cell Death Dis. 2014, 5, e1509. [Google Scholar] [CrossRef] [PubMed]
- Weir, N.M.; Selvendiran, K.; Kutala, V.K.; Tong, L.; Vishwanath, S.; Rajaram, M.; Tridandapani, S.; Anant, S.; Kuppusamy, P. Curcumin induces G2/M arrest and apoptosis in cisplatin-resistant human ovarian cancer cells by modulating Akt and p38 MAPK. Cancer Biol. Ther. 2007, 6, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Rainey, N.; Motte, L.; Aggarwal, B.B.; Petit, P.X. Curcumin hormesis mediates a cross-talk between autophagy and cell death. Cell Death Dis. 2015, 6, e2003. [Google Scholar] [CrossRef] [PubMed]
- Dai, X.; Zhang, J.; Arfuso, F.; Chinnathambi, A.; Zayed, M.E.; Alharbi, S.A.; Kumar, A.P.; Ahn, K.S.; Sethi, G. Targeting TNF-related apoptosis-inducing ligand (TRAIL) receptor by natural products as a potential therapeutic approach for cancer therapy. Exp. Biol. Med. (Maywood) 2015, 240, 760–773. [Google Scholar] [CrossRef] [PubMed]
- Reuss, D.E.; Mucha, J.; Hagenlocher, C.; Ehemann, V.; Kluwe, L.; Mautner, V.; Von Deimling, A. Sensitivity of malignant peripheral nerve sheath tumor cells to TRAIL is augmented by loss of NF1 through modulation of MYC/MAD and is potentiated by curcumin through induction of ROS. PLoS ONE 2013, 8, e57152. [Google Scholar] [CrossRef] [PubMed]
- Ling, B.C.; Wu, J.; Miller, S.J.; Monk, K.R.; Shamekh, R.; Rizvi, T.A.; Decourten-Myers, G.; Vogel, K.S.; Declue, J.E.; Ratner, N. Role for the epidermal growth factor receptor in neurofibromatosis-related peripheral nerve tumorigenesis. Cancer Cell 2005, 7, 65–75. [Google Scholar] [CrossRef] [PubMed]
- Conte, R.; Calarco, A.; Napoletano, A.; Valentino, A.; Margarucci, S.; Di Cristo, F.; Di Salle, A.; Peluso, G. Polyphenols Nanoencapsulation for Therapeutic Applications. J. Biomol. Res. Ther. 2016, 5. [Google Scholar] [CrossRef]

| Diet | Patient ID | Age | Sex | Familiar NF1 | Sporadic NF1 | Café-Au-Lait Spots Number > 6 | Cutaneous or Subcutaneous Neurofibromas | Freckling | Lisch Nodules | Plexiform Neurofibroma | Scoliosis | Optic Pathway Glioma | Molecular Testing | Short Stature | Pathological Findings on Brain MRI |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| WesDiet | 1 A.S. | 38 | M | yes | no | yes | yes | yes | yes | no | yes | yes | yes | no | T2-Weighted Hyperintensities (Ubo’s) |
| 2 A.F. | 22 | M | yes | no | yes | yes | yes | yes | yes | yes | yes | yes | no | T2-Weighted Hyperintensities (Ubo’s) | |
| MedDiet | 3 E.M. | 27 | M | yes | no | yes | yes | yes | yes | yes | no | no | yes | no | Fusiform aneurysms of both ICAs (ref) |
| 4 B.E. | 18 | M | no | yes | yes | yes | yes | yes | yes | yes | no | yes | yes | T2-Weighted Hyperintensities (Ubo’s) | |
| 5 D.M.M. | 22 | M | no | yes | yes | yes | yes | yes | no | yes | no | yes | no | No signs | |
| WesDietCurcumin | 6 A.M.C. | 41 | F | yes | no | yes | yes | yes | yes | no | yes | no | no | no | T2-Weighted Hyperintensities (Ubo’s); vascular malformations (hypoplastic mid-distal portion of basilar artery and intra-cranial vertebral artery; intracavernous right carotid aneurysm) |
| 7 A.N. | 59 | M | no | yes | yes | yes | yes | yes | yes | yes | no | no | no | No signs | |
| 8 A.F. | 44 | F | no | yes | yes | yes | yes | yes | no | no | no | no | no | T2-Weighted Hyperintensities (Ubo’s); hypoplasia of PCA | |
| MedDietCurcumin | 9 P.C. | 54 | M | no | yes | yes | yes | yes | yes | no | no | no | yes | no | No signs |
| 10 F.L. | 27 | F | no | yes | yes | yes | yes | yes | no | no | no | yes | no | No signs | |
| 11 R.S. | 50 | M | no | yes | yes | yes | yes | yes | yes | yes | no | yes | no | Multiple foci of T2 hyper intensity (vascular gliosis) |
| Diet | Patient ID | Age (Years) | Sex | Time | % Cell Mass | % Tot Water | % Extracell Water | % Intracell Water | % Fat | % FFM 1 | BMR 1 | BMI 1 | PA 1 | NA/K |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| WesDiet | 1 A.S. | Baseline | 52.3 | 54 | 49.7 | 50.3 | 26.7 | 73.3 | 1235 | 25 | 5.7 | 1.2 | ||
| 38 | M | 6 months | 51.8 | 53 | 53.2 | 46.8 | 27.2 | 72.8 | 1198 | 25.4 | 5.5 | 1.3 | ||
| 2 A.F. | Baseline | 49.7 | 46.8 | 56.2 | 43.8 | 32.7 | 63.7 | 1065 | 28 | 6 | 1.2 | |||
| 22 | M | 6 months | 48.2 | 44.6 | 55.8 | 44.2 | 35.6 | 64.4 | 998.6 | 28.5 | 5.8 | 1.2 | ||
| MedDiet | 3 E.M. | Baseline | 49.7 | 54 | 48.3 | 51.7 | 24.6 | 75.4 | 1324 | 26 | 5.5 | 1.2 | ||
| 27 | M | 6 months | 51.2 | 59.6 | 45.7 | 54.3 | 21.2 | 78.8 | 1435 | 23 | 6.1 | 0.9 | ||
| 4 B.E. | Baseline | 46.8 | 42.8 | 52 | 48 | 43.5 | 56.5 | 1129 | 36 | 4.8 | 1.3 | |||
| 18 | M | 6 months | 51.4 | 45.7 | 46 | 54 | 37.8 | 62.2 | 1326 | 30 | 5.8 | 1 | ||
| 5 D.M.M. | Baseline | 42.7 | 54.1 | 53.3 | 46.7 | 26.8 | 73.2 | 1223 | 27 | 5.9 | 1.1 | |||
| 22 | M | 6 months | 43.4 | 56.7 | 46.8 | 53.2 | 25 | 75 | 1276 | 26.7 | 6 | 1.1 | ||
| WesDietCurcumin | 6 A.M.C. | Baseline | 50.9 | 58 | 48 | 52 | 21.4 | 79.6 | 1345.2 | 25 | 5.7 | 1.1 | ||
| 41 | F | 6 months | 51.6 | 59 | 47.2 | 52.8 | 20.9 | 79.1 | 1365 | 24.9 | 5.6 | 1.2 | ||
| 7 A.N. | Baseline | 47 | 48.8 | 54 | 46 | 38.6 | 61.4 | 1237 | 32 | 4.9 | 1.2 | |||
| 59 | M | 6 months | 47.1 | 47.6 | 55 | 45 | 38 | 62 | 1195 | 31.7 | 4.8 | 1.1 | ||
| 8 A.F. | Baseline | 49.2 | 48.7 | 50 | 50 | 34.4 | 65.6 | 1356 | 30 | 5.3 | 0.9 | |||
| 44 | F | 6 months | 50 | 48.2 | 48.5 | 51.5 | 33.6 | 66.4 | 1376.2 | 29.7 | 5.4 | 1 | ||
| MedDietCurcumin | 9 P.C. | Baseline | 41.2 | 55.2 | 50.2 | 49.8 | 24.8 | 75.2 | 956.4 | 23 | 4.5 | 1.3 | ||
| 54 | F | 6 months | 51.5 | 59.3 | 48 | 52 | 19 | 81 | 1250.6 | 22 | 5.5 | 1.2 | ||
| 10 F.L. | Baseline | 49.1 | 45.4 | 49 | 51 | 38 | 62 | 1343.3 | 34 | 5.3 | 1 | |||
| 27 | F | 6 months | 57.1 | 48.3 | 45 | 55 | 34.1 | 65.9 | 1519.4 | 31 | 6.1 | 0.9 | ||
| 11 R.S. | Baseline | 50.2 | 59 | 47.2 | 52.8 | 19.4 | 80.6 | 1276.7 | 24 | 5.7 | 1.1 | |||
| 50 | M | 6 months | 52.2 | 64.4 | 47.6 | 52.4 | 12 | 88 | 1407.6 | 23 | 5.6 | 1.3 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Esposito, T.; Schettino, C.; Polverino, P.; Allocca, S.; Adelfi, L.; D’Amico, A.; Capaldo, G.; Varriale, B.; Di Salle, A.; Peluso, G.; et al. Synergistic Interplay between Curcumin and Polyphenol-Rich Foods in the Mediterranean Diet: Therapeutic Prospects for Neurofibromatosis 1 Patients. Nutrients 2017, 9, 783. https://doi.org/10.3390/nu9070783
Esposito T, Schettino C, Polverino P, Allocca S, Adelfi L, D’Amico A, Capaldo G, Varriale B, Di Salle A, Peluso G, et al. Synergistic Interplay between Curcumin and Polyphenol-Rich Foods in the Mediterranean Diet: Therapeutic Prospects for Neurofibromatosis 1 Patients. Nutrients. 2017; 9(7):783. https://doi.org/10.3390/nu9070783
Chicago/Turabian StyleEsposito, Teresa, Carla Schettino, Paola Polverino, Salvatore Allocca, Laura Adelfi, Alessandra D’Amico, Guglielmo Capaldo, Bruno Varriale, Anna Di Salle, Gianfranco Peluso, and et al. 2017. "Synergistic Interplay between Curcumin and Polyphenol-Rich Foods in the Mediterranean Diet: Therapeutic Prospects for Neurofibromatosis 1 Patients" Nutrients 9, no. 7: 783. https://doi.org/10.3390/nu9070783
APA StyleEsposito, T., Schettino, C., Polverino, P., Allocca, S., Adelfi, L., D’Amico, A., Capaldo, G., Varriale, B., Di Salle, A., Peluso, G., Sorrentino, G., Lus, G., Sampaolo, S., Di Iorio, G., & Melone, M. A. B. (2017). Synergistic Interplay between Curcumin and Polyphenol-Rich Foods in the Mediterranean Diet: Therapeutic Prospects for Neurofibromatosis 1 Patients. Nutrients, 9(7), 783. https://doi.org/10.3390/nu9070783







