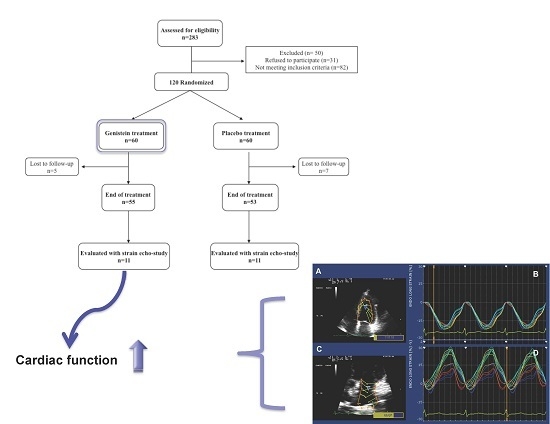
Genistein Supplementation and Cardiac Function in Postmenopausal Women with Metabolic Syndrome: Results from a Pilot Strain-Echo Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design and Setting
2.2. Randomization
2.3. Diet and Exercise
2.4. Electrocardiogram and Echocardiogram
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Clinical and Laboratory Results at Follow-Up
3.3. Cardiac Morphofunctional Indices
3.4. Adverse Events and Side-Effects
4. Discussion
Acknowledgments
Author Contributions
Conflict of Interest
References
- Giampaoli, S.; Stamler, J.; Donfrancesco, C.; Panico, S.; Vanuzzo, D.; Cesana, G.; Mancia, G.; Pilotto, L.; Mattiello, A.; Chiodini, P.; et al. The metabolic syndrome: A critical appraisal based on the cuore epidemiologic study. Prev. Med. 2009, 48, 525–531. [Google Scholar] [CrossRef] [PubMed]
- Janssen, I.; Powell, L.H.; Crawford, S.; Lasley, B.; Sutton-Tyrrell, K. Menopause and the metabolic syndrome: The study of women’s health across the nation. Arch. Intern. Med. 2008, 168, 1568–1575. [Google Scholar] [CrossRef] [PubMed]
- Xing, D.; Nozell, S.; Chen, Y.F.; Hage, F.; Oparil, S. Estrogen and mechanisms of vascular protection. Arterioscler. Thromb. Vasc. Biol. 2009, 29, 289–295. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.P.; Reckelhoff, J.F. Estrogen, hormonal replacement therapy and cardiovascular disease. Curr. Opin. Nephrol. Hypertens. 2011, 20, 133–138. [Google Scholar] [CrossRef] [PubMed]
- Caputi, A.P.; Arcoraci, V.; Benvenuti, C. Soy isoflavones, lactobacilli, vitamin d3 and calcium. Observational study in menopause. G. Ital. Ostet. Ginecol. 2006, 28, 212–221. [Google Scholar]
- Bonora, E.; Targher, G.; Formentini, G.; Calcaterra, F.; Lombardi, S.; Marini, F.; Zenari, L.; Saggiani, F.; Poli, M.; Perbellini, S.; et al. The metabolic syndrome is an independent predictor of cardiovascular disease in type 2 diabetic subjects. Prospective data from the verona diabetes complications study. Diabet. Med. J. Br. Diabet. Assoc. 2004, 21, 52–58. [Google Scholar] [CrossRef]
- Rexrode, K.M.; Manson, J.E.; Lee, I.M.; Ridker, P.M.; Sluss, P.M.; Cook, N.R.; Buring, J.E. Sex hormone levels and risk of cardiovascular events in postmenopausal women. Circulation 2003, 108, 1688–1693. [Google Scholar] [CrossRef] [PubMed]
- Ferrajolo, C.; Arcoraci, V.; Sullo, M.G.; Rafaniello, C.; Sportiello, L.; Ferrara, R.; Cannata, A.; Pagliaro, C.; Tari, M.G.; Caputi, A.P.; et al. Pattern of statin use in southern italian primary care: Can prescription databases be used for monitoring long-term adherence to the treatment? PLoS ONE 2014, 9, e102146. [Google Scholar] [CrossRef] [PubMed]
- Trifiro, G.; Alacqua, M.; Corrao, S.; Moretti, S.; Tari, D.U.; Galdo, M.; Caputi, A.P.; Arcoraci, V. Lipid-lowering drug use in italian primary care: Effects of reimbursement criteria revision. Eur. J. Clin. Pharmacol. 2008, 64, 619–625. [Google Scholar] [CrossRef] [PubMed]
- Trifiro, G.; Alacqua, M.; Corrao, S.; Tari, M.; Arcoraci, V. Statins for the primary prevention of cardiovascular events in elderly patients: A picture from clinical practice without strong evidence from clinical trials. J. Am. Geriatr. Soc. 2008, 56, 175–177. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, S.; Gustafsson, J.A. Estrogen receptors: Therapies targeted to receptor subtypes. Clin. Pharmacol. Ther. 2011, 89, 44–55. [Google Scholar] [CrossRef] [PubMed]
- Sbarouni, E.; Iliodromitis, E.K.; Zoga, A.; Vlachou, G.; Andreadou, I.; Kremastinos, D.T. The effect of the phytoestrogen genistein on myocardial protection, preconditioning and oxidative stress. Cardiovasc. Drugs Ther. Spons. Int. Soc. Cardiovasc. Pharmacother. 2006, 20, 253–258. [Google Scholar] [CrossRef] [PubMed]
- Taylor, H.S.; Manson, J.E. Update in hormone therapy use in menopause. J. Clin. Endocrinol. Metab. 2011, 96, 255–264. [Google Scholar] [CrossRef] [PubMed]
- Irace, C.; Marini, H.; Bitto, A.; Altavilla, D.; Polito, F.; Adamo, E.B.; Arcoraci, V.; Minutoli, L.; Di Benedetto, A.; Di Vieste, G.; et al. Genistein and endothelial function in postmenopausal women with metabolic syndrome. Eur. J. Clin. Investig. 2013, 43, 1025–1031. [Google Scholar] [CrossRef] [PubMed]
- Marini, H.; Bitto, A.; Altavilla, D.; Burnett, B.P.; Polito, F.; Di Stefano, V.; Minutoli, L.; Atteritano, M.; Levy, R.M.; Frisina, N.; et al. Efficacy of genistein aglycone on some cardiovascular risk factors and homocysteine levels: A follow-up study. Nutr. Metab. Cardiovasc. Dis. NMCD 2010, 20, 332–340. [Google Scholar] [CrossRef] [PubMed]
- Squadrito, F.; Marini, H.; Bitto, A.; Altavilla, D.; Polito, F.; Adamo, E.B.; D’Anna, R.; Arcoraci, V.; Burnett, B.P.; Minutoli, L.; et al. Genistein in the metabolic syndrome: Results of a randomized clinical trial. J. Clin. Endocrinol. Metab. 2013, 98, 3366–3374. [Google Scholar] [CrossRef] [PubMed]
- Arcoraci, V.; Atteritano, M.; Squadrito, F.; D’Anna, R.; Marini, H.; Santoro, D.; Minutoli, L.; Messina, S.; Altavilla, D.; Bitto, A. Antiosteoporotic activity of genistein aglycone in postmenopausal women: Evidence from a post-hoc analysis of a multicenter randomized controlled trial. Nutrients 2017, 9. [Google Scholar] [CrossRef] [PubMed]
- Bitto, A.; Granese, R.; Triolo, O.; Villari, D.; Maisano, D.; Giordano, D.; Altavilla, D.; Marini, H.; Adamo, E.B.; Nicotina, P.A.; et al. Genistein aglycone: A new therapeutic approach to reduce endometrial hyperplasia. Phytomedicine 2010, 17, 844–850. [Google Scholar] [CrossRef] [PubMed]
- Grundy, S.M.; Cleeman, J.I.; Daniels, S.R.; Donato, K.A.; Eckel, R.H.; Franklin, B.A.; Gordon, D.J.; Krauss, R.M.; Savage, P.J.; Smith, S.C., Jr.; et al. Diagnosis and management of the metabolic syndrome: An american heart association/national heart, lung, and blood institute scientific statement. Circulation 2005, 112, 2735–2752. [Google Scholar] [CrossRef] [PubMed]
- Task Force, M.; Ryden, L.; Grant, P.J.; Anker, S.D.; Berne, C.; Cosentino, F.; Danchin, N.; Deaton, C.; Escaned, J.; Hammes, H.P.; et al. Esc guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the easd: The task force on diabetes, pre-diabetes, and cardiovascular diseases of the european society of cardiology (esc) and developed in collaboration with the european association for the study of diabetes (easd). Eur. Heart J. 2013, 34, 3035–3087. [Google Scholar]
- Bitto, A.; Burnett, B.P.; Polito, F.; Russo, S.; D’Anna, R.; Pillai, L.; Squadrito, F.; Altavilla, D.; Levy, R.M. The steady-state serum concentration of genistein aglycone is affected by formulation: A bioequivalence study of bone products. Biomed. Res. Int. 2013, 2013, 273498. [Google Scholar] [CrossRef] [PubMed]
- Lang, R.M.; Bierig, M.; Devereux, R.B.; Flachskampf, F.A.; Foster, E.; Pellikka, P.A.; Picard, M.H.; Roman, M.J.; Seward, J.; Shanewise, J.; et al. Recommendations for chamber quantification. Eur. J. Echocardiogr. J. Work. Group Echocardiogr. Eur. Soc. Cardiol. 2006, 7, 79–108. [Google Scholar] [CrossRef] [PubMed]
- Mor-Avi, V.; Lang, R.M.; Badano, L.P.; Belohlavek, M.; Cardim, N.M.; Derumeaux, G.; Galderisi, M.; Marwick, T.; Nagueh, S.F.; Sengupta, P.P.; et al. Current and evolving echocardiographic techniques for the quantitative evaluation of cardiac mechanics: Ase/eae consensus statement on methodology and indications endorsed by the japanese society of echocardiography. Eur. J. Echocardiogr. J. Work. Group Echocardiogr. Eur. Soc. Cardiol. 2011, 12, 167–205. [Google Scholar] [CrossRef] [PubMed]
- Arcoraci, V.; Santoni, L.; Ferrara, R.; Furneri, G.; Cannata, A.; Sultana, J.; Moretti, S.; Di Luccio, A.; Tari, D.U.; Pagliaro, C.; et al. Effect of an educational program in primary care: The case of lipid control in cardio-cerebrovascular prevention. Int. J. Immunopathol. Pharmacol. 2014, 27, 351–363. [Google Scholar] [CrossRef] [PubMed]
- Corrao, S.; Arcoraci, V.; Arnone, S.; Calvo, L.; Scaglione, R.; Di Bernardo, C.; Lagalla, R.; Caputi, A.P.; Licata, G. Evidence-based knowledge management: An approach to effectively promote good health-care decision-making in the information era. Intern. Emerg. Med. 2009, 4, 99–106. [Google Scholar] [CrossRef] [PubMed]
- McCullough, A.J. Epidemiology of the metabolic syndrome in the USA. J. Dig. Dis. 2011, 12, 333–340. [Google Scholar] [CrossRef] [PubMed]
- Li, S.H.; Yang, B.; Gong, H.P.; Tan, H.W.; Zhong, M.; Zhang, Y.; Zhang, W. Impaired atrial synchronicity in patients with metabolic syndrome associated with insulin resistance and independent of hypertension. Hypertens. Res. Off. J. Jpn. Soc. Hypertens. 2009, 32, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Lin, K.J.; Cho, S.I.; Tiwari, N.; Bergman, M.; Kizer, J.R.; Palma, E.C.; Taub, C.C. Impact of metabolic syndrome on the risk of atrial fibrillation recurrence after catheter ablation: Systematic review and meta-analysis. J. Interv. Card. Electrophysiol. Int. J. Arrhythm. Pacing 2014, 39, 211–223. [Google Scholar] [CrossRef] [PubMed]
- Seo, J.M.; Park, T.H.; Lee, D.Y.; Cho, Y.R.; Baek, H.K.; Park, J.S.; Kim, M.H.; Kim, Y.D.; Choi, S.Y.; Lee, S.M.; et al. Subclinical myocardial dysfunction in metabolic syndrome patients without hypertension. J. Cardiovasc. Ultrasound 2011, 19, 134–139. [Google Scholar] [CrossRef] [PubMed]
- Gil-Campos, M.; Canete, R.R.; Gil, A. Adiponectin, the missing link in insulin resistance and obesity. Clin. Nutr. 2004, 23, 963–974. [Google Scholar] [CrossRef] [PubMed]
- Havel, P.J. Control of energy homeostasis and insulin action by adipocyte hormones: Leptin, acylation stimulating protein, and adiponectin. Curr. Opin. Lipidol. 2002, 13, 51–59. [Google Scholar] [CrossRef] [PubMed]
- Northcott, J.M.; Yeganeh, A.; Taylor, C.G.; Zahradka, P.; Wigle, J.T. Adipokines and the cardiovascular system: Mechanisms mediating health and disease. Can. J. Physiol. Pharmacol. 2012, 90, 1029–1059. [Google Scholar] [CrossRef] [PubMed]
- Rabe, K.; Lehrke, M.; Parhofer, K.G.; Broedl, U.C. Adipokines and insulin resistance. Mol. Med. 2008, 14, 741–751. [Google Scholar] [CrossRef] [PubMed]
- Diaz-Melean, C.M.; Somers, V.K.; Rodriguez-Escudero, J.P.; Singh, P.; Sochor, O.; Llano, E.M.; Lopez-Jimenez, F. Mechanisms of adverse cardiometabolic consequences of obesity. Curr. Atheroscler. Rep. 2013, 15, 364. [Google Scholar] [CrossRef] [PubMed]
- Ouchi, N.; Walsh, K. Cardiovascular and metabolic regulation by the adiponectin/c1q/tumor necrosis factor-related protein family of proteins. Circulation 2012, 125, 3066–3068. [Google Scholar] [CrossRef] [PubMed]
- Bitto, A.; Arcoraci, V.; Alibrandi, A.; D’Anna, R.; Corrado, F.; Atteritano, M.; Minutoli, L.; Altavilla, D.; Squadrito, F. Visfatin correlates with hot flashes in postmenopausal women with metabolic syndrome: Effects of genistein. Endocrine 2017, 55, 899–906. [Google Scholar] [CrossRef] [PubMed]
- Grzywocz, P.; Mizia-Stec, K.; Wybraniec, M.; Chudek, J. Adipokines and endothelial dysfunction in acute myocardial infarction and the risk of recurrent cardiovascular events. J. Cardiovasc. Med. 2015, 16, 37–44. [Google Scholar]
- Romacho, T.; Sanchez-Ferrer, C.F.; Peiro, C. Visfatin/nampt: An adipokine with cardiovascular impact. Med. Inflamm. 2013, 2013, 946427. [Google Scholar] [CrossRef] [PubMed]
- Straburzynska-Migaj, E.; Pilaczynska-Szczesniak, L.; Nowak, A.; Straburzynska-Lupa, A.; Sliwicka, E.; Grajek, S. Serum concentration of visfatin is decreased in patients with chronic heart failure. Acta Biochim. Pol. 2012, 59, 339–343. [Google Scholar] [PubMed]
- Mattu, H.S.; Randeva, H.S. Role of adipokines in cardiovascular disease. J. Endocrinol. 2013, 216, T17–T36. [Google Scholar] [CrossRef] [PubMed]
- Bugyei-Twum, A.; Advani, A.; Advani, S.L.; Zhang, Y.; Thai, K.; Kelly, D.J.; Connelly, K.A. High glucose induces smad activation via the transcriptional coregulator p300 and contributes to cardiac fibrosis and hypertrophy. Cardiovasc. Diabetol. 2014, 13, 89. [Google Scholar] [CrossRef] [PubMed]
- Hintz, K.K.; Ren, J. Phytoestrogenic isoflavones daidzein and genistein reduce glucose-toxicity-induced cardiac contractile dysfunction in ventricular myocytes. Endocr. Res. 2004, 30, 215–223. [Google Scholar] [CrossRef] [PubMed]
- Abraham, J.M.; Cho, L. The homocysteine hypothesis: Still relevant to the prevention and treatment of cardiovascular disease? Clevel. Clin. J. Med. 2010, 77, 911–918. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Genistein | Controls | ||||
|---|---|---|---|---|---|---|
| Basal Median (IQ) | 12 Month Median (IQ) | # p Value | Basal Median (IQ) | 12 Month Median (IQ) | # p Value | |
| Body mass index (kg/m2) | 30.3 (5.0) | 31.5 (7.0) | 0.167 | 30.4 (11.2) | 29.9 (10.8) | 0.593 |
| Waist circumference (cm) | 105.0 (16.0) | 104.0 (25.0) | 0.798 | 99.0 (19.0) | 98.0 (17.0) | 0.438 |
| Systolic blood pressure (mm Hg) | 130.0 (38.0) | 120.0 (40.0) | 0.075 | 130.0 (30.0) | 130.0 (20.0) | 0.320 |
| Diastolic blood pressure (mm Hg) | 80.0 (15.0) | 70.0 (30.0) | 0.085 | 80.0 (10.0) | 80.0 (0.0) | 0.496 |
| Fasting glucose (mmol/L) | 7.1 (2.7) | 7.0 (0.9) | 0.099 | 7.8 (2.2) | 6.5 (4.3) | 0.959 |
| Total cholesterol (mmol/L) | 4.9 (1.4) | 4.2 (0.7) | 0.003 | 4.9 (1.1) | 4.4 (1.1) | 0.051 |
| LDL-cholesterol (mmol/L) | 2.9 (1.1) | 1.6 (0.8) | 0.009 | 2.8 (1.3) | 2.5 (0.6) | 0.120 |
| HDL-cholesterol (mmol/L) | 1.3 (0.7) | 1.5 (0.6) | 0.093 | 1.3 (0.4) | 1.4 (0.6) | 0.798 |
| Triglycerides (mmol/L) | 1.5 (0.9) | 1.2 (0.8) | 0.008 | 1.4 (0.8) | 1.2 (0.7) | 0.075 |
| Insulin levels (nUI/L) | 9.7 (7.8) | 8.5 (5.3) | 0.050 | 12.2 (12.3) | 13.4 (17.9) | 0.477 |
| HOMA-IR | 3.4 (1.5) | 3.0 (1.7) | 0.010 | 3.7 (4.8) | 4.7 (5.2) | 0.110 |
| Visfatin (ng/mL) | 3.1 (2.0) | 1.3 (0.7) | 0.016 | 2.1 (2.2) | 2.4 (1.3) | 0.477 |
| Adiponectin (μg/mL) | 6.2 (1.1) | 8.0 (5.9) | 0.003 | 5.3 (2.6) | 6.2 (2.6) | 0.021 |
| Homocysteine (μmol/L) | 13.3 (15.3) | 10.0 (2.2) | 0.003 | 17.5 (10.8) | 14.2 (7.7) | 0.091 |
| Left Ventricle | ||||||
| End-diastolic diameter (mm) | 47.4 (9.2) | 46.2 (8.2) | 0.929 | 45.8 (7.7) | 44.2 (5.1) | 0.859 |
| BSA-index mass (g/m2) | 82.9 (33.7) | 73.0 (27.8) | 0.657 | 78.6 (15.3) | 84.7 (19.9) | 1.000 |
| Height-indexed mass (g/m2.7) | 38.0 (27.7) | 44.6 (16.9) | 0.328 | 41.1 (7.9) | 39.2 (11.6) | 0.859 |
| End-diastolic volume (mL) | 67.0 (14.9) | 65.0 (26.0) | 0.533 | 72.0 (23.0) | 70.0 (28.0) | 0.894 |
| BSA-index end-diastolic vol. (mL/m2) | 40.3 (13.9) | 37.9 (10.5) | 0.328 | 37.2 (10.9) | 39.2 (15.1) | 0.790 |
| End-diastolic shape | 0.6 (0.09) | 0.6 (0.1) | 0.241 | 0.6 (0.08) | 0.6 (0.1) | 0.859 |
| Ejection fraction | 0.6 (0.04) | 0.7 (0.05) | 0.009 | 0.7 (0.11) | 0.7 (0.10) | 0.790 |
| MAPSE (mm) | 15.8 (4.1) | 16.5 (1.3) | 0.182 | 16.3 (4.8) | 16.0 (4.9) | 0.790 |
| TDV Septal S’-wave (cm/s) | 10.0 (3.0) | 10.0 (2.0) | 0.764 | 8.0 (4.0) | 8.0 (3.0) | 0.258 |
| TDV Lateral S’-wave (cm/s) | 10.0 (1.0) | 12.0 (2.0) | 0.022 | 10.0 (2.0) | 11.0 (3.0) | 0.305 |
| Left Ventricular Diastolic Indices | ||||||
| Mitral E/A velocity ratio | 1.0 (0.23) | 0.8 (0.33) | 0.449 | 0.8 (0.44) | 0.9 (0.28) | 0.965 |
| Mitral E-wave DT (ms) | 204.0 (16.0) | 216.0 (13.0) | 0.075 | 223.0 (24.0) | 242.0 (27.0) | 0.059 |
| E/E’ velocity ratio | 6.8 (1.0) | 7.5 (2.6) | 0.533 | 7.2 (3.5) | 7.8 (3.3) | 0.859 |
| Left Ventricular Global Strain Measurements | ||||||
| Radial Strain (%) | 32.0 (10.9) | 30.0 (15.0) | 0.789 | 36.0 (9.5) | 27.9 (12.3) | 0.110 |
| Circumferential Strain (%) | −21.0 (7.7) | −22.5 (4.9) | 1.000 | −23.5 (9.2) | −25.3 (5.0) | 0.594 |
| Longitudinal Strain (%) | −17.5 (1.5) | −17.3 (1.6) | 0.328 | −15.8 (4.7) | −18.8 (4.9) | 0.213 |
| Left Atrium | ||||||
| BSA-indexed ES volume (mL/m2) | 29.5 (4.2) | 22.6 (11.0) | 0.041 | 32.3 (10.2) | 27.5 (7.2) | 0.248 |
| Fractional area change (%) | 37.0 (6.0) | 41.0 (6.0) | 0.035 | 35.0 (2.0) | 35.0 (5.0) | 0.510 |
| PALS (%) | 25.5 (5.8) | 31.0 (8.5) | 0.021 | 23.6 (10.2) | 24.0 (6.5) | 0.929 |
| Parameters | Percentage Changes from Baseline after 12 Months Treatment | ||
|---|---|---|---|
| Genistein Median (IQ) | Controls Median (IQ) | # p Value | |
| Body mass index (kg/m2) | 1.6 (5.7) | 0.9 (4.5) | 0.171 |
| Waist circumference (cm) | 0.0 (4.9) | 0.0 (4.4) | 0.898 |
| Systolic blood pressure (mm Hg) | 0.0 (11.8) | 0.0 (12.2) | 0.076 |
| Diastolic blood pressure (mm Hg) | −8.3 (12.5) | 0.0 (6.7) | 0.057 |
| Fasting glucose (mmol/L) | −7.1 (23.5) | −0.9 (18.3) | 0.332 |
| Total cholesterol (mmol/L) | −12.4 (14.9) | −15.5 (23.3) | 0.748 |
| LDL-cholesterol (mmol/L) | −18.1 (45.1) | −16.8 (43.2) | 0.270 |
| HDL-cholesterol (mmol/L) | 16.3 (27.6) | −2.1 (15.6) | 0.243 |
| Triglycerides (mmol/L) | −12.5 (13.8) | −21.5 (56.6) | 0.898 |
| Insulin levels (nUI/L) | −21.5 (27.9) | 1.7 (81.0) | 0.193 |
| HOMA-IR | −19.7 (39.0) | 18.0 (71.2) | 0.007 |
| Visfatin (ng/mL) | −50.9 (73.2) | −7.0 (32.2) | 0.016 |
| Adiponectin (μg/mL) | 29.4 (62.8) | 12.6 (38.6) | 0.088 |
| Homocysteine (μmol/L) | −24.3 (34.4) | −8.1 (50.1) | 0.034 |
| Left Ventricle | |||
| End-diastolic diameter (mm) | 3.2 (14.7) | 0.2 (26.5) | 0.949 |
| BSA-index mass (g/m2) | 2.9 (30.4) | 10.5 (41.6) | 0.748 |
| Height-indexed mass (g/m2.7) | 16.3 (22.2) | −5.4 (45.1) | 0.519 |
| End-diastolic volume (mL) | −1.3 (45.5) | −7.8 (67.8) | 0.898 |
| BSA-index end-diastolic vol. (mL/m2) | −0.4 (49.1) | 7.0 (48.5) | 1.000 |
| End-diastolic shape | 3.2 (5.8) | −1.6 (7.6) | 0.606 |
| Ejection fraction | 20.3 (12.5) | −1.7 (24.8) | 0.040 |
| MAPSE (mm) | 4.4 (38.0) | 0.6 (26.4) | 0.606 |
| TDV Septal S’-wave (cm/s) | 0.0 (26.5) | −12.5 (48.1) | 0.332 |
| TDV Lateral S’-wave (cm/s) | 10.0 (9.1) | 9.1 (31.3) | 0.606 |
| Left Ventricular Diastolic Indices | |||
| Mitral E/A velocity ratio | −9.8 (34.8) | 6.0 (56.8) | 0.652 |
| Mitral E-wave DT (ms) | 10.0 (12.4) | 6.0 (11.9) | 0.748 |
| E/E’ velocity ratio | 6.4 (72.6) | 3.9 (49.9) | 0.748 |
| Left Ventricular Global Strain Measurements | |||
| Radial Strain (%) | 12.6 (44.3) | −13.4 (35.1) | 0.133 |
| Circumferential Strain (%) | 0.9 (30.9) | 3.7 (38.9) | 0.797 |
| Longitudinal Strain (%) | −2.8 (11.3) | 4.3 (24.9) | 0.243 |
| Left Atrium | |||
| BSA-indexed ES volume (mL/m2) | −22.6 (47.7) | −20.8 (61.1) | 0.151 |
| Fractional area change (%) | 11.1 (22.6) | 2.8 (9.5) | 0.034 |
| PALS (%) | 13.3 (25.4) | −11.2 (51.3) | 0.270 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Gregorio, C.; Marini, H.; Alibrandi, A.; Di Benedetto, A.; Bitto, A.; Adamo, E.B.; Altavilla, D.; Irace, C.; Di Vieste, G.; Pancaldo, D.; et al. Genistein Supplementation and Cardiac Function in Postmenopausal Women with Metabolic Syndrome: Results from a Pilot Strain-Echo Study. Nutrients 2017, 9, 584. https://doi.org/10.3390/nu9060584
De Gregorio C, Marini H, Alibrandi A, Di Benedetto A, Bitto A, Adamo EB, Altavilla D, Irace C, Di Vieste G, Pancaldo D, et al. Genistein Supplementation and Cardiac Function in Postmenopausal Women with Metabolic Syndrome: Results from a Pilot Strain-Echo Study. Nutrients. 2017; 9(6):584. https://doi.org/10.3390/nu9060584
Chicago/Turabian StyleDe Gregorio, Cesare, Herbert Marini, Angela Alibrandi, Antonino Di Benedetto, Alessandra Bitto, Elena Bianca Adamo, Domenica Altavilla, Concetta Irace, Giacoma Di Vieste, Diego Pancaldo, and et al. 2017. "Genistein Supplementation and Cardiac Function in Postmenopausal Women with Metabolic Syndrome: Results from a Pilot Strain-Echo Study" Nutrients 9, no. 6: 584. https://doi.org/10.3390/nu9060584
APA StyleDe Gregorio, C., Marini, H., Alibrandi, A., Di Benedetto, A., Bitto, A., Adamo, E. B., Altavilla, D., Irace, C., Di Vieste, G., Pancaldo, D., Granese, R., Atteritano, M., Corrao, S., Licata, G., Squadrito, F., & Arcoraci, V. (2017). Genistein Supplementation and Cardiac Function in Postmenopausal Women with Metabolic Syndrome: Results from a Pilot Strain-Echo Study. Nutrients, 9(6), 584. https://doi.org/10.3390/nu9060584