Does the Dietary Pattern of Shanghai Residents Change across Seasons and Area of Residence: Assessing Dietary Quality Using the Chinese Diet Balance Index (DBI)
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Dietary Data Collection
2.3. Dietary Balance Index-07
2.4. Assessment of Other Variables
2.5. Statistical Analysis
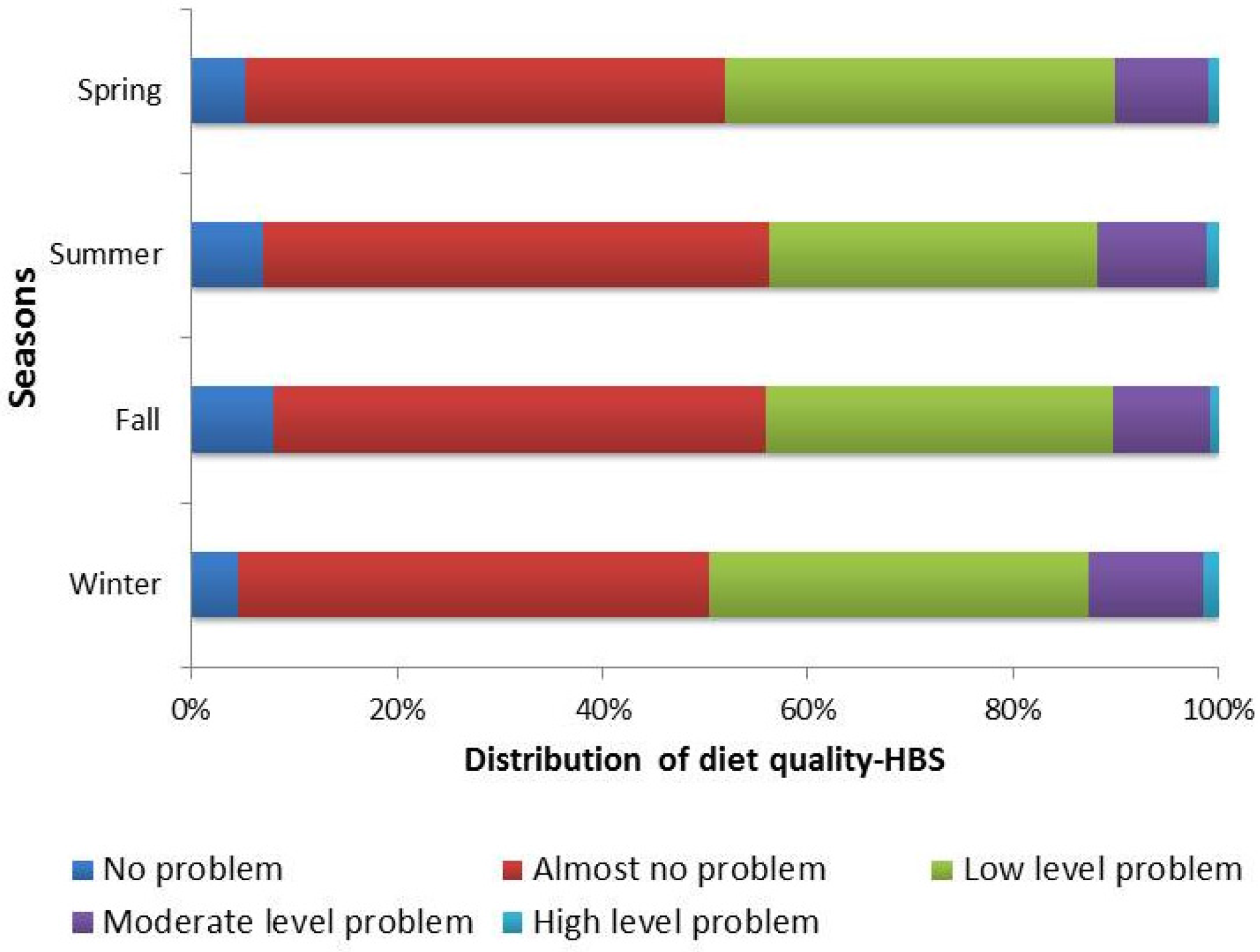
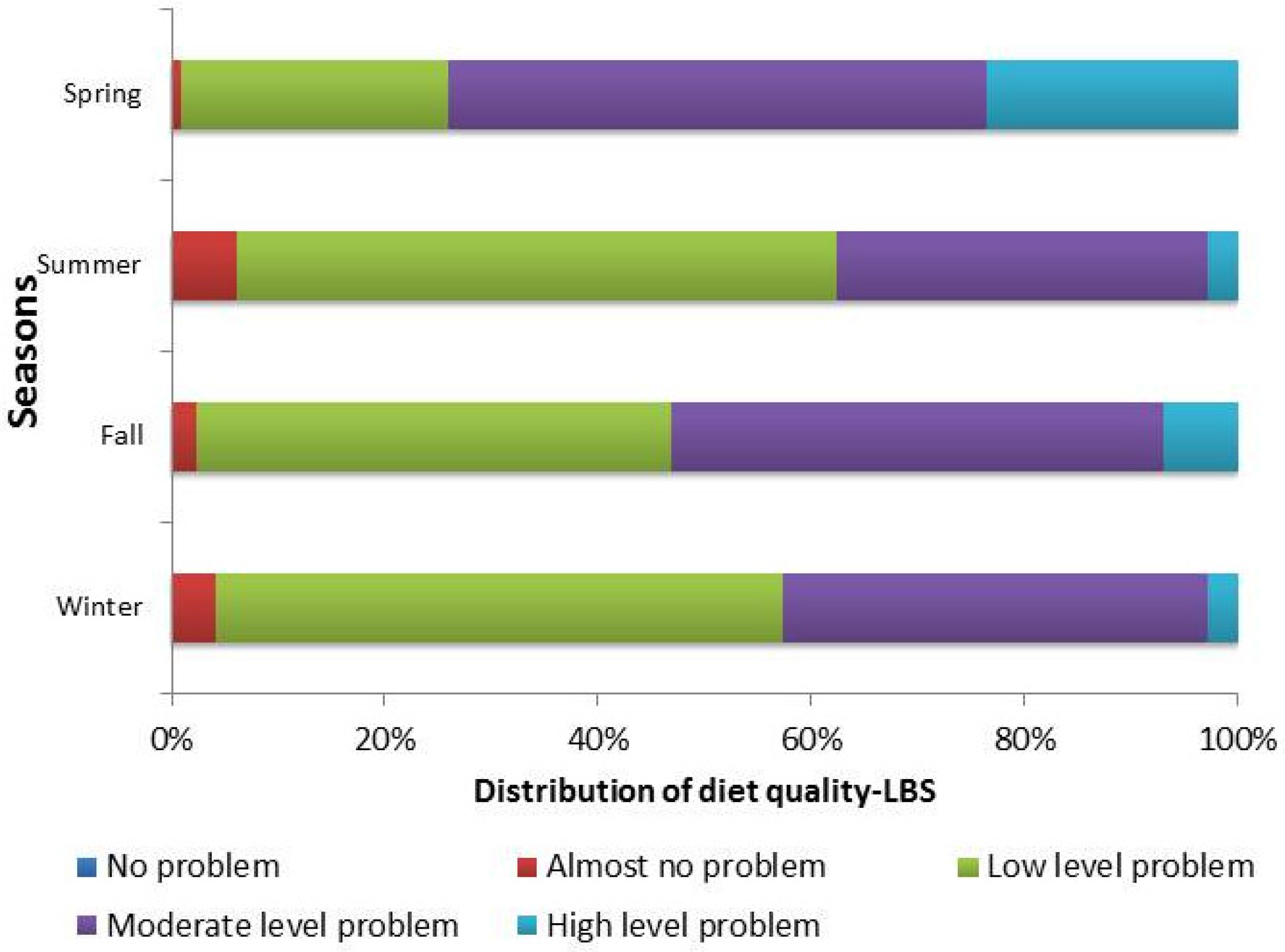
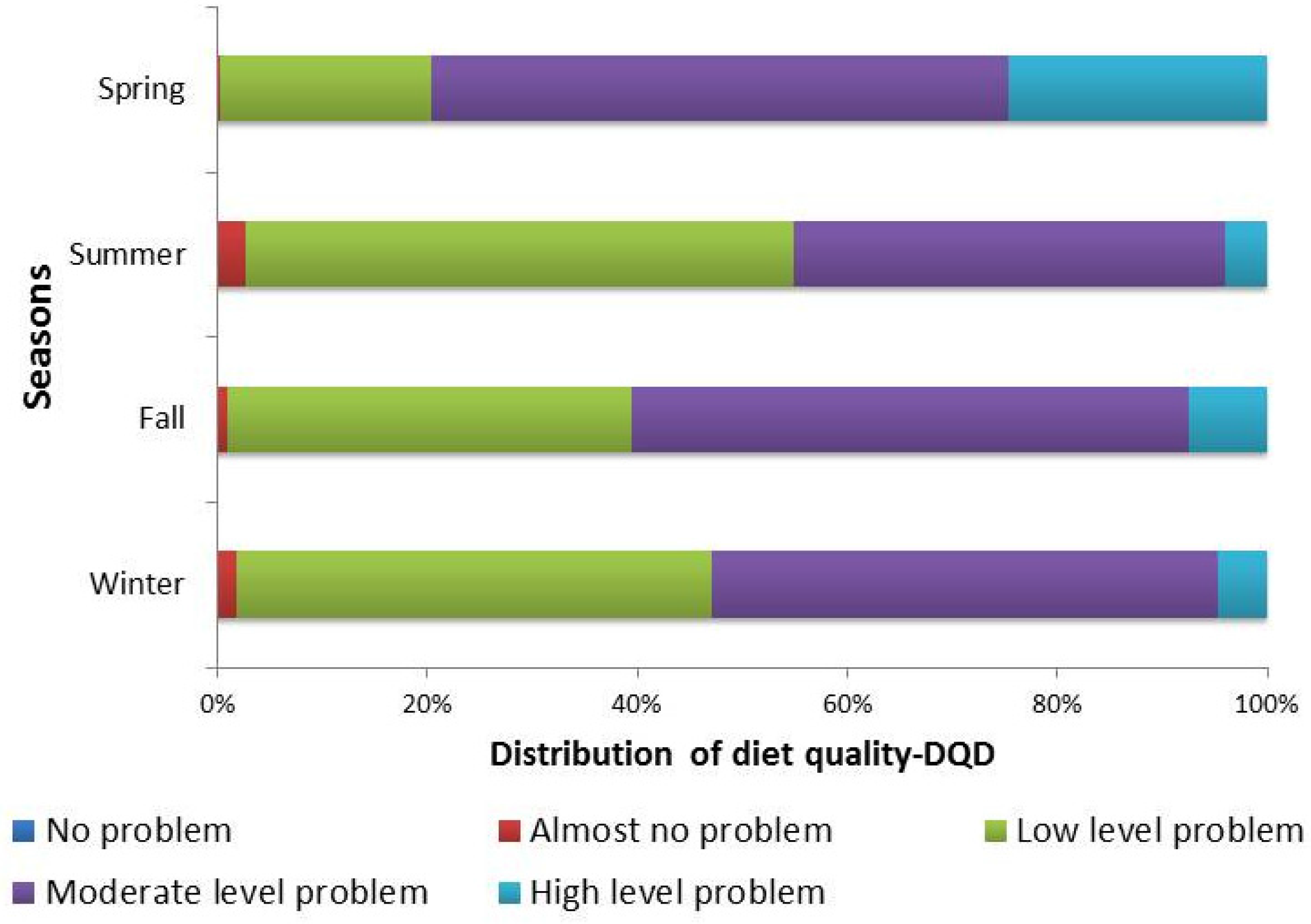
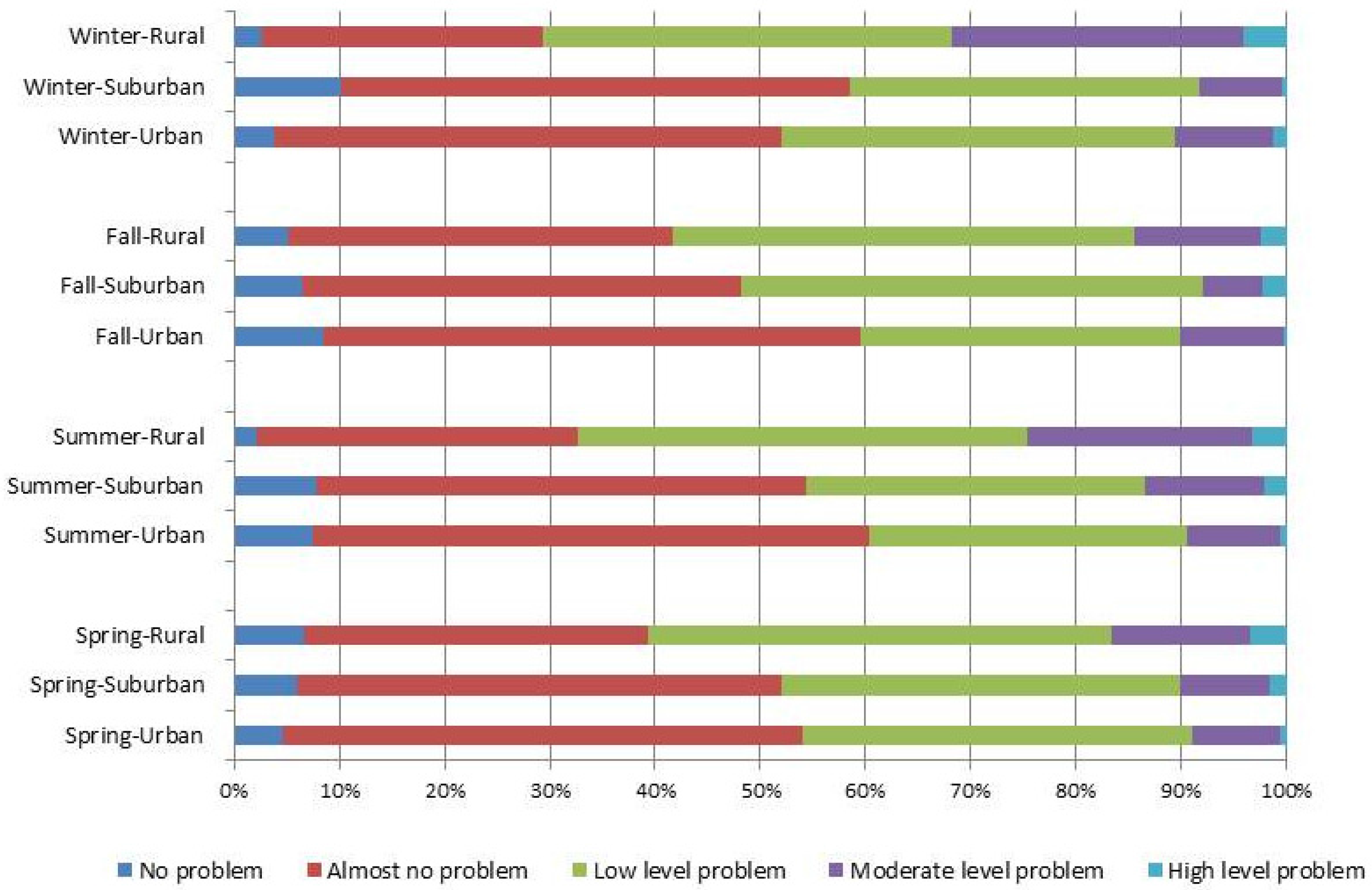
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization. Diet, Nutrition and the Prevention of Chronic Diseases: Report of the Joint WHO/FAO Expert Consultation. WHO, 2014. Available online: http://www.who.int/dietphysicalactivity/publications/trs916/summary/en/ (accessed on 21 September 2016).
- Brownie, S. Why are elderly individuals at risk of nutritional deficiency? Int. J. Nurs. Pract. 2005, 12, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Maynard, M.; Gunnell, D.; Ness, A.R.; Abraham, L.B.C.; Blane, D. What influences diet in early old age? Prospective and cross-sectional analyses of the Boyd Orr cohort. Eur. J. Public Health 2005, 16, 315–323. [Google Scholar] [CrossRef] [PubMed]
- Guenther, P.M.; Casavale, K.O.; Reedy, J.; Kirkpatrick, S.I.; Hiza, H.A.; Kuczynski, K.J.; Kahle, L.L.; Krebs-Smith, S.M. Update of the Healthy Eating Index: HEI-2010. J. Acad. Nutr. Diet. 2013, 113, 569–580. [Google Scholar] [CrossRef] [PubMed]
- Guenther, P.M.; Kirkpatrick, S.I.; Reedy, J.; Krebs-Smith, S.M.; Buckman, D.W.; Dodd, K.W.; Casavale, K.O.; Carroll, R.J. The Healthy Eating Index-2010 is a valid and reliable measure of diet quality according to the 2010 Dietary Guidelines for Americans. J. Nutr. 2014, 144, 399–407. [Google Scholar] [CrossRef] [PubMed]
- McCullough, M.L.; Willett, W.C. Evaluating adherence to recommended diets in adults: The Alternate Healthy Eating Index. Public Health Nutr. 2006, 9, 152–157. [Google Scholar] [CrossRef] [PubMed]
- Sotos-Prieto, M.; Luben, R.; Khaw, K.T.; Wareham, N.J.; Forouhi, N.G. The association between Mediterranean Diet Score and glucokinase regulatory protein gene variation on the markers of cardiometabolic risk: An analysis in the European Prospective Investigation into Cancer (EPIC)-Norfolk study. Br. J. Nutr. 2014, 112, 122–131. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Farioli, A.; Korre, M.; Kales, S.N. Modified Mediterranean diet score and cardiovascular risk in a North American working population. PLoS ONE 2014, 9, e87539. [Google Scholar] [CrossRef] [PubMed]
- Esposito, K.; Maiorino, M.I.; di Palo, C.; Giugliano, D.; Campanian Postprandial Hyperglycemia Study Group. Adherence to a Mediterranean diet and glycaemic control in Type 2 diabetes mellitus. Diabet. Med. 2009, 26, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Chiuve, S.E.; Fung, T.T.; Rimm, E.B.; Hu, F.B.; McCullough, M.L.; Wang, M.; Stampfer, M.J.; Willett, W.C. Alternative dietary indices both strongly predict risk of chronic disease. J. Nutr. 2012, 142, 1009–1018. [Google Scholar] [CrossRef] [PubMed]
- Fransen, H.P.; Ocke, M.C. Indices of diet quality. Curr. Opin. Clin. Nutr. Metab. Care 2008, 11, 559–565. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Kant, A.K. Dietary patterns and health outcomes. J. Am. Diet. Assoc. 2004, 104, 615–635. [Google Scholar] [CrossRef] [PubMed]
- Stookey, J.D.; Wang, Y.; Ge, K.; Lin, H.; Popkin, B.M. Measuring diet quality in china: The INFH-UNC-CH diet quality index. Eur. J. Clin. Nutr. 2000, 54, 811–821. [Google Scholar] [CrossRef] [PubMed]
- He, Y.; Zhai, F.; Yang, X.; Ge, K. The Chinese Diet Balance Index Revised. Acta Nutr. Sin. 2009, 31, 532–536. [Google Scholar]
- Capita, R.; Alonso-Calleja, C. Differences in reported winter and summer dietary intakes in young adults in Spain. Int. J. Food Sci. Nutr. 2005, 56, 431–443. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Olendzki, B.C.; Li, W.; Hafner, A.R.; Chiriboga, D.; Hebert, J.R.; Campbell, M.; Sarnie, M.; Ockene, I.S. Seasonal variation in food intake, physical activity, and body weight in a predominantly overweight population. Eur. J. Clin. Nutr. 2006, 60, 519–528. [Google Scholar] [CrossRef] [PubMed]
- Rossato, S.L.; Olinto, M.T.; Henn, R.L.; Anjos, L.A.; Bressan, A.W.; Wahrlich, V. Seasonal effect on nutrient intake in adults living in Southern Brazil. Cad. Saude Publica 2010, 26, 2177–2187. [Google Scholar] [CrossRef] [PubMed]
- Shahar, D.R.; Froom, P.; Harari, G.; Yerushalmi, N.; Lubin, F.; Kristal-Boneh, E. Changes in dietary intake account for seasonal changes in cardiovascular disease risk factors. Eur. J. Clin. Nutr. 1999, 53, 395–400. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; He, M.; Pan, X. China Food Composition Table; China Institute of Nutrition and Food Safety, China CDC Press: Beijing, China, 2002. [Google Scholar]
- Cui, Z.; Dibley, M.J. Trends in dietary energy, fat, carbohydrate and protein intake in Chinese children and adolescents from 1991 to 2009. Br. J. Nutr. 2012, 108, 1292–1299. [Google Scholar] [CrossRef] [PubMed]
- Shi, Z.; Luscombe-Marsh, N.D.; Wittert, G.A.; Yuan, B.; Dai, Y.; Pan, X.; Taylor, A.W. Monosodium glutamate is not associated with obesity or a greater prevalence of weight gain over 5 years: Findings from the Jiangsu Nutrition Study of Chinese adults. Br. J. Nutr. 2010, 104, 457–463. [Google Scholar] [CrossRef] [PubMed]
- He, Y.N.; Zhai, F.Y.; Ge, K.Y. Measuring diet quality of Chinese 18–59 years adult using chinese Diet Balance Index. Wei Sheng Yan Jiu 2005, 34, 442–444. (In Chinese) [Google Scholar] [PubMed]
- Meng, L.; Liu, J.; Zhang, J.; Wang, C.; Man, Q.; Li, L. Effect of dietary factors on anaemia among rural elderly women in south-west China: A case-control study. Public Health Nutr. 2009, 12, 1540–1547. [Google Scholar] [CrossRef] [PubMed]
- Zhou, B.F.; Cooperative Meta-Analysis Group of the Working Group on Obesity in China. Predictive values of body mass index and waist circumference for risk factors of certain related diseases in Chinese adults—Study on optimal cut-off points of body mass index and waist circumference in Chinese adults. Biomed. Environ. Sci. 2002, 15, 83–96. [Google Scholar] [PubMed]
- Du, S.F.; Wang, H.J.; Zhang, B.; Zhai, F.Y.; Popkin, B.M. China in the period of transition from scarcity and extensive undernutrition to emerging nutrition-related non-communicable diseases, 1949–1992. Obes. Rev. 2014, 15 (Suppl. 1), 8–15. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Lu, Y.; Zang, J.; Wang, Z.; Zhou, J.; Zhu, Z.; Zou, S. The Trend in Dietary Structure and Nutrition Transition among Residents in Shanghai, from 1982 to 2012. J. Environ. Occup. Med. 2016, 33, 845–848. [Google Scholar]
- Xu, X.; Hall, J.; Byles, J.; Shi, Z. Assessing dietary quality of older Chinese people using the Chinese Diet Balance Index (DBI). PLoS ONE 2015, 10, e0121618. [Google Scholar] [CrossRef] [PubMed]
- Ponce, X.; Rodriguez-Ramirez, S.; Mundo-Rosas, V.; Shamah, T.; Barquera, S.; Gonzalez de Cossio, T. Dietary quality indices vary with sociodemographic variables and anthropometric status among Mexican adults: A cross-sectional study. Results from the 2006 National Health and Nutrition Survey. Public Health Nutr. 2014, 17, 1717–1728. [Google Scholar] [CrossRef] [PubMed]
- Van der Horst, K.; Brunner, T.A.; Siegrist, M. Fast food and take-away food consumption are associated with different lifestyle characteristics. J. Hum. Nutr. Diet. 2011, 24, 596–602. [Google Scholar] [CrossRef] [PubMed]
- Chinese Society of Nutrition. Chinese Dietary Guidelines; People’s Medical Publishing House: Beijing, China, 2016. [Google Scholar]
- Chang, J.; Wang, Y. Chinese Nutrtion and Health Surveillance 2010–2013; Peking University Health Science Center Press: Beijing, China, 2016. [Google Scholar]
- Van Staveren, W.A.; Deurenberg, P.; Burema, J.; De Groot, L.C.; Hautvast, J.G. Seasonal variation in food intake, pattern of physical activity and change in body weight in a group of young adult Dutch women consuming self-selected diets. Int. J. Obes. 1986, 10, 133–145. [Google Scholar] [PubMed]
- Prasad, M.; Lumia, M.; Erkkola, M.; Tapanainen, H.; Kronberg-Kippila, C.; Tuokkola, J.; Uusitalo, U.; Simell, O.; Veijola, R.; Knip, M.; et al. Diet composition of pregnant Finnish women: Changes over time and across seasons. Public Health Nutr. 2010, 13, 939–946. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, S.; Zambell, K.; Amar, M.J.; Arango, C.; Kelley, R.C.; Miszewski, S.G.; Tryon, S.; Courville, A.B. Dietary Intake Patterns Are Consistent Across Seasons in a Cohort of Healthy Adults in a Metropolitan Population. J. Acad. Nutr. Diet. 2016, 116, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Vandenplas, Y. Lactose intolerance. Asia Pac. J. Clin. Nutr. 2015, 24 (Suppl. 1), S9–S13. [Google Scholar] [PubMed]
- Wang, Y.; Li, S. Worldwide trends in dairy production and consumption and calcium intake: Is promoting consumption of dairy products a sustainable solution for inadequate calcium intake? Food Nutr. Bull. 2008, 29, 172–185. [Google Scholar] [CrossRef] [PubMed]
- Astrup, A.; Dyerberg, J.; Selleck, M.; Stender, S. Nutrition transition and its relationship to the development of obesity and related chronic diseases. Obes. Rev. 2008, 9 (Suppl. 1), 48–52. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Fahimi, S.; Singh, G.M.; Micha, R.; Khatibzadeh, S.; Engell, R.E.; Lim, S.; Danaei, G.; Ezzati, M.; Powles, J.; et al. Global sodium consumption and death from cardiovascular causes. N. Engl. J. Med. 2014, 371, 624–634. [Google Scholar] [CrossRef] [PubMed]
- Kojima, C.; Sasaki, H.; Tsuchiya, Y.; Goto, K. The influence of environmental temperature on appetite-related hormonal responses. J. Physiol. Anthropol. 2015, 34, 22. [Google Scholar] [CrossRef] [PubMed]
- Ge, K. The transition of Chinese dietary guidelines and food guide pagoda. Asia Pac. J. Clin. Nutr. 2011, 20, 439–446. [Google Scholar] [PubMed]
- Xi, B.; Hao, Y.; Liu, F. Salt reduction strategies in China. Lancet 2014, 383, 1128. [Google Scholar] [CrossRef]
- Wang, Y.; Shi, Y.; Wu, C.; Ding, J.; Li, M.; Lu, W.; Luo, C.; Wang, X.; Zou, S. Evaluation on a Mass Campaign for Salt Control in Shanghai: Change in Salt Consumption. J. Environ. Occup. Med. 2015, 32, 38–42. [Google Scholar]
- Li, J.R.; Hsieh, Y.H. Traditional Chinese food technology and cuisine. Asia Pac. J. Clin. Nutr. 2004, 13, 147–155. [Google Scholar] [PubMed]
- Jahns, L.; Johnson, L.K.; Scheett, A.J.; Stote, K.S.; Raatz, S.K.; Subar, A.F.; Tande, D. Measures of Diet Quality across Calendar and Winter Holiday Seasons among Midlife Women: A 1-Year Longitudinal Study Using the Automated Self-Administered 24-Hour Recall. J. Acad. Nutr. Diet. 2016, 116, 1961–1969. [Google Scholar] [CrossRef] [PubMed]
- Darmon, N.; Drewnowski, A. Does social class predict diet quality? Am. J. Clin. Nutr. 2008, 87, 1107–1117. [Google Scholar] [PubMed]
- Sicular, T.; Ximing, Y.; Gustafsson, B.; Shi, L. The urban–rural income gap and inequality in China. Rev. Income Wealth 2007, 53, 93–126. [Google Scholar] [CrossRef]
| Characteristics | Men (n = 836) | Women (n = 844) | ||
|---|---|---|---|---|
| n | % of Sub-Group | n | % of Sub-Group | |
| Age group (years) | ||||
| 15–44 | 257 | 30.74 | 253 | 29.98 |
| 45–59 | 281 | 33.61 | 292 | 34.60 |
| >60 | 298 | 35.65 | 299 | 35.43 |
| Marital Status | ||||
| Married | 668 | 79.90 | 643 | 76.18 |
| Other marital status | 168 | 20.10 | 201 | 23.82 |
| Occupation | ||||
| Professional job | 215 | 25.72 | 144 | 17.06 |
| Labor job | 103 | 12.32 | 75 | 8.89 |
| Others | 518 | 61.96 | 625 | 74.05 |
| Years of education | ||||
| ≤6 years | 170 | 20.33 | 227 | 26.90 |
| 7–9 years | 237 | 28.35 | 254 | 30.09 |
| 10–12 years | 215 | 25.72 | 191 | 22.63 |
| >12 years | 214 | 25.60 | 172 | 20.38 |
| Weight Status | ||||
| Underweight | 26 | 3.11 | 31 | 3.67 |
| Normal | 401 | 47.97 | 492 | 58.29 |
| Overweight | 320 | 38.28 | 258 | 30.57 |
| Obese | 80 | 9.57 | 35 | 4.15 |
| Non-reported | 9 | 1.08 | 28 | 3.32 |
| Smoker | ||||
| No | 424 | 50.72 | 838 | 99.29 |
| Yes | 412 | 49.28 | 6 | 0.71 |
| Drinker | ||||
| No | 500 | 59.81 | 775 | 91.82 |
| Yes | 275 | 32.89 | 43 | 5.09 |
| Non-reported | 61 | 7.30 | 26.00 | 3.08 |
| Family Income | ||||
| <20,000 RMB/person | 48 | 5.74 | 59 | 6.99 |
| 20,000–50,000 RMB/person | 251 | 30.02 | 273 | 32.35 |
| >50,000 RMB/person | 204 | 24.40 | 204 | 24.17 |
| Non-reported | 333 | 39.83 | 308 | 36.49 |
| Region | ||||
| Urban | 350 | 41.87 | 364 | 43.13 |
| Suburban | 189 | 22.61 | 187 | 22.16 |
| Rural | 220 | 30.74 | 213 | 29.98 |
| Non-reported | 77 | 9.21 | 80.00 | 9.48 |
| Components | Score Range | Seasons | Score | p-Value * | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (−12)–(−11) | (−10)–(−9) | (−8)–(−7) | (−6)–(−5) | (−4)–(−3) | (−2)–(−1) | 0 | (1)–(2) | (3)–(4) | (5)–(6) | (7)–(8) | (9)–(10) | (11)–(12) | ||||
| Cereals | (−12)–(12) | Spring | 0.59 | 1.14 | 1.24 | 3.97 | 8.44 | 16.19 | 15.65 | 18.13 | 14.81 | 7.67 | 5.39 | 2.14 | 4.64 | <0.001 |
| Summer | 0.67 | 0.39 | 1.62 | 6.17 | 12.06 | 17.53 | 18.43 | 15.36 | 10.85 | 5.72 | 4.42 | 3.28 | 3.49 | |||
| Fall | 1.76 | 1.93 | 3.16 | 6.69 | 12.94 | 17.39 | 16.41 | 13.80 | 10.93 | 6.43 | 4.84 | 2.15 | 1.57 | |||
| Winter | 0.35 | 0.98 | 1.70 | 4.33 | 10.71 | 16.17 | 19.99 | 14.60 | 10.57 | 7.97 | 5.21 | 2.45 | 4.97 | |||
| Vegetables | (−6)–(0) | Spring | 0.25 | 44.14 | 41.96 | 13.65 | <0.001 | |||||||||
| Summer | 0.23 | 33.11 | 47.74 | 18.92 | ||||||||||||
| Fall | 0.71 | 42.63 | 45.16 | 11.50 | ||||||||||||
| Winter | 0.00 | 36.07 | 49.90 | 14.03 | ||||||||||||
| Fruits | (−6)–(0) | Spring | 39.64 | 42.56 | 14.07 | 3.73 | 0.003 | |||||||||
| Summer | 23.45 | 26.82 | 23.54 | 26.19 | ||||||||||||
| Fall | 36.41 | 39.38 | 19.82 | 4.39 | ||||||||||||
| Winter | 34.41 | 39.05 | 21.09 | 5.45 | ||||||||||||
| Dairy | (−6)–(0) | Spring | 66.28 | 15.72 | 15.74 | 2.26 | <0.001 | |||||||||
| Summer | 61.37 | 18.36 | 16.20 | 4.07 | ||||||||||||
| Fall | 62.54 | 17.57 | 16.04 | 3.84 | ||||||||||||
| Winter | 63.80 | 15.51 | 14.84 | 5.85 | ||||||||||||
| Soybean | (−6)–(0) | Spring | 42.24 | 14.26 | 9.89 | 33.60 | <0.001 | |||||||||
| Summer | 41.30 | 10.58 | 10.18 | 37.95 | ||||||||||||
| Fall | 35.85 | 12.55 | 14.28 | 37.32 | ||||||||||||
| Winter | 32.42 | 11.39 | 13.29 | 42.91 | ||||||||||||
| Red meat, products, Poultry and game | (−4)–(4) | Spring | 4.02 | 10.84 | 33.34 | 31.29 | 20.51 | <0.001 | ||||||||
| Summer | 4.31 | 5.38 | 32.49 | 29.40 | 28.42 | |||||||||||
| Fall | 2.56 | 6.04 | 30.40 | 30.60 | 30.41 | |||||||||||
| Winter | 1.88 | 4.24 | 26.31 | 30.17 | 37.42 | |||||||||||
| Fish and shrimp | (−4)–(0) | Spring | 41.62 | 30.02 | 28.37 | <0.001 | ||||||||||
| Summer | 30.60 | 31.41 | 37.99 | |||||||||||||
| Fall | 33.40 | 31.47 | 35.14 | |||||||||||||
| Winter | 33.25 | 33.95 | 32.81 | |||||||||||||
| Egg | (−4)–(4) | Spring | 13.81 | 25.28 | 33.83 | 16.48 | 10.60 | <0.001 | ||||||||
| Summer | 9.21 | 24.42 | 33.53 | 21.08 | 11.75 | |||||||||||
| Fall | 15.43 | 28.19 | 30.75 | 18.43 | 7.20 | |||||||||||
| Winter | 14.77 | 27.86 | 34.08 | 16.44 | 6.85 | |||||||||||
| Cooking oil | (0)–(4) | Spring | 46.31 | 37.95 | 15.74 | <0.001 | ||||||||||
| Summer | 53.64 | 34.33 | 12.03 | |||||||||||||
| Fall | 50.63 | 32.14 | 17.24 | |||||||||||||
| Winter | 51.08 | 33.84 | 15.08 | |||||||||||||
| Salt | (0)–(4) | Spring | 58.33 | 31.36 | 10.31 | <0.001 | ||||||||||
| Summer | 60.03 | 28.65 | 11.32 | |||||||||||||
| Fall | 55.35 | 32.82 | 11.84 | |||||||||||||
| Winter | 52.04 | 34.40 | 13.57 | |||||||||||||
| Alcoholic beverage | (0)–(4) | Spring | 98.22 | 1.60 | 0.18 | 0.3085 | ||||||||||
| Summer | 98.99 | 0.98 | 0.03 | |||||||||||||
| Fall | 98.58 | 1.42 | 0.00 | |||||||||||||
| Winter | 98.41 | 1.58 | 0.02 | |||||||||||||
| Drinking water | (−12)–(0) | Spring | 28.62 | 18.12 | 17.19 | 13.34 | 10.32 | 4.42 | 7.98 | <0.001 | ||||||
| Summer | 20.71 | 10.94 | 14.43 | 11.68 | 12.76 | 9.59 | 19.89 | |||||||||
| Fall | 22.29 | 18.42 | 16.73 | 14.79 | 9.72 | 6.07 | 11.97 | |||||||||
| Winter | 11.31 | 17.17 | 16.55 | 15.64 | 12.33 | 10.03 | 16.97 | |||||||||
| Diet variety | (−12)–(0) | Spring | 0.05 | 1.70 | 12.82 | 30.66 | 39.17 | 14.98 | 0.62 | <0.001 | ||||||
| Summer | 0.06 | 1.34 | 6.54 | 26.57 | 41.36 | 21.89 | 2.23 | |||||||||
| Fall | 0.69 | 1.14 | 8.93 | 29.49 | 39.44 | 19.67 | 0.65 | |||||||||
| Winter | 0.00 | 0.68 | 8.19 | 22.95 | 44.91 | 21.61 | 1.67 | |||||||||
| Seasons | Indicator | Mean (SD) | Range | p-Value * | Mean Difference and 95% CI of Pairwise Comparison † | |||
|---|---|---|---|---|---|---|---|---|
| Summer | Fall | Winter | ||||||
| Over-intake | Spring | HBS | 6.96 (5.46) | 0–29 | <0.001 | −0.53 (−0.87, −0.20) | 0.17 (−0.17, 0.50) | −1.23 (−1.56, −0.89) |
| Summer | HBS | 7.49 (4.79) | 0–26 | 0.70 (0.36, 1.04) | −0.69 ( −1.03, −0.35) | |||
| Fall | HBS | 6.79 (4.42) | 0–28 | −1.39 ( −1.73, −1.05) | ||||
| Winter | HBS | 8.18 (4.93) | 2–27 | |||||
| Under-intake | Spring | LBS | 35.98 (10.76) | 2–67 | <0.001 | 7.80 (7.06, 8.54) | 3.59 (2.85, 4.32) | 7.32 (6.59, 8.06) |
| Summer | LBS | 28.18 (8.88) | 3–60 | −4.21 (−4.95, −3.48) | −0.48 ( −1.21, 0.26) | |||
| Fall | LBS | 32.40 (9.16) | 8–68 | 3.74 (3.00, 4.47) | ||||
| Winter | LBS | 28.66 (8.38) | 6–64 | |||||
| Overall imbalance | Spring | DQD | 43.27 (10.21) | 15–76 | <0.001 | 7.60 (6.77, 8.42) | 4.08 (3.26, 4.91) | 6.43 (5.60, 0.25) |
| Summer | DQD | 35.67 (9.71) | 12–60 | −3.51 (−4.33, −2.69) | −1.17 (−1.99, −0.34) | |||
| Fall | DQD | 39.19 (9.36) | 18–68 | 2.34 (1.52, 3.17) | ||||
| Winter | DQD | 36.84 (9.45) | 22–50 | |||||
| Items | DQD | Univariable Model | Multivariable Model | Standardized Multivariable Model | |||
|---|---|---|---|---|---|---|---|
| Mean(SD) | Coeff. (95% CI) | p-Value | Coeff. (95% CI) | p-Value | Standard Coeff. (95% CI) | p-Value | |
| Sex | |||||||
| Men | 40.00 (12.35) | Reference | Reference | Reference | |||
| Women | 37.65 (11.97) | −2.35 (−2.97, −1.73) | <0.001 | −1.09 (−1.79, −0.39) | 0.002 | −0.04 (−0.07, −0.02) | 0.003 |
| Age group (years) | |||||||
| 15–44 | 37.98 (12.26) | Reference | Reference | Reference | |||
| 45–59 | 38.33 (11.90) | 0.35 (−0.40, 1.10) | 0.359 | −1.38 (−2.19, −0.57) | 0.001 | −0.05 (−0.08, −0.02) | 0.003 |
| >60 | 39.78 (12.50) | 1.80 (1.06, 2.54) | <0.001 | −1.19 (−2.07, −0.32) | 0.008 | −0.04 (−0.08, −0.01) | 0.020 |
| Marital Status | |||||||
| Married | 38.86 (12.19) | Reference | Reference | Reference | |||
| Other marital status | 38.30 (12.46) | −0.57 (−1.30, 0.17) | 0.130 | 0.06 (−0.69, 0.82) | 0.866 | 0.00 (−0.03, 0.03) | 0.998 |
| Occupation | |||||||
| Professional job | 36.63 (12.47) | Reference | Reference | Reference | |||
| Labor job | 44.02 (11.58) | 7.39 (6.28, 8.50) | <0.001 | 2.53 (1.37, 3.70) | <0.001 | 0.06 (0.03, 0.09) | <0.001 |
| Others | 38.58 (12.04) | 1.95 (1.21, 2.68) | <0.001 | 0.45 (−0.37, 1.28) | 0.279 | 0.02 (−0.01, 0.05) | 0.211 |
| Years of education | |||||||
| ≤6 yrs | 43.27 (11.87) | Reference | Reference | Reference | |||
| 7~9 yrs | 39.15 (11.76) | −4.12 (−4.92, −3.32) | <0.001 | −2.30 (−3.15, −1.45) | <0.001 | −0.09 (−0.12, −0.05) | <0.001 |
| 10~12 yrs | 37.48 (11.77) | −5.79 (−6.63, −4.95) | <0.001 | −3.06 (−4.00, −2.12) | <0.001 | −0.11 (−0.14, −0.07) | <0.001 |
| >12 yrs | 34.86 (12.21) | −8.41 (−9.26, −7.55) | <0.001 | −4.51 (−5.60, −3.41) | <0.001 | −0.15 (−0.19, −0.11) | <0.001 |
| Smoker | |||||||
| No | 37.90 (12.18) | Reference | Reference | Reference | |||
| Yes | 41.23 (12.10) | 1.09 (0.39, 1.79) | 0.002 | 1.87 (1.05, 2.70) | <0.001 | 0.07 (0.04, 0.10) | <0.001 |
| Drinker | |||||||
| No | 38.20 (12.18) | Reference | Reference | Reference | |||
| Yes | 41.26 (12.23) | 3.06 (2.30, 3.83) | <0.0001 | 1.18 (0.38, 1.97) | 0.004 | 0.04 (0.01, 0.07) | 0.002 |
| Weight Status | |||||||
| Underweight | 40.07 (12.48) | 1.67 (−0.01, 3.36) | 0.0512 | 0.97 (−0.59, 2.53) | 0.222 | 0.01 (−0.01, 0.04) | 0.202 |
| Normal | 37.95 (12.38) | Reference | Reference | Reference | |||
| Overweight | 38.87 (12.16) | 0.48 (−0.19, 1.15) | 0.1613 | −0.12 (−0.75, 0.51) | 0.706 | −0.01 (−0.03, 0.02) | 0.620 |
| Obese | 41.04 (11.27) | 2.65 (1.34, 3.96) | <0.0001 | 1.16 (0.00, 2.36) | 0.049 | 0.02 (0.00, 0.04) | 0.050 |
| Region | |||||||
| Urban | 35.27 (11.71) | Reference | Reference | Reference | |||
| Suburban | 40.17 (10.40) | 5.70 (5.01, 6.40) | <0.001 | 4.58 (3.85, 5.30) | <0.001 | 0.15 (0.12, 0.17) | <0.001 |
| Rural | 45.62 (10.51) | 11.16 (10.50, 11.82) | <0.001 | 8.64 (7.90, 9.38) | <0.001 | 0.31 (0.28, 0.33) | <0.001 |
| Family Income | |||||||
| <20,000 RMB/person | 41.97 (12.01) | Reference | Reference | Reference | |||
| 20,000–50,000 RMB/person | 39.18 (11.95) | −2.79 (−3.58, −1.99) | <0.001 | −0.22 (−1.00,0.56) | 0.582 | −0.01 (−0.03, 0.02) | 0.614 |
| >50,000 RMB/person | 36.34 (11.87) | −5.63 (−6.34, −4.92) | <0.001 | −1.63 (−2.38, −0.89) | <0.001 | −0.07 (−0.10, −0.04) | <0.0001 |
| Non–reported | 35.53 (12.87) | −6.45 (−7.74, −5.15) | <0.001 | −1.58 (−2.84, −0.32) | 0.014 | −0.03 (−0.06, −0.01) | 0.010 |
| Season | |||||||
| Spring | 43.27 (17.21) | Reference | Reference | Reference | |||
| Summer | 35.67 (9.71) | −7.60 (−8.42, −6.77) | <0.001 | −7.80 (−8.59, −7.01) | <0.001 | −0.28 (−0.30, −0.25) | <0.001 |
| Fall | 39.19 (9.36) | −4.08 (−4.91, −3.26) | <0.001 | −4.18 (−4.97, −3.40) | <0.001 | −0.15 (−0.18, −0.12) | <0.001 |
| Winter | 36.84 (9.45) | −6.43 (−7.25, −5.60) | <0.001 | −6.69 (−7.49, −5.90) | <0.001 | −0.24 (−0.26, −0.21) | <0.001 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zang, J.; Yu, H.; Zhu, Z.; Lu, Y.; Liu, C.; Yao, C.; Bai, P.; Guo, C.; Jia, X.; Zou, S.; et al. Does the Dietary Pattern of Shanghai Residents Change across Seasons and Area of Residence: Assessing Dietary Quality Using the Chinese Diet Balance Index (DBI). Nutrients 2017, 9, 251. https://doi.org/10.3390/nu9030251
Zang J, Yu H, Zhu Z, Lu Y, Liu C, Yao C, Bai P, Guo C, Jia X, Zou S, et al. Does the Dietary Pattern of Shanghai Residents Change across Seasons and Area of Residence: Assessing Dietary Quality Using the Chinese Diet Balance Index (DBI). Nutrients. 2017; 9(3):251. https://doi.org/10.3390/nu9030251
Chicago/Turabian StyleZang, Jiajie, Huiting Yu, Zhenni Zhu, Ye Lu, Changhe Liu, Chunxia Yao, Pinqing Bai, Changyi Guo, Xiaodong Jia, Shurong Zou, and et al. 2017. "Does the Dietary Pattern of Shanghai Residents Change across Seasons and Area of Residence: Assessing Dietary Quality Using the Chinese Diet Balance Index (DBI)" Nutrients 9, no. 3: 251. https://doi.org/10.3390/nu9030251
APA StyleZang, J., Yu, H., Zhu, Z., Lu, Y., Liu, C., Yao, C., Bai, P., Guo, C., Jia, X., Zou, S., & Wu, F. (2017). Does the Dietary Pattern of Shanghai Residents Change across Seasons and Area of Residence: Assessing Dietary Quality Using the Chinese Diet Balance Index (DBI). Nutrients, 9(3), 251. https://doi.org/10.3390/nu9030251





