The Effects of Low-Carbohydrate Diets on Psychosocial Outcomes in Obesity/Overweight: A Systematic Review of Randomized, Controlled Studies
Abstract
:1. Introduction
2. Methods
2.1. Inclusion and Exclusion Criteria
2.2. Information Source and Search Strategy
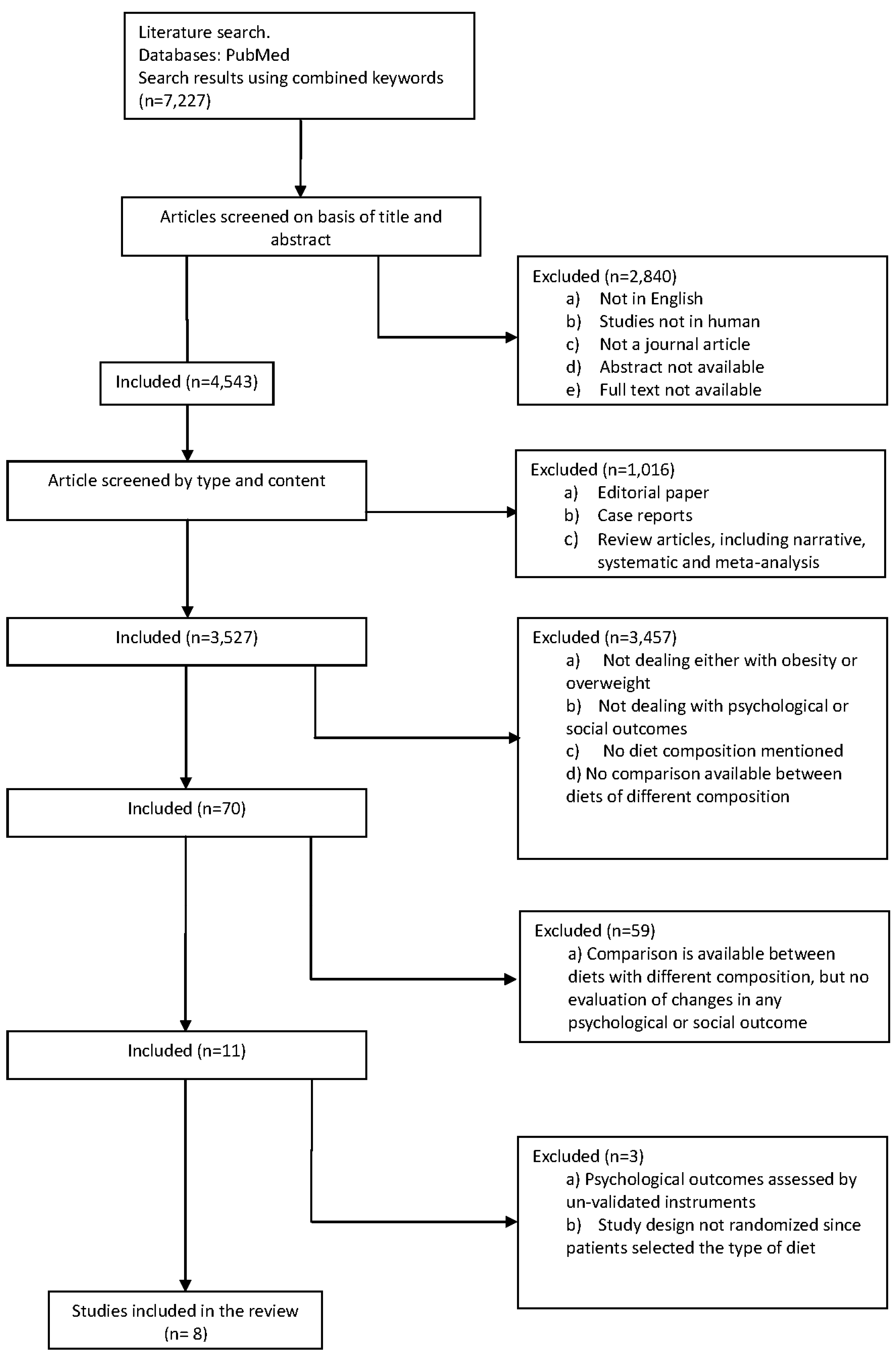
2.3. Study Selection
2.4. Data Collection Process and Data Items
2.5. Data Synthesis
3. Results
3.1. The Short-Term Psychosocial Effects of a Low-Carbohydrate Diet
3.2. The Long-Term Psychosocial Effects of a Low-Carbohydrate Diet
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Stunkard, A.J.; Rush, J. Dieting and depression reexamined. A critical review of reports of untoward responses during weight reduction for obesity. Ann. Intern. Med. 1974, 81, 526–533. [Google Scholar] [CrossRef] [PubMed]
- Bryan, J.; Tiggemann, M. The effect of weight-loss dieting on cognitive performance and psychological well-being in overweight women. Appetite 2001, 36, 147–156. [Google Scholar] [CrossRef] [PubMed]
- Wadden, T.A.; Stunkard, A.J. Controlled trial of very low calorie diet, behavior therapy, and their combination in the treatment of obesity. J. Consult. Clin. Psychol. 1986, 54, 482–488. [Google Scholar] [CrossRef] [PubMed]
- Taylor, C.B.; Ferguson, J.M.; Reading, J.C. Gradual weight loss and depression. Behav. Ther. 1978, 9, 622–625. [Google Scholar] [CrossRef]
- Wing, R.; Marcus, B.H.; Epstein, L.H.; Blair, S.N.; Burton, L.R. Binge eating in obese patients with type 2 diabetes. Int. J. Eat. Disord. 1989, 8, 671–679. [Google Scholar] [CrossRef]
- Wadden, T.A.; Foster, G.D.; Letizia, K.A. One-year behavioral treatment of obesity: Comparison of moderate and severe caloric restriction and the effects of weight maintenance therapy. J. Consult. Clin. Psychol. 1994, 62, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Wadden, T.A.; Stunkard, A.J.; Brownell, K.D.; Day, S.C. A comparison of two very-low-calorie diets: Protein-sparing-modified fast versus protein-formula-liquid diet. Am. J. Clin. Nutr. 1985, 41, 533–539. [Google Scholar] [PubMed]
- Wing, R.R.; Marcus, M.D.; Blair, E.H.; Burton, L.R. Psychological responses of obese type II diabetic subjects to very-low-calorie diet. Diabetes Care 1991, 14, 596–599. [Google Scholar] [CrossRef] [PubMed]
- Brownell, K.D.; Stunkard, A.J. Couples training, pharmacotherapy, and behavior therapy in the treatment of obesity. Arch. Gen. Psychiatry 1981, 38, 1224–1229. [Google Scholar] [CrossRef] [PubMed]
- Kiortsis, D.N.; Tsouli, S.; Filippatos, T.D.; Konitsiotis, S.; Elisaf, M.S. Effects of sibutramine and orlistat on mood in obese and overweight subjects: A randomised study. Nutr. Metab. Cardiovasc. Dis. 2008, 18, 207–210. [Google Scholar] [CrossRef] [PubMed]
- Wadden, T.A.; Berkowitz, R.I.; Vogt, R.A.; Steen, S.N.; Stunkard, A.J.; Foster, G.D. Lifestyle modification in the pharmacologic treatment of obesity: A pilot investigation of a potential primary care approach. Obes. Res. 1997, 5, 218–226. [Google Scholar] [CrossRef] [PubMed]
- Dalle Grave, R.; Calugi, S.; Petroni, M.L.; di Domizio, S.; Marchesini, G. Weight management, psychological distress and binge eating in obesity. A reappraisal of the problem. Appetite 2010, 54, 269–273. [Google Scholar] [CrossRef] [PubMed]
- Rubin, R.R.; Wadden, T.A.; Bahnson, J.L.; Blackburn, G.L.; Brancati, F.L.; Bray, G.A.; Coday, M.; Crow, S.J.; Curtis, J.M.; Dutton, G.; et al. Impact of intensive lifestyle intervention on depression and health-related quality of life in type 2 diabetes: The Look AHEAD Trial. Diabetes Care 2014, 37, 1544–1553. [Google Scholar] [PubMed]
- Purnell, J.Q. Obesity: Calories or content: What is the best weight-loss diet? Nat. Rev. Endocrinol. 2009, 5, 419–420. [Google Scholar] [CrossRef] [PubMed]
- Skov, A.R.; Toubro, S.; Ronn, B.; Holm, L.; Astrup, A. Randomized trial on protein vs. carbohydrate in ad libitum fat reduced diet for the treatment of obesity. Int. J. Obes. Relat. Metab. Disord. 1999, 23, 528–536. [Google Scholar] [CrossRef] [PubMed]
- Weigle, D.S.; Breen, P.A.; Matthys, C.C.; Callahan, H.S.; Meeuws, K.E.; Burden, V.R.; Purnell, J.Q. A high-protein diet induces sustained reductions in appetite, ad libitum caloric intake, and body weight despite compensatory changes in diurnal plasma leptin and ghrelin concentrations. Am. J. Clin. Nutr. 2005, 82, 41–48. [Google Scholar] [PubMed]
- Foster, G.D.; Wyatt, H.R.; Hill, J.O.; McGuckin, B.G.; Brill, C.; Mohammed, B.S.; Szapary, P.O.; Rader, D.J.; Edman, J.S.; Klein, S. A randomized trial of a low-carbohydrate diet for obesity. N. Engl. J. Med. 2003, 348, 2082–2090. [Google Scholar] [CrossRef] [PubMed]
- Samaha, F.F.; Iqbal, N.; Seshadri, P.; Chicano, K.L.; Daily, D.A.; McGrory, J.; Williams, T.; Williams, M.; Gracely, E.J.; Stern, L. A low-carbohydrate as compared with a low-fat diet in severe obesity. N. Engl. J. Med. 2003, 348, 2074–2081. [Google Scholar] [CrossRef] [PubMed]
- Sondike, S.B.; Copperman, N.; Jacobson, M.S. Effects of a low-carbohydrate diet on weight loss and cardiovascular risk factor in overweight adolescents. J. Pediatr. 2003, 142, 253–258. [Google Scholar] [CrossRef] [PubMed]
- Brehm, B.J.; Seeley, R.J.; Daniels, S.R.; D’Alessio, D.A. A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J. Clin. Endocrinol. Metab. 2003, 88, 1617–1623. [Google Scholar] [CrossRef] [PubMed]
- Aude, Y.W.; Agatston, A.S.; Lopez-Jimenez, F.; Lieberman, E.H.; Marie, A.; Hansen, M.; Rojas, G.; Lamas, G.A.; Hennekens, C.H. The national cholesterol education program diet vs. a diet lower in carbohydrates and higher in protein and monounsaturated fat: A randomized trial. Arch. Intern. Med. 2004, 164, 2141–2146. [Google Scholar] [CrossRef] [PubMed]
- Yancy, W.S., Jr.; Olsen, M.K.; Guyton, J.R.; Bakst, R.P.; Westman, E.C. A low-carbohydrate, ketogenic diet versus a low-fat diet to treat obesity and hyperlipidemia: A randomized, controlled trial. Ann. Intern. Med. 2004, 140, 769–777. [Google Scholar] [CrossRef] [PubMed]
- Volek, J.; Sharman, M.; Gomez, A.; Judelson, D.; Rubin, M.; Watson, G.; Sokmen, B.; Silvestre, R.; French, D.; Kraemer, W. Comparison of energy-restricted very low-carbohydrate and low-fat diets on weight loss and body composition in overweight men and women. Nutr. Metab. (Lond.) 2004, 1, 13. [Google Scholar] [CrossRef] [PubMed]
- Nickols-Richardson, S.M.; Coleman, M.D.; Volpe, J.J.; Hosig, K.W. Perceived hunger is lower and weight loss is greater in overweight premenopausal women consuming a low-carbohydrate/high-protein vs. high-carbohydrate/low-fat diet. J. Am. Diet. Assoc. 2005, 105, 1433–1437. [Google Scholar] [CrossRef] [PubMed]
- Daly, M.E.; Paisey, R.; Millward, B.A.; Eccles, C.; Williams, K.; Hammersley, S.; MacLeod, K.M.; Gale, T.J. Short-term effects of severe dietary carbohydrate-restriction advice in type 2 diabetes—A randomized controlled trial. Diabet. Med. 2006, 23, 15–20. [Google Scholar] [CrossRef] [PubMed]
- McClernon, F.J.; Yancy, W.S., Jr.; Eberstein, J.A.; Atkins, R.C.; Westman, E.C. The effects of a low-carbohydrate ketogenic diet and a low-fat diet on mood, hunger, and other self-reported symptoms. Obesity (Silver Spring) 2007, 15, 182–187. [Google Scholar] [CrossRef] [PubMed]
- Halyburton, A.K.; Brinkworth, G.D.; Wilson, C.J.; Noakes, M.; Buckley, J.D.; Keogh, J.B.; Clifton, P.M. Low- and high-carbohydrate weight-loss diets have similar effects on mood but not cognitive performance. Am. J. Clin. Nutr. 2007, 86, 580–587. [Google Scholar] [PubMed]
- Dyson, P.A.; Beatty, S.; Matthews, D.R. A low-carbohydrate diet is more effective in reducing body weight than healthy eating in both diabetic and non-diabetic subjects. Diabet. Med. 2007, 24, 1430–1435. [Google Scholar] [CrossRef] [PubMed]
- Westman, E.C.; Yancy, W.S., Jr.; Mavropoulos, J.C.; Marquart, M.; McDuffie, J.R. The effect of a low-carbohydrate, ketogenic diet versus a low-glycemic index diet on glycemic control in type 2 diabetes mellitus. Nutr. Metab. (Lond.) 2008, 5, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Keogh, J.B.; Brinkworth, G.D.; Noakes, M.; Belobrajdic, D.P.; Buckley, J.D.; Clifton, P.M. Effects of weight loss from a very-low-carbohydrate diet on endothelial function and markers of cardiovascular disease risk in subjects with abdominal obesity. Am. J. Clin. Nutr. 2008, 87, 567–576. [Google Scholar] [PubMed]
- Volek, J.S.; Phinney, S.D.; Forsythe, C.E.; Quann, E.E.; Wood, R.J.; Puglisi, M.J.; Kraemer, W.J.; Bibus, D.M.; Fernandez, M.L.; Feinman, R.D. Carbohydrate restriction has a more favorable impact on the metabolic syndrome than a low fat diet. Lipids 2009, 44, 297–309. [Google Scholar] [CrossRef] [PubMed]
- Krebs, N.F.; Gao, D.; Gralla, J.; Collins, J.S.; Johnson, S.L. Efficacy and safety of a high protein, low carbohydrate diet for weight loss in severely obese adolescents. J. Pediatr. 2010, 157, 252–258. [Google Scholar] [CrossRef] [PubMed]
- Clifton, P.M.; Condo, D.; Keogh, J.B. Long term weight maintenance after advice to consume low carbohydrate, higher protein diets—A systematic review and meta analysis. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 224–235. [Google Scholar] [CrossRef] [PubMed]
- Shai, I.; Schwarzfuchs, D.; Henkin, Y.; Shahar, D.R.; Witkow, S.; Greenberg, I.; Golan, R.; Fraser, D.; Bolotin, A.; Vardi, H.; et al. Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. N. Engl. J. Med. 2008, 359, 229–241. [Google Scholar] [CrossRef] [PubMed]
- Volek, J.S.; Sharman, M.J.; Gomez, A.L.; DiPasquale, C.; Roti, M.; Pumerantz, A.; Kraemer, W.J. Comparison of a very low-carbohydrate and low-fat diet on fasting lipids, LDL subclasses, insulin resistance, and postprandial lipemic responses in overweight women. J. Am. Coll. Nutr. 2004, 23, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Meckling, K.A.; O'Sullivan, C.; Saari, D. Comparison of a low-fat diet to a low-carbohydrate diet on weight loss, body composition, and risk factors for diabetes and cardiovascular disease in free-living, overweight men and women. J. Clin. Endocrinol. Metab. 2004, 89, 2717–2723. [Google Scholar] [CrossRef] [PubMed]
- Brinkworth, G.D.; Noakes, M.; Buckley, J.D.; Keogh, J.B.; Clifton, P.M. Long-term effects of a very-low-carbohydrate weight loss diet compared with an isocaloric low-fat diet after 12 months. Am. J. Clin. Nutr. 2009, 90, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Hernandez, T.L.; Sutherland, J.P.; Wolfe, P.; Allian-Sauer, M.; Capell, W.H.; Talley, N.D.; Wyatt, H.R.; Foster, G.D.; Hill, J.O.; Eckel, R.H. Lack of suppression of circulating free fatty acids and hypercholesterolemia during weight loss on a high-fat, low-carbohydrate diet. Am. J. Clin. Nutr. 2010, 91, 578–585. [Google Scholar] [CrossRef] [PubMed]
- Hashimoto, Y.; Fukuda, T.; Oyabu, C.; Tanaka, M.; Asano, M.; Yamazaki, M.; Fukui, M. Impact of low-carbohydrate diet on body composition: Meta-analysis of randomized controlled studies. Obes. Rev. 2016, 17, 499–509. [Google Scholar] [CrossRef] [PubMed]
- Bray, G.A. Low-carbohydrate diets and realities of weight loss. JAMA 2003, 289, 1853–1855. [Google Scholar] [CrossRef] [PubMed]
- Richardson, W.S.; Wilson, M.C.; Nishikawa, J.; Hayward, R.S. The well-built clinical question: A key to evidence-based decisions. ACP J. Club 1995, 123, 12–13. [Google Scholar]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gotzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. Ann. Intern. Med. 2009, 151, 65–94. [Google Scholar] [CrossRef]
- Altman, D.G.; Schulz, K.F.; Moher, D.; Egger, M.; Davidoff, F.; Elbourne, D.; Gotzsche, P.C.; Lang, T. The revised CONSORT statement for reporting randomized trials: Explanation and elaboration. Ann. Intern. Med. 2001, 134, 663–694. [Google Scholar] [CrossRef] [PubMed]
- Pubmed Database. Available online: http://www.ncbi.nlm.nih.gov/pubmed (accessed on 27 June 2016).
- Chess, L.E.; Gagnier, J. Risk of bias of randomized controlled trials published in orthopaedic journals. BMC Med. Res. Methodol. 2013, 13, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Jadad, A.R.; Tugwell, P. Assessing the quality of randomized controlled trials. Current issues and future directions. Int. J. Technol. Assess. Health Care 1996, 12, 195–208. [Google Scholar] [CrossRef] [PubMed]
- Popay, J.; Roberts, H.; Sowden, A.; Petticrew, M.; Britten, N.; Arai, L.; Roen, K.; Rodgers, M. Guidance on the Conduct of Narrative Synthesis in Systematic Reviews. Available online: http://www.lancaster.ac.uk/shm/research/nssr/research/dissemination/publications/NS_Synthesis_Guidance_v1.pdf (accessed on 27 June 2016).
- Accurso, A.; Bernstein, R.K.; Dahlqvist, A.; Draznin, B.; Feinman, R.D.; Fine, E.J.; Gleed, A.; Jacobs, D.B.; Larson, G.; Lustig, R.H.; et al. Dietary carbohydrate restriction in type 2 diabetes mellitus and metabolic syndrome: Time for a critical appraisal. Nutr. Metab. (Lond.) 2008, 5, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Kogon, M.M.; Krauchi, K.; van der Velde, P.; van der Werf, H.; Keller, U. Psychological and metabolic effects of dietary carbohydrates and dexfenfluramine during a low-energy diet in obese women. Am. J. Clin. Nutr. 1994, 60, 488–493. [Google Scholar] [PubMed]
- D’Anci, K.E.; Watts, K.L.; Kanarek, R.B.; Taylor, H.A. Low-carbohydrate weight-loss diets. Effects on cognition and mood. Appetite 2009, 52, 96–103. [Google Scholar] [CrossRef] [PubMed]
- Rosen, J.C.; Hunt, D.A.; Sims, E.A.; Bogardus, C. Comparison of carbohydrate-containing and carbohydrate-restricted hypocaloric diets in the treatment of obesity: Effects of appetite and mood. Am. J. Clin. Nutr. 1982, 36, 463–469. [Google Scholar] [PubMed]
- Rosen, J.C.; Gross, J.; Loew, D.; Sims, E.A. Mood and appetite during minimal-carbohydrate and carbohydrate-supplemented hypocaloric diets. Am. J. Clin. Nutr. 1985, 42, 371–379. [Google Scholar] [PubMed]
- Galletly, C.; Moran, L.; Noakes, M.; Clifton, P.; Tomlinson, L.; Norman, R. Psychological benefits of a high-protein, low-carbohydrate diet in obese women with polycystic ovary syndrome—A pilot study. Appetite 2007, 49, 590–593. [Google Scholar] [CrossRef] [PubMed]
- Saslow, L.R.; Kim, S.; Daubenmier, J.J.; Moskowitz, J.T.; Phinney, S.D.; Goldman, V.; Murphy, E.J.; Cox, R.M.; Moran, P.; Hecht, F.M. A randomized pilot trial of a moderate carbohydrate diet compared to a very low carbohydrate diet in overweight or obese individuals with type 2 diabetes mellitus or prediabetes. PLoS ONE 2014, 9, e91027. [Google Scholar] [CrossRef] [PubMed]
- Brinkworth, G.D.; Buckley, J.D.; Noakes, M.; Clifton, P.M.; Wilson, C.J. Long-term effects of a very low-carbohydrate diet and a low-fat diet on mood and cognitive function. Arch. Intern. Med. 2009, 169, 1873–1880. [Google Scholar] [CrossRef] [PubMed]
- Dalle Grave, R.; Calugi, S.; Gavasso, I.; El Ghoch, M.; Marchesini, G. A randomized trial of energy-restricted high-protein versus high-carbohydrate, low-fat diet in morbid obesity. Obesity (Silver Spring) 2013, 21, 1774–1781. [Google Scholar] [CrossRef] [PubMed]
- Brinkworth, G.D.; Luscombe-Marsh, N.D.; Thompson, C.H.; Noakes, M.; Buckley, J.D.; Wittert, G.; Wilson, C.J. Long-term effects of very low-carbohydrate and high-carbohydrate weight-loss diets on psychological health in obese adults with type 2 diabetes: Randomized controlled trial. J. Intern. Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Gaudry, E.; Spielberger, C.D. Anxiety and intelligence in paired-associate learning. J. Educ. Psychol. 1970, 61, 386–391. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Ward, C.H.; Mendelson, M.; Mock, J.; Erbaugh, J. An inventory for measuring depression. Arch. Gen. Psychiatry 1961, 4, 561–571. [Google Scholar] [CrossRef] [PubMed]
- Zuckerman, M.; Lubin, B.; Vogel, L.; Valerius, E. Measurement of experimentally induced affects. J. Consult. Psychol. 1964, 28, 418–425. [Google Scholar] [CrossRef] [PubMed]
- Fitts, W. Tennessee Self-Concept Scale; Counselor Recordings and Tests: Nashville, TN, USA, 1965. [Google Scholar]
- Spielberger, C.; Gorsuch, R.; Lushene, R.; Vagg, P.; Jacobs, G. Manual for the State-Trait Anxiety Inventory; Consulting Psychologists Press, Inc.: Palo Alto, CA, USA, 1983. [Google Scholar]
- McNair, D.; Lorr, M.; Droppleman, L. Profile of Mood States Manual; Educational and Industrial Testing Service: San Diego, CA, USA, 1971. [Google Scholar]
- Radloff, L. The CES-D scale A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Van Strien, T.; Frijters, J.; Bergers, G.; Defares, P. The Dutch Eating Behavior Questionnaire (DEBQ) for assessment of restrained, emotional, and external eating behavior. Int. J. Eat. Disord. 1986, 5, 295–315. [Google Scholar] [CrossRef]
- Daubenmier, J. The relationship of yoga, body awareness, and body responsiveness to self-objectification and disordered eating. Psychol. Women Q. 2005, 29, 207–219. [Google Scholar] [CrossRef]
- Stunkard, A.J.; Messick, S. The three-factor eating questionnaire to measure dietary restraint, disinhibition and hunger. J. Psychosom. Res. 1985, 29, 71–83. [Google Scholar] [CrossRef]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Rosenberg, M. Society and the Adolescent Self Image, 2nd ed.; Princeton University Press: Princeton, NJ, USA, 1965. [Google Scholar]
- Cuzzolaro, M.; Vetrone, G.; Marano, G.; Garfinkel, P.E. The Body Uneasiness Test (BUT): Development and validation of a new body image assessment scale. Eat. Weight Disord. 2006, 11, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Gormally, J.; Black, S.; Daston, S.; Rardin, D. The assessment of binge eating severity among obese persons. Addict. Behav. 1982, 7, 47–55. [Google Scholar] [CrossRef]
- Coradeschi, D.; Sica, C.; Ghisi, M.; Sanavio, E.; Novara, C.; Dorz, S.; Chiri, L. Psychometric properties of the Italian version of the Beck Anxiety Inventory: A preliminary study. Boll. Psicopatol. Appl. 2007, 253, 15–25. [Google Scholar]
- Polonsky, W.H.; Anderson, B.J.; Lohrer, P.A.; Welch, G.; Jacobson, A.M.; Aponte, J.E.; Schwartz, C.E. Assessment of diabetes-related distress. Diabetes Care 1995, 18, 754–760. [Google Scholar] [CrossRef] [PubMed]
- Boyer, J.G.; Earp, J.A. The development of an instrument for assessing the quality of life of people with diabetes. Diabetes-39. Med. Care 1997, 35, 440–453. [Google Scholar] [CrossRef] [PubMed]
| First Author | Year | Gender | Duration | Sample | Age Range | Diet Composition | Outcome Measure | Change in Outcome |
|---|---|---|---|---|---|---|---|---|
| Short-Term Studies | ||||||||
| Rosen et al. [51] | 1982 | F | 8 weeks | Eight females treated for obesity | 25–33 years | CHO: 35% proteins, 36% fats, 29% carbs NO CHO: 35% proteins, 64% fats, 1% carbs | STAI-T BDI | No difference in psychological effects between the two diets |
| Rosen et al. [52] | 1985 | F and M | 8 weeks | 19 females and 1 male treated for obesity/overweight | 20–38 years | MCD: 58% proteins, 42% fats, 0% carbs CCD: 42% proteins, 30% fats, 28% carbs | MAACL TSC | No difference in psychological effects between the two diets |
| Halyburton et al. [27] | 2007 | F and M | 8 weeks | 121 men and women treated for obesity/overweight | 24–64 years | HFLC: 35% proteins, 61% fats, 4% carbs LFHC: 24% proteins, 30% fats, 46% carbs | SAI POMS TMDS | Similar effects of diets on psychological well-being effects |
| Galletly et al. [53] | 2007 | F | 4 months | n = 14 LPHC n = 14 HPLC | 33.0 ± 1.2 years 32.0 ± 1.2 years | LPHC: 15% proteins, 30% fats, 55% carbs HPLC: 30% proteins, 30% fats, 40% carbs | HAD RSES | Significant improvement in depression and self-esteem in the In the HPLC group |
| Saslow et al. [54] | 2014 | F and M | 3 months | 34 patients with type-2 diabetes mellitus or pre-diabetes treated for obesity/overweight | 64.8 ± 7.7 years 55.1 ± 13.5 years | LCK: 20–50 grams of carbohydrate day MCCR: 45%–50% carbohydrate | Diabetes Distress Scale CES-D Dutch Eating Behaviour Scale Body Responsiveness-Q Three-Factor Eating-Q | No difference in psychological measures between the two diets |
| Long Term Studies | ||||||||
| Brinkworth et al. [55] | 2009 | F and M | 1 year | Participants treated for obesity/overweight, n = 57 HFLC n = 61 LFHC | 24–64 years | HFLC: 35% proteins, 61% fats, 4% carbs LFHC: 24% proteins, 30% fats, 46% carbs | STAI BDI POMS | Greater improvements in psychological outcomes for the LFHC diet compared with the LC diet |
| Dalle Grave et al. [56] | 2013 | F and M | 1 year | 88 class II–III obesity patients randomized to LPHC and HPLC | 18–65 years | LPHC: 17% proteins, 20% fats, 63% carbs HPLC: 34% proteins, 20% fats, 46% carbs | BAI BDI BES BUT-GSI | All psychosocial measures decreased from baseline to 1 year, with no differences between groups |
| Brinkworth et al. [57] | 2016 | F and M | 1 year | n = 58 LC n = 57 HC | 35–68 years | LC: 28% proteins, 58% fat, 14% carbs HC: 17% proteins, 15% fat, 53% carbs | POMS BDI SAI PAID D-39 | Improvements in psychosocial measures (POMS, BDI and PAID) after 1 year, with no differences between groups |
| Authors | Rosen 1982 [51] | Rosen 1985 [52] | Halyburton 2007 [27] | Galletly 2007 [53] | Brinkworth 2009 [55] | Dalle Grave 2013 [56] | Saslow 2014 [54] | Brinkworth 2016 [57] |
|---|---|---|---|---|---|---|---|---|
| Was the method of randomization to groups appropriate? | + | + | + | + | + | + | + | + |
| Was the allocation sequence concealed from those assigning patients to groups? | nr | nr | nr | nr | nr | nr | + | + |
| Was the outcome measurement performed in the same manner with similar intensity in all groups being compared? | + | + | + | + | + | + | + | + |
| Were similarly trained individuals administering the intervention across groups? | + | + | + | + | + | + | + | + |
| Were all the withdrawals described? | − | − | + | − | + | + | − | + |
| Were all originally randomized participants analysed in the groups they were assigned to (i.e., an intention-to-treat analysis)? | − | − | + | − | + | + | + | + |
| Was clustering at the group level accounted for in the analyses? | − | − | nr | nr | nr | nr | − | + |
| Were the groups similar at baseline? | nr | + | + | + | + | + | + | + |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
El Ghoch, M.; Calugi, S.; Dalle Grave, R. The Effects of Low-Carbohydrate Diets on Psychosocial Outcomes in Obesity/Overweight: A Systematic Review of Randomized, Controlled Studies. Nutrients 2016, 8, 402. https://doi.org/10.3390/nu8070402
El Ghoch M, Calugi S, Dalle Grave R. The Effects of Low-Carbohydrate Diets on Psychosocial Outcomes in Obesity/Overweight: A Systematic Review of Randomized, Controlled Studies. Nutrients. 2016; 8(7):402. https://doi.org/10.3390/nu8070402
Chicago/Turabian StyleEl Ghoch, Marwan, Simona Calugi, and Riccardo Dalle Grave. 2016. "The Effects of Low-Carbohydrate Diets on Psychosocial Outcomes in Obesity/Overweight: A Systematic Review of Randomized, Controlled Studies" Nutrients 8, no. 7: 402. https://doi.org/10.3390/nu8070402
APA StyleEl Ghoch, M., Calugi, S., & Dalle Grave, R. (2016). The Effects of Low-Carbohydrate Diets on Psychosocial Outcomes in Obesity/Overweight: A Systematic Review of Randomized, Controlled Studies. Nutrients, 8(7), 402. https://doi.org/10.3390/nu8070402







