Assessing Performance of Contemporary Plant-Based Diets against the UK Dietary Guidelines: Findings from the Feeding the Future (FEED) Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Recruitment
2.2. Survey
2.3. Database
2.4. Intakes
2.5. Dietary and Nutritional Guidelines
2.6. Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A

Appendix B
Appendix B.1. Additional Foods
Appendix B.2. Missing Values
Appendix B.3. Mapping
References
- Stewart, C.; Piernas, C.; Cook, B.; Jebb, S.A. Trends in UK meat consumption: Analysis of data from years 1-11 (2008-09 to 2018-19) of the National Diet and Nutrition Survey rolling programme. Lancet Planet Health 2021, 5, e699–e708. [Google Scholar] [CrossRef] [PubMed]
- YouGov. Dietary Choices of Brits (e.g., Vegeterian, Flexitarian, Meat-Eater etc.)? 2023. Available online: https://yougov.co.uk/topics/society/trackers/dietery-choices-of-brits-eg-vegeterian-flexitarian-meat-eater-etc (accessed on 25 March 2024).
- Scarborough, P.; Clark, M.; Cobiac, L.; Papier, K.; Knuppel, A.; Lynch, J.; Harrington, R.; Key, T.; Springmann, M. Vegans, vegetarians, fish-eaters and meat-eaters in the UK show discrepant environmental impacts. Nat. Food 2023, 4, 565–574. [Google Scholar] [CrossRef]
- Key, T.J.; Papier, K.; Tong, T.Y.N. Plant-based diets and long-term health: Findings from the EPIC-Oxford study. Proc. Nutr. Soc. 2022, 81, 190–198. [Google Scholar] [CrossRef] [PubMed]
- Orlich, M.J.; Singh, P.N.; Sabaté, J.; Jaceldo-Siegl, K.; Fan, J.; Knutsen, S.; Beeson, W.L.; Fraser, G.E. Vegetarian dietary patterns and mortality in Adventist Health Study 2. JAMA Intern. Med. 2013, 173, 1230–1238. [Google Scholar] [CrossRef] [PubMed]
- Davey, G.K.; Spencer, E.A.; Appleby, P.N.; Allen, N.E.; Knox, K.H. Key TJEPIC-Oxford: Lifestyle characteristics and nutrient intakes in a cohort of 33 883 meat-eaters 31 546 non meat-eaters in the, U.K. Public Health Nutr. 2003, 6, 259–269. [Google Scholar] [CrossRef] [PubMed]
- Alae-Carew, C.; Green, R.; Stewart, C.; Cook, B.; Dangour, A.D.; Scheelbeek, P.F.D. The role of plant-based alternative foods in sustainable and healthy food systems: Consumption trends in the UK. Sci. Total Environ. 2022, 807 Pt 3, 151041. [Google Scholar] [CrossRef] [PubMed]
- Sainsbury’s. Future of Food Report 2019. Available online: https://www.about.sainsburys.co.uk/~/media/Files/S/Sainsburys/pdf-downloads/future-of-food-08.pdf (accessed on 25 March 2024).
- Hercberg, S.; Castetbon, K.; Czernichow, S.; Malon, A.; Mejean, C.; Kesse, E.; Touvier, M.; Galan, P. The Nutrinet-Santé Study: A web-based prospective study on the relationship between nutrition and health and determinants of dietary patterns and nutritional status. BMC Public Health 2010, 10, 242. [Google Scholar] [CrossRef] [PubMed]
- Lapointe, A.; Laramée, C.; Belanger-Gravel, A.; Buckeridge, D.L.; Desroches, S.; Garriguet, D.; Gauvin, L.; Lemieux, S.; Plante, C.; Lamarche, B. NutriQuébec: A unique web-based prospective cohort study to monitor the population’s eating and other lifestyle behaviours in the province of Québec. BMJ Open 2020, 10, e039889. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.; Young, H.; Crowe, F.L.; Benson, V.S.; Spencer, E.A.; Key, T.J.; Appleby, P.N.; Beral, V. Development and evaluation of the Oxford WebQ, a low-cost, web-based method for assessment of previous 24 h dietary intakes in large-scale prospective studies. Public Health Nutr. 2011, 14, 1998–2005. [Google Scholar] [CrossRef]
- Fallaize, R.; Forster, H.; Macready, A.L.; Walsh, M.C.; Mathers, J.C.; Brennan, L.; Gibney, E.R.; Gibney, M.J.; A Lovegrove, J. Online dietary intake estimation: Reproducibility and validity of the Food4Me food frequency questionnaire against a 4-day weighed food record. J. Med. Internet Res. 2014, 16, e190. [Google Scholar] [CrossRef]
- Forster, H.; Fallaize, R.; Gallagher, C.; O’donovan, C.B.; Woolhead, C.; Walsh, M.C.; Macready, A.L.; A Lovegrove, J.; Mathers, J.C.; Gibney, M.J.; et al. Online dietary intake estimation: The Food4Me food frequency questionnaire. J. Med. Internet Res. 2014, 16, e150. [Google Scholar] [CrossRef] [PubMed]
- Foster, E.; Lee, C.; Imamura, F.; Hollidge, S.E.; Westgate, K.L.; Venables, M.C.; Poliakov, I.; Rowland, M.K.; Osadchiy, T.; Bradley, J.C.; et al. Validity and reliability of an online self-report 24-h dietary recall method (Intake24): A doubly labelled water study and repeated-measures analysis. J. Nutr. Sci. 2019, 8, e29. [Google Scholar] [CrossRef] [PubMed]
- Wark, P.A.; Hardie, L.J.; Frost, G.S.; Alwan, N.A.; Carter, M.; Elliott, P.; Ford, H.E.; Hancock, N.; Morris, M.A.; Mulla, U.Z.; et al. Validity of an online 24-h recall tool (myfood24) for dietary assessment in population studies: Comparison with biomarkers and standard interviews. BMC Med. 2018, 16, 136. [Google Scholar] [CrossRef] [PubMed]
- Office for National Statistics. Internet Users, UK 2020. 2021. Available online: https://www.ons.gov.uk/businessindustryandtrade/itandinternetindustry/bulletins/internetusers/2020 (accessed on 25 March 2024).
- Bingham, S.A.; Cassidy, A.; Cole, T.J.; Welch, A.; Runswick, S.A.; Black, A.E.; Thurnham, D.; Bates, C.; Khaw, K.T.; Key, T.J.A.; et al. Validation of weighed records and other methods of dietary assessment using the 24 h urine nitrogen technique and other biological markers. Br. J. Nutr. 1995, 73, 531–550. [Google Scholar] [CrossRef]
- Bingham, S.A.; Gill, C.; Welch, A.; Day, K.; Cassidy, A.; Khaw, K.T.; Sneyd, M.J.; Key, T.J.; Roe, L.; Day, N.E. Comparison of dietary assessment methods in nutritional epidemiology: Weighed records v. 24 h recalls, food-frequency questionnaires and estimated-diet records. Br. J. Nutr. 1994, 72, 619–643. [Google Scholar] [CrossRef] [PubMed]
- Bingham, S.A.; Gill, C.; Welch, A.; Cassidy, A.; Runswick, S.A.; Oakes, S.; Lubin, R.; Thurnham, D.I.; Key, T.J.; Roe, L.; et al. Validation of dietary assessment methods in the UK arm of EPIC using weighed records, and 24-h urinary nitrogen and potassium and serum vitamin C and carotenoids as biomarkers. Int. J. Epidemiol. 1997, 26 (Suppl. 1), S137. [Google Scholar] [CrossRef] [PubMed]
- Amoutzopoulos, B.; Steer, T.; Roberts, C.; Collins, D.; Trigg, K.; Barratt, R.; Abraham, S.; Cole, D.J.; Mulligan, A.; Foreman, J.; et al. Rationalisation of the UK Nutrient Databank for Incorporation in a Web-Based Dietary Recall for Implementation in the UK National Diet and Nutrition Survey Rolling Programme. Nutrients 2022, 14, 4551. [Google Scholar] [CrossRef] [PubMed]
- UK_NDB_1.2. Available on Request. 2023. [email protected]
- Roe, M.; Pinchen, H.; Church, S.; Finglas, P. McCance and Widdowson’s the composition of foods seventh summary edition and updated composition of foods integrated dataset. Nutr. Bull. 2015, 40, 36–39. [Google Scholar] [CrossRef]
- Harrington, R.A.; Adhikari, V.; Rayner, M.; Scarborough, P. Nutrient composition databases in the age of big data: FoodDB, a comprehensive, real-time database infrastructure. BMJ Open 2019, 9, e026652. [Google Scholar] [CrossRef] [PubMed]
- Perez-Cornago, A.; Pollard, Z.; Young, H.; van Uden, M.; Andrews, C.; Piernas, C.; Key, T.J.; Mulligan, A.; Lentjes, M. Description of the updated nutrition calculation of the Oxford WebQ questionnaire and comparison with the previous version among 207,144 participants in UK Biobank. Eur. J. Nutr. 2021, 60, 4019–4030. [Google Scholar] [CrossRef]
- Crawley, H. Food Portion Sizes; Ministry of Agriculture, Fisheries, and Food; HM Stationery Office: London, UK, 1988. [Google Scholar]
- Department of Health. Dietary Reference Values for Food Energy and Nutrients for the United Kingdom: Report of the Panel on Dietary Reference Values of the Committee on Medical Aspects of Food Policy; HM Stationery Office: London, UK, 1991.
- Food and Nutrition Board Institute of Medicine. Dietary Reference Intakes for Vitamin C, Vitamin E, Selenium and Carotenoids; National Academy Press: Washington, DC, USA, 2000.
- Trumbo, P.; Yates, A.A.; Schlicker, S.; Poos, M. Dietary reference intakes: Vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. J. Am. Diet. Assoc. 2001, 101, 294–301. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids; The National Academies Press: Washington, DC, USA, 2005.
- Scientific Advisory Committee on Nutrition. Carbohydrates and Health. 2015. Available online: https://assets.publishing.service.gov.uk/media/5a7f7cc3ed915d74e622ac2a/SACN_Carbohydrates_and_Health.pdf (accessed on 25 March 2024).
- Scientific Advisory Committee on Nutrition. Salt and Health. 2003. Available online: https://assets.publishing.service.gov.uk/media/5a74983de5274a44083b7ef6/SACN_Salt_and_Health_report.pdf (accessed on 25 March 2024).
- Institute of Medicine; Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. DRI Dietary Reference Intakes: Applications in Dietary Assessment; National Academies Press: Washington DC, USA, 2000. [Google Scholar]
- Willett, W. Nutritional Epidemiology; Oxford University Press: Oxford, UK, 2012. [Google Scholar]
- Tonstad, S.; Butler, T.; Yan, R.; Fraser, G.E. Type of vegetarian diet, body weight, and prevalence of type 2 diabetes. Diabetes Care 2009, 32, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Bradbury, K.E.; Tong, T.Y.N.; Key, T.J. Dietary Intake of High-Protein Foods and Other Major Foods in Meat-Eaters, Poultry-Eaters, Fish-Eaters, Vegetarians, and Vegans in UK Biobank. Nutrients 2017, 9, 1317. [Google Scholar] [CrossRef] [PubMed]
- Spencer, E.A.; Appleby, P.N.; Davey, G.K.; Key, T.J. Diet and body mass index in 38000 EPIC-Oxford meat-eaters, fish-eaters, vegetarians and vegans. Int. J. Obes. Relat. Metab. Disord. 2003, 27, 728–734. [Google Scholar] [CrossRef] [PubMed]
- Greenwood, D.C.; Cade, J.E.; Draper, A.; Barrett, J.H.; Calvert, C.; Greenhalgh, A. Seven unique food consumption patterns identified among women in the UK Women’s Cohort Study. Eur. J. Clin. Nutr. 2000, 54, 314–320. [Google Scholar] [CrossRef] [PubMed]
- Spencer, E.A.; Appleby, P.N.; Davey, G.K.; Key, T.J. Validity of self-reported height and weight in 4808 EPIC-Oxford participants. Public Health Nutr. 2002, 5, 561–565. [Google Scholar] [CrossRef]
- Bes-Rastrollo, M.; Sabate, J.; Jaceldo-Siegl, K.; Fraser, G.E. Validation of self-reported anthropometrics in the Adventist Health Study 2. BMC Public Health 2011, 11, 213. [Google Scholar] [CrossRef] [PubMed]
- Papier, K.; Tong, T.Y.; Appleby, P.N.; Bradbury, K.E.; Fensom, G.K.; Knuppel, A.; Perez-Cornago, A.; Schmidt, J.A.; Travis, R.C.; Key, T.J. Comparison of Major Protein-Source Foods and Other Food Groups in Meat-Eaters and Non-Meat-Eaters in the EPIC-Oxford Cohort. Nutrients 2019, 11, 824. [Google Scholar] [CrossRef]
- Lehto, E.; Kaartinen, N.E.; Saaksjarvi, K.; Mannisto, S.; Jallinoja, P. Vegetarians and different types of meat eaters among the Finnish adult population from 2007 to 2017. Br. J. Nutr. 2022, 127, 1060–1072. [Google Scholar] [CrossRef]
- Dagevos, H. Finding flexitarians: Current studies on meat eaters and meat reducers. Trends Food Sci. Technol. 2021, 114, 530–539. [Google Scholar] [CrossRef]
- Peschel, A.O.; Grebitus, C. Flexitarians’ and meat eaters’ heterogeneous preferences for beef: Gourmets and value seekers. Food Qual. Prefer. 2023, 104, 104756. [Google Scholar] [CrossRef]
- Sobiecki, J.G.; Appleby, P.N.; Bradbury, K.E.; Key, T.J. High compliance with dietary recommendations in a cohort of meat eaters, fish eaters, vegetarians, and vegans: Results from the European Prospective Investigation into Cancer and Nutrition-Oxford study. Nutr. Res. 2016, 36, 464–477. [Google Scholar] [CrossRef] [PubMed]
- Rizzo, N.S.; Jaceldo-Siegl, K.; Sabate, J.; Fraser, G.E. Nutrient profiles of vegetarian and nonvegetarian dietary patterns. J. Acad. Nutr. Diet. 2013, 113, 1610–1619. [Google Scholar] [CrossRef] [PubMed]
- Neufingerl, N.; Eilander, A. Nutrient Intake and Status in Adults Consuming Plant-Based Diets Compared to Meat-Eaters: A Systematic Review. Nutrients 2021, 14, 29. [Google Scholar] [CrossRef] [PubMed]
- Public Health England. NDNS: Results from Years 9 to 11 (Combined)—Statistical Summary 2020. Available online: https://www.gov.uk/government/statistics/ndns-results-from-years-9-to-11-2016-to-2017-and-2018-to-2019/ndns-results-from-years-9-to-11-combined-statistical-summary (accessed on 25 March 2024).
- Bakaloudi, D.R.; Halloran, A.; Rippin, H.L.; Oikonomidou, A.C.; Dardavesis, T.I.; Williams, J.; Wickramasinghe, K.; Breda, J.; Chourdakis, M. Intake and adequacy of the vegan diet. A systematic review of the evidence. Clin. Nutr. 2021, 40, 3503–3521. [Google Scholar] [CrossRef] [PubMed]
- Stoffaneller, R.; Morse, N.L. A Review of Dietary Selenium Intake and Selenium Status in Europe and the Middle East. Nutrients 2015, 7, 1494–1537. [Google Scholar] [CrossRef] [PubMed]
- Gibson, R.S.; Perlas, L.; Hotz, C. Improving the bioavailability of nutrients in plant foods at the household level. Proc. Nutr. Soc. 2006, 65, 160–168. [Google Scholar] [CrossRef]
- Gibson, R.S.; Bailey, K.B.; Gibbs, M.; Ferguson, E.L. A review of phytate, iron, zinc, and calcium concentrations in plant-based complementary foods used in low-income countries and implications for bioavailability. Food Nutr. Bull. 2010, 31 (Suppl. S2), S134–S146. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.; Lovegrove, J.; Givens, D. Food fortification and biofortification as potential strategies for prevention of vitamin D deficiency. Nutr. Bull. 2019, 44, 36–42. [Google Scholar] [CrossRef]
- Wilson, L.R.; Tripkovic, L.; Hart, K.H.; Lanham-New, S.A. Vitamin D deficiency as a public health issue: Using vitamin D2 or vitamin D3 in future fortification strategies. Proc. Nutr. Soc. 2017, 76, 392–399. [Google Scholar] [CrossRef]
- Crowe, F.L.; Steur, M.; Allen, N.E.; Appleby, P.N.; Travis, R.C.; Key, T.J. Plasma concentrations of 25-hydroxyvitamin D in meat eaters, fish eaters, vegetarians and vegans: Results from the EPIC-Oxford study. Public Health Nutr. 2011, 14, 340–346. [Google Scholar] [CrossRef] [PubMed]
- Clegg, M.E.; Tarrado Ribes, A.; Reynolds, R.; Kliem, K.; Stergiadis, S. A comparative assessment of the nutritional composition of dairy and plant-based dairy alternatives available for sale in the UK and the implications for consumers’ dietary intakes. Food Res. Int. 2021, 148, 110586. [Google Scholar] [CrossRef] [PubMed]
- Nicol, K.; Thomas, E.L.; Nugent, A.P.; Woodside, J.V.; Hart, K.H.; Bath, S.C. Iodine fortification of plant-based dairy and fish alternatives: The effect of substitution on iodine intake based on a market survey in the UK. Br. J. Nutr. 2023, 129, 832–842. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Martin, B.R.; Weaver, C.M. Calcium bioavailability of calcium carbonate fortified soymilk is equivalent to cow’s milk in young women. J. Nutr. 2005, 135, 2379–2382. [Google Scholar] [CrossRef] [PubMed]
- Peacock, M. Calcium metabolism in health and disease. Clin. J. Am. Soc. Nephrol. 2010, 5 (Suppl. 1), S23–S30. [Google Scholar] [CrossRef]
- Vaisman, N.; Shaltiel, G.; Daniely, M.; Meiron, O.E.; Shechter, A.; Abrams, S.A.; Niv, E.; Shapira, Y.; Sagi, A. Increased Calcium Absorption from Synthetic Stable Amorphous Calcium Carbonate: Double-Blind Randomized Crossover Clinical Trial in Postmenopausal Women. J. Bone Miner. Res. 2014, 29, 2203–2209. [Google Scholar] [CrossRef] [PubMed]
- Damayanti, D.; Jaceldo-Siegl, K.; Beeson, W.L.; Fraser, G.; Oda, K.; Haddad, E.H. Foods and Supplements Associated with Vitamin B(12) Biomarkers among Vegetarian and Non-Vegetarian Participants of the Adventist Health Study-2 (AHS-2) Calibration Study. Nutrients 2018, 10, 722. [Google Scholar] [CrossRef]
- Bath, S.C.; Hill, S.; Infante, H.G.; Elghul, S.; Nezianya, C.J.; Rayman, M.P. Iodine concentration of milk-alternative drinks available in the UK in comparison with cows’ milk. Br. J. Nutr. 2017, 118, 525–532. [Google Scholar] [CrossRef]
- Bath, S.C.; Rayman, M.P. Dairy Foods as a Source of Dietary Iodine. Milk and Dairy Foods; Elsevier: Oxford, UK, 2020; pp. 323–345. [Google Scholar]
- Van der Reijden, O.L.; Zimmermann, M.B.; Galetti, V. Iodine in dairy milk: Sources, concentrations and importance to human health. Best Pract. Res. Clin. Endocrinol. Metab. 2017, 31, 385–395. [Google Scholar] [CrossRef]
- Department of Health and Social Care. Folic Acid Added to Flour to Prevent Spinal Conditions in Babies 2021. Available online: https://www.gov.uk/government/news/folic-acid-added-to-flour-to-prevent-spinal-conditions-in-babies (accessed on 25 March 2024).
- Department of Health Committee on Medical Aspects of Food Policy. The Fortification of Yellow Fats with Vitamins A and D. Report on Health and Social Subjects; HM Stationery Office: London, UK, 1991.
- Bird, J.K.; Barron, R.; Pigat, S.; Bruins, M.J. Contribution of base diet, voluntary fortified foods and supplements to micronutrient intakes in the UK. J. Nutr. Sci. 2022, 11, e51. [Google Scholar] [CrossRef]
- Hebert, J.R.; Ma, Y.; Clemow, L.; Ockene, I.S.; Saperia, G.; Stanek, E.J., 3rd; Merriam, P.A.; Ockene, J.K. Gender differences in social desirability and social approval bias in dietary self-report. Am. J. Epidemiol. 1997, 146, 1046–1055. [Google Scholar] [CrossRef] [PubMed]
- Danish Food Composition Database [Internet]. 2019. Available online: https://frida.fooddata.dk/ (accessed on 25 March 2024).

| Omnivorous | Flexitarian | Pescatarian | Vegetarian | Vegan | All | p-Value | |
|---|---|---|---|---|---|---|---|
| N | 1562 (24.6%) | 1349 (21.3%) | 568 (9.0%) | 1292 (20.4%) | 1571 (24.8%) | 6342 (100.0%) | |
| Length following diet | |||||||
| <1 year | 56 (3.6%) | 90 (6.7%) | 23 (4.0%) | 23 (1.8%) | 106 (6.7%) | 298 (4.7%) | <0.001 |
| 1–4 years | 161 (10.3%) | 386 (28.6%) | 138 (24.3%) | 148 (11.5%) | 572 (36.4%) | 1405 (22.2%) | |
| 5–19 years | 154 (9.9%) | 463 (34.3%) | 154 (27.1%) | 212 (16.4%) | 648 (41.2%) | 1631 (25.7%) | |
| 20+ years | 1191 (76.2%) | 410 (30.4%) | 253 (44.5%) | 909 (70.4%) | 245 (15.6%) | 3008 (47.4%) | |
| Age (years) | 52.8 ± 14.6 | 52.0 ± 16.9 | 53.3 ± 16.3 | 53.0 ± 16.2 | 48.1 ± 15.2 | 51.5 ± 15.9 | <0.001 |
| Gender | |||||||
| Female | 1243 (79.6%) | 1153 (85.5%) | 493 (86.8%) | 1060 (82.0%) | 1167 (74.3%) | 5116 (80.7%) | |
| Male | 310 (19.8%) | 176 (13.0%) | 71 (12.5%) | 216 (16.7%) | 353 (22.5%) | 1126 (17.8%) | <0.001 |
| Prefer not to say | 9 (0.6%) | 20 (1.5%) | 4 (0.7%) | 16 (1.2%) | 51 (3.2%) | 100 (1.6%) | |
| BMI (kg/m2) | 30.0 ± 7.0 | 27.5 ± 6.2 | 28.0 ± 6.2 | 28.7 ± 6.6 | 27.5 ± 6.2 | 28.4 ± 6.6 | <0.001 |
| Ethnicity | |||||||
| White | 1468 (94.0%) | 1254 (93.0%) | 536 (94.4%) | 1245 (96.4%) | 1482 (94.3%) | 5985 (94.4%) | 0.012 |
| Black | 4 (0.3%) | 10 (0.7%) | 5 (0.9%) | 3 (0.2%) | 4 (0.3%) | 26 (0.4%) | |
| Asian | 39 (2.5%) | 47 (3.5%) | 12 (2.1%) | 23 (1.8%) | 32 (2.0%) | 153 (2.4%) | |
| Other | 28 (1.8%) | 23 (1.7%) | 11 (1.9%) | 11 (0.9%) | 30 (1.9%) | 103 (1.6%) | |
| Do not want to disclose | 23 (1.5%) | 15 (1.1%) | 4 (0.7%) | 10 (0.8%) | 23 (1.5%) | 75 (1.2%) | |
| Overall health | |||||||
| Good or excellent | 1204 (77.1%) | 1077 (79.8%) | 456 (80.3%) | 969 (75.0%) | 1293 (82.3%) | 4999 (78.8%) | <0.001 |
| Fair | 308 (19.7%) | 232 (17.2%) | 98 (17.3%) | 258 (20.0%) | 217 (13.8%) | 1113 (17.5%) | |
| Poor | 47 (3.0%) | 38 (2.8%) | 14 (2.5%) | 59 (4.6%) | 54 (3.4%) | 212 (3.3%) | |
| Do not know/prefer not to say | 3 (0.2%) | 2 (0.1%) | 0 (0.0%) | 6 (0.5%) | 7 (0.4%) | 18 (0.3%) | |
| Ever smoked tobacco | |||||||
| No, never | 958 (61.3%) | 886 (65.7%) | 341 (60.0%) | 827 (64.0%) | 944 (60.1%) | 3956 (62.4%) | 0.004 |
| Yes, in the past | 524 (33.5%) | 422 (31.3%) | 202 (35.6%) | 428 (33.1%) | 558 (35.5%) | 2134 (33.6%) | |
| Yes, now | 80 (5.1%) | 41 (3.0%) | 25 (4.4%) | 37 (2.9%) | 69 (4.4%) | 252 (4.0%) | |
| Vigorous exercise in the last 12 months | |||||||
| No | 340 (21.8%) | 266 (19.7%) | 115 (20.2%) | 327 (25.3%) | 301 (19.2%) | 1349 (21.3%) | <0.001 |
| Yes | 1222 (78.2%) | 1083 (80.3%) | 453 (79.8%) | 965 (74.7%) | 1270 (80.8%) | 4993 (78.7%) | |
| Highest attained education | |||||||
| GCSEs * | 127 (8.1%) | 71 (5.3%) | 37 (6.5%) | 101 (7.8%) | 121 (7.7%) | 457 (7.2%) | <0.001 |
| A levels Ɨ | 225 (14.4%) | 155 (11.5%) | 73 (12.9%) | 221 (17.1%) | 273 (17.4%) | 947 (14.9%) | |
| University degree | 1163 (74.5%) | 1101 (81.6%) | 441 (77.6%) | 934 (72.3%) | 1128 (71.8%) | 4767 (75.2%) | |
| None | 12 (0.8%) | 7 (0.5%) | 7 (1.2%) | 16 (1.2%) | 17 (1.1%) | 59 (0.9%) | |
| Do not want to disclose | 35 (2.2%) | 15 (1.1%) | 10 (1.8%) | 20 (1.5%) | 32 (2.0%) | 112 (1.8%) | |
| Paid job at present | |||||||
| Yes | 961 (61.5%) | 792 (58.7%) | 332 (58.5%) | 729 (56.4%) | 1020 (64.9%) | 3834 (60.5%) | <0.001 |
| No | 131 (8.4%) | 108 (8.0%) | 48 (8.5%) | 127 (9.8%) | 197 (12.5%) | 611 (9.6%) | |
| Retired | 429 (27.5%) | 424 (31.4%) | 178 (31.3%) | 405 (31.3%) | 300 (19.1%) | 1736 (27.4%) | |
| Do not want to disclose | 41 (2.6%) | 25 (1.9%) | 10 (1.8%) | 31 (2.4%) | 54 (3.4%) | 161 (2.5%) | |
| Average total income before tax received by household | |||||||
| <GBP 18,000-GBP 49,999 | 673 (43.1%) | 624 (46.3%) | 258 (45.4%) | 586 (45.4%) | 808 (51.4%) | 2949 (46.5%) | <0.001 |
| GBP 50,000–GBP 100,000 | 585 (37.5%) | 474 (35.1%) | 197 (34.7%) | 396 (30.7%) | 460 (29.3%) | 2112 (33.3%) | |
| Do not want to disclose | 304 (19.5%) | 251 (18.6%) | 113 (19.9%) | 310 (24.0%) | 303 (19.3%) | 1281 (20.2%) | |
| Region | |||||||
| England | |||||||
| East Midlands | 205 (13.2%) | 130 (9.7%) | 73 (12.9%) | 161 (12.5%) | 210 (13.4%) | 779 (12.3%) | <0.001 |
| Greater London | 131 (8.4%) | 207 (15.5%) | 81 (14.3%) | 157 (12.2%) | 191 (12.2%) | 767 (12.2%) | |
| North East | 82 (5.3%) | 55 (4.1%) | 39 (6.9%) | 88 (6.8%) | 109 (7.0%) | 373 (5.9%) | |
| North West | 109 (7.0%) | 92 (6.9%) | 38 (6.7%) | 131 (10.2%) | 169 (10.8%) | 539 (8.5%) | |
| South East | 542 (34.9%) | 442 (33.0%) | 163 (28.8%) | 320 (24.8%) | 349 (22.3%) | 1816 (28.8%) | |
| South West | 189 (12.2%) | 180 (13.5%) | 78 (13.8%) | 150 (11.6%) | 217 (13.9%) | 814 (12.9%) | |
| West Midlands | 125 (8.0%) | 94 (7.0%) | 36 (6.4%) | 117 (9.1%) | 112 (7.2%) | 484 (7.7%) | |
| Northern Ireland | 12 (0.8%) | 7 (0.5%) | 3 (0.5%) | 13 (1.0%) | 19 (1.2%) | 54 (0.9%) | |
| Scotland | 93 (6.0%) | 85 (6.4%) | 29 (5.1%) | 100 (7.8%) | 95 (6.1%) | 402 (6.4%) | |
| Wales | 66 (4.2%) | 46 (3.4%) | 26 (4.6%) | 52 (4.0%) | 91 (5.8%) | 281 (4.5%) | |
| (a) | ||||||
| Omnivorous | Flexitarian | Pescatarian | Vegetarian | Vegan | p-Value | |
| N | 1243 (24.3%) | 1153 (22.5%) | 493 (9.6%) | 1060 (20.7%) | 1167 (22.8%) | |
| Meat (g/day) | 132.6 ± 112.9 | 46.5 ± 29.8 | 1.0 ± 6.7 | 0.0 ± 0.7 | 0.1 ± 1.0 | <0.001 |
| Fish (g/day) | 51.0 ± 29.8 | 48.8 ± 30.8 | 52.8 ± 33.0 | 1.0 ± 4.7 | 0.4 ± 3.8 | <0.001 |
| Plant-based meat alternatives (g/day) | 10.9 ± 14.8 | 30.8 ± 30.5 | 50.3 ± 37.4 | 59.1 ± 40.4 | 73.3 ± 47.4 | <0.001 |
| Eggs (g/day) | 46.0 ± 53.1 | 32.7 ± 39.1 | 37.2 ± 53.8 | 33.0 ± 47.9 | 0.6 ± 5.4 | <0.001 |
| Milk (mL/day) | 188.0 ± 159.4 | 142.1 ± 146.6 | 114.9 ± 138.8 | 99.8 ± 132.2 | 0.6 ± 10.0 | <0.001 |
| Plant-based milk alternatives (mL/day) | 36.2 ± 88.5 | 83.7 ± 121.6 | 112.9 ± 140.5 | 120.5 ± 141.9 | 225.9 ± 159.7 | <0.001 |
| Cheese (g/day) | 20.7 ± 20.6 | 16.9 ± 14.2 | 16.4 ± 14.4 | 19.4 ± 19.0 | 0.1 ± 1.4 | <0.001 |
| Plant-based cheese alternatives (g/day) | 0.5 ± 3.5 | 0.9 ± 2.7 | 1.6 ± 4.1 | 2.5 ± 4.8 | 8.3 ± 9.3 | <0.001 |
| Yogurt (g/day) | 50.9 ± 54.0 | 55.9 ± 62.6 | 48.9 ± 54.6 | 42.6 ± 52.8 | 0.3 ± 4.7 | <0.001 |
| Plant-based yogurt alternatives (g/day) | 2.7 ± 15.1 | 7.7 ± 23.8 | 9.4 ± 25.1 | 14.2 ± 31.1 | 37.0 ± 47.4 | <0.001 |
| Pulses (g/day) | 35.8 ± 31.2 | 59.0 ± 42.0 | 70.1 ± 47.7 | 72.2 ± 44.2 | 104.5 ± 66.6 | <0.001 |
| Nuts/seeds (g/day) | 16.3 ± 21.5 | 22.4 ± 23.4 | 23.8 ± 24.5 | 23.2 ± 23.4 | 34.0 ± 31.6 | <0.001 |
| Grains (g/day) | 221.9 ± 143.4 | 284.8 ± 126.7 | 294.4 ± 124.9 | 289.4 ± 123.6 | 314.8 ± 133.0 | <0.001 |
| Vegetables (g/day) | 353.1 ± 207.0 | 406.1 ± 215.4 | 415.6 ± 213.4 | 385.2 ± 208.6 | 459.6 ± 247.9 | <0.001 |
| Fruit (g/day) | 185.4 ± 149.9 | 249.4 ± 170.2 | 234.8 ± 158.1 | 220.8 ± 148.1 | 254.5 ± 197.9 | <0.001 |
| Confectionery (g/day) | 59.7 ± 50.1 | 62.8 ± 47.2 | 60.7 ± 46.3 | 69.1 ± 45.4 | 52.4 ± 37.9 | <0.001 |
| Protein shakes/bars (g/day) | 1.6 ± 7.8 | 1.8 ± 7.9 | 1.7 ± 6.6 | 2.0 ± 8.5 | 3.7 ± 12.9 | <0.001 |
| Meal replacements (g/day) | 1.0 ± 9.7 | 1.2 ± 12.4 | 0.6 ± 5.4 | 1.5 ± 11.7 | 2.0 ± 12.9 | 0.139 |
| Tea/coffee (mL/day) | 631.2 ± 331.7 | 631.9 ± 314.2 | 625.0 ± 303.8 | 593.3 ± 317.7 | 581.8 ± 327.7 | <0.001 |
| Non-alcoholic drinks (mL/day) | 261.0 ± 365.6 | 194.2 ± 269.4 | 202.6 ± 292.8 | 249.1 ± 327.2 | 237.0 ± 310.6 | <0.001 |
| Alcoholic drinks (mL/day) | 93.6 ± 135.1 | 97.6 ± 115.6 | 103.9 ± 133.3 | 96.4 ± 123.6 | 80.2 ± 121.6 | 0.001 |
| (b) | ||||||
| Omnivorous | Flexitarian | Pescatarian | Vegetarian | Vegan | p-Value | |
| N | 310 (27.5%) | 176 (15.6%) | 71 (6.3%) | 216 (19.2%) | 353 (31.3%) | |
| Meat (g/day) | 158.9 ± 134.9 | 49.0 ± 30.1 | 2.6 ± 10.7 | 0.5 ± 4.6 | 0.2 ± 2.7 | <0.001 |
| Fish (g/day) | 56.3 ± 69.6 | 48.7 ± 39.4 | 67.8 ± 56.0 | 0.7 ± 4.1 | 0.4 ± 3.5 | <0.001 |
| Plant-based meat alternatives (g/day) | 10.7 ± 17.8 | 36.0 ± 35.6 | 53.1 ± 38.6 | 71.0 ± 48.8 | 84.1 ± 54.7 | <0.001 |
| Eggs (g/day) | 55.4 ± 64.1 | 32.5 ± 39.5 | 39.1 ± 44.3 | 40.1 ± 62.7 | 1.4 ± 15.3 | <0.001 |
| Milk (mL/day) | 232.0 ± 191.5 | 151.3 ± 160.3 | 124.6 ± 165.3 | 126.7 ± 141.8 | 1.9 ± 25.5 | <0.001 |
| Plant-based milk alternatives (mL/day) | 24.4 ± 81.9 | 73.7 ± 120.9 | 113.0 ± 158.3 | 114.6 ± 156.5 | 233.1 ± 166.7 | <0.001 |
| Cheese (g/day) | 21.7 ± 21.5 | 17.8 ± 17.1 | 19.6 ± 23.3 | 20.4 ± 17.5 | 0.1 ± 1.4 | <0.001 |
| Plant-based cheese alternatives (g/day) | 0.3 ± 1.5 | 1.3 ± 4.7 | 1.6 ± 4.7 | 2.7 ± 4.8 | 8.5 ± 10.4 | <0.001 |
| Yogurt (g/day) | 43.2 ± 51.3 | 51.3 ± 56.2 | 49.0 ± 75.8 | 44.8 ± 49.2 | 0.6 ± 7.5 | <0.001 |
| Plant-based yogurt alternatives (g/day) | 1.5 ± 10.7 | 7.7 ± 23.3 | 8.4 ± 19.4 | 8.7 ± 19.0 | 32.3 ± 50.7 | <0.001 |
| Pulses (g/day) | 33.6 ± 31.1 | 57.4 ± 46.0 | 92.5 ± 102.7 | 73.5 ± 44.4 | 126.6 ± 101.3 | <0.001 |
| Nuts/seeds (g/day) | 15.1 ± 20.3 | 26.2 ± 29.0 | 27.6 ± 23.2 | 24.3 ± 24.9 | 40.9 ± 39.0 | <0.001 |
| Grains (g/day) | 252.2 ± 165.2 | 322.0 ± 142.4 | 362.2 ± 182.8 | 348.0 ± 131.7 | 379.5 ± 180.8 | <0.001 |
| Vegetables (g/day) | 291.4 ± 203.3 | 339.7 ± 160.7 | 413.2 ± 220.1 | 367.5 ± 185.6 | 433.5 ± 231.9 | <0.001 |
| Fruit (g/day) | 183.0 ± 168.5 | 259.8 ± 166.3 | 280.5 ± 200.3 | 240.4 ± 183.3 | 291.0 ± 224.7 | <0.001 |
| Confectionery (g/day) | 62.0 ± 58.1 | 62.3 ± 45.6 | 51.5 ± 36.1 | 68.2 ± 48.6 | 56.1 ± 50.2 | 0.037 |
| Protein shakes/bars (g/day) | 2.6 ± 9.9 | 4.7 ± 17.9 | 4.6 ± 17.1 | 1.8 ± 6.8 | 4.7 ± 13.2 | 0.031 |
| Meal replacements (g/day) | 2.2 ± 15.2 | 4.0 ± 27.7 | 1.4 ± 9.2 | 1.2 ± 10.5 | 7.2 ± 36.9 | 0.031 |
| Tea/coffee (mL/day) | 573.5 ± 346.0 | 625.9 ± 330.9 | 668.5 ± 295.6 | 640.9 ± 316.1 | 518.2 ± 346.6 | <0.001 |
| Non-alcoholic drinks (mL/day) | 294.1 ± 428.2 | 187.3 ± 233.6 | 177.0 ± 248.9 | 265.5 ± 301.0 | 237.0 ± 338.1 | 0.004 |
| Alcoholic drinks (mL/day) | 204.2 ± 286.8 | 194.2 ± 232.9 | 295.4 ± 390.3 | 186.1 ± 247.4 | 141.8 ± 222.2 | <0.001 |
| Omnivores | Flexitarians | Pescatarians | Vegetarians | Vegans | |
|---|---|---|---|---|---|
| Energy (kJ) | 9511 b | 9388 b | 9277 a,b | 9047 a | 9132 a |
| Energy/BMR ratio | 1.59 a,b | 1.63 b | 1.60 a,b | 1.55 a | 1.59 a |
| Energy/BMR ratio < 1.2 (%) | 18.1 a | 16.7 a | 18.1 a | 20.6 a | 20.0 a |
| Carbohydrate (%E) | 37.8 | 44.8 | 46.4 | 48.9 a | 49.2 a |
| Total sugars (%E) | 17.4 | 19.9 a | 20.1 a,b | 20.6 b | 20.2 a,b |
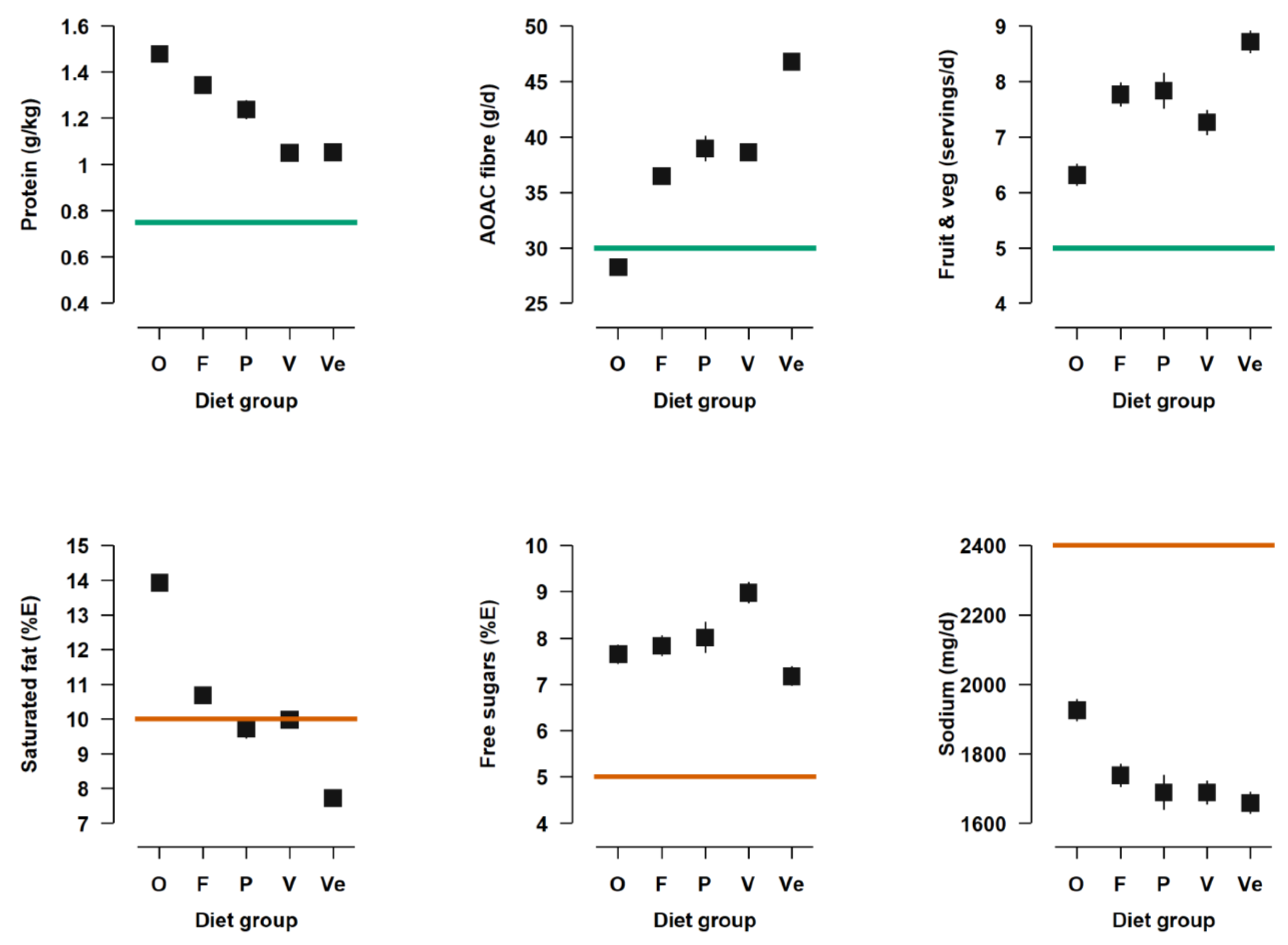
| Free sugars (%E) | 7.67 a,b | 7.85 b | 8.02 b | 8.99 | 7.40 a |
| Starch (%E) | 20.5 | 25.0 | 26.4 | 28.4 | 30.8 |
| Protein (%E) | 17.8 | 15.1 | 14.2 | 12.6 | 12.2 |
| Protein (g) per kg body weight | 1.49 | 1.34 | 1.24 | 1.06 a | 1.06 a |
| Fat (%E) | 40.4 | 36.2 b | 35.3 a,b | 34.8 a | 35.1 a |
| SFA (%E) | 14.2 | 10.9 | 9.9 a | 10.2 a | 7.9 |
| MUFA (%E) | 16.0 | 14.9 b | 14.7 a,b | 14.1 a | 14.9 b |
| PUFA (%E) | 6.5 | 7.0 | 7.4 a | 7.4 a | 9.2 |
| P/S ratio | 0.50 | 0.68 | 0.78 a | 0.76 a | 1.21 |
| Cholesterol (mg) | 415 | 248 | 217 | 168 | 20 |
| n-3 fatty acids (g) | 2.83 a | 2.80 a | 2.86 a | 2.35 | 2.83 a |
| n-6 fatty acids (g) | 13.8 | 15.1 a | 15.7 a,b | 15.9 b | 20.2 |
| Trans fatty acids (g) | 1.45 | 0.95 a | 0.77 a | 0.80 | 0.38 |
| Alcohol (%E) | 2.85 a | 2.85 a | 3.16 a | 2.72 a | 2.23 |
| Alcohol (g) | 9.38 a,b | 9.24 a,b | 10.26 b | 8.45 a | 6.98 |
| AOAC Fibre (g) | 28.4 | 36.7 | 39.3 a | 38.8 a | 46.7 |
| β-Carotene (μg) | 3668 | 4240 a | 4204 a | 4039 a | 4859 |
| Retinol (μg) | 997 | 466 | 272 a | 259 a | 102 |
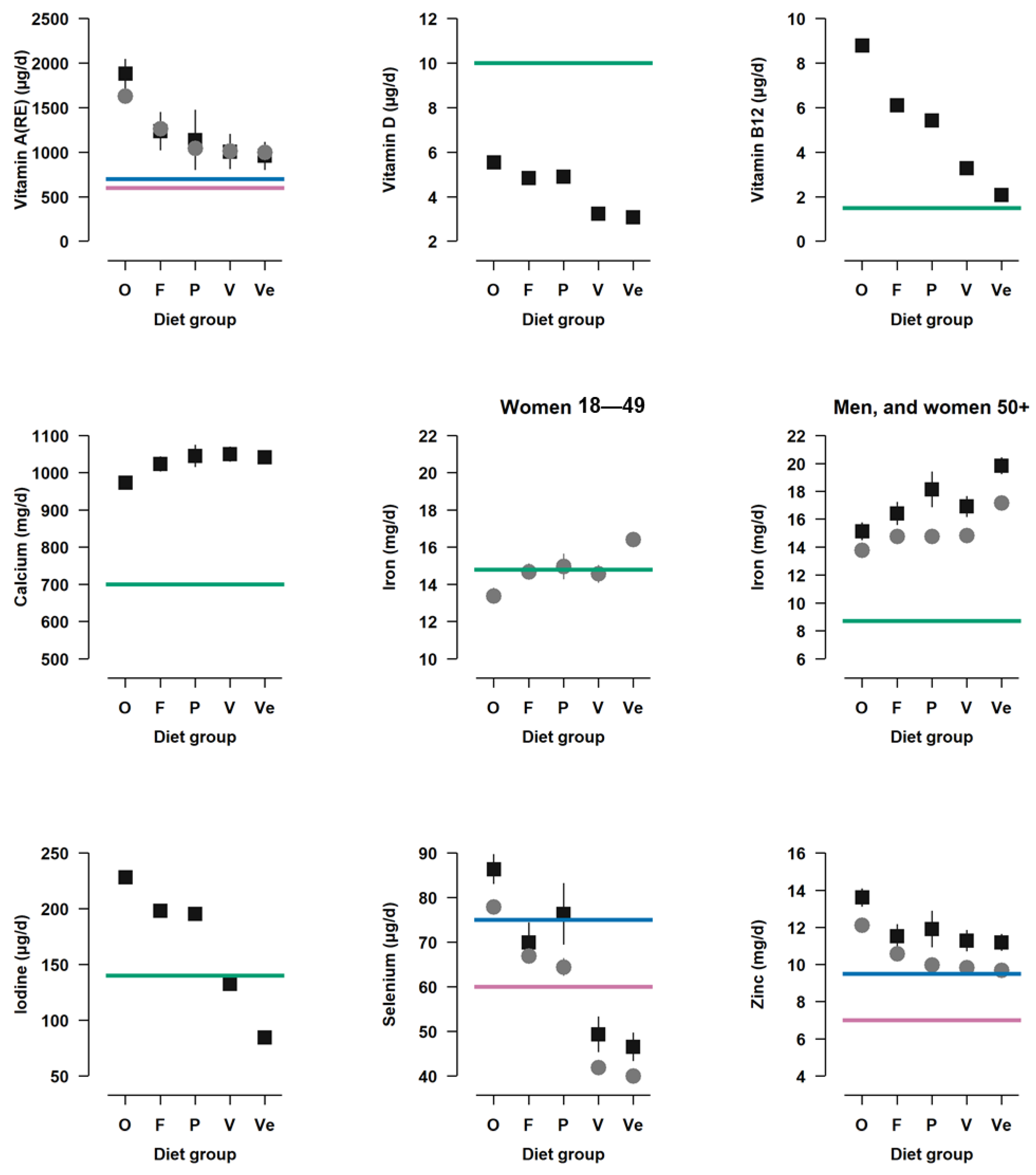
| Vitamin A (RE) (µg) | 1682 | 1261 | 1057 a | 1009 a | 989 a |
| Vitamin D (μg) | 5.57 | 4.82 a | 4.82 a | 3.07 | 2.60 |
| Thiamin (mg) | 2.07 | 2.19 a | 2.23 a,b | 2.28 b | 2.62 |
| Riboflavin (mg) | 2.26 | 2.03 b | 1.96 a,b | 1.94 a | 1.80 |
| Niacin equivalent (mg) | 47.0 | 40.2 | 36.9 | 31.9 | 33.3 |
| Vitamin C (mg) | 151 | 170 a | 175 a | 167 a | 193 |
| Vitamin E (mg) | 14.1 | 15.7 a | 16.7 b | 16.0 a,b | 18.7 |
| Vitamin B6 (mg) | 2.30 | 2.15 | 2.05 a | 1.90 | 2.04 a |
| Vitamin B12 (μg) | 9.78 | 6.49 | 5.55 | 3.35 | 2.04 |
| Folate (μg) | 362 | 401 a | 413 a | 411 a | 453 |
| Pantothenic acid (mg) | 8.25 | 7.42 | 6.90 | 6.42 | 5.84 |
| Biotin (µg) | 56.2 | 59.4 a | 61.4 a | 59.2 a | 67.4 |
| Sodium (mg) | 1973 | 1816 b | 1769 a,b | 1761 a,b | 1712 a |
| Potassium (mg) | 3923 a | 4072 b | 4085 b | 3836 a | 4144 b |
| Calcium (mg) | 976 | 1031 a | 1054 a | 1055 a | 1022 a |
| Magnesium (mg) | 363 | 414 a | 430 a | 413 a | 478 |
| Phosphorus (mg) | 1619 | 1557 b | 1537 b | 1420 a | 1397 a |
| Iron (mg) | 13.9 | 15.1 a | 15.4 a | 15.2 a | 17.6 |
| Haem iron (mg) | 1.05 | 0.49 | 0.30 | 0.16 | 0.18 a |
| Non-haem iron (mg) | 12.8 | 14.5 a | 15.1 a,b | 15.1 b | 17.3 |
| Copper (mg) | 1.80 a | 1.86 a | 1.86 a | 1.81 a | 2.20 |
| Zinc (mg) | 12.4 | 10.8 | 10.3 a | 10.1 a | 10.0 a |
| Chloride (mg) | 3472 | 3269 a,b | 3177 a | 3166 a | 3363 b |
| Iodine (μg) | 232 | 203 a | 200 a | 135 | 89 |
| Manganese (mg) | 4.23 | 5.64 | 6.12 a | 6.14 a | 7.37 |
| Selenium (μg) | 79.7 | 67.5 b | 66.4 b | 43.2 a | 41.3 a |
| Nutrient | EAR Value a | Omnivores | Flexitarians | Pescatarians | Vegetarians | Vegans | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| W | M | W | M | W | M | W | M | W | M | ||
| Protein | 0.66 g/kg of body weight b | 5.2% | 4.8% | 5.7% | 7.4% | 10.1% | 8.5% | 16.7% | 15.3% | 18.8% | 16.7% |
| Vitamin A (RE) | M: 500 µg, W: 400 µg | 1.2% | 4.2% | 1.5% | 5.1% | 2.6% | 8.5% | 4.8% | 8.3% | 8.9% | 19.3% |
| Thiamin | 0.3 mg per 1000 kcal energy | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% |
| Riboflavin | M: 1.0 mg, W: 0.9 mg | 0.6% | 1.9% | 1.7% | 2.8% | 3.4% | 1.4% | 2.7% | 1.4% | 5.6% | 7.4% |
| Niacin | 5.5 mg per 1000 kcal energy | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% |
| Vitamin B6 | 13 µg per g protein | 0.9% | 1.3% | 0.3% | 0.0% | 0.0% | 0.0% | 0.0% | 0.0% | 0.3% | 0.3% |
| Vitamin B12 | 1.25 µg | 0.1% | 0.0% | 0.8% | 0.0% | 0.2% | 1.4% | 4.7% | 3.2% | 31.2% | 30.0% |
| Folate | 150 µg | 3.7% | 2.9% | 0.6% | 0.0% | 0.6% | 0.0% | 0.8% | 0.0% | 0.8% | 0.0% |
| Vitamin C | 25 mg | 4.1% | 6.1% | 0.2% | 0.0% | 0.2% | 0.0% | 0.0% | 0.0% | 0.1% | 0.0% |
| Calcium | 525 mg | 8.4% | 9.7% | 3.1% | 1.7% | 5.1% | 1.4% | 3.0% | 1.4% | 5.6% | 2.8% |
| Magnesium | M: 250 mg, W: 200 mg | 6.4% | 12.6% | 1.3% | 4.0% | 1.0% | 1.4% | 1.7% | 3.7% | 1.5% | 2.5% |
| Iron * | M, and W aged 50+: 6.7 mg | 0.8% | 1.9% | 0.4% | 0.0% | 0.6% | 1.4% | 0.6% | 0.9% | 0.2% | 0.3% |
| Bioavailability adjusted Iron * | M, and W aged 50+: 12.06 mg c | 16.0% | 19.4% | 6.7% | 9.3% | ||||||
| Zinc | M: 7.3 mg, W: 5.5 mg | 0.9% | 5.2% | 2.0% | 7.4% | 4.7% | 4.2% | 4.2% | 10.6% | 6.3% | 13.3% |
| Bioavailability adjusted Zinc | M: 10.95 mg, W: 8.25 mg c | 31.5% | 47.2% | 34.8% | 49.9% | ||||||
| Iodine | 95 µg c | 1.9% | 1.0% | 5.1% | 5.1% | 5.9% | 8.5% | 26.3% | 16.7% | 67.3% | 60.9% |
| Selenium | 45 µg d | 6.4% | 6.8% | 11.4% | 10.8% | 17.4% | 11.3% | 67.3% | 50.0% | 68.0% | 54.7% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lawson, I.; Wood, C.; Syam, N.; Rippin, H.; Dagless, S.; Wickramasinghe, K.; Amoutzopoulos, B.; Steer, T.; Key, T.J.; Papier, K. Assessing Performance of Contemporary Plant-Based Diets against the UK Dietary Guidelines: Findings from the Feeding the Future (FEED) Study. Nutrients 2024, 16, 1336. https://doi.org/10.3390/nu16091336
Lawson I, Wood C, Syam N, Rippin H, Dagless S, Wickramasinghe K, Amoutzopoulos B, Steer T, Key TJ, Papier K. Assessing Performance of Contemporary Plant-Based Diets against the UK Dietary Guidelines: Findings from the Feeding the Future (FEED) Study. Nutrients. 2024; 16(9):1336. https://doi.org/10.3390/nu16091336
Chicago/Turabian StyleLawson, Izabella, Caroline Wood, Nandana Syam, Holly Rippin, Selina Dagless, Kremlin Wickramasinghe, Birdem Amoutzopoulos, Toni Steer, Timothy J. Key, and Keren Papier. 2024. "Assessing Performance of Contemporary Plant-Based Diets against the UK Dietary Guidelines: Findings from the Feeding the Future (FEED) Study" Nutrients 16, no. 9: 1336. https://doi.org/10.3390/nu16091336





