How to Measure Adherence to a Mediterranean Diet in Dental Studies: Is a Short Adherence Screener Enough? A Comparative Analysis
Abstract
:1. Introduction
2. Materials and Methods
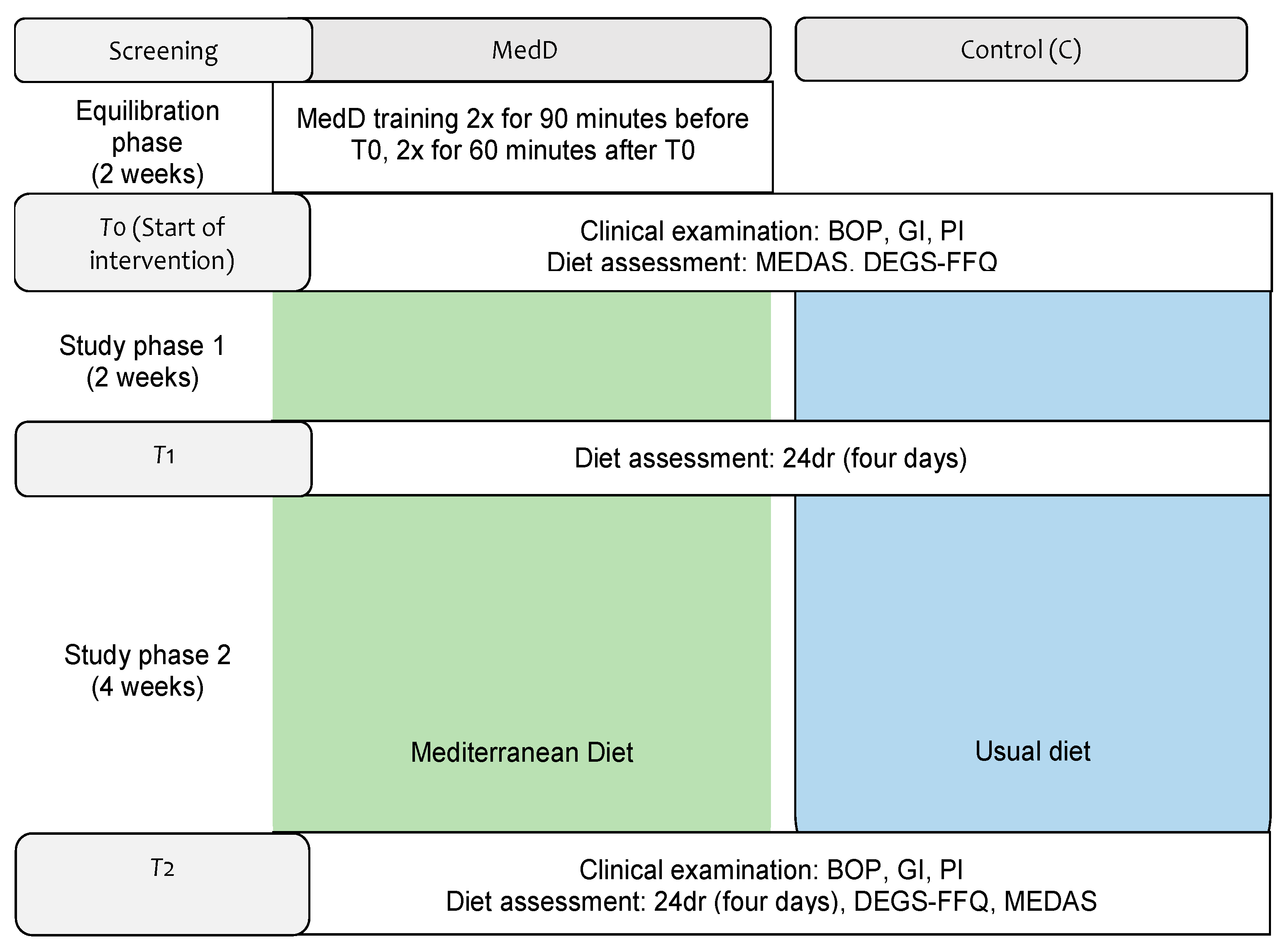
2.1. Study Design
2.2. Inclusion Criteria
2.3. Exclusion Criteria
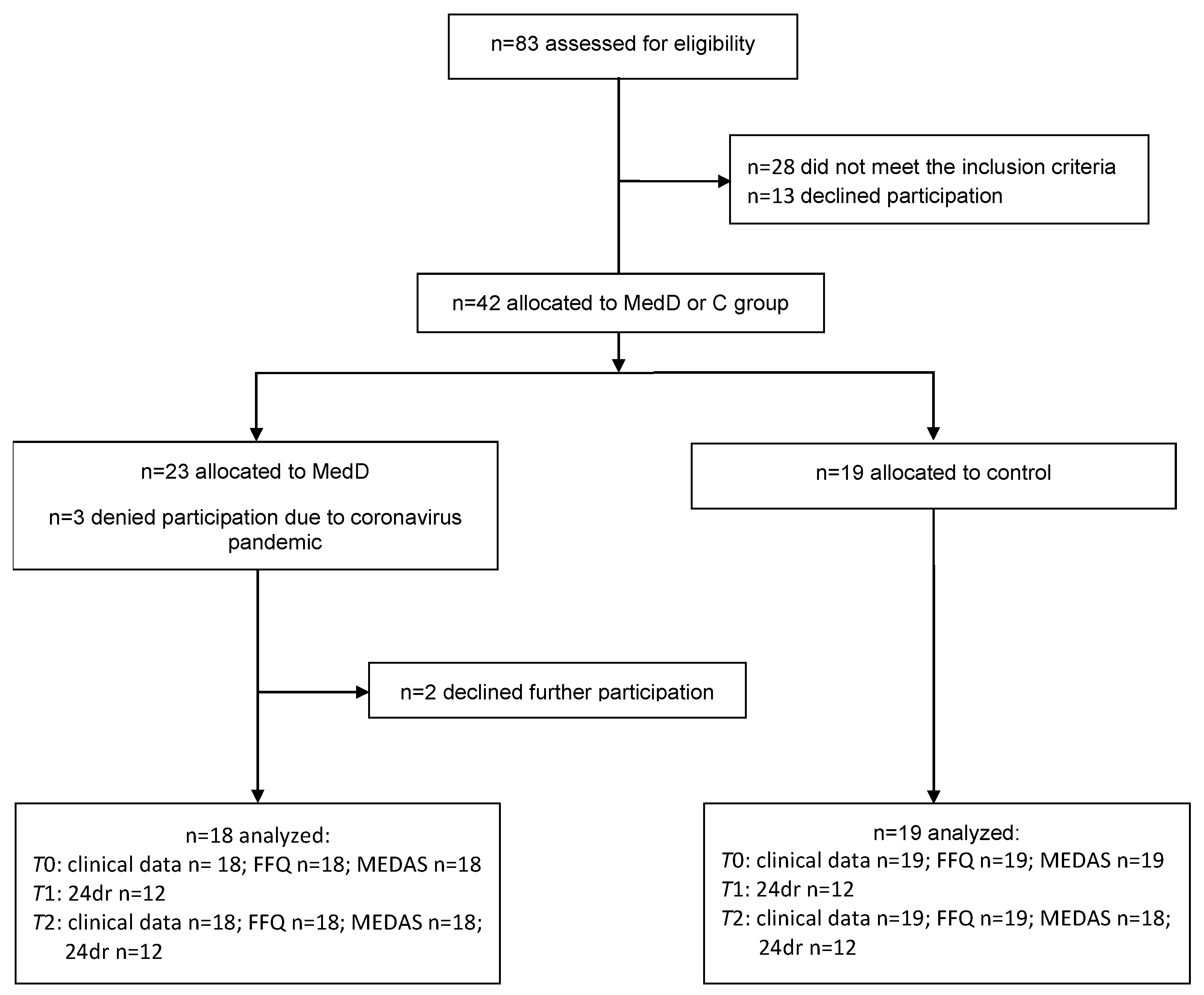
2.4. Patient Recruitment and Allocation
2.5. Diet Intervention
2.6. Diet Assessment and Clinical Examinations
2.7. Study Outcomes
2.8. Statistical Methods
3. Results
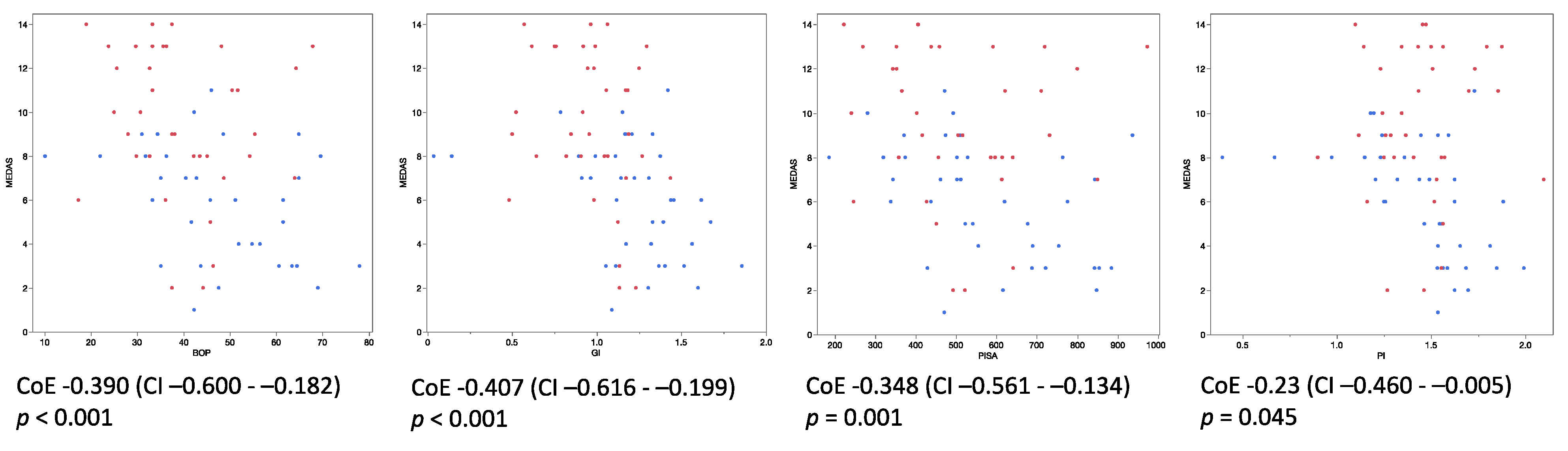
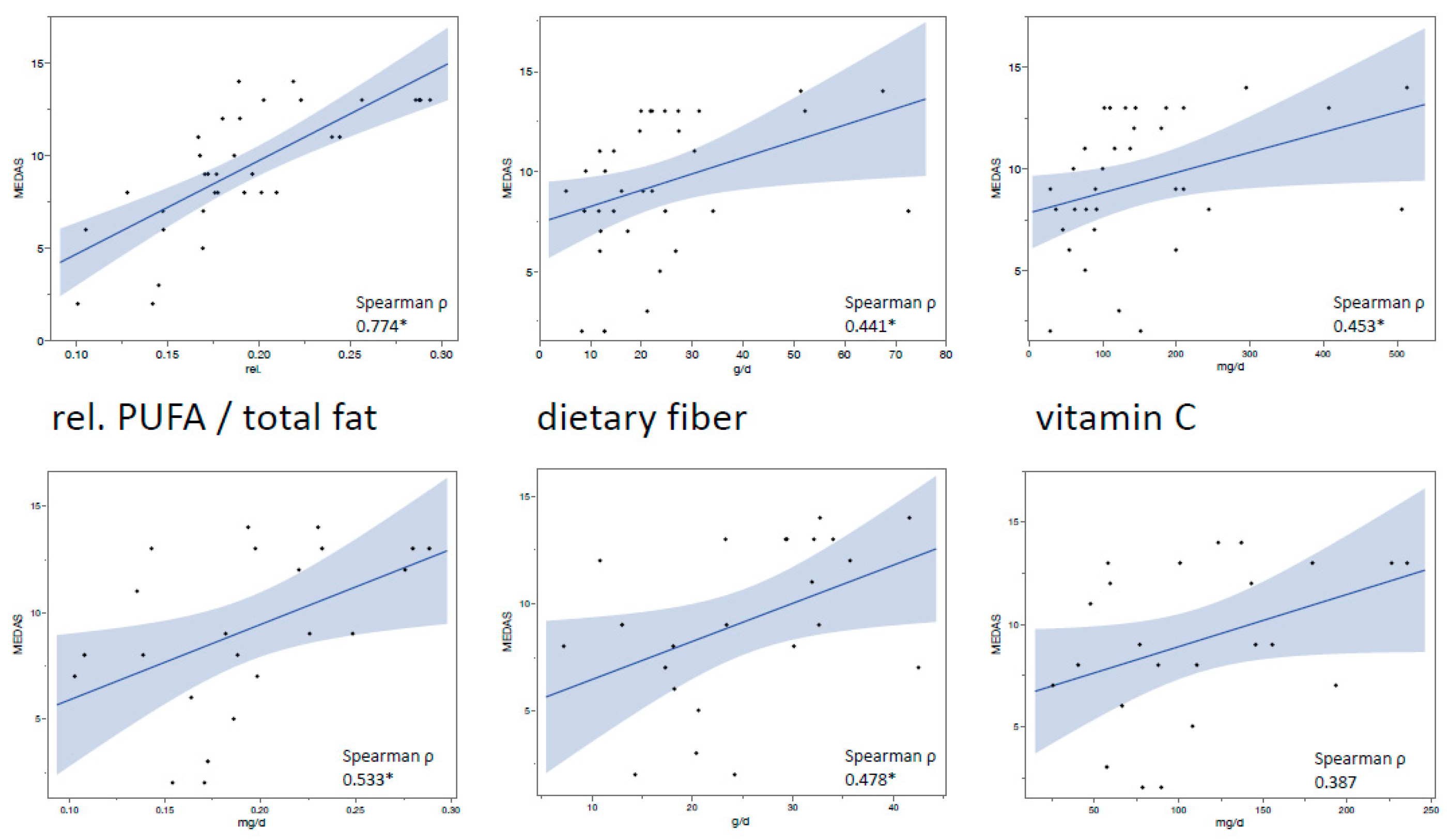
3.1. The MEDAS Score Was Negatively Correlated with Periodontal Inflammation and Positively Correlated with the Intake of MedD-Associated Nutrients
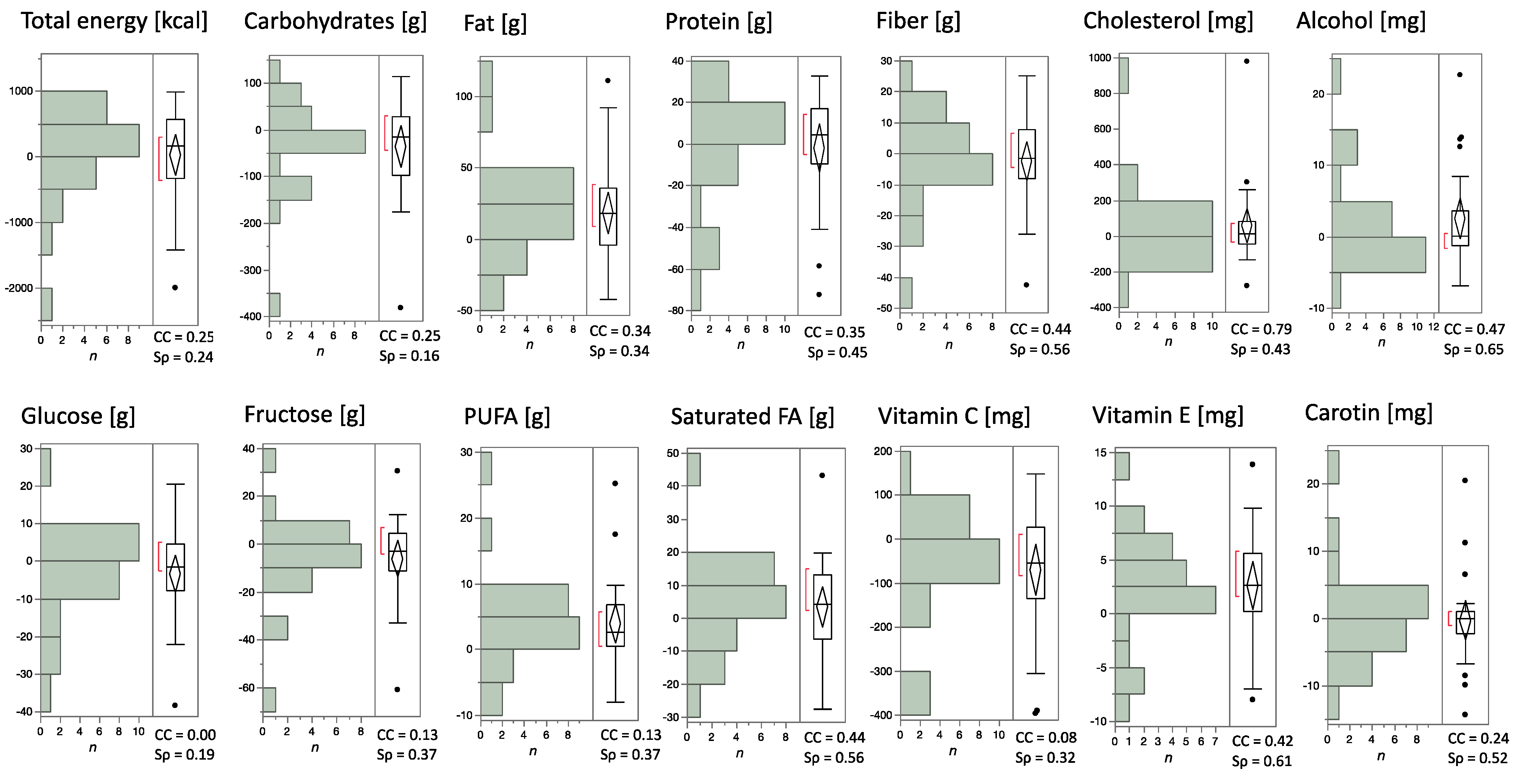
3.2. DEGS-FFQ and 24dr Nutrient Intake Results Were Heterogeneous Comparable
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dinu, M.; Pagliai, G.; Casini, A.; Sofi, F. Mediterranean diet and multiple health outcomes: An umbrella review of meta-analyses of observational studies and randomised trials. Eur. J. Clin. Nutr. 2018, 72, 30–43. [Google Scholar] [CrossRef] [PubMed]
- Machowicz, A.; Hall, I.; de Pablo, P.; Rauz, S.; Richards, A.; Higham, J.; Poveda-Gallego, A.; Imamura, F.; Bowman, S.J.; Barone, F.; et al. Mediterranean diet and risk of Sjögren’s syndrome. Clin. Exp. Rheumatol. 2020, 38 (Suppl. 126), 216–221. [Google Scholar]
- Sofi, F.; Macchi, C.; Abbate, R.; Gensini, G.F.; Casini, A. Mediterranean diet and health status: An updated meta-analysis and a proposal for a literature-based adherence score. Public Health Nutr. 2014, 17, 2769–2782. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Willett, W.C.; Sacks, F.; Trichopoulou, A.; Drescher, G.; Ferro-Luzzi, A.; Helsing, E.; Trichopoulos, D. Mediterranean diet pyramid: A cultural model for healthy eating. Am. J. Clin. Nutr. 1995, 61, 1402S–1406S. [Google Scholar] [CrossRef] [PubMed]
- Chapple, I.L.C.; Bouchard, P.; Cagetti, M.G.; Campus, G.; Carra, M.-C.; Cocco, F.; Nibali, L.; Hujoel, P.; Laine, M.L.; Lingström, P.; et al. Interaction of lifestyle, behaviour or systemic diseases with dental caries and periodontal diseases: Consensus report of group 2 of the joint EFP/ORCA workshop on the boundaries between caries and periodontal diseases. J. Clin. Periodontol. 2017, 44 (Suppl. 18), S39–S51. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hujoel, P. Dietary Carbohydrates and Dental-Systemic Diseases. J. Dent. Res. 2009, 88, 490–502. [Google Scholar] [CrossRef]
- Woelber, J.P.; Tennert, C. Chapter 13: Diet and Periodontal Diseases. Monogr. Oral Sci. 2020, 28, 125–133. [Google Scholar] [CrossRef]
- Sanz, M.; Herrera, D.; Kebschull, M.; Chapple, I.; Jepsen, S.; Berglundh, T.; Sculean, A.; Tonetti, M.S.; Aass, A.M.; Aimetti, M.; et al. Treatment of stage I-III periodontitis-The EFP S3 level clinical practice guideline. J. Clin. Periodontol. 2020, 47 (Suppl. 22), 4–60. [Google Scholar] [CrossRef]
- Baumgartner, S.; Imfeld, T.; Schicht, O.; Rath, C.; Persson, R.E.; Persson, G.R. The Impact of the Stone Age Diet on Gingival Conditions in the Absence of Oral Hygiene. J. Periodontol. 2009, 80, 759–768. [Google Scholar] [CrossRef]
- Jockel-Schneider, Y.; Goßner, S.K.; Petersen, N.; Stölzel, P.; Hägele, F.; Schweiggert, R.M.; Haubitz, I.; Eigenthaler, M.; Carle, R.; Schlagenhauf, U. Stimulation of the nitrate-nitrite-NO-metabolism by repeated lettuce juice consumption decreases gingival inflammation in periodontal recall patients: A randomized, double-blinded, placebo-controlled clinical trial. J. Clin. Periodontol. 2016, 43, 603–608. [Google Scholar] [CrossRef] [PubMed]
- Woelber, J.P.; Gärtner, M.; Breuninger, L.; Anderson, A.; König, D.; Hellwig, E.; Al-Ahmad, A.; Vach, K.; Dötsch, A.; Ratka-Krüger, P.; et al. The influence of an anti-inflammatory diet on gingivitis. A randomized controlled trial. J. Clin. Periodontol. 2019, 46, 481–490. [Google Scholar] [CrossRef]
- Woelber, J.P.; Bremer, K.; Vach, K.; König, D.; Hellwig, E.; Ratka-Krüger, P.; Al-Ahmad, A.; Tennert, C. An oral health optimized diet can reduce gingival and periodontal inflammation in humans—A randomized controlled pilot study. BMC Oral Health 2016, 17, 28. [Google Scholar] [CrossRef] [Green Version]
- Bartha, V.; Exner, L.; Schweikert, D.; Woelber, J.P.; Vach, K.; Meyer, A.; Basrai, M.; Bischoff, S.C.; Meller, C.; Wolff, D. Effect of the Mediterranean diet on gingivitis. A randomized controlled trial. J. Clin. Periodontol. 2021, 49, 111–122. [Google Scholar] [CrossRef]
- Altun, E.; Walther, C.; Borof, K.; Petersen, E.; Lieske, B.; Kasapoudis, D.; Jalilvand, N.; Beikler, T.; Jagemann, B.; Zyriax, B.-C.; et al. Association between Dietary Pattern and Periodontitis-A Cross-Sectional Study. Nutrients 2021, 13, 4167. [Google Scholar] [CrossRef]
- Haftenberger, M.; Heuer, T.; Heidemann, C.; Kube, F.; Krems, C.; Mensink, G.B. Relative validation of a food frequency questionnaire for national health and nutrition monitoring. Nutr. J. 2010, 9, 36. [Google Scholar] [CrossRef] [Green Version]
- Schröder, H.; Fitó, M.; Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Lamuela-Raventós, R.; Ros, E.; Salaverría, I.; Fiol, M.; et al. A Short Screener Is Valid for Assessing Mediterranean Diet Adherence among Older Spanish Men and Women. J. Nutr. 2011, 141, 1140–1145. [Google Scholar] [CrossRef] [Green Version]
- Papadaki, A.; Johnson, L.; Toumpakari, Z.; England, C.; Rai, M.; Toms, S.; Penfold, C.; Zazpe, I.; Martínez-González, M.A.; Feder, G. Validation of the English Version of the 14-Item Mediterranean Diet Adherence Screener of the PREDIMED Study, in People at High Cardiovascular Risk in the UK. Nutrients 2018, 10, 138. [Google Scholar] [CrossRef] [Green Version]
- Vieira, L.M.; Gottschall, C.B.A.; Vinholes, D.B.; Martinez-Gonzalez, M.A.; Marcadenti, A. Translation and cross-cultural adaptation of 14-item Mediterranean Diet Adherence Screener and low-fat diet adherence questionnaire. Clin. Nutr. ESPEN 2020, 39, 180–189. [Google Scholar] [CrossRef]
- Abu-Saad, K.; Endevelt, R.; Goldsmith, R.; Shimony, T.; Nitsan, L.; Shahar, D.R.; Keinan-Boker, L.; Ziv, A.; Kalter-Leibovici, O. Adaptation and predictive utility of a Mediterranean diet screener score. Clin. Nutr. 2019, 38, 2928–2935. [Google Scholar] [CrossRef]
- Ballesteros, J.-M.; Struijk, E.A.; Rodríguez-Artalejo, F.; López-García, E. Mediterranean diet and risk of falling in community-dwelling older adults. Clin. Nutr. 2020, 39, 276–281. [Google Scholar] [CrossRef]
- Giacalone, D.; Frøst, M.B.; Rodríguez-Pérez, C. Reported Changes in Dietary Habits During the COVID-19 Lockdown in the Danish Population: The Danish COVIDiet Study. Front. Nutr. 2020, 7, 592112. [Google Scholar] [CrossRef]
- Jacobs, D.R.; Petersen, K.; Svendsen, K.; Ros, E.; Sloan, C.B.; Steffen, L.M.; Tapsell, L.C.; Kris-Etherton, P. Considerations to facilitate a US study that replicates PREDIMED. Metab. -Clin. Exp. 2018, 85, 361–367. [Google Scholar] [CrossRef]
- Young, C.L.; Mohebbi, M.; Staudacher, H.; Berk, M.; Jacka, F.N.; O’Neil, A. Assessing the feasibility of an m-Health intervention for changing diet quality and mood in individuals with depression: The My Food & Mood program. Int. Rev. Psychiatry 2021, 33, 266–279. [Google Scholar] [CrossRef]
- Zhao, L.; Zhang, P.; Zheng, Q.; Deka, A.; Choudhury, R.; Rastogi, S. Does a MediDiet with additional extra virgin olive oil (EVOO) and pistachios reduce the incidence of gestational diabetes? Endocr. Pract. 2021, 28, 135–141. [Google Scholar] [CrossRef]
- Bottcher, M.R.; Marincic, P.Z.; Nahay, K.L.; Baerlocher, B.E.; Willis, A.W.; Park, J.; Gaillard, P.; Greene, M.W. Nutrition knowledge and Mediterranean diet adherence in the southeast United States: Validation of a field-based survey instrument. Appetite 2017, 111, 166–176. [Google Scholar] [CrossRef]
- Cobo-Cuenca, A.I.; Garrido-Miguel, M.; Soriano-Cano, A.; Ferri-Morales, A.; Martínez-Vizcaíno, V.; Martín-Espinosa, N.M. Adherence to the Mediterranean Diet and Its Association with Body Composition and Physical Fitness in Spanish University Students. Nutrients 2019, 11, 2830. [Google Scholar] [CrossRef] [Green Version]
- Mieziene, B.; Emeljanovas, A.; Fatkulina, N.; Stukas, R. Dietary Pattern and Its Correlates among Lithuanian Young Adults: Mediterranean Diet Approach. Nutrients 2020, 12, 2025. [Google Scholar] [CrossRef]
- Pala, V.; Sieri, S.; Palli, D.; Salvini, S.; Berrino, F.; Bellegotti, M.; Frasca, G.; Tumino, R.; Sacerdote, C.; Fiorini, L.; et al. Diet in the Italian Epic Cohorts: Presentation of Data and Methodological Issues. Tumori 2003, 89, 594–607. [Google Scholar] [CrossRef]
- Hebestreit, K.; Yahiaoui-Doktor, M.; Engel, C.; Vetter, W.; Siniatchkin, M.; Erickson, N.; Halle, M.; Kiechle, M.; Bischoff, S.C. Validation of the German version of the Mediterranean Diet Adherence Screener (MEDAS) questionnaire. BMC Cancer 2017, 17, 341. [Google Scholar] [CrossRef]
- Lenth, R.V. Statistical power calculations. J. Anim. Sci. 2007, 85, E24–E29. [Google Scholar] [CrossRef]
- Axelsson, P.; Lindhe, J. The significance of maintenance care in the treatment of periodontal disease. J. Clin. Periodontol. 1981, 8, 281–294. [Google Scholar] [CrossRef]
- Reiniger, A.P.P.; Maier, J.; Wikesjö, U.M.E.; Moreira, C.H.C.; Kantorski, K.Z. Correlation between dental plaque accumulation and gingival health in periodontal maintenance patients using short or extended personal oral hygiene intervals. J. Clin. Periodontol. 2021, 48, 834–842. [Google Scholar] [CrossRef]
- Chapple, I.L.C.; Mealey, B.L.; Van Dyke, T.E.; Bartold, P.M.; Dommisch, H.; Eickholz, P.; Geisinger, M.L.; Genco, R.J.; Glogauer, M.; Goldstein, M.; et al. Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup 1 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Periodontol. 2018, 89, S74–S84. [Google Scholar] [CrossRef]
- Cena, H.; Calder, P.C. Defining a Healthy Diet: Evidence for The Role of Contemporary Dietary Patterns in Health and Disease. Nutrients 2020, 12, 334. [Google Scholar] [CrossRef] [Green Version]
- Irimata, K.; Li, X. Estimation of Correlation Coefficient in Data with Repeated Measures. Proc. SAS Glob. Forum 2018, 2018, 8–11. [Google Scholar]
- Lobo, E.; Tamayo, M.; Sanclemente, T. Nutrition Literacy and Healthy Diet: Findings from the Validation of a Short Seniors-Oriented Screening Tool, the Spanish Myths-NL. Int. J. Environ. Res. Public Health 2021, 18, 12107. [Google Scholar] [CrossRef]
- Harjola, U.; Liesmaa, H. Effects of poly of and sucrose candies on plaque, gingivitis and lactobacillus index scores: Observations on Helsinki school children. Acta Odontol. Scand. 1978, 36, 237–242. [Google Scholar] [CrossRef]
- Rateitschak-Plüss, E.M.; Guggenheim, B. Effects of a carbohydrate-free diet and sugar substitutes on dental plaque accumulation. J. Clin. Periodontol. 1982, 9, 239–251. [Google Scholar] [CrossRef]
- Teles, R.; Teles, F.; Frias-Lopez, J.; Paster, B.; Haffajee, A. Lessons learned and unlearned in periodontal microbiology: Lessons learned and unlearned in periodontal microbiology. Periodontol. 2000 2013, 62, 95–162. [Google Scholar] [CrossRef]
- Li, J.; Guasch-Ferré, M.; Chung, W.; Ruiz-Canela, M.; Toledo, E.; Corella, D.; Bhupathiraju, S.N.; Tobias, D.K.; Tabung, F.K.; Hu, J.; et al. The Mediterranean diet, plasma metabolome, and cardiovascular disease risk. Eur. Heart J. 2020, 41, 2645–2656. [Google Scholar] [CrossRef]
- Oliván-Blázquez, B.; Aguilar-Latorre, A.; Motrico, E.; Gómez-Gómez, I.; Zabaleta-Del-Olmo, E.; Couso-Viana, S.; Clavería, A.; Maderuelo-Fernandez, J.; Recio-Rodríguez, J.; Moreno-Peral, P.; et al. The Relationship between Adherence to the Mediterranean Diet, Intake of Specific Foods and Depression in an Adult Population (45–75 Years) in Primary Health Care. A Cross-Sectional Descriptive Study. Nutrients 2021, 13, 2724. [Google Scholar] [CrossRef]
- Bohlscheid-Thomas, S.; Hoting, I.; Boeing, H.; Wahrendorf, J. Reproducibility and relative validity of food group intake in a food frequency questionnaire developed for the German part of the EPIC project. European Prospective Investigation into Cancer and Nutrition. Int. J. Epidemiol. 1997, 26 (Suppl. 1), S59–S70. [Google Scholar] [CrossRef]
- Deschamps, V.; de Lauzon-Guillain, B.; Lafay, L.; Borys, J.-M.; Charles, M.A.; Romon, M. Reproducibility and relative validity of a food-frequency questionnaire among French adults and adolescents. Eur. J. Clin. Nutr. 2009, 63, 282–291. [Google Scholar] [CrossRef] [Green Version]
- Paalanen, L.; Männistö, S.; Virtanen, M.J.; Knekt, P.; Räsänen, L.; Montonen, J.; Pietinen, P. Validity of a food frequency questionnaire varied by age and body mass index. J. Clin. Epidemiol. 2006, 59, 994–1001. [Google Scholar] [CrossRef]
- Hill, R.J.; Davies, P.S.W. The validity of self-reported energy intake as determined using the doubly labelled water technique. Br. J. Nutr. 2001, 85, 415–430. [Google Scholar] [CrossRef] [Green Version]
- Mahabir, S.; Baer, D.J.; Giffen, C.; Subar, A.; Campbell, W.; Hartman, T.J.; Clevidence, B.; Albanes, D.; Taylor, P.R. Calorie intake misreporting by diet record and food frequency questionnaire compared to doubly labeled water among postmenopausal women. Eur. J. Clin. Nutr. 2006, 60, 561–565. [Google Scholar] [CrossRef]
- Praxedes, D.R.S.; Pureza, I.R.O.M.; Vasconcelos, L.G.L.; Júnior, A.E.D.S.; Macena, M.D.L.; Florêncio, T.M.D.M.T.; de Melo, I.S.V.; Bueno, N.B. Association between energy intake under-reporting and previous professional nutritional counselling in low-income women with obesity: A cross-sectional study. Nutr. Bull. 2021, 46, 310–320. [Google Scholar] [CrossRef]
- McLean, R.M.; Farmer, V.L.; Nettleton, A.; Cameron, C.M.; Cook, N.R.; Woodward, M.; Campbell, N.R.C.; TRUE Consortium (in Ternational Consortium for Quality Research on Dietary Sodium/Salt). Twenty-Four-Hour Diet recall and Diet records compared with 24-hour urinary excretion to predict an individual’s sodium consumption: A Systematic Review. J. Clin. Hypertens. 2018, 20, 1360–1376. [Google Scholar] [CrossRef] [Green Version]
- Wehling, H.; Lusher, J. People with a body mass index ≥30 under-report their dietary intake: A systematic review. J. Health Psychol. 2019, 24, 2042–2059. [Google Scholar] [CrossRef]
- Willett, W. Nutritional Epidemiology; Oxford University Press: Oxford, UK, 2012. [Google Scholar]
| MedDG | CG | Intergroup p-Value | |
|---|---|---|---|
| Men | 10 | 7 | 0.2536 |
| Women | 8 | 12 | |
| Age (years) | 32.71 ± 8.87 | 29.21 ± 7.17 | 0.198 |
| T1 | T2 | |||||
|---|---|---|---|---|---|---|
| MedDG, T1 | CG, T1 | MedDG, T2 | CG, T2 | MedDG T1-T2 Intra p-Value * | CG T1-T2 Intra p-Value * | |
| PI | 1.51 ± 0.21 | 1.37 ± 0.38 | 1.49 ± 0.24 | 1.39 ± 0.24 | 0.560 | 0.823 |
| GI | 1.3 ± 0.25 | 1.11 ± 0.42 | 0.99 ± 0.22 | 0.97 ± 0.27 | <0.001 | 0.093 |
| BOP [%] | 51.00 ± 14.65 | 43.21 ± 14.25 | 39.93 ± 13.74 | 39.74 ± 11.0 | <0.001 | 0.151 |
| PD [mm] | 2.26 ± 0.18 | 2.29 ± 0.18 | 2.36 ± 0.17 | 2.36 ± 0.18 | 0.008 | 0.044 |
| PISA [mm2] | 616.33 ± 201.39 | 528.94 ± 173.48 | 512.02 ± 205.83 | 514.26 ± 148.79 | 0.004 | 0.589 |
| MEDAS Score | 5.55 ± 3.01 | 6.52 ± 2.17 | 11.89 ± 1.90 | 7.22 ± 2.88 | <0.001 | 0.310 |
| MedD Group | C Group | 24dr Inter-p-Value * | FFQ Inter-p-Value * | Matching Results Regarding Both Intragroup Comparisons | Spearman ρ: 24dr and FFQ | CC: 24dr and FFQ | |||
|---|---|---|---|---|---|---|---|---|---|
| 24dr (n = 12) | FFQ (n = 18) | 24dr (n = 12) | FFQ (n = 19) | ||||||
| Energy [kcal/d] | 1647.21 ± 394.61 | 1769.11 ± 650.52 | 1963.00 ± 474.25 | 1785.46 ± 830.00 | 0.112 | 0.885 | + | 0.24 | 0.25 (–0.11–0.56) |
| Total carbohydrates [g] | 160.03 ± 35.11 | 219.53 ± 74.74 | 210.39 ± 52.30 | 223.29 ± 146.51 | 0.030 | 0.507 | 0.16 | 0.25 (–0.03–0.49) | |
| Total fat [g] | 70.13 ± 24.65 | 52.83 ± 29.08 | 84.96 ± 44.54 | 64.84 ± 24.63 | 0.312 | 0.215 | + | 0.34 | 0.34 (0.01–0.60) |
| Total protein [g] | 71.70 ± 19.90 | 82.06 ± 32.61 | 72.03 ± 18.51 | 65.04 ± 22.34 | 0.977 | 0.157 | + | 0.45 | 0.35 (–0.01–0.63) |
| Fibre [g] | 29.29 ± 8.28 | 33.87 ± 15.24 | 20.40 ± 8.29 | 20.45 ± 17.05 | 0.026 | 0.003 | + | 0.56 | 0.44 (0.13–0.67) |
| Cholesterol | 184.55 ± 102.15 | 205.10 ± 118.70 | 481.52 ± 609.69 | 341.62 ± 340.60 | 0.002 | 0.090 | 0.43 | 0.79 (0.69–0.86) | |
| Glucose [g] | 12.98 ± 9.90 | 18.80 ± 8.63 | 15.57 ± 5.31 | 16.36 ± 13.15 | 0.125 | 0.312 | + | 0.19 | 0.00 (–0.28–0.27) |
| Fructose [g] | 16.38 ± 4.85 | 26.35 ± 12.75 | 19.46 ± 9.77 | 21.55 ± 21.73 | 0.624 | 0.126 | + | 0.37 | 0.13 (–0.15–0.38) |
| Polyunsatured fatty acids [g] | 15.16 ± 5.65 | 11.37 ± 5.22 | 14.08 ± 9.78 | 9.93 ± 4.28 | 0.370 | 0.471 | + | 0.34 | 0.32 (0.02–0.56) |
| Satured fatty acids [g] | 21.74 ± 6.77 | 20.32 ± 13.06 | 35.38 ± 17.52 | 29.73 ± 11.73 | 0.005 | 0.046 | + | 0.56 | 0.44 (0.07–0.70) |
| Total alcohol [g] | 10.60 ± 7.51 | 8.48 ± 5.28 | 6.91 ± 8.65 | 3.84 ± 4.05 | 0.126 | 0.020 | 0.65 | 0.47 (0.16–0.69) | |
| Vitamin C [mg] | 129.79 ± 62.71 | 228.47 ± 123.64 | 89.75 ± 45.86 | 128.33 ± 129.74 | 0.126 | 0.009 | 0.32 | 0.08 (–0.16–0.32) | |
| Vitamine E [mg] | 15.15 ± 5.35 | 12.57 ± 5.93 | 11.50 ± 3.09 | 8.82 ± 5.06 | 0.133 | 0.035 | 0.61 | 0.42 (0.08–0.67) | |
| Carotin [mg] | 6.99 ± 5.17 | 9.37 ± 5.81 | 5.32 ± 6.23 | 3.41 ± 2.43 | 0.285 | 0.002 | 0.52 | 0.24 (–0.17–0.58) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bartha, V.; Exner, L.; Meyer, A.-L.; Basrai, M.; Schweikert, D.; Adolph, M.; Bruckner, T.; Meller, C.; Woelber, J.P.; Wolff, D. How to Measure Adherence to a Mediterranean Diet in Dental Studies: Is a Short Adherence Screener Enough? A Comparative Analysis. Nutrients 2022, 14, 1300. https://doi.org/10.3390/nu14061300
Bartha V, Exner L, Meyer A-L, Basrai M, Schweikert D, Adolph M, Bruckner T, Meller C, Woelber JP, Wolff D. How to Measure Adherence to a Mediterranean Diet in Dental Studies: Is a Short Adherence Screener Enough? A Comparative Analysis. Nutrients. 2022; 14(6):1300. https://doi.org/10.3390/nu14061300
Chicago/Turabian StyleBartha, Valentin, Lea Exner, Anna-Lisa Meyer, Maryam Basrai, Daniela Schweikert, Michael Adolph, Thomas Bruckner, Christian Meller, Johan Peter Woelber, and Diana Wolff. 2022. "How to Measure Adherence to a Mediterranean Diet in Dental Studies: Is a Short Adherence Screener Enough? A Comparative Analysis" Nutrients 14, no. 6: 1300. https://doi.org/10.3390/nu14061300
APA StyleBartha, V., Exner, L., Meyer, A.-L., Basrai, M., Schweikert, D., Adolph, M., Bruckner, T., Meller, C., Woelber, J. P., & Wolff, D. (2022). How to Measure Adherence to a Mediterranean Diet in Dental Studies: Is a Short Adherence Screener Enough? A Comparative Analysis. Nutrients, 14(6), 1300. https://doi.org/10.3390/nu14061300







