Social Inequalities in Changes in Diet in Adolescents during Confinement Due to COVID-19 in Spain: The DESKcohort Project
Abstract
1. Introduction
2. Materials and Methods
Data Analysis
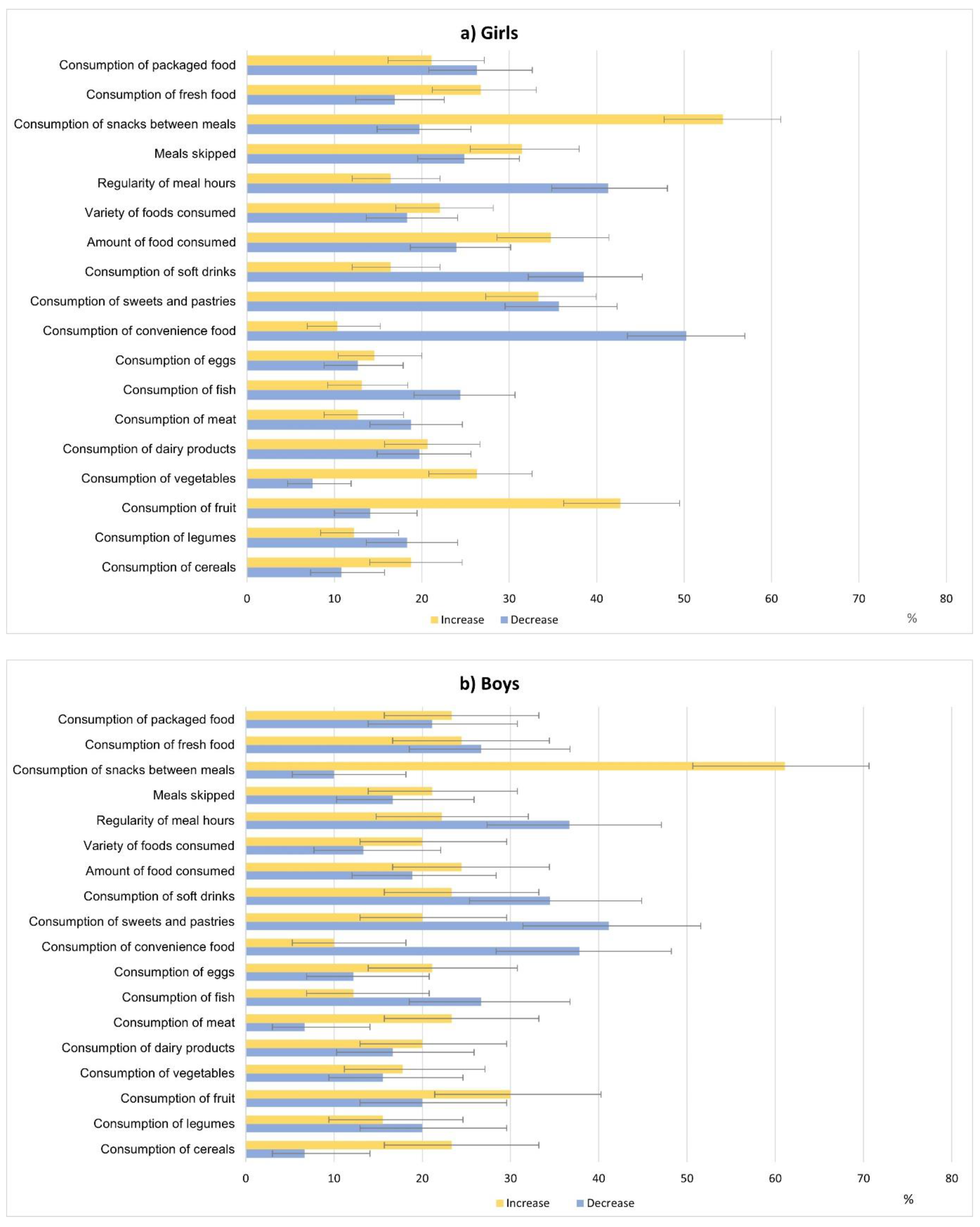
3. Results
4. Discussion
4.1. Changes in Food Consumption and Eating Behaviours during the COVID-19 Confinement
4.2. Changes in Diet and Dietary Patterns according to the Quality of the Diet before the COVID-19 Pandemic
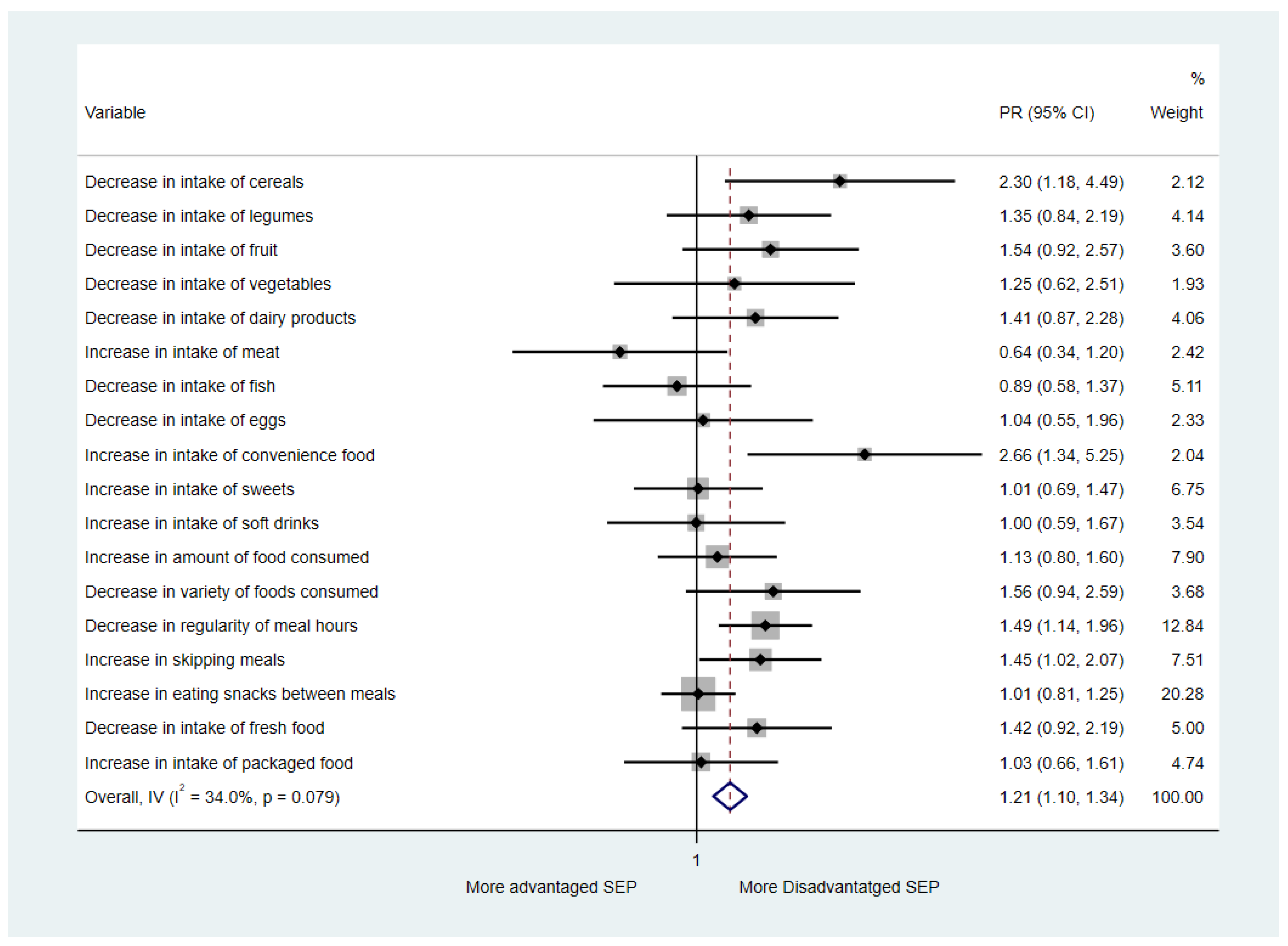
4.3. Changes in Diet and Dietary Patterns during the COVID-19 Pandemic Confinement according to the Perceived Socioeconomic Position
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Coronavirus Disease (COVID-2019) Situation Reports. World Health Organization. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports/ (accessed on 14 December 2020).
- Real Decreto 463/2020, de 14 de Marzo, Por El Que Se Declara El Estado de Alarma Para La Gestión de La Situación de Crisis Sanitaria Ocasionada Por El COVID-19. 2020. Available online: https://www.boe.es/eli/es/rd/2020/03/14/463 (accessed on 30 April 2021).
- Frühbeck, G.; Baker, J.L.; Busetto, L.; Dicker, D.; Goossens, G.H.; Halford, J.C.G.; Handjieva-Darlenska, T.; Hassapidou, M.; Holm, J.-C.; Lehtinen-Jacks, S.; et al. European Association for the Study of Obesity Position Statement on the Global COVID-19 Pandemic. Obes. Facts 2020, 13, 292–296. [Google Scholar] [CrossRef] [PubMed]
- Hämmig, O. Health Risks Associated with Social Isolation in General and in Young, Middle and Old Age. PLoS ONE 2019, 14, e0219663. [Google Scholar] [CrossRef]
- López-Bueno, R.; Calatayud, J.; Casaña, J.; Casajús, J.A.; Smith, L.; Tully, M.A.; Andersen, L.L.; López-Sánchez, G.F. COVID-19 Confinement and Health Risk Behaviors in Spain. Front. Psychol. 2020, 11, 1426. [Google Scholar] [CrossRef] [PubMed]
- Mattioli, A.V.; Sciomer, S.; Cocchi, C.; Maffei, S.; Gallina, S. Quarantine during COVID-19 Outbreak: Changes in Diet and Physical Activity Increase the Risk of Cardiovascular Disease. Nutr. Metab. Cardiovasc. Dis. 2020, 30, 1409–1417. [Google Scholar] [CrossRef] [PubMed]
- Sawyer, S.M.; Afifi, R.A.; Bearinger, L.H.; Blakemore, S.-J.; Dick, B.; Ezeh, A.C.; Patton, G.C. Adolescence: A Foundation for Future Health. Lancet 2012, 379, 1630–1640. [Google Scholar] [CrossRef]
- Viner, R.M.; Ozer, E.M.; Denny, S.; Marmot, M.; Resnick, M.; Fatusi, A.; Currie, C. Adolescence and the Social Determinants of Health. Lancet 2012, 379, 1641–1652. [Google Scholar] [CrossRef]
- Healthy Diet. World Health Organization. Available online: https://www.who.int/news-room/fact-sheets/detail/healthy-diet (accessed on 11 January 2021).
- García-Cabrera, S.; Herrera-Fernández, N.; Rodríguez-Hernández, C.; Nissensohn, M.; Román-Viñas, B.; Serra-Majem, L. KIDMED Test; Prevalence of Low Adherence to the Mediterranean Diet in Children and Young; a Systematic Review. Nutr. Hosp. 2015, 32, 2390–2399. [Google Scholar] [CrossRef]
- Mistretta, A.; Marventano, S.; Antoci, M.; Cagnetti, A.; Giogianni, G.; Nolfo, F.; Rametta, S.; Pecora, G.; Marranzano, M. Mediterranean Diet Adherence and Body Composition among Southern Italian Adolescents. Obes. Res. Clin. Pract. 2017, 11, 215–226. [Google Scholar] [CrossRef]
- Moreno, L.A.; Gottrand, F.; Huybrechts, I.; Ruiz, J.R.; González-Gross, M.; DeHenauw, S.; HELENA Study Group. Nutrition and Lifestyle in European Adolescents: The HELENA (Healthy Lifestyle in Europe by Nutrition in Adolescence) Study. Adv. Nutr. 2014, 5, 615S–623S. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The Psychological Impact of Quarantine and How to Reduce It: Rapid Review of the Evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Woodruff, S.J.; Hanning, R.M. A Review of Family Meal Influence on Adolescents’ Dietary Intake. Can. J. Diet. Pract. Res. 2008, 69, 14–22. [Google Scholar] [CrossRef]
- Middleton, G.; Golley, R.; Patterson, K.; Le Moal, F.; Coveney, J. What Can Families Gain from the Family Meal? A Mixed-Papers Systematic Review. Appetite 2020, 153, 104725. [Google Scholar] [CrossRef] [PubMed]
- Rey-López, J.P.; Vicente-Rodríguez, G.; Répásy, J.; Mesana, M.I.; Ruiz, J.R.; Ortega, F.B.; Kafatos, A.; Huybrechts, I.; Cuenca-García, M.; León, J.F.; et al. Food and Drink Intake during Television Viewing in Adolescents: The Healthy Lifestyle in Europe by Nutrition in Adolescence (HELENA) Study. Public Health Nutr. 2011, 14, 1563–1569. [Google Scholar] [CrossRef] [PubMed]
- Moynihan, A.B.; van Tilburg, W.A.P.; Igou, E.R.; Wisman, A.; Donnelly, A.E.; Mulcaire, J.B. Eaten up by Boredom: Consuming Food to Escape Awareness of the Bored Self. Front. Psychol. 2015, 6, 369. [Google Scholar] [CrossRef]
- Skafida, V. The Family Meal Panacea: Exploring How Different Aspects of Family Meal Occurrence, Meal Habits and Meal Enjoyment Relate to Young Children’s Diets: The Family Meal Panacea. Sociol. Health Illn. 2013, 35, 906–923. [Google Scholar] [CrossRef]
- De Clercq, B.; Abel, T.; Moor, I.; Elgar, F.J.; Lievens, J.; Sioen, I.; Braeckman, L.; Deforche, B. Social Inequality in Adolescents’ Healthy Food Intake: The Interplay between Economic, Social and Cultural Capital. Eur. J. Public Health 2016, ckw236. [Google Scholar] [CrossRef] [PubMed][Green Version]
- DESK Cohort. Available online: http://deskcohort.cat/ (accessed on 14 December 2020).
- Norte-Navarro, A.; Ortiz-Moncada, R. Calidad de la dieta española según el índice de alimentación saludable. Nutr. Hosp. 2011, 330–336. [Google Scholar] [CrossRef]
- ISCED: International Standard Classification of Education 2011, 2012th ed.; UNESCO Institute for Statistics: Montreal, QC, Canada, 2014.
- Goodman, E.; Adler, N.E.; Kawachi, I.; Frazier, A.L.; Huang, B.; Colditz, G.A. Adolescents’ Perceptions of Social Status: Development and Evaluation of a New Indicator. Pediatrics 2001, 108, e31. [Google Scholar] [CrossRef]
- de Onis, M. Development of a WHO Growth Reference for School-Aged Children and Adolescents. Bull. World Health Organ. 2007, 85, 660–667. [Google Scholar] [CrossRef] [PubMed]
- Global Recommendations on Physical Activity for Health; World Health Organization (WHO): Geneva, Switzerland, 2010.
- Espelt, A.; Mari-Dell’Olmo, M.; Penelo, E.; Bosque-Prous, M. Applied Prevalence Ratio Estimation with Different Regression Models: An Example from a Cross-National Study on Substance Use Research. Adicciones 2017, 29, 105–112. [Google Scholar] [CrossRef] [PubMed]
- Espelt, A.; Bosque-Prous, M.; Marí-Dell’Olmo, M. Considerations on the Use of Odds Ratio versus Prevalence or Proportion Ratio. Adicciones 2019, 31, 257–259. [Google Scholar] [CrossRef]
- Pérez-Rodrigo, C.; Gianzo, M.; Gotzone, B.; Ruiz, F.; Casis, L.; Aranceta-Bartrina, J.; Grupo Colaborativo de la Sociedad Española de Nutrición Comunitaria. Cambios en los Hábitos Alimentarios Durante el Periodo de Confinamiento por la Pandemia COVID-19 en España. Rev. Esp. Nutr. Comunitaria 2020, 26, 101–111. [Google Scholar] [CrossRef]
- Robinson, E.; Otten, R.; Hermans, R.C.J. Descriptive Peer Norms, Self-Control and Dietary Behaviour in Young Adults. Psychol. Health 2016, 31, 9–20. [Google Scholar] [CrossRef]
- Cruwys, T.; Bevelander, K.E.; Hermans, R.C.J. Social Modeling of Eating: A Review of When and Why Social Influence Affects Food Intake and Choice. Appetite 2015, 86, 3–18. [Google Scholar] [CrossRef] [PubMed]
- Guidetti, M.; Conner, M.; Prestwich, A.; Cavazza, N. The Transmission of Attitudes towards Food: Twofold Specificity of Similarities with Parents and Friends. Br. J. Health Psychol. 2012, 17, 346–361. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Roso, M.B.; de Carvalho Padilha, P.; Mantilla-Escalante, D.C.; Ulloa, N.; Brun, P.; Acevedo-Correa, D.; Arantes Ferreira Peres, W.; Martorell, M.; Aires, M.T.; de Oliveira Cardoso, L.; et al. Covid-19 Confinement and Changes of Adolescent’s Dietary Trends in Italy, Spain, Chile, Colombia and Brazil. Nutrients 2020, 12, 1807. [Google Scholar] [CrossRef] [PubMed]
- Zupo, R.; Castellana, F.; Sardone, R.; Sila, A.; Giagulli, V.A.; Triggiani, V.; Cincione, R.I.; Giannelli, G.; De Pergola, G. Preliminary Trajectories in Dietary Behaviors during the COVID-19 Pandemic: A Public Health Call to Action to Face Obesity. Int. J. Environ. Res. Public. Health 2020, 17, 7073. [Google Scholar] [CrossRef] [PubMed]
- Chang, M.; Green, L.; Cummins, S. All Change. Has COVID-19 Transformed the Way We Need to Plan for a Healthier and More Equitable Food Environment? URBAN Des. Int. 2020. [Google Scholar] [CrossRef]
- Huber, B.C. Altered Nutrition Behavior during COVID-19 Pandemic Lockdown in Young Adults. Eur. J. Nutr. 2020. [Google Scholar] [CrossRef]
- Pietrobelli, A.; Pecoraro, L.; Ferruzzi, A.; Heo, M.; Faith, M.; Zoller, T.; Antoniazzi, F.; Piacentini, G.; Fearnbach, S.N.; Heymsfield, S.B. Effects of COVID-19 Lockdown on Lifestyle Behaviors in Children with Obesity Living in Verona, Italy: A Longitudinal Study. Obesity 2020, 28, 1382–1385. [Google Scholar] [CrossRef]
- Borges, C.; Slater, B.; Santaliestra-Pasías, A.; Mouratidou, T.; Huybrechts, I.; Widhalm, K.; Gottrand, F.; Manios, Y.; Jimenez-Pavón, D.; Valtueña, J.; et al. Dietary Patterns in European and Brazilian Adolescents: Comparisons and Associations with Socioeconomic Factors. Nutrients 2018, 10, 57. [Google Scholar] [CrossRef]
- Miqueleiz, E.; Lostao, L.; Ortega, P.; Santos, J.M.; Astasio, P.; Regidor, E. Patrón Socioeconómico en la Alimentación no Saludable en Niños y Adolescentes en España. Aten. Primaria 2014, 46, 433–439. [Google Scholar] [CrossRef]
- Giskes, K.; Avendaňo, M.; Brug, J.; Kunst, A.E. A Systematic Review of Studies on Socioeconomic Inequalities in Dietary Intakes Associated with Weight Gain and Overweight/Obesity Conducted among European Adults: Socioeconomic Inequalities in Dietary Intakes. Obes. Rev. 2009, 11, 413–429. [Google Scholar] [CrossRef] [PubMed]
- Serra-Majem, L.; Tomaino, L.; Dernini, S.; Berry, E.M.; Lairon, D.; Ngo de la Cruz, J.; Bach-Faig, A.; Donini, L.M.; Medina, F.-X.; Belahsen, R.; et al. Updating the Mediterranean Diet Pyramid towards Sustainability: Focus on Environmental Concerns. Int. J. Environ. Res. Public. Health 2020, 17, 8758. [Google Scholar] [CrossRef] [PubMed]
- Dernini, S.; Berry, E.M.; Serra-Majem, L.; Vecchia, C.L.; Capone, R.; Medina, F.X.; Aranceta-Bartrina, J.; Belahsen, R.; Burlingame, B.; Calabrese, G.; et al. Med Diet 4.0: The Mediterranean Diet with Four Sustainable Benefits. Public Health Nutr. 2017, 20, 1322–1330. [Google Scholar] [CrossRef]
- Vilela, S.; Muresan, I.; Correia, D.; Severo, M.; Lopes, C. The Role of Socio-Economic Factors in Food Consumption of Portuguese Children and Adolescents: Results from the National Food, Nutrition and Physical Activity Survey 2015–2016. Br. J. Nutr. 2020, 124, 591–601. [Google Scholar] [CrossRef] [PubMed]
- Ranjit, N.; Wilkinson, A.V.; Lytle, L.M.; Evans, A.E.; Saxton, D.; Hoelscher, D.M. Socioeconomic Inequalities in Children’s Diet: The Role of the Home Food Environment. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 1–19. [Google Scholar] [CrossRef]
- Mekonnen, T.; Havdal, H.H.; Lien, N.; O’Halloran, S.A.; Arah, O.A.; Papadopoulou, E.; Gebremariam, M.K. Mediators of Socioeconomic Inequalities in Dietary Behaviours among Youth: A Systematic Review. Obes. Rev. 2020, 21. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Specter, S. Poverty and Obesity: The Role of Energy Density and Energy Costs. Am. J. Clin. Nutr. 2004, 79, 6–16. [Google Scholar] [CrossRef]
- McKinnon, L.; Giskes, K.; Turrell, G. The Contribution of Three Components of Nutrition Knowledge to Socio-Economic Differences in Food Purchasing Choices. Public Health Nutr. 2014, 17, 1814–1824. [Google Scholar] [CrossRef] [PubMed]
- Mackenbach, J.D.; Nelissen, K.G.M.; Dijkstra, S.C.; Poelman, M.P.; Daams, J.G.; Leijssen, J.B.; Nicolaou, M. A Systematic Review on Socioeconomic Differences in the Association between the Food Environment and Dietary Behaviors. Nutrients 2019, 11, 2215. [Google Scholar] [CrossRef] [PubMed]
- De Buhr, E.; Tannen, A. Parental Health Literacy and Health Knowledge, Behaviours and Outcomes in Children: A Cross-Sectional Survey. BMC Public Health 2020, 20, 1096. [Google Scholar] [CrossRef]
- Caspi, C.E.; Sorensen, G.; Subramanian, S.V.; Kawachi, I. The Local Food Environment and Diet: A Systematic Review. Health Place 2012, 18, 1172–1187. [Google Scholar] [CrossRef]
- AQuAS Mapa per ABS. Available online: http://aquas.gencat.cat/ca/actualitat/ultimes-dades-coronavirus/mapa-per-abs/ (accessed on 10 February 2021).
- Oliver-Parra, A.; González-Viana, A. Facilitando la Salud Comunitaria. Indicadores Básicos de Salud por Área Básica de Salud en Cataluña. Gac. Sanit. 2020, 34, 204–207. [Google Scholar] [CrossRef] [PubMed]
- Bambra, C.; Riordan, R.; Ford, J.; Matthews, F. The COVID-19 Pandemic and Health Inequalities. J. Epidemiol. Community Health 2020, 74, 964–968. [Google Scholar] [CrossRef]
- De la Torre-Moral, A.; Fàbregues, S.; Bach-Faig, A.; Fornieles-Deu, A.; Medina, F.X.; Aguilar-Martínez, A.; Sánchez-Carracedo, D. Family Meals, Conviviality, and the Mediterranean Diet among Families with Adolescents. Int. J. Environ. Res. Public. Health 2021, 18, 2499. [Google Scholar] [CrossRef] [PubMed]
- United Nations Sustainable Development Goals. Available online: https://www.un.org/sustainabledevelopment/ (accessed on 30 April 2021).
| Variable | n | % |
|---|---|---|
| Gender | ||
| Girl | 213 | 70.3 |
| Boy | 90 | 29.7 |
| Course | ||
| ISCED 2 | 169 | 55.8 |
| ISCED 3 | 134 | 44.2 |
| Perceived socioeconomic position * (mean, SD) | 62.48 | 13.8 |
| Size of municipality | ||
| ≤5000 inhabitants | 87 | 28.7 |
| 5001–20,000 inhabitants | 126 | 41.6 |
| >20,000 inhabitants | 79 | 26.1 |
| No data available | 11 | 3.6 |
| Body mass index | ||
| Underweight or normal weight ** | 250 | 82.5 |
| Overweight or obesity | 50 | 16.5 |
| No data | 3 | 1.0 |
| Physical activity | ||
| Compliance with WHO recommendations | 107 | 35.3 |
| Under WHO recommendations | 181 | 59.7 |
| No data | 15 | 5.0 |
| Self-perceived health status | ||
| Excellent or very good | 163 | 53.8 |
| Good, fair, or poor | 140 | 46.2 |
| Sleep quality | ||
| Very good or good | 184 | 60.7 |
| Very poor or poor | 119 | 39.3 |
| Total (n = 303) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Decrease | No Changes | Increase | |||||||
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | |
| Highest tertile Spanish HEI (n = 100) | |||||||||
| Consumption of cereals | 12 | 12.0 | (6.9–20.0) | 70 | 70.0 | (60.3–78.2) | 18 | 18.0 | (11.6–26.8) |
| Consumption of legumes | 15 | 15.0 | (9.2–23.4) | 73 | 73.0 | (63.4–80.8) | 12 | 12.0 | (6.9–20.0) |
| Consumption of fruit | 12 | 12.0 | (6.9–20.0) | 46 | 46.0 | (36.5–55.8) | 42 | 42.0 | (32.7–51.9) |
| Consumption of vegetables | 3 | 3.0 | (1.0–8.9) | 83 | 83.0 | (74.3–89.2) | 14 | 14.0 | (8.5–22.3) |
| Consumption of dairy products | 23 | 23.0 | (15.8–32.3) | 56 | 56.0 | (46.1–65.4) | 21 | 21.0 | (14.1–30.1) |
| Consumption of meat | 16 | 16.0 | (10.0–24.6) | 74 | 74.0 | (64.5–81.7) | 10 | 10.0 | (5.5–17.6) |
| Consumption of fish | 21 | 21.0 | (14.1–30.1) | 72 | 72.0 | (62.4–79.9) | 7 | 7.0 | (3.4–14.0) |
| Consumption of eggs | 14 | 14.0 | (8.5–22.3) | 71 | 71.0 | (61.3–79.1) | 15 | 15.0 | (9.2–23.4) |
| Consumption of convenience food | 50 | 50.0 | (40.3–59.7) | 42 | 42.0 | (32.7–51.9) | 8 | 8.0 | (4.0–15.2) |
| Consumption of sweets | 39 | 39.0 | (29.9–48.9) | 34 | 34.0 | (25.4–43.8) | 27 | 27.0 | (19.2–36.6) |
| Consumption of soft drinks | 44 | 44.0 | (34.6–53.9) | 44 | 44.0 | (34.6–53.9) | 12 | 12.0 | (6.9–20.0) |
| Intermediate tertile Spanish HEI (n = 98) | |||||||||
| Consumption of cereals | 8 | 8.2 | (4.1–15.5) | 69 | 70.4 | (60.6–78.6) | 21 | 21.4 | (14.4–30.7) |
| Consumption of legumes | 16 | 16.3 | (10.2–25.0) | 67 | 68.4 | (58.5–76.8) | 15 | 15.3 | (9.4–23.9) |
| Consumption of fruit | 14 | 14.3 | (8.6–22.7) | 46 | 46.9 | (37.3–56.8) | 38 | 38.8 | (29.6–48.8) |
| Consumption of vegetables | 13 | 13.3 | (7.8–21.6) | 57 | 58.2 | (48.2–67.5) | 28 | 28.6 | (20.5–38.3) |
| Consumption of dairy products | 20 | 20.4 | (13.5–29.6) | 57 | 58.2 | (48.2–67.5) | 21 | 21.4 | (14.4–30.7) |
| Consumption of meat | 21 | 21.4 | (14.4–30.7) | 62 | 63.3 | (53.3–72.2) | 15 | 15.3 | (9.4–23.9) |
| Consumption of fish | 28 | 28.6 | (20.5–38.3) | 56 | 57.1 | (47.2–66.6) | 14 | 14.3 | (8.6–22.7) |
| Consumption of eggs | 10 | 10.2 | (5.6–18.0) | 71 | 72.4 | (62.8–80.4) | 17 | 17.3 | (11.0–26.2) |
| Consumption of convenience food | 51 | 52.0 | (42.2–61.8) | 39 | 39.8 | (30.6–49.8) | 8 | 8.2 | (4.1–15.5) |
| Consumption of sweets | 38 | 38.8 | (29.6–48.8) | 32 | 32.7 | (24.1–42.6) | 28 | 28.6 | (20.5–38.3) |
| Consumption of soft drinks | 38 | 38.8 | (29.6–48.8) | 43 | 43.9 | (34.4–53.9) | 17 | 17.3 | (11.0–26.2) |
| Lowest tertile Spanish HEI (n = 105) | |||||||||
| Consumption of cereals | 9 | 8.6 | (4.5–15.7) | 74 | 70.5 | (61.0–78.4) | 22 | 21.0 | (14.2–29.8) |
| Consumption of legumes | 26 | 24.8 | (17.4–33.9) | 66 | 62.9 | (53.2–71.6) | 13 | 12.4 | (7.3–20.2) |
| Consumption of fruit | 22 | 21.0 | (14.2–29.8) | 45 | 42.9 | (33.7–52.5) | 38 | 36.2 | (27.6–45.8) |
| Consumption of vegetables | 14 | 13.3 | (8.0–21.3) | 61 | 58.1 | (48.4–67.2) | 30 | 28.6 | (20.7–38.0) |
| Consumption of dairy products | 14 | 13.3 | (8.0–21.3) | 71 | 67.6 | (58.1–75.9) | 20 | 19.0 | (12.6–27.7) |
| Consumption of meat | 9 | 8.6 | (4.5–15.7) | 73 | 69.5 | (60.0–77.6) | 23 | 21.9 | (15.0–30.9) |
| Consumption of fish | 27 | 25.7 | (18.2–34.9) | 60 | 57.1 | (47.5–66.3) | 18 | 17.1 | (11.1–25.6) |
| Consumption of eggs | 14 | 13.3 | (8.0–21.3) | 73 | 69.5 | (60.0–77.6) | 18 | 17.1 | (11.1–25.6) |
| Consumption of convenience food | 40 | 38.1 | (29.3–47.8) | 50 | 47.6 | (38.2–57.2) | 15 | 14.3 | (8.8–22.4) |
| Consumption of sweets | 36 | 34.3 | (25.8–43.9) | 35 | 33.3 | (25.0–42.9) | 34 | 32.4 | (24.1–41.9) |
| Consumption of soft drinks | 31 | 29.5 | (21.6–39.0) | 47 | 44.8 | (35.5–54.4) | 27 | 25.7 | (18.2–34.9) |
| Total (n = 303) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Decrease | No Changes | Increase | |||||||
| n | % | 95% CI | n | % | 95% CI | n | % | 95% CI | |
| Highest tertile Spanish HEI (n = 100) | |||||||||
| Amount of food consumed | 21 | 21.0 | (14.1–30.1) | 50 | 50.0 | (40.3–59.7) | 29 | 29.0 | (20.9–38.7) |
| Variety of foods consumed | 13 | 13.0 | (7.7–21.2) | 67 | 67.0 | (57.2–75.5) | 20 | 20.0 | (13.3–29.0) |
| Regularity of meal hours | 33 | 33.0 | (24.5–42.8) | 49 | 49.0 | (39.3–58.8) | 18 | 18.0 | (11.6–26.8) |
| Meals skipped | 23 | 23.0 | (15.8–32.3) | 50 | 50.0 | (40.3–59.7) | 27 | 27.0 | (19.2–36.6) |
| Consumption of snacks between meals | 18 | 18.0 | (11.6–26.8) | 27 | 27.0 | (19.2–36.6) | 55 | 55.0 | (45.1–64.5) |
| Consumption of fresh food | 18 | 18.0 | (11.6–26.8) | 57 | 57.0 | (47.1–66.4) | 25 | 25.0 | (17.5–34.4) |
| Consumption of packaged food | 22 | 22.0 | (14.9–31.2) | 57 | 57.0 | (47.1–66.4) | 21 | 21.0 | (14.1–30.1) |
| Intermediate tertile Spanish HEI (n = 98) | |||||||||
| Amount of food consumed | 23 | 23.5 | (16.1–32.9) | 46 | 46.9 | (37.3–56.8) | 29 | 29.6 | (21.4–39.4) |
| Variety of foods consumed | 17 | 17.3 | (11.0–26.2) | 64 | 65.3 | (55.4–74.1) | 17 | 17.3 | (11.0–26.2) |
| Regularity of meal hours | 42 | 42.9 | (33.4–52.8) | 39 | 39.8 | (30.6–49.8) | 17 | 17.3 | (11.0–26.2) |
| Meals skipped | 24 | 24.5 | (17.0–34.0) | 47 | 48.0 | (38.2–57.8) | 27 | 27.6 | (19.6–37.2) |
| Consumption of snacks between meals | 11 | 11.2 | (6.3–19.2) | 25 | 25.5 | (17.8–35.1) | 62 | 63.3 | (53.3–72.2) |
| Consumption of fresh food | 17 | 17.3 | (11.0–26.2) | 51 | 52.0 | (42.2–61.8) | 30 | 30.6 | (22.3–40.4) |
| Consumption of packaged food | 22 | 22.4 | (15.2–31.8) | 55 | 56.1 | (46.1–65.6) | 21 | 21.4 | (14.4–30.7) |
| Lowest tertile Spanish HEI (n = 105) | |||||||||
| Amount of food consumed | 24 | 22.9 | (15.8–31.9) | 43 | 41.0 | (31.9–50.6) | 38 | 36.2 | (27.6–45.8) |
| Variety of foods consumed | 21 | 20.0 | (13.4–28.8) | 56 | 53.3 | (43.7–62.7) | 28 | 26.7 | (19.1–36.0) |
| Regularity of meal hours | 46 | 43.8 | (34.6–53.4) | 39 | 37.1 | (28.4–46.8) | 20 | 19.0 | (12.6–27.7) |
| Meals skipped | 21 | 20.0 | (13.4–28.8) | 52 | 49.5 | (40.1–59.0) | 32 | 30.5 | (22.4–40.0) |
| Consumption of snacks between meals | 22 | 21.0 | (14.2–29.8) | 29 | 27.6 | (19.9–37.0) | 54 | 51.4 | (41.9–60.9) |
| Consumption of fresh food | 25 | 23.8 | (16.6–32.9) | 56 | 53.3 | (43.7–62.7) | 24 | 22.9 | (15.8–31.9) |
| Consumption of packaged food | 31 | 29.5 | (21.6–39.0) | 50 | 47.6 | (38.2–57.2) | 24 | 22.9 | (15.8–31.9) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aguilar-Martínez, A.; Bosque-Prous, M.; González-Casals, H.; Colillas-Malet, E.; Puigcorbé, S.; Esquius, L.; Espelt, A. Social Inequalities in Changes in Diet in Adolescents during Confinement Due to COVID-19 in Spain: The DESKcohort Project. Nutrients 2021, 13, 1577. https://doi.org/10.3390/nu13051577
Aguilar-Martínez A, Bosque-Prous M, González-Casals H, Colillas-Malet E, Puigcorbé S, Esquius L, Espelt A. Social Inequalities in Changes in Diet in Adolescents during Confinement Due to COVID-19 in Spain: The DESKcohort Project. Nutrients. 2021; 13(5):1577. https://doi.org/10.3390/nu13051577
Chicago/Turabian StyleAguilar-Martínez, Alicia, Marina Bosque-Prous, Helena González-Casals, Ester Colillas-Malet, Susanna Puigcorbé, Laura Esquius, and Albert Espelt. 2021. "Social Inequalities in Changes in Diet in Adolescents during Confinement Due to COVID-19 in Spain: The DESKcohort Project" Nutrients 13, no. 5: 1577. https://doi.org/10.3390/nu13051577
APA StyleAguilar-Martínez, A., Bosque-Prous, M., González-Casals, H., Colillas-Malet, E., Puigcorbé, S., Esquius, L., & Espelt, A. (2021). Social Inequalities in Changes in Diet in Adolescents during Confinement Due to COVID-19 in Spain: The DESKcohort Project. Nutrients, 13(5), 1577. https://doi.org/10.3390/nu13051577










