Cardiovascular Imaging in Obesity
Abstract
1. Introduction
2. Cardiovascular Imaging in Obesity
2.1. Transthoracic Echocardiography (TTE)
2.2. Nuclear Cardiology (NC)
2.3. Coronary Computed Tomography Angiography (CCTA)
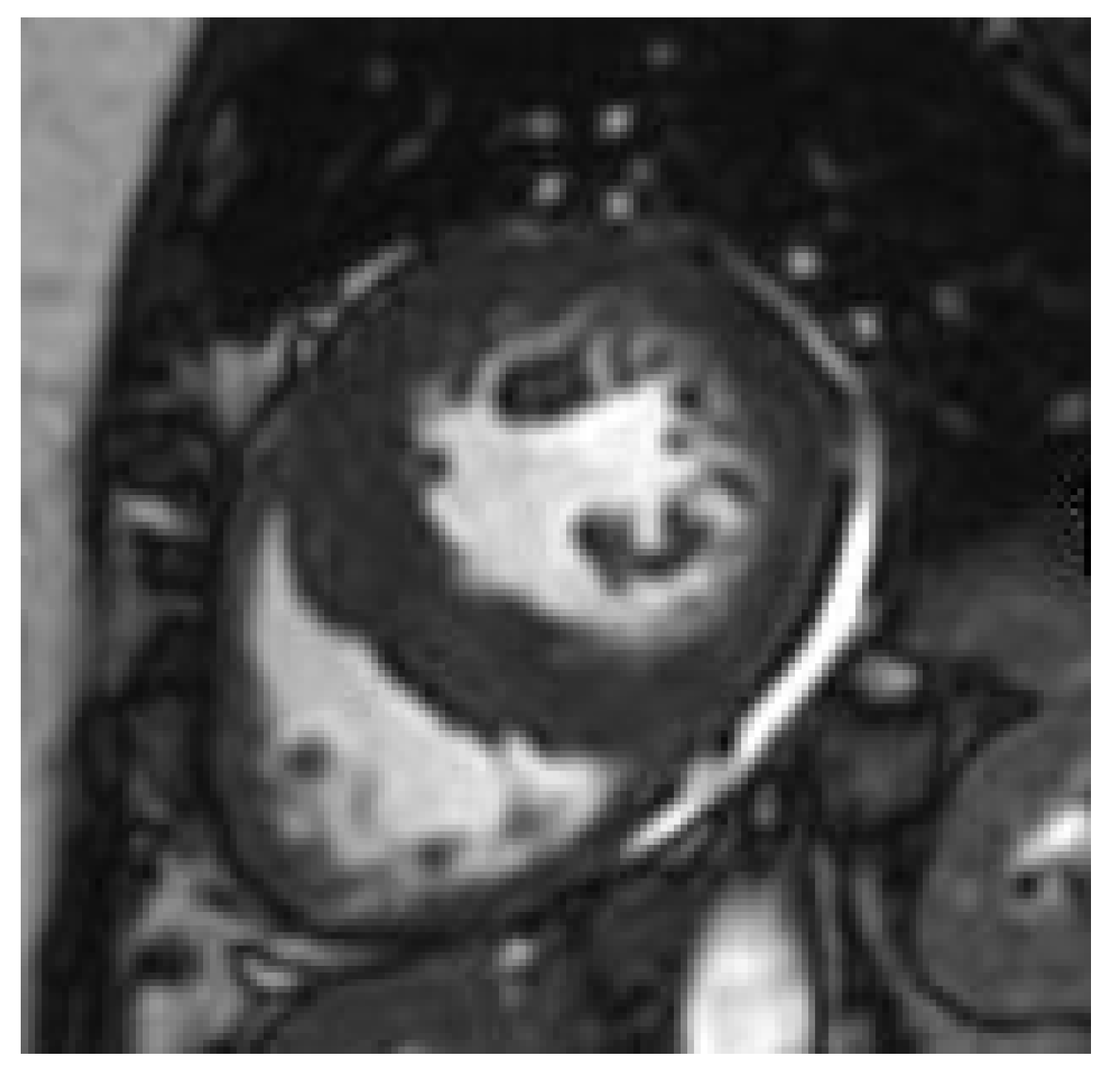
2.4. The Emerging Role of CMR in Obesity
3. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization (WHO). Obesity and Overweight. Fact Sheet No 311. 2015. Available online: https://www.who.int/news-room/factsheets/detail/obesity-and-overweight (accessed on 17 September 2020).
- Lobstein, T.; Jackson-Leach, R.; Moodie, M.L.; Hall, K.D.; Gortmaker, S.L.; Swinburn, B.; James, W.P.T.; Wang, Y.; McPherson, K. Child and adolescent obesity: Part of a bigger picture. Lancet 2015, 385, 2510–2520. [Google Scholar] [CrossRef]
- Ogden, C.L.; Carroll, M.D.; Kit, B.K.; Flegal, K.M. Prevalence of Obesity and Trends in Body Mass Index Among US Children and Adolescents, 1999–2010. JAMA 2012, 307, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Coelho, M.; Oliveira, T.; Fernandes, R. State of the art paper Biochemistry of adipose tissue: An endocrine organ. Arch. Med. Sci. 2013, 9, 191–200. [Google Scholar] [CrossRef]
- Valle, M.; Martos, R.; Gascón, F.; Cañete, R.; Zafra, M.; Morales, R. Low-grade systemic inflammation, hypoadiponectinemia and a high concentration of leptin are present in very young obese children, and correlate with metabolic syndrome. Diabetes Metab. 2005, 31, 55–62. [Google Scholar] [CrossRef]
- Skinner, A.C.; Perrin, E.M.; Moss, L.A.; Skelton, J.A. Cardiometabolic Risks and Severity of Obesity in Children and Young Adults. N. Engl. J. Med. 2015, 373, 1307–1317. [Google Scholar] [CrossRef]
- Bjerregaard, L.G.; Jensen, B.W.; Ängquist, L.; Osler, M.; Sørensen, T.I.; Baker, J.L. Change in Overweight from Childhood to Early Adulthood and Risk of Type 2 Diabetes. N. Engl. J. Med. 2018, 378, 1302–1312. [Google Scholar] [CrossRef] [PubMed]
- Geserick, M.; Vogel, M.; Gausche, R.; Lipek, T.; Spielau, U.; Keller, E.; Pfäffle, R.; Kiess, W.; Körner, A. Acceleration of BMI in Early Childhood and Risk of Sustained Obesity. N. Engl. J. Med. 2018, 379, 1303–1312. [Google Scholar] [CrossRef]
- Dobbs, R.; Sawers, C.; Thompson, F.; Manyika, J.; Woetzel, J.; Child, P.; McKenna, S.; Spatharou, A. Overcoming Obesity: An Initial Economic Analysis; McKinsey Global Institute: Jakarta, Indonesia, 2014; pp. 1–120. [Google Scholar]
- Bouzas-Mosquera, A.; Broullón, F.J.; Álvarez-García, N.; Peteiro, J.; Mosquera, V.X.; Castro-Beiras, A. Association of Left Ventricular Mass with All-Cause Mortality, Myocardial Infarction and Stroke. PLoS ONE 2012, 7, e45570. [Google Scholar] [CrossRef]
- Stanton, T.; Leano, R.; Marwick, T.H. Prediction of all-cause mortality from global longitudinal speckle strain: Comparison with ejection fraction and wall motion scoring. Circ. Cardiovasc. Imaging 2009, 2, 356–364. [Google Scholar] [CrossRef]
- Ng, A.C.; Strudwick, M.; Van Der Geest, R.J.; Ng, A.C.; Gillinder, L.; Goo, S.Y.; Cowin, G.; Delgado, V.; Wang, W.Y.; Bax, J.J. Impact of Epicardial Adipose Tissue, Left Ventricular Myocardial Fat Content, and Interstitial Fibrosis on Myocardial Contractile Function. Circ. Cardiovasc. Imaging 2018, 11, e007372. [Google Scholar] [CrossRef]
- Manson, J.E.; Colditz, G.A.; Stampfer, M.J.; Willett, W.C.; Rosner, B.; Monson, R.R.; Speizer, F.E.; Hennekens, C.H. A Prospective Study of Obesity and Risk of Coronary Heart Disease in Women. N. Engl. J. Med. 1990, 322, 882–889. [Google Scholar] [CrossRef]
- Wilson, P.W.; D’Agostino, R.B.; Sullivan, L.; Parise, H.; Kannel, W.B. Overweight and obesity as determinants of cardiovascular risk: The Framingham experience. Arch. Int. Med. 2002, 162, 1867–1872. [Google Scholar] [CrossRef] [PubMed]
- Poirier, P.; Giles, T.D.; Bray, G.A.; Hong, Y.; Stern, J.S.; Pi-Sunyer, F.X.; Eckel, R.H.; American Heart Association. Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Obesity and cardiovascular disease: Pathophysiology, evalua-tion, and effect of weight loss: An update of the 1997 American Heart Association Scientific Statement on Obesity and Heart Disease from the Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Circulation 2006, 113, 898–918. [Google Scholar]
- Oreopoulos, A.; Padwal, R.; Kalantar-Zadeh, K.; Fonarow, G.C.; Norris, C.M.; McAlister, F.A. Body mass index and mortality in heart failure: A meta-analysis. Am. Hear. J. 2008, 156, 13–22. [Google Scholar] [CrossRef]
- Ahmed, A.; Blackman, M.R.; White, M.; Anker, S.D. Emphasis on abdominal obesity as a modifier of eplerenone effect in heart failure: Hypothesis-generating signals from EMPHASIS-HF. Eur. J. Hear. Fail. 2017, 19, 1198–1200. [Google Scholar] [CrossRef]
- Olivier, A.; Pitt, B.; Girerd, N.; Lamiral, Z.; Machu, J.-L.; McMurray, J.J.V.; Swedberg, K.; Van Veldhuisen, D.J.; Collier, T.J.; Pocock, S.J.; et al. Effect of eplerenone in patients with heart failure and reduced ejection fraction: Potential effect modification by abdominal obesity. Insight from the EMPHASIS-HF trial. Eur. J. Hear. Fail. 2017, 19, 1186–1197. [Google Scholar] [CrossRef] [PubMed]
- Karason, K.; Mølgaard, H.; Wikstrand, J.; Sjöström, L. Heart rate variability in obesity and the effect of weight loss. Am. J. Cardi-ol. 1999, 83, 1242–1247. [Google Scholar] [CrossRef]
- Jouven, X.; Desnos, M.; Guerot, C.; Ducimetière, P. Predicting sudden death in the population: The Paris Prospective Study I. Circulation 1999, 99, 1978–1983. [Google Scholar] [CrossRef] [PubMed]
- Di Salvo, G.; Pacileo, G.; Del Giudice, E.M.; Natale, F.; Limongeli, G.; Verrengia, M.; Rea, A.; Fratta, F.; Castaldi, B.; D’Andrea, A.; et al. Abnormal myocardial deformation properties in obese, non-hypertensive children: An ambulatory blood pressure monitor-ing, standard echocardiographic, and strain rate imaging study. Eur. Heart J. 2006, 27, 2689–2695. [Google Scholar] [CrossRef]
- Krumholz, H.M.; Larson, M.; Levy, D. Prognosis of left ventricular geometric patterns in the Framingham heart study. J. Am. Coll. Cardiol. 1995, 25, 879–884. [Google Scholar] [CrossRef]
- Dhuper, S.; Abdullah, R.A.; Weichbrod, L.; Mahdi, E.; Cohen, H.W. Association of Obesity and Hypertension With Left Ventricular Geometry and Function in Children and Adolescents. Obesity 2011, 19, 128–133. [Google Scholar] [CrossRef]
- Rider, O.J.; Lewandowski, A.; Nethononda, R.; Petersen, S.E.; Francis, J.M.; Pitcher, A.; Holloway, C.J.; Dass, S.; Banerjee, R.; Byrne, J.P.; et al. Gender specific differences in left ventricular remodelling in obesity: Insights from cardiovascular magnetic resonance im-aging. Eur. Heart J. 2013, 34, 292–299. [Google Scholar] [CrossRef]
- Saritas, T.; Tascilar, E.; Abaci, A.; Yozgat, Y.; Dogan, M.; Dundaroz, R.; Hasimi, A.; Yesilkaya, E.; Lenk, M.K.; Kilic, A. Importance of plasma N-terminal pro B-type natriuretic peptide, epicardial adipose tissue, and carotid intima-media thicknesses in asymp-tomatic obese children. Pediatr. Cardiol. 2010, 31, 792–799. [Google Scholar] [CrossRef]
- Chinali, M.; De Simone, G.; Roman, M.J.; Lee, E.T.; Best, L.G.; Howard, B.V.; Devereux, R.B. Impact of Obesity on Cardiac Geometry and Function in a Population of Adolescents. J. Am. Coll. Cardiol. 2006, 47, 2267–2273. [Google Scholar] [CrossRef] [PubMed]
- Mehta, S.K.; Richards, N.; Lorber, R.; Rosenthal, G.L. Abdominal obesity, waist circumference, body mass index, and echocardio-graphic measures in children and adolescents. Congenit. Hear. Dis. 2009, 4, 338–347. [Google Scholar] [CrossRef] [PubMed]
- Mogelvang, R.; Sogaard, P.; Pedersen, S.A.; Olsen, N.T.; Marott, J.L.; Schnohr, P.; Goetze, J.P.; Jensen, J.S. Cardiac Dysfunction Assessed by Echocardiographic Tissue Doppler Imaging Is an Independent Predictor of Mortality in the General Population. Circ. 2009, 119, 2679–2685. [Google Scholar] [CrossRef]
- Koopman, L.P.; McCrindle, B.W.; Slorach, C.; Chahal, N.; Hui, W.; Sarkola, T.; Manlhiot, C.; Jaeggi, E.T.; Bradley, T.J.; Mertens, L. Interac-tion between myocardial and vascular changes in obese children: A pilot study. J. Am. Soc. Echocardiogr. 2012, 25, 401–410. [Google Scholar] [CrossRef] [PubMed]
- Saltijeral, A.; De Isla, L.P.; Pérez-Rodríguez, O.; Rueda, S.; Fernandez-Golfin, C.; Almeria, C.; Rodrigo, J.L.; Gorissen, W.; Rementeria, J.; Marcos-Alberca, P.; et al. Early myocardial deformation changes associated to isolated obesity: A study based on 3D-wall mo-tion tracking analysis. Obesity 2011, 19, 2268–2273. [Google Scholar] [CrossRef] [PubMed]
- Mavrogeni, S.I.; Kitas, G.D.; Dimitroulas, T.; Sfikakis, P.P.; Seo, P.; Gabriel, S.; Patel, A.R.; Gargani, L.; Bombardieri, S.; Matucci-Cerinic, M.; et al. Cardiovascular magnetic resonance in rheumatology: Current status and recommendations for use. Int. J. Cardiol. 2016, 217, 135–148. [Google Scholar] [CrossRef] [PubMed]
- Abel, E.D.; Litwin, S.E.; Sweeney, G. Cardiac remodelling in obesity. Physiol. Rev. 2008, 88, 389–419. [Google Scholar] [CrossRef]
- Aurigemma, G.P.; Zile, M.R.; Gaasch, W.H. Response to Letter Regarding Article “Contractile Behavior of the Left Ventricle in Diastolic Heart Failure: With Emphasis on Regional Systolic Function”. Circulation 2006, 114, e14. [Google Scholar] [CrossRef]
- Di Bello, V.; Santini, F.; Di Cori, A.; Pucci, A.; Palagi, C.; Delle Donne, M.G.; Giannetti, M.; Talini, E.; Nardi, C.; Pedrizzetti, G.; et al. Rela-tionship between preclinical abnormalities of global and regional left ventricular function and insulin resistance in severe obesity: A Color Doppler Imaging Study. Int. J. Obes. 2006, 30, 948–956. [Google Scholar] [CrossRef][Green Version]
- Miyoshi, H.; Oishi, Y.; Mizuguchi, Y.; Iuchi, A.; Nagase, N.; Ara, N.; Oki, T. Contribution of obesity to left atrial and left ventricular dysfunction in asymptomatic patients with hypertension: A two-dimensional speckle-tracking echocardiographic study. J. Am. Soc. Hypertens. 2014, 8, 54–63. [Google Scholar] [CrossRef] [PubMed]
- Barbosa, M.M.; Beleigoli, A.M.; de Fatima Diniz, M.; Freire, C.V.; Ribeiro, A.L.; Nunes, M.C. Strain imaging in morbid obesity: In-sights into subclinical ventricular dysfunction. Clin. Cardiol. 2011, 34, 288–293. [Google Scholar] [CrossRef]
- Di Bello, V.; Fabiani, I.; Conte, L.; Barletta, V.; Delle Donne, M.G.; Cuono, C.; Leo, L.A.; Dini, F.L.; Marzilli, M.; Pinchera, A.; et al. New echocardiographic techniques in the evaluation of left ventricular function in obesity. Obesity 2013, 21, 881–892. [Google Scholar] [CrossRef] [PubMed]
- Monte, I.P.; Mangiafico, S.; Buccheri, S.; Arcidiacono, A.A.; Lavanco, V.; Privitera, F.; Leggio, S.; Deste, W.; Tamburino, C. Early changes of left ventricular geometry and deformational analysis in obese subjects without cardiovascular risk factors: A three-dimensional and speckle tracking echocardiographic study. Int. J. Cardiovasc. Imaging 2014, 30, 1037–1047. [Google Scholar] [CrossRef] [PubMed]
- Wong, C.Y.; O’Moore-Sullivan, T.; Leano, R.; Byrne, N.; Beller, E.; Marwick, T.H. Alterations of left ventricular myocardial charac-teristics associated with obesity. Circulation 2004, 110, 3081–3087. [Google Scholar] [CrossRef]
- Powell, B.D.; Redfield, M.M.; Bybee, K.A.; Freeman, W.K.; Rihal, C.S. Association of Obesity With Left Ventricular Remodeling and Diastolic Dysfunction in Patients Without Coronary Artery Disease. Am. J. Cardiol. 2006, 98, 116–120. [Google Scholar] [CrossRef] [PubMed]
- McManus, D.D.; Xanthakis, V.; Sullivan, L.M.; Zachariah, J.; Aragam, J.; Larson, M.G.; Benjamin, E.J.; Vasan, R.S. Longitudinal Tracking of Left Atrial Diameter Over the Adult Life Course: Clinical Correlates in the Community. Circ. 2010, 121, 667–674. [Google Scholar] [CrossRef]
- Di Salvo, G.; Pacileo, G.; Del Giudice, E.M.; Natale, F.; Limongelli, G.; Verrengia, M.; Rea, A.; Fratta, F.; Castaldi, B.; Gala, S.; et al. Atrial myocardial deformation properties in obese non hypertensive children. J. Am. Soc. Echocardiogr. 2008, 21, 151–156. [Google Scholar] [CrossRef]
- Taguchi, R.; Takasu, J.; Itani, Y.; Yamamoto, R.; Yokoyama, K.; Watanabe, S.; Masuda, Y. Pericardial fat accumulation in men as a risk factor for coronary artery disease. Atheroscler. 2001, 157, 203–209. [Google Scholar] [CrossRef]
- Natale, F.; Tedesco, M.A.; Mocerino, R.; De Simone, V.; Di Marco, G.M.; Aronne, L.; Credendino, M.; Siniscalchi, C.; Calabrò, P.; Cotrufo, M.; et al. Visceral adiposity and arterial stiffness: Echocardiographic epicardial fat thickness reflects, better than waist circumference, carotid arterial stiffness in a large population of hypertensives. Eur. J. Echocardiogr. 2009, 10, 549–555. [Google Scholar] [CrossRef]
- Mahabadi, A.A.; Massaro, J.M.; Rosito, G.A.; Levy, D.; Murabito, J.M.; Wolf, P.A.; O’Donnell, C.J.; Fox, C.S.; Hoffmann, U. Association of pericardial fat, intrathoracic fat, and visceral abdominal fat with cardiovascular disease burden: The Framingham Heart Study. Eur. Hear. J. 2008, 30, 850–856. [Google Scholar] [CrossRef]
- Chahal, H.; McClelland, R.L.; Tandri, H.; Jain, A.; Turkbey, E.B.; Hundley, W.G.; Barr, R.G.; Kizer, J.; Lima, J.A.C.; Bluemke, D.A.; et al. Obesi-ty and right ventricular structure and function: The MESA-Right Ventricle Study. Chest 2012, 141, 388–395. [Google Scholar] [CrossRef] [PubMed]
- Senior, R.; Becher, H.; Monaghan, M.; Agati, L.; Zamorano, J.; Vanoverschelde, J.L.; Nihoyannopoulos, P. Contrast echocardiog-raphy: Evidence-based recommendations by European Association of Echocardiography. Eur. J. Echocardiogr. 2009, 10, 194–212. [Google Scholar] [CrossRef] [PubMed]
- Crea, P.; Zito, C.; Piccione, M.C.; Arcidiaco, S.; Todaro, M.C.; Oreto, L.; Navarra, G.; Carerj, S. The Role of Echocardiography in the Evaluation of Cardiac Damage in Hypertensive Obese Patient. High Blood Press. Cardiovasc. Prev. 2014, 22, 23–27. [Google Scholar] [CrossRef]
- Aurigemma, G.P.; De Simone, G.; Fitzgibbons, T.P. Cardiac Remodeling in Obesity. Circ. Cardiovasc. Imaging 2013, 6, 142–152. [Google Scholar] [CrossRef]
- Cerqueira, M.D.; Nguyen, P.; Staehr, P.; Underwood, S.R.; Iskandrian, A.E. ADVANCE-MPI Trial Investigators. Effects of age, gen-der, obesity, and diabetes on the efficacy and safety of the selective A2A agonist regadenoson versus adenosine in myocar-dial perfusion imaging integrated ADVANCE-MPI trial results. JACC Cardiovasc. Imaging 2008, 1, 307–316. [Google Scholar] [CrossRef]
- Lim, S.P.; Arasaratnam, P.; Chow, B.J.; Beanlands, R.S.; Hessian, R.C. Obesity and the Challenges of Noninvasive Imaging for the Detection of Coronary Artery Disease. Can. J. Cardiol. 2015, 31, 223–226. [Google Scholar] [CrossRef] [PubMed]
- Bateman, T.M.; Maddahi, J.; Udelson, J.; Beanlands, R.; Knuuti, J.; Heller, G.; Berman, D.; Lazewatsky, J.; Orlandi, C. IMPROVED ASSESSMENT OF CAD IN OBESE SUBJECTS WITH FLURPIRIDAZ F18 PET MYOCARDIAL PERFUSION IMAGING: A SUBSET ANALYSIS OF THE FLURPIRIDAZ F18 301 PHASE 3 STUDY. J. Am. Coll. Cardiol. 2016, 67, 1578. [Google Scholar] [CrossRef]
- Nakazato, R.; Tamarappoo, B.K.; Kang, X.; Wolak, A.; Kite, F.; Hayes, S.W.; Thomson, L.E.; Friedman, J.D.; Berman, D.S.; Slomka, P.J. Quan-titative upright-supine high-speed SPECT myocardial perfusion imaging for detection of coronary artery disease: Correla-tion with invasive coronary angiography. J. Nucl. Med. 2010, 51, 1724–1731. [Google Scholar] [CrossRef]
- Petretta, M.; Storto, G.; Pellegrino, T.; Bonaduce, D.; Cuocolo, A. Quantitative Assessment of Myocardial Blood Flow with SPECT. Prog. Cardiovasc. Dis. 2015, 57, 607–614. [Google Scholar] [CrossRef]
- Pellegrino, T.; Piscopo, V.; Boemio, A.; Russo, B.; De Matteis, G.; Pellegrino, S.; Giorgio, S.M.; Amato, M.; Petretta, M.; Cuocolo, A. Im-pact of obesity and acquisition protocol on (123)I-metaiodobenzylguanidine indexes of cardiac sympathetic innervation. Quant. Imaging Med. Surg. 2015, 5, 822–828. [Google Scholar] [PubMed]
- Cecco, C.N.; Schoepf, U.J. Future of cardiac computed tomography. World J. Radiol. 2015, 7, 421–423. [Google Scholar] [CrossRef]
- Messerli, M.; Maywald, C.; Wälti, S.; Warschkow, R.; Wildermuth, S.; Alkadhi, H.; Leschka, S.; Schiesser, M. Prognostic Value of Neg-ative Coronary CT Angiography in Severely Obese Patients Prior to Bariatric Surgery: A Follow-Up After 6 Years. Obes. Surg. 2017, 27, 2044–2049. [Google Scholar] [CrossRef] [PubMed]
- Mangold, S.; Wichmann, J.L.; Schoepf, U.J.; Caruso, D.; Tesche, C.; Steinberg, D.H.; Varga-Szemes, A.; Stubenrauch, A.C.; Bayer, R.R., 2nd; Biancalana, M.; et al. Diagnostic accuracy of coronary CT angiography using 3rd-generation dual-source CT and automated tube voltage selection: Clinical application in a non-obese and obese patient population. Eur. Radiol. 2017, 27, 2298–2308. [Google Scholar] [CrossRef]
- Mitchell, B.M.; Gutin, B.; Kapuku, G.; Barbeau, P.; Humphries, M.C.; Owens, S.; Vemulapalli, S.; Allison, J. Left Ventricular Structure and Function in Obese Adolescents: Relations to Cardiovascular Fitness, Percent Body Fat, and Visceral Adiposity, and Effects of Physical Training. Pediatr. 2002, 109, e73. [Google Scholar] [CrossRef] [PubMed]
- Heydari, B.; Jerosch-Herold, M.; Kwong, R.Y. Assessment of Myocardial Ischemia with Cardiovascular Magnetic Resonance. Prog. Cardiovasc. Dis. 2011, 54, 191–203. [Google Scholar] [CrossRef]
- Shah, R.V.; Heydari, B.; Coelho-Filho, O.; Abbasi, S.A.; Feng, J.H.; Neilan, T.G.; Francis, S.; Blankstein, R.; Steigner, M.; Jerosch-Herold, M.; et al. Vasodilator Stress Perfusion CMR Imaging Is Feasible and Prognostic in Obese Patients. JACC Cardiovasc. Imaging 2014, 7, 462–472. [Google Scholar] [CrossRef] [PubMed]
- Jing, L.; Binkley, C.M.; Suever, J.D.; Umasankar, N.; Haggerty, C.M.; Rich, J.; Nevius, C.D.; Wehner, G.J.; Hamlet, S.M.; Powell, D.K.; et al. Cardiac remodeling and dysfunction in childhood obesity: A cardiovascular magnetic resonance study. J. Cardiovasc. Magn. Reson. 2016, 18, 28. [Google Scholar] [CrossRef]
- Jing, L.; Pulenthiran, A.; Nevius, C.D.; Mejia-Spiegeler, A.; Suever, J.D.; Wehner, G.J.; Kirchner, H.L.; Haggerty, C.M.; Fornwalt, B.K. Im-paired right ventricular contractile function in childhood obesity and its association with right and left ventricular changes: A cine DENSE cardiac magnetic resonance study. J. Cardiovasc. Magn. Reson. 2017, 19, 49. [Google Scholar] [CrossRef] [PubMed]

| Modalities | Availability | Cost | Expertise | Radiation | Kidney Toxicity | Acoustic Window Dependency | Operator Dependency | Attenuation Artifacts |
|---|---|---|---|---|---|---|---|---|
| Echo | ++++ | + | ++++ | ‒ | ‒ | ++++ | ++++ | − |
| SPECT/PET | ++++ | +++ | +++ | +++ | − | − | − | ++++ |
| CCTA | +++ | +++ | +++ | +++ | +++ | − | − | − |
| CMR | ++ | ++++ | ++ | − | ++ | − | − | − |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mavrogeni, S.I.; Bacopoulou, F.; Markousis-Mavrogenis, G.; Chrousos, G.; Charmandari, E. Cardiovascular Imaging in Obesity. Nutrients 2021, 13, 744. https://doi.org/10.3390/nu13030744
Mavrogeni SI, Bacopoulou F, Markousis-Mavrogenis G, Chrousos G, Charmandari E. Cardiovascular Imaging in Obesity. Nutrients. 2021; 13(3):744. https://doi.org/10.3390/nu13030744
Chicago/Turabian StyleMavrogeni, Sophie I., Flora Bacopoulou, George Markousis-Mavrogenis, George Chrousos, and Evangelia Charmandari. 2021. "Cardiovascular Imaging in Obesity" Nutrients 13, no. 3: 744. https://doi.org/10.3390/nu13030744
APA StyleMavrogeni, S. I., Bacopoulou, F., Markousis-Mavrogenis, G., Chrousos, G., & Charmandari, E. (2021). Cardiovascular Imaging in Obesity. Nutrients, 13(3), 744. https://doi.org/10.3390/nu13030744










