Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids
Abstract
1. Introduction
2. Obesity Related Diseases
3. Appetite Regulation
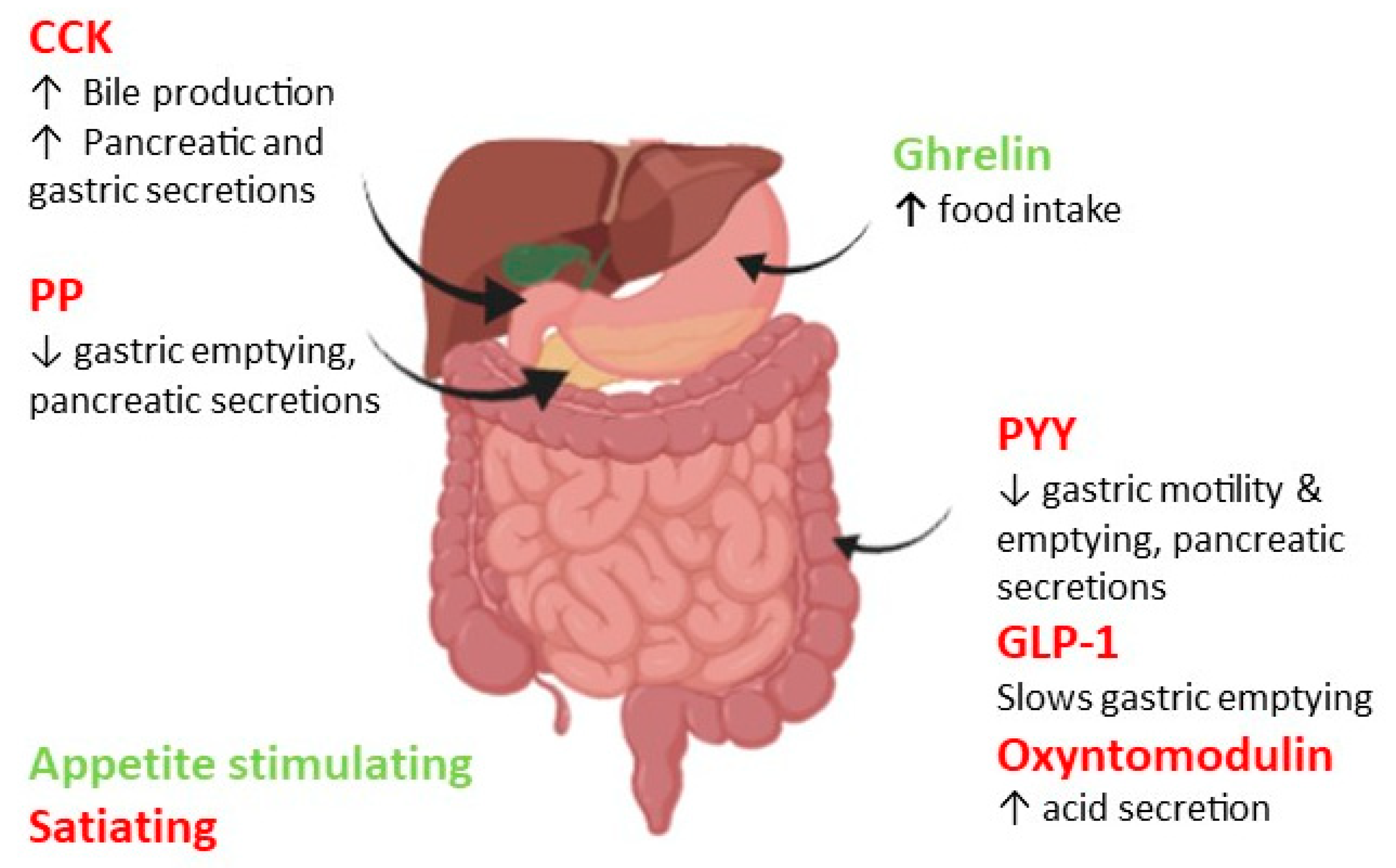
4. Gut Hormones and Appetite Regulation
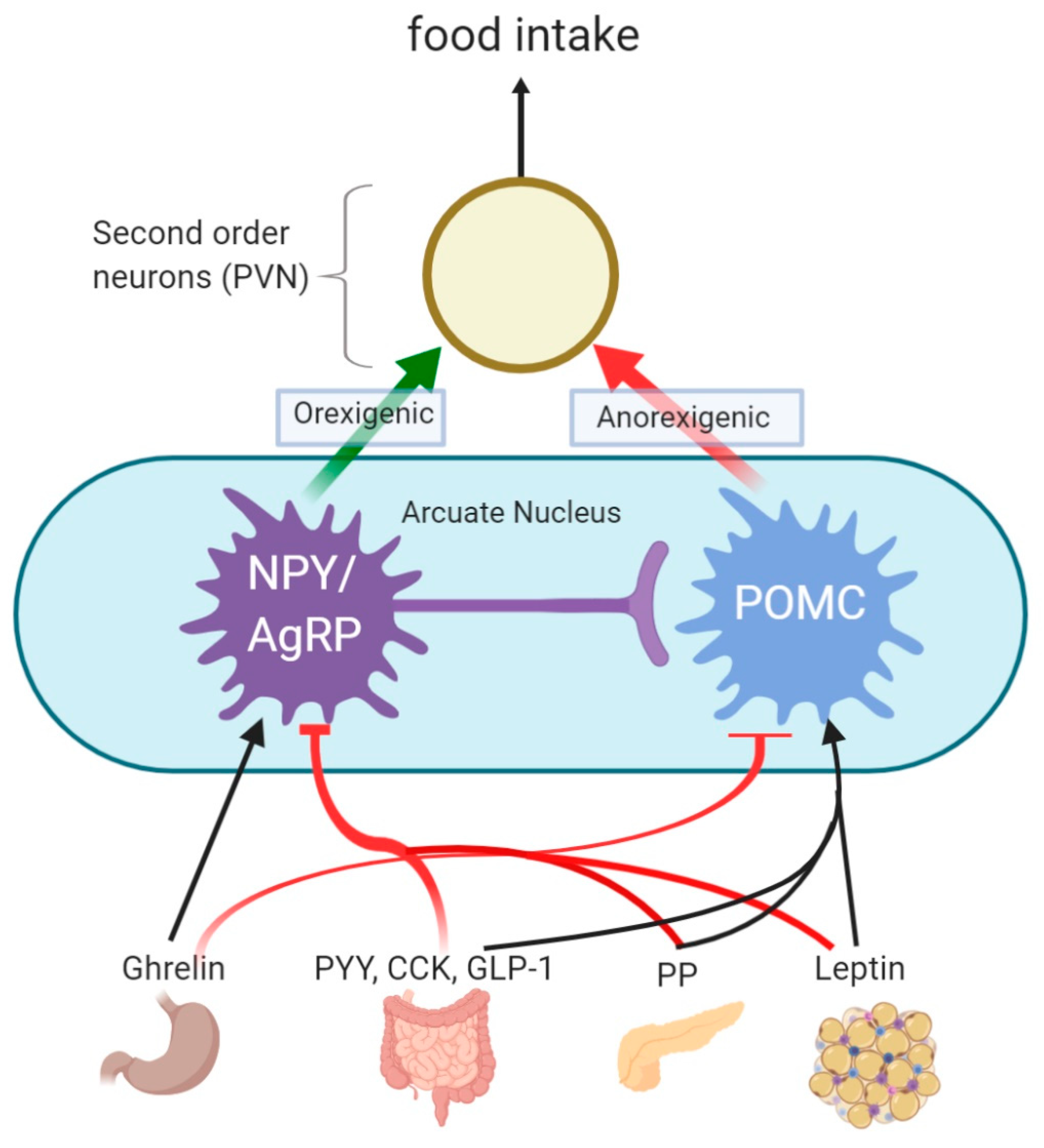
5. Signalling Pathways of Appetite Regulation
6. The Gastrointestinal Tract and Appetite Regulation
7. Relationship between Gut Hormones and Obesity
8. Gut Hormones in the Treatment of Obesity
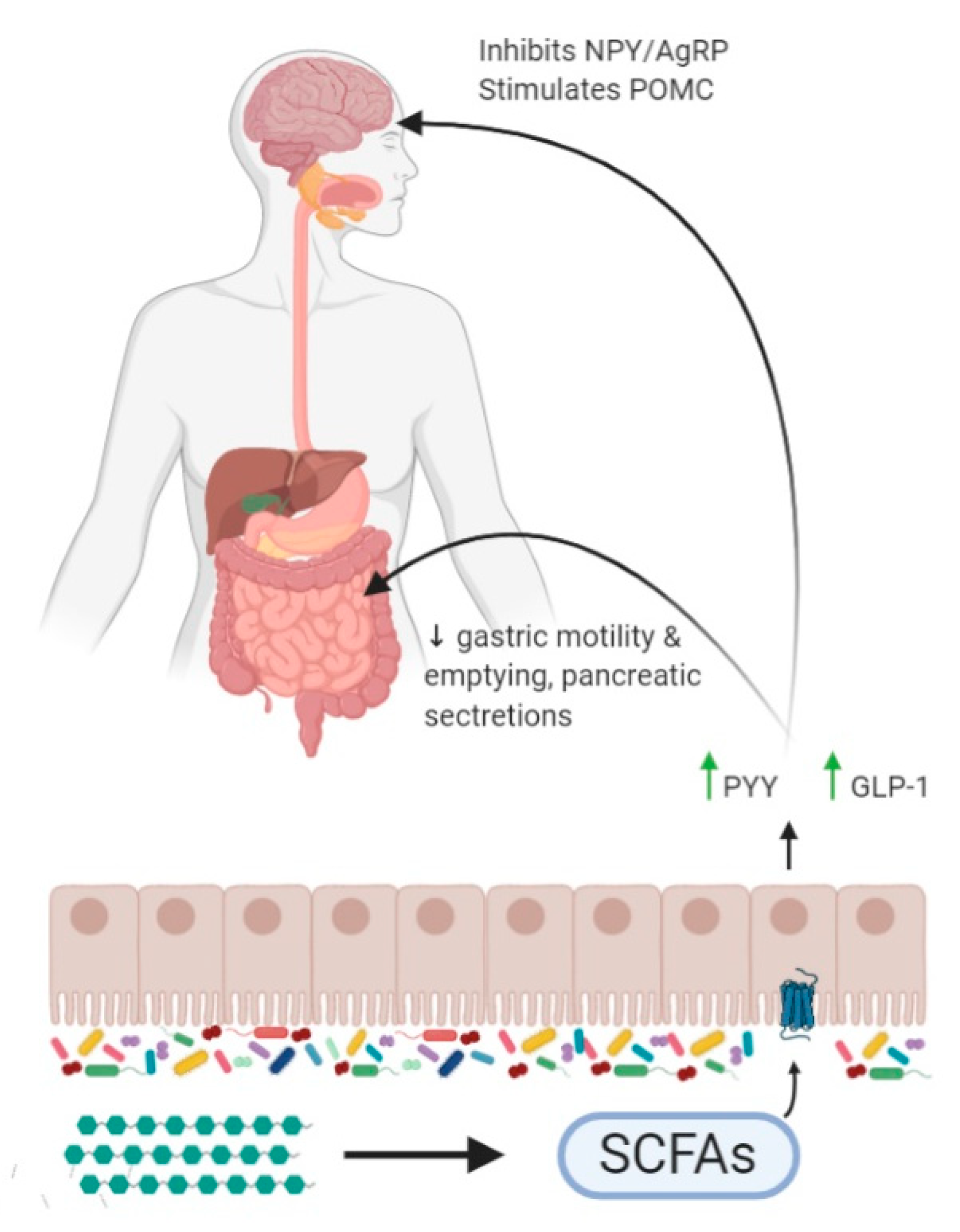
9. Short Chain Fatty Acids and Appetite Regulation
10. The Role of Other Dietary Factors in the Treatment of Obesity
11. Future Directions
12. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| T2DM | Type 2 diabetes mellitus |
| NICE | The National Institute of Care and Excellence |
| RYGB | Roux-en-Y gastric bypass |
| VTA | ventral tegmental area |
| NA | nucleus acumbens |
| ARC | arcuate nucleus |
| AgRP | Agouti-related peptide |
| POMC | proopiomelanocortin |
| CART | Cocaine and amphetamine-regulated transcript |
| MC3/4R | melanocortin 3 and 4 receptors |
| NTS | nucleus of the solitary tract |
| LPN | lateral parabrachial nucleus |
| CCK | cholecystokinin |
| GLP-1 | Glucagon-like peptide-1 |
| PYY | peptide tyrosine tyrosine |
| PP | Pancreatic polypeptide |
| PVN | Paraventricular nucleus of hypothalamus |
| PP | pancreatic polypeptide |
| NPY | Neuropeptide Y |
| OXM | Oxyntomodulin |
| GOAT | Ghrelin O-acyltransferase |
| RCT | Randomised Controlled Trial |
| SNPs | single nucleotide polymorphisms |
| FTO | fat mass and obesity-associated |
| SCFAs | Short-chain fatty acids |
| NDC | non-digestible carbohydrates |
| FFAR2/3 | free fatty acids receptors 2 and 3 |
References
- Swinburn, B.A.; Kraak, V.I.; Allender, S.; Atkins, V.J.; Baker, P.I.; Bogard, J.R.; Brinsden, H.; Calvillo, A.; De Schutter, O.; Devarajan, R.; et al. The Global Syndemic of Obesity, Undernutrition, and Climate Change: The Lancet Commission Report. Lancet 2019, 23, 791–846. [Google Scholar] [CrossRef]
- The World Health Organisation. Obesity and Overweight; The World Health Organisation: Geneva, Switzerland, 2018. [Google Scholar]
- Baker, C. Obesity Statistics, House of Commons Library Briefing Paper 3336; London, UK, 2019.
- Hales, C.M.; Carroll, M.D.; Fryar, C.D.; Ogden, C.L. Prevalence of Obesity and Severe Obesity among Adults: United States, 2017–2018, Key Findings Data from the National Health and Nutrition Examination Survey; Department of Health and Human Services: Washington, DC, USA, 2020.
- WHO. Attaining the Nine Global Noncommunicable Diseases Targets; A Shared Responsibility; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- Lauby-Secretan, B.; Scoccianti, C.; Loomis, D.; Grosse, Y.; Bianchini, F.; Straif, K. Body Fatness and Cancer—Viewpoint of the IARC Working Group. N. Engl. J. Med. 2016, 375, 794–798. [Google Scholar] [CrossRef] [PubMed]
- Afshin, A.; Forouzanfar, M.H.; Reitsma, M.B.; Sur, P.; Estep, K.; Lee, A.; Marczak, L.; Mokdad, A.H.; Moradi-Lakeh, M.; Naghavi, M.; et al. Health Effects of Overweight and Obesity in 195 Countries over 25 Years. N. Engl. J. Med. 2017, 377, 13–27. [Google Scholar] [CrossRef] [PubMed]
- Must, A.; Spadano, J.; Coakley, E.H.; Field, A.E.; Colditz, G.; Dietz, W.H. The Disease Burden Associated with Overweight and Obesity. J. Am. Med. Assoc. 1999, 282, 1523–1529. [Google Scholar] [CrossRef] [PubMed]
- Pi-Sunyer, X. The Medical Risks of Obesity. Postgrad. Med. 2009, 121, 21–33. [Google Scholar] [CrossRef]
- Wang, Y.C.; McPherson, K.; Marsh, T.; Gortmaker, S.L.; Brown, M. Health and Economic Burden of the Projected Obesity Trends in the USA and the UK. Lancet 2011, 378, 815–825. [Google Scholar] [CrossRef]
- Lobstein, T.; Jackson-Leach, R. Estimated Burden of Paediatric Obesity and Co-Morbidities in Europe. Part 2. Numbers of Children with Indicators of Obesity-Related Disease. Int. J. Pediatr. Obes. 2006, 1, 33–41. [Google Scholar] [CrossRef]
- Gov.uk. Health Matters: Obesity and the Food Environment. 2017; p. 1. Available online: https://www.gov.uk/government/publications/health-matters-obesity-and-the-food-environment/health-matters-obesity-and-the-food-environment--2 (accessed on 31 March 2017).
- Waters, H.; Graf, M. America’s Obesity Crisis: The Health and Economic Costs of Excess Weight. Available online: https://milkeninstitute.org/sites/default/files/reports-pdf/Mi-Americas-Obesity-Crisis-WEB.pdf (accessed on 2 May 2020).
- Nguyen, D.M.; El-Serag, H.B. The Epidemiology of Obesity. Gastroenterol. Clin. N. Am. 2010, 1–7. [Google Scholar] [CrossRef]
- Huvenne, H.; Dubern, B.; Clément, K.; Poitou, C. Rare Genetic Forms of Obesity: Clinical Approach and Current Treatments in 2016. Obes. Facts 2016, 9, 158–173. [Google Scholar] [CrossRef]
- Grimm, E.R.; Steinle, N.I. Genetics of Eating Behavior: Established and Emerging Concepts. Nutr. Rev. 2011, 69, 52–60. [Google Scholar] [CrossRef]
- Delzenne, N.; Blundell, J.; Brouns, F.; Cunningham, K.; De Graaf, K.; Erkner, A.; Lluch, A.; Mars, M.; Peters, H.P.F.; Westerterp-Plantenga, M. Gastrointestinal Targets of Appetite Regulation in Humans. Obes. Rev. 2010, 234–250. [Google Scholar] [CrossRef] [PubMed]
- Cummings, D.E.; Overduin, J. Gastrointestinal Regulation of Food Intake. J. Clin. Investig. 2007, 117, 13–23. [Google Scholar] [CrossRef] [PubMed]
- Field, B.C.T. Neuroendocrinology of Obesity. Br. Med. Bull. 2014, 109, 73–82. [Google Scholar] [CrossRef] [PubMed]
- Hall, K.D.; Kahan, S. Maintenance of Lost Weight and Long-Term Management of Obesity. Med. Clin. N. Am. 2018, 102, 183–197. [Google Scholar] [CrossRef]
- Jeffery, R.W.; Epstein, L.H.; Wilson, G.T.; Drewnowski, A.; Stunkard, A.J.; Wing, R.R. Long-Term Maintenance of Weight Loss: Current Status. Health Psychol. 2000, 19 (Suppl. 1), 5–16. [Google Scholar] [CrossRef]
- Turk, M.W.; Yang, K.; Hravnak, M.; Sereika, S.M.; Ewing, L.J.; Burke, L.E. Randomized Clinical Trials of Weight-Loss Maintenance: A Review. J. Cardiovasc. Nurs. 2009, 24, 58–80. [Google Scholar] [CrossRef]
- NICE. Recommendations | Obesity: Identification, Assessment and Management; NICE: London, UK, 2019. [Google Scholar]
- Rucker, D.; Padwal, R.; Li, S.K.; Curioni, C.; Lau, D.C.W. Long Term Pharmacotherapy for Obesity and Overweight: Updated Meta-Analysis. Br. Med. J. 2007, 335, 1194–1199. [Google Scholar] [CrossRef]
- Ballinger, A. Orlistat in the Treatment of Obesity. Expert Opin. Pharmacother. 2000, 1, 841–847. [Google Scholar] [CrossRef]
- Smith, B.R.; Schauer, P.; Nguyen, N.T. Surgical Approaches to the Treatment of Obesity: Bariatric Surgery. Med. Clin. N. Am. 2008, 95, 943–964. [Google Scholar] [CrossRef]
- Marczuk, P.; Kubisa, M.J.; Święch, M.; Walędziak, M.; Kowalewski, P.; Major, P.; Pędziwiatr, M.; Paśnik, K.; Janik, M.R. Effectiveness and Safety of Roux-En-Y Gastric Bypass in Elderly Patients—Systematic Review and Meta-Analysis. Obes. Surg. 2019, 29, 361–368. [Google Scholar] [CrossRef]
- Dayan, D.; Kuriansky, J.; Abu-Abeid, S. Weight Regain Following Roux-En-Y Gastric Bypass: Etiology and Surgical Treatment. Isr. Med. Assoc. J. 2019, 21, 823–828. [Google Scholar] [PubMed]
- Le Roux, C.W.; Aylwin, S.J.B.; Batterham, R.L.; Borg, C.M.; Coyle, F.; Prasad, V.; Shurey, S.; Ghatei, M.A.; Patel, A.G.; Bloom, S.R. Gut Hormone Profiles Following Bariatric Surgery Favor an Anorectic State, Facilitate Weight Loss, and Improve Metabolic Parameters. Ann. Surg. 2006, 243, 108–114. [Google Scholar] [CrossRef] [PubMed]
- Pournaras, D.J.; Osborne, A.; Hawkins, S.C.; Mahon, D.; Ghatei, M.A.; Bloom, S.R.; Welbourn, R.; Le Roux, C.W. The Gut Hormone Response Following Roux-En-Y Gastric Bypass: Cross-Sectional and Prospective Study. Obes. Surg. 2010, 20, 56–60. [Google Scholar] [CrossRef] [PubMed]
- Le Roux, C.W.; Welbourn, R.; Werling, M.; Osborne, A.; Kokkinos, A.; Laurenius, A.; Lönroth, H.; Fändriks, L.; Ghatei, M.A.; Bloom, S.R.; et al. Gut Hormones as Mediators of Appetite and Weight Loss after Roux-En-Y Gastric Bypass. Ann. Surg. 2007, 246, 780–785. [Google Scholar] [CrossRef]
- Druce, M.; Bloom, S.R. The Regulation of Appetite. Arch. Dis. Child. 2006, 92, 183–187. [Google Scholar] [CrossRef]
- Hinney, A.; Vogel, C.I.G.; Hebebrand, J. From Monogenic to Polygenic Obesity: Recent Advances. Eur. Child Adolesc. Psychiatry 2010, 297–310. [Google Scholar] [CrossRef]
- Yu, J.H.; Kim, M.-S. Molecular Mechanisms of Appetite Regulation. Diabetes Metab. J. 2012, 36, 391–398. [Google Scholar] [CrossRef]
- Farr, O.M.; Li, C.R.; Mantzoros, C.S.; Farr, O. Central Nervous System Regulation of Eating: Insights from Human Brain Imaging HHS Public Access. Metabolism 2016, 65, 699–713. [Google Scholar] [CrossRef]
- Wren, A.M.; Bloom, S.R. Gut Hormones and Appetite Control. Gastroenterology 2007, 132, 2116–2130. [Google Scholar] [CrossRef]
- Vogel, H.; Mendoza, J.; Coccurello, R.; Maccarrone, M. Hedonic Eating and the Delicious Circle: From Lipid-Derived Mediators to Brain Dopamine and Back. Front. Neurosci. 2018, 1, 271. [Google Scholar] [CrossRef]
- Rehfeld, J.F. The New Biology of Gastrointestinal Hormones. Physiol. Rev. 1998, 1087–1108. [Google Scholar] [CrossRef] [PubMed]
- Latorre, R.; Sternini, C.; De Giorgio, R.; Greenwood-Van Meerveld, B. Enteroendocrine Cells: A Review of Their Role in Brain-Gut Communication. Neurogastroenterol. Motil. 2016, 28, 620–630. [Google Scholar] [CrossRef] [PubMed]
- Lénárd, L.; Karádi, Z. Regulatory Processes of Hunger Motivated Behavior. Acta Biol. Hung. 2012, 63 (Suppl. 1), 80–88. [Google Scholar] [CrossRef] [PubMed]
- Sam, A.H.; Troke, R.C.; Tan, T.M.; Bewick, G.A. The Role of the Gut/Brain Axis in Modulating Food Intake. Neuropharmacology 2012, 46–56. [Google Scholar] [CrossRef]
- Marić, G.; Gazibara, T.; Zaletel, I.; Labudović Borović, M.; Tomanović, N.; Cirić, M.; Puškaš, N. The Role of Gut Hormones in Appetite Regulation (Review). Acta Physiol. Hung. 2014, 395–407. [Google Scholar] [CrossRef]
- Egerod, K.L.; Engelstoft, M.S.; Grunddal, K.V.; Nøhr, M.K.; Secher, A.; Sakata, I.; Pedersen, J.; Windeløv, J.A.; Füchtbauer, E.M.; Olsen, J.; et al. A Major Lineage of Enteroendocrine Cells Coexpress CCK, Secretin, GIP, GLP-1, PYY, and Neurotensin but Not Somatostatin. Endocrinology 2012, 153, 5782–5795. [Google Scholar] [CrossRef]
- Van Der Klaauw, A.A.; Keogh, J.M.; Henning, E.; Trowse, V.M.; Dhillo, W.S.; Ghatei, M.A.; Farooqi, I.S. High Protein Intake Stimulates Postprandial GLP1 and PYY Release. Obesity 2013, 21, 1602–1607. [Google Scholar] [CrossRef]
- Batterham, R.L.; Cowley, M.A.; Small, C.J.; Herzog, H.; Cohen, M.A.; Dakin, C.L.; Wren, A.M.; Brynes, A.E.; Low, M.J.; Ghatei, M.A.; et al. Gut Hormone PYY3-36 Physiologically Inhibits Food Intake. Nature 2002, 418, 650–654. [Google Scholar] [CrossRef]
- Koda, S.; Date, Y.; Murakami, N.; Shimbara, T.; Hanada, T.; Toshinai, K.; Niijima, A.; Furuya, M.; Inomata, N.; Osuye, K.; et al. The Role of the Vagal Nerve in Peripheral PYY 3–36 -Induced Feeding Reduction in Rats. Endocrinology 2005, 146, 2369–2375. [Google Scholar] [CrossRef]
- De Silva, A.; Salem, V.; Long, C.J.; Makwana, A.; Newbould, R.D.; Rabiner, E.A.; Ghatei, M.A.; Bloom, S.R.; Matthews, P.M.; Beaver, J.D.; et al. The Gut Hormones PYY 3-36 and GLP-1 7-36 Amide Reduce Food Intake and Modulate Brain Activity in Appetite Centers in Humans. Cell Metab. 2011, 14, 700–706. [Google Scholar] [CrossRef]
- Steinert, R.E.; Feinle-Bisset, C.; Asarian, L.; Horowitz, M.; Beglinger, C.; Geary, N.; Ghrelin, C.C.K. GLP-1, and PYY(3-36): Secretory Controls and Physiological Roles in Eating and Glycemia in Health, Obesity, and after RYGB. Physiol. Rev. 2017, 97, 411–463. [Google Scholar] [CrossRef] [PubMed]
- Brereton, M.F.; Vergari, E.; Zhang, Q.; Clark, A. Alpha-, Delta- and PP-Cells: Are They the Architectural Cornerstones of Islet Structure and Co-Ordination? J. Histochem. Cytochem. 2015, 63, 575–591. [Google Scholar] [CrossRef] [PubMed]
- Forssmann, W.G.; Helmstaedter, V.; Metz, J.; Greenberg, J.; Chance, R.E. The Identification of the F-Cell in the Dog Pancreas as the Pancreatic Polypeptide Producing Cell. Histochemistry 1977, 50, 281–290. [Google Scholar] [CrossRef] [PubMed]
- Greider, M.H.; Gersell, D.J.; Gingerich, R.L. Ultrastructural Localization of Pancreatic Polypeptide in the F Cell of the Dog Pancreas. J. Histochem. Cytochem. 1978, 26, 1103–1108. [Google Scholar] [CrossRef]
- Larsson, L.I.; Sundler, F.; Håkanson, R.; Pollock, H.G.; Kimmel, J.R. Localization of APP, a Postulated New Hormone, to a Pancreatic Endocrine Cell Type. Histochemistry 1974, 42, 377–382. [Google Scholar] [CrossRef]
- Michel, M.C.; Beck-Sickinger, A.; Cox, H.; Doods, H.N.; Herzog, H.; Larhammar, D.; Quirion, R.; Schwartz, T.; Westfall, T. International Union of Pharmacology Recommendations for the Nomenclature of Neuropeptide Y, Peptide YY, and Pancreatic Polypeptide Receptors. Pharmacol. Rev. 1998, 50, 143–150. [Google Scholar]
- Essah, P.A.; Levy, J.R.; Sistrun, S.N.; Kelly, S.M.; Nestler, J.E. Effect of Macronutrient Composition on Postprandial Peptide YY Levels. J. Clin. Endocrinol. Metab. 2007, 92, 4052–4055. [Google Scholar] [CrossRef]
- Holst, J.J. On the Physiology of GIP and GLP-1. Horm. Metab. Res. 2004, 747–754. [Google Scholar] [CrossRef]
- Tang-Christensen, M.; Vrang, N.; Larsen, P.J. Glucagon-like Peptide Containing Pathways in the Regulation of Feeding Behaviour. Int. J. Obes. 2001, 25, S42–S47. [Google Scholar] [CrossRef]
- Tucker, J.D.; Dhanvantari, S.; Brubaker, P.L. Proglucagon Processing in Islet and Intestinal Cell Lines. Regul. Pept. 1996, 62, 29–35. [Google Scholar] [CrossRef]
- Yamato, E.; Ikegami, H.; Takekawa, K.; Fujisawa, T.; Nakagawa, Y.; Hamada, Y.; Uedo, H.; Ogihara, T. Tissue-Specific and Glucose-Dependent Expression of Receptor Genes for Glucagon and Glucagon-Like Peptide-1 (GLP-1). Horm. Metab. Res. 1997, 29, 56–59. [Google Scholar] [CrossRef] [PubMed]
- Dakin, C.L.; Gunn, I.; Small, C.J.; Edwards, C.M.B.; Hay, D.L.; Smith, D.M.; Ghatei, M.A.; Bloom, S.R. Oxyntomodulin Inhibits Food Intake in the Rat. Endocrinology 2001, 142, 4244–4250. [Google Scholar] [CrossRef] [PubMed]
- Baggio, L.L.; Huang, Q.; Brown, T.J.; Drucker, D.J. Oxyntomodulin and Glucagon-like Peptide-1 Differentially Regulate Murine Food Intake and Energy Expenditure. Gastroenterology 2004, 127, 546–558. [Google Scholar] [CrossRef] [PubMed]
- Cohen, M.A.; Ellis, S.M.; Le Roux, C.W.; Batterham, R.L.; Park, A.; Patterson, M.; Frost, G.S.; Ghatei, M.A.; Bloom, S.R. Oxyntomodulin Suppresses Appetite and Reduces Food Intake in Humans. J. Clin. Endocrinol. Metab. 2003, 88, 4696–4701. [Google Scholar] [CrossRef] [PubMed]
- Buchman, A.L.; Katz, S.; Fang, J.C.; Bernstein, C.N.; Abou-Assi, S.G. Teduglutide, a Novel Mucosally Active Analog of Glucagon-like Peptide-2 (GLP-2) for the Treatment of Moderate to Severe Crohn’s Disease. Inflamm. Bowel Dis. 2010, 16, 962–973. [Google Scholar] [CrossRef] [PubMed]
- Drucker, D.J.; Ehrlich, P.; Asa, S.L.; Brubaker, P.L. Induction of Intestinal Epithelial Proliferation by Glucagon-like Peptide 2. Proc. Natl. Acad. Sci. USA 1996, 93, 7911–7916. [Google Scholar] [CrossRef]
- Wallis, K.; Walters, J.R.F.; Forbes, A. Review Article: Glucagon-like Peptide 2-Current Applications and Future Directions. Aliment. Pharmacol. Ther. 2007, 365–372. [Google Scholar] [CrossRef]
- Parker, J.A.; McCullough, K.A.; Field, B.C.T.; Minnion, J.S.; Martin, N.M.; Ghatei, M.A.; Bloom, S.R. Glucagon and GLP-1 Inhibit Food Intake and Increase c-Fos Expression in Similar Appetite Regulating Centres in the Brainstem and Amygdala. Int. J. Obes. 2013, 37, 1391–1398. [Google Scholar] [CrossRef]
- Nauck, M.A.; Meier, J.J. Incretin Hormones: Their Role in Health and Disease. Diabetes Obes. Metab. 2018, 5–21. [Google Scholar] [CrossRef]
- Willms, B.; Werner, J.; Holst, J.J.; Ørskov, C.; Creutzfeldt, W.; Nauck, M.A. Gastric Emptying, Glucose Responses, and Insulin Secretion after a Liquid Test Meal: Effects of Exogenous Glucagon-Like Peptide-1 (GLP-1)-(7-36) Amide in Type 2 (Noninsulin-Dependent) Diabetic Patients. J. Clin. Endocrinol. Metab. 1996, 81, 327–332. [Google Scholar] [CrossRef]
- Zander, M.; Madsbad, S.; Madsen, J.L.; Holst, J.J. Effect of 6-Week Course of Glucagon-like Peptide 1 on Glycaemic Control, Insulin Sensitivity, and β-Cell Function in Type 2 Diabetes: A Parallel-Group Study. Lancet 2002, 359, 824–830. [Google Scholar] [CrossRef]
- Yang, N.; Liu, X.; Ding, E.L.; Xu, M.; Wu, S.; Liu, L.; Sun, X.; Hu, F.B. Impaired Ghrelin Response after High-Fat Meals Is Associated with Decreased Satiety in Obese and Lean Chinese Young Adults. J. Nutr. 2009, 139, 1286–1291. [Google Scholar] [CrossRef] [PubMed]
- Wynne, K.; Park, A.J.; Small, C.J.; Meeran, K.; Ghatei, M.A.; Frost, G.S.; Bloom, S.R. Oxyntomodulin Increases Energy Expenditure in Addition to Decreasing Energy Intake in Overweight and Obese Humans: A Randomised Controlled Trial. Int. J. Obes. 2006, 30, 1729–1736. [Google Scholar] [CrossRef] [PubMed]
- Meeran, K.; O’Shea, D.; Edwards, C.M.B.; Turton, M.D.; Heath, M.M.; Gunn, I.; Abusnana, S.; Rossi, M.; Small, C.J.; Goldstone, A.P.; et al. Repeated Intracerebroventricular Administration of Glucagon-Like Peptide-1-(7–36) Amide or Exendin-(9–39) Alters Body Weight in the Rat 1. Endocrinology 1999, 140, 244–250. [Google Scholar] [CrossRef]
- Verdich, C.; Flint, A.; Gutzwiller, J.P.; Näslund, E.; Beglinger, C.; Hellström, P.M.; Long, S.J.; Morgan, L.M.; Holst, J.J.; Astrup, A. A Meta-Analysis of the Effect of Glucagon-like Peptide-1 (7-36) Amide on Ad Libitum Energy Intake in Humans. J. Clin. Endocrinol. Metab. 2001, 86, 4382–4389. [Google Scholar] [CrossRef]
- Drucker, D.J. Glucagon-Like Peptide 2 1. J. Clin. Endocrinol. Metab. 2001, 86, 1759–1764. [Google Scholar] [CrossRef]
- Schmidt, P.T.; Näslund, E.; Grybäck, P.; Jacobsson, H.; Hartmann, B.; Holst, J.J.; Hellström, P.M. Peripheral Administration of GLP-2 to Humans Has No Effect on Gastric Emptying or Satiety. Regul. Pept. 2003, 116, 21–25. [Google Scholar] [CrossRef]
- Liou, A.P.; Lu, X.; Sei, Y.; Zhao, X.; Pechhold, S.; Carrero, R.J.; Raybould, H.E.; Wank, S. The G-Protein-Coupled Receptor GPR40 Directly Mediates Long-Chain Fatty Acid-Induced Secretion of Cholecystokinin. Gastroenterology 2011, 140, 903–912.e4. [Google Scholar] [CrossRef]
- Liou, A.P.; Sei, Y.; Zhao, X.; Feng, J.; Lu, X.; Thomas, C.; Pechhold, S.; Raybould, H.E.; Wank, S.A. The Extracellular Calcium-Sensing Receptor Is Required for Cholecystokinin Secretion in Response to L-Phenylalanine in Acutely Isolated Intestinal I Cells. Am. J. Physiol.-Gastrointest. Liver Physiol. 2011, 300, G538–G546. [Google Scholar] [CrossRef]
- Dockray, G.J. Cholecystokinin. Curr. Opin. Endocrinol. Diabetes Obes. 2012, 19, 8–12. [Google Scholar] [CrossRef]
- Beglinger, S.; Drewe, J.; Schirra, J.; Göke, B.; D’Amato, M.; Beglinger, C. Role of Fat Hydrolysis in Regulating Glucagon-like Peptide-1 Secretion. J. Clin. Endocrinol. Metab. 2010, 95, 879–886. [Google Scholar] [CrossRef] [PubMed]
- Degen, L.; Drewe, J.; Piccoli, F.; Gräni, K.; Oesch, S.; Bunea, R.; D’Amato, M.; Beglinger, C. Effect of CCK-1 Receptor Blockade on Ghrelin and PYY Secretion in Men. Am. J. Physiol.-Regul. Integr. Comp. Physiol. 2007, 292, R1391–R1399. [Google Scholar] [CrossRef] [PubMed]
- Cummings, D.E.; Purnell, J.Q.; Frayo, R.S.; Schmidova, K.; Wisse, B.E.; Weigle, D.S. A Preprandial Rise in Plasma Ghrelin Levels Suggests a Role in Meal Initiation in Humans. Diabetes 2001, 50, 1714–1719. [Google Scholar] [CrossRef] [PubMed]
- Müller, T.D.; Nogueiras, R.; Andermann, M.L.; Andrews, Z.B.; Anker, S.D.; Argente, J.; Batterham, R.L.; Benoit, S.C.; Bowers, C.Y.; Broglio, F.; et al. Ghrelin. Mol. Metab. 2015, 437–460. [Google Scholar] [CrossRef]
- Druce, M.R.; Wren, A.M.; Park, A.J.; Milton, J.E.; Patterson, M.; Frost, G.; Ghatei, M.A.; Small, C.; Bloom, S.R. Ghrelin Increases Food Intake in Obese as Well as Lean Subjects. Int. J. Obes. 2005, 29, 1130–1136. [Google Scholar] [CrossRef]
- Le Roux, C.W.; Patterson, M.; Vincent, R.P.; Hunt, C.; Ghatei, M.A.; Bloom, S.R. Postprandial Plasma Ghrelin Is Suppressed Proportional to Meal Calorie Content in Normal-Weight but Not Obese Subjects. J. Clin. Endocrinol. Metab. 2005, 90, 1068–1071. [Google Scholar] [CrossRef]
- Timper, K.; Brüning, J.C. Hypothalamic Circuits Regulating Appetite and Energy Homeostasis: Pathways to Obesity. DMM Dis. Model. Mech. 2017, 10, 679–689. [Google Scholar] [CrossRef]
- Ilnytska, O.; Argyropoulos, G. The Role of the Agouti-Related Protein in Energy Balance Regulation. Cell. Mol. Life Sci. 2008, 2721–2731. [Google Scholar] [CrossRef]
- Huszar, D.; Lynch, C.A.; Fairchild-Huntress, V.; Dunmore, J.H.; Fang, Q.; Berkemeier, L.R.; Gu, W.; Kesterson, R.A.; Boston, B.A.; Cone, R.D.; et al. Targeted Disruption of the Melanocortin-4 Receptor Results in Obesity in Mice. Cell 1997, 88, 131–141. [Google Scholar] [CrossRef]
- Tao, Y.X. Molecular Mechanisms of the Neural Melanocortin Receptor Dysfunction in Severe Early Onset Obesity. Mol. Cell. Endocrinol. 2005, 239, 1–14. [Google Scholar] [CrossRef]
- Schwartz, G.J. The Role of Gastrointestinal Vagal Afferents in the Control of Food Intake: Current Prospects. Nutrition 2000, 16, 866–873. [Google Scholar] [CrossRef]
- Roman, C.W.; Derkach, V.A.; Palmiter, R.D. Genetically and Functionally Defined NTS to PBN Brain Circuits Mediating Anorexia. Nat. Commun. 2016, 7. [Google Scholar] [CrossRef] [PubMed]
- Ellacott, K.L.J.; Halatchev, I.G.; Cone, R.D. Characterization of Leptin-Responsive Neurons in the Caudal Brainstem. Endocrinology 2006, 147, 3190–3195. [Google Scholar] [CrossRef] [PubMed]
- Ahituv, N.; Kavaslar, N.; Schackwitz, W.; Ustaszewska, A.; Collier, J.M.; Hébert, S.; Doelle, H.; Dent, R.; Pennacchio, L.A.; McPherson, R. A PYY Q62P Variant Linked to Human Obesity. Hum. Mol. Genet. 2006, 15, 387–391. [Google Scholar] [CrossRef][Green Version]
- Bewick, G.A. Bowels Control Brain: Gut Hormones and Obesity. Biochem. Med. 2012, 283–297. [Google Scholar] [CrossRef]
- Clark, J.T.; Kalra, P.S.; Crowley, W.R.; Kalra, S.P. Neuropeptide γ and Human Pancreatic Polypeptide Stimulate Feeding Behavior in Rats. Endocrinology 1984, 115, 427–429. [Google Scholar] [CrossRef]
- Pittner, R.A.; Moore, C.X.; Bhavsar, S.P.; Gedulin, B.R.; Smith, P.A.; Jodka, C.M.; Parkes, D.G.; Paterniti, J.R.; Srivastava, V.P.; Young, A.A. Effects of PYY [3 -36] in Rodent Models of Diabetes and Obesity. Int. J. Obes. 2004, 28, 963–971. [Google Scholar] [CrossRef]
- Sahu, A. Leptin Signaling in the Hypothalamus: Emphasis on Energy Homeostasis and Leptin Resistance. Front. Neuroendocrinol. 2003, 24, 225–253. [Google Scholar] [CrossRef]
- Deloose, E.; Janssen, P.; Depoortere, I.; Tack, J. The Migrating Motor Complex: Control Mechanisms and Its Role in Health and Disease. Nat. Rev. Gastroenterol. Hepatol. 2012, 9, 271–285. [Google Scholar] [CrossRef]
- Deloose, E.; Verbeure, W.; Depoortere, I.; Tack, J. Motilin: From Gastric Motility Stimulation to Hunger Signalling. Nat. Rev. Endocrinol. 2019, 15, 238–250. [Google Scholar] [CrossRef]
- Deloose, E.; Janssen, P.; Lannoo, M.; Van Der Schueren, B.; Depoortere, I.; Tack, J. Higher Plasma Motilin Levels in Obese Patients Decrease after Roux-En-Y Gastric Bypass Surgery and Regulate Hunger. Gut 2016, 65, 1110–1118. [Google Scholar] [CrossRef] [PubMed]
- Montague, C.T.; Farooqi, I.S.; Whitehead, J.P.; Soos, M.A.; Rau, H.; Wareham, N.J.; Sewter, C.P.; Digby, J.E.; Mohammed, S.N.; Hurst, J.A.; et al. Congenital Leptin Deficiency Is Associated with Severe Early-Onset Obesity in Humans. Nature 1997, 387, 903–908. [Google Scholar] [CrossRef] [PubMed]
- Frayling, T.M.; Timpson, N.J.; Weedon, M.N.; Zeggini, E.; Freathy, R.M.; Lindgren, C.M.; Perry, J.R.B.; Elliott, K.S.; Lango, H.; Rayner, N.W.; et al. A Common Variant in the FTO Gene Is Associated with Body Mass Index and Predisposes to Childhood and Adult Obesity. Science 2007, 316, 889–894. [Google Scholar] [CrossRef] [PubMed]
- Fawcett, K.A.; Barroso, I. The Genetics of Obesity: FTO Leads the Way. Trends Genet. 2010, 26, 266–274. [Google Scholar] [CrossRef] [PubMed]
- Karra, E.; O’Daly, O.G.; Choudhury, A.I.; Yousseif, A.; Millership, S.; Neary, M.T.; Scott, W.R.; Chandarana, K.; Manning, S.; Hess, M.E.; et al. A Link between FTO, Ghrelin, and Impaired Brain Food-Cue Responsivity. J. Clin. Investig. 2013, 123, 3539–3551. [Google Scholar] [CrossRef] [PubMed]
- Batterham, R.L.; Cohen, M.A.; Ellis, S.M.; Le Roux, C.W.; Withers, D.J.; Frost, G.S.; Ghatei, M.A.; Bloom, S.R. Inhibition of Food Intake in Obese Subjects by Peptide YY3-36. N. Engl. J. Med. 2003, 349, 941–948. [Google Scholar] [CrossRef] [PubMed]
- Reinehr, T.; Enriori, P.J.; Harz, K.; Cowley, M.A.; Roth, C.L. Pancreatic Polypeptide in Obese Children before and after Weight Loss. Int. J. Obes. 2006, 30, 1476–1481. [Google Scholar] [CrossRef]
- Zipf, W.B.; O’Dorision, T.M.; Cataland, S.; Dixon, K. Pancreatic Polypeptide Responses to Protein Meal Challenges in Obese but Otherwise Normal Children and Obese Children with Prader-Willi Syndrome. J. Clin. Endocrinol. Metab. 1983, 57, 1074–1080. [Google Scholar] [CrossRef]
- Irizarry, K.A.; Miller, M.; Freemark, M.; Haqq, A.M. Prader Willi Syndrome: Genetics, Metabolomics, Hormonal Function, and New Approaches to Therapy. Adv. Pediatr. 2016, 47–77. [Google Scholar] [CrossRef]
- Schellekens, H.; Finger, B.C.; Dinan, T.G.; Cryan, J.F. Ghrelin Signalling and Obesity: At the Interface of Stress, Mood and Food Reward. Pharmacol. Ther. 2012, 316–326. [Google Scholar] [CrossRef]
- Lean, M.E.J.; Malkova, D. Altered Gut and Adipose Tissue Hormones in Overweight and Obese Individuals: Cause or Consequence. Int. J. Obes. 2016, 622–632. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.K.; Singh, R. Pharmacotherapy in Obesity: A Systematic Review and Meta-Analysis of Randomized Controlled Trials of Anti-Obesity Drugs. Expert Rev. Clin. Pharmacol. 2020, 13, 53–64. [Google Scholar] [CrossRef] [PubMed]
- Gantz, I.; Erondu, N.; Mallick, M.; Musser, B.; Krishna, R.; Tanaka, W.K.; Snyder, K.; Stevens, C.; Stroh, M.A.; Zhu, H.; et al. Efficacy and Safety of Intranasal Peptide YY3-36 for Weight Reduction in Obese Adults. J. Clin. Endocrinol. Metab. 2007, 92, 1754–1757. [Google Scholar] [CrossRef] [PubMed]
- Mehta, A.; Marso, S.P.; Neeland, I.J. Liraglutide for Weight Management: A Critical Review of the Evidence. Obes. Sci. Pract. 2017, 3, 3–14. [Google Scholar] [CrossRef]
- O’Neil, P.M.; Birkenfeld, A.L.; McGowan, B.; Mosenzon, O.; Pedersen, S.D.; Wharton, S.; Carson, C.G.; Jepsen, C.H.; Kabisch, M.; Wilding, J.P.H. Efficacy and Safety of Semaglutide Compared with Liraglutide and Placebo for Weight Loss in Patients with Obesity: A Randomised, Double-Blind, Placebo and Active Controlled, Dose-Ranging, Phase 2 Trial. Lancet 2018, 392, 637–649. [Google Scholar] [CrossRef]
- STEP 1: Research Study Investigating How Well Semaglutide Works in People Suffering from Overweight or Obesity. Available online: https://clinicaltrials.gov/ct2/show/NCT03548935 (accessed on 3 December 2020).
- Research Study Investigating How Well Semaglutide Works in People With Type 2 Diabetes Suffering from Overweight or Obesity. Available online: https://clinicaltrials.gov/ct2/show/NCT03552757 (accessed on 3 December 2020).
- Research Study to Look at How Well Semaglutide is at Lowering Weight When Taken Together with an Intensive Lifestyle Program. Available online: https://clinicaltrials.gov/ct2/show/results/NCT03611582 (accessed on 3 December 2020).
- Research Study Investigating How Well Semaglutide Works in People Suffering from Overweight or Obesity. Available online: https://clinicaltrials.gov/ct2/show/results/NCT03548987 (accessed on 3 December 2020).
- Wynne, K.; Park, A.J.; Small, C.J.; Patterson, M.; Ellis, S.M.; Murphy, K.G.; Wren, A.M.; Frost, G.S.; Meeran, K.; Ghatei, M.A.; et al. Subcutaneous Oxyntomodulin Reduces Body Weight in Overweight and Obese Subjects: A Double-Blind, Randomized, Controlled Trial. Diabetes 2005, 54, 2390–2395. [Google Scholar] [CrossRef]
- Mosa, R.; Huang, L.; Li, H.; Grist, M.; LeRoith, D.; Chen, C. Long-Term Treatment with the Ghrelin Receptor Antagonist [D-Lys3]-GHRP-6 Does Not Improve Glucose Homeostasis in Nonobese Diabetic MKR Mice. Am. J. Physiol. Integr. Comp. Physiol. 2018, 314, R71–R83. [Google Scholar] [CrossRef]
- Asakawa, A.; Inui, A.; Kaga, T.; Katsuura, G.; Fujimiya, M.; Fujino, M.A.; Kasuga, M. Antagonism of Ghrelin Receptor Reduces Food Intake and Body Weight Gain in Mice. Gut 2003, 52, 947–952. [Google Scholar] [CrossRef]
- Costantini, V.J.A.; Vicentini, E.; Sabbatini, F.M.; Valerio, E.; Lepore, S.; Tessari, M.; Sartori, M.; Michielin, F.; Melotto, S.; Merlo Pich, E.; et al. GSK1614343, a Novel Ghrelin Receptor Antagonist, Produces an Unexpected Increase of Food Intake and Body Weight in Rodents and Dogs. Neuroendocrinology 2011, 94, 158–168. [Google Scholar] [CrossRef]
- Little, T.J.; Horowitz, M.; Feinle-Bisset, C. Role of Cholecystokinin in Appetite Control and Body Weight Regulation. Obes. Rev. 2005, 297–306. [Google Scholar] [CrossRef]
- Jordan, J.; Greenway, F.; Leiter, L.; Li, Z.; Jacobson, P.; Murphy, K.; Hill, J.; Kler, L.; Aftring, R. Stimulation of Cholecystokinin-A Receptors with GI181771X Does Not Cause Weight Loss in Overweight or Obese Patients. Clin. Pharmacol. Ther. 2008, 83, 281–287. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, J.B.; Gregersen, N.T.; Pedersen, S.D.; Arentoft, J.L.; Ritz, C.; Schwartz, T.W.; Holst, J.J.; Astrup, A.; Sjödin, A. Effects of PYY3-36 and GLP-1 on Energy Intake, Energy Expenditure, and Appetite in Overweight Men. Am. J. Physiol.-Endocrinol. Metab. 2014, 306, E1248–E1256. [Google Scholar] [CrossRef] [PubMed]
- Steinert, R.E.; Poller, B.; Castelli, M.C.; Drewe, J.; Beglinger, C. Oral Administration of Glucagon-like Peptide 1 or Peptide YY 3–36 Affects Food Intake in Healthy Male Subjects. Am. J. Clin. Nutr. 2010, 92, 810–817. [Google Scholar] [CrossRef] [PubMed]
- Behary, P.; Tharakan, G.; Alexiadou, K.; Johnson, N.; Wewer Albrechtsen, N.J.; Kenkre, J.; Cuenco, J.; Hope, D.; Anyiam, O.; Choudhury, S.; et al. Combined GLP-1, Oxyntomodulin, and Peptide YY Improves Body Weight and Glycemia in Obesity and Prediabetes/Type 2 Diabetes: A Randomized, Single-Blinded, Placebo-Controlled Study. Diabetes Care 2019, 42, 1446–1453. [Google Scholar] [CrossRef]
- Ambery, P.; Parker, V.E.; Stumvoll, M.; Posch, M.G.; Heise, T.; Plum-Moerschel, L.; Tsai, L.F.; Robertson, D.; Jain, M.; Petrone, M.; et al. MEDI0382, a GLP-1 and Glucagon Receptor Dual Agonist, in Obese or Overweight Patients with Type 2 Diabetes: A Randomised, Controlled, Double-Blind, Ascending Dose and Phase 2a Study. Lancet 2018, 391, 2607–2618. [Google Scholar] [CrossRef]
- Liu, S.; Willett, W.C.; Manson, J.A.E.; Hu, F.B.; Rosner, B.; Colditz, G. Relation between Changes in Intakes of Dietary Fiber and Grain Products and Changes in Weight and Development of Obesity among Middle-Aged Women. Am. J. Clin. Nutr. 2003, 78, 920–927. [Google Scholar] [CrossRef]
- Ludwig, D.S.; Pereira, M.A.; Kroenke, C.H.; Hilner, J.E.; Van Horn, L.; Slattery, M.L.; Jacobs, D.R. Dietary Fiber, Weight Gain, and Cardiovascular Disease Risk Factors in Young Adults. J. Am. Med. Assoc. 1999, 282, 1539–1546. [Google Scholar] [CrossRef]
- Maskarinec, G.; Takata, Y.; Pagano, I.; Carlin, L.; Goodman, M.T.; Marchand, L.L.; Nomura, A.M.Y.; Wilkens, L.R.; Kolonel, L.N. Trends and Dietary Determinants of Overweight and Obesity in a Multiethnic Population. Obesity 2006, 14, 717–726. [Google Scholar] [CrossRef]
- Cani, P.D.; Joly, E.; Horsmans, Y.; Delzenne, N.M. Oligofructose Promotes Satiety in Healthy Human: A Pilot Study. Eur. J. Clin. Nutr. 2006, 60, 567–572. [Google Scholar] [CrossRef]
- Rigaud, D.; Ryttig, K.R.; Angel, L.A.; Apfelbaum, M. Overweight Treated with Energy Restriction and a Dietary Fibre Supplement: A 6-Month Randomized, Double-Blind, Placebo-Controlled Trial. Int. J. Obes. 1990, 14, 763–769. [Google Scholar]
- Howarth, N.C.; Saltzman, E.; Roberts, S.B. Dietary Fiber and Weight Regulation. Nutr. Rev. 2001, 59, 129–139. [Google Scholar] [CrossRef]
- Cani, P.D. The Gut Microbiota Manages Host Metabolism. Nat. Rev. Endocrinol. 2014, 74–76. [Google Scholar] [CrossRef] [PubMed]
- David, L.A.; Maurice, C.F.; Carmody, R.N.; Gootenberg, D.B.; Button, J.E.; Wolfe, B.E.; Ling, A.V.; Devlin, A.S.; Varma, Y.; Fischbach, M.A.; et al. Diet Rapidly and Reproducibly Alters the Human Gut Microbiome. Nature 2014, 505, 559–563. [Google Scholar] [CrossRef] [PubMed]
- O’Keefe, S.J.D.; Li, J.V.; Lahti, L.; Ou, J.; Carbonero, F.; Mohammed, K.; Posma, J.M.; Kinross, J.; Wahl, E.; Ruder, E.; et al. Fat, Fibre and Cancer Risk in African Americans and Rural Africans. Nat. Commun. 2015, 6. [Google Scholar] [CrossRef] [PubMed]
- Vinolo, M.A.R.; Rodrigues, H.G.; Hatanaka, E.; Sato, F.T.; Sampaio, S.C.; Curi, R. Suppressive Effect of Short-Chain Fatty Acids on Production of Proinflammatory Mediators by Neutrophils. J. Nutr. Biochem. 2011, 22, 849–855. [Google Scholar] [CrossRef] [PubMed]
- Hernández, M.A.G.; Canfora, E.E.; Jocken, J.W.E.; Blaak, E.E. The Short-Chain Fatty Acid Acetate in Body Weight Control and Insulin Sensitivity. Nutrients 2019, 1943. [Google Scholar] [CrossRef] [PubMed]
- Lin, H.V.; Frassetto, A.; Kowalik, E.J.; Nawrocki, A.R.; Lu, M.M.; Kosinski, J.R.; Hubert, J.A.; Szeto, D.; Yao, X.; Forrest, G.; et al. Butyrate and Propionate Protect against Diet-Induced Obesity and Regulate Gut Hormones via Free Fatty Acid Receptor 3-Independent Mechanisms. PLoS ONE 2012, 7, e35240. [Google Scholar] [CrossRef]
- Canfora, E.E.; Van Der Beek, C.M.; Jocken, J.W.E.; Goossens, G.H.; Holst, J.J.; Olde Damink, S.W.M.; Lenaerts, K.; Dejong, C.H.C.; Blaak, E.E. Colonic Infusions of Short-Chain Fatty Acid Mixtures Promote Energy Metabolism in Overweight/Obese Men: A Randomized Crossover Trial. Sci. Rep. 2017, 7. [Google Scholar] [CrossRef]
- Murphy, K.G.; Bloom, S.R. Gut Hormones and the Regulation of Energy Homeostasis. Nature 2006, 854–859. [Google Scholar] [CrossRef]
- Tolhurst, G.; Heffron, H.; Lam, Y.S.; Parker, H.E.; Habib, A.M.; Diakogiannaki, E.; Cameron, J.; Grosse, J.; Reimann, F.; Gribble, F.M. Short-Chain Fatty Acids Stimulate Glucagon-like Peptide-1 Secretion via the G-Protein-Coupled Receptor FFAR2. Diabetes 2012, 61, 364–371. [Google Scholar] [CrossRef]
- Kimura, I.; Inoue, D.; Hirano, K.; Tsujimoto, G. The SCFA Receptor GPR43 and Energy Metabolism. Front. Endocrinol. 2014. [Google Scholar] [CrossRef] [PubMed]
- Bolognini, D.; Tobin, A.B.; Milligan, G.; Moss, C.E. The Pharmacology and Function of Receptors for Short-Chain Fatty Acids. Mol. Pharmacol. 2016, 388–398. [Google Scholar] [CrossRef] [PubMed]
- Licciardi, P.V.; Ververis, K.; Karagiannis, T.C. Histone Deacetylase Inhibition and Dietary Short-Chain Fatty Acids. ISRN Allergy 2011, 2011. [Google Scholar] [CrossRef] [PubMed]
- Frost, G.; Sleeth, M.L.; Sahuri-Arisoylu, M.; Lizarbe, B.; Cerdan, S.; Brody, L.; Anastasovska, J.; Ghourab, S.; Hankir, M.; Zhang, S.; et al. The Short-Chain Fatty Acid Acetate Reduces Appetite via a Central Homeostatic Mechanism. Nat. Commun. 2014, 5. [Google Scholar] [CrossRef]
- Perry, R.J.; Peng, L.; Barry, N.A.; Cline, G.W.; Zhang, D.; Cardone, R.L.; Petersen, K.F.; Kibbey, R.G.; Goodman, A.L.; Shulman, G.I. Acetate Mediates a Microbiome-Brain-β-Cell Axis to Promote Metabolic Syndrome. Nature 2016, 534, 213–217. [Google Scholar] [CrossRef]
- Chambers, E.S.; Viardot, A.; Psichas, A.; Morrison, D.J.; Murphy, K.G.; Zac-Varghese, S.E.K.; MacDougall, K.; Preston, T.; Tedford, C.; Finlayson, G.S.; et al. Effects of Targeted Delivery of Propionate to the Human Colon on Appetite Regulation, Body Weight Maintenance and Adiposity in Overweight Adults. Gut 2015, 64, 1744–1754. [Google Scholar] [CrossRef]
- Chambers, E.S.; Byrne, C.S.; Rugyendo, A.; Morrison, D.J.; Preston, T.; Tedford, C.; Bell, J.D.; Thomas, L.; Akbar, A.N.; Riddell, N.E.; et al. The Effects of Dietary Supplementation with Inulin and Inulin-Propionate Ester on Hepatic Steatosis in Adults with Non-Alcoholic Fatty Liver Disease. Diabetes. Obes. Metab. 2019, 21, 372–376. [Google Scholar] [CrossRef]
- Weitkunat, K.; Schumann, S.; Nickel, D.; Kappo, K.A.; Petzke, K.J.; Kipp, A.P.; Blaut, M.; Klaus, S. Importance of Propionate for the Repression of Hepatic Lipogenesis and Improvement of Insulin Sensitivity in High-Fat Diet-Induced Obesity. Mol. Nutr. Food Res. 2016, 60, 2611–2621. [Google Scholar] [CrossRef]
- Singh, N.; Gurav, A.; Sivaprakasam, S.; Brady, E.; Padia, R.; Shi, H.; Thangaraju, M.; Prasad, P.D.; Manicassamy, S.; Munn, D.H.; et al. Activation of Gpr109a, Receptor for Niacin and the Commensal Metabolite Butyrate, Suppresses Colonic Inflammation and Carcinogenesis. Immunity 2014, 40, 128–139. [Google Scholar] [CrossRef]
- Mathewson, N.D.; Jenq, R.; Mathew, A.V.; Koenigsknecht, M.; Hanash, A.; Toubai, T.; Oravecz-Wilson, K.; Wu, S.R.; Sun, Y.; Rossi, C.; et al. Gut Microbiome-Derived Metabolites Modulate Intestinal Epithelial Cell Damage and Mitigate Graft-versus-Host Disease. Nat. Immunol. 2016, 17, 505–513. [Google Scholar] [CrossRef]
- Hong, J.; Jia, Y.; Pan, S.; Jia, L.; Li, H.; Han, Z.; Cai, D.; Zhao, R. Butyrate Alleviates High Fat Diet-Induced Obesity through Activation of Adiponectin-Mediated Pathway and Stimulation of Mitochondrial Function in the Skeletal Muscle of Mice. Oncotarget 2016, 7, 56071. [Google Scholar] [CrossRef] [PubMed]
- Jia, Y.; Hong, J.; Li, H.; Hu, Y.; Jia, L.; Cai, D.; Zhao, R. Butyrate Stimulates Adipose Lipolysis and Mitochondrial Oxidative Phosphorylation through Histone Hyperacetylation-Associated Β3-Adrenergic Receptor Activation in High-Fat Diet-Induced Obese Mice. Exp. Physiol. 2017, 102, 273–281. [Google Scholar] [CrossRef] [PubMed]
- Byrne, C.S.; Chambers, E.S.; Morrison, D.J.; Frost, G. The Role of Short Chain Fatty Acids in Appetite Regulation and Energy Homeostasis. Int. J. Obes. 2015, 39, 1331–1338. [Google Scholar] [CrossRef] [PubMed]
- Burwick, R.; Shipp, T. Early Neonatal Weight Loss Differs by Mode of Delivery in Healthy Term and Late Preterm Neonates. Am. J. Obstet. Gynecol. 2012, 206, S91. [Google Scholar] [CrossRef]
- Kohanmoo, A.; Faghih, S.; Akhlaghi, M. Effect of Short-and Long-Term Protein Consumption on Appetite and Appetite-Regulating Gastrointestinal Hormones, a Systematic Review and Meta-Analysis of Randomized Controlled Trials. Physiol. Behav. 2020, 226, 113123. [Google Scholar] [CrossRef]
- Bendtsen, L.Q.; Lorenzen, J.K.; Gomes, S.; Liaset, B.; Holst, J.J.; Ritz, C.; Reitelseder, S.; Sjödin, A.; Astrup, A. Effects of Hydrolysed Casein, Intact Casein and Intact Whey Protein on Energy Expenditure and Appetite Regulation: A Randomised, Controlled, Cross-over Study. Br. J. Nutr. 2014, 112, 1412–1422. [Google Scholar] [CrossRef]
- Pesta, D.H.; Samuel, V.T. A High-Protein Diet for Reducing Body Fat: Mechanisms and Possible Caveats. Nutr. Metab. 2014, 11. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alhabeeb, H.; AlFaiz, A.; Kutbi, E.; AlShahrani, D.; Alsuhail, A.; AlRajhi, S.; Alotaibi, N.; Alotaibi, K.; AlAmri, S.; Alghamdi, S.; et al. Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids. Nutrients 2021, 13, 481. https://doi.org/10.3390/nu13020481
Alhabeeb H, AlFaiz A, Kutbi E, AlShahrani D, Alsuhail A, AlRajhi S, Alotaibi N, Alotaibi K, AlAmri S, Alghamdi S, et al. Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids. Nutrients. 2021; 13(2):481. https://doi.org/10.3390/nu13020481
Chicago/Turabian StyleAlhabeeb, Habeeb, Ali AlFaiz, Emad Kutbi, Dayel AlShahrani, Abdullah Alsuhail, Saleh AlRajhi, Nemer Alotaibi, Khalid Alotaibi, Saad AlAmri, Saleh Alghamdi, and et al. 2021. "Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids" Nutrients 13, no. 2: 481. https://doi.org/10.3390/nu13020481
APA StyleAlhabeeb, H., AlFaiz, A., Kutbi, E., AlShahrani, D., Alsuhail, A., AlRajhi, S., Alotaibi, N., Alotaibi, K., AlAmri, S., Alghamdi, S., & AlJohani, N. (2021). Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids. Nutrients, 13(2), 481. https://doi.org/10.3390/nu13020481





