Association between Egg Consumption and Cholesterol Concentration: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Abstract
1. Introduction
2. Methods
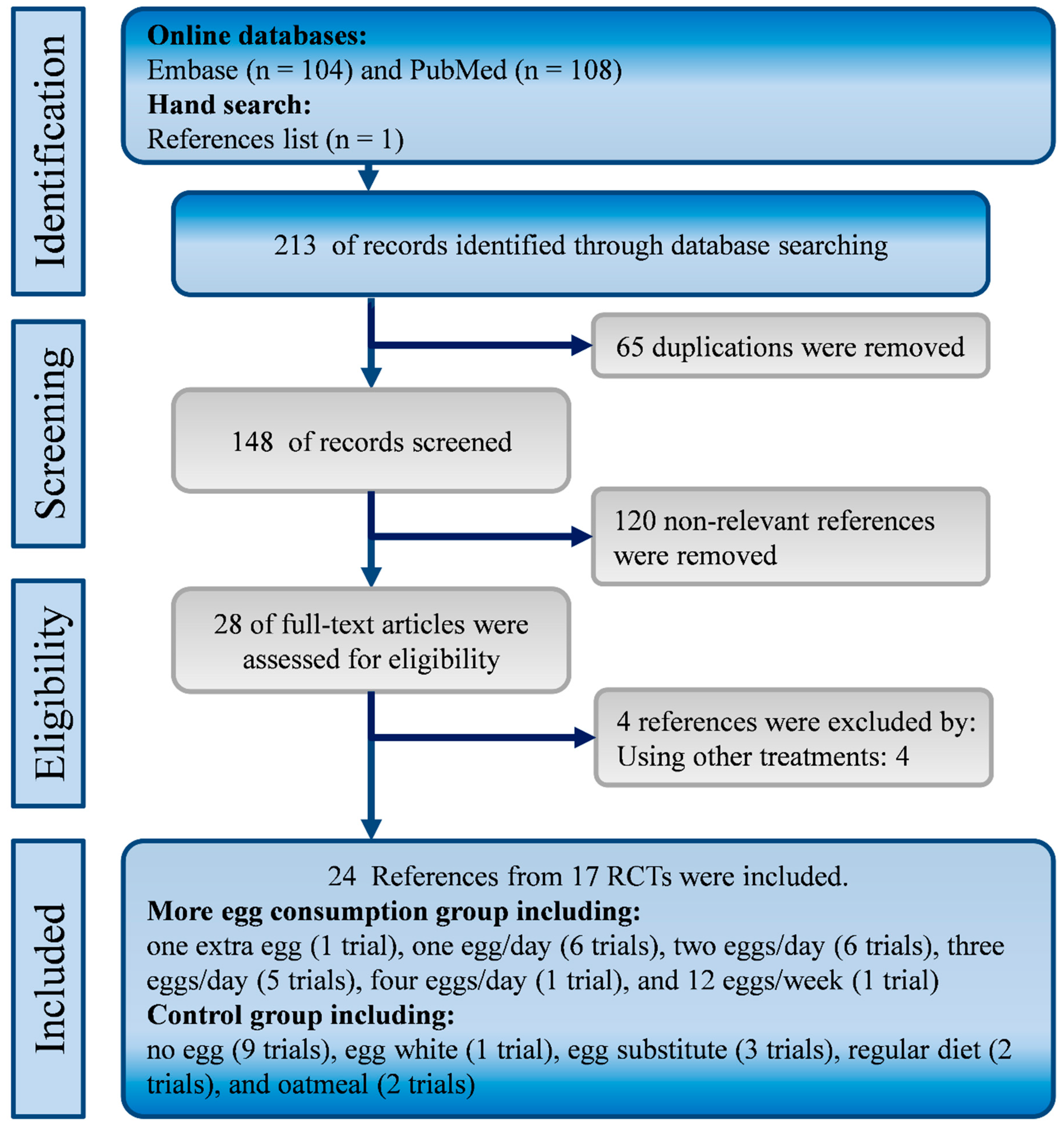
2.1. Eligibility Criteria, Evidence Search and Study Selection
2.2. Data Extraction
2.3. Quality Assessment
2.4. Evidence Synthesis and Statistical Analysis
3. Results
3.1. Characteristics and Quality of Included Studies
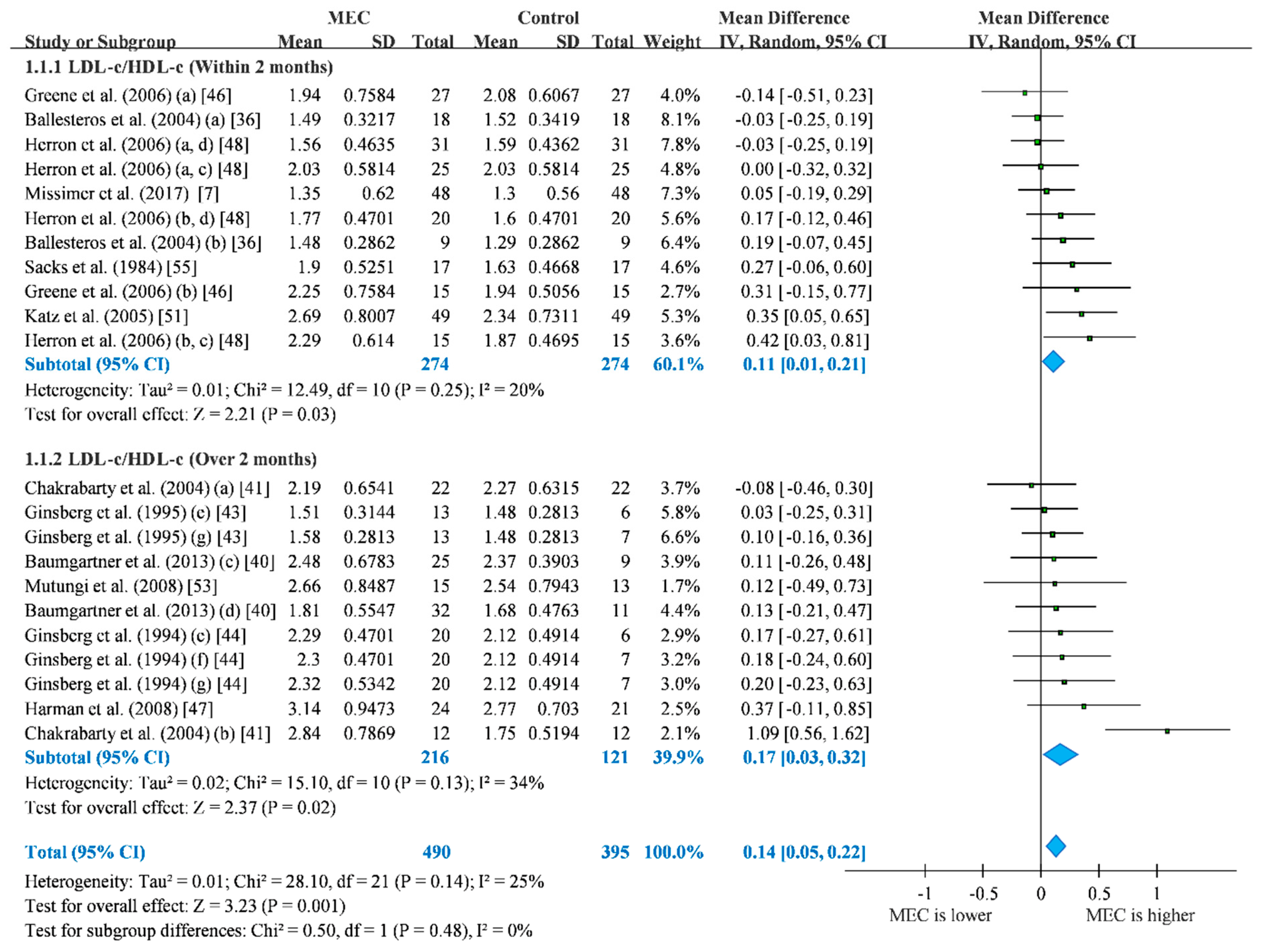
3.2. LDL-c/HDL-c Ratio
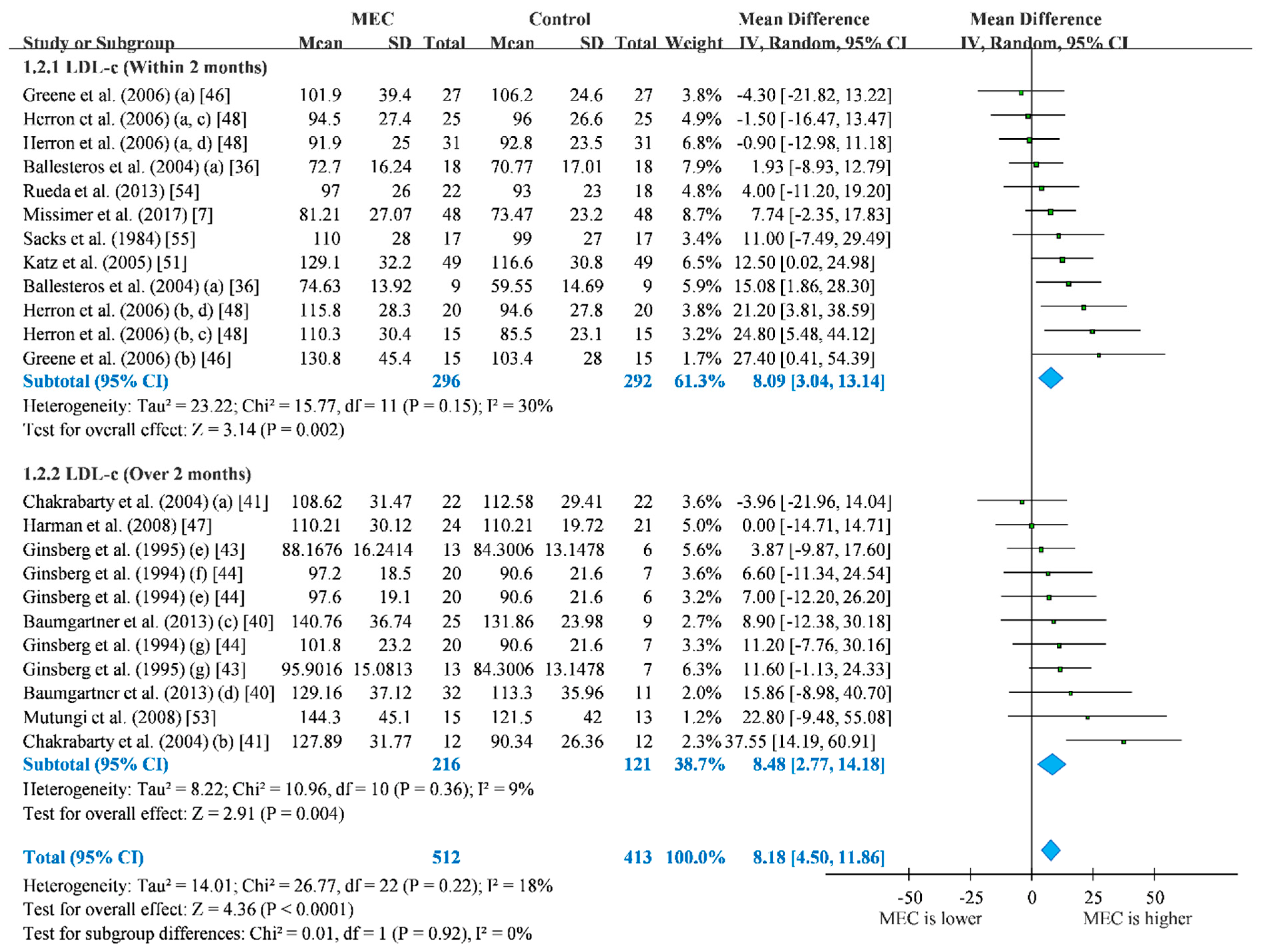
3.3. Low-Density Lipoprotein Cholesterol
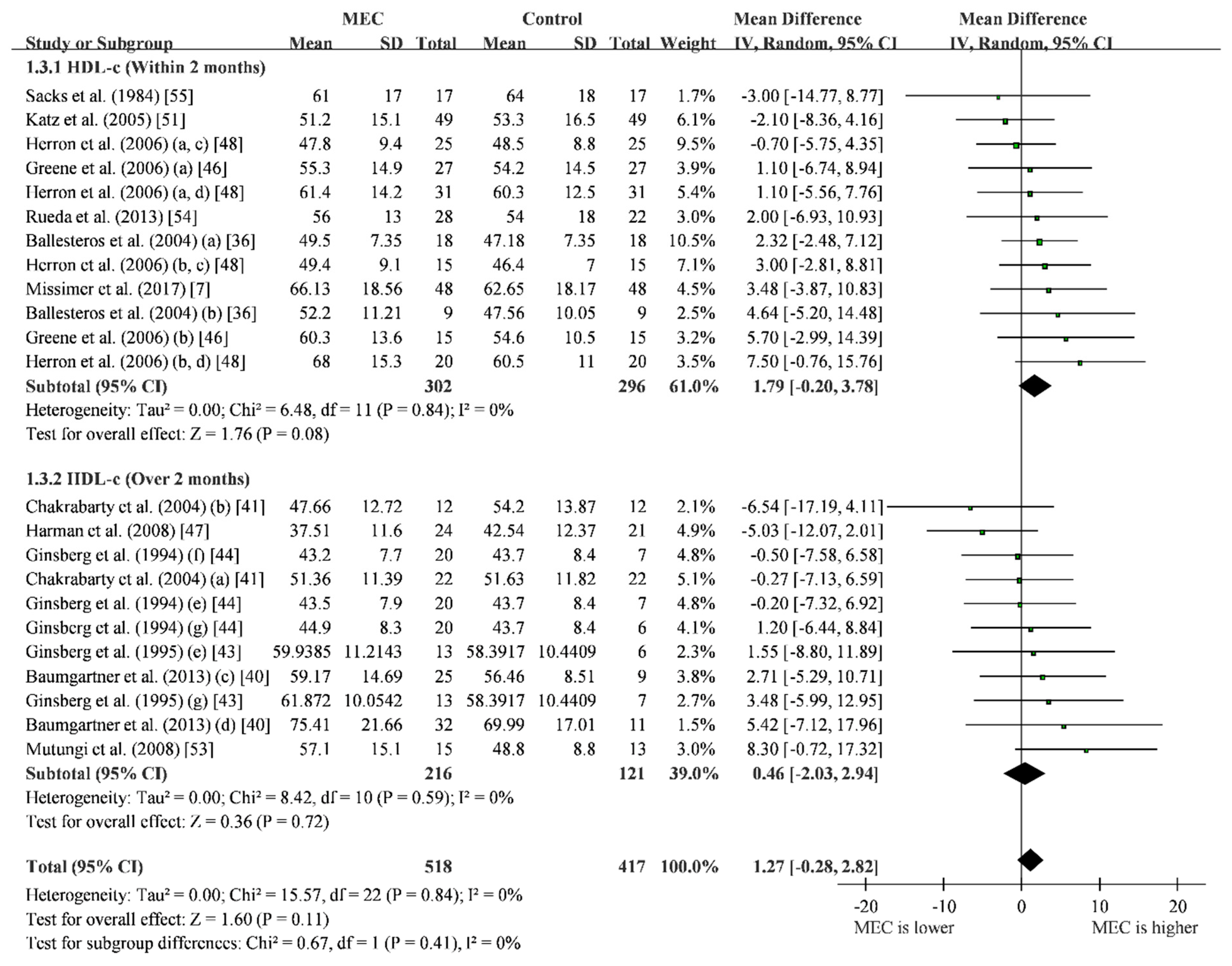
3.4. High-Density Lipoprotein Cholesterol
3.5. Further Analysis
4. Discussion
4.1. Summary of Main Results
4.2. Overall, Completeness and Applicability of the Evidence
4.3. Comparison to Previous Syntheses
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| CI | Confidence interval |
| HDL-c | high-density lipoprotein cholesterol |
| LDL-c | low-density lipoprotein cholesterol |
| MEC | more egg consumption |
| MD | mean difference |
| NSR | nonspecific responders |
| PRISMA | preferred reporting items for systematic reviews and meta-analyses |
| RCT | randomized clinical trial |
| SD | standard deviation |
References
- Krauss, R.M.; Eckel, R.H.; Howard, B.; Appel, L.J.; Daniels, S.R.; Deckelbaum, R.J.; Erdman, J.W., Jr.; Kris-Etherton, P.; Goldberg, I.J.; Kotchen, T.A.; et al. Aha dietary guidelines: Revision 2000: A statement for healthcare professionals from the nutrition committee of the american heart association. Circulation 2000, 102, 2284–2299. [Google Scholar] [CrossRef] [PubMed]
- Spence, J.D.; Jenkins, D.J.; Davignon, J. Dietary cholesterol and egg yolks: Not for patients at risk of vascular disease. Can. J. Cardiol. 2010, 26, e336–e339. [Google Scholar] [CrossRef]
- Clayton, Z.S.; Fusco, E.; Kern, M. Egg consumption and heart health: A review. Nutr. (BurbankLos Angeles Cty. Calif.) 2017, 37, 79–85. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services; U.S. Department of Agriculture Agriculture. 2015–2020 Dietary Guidelines for Americans, 8th ed.; U.S. Department of Health and Human Services; U.S. Department of Agriculture Agriculture: Washington, DC, USA, 2015.
- Kim, J.E.; Campbell, W.W. Dietary cholesterol contained in whole eggs is not well absorbed and does not acutely affect plasma total cholesterol concentration in men and women: Results from 2 randomized controlled crossover studies. Nutrients 2018, 10, 1272. [Google Scholar] [CrossRef]
- Greene, C.M.; Zern, T.L.; Wood, R.J.; Shrestha, S.; Aggarwal, D.; Sharman, M.J.; Volek, J.S.; Fernandez, M.L. Maintenance of the ldl cholesterol:Hdl cholesterol ratio in an elderly population given a dietary cholesterol challenge. J. Nutr. 2005, 135, 2793–2798. [Google Scholar] [CrossRef]
- Missimer, A.; DiMarco, D.M.; Andersen, C.J.; Murillo, A.G.; Vergara-Jimenez, M.; Fernandez, M.L. Consuming two eggs per day, as compared to an oatmeal breakfast, decreases plasma ghrelin while maintaining the ldl/hdl ratio. Nutrients 2017, 9, 89. [Google Scholar] [CrossRef]
- Alexander, D.D.; Miller, P.E.; Vargas, A.J.; Weed, D.L.; Cohen, S.S. Meta-analysis of egg consumption and risk of coronary heart disease and stroke. J. Am. Coll. Nutr. 2016, 35, 704–716. [Google Scholar] [CrossRef]
- Rouhani, M.H.; Rashidi-Pourfard, N.; Salehi-Abargouei, A.; Karimi, M.; Haghighatdoost, F. Effects of egg consumption on blood lipids: A systematic review and meta-analysis of randomized clinical trials. J. Am. Coll. Nutr. 2017, 37, 99–110. [Google Scholar] [CrossRef]
- Wang, M.X.; Wong, C.H.; Kim, J.E. Impact of whole egg intake on blood pressure, lipids and lipoproteins in middle-aged and older population: A systematic review and meta-analysis of randomized controlled trials. Lipid 2019, 29, 653–664. [Google Scholar] [CrossRef]
- Weggemans, R.M.; Zock Pl Fau-Katan, M.B.; Katan, M.B. Dietary cholesterol from eggs increases the ratio of total cholesterol to high-density lipoprotein cholesterol in humans: A meta-analysis. Am. J. Clin. Nutr. 2001, 73, 885–891. [Google Scholar] [CrossRef]
- Millan, J.; Pinto, X.; Fau-Munoz, A.; Munoz, A.; Fau-Zuniga, M.; Zuniga, M.; Fau-Rubies-Prat, J.; Rubies-Prat, J.; Fau-Pallardo, L.F.; Masana, L.; et al. Lipoprotein ratios: Physiological significance and clinical usefulness in cardiovascular prevention. Vasc. Health Risk Manag. 2009, 5, 757. [Google Scholar]
- Kovacs-Nolan, J.; Phillips, M.; Mine, Y. Advances in the value of eggs and egg components for human health. J. Agric. Food Chem. 2005, 53, 8421–8431. [Google Scholar] [CrossRef]
- Kuang, H.; Yang, F.; Zhang, Y.; Wang, T.; Chen, G. The impact of egg nutrient composition and its consumption on cholesterol homeostasis. Cholesterol 2018, 2018, 6303810. [Google Scholar] [CrossRef] [PubMed]
- Cohen, D.E. Balancing cholesterol synthesis and absorption in the gastrointestinal tract. J. Clin. Lipidol. 2008, 2, S1–S3. [Google Scholar] [CrossRef] [PubMed]
- Lu, K.; Lee, M.H.; Patel, S.B. Dietary cholesterol absorption; more than just bile. Trends Endocrinol. Metab. 2001, 12, 314–320. [Google Scholar] [CrossRef]
- Afonso, M.S.; Machado, R.M.; Lavrador, M.S.; Quintao, E.C.R.; Moore, K.J.; Lottenberg, A.M. Molecular pathways underlying cholesterol homeostasis. Nutrients 2018, 10, 760. [Google Scholar] [CrossRef]
- Hussain, M.M.; Maxfield, F.R.; Mas-Oliva, J.; Tabas, I.; Ji, Z.-S.; Innerarity, T.L.; Mahley, R.W. Clearance of chylomicron remnants by the low density lipoprotein receptor-related protein/α2-macroglobulin receptor. J. Biol. Chem. 1991, 266, 13936–13940. [Google Scholar]
- Pirahanchi, Y.; Huecker, M.R. Biochemistry, Ldl Cholesterol; StatPearls [Internet]; 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK519561/ (accessed on 16 January 2019).
- Rosenson, R.S. Patient Education: High Cholesterol and Lipids (Hyperlipidemia) (Beyond the Basics). 2019; Available online: https://www.uptodate.com/contents/high-cholesterol-and-lipids-beyond-the-basics (accessed on 9 September 2019).
- Nelson, R.H. Hyperlipidemia as a risk factor for cardiovascular disease. Prim. Care 2013, 40, 195–211. [Google Scholar] [CrossRef]
- Karr, S. Epidemiology and management of hyperlipidemia. Am. J. Manag. Care 2017, 23, S139–S148. [Google Scholar]
- World Health Organization. Global Health Observatory (gho) Data-raised Cholesterol; Global Status Report on Noncommunicable Diseases 2014; WHO: Genève, Switzerland, 2014. [Google Scholar]
- Blesso, C.N.; Fernandez, M.L. Dietary cholesterol, serum lipids, and heart disease: Are eggs working for or against you? Nutrients 2018, 10, 426. [Google Scholar] [CrossRef]
- DiMarco, D.M.; Missimer, A.; Murillo, A.G.; Lemos, B.S.; Malysheva, O.V.; Caudill, M.A.; Blesso, C.N.; Fernandez, M.L. Intake of up to 3 eggs/day increases hdl cholesterol and plasma choline while plasma trimethylamine-n-oxide is unchanged in a healthy population. Lipids 2017, 52, 255–263. [Google Scholar] [CrossRef] [PubMed]
- Lemos, B.S.; Medina-Vera, I.; Blesso, C.N.; Fernandez, M.L. Intake of 3 eggs per day when compared to a choline bitartrate supplement, downregulates cholesterol synthesis without changing the ldl/hdl ratio. Nutrients 2018, 10, 258. [Google Scholar] [CrossRef] [PubMed]
- Hutton, B.; Salanti, G.; Caldwell, D.M.; Chaimani, A.; Schmid, C.H.; Cameron, C.; Ioannidis, J.P.; Straus, S.; Thorlund, K.; Jansen, J.P.; et al. The prisma extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: Checklist and explanations. Ann. Intern. Med. 2015, 162, 777–784. [Google Scholar] [CrossRef] [PubMed]
- Papadakis, J.A.; Ganotakis, E.S.; Jagroop, I.A.; Mikhailidis, D.P.; Winder, A.F. Effect of hypertension and its treatment on lipid, lipoprotein(a), fibrinogen, and bilirubin levels in patients referred for dyslipidemia. Am. J. Hypertens. 1999, 12, 673–681. [Google Scholar] [CrossRef]
- Severins, N.; Mensink, R.P.; Plat, J. Effects of lutein-enriched egg yolk in buttermilk or skimmed milk on serum lipids & lipoproteins of mildly hypercholesterolemic subjects. Nutr. Metab. Cardiovasc. Dis. NMCD 2015, 25, 210–217. [Google Scholar]
- Bautista, L.E.; Herran, O.F.; Serrano, C. Effects of palm oil and dietary cholesterol on plasma lipoproteins: Results from a dietary crossover trial in free-living subjects. Eur. J. Clin. Nutr. 2001, 55, 748–754. [Google Scholar] [CrossRef]
- Rugge, B.; Balshem, H.; Sehgal, R.; Relevo, R.; Gorman, P.; Helfand, M. Screening and treatment of subclinical hypothyroidism or hyperthyroidism. In Ahrq Comparative Effectiveness Reviews; Agency for Healthcare Research and Quality (US): Rockville, MD, USA, 2011. [Google Scholar]
- Stuart, A.; Ord, J.K. Kendall’s Advanced Theory of Statistics; Charles Griffin and Co., Ltd.: London, UK, 1998; Volume 1. [Google Scholar]
- Wiley, J.; NY, S. Survival Models and Data Analysis; John Wiley & Sons: Hoboken, NJ, USA, 1980. [Google Scholar]
- Effective Public Health Practice Project (EPHPP). Quality Assessment Tool for Quantitative Studies. Hamilton, on: Effective Public Health Practice Project. Available online: https://merst.ca/ephpp/ (accessed on 9 June 2020).
- Graves, R.S. Users’ guides to the medical literature: A manual for evidence-based clinical practice. J. Med. Libr. Assoc. 2002, 90, 483. [Google Scholar]
- Ballesteros, M.N.; Cabrera, R.M.; Saucedo Mdel, S.; Fernandez, M.L. Dietary cholesterol does not increase biomarkers for chronic disease in a pediatric population from northern mexico. Am. J. Clin. Nutr. 2004, 80, 855–861. [Google Scholar] [CrossRef]
- Chakrabarty, G.; Bijlani, R.L.; Mahapatra, S.C.; Mehta, N.; Lakshmy, R.; Vashisht, S.; Manchanda, S.C. The effect of ingestion of egg on serum lipid profile in healthy young free-living subjects. Indian J. Physiol. Pharmacol. 2002, 46, 492–498. [Google Scholar]
- Clark, R.M.; Herron, K.L.; Waters, D.; Fernandez, M.L. Hypo- and hyperresponse to egg cholesterol predicts plasma lutein and beta-carotene concentrations in men and women. J. Nutr. 2006, 136, 601–607. [Google Scholar] [CrossRef]
- Herron, K.L.; Lofgren, I.E.; Sharman, M.; Volek, J.S.; Fernandez, M.L. High intake of cholesterol results in less atherogenic low-density lipoprotein particles in men and women independent of response classification. Metab. Clin. Exp. 2004, 53, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Baumgartner, S.; Kelly, E.R.; van der Made, S.; Berendschot, T.T.; Husche, C.; Lutjohann, D.; Plat, J. The influence of consuming an egg or an egg-yolk buttermilk drink for 12 wk on serum lipids, inflammation, and liver function markers in human volunteers. Nutr. (BurbankLos Angeles Cty. Calif.) 2013, 29, 1237–1244. [Google Scholar] [CrossRef] [PubMed]
- Chakrabarty, G.; Manjunatha, S.; Bijlani, R.L.; Ray, R.B.; Mahapatra, S.C.; Mehta, N.; Lakshmy, R.; Vashisht, S.; Manchanda, S.C. The effect of ingestion of egg on the serum lipid profile of healthy young indians. Indian J. Physiol. Pharmacol. 2004, 48, 286–292. [Google Scholar] [PubMed]
- Garwin, J.L.; Morgan, J.M.; Stowell, R.L.; Richardson, M.P.; Walker, M.C.; Capuzzi, D.M. Modified eggs are compatible with a diet that reduces serum cholesterol concentrations in humans. J. Nutr. 1992, 122, 2153–2160. [Google Scholar] [CrossRef]
- Ginsberg, H.N.; Karmally, W.; Siddiqui, M.; Holleran, S.; Tall, A.R.; Blaner, W.S.; Ramakrishnan, R. Increases in dietary cholesterol are associated with modest increases in both ldl and hdl cholesterol in healthy young women. Arterioscler. Thromb. Vasc. Biol. 1995, 15, 169–178. [Google Scholar] [CrossRef] [PubMed]
- Ginsberg, H.N.; Karmally, W.; Siddiqui, M.; Holleran, S.; Tall, A.R.; Rumsey, S.C.; Deckelbaum, R.J.; Blaner, W.S.; Ramakrishnan, R. A dose-response study of the effects of dietary cholesterol on fasting and postprandial lipid and lipoprotein metabolism in healthy young men. Arterioscler. Thromb. A J. Vasc. Biol. 1994, 14, 576–586. [Google Scholar] [CrossRef]
- Goodrow, E.F.; Wilson, T.A.; Houde, S.C.; Vishwanathan, R.; Scollin, P.A.; Handelman, G.; Nicolosi, R.J. Consumption of one egg per day increases serum lutein and zeaxanthin concentrations in older adults without altering serum lipid and lipoprotein cholesterol concentrations. J. Nutr. 2006, 136, 2519–2524. [Google Scholar] [CrossRef]
- Greene, C.M.; Waters, D.; Clark, R.M.; Contois, J.H.; Fernandez, M.L. Plasma ldl and hdl characteristics and carotenoid content are positively influenced by egg consumption in an elderly population. Nutr. Metab. 2006, 3, 6. [Google Scholar] [CrossRef]
- Harman, N.L.; Leeds, A.R.; Griffin, B.A. Increased dietary cholesterol does not increase plasma low density lipoprotein when accompanied by an energy-restricted diet and weight loss. Eur. J. Nutr. 2008, 47, 287–293. [Google Scholar] [CrossRef]
- Herron, K.L.; Lofgren, I.E.; Adiconis, X.; Ordovas, J.M.; Fernandez, M.L. Associations between plasma lipid parameters and apoc3 and apoa4 genotypes in a healthy population are independent of dietary cholesterol intake. Atherosclerosis 2006, 184, 113–120. [Google Scholar] [CrossRef]
- Herron, K.L.; Vega-Lopez, S.; Conde, K.; Ramjiganesh, T.; Roy, S.; Shachter, N.S.; Fernandez, M.L. Pre-menopausal women, classified as hypo- or hyperresponders, do not alter their ldl/hdl ratio following a high dietary cholesterol challenge. J. Am. Coll. Nutr. 2002, 21, 250–258. [Google Scholar] [CrossRef] [PubMed]
- Herron, K.L.; Vega-Lopez, S.; Conde, K.; Ramjiganesh, T.; Shachter, N.S.; Fernandez, M.L. Men classified as hypo- or hyperresponders to dietary cholesterol feeding exhibit differences in lipoprotein metabolism. J. Nutr. 2003, 133, 1036–1042. [Google Scholar] [CrossRef]
- Katz, D.L.; Evans, M.A.; Nawaz, H.; Njike, V.Y.; Chan, W.; Comerford, B.P.; Hoxley, M.L. Egg consumption and endothelial function: A randomized controlled crossover trial. Int. J. Cardiol. 2005, 99, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Missimer, A.; Fernandez, M.L.; DiMarco, D.M.; Norris, G.H.; Blesso, C.N.; Murillo, A.G.; Vergara-Jimenez, M.; Lemos, B.S.; Medina-Vera, I.; Malysheva, O.V.; et al. Compared to an oatmeal breakfast, two eggs/day increased plasma carotenoids and choline without increasing trimethyl amine n-oxide concentrations. J. Am. Coll. Nutr. 2018, 37, 140–148. [Google Scholar] [CrossRef]
- Mutungi, G.; Ratliff, J.; Puglisi, M.; Torres-Gonzalez, M.; Vaishnav, U.; Leite, J.O.; Quann, E.; Volek, J.S.; Fernandez, M.L. Dietary cholesterol from eggs increases plasma hdl cholesterol in overweight men consuming a carbohydrate-restricted diet. J. Nutr. 2008, 138, 272–276. [Google Scholar] [CrossRef]
- Rueda, J.M.; Khosla, P. Impact of breakfasts (with or without eggs) on body weight regulation and blood lipids in university students over a 14-week semester. Nutrients 2013, 5, 5097–5113. [Google Scholar] [CrossRef]
- Sacks, F.M.; Salazar, J.; Miller, L.; Foster, J.M.; Sutherland, M.; Samonds, K.W.; Albers, J.J.; Kass, E.H. Ingestion of egg raises plasma low density lipoproteins in free-living subjects. Lancet (Lond. Engl.) 1984, 1, 647–649. [Google Scholar] [CrossRef]
- Vander Wal, J.S.; Gupta, A.; Khosla, P.; Dhurandhar, N.V. Egg breakfast enhances weight loss. Int. J. Obes. 2008, 32, 1545–1551. [Google Scholar]
- Waters, D.; Clark, R.M.; Greene, C.M.; Contois, J.H.; Fernandez, M.L. Change in plasma lutein after egg consumption is positively associated with plasma cholesterol and lipoprotein size but negatively correlated with body size in postmenopausal women. J. Nutr. 2007, 137, 959–963. [Google Scholar] [CrossRef] [PubMed]
- Kunutsor, S.K.; Zaccardi, F.; Karppi, J.; Kurl, S.; Laukkanen, J.A. Is high serum ldl/hdl cholesterol ratio an emerging risk factor for sudden cardiac death? Findings from the kihd study. J. Atheroscler. Thromb. 2017, 24, 600–608. [Google Scholar] [CrossRef]
- Olvera Lopez, E.; Ballard, B.D.; Jan, A. Cardiovascular Disease; StatPearls [Internet]; 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK535419/ (accessed on 29 May 2020).
- Vergeer, M.; Holleboom, A.G.; Kastelein, J.J.; Kuivenhoven, J.A. The hdl hypothesis: Does high-density lipoprotein protect from atherosclerosis? J. Lipid Res. 2010, 51, 2058–2073. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.; Siddiqui, W.J. Cholesterol Levels; StatPearls [Internet]; 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK542294/ (accessed on 3 June 2019).
- Asato, L.; Wang, M.F.; Chan, Y.C.; Yeh, S.H.; Chung, H.M.; Chung, S.Y.; Chida, S.; Uezato, T.; Suzuki, I.; Yamagata, N.; et al. Effect of egg white on serum cholesterol concentration in young women. J. Nutr. Sci. Vitaminol. 1996, 42, 87–96. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.C.; Chen, K.H. The oxidation of cholesterol in the yolk of selective traditional chinese egg products. Poult. Sci. 2001, 80, 370–375. [Google Scholar] [CrossRef] [PubMed]
- Schwab, U.S.; Ausman, L.M.; Vogel, S.; Li, Z.; Lammi-Keefe, C.J.; Goldin, B.R.; Ordovas, J.M.; Schaefer, E.J.; Lichtenstein, A.H. Dietary cholesterol increases the susceptibility of low density lipoprotein to oxidative modification. Atherosclerosis 2000, 149, 83–90. [Google Scholar] [CrossRef]
| Trial | Male/Female | Age Range | Intervention | Duration | Result (↑: increased concentration; ↓: decreased concentration) | |
|---|---|---|---|---|---|---|
| Egg Group | Control | |||||
| Missimer et al. (2017) [7] | 24/26 | 18–30 | 2 eggs/day | Oatmeal | 28 days | LDL-c↑; HDL-c↑ |
| Baumgartner et al. (2013) [40] | 34/63 | 18–65 | One extra egg | Regular diet | 84 days | TC↑; LDL-c↑ |
| Rueda et al. (2013) [54] | 27/46 | 17–20 | 1 egg/day | No egg | 28 days | Statistically insignificant change |
| Harman et al. (2008) [47] | 14/31 | 18–55 | 2 eggs/day | No egg | 84 days | Statistically insignificant change |
| Mutungi et al. (2008) [53] | 28/0 | 40–70 | 3 eggs/day | No egg | 84 days | HDL-c↑ |
| Wal et al. (2008) [56] | 10/63 | 25–60 | 2 eggs/day | Regular diet | 56 days | Statistically insignificant change |
| Waters et al. (2007) [57] | 0/22 | 50–77 | 3 eggs/day | No egg | 30 days | TC↑; HDL-c↑; LDL-c↑ |
| Herron et al. (2006) [48] | 40/51 | 21–43 | 3 eggs/day | Egg substitute | 30 days | TC↑; HDL-c↑; LDL-c↑ |
| Greene et al. (2006) [46] | 13/29 | 50–80 | 3 eggs/day | Egg substitute | 30 days | HDL-c↑; LDL-c↑ |
| Goodrow et al. (2006 [45]) | 7/26 | 60–96 | 1 egg/day | Egg substitute | 35 days | Statistically insignificant change |
| Katz et al. (2005) [51] | 30/19 | 36–73 | 2 eggs/day | Oatmeal | 42 days | Statistically insignificant change |
| Ballesteros et al. (2004) [36] | 25/29 | 8–12 | 2 eggs/day | Egg white | 30 days | LDL-c↑; HDL-c↑ |
| Chakrabarty et al. (2004) [41] | 22/12 | 19–32 | 1 egg/day | No egg | 56 days | TC↑; LDL-c↑; TC/HDL-c↑ |
| Ginsberg et al. (1995) [43] | 0/13 | 22–31 | 3 eggs/day1 egg/day | No egg | 56 days | TC↑; HDL-c↑; LDL-c↑ |
| Ginsberg et al. (1994) [44] | 24/0 | 22–31 | 1 egg/day2 eggs/day4 eggs/day | No egg | 56 days | TC↑; LDL-c↑ |
| Garwin et al. (1992) [42] | 42/56 | 41–48 | 12 eggs/week | No egg | 42 days | TC↓; HDL-c↓; LDL-c↓ |
| Sacks et al. (1984) [55] | 4/13 | 18–24 | 1 egg/day | No egg | 21 days | LDL-c↑ |
| Outcome/ | |||||
|---|---|---|---|---|---|
| Subgroup | Studies | Patients | MD | 95% CI | I-Square |
| LDL-c/HDL-c ratio | |||||
| 1 egg | 5 | 226 | 0.20 | −0.01–0.42 | 59% |
| 2 eggs | 5 | 320 | 0.13 | 0.01–0.26 | 13% |
| ≥ 3 eggs | 5 | 339 | 0.09 | −0.02–0.20 | 0% |
| LDL-c | |||||
| 1 egg | 6 | 266 | 8.37 | 1.06–15.69 | 22% |
| 2 eggs | 5 | 320 | 7.32 | 2.20–12.44 | 0% |
| ≥ 3 eggs | 5 | 339 | 9.87 | 2.09–17.65 | 42% |
| HDL-c | |||||
| 1 egg | 6 | 276 | 0.28 | −2.85–3.42 | 0% |
| 2 eggs | 5 | 320 | 0.35 | −2.35–3.04 | 0% |
| ≥ 3 eggs | 5 | 339 | 2.55 | 0.16–4.94 | 0% |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, M.-Y.; Chen, J.-H.; Chen, C.; Kang, Y.-N. Association between Egg Consumption and Cholesterol Concentration: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Nutrients 2020, 12, 1995. https://doi.org/10.3390/nu12071995
Li M-Y, Chen J-H, Chen C, Kang Y-N. Association between Egg Consumption and Cholesterol Concentration: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Nutrients. 2020; 12(7):1995. https://doi.org/10.3390/nu12071995
Chicago/Turabian StyleLi, Man-Yun, Jin-Hua Chen, Chiehfeng Chen, and Yi-No Kang. 2020. "Association between Egg Consumption and Cholesterol Concentration: A Systematic Review and Meta-Analysis of Randomized Controlled Trials" Nutrients 12, no. 7: 1995. https://doi.org/10.3390/nu12071995
APA StyleLi, M.-Y., Chen, J.-H., Chen, C., & Kang, Y.-N. (2020). Association between Egg Consumption and Cholesterol Concentration: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Nutrients, 12(7), 1995. https://doi.org/10.3390/nu12071995





