1. Introduction
The research interest in vitamin D has increased significantly due to the high prevalence of vitamin D insufficiency worldwide [
1] and the multiple functions of vitamin D besides mineral metabolism, e.g., in the immune system [
2,
3]. Thus, numerous epidemiological studies have been conducted linking vitamin D to health outcomes. The concentration of 25-hydroxyvitamin D (25(OH)D), which is analyzed in serum, plasma or dried blood spots by different measures, has widely been accepted as a good biomarker of vitamin D status in adults and infants [
4,
5]. The suitability of 25(OH)D as a vitamin D status biomarker is based on the finding that 25(OH)D has a long-term half-life of at least 2 weeks in plasma, thereby reflecting vitamin D stores in the body [
6,
7]. Additionally, it is assumed that the synthesis of 25(OH)D in the liver is not strictly regulated and depends on the available quantity of vitamin D [
5]. In contrast to 25(OH)D, bioactive 1α,25-dihydroxyvitamin D (1,25(OH)
2D) has been considered an inappropriate biomarker of vitamin D status because its synthesis and activity are tightly regulated by the parathyroid hormone and fibroblast growth factor 23 [
8]. Both hormones ensure constant levels of plasma 1,25(OH)
2D for a wide range of vitamin D concentrations in the body. 24,25-Dihydroxyvitamin D (24,25(OH)
2D), which is formed from 25(OH)D and 1,25(OH)
2D by the multicatalytic enzyme 25-hydroxyvitamin D-24-hydroxylase (CYP24A1) [
9] and destined for excretion, is usually not used as a biomarker of vitamin D status. The measurement of 24,25(OH)
2D, for example, has been recommended for the diagnosis of patients with mutations in CYP24A1 [
10].
However, a few scientists recommend assessing the ratio of 25(OH)D to 24,25(OH)
2D to evaluate vitamin D status [
11,
12]. Currently, few data are available regarding the suitability of nonhydroxylated vitamin D as a status marker. In the
First International Conference on Controversies in Vitamin D, the measurement of potential vitamin D biomarkers other than 25(OH)D was discussed [
13]. Recently, the reliability of 25(OH)D as a biomarker of vitamin D status has been critically discussed. In 2018, Jorde and Grimnes hypothesized that nonhydroxylated vitamin D in serum could be a more useful parameter for assessing vitamin D status [
14]. The authors argued that vitamin D-dependent cells possibly prefer circulating vitamin D, not 25(OH)D or 1,25(OH)
2D, to synthesize bioactive vitamin D metabolites for their own needs.
Additionally, data from human intervention studies indicate that the activity of the 25-hydroxylases that catalyze the synthesis of 25(OH)D from vitamin D is regulated because the increase in circulating 25(OH)D following vitamin D treatment is higher in individuals with low baseline levels of 25(OH)D than in those with high 25(OH)D levels [
15,
16]. Other data, which indicate that circulating levels of 25(OH)D do not necessarily reflect vitamin D stores in the body, come from mouse studies. Mice that were fed diets containing 7-dehydrocholesterol or ergosterol showed significantly increased vitamin D stores in the liver and kidney, while having unchanged serum concentrations of 25(OH)D [
17,
18]. Additionally, mice that received ezetimibe, an inhibitor of the sterol transporter Niemann-Pick C1-like 1 protein, had markedly reduced vitamin D stores in the liver, kidney, adipose tissues and muscle, while the circulating concentrations of 25(OH)D had increased [
19].
Due to many open issues concerning the best and most sensitive biomarker reflecting tissue vitamin D stores and changes in vitamin D consumption, we conducted two mouse studies. The first study addressed response relationships between vitamin D3 intake, tissue levels of vitamin D3 and circulating concentrations of different vitamin D3 metabolites. The second study aimed to ascertain the response of plasma and tissue concentrations of vitamin D metabolites to changes in the oral vitamin D3 supply in mice with a low, adequate or high vitamin D status. Additionally, we studied the rate of mobilization of vitamin D3 from the liver and different types of adipose tissues in response to an absent vitamin D intake.
2. Materials and Methods
2.1. Mouse Studies
In total, two studies using male wild-type mice (C57BL/6N; Charles River, Sulzfeld, Germany) were conducted. The experimental procedures were approved by the local ethics committee (Martin Luther University Halle-Wittenberg, Germany; approval numbers: H1-4/T1-18, H1-4/T1-19; date of approval: 17 July 2018, 1 March 2019, respectively). All experimental procedures followed the guidelines for the care and handling of laboratory animals according to the US National Research Council [
20]. Mice were housed in a room controlled for temperature (22 ± 2 °C), light (12-h light, 12-h dark cycle, lamps emitting no ultraviolet irradiation) and relative humidity (50–60%) and had free access to food and water. The basal diets used in these studies consisted of (per kg): 288 g starch, 200 g sucrose, 200 g casein, 175 g coconut fat, 60 g of a vitamin and mineral mixture, 50 g cellulose, 25 g soybean oil and 2 g of DL-methionine. Except for vitamin D
3, vitamins and minerals were added to the diet according to the recommendation of the National Research Council [
21].
The first experiment was conducted as a dose-response study to elucidate concentrations of vitamin D metabolites in plasma, the liver and adipose tissues (mesenteric, retroperitoneal and subcutaneous) in response to increasing doses of dietary vitamin D3 and to assess the most suitable plasma marker indicating tissue stores of vitamin D3. Therefore, 30 five-week-old mice with an initial body weight of 19.6 ± 0.6 g were randomly assigned to 10 groups (n = 3), receiving 5 µg, 10 µg, 15 µg, 20 µg, 25 µg, 30 µg, 35 µg, 40 µg, 45 µg or 50 µg of vitamin D3 per kg of diet for three weeks. The dietary vitamin D concentrations chosen for the study included levels below and above the presumed need for vitamin D.
The second study aimed to assess the extent and rate of changes in the plasma and tissue vitamin D metabolites in response to switching the vitamin D3 supply from low to adequate and from high to adequate. Therefore, 72 five-week-old mice (initial body weight: 18.4 ± 2.0 g) were randomly assigned to 3 groups (n = 24) and fed diets with either low (5 µg/kg), adequate (25 µg/kg) or high (50 µg/kg) concentrations of vitamin D3 for four weeks to induce different statuses of vitamin D3. Then, all mice received a diet containing 25 µg/kg of vitamin D3. Thus, the study included three intervention groups: a low vitamin D3 status group that received a vitamin D3-adequate diet (5→25 D3), a high vitamin D3 status group that received a vitamin D3-adequate diet (50→25 D3) and a control group that was fed the vitamin D3-adequate diet (25→25 D3) over the whole experimental period. Six mice from each group were analyzed for plasma and liver concentrations of vitamin D metabolites at the baseline (after the 4-week treatment with 5, 25 and 50 µg/kg vitamin D3, respectively) and 7, 14 and 21 days after switching the dietary vitamin D3 concentrations.
Additionally, to elucidate the response of circulating vitamin D metabolites and vitamin D stores in liver and adipose tissues to an absent vitamin D supply, 24 five-week-old mice (initial body weight: 17.4 ± 1.8 g), which received a vitamin D3-adequate diet (25 µg/kg) for 3 weeks, were placed on a vitamin D-free diet (0 µg/kg). Over a two-day interval, three mice each were analyzed for vitamin D metabolites in the plasma, liver, and mesenteric, retroperitoneal and subcutaneous adipose tissues over a period of 14 days.
2.2. Blood and Tissue Sampling
Prior to sampling, each mouse was food deprived for 4 h, anesthetized with diethyl ether, decapitated and exsanguinated. Blood was used for the analyses of vitamin D metabolites in whole blood, the erythrocytes and the plasma. The liver and mesenteric, retroperitoneal and subcutaneous adipose tissues were harvested, immediately snap-frozen in liquid nitrogen and subsequently stored at −80 °C until the analysis of the vitamin D metabolites.
To quantify vitamin D metabolites in the erythrocytes, blood was collected in heparinized tubes (Sarstedt, Nümbrecht, Germany) and centrifuged at 2000 × g for 10 min at 20 °C. The obtained plasma was removed and stored for further analyses. The erythrocyte fraction was washed three times with ice-cold isotonic sodium chloride solution and then centrifuged (2000× g, 10 min, 20 °C). To ensure that the erythrocytes contained no adherent vitamin D, the supernatant obtained after each washing step was analyzed for vitamin D metabolites. After the second washing cycle, all vitamin D metabolites in the supernatant were below the limit of quantitation (LOQ, vitamin D3: 0.1 nmol/L, 25(OH)D3: 0.8 nmol/L, 24,25(OH)2D3: 5.1 nmol/L).
2.3. Analysis of Vitamin D Metabolites
Vitamin D
3, 25(OH)D
3 and 24,25(OH)
2D
3 were quantified by liquid chromatography-tandem mass spectrometry (LC-MS/MS). Blood and tissue samples were prepared as previously described [
18,
19]. A mixture of 7-fold deuterated vitamin D
3 (Toronto Research Chemicals Inc., Toronto, ON, Canada) and 6-fold deuterated 25(OH)D
3 (Chemaphor Chemical Services, Ottawa, ON, Canada) was used as an internal standard. All samples were subjected to HPLC (1260 Infinity Series, Agilent Technologies, Waldbronn, Germany) coupled to a tandem mass spectrometer (QTRAP 5500, SCIEX, Darmstadt, Germany). The HPLC conditions have been described elsewhere [
19]. For quantification of vitamin D
3 and 25(OH)D
3, a Hypersil ODS C18 column (120 A, 5 μm, 150 × 2.0 mm
2, VDS Optilab, Berlin, Germany) was used, and for quantification of 24,25(OH)
2D
3, a Poroshell C18 column (120 A, 2.7 μm, 50 × 4.6 mm
2, Agilent Technologies) was used.
Ionization was achieved by positive electrospray, and data were recorded in multiple reaction monitoring mode with the following transitions: vitamin D3 560 > 298, 7-fold deuterated vitamin D3 567 > 298, 25(OH)D3 576 > 298, 24,25(OH)2D3 592 > 298, and 6-fold deuterated 25(OH)D3 582 > 298. Metabolites were present as adducts of 4-phenyl-1,2,4-triazoline-3,5-dione (Sigma-Aldrich, Steinheim, Germany).
The intraday precisions of the analytical method for vitamin D3, 25(OH)D3 and 24,25(OH)2D3 were 5.15%, 2.07% and 12.9%, respectively, determined in pooled plasma samples.
The circulating concentration of 1,25(OH)
2D was analyzed by a commercial enzyme-linked immunoassay (Immunodiagnostic Systems, Frankfurt am Main, Germany) following the procedure given by the manufacturer with modifications [
17].
2.4. Statistical Analysis
Statistical analysis was performed using the SAS 9.4 software package (SAS Institute Inc., Cary, NC, USA). Least-squares means (LSM) were estimated using the MIXED procedure, and the differences in LSM were tested for significance. LSM were considered to be significantly different at
p < 0.05. Regression models (M1, M1a) were fitted using PROC REG and PROC NLIN. Depending on the experimental design and data structure, one of the following models was used for the measured traits:
Regression models (M1, M1a) were used to model the traits of the dose-response study (
Section 2.1) depending on vitamin D
3 doses ranging from 5 to 50 µg/kg of diet with 5 µg/kg increments and 3 mice per dose. The M1 model used a linear regression, and M1a used a curvilinear-plateau model [
22]. Model M2 was used to analyze the diet and time effects, including the 2-way interactions for the second study described in
Section 2.1. Model M3 was used to analyze the time effect for the last study described in
Section 2.1.
The factors diet and time as well as their interaction were considered fixed effects in the models. The F-test was used to assess differences in fixed effects levels (p < 0.05). Finally, the Tukey adjusted t-test (for main effects with more than 2 levels) or a t-test (main effects with 2 levels and interactions) was used to assess pairwise differences (p < 0.05). To assess correlations between vitamin D metabolites in plasma and stores of vitamin D in tissues, Pearson correlation coefficients were calculated using the CORR procedure.
4. Discussion
It is a consensus that circulating 25(OH)D is the most representative measure for vitamin D status [
23,
24,
25]. 25(OH)D is primarily used for the diagnosis of vitamin D deficiency and to evaluate associations between vitamin D status and disease morbidity and mortality in epidemiological studies. The question, however, arose whether circulating 25(OH)D may also reflect the quantity of stored vitamin D. This is important with respect to the fact that stored vitamin D, particularly in the liver and adipose tissue, has been suggested to serve as an important source of vitamin D that can be mobilized in times of absent endogenous vitamin D synthesis or low vitamin D intake to counteract vitamin D insufficiency [
26,
27]. The contribution of stored vitamin D to improving vitamin D status became evident in a prospective, double-blind cohort study that was published in 2017 [
28]. In this human study, large subcutaneous adipose tissue stores of vitamin D were associated with a reduced decline in serum 25(OH)D concentrations in the following year. This finding suggests the importance of stored vitamin D in reducing the risk of vitamin D insufficiency. Having a good serum biomarker that reliably indicates vitamin D stores would, therefore, be important for public health and clinical practice. As it is difficult to assess the liver and adipose tissue stores of vitamin D in humans, we conducted two studies in mice.
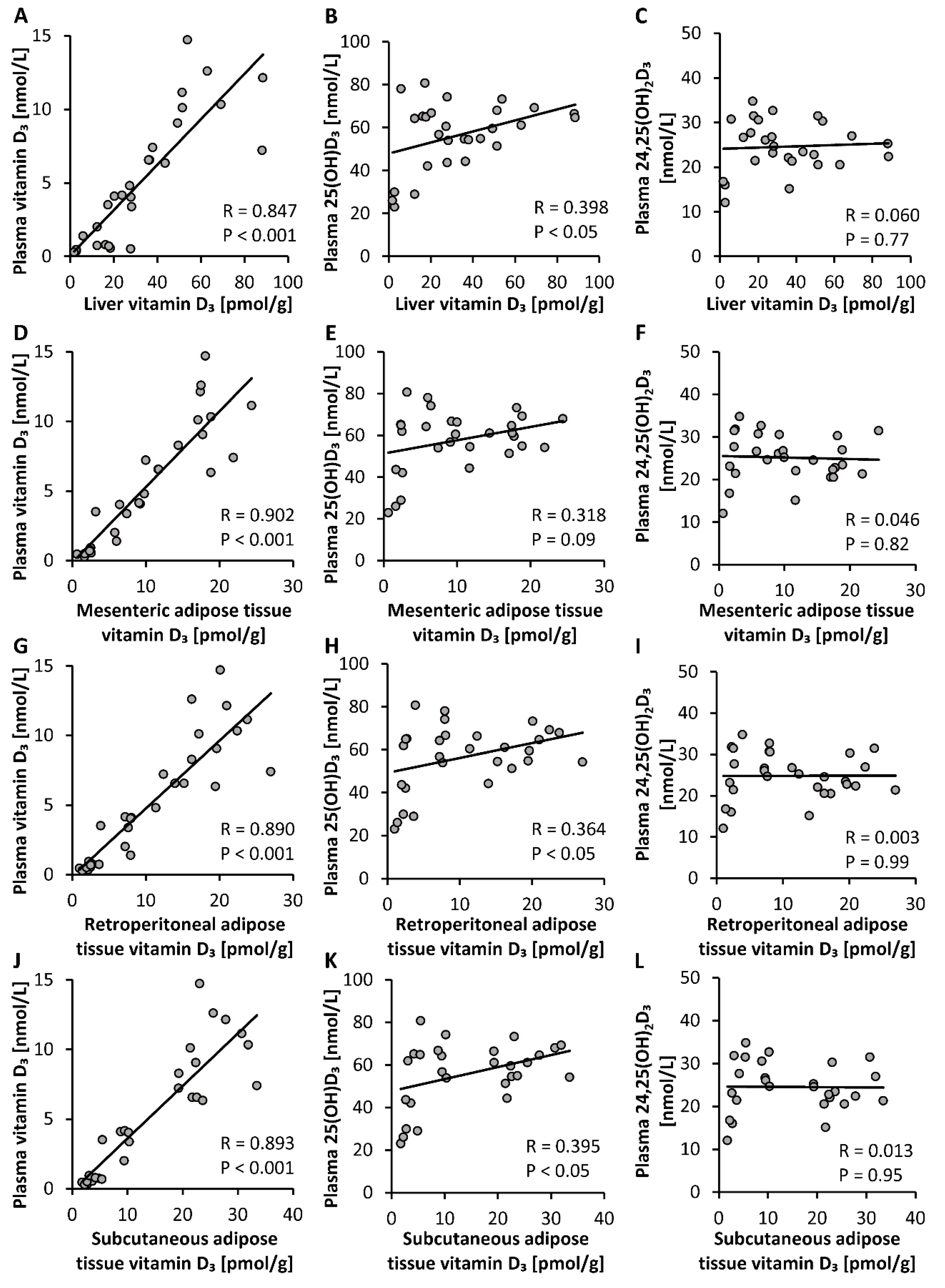
The important findings of the first study were that the plasma, liver and adipose tissue concentrations of vitamin D3 increased linearly with increasing doses of orally administered vitamin D3, and that the circulating vitamin D3 strongly correlated with the vitamin D3 stores in the liver and all adipose tissues analyzed (R between 0.85 and 0.90). However, current data also show that blood cells, in particular erythrocytes, may not serve as important vitamin D stores. In contrast to vitamin D3, circulating 25(OH)D3 showed only a weak correlation (R between 0.36 and 0.40), and 24,25(OH)2D3 showed no correlation with vitamin D3 in the liver and adipose tissues. Therefore, it seems that neither vitamin D metabolite is an ideal parameter reflecting tissue stores of vitamin D in the body.
The weak correlation between circulating 25(OH)D
3 and the tissue stores of vitamin D
3 is attributable to the fact that the response of 25(OH)D
3 to increasing doses of vitamin D
3 does not follow a linear relationship. Current data from a dose-relationship study in mice and several findings from human studies (e.g., [
29,
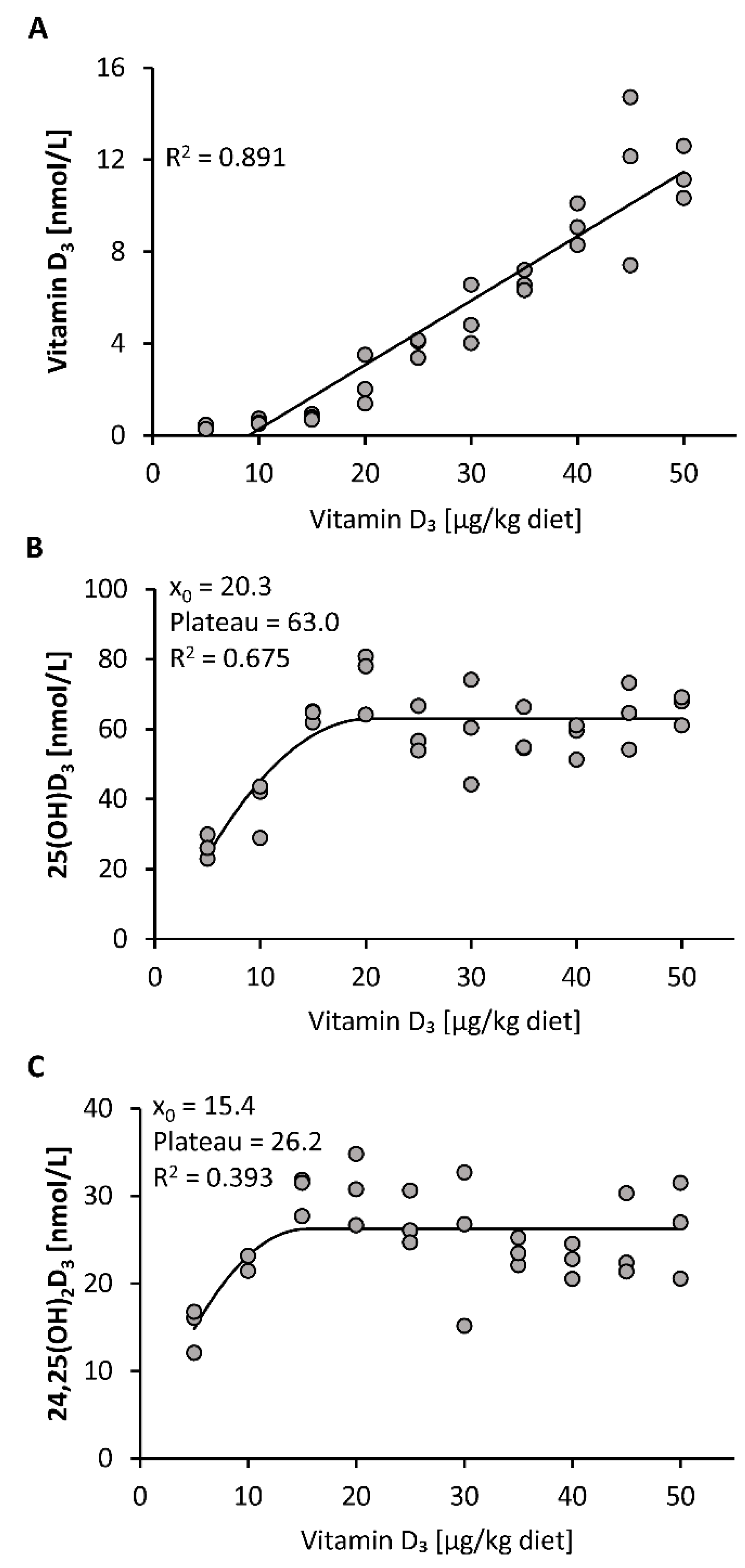
30]) show a disproportional increase in circulating 25(OH)D following increasing vitamin D doses. In general, dose-response curves of nutrient status markers normally follow a quadratic or curvilinear function and reach a transient plateau, or flattening of the curve, when the nutrient need is covered. Thus, the observed curvilinear-plateau response of 25(OH)D
3 to increasing vitamin D
3 doses indicates regulation and makes 25(OH)D a sensitive biomarker of low and adequate vitamin D status. Gallagher et al. assume that the curvilinear plateau of 25(OH)D is a result of an increased degradation of 25(OH)D to 24,25(OH)
2D [
31]. However, as we also observed a plateau in 24,25(OH)
2D
3 despite increasing vitamin D
3 doses, we assume that 25(OH)D is not primarily regulated via its degradation to 24,25(OH)
2D but rather by hepatic synthesis. This contradicts, at least in part, the common view that the production of 25(OH)D is not significantly regulated and primarily depends on the availability of vitamin D [
5]. Another interesting finding of the current study was the observation that 25(OH)D
3 showed no decline when switching mice from a vitamin D
3-rich diet to a vitamin D
3-adequate diet. Based on the findings that circulating levels of 25(OH)D do not linearly respond to vitamin D intake and do not necessarily reflect tissue stores of vitamin D, the significance and reliability of analyzed plasma 25(OH)D for classifying vitamin D deficiency/inadequacy is limited. The measurement of plasma vitamin D could provide additional and more reliable information concerning vitamin D uptake and the body’s stores of vitamin D than 25(OH)D. Thus, plasma vitamin D could serve as a clinically relevant parameter to estimate the body’s stores of vitamin D in humans. The clinical implementation of plasma vitamin D analysis could be used to assess depleted vitamin D stores or to avoid an unnecessary use of vitamin D supplements. However, it must be noted that data on human tissue stores of vitamin D and the ability of mobilization are currently insufficient. Further studies are necessary to elucidate cut-off values of vitamin D that indicate adequate or insufficient tissue storages of vitamin D.
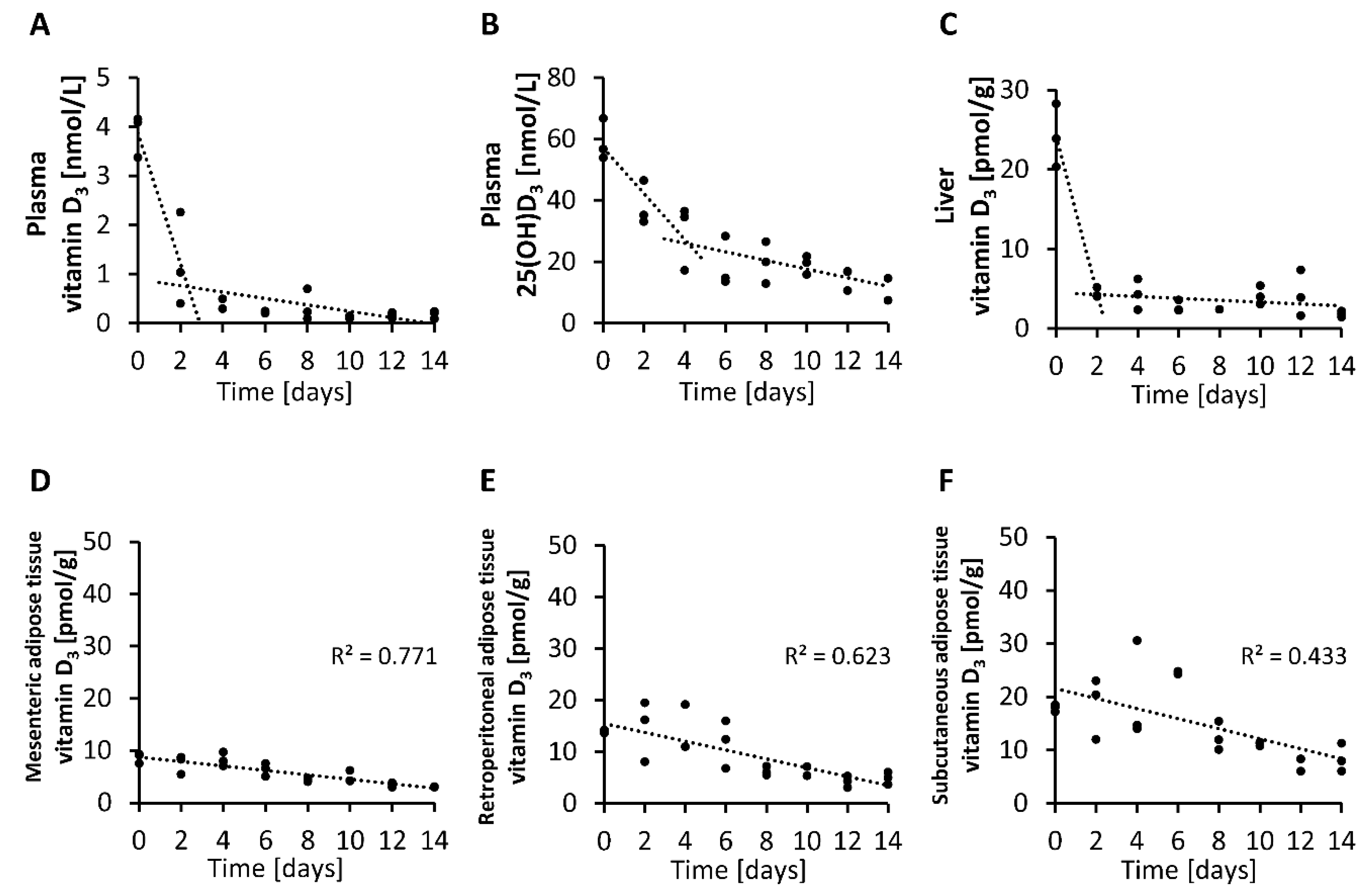
To elucidate the suitability of liver and adipose tissues to mobilize vitamin D in times of an absent vitamin D supply, we investigated the decline in vitamin D
3 in the tissues of mice consuming no vitamin D. Here, we found a rapid and strong reduction in vitamin D
3 in the liver that corresponded to the decline in vitamin D
3 in plasma. However, in contrast to plasma vitamin D
3, 25(OH)D
3 showed a less rapid decline to a vitamin D-free diet, which is suggested to be a result of stimulated hepatic synthesis of 25(OH)D and possibly by the longer half-life of 25(OH)D compared to vitamin D [
6,
7]. In contrast to that in the liver, vitamin D
3 in adipose tissues showed a weak and continuous reduction after the consumption of a vitamin D-free diet. The data suggest that adipose tissues can principally release vitamin D, but in contrast to the liver, this mobilization is lower and less rapid. This is an interesting finding because the vitamin D
3 levels in the adipose tissues increased to a similar extent as the vitamin D
3 levels in the liver in response to the feeding of increasing doses of vitamin D
3.
The observation that adipose tissues may contribute to maintaining circulating vitamin D and 25(OH)D to only a minor extent was also shown in a study conducted with obese patients who underwent a gastric bypass [
32]. The authors of this study concluded that vitamin D in adipose tissue does not significantly contribute to circulating 25(OH)D, although the individuals included in that study showed a marked loss of body fat [
32].
The role of adipose tissues in vitamin D metabolism is a fundamental question because of the high prevalence of overweight and obesity worldwide [
33]. In the first study, we observed a linear increase in vitamin D
3 in the liver and adipose tissues with increasing doses of dietary vitamin D
3. Interestingly, the storage of vitamin D
3 in adipose tissues has already been started when feeding low doses of vitamin D
3 that are noticeably below the requirement. If vitamin D is trapped in adipose tissue and not released, if necessary, the question will arise as to why adipose tissue has this great potential to store vitamin D, although it appears not to take part significantly in combating vitamin D deficiency. However, the current data assume that vitamin D in adipose tissues is not completely trapped and can be released, although to a significantly lesser extent and much more slowly than vitamin D in the liver. It is possible that the decline in vitamin D in adipose tissues is merely a consequence of adipose tissue turnover associated with the release of vitamin D that can be used for 25(OH)D synthesis.
To conclude, vitamin D status is currently assessed by the measurement of only one vitamin D metabolite: 25(OH)D. Here, we found that tissue stores of vitamin D3 were best reflected by circulating vitamin D, not by 25(OH)D. Importantly, we observed that adipose tissues can release vitamin D as their vitamin D concentrations decrease continuously in cases of an absent vitamin D consumption, but in contrast to the liver this mobilization was comparatively very small. The measurement of plasma vitamin D can be a valuable tool to estimate the body’s vitamin D store, and help to prevent a pending decline in vitamin D status or to avoid an unnecessary use of vitamin D supplements.