Association of Free Sugars Intake with Cardiometabolic Risk Factors among Japanese Adults: The 2016 National Health and Nutrition Survey, Japan
Abstract
:1. Introduction
2. Materials and Methods
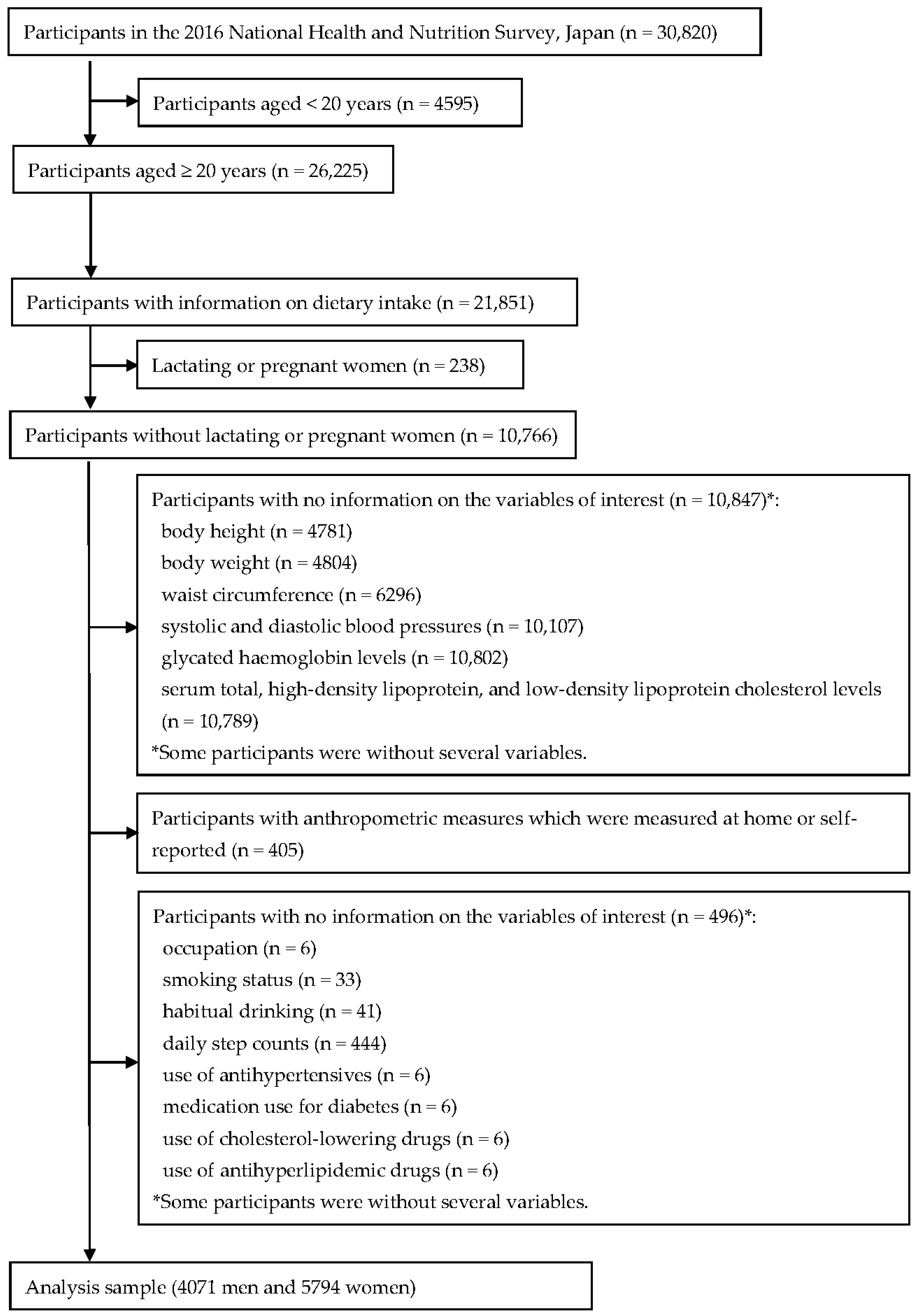
2.1. Data Source and Analytic Sample
2.2. Dietary Assessment
2.3. Assessment of Cardiometabolic Risk Factors and Covariates
2.4. Statistical Analysis
2.5. Sensitivity Analysis
3. Results
3.1. Free Sugars Intake and Food Sources
3.2. Characteristics of the Participants
3.3. Association Between Free Sugars Intake and Cardiometabolic Risk Factors
3.4. Sensitivity Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- GBD 2016 Causes of Death Collaborators. Global, regional, and national age-sex specific mortality for 264 causes of death, 1980–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet 2017, 390, 1151–1210. [Google Scholar] [CrossRef] [Green Version]
- Te Morenga, L.; Mallard, S.; Mann, J. Dietary sugars and body weight: Systematic review and meta-analyses of randomised controlled trials and cohort studies. BMJ 2012, 346, e7492. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Te Morenga, L.A.; Howatson, A.J.; Jones, R.M.; Mann, J. Dietary sugars and cardiometabolic risk: Systematic review and meta-analyses of randomized controlled trials of the effects on blood pressure and lipids. Am. J. Clin. Nutr. 2014, 100, 65–79. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Malik, V.S.; Hu, F.B. Sugar-Sweetened Beverages and Cardiometabolic Health: An Update of the Evidence. Nutrients 2019, 11, 1840. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fattore, E.; Botta, F.; Agostoni, C.; Bosetti, C. Effects of free sugars on blood pressure and lipids: A systematic review and meta-analysis of nutritional isoenergetic intervention trials. Am. J. Clin. Nutr. 2017, 105, 42–56. [Google Scholar] [CrossRef] [Green Version]
- Stanhope, K.L.; Schwarz, J.-M.; Havel, P.J. Adverse metabolic effects of dietary fructose. Curr. Opin. Lipidol. 2013, 24, 198–206. [Google Scholar] [CrossRef] [Green Version]
- Schwingshackl, L.; Neuenschwander, M.; Hoffmann, G.; Buyken, A.E.; Schlesinger, S. Dietary sugars and cardiometabolic risk factors: A network meta-analysis on isocaloric substitution interventions. Am. J. Clin. Nutr. 2020, 111, 187–196. [Google Scholar] [CrossRef]
- Chiu, S.; Sievenpiper, J.L.; De Souza, R.J.; Cozma, A.I.; Mirrahimi, A.; Carleton, A.J.; Ha, V.; Di Buono, M.; Jenkins, A.L.; Leiter, L.A.; et al. Effect of fructose on markers of non-alcoholic fatty liver disease (NAFLD): A systematic review and meta-analysis of controlled feeding trials. Eur. J. Clin. Nutr. 2014, 68, 416–423. [Google Scholar] [CrossRef]
- Ha, V.; Sievenpiper, J.L.; De Souza, R.J.; Chiavaroli, L.; Wang, D.D.; Cozma, A.I.; Mirrahimi, A.; Yu, M.E.; Carleton, A.J.; Dibuono, M.; et al. Effect of fructose on blood pressure: A systematic review and meta-analysis of controlled feeding trials. Hypertension 2012, 59, 787–795. [Google Scholar] [CrossRef] [Green Version]
- He, F.J.; Marrero, N.M.; MacGregor, G.A. Salt intake is related to soft drink consumption in children and adolescents: A link to obesity? Hypertension 2008, 51, 629–634. [Google Scholar] [CrossRef] [Green Version]
- Ludwig, D.S. The glycemic index: Physiological mechanisms relating to obesity, diabetes, and cardiovascular disease. JAMA 2002, 287, 2414–2423. [Google Scholar] [CrossRef] [PubMed]
- Bosma-Den Boer, M.M.; Van Wetten, M.L.; Pruimboom, L. Chronic inflammatory diseases are stimulated by current lifestyle: How diet, stress levels and medication prevent our body from recovering. Nutr. Metab. 2012, 9, 1–14. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barrett, P.; Imamura, F.; Brage, S.; Griffin, S.J.; Wareham, N.J.; Forouhi, N.G. Sociodemographic, lifestyle and behavioural factors associated with consumption of sweetened beverages among adults in Cambridgeshire, UK: The Fenland Study. Public Health Nutr. 2017, 20, 2766–2777. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yamada, M.; Murakami, K.; Sasaki, S.; Takahashi, Y.; Okubo, H. Soft Drink Intake Is Associated with Diet Quality Even among Young Japanese Women with Low Soft Drink Intake. J. Am. Diet. Assoc. 2008, 108, 1997–2004. [Google Scholar] [CrossRef]
- Fujiwara, A.; Murakami, K.; Asakura, K.; Uechi, K.; Sugimoto, M.; Wang, H.-C.; Masayasu, S.; Sasaki, S. Estimation of Starch and Sugar Intake in a Japanese Population Based on a Newly Developed Food Composition Database. Nutrients 2018, 10, 1474. [Google Scholar] [CrossRef] [Green Version]
- Yamakawa, M.; Wada, K.; Koda, S.; Mizuta, F.; Uji, T.; Oba, S.; Nagata, C. High Intake of Free Sugars, Fructose, and Sucrose Is Associated with Weight Gain in Japanese Men. J. Nutr. 2020, 150, 322–330. [Google Scholar] [CrossRef]
- Okuda, M.; Fujiwara, A.; Sasaki, S. Added and Free Sugars Intake and Metabolic Biomarkers in Japanese Adolescents. Nutrients 2020, 12, 2046. [Google Scholar] [CrossRef]
- Ministry of Health, Labour, and Welfare of Japan. The National Health and Nutrition Survey in Japan. 2016. Available online: http://www.mhlw.go.jp/bunya/kenkou/eiyou/h28-houkoku.html (accessed on 22 November 2020). (In Japanese)
- Ikeda, N.; Takimoto, H.; Imai, S.; Miyachi, M.; Nishi, N. Data Resource Profile: The Japan National Health and Nutrition Survey (NHNS). Int. J. Epidemiol. 2015, 44, 1842–1849. [Google Scholar] [CrossRef]
- Takimoto, H.; Yoshiike, N.; Katagiri, A.; Ishida, H.; Abe, S. Nutritional status of pregnant and lactating women in Japan: A comparison with non-pregnant/non-lactating controls in the National Nutrition Survey. J. Obstet. Gynaecol. Res. 2003, 29, 96–103. [Google Scholar] [CrossRef]
- Ministry of Health, Labour, and Welfare of Japan. Ethical Guidelines for Medical and Health Research Involving Human Subjects. Available online: https://www.mhlw.go.jp/file/06-Seisakujouhou-10600000-Daijinkanboukouseikagakuka/0000080278.pdf. (accessed on 22 November 2020).
- Science and Technology Agency. Standard Tables of Food Composition in Japan, 2010; National Printing Bureau: Tokyo, Japan, 2010. (In Japanese) [Google Scholar]
- Science and Technology Agency. Standard Tables of Food Composition in Japan, 2015 (Seventh Revised Edition); National Printing Bureau: Tokyo, Japan, 2015. (In Japanese) [Google Scholar]
- Science and Technology Agency. Standard Tables of Food Composition in Japan, 2015 (Seventh Revised Edition) Addendum, 2016; National Printing Bureau: Tokyo, Japan, 2016. (In Japanese) [Google Scholar]
- World Health Organization. Guideline: Sugars Intake for Adults and Children; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- Louie, J.C.Y.; Moshtaghian, H.; Boylan, S.; Flood, V.M.; Rangan, A.M.; Barclay, A.W.; Brand-Miller, J.C.; Gill, T.P. A systematic methodology to estimate added sugar content of foods. Eur. J. Clin. Nutr. 2015, 69, 154–161. [Google Scholar] [CrossRef]
- Mok, A.; Ahmad, R.; Rangan, A.; Louie, J.C.Y. Intake of free sugars and micronutrient dilution in Australian adults. Am. J. Clin. Nutr. 2018, 107, 94–104. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Iwaoka, F.; Yoshiike, N.; Date, C.; Shimada, T.; Tanaka, H. A validation study on a method to estimate nutrient intake by family members through a household-based food-weighing survey. J. Nutr. Sci. Vitaminol. 2001, 47, 222–227. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nakamura, M.; Kiyama, M.; Kitamura, A.; Ishikawa, Y.; Sato, S.; Noda, H.; Yoshiike, N. Revised system to evaluate measurement of blood chemistry data from the Japanese National health and nutrition survey and prefectural health and nutrition surveys. J. Epidemiol. 2013, 23, 28–34. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Livingstone, M.B.E.; Black, A.E. Markers of the validity of reported energy intake. J. Nutr. 2003, 133, 895S–920S. [Google Scholar] [CrossRef]
- Willett, W.C. Nutritional Epidemiology, 3rd ed.; Oxford University Press: New York, NY, USA, 2013. [Google Scholar]
- Murakami, K.; Sasaki, S.; Okubo, H. Freshmen in Dietetic Courses Study II Group Characteristics of under- and over-reporters of energy intake among young Japanese women. J. Nutr. Sci. Vitaminol. 2012, 58, 253–262. [Google Scholar] [CrossRef] [Green Version]
- Murakami, K.; Miyake, Y.; Sasaki, S.; Tanaka, K.; Arakawa, M. Characteristics of under- and over-reporters of energy intake among Japanese children and adolescents: The Ryukyus Child Health Study. Nutrition 2012, 28, 532–538. [Google Scholar] [CrossRef]
- Gibson, S.; Francis, L.; Newens, K.; Livingstone, B. Associations between free sugars and nutrient intakes among children and adolescents in the UK. Br. J. Nutr. 2016, 116, 1265–1274. [Google Scholar] [CrossRef] [Green Version]
- Wong, T.H.T.; Sui, Z.; Rangan, A.; Louie, J.C.Y. Discrepancy in socioeconomic status does not fully explain the variation in diet quality between consumers of different coffee types. Eur. J. Nutr. 2018, 57, 2123–2131. [Google Scholar] [CrossRef]
- Black, A. Critical evaluation of energy intake using the Goldberg cut-off for energy intake:basal metabolic rate. A practical guide to its calculation, use and limitations. Int. J. Obes. Relat. Metab. Disord. 2000, 24, 1119–1130. [Google Scholar] [CrossRef] [Green Version]
- Fujiwara, A.; Okada, E.; Okada, C.; Matsumoto, M.; Takimoto, H. Association between free sugars intake and nutrient dilution among Japanese adults: The 2016 National Health and Nutrition Survey, Japan. Eur. J. Nutr. 2020. [Google Scholar] [CrossRef]
- Murakami, K.; Livingstone, M.B.E.; Sasaki, S. Diet quality scores in relation to metabolic risk factors in Japanese adults: A cross-sectional analysis from the 2012 National Health and Nutrition Survey, Japan. Eur. J. Nutr. 2019, 58, 2037–2050. [Google Scholar] [CrossRef] [PubMed]
- Ganpule, A.A.; Tanaka, S.; Ishikawa-Takata, K.; Tabata, I. Interindividual variability in sleeping metabolic rate in Japanese subjects. Eur. J. Clin. Nutr. 2007, 61, 1256–1261. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Miyake, R.; Tanaka, S.; Ohkawara, K.; Ishikawa-Takata, K.; Hikihara, Y.; Taguri, E.; Kayashita, J.; Tabata, I. Validity of predictive equations for basal metabolic rate in Japanese adults. J. Nutr. Sci. Vitaminol. 2011, 57, 224–232. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ahmad, R.; Mok, A.; Rangan, A.M.; Louie, J.C.Y. Association of free sugar intake with blood pressure and obesity measures in Australian adults. Eur. J. Nutr. 2019, 59, 651–659. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, L.; Imamura, F.; Brage, S.; Griffin, S.J.; Wareham, N.J.; Forouhi, N.G. Intakes and sources of dietary sugars and their association with metabolic and inflammatory markers. Clin. Nutr. 2018, 37, 1313–1322. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xi, B.; Huang, Y.; Reilly, K.H.; Li, S.; Zheng, R.; Barrio-Lopez, M.T.; Martinez-Gonzalez, M.A.; Zhou, D. Sugar-sweetened beverages and risk of hypertension and CVD: A dose–response meta-analysis. Br. J. Nutr. 2015, 113, 709–717. [Google Scholar] [CrossRef] [Green Version]
- Lei, L.; Rangan, A.; Flood, V.M.; Louie, J.C.Y. Dietary intake and food sources of added sugar in the Australian population. Br. J. Nutr. 2016, 115, 868–877. [Google Scholar] [CrossRef] [Green Version]
- Public Health England and the Food Standards Agency. National Diet and Nutrition Survey: Results from Years 7 and 8 (Combined) of the Rolling Programme (2014/2015 to 2015/2016); Public Health England: London, UK, 2018. [Google Scholar]
- Imamura, F.; O’Connor, L.; Ye, Z.; Mursu, J.; Hayashino, Y.; Bhupathiraju, S.N.; Forouhi, N.G. Consumption of sugar sweetened beverages, artificially sweetened beverages, and fruit juice and incidence of type 2 diabetes: Systematic review, meta-analysis, and estimation of population attributable fraction. BMJ 2015, 351, h3576. [Google Scholar] [CrossRef] [Green Version]
- Sasaki, S.; Takahashi, T.; Iitoi, Y.; Iwase, Y.; Kobayashi, M.; Ishihara, J.; Akabane, M.; Tsugane, S. JPHC Food and nutrient intakes assessed with dietary records for the validation study of a self-administered food frequency questionnaire in JPHC Study Cohort I. J. Epidemiol. 2003, 13, S23–S50. [Google Scholar] [CrossRef] [Green Version]
- Tani, Y.; Asakura, K.; Sasaki, S.; Hirota, N.; Notsu, A.; Todoriki, H.; Miura, A.; Fukui, M.; Date, C. The influence of season and air temperature on water intake by food groups in a sample of free-living Japanese adults. Eur. J. Clin. Nutr. 2015, 69, 907–913. [Google Scholar] [CrossRef]
- Ministry of Health, Labour, and Welfare of Japan. Dietary Reference Intakes for Japanese. 2020. Available online: https://www.mhlw.go.jp/content/10904750/000586553.pdf (accessed on 22 November 2020). (In Japanese)
| Men | Women | |||
|---|---|---|---|---|
| Mean | SD | Mean | SD | |
| Intake (%E) | 4.8 | 3.9 | 5.8 | 4.2 |
| Contribution (%) 1,2 | ||||
| Bread | 0.2 | 2.3 | 0.3 | 2.5 |
| Noodles | 0.6 | 4.5 | 0.3 | 2.6 |
| Other grain products | 0.4 | 3.1 | 0.7 | 4.5 |
| Potatoes | 0.0 | 0.1 | 0.0 | 0.4 |
| Sugars and jams | 30.1 | 27.4 | 29.8 | 26.6 |
| Pulses and nuts | 1.2 | 6.7 | 1.6 | 7.3 |
| Vegetables 3 | 2.2 | 7.0 | 1.6 | 5.9 |
| Fruits | 0.3 | 2.8 | 0.3 | 2.6 |
| Fish and shellfish | 5.1 | 11.5 | 4.2 | 10.1 |
| Meats | 2.0 | 6.7 | 1.4 | 5.1 |
| Eggs | 0.1 | 0.7 | 0.1 | 0.9 |
| Dairy products | 2.8 | 9.7 | 4.1 | 11.7 |
| Fat and oil | 0.4 | 2.9 | 0.3 | 2.8 |
| Confectioneries | 17.0 | 25.9 | 23.0 | 28.0 |
| Fruit and vegetable juices | 1.0 | 7.4 | 1.0 | 7.1 |
| Alcoholic beverages | 0.8 | 5.9 | 0.5 | 4.7 |
| Soft drinks 4 | 11.3 | 23.4 | 9.4 | 20.5 |
| Seasonings 5 | 24.4 | 24.8 | 21.3 | 22.1 |
| Quartile 1 (n = 1017) | Quartile 2 (n = 1018) | Quartile 3 (n = 1018) | Quartile 4 (n = 1018) | p1 | |||||
|---|---|---|---|---|---|---|---|---|---|
| Free sugars intake (%E), mean ± SD | 1.2 | 0.5 | 289 | 0.5 | 5.0 | 0.8 | 10.0 | 3.9 | <0.0001 |
| Age (years), mean ± SD | 58.9 | 15.6 | 61.4 | 15.5 | 62.0 | 15.9 | 60.4 | 17.0 | 0.16 |
| Age category (years), n (%) | |||||||||
| 20–29 | 36 | (3.5) | 35 | (3.4) | 38 | (3.7) | 68 | (6.7) | 0.02 |
| 30–39 | 96 | (9.4) | 88 | (8.6) | 89 | (8.7) | 87 | (8.6) | |
| 40–49 | 178 | (17.5) | 117 | (11.5) | 111 | (10.9) | 115 | (11.3) | |
| 50–59 | 150 | (14.7) | 129 | (12.7) | 129 | (12.7) | 118 | (11.6) | |
| 60–69 | 284 | (27.9) | 312 | (30.6) | 288 | (28.3) | 277 | (27.2) | |
| 70–79 | 200 | (19.7) | 239 | (23.5) | 257 | (25.2) | 251 | (24.7) | |
| ≥80 | 73 | (7.2) | 98 | (9.6) | 106 | (10.4) | 102 | (10.0) | |
| Occupation, n (%) | |||||||||
| Professional/manager | 219 | (21.5) | 199 | (19.5 | 191 | (18.8) | 177 | (17.4) | 0.003 |
| Sales/service/clerical | 172 | (16.9) | 170 | (16.7) | 155 | (15.2) | 175 | (17.2) | |
| Security/transportation/labour | 296 | (29.1) | 284 | (27.9 | 297 | (29.2) | 274 | (26.9) | |
| Not in paid employment | 330 | (32.4) | 365 | (35.9) | 375 | (36.8) | 392 | (38.5) | |
| Smoking status, n (%) | |||||||||
| Never | 542 | (53.3) | 577 | (56.0) | 589 | (57.9) | 596 | (58.5) | 0.02 |
| Past | 180 | (17.7) | 202 | (19.8) | 200 | (19.6) | 159 | (15.6) | |
| Current | 295 | (29.0) | 239 | (23.5) | 229 | (22.5) | 263 | (25.8) | |
| Habitual drinking, n (%) 2 | |||||||||
| Yes | 722 | (71.0) | 707 | (69.4) | 669 | (65.7) | 561 | (55.1) | <0.0001 |
| Daily step counts, n (%) 3 | |||||||||
| Low | 347 | (34.1) | 338 | (33.2) | 325 | (31.9) | 347 | (34.1) | 0.35 |
| Middle | 353 | (34.7) | 336 | (33.0) | 344 | (33.8) | 324 | (31.8) | |
| High | 317 | (31.2) | 344 | (33.8) | 349 | (34.3) | 347 | (34.1) | |
| Use of medication, n (%) | |||||||||
| Antihypertensives | 312 | (30.7) | 352 | (34.6) | 346 | (34.0) | 323 | (31.7) | 0.70 |
| For diabetes | 97 | (9.5) | 125 | (12.3) | 94 | (9.2) | 89 | (8.7) | 0.20 |
| Cholesterol-lowering drugs | 104 | (10.2) | 122 | (12.0) | 152 | (14.9) | 140 | (13.8) | 0.002 |
| Antihyperlipidemic drugs | 54 | (5.3) | 63 | (6.2) | 70 | (6.9) | 49 | (4.8) | 0.81 |
| Energy intake (kcal), mean ± SD | 2110 | 574 | 2189 | 564 | 2265 | 531 | 2247 | 571 | <0.0001 |
| Fat intake (%E), mean ± SD | 26.2 | 7.8 | 26.5 | 7.9 | 25.7 | 6.9 | 25.1 | 7.4 | <0.0001 |
| Dietary fibre intake (g/1000 kcal), mean ± SD | 6.8 | 2.7 | 7.3 | 2.8 | 7.6 | 2.8 | 7.4 | 2.9 | <0.0001 |
| Quartile 1 (n = 1448) | Quartile 2 (n = 1449) | Quartile 3 (n = 1449) | Quartile 4 (n = 1448) | p1 | |||||
|---|---|---|---|---|---|---|---|---|---|
| Free sugars intake (%E), mean ± SD | 1.7 | 0.7 | 3.9 | 0.6 | 6.2 | 0.8 | 11.3 | 4.4 | <0.0001 |
| Age (years), mean ± SD | 59.2 | 15.6 | 59.6 | 15.6 | 60.5 | 15.5 | 60.3 | 16.3 | 0.03 |
| Age category (years), n (%) | |||||||||
| 20–29 | 48 | (3.3) | 50 | (3.5) | 48 | (3.3) | 55 | (3.8) | 0.02 |
| 30–39 | 137 | (9.5) | 140 | (9.7) | 130 | (9.0) | 144 | (9.9) | |
| 40–49 | 239 | (16.5) | 208 | (14.4) | 189 | (13.0) | 193 | (13.3) | |
| 50–59 | 228 | (15.7) | 237 | (16.4) | 235 | (16.2) | 197 | (13.6) | |
| 60–69 | 400 | (27.6) | 385 | (26.6) | 400 | (27.6) | 398 | (27.5) | |
| 70–79 | 272 | (18.8) | 318 | (21.9) | 308 | (21.3) | 303 | (20.9) | |
| ≥80 | 124 | (8.6) | 111 | (7.7) | 139 | (9.6) | 158 | (10.9) | |
| Occupation, n (%) | |||||||||
| Professional/manager | 170 | (11.7) | 188 | (13.0) | 155 | (10.7) | 155 | (10.7) | 0.04 |
| Sales/service/clerical | 401 | (27.7) | 403 | (27.8) | 376 | (25.9) | 387 | (26.7) | |
| Security/transportation/labour | 146 | (10.1) | 129 | (8.9) | 128 | (8.8) | 139 | (9.6) | |
| Not in paid employment | 731 | (50.5) | 729 | (50.3) | 790 | (54.5) | 767 | (53.0) | |
| Smoking status, n (%) | |||||||||
| Never | 1305 | (90.1) | 1317 | (90.9) | 1332 | (91.9) | 1313 | (90.7) | 0.37 |
| Past | 41 | (2.8) | 60 | (4.1) | 40 | (2.8) | 47 | (3.2) | |
| Current | 102 | (7.0) | 72 | (5.0) | 77 | (5.3) | 88 | (6.1) | |
| Habitual drinking, n (%) 2 | |||||||||
| Yes | 478 | (33.0) | 461 | (31.8) | 440 | (30.4) | 432 | (29.8) | 0.04 |
| Daily step counts, n (%) 3 | |||||||||
| Low | 489 | (33.8) | 461 | (31.8) | 459 | (31.7) | 523 | (36.1) | 0.13 |
| Middle | 463 | (32.0) | 491 | (33.9) | 519 | (35.8) | 458 | (31.6) | |
| High | 496 | (34.3) | 497 | (34.3) | 471 | (32.5) | 467 | (32.3) | |
| Use of medication, n (%) | |||||||||
| Antihypertensives | 375 | (25.9) | 380 | (26.2) | 404 | (27.9) | 384 | (26.5) | 0.50 |
| For diabetes | 97 | (6.7) | 76 | (5.2) | 58 | (4.0) | 59 | (4.1) | 0.0004 |
| Cholesterol-lowering drugs | 232 | (16.0) | 256 | (17.7) | 289 | (19.9) | 268 | (18.5) | 0.03 |
| Antihyperlipidemic drugs | 52 | (3.6) | 59 | (4.1) | 49 | (3.4) | 66 | (4.6) | 0.33 |
| Energy intake (kcal), mean ± SD | 1675 | 442 | 1789 | 432 | 1801 | 432 | 1829 | 482 | <0.0001 |
| Fat intake (%E), mean ± SD | 28.5 | 8.1 | 28.6 | 7.1 | 27.9 | 7.2 | 26.4 | 7.4 | <0.0001 |
| Dietary fibre intake (g/1000 kcal), mean ± SD | 8.6 | 3.2 | 8.9 | 3.1 | 8.9 | 3.3 | 8.5 | 3.0 | 0.19 |
| Men | Women | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Quartile 1 (n = 1017) | Quartile 2 1 (n = 1018) | Quartile 3 1 (n = 1018) | Quartile 4 1 (n = 1018) | p2 | Quartile 1 (n = 1448) | Quartile 2 1 (n = 1449) | Quartile 3 1 (n = 1449) | Quartile 4 1 (n = 1448) | p2 | |||||||||
| BMI (kg/m2) | ||||||||||||||||||
| Crude | 24.1 | 0.1 | 24.0 | 0.1 | 23.7 | 0.1 | 24.0 | 0.1 | 0.50 | 22.6 | 0.1 | 22.6 | 0.1 | 22.7 | 0.1 | 22.6 | 0.1 | 0.80 |
| Adjusted 3 | 24.0 | 0.1 | 24.0 | 0.1 | 23.7 | 0.1 | 24.0 | 0.1 | 0.98 | 22.6 | 0.1 | 22.7 | 0.1 | 22.7 | 0.1 | 22.5 | 0.1 | 0.42 |
| WC (cm) | ||||||||||||||||||
| Crude | 87.0 | 0.3 | 86.9 | 0.3 | 86.2 | 0.3 | 87.0 | 0.3 | 0.82 | 81.6 | 0.3 | 82.1 | 0.3 | 82.4 | 0.3 | 82.2 | 0.3 | 0.17 |
| Adjusted 3 | 87.0 | 0.3 | 86.8 | 0.3 | 86.2 | 0.3 | 87.2 | 0.3 | 0.65 | 81.8 | 0.3 | 82.2 | 0.3 | 82.3 | 0.3 | 82.0 | 0.3 | 0.67 |
| SBP (mmHg) | ||||||||||||||||||
| Crude | 135 | 1 | 135 | 1 | 135 | 1 | 132 | 1 * | 0.0005 | 129 | 0 | 128 | 0 | 128 | 0 | 128 | 0 | 0.98 |
| Adjusted 4 | 135 | 0 | 134 | 0 | 135 | 0 | 133 | 0 * | 0.0003 | 129 | 0 | 128 | 0 | 128 | 0 | 128 | 0 | 0.16 |
| DBP (mmHg) | ||||||||||||||||||
| Crude | 82 | 0 | 82 | 0 | 81 | 0 * | 80 | 0 * | <0.0001 | 77 | 0 | 77 | 0 | 77 | 0 | 77 | 0 | 0.89 |
| Adjusted 4 | 82 | 0 | 81 | 0 | 81 | 0 | 81 | 0 | 0.04 | 77 | 0 | 77 | 0 | 77 | 0 | 77 | 0 | 0.89 |
| HbA1c (%) | ||||||||||||||||||
| Crude | 5.7 | 0.0 | 5.8 | 0.0 * | 5.8 | 0.0 | 5.8 | 0.0 | 0.58 | 5.7 | 0.0 | 5.7 | 0.0 | 5.7 | 0.0 | 5.7 | 0.0 | 0.10 |
| Adjusted 5 | 5.8 | 0.0 | 5.8 | 0.0 | 5.8 | 0.0 | 5.8 | 0.0 | 0.78 | 5.7 | 0.0 | 5.7 | 0.0 | 5.7 | 0.0 | 5.7 | 0.0 | 0.40 |
| TC (mg/dl) | ||||||||||||||||||
| Crude | 197 | 1 | 197 | 1 | 197 | 1 | 195 | 1 | 0.14 | 207 | 1 | 208 | 1 | 208 | 1 | 208 | 1 | 0.52 |
| Adjusted 6 | 196 | 1 | 197 | 1 | 197 | 1 | 197 | 1 | 0.43 | 207 | 1 | 207 | 1 | 208 | 1 | 209 | 1 | 0.04 |
| HDL-C (mg/dl) | ||||||||||||||||||
| Crude | 58 | 0 | 57 | 0 | 57 | 0 | 54 | 0 * | <0.0001 | 68 | 0 | 67 | 0 | 66 | 0 | 66 | 0 * | 0.002 |
| Adjusted 6 | 58 | 0 | 57 | 0 | 56 | 0* | 55 | 0 * | <0.0001 | 68 | 0 | 66 | 0 | 66 | 0 | 66 | 0 * | 0.02 |
| LDL-C (mg/dl) | ||||||||||||||||||
| Crude | 115 | 1 | 115 | 1 | 116 | 1 | 117 | 1 | 0.04 | 119 | 1 | 120 | 1 | 121 | 1 | 121 | 1 | 0.15 |
| Adjusted 6 | 113 | 1 | 115 | 1 | 117 | 1 * | 118 | 1 * | 0.0003 | 119 | 1 | 120 | 1 | 121 | 1 | 122 | 1 * | 0.002 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fujiwara, A.; Okada, E.; Okada, C.; Matsumoto, M.; Takimoto, H. Association of Free Sugars Intake with Cardiometabolic Risk Factors among Japanese Adults: The 2016 National Health and Nutrition Survey, Japan. Nutrients 2020, 12, 3624. https://doi.org/10.3390/nu12123624
Fujiwara A, Okada E, Okada C, Matsumoto M, Takimoto H. Association of Free Sugars Intake with Cardiometabolic Risk Factors among Japanese Adults: The 2016 National Health and Nutrition Survey, Japan. Nutrients. 2020; 12(12):3624. https://doi.org/10.3390/nu12123624
Chicago/Turabian StyleFujiwara, Aya, Emiko Okada, Chika Okada, Mai Matsumoto, and Hidemi Takimoto. 2020. "Association of Free Sugars Intake with Cardiometabolic Risk Factors among Japanese Adults: The 2016 National Health and Nutrition Survey, Japan" Nutrients 12, no. 12: 3624. https://doi.org/10.3390/nu12123624
APA StyleFujiwara, A., Okada, E., Okada, C., Matsumoto, M., & Takimoto, H. (2020). Association of Free Sugars Intake with Cardiometabolic Risk Factors among Japanese Adults: The 2016 National Health and Nutrition Survey, Japan. Nutrients, 12(12), 3624. https://doi.org/10.3390/nu12123624





