Whey Protein Combined with Low Dietary Fiber Improves Lipid Profile in Subjects with Abdominal Obesity: A Randomized, Controlled Trial
Abstract
1. Introduction
2. Materials and Methods
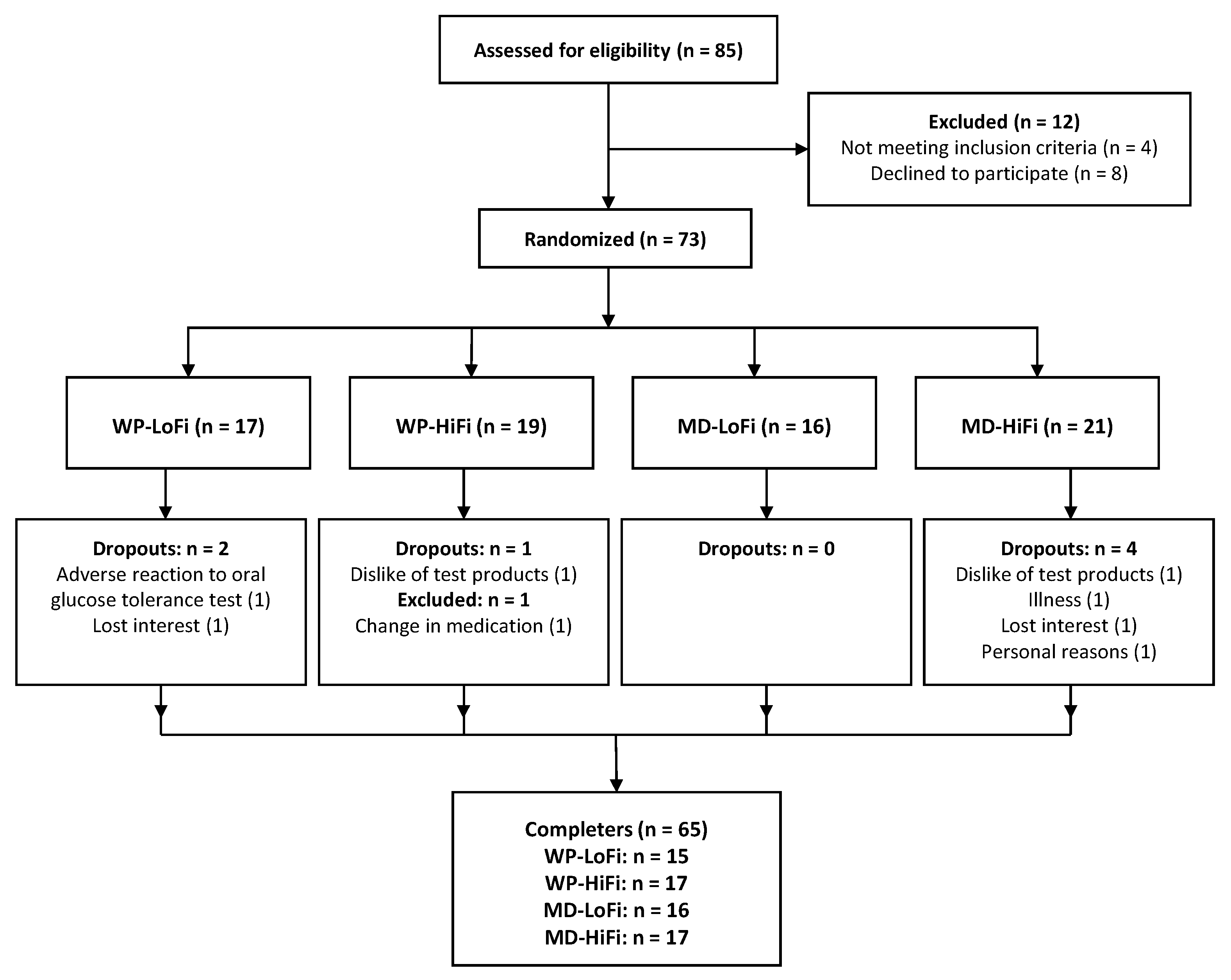
2.1. Study Design
2.2. Study Participants
2.3. Dietary Intervention
2.4. Test Products
2.5. Study Visits and Experimental Procedures
2.6. Biochemical Analyses
2.7. Calculations and Statistical Analyses
3. Results
3.1. Baseline Characteristics
3.2. Compliance
3.3. Dietary Intake
3.4. Lipid Profile
3.5. Glucose, Insulin and Glucagon
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Mekki, N.; Christofilis, M.A.; Charbonnier, M.; Atlan-Gepner, C.; Defoort, C.; Juhel, C.; Borel, P.; Portugal, H.; Pauli, A.M.; Vialettes, B.; et al. Influence of obesity and body fat distribution on postprandial lipemia and triglyceride-rich lipoproteins in adult women. J. Clin. Endocrinol. Metab. 1999, 84, 184–191. [Google Scholar] [CrossRef] [PubMed]
- Klop, B.; Elte, J.W.F.; Castro Cabezas, M. Dyslipidemia in Obesity: Mechanisms and Potential Targets. Nutrients 2013, 5, 1218–1240. [Google Scholar] [CrossRef] [PubMed]
- Reeder, B.A.; Senthilselvan, A.; Despres, J.P.; Angel, A.; Liu, L.; Wang, H.; Rabkin, S.W. The association of cardiovascular disease risk factors with abdominal obesity in Canada. Canadian Heart Health Surveys Research Group. CMAJ Can. Med Assoc. J. J. Assoc. Med Can. 1997, 157 (Suppl. S1), S39–S45. [Google Scholar]
- Bansal, S.; Buring, J.E.; Rifai, N.; Mora, S.; Sacks, F.M.; Ridker, P. Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. JAMA 2007, 298, 309–316. [Google Scholar] [CrossRef] [PubMed]
- Ridker, P.M. Fasting versus nonfasting triglycerides and the prediction of cardiovascular risk: Do we need to revisit the oral triglyceride tolerance test? Clin. Chem. 2008, 54, 11–13. [Google Scholar] [CrossRef] [PubMed]
- Kolovou, G.; Mikhailidis, D.P.; Kovar, J.; Lairon, D.; Nordestgaard, B.G.; Chye Ooi, T.; Perez-Martinez, P.; Bilianou, H.; Anagnostopoulou, K.; Panotopoulos, G. Assessment and clinical relevance of non-fasting and postprandial triglycerides: An expert panel statement. Curr. Vasc. Pharmacol. 2011, 9, 258–270. [Google Scholar] [CrossRef] [PubMed]
- Cornier, M.-A.; Dabelea, D.; Hernandez, T.L.; Lindstrom, R.C.; Steig, A.J.; Stob, N.R.; Van Pelt, R.E.; Wang, H.; Eckel, R.H. The Metabolic Syndrome. Endocr. Rev. 2008, 29, 777–822. [Google Scholar] [CrossRef]
- Alberti, G.; Zimmet, P.; Shaw, J.; Grundy, S.M. The IDF Consensus Worldwide Definition of the Metabolic Syndrome; International Diabetes Federation: Brussels, Belgium, 2006. [Google Scholar]
- Stevens, G.A.; Singh, G.M.; Lu, Y.; Danaei, G.; Lin, J.K.; Finucane, M.M.; Bahalim, A.N.; McIntire, R.K.; Gutierrez, H.R.; Cowan, M. National, regional, and global trends in adult overweight and obesity prevalences. Popul. Health Metr. 2012, 10, 22. [Google Scholar] [CrossRef]
- O’Neill, S.; O’Driscoll, L. Metabolic syndrome: A closer look at the growing epidemic and its associated pathologies. Obes. Rev. 2015, 16, 1–12. [Google Scholar] [CrossRef]
- Grundy, S.M.; Cleeman, J.I.; Daniels, S.R.; Donato, K.A.; Eckel, R.H.; Franklin, B.A.; Gordon, D.J.; Krauss, R.M.; Savage, P.J.; Smith, S.C., Jr. Diagnosis and management of the metabolic syndrome: An American Heart Association/National Heart, Lung, and Blood Institute scientific statement. Circulation 2005, 112, 2735–2752. [Google Scholar] [CrossRef]
- Fappa, E.; Yannakoulia, M.; Pitsavos, C.; Skoumas, I.; Valourdou, S.; Stefanadis, C. Lifestyle intervention in the management of metabolic syndrome: Could we improve adherence issues? Nutrition 2008, 24, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Fekete, Á.A.; Givens, D.I.; Lovegrove, J.A. Can milk proteins be a useful tool in the management of cardiometabolic health? An updated review of human intervention trials. Proc. Nutr. Soc. 2016, 75, 328–341. [Google Scholar] [CrossRef] [PubMed]
- Bjornshave, A.; Hermansen, K. Effects of dairy protein and fat on the metabolic syndrome and type 2 diabetes. Rev. Diabet. Stud. RDS 2014, 11, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Radavelli-Bagatini, S. The effects of whey protein on cardiometabolic risk factors. Obes. Rev. 2013, 14, 324–343. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Ellis, V.; Ho, S. Acute effects of whey protein isolate on cardiovascular risk factors in overweight, post-menopausal women. Atherosclerosis 2010, 212, 339–344. [Google Scholar] [CrossRef] [PubMed]
- Holmer-Jensen, J.; Mortensen, L.S.; Astrup, A.; de Vrese, M.; Holst, J.J.; Thomsen, C.; Hermansen, K. Acute differential effects of dietary protein quality on postprandial lipemia in obese non-diabetic subjects. Nutr. Res. 2013, 33, 34–40. [Google Scholar] [CrossRef] [PubMed]
- Mortensen, L.S.; Hartvigsen, M.L.; Brader, L.J.; Astrup, A.; Schrezenmeir, J.; Holst, J.J.; Thomsen, C.; Hermansen, K. Differential effects of protein quality on postprandial lipemia in response to a fat-rich meal in type 2 diabetes: Comparison of whey, casein, gluten, and cod protein. Am. J. Clin. Nutr. 2009, 90, 41–48. [Google Scholar] [CrossRef]
- Fekete, Á.A.; Giromini, C.; Chatzidiakou, Y.; Givens, D.I.; Lovegrove, J.A. Whey protein lowers blood pressure and improves endothelial function and lipid biomarkers in adults with prehypertension and mild hypertension: Results from the chronic Whey2Go randomized controlled trial. Am. J. Clin. Nutr. 2016, 104, 1534–1544. [Google Scholar] [CrossRef]
- Pal, S.; Ellis, V.; Dhaliwal, S. Effects of whey protein isolate on body composition, lipids, insulin and glucose in overweight and obese individuals. Br. J. Nutr. 2010, 104, 716–723. [Google Scholar] [CrossRef]
- Bohl, M.; Bjørnshave, A.; Rasmussen, K.V.; Schioldan, A.G.; Amer, B.; Larsen, M.K.; Dalsgaard, T.K.; Holst, J.J.; Herrmann, A.; O’Neill, S.; et al. Dairy proteins, dairy lipids, and postprandial lipemia in persons with abdominal obesity (DairyHealth): A 12-wk, randomized, parallel-controlled, double-blinded, diet intervention study. Am. J. Clin. Nutr. 2015, 101, 870–878. [Google Scholar] [CrossRef]
- Threapleton, D.E.; Greenwood, D.C.; Evans, C.E.L.; Cleghorn, C.L.; Nykjaer, C.; Woodhead, C.; Cade, J.E.; Gale, C.P.; Burley, V.J. Dietary fibre intake and risk of cardiovascular disease: Systematic review and meta-analysis. BMJ (Clin. Res. Ed.) 2013, 347, f6879. [Google Scholar] [CrossRef] [PubMed]
- The InterAct Consortium. Dietary fibre and incidence of type 2 diabetes in eight European countries: The EPIC-InterAct Study and a meta-analysis of prospective studies. Diabetologia 2015, 58, 1394–1408. [CrossRef] [PubMed]
- Pereira, M.A.; O’Reilly, E.; Augustsson, K.; Fraser, G.E.; Goldbourt, U.; Heitmann, B.L.; Hallmans, G.; Knekt, P.; Liu, S.; Pietinen, P.; et al. Dietary fiber and risk of coronary heart disease: A pooled analysis of cohort studies. Arch. Intern. Med. 2004, 164, 370–376. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.W.; Gilinsky, N.H.; Deakins, D.A.; Smith, S.F.; O’Neal, D.S.; Dillon, D.W.; Oeltgen, P.R. Lipid responses of hypercholesterolemic men to oat-bran and wheat-bran intake. Am. J. Clin. Nutr. 1991, 54, 678–683. [Google Scholar] [CrossRef] [PubMed]
- Tredger, J.A.; Morgan, L.M.; Travis, J.; Marks, V. The effects of guar gum, sugar beet fibre and wheat bran supplementation on serum lipoprotein levels in normocholesterolaemic volunteers. J. Hum. Nutr. Diet. 1991, 4, 375–384. [Google Scholar] [CrossRef]
- Cara, L.; Dubois, C.; Borel, P.; Armand, M.; Senft, M.; Portugal, H.; Pauli, A.; Bernard, P.; Lairon, D. Effects of oat bran, rice bran, wheat fiber, and wheat germ on postprandial lipemia in healthy adults. Am. J. Clin. Nutr. 1992, 55, 81–88. [Google Scholar] [CrossRef]
- Garcia, A.L.; Steiniger, J.; Reich, S.C.; Weickert, M.O.; Harsch, I.; Machowetz, A.; Mohlig, M.; Spranger, J.; Rudovich, N.N.; Meuser, F.; et al. Arabinoxylan fibre consumption improved glucose metabolism, but did not affect serum adipokines in subjects with impaired glucose tolerance. Horm. Metab. Res. Horm. Und Stoffwechs. Horm. Et Metab. 2006, 38, 761–766. [Google Scholar] [CrossRef]
- Garcia, A.L.; Otto, B.; Reich, S.C.; Weickert, M.O.; Steiniger, J.; Machowetz, A.; Rudovich, N.N.; Möhlig, M.; Katz, N.; Speth, M.; et al. Arabinoxylan consumption decreases postprandial serum glucose, serum insulin and plasma total ghrelin response in subjects with impaired glucose tolerance. Eur. J. Clin. Nutr. 2007, 61, 334–341. [Google Scholar] [CrossRef]
- Giacco, R.; Costabile, G.; Della Pepa, G.; Anniballi, G.; Griffo, E.; Mangione, A.; Cipriano, P.; Viscovo, D.; Clemente, G.; Landberg, R.; et al. A whole-grain cereal-based diet lowers postprandial plasma insulin and triglyceride levels in individuals with metabolic syndrome. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 837–844. [Google Scholar] [CrossRef]
- Schioldan, A.G.; Gregersen, S.; Hald, S.; Bjørnshave, A.; Bohl, M.; Hartmann, B.; Holst, J.J.; Stødkilde-Jørgensen, H.; Hermansen, K. Effects of a diet rich in arabinoxylan and resistant starch compared with a diet rich in refined carbohydrates on postprandial metabolism and features of the metabolic syndrome. Eur. J. Nutr. 2018, 57, 795–807. [Google Scholar] [CrossRef]
- Doig, G.S.; Simpson, F. Randomization and allocation concealment: A practical guide for researchers. J. Crit. Care 2005, 20, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Ingerslev, A.K.; Theil, P.K.; Hedemann, M.S.; Laerke, H.N.; Bach Knudsen, K.E. Resistant starch and arabinoxylan augment SCFA absorption, but affect postprandial glucose and insulin responses differently. Br. J. Nutr. 2014, 111, 1564–1576. [Google Scholar] [CrossRef] [PubMed]
- Saarinen, M.T.; Lahtinen, S.J.; Sørensen, J.F.; Tiihonen, K.; Ouwehand, A.C.; Rautonen, N.; Morgan, A. Treatment of Bran Containing Bread by Baking Enzymes; Effect on the Growth of Probiotic Bacteria on Soluble Dietary Fiber Extract in Vitro. Biosci. Biotechnol. Biochem. 2012, 76, 1135–1139. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Knudsen, K.E.B. Carbohydrate and lignin contents of plant materials used in animal feeding. Anim. Feed Sci. Technol. 1997, 67, 319–338. [Google Scholar] [CrossRef]
- Kasprzak, M.M.; Lærke, H.N.; Knudsen, K.E.B. Effects of isolated and complex dietary fiber matrices in breads on carbohydrate digestibility and physicochemical properties of ileal effluent from pigs. J. Agric. Food Chem. 2012, 60, 12469–12476. [Google Scholar] [CrossRef] [PubMed]
- Wierzbicka, R.; Wu, H.; Franek, M.; Kamal-Eldin, A.; Landberg, R. Determination of alkylresorcinols and their metabolites in biological samples by gas chromatography-mass spectrometry. J. Chromatogr. B 2015, 1000, 120–129. [Google Scholar] [CrossRef]
- Nilsson-Ehle, P.; Schotz, M.C. A stable, radioactive substrate emulsion for assay of lipoprotein lipase. J. Lipid Res. 1976, 17, 536–541. [Google Scholar]
- Allison, D.B.; Paultre, F.; Maggio, C.; Mezzitis, N.; Pi-Sunyer, F.X. The Use of Areas Under Curves in Diabetes Research. Diabet. Care 1995, 18, 245–250. [Google Scholar] [CrossRef]
- Carstensen, M.; Thomsen, C.; Hermansen, K. Incremental area under response curve more accurately describes the triglyceride response to an oral fat load in both healthy and type 2 diabetic subjects. Metab. Clin. Exp. 2003, 52, 1034–1037. [Google Scholar] [CrossRef]
- Weiss, E.P.; Fields, D.A.; Mittendorfer, B.; Haverkort, M.A.D.; Klein, S. Reproducibility of postprandial lipemia tests and validity of an abbreviated 4-hour test. Metab. Clin. Exp. 2008, 57, 1479–1485. [Google Scholar] [CrossRef]
- Zhang, J.W.; Tong, X.; Wan, Z.; Wang, Y.; Qin, L.Q.; Szeto, I.M.Y. Effect of whey protein on blood lipid profiles: A meta-analysis of randomized controlled trials. Eur. J. Clin. Nutr. 2016, 70, 879–885. [Google Scholar] [CrossRef] [PubMed]
- Miller, M. Current perspectives on the management of hypertriglyceridemia. Am. Heart J. 2000, 140, 232–240. [Google Scholar] [CrossRef] [PubMed]
- Smith, D.; Watts, G.F.; Dane-Stewart, C.; Mamo, J.C. Post-prandial chylomicron response may be predicted by a single measurement of plasma apolipoprotein B48 in the fasting state. Eur. J. Clin. Invest. 1999, 29, 204–209. [Google Scholar] [CrossRef] [PubMed]
- Masuda, D.; Sugimoto, T.; Tsujii, K.-I.; Inagaki, M.; Nakatani, K.; Yuasa-Kawase, M.; Tsubakio-Yamamoto, K.; Ohama, T.; Nishida, M.; Ishigami, M.; et al. Correlation of fasting serum apolipoprotein B-48 with coronary artery disease prevalence. Eur. J. Clin. Invest. 2012, 42, 992–999. [Google Scholar] [CrossRef] [PubMed]
- Nakajima, K.; Nagamine, T.; Fujita, M.Q.; Ai, M.; Tanaka, A.; Schaefer, E. Chapter Three—Apolipoprotein B-48: A Unique Marker of Chylomicron Metabolism. In Advances in Clinical Chemistry; Makowski, G.S., Ed.; Elsevier: Amsterdam, The Netherlands, 2014; Volume 64, pp. 117–177. [Google Scholar]
- Eckel, R.H. Lipoprotein lipase. A multifunctional enzyme relevant to common metabolic diseases. New Engl. J. Med. 1989, 320, 1060–1068. [Google Scholar] [CrossRef] [PubMed]
- Adams, R.L.; Broughton, K.S. Insulinotropic Effects of Whey: Mechanisms of Action, Recent Clinical Trials, and Clinical Applications. Ann. Nutr. Metab. 2016, 69, 56–63. [Google Scholar] [CrossRef]
- Hermansen, K.; Bækdal, T.A.; Düring, M.; Pietraszek, A.; Mortensen, L.S.; Jørgensen, H.; Flint, A. Liraglutide suppresses postprandial triglyceride and apolipoprotein B48 elevations after a fat-rich meal in patients with type 2 diabetes: A randomized, double-blind, placebo-controlled, cross-over trial. Diabet. Obes. Metab. 2013, 15, 1040–1048. [Google Scholar] [CrossRef]
- Weickert, M.O.; Roden, M.; Isken, F.; Hoffmann, D.; Nowotny, P.; Osterhoff, M.; Blaut, M.; Alpert, C.; Gögebakan, Ö.; Bumke-Vogt, C.; et al. Effects of supplemented isoenergetic diets differing in cereal fiber and protein content on insulin sensitivity in overweight humans. Am. J. Clin. Nutr. 2011, 94, 459–471. [Google Scholar] [CrossRef]
- Schutte, S.; Esser, D.; Hoevenaars, F.P.M.; Hooiveld, G.J.E.J.; Priebe, M.G.; Vonk, R.J.; Wopereis, S.; Afman, L.A. A 12-wk whole-grain wheat intervention protects against hepatic fat: The Graandioos study, a randomized trial in overweight subjects. Am. J. Clin. Nutr. 2018, 108, 1264–1274. [Google Scholar] [CrossRef]
- Smith, C.E.; Tucker, K.L. Health benefits of cereal fibre: A review of clinical trials. Nutr. Res. Rev. 2011, 24, 118–131. [Google Scholar] [CrossRef]
- Giacco, R.; Clemente, G.; Cipriano, D.; Luongo, D.; Viscovo, D.; Patti, L.; Di Marino, L.; Giacco, A.; Naviglio, D.; Bianchi, M.A.; et al. Effects of the regular consumption of wholemeal wheat foods on cardiovascular risk factors in healthy people. Nutr. Metab. Cardiovasc. Dis. 2010, 20, 186–194. [Google Scholar] [CrossRef] [PubMed]
- Jenkins, D.J.; Kendall, C.W.; Augustin, L.S.; Martini, M.C.; Axelsen, M.; Faulkner, D.; Vidgen, E.; Parker, T.; Lau, H.; Connelly, P.W.; et al. Effect of wheat bran on glycemic control and risk factors for cardiovascular disease in type 2 diabetes. Diabet. Care 2002, 25, 1522–1528. [Google Scholar] [CrossRef] [PubMed]
- Drummen, M.; Tischmann, L.; Gatta-Cherifi, B.; Adam, T.; Westerterp-Plantenga, M. Dietary Protein and Energy Balance in Relation to Obesity and Co-morbidities. Front. Endocrinol. 2018, 9, 443. [Google Scholar] [CrossRef] [PubMed]
- US Department of Agriculture. What We Eat in America. Nutrient Intakes from Food by Gender and Age. National Health and Nutrition Examination Survey 2009–2010. (NHANES). Available online: http://www.ars.usda.gov/Sp2userfiles/Place/12355000/Pdf/0910/Table_1_Nin_Gen_09.Pdf (accessed on 1 April 2019).
- Pedersen, A.N.; Christensen, T.; Matthiessen, J.; Knudsen, V.K.; Sørensen, M.R.; Biltoft-Jensen, A.P.; Hinsch, H.-J.; Ygil, K.H.; Kørup, K.; Saxholt, E. Danskernes Kostvaner 2011-2013; DTU Fødevareinstituttet, Danmarks Tekniske Universitet: Søborg, Denmark, 2015. [Google Scholar]
| Bread | Breakfast Cereals | Whey Protein | Malto-dextrin | |||
|---|---|---|---|---|---|---|
| High Fiber | Low Fiber | High Fiber | Low Fiber | |||
| Serving size (g) | 40 | 33 | 33 | 29 | 36 | 34 |
| Energy (kJ) | 371 | 359 | 455 | 443 | 527 | 527 |
| Available carbohydrate (g) | 11.0 | 15.5 | 18.6 | 21.6 | 0.4 | 31.0 |
| Starch (g) | 9.3 | 15.2 | 18.2 | 21.5 | - | - |
| Sugars (g) | 1.7 | 0.4 | 0.5 | 0.2 | - | - |
| Protein (g) | 6.1 | 3.3 | 3.9 | 3.2 | 30.1 | 0.2 |
| Fat (g) | 1.2 | 0.8 | 0.8 | 0.3 | 0.4 | 0.1 |
| Total dietary fiber (g) | 4.4 | 1.4 | 5.4 | 1.2 | 0 | 0 |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 16) | MD-HiFi (n = 17) | |
|---|---|---|---|---|
| Age, years 1 | 67 (60–69) | 65 (59–68) | 62 (58–68) | 64 (56–67) |
| Sex, n (male/female) | 9/6 | 7/10 | 8/8 | 7/10 |
| BMI, kg/m2 | 28.4 (4.1) | 29.6 (2.3) | 30.3 (4.5) | 29.1 (3.6) |
| Waist circumference, cm (male/female) | 105 (10)/91 (7) | 108 (8)/93 (6) | 105 (7)/100 (12) | 109 (8)/90 (7) |
| Drug treatment for dyslipidemia, n | 4 | 1 | 6 | 3 |
| Drug treatment for hypertension, n | 5 | 6 | 3 | 3 |
| Metabolic syndrome, n (%) | 10 (67) | 9 (53) | 8 (50) | 7 (41) |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 14) | MD-HiFi (n = 17) | p Value | |
|---|---|---|---|---|---|
| Bread (g/day) | 146.9 (28.0) | 174.6 (44.4) | 165.6 (33.1) | 166.5 (32.1) | 0.17 |
| Breakfast cereals (g/day) | 24.4 (21.2) | 34.5 (28.1) | 13.1 (16.2) | 33.7 (24.5) | 0.05 |
| Powder (sachets/day) | 1.83 (0.14) | 1.87 (0.24) | 1.96 (0.12) | 1.86 (0.16) | 0.25 |
| Energy (kJ/day) | 2941 (405) | 3078 (333) | 3017 (265) | 2971 (407) | 0.72 |
| Protein (g/day) | 72.4 (5.9) a | 86.7 (9.9) b | 18.1 (2.4) c | 29.3 (4.8) d | <0.01 |
| Fat (g/day) | 4.4 (0.6) a | 7.0 (1.0) b | 4.2 (0.6) a | 6.2 (1.0) c | <0.01 |
| Carbohydrate (g/day) | 88.4 (17.5) a | 68.4 (10.0) b | 147.7 (12.1) c | 121.9 (15.8) d | <0.01 |
| Dietary fiber (g/day) | 7.2 (1.3) a | 25.0 (3.2) b | 7.5 (1.0) a | 24.0 (4.4) b | <0.01 |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 16) | MD-HiFi (n = 17) | p Value, ∆ | |||||
|---|---|---|---|---|---|---|---|---|---|
| Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | ||
| Body weight (kg) 1 | 83.9 (14.6) | 83.8 (15.3) | 87.9 (13.2) | 88.5 (12.9) | 89.9 (14.0) | 90.5 (14.0) | 81.7 (15.1) | 82.3 (15.3) | 0.38 |
| Alkylresorcinols (nmol/L) 2 | 46.3 (30.4–56.6) | 27.2 (22.7–37.4) *,a | 32.8 (27.3–39.9) | 179.9 (84.2–246.5) *,b | 37.6 (24.7–62.7) | 40.8 (25.6–75.1) a | 46.7 (30.1–58.4) | 226.8 (150.4–280.3) *,b | <0.01 |
| Urinary carbamide excretion (mmol/24 h) 1 | 369 (103) | 576 (156) *,a | 311 (114) | 534 (144) *,a | 396 (150) | 368 (91) b | 315 (132) | 373 (175) *,b | <0.01 |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 16) | MD-HiFi (n = 16) | p Value, ∆ | |||||
|---|---|---|---|---|---|---|---|---|---|
| Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | ||
| Energy (kJ/day) | 8325 (2261) | 8230 (1603) | 9242 (2837) | 8827 (1787) | 8812 (1850) | 8890 (2141) | 8642 (2593) | 10016 (2226) * | 0.17 |
| Protein (g/day) | 79.1 (20.0) | 133.3 (17.1) *,a | 83.1 (15.9) | 149.7 (11.2) *,a | 85.9 (22.8) | 78.7 (14.8) b | 79.4 (18.0) | 94.9 (17.8) *c | <0.01 |
| Protein (E%) | 17 (3) | 28 (4) | 16 (3) | 30 (5) | 17 (3) | 15 (2) | 16 (3) | 16 (2) | |
| Carbohydrate (g/day) | 203.3 (84.9) | 184.6 (46.6) a, b | 254.2 (91.3) | 183.0 (54.5) *,a | 224.1 (66.7) | 254.0 (52.8) b, c | 217.8 (64.1) | 274.7 (62.1) *,c | <0.01 |
| Carbohydrate (E%) | 40 (8) | 38 (7) | 46 (9) | 35 (6) | 43 (10) | 49 (7) | 43 (7) | 47 (6) | |
| Fat (g/day) | 83.5 (25.4) | 66.8 (26.5) | 83.4 (34.9) | 73.6 (30.3) | 84.2 (27.3) | 76.0 (34.2) | 85.6 (36.6) | 86.5 (36.8) | 0.50 |
| Fat (E%) | 37 (7) | 29 (7) | 33 (8) | 30 (8) | 35 (8) | 31 (9) | 36 (7) | 31 (7) | |
| SFA (g/day) | 31.8 (13.6) | 28.0 (14.7) | 28.3 (14.3) | 27.8 (15.2) | 29.8 (12.3) | 27.6 (16.3) | 29.3 (14.1) | 31.0 (16.6) | 0.74 |
| Dietary fiber (g/day) | 20.2 (8.2) | 15.0 (4.6) *,a | 22.7 (4.9) | 33.7 (4.8)*,b | 23.4 (6.4) | 16.9 (5.6) *,a | 24.4 (8.8) | 35.6 (4.8) *,b | <0.01 |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 16) | MD-HiFi (n = 17) | Two-Factor ANOVA, p 6 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Protein Level | Fiber Level | Inter-Action | |
| TG iAUC (mmol/L × 360 min) 1 | 276 (132) | 223 (99) | 232 (95) | 208 (65) | 234 (108) | 292 (159) | 310 (217) | 274 (150) | 0.11 | 0.24 | 0.04 |
| TG tAUC (mmol/L × 360 min) 2 | 802 (560–1048) | 544 (424–681) *,a | 615 (565–907) | 601 (517–753) *,b | 790 (488–1053) | 816 (550–1105) b | 622 (491–1051) | 583 (508–892) b | <0.01 | 0.64 | <0.01 |
| ApoB–48 tAUC (mg/L × 360 min) 2 | 2800 (2066–3683) | 2144 (1424–2672) * | 4162 (2596–5459) 3 | 3555 (1915–5294) 3 | 3002 (1988–4408) | 2563 (1837–5261) | 3667 (2518–4324) | 2923 (2626–4118) | 0.14 | 0.59 | 0.04 |
| ApoB-100 tAUC (mg/dL × 360 min) 1 | 27317 (7496) | 25315 (9081) * | 28638 (5416) | 27305 (5426) | 26664 (10864) | 26393 (10987) | 24015 (10762) | 24784 (8336) | 0.06 | 0.26 | 0.95 |
| FFA tAUC (mmol/L × 360 min) 1 | 117 (22) | 117 (33) | 126 (31) | 125 (25) | 120 (34) | 119 (29) | 114 (35) | 125 (30) | 0.49 | 0.49 | 0.45 |
| Fasting TG (mmol/L) 2 | 1.63 (1.03–1.90) | 0.85 (0.76–1.11) *,a | 1.16 (1.06–1.51) | 1.05 (0.84–1.24) b | 1.31 (0.81–1.87) | 1.22 (0.98–2.47) b | 0.93 (0.79–1.25) | 0.90 (0.76–1.37) b | <0.01 | 0.17 | <0.01 |
| Fasting apoB-48 (mg/L) 2 | 4.2 (3.0–5.3) | 2.8 (1.7–3.7) *,a | 6.9 (3.8–10.8) | 6.4 (3.0–10.4) a, b | 6.4 (3.5–7.8) | 4.5 (3.1–11.3) b | 6.7 (5.5–7.8) | 5.5 (3.8–7.3) a, b | 0.06 | 0.59 | <0.01 |
| Fasting apoB-100 (mg/dL) 1 | 77.5 (19.7) | 69.9 (23.8) *,a | 83.8 (15.6) | 78.5 (15.9) a, b | 74.4 (30.4) | 75.2 (32.0) a, b | 64.1 (35.0) | 70.9 (23.2) *,b | <0.01 | 0.16 | 0.66 |
| Fasting FFA (mmol/L) 1 | 0.39 (0.12) | 0.39 (0.15) | 0.44 (0.15) | 0.41 (0.12) | 0.42 (0.09) | 0.37 (0.12) | 0.36 (0.16) | 0.39 (0.12) | 0.89 | 0.39 | 0.17 |
| Total cholesterol (mmol/L) 1 | 5.2 (0.8) | 5.0 (0.8) *,a | 5.5 (1.0) | 5.4 (1.0) a | 5.3 (1.3) | 5.3 (1.3) a, b | 5.1 (1.1) | 5.4 (1.0) *,b | <0.01 | 0.04 | 0.78 |
| LDL (mmol/L) 2 | 3.4 (2.5–3.6) | 3.3 (2.2–3.8) | 3.7 (3.3–4.0) | 3.4 (3.2–3.9) | 3.6 (2.3–3.9) | 3.3 (1.9–3.7) 4 | 2.9 (2.3–3.6) | 3.2 (2.7–3.9) * | 0.09 | 0.08 | 0.07 |
| HDL (mmol/L) 2 | 1.3 (1.1–1.6) | 1.4 (1.2–1.9) * | 1.3 (1.2–1.6) | 1.3 (1.2–1.5) | 1.2 (1.1–1.5) | 1.3 (1.0–1.6) | 1.5 (1.3–1.7) | 1.6 (1.3–2.0) * | 0.85 | 0.84 | 0.08 |
| LPL activity (μmol FFA/h/g) 2 | 1.9 (1.5–2.2) 5 | 1.6 (1.3–2.7) 5 | 2.3 (1.2–2.6) 5 | 2.1 (1.0–4.0) 5 | 1.6 (1.1–2.0) 5 | 1.7 (0.9–2.4) 5 | 1.3 (0.9–1.8) 3 | 1.5 (0.8–2.0) 3 | 0.80 | 0.79 | 0.55 |
| WP-LoFi (n = 15) | WP-HiFi (n = 17) | MD-LoFi (n = 16) | MD-HiFi (n = 17) | Two-factor ANOVA, p3 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Baseline | Week 12 | Protein Level | Fiber Level | Inter-Action | |
| Glucose iAUC (mmol/L × 360 min) 1 | 54 (180) | 49 (78) | 45 (107) | 105 (138) | 171 (239) | 65 (180) * | 84 (231) | 105 (153) | 0.13 | 0.04 | 0.50 |
| Insulin iAUC (pmol/L × 360 min) 2 | 67,996 (53,001–90,413) | 68,804 (45,510–88,895) | 64,370 (52,105–77,430) | 61,526 (48,408–79,128) | 66,701 (383,75–117,323) | 62,495 (44,173–114,925) | 61,093 (42,746–82,741) | 48,267 (39,350–81,683) | 0.34 | 0.21 | 0.74 |
| Glucagon iAUC (pg/mL × 360 min) 1 | 11,671 (4430) | 12,691 (2427) | 13,958 (6855) | 11,477 (5983) * | 3567 (3625) | 4389 (3069) | 5901 (3046) | 5713 (2683) | 0.31 | 0.04 | 0.24 |
| Fasting glucose (mmol/L) 1 | 5.6 (0.3) | 5.6 (0.4) | 5.5 (0.6) | 5.7 (0.6) * | 5.6 (0.3) | 5.8 (0.4) | 5.5 (0.4) | 5.6 (0.6) | 0.52 | 0.39 | 0.20 |
| Fasting insulin (pmol/L) 2 | 50 (36–75) | 47 (35–69) | 44 (31–48) | 43 (30–49) | 45 (32–69) | 51 (41–82) | 31 (24–56) | 31 (23–46) | 0.48 | 0.68 | 0.26 |
| Fasting glucagon (pmol/mL) 1 | 64 (16) | 64 (16) | 63 (17) | 66 (20) | 63 (16) | 64 (17) | 61 (17) | 65 (16) | 0.90 | 0.31 | 0.89 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rakvaag, E.; Fuglsang-Nielsen, R.; Bach Knudsen, K.E.; Landberg, R.; Johannesson Hjelholt, A.; Søndergaard, E.; Hermansen, K.; Gregersen, S. Whey Protein Combined with Low Dietary Fiber Improves Lipid Profile in Subjects with Abdominal Obesity: A Randomized, Controlled Trial. Nutrients 2019, 11, 2091. https://doi.org/10.3390/nu11092091
Rakvaag E, Fuglsang-Nielsen R, Bach Knudsen KE, Landberg R, Johannesson Hjelholt A, Søndergaard E, Hermansen K, Gregersen S. Whey Protein Combined with Low Dietary Fiber Improves Lipid Profile in Subjects with Abdominal Obesity: A Randomized, Controlled Trial. Nutrients. 2019; 11(9):2091. https://doi.org/10.3390/nu11092091
Chicago/Turabian StyleRakvaag, Elin, Rasmus Fuglsang-Nielsen, Knud Erik Bach Knudsen, Rikard Landberg, Astrid Johannesson Hjelholt, Esben Søndergaard, Kjeld Hermansen, and Søren Gregersen. 2019. "Whey Protein Combined with Low Dietary Fiber Improves Lipid Profile in Subjects with Abdominal Obesity: A Randomized, Controlled Trial" Nutrients 11, no. 9: 2091. https://doi.org/10.3390/nu11092091
APA StyleRakvaag, E., Fuglsang-Nielsen, R., Bach Knudsen, K. E., Landberg, R., Johannesson Hjelholt, A., Søndergaard, E., Hermansen, K., & Gregersen, S. (2019). Whey Protein Combined with Low Dietary Fiber Improves Lipid Profile in Subjects with Abdominal Obesity: A Randomized, Controlled Trial. Nutrients, 11(9), 2091. https://doi.org/10.3390/nu11092091






