Validity of a Portable Breath Analyser (AIRE) for the Assessment of Lactose Malabsorption
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Procedure
2.3. Breath Analysis
2.4. Statistical Analysis
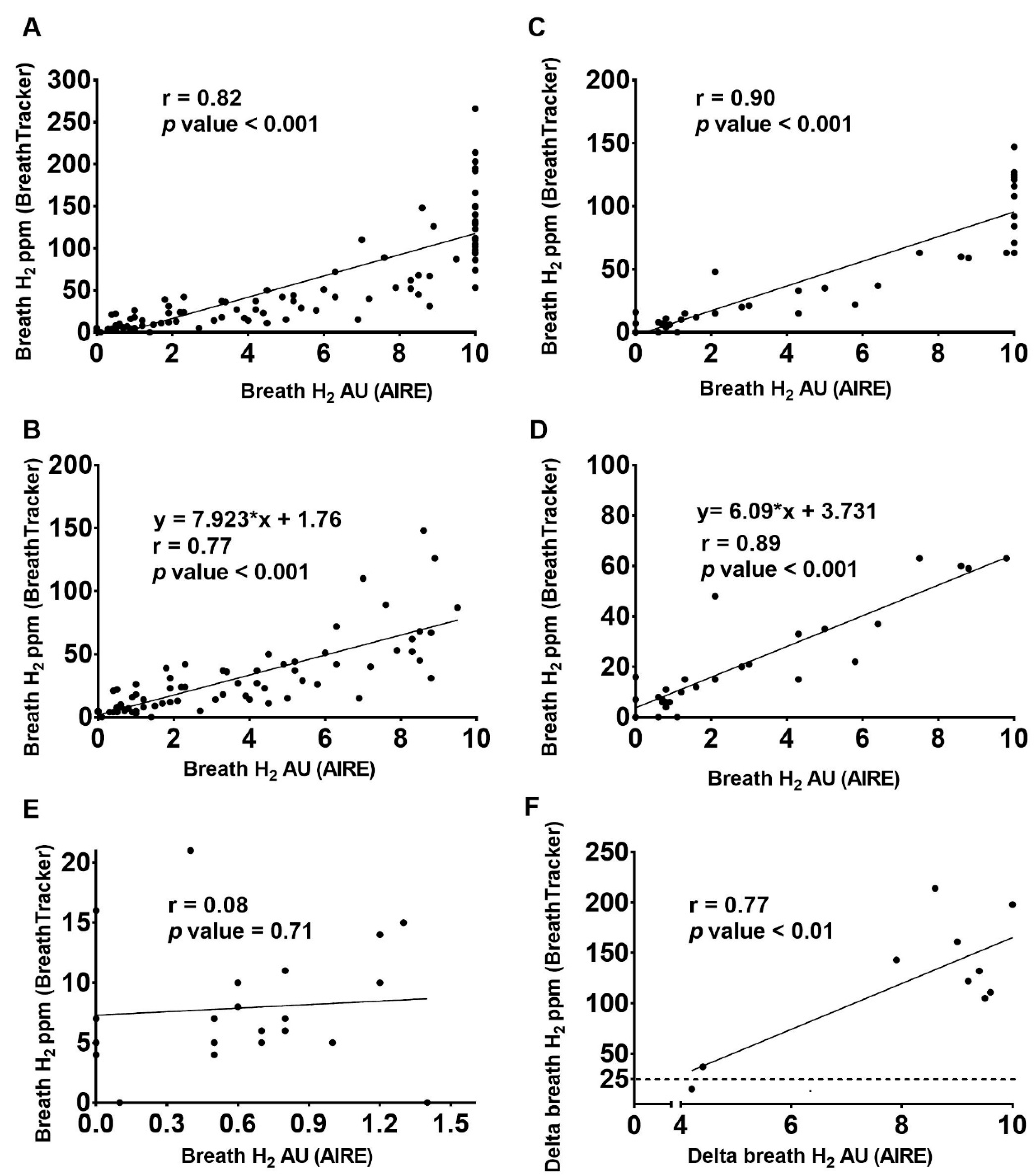
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lomer, M.C.E. Review article: The aetiology, diagnosis, mechanisms and clinical evidence for food intolerance. Aliment. Pharmacol. Ther. 2015, 41, 262–275. [Google Scholar] [CrossRef] [PubMed]
- Barrett, J.S.; Gearry, R.B.; Muir, J.G.; Irving, P.M.; Rose, R.; Rosella, O.; Haines, M.L.; Shepherd, S.J.; Gibson, P.R. Dietary poorly absorbed, short-chain carbohydrates increase delivery of water and fermentable substrates to the proximal colon. Aliment. Pharmacol. Ther. 2010, 31, 874–882. [Google Scholar] [CrossRef] [PubMed]
- Misselwitz, B.; Pohl, D.; Frühauf, H.; Fried, M.; Vavricka, S.R.; Fox, M. Lactose malabsorption and intolerance: Pathogenesis, diagnosis and treatment. United Eur. Gastroenterol. J. 2013, 1, 151–159. [Google Scholar] [CrossRef] [PubMed]
- Enattah, N.S.; Sahi, T.; Savilahti, E.; Terwilliger, J.D.; Peltonen, L.; Järvelä, I. Identification of a variant associated with adult-type hypolactasia. Nat. Genet. 2002, 30, 233–237. [Google Scholar] [CrossRef] [PubMed]
- Fassio, F.; Facioni, M.S.; Guagnini, F. Lactose Maldigestion, Malabsorption, and Intolerance: A Comprehensive Review with a Focus on Current Management and Future Perspectives. Nutrients 2018, 10, 1599. [Google Scholar] [CrossRef] [PubMed]
- Usai-Satta, P.; Scarpa, M.; Oppia, F.; Cabras, F. Lactose malabsorption and intolerance: What should be the best clinical management? World J. Gastrointest. Pharmacol. Ther. 2012, 3, 29–33. [Google Scholar] [CrossRef]
- Deng, Y.; Misselwitz, B.; Dai, N.; Fox, M. Lactose Intolerance in Adults: Biological Mechanism and Dietary Management. Nutrients 2015, 7, 8020–8035. [Google Scholar] [CrossRef]
- Mattar, R.; Mazo, D.F.D.C.; Carrilho, F.J. Lactose intolerance: Diagnosis, genetic, and clinical factors. Clin. Exp. Gastroenterol. 2012, 201, 113–121. [Google Scholar] [CrossRef]
- Suchy, F.J.; Brannon, P.M.; Carpenter, T.O.; Fernandez, J.R.; Gilsanz, V.; Gould, J.B.; Hall, K.; Hui, S.L.; Lupton, J.; Mennella, J.; et al. NIH consensus development conference statement: Lactose intolerance and health. NIH Consens. State Sci. Statements 2010, 27, 1–27. [Google Scholar]
- Gasbarrini, A.; Corazza, G.R.; Gasbarrini, G.; Montalto, M.; Di Stefano, M.B.G.; Basilisco, G.; Parodi, A.; Satta, P.; Vernia, P.; Ananis, C.; et al. H2-breath testing for carbohydrate malabsorption. Aliment. Pharmacol. Ther. 2009, 29, 1–49. [Google Scholar] [CrossRef]
- Gibson, P.R. Food intolerance in functional bowel disorders. J. Gastroenterol. Hepatol. 2011, 26, 128–131. [Google Scholar] [CrossRef] [PubMed]
- Casellas, F.; Malagelada, J.R. Applicability of short hydrogen breath test for screening of lactose malabsorption. Dig. Dis. Sci. 2003, 48, 1333–1338. [Google Scholar] [CrossRef] [PubMed]
- Wong, F.H.; Yeung, C.Y.; Fung, K.W.; Tam, A.Y. Breath Hydrogen (H2) Analysis in Southern Chinese Children and Infants by Gas Chromatography and a Novel Automatic Sampling System. Singap. Med. J. 1996, 37, 72–81. [Google Scholar]
- Fox, N.J. Personal health technologies, micropolitics and resistance: A new materialist analysis. Health 2017, 21, 136–153. [Google Scholar] [CrossRef] [PubMed]
- Wen, D.; Zhang, X.; Liu, X.; Lei, J. Evaluating the Consistency of Current Mainstream Wearable Devices in Health Monitoring: A Comparison Under Free-Living Conditions. J. Med. Internet Res. 2017, 19, 68. [Google Scholar] [CrossRef] [PubMed]
- Henriksen, A.; Haugen Mikalsen, M.; Woldaregay, A.Z.; Muzny, M.; Hartvigsen, G.; Hopstock, L.A.; Grimsgaard, S. Using Fitness Trackers and Smartwatches to Measure Physical Activity in Research: Analysis of Consumer Wrist-Worn Wearables. J. Med. Internet Res. 2018, 20, 110. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, F.L.; Marling, C.R.; Bunescu, R.C. The Promise and Perils of Wearable Physiological Sensors for Diabetes Management. J. Diabetes Sci. Technol. 2018, 12, 587–591. [Google Scholar] [CrossRef]
- FoodMarble Launches World’s First Personal Digestive Tracker. Available online: https://www.prnewswire.com/news-releases/foodmarble-launches-worlds-first-personal-digestive-tracker-300759518.html (accessed on 8 April 2019).
- FoodMarble. Available online: https://www.foodmarble.com/ (accessed on 16 February 2019).
- Peuhkuri, K.; Poussa, T.; Korpela, R. Comparison of a portable breath hydrogen analyser (Micro H2) with a Quintron MicroLyzer in measuring lactose maldigestion, and the evaluation of a Micro H2 for diagnosing hypolactasia. Scand. J. Clin. Lab. Investig. 2009. [Google Scholar] [CrossRef]
- Lee, W.; Davidson, G.; Moore, D.; Butler, R. Analysis of the breath hydrogen test for carbohydrate malabsorption: Validation of a pocket-sized breath test analyser. J. Paediatr. Child Health 2000, 36, 340–342. [Google Scholar] [CrossRef]
- Boyd, R.; Leigh, B.; Stuart, P. Capillary versus venous bedside blood glucose estimations. Emerg. Med. J. 2005, 22, 177–179. [Google Scholar] [CrossRef]
- de Villiers, F.P. Standarized milk tolerance test. J. Clin. Gastroenterol. 1987, 9, 320–323. [Google Scholar] [CrossRef] [PubMed]
- Ghoshal, U.C.; Kumar, S.; Misra, A.; Mittal, B. Lactose malabsorption diagnosed by 50-g dose is inferior to assess clinical intolerance and to predict response to milk withdrawal than 25-g dose in an endemic area. J. Gastroenterol. Hepatol. 2013, 28, 1462–1468. [Google Scholar] [CrossRef] [PubMed]
- QuinTron Catalogue and Information. Available online: http://www.quintron-eu.com/qt02444_catalog.pdf (accessed on 20 May 2019).
- Celiac Disease Foundation Glutenostics Launches Gluten Detective, the First At-Home Gluten Consumption Monitoring Test Celiac Disease Foundation. Available online: https://celiac.org/about-the-foundation/featured-news/2017/10/glutenostics-launches-gluten-detective-first-home-gluten-consumption-monitoring-test/ (accessed on 4 July 2019).
- Jenkins, D.J.A.; Kendall, C.W.C.; Vuksan, V. Inulin, Oligofructose and Intestinal Function. J. Nutr. 1999, 129, 1431–1433. [Google Scholar] [CrossRef] [PubMed]
- Briet, F.; Pochart, P.; Marteau, P.; Flourie, B.; Arrigoni, E.; Rambaud, J.C. Improved clinical tolerance to chronic lactose ingestion in subjects with lactose intolerance: A placebo effect? Gut 1997, 41, 632–635. [Google Scholar] [CrossRef] [PubMed]
- Mcintosh, K.; Reed, D.E.; Schneider, T.; Dang, F.; Keshteli, A.H.; De Palma, G.; Madsen, K.; Bercik, P.; Vanner, S. FODMAPs alter symptoms and the metabolome of patients with IBS: A randomised controlled trial. Neurogastroenterology 2015, 66, 1241–1251. [Google Scholar] [CrossRef] [PubMed]
- Staudacher, H.M.; Lomer, M.C.E.; Anderson, J.L.; Barrett, J.S.; Muir, J.G.; Irving, P.M.; Whelan, K. Fermentable Carbohydrate Restriction Reduces Luminal Bifidobacteria and Gastrointestinal Symptoms in Patients with Irritable Bowel Syndrome. J. Nutr. 2012, 142, 1510–1518. [Google Scholar] [CrossRef] [PubMed]
- Zhan, Y.L.; Zhan, Y.A.; Dai, S.X. Is a low FODMAP diet beneficial for patients with inflammatory bowel disease? A meta-analysis and systematic review. Clin. Nutr. 2018, 37, 123–129. [Google Scholar] [CrossRef] [PubMed]
- Testa, A.; Imperatore, N.; Rispo, A.; Rea, M.; Tortora, R.; Nardone, O.M.; Lucci, L.; Accarino, G.; Caporaso, N.; Castiglione, F. Beyond Irritable Bowel Syndrome: The Efficacy of the Low Fodmap Diet for Improving Symptoms in Inflammatory Bowel Diseases and Celiac Disease. Dig. Dis. 2018, 36, 271–280. [Google Scholar] [CrossRef]
- Catassi, G.; Lionetti, E.; Gatti, S.; Catassi, C. The Low FODMAP Diet: Many Question Marks for a Catchy Acronym. Nutrients 2017, 9, 292. [Google Scholar] [CrossRef]
- Nanayakkara, W.S.; Skidmore, P.M.; O’Brien, L.; Wilkinson, T.J.; Gearry, R.B. Efficacy of the low FODMAP diet for treating irritable bowel syndrome: The evidence to date. Clin. Exp. Gastroenterol. 2016, 9, 131–142. [Google Scholar] [CrossRef]
| No. of H2 Measurements | R2 | Slope (Mean ± SD) | Pearson Correlation (r) | p Value | |
|---|---|---|---|---|---|
| Lactose challenge 2 (n = 12) | |||||
| All readings including AIRE score = 10 | 96 | 0.67 | 12.64 ± 0.90 | 0.82 | <0.001 |
| Without AIRE score = 10 | 71 | 0.60 | 7.92 ± 0.77 | 0.77 | <0.001 |
| Milk challenge 3 (n = 7) | |||||
| All readings including AIRE score = 10 | 40 | 0.81 | 9.79 ± 0.76 | 0.90 | <0.001 |
| Without AIRE score = 10 | 29 | 0.80 | 6.09 ± 0.57 | 0.89 | <0.001 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shrestha, A.; Prodhan, U.K.; Mitchell, S.M.; Sharma, P.; Barnett, M.P.G.; Milan, A.M.; Cameron-Smith, D. Validity of a Portable Breath Analyser (AIRE) for the Assessment of Lactose Malabsorption. Nutrients 2019, 11, 1636. https://doi.org/10.3390/nu11071636
Shrestha A, Prodhan UK, Mitchell SM, Sharma P, Barnett MPG, Milan AM, Cameron-Smith D. Validity of a Portable Breath Analyser (AIRE) for the Assessment of Lactose Malabsorption. Nutrients. 2019; 11(7):1636. https://doi.org/10.3390/nu11071636
Chicago/Turabian StyleShrestha, Aahana, Utpal K. Prodhan, Sarah M. Mitchell, Pankaja Sharma, Matthew P.G. Barnett, Amber M. Milan, and David Cameron-Smith. 2019. "Validity of a Portable Breath Analyser (AIRE) for the Assessment of Lactose Malabsorption" Nutrients 11, no. 7: 1636. https://doi.org/10.3390/nu11071636
APA StyleShrestha, A., Prodhan, U. K., Mitchell, S. M., Sharma, P., Barnett, M. P. G., Milan, A. M., & Cameron-Smith, D. (2019). Validity of a Portable Breath Analyser (AIRE) for the Assessment of Lactose Malabsorption. Nutrients, 11(7), 1636. https://doi.org/10.3390/nu11071636







