Effect of High Fiber Cereal Intake on Satiety and Gastrointestinal Symptoms during Ramadan
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Research Participants
2.3. Inclusion and Exclusion Criteria
2.4. Research Procedures
2.5. Anthropometric Measurements
2.6. Diet and Physical Activity Assessment
2.7. Gastrointestinal Symptom and Satiety Questionnaires
2.8. Biochemical Parameters
2.9. Statistical Analysis
3. Results
3.1. Characteristics of the Study Population
3.2. Gastrointestinal Symptoms
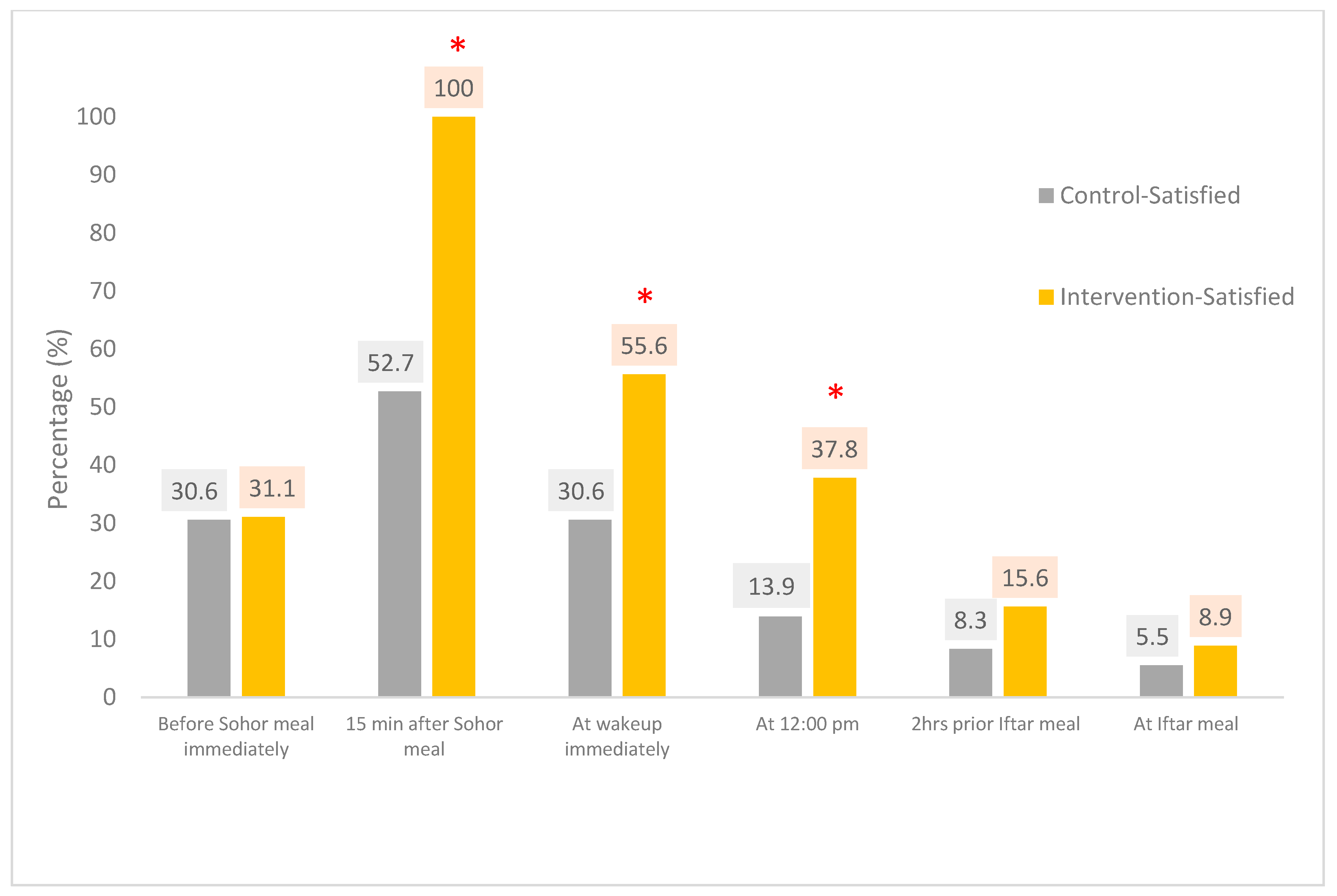
3.3. Satiety
3.4. Diet Records
3.5. Biochemical Measurements
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Jones, J.M. CODEX-aligned dietary fiber definitions help to bridge the ‘fiber gap’. Nutr. J. 2014, 13, 34. [Google Scholar] [CrossRef]
- Joint FAO/WHO Food Standards Programme. Secretariat of the CODEX Alimentarius Commission: CODEX Alimentarius (CODEX) Guidelines on Nutrition Labeling CAC/GL 2–1985 as Last Amended 2010; FAO: Rome, Italy, 2010. [Google Scholar]
- Bureau of Nutritional Sciences Food Directorate, Health Products and Food Branch, Health Canada. Policy for Labelling and Advertising of Dietary fibre-Containing Food. 2013. Available online: http://www.hc-sc.gc.ca (accessed on 22 August 2018).
- American Association of Cereal Chemists Fiber Committee. Dietary Fiber Definition Committee: Definition of dietary fiber: Report of the Dietary Fiber Definition Committee to the Board of Directors of the American Association of Cereal Chemists. Cereal Foods World 2001, 46, 112–126. [Google Scholar]
- Pereira, M.A.; Ludwig, D.S. Dietary fiber and body-weight regulation: Observations and mechanisms. Pediatr. Clin. N. Am. 2001, 48, 969–980. [Google Scholar] [CrossRef]
- Jenkins, D.; Wolever, T.; Leeds, A.R.; Gassull, M.A.; Haisman, P.; Dilawari, J.; Goff, D.V.; Metz, G.L.; Alberti, K. Dietary fibres, fibre analogues, and glucose tolerance: Importance of viscosity. Br. Med. J. 1978, 1, 1392–1394. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A. Energy density, palatability, and satiety: Implications for weight control. Nutr. Rev. 1998, 56, 347–353. [Google Scholar] [CrossRef]
- Sakata, T. A very-low-calorie conventional Japanese diet: Its implications for prevention of obesity. Obes. Res. 1995, 3, 233s–239s. [Google Scholar] [CrossRef]
- Burton-Freeman, B. Dietary fiber and energy regulation. J. Nutr. 2000, 130, 272S–275S. [Google Scholar] [CrossRef]
- Toma, R.; Curtis, D. Ready-to-eat cereals: Role in a balanced diet. Cereal Foods World 1989, 34, 387–390. [Google Scholar]
- McKevith, B. Nutritional aspects of cereals. Nutr. Bull. 2004, 29, 111–142. [Google Scholar] [CrossRef]
- McKevith, B.; Jarzebowska, A. The role of breakfast cereals in the UK diet: Headline results from the National Diet and Nutrition Survey (NDNS) year 1. Nutr. Bull. 2010, 35, 314–319. [Google Scholar] [CrossRef]
- Council of National Health and Medical Research. Australian Dietary Guidelines; NHMRC: Canberra ACT, Australia, 2013.
- Williams, P.G. The Benefits of Breakfast Cereal Consumption: A Systematic Review of the Evidence Base. Adv. Nutr. 2014, 5, 636S–673S. [Google Scholar] [CrossRef] [PubMed]
- Nomani, M.; Hallak, M.; Nomani, S.; Siddiqui, I. Changes in blood urea and glucose and their association with energy-containing nutrients in men on hypocaloric diets during Ramadan fasting. Am. J. Clin. Nutr. 1989, 49, 1141–1145. [Google Scholar] [CrossRef] [PubMed]
- Qujeq, D.; Bijani, K.; Kalavi, K.; Mohiti, J.; Aliakbarpour, H. Effects of Ramadan fasting on serum low-density and high-density lipoprotein-cholesterol concentrations. Ann. Saudi Med. 2002, 22, 297–299. [Google Scholar] [CrossRef] [PubMed]
- Darvish, M.S. Relative frequency of minor digestive symptoms in healthy fasting Muslems and their relation to dietary pattern. SID 2002, 45, 59–66. [Google Scholar]
- Noordzij, M.; Tripepi, G.; Dekker, F.W.; Zoccali, C.; Tanck, M.W.; Jager, K.J. Sample size calculations: Basic principles and common pitfalls. Nephrol. Dial. Transplant. 2010, 25, 1388–1393. [Google Scholar] [CrossRef] [PubMed]
- Holt, S.H.A.; Miller, J.C.B.; Petocz, P.; Farmakalidis, E. A Satiety Index of Common Foods. Eur. J. Clin. Nutr. 1995, 49, 675–690. [Google Scholar] [PubMed]
- Ludwig, D.S.; Pereira, M.A.; Kroenke, C.H.; Hilner, J.E.; Van Horn, L.; Slattery, M.L.; Jacobs, D.R., Jr. Dietary fiber, weight gain, and cardiovascular disease risk factors in young adults. JAMA 1999, 282, 1539–1546. [Google Scholar] [CrossRef] [PubMed]
- Brownlee, I.A.; Chater, P.I.; Pearson, J.P.; Wilcox, M.D. Dietary fibre and weight loss: Where are we now? Food Hydrocoll. 2017, 68, 186–191. [Google Scholar] [CrossRef]
- Bertoia, M.L.; Mukamal, K.J.; Cahill, L.E.; Hou, T.; Ludwig, D.S.; Mozaffarian, D.; Willett, W.C.; Hu, F.B.; Rimm, E.B. Changes in intake of fruits and vegetables and weight change in United States men and women followed for up to 24 years: Analysis from three prospective cohort studies. PLoS Med. 2015, 12, e1001878. [Google Scholar] [CrossRef] [PubMed]
- Berry, S.E.; Mulla, U.Z.; Chowienczyk, P.J.; Sanders, T.A. Increased potassium intake from fruit and vegetables or supplements does not lower blood pressure or improve vascular function in UK men and women with early hypertension: A randomised controlled trial. Br. J. Nutr. 2010, 104, 1839–1847. [Google Scholar] [CrossRef]
- Andersson, A.; Tengblad, S.; Karlstrom, B.; Kamal-Eldin, A.; Landberg, R.; Basu, S.; Aman, P.; Vessby, B. Whole-grain foods do not affect insulin sensitivity or markers of lipid peroxidation and inflammation in healthy, moderately overweight subjects. J. Nutr. 2007, 137, 1401–1407. [Google Scholar] [CrossRef] [PubMed]
- Hajihashemi, P.; Azadbakht, L.; Hashemipor, M.; Kelishadi, R.; Esmaillzadeh, A. Whole-grain intake favorably affects markers of systemic inflammation in obese children: A randomized controlled crossover clinical trial. Mol. Nutr. Food Res. 2014, 58, 1301–1308. [Google Scholar] [CrossRef] [PubMed]
- Harris Jackson, K.; West, S.G.; Vanden Heuvel, J.P.; Jonnalagadda, S.S.; Ross, A.B.; Hill, A.M.; Grieger, J.A.; Lemieux, S.K.; Kris-Etherton, P.M. Effects of whole and refined grains in a weight-loss diet on markers of metabolic syndrome in individuals with increased waist circumference: A randomized controlled-feeding trial. Am. J. Clin. Nutr. 2014, 100, 577–586. [Google Scholar] [CrossRef] [PubMed]
- Mueller-Cunningham, W.M.; Quintana, R.; Kasim-Karakas, S.E. An ad libitum, very low-fat diet results in weight loss and changes in nutrient intakes in postmenopausal women. J. Am. Diet. Assoc. 2003, 103, 1600–1606. [Google Scholar] [CrossRef] [PubMed]
- Birketvedt, G.; Aaseth, J.; Florholmen, J.; Ryttig, K. Long-term effect of fibre supplement and reduced energy intake on body weight and blood lipids in overweight subjects. Acta Med. 2000, 43, 129–132. [Google Scholar]
- Liu, S.; Willett, W.C.; Manson, J.E.; Hu, F.B.; Rosner, B.; Colditz, G. Relation between changes in intakes of dietary fiber and grain products and changes in weight and development of obesity among middle-aged women. Am. J. Clin. Nutr. 2003, 78, 920–927. [Google Scholar] [CrossRef] [PubMed]
- Heaton, K. Food fibre as an obstacle to energy intake. Lancet 1973, 302, 1418–1421. [Google Scholar] [CrossRef]
- Maki, K.C.; Beiseigel, J.M.; Jonnalagadda, S.S.; Gugger, C.K.; Reeves, M.S.; Farmer, M.V.; Kaden, V.N.; Rains, T.M. Whole-grain ready-to-eat oat cereal, as part of a dietary program for weight loss, reduces low-density lipoprotein cholesterol in adults with overweight and obesity more than a dietary program including low-fiber control foods. J. Am. Diet. Assoc. 2010, 110, 205–214. [Google Scholar] [CrossRef]
- Schlundt, D.G.; Hill, J.O.; Sbrocco, T.; Pope-Cordle, J.; Sharp, T. The role of breakfast in the treatment of obesity: A randomized clinical trial. Am. J. Clin. Nutr. 1992, 55, 645–651. [Google Scholar] [CrossRef] [PubMed]
- Saltzman, E.; Moriguti, J.C.; Das, S.K.; Corrales, A.; Fuss, P.; Greenberg, A.S.; Roberts, S.B. Effects of a cereal rich in soluble fiber on body composition and dietary compliance during consumption of a hypocaloric diet. J. Am. Coll. Nutr. 2001, 20, 50–57. [Google Scholar] [CrossRef]
- Melanson, K.J.; Angelopoulos, T.J.; Nguyen, V.T.; Martini, M.; Zukley, L.; Lowndes, J.; Dube, T.J.; Fiutem, J.J.; Yount, B.W.; Rippe, J.M. Consumption of whole-grain cereals during weight loss: Effects on dietary quality, dietary fiber, magnesium, vitamin B-6, and obesity. J. Am. Diet. Assoc. 2006, 106, 1380–1388. [Google Scholar] [CrossRef] [PubMed]
- Haouari-Oukerro, F.; Ben-Attia, M.; Kaâbachi, N.; Haouari, M. Ramadan fasting influences on food intake consumption, sleep schedule, body weight and some plasma parameters in healthy fasting volunteers. Afr. J. Biotechnol. 2013, 12, 3327–3332. [Google Scholar]
- Beltaifa, L.; Bouguerra, R.; Ben, C.S.; Jabrane, H.; El-Khadhi, A.; Ben, M.R.; Doghri, T. Food intake, and anthropometrical and biological parameters in adult Tunisians during fasting at Ramadan. East Mediterr. Health J. 2002, 8, 603–611. [Google Scholar] [PubMed]
- Slavin, J.L. Dietary fiber and body weight. Nutrition 2005, 21, 411–418. [Google Scholar] [CrossRef] [PubMed]
- de Vries, J.; Miller, P.E.; Verbeke, K. Effects of cereal fiber on bowel function: A systematic review of intervention trials. World J. Gastroenterol. 2015, 21, 8952. [Google Scholar] [CrossRef] [PubMed]
- Keshteli, A.; Sadeghpour, S.; Feizi, A.; Boyce, P.; Adibi, P. Evaluation of self-perceived changes in gastrointestinal symptoms during Ramadan fasting. J. Relig. Health 2017, 56, 1620–1627. [Google Scholar] [CrossRef]
- Baig, A.; Baig, S.; Ghoto, M.A.; Baloch, M.A. Dietary intake during fasting in the month of Ramadan. N. Y. Sci. 2014, 7, 15–18. [Google Scholar]
- Saris, W.H. Glycemic carbohydrate and body weight regulation. Nutr. Rev. 2003, 61, S10–S16. [Google Scholar] [CrossRef]
- Norouzy, A.; Salehi, M.; Philippou, E.; Arabi, H.; Shiva, F.; Mehrnoosh, S.; Mohajeri, S.; Mohajeri, S.R.; Motaghedi Larijani, A.; Nematy, M. Effect of fasting in Ramadan on body composition and nutritional intake: A prospective study. J. Hum. Nutr. Diet. 2013, 26, 97–104. [Google Scholar] [CrossRef]
- Chen, J.; He, J.; Wildman, R.; Reynolds, K.; Streiffer, R.; Whelton, P. A randomized controlled trial of dietary fiber intake on serum lipids. Eur. J. Clin. Nutr. 2006, 60, 62. [Google Scholar] [CrossRef]
- Zhou, Q.; Wu, J.; Tang, J.; Wang, J.-J.; Lu, C.-H.; Wang, P.-X. Beneficial effect of higher dietary fiber intake on plasma HDL-C and TC/HDL-C ratio among Chinese rural-to-urban migrant workers. Int. J. Environ. Res. Public Health 2015, 12, 4726–4738. [Google Scholar] [CrossRef] [PubMed]
- Streppel, M.T.; Ocké, M.C.; Boshuizen, H.C.; Kok, F.J.; Kromhout, D. Dietary fiber intake in relation to coronary heart disease and all-cause mortality over 40 y: The Zutphen Study. Am. J. Clin. Nutr. 2008, 88, 1119–1125. [Google Scholar] [CrossRef] [PubMed]
- Schulze, M.B.; Liu, S.; Rimm, E.B.; Manson, J.E.; Willett, W.C.; Hu, F.B. Glycemic index, glycemic load, and dietary fiber intake and incidence of type 2 diabetes in younger and middle-aged women. Am. J. Clin. Nutr. 2004, 80, 348–356. [Google Scholar] [CrossRef] [PubMed]
| Control (n = 36, 31 Females) | Intervention (n = 45, 45 Females) | Overall p-Value | |||||
|---|---|---|---|---|---|---|---|
| Age (Year) | 21.5 ± 1.9 | 22.6 ± 5.7 | 0.289 | ||||
| Height (cm) | 161.1 ± 8.5 | 161.3 ± 5.6 | 0.888 | ||||
| Baseline M ± SD | Endpoint M ± SD | p-Value | Baseline M ± SD | Endpoint M ± SD | p-Value | ||
| Weight (kg) | 60.5 ± 11.5 | 59.9 ± 11.2 | 0.002 | 62.5 ±11.1 | 62.0 ± 11.1 | 0.003 | 0.667 |
| BMI (kg/cm²) | 23.2 ± 3.6 | 23.0 ± 3.6 | 0.002 | 24.0 ± 3.9 | 23.8 ± 3.9 | 0.004 | 0.890 |
| WC (cm) | 73.8 ± 9.0 | 74.9 ± 8.4 | 0.053 | 75.1 ± 8.0 | 75.6 ± 8.7 | 0.221 | 0.391 |
| % Body fat | 31.0 ±8.9 | 30.4 ± 9.0 | 0.059 | 34.0 ± 7.1 | 34.1 ± 7.3 | 0.808 | 0.141 |
| Gastrointestinal Symptoms | Response/Frequency | Control (n = 36) Count (%) | Intervention (n = 45) Count (%) | p-Value |
|---|---|---|---|---|
| Bowel habits increase | Yes | 9 (25) | 22 (49) | 0.029 |
| No | 27 (75) | 23 (51) | ||
| Constipation | Yes | 3 (8) | 2 (4) | 0.417 |
| Bowel movement frequency | ≤1/week | 6 (16.6) | 4 (9) | 0.294 |
| 2/week | 8 (22.2) | 12 (27) | ||
| ≥3/week | 22 (61.1) | 29 (64) | ||
| Vomiting frequency | None | 23 (64) | 34 (75.5) | 0.467 |
| 1–2/week | 13 (36) | 11 (24.5) | ||
| Bloating frequency | ≤1/week | 18 (50) | 28 (62.2) | <0.001 |
| 2/week | 13 (36) | 12 (26.6) | ||
| ≥3/week | 5 (14) | 5 (11.1) | ||
| Heartburn frequency | ≤1/week | 23 (64) | 29 (64.4) | 0.418 |
| 2/week | 9 (25) | 12 (26.6) | ||
| ≥3/week | 4 (11) | 4 (9) |
| Time | Control (n = 36) Count (%) | Intervention (n = 45) Count (%) | ||||
|---|---|---|---|---|---|---|
| Neutral | Hungry | Satisfied | Neutral | Hungry | Satisfied | |
| Before Sohor meal immediately | 6 (16.6) | 19 (52.8) | 11 (30.6) | 9 (20.0) | 22 (48.9) | 14 (31.1) |
| 15 min after Sohor meal | 16 (44.4) | 1 (3) | 19 (52.7) | 0 (0) | 0 (0) | 45 (100) |
| At wakeup immediately | 19 (52.7) | 6 (16.7) | 11 (30.6) | 15 (33.3) | 5 (11.1) | 25 (55.6) |
| At 12:00 pm | 12 (33.3) | 19 (52.8) | 5 (13.9) | 18 (40.0) | 10 (22.2) | 17 (37.8) |
| 2 h prior Iftar meal | 6 (16.7) | 27 (75.0) | 3 (8.3) | 9 (20) | 29 (64.4) | 7 (15.6) |
| At Iftar meal | 7 (19.4) | 27 (75.0) | 2 (5.5) | 7 (15.5) | 34 (75.6) | 4 (8.9) |
| Control (n = 36) | Intervention (n = 45) | Overall p-Value | |||||
|---|---|---|---|---|---|---|---|
| Baseline M ± SD | Endpoint M ± SD | p-Value | Baseline M ± SD | Endpoint M ± SD | p-Value | ||
| Energy (kcal) | 1913 ± 154 | 1876 ± 123 | 0.480 | 2021 ± 108 | 1939 ± 71 | 0.480 | 0.957 |
| Carbohydrate (g) (% of total kcal) | 244 ± 30 (51%) | 220 ± 16 (47%) | 0.343 | 266 ± 8 (53%) | 264 ±11 (55%) | 0.602 | 0.048 |
| Protein (g) (% of total kcal) | 64.4 ± 4.9 (14%) | 66.4 ± 4.6 (14%) | 0.935 | 66.1 ± 4.8 (13%) | 60.9 ± 2.6 (13%) | 0.348 | 0.931 |
| Fat (g) (% of total kcal) | 68.9 ± 5.5 (33%) | 74.8 ± 6.3 (36%) | 0.431 | 69.2 ± 7.9 (31%) | 65.4 ± 3.9 (30%) | 0.667 | 0.784 |
| Dietary fiber (g) (% of RDA) | 18.5 ± 1.8 (74%) | 18.6 ± 1.3 (74%) | 0.901 | 17.8 ± 1.7 (71%) | 25.6 ± 1. (102%) | <0.001 | <0.001 |
| Control (n = 36) | Intervention (n = 45) | Overall p-Value | |||||
|---|---|---|---|---|---|---|---|
| Baseline M ± SD | Endpoint M ± SD | p-Value | Baseline M ± SD | Endpoint M ± SD | p-Value | ||
| Glucose (mg) | 85.7 ± 11.0 | 89.9 ± 12.2 | 0.092 | 83.7 ± 13.5 | 83.6 ± 15.2 | 0.991 | 0.271 |
| Total cholesterol (mg) | 149.5 ± 32.3 | 167.7 ± 33.6 | 0.012 | 140.7 ± 34.4 | 138.8 ± 42.8 | 0.778 | 0.043 |
| HDL cholesterol (mg) | 53.3 ± 14.8 | 53.5 ± 13.7 | 0.921 | 50.6 ± 14.3 | 51.1 ± 15.3 | 0.815 | 0.922 |
| LDL cholesterol (mg) | 81.6 ± 23.8 | 96.3 ± 26.3 | 0.006 | 77.6 ± 29.0 | 78.7 ± 28.6 | 0.786 | 0.033 |
| Triglycerides (mg) | 65.8 ± 18.9 | 77.1 ± 32.7 | 0.083 | 64.2 ± 19.8 | 71.5 ± 31.6 | 0.180 | 0.631 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jarrar, A.H.; Beasley, J.M.; Ohuma, E.O.; Cheikh Ismail, L.; Qeshta, D.A.; Mohamad, M.N.; Al Dhaheri, A.S. Effect of High Fiber Cereal Intake on Satiety and Gastrointestinal Symptoms during Ramadan. Nutrients 2019, 11, 939. https://doi.org/10.3390/nu11040939
Jarrar AH, Beasley JM, Ohuma EO, Cheikh Ismail L, Qeshta DA, Mohamad MN, Al Dhaheri AS. Effect of High Fiber Cereal Intake on Satiety and Gastrointestinal Symptoms during Ramadan. Nutrients. 2019; 11(4):939. https://doi.org/10.3390/nu11040939
Chicago/Turabian StyleJarrar, Amjad H., Jeannette M. Beasley, Eric O. Ohuma, Leila Cheikh Ismail, Dina A. Qeshta, Maysm N. Mohamad, and Ayesha S. Al Dhaheri. 2019. "Effect of High Fiber Cereal Intake on Satiety and Gastrointestinal Symptoms during Ramadan" Nutrients 11, no. 4: 939. https://doi.org/10.3390/nu11040939
APA StyleJarrar, A. H., Beasley, J. M., Ohuma, E. O., Cheikh Ismail, L., Qeshta, D. A., Mohamad, M. N., & Al Dhaheri, A. S. (2019). Effect of High Fiber Cereal Intake on Satiety and Gastrointestinal Symptoms during Ramadan. Nutrients, 11(4), 939. https://doi.org/10.3390/nu11040939









