Ethical, Stigma, and Policy Implications of Food Addiction: A Scoping Review
Abstract
1. Introduction
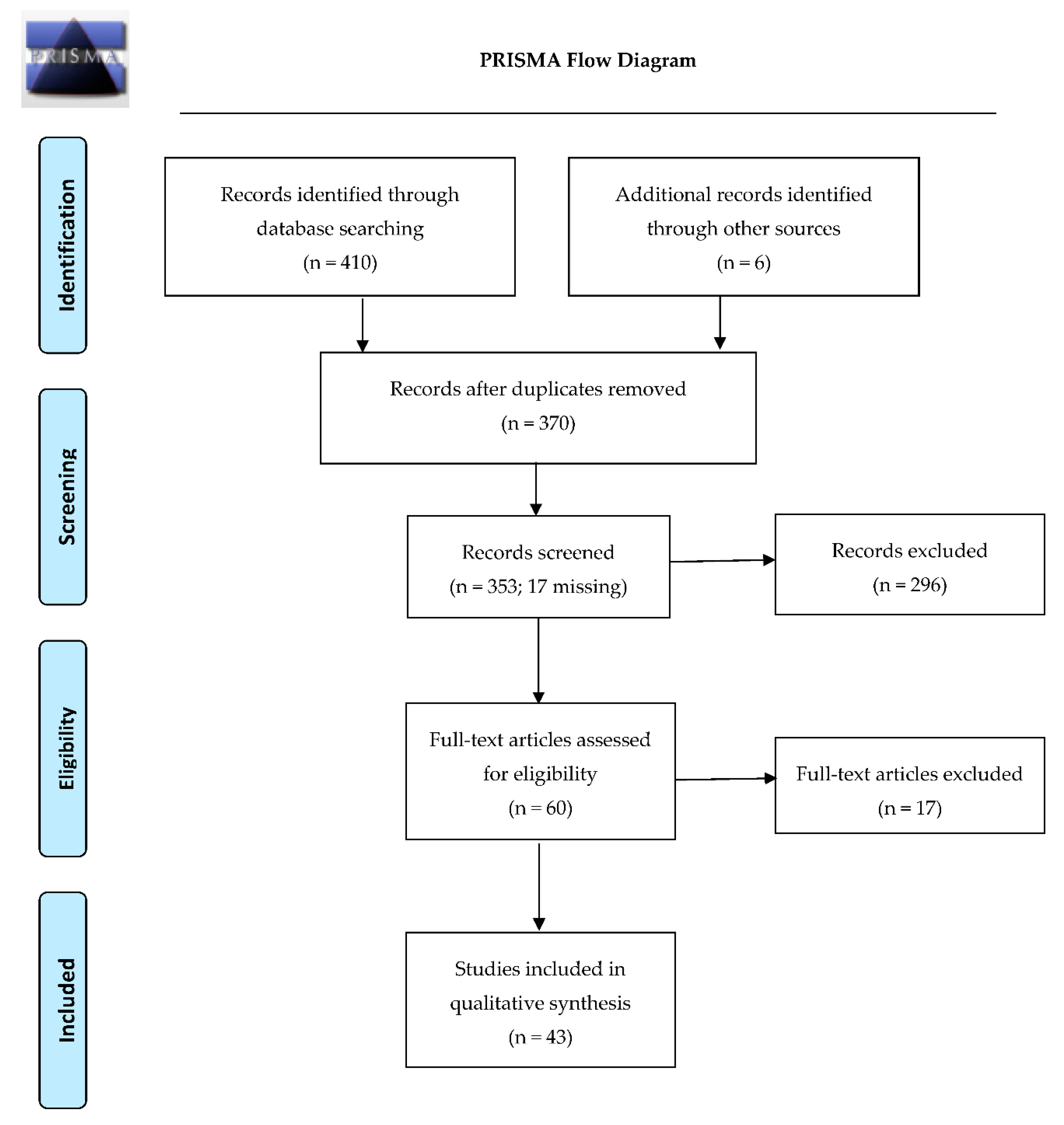
2. Materials and Methods
- Were published in English;
- Were human studies;
- Established a link between obesity or binge eating and addiction or substance use;
- Presented a conceptual or mechanistic model of food addiction (i.e., had to include terms such as “reward,” “reward pathway,” “compulsion,” “substance use,” or “pleasurable” somewhere in the article); and
- Presented the issue of food addiction using a key concept (rather than quoting a prevalence).
3. Results
3.1. The Intersection of Ethics and Food Addiction
3.1.1. Personal Control, Will Power, and Choice
3.1.2. Blame and Weight Bias
3.2. Potential Implications of Food Addiction on Stigma
3.2.1. The Impact on Self-Stigma and Stigma from Others
3.2.2. Differential Impact of Substance Use Disorder Versus Behavioral Addiction on Stigma
3.2.3. Additive Stigma of Addiction Plus Obesity/Eating Disorder
3.3. Potential Policy Implications of Food Addiction
3.3.1. Comparisons to “Big Tobacco”
3.3.2. Reducing Access to Addictive Foods Through Regulation
3.3.3. Food Taxation
3.3.4. Limiting Advertising for Addictive Foods
3.3.5. Limited Information on Food Addiction in Obesity Guidelines
4. Discussion
4.1. Potential Ethical Implications of Food Addiction
4.2. Potential Stigma Implications of Food Addiction
4.3. Potential Policy Implications of Food Addiction
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Kuczmarski, R.J.; Flegal, K.M.; Campbell, S.M.; Johnson, C.L. Increasing prevalence of overweight among US adults. The National Health and Nutrition Examination Surveys, 1960 to 1991. JAMA 1994, 272, 205–211. [Google Scholar] [PubMed]
- Kessler, D.A. The End of Overeating: Taking Control of the Insatiable American Appetite; Rodale: New York, NY, USA, 2009. [Google Scholar]
- Johnson, P.M.; Kenny, P.J. Dopamine D2 receptors in addiction-like reward dysfunction and compulsive eating in obese rats. Nat. Neurosci. 2010, 13, 635–641. [Google Scholar]
- Parr, J.; Rasmussen, N. Making addicts of the fat: Obesity, psychiatry and the ‘Fatties Anonymous’ Model of Self-Help Weight Loss in the Post-War United States. In Critical Perspectives on Addiction (Advances in Medical Sociology, Volume 14); Netherland, J., Ed.; Emerald Group Publishing Limited: Bingley, UK, 2012; pp. 181–200. [Google Scholar]
- Rasmussen, N. Stigma and the addiction paradigm for obesity: Lessons from 1950s America. Addiction 2014, 110, 217–225. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Preliminary validation of the Yale food addiction Scale. Appetite 2009, 52, 430–436. [Google Scholar]
- Gordon, E.L.; Ariel-Donges, A.H.; Bauman, V.; Merlo, L.J. What is the evidence for “food addiction”? A systematic review. Nutrients 2018, 12, 477. [Google Scholar]
- Ivezaj, V.; White, M.A.; Grilo, C.M. Examining binge-eating disorder and food addiction in adults with overweight and obesity. Obesity 2016, 24, 2064–2069. [Google Scholar]
- Chao, A.M.; Shaw, J.A.; Pearl, R.L.; Alamuddin, N.; Hopkins, C.M.; Bakizada, Z.M.; Berkowitz, R.I.; Wadden, T.A. Prevalence and psychosocial correlated of food addiction in persons with obesity seeking weight reduction. Compr. Psychiatry 2016, 73, 97–104. [Google Scholar] [PubMed]
- Gearhardt, A.N.; White, M.A.; Masheb, R.M.; Morgan, P.T.; Crosby, R.D.; Grilo, C.M. An examination of the food addiction construct in obese patients with binge eating disorder. Int. J. Eat. Disord. 2012, 45, 657–663. [Google Scholar] [PubMed]
- Gearhardt, A.N.; Davis, C.; Kuschner, R.; Brownell, K.D. The addiction potential of hyperpalatable foods. Curr. Drug Abuse Rev. 2011, 4, 140–145. [Google Scholar]
- Schulte, E.M.; Avena, N.M.; Gearhardt, A.N. Which foods may be addictive? The roles of processing, fat content, and glycemic load. PLoS ONE 2015, 10, e0117959. [Google Scholar]
- Curtis, C.; Davis, C. A qualitative study of binge eating and obesity from an addiction perspective. Eat. Disord. 2014, 22, 19–32. [Google Scholar]
- Gihooly, C.H.; Das, S.K.; Golden, J.K.; McCrory, M.A.; Dallal, G.E.; Saltzman, E.; Kramer, F.M.; Roberts, S.B. Food cravings and energy regulation: The characteristics of craved foods and their relationship with eating behaviors and weight change during 6 months of dietary energy restriction. Int. J. Obes. 2007, 31, 1849–1858. [Google Scholar]
- Smith, D.G.; Robbins, T.W. The neurobiological underpinnings of obesity and being eating: A rationale for adopting the food addiction model. Biol. Psychiatry 2013, 73, 804–810. [Google Scholar]
- Volkow, N.D.; Wang, G.J.; Fowler, J.S.; Tomais, D.; Baler, R. Food and drug reward: Overlapping circuits in human obesity and addiction. Curr. Top. Behav. Neurosci. 2012, 11, 1–24. [Google Scholar] [PubMed]
- Gearhardt, A.N.; Yokum, S.; Orr, P.; Stice, E.; Corbin, W.; Brownell, K.D. The neural correlates of ‘food addiction’. Arch. Gen. Psychiatry 2011, 68, 808–816. [Google Scholar] [PubMed]
- Davis, C.; Loxton, N.J.; Levitan, R.D.; Kaplan, A.S.; Carter, J.C.; Kennedy, J.L. ‘Food addiction’ and its association with a dopaminergic multilocus genetic profile. Physiol. Behav. 2013, 118, 63–69. [Google Scholar] [PubMed]
- Fletcher, P.C.; Kenny, P.J. Food addiction: A valid concept? Neuropsychopharmacology 2018, 43, 2506–2513. [Google Scholar]
- Burrows, T.; Skinner, J.; McKenna, R.; Rollo, M. Food addiction, binge eating disorder, and obesity: Is there a relationship? Behav. Sci. 2017, 7, 54. [Google Scholar]
- Leigh, S.J.; Morris, M.J. The role of reward circuitry and food addiction in the obesity epidemic: An update. Biol. Psychol. 2018, 131, 31–42. [Google Scholar]
- Muele, A.; Gearhardt, A.N. Food addiction in the light of DSM-5. Nutrients 2014, 6, 2652–2671. [Google Scholar]
- Corwin, R.L.; Grigson, P.S. Symposium overview - food addiction: Fact or fiction? J. Nutr. 2009, 139, 617–619. [Google Scholar]
- Davis, C. A commentary on the associations among ‘food addiction’, binge eating disorder, and obesity: Overlapping conditions with idiosyncratic clinical features. Appetite 2017, 115, 3–8. [Google Scholar] [PubMed]
- Schulte, E.M.; Potenza, M.N.; Gearhardt, A.N. A commentary on the “eating addiction” versus “food addiction” perspectives on addictive-like food consumption. Appetite 2017, 115, 9–15. [Google Scholar]
- Bell, K.; Salmon, A.; Bowers, M.; Bell, J.; McCullough, L. Smoking, stigma and tobacco ‘denormalization’: Further reflections on the use of stigma as a public health tool. Soc. Sci. Med. 2010, 70, 795–799. [Google Scholar]
- Guttman, N.; Salmon, C.T. Guilt, fear, stigma and knowledge gaps: Ethical issues in public health communication interventions. Bioethics 2004, 18, 531–552. [Google Scholar] [PubMed]
- Bayer, R. Stigma and the ethics of public health: Not can we but should we. Soc. Sci. Med. 2008, 67, 463–472. [Google Scholar]
- Goldberg, D.S.; Puhl, R.M. Obesity stigma: A failed and ethically dubious strategy. Hastings Cent. Rep. 2013, 43, 5–6. [Google Scholar] [PubMed]
- Reid, J.; O’Brien, K.S.; Puhl, R.; Hardman, C.A.; Carter, A. Food addiction and its potential links with weight stigma. Curr. Addict. Rep. 2018, 5, 192–201. [Google Scholar]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar]
- Lee, N.M.; Hall, W.D.; Lucke, J.; Forlini, C.; Carter, A. Food Addiction and Its Impact on Weight-Based Stigma and the Treatment of Obese Individuals in the U.S. and Australia. Nutrients 2014, 6, 5312–5326. [Google Scholar]
- Lee, N.M.; Lucke, J.; Hall, W.D.; Meurk, C.; Boyle, F.M.; Carter, A. Public Views on Food Addiction and Obesity: Implications for Policy and Treatment. PLoS ONE 2013, 8, e74836. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. The PRISMA Group (2009). Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Foddy, B. Addicted to Food, Hungry for Drugs. Neuroethics 2011, 4, 79–89. [Google Scholar]
- Thibodeau, P.H.; Perko, V.L.; Flusberg, S.J. The relationship between narrative classification of obesity and support for public policy interventions. Soc. Sci. Med. 2015, 141, 27–35. [Google Scholar] [PubMed]
- Gearhardt, A.N.; Bragg, M.A.; Pearl, R.L.; Schvey, N.A.; Roberto, C.A.; Brownell, K.D. Obesity and public policy. Annu. Rev. Clin. Psychol. 2012, 8, 405–430. [Google Scholar] [PubMed]
- Burmeister, J.M.; Hinman, N.; Koball, A.; Hoffmann, D.A.; Carels, R.A. Food addiction in adults seeking weight loss treatment. Implications for psychosocial health and weight loss. Appetite 2013, 60, 103–110. [Google Scholar] [PubMed]
- DePierre, J.A.; Puhl, R.; Luedicke, J. A new stigmatized identity? Comparisons of a ‘food addict’ label with other stigmatized health conditions. Basic Appl. Soc. Psych. 2013, 35, 10–21. [Google Scholar]
- DePierre, J.A.; Puhl, R.; Luedicke, J. Public perceptions of food addiction: A comparison with alcohol and tobacco. J. Subst. Use 2014, 19, 1–6. [Google Scholar]
- Allen, P.J.; Batra, P.; Geiger, B.M.; Wommack, T.; Gilhooly, C.; Pothos, E.N. Rationale and consequences of reclassifying obesity as an addictive disorder: Neurobiology, food environment and social policy perspectives. Physiol. Behav. 2012, 107, 126–137. [Google Scholar]
- Cullen, A.J.; Barnett, A.; Komesaroff, P.A.; Brown, W.; O’Brien, K.S.O.; Hall, W.; Carter, A. A qualitative study of overweight and obese Australians’ views of food addiction. Appetite 2017, 115, 62–70. [Google Scholar] [PubMed]
- Pretlow, R.A. Addiction to highly pleasurable food as a cause of the childhood obesity epidemic: A qualitative Internet study. Eat. Disord. 2011, 19, 295–307. [Google Scholar]
- Appelhans, B.M.; Whited, M.C.; Schneider, K.L.; Pagoto, S.L. Time to abandon the notion of personal choice in dietary counseling for obesity? J. Am. Diet. Assoc. 2011, 111, 1130–1136. [Google Scholar] [PubMed]
- Latner, J.D.; Puhl, R.M.; Murakami, J.M.; O’Brien, K.S. Food addiction as a causal model of obesity. Effects on stigma, blame, and perceived psychopathology. Appetite 2014, 77, 77–82. [Google Scholar] [PubMed]
- Ho, A.L.; Sussman, E.S.; Pendharkar, A.V.; Azagury, D.E.; Bohon, C.; Halpern, C.H. Deep brain stimulation for obesity: Rationale and approach to trial design. Neurosurg. Focus 2015, 38, E8. [Google Scholar]
- Ortiz, S.E.; Zimmerman, F.J.; Gilliam, F.D., Jr. Weighing in: The taste-engineering frame in obesity expert discourse. Am. J. Public Health 2015, 105, 554–559. [Google Scholar] [PubMed]
- Green, R. The Ethics of Sin Taxes. Public Health Nurs. 2011, 28, 68–77. [Google Scholar] [PubMed]
- Franck, C.; Grandi, S.M.; Eisenberg, M.J. Taxing Junk Food to Counter Obesity. Am. J. Public Health 2013, 103, 1949–1953. [Google Scholar]
- Brownell, K.D.; Schwartz, M.B.; Puhl, R.M.; Henderson, K.E.; Harris, J.L. The need for bold action to prevent adolescent obesity. J. Adolesc. Health 2009, 45, S8–S17. [Google Scholar]
- Pomeranz, J.L.; Teret, S.P.; Sugarman, S.D.; Rutkow, L.; Brownell, K.D. Innovative Legal Approaches to Address Obesity. Milbank Q 2009, 87, 185–213. [Google Scholar]
- Hebebrand, J. Obesity prevention: Moving beyond the food addiction debate. J. Neuroendocrinol. 2015, 27, 737–738. [Google Scholar] [PubMed]
- Blundell, J.E.; Finlayson, G. Food addiction not helpful: The hedonic component—Implicit wanting—Is important. Addiction 2011, 106, 1216–1218. [Google Scholar] [PubMed]
- Mackenzie, R. Don’t Let Them Eat Cake! A View from Across the Pond. Am. J. Bioeth. 2010, 10, 16–18. [Google Scholar] [PubMed]
- deShazo, R.D.; Hall, J.E.; Skipworth, L.B. Obesity bias, medical technology, and the hormonal hypothesis: Should we stop demonizing fat people? Am. J. Med. 2015, 128, 456–460. [Google Scholar] [PubMed]
- Rasmussen, N. Weight stigma, addiction, science, and the medication of fatness in mid-twentieth century America. Sociol. Health Illn. 2012, 34, 880–895. [Google Scholar]
- Goffman, E. Stigma: Notes on the Management of Spoiled Identity; Simon & Schuster: New York, NY, USA, 1963. [Google Scholar]
- Bannon, K.L.; Hunter-Reel, D.; Wilson, G.T.; Karlin, R.A. The effects of casual beliefs and binge eating on the stigmatization of obesity. Int. J. Eat. Disord. 2009, 42, 118–124. [Google Scholar]
- Battle, E.K.; Brownell, K.D. Confronting a rising tide of eating disorders and obesity: Treatment vs. prevention and policy. Addict. Behav. 1996, 21, 755–765. [Google Scholar]
- Schulte, E.M.; Tuttle, H.M.; Gearhardt, A.N. Belief in Food Addiction and Obesity-Related Policy Support. PLoS ONE 2016, 11, e0147557. [Google Scholar]
- Moran, A.; Musicus, A.; Soo, J.; Gearhardt, A.N.; Gollust, S.E.; Roberto, C.A. Believing that certain foods are addictive is associated with support for obesity-related public policies. Prev. Med. 2016, 90, 39–46. [Google Scholar] [PubMed]
- Alonso-Alonso, M.; Woods, S.C.; Pelchat, M.; Grigson, P.S.; Stice, E.; Faroogi, S.; Khoo, C.S.; Mattes, R.D.; Beauchamp, G.K. Food reward system: Current perspectives and future research needs. Nutr. Rev. 2015, 73, 296–307. [Google Scholar] [PubMed]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Food addiction: An examination of the diagnostic criteria for dependence. J. Addict. Med. 2009, 3, 1–7. [Google Scholar]
- Volkow, N.D.; Wise, R.A. How can drug addiction help us understand obesity? Nat. Neurosci. 2005, 8, 555–560. [Google Scholar] [PubMed]
- Willette, A.L. Where have all the parents gone? Do efforts to regulate food advertising to curb childhood obesity pass constitutional muster? J. Leg. Med. 2007, 28, 561–577. [Google Scholar]
- Morphett, K.; Partridge, B.; Gartner, C.; Carter, A.; Hall, W. Why Don’t Smokers Want Help to Quit? A Qualitative Study of Smokers’ Attitudes towards Assisted vs. Unassisted Quitting. Int. J. Environ. Res. Public Health 2015, 12, 6591–6607. [Google Scholar]
- Uppal, N.; Shahab, L.; Britton, J.; Ratschen, E. The forgotten smoker: A qualitative study of attitudes towards smoking, quitting, and tobacco control policies among continuing smokers. BMC Public Health 2013, 13, 432. [Google Scholar]
- Smith, T.G. All foods are habit-forming—What I want to know is which will kill me! Addiction 2011, 106, 1218–1220. [Google Scholar]
- Andreyeva, T.; Long, M.W.; Brownell, K.D. The impact of food prices on consumption: A systematic review of research on the price elasticity of demand for food. Am. J. Public Health 2010, 100, 216–222. [Google Scholar]
- Brownell, K.D.; Frieden, T.R. Ounces of prevention—The public policy case for taxes on sugared beverages. N. Engl. J. Med. 2009, 360, 1805–1808. [Google Scholar] [PubMed]
- Gearhardt, A.N.; Grilo, C.M.; DiLeone, R.J.; Brownell, K.D.; Potenza, M.N. Can food be addictive? Public health and policy implications. Addiction 2011, 106, 1208–1212. [Google Scholar]
- Gostin, L.O. Limiting what we can eat: A bridge too far? Milbank Q. 2014, 92, 173–176. [Google Scholar]
- Rush, B. An Inquiry into the Effects of Ardent Spirits Upon the Human Body and Mind: With an Account of the Means of Preventing, and of the Remedies for Curing Them; James Loring: Boston, NY, USA, 1823. [Google Scholar]
- Jellinek, E.M. The Disease Concept of Alcoholism; Hillhouse: New Haven, CT, USA, 1960. [Google Scholar]
- Leshner, A.I. Addiction is a brain disease, and it matters. Science 1997, 278, 45–47. [Google Scholar] [PubMed]
- Barnett, A.I.; Hall, W.; Fry, C.L.; Dilkes-Frayne, E.; Carter, A. Drug and alcohol treatment providers’ views about the disease model of addiction and its impact on clinical practice: A systematic review. Drug Alcohol Rev. 2018, 37, 697–720. [Google Scholar]
- Rich, E.; Evans, J. ‘Fat ethics’—The obesity discourse and body politics. Soc. Theory Health 2005, 3, 341–358. [Google Scholar]
- Crawford, R. Healthism and the medicalization of everyday life. Int. J. Health Serv. 1980, 10, 365–388. [Google Scholar] [PubMed]
- Pescosolido, B.A.; Martin, J.K. The stigma complex. Annu. Rev. Sociol. 2015, 41, 87–116. [Google Scholar] [PubMed]
- Meadows, A.; Nolan, L.J.; Higgs, S. Self-perceived food addiction: Prevalence, predictors, and prognosis. Appetite 2017, 114, 282–298. [Google Scholar] [PubMed]
- Pearl, R.L.; Puhl, R.M. Weight bias internalization and health: A systematic review. Obes. Rev. 2018, 19, 1141–1163. [Google Scholar] [PubMed]
- Schulte, E.M.; Joyner, M.A.; Schiestl, E.T.; Gearhardt, A.N. Future directions in “food addiction”: Next steps and treatment implications. Curr. Addict. Rep. 2017, 4, 165–171. [Google Scholar]
- Vella, S.C.; Pai, N.B. A narrative review of potential treatment strategies for food addiction. Eat. Weight Disord. 2017, 22, 387–393. [Google Scholar] [PubMed]
- Grant, J.E.; Potenza, M.N.; Weinstein, A.; Gorelick, D.A. Introduction to behavioral addictions. Am. J. Drug Alcohol Abuse 2010, 36, 233–241. [Google Scholar]
- Leeman, R.F.; Potenza, M.N. A targeted review of the neurobiology and genetics of behavioral additions: An emerging area of research. Can. J. Psychiatry 2014, 58, 260–273. [Google Scholar]
| Themes and Sub-Themes | Authors | Sample Quote |
|---|---|---|
| ETHICS | ||
| Personal control, will power, and choice | Foddy (2011) [36] | “The disease label implies a reduction in the autonomy of the addicted and obese. If their strong preferences for consuming food or drugs are merely the symptoms of disease, then these preferences should be viewed as irrelevant in assessing whether their behaviour is willful or not” (p. 86). |
| Lee et al. (2014) [33] | “Equating obesity with food addiction could even justify the use of coercive treatments if obese individuals are seen to suffer from a form of addiction over which they have limited control” (pp. 5313–5314). | |
| Blame and weight bias | Thibodeau et al. (2015) [37] | “The narrative of ‘addiction’ attributed relatively more blame to the behavior of an [obese] individual, evoking comparisons to alcoholism or drug abuse” (p. 29). |
| Gearhardt et al. (2012) [38] | “[I]n addition to causing individual suffering weight bias creates personal and societal injustices for obese persons” (p. 409). | |
| STIGMA | ||
| Impact on self-stigma and stigma from others | Burmeister et al. (2013) [39] | “Food addiction symptoms were related to self-reports of internalized weight bias as well as a form of explicit weight bias in which participants indicated dislike of people who carry excess weight and fears related to becoming or remaining overweight. Given our culture’s traditional views of addiction being a blameworthy illness, it may come as no surprise that obese food ‘addicts’ might tend to internalize these stigmatizing beliefs (p. 108).” |
| Differential impact of substance use disorder versus behavioral addiction | DePierre et al. (2013) [40] | “From the perspective of attribution theory, applying a food addict label to an obese individual could either ameliorate or exacerbate weight stigma. Attribution theory posits that the more a person is seen as responsible for his or her condition, the more people will blame and react to him or her negatively. Indeed, ascribing the cause of obesity to behavioral factors within personal control has been demonstrated to increase stigma, whereas people display fewer negative attitudes toward an individual whose overweight is attributed to biogenetic or physiological factors outside of personal control. Food addiction could be perceived as an external explanation for obesity, reducing blame and stigma. Alternatively, a food addict label could instead act as a behavioral causal attribution, leading obesity to be perceived simply as a result of overeating, potentially increasing weight bias (p. 11).” |
| DePierre et al. (2014) [41] | “Food addiction was perceived as a problem of the mind more than either smoking or alcoholism, and received high endorsement as a behaviour resulting from personal unhappiness, indicating that food addiction is viewed as a mental or behavioural problem rather than a physical addiction. Such a perception may detract from beliefs that certain foods can be addictive, with food addiction instead being seen as rooted in an individual’s psychological make-up. Additionally, given that mental illnesses elicit more stigma and blame than physical ailments, it is possible that food addiction may increase bias towards overweight/obese individuals with this disorder (p. 5).” | |
| Additive stigma of addiction plus obesity and/or eating disorder | DePierre et al. (2013) [40] | “In the context of attribution theory, the food addict label may have increased blame toward obese individuals by attributing weight to eating behavior, where food addiction may be interpreted as a euphemism for overeating. Or perhaps, in line with Goffman’s (1963) framework, categorizing obesity as the result of an addiction added to this ‘abomination of the body’ the stigma of a ‘blemish of character’. Perceiving obesity as the result of a personal failing such as addiction may extend the domains in which it is stigmatized from the immediate social interaction to perceptions of competency for more solitary tasks (or, obesity may extend the otherwise concealable stigma of food addiction to social interactions), potentially explaining why an obese food addict was more negatively perceived than a food addict alone (p. 18).” |
| POLICY | ||
| Comparison to “Big Tobacco” | Allen et al. (2012) [42] | “It is also vital to consider the numerous elements unique to the obesity epidemic that may require novel policy strategies. Most evident is the fact that food is essential for survival, whereas tobacco use is viewed as a dispensable, or even recreational, activity.” |
| Reducing access to addictive foods through regulation | Cullen et al. (2017) [43] | “[Restrictions] would probably help but if the person really wants a Coke every day, they would probably find the means to get it.” |
| Food taxation | Pretlow RA. 2011 [44] | “Taxation of sugar-sweetened beverages, and possibly junk food and fast food, and restriction of such outlets to children, would seem warranted and even embraced by some children.” |
| Limiting advertising for addictive foods | Gearhardt et al. (2012) [38] | “[The food industry] has pledged to remove its unhealthy products from schools and to market fewer unhealthy foods to children, in addition to a variety of other promises. Whether the public and elected officials find the industry trustworthy will determine in part how aggressive government will be in regulating industry practices.” |
| Limited information on food addiction in obesity guidelines | Allen et al. (2012) [42] | “In these guidelines, nothing is said about the potential that an unhealthy diet may not be easily changed due to addictive aspects of hyperphagia. Furthermore, while they do recommend using interventions like taxation on high-energy food, they do not discuss more strict strategies like limiting the access of children to such food.” |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cassin, S.E.; Buchman, D.Z.; Leung, S.E.; Kantarovich, K.; Hawa, A.; Carter, A.; Sockalingam, S. Ethical, Stigma, and Policy Implications of Food Addiction: A Scoping Review. Nutrients 2019, 11, 710. https://doi.org/10.3390/nu11040710
Cassin SE, Buchman DZ, Leung SE, Kantarovich K, Hawa A, Carter A, Sockalingam S. Ethical, Stigma, and Policy Implications of Food Addiction: A Scoping Review. Nutrients. 2019; 11(4):710. https://doi.org/10.3390/nu11040710
Chicago/Turabian StyleCassin, Stephanie E., Daniel Z. Buchman, Samantha E. Leung, Karin Kantarovich, Aceel Hawa, Adrian Carter, and Sanjeev Sockalingam. 2019. "Ethical, Stigma, and Policy Implications of Food Addiction: A Scoping Review" Nutrients 11, no. 4: 710. https://doi.org/10.3390/nu11040710
APA StyleCassin, S. E., Buchman, D. Z., Leung, S. E., Kantarovich, K., Hawa, A., Carter, A., & Sockalingam, S. (2019). Ethical, Stigma, and Policy Implications of Food Addiction: A Scoping Review. Nutrients, 11(4), 710. https://doi.org/10.3390/nu11040710







