Differences in the Quantity and Types of Foods and Beverages Consumed by Canadians between 2004 and 2015
Abstract
1. Introduction
2. Materials and Methods
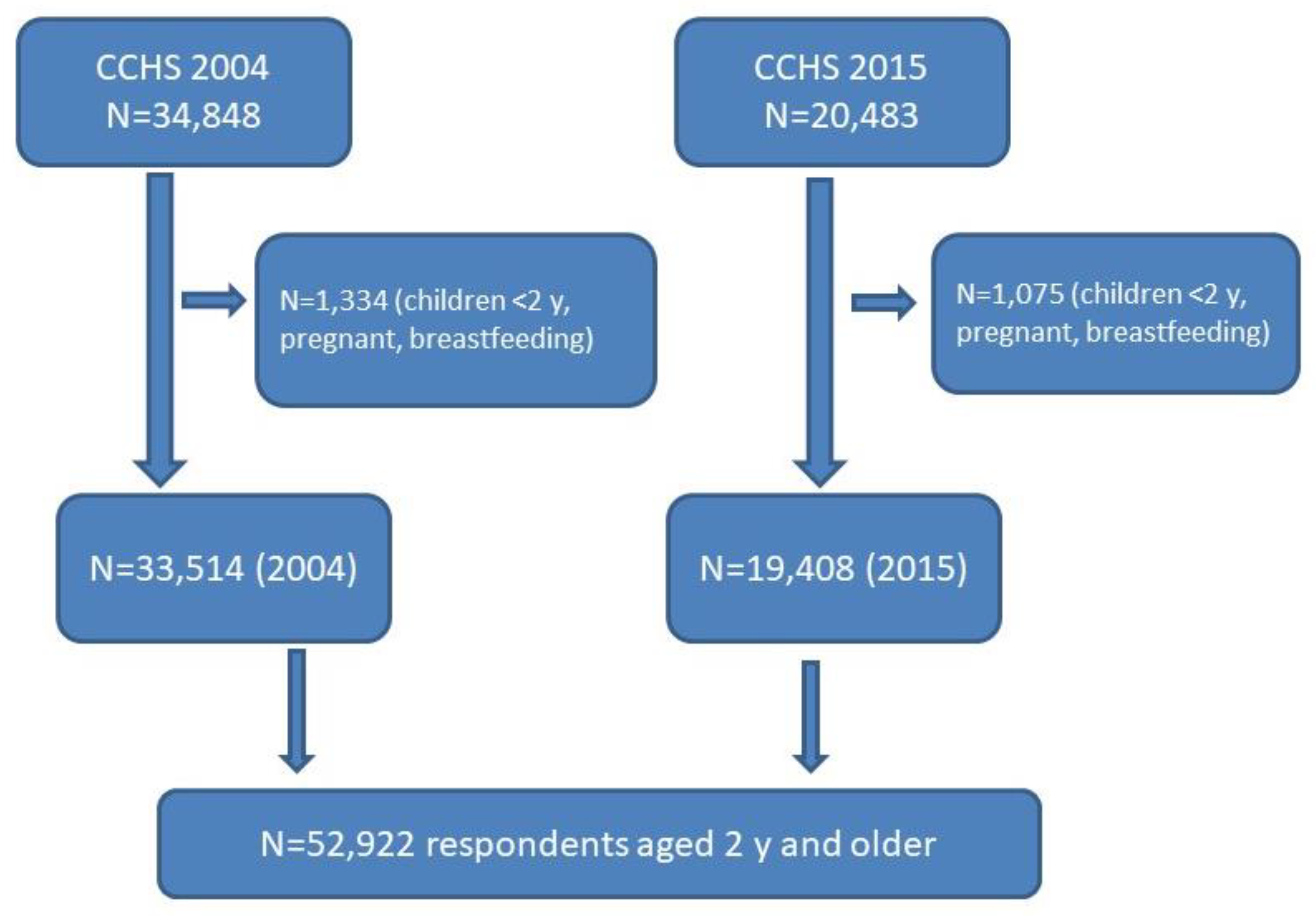
2.1. Data Source and Analytical Sample
2.2. Food Groupings
2.3. Sample Characteristics
2.4. Energy Misreporting
2.5. Statistical Analyses
3. Results
3.1. Sociodemographic Characteristics: 2004 vs. 2015
3.2. Energy Intake of Canadians by Energy Reporting Status: 2004 vs. 2015
3.3. Mean Daily Intakes from the Four 2007 CFG Foods Groups: 2004 vs. 2015
4. Vegetables and Fruit
5. Grain Products
6. Milk and Alternatives
7. Meat and Alternatives
7.1. Mean Daily Intakes from Other Foods and Beverages: 2004 vs. 2015
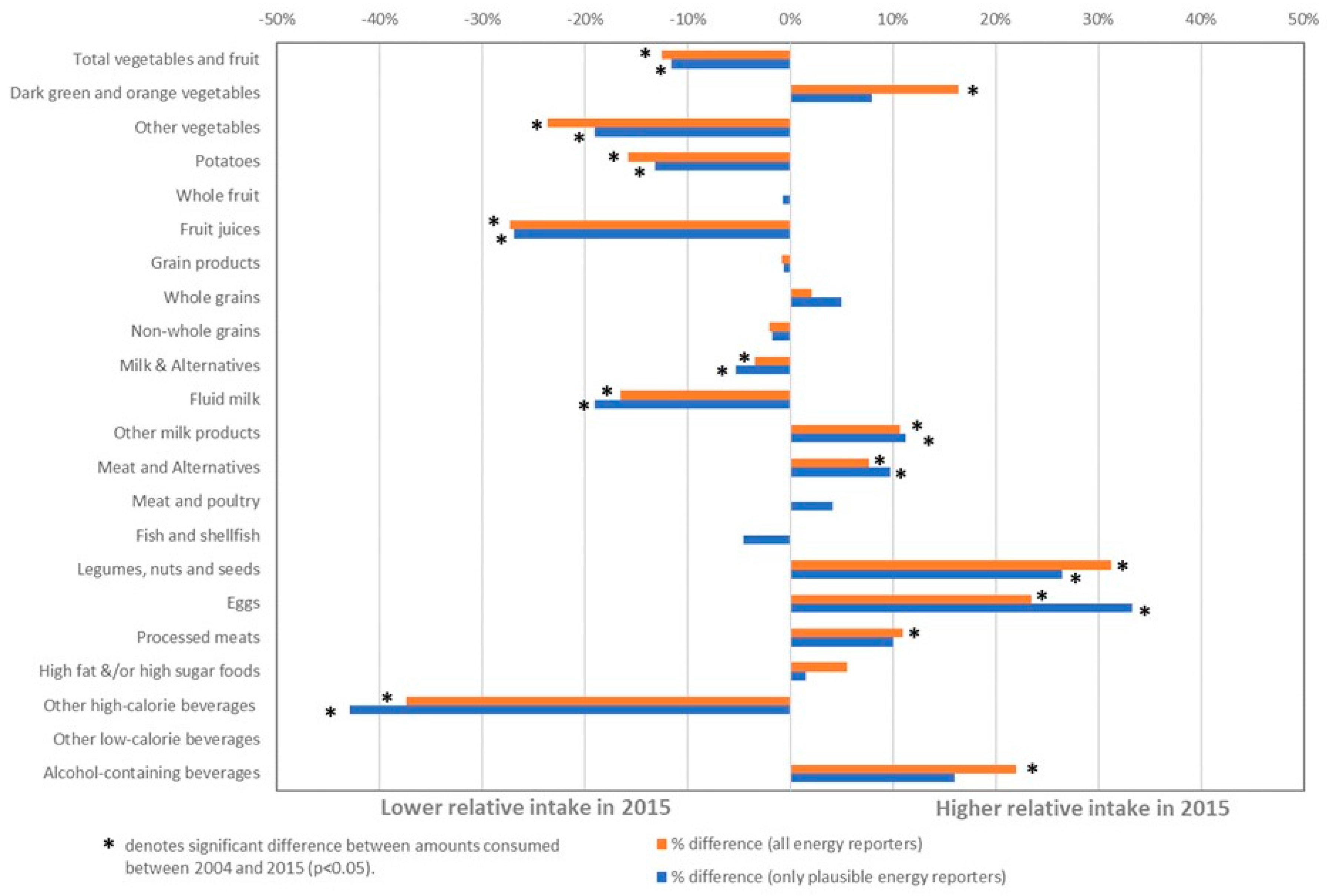
7.2. Relative Percent Change in Food and Beverages Intake from 2004 to 2015
8. Discussion
9. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Institute for Health Metrics and Evaluation. Global Burden of Disease (GBD) Profile: Canada. Available online: http://www.healthdata.org/canada (accessed on 24 April 2017).
- Lieffers, J.R.L.; Ekwaru, J.P.; Ohinmaa, A.; Veugelers, P.J. The economic burden of not meeting food recommendations in Canada: The cost of doing nothing. PLoS ONE 2018, 13, e0196333. [Google Scholar] [CrossRef] [PubMed]
- Black, J.L.; Billette, J.-M. Do Canadians meet Canada’s Food Guide’s recommendations for fruits and vegetables? Appl. Physiol. Nutr. Metab. 2013, 38, 234–242. [Google Scholar] [CrossRef] [PubMed]
- Garriguet, D. Canadians’ eating habits. Health Rep. 2006, 18, 17–32. [Google Scholar]
- Health Canada. Eating Well with Canada’s Food Guide; Health Canada: Ottawa, ON, Canada, 2007.
- Katamay, S.W.; Esslinger, K.A.; Vigneault, M.; Johnston, J.L.; Junkins, B.A.; Robbins, L.G.; Sirois, I.V.; Jones-Mclean, E.M.; Kennedy, A.F.; Bush, M.A.A.; et al. Eating well with Canada’s Food Guide (2007): Development of the food intake pattern. Nutr. Rev. 2007, 65, 155–166. [Google Scholar] [CrossRef] [PubMed]
- Health Canada. Canada’s Dietary Guidelines; Health Canada: Ottawa, ON, Canada, 2019. Available online: https://food-guide.canada.ca/static/assets/pdf/CDG-EN-2018.pdf (accessed on 28 January 2019).
- Health Canada. Reference Guide to Understanding and Using the Data—2015 Canadian Community Health Survey (Nutrition). Available online: https://www.canada.ca/content/dam/hc-sc/documents/services/food-nutrition/food-nutrition-surveillance/ReferenceGuide2015CCHS-Nutr_Eng_Final_06192017.pdf (accessed on 13 June 2017).
- Statistics Canada The Daily—Canadian Community Health Survey—Nutrition: Nutrient Intakes from food and Nutritional Supplements. Available online: http://www.statcan.gc.ca/daily-quotidien/170620/dq170620b-eng.htm (accessed on 25 February 2018).
- Langlois, K.; Garriguet, D.; Gonzalez, A.; Sinclair, S.; Colapinto, C.K. Change in total sugars consumption among Canadian children and adults. Health Rep. 2019, 30, 10–19. [Google Scholar] [PubMed]
- Garriguet, D. Accounting for misreporting when comparing energy intake across time in Canada. Health Rep. 2018, 29, 3–12. [Google Scholar] [PubMed]
- Health Canada Canadian Community Health Survey Cycle 2.2, Nutrition (2004): A Guide to Accessing and Interpreting the Data. Available online: https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/fn-an/alt_formats/hpfb-dgpsa/pdf/surveill/cchs-guide-escc-eng.pdf (accessed on 13 June 2018).
- Statistics Canada. Canadian Community Health Survey Cycle 2.2 Nutrition—General Health (Including Vitamin & Mineral Supplements) & 24-Hour Dietary Recall Components User Guide; Statistics Canada: Ottawa, ON, Canada, 2008.
- Statistics Canada. 2015 Canadian Community Health Survey (CCHS)—Nutrition; Statistics Canada: Ottawa, ON, Canada, 2017.
- United States Department of Agriculture AMPM—USDA Automated Multiple Pass Method. Available online: www.ars.usda.gov/Services/docs.htm?docid=7710 (accessed on 21 May 2018).
- Freedman, L.S.; Guenther, P.M.; Krebs-Smith, S.M.; Kott, P.S. A population’s mean Healthy Eating Index-2005 scores are best estimated by the score of the population ratio when one 24-hour recall is available. J. Nutr. 2008, 138, 1725–1729. [Google Scholar] [CrossRef] [PubMed]
- The Canadian Research Data Centres Network (CRDCN). 2016. Available online: https://crdcn.org/ (accessed on 17 December 2018).
- Health Canada. The Development and Use of a Surveillance Tool: The Classification of Foods in the Canadian Nutrient File According to Eating Well with Canada’s Food Guide; Health Canada: Ottawa, ON, Canada, 2014. Available online: http://publications.gc.ca/collections/collection_2014/sc-hc/H164-158-2-2014-eng.pdf (accessed on 13 June 2018).
- Elvidge Munene, L.-A.; Dumais, L.; Esslinger, K.; Jones-Mclean, E.; Mansfield, E.; Verreault, M.-F.; Villeneuve, M.; Miller, D.; St-Pierre, S. A surveillance tool to assess diets according to Eating Well with Canada’s Food Guide. Health Rep. 2015, 26, 12–20. [Google Scholar] [PubMed]
- Barr, S.I.; Vatanparast, H.; Smith, J. Breakfast in Canada: Prevalence of consumption, contribution to nutrient and food group intakes, and variability across tertiles of daily diet quality. A study from the International Breakfast Research Initiative. Nutrients 2018, 10, 985. [Google Scholar] [CrossRef] [PubMed]
- Garriguet, D. Under-reporting of energy intake in the Canadian Community Health Survey. Health Rep. 2008, 19, 47–55. [Google Scholar] [PubMed]
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein and Amino Acids; National Academy Press: Washington, DC, USA, 2005. [Google Scholar]
- McCrory, M.A.; Hajduk, C.L.; Roberts, S.B. Procedures for screening out inaccurate reports of dietary energy intake. Pub. Health Nutr. 2002, 5, 873–882. [Google Scholar] [CrossRef] [PubMed]
- Colley, R.C.; Carson, V.; Garriguet, D.; Janssen, I.; Roberts, K.C.; Tremblay, M.S. Physical activity of Canadian children and youth, 2007 to 2015. Health Rep. 2017, 28, 8–16. [Google Scholar] [PubMed]
- Thomas, S.; Wannell, B. Combining cycles of the Canadian Community Health Survey. Health Rep. 2009, 20, 1–6. [Google Scholar]
- Statistics Canada. CCHS 2.2 Data Dictionnary; Statistics Canada: Ottawa, ON, Canada, 2005.
- Statistics Canada. Canadian Community Health Survey (CCHS)—Nutrition, 2015 General Health and Summary Data for 24-Hour Dietary Recall and Nutritional Supplements Master File Version (Rounded Frequencies); Statistics Canada: Ottawa, ON, Canada, 2018.
- Statistics Canada. Canada at a Glance: 2017; Statistics Canada: Ottawa, ON, Canada, 2017. Available online: http://publications.gc.ca/collections/collection_2017/statcan/12-581-x/12-581-x2017000-eng.pdf (accessed on 23 February 2019).
- Food and Agricultural Organisation Food Balance Sheets. Available online: http://www.fao.org/faostat/en/#data/FBS (accessed on 21 November 2018).
- Ford, E.S.; Dietz, W.H. Trends in energy intake among adults in the United States: Findings from NHANES. Am. J. Clin. Nutr. 2013, 97, 848–853. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.; Rockström, J.; Loken, B.; Springmann, M.; Lang, T.; Vermeulen, S.; Garnett, T.; Tilman, D.; DeClerck, F.; Wood, A.; et al. Food in the Anthropocene: The EAT-Lancet Commission on healthy diets from sustainable food systems. Lancet 2019, 393, 447–492. [Google Scholar] [CrossRef]
- Hanley, D.A.; Cranney, A.; Jones, G.; Whiting, S.J.; Leslie, W.D.; Cole, D.E.C.; Atkinson, S.A.; Josse, R.G.; Feldman, S.; Kline, G.A.; et al. Vitamin D in adult health and disease: A review and guideline statement from Osteoporosis Canada. CMAJ 2010, 182, E610–E618. [Google Scholar] [CrossRef] [PubMed]
- Health Canada. Do Canadian Adolescent Meet Their Nutrient Requirements through Food Alone? Health Canada: Ottawa, ON, Canada, 2012.
- Health Canada. Do Canadian Adults Meet Their Nutrient Requirements through Food Intake Alone? Health Canada: Ottawa, ON, Canada, 2012. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-nutrition-surveillance/health-nutrition-surveys/canadian-community-health-survey-cchs/canadian-adults-meet-their-nutrient-requirements-through-food-intake-alone-health-canada-2012.html (accessed on 22 October 2018).
- Garriguet, D. Bone health: Osteoporosis, calcium and vitamin D. Health Rep 2011, 22, 7–14. [Google Scholar] [PubMed]
- Health Canada. Do Canadian Children Meet Their Nutrient Requirements through Food Intake Alone? Health Canada: Ottawa, ON, Canada, 2012. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-nutrition-surveillance/health-nutrition-surveys/canadian-community-health-survey-cchs/canadian-children-meet-their-nutrient-requirements-through-food-intake-alone-health-canada-2012.html (accessed on 22 October 2018).
- Kit, B.K.; Fakhouri, T.H.; Park, S.; Nielsen, S.J.; Ogden, C.L. Trends in sugar-sweetened beverage consumption among youth and adults in the United States: 1999–2010. Am. J. Clin. Nutr. 2013, 98, 180–188. [Google Scholar] [CrossRef] [PubMed]
- Rehm, C.D.; Peñalvo, J.L.; Afshin, A.; Mozaffarian, D. Dietary intake among US adults, 1999-2012. JAMA 2016, 315, 2542. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.D.; Leung, C.W.; Li, Y.; Ding, E.L.; Chiuve, S.E.; Hu, F.B.; Willett, W.C. Trends in Dietary Quality Among Adults in the United States, 1999 Through 2010. JAMA Int. Med. 2014, 174, 1587. [Google Scholar] [CrossRef] [PubMed]
- Gu, X.; Tucker, K.L. Dietary quality of the US child and adolescent population: Trends from 1999 to 2012 and associations with the use of federal nutrition assistance programs. Am. J. Clin. Nutr. 2017, 105, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Tugault-Lafleur, C. Examining School Day Dietary Quality: An Analysis of National Dietary Data from the 2004 and 2015 Canadian Community Health Surveys; University of British Columbia: Vancouver, BC, Canada, 2018. [Google Scholar]
- Fismen, A.-S.; Smith, O.; Torsheim, T.; Samdal, O. A school based study of time trends in food habits and their relation to socio-economic status among Norwegian adolescents, 2001–2009. Int. J. Behav. Nutr. Phys. Act 2014, 11, 115. [Google Scholar] [CrossRef] [PubMed]
- Levin, K.A.; Kirby, J.; Currie, C.; Inchley, J. Trends in adolescent eating behaviour: A multilevel cross-sectional study of 11-15 year olds in Scotland, 2002-2010. J. Pub. Heal. 2012, 34, 523–531. [Google Scholar] [CrossRef] [PubMed]
- Jessri, M.; Nishi, S.K.; L’Abbe, M.R. Assessing the nutritional quality of diets of Canadian children and adolescents using the 2014 Health Canada Surveillance Tool Tier System. BMC Pub. Heal. 2016, 16, 381. [Google Scholar] [CrossRef] [PubMed]
- Statistics Canada. Canadian Community Health Survey Cycle 2.2 (2004)—Derived Variables Documentation; Statistics Canada: Ottawa, ON, Canada, 2008.
- Statistics Canada 2015 Canadian Community Health Survey (Nutrition) Derived Variables Specifications; Statistics Canada: Ottawa, ON, Canada, 2017.
- Garriguet, D. Comparison of Results from the Canadian Community Health Surveys-Nutrition 2004 vs. 2015. In Proceedings of the CCHS Webinar Series, Ottawa, ON, Canada, 25 September 2018. [Google Scholar]
- Vigneault, M.; Sadeghpour, A. Comparison of Results from CCHS—2004 vs. 2015. In Proceedings of the CCHS Webinar Series, Ottawa, ON, Canada, 25 September 2018. [Google Scholar]
| Food Groups | Food Subgroups | Food Examples with Examples of Serving Sizes | 2007 CFG Guidance Statements |
|---|---|---|---|
| Vegetables and fruit | Dark green and orange vegetables | Raw spinach or romaine lettuce (1 cup), sweet potato, carrots (125 mL) | Eat at least one dark green and one orange vegetable each day. |
| ‘Other’ vegetables | Zucchini, corn, celery, cucumbers (125 mL) | ||
| Potatoes | Potatoes (baked, mashed, fried) (125 mL) | ||
| Whole fruit | Bananas, apple, pears, grapes (1 fruit or 125 mL) | Have vegetables and fruit more often than juice. | |
| Fruit juice | 100% orange juice (125 mL) | ||
| Grain products | Non-whole grains | White bread (1 slice or 35 g), white rice (125 mL), pita or tortilla (35 g), corn flakes (35 g) | |
| Whole grains | Whole oats or oatmeal (175 mL), whole grain brown or wild rice or pasta (125 mL) | Make at least half of your grain products whole grain each day. | |
| Milk and alternatives | Fluid milk and fortified soy-based beverages | Cow’s milk, fortified soy milk, flavored milk (250 mL) | Drink skim, 1%, or 2% milk each day. Have 500 mL (2 cups) of milk every day for adequate vitamin D. |
| Other milk products | Plain or flavored yogurt (175 g), cheese (50 g) | ||
| Meat and alternatives | Beef, pork, veal, lamb, poultry, game and organ meats | Roasted chicken, turkey, ground beef (75 g) | |
| Fish and shellfish | Salmon, shrimp | Eat at least two food guide servings of fish each week. | |
| Legumes, nuts and seeds and soy | Peanut butter (30 mL), cooked legumes (175 mL), shelled nuts and seeds (60 mL), tofu (150 g) | Have meat alternatives such as beans, lentils and tofu often. | |
| Eggs | Scrambled eggs (2 eggs) | ||
| Processed meats | Smoked turkey, salami (75 g) | ||
| Other foods 1 | High fat and/or high sugar foods | Candies, chocolate, syrups, sauces, fruit jams | Limit foods and beverages high in calories, fat, sugar or salt (sodium) such as cakes and pastries, chocolate and candies, cookies and granola bars, doughnuts and muffins, ice cream and frozen desserts, French fries, potato chips, nachos and other salty snacks, alcohol, fruit flavored drinks, soft drinks, sports and energy drinks, and sweetened hot or cold drinks. |
| Other beverages 1 | High calorie other beverages (>40 kcal/100 g) | Sodas such as Coca Cola©, Sprite© | |
| Low calorie other beverages (≤40 kcal/100 g) | Tea and coffee (unsweetened or lightly sweetened), vitamin water, almond milk | ||
| Alcohol-containing beverages | Wine, beer |
| Survey Cycle | ||||
|---|---|---|---|---|
| 2004 | 2015 | |||
| Mean | SE | Mean | SE | |
| Energy reporting category | ||||
| Underreporter (%) | 22.3 | 0.6 | 30.1 * | 0.8 |
| Plausible reporter (%) | 60.6 | 0.7 | 60.6 | 0.8 |
| Overreporter (%) | 17.1 | 0.6 | 9.3 * | 0.4 |
| Survey Cycle | ||||
|---|---|---|---|---|
| 2004 | 2015 | |||
| Mean | SE | Mean | SE | |
| Mean age (years) | 38.6 | 0.1 | 41.4 * | 0.1 |
| Sex (% male) | 50.6 | 0.1 | 51.1 | 0.2 |
| Location of residence (% urban) | 82.2 | 0.5 | 82.4 | 0.7 |
| Ethnicity (% White/Caucasian) 1 | 82.6 | 0.5 | 76.1 * | 0.7 |
| Immigrant status (% immigrant) 2 | 19.8 | 0.5 | 23.6 * | 0.8 |
| Education (% university graduate) 3 | 34.1 | 0.6 | 45.7 * | 0.9 |
| Body Mass Index (BMI), adults ≥ 18 years (kg/m2) 4 | 27.2 | 0.1 | 27.6 * | 0.1 |
| Overweight/obese, adults ≥ 18 years (% yes) 4 | 60.8 | 0.9 | 63.3 | 1.1 |
| Overweight/obese, children 2–17 years (% yes) 5 | 26.3 | 0.8 | 24.1 | 1.2 |
| Smoking status (% yes) 6 | 23.7 | 0.6 | 17.6 * | 0.7 |
| Supplement use in past 30 days (% yes) 7 | 40.1 | 0.5 | 45.1 * | 0.7 |
| All Energy Reporters | Only Plausible Energy Reporters 1 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Survey Cycle | Survey Cycle | |||||||||||
| 2004 | 2015 | Difference | 2004 | 2015 | Difference | |||||||
| n = 33,314 | n = 19,408 | n = 12,796 | n = 8227 | |||||||||
| Mean | SE | Mean | SE | Mean | 95% CI | Mean | SE | Mean | SE | Mean | 95% CI | |
| Daily energy intake, kcal | ||||||||||||
| Young children, 2–5 y | 1681 | 19 | 1430 | 22 | −250 * | −306, −195 | 1496 | 14 | 1412 | 20 | −85 * | −132, −37 |
| Children, 6–12 y | 2106 | 20 | 1849 | 21 | −256 * | −311, −201 | 1977 | 15 | 1870 | 17 | −106 * | −152, −59 |
| Adolescents, 13–17 y | 2452 | 25 | 2115 | 37 | −337 * | −425, −248 | 2301 | 22 | 2170 | 25 | −131 * | −197, −66 |
| Adults, 18–54 y | 2219 | 18 | 1977 | 20 | −241 * | −294, −189 | 2263 | 18 | 2194 | 23 | −69 * | −125, −14 |
| Older adults, ≥55 y | 1832 | 15 | 1752 | 18 | −80 * | −126, −34 | 1950 | 15 | 1940 | 18 | −10 | −56, 38 |
| All ages | 2108 | 11 | 1880 | 12 | −228 * | −260, −195 | 2123 | 10 | 2049 | 14 | −74 * | −107, −41 |
| All Energy Reporters | Only Plausible Energy Reporters 1 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Survey Cycle | Survey Cycle | |||||||||||
| 2004 | 2015 | Difference | 2004 | 2015 | Difference | |||||||
| n = 32,890 | n = 18,447 | n = 12,602 | n = 7833 | |||||||||
| Mean | SE | Mean | SE | Mean | 95% CI | Mean | SE | Mean | SE | Mean | 95% CI | |
| Total vegetables and fruit, servings | ||||||||||||
| Young children, 2–5 y | 4.2 | 0.1 | 4.2 | 0.1 | 0.0 | −0.3, 0.3 | 4.3 | 0.1 | 3.9 | 0.1 | −0.3 | −0.7, 0.1 |
| Children, 6–12 y | 4.5 | 0.1 | 4.3 | 0.1 | −0.1 | −0.4, 0.1 | 4.4 | 0.1 | 4.5 | 0.1 | 0.1 | −0.3, 0.4 |
| Adolescents, 13–17 y | 4.9 | 0.1 | 4.5 | 0.1 | −0.4 * | −0.7, −0.0 | 4.9 | 0.1 | 4.5 | 0.2 | −0.5 | −0.9, 0.0 |
| Adults, 18–54 y | 5.4 | 0.1 | 4.6 | 0.1 | −0.8 * | −1.0, −0.6 | 5.6 | 0.1 | 4.7 | 0.1 | −0.9 * | −1.2, −0.6 |
| Older adults, ≥55 y | 5.5 | 0.1 | 4.7 | 0.1 | −0.8 * | −1.0, −0.6 | 5.7 | 0.1 | 5.1 | 0.1 | −0.6 * | −0.9, −0.3 |
| All ages | 5.2 | 0.0 | 4.6 | 0.0 | −0.7 *,† | −0.8, −0.5 | 5.4 | 0.1 | 4.7 | 0.1 | −0.6 *,† | −0.8, −0.4 |
| Dark green and orange vegetables, servings | ||||||||||||
| Young children, 2–5 y | 0.3 | 0.0 | 0.4 | 0.0 | 0.1 | 0.0, 0.2 | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 |
| Children, 6–12 y | 0.4 | 0.0 | 0.4 | 0.0 | 0.0 | −0.0, 0.1 | 0.4 | 0.0 | 0.4 | 0.0 | 0.1 * | 0.0, 0.1 |
| Adolescents, 13–17 y | 0.4 | 0.0 | 0.5 | 0.0 | 0.1 * | 0.0, 0.2 | 0.4 | 0.0 | 0.5 | 0.0 | 0.1 | −0.0, 0.2 |
| Adults, 18–54 y | 0.6 | 0.0 | 0.8 | 0.0 | 0.1 * | 0.1, 0.2 | 0.7 | 0.0 | 0.7 | 0.0 | 0.1 | −0.0, 0.2 |
| Older adults, ≥55 y | 0.7 | 0.0 | 0.7 | 0.0 | 0.0 | −0.1, 0.1 | 0.8 | 0.0 | 0.8 | 0.0 | 0.0 | −0.1, 0.1 |
| All ages | 0.6 | 0.0 | 0.7 | 0.0 | 0.1 * | 0.0, 0.1 | 0.6 | 0.0 | 0.7 | 0.0 | 0.1 | −0.0, 0.1 |
| Other vegetables, servings | ||||||||||||
| Young children, 2–5 y | 0.7 | 0.0 | 0.7 | 0.0 | 0.0 | −0.1, 0.1 | 0.7 | 0.1 | 0.7 | 0.1 | 0.0 | −0.2, 0.2 |
| Children, 6–12 y | 1.0 | 0.0 | 0.9 | 0.0 | 0.0 | −0.1, 0.1 | 0.9 | 0.0 | 1.0 | 0.1 | 0.1 * | 0.0, 0.3 |
| Adolescents, 13–17 y | 1.3 | 0.0 | 1.0 | 0.0 | −0.2 * | −0.4, −0.1 | 1.2 | 0.1 | 1.0 | 0.1 | −0.2 * | −0.4, −0.1 |
| Adults, 18–54 y | 1.8 | 0.0 | 1.4 | 0.0 | −0.5 * | −0.6, −0.4 | 1.9 | 0.1 | 1.4 | 0.1 | −0.5 * | −0.6, −0.3 |
| Older adults, ≥55 y | 1.8 | 0.0 | 1.3 | 0.0 | −0.5 * | −0.6, −0.3 | 1.8 | 0.1 | 1.5 | 0.1 | −0.3 * | −0.5, −0.2 |
| All ages | 1.7 | 0.0 | 1.3 | 0.0 | −0.4 *,† | −0.5, −0.3 | 1.6 | 0.0 | 1.3 | 0.0 | −0.3 *,† | −0.4, −0.2 |
| Potatoes, servings | ||||||||||||
| Young children, 2–5 y | 0.4 | 0.0 | 0.3 | 0.0 | −0.1 * | −0.2, −0.0 | 0.4 | 0.0 | 0.3 | 0.0 | −0.1 | −0.2, 0.0 |
| Children, 6–12 y | 0.7 | 0.0 | 0.5 | 0.0 | −0.2 * | −0.2, −0.1 | 0.7 | 0.0 | 0.5 | 0.0 | −0.2 * | −0.3, −0.1 |
| Adolescents, 13–17 y | 0.9 | 0.0 | 0.7 | 0.1 | −0.2 * | −0.3, −0.1 | 0.8 | 0.0 | 0.7 | 0.1 | −0.2 * | −0.3, −0.0 |
| Adults, 18–54 y | 0.8 | 0.0 | 0.6 | 0.0 | −0.2 * | −0.2, −0.1 | 0.8 | 0.0 | 0.6 | 0.0 | −0.1 * | −0.2, −0.0 |
| Older adults, ≥55 y | 0.8 | 0.0 | 0.8 | 0.0 | 0.0 | −0.1, 0.1 | 0.8 | 0.0 | 0.8 | 0.0 | 0.0 | −0.1, 0.2 |
| All ages | 0.8 | 0.0 | 0.6 | 0.0 | −0.1 * | −0.2, −0.1 | 0.8 | 0.0 | 0.7 | 0.0 | −0.1 * | −0.2, −0.0 |
| Whole fruit, servings | ||||||||||||
| Young children, 2–5 y | 1.3 | 0.1 | 1.8 | 0.1 | 0.4 * | 0.2, 0.6 | 1.5 | 0.1 | 1.6 | 0.1 | 0.2 | −0.1, 0.5 |
| Children, 6–12 y | 1.3 | 0.1 | 1.5 | 0.1 | 0.2 * | 0.0, 0.3 | 1.4 | 0.1 | 1.5 | 0.1 | 0.2 | −0.1, 0.4 |
| Adolescents, 13–17 y | 1.0 | 0.4 | 1.3 | 0.1 | 0.2 * | 0.0, 0.4 | 1.0 | 0.1 | 1.3 | 0.1 | 0.2 * | 0.0, 0.5 |
| Adults, 18–54 y | 1.3 | 0.0 | 1.2 | 0.0 | −0.1 | −0.2, 0.1 | 1.4 | 0.1 | 1.3 | 0.1 | −0.1 | −0.3, 0.1 |
| Older adults, ≥55 y | 1.5 | 0.0 | 1.4 | 0.0 | −0.1 | −0.2, 0.0 | 1.5 | 0.1 | 1.5 | 0.1 | −0.1 | −0.2, 0.1 |
| All ages | 1.3 | 0.0 | 1.3 | 0.0 | 0.0 † | −0.1, 0.1 | 1.4 | 0.1 | 1.4 | 0.0 | 0.0 † | −0.1, 0.1 |
| Fruit juices, servings | ||||||||||||
| Young children, 2–5 y | 1.4 | 0.1 | 1.0 | 0.1 | −0.4 * | −0.6, −0.2 | 1.4 | 0.1 | 0.9 | 0.1 | −0.4 * | −0.7, −0.2 |
| Children, 6–12 y | 1.2 | 0.0 | 1.0 | 0.0 | −0.1 * | −0.3, −0.0 | 1.2 | 0.1 | 1.0 | 0.1 | −0.1 | −0.3, 0.0 |
| Adolescents, 13–17 y | 1.3 | 0.1 | 1.0 | 0.1 | −0.3 * | −0.5, −0.1 | 1.5 | 0.1 | 1.1 | 0.1 | −0.4 * | −0.7, −0.1 |
| Adults, 18–54 y | 0.8 | 0.0 | 0.6 | 0.0 | −0.2 * | −0.3, −0.2 | 0.9 | 0.1 | 0.6 | 0.1 | −0.2 * | −0.4, −0.1 |
| Older adults, ≥55 y | 0.7 | 0.0 | 0.4 | 0.0 | −0.2 * | −0.3, −0.1 | 0.7 | 0.0 | 0.5 | 0.0 | −0.3 * | −0.4, −0.2 |
| All ages | 0.9 | 0.0 | 0.6 | 0.0 | −0.2 *,† | −0.3, −0.2 | 0.9 | 0.0 | 0.7 | 0.0 | −0.2 * | −0.3, −0.2 |
| Total grain products, servings | ||||||||||||
| Young children, 2–5 y | 4.5 | 0.1 | 4.6 | 0.1 | −0.2 | −0.1, 0.4 | 4.3 | 0.1 | 4.6 | 0.1 | 0.3 * | 0.0, 0.7 |
| Children, 6–12 y | 6.4 | 0.1 | 7.1 | 0.1 | 0.7 * | 0.4, 0.9 | 6.2 | 0.1 | 6.9 | 0.1 | 0.7 * | 0.5, 1.0 |
| Adolescents, 13–17 y | 7.2 | 0.1 | 7.2 | 0.1 | 0.1 | −0.2, 0.3 | 7.1 | 0.1 | 7.3 | 0.1 | 0.1 | −0.3, 0.5 |
| Adults, 18–54 y | 6.1 | 0.1 | 5.9 | 0.1 | −0.2 | −0.4, 0.0 | 6.6 | 0.1 | 6.3 | 0.1 | −0.3 | −0.6, 0.1 |
| Older adults, ≥55 y | 5.2 | 0.1 | 5.1 | 0.1 | −0.1 | −0.3, 0.1 | 5.7 | 0.1 | 5.7 | 0.1 | −0.1 | −0.3, 0.2 |
| All ages | 5.9 | 0.0 | 5.8 | 0.0 | 0.0 † | −0.2, 0.1 | 6.2 | 0.1 | 6.2 | 0.1 | 0.0 † | −0.2, 0.2 |
| Whole grains, servings | ||||||||||||
| Young children, 2–5 y | 0.7 | 0.0 | 0.8 | 0.1 | 0.0 | −0.1, 0.2 | 0.6 | 0.0 | 0.8 | 0.1 | 0.2 | −0.0, 0.3 |
| Children, 6–12 y | 0.9 | 0.0 | 1.0 | 0.0 | 0.1 | −0.0, 0.2 | 1.0 | 0.1 | 1.1 | 0.1 | 0.1 | −0.1, 0.3 |
| Adolescents, 13–17 y | 0.9 | 0.0 | 1.1 | 0.1 | 0.2 * | 0.0, 0.4 | 0.9 | 0.1 | 1.3 | 1.1 | 0.4 * | 0.1, 0.6 |
| Adults, 18–54 y | 1.0 | 0.0 | 1.0 | 0.0 | 0.0 | −0.2, 0.1 | 1.0 | 0.1 | 1.0 | 0.1 | 0.0 | −0.1, 0.2 |
| Older adults, ≥55 y | 1.1 | 0.0 | 1.0 | 0.0 | -0.1 | −0.2, 0.0 | 1.2 | 0.1 | 1.1 | 0.1 | −0.1 | −0.2, 0.1 |
| All ages | 1.0 | 0.0 | 1.0 | 0.0 | 0.0 † | −0.0, 0.1 | 1.0 | 0.0 | 1.1 | 0.0 | 0.1 | 0.0, 0.2 |
| Non-whole grains, servings | ||||||||||||
| Young children, 2–5 y | 3.7 | 0.1 | 3.8 | 0.1 | 0.1 | −0.1, 0.3 | 3.6 | 0.1 | 3.8 | 0.1 | 0.2 | −0.2, 0.5 |
| Children, 6–12 y | 5.5 | 0.1 | 6.0 | 0.1 | 0.5 * | 0.3, 0.8 | 5.2 | 0.1 | 5.8 | 0.1 | 0.6 * | 0.3, 0.9 |
| Adolescents, 13–17 y | 6.2 | 0.1 | 6.1 | 0.1 | −0.1 | −0.4, 0.2 | 6.2 | 0.1 | 6.0 | 0.1 | −0.2 | −0.4, 0.2 |
| Adults, 18–54 y | 6.2 | 0.1 | 6.0 | 0.2 | −0.2 | −0.6, 0.2 | 5.2 | 0.1 | 5.0 | 0.1 | −0.2 * | −0.4, −0.0 |
| Older adults, ≥55 y | 4.1 | 0.1 | 4.1 | 0.1 | 0.0 | −0.2, 0.1 | 4.5 | 0.1 | 4.5 | 0.1 | 0.0 | −0.3, 0.3 |
| All ages | 4.9 | 0.0 | 4.8 | 0.0 | −0.1 | −0.2, 0.0 | 5.2 | 0.1 | 5.1 | 0.1 | −0.1 † | −0.3, 0.1 |
| Milk & alternatives, servings | ||||||||||||
| Young children, 2–5 y | 2.4 | 0.0 | 2.5 | 0.1 | 0.1 | −0.1, 0.2 | 2.2 | 0.1 | 2.3 | 0.1 | 0.1 | −0.2, 0.3 |
| Children, 6–12 y | 2.5 | 0.0 | 2.3 | 0.0 | −0.1 * | −0.3, −0.0 | 2.4 | 0.1 | 2.3 | 0.1 | -0.1 | −0.3, 0.1 |
| Adolescents, 13–17 y | 2.4 | 0.0 | 2.4 | 0.1 | 0.0 | −0.1, 0.2 | 2.4 | 0.1 | 2.3 | 0.1 | -0.1 | −0.3, 0.2 |
| Adults, 18–54 y | 1.7 | 0.0 | 1.6 | 0.0 | -0.1 | −0.2, 0.0 | 1.8 | 0.0 | 1.7 | 0.1 | −0.1 | −0.3, 0.0 |
| Older adults, ≥55 y | 1.4 | 0.0 | 1.4 | 0.0 | 0.0 | −0.1, 0.1 | 1.6 | 0.0 | 1.5 | 0.0 | 0.0 | −0.1, 0.1 |
| All ages | 1.7 | 0.0 | 1.7 | −0.1 | −0.1 *,† | −0.1, −0.0 | 1.9 | 0.0 | 1.8 | 0.0 | −0.1 * | −0.2, -0.0 |
| Fluid milk, servings | ||||||||||||
| Young children, 2–5 y | 1.6 | 0.0 | 1.4 | 0.1 | −0.2 * | −0.3, −0.0 | 1.4 | 0.1 | 1.2 | 0.1 | −0.2 * | −0.4, −0.0 |
| Children, 6–12 y | 1.4 | 0.0 | 1.1 | 0.0 | −0.3 * | −0.4, −0.2 | 1.4 | 0.0 | 1.1 | 0.0 | −0.3 * | −0.4, −0.1 |
| Adolescents, 13–17 y | 1.4 | 0.0 | 1.2 | 0.0 | −0.2 * | −0.3, −0.1 | 1.4 | 0.1 | 1.1 | 0.1 | −0.2 * | −0.4, −0.1 |
| Adults, 18–54 y | 0.8 | 0.0 | 0.7 | 0.0 | −0.1 * | −0.2, −0.1 | 0.9 | 0.0 | 0.7 | 0.0 | −0.2 * | −0.3, −0.1 |
| Older adults, ≥55 y | 0.7 | 0.0 | 0.6 | 0.0 | −0.2 * | −0.2, −0.1 | 0.8 | 0.0 | 0.7 | 0.0 | −0.2 * | −0.3, −0.1 |
| All ages | 0.9 | 0.0 | 0.8 | 0.0 | −0.1 *,† | −0.2, −0.1 | 1.0 | 0.0 | 0.8 | 0.0 | −0.2 * | −0.2, −0.1 |
| Other milk products (yogurt, cheese), servings | ||||||||||||
| Young children, 2–5 y | 0.9 | 0.0 | 1.1 | 0.1 | 0.2 * | 0.1, 0.3 | 0.8 | 0.0 | 1.0 | 0.1 | 0.3 * | 0.1, 0.4 |
| Children, 6–12 y | 1.0 | 0.0 | 1.2 | 0.0 | 0.1 * | 0.1, 0.2 | 1.0 | 0.0 | 1.1 | 0.0 | 0.2 * | 0.0, 0.3 |
| Adolescents, 13–17 y | 1.0 | 0.0 | 1.2 | 0.1 | 0.2 * | 0.1, 0.3 | 1.0 | 0.0 | 1.1 | 0.1 | 0.2 | −0.1, 0.3 |
| Adults, 18–54 y | 0.9 | 0.0 | 0.9 | 0.0 | 0.0 | −0.0, 0.1 | 0.9 | 0.0 | 1.0 | 0.0 | 0.0 | −0.1, 0.2 |
| Older adults, ≥55 y | 0.7 | 0.0 | 0.8 | 0.0 | 0.1 * | 0.1, 0.2 | 0.8 | 0.0 | 0.9 | 0.0 | 0.1 * | 0.0, 0.2 |
| All ages | 0.8 | 0.0 | 0.9 | 0.0 | 0.1 * | 0.0, 0.1 | 0.9 | 0.0 | 1.0 | 0.0 | 0.1 * | 0.0, 0.2 |
| Meat and alternatives, servings | ||||||||||||
| Young children, 2–5 y | 1.1 | 0.0 | 1.3 | 0.1 | 0.2 * | 0.1, 0.4 | 1.0 | 0.0 | 1.1 | 0.1 | 0.1 | −0.0, 0.3 |
| Children, 6–12 y | 1.6 | 0.0 | 1.6 | 0.0 | 0.0 | −0.1, 0.1 | 1.6 | 0.0 | 1.6 | 0.1 | 0.0 | −0.1, 0.1 |
| Adolescents, 13–17 y | 2.1 | 0.0 | 2.3 | 0.1 | 0.2 * | 0.0, 0.3 | 2.0 | 0.1 | 2.2 | 0.1 | 0.2 | −0.0, 0.4 |
| Adults, 18–54 y | 2.5 | 0.0 | 2.7 | 0.0 | 0.3 * | 0.2, 0.4 | 2.5 | 0.1 | 2.9 | 0.1 | 0.5 * | 0.2, 0.7 |
| Older adults, ≥55 y | 2.2 | 0.0 | 2.2 | 0.0 | 0.0 | −0.1, 0.1 | 2.4 | 0.0 | 2.3 | 0.1 | −0.2 * | −0.3, −0.0 |
| All ages | 2.2 | 0.0 | 2.4 | 0.0 | 0.2 *,† | 0.1, 0.2 | 2.3 | 0.0 | 2.5 | 0.0 | 0.2 *,† | 0.1, 0.3 |
| Meat and poultry, servings | ||||||||||||
| Young children, 2–5 y | 0.5 | 0.0 | 0.6 | 0.0 | 0.0 | −0.0, 0.1 | 0.5 | 0.0 | 0.5 | 0.1 | 0.0 | −0.1, 0.1 |
| Children, 6–12 y | 0.9 | 0.0 | 0.8 | 0.0 | −0.1 | −0.1, 0.0 | 0.8 | 0.0 | 0.8 | 0.0 | −0.1 | −0.2, 0.0 |
| Adolescents, 13–17 y | 1.3 | 0.0 | 1.3 | 0.1 | 0.0 | −0.1, 0.1 | 1.2 | 0.1 | 1.2 | 0.1 | 0.0 | −0.2, 0.1 |
| Adults, 18–54 y | 1.4 | 0.0 | 1.4 | 0.0 | 0.0 | −0.1, 0.2 | 1.3 | 0.1 | 1.6 | 0.1 | 0.2 * | 0.0, 0.5 |
| Older adults, ≥55 y | 1.1 | 0.0 | 1.0 | 0.0 | −0.1 * | −0.2, −0.0 | 1.3 | 0.0 | 1.0 | 0.0 | −0.3 * | −0.4, −0.1 |
| All ages | 1.2 | 0.0 | 1.2 | 0.0 | 0.0 † | −0.1, 0.1 | 1.2 | 0.0 | 1.3 | 0.0 | 0.1 † | −0.1, 0.2 |
| Fish and shellfish, servings | ||||||||||||
| Young children, 2–5 y | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 * | 0.0, 0.1 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0, 0.1 |
| Children, 6–12 y | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | 0.0, 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.1, 0.0 |
| Adolescents, 13–17 y | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | 0.0, 0.1 | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.0, 0.1 |
| Adults, 18–54 y | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | −0.0, 0.0 | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | −0.1, 0.0 |
| Older adults, ≥55 y | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.1, 0.0 | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.1, 0.0 |
| All ages | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 † | −0.0, 0.0 | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | −0.0, 0.0 |
| Legumes, nuts and seeds, servings | ||||||||||||
| Young children, 2–5 y | 0.1 | 0.0 | 0.2 | 0.0 | 0.1 | −0.0, 0.1 | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.0, 0.1 |
| Children, 6–12 y | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | −0.1, 0.0 | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | 0.0, 0.1 |
| Adolescents, 13–17 y | 0.2 | 0.0 | 0.3 | 0.0 | 0.1 * | 0.0, 0.2 | 0.2 | 0.0 | 0.3 | 0.1 | 0.1 | −0.0, 0.3 |
| Adults, 18–54 y | 0.4 | 0.0 | 0.5 | 0.0 | 0.1 * | 0.1, 0.2 | 0.4 | 0.0 | 0.5 | 0.0 | 0.1 * | 0.0, 0.2 |
| Older adults, ≥55 y | 0.3 | 0.0 | 0.4 | 0.0 | 0.1 | −0.0, 0.1 | 0.4 | 0.0 | 0.4 | 0.0 | 0.1 | −0.0, 0.2 |
| All ages | 0.3 | 0.0 | 0.4 | 0.0 | 0.1 * | 0.1, 0.1 | 0.3 | 0.1 | 0.4 | 0.0 | 0.1 * | 0.0, 0.1 |
| Eggs, servings | ||||||||||||
| Young children, 2–5 y | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.0, 0.0 | 0.1 | 0.0 | 0.0 | 0.0 | 0.0 | −0.0, 0.0 |
| Children, 6–12 y | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.0, 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | −0.0, 0.1 |
| Adolescents, 13–17 y | 0.1 | 0.0 | 0.2 | 0.0 | 0.1 * | 0.0, 0.1 | 0.1 | 0.0 | 0.2 | 0.0 | 0.1 * | 0.0, 0.1 |
| Adults, 18–54 y | 0.2 | 0.0 | 0.3 | 0.0 | 0.1 * | 0.0, 0.1 | 0.2 | 0.0 | 0.3 | 0.0 | 0.1 * | 0.0, 0.1 |
| Older adults, ≥55 y | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 * | 0.0, 0.1 | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 | −0.0, 0.1 |
| All ages | 0.2 | 0.0 | 0.2 | 0.0 | 0.0 * | 0.0, 0.1 | 0.2 | 0.0 | 0.2 | 0.0 | 0.1 * | 0.0, 0.1 |
| Processed meats, servings | ||||||||||||
| Young children, 2–5 y | 0.2 | 0.0 | 0.3 | 0.0 | 0.1 | −0.0, 0.2 | 0.2 | 0.0 | 0.3 | 0.0 | 0.0 | −0.1, 0.1 |
| Children, 6–12 y | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.0 | 0.3 | 0.0 | 0.4 | 0.0 | 0.0 | −0.0, 0.1 |
| Adolescents, 13–17 y | 0.4 | 0.0 | 0.4 | 0.0 | 0.0 | −0.0, 0.1 | 0.4 | 0.0 | 0.4 | 0.0 | 0.0 | −0.1, 0.1 |
| Adults, 18–54 y | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 |
| Older adults, ≥55 y | 0.2 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 |
| All ages | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 * | 0.0, 0.1 | 0.3 | 0.0 | 0.3 | 0.0 | 0.0 | −0.0, 0.1 |
| High fat &/or high sugar foods, kcal | ||||||||||||
| Young children, 2–5 y | 89 | 5 | 88 | 5 | −2 | −15, 12 | 82 | 6 | 93 | 8 | 11 | −9, 32 |
| Children, 6–12 y | 153 | 4 | 148 | 6 | 5 | −9, 19 | 145 | 6 | 131 | 7 | −12 | −29, 6 |
| Adolescents, 13–17 y | 166 | 7 | 178 | 10 | 12 | −11, 35 | 145 | 7 | 157 | 10 | 12 | −14, 37 |
| Adults, 18–54 y | 132 | 3 | 138 | 5 | 6 | −6, 19 | 143 | 6 | 140 | 6 | −3 | −19, 13 |
| Older adults, ≥55 y | 104 | 3 | 115 | 4 | 12 * | 3, 21 | 112 | 4 | 125 | 6 | 13 | −2, 28 |
| All ages | 126 | 2 | 133 | 3 | 7 † | 0, 15 | 132 | 3 | 134 | 4 | 2 | −8, 11 |
| High-calorie beverages (>40 kcal/100g), kcal | ||||||||||||
| Young children, 2–5 y | 66 | 3 | 17 | 2 | −49 * | −57, −42 | 57 | 4 | 17 | 3 | −41 * | −51, −31 |
| Children, 6–12 y | 108 | 3 | 51 | 3 | −58 * | −65, −50 | 109 | 4 | 46 | 3 | −63 * | −73, −52 |
| Adolescents, 13–17 y | 169 | 5 | 96 | 6 | −73 * | −88, −58 | 159 | 6 | 90 | 7 | −69 * | −88, −50 |
| Adults, 18–54 y | 91 | 2 | 62 | 3 | −30 * | −37, −21 | 103 | 5 | 64 | 5 | −38 * | −51, −25 |
| Older adults, ≥55 y | 40 | 2 | 28 | 2 | −12 * | −17, −6 | 42 | 3 | 26 | 2 | −16 * | −23, −9 |
| All ages | 83 | 2 | 52 | 2 | −32 *,† | −36, −27 | 91 | 2 | 52 | 2 | −39 *,† | −46, −32 |
| Low-calorie beverages (≤40 kcal/100 g), kcal | ||||||||||||
| Young children, 2–5 y | 9 | 1 | 8 | 2 | −1 | −5, 2 | 9 | 2 | 11 | 3 | 2 | −4, 8 |
| Children, 6–12 y | 15 | 1 | 17 | 1 | 2 | −2, 5 | 15 | 1 | 14 | 1 | −1 | −5, 3 |
| Adolescents, 13–17 y | 25 | 2 | 33 | 3 | 8 * | 2, 15 | 25 | 3 | 36 | 4 | 11 * | 1, 20 |
| Adults, 18–54 y | 25 | 1 | 25 | 2 | −1 | −6, 6 | 26 | 2 | 25 | 4 | −1 | −12, 10 |
| Older adults, ≥55 y | 19 | 1 | 18 | 1 | −1 | −4, 2 | 20 | 2 | 21 | 2 | 1 | −5, 6 |
| All ages | 22 | 1 | 22 | 1 | 0 | −3, 3 | 23 | 1 | 23 | 2 | 0 | −6, 6 |
| Alcohol-containing beverages, kcal | ||||||||||||
| Adolescents, 13–17 y | 5 | 1 | 7 | 2 | 2 | −4, 8 | 4 | 1 | 3 | 1 | −1 | −5, 2 |
| Adults, 18–54 y | 88 | 4 | 101 | 6 | 13 | −1, 27 | 92 | 6 | 105 | 8 | 12 | −8, 32 |
| Older adults, ≥55 y | 63 | 3 | 89 | 5 | 26 * | 15, 37 | 73 | 6 | 88 | 8 | 15 | −4, 34 |
| All ages | 74 | 2 | 90 | 4 | 16 * | 7, 25 | 79 | 4 | 91 | 6 | 13 | −1, 26 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tugault-Lafleur, C.N.; Black, J.L. Differences in the Quantity and Types of Foods and Beverages Consumed by Canadians between 2004 and 2015. Nutrients 2019, 11, 526. https://doi.org/10.3390/nu11030526
Tugault-Lafleur CN, Black JL. Differences in the Quantity and Types of Foods and Beverages Consumed by Canadians between 2004 and 2015. Nutrients. 2019; 11(3):526. https://doi.org/10.3390/nu11030526
Chicago/Turabian StyleTugault-Lafleur, Claire N., and Jennifer L. Black. 2019. "Differences in the Quantity and Types of Foods and Beverages Consumed by Canadians between 2004 and 2015" Nutrients 11, no. 3: 526. https://doi.org/10.3390/nu11030526
APA StyleTugault-Lafleur, C. N., & Black, J. L. (2019). Differences in the Quantity and Types of Foods and Beverages Consumed by Canadians between 2004 and 2015. Nutrients, 11(3), 526. https://doi.org/10.3390/nu11030526






