Effect of Energy Restriction on Eating Behavior Traits and Psychobehavioral Factors in the Low Satiety Phenotype
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Diet-Based Weight-Reducing Intervention
2.3. Anthropometric Measurements
2.4. Subjective Appetite Sensations and Satiety Responsiveness
2.5. Ad Libitum Energy Intake
2.6. Eating Behavior Traits
2.7. Psychobehavioral Factors
2.8. Procedures
2.9. Statistical Analysis
3. Results
3.1. Baseline Participant Characteristics
3.2. Baseline Eating Behavior Traits and Psychobehavioral Factors
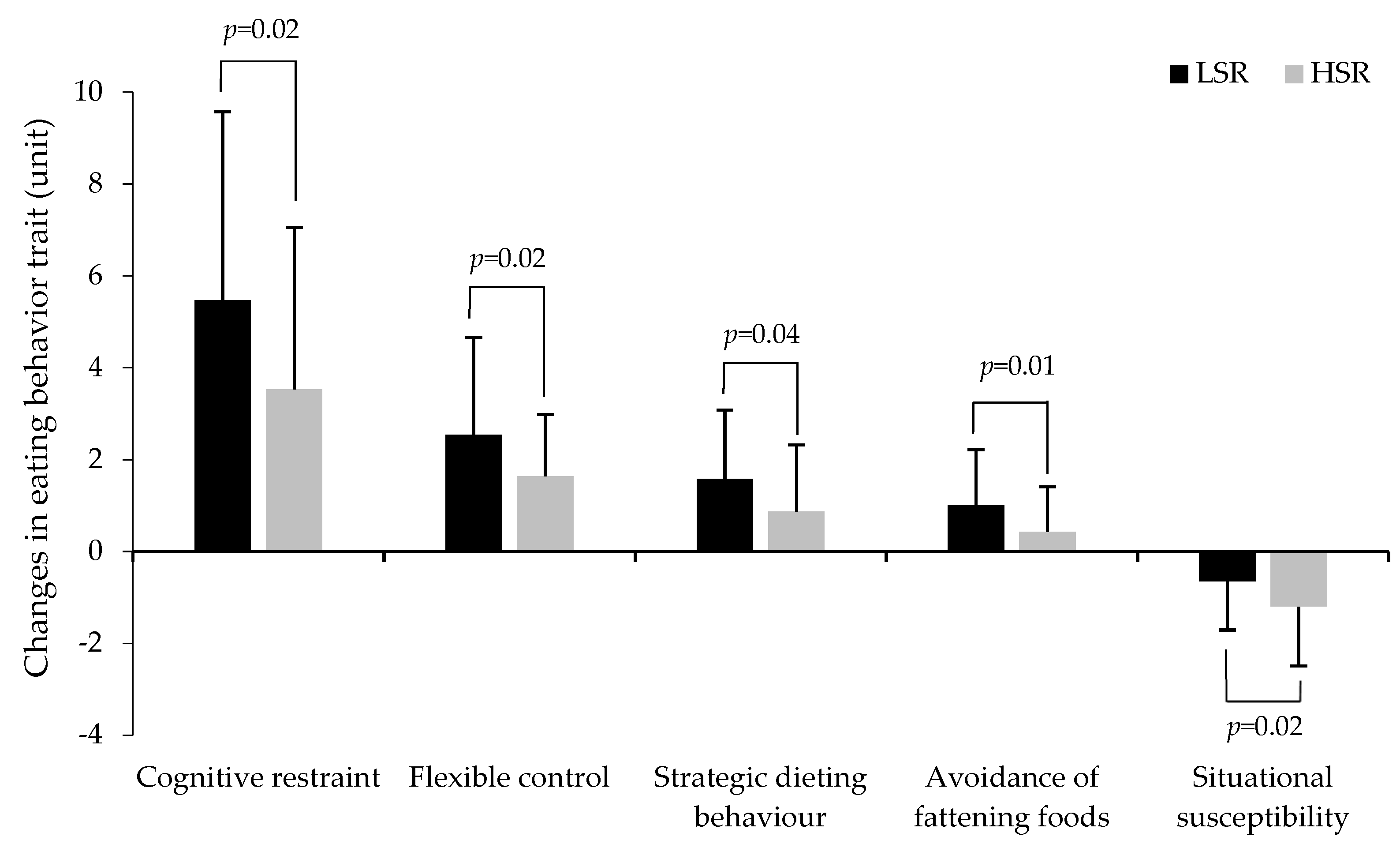
3.3. Changes in Body Weight, Satiety Efficiency, Eating Behavior Traits, and Psychobehavioral Factors
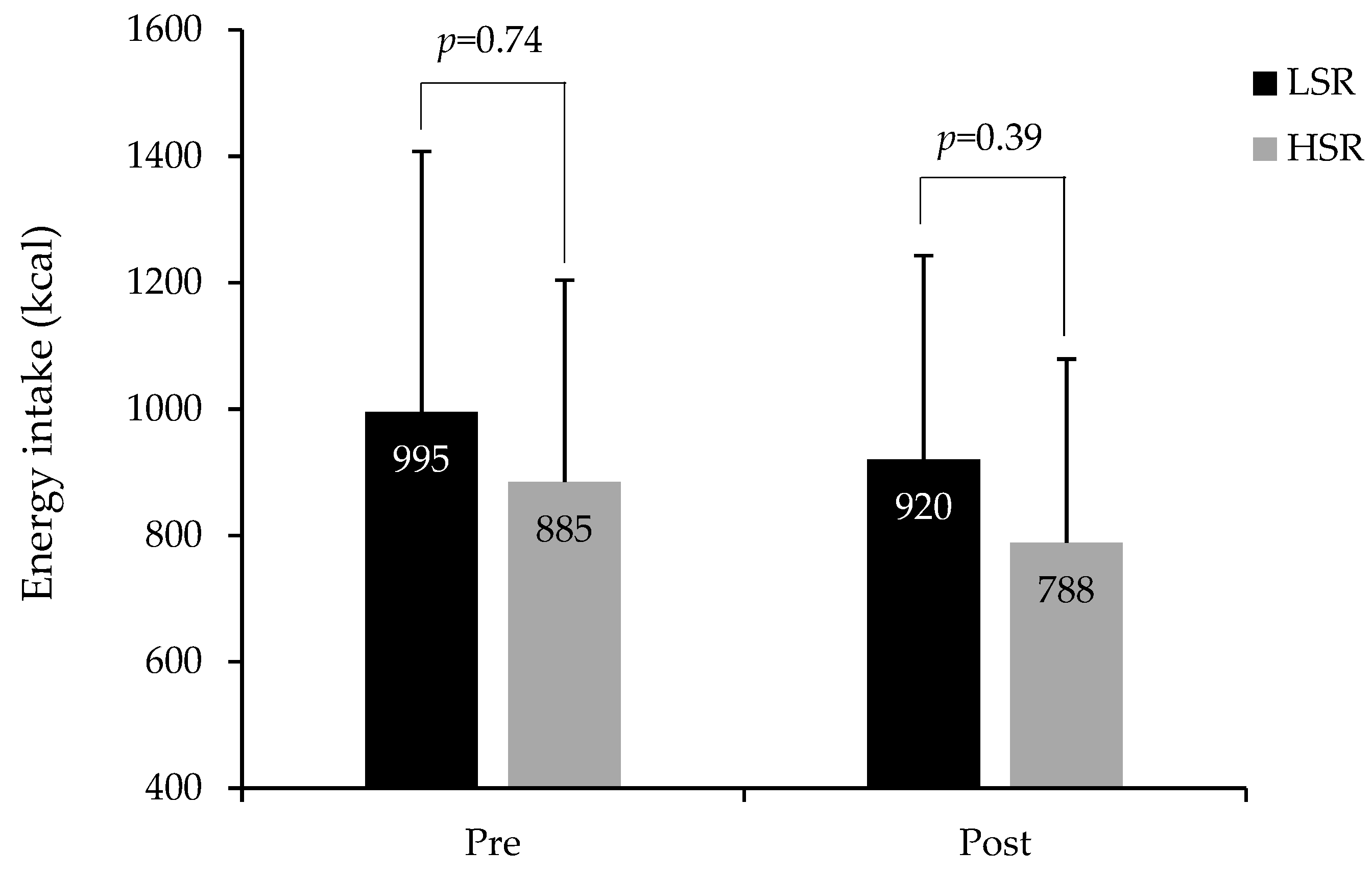
3.4. Ad Libitum Energy Intake at the Buffet-Type Meal
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- James, P.T.; Leach, R.; Kalamara, E.; Shayeghi, M. The worldwide obesity epidemic. Obes. Res. 2001, 9 (Suppl. 4), 228S–233S. [Google Scholar] [CrossRef] [PubMed]
- Blundell, J.E.; Gillett, A. Control of food intake in the obese. Obes. Res. 2001, 9 (Suppl. 4), 263S–270S. [Google Scholar] [CrossRef] [PubMed]
- Llewellyn, C.; Wardle, J. Behavioral susceptibility to obesity: Gene-environment interplay in the development of weight. Physiol. Behav. 2015, 152, 494–501. [Google Scholar] [CrossRef] [PubMed]
- Finlayson, G.; Halford, J.C.; King, N.; Blundell, J. The Regulation of Food Intake in Humans. In Obesitext—The Source; Weickert, M.O., Ed.; Endotext.com: South Dartmouth, MA, USA, 2008; Chapter 7.3. [Google Scholar]
- Barkeling, B.; King, N.A.; Naslund, E.; Blundell, J.E. Characterization of obese individuals who claim to detect no relationship between their eating pattern and sensations of hunger or fullness. Int. J. Obes. (Lond.) 2007, 31, 435–439. [Google Scholar] [CrossRef] [PubMed]
- Drapeau, V.; Hetherington, M.; Tremblay, A. Impact of Eating and Lifestyle Behaviors on Body Weight: Beyond Energy Value. In Handbook of Behavior, Food and Nutrition; Preedy, V.R., Watson, R.R., Martin, C.R., Eds.; Springer: New York, NY, USA, 2011; pp. 693–706. [Google Scholar]
- Drapeau, V.; Blundell, J.; Therrien, F.; Lawton, C.; Richard, D.; Tremblay, A. Appetite sensations as a marker of overall intake. Br. J. Nutr. 2005, 93, 273–280. [Google Scholar] [CrossRef] [PubMed]
- Blundell, J.E.; Finlayson, G. Is susceptibility to weight gain characterized by homeostatic or hedonic risk factors for overconsumption? Physiol. Behav. 2004, 82, 21–25. [Google Scholar] [CrossRef] [PubMed]
- Dalton, M.; Hollingworth, S.; Blundell, J.; Finlayson, G. Weak Satiety Responsiveness Is a Reliable Trait Associated with Hedonic Risk Factors for Overeating among Women. Nutrients 2015, 7, 7421–7436. [Google Scholar] [CrossRef]
- Drapeau, V.; Blundell, J.; Gallant, A.R.; Arguin, H.; Despres, J.P.; Lamarche, B.; Tremblay, A. Behavioural and metabolic characterisation of the low satiety phenotype. Appetite 2013, 70, 67–72. [Google Scholar] [CrossRef]
- Bryant, E.J.; King, N.A.; Blundell, J.E. Disinhibition: Its effects on appetite and weight regulation. Obes. Rev. 2008, 9, 409–419. [Google Scholar] [CrossRef]
- Gallant, A.; Lundgren, J.; O’Loughlin, J.; Allison, K.; Tremblay, A.; Henderson, M.; Drapeau, V. Night-eating symptoms and 2-year weight change in parents enrolled in the QUALITY cohort. Int. J. Obes. (Lond.) 2015, 39, 1161–1165. [Google Scholar] [CrossRef]
- Boswell, R.G.; Kober, H. Food cue reactivity and craving predict eating and weight gain: A meta-analytic review. Obes. Rev. 2016, 17, 159–177. [Google Scholar] [CrossRef] [PubMed]
- Drapeau, V.; Therrien, F.; Richard, D.; Tremblay, A. Is visceral obesity a physiological adaptation to stress? Panminerva Med. 2003, 45, 189–195. [Google Scholar] [PubMed]
- Drapeau, V.; King, N.; Hetherington, M.; Doucet, E.; Blundell, J.; Tremblay, A. Appetite sensations and satiety quotient: Predictors of energy intake and weight loss. Appetite 2007, 48, 159–166. [Google Scholar] [CrossRef] [PubMed]
- Arguin, H.; Tremblay, A.; Blundell, J.E.; Despres, J.P.; Richard, D.; Lamarche, B.; Drapeau, V. Impact of a non-restrictive satiating diet on anthropometrics, satiety responsiveness and eating behaviour traits in obese men displaying a high or a low satiety phenotype. Br. J. Nutr. 2017, 118, 750–760. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, J.A.; Drapeau, V.; Astrup, A.; Tremblay, A. Relationship between diet-induced changes in body fat and appetite sensations in women. Appetite 2009, 52, 809–812. [Google Scholar] [CrossRef]
- Chaput, J.P.; Drapeau, V.; Hetherington, M.; Lemieux, S.; Provencher, V.; Tremblay, A. Psychobiological impact of a progressive weight loss program in obese men. Physiol. Behav. 2005, 86, 224–232. [Google Scholar] [CrossRef]
- Urbanek, J.K.; Metzgar, C.J.; Hsiao, P.Y.; Piehowski, K.E.; Nickols-Richardson, S.M. Increase in cognitive eating restraint predicts weight loss and change in other anthropometric measurements in overweight/obese premenopausal women. Appetite 2015, 87, 244–250. [Google Scholar] [CrossRef]
- Chaput, J.P.; Drapeau, V.; Hetherington, M.; Lemieux, S.; Provencher, V.; Tremblay, A. Psychobiological effects observed in obese men experiencing body weight loss plateau. Depress. Anxiety 2007, 24, 518–521. [Google Scholar] [CrossRef]
- Sanchez, M.; Darimont, C.; Drapeau, V.; Emady-Azar, S.; Lepage, M.; Rezzonico, E.; Ngom-Bru, C.; Berger, B.; Philippe, L.; Ammon-Zuffrey, C.; et al. Effect of Lactobacillus rhamnosus CGMCC1.3724 supplementation on weight loss and maintenance in obese men and women. Br. J. Nutr. 2014, 111, 1507–1519. [Google Scholar] [CrossRef]
- Major, G.C.; Alarie, F.; Dore, J.; Phouttama, S.; Tremblay, A. Supplementation with calcium + vitamin D enhances the beneficial effect of weight loss on plasma lipid and lipoprotein concentrations. Am. J. Clin. Nutr. 2007, 85, 54–59. [Google Scholar] [CrossRef]
- Major, G.C.; Doucet, E.; Jacqmain, M.; St-Onge, M.; Bouchard, C.; Tremblay, A. Multivitamin and dietary supplements, body weight and appetite: Results from a cross-sectional and a randomised double-blind placebo-controlled study. Br. J. Nutr. 2008, 99, 1157–1167. [Google Scholar] [CrossRef] [PubMed]
- Diabète Québec. Guide D’alimentation de la Personne Diabétique (Meal Planning for People with Diabetes); Diabète Québec: Quebec, QC, Canada, 2003. [Google Scholar]
- The Airlie (VA) Consensus Conference. In Standardization of Anthropometric Measurements; Lohman, T., Roche, A., Martorell, R., Eds.; Human Kinetics: Champaign, IL, USA, 1988; pp. 39–80. [Google Scholar]
- Hill, A.J.; Blundell, J.E. The effects of a high-protein or high-carbohydrate meal on subjective motivation to eat and food preferences. Nutr. Behav. 1986, 3, 133–144. [Google Scholar]
- Green, S.M.; Delargy, H.J.; Joanes, D.; Blundell, J.E. A satiety quotient: A formulation to assess the satiating effect of food. Appetite 1997, 29, 291–304. [Google Scholar] [CrossRef] [PubMed]
- Arvaniti, K.; Richard, D.; Tremblay, A. Reproducibility of energy and macronutrient intake and related substrate oxidation rates in a buffet-type meal. Br. J. Nutr. 2000, 83, 489–495. [Google Scholar] [CrossRef] [PubMed]
- The Canadian Nutrient File. Available online: https://food-nutrition.canada.ca/cnf-fce/index-eng.jsp (accessed on 18 January 2019).
- Stunkard, A.J.; Messick, S. The three-factor eating questionnaire to measure dietary restraint, disinhibition and hunger. J. Psychosol. Res. 1985, 29, 71–83. [Google Scholar] [CrossRef]
- Bond, M.J.; McDowell, A.J.; Wilkinson, J.Y. The measurement of dietary restraint, disinhibition and hunger: An examination of the factor structure of the Three Factor Eating Questionnaire (TFEQ). Int. J. Obes. Relat. Meta Disor. 2001, 25, 900–906. [Google Scholar] [CrossRef] [PubMed]
- Gormally, J.; Black, S.; Daston, S.; Rardin, D. The assessment of binge eating severity among obese persons. Addict. Behav. 1982, 7, 47–55. [Google Scholar] [CrossRef]
- Moreno, S.; Rodriguez, S.; Fernandez, M.C.; Tamez, J.; Cepeda-Benito, A. Clinical validation of the trait and state versions of the Food Craving Questionnaire. Assessment 2008, 15, 375–387. [Google Scholar] [CrossRef]
- Beck, A.T.; Steer, R.A.; Carbin, M.G. Psychometric properties of the Beck Depression Inventory: Twenty-five years of evaluation. Clin. Psychol. Rev. 1988, 8, 77–100. [Google Scholar] [CrossRef]
- Spielberger, C.D.; Gorsuch, R.L.; Lushene, P.R.; Vagg, P.R.; Jacobs, A.G. Manual for the State-Trait Anxiety Inventory (Form Y); Consulting Psychologists Press, Inc.: Palo Alto, CA, USA, 1983. [Google Scholar]
- Buysse, D.J.; Reynolds, C.F., 3rd; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Chaput, J.P.; Leblanc, C.; Perusse, L.; Despres, J.P.; Bouchard, C.; Tremblay, A. Risk factors for adult overweight and obesity in the Quebec Family Study: Have we been barking up the wrong tree? Obesity (Silver Spring) 2009, 17, 1964–1970. [Google Scholar] [CrossRef] [PubMed]
- Park, S.K.; Jung, J.Y.; Oh, C.M.; McIntyre, R.S.; Lee, J.H. Association Between Sleep Duration, Quality and Body Mass Index in the Korean Population. J. Clin. Sleep Med. 2018, 14, 1353–1360. [Google Scholar] [CrossRef] [PubMed]
- Petry, N.M.; Barry, D.; Pietrzak, R.H.; Wagner, J.A. Overweight and obesity are associated with psychiatric disorders: Results from the National Epidemiologic Survey on Alcohol and Related Conditions. Psychosom. Med. 2008, 70, 288–297. [Google Scholar] [CrossRef] [PubMed]
- McNeil, J.; Drapeau, V.; Gallant, A.R.; Tremblay, A.; Doucet, E.; Chaput, J.P. Short sleep duration is associated with a lower mean satiety quotient in overweight and obese men. Eur. J. Clin. Nutr. 2013, 67, 1328–1330. [Google Scholar] [CrossRef]
- Drapeau, V.; Provencher, V.; Lemieux, S.; Despres, J.P.; Bouchard, C.; Tremblay, A. Do 6-y changes in eating behaviors predict changes in body weight? Results from the Quebec Family Study. Int. J. Obes. Relat. Metab. Disord. 2003, 27, 808–814. [Google Scholar] [CrossRef] [PubMed]
- Jospe, M.R.; Taylor, R.W.; Athens, J.; Roy, M.; Brown, R.C. Adherence to Hunger Training over 6 Months and the Effect on Weight and Eating Behavior: Secondary Analysis of a Randomised Controlled Trial. Nutrients 2017, 9, 1260. [Google Scholar] [CrossRef] [PubMed]
- Dunn, C.; Haubenreiser, M.; Johnson, M.; Nordby, K.; Aggarwal, S.; Myer, S.; Thomas, C. Mindfulness Approaches and Weight Loss, Weight Maintenance, and Weight Regain. Curr. Obes. Rep. 2018, 7, 37–49. [Google Scholar] [CrossRef] [PubMed]
- Lemoine, S.; Rossell, N.; Drapeau, V.; Poulain, M.; Garnier, S.; Sanguignol, F.; Mauriege, P. Effect of weight reduction on quality of life and eating behaviors in obese women. Menopause 2007, 14, 432–440. [Google Scholar] [CrossRef] [PubMed]
- Carbonneau, E.; Royer, M.M.; Richard, C.; Couture, P.; Desroches, S.; Lemieux, S.; Lamarche, B. Effects of the Mediterranean Diet before and after Weight Loss on Eating Behavioral Traits in Men with Metabolic Syndrome. Nutrients 2017, 9, 305. [Google Scholar] [CrossRef] [PubMed]
- Kahathuduwa, C.N.; Binks, M.; Martin, C.K.; Dawson, J.A. Extended calorie restriction suppresses overall and specific food cravings: A systematic review and a meta-analysis. Obes. Rev. 2017, 18, 1122–1135. [Google Scholar] [CrossRef] [PubMed]
| Study 1 [22] | Study 2 [23] | Study 3 [21] | |
|---|---|---|---|
| n1 | 29 | 18 | 53 |
| Women, n (%) | 29 (100) | 11 (61.1) | 31 (58.5) |
| Control group intervention | Diet + placebo | Diet + placebo | Diet + placebo |
| Prescribed energy-restriction (diet), kcal/day | −700 | −700 | −500 |
| Duration, weeks | 15 | 15 | 12 |
| Consultation with the dietitian | Each 2 weeks | Each 2 weeks | Each 2 weeks |
| Questionnaires 2 | |||
| TFEQ | x | x | x |
| BES | x | ||
| FCQ (S and T) | x | ||
| PSQI | x | x | x |
| BDI | x | x | x |
| STAI | x | ||
| Anthropometric measurements 2 | x | x | x |
| Standardized breakfast and VAS measurements 2 | x | x | x |
| Buffet-type meal 2 | x | x | x |
| All (n = 100) | LSR (n = 50) | HSR (n = 50) | p1 | |
|---|---|---|---|---|
| Women, % (n) | 71.0 (71) | 54.0 (27) | 88.0 (44) | 0.0002 |
| Men, % (n) | 29.0 (29) | 46.0 (23) | 12.0 (6) | |
| Age, years | 38.7 ± 8.7 | 37.8 ± 9.5 | 39.6 ± 7.8 | 0.30 |
| Anthropometric measures | ||||
| Weight, kg | 91.4 ± 14.4 | 95.6 ± 15.0 | 87.1 ± 12.5 | 0.15 |
| Height, cm | 165.7 ± 8.9 | 168.1 ± 9.8 | 163.3 ± 7.1 | 0.69 |
| BMI, kg/m2 | 33.2 ± 3.6 | 33.7 ± 3.9 | 32.6 ± 3.3 | 0.11 |
| Waist circumference, cm | 103.4 ± 10.5 | 106.3 ± 11.2 | 100.5 ± 8.8 | 0.18 |
| Satiety Quotient (SQ) | ||||
| SQ mean, mm/100 kcal | 10.4 ± 5.4 | 6.0 ± 2.6 | 14.8 ± 3.5 | <0.0001 |
| SQ desire to eat, mm/100 kcal | 10.7 ± 6.5 | 6.3 ± 4.7 | 15.1 ± 5.0 | <0.0001 |
| SQ hunger, mm/100 kcal | 10.7 ± 6.5 | 5.6 ± 4.0 | 15.8 ± 4.0 | <0.0001 |
| SQ fullness, mm/100 kcal | 12.0 ± 7.1 | 7.7 ± 6.0 | 16.3 ± 5.3 | <0.0001 |
| SQ PFC, mm/100 kcal | 8.2 ± 5.4 | 4.3 ± 3.3 | 12.0 ± 4.3 | <0.0001 |
| Fasting Appetite Sensations | ||||
| Fasting desire to eat, mm | 92.7 ± 38.8 | 78.4 ± 41.5 | 107.0 ± 30.0 | <0.0001 |
| Fasting hunger, mm | 93.9 ± 38.1 | 76.5 ± 40.5 | 111.3 ± 25.8 | <0.0001 |
| Fasting fullness, mm 2 | 25.0 ± 28.4 | 32.6 ± 32.7 | 17.3 ± 20.9 | 0.049 |
| Fasting PFC, mm | 87.8 ± 32.0 | 80.3 ± 34.8 | 95.2 ± 27.3 | 0.0004 |
| LSR | HSR | p Group | p Time | p Group × Time | |||
|---|---|---|---|---|---|---|---|
| Pre 1 | Post 2 | Pre | Post 2 | ||||
| Three-Factor Eating Questionnaire | |||||||
| Cognitive restraint (0–21) | 7.0 ± 3.4 | 12.3 ± 3.8 **** | 8.8 ± 4.3 | 12.5 ± 4.0 **** | 0.51 | <0.0001 | 0.02 |
| Flexible control (0–7) | 1.8 ± 1.6 | 4.2 ± 1.9 **** | 2.7 ± 1.6 | 4.3 ± 1.5 **** | 0.44 | <0.0001 | 0.02 |
| Rigid control (0–7) | 2.4 ± 1.5 | 3.4 ± 1.6 | 2.8 ± 1.7 | 3.6 ± 1.8 | 0.99 | <0.0001 | 0.28 |
| Strategic dieting behavior (0–4) 3 | 0.4 ± 0.7 | 1.9 ± 1.4 **** | 0.9 ± 1.1 | 1.8 ± 1.2 *** | 0.50 | <0.0001 | 0.04 |
| Attitude to self-regulation (0–5) | 2.5 ± 1.2 | 3.5 ± 1.1 | 2.9 ± 1.5 | 3.4 ± 1.5 | 0.99 | <0.0001 | 0.07 |
| Avoidance of fattening foods (0–4) | 2.0 ± 1.2 | 3.0 ± 1.0 **** | 2.3 ± 1.1 | 2.7 ± 1.1 | 0.62 | <0.0001 | 0.01 |
| Disinhibition (0–16) | 8.5 ± 3.1 | 6.9 ± 2.8 | 8.5 ± 2.9 | 6.1 ± 2.8 | 0.25 | <0.0001 | 0.20 |
| Habitual susceptibility (0–5) | 1.7 ± 1.3 | 1.0 ± 0.9 | 1.7 ± 1.5 | 1.0 ± 1.0 | 0.59 | <0.0001 | 0.67 |
| Emotional susceptibility (0–3) | 1.7 ± 1.3 | 1.2 ± 1.3 | 1.9 ± 1.1 | 1.2 ± 1.2 | 0.30 | <0.0001 | 0.42 |
| Situational susceptibility (0–5) | 3.3 ± 1.4 | 2.7 ± 1.4 ** | 3.3 ± 1.1 | 2.1 ± 1.4 **** | 0.80 | <0.0001 | 0.02 |
| Susceptibility to hunger (0–14) | 6.7 ± 3.6 | 4.2 ± 3.2 | 5.2 ± 2.9 | 2.8 ± 2.2 | 0.04 | <0.0001 | 0.84 |
| Internal locus of hunger (0–6) | 2.2 ± 1.7 | 1.4 ± 1.6 | 2.0 ± 1.6 | 0.8 ± 1.1 | 0.19 | <0.0001 | 0.42 |
| External locus of hunger (0–6) | 3.3 ± 1.8 †† | 1.9 ± 1.6 | 2.3 ± 1.5 | 1.2 ± 1.1 | 0.01 | <0.0001 | 0.36 |
| Binge Eating Scale (BES) | |||||||
| Binge Eating (0–46) | 12.7 ± 6.7 | 9.5 ± 6.3 | 10.3 ± 5.2 | 6.5 ± 5.0 | 0.08 | <0.0001 | 0.52 |
| State-Trait Food Craving Questionnaire | |||||||
| State Food Craving Questionnaire | |||||||
| Desire to eat (3–15) | 7.2 ± 3.3 | 6.9 ± 3.1 | 6.3 ± 3.1 | 5.7 ± 2.5 | 0.74 | 0.20 | 0.49 |
| Anticipation of Positive Reinforcement (3–15) | 6.2 ± 2.7 | 6.1 ± 2.2 | 5.7 ± 2.7 | 4.9 ± 2.1 | 0.37 | 0.17 | 0.35 |
| Anticipation of Relief from Negative states (3–15) 3 | 5.5 ± 2.3 | 5.4 ± 2.4 | 4.8 ± 2.5 | 4.5 ± 2.2 | 0.33 | 0.59 | 0.78 |
| Lack of Control over Eating (3–15) | 6.4 ± 3.0 | 5.7 ± 2.6 | 6.1 ± 2.6 | 5.0 ± 2.0 | 0.74 | 0.006 | 0.41 |
| Craving as a Physiological State (3–15) | 7.8 ± 3.1 | 6.7 ± 2.1 | 5.8 ± 2.5 | 5.5 ± 1.8 | 0.04 | 0.05 | 0.30 |
| Trait Food Craving Questionnaire | |||||||
| Intention and planning to consume food (3–18) | 8.3 ± 2.9 | 7.5 ± 2.4 | 8.0 ± 1.6 | 7.0 ± 2.3 | 0.49 | 0.02 | 0.85 |
| Anticipation of Positive Reinforcement (5–30) | 15.6 ± 3.6 | 13.9 ± 4.5 | 13.8 ± 3.1 | 12.4 ± 2.7 | 0.11 | 0.02 | 0.91 |
| Anticipation of Relief from Negative states (3–18) | 7.8 ± 2.9 | 6.6 ± 2.4 | 6.7 ± 2.0 | 5.6 ± 1.8 | 0.05 | 0.003 | 0.91 |
| Lack of Control over Eating (6–36) | 17.0 ± 6.5 | 14.6 ± 5.6 | 15.0 ± 3.8 | 12.5 ± 2.9 | 0.11 | <0.0001 | 0.75 |
| Thoughts or Preoccupation with Food (7–42) | 16.4 ± 5.4 | 15.2 ± 5.5 | 16.0 ± 5.5 | 14.0 ± 5.2 | 0.61 | 0.009 | 0.37 |
| Craving as a Physiological State (4–24) | 13.6 ± 3.8 | 12.7 ± 3.1 | 13.7 ± 2.2 | 12.0 ± 1.8 | 0.89 | 0.0002 | 0.12 |
| Emotions that may be experienced (4–24) | 11.2 ± 5.0 | 10.6 ± 4.7 | 10.6 ± 2.9 | 8.5 ± 2.7 | 0.07 | 0.006 | 0.07 |
| Cues that may trigger food cravings (4–24) | 15.5 ± 4.7 | 13.7 ± 4.7 | 14.3 ± 2.8 | 12.4 ± 2.4 | 0.33 | <0.0001 | 0.66 |
| Guilt that may be experienced (3–18) | 8.8 ± 3.6 | 8.5 ± 3.1 | 8.3 ± 2.2 | 7.1 ± 2.7 | 0.09 | 0.06 | 0.26 |
| Pittsburg Sleep Quality Index (PSQI) | |||||||
| Sleep Quality (total score) (0–21) 3 | 5.1 ± 2.4 †† | 4.0 ± 2.1 | 3.9 ± 2.5 | 3.3 ± 1.9 | 0.02 | 0.002 | 0.24 |
| Sleep Duration (Hours) | 7.2 ± 0.8 † | 7.4 ± 0.9 | 7.6 ± 0.8 | 7.5 ± 0.8 | 0.11 | 0.28 | 0.25 |
| Beck Depression Inventory (BDI) | |||||||
| Depressive symptoms (0–63) 3, 4 | 5.5 ± 6.2 | 4.3 ± 4.2 | 3.9 ± 4.0 | 3.9 ± 3.6 | 0.43 | 0.71 | 0.10 |
| State-Trait Anxiety Inventory | |||||||
| Present-state anxiety (20–80) 4 | 28.9 ± 6.3 ††† | 29.7 ± 9.0 | 26.0 ± 3.4 | 25.1 ± 4.9 | 0.002 | 0.58 | 0.48 |
| General-state anxiety (20–80) | 38.8 ± 7.6 | 36.0 ± 7.4 | 35.2 ± 6.1 | 32.7 ± 4.6 | 0.04 | 0.002 | 0.93 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Drapeau, V.; Jacob, R.; Panahi, S.; Tremblay, A. Effect of Energy Restriction on Eating Behavior Traits and Psychobehavioral Factors in the Low Satiety Phenotype. Nutrients 2019, 11, 245. https://doi.org/10.3390/nu11020245
Drapeau V, Jacob R, Panahi S, Tremblay A. Effect of Energy Restriction on Eating Behavior Traits and Psychobehavioral Factors in the Low Satiety Phenotype. Nutrients. 2019; 11(2):245. https://doi.org/10.3390/nu11020245
Chicago/Turabian StyleDrapeau, Vicky, Raphaëlle Jacob, Shirin Panahi, and Angelo Tremblay. 2019. "Effect of Energy Restriction on Eating Behavior Traits and Psychobehavioral Factors in the Low Satiety Phenotype" Nutrients 11, no. 2: 245. https://doi.org/10.3390/nu11020245
APA StyleDrapeau, V., Jacob, R., Panahi, S., & Tremblay, A. (2019). Effect of Energy Restriction on Eating Behavior Traits and Psychobehavioral Factors in the Low Satiety Phenotype. Nutrients, 11(2), 245. https://doi.org/10.3390/nu11020245





