Experimental Outcomes of the Mediterranean Diet: Lessons Learned from the Predimed Randomized Controlled Trial
Abstract
1. Introduction
The PREDIMED Study
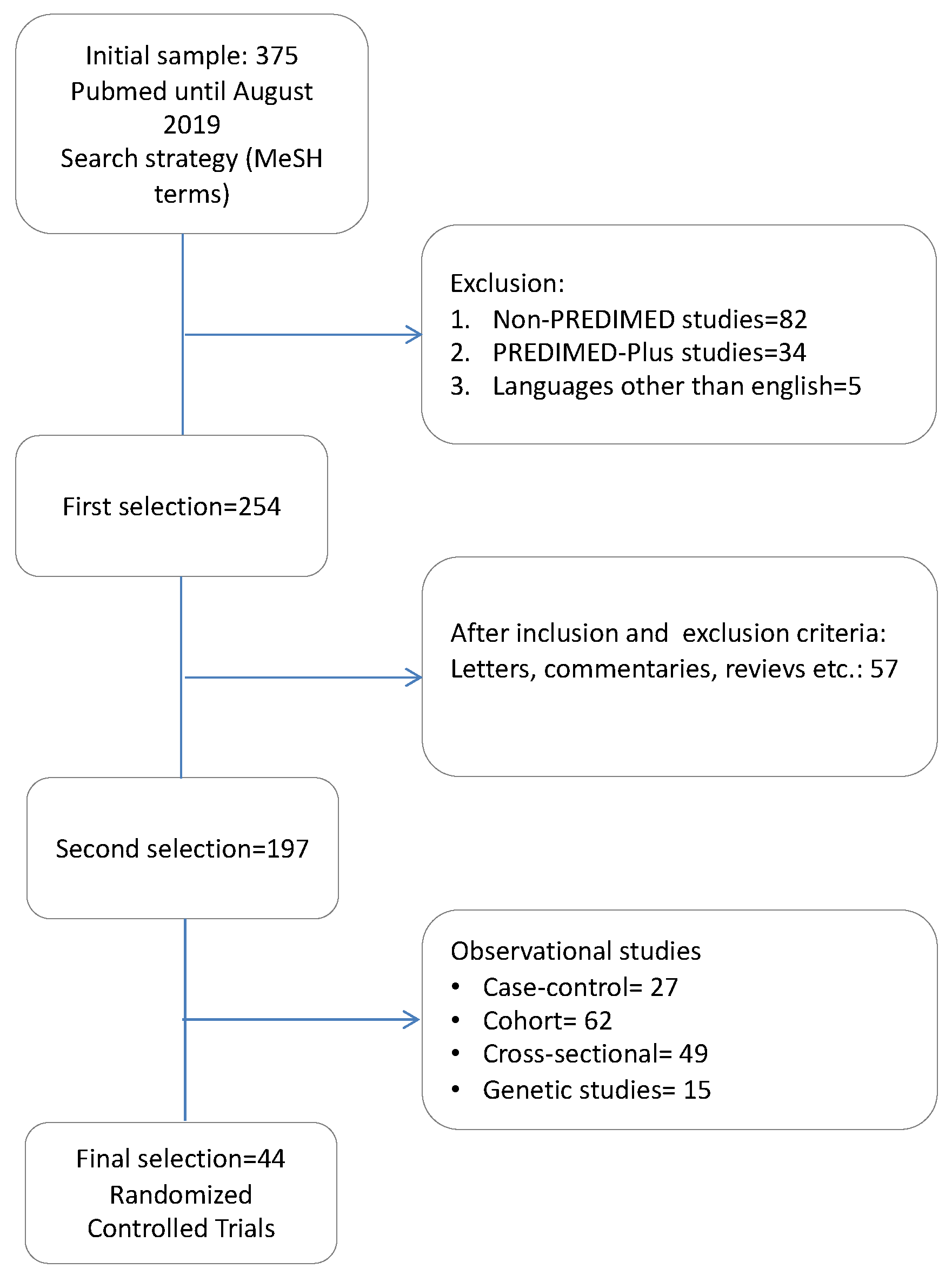
2. Materials and Methods
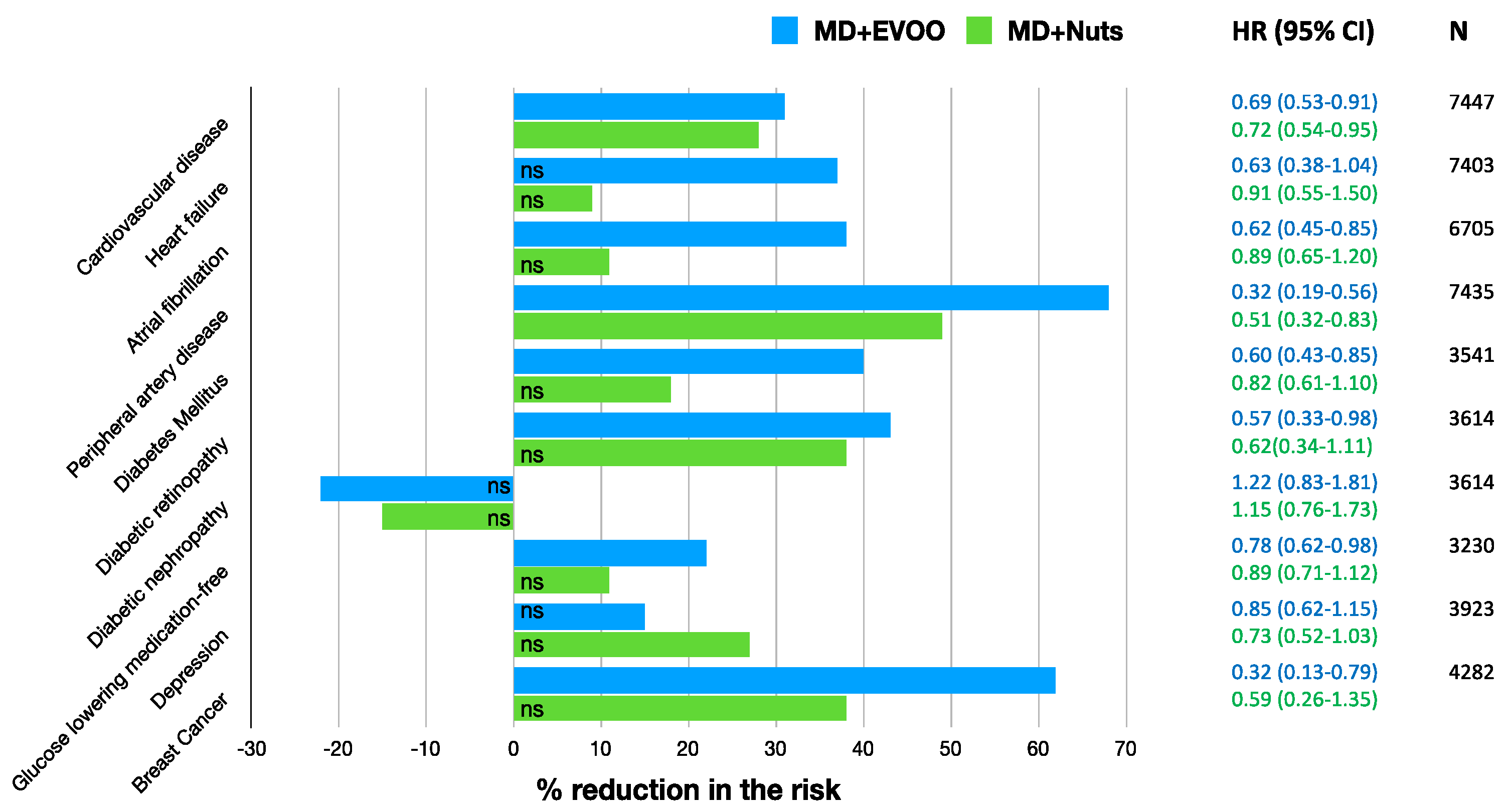
3. Results
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Serra-Majem, L.; Roman-Vinas, B.; Sánchez-Villegas, A.; Guasch-Ferré, M.; Corella, D.; La Vecchia, C. Benefits of the Mediterranean diet: Epidemiological and molecular aspects. Mol. Asp. Med. 2019, 67, 1–55. [Google Scholar] [CrossRef] [PubMed]
- Trichopoulou, A.; Martínez-González, M.A.; Tong, T.Y.; Forouhi, N.G.; Khandelwal, S.; Prabhakaran, D.; Mozaffarian, D.; de Lorgeril, M. Definitions and potential health benefits of the Mediterranean diet: Views from experts around the world. BMC Med. 2014, 12, 112. [Google Scholar] [CrossRef] [PubMed]
- Trichopoulou, A.; Lagiou, P. Healthy traditional Mediterranean diet: An expression of culture, history, and lifestyle. Nutr. Rev. 1997, 55, 383–389. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Sacks, F.; Trichopoulou, A.; Drescher, G.; Ferro-Luzzi, A.; Helsing, E.; Trichopoulos, D. Mediterranean diet pyramid: A cultural model for healthy eating. Am. J. Clin. Nutr. 1995, 61, 1402S–1406S. [Google Scholar] [CrossRef]
- Tosti, V.; Bertozzi, B.; Fontana, L. Health Benefits of the Mediterranean Diet: Metabolic and Molecular Mechanisms. J. Gerontol. Ser. A 2018, 73, 318–326. [Google Scholar] [CrossRef]
- Bach-Faig, A.; Berry, E.M.; Lairon, D.; Reguant, J.; Trichopoulou, A.; Dernini, S.; Medina, F.X.; Battino, M.; Belahsen, R.; Miranda, G.; et al. Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr. 2011, 14, 2274–2284. [Google Scholar] [CrossRef]
- Keys, A.; Mienotti, A.; Karvonen, M.J.; Aravanis, C.; Blackburn, H.; Buzina, R.; Djordjevic, B.; Dontas, A.; Fidanza, F.; Keys, M.H. The diet and 15-year death rate in the seven countries study. Am. J. Epidemiol. 1986, 124, 903–915. [Google Scholar] [CrossRef]
- Trichopoulou, A. Traditional Mediterranean diet and longevity in the elderly: A review. Public Health Nutr. 2004, 7, 943–947. [Google Scholar] [CrossRef] [PubMed]
- Serra-Majem, L.; Roman, B.; Estruch, R. Scientific evidence of interventions using the Mediterranean diet: A systematic review. Nutr. Rev. 2006, 64, S27–S47. [Google Scholar] [CrossRef]
- Dinu, M.; Pagliai, G.; Casini, A.; Sofi, F. Mediterranean diet and multiple health outcomes: An umbrella review of meta-analyses of observational studies and randomised trials. Eur. J. Clin. Nutr. 2018, 72, 30–43. [Google Scholar] [CrossRef]
- Kris-Etherton, P.; Eckel, R.H.; Howard, B.V.; St. Jeor, S.; Bazzarre, T.L. AHA Science Adivsory: Lyon diet heart study: Benefits of a Mediterranean-Style, National Cholesterol Education Program/American Heart Association Step I dietary pattern on cardiovascular disease. Circulation 2001, 103, 1823–1825. [Google Scholar] [CrossRef] [PubMed]
- Martínez-González, M.A.; Bes-Rastrollo, M.; Serra-Majem, L.; Lairon, D.; Estruch, R.; Trichopoulou, A. Mediterranean food pattern and the primary prevention of chronic disease: Recent developments. Nutr. Rev. 2009, 67, S111–S116. [Google Scholar] [CrossRef] [PubMed]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.I.; Corella, D.; Arós, F. Primary prevention of cardiovascular disease with a Mediterranean diet. N. Engl. J. Med. 2013, 368, 1279–1290. [Google Scholar] [CrossRef] [PubMed]
- PREDIMED Study. Available online: http://www.predimed.es (accessed on 24 July 2019).
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.I.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; Fiol, M.; Lapetra, J.; et al. PREDIMED Study Investigators, Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Supplemented with Extra-Virgin Olive Oil or Nuts. N. Engl. J. Med. 2018, 378, e34. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Ros, E.; Covas, M.I.; Fiol, M.; Warnberg, J.; Arós, F.; Ruiz-Gutiérrez, V.; Lamuela-Raventos, R.M.; et al. Cohort profile: Design and methods of the PREDIMED study. Int. J. Epidemiol. 2012, 41, 377–385. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Garcia-Arellano, A.; Toledo, E.; Salas-Salvadó, J.; Buil-Cosiales, P.; Corella, D.; Covas, M.I.; Schroder, H.; Arós, F.; Gomez-Gracia, E.; et al. PREDIMED Study Investigators, A 14-item Mediterranean diet assessment tool and obesity indexes among high-risk subjects: The PREDIMED trial. PLoS ONE 2012, 7, e43134. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Salas-Salvadó, J.; Estruch, R.; Corella, D.; Fitó, M.; Ros, E. PREDIMED Investigators, Benefits of the Mediterranean Diet: Insights From the PREDIMED Study. Prog. Cardiovasc. Dis. 2015, 58, 50–60. [Google Scholar] [CrossRef]
- Sackett, D.L.; Rosenberg, W.M.; Gray, J.M.; Haynes, R.B.; Richardson, W.S. Evidence based medicine: What it is and what it isn’t. BMJ 1996, 312, 71–72. [Google Scholar] [CrossRef]
- Papadaki, A.; Martnez-Gonzalez, M.A.; Alonso-Gomez, A.; Rekondo, J.; Salas-Salvadó, J.; Corella, D.; Ros, E.; Fitó, M.; Estruch, R.; Lapetra, J.; et al. Mediterranean diet and risk of heart failure: Results from the PREDIMED randomized controlled trial. Eur. J. Heart Fail. 2017, 19, 1179–1185. [Google Scholar] [CrossRef]
- Papadaki, A.; Martínez-González, M.A.; Alonso-Gomez, A.; Rekondo, J.; Salas-Salvadó, J.; Corella, D.; Ros, E.; Fitó, M.; Estruch, R.; Lapetra, J.; et al. Erratum for Mediterranean diet and risk of heart failure: Results from the PREDIMED randomized controlled trial. Eur. J. Heart Fail. 2019, 21, 389–391. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Toledo, E.; Arós, F.; Fiol, M.; Corella, D.; Salas-Salvadó, J.; Ros, E.; Covas, M.I.; Fernandez-Crehuet, J.; Lapetra, J.; et al. PREDIMED Investigators, Extravirgin olive oil consumption reduces risk of atrial fibrillation: The PREDIMED (Prevencion con Dieta Mediterranea) trial. Circulation 2014, 130, 18–26. [Google Scholar] [CrossRef] [PubMed]
- Hernáez, A.; Castañer, O.; Goday, A.; Ros, E.; Pintó, X.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Arós, F.; Serra-Majem, L.; et al. The Mediterranean Diet decreases LDL atherogenicity in high cardiovascular risk individuals: A randomized controlled trial. Mol. Nutr. Food Res. 2017, 61, 1601015. [Google Scholar] [CrossRef] [PubMed]
- Storniolo, C.E.; Casillas, R.; Bullo, M.; Castaner, O.; Ros, E.; Saez, G.T.; Toledo, E.; Estruch, R.; Ruiz-Gutiérrez, V.; Fitó, M.; et al. A Mediterranean diet supplemented with extra virgin olive oil or nuts improves endothelial markers involved in blood pressure control in hypertensive women. Eur. J. Nutr. 2017, 56, 89–97. [Google Scholar] [CrossRef] [PubMed]
- Medina-Remon, A.; Tresserra-Rimbau, A.; Pons, A.; Tur, J.A.; Martorell, M.; Ros, E.; Buil-Cosiales, P.; Sacanella, E.; Covas, M.I.; Corella, D.; et al. Effects of total dietary polyphenols on plasma nitric oxide and blood pressure in a high cardiovascular risk cohort. The PREDIMED randomized trial. Nutr. Metab. Cardiovasc. Dis. 2015, 25, 60–67. [Google Scholar] [CrossRef]
- Casas, R.; Sacanella, E.; Urpí-Sardà, M.; Chiva-Blanch, G.; Ros, E.; Martínez-González, M.-A.; Covas, M.-I.; Lamuela-Raventos, R.M.; Salas-Salvadó, J.; Fiol, M.; et al. The effects of the mediterranean diet on biomarkers of vascular wall inflammation and plaque vulnerability in subjects with high risk for cardiovascular disease. A randomized trial. PLoS ONE 2014, 9, e100084. [Google Scholar] [CrossRef]
- Doménech, M.; Roman, P.; Lapetra, J.; García de la Corte, F.J.; Sala-Vila, A.; de la Torre, R.; Corella, D.; Salas-Salvadó, J.; Ruiz-Gutiérrez, V.; Lamuela-Raventós, R.M.; et al. Mediterranean diet reduces 24-h ambulatory blood pressure, blood glucose, and lipids: One-year randomized, clinical trial. Hypertension 2014, 64, 69–76. [Google Scholar] [CrossRef]
- Fitó, M.; Estruch, R.; Salas-Salvadó, J.; Martínez-González, M.A.; Arós, F.; Vila, J.; Corella, D.; Díaz, O.; Saez, G.; de la Torre, R.; et al. PREDIMED Study Investigators, Effect of the Mediterranean diet on heart failure biomarkers: A randomized sample from the PREDIMED trial. Eur. J. Heart. Fail. 2014, 16, 543–550. [Google Scholar] [CrossRef]
- Ruiz-Canela, M.; Estruch, R.; Corella, D.; Salas-Salvadó, J.; Martínez-González, M.A. Association of Mediterranean diet with peripheral artery disease: The PREDIMED randomized trial. Jama 2014, 311, 415–417. [Google Scholar] [CrossRef]
- Toledo, E.; Hu, F.B.; Estruch, R.; Buil-Cosiales, P.; Corella, D.; Salas-Salvadó, J.; Covas, M.I.; Arós, F.; Gómez-Gracia, E.; Fiol, M.; et al. Effect of the Mediterranean diet on blood pressure in the PREDIMED trial: Results from a randomized controlled trial. BMC Med. 2013, 11, 207. [Google Scholar] [CrossRef]
- Murie-Fernandez, M.; Irimia, P.; Toledo, E.; Martínez-Vila, E.; Buil-Cosiales, P.; Serrano-Martínez, M.; Ruiz-Gutiérrez, V.; Ros, E.; Estruch, R.; Martínez-González, M.A. PREDIMED Investigators, Carotid intima-media thickness changes with Mediterranean diet: A randomized trial (PREDIMED-Navarra). Atherosclerosis 2011, 219, 158–162. [Google Scholar] [CrossRef]
- Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Ruiz-Gutiérrez, V.; Covas, M.I.; Fiol, M.; Gómez-Gracia, E.; López-Sabater, M.C.; Vinyoles, E.; et al. Effects of a Mediterranean-style diet on cardiovascular risk factors: A randomized trial. Ann. Int. Med. 2006, 145, 1–11. [Google Scholar] [CrossRef]
- Basterra-Gortari, F.J.; Ruiz-Canela, M.; Martínez-González, M.A.; Babio, N.; Sorlí, J.V.; Fitó, M.; Ros, E.; Gómez-Gracia, E.; Fiol, M.; Lapetra, J.; et al. PREDIMED Study Investigators, Effects of a Mediterranean Eating Plan on the Need for Glucose-Lowering Medications in Participants With Type 2 Diabetes: A Subgroup Analysis of the PREDIMED Trial. Diabetes Care 2019, 42, 1390–1397. [Google Scholar] [CrossRef]
- Díaz-López, A.; Babio, N.; Martínez-González, M.A.; Corella, D.; Amor, A.J.; Fitó, M.; Estruch, R.; Arós, F.; Gómez-Gracia, E.; Fiol, M. Mediterranean diet, retinopathy, nephropathy, and microvascular diabetes complications: A post hoc analysis of a randomized trial. Diabetes Care 2015, 38, 2134–2141. [Google Scholar] [CrossRef]
- Díaz-López, A.; Babio, N.; Martínez-González, M.A.; Corella, D.; Amor, A.J.; Fitó, M.; Estruch, R.; Arós, F.; Gomez-Gracia, E.; Fiol, M.; et al. PREDIMED Study Investigators, Erratum. Mediterranean Diet, Retinopathy, Nephropathy, and Microvascular Diabetes Complications: A Post Hoc Analysis of a Randomized Trial. Diabetes Care 2018, 41, 2260–2261. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Bulló, M.; Estruch, R.; Ros, E.; Covas, M.I.; Ibarrola-Jurado, N.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; et al. PREDIMED Study Investigators, Prevention of diabetes with Mediterranean diets. Ann. Int. Med. 2014, 160, 1–10. [Google Scholar] [CrossRef]
- Sureda, A.; Bibiloni, M.D.; Martorell, M.; Buil-Cosiales, P.; Marti, A.; Pons, A.; Tur, J.A.; Martínez-González, M.A. PREDIMED Study Investigators, Mediterranean diets supplemented with virgin olive oil and nuts enhance plasmatic antioxidant capabilities and decrease xanthine oxidase activity in people with metabolic syndrome: The PREDIMED study. Mol. Nutr. Food. Res. 2016, 60, 2654–2664. [Google Scholar] [CrossRef]
- Babio, N.; Toledo, E.; Estruch, R.; Ros, E.; Martínez-González, M.A.; Castañer, O.; Bulló, M.; Corella, D.; Arós, F.; Gómez-Gracia, E.; et al. Mediterranean diets and metabolic syndrome status in the PREDIMED randomized trial. CMAJ 2014, 186, E649–E657. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Fernández-Ballart, J.; Ros, E.; Martínez-González, M.-A.; Fitó, M.; Estruch, R.; Corella, D.; Fiol, M.; Gómez-Gracia, E.; Arós, F. Effect of a Mediterranean diet supplemented with nuts on metabolic syndrome status: One-year results of the PREDIMED randomized trial. Arch. Int. Med. 2008, 168, 2449–2458. [Google Scholar] [CrossRef]
- Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Fitó, M.; Chiva-Blanch, G.; Fiol, M.; Gómez-Gracia, E.; Arós, F.; Lapetra, J.; et al. Effect of a high-fat Mediterranean diet on bodyweight and waist circumference: A prespecified secondary outcomes analysis of the PREDIMED randomised controlled trial. Lancet Diabetes Endocrinol. 2019, 7, e6–e17. [Google Scholar] [CrossRef]
- Álvarez-Pérez, J.; Sánchez-Villegas, A.; Díaz-Benítez, E.M.; Ruano-Rodriguez, C.; Corella, D.; Martínez-González, M.A.; Estruch, R.; Salas-Salvadó, J.; Serra-Majem, L. PREDIMED Study Investigators, Influence of a Mediterranean Dietary Pattern on Body Fat Distribution: Results of the PREDIMED-Canarias Intervention Randomized Trial. J. Am. Coll. Nutr. 2016, 35, 568–580. [Google Scholar] [CrossRef]
- Razquín, C.; Martínez, J.A.; Martínez-González, M.A.; Mitjavila, M.T.; Estruch, R.; Marti, A. A 3 years follow-up of a Mediterranean diet rich in virgin olive oil is associated with high plasma antioxidant capacity and reduced body weight gain. Eur. J. Clin. Nutr. 2009, 63, 1387–1393. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Lapiscina, E.H.; Clavero, P.; Toledo, E.; Estruch, R.; Salas-Salvadó, J.; San Julián, B.; Sanchez-Tainta, A.; Ros, E.; Valls-Pedret, C.; Martínez-González, M.Á. Mediterranean diet improves cognition: The PREDIMED-NAVARRA randomised trial. J. Neurol. Neurosurg. Psychiatry 2013, 84, 1318–1325. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Lapiscina, E.H.; Clavero, P.; Toledo, E.; San Julian, B.; Sanchez-Tainta, A.; Corella, D.; Lamuela-Raventos, R.; Martínez, J.; Martínez-González, M.A. Virgin olive oil supplementation and long-term cognition: The PREDIMED-NAVARRA randomized, trial. J. Nutr. Health Aging 2013, 17, 544–552. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Villegas, A.; Martínez-González, M.A.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Covas, M.I.; Arós, F.; Romaguera, D.; Gómez-Gracia, E.; Lapetra, J.; et al. Mediterranean dietary pattern and depression: The PREDIMED randomized trial. BMC Med. 2013, 11, 208. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Villegas, A.; Galbete, C.; Martínez-González, M.A.; Martínez, J.A.; Razquin, C.; Salas-Salvadó, J.; Estruch, R.; Buil-Cosiales, P.; Martí, A. The effect of the Mediterranean diet on plasma brain-derived neurotrophic factor (BDNF) levels: The PREDIMED-NAVARRA randomized trial. Nutr. Neurosci. 2011, 14, 195–201. [Google Scholar] [CrossRef]
- Pintó, X.; Fanlo-Maresma, M.; Corbella, E.; Corbella, X.; Mitjavila, M.T.; Moreno, J.J.; Casas, R.; Estruch, R.; Corella, D.; Bulló, M.; et al. A Mediterranean Diet Rich in Extra-Virgin Olive Oil Is Associated with a Reduced Prevalence of Nonalcoholic Fatty Liver Disease in Older Individuals at High Cardiovascular Risk. J. Nutr. 2019, 149, 1920–1929. [Google Scholar] [CrossRef]
- Cueto-Galán, R.; Barón, F.J.; Valdivielso, P.; Pintó, X.; Corbella, E.; Gómez-Gracia, E.; Wärnberg, J. Changes in fatty liver index after consuming a Mediterranean diet: 6-Year follow-up of the PREDIMED-Malaga trial. Med. Clin. 2017, 148, 435–443. [Google Scholar] [CrossRef]
- García-Layana, A.; Ciufo, G.; Toledo, E.; Martínez-González, M.; Corella, D.; Fitó, M.; Estruch, R.; Gómez-Gracia, E.; Fiol, M.; Lapetra, J.; et al. The effect of a Mediterranean diet on the incidence of cataract surgery. Nutrients 2017, 9, 453. [Google Scholar] [CrossRef]
- Hernáez, Á.; Castañer, O.; Elosua, R.; Pintó, X.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; Arós, F.; Serra-Majem, L.; Fiol, M.; et al. Mediterranean diet improves high-density lipoprotein function in high-cardiovascular-risk individuals: A randomized controlled trial. Circulation 2017, 135, 633–643. [Google Scholar] [CrossRef]
- Casas, R.; Sacanella, E.; Urpí-Sardà, M.; Corella, D.; Castaner, O.; Lamuela-Raventos, R.-M.; Salas-Salvadó, J.; Martínez-González, M.-A.; Ros, E.; Estruch, R. Long-term immunomodulatory effects of a Mediterranean diet in adults at high risk of cardiovascular disease in the PREvención con DIeta MEDiterránea (PREDIMED) randomized controlled trial. J. Nutr. 2016, 146, 1684–1693. [Google Scholar] [CrossRef]
- García-Calzón, S.; Martínez-González, M.A.; Razquin, C.; Arós, F.; Lapetra, J.; Martínez, J.A.; Zalba, G.; Marti, A. Mediterranean diet and telomere length in high cardiovascular risk subjects from the PREDIMED-NAVARRA study. Clin. Nutr. 2016, 35, 1399–1405. [Google Scholar] [CrossRef] [PubMed]
- Toledo, E.; Salas-Salvadó, J.; Donat-Vargas, C.; Buil-Cosiales, P.; Estruch, R.; Ros, E.; Corella, D.; Fitó, M.; Hu, F.B.; Arós, F.; et al. Mediterranean diet and invasive breast cancer risk among women at high cardiovascular risk in the PREDIMED trial: A randomized clinical trial. JAMA Int. Med. 2015, 175, 1752–1760. [Google Scholar] [CrossRef] [PubMed]
- Damasceno, N.R.; Sala-Vila, A.; Cofán, M.; Pérez-Heras, A.M.; Fitó, M.; Ruiz-Gutiérrez, V.; Martínez-González, M.-Á.; Corella, D.; Arós, F.; Estruch, R.; et al. Mediterranean diet supplemented with nuts reduces waist circumference and shifts lipoprotein subfractions to a less atherogenic pattern in subjects at high cardiovascular risk. Atherosclerosis 2013, 230, 347–353. [Google Scholar] [CrossRef] [PubMed]
- Zamora-Ros, R.; Serafini, M.; Estruch, R.; Lamuela-Raventós, R.; Martínez-González, M.; Salas-Salvadó, J.; Fiol, M.; Lapetra, J.; Arós, F.; Covas, M.; et al. PREDIMED Study Investigators, Mediterranean diet and non enzymatic antioxidant capacity in the PREDIMED study: Evidence for a mechanism of antioxidant tuning. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 1167–1174. [Google Scholar] [CrossRef] [PubMed]
- Mitjavila, M.T.; Fandos, M.; Salas-Salvadó, J.; Covas, M.-I.; Borrego, S.; Estruch, R.; Lamuela-Raventós, R.; Corella, D.; Martínez-Gonzalez, M.Á.; Sánchez, J.M.; et al. The Mediterranean diet improves the systemic lipid and DNA oxidative damage in metabolic syndrome individuals. A randomized, controlled, trial. Clin. Nutr. 2013, 32, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Solá, R.; Fitó, M.; Estruch, R.; Salas-Salvadó, J.; Corella, D.; de La Torre, R.; Muñoz, M.A.; Lopez-Sabater Mdel, C.; Martínez-González, M.A.; Arós, F.; et al. Effect of a traditional Mediterranean diet on apolipoproteins B, A-I, and their ratio: A randomized, controlled trial. Atherosclerosis 2011, 218, 174–180. [Google Scholar] [CrossRef]
- Perona, J.S.; Covas, M.-I.; Fitó, M.; Cabello-Moruno, R.; Arós, F.; Corella, D.; Ros, E.; Garcia, M.; Estruch, R.; Martínez-González, M.A.; et al. Reduction in systemic and VLDL triacylglycerol concentration after a 3-month Mediterranean-style diet in high-cardiovascular-risk subjects. J. Nutr. Biochem. 2010, 21, 892–898. [Google Scholar] [CrossRef]
- Escurriol, V.; Cofán, M.; Serra, M.; Bulló, M.; Basora, J.; Salas-Salvadó, J.; Corella, D.; Zazpe, I.; Martínez-González, M.A.; Ruiz-Gutiérrez, V.; et al. Serum sterol responses to increasing plant sterol intake from natural foods in the Mediterranean diet. Eur. J. Nutr. 2009, 48, 373–382. [Google Scholar] [CrossRef]
- Fitó, M.; Guxens, M.; Corella, D.; Sáez, G.; Estruch, R.; de la Torre, R.; Francés, F.; Cabezas, C.; del Carmen López-Sabater, M.; Marrugat, J.; et al. PREDIMED Study Investigators, Effect of a traditional Mediterranean diet on lipoprotein oxidation: A randomized controlled trial. Arch. Int. Med. 2007, 167, 1195–1203. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Estruch, R.; Corella, D.; Ros, E.; Salas-Salvadó, J. Prevention of diabetes with mediterranean diets. Ann. Int. Med. 2014, 161, 157–158. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Bulló, M.; Babio, N.; Martínez-González, M.A.; Ibarrola-Jurado, N.; Basora, J.; Estruch, R.; Covas, M.I.; Corella, D.; Arós, F.; et al. PREDIMED Study Investigators, Reduction in the incidence of type 2 diabetes with the Mediterranean diet: Results of the PREDIMED-Reus nutrition intervention randomized trial. Diabetes Care 2011, 34, 14–19. [Google Scholar] [CrossRef] [PubMed]
- Salas-Salvadó, J.; Bulló, M.; Babio, N.; Martínez-González, M.A.; Ibarrola-Jurado, N.; Basora, J.; Estruch, R.; Covas, M.I.; Corella, D.; Arós, F.; et al. PREDIMED Study Investigators, Erratum. Reduction in the Incidence of Type 2 Diabetes With the Mediterranean Diet: Results of the PREDIMED-Reus nutrition intervention randomized trial. Diabetes Care 2018, 41, 2259–2260. [Google Scholar] [CrossRef] [PubMed]
- Liyanage, T.; Ninomiya, T.; Wang, A.; Neal, B.; Jun, M.; Wong, M.G.; Jardine, M.; Hillis, G.S.; Perkovic, V. Effects of the Mediterranean Diet on Cardiovascular Outcomes-A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0159252. [Google Scholar] [CrossRef] [PubMed]
- Salas-Salvadó, J.; Guasch-Ferre, M.; Lee, C.H.; Estruch, R.; Clish, C.B.; Ros, E. Protective Effects of the Mediterranean Diet on Type 2 Diabetes and Metabolic Syndrome. J. Nutr. 2016, 146, 920S–927S. [Google Scholar] [CrossRef] [PubMed]
- Esposito, K.; Maiorino, M.I.; Bellastella, G.; Chiodini, P.; Panagiotakos, D.; Giugliano, D. A journey into a Mediterranean diet and type 2 diabetes: A systematic review with meta-analyses. BMJ Open 2015, 5, e008222. [Google Scholar] [CrossRef]
- Rumawas, M.E.; Meigs, J.B.; Dwyer, J.T.; McKeown, N.M.; Jacques, P.F. Mediterranean-style dietary pattern, reduced risk of metabolic syndrome traits, and incidence in the Framingham Offspring Cohort. Am. J. Clin. Nutr. 2009, 90, 1608–1614. [Google Scholar] [CrossRef]
- Petersson, S.D.; Philippou, E. Mediterranean Diet, Cognitive Function, and Dementia: A Systematic Review of the Evidence. Adv. Nutr. 2016, 7, 889–940. [Google Scholar] [CrossRef]
- Van der Brandt, P.A.; Schulpen, M. Mediterranean diet adherence and risk of portmenopausal breast cancer: Results of a cohort study and meta-analysis. Int. J. Cancer 2017, 140, 2220–2231. [Google Scholar] [CrossRef]
- Turati, F.; Cairoli, G.; Bravi, F.; Ferraroni, M.; Serraino, D.; Montella, M. Mediterranean Diet and Breast Cancer Risk. Nutrients 2018, 10, 326. [Google Scholar] [CrossRef]
| Aim of the Study | Number of Subjects | Follow-Up Median (Years) | Main Results of the Study | 1st Author, Journal, Year | Ref. |
|---|---|---|---|---|---|
| Cardiovascular Disease | |||||
| Incidence of primary endpoint (a composite of CV events: Non-fatal acute myocardial infarction, non-fatal stroke or death from CV causes) | 7447 | 4.8 | 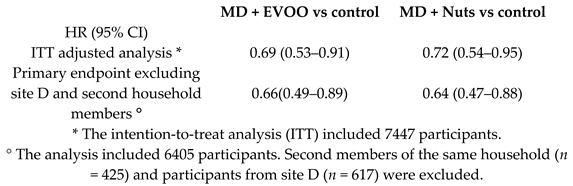 | Estruch et al. N. Engl. J. Med. 2018 | [15] |
| Incidence of heart failure | 7403 | 4.8 |  | Papadaki et al. Eur. J. Heart. Fail. 2017 | [20] |
| Papadaki et al. Eur. J. Heart. Fail. 2019 | [21] | ||||
| Incidence of atrial fibrillation | 6705 | 4.7 | 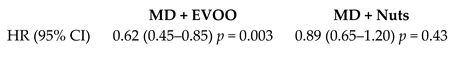 | Martínez-González et al. Circulation 2014 | [22] |
| Cardiovascular Risk Factors | |||||
| Long-term consumption of a MD could decrease the atherogenicity of LDL particles | 210 | 1.0 | 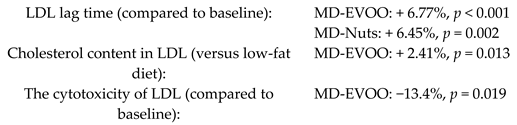 | Hernaez et al. Mol. Nutr. Food Res. 2017 | [23] |
| Improvement of BP induced by a MD would be mediated by the modulation of NO bioavailability/ET-1 levels | 90 Non-smoking women with moderate hypertension | 1.0 | 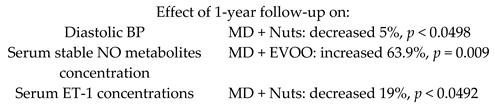 | Storniolo et al. Eur. J. Nutr. 2017 | [24] |
| Effects of high polyphenol consumption on BP and its relation about production of plasma NO | 200 | 1.0 |  | Medina-Remón et al. Nutr. Metab. Cardiovasc Dis. 2015 | [25] |
| Effects of MD on inflammatory biomarkers related to atherosclerosis and plaque vulnerability | 164 | 1.0 | 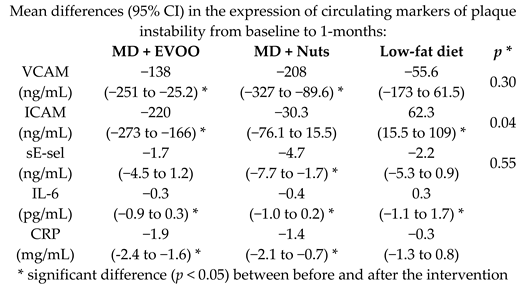 | Casas et al. PLoS ONE 2014 | [26] |
| MD effect on 24-h ambulatory BP, blood glucose, and lipids | 235 | 1.0 | 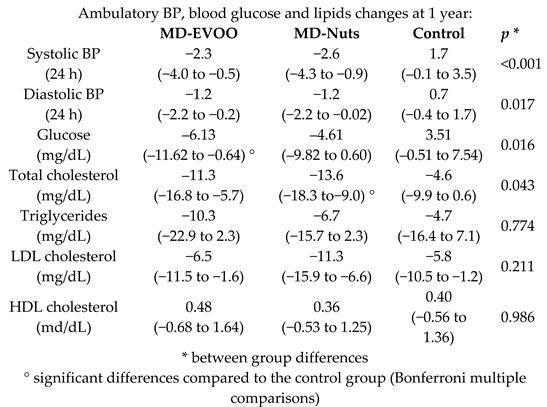 | Doménech et al. Hypertension 2014 | [27] |
| Effect of the MD on heart failure biomarkers | 930 | 1.0 | 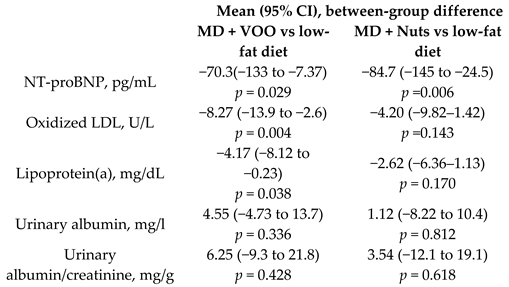 | Fitó et al. Eur. J. Heart Fail. 2014 | [28] |
| Incidence of Peripheral Artery Disease (PAD) | 7435 | 4.8 | 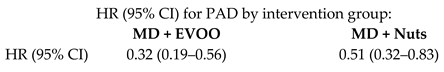 | Ruiz-Canela et al. JAMA 2014 | [29] |
| Effects of MD on BP | 7158 | 3.8 |  | Toledo et al. BMC medicine 2013 | [30] |
| Effects of MD on progression of subclinical carotid atherosclerosis | 187 | 1.0 |  | Murie-Fernández et al. Atherosclerosis 2011 | [31] |
| The short-term effects of MD versus those of a low-fat diet on intermediate markers of CV risk. | 772 | 0.25 | 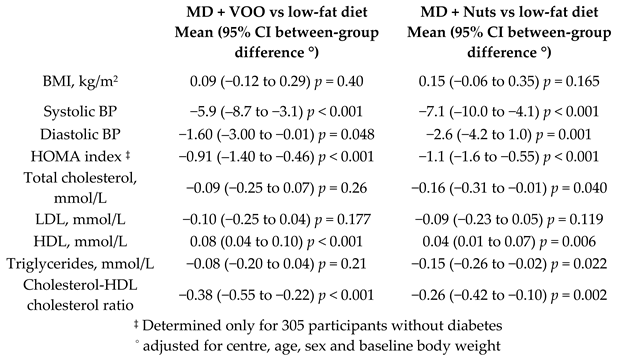 | Estruch et al. Ann. Int. Med. 2006 | [32] |
| Aim of the Study | Number of Subjects | Follow-Up Median (Years) | Main Results of the Study | 1st Author, Journal, Year | Ref. |
|---|---|---|---|---|---|
| Diabetes Mellitus | |||||
| Effects of MD versus a low-fat diet on the need for glucose-lowering medications | 3230 T2DM | 3.2 |  | Basterra-Gortari et al. Diab. Care. 2019 | [33] |
| Long-term effect of a MD on microvascular diabetes complications | 3614 T2DM | 6.0 | 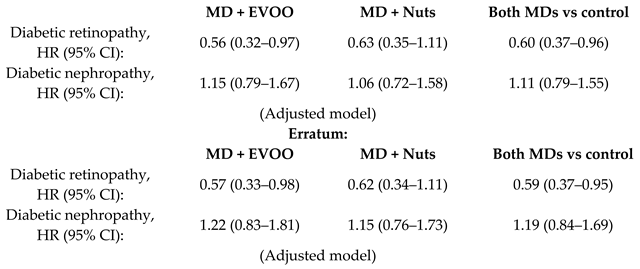 | Díaz-López et al. Diab. Care. 2015 | [34] |
| Díaz-López et al. Diab. Care. 2018 | [35] | ||||
| Incidence of diabetes | 3541 | 4.1 | 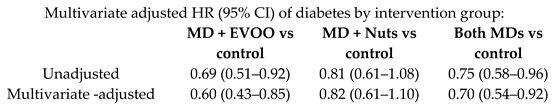 | Salas-Salvadó et al. Ann Int Med. 014 | [36] |
| Metabolic Syndrome | |||||
| Plasmatic antioxidant capabilities in Metabolic Syndrome (MetS) patients | 75 | 5.0 | 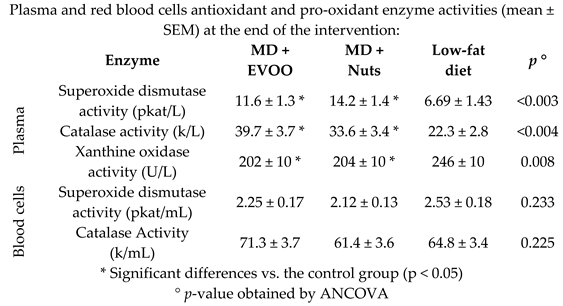 | Sureda et al. Mol. Nutr. Food Res. 2016 | [37] |
| Long-term effects of MD on MetS | 5801 | 4.8 |  | Babio et al. Cmaj 2014 | [38] |
| MD effects on MetS status | 1224 | 1.0 |  | Salas-Salvadó et al. Arch. Int. Med. 2008 | [39] |
| Obesity | |||||
| Effect of a MD on bodyweight and waist circumference | 3985 | 4.8 |  | Estruch et al. The Lancet. Diab. Endocr. 2019 | [40] |
| Effect of MD on anthropometric variables and body composition parameters | 305 | 1.0 | 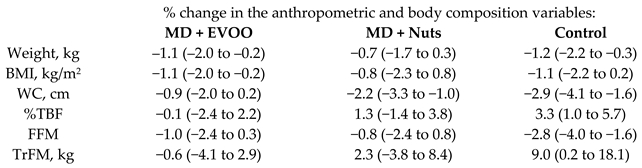 | Álvarez-Pérez et al. J. Am. Coll. Nutr. 2016 | [41] |
| Effect of MedD on plasma total antioxidant capacity (TAC) | 187 | 3.0 |  | Razquin et al. Eur. J. Clin. Nutr. 2009 | [42] |
| Aim of the Study | Number of Subjects | Follow-Up Median (Years) | Main Results of the Study | 1st Author, Journal, Year | Ref. |
|---|---|---|---|---|---|
| Neurologic Disorders | |||||
| Effect of MD on cognition | 522 | 6.5 | 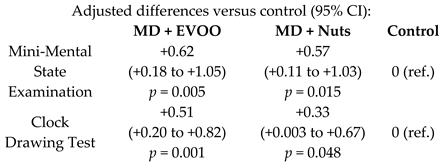 | Martínez-Lapiscina et al. J. Neurol. Neurosurg Psychiatry 2013 | [43] |
| Effect of MD on Mild Cognitive Impairment (MCI) | 268 | 6.5 | 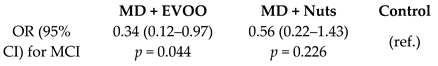 | Martínez-Lapiscina et al. J. Nutr. Health Aging 2013 | [44] |
| Effects of MD on depression risk | 3923 | 5.4 |  | Sánchez-Villegas et al. BMC medicine 2013 | [45] |
| Effect of MD on plasma Brain-Derived Neurotrophic Factor (BDNF) levels | 243 | 3 |  | Sánchez-Villegas et al. Nutr. Neurosci. 2011 | [46] |
| Other Conditions | |||||
| MD effect on liver steatosis | 100 | 3.0 |  | Pintó et al. J. Nutr. 2019 | [47] |
| MD effects on the Fatty Liver Index (FLI) | 276 | 6.0 |  | Cueto-Galán et al. Med. Clin. 2017 | [48] |
| Incidence of cataract surgery | 5802 | 5.9 | 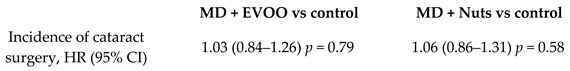 | García-Layana et al. Nutrients 2017 | [49] |
| Effect of MD on HDL properties | 296 | 1.0 | 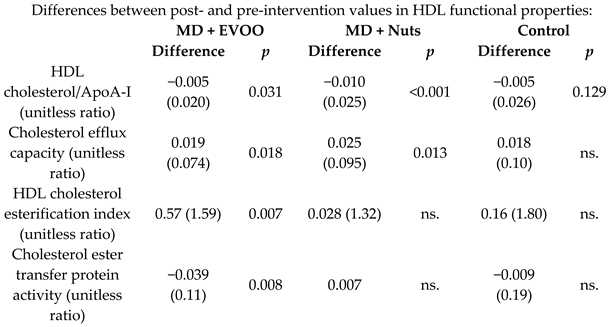 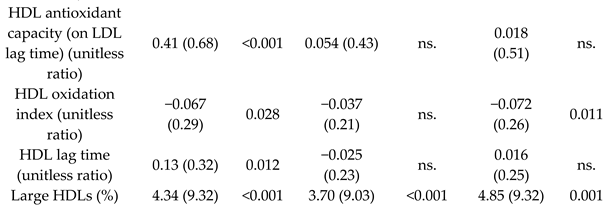 | Hernáez et al. Circulation 20 | [50] |
| Effect of the MD on inflammatory markers related to atherogenesis | 160 | 3.0 5.0 |  | Casas et al. J. Nutr. 2016 | [51] |
| Effect of MD on telomere lenght | 520 | 5.0 |  | García-Calzón et al. Clin. Nutr. 2016 | [52] |
| Breast cancer incidence | 4282 | 4.8 | 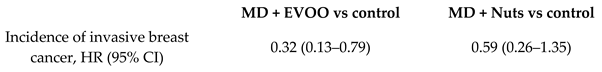 | Toledo et al. JAMA int. Med., 2015 | [53] |
| MD effect on lipoprotein subfractions | 169 | 1.0 | 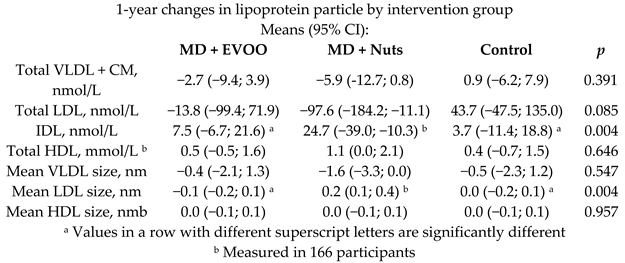 | Damasceno et al. Atherosclerosis 2013 | [54] |
| Effect of MD on plasma Non-Enzymatic Antioxidant Capacity (NEAC) | 564 | 1.0 | 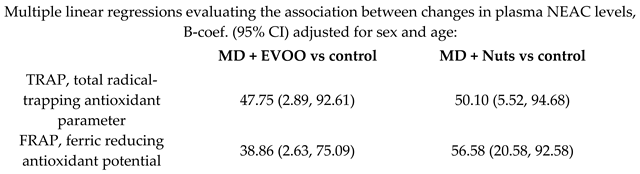 | Zamora-Ros et al. Nutr. Metab. Cardiovasc Dis. 2013 | [55] |
| Effect of the MD on systemic oxidative biomarkers in MetS individuals | 110 female participants with the diagnosis of MetS | 1.0 | 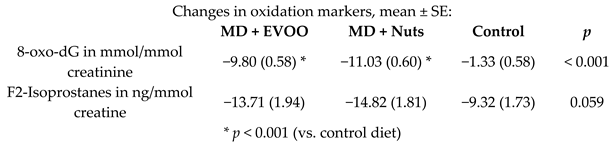 | Mitjavila et al. Clin. Nutr. 2013 | [56] |
| Effects of MD on apolipoproteins B, A-I, and their ratio | 551 | 0.25 | 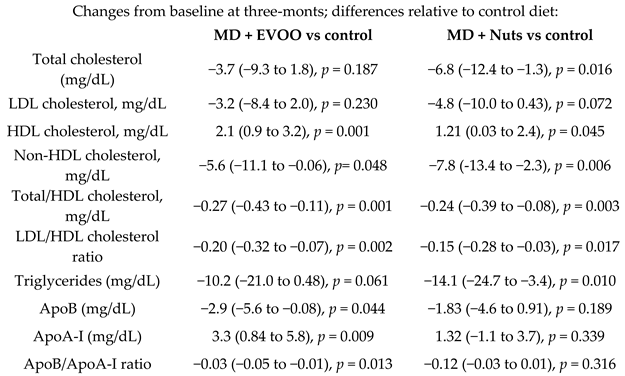 | Solá et al. Atherosclerosis 2011 | [57] |
| Effects of MD on VLDL concentration | 50 | 0.25 |  | Perona et al. J. Nutr. Biochem. 2010 | [58] |
| Phytosterol intake from natural foods association with a cholesterol- lowering effect of MD | 106 | 1.0 | 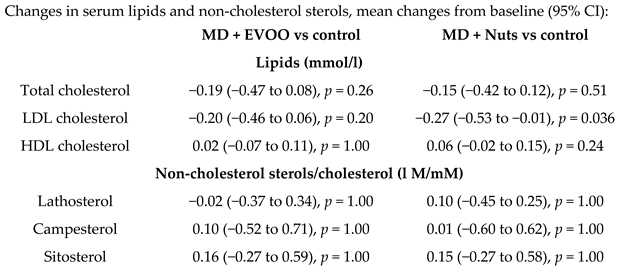 | Escurriol et al. Europ. J. Nutr. 2009 | [59] |
| Effects of MD on in vivo lipoprotein oxidation | 372 | 0.25 |  | Fitó et al. Arch. Int. Med. 2007 | [60] |
| MD + EVOO | MD + Nuts | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Continuous Variable | Time (yr) | N | Mean Value at Baseline | Mean Change | % Change from Baseline | p-Value * | N | Mean Value at Baseline | Mean Change | % Change from Baseline | p-Value * | Ref. |
| Sistolic BP (24 h) | 1.0 | 78 | 127.3 | −3.14 | −2.5% | - | 82 | 125.3 | −2.35 | −1.9% | - | [27] |
| Diastolic BP (24 h) | 1.0 | 78 | 71.8 | −1.68 | −2.3% | - | 82 | 71.2 | −1.00 | −1.4% | - | [27] |
| BMI, kg/m2 | 0.25 | 257 | 29.7 | −0.12 | −0.4% | - | 257 | 29.4 | −0.09 | −0.3% | - | [32] |
| Weight, kg | 1.0 | 112 | 77.9 | −1.0 | −1.3% | 0.008 | 102 | 80.3 | −0.5 | −0.6% | 0.197 | [41] |
| BMI, kg/m2 | 1.0 | 112 | 30.7 | −0.5 | −1.6% | 0.012 | 102 | 31.2 | −0.5 | −1.6% | 0.314 | [41] |
| WC, cm | 1.0 | 112 | 100.5 | −1.1 | −1.0% | 0.046 | 102 | 102.6 | −2.3 | −2.2% | <0.001 | [41] |
| Urinary albumin, mg/L | 1.0 | 310 | 5.0 | 0.55 | 11.0% | - | 310 | 5.1 | −2.85 | −55.9% | - | [28] |
| Urinary albumin/creatinine, mg/g | 1.0 | 310 | 7.09 | 1.13 | 15.9% | - | 310 | 7.21 | −1.62 | −22.5% | - | [28] |
| Intima-media thickness, mm | 1.0 | 66 | 0.825 | −0.016 | −1.9% | - | 59 | 0.854 | −0.033 | −3.8% | - | [31] |
| Total cholesterol, mg/dL | 0.25 | 181 | 219.7 | −3.7 | −1.7% | ns. | 193 | 216.7 | −6.8 | −3.1% | <0.05 | [57] |
| Oxidized LDL, U/L | 1.0 | 310 | 74.3 | −9.75 | −13.1% | - | 310 | 71.1 | −5.68 | −8.0% | - | [28] |
| Ox-LDL, U/L | 0.25 | 123 | 77.9 | −10.1 | −13.0% | - | 128 | 74.4 | −7.5 | −10.1% | - | [60] |
| LDL cholesterol, mg/dL | 0.25 | 181 | 146.2 | −4.3 | −2.9% | <0.05 | 193 | 141.6 | −5.9 | −4.2 | <0.05 | [57] |
| HDL cholesterol, mg/dL | 0.25 | 181 | 51.9 | 1.8 | +3.5% | <0.05 | 193 | 53.9 | 0.95 | 1.8% | <0.05 | [57] |
| Non-HDL cholesterol, mg/dL | 0.25 | 181 | 174.2 | −5.4 | −3.1% | <0.05 | 193 | 169.6 | −7.6 | −4.5% | <0.05 | [57] |
| Total/HDL cholesterol, mg/dL | 0.25 | 181 | 5.0 | −0.24 | −4.8% | <0.05 | 193 | 4.8 | −0.20 | −4.2% | <0.05 | [57] |
| LDL/HDL cholesterol ratio | 0.25 | 181 | 3.4 | −0.20 | −5.9% | <0.05 | 193 | 3.1 | −0.15 | −4.8% | <0.05 | [57] |
| Triglycerides, mg/dL | 0.25 | 181 | 139.9 | −4.8 | −3.4% | ns. | 193 | 138.2 | −8.62 | −6.2% | <0.05 | [57] |
| ApoB, mg/dL | 0.25 | 181 | 102 | −2.8 | −4.4% | <0.05 | 193 | 101 | −1.7 | −1.4% | ns. | [57] |
| ApoA-I, mg/dL | 0.25 | 181 | 135 | 2.5 | +3.2% | <0.05 | 193 | 134 | 0.16 | 1.4% | ns. | [57] |
| ApoB/ApoA-I ratio | 0.25 | 181 | 0.78 | −0.03 | −6.2% | <0.05 | 193 | 0.78 | −0.009 | −1.2% | ns. | [57] |
| Lipoprotein(a), mg/dL | 1.0 | 310 | 24.8 | 0.68 | 2.7% | - | 310 | 24.4 | 2.23 | 9.1% | - | [28] |
| NT-proBNP, pg/mL | 1.0 | 310 | 572 | −27.7 | −4.8% | - | 310 | 562 | −42.0 | −7.4% | - | [28] |
| GSH-Px, U/L | 0.25 | 123 | 626 | −16.4 | −2.6% | - | 128 | 613 | −10.4 | -1.7% | - | [60] |
| sVCAM-1, ng/mL | 1.0 | 55 | 872 | −138 | −15.8% | 0.02 | 55 | 935 | −208 | −22.2% | 0.001 | [26] |
| sICAM-1, ng/mL | 1.0 | 55 | 437 | −220 | −50.3% | <0.001 | 55 | 394 | −30.3 | −7.7% | 0.20 | [26] |
| sE-SEL, ng/mL | 1.0 | 55 | 28.6 | −1.7 | −5.9% | 0.26 | 55 | 33.0 | −4.7 | −14,2% | 0.003 | [26] |
| MCP-1, pg/mL vs. baseline | 3.0. | 55 | 4.3 | −1.4 | −32.6% | <0.05 | 55 | 4.6 | −0.7 | −15.2% | <0.05 | [51] |
| 5.0. | −1.2 | −28.0% | <0.05 | −1.4 | −30.4% | <0.05 | ||||||
| IL-6, pg/mL vs. baseline | 3.0 | 55 | 1.3 | −0.5 | −38.4% | <0.05 | 55 | 1.4 | −0.4 | −28.6% | <0.05 | [51] |
| 5.0 | −0.5 | −46.2% | <0.05 | −0.6 | −42.9% | <0.05 | ||||||
| TNF-α, pg/mL vs. baseline | 3.0 | 55 | 3.6 | 1.6 | −44.4% | <0.05 | 55 | 3.6 | −1.0 | −27.8% | <0.05 | [51] |
| 5.0 | −1.9 | −52.8% | <0.05 | −1.2 | −33.3% | <0.05 | ||||||
| Hs-CRP, g/L vs. baseline | 3.0 | 55 | 3.7 | −1.8 | −48.6% | <0.05 | 55 | 3.5 | −1.3 | −37.1% | <0.05 | [51] |
| 5.0 | −2.0 | −54.0% | <0.05 | −1.5 | −42.9% | <0.05 | ||||||
| 8-oxo-dG in mmol/mmol creatinine | 1.0 | 38 | 20.24 | −9.80 | −48.4% | <0.001 | 35 | 19.98 | −11.03 | −55.2% | <0.001 | [56] |
| F2-Isoprostanes in ng/mmol creatine | 1.0 | 38 | 76.15 | −13.71 | −18.0% | - | 35 | 97.40 | −14.82 | −15.2% | - | [56] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kargin, D.; Tomaino, L.; Serra-Majem, L. Experimental Outcomes of the Mediterranean Diet: Lessons Learned from the Predimed Randomized Controlled Trial. Nutrients 2019, 11, 2991. https://doi.org/10.3390/nu11122991
Kargin D, Tomaino L, Serra-Majem L. Experimental Outcomes of the Mediterranean Diet: Lessons Learned from the Predimed Randomized Controlled Trial. Nutrients. 2019; 11(12):2991. https://doi.org/10.3390/nu11122991
Chicago/Turabian StyleKargin, Dicle, Laura Tomaino, and Lluís Serra-Majem. 2019. "Experimental Outcomes of the Mediterranean Diet: Lessons Learned from the Predimed Randomized Controlled Trial" Nutrients 11, no. 12: 2991. https://doi.org/10.3390/nu11122991
APA StyleKargin, D., Tomaino, L., & Serra-Majem, L. (2019). Experimental Outcomes of the Mediterranean Diet: Lessons Learned from the Predimed Randomized Controlled Trial. Nutrients, 11(12), 2991. https://doi.org/10.3390/nu11122991






