Effect of Probiotics on Oral Candidiasis: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Systematic Review and Meta-Analysis
2.1. Materials and Methods
2.1.1. Literature Search
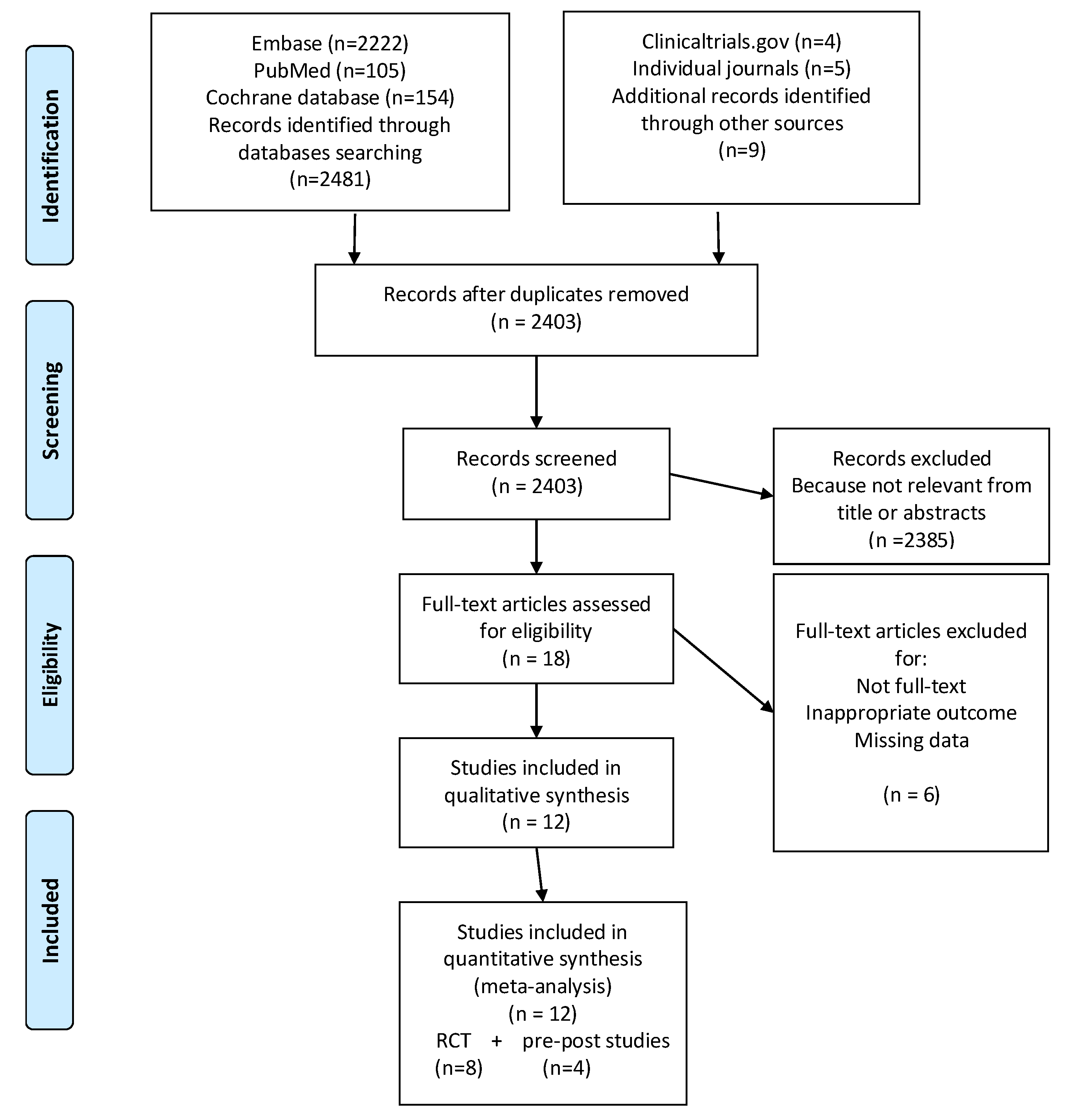
2.1.2. Study Selection
- (1)
- Randomized clinical trials or pre–post intervention studies;
- (2)
- Availability of full text;
- (3)
- Patients regardless of age, race, nationality, sex, and health status;
- (4)
- Comparison between oral intake of probiotics, prebiotics, or synbiotics (of any type and dosage) with a control treatment or a placebo in RCT; and between pre- and post-treatment conditions in pre–post intervention studies;
- (5)
- Outcome measurement expressed in CFU/mL of oral Candida spp. counts in saliva or palatal samples.
- (1)
- Studies with fewer than 10 participants;
- (2)
- Reviews, articles, and case reports;
- (3)
- Studies with incomplete outcome data;
- (4)
- Studies reporting results in a format which was not suitable for a meta-analysis, for example, without Candida spp. counts/carriage.
2.1.3. Data Extraction
2.1.4. Outcome Assessment
2.1.5. Risk of Bias
2.1.6. Statistical Analysis
2.2. Results
Study Selection
2.3. Characteristics of the Included Studies
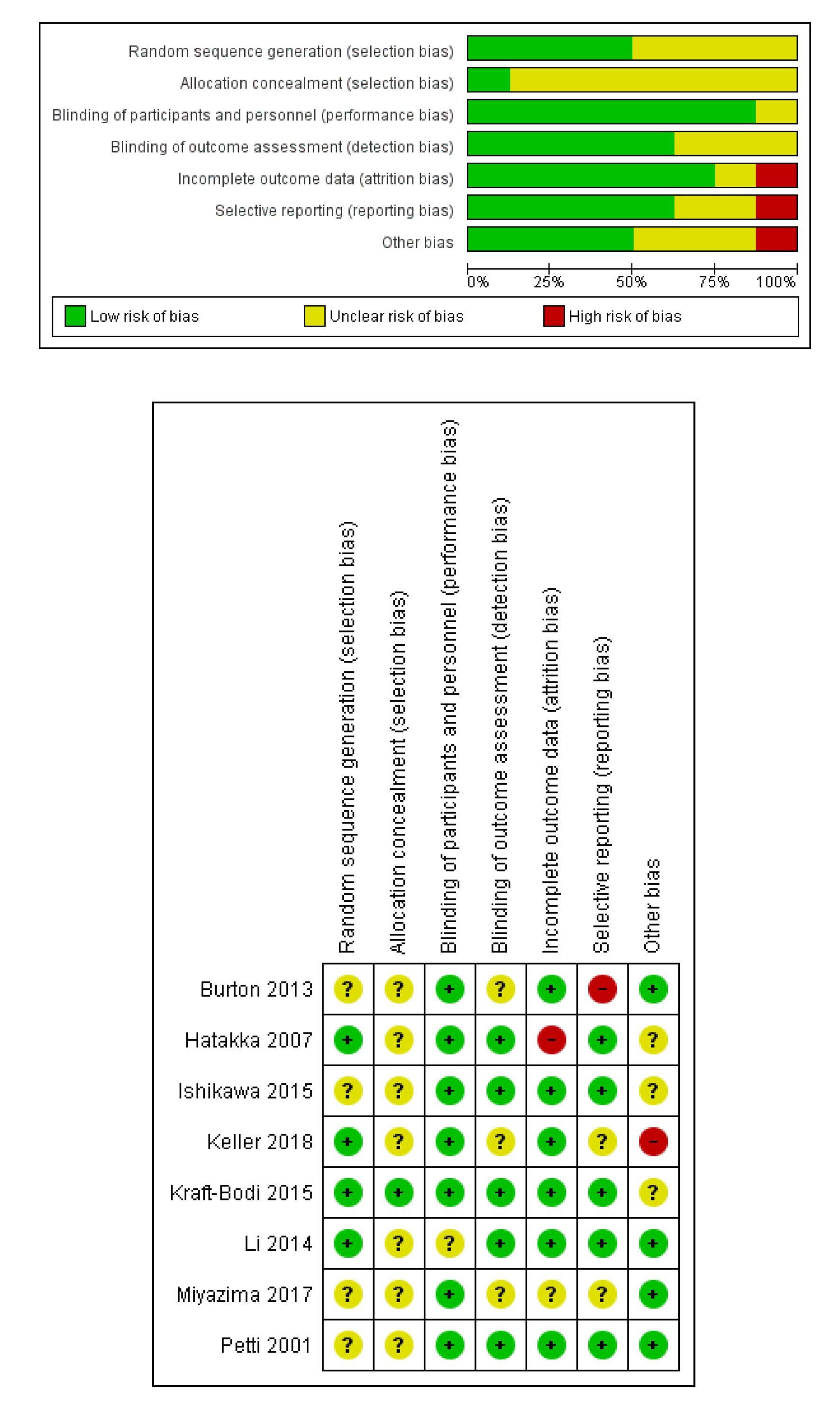
2.4. Evaluation of the Risk of Bias for RCTs
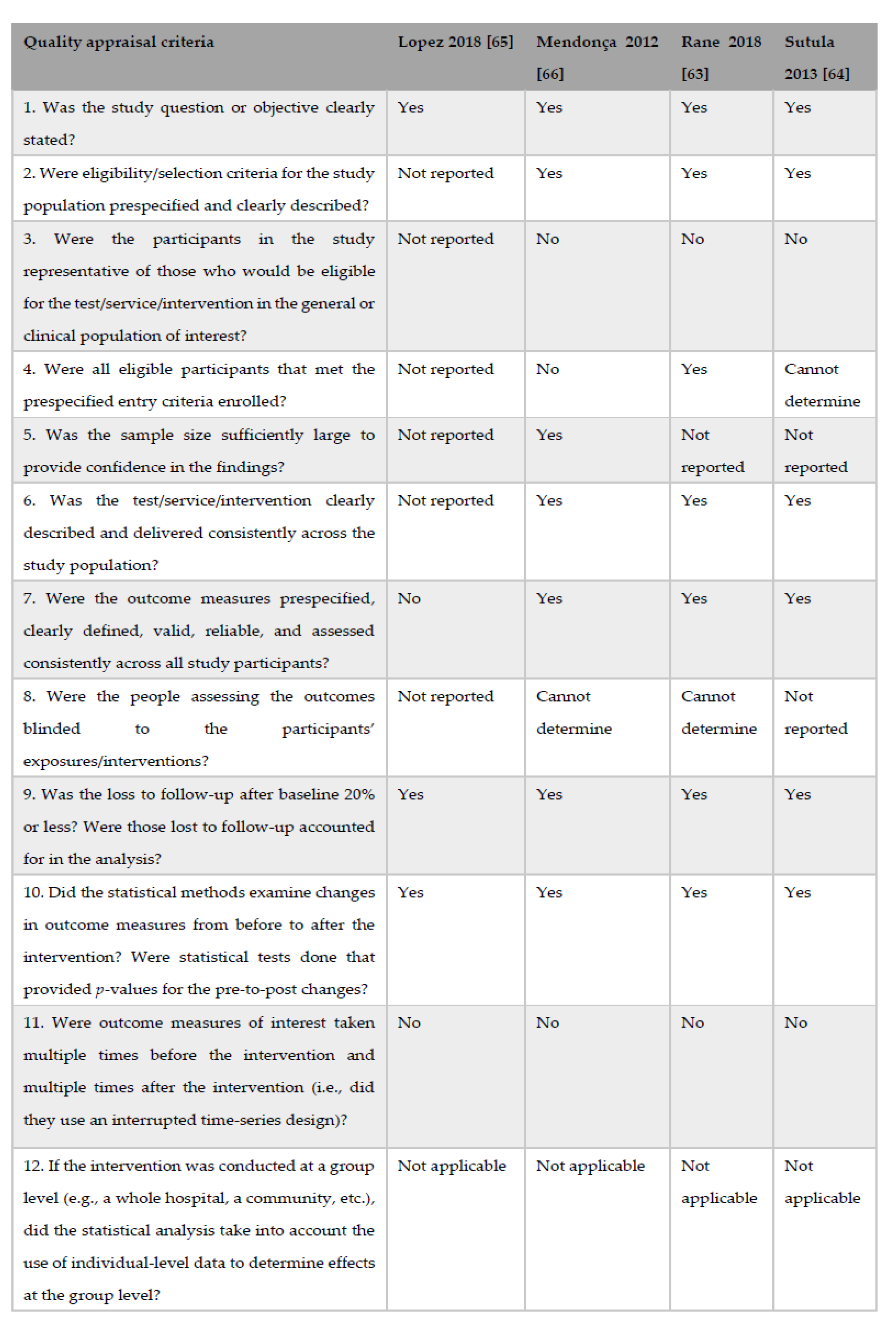
2.5. Evaluation of the Risk of Bias for Pre–Post Intervention Studies
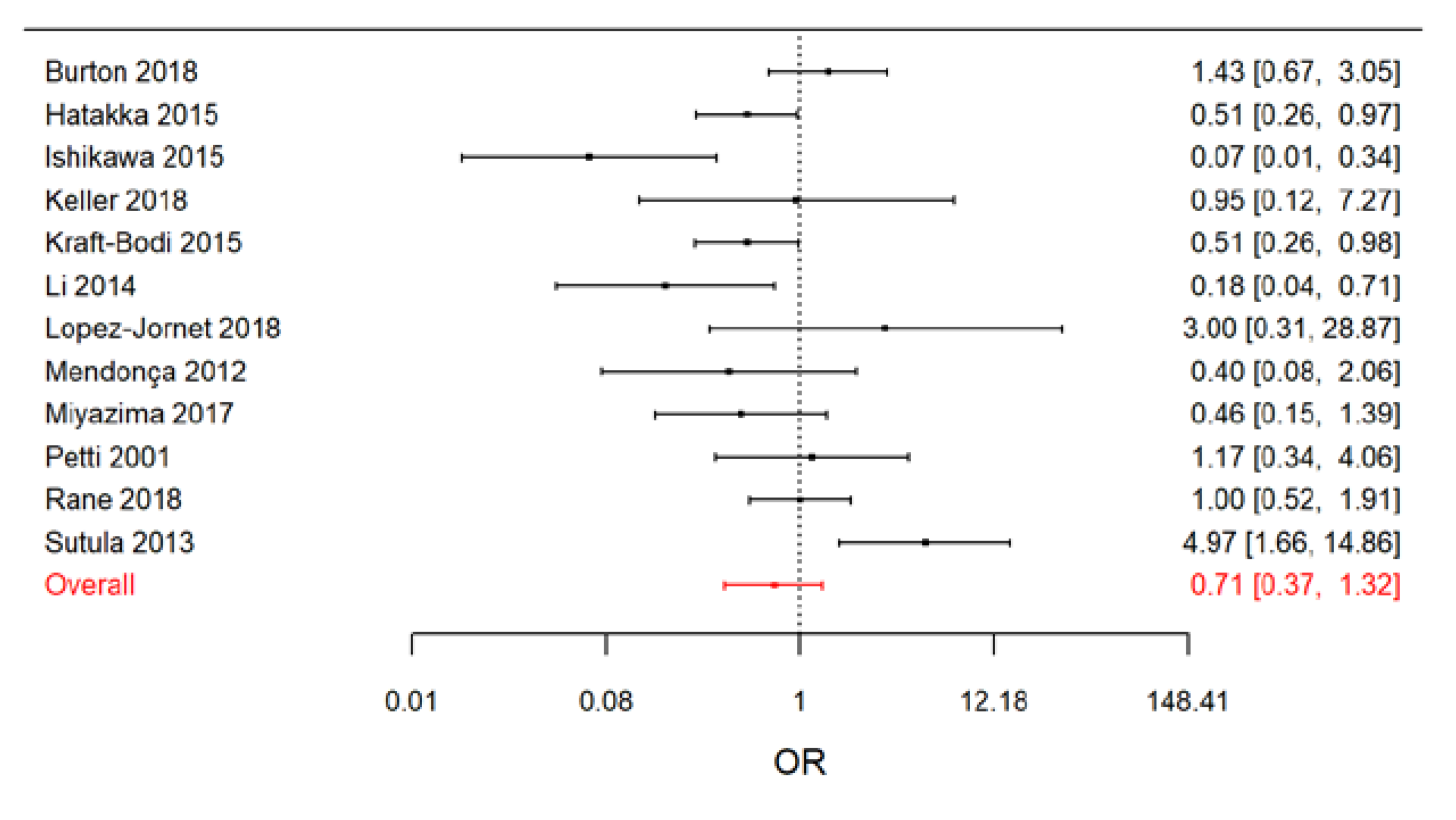
2.6. Meta-Analysis Results
3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
PRISMA 2009 Checklist statement
References
- Sardi, J.; Scorzoni, L.; Bernardi, T.; Fusco-Almeida, A.; Mendes Giannini, M.J. Candida species: Current epidemiology, pathogenicity, biofilm formation, natural antifungal products and new therapeutic options. J. Med. Microbiol. 2013, 62, 10–24. [Google Scholar] [CrossRef]
- Waggoner-Fountain, L.A.; Walker, M.W.; Hollis, R.J.; Pfaller, M.A.; Ferguson, J.E., 2nd; Wenzel, R.P.; Donowitz, L.G. Vertical and horizontal transmission of unique Candida species to premature newborns. Clin. Infect. Dis. 1996, 22, 803–808. [Google Scholar] [CrossRef] [PubMed]
- Mayer, F.L.; Wilson, D.; Hube, B. Candida albicans pathogenicity mechanisms. Virulence J. 2013, 4, 119–128. [Google Scholar] [CrossRef] [PubMed]
- Epstein, J.B.; Pearsall, N.N.; Truelove, E.L. Quantitative relationships between Candida albicans in saliva and the clinical status of human subjects. J. Clin. Microbiol. 1980, 12, 475–476. [Google Scholar] [PubMed]
- Ghannoum, M.A.; Jurevic, R.J.; Mukherjee, P.K.; Cui, F.; Sikaroodi, M.; Naqvi, A.; Gillevet, P.M. Characterization of the oral fungal microbiome (mycobiome) in healthy individuals. PLoS Pathog. 2010, 6, e1000713. [Google Scholar] [CrossRef]
- Fidel, P.L.; Vazquez, J.A.; Sobel, J.D. Candida glabrata: Review of epidemiology, pathogenesis, and clinical disease with comparison to C. albicans. Clin. Microbiol. Rev. 1999, 12, 80–96. [Google Scholar] [CrossRef]
- Tintelnot, K.; Haase, G.; Seibold, M.; Bergmann, F.; Staemmler, M.; Franz, T.; Naumann, D. Evaluation of phenotypic markers for selection and identification of Candida dubliniensis. J. Clin. Microbiol. 2000, 38, 1599–1608. [Google Scholar]
- Greenberg, M.S.; Glick, M.; Ship, J.A. Burket Oral Medicine, 11th ed.; BC Decker: Hamilton, ON, Canada, 2008; pp. 79–84. [Google Scholar]
- Williams, D.; Lewis, M. Pathogenesis and treatment of oral candidosis. J. Oral Microbiol. 2011, 3, 5771. [Google Scholar] [CrossRef]
- Webb, B.C.; Thomas, C.J.; Willcox, M.D.; Harty, D.W.; Knox, K.W. Candida-associated denture stomatitis. Aetiology and management: A review. Part 3. Treatment of oral candidosis. Aust. Dent. J. 1998, 43, 244–249. [Google Scholar] [CrossRef]
- Portela, M.B.; Souza, I.P.R.; Abreu, C.M.; Bertolini, M.; Holandino, C.; Alviano, C.S.; Santos, A.L.S.; Soares, R.M.A. Effect of serine-type protease of Candida spp. isolated from linear gingival erythema of HIV-positive children: Critical factors in the colonization. J. Oral Pathol. Med. 2010, 39, 753–760. [Google Scholar]
- Farah, C.S.; Lynch, N.; McCullough, M.J. Oral fungal infections: An update for the general practitioner. Aust. Dent. J. 2010, 55, 48–54. [Google Scholar] [CrossRef] [PubMed]
- Akpan, A.; Morgan, R. Oral candidiasis. Postgrad. Med. J. 2002, 78, 455–459. [Google Scholar] [CrossRef] [PubMed]
- Van Boven, J.F.; De Jong-van den Berg, L.T.W.; Vegter, S. Inhaled Corticosteroids and the Occurrence of Oral Candidiasis: A Prescription Sequence Symmetry Analysis. Drug Saf. 2013, 36, 231–236. [Google Scholar] [CrossRef] [PubMed]
- Daya, A.M.; Anderson, I.; Portnof, J. Mandibular osteomyelitis associated with Candida albicans in marijuana and heroin abusers. Ann. Maxillofac. Surg. 2018, 8, 355. [Google Scholar] [CrossRef]
- Keten, H.S.; Keten, D.; Ucer, H.; Yildirim, F.; Hakkoymaz, H.; Isik, O. Prevalence of oral Candida carriage and Candida species among cigarette and maras powder users. Int. J. Clin. Exp. Med. 2015, 8, 9847–9854. [Google Scholar]
- Nishimaki, F.; Yamada, S.; Kawamoto, M.; Sakurai, A.; Hayashi, K.; Kurita, H. Relationship Between the Quantity of Oral Candida spp. and Systemic Condition/Diseases of the Host: Oral Candida Increases with Advancing Age and Anemia. Mycopathologia 2019. [Google Scholar] [CrossRef]
- Santos, S.B.D.; Sabadin, C.E.S.; Mario, D.N.; Rigo, L.; Barbosa, D.A. Presence of Candida spp. and candidiasis in liver transplant patients. Anais Brasileiros de Dermatologia 2018, 93, 356–361. [Google Scholar]
- Nadig, S.; Ashwathappa, D.; Manjunath, M.; Krishna, S.; Annaji, A.; Shivaprakash, P. A relationship between salivary flow rates and Candida counts in patients with xerostomia. J. Oral Maxillofac. Pathol. 2017, 21, 316. [Google Scholar] [CrossRef]
- Mothibe, J.V.; Patel, M. Pathogenic characteristics of Candida albicans isolated from oral cavities of denture wearers and cancer patients wearing oral prostheses. Microb. Pathog. 2017, 110, 128–134. [Google Scholar] [CrossRef]
- Lalla, R.V.; Patton, L.L.; Dongari-Bagtzoglou, A. Oral candidiasis: Pathogenesis, clinical presentation, diagnosis and treatment strategies. J. Calif. Dent. Assoc. 2013, 41, 263–268. [Google Scholar]
- Al-Maskari, A.Y.; Al-Maskari, M.Y.; Al-Sudairy, S. Oral Manifestations and Complications of Diabetes Mellitus: A review. Sultan Qaboos Univ. Med. J. 2011, 11, 179–186. [Google Scholar] [PubMed]
- Mushi, M.F.; Bader, O.; Taverne-Ghadwal, L.; Bii, C.; Groß, U.; Mshana, S.E. Oral candidiasis among African human immunodeficiency virus-infected individuals: 10 years of systematic review and meta-analysis from sub-Saharan Africa. J. Oral Microbiol. 2017, 9, 1317579. [Google Scholar] [CrossRef] [PubMed]
- Bett, J.V.S.; Batistella, E.Â.; Melo, G.; Munhoz, E.A.; Silva, C.A.B.; Guerra, E.N.D.S.; Porporatti, A.L.; De Luca Canto, G. Prevalence of oral mucosal disorders during pregnancy: A systematic review and meta-analysis. J. Oral. Pathol. Med. 2019, 48, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Russo, E.; Bacci, G.; Chiellini, C.; Fagorzi, C.; Niccolai, E.; Taddei, A.; Ricci, F.; Ringressi, M.N.; Borrelli, R.; Melli, F.; et al. Preliminary Comparison of Oral and Intestinal Human Microbiota in Patients with Colorectal Cancer: A Pilot Study. Front Microbiol. 2018, 8, 2699. [Google Scholar] [CrossRef]
- Amedei, A.; Boem, F. I’ve Gut A Feeling: Microbiota Impacting the Conceptual and Experimental Perspectives of Personalized Medicine. Int. J. Mol. Sci. 2018, 19, 3756. [Google Scholar] [CrossRef]
- Niccolai, E.; Boem, F.; Russo, E.; Amedei, A. The Gut-Brain Axis in the Neuropsychological Disease Model of Obesity: A Classical Movie Revised by the Emerging Director “Microbiome”. Nutrients 2019, 11, 156. [Google Scholar] [CrossRef]
- Milosevic, I.; Vujovic, A.; Barac, A.; Djelic, M.; Korac, M.; Spurnic, A.R.; Gmizic, I.; Stevanovic, O.; Djordjevic, V.; Lekic, N.; et al. Gut-Liver Axis, Gut Microbiota, and Its Modulation in the Management of Liver Diseases: A Review of the Literature. Int. J. Mol. Sci. 2019, 20, 395. [Google Scholar] [CrossRef]
- De Almeida, C.V.; De Camargo, M.R.; Russo, E.; Amedei, A. Role of diet and gut microbiota on colorectal cancer immunomodulation. World J. Gastroenterol. 2019, 25, 151–162. [Google Scholar] [CrossRef]
- Hill, C.; Guarner, F.; Reid, G.; Gibson, G.R.; Merenstein, D.J.; Pot, B.; Morelli, L.; Canani, R.B.; Flint, H.J.; Salminen, S.; et al. Expert consensus document. The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nat. Rev. Gastroenterol. Hepatol. 2014, 11, 506–514. [Google Scholar] [CrossRef]
- Guarner, F.; Sanders, M.E.; Eliakim, R.; Gangl, A.; Thomson, A.; Krabshuis, J.; Lemair, T.; Kaufmann, P.; de Paula, J.A.; Fedorak, R.; et al. World Gastroenterology Organisation; Global Guidelines Probiotics and Prebiotics. J. Clin. Gastroenterol. 2012, 46, 468–481. [Google Scholar] [CrossRef]
- Fuller, R. Probiotics in human medicine. Gut 1991, 32, 439–442. [Google Scholar] [CrossRef] [PubMed]
- Blaut, M. Relationship of prebiotics and food to intestinal microflora. Eur. J. Nutr. 2002, 41, i11–i16. [Google Scholar] [CrossRef] [PubMed]
- Nagpal, R.; Wang, S.; Ahmadi, S.; Hayes, J.; Gagliano, J.; Subashchandrabose, S.; Kitzman, D.W.; Becton, T.; Read, R.; Yadav, H. Human-origin probiotic cocktail increases short-chain fatty acid production via modulation of mice and human gut microbiome. Sci. Rep. 2018, 8, 12649. [Google Scholar] [CrossRef] [PubMed]
- Almeida, C.C.; Lorena, S.L.; Pavan, C.R.; Akasaka, H.M.; Mesquita, M.A. Beneficial effects of long-term consumption of a probiotic combination of Lactobacillus casei Shirota and Bifidobacterium breve Yakult may persist after suspension of therapy in lactose-intolerant patients. Nutr. Clin. Pract. 2012, 27, 247–251. [Google Scholar] [CrossRef] [PubMed]
- LeBlanc, J.G.; Milani, C.; de Giori, G.S.; Sesma, F.; van Sinderen, D.; Ventura, M. Bacteria as vitamin suppliers to their host: A gut microbiota perspective. Curr. Opin. Biotechnol. 2013, 24, 160–168. [Google Scholar] [CrossRef] [PubMed]
- Cho, Y.A.; Kim, J. Effect of Probiotics on Blood Lipid Concentrations: A Meta-Analysis of Randomized Controlled Trials. Medicine 2015, 94, 1714. [Google Scholar] [CrossRef]
- Collado, M.C.; Jalonen, L.; Meriluoto, J.; Salminen, S. Protection mechanism of probiotic combination against human pathogens: In vitro adhesion to human intestinal mucus. Asia Pac. J. Clin. Nutr. 2006, 15, 570–575. [Google Scholar]
- Oldak, A.; Zielinska, D. Bacteriocins from lactic acid bacteria as an alternative to antibiotics. Postepy higieny i medycyny doswiadczalnej 2017, 71, 328–338. [Google Scholar]
- Castagliuolo, I.; LaMont, J.T.; Nikulasson, S.T.; Pothoulakis, C. Saccharomyces boulardii protease inhibits Clostridium difficile toxin A effects in the rat ileum. Infect. Immun. 1996, 64, 5225–5232. [Google Scholar]
- Guo, S.; Gillingham, T.; Guo, Y.; Meng, D.; Zhu, W.; Walker, W.A.; Ganguli, K. Secretions of Bifidobacterium infantis and Lactobacillus acidophilus Protect Intestinal Epithelial Barrier Function. J. Pediatr. Gastroenterol. Nutr. 2017, 64, 404–412. [Google Scholar] [CrossRef]
- Maldonado Galdeano, C.; Cazorla, S.I.; Lemme Dumit, J.M.; Velez, E.; Perdigon, G. Beneficial Effects of Probiotic Consumption on the Immune System. Ann. Nutr. Metab. 2019, 74, 115–124. [Google Scholar] [CrossRef] [PubMed]
- Wagner, R.D.; Pierson, C.; Warner, T.; Dohnalek, M.; Farmer, J.; Roberts, L.; Hilty, M.; Balish, E. Biotherapeutic effects of probiotic bacteria on candidiasis in immunodeficient mice. Infect. Immun. 1997, 65, 4165–4172. [Google Scholar] [PubMed]
- Sookkhee, S.; Chulasiri, M.; Prachyabrued, W. Lactic acid bacteria from healthy oral cavity of Thai volunteers: Inhibition of oral pathogens. J. Appl. Microbiol. 2001, 90, 172–179. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, M.R.; Kragelund, C.; Jensen, P.Ø.; Keller, M.K.; Twetman, S. Probiotic Lactobacillus reuteri has antifungal effects on oral Candida species in vitro. J. Oral Microbiol. 2017, 9, 1274582. [Google Scholar] [CrossRef] [PubMed]
- Coman, M.M.; Verdenelli, M.C.; Cecchini, C.; Silvi, S.; Orpianesi, C.; Boyko, N.; Cresci, A. In vitro evaluation of antimicrobial activity of Lactobacillus rhamnosus IMC 501(®), Lactobacillus paracasei IMC 502(®) and SYNBIO(®) against pathogens. J. Appl. Microbiol. 2014, 117, 518–527. [Google Scholar] [CrossRef] [PubMed]
- Denkova, R.; Yanakieva, V.; Denkova, Z.; Nikolova, V.; Radeva, V. In vitro inhibitory activity of Bifidobacterium and lactobacillus strains against Candida Albicans. Bulg. J. Vet. Med. 2013, 16, 186–197. [Google Scholar]
- Chew, S.Y.; Cheah, Y.K.; Seow, H.F.; Sandai, D.; Than, L.T.L. In vitro modulation of probiotic bacteria on the biofilm of Candida glabrata. Anaerobe 2015, 34, 132–138. [Google Scholar] [CrossRef]
- Vilela, S.F.; Barbosa, J.O.; Rossoni, R.D.; Santos, J.D.; Prata, M.C.; Anbinder, A.L.; Jorge, A.O.; Junqueira, J.C. Lactobacillus acidophilus ATCC 4356 inhibits biofilm formation by C. albicans and attenuates the experimental candidiasis in Galleria mellonella. Virulence 2015, 6, 29–39. [Google Scholar]
- Wannun, P.; Piwat, S.; Teanpaisan, R. Purification, Characterization, and Optimum Conditions of Fermencin SD11, a Bacteriocin Produced by Human Orally Lactobacillus fermentum SD11. Appl. Biochem. Biotechnol. 2016, 179, 572–582. [Google Scholar] [CrossRef]
- Matsubara, V.H.; Silva, E.G.; Paula, C.R.; Ishikawa, K.H.; Nakamae, A.E. Treatment with probiotics in experimental oral colonization by Candida albicans in murine model (DBA/2). Oral Dis. 2012, 18, 260–264. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Hatakka, K.; Ahola, A.J.; Yli-Knuuttila, H.; Richardson, M.; Poussa, T.; Meurman, J.H.; Korpela, R. Probiotics reduce the prevalence of oral candida in the elderly—A randomized controlled trial. J. Dent. Res. 2007, 86, 125–130. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, K.H.; Mayer, M.P.A.; Miyazima, T.Y.; Matsubara, V.H.; Silva, E.G.; Paula, C.R.; Campos, T.T.; Nakamae, A.E. A multispecies probiotic reduces oral Candida colonization in denture wearers. J. Prosthodont. 2015, 24, 194–199. [Google Scholar] [CrossRef] [PubMed]
- Keller, M.K.; Kragelund, C. Randomized pilot study on probiotic effects on recurrent candidiasis in oral lichen planus patients. Oral Dis. 2018, 24, 1107–1114. [Google Scholar] [CrossRef]
- Kraft-Bodi, E.; Jørgensen, M.R.; Keller, M.K.; Kragelund, C.; Twetman, S. Effect of Probiotic Bacteria on Oral Candida in Frail Elderly. J. Dent. Res. 2015, 94, 181S–186S. [Google Scholar] [CrossRef]
- Li, D.; Li, Q.; Liu, C.; Lin, M.; Li, X.; Xiao, X.; Zhu, Z.; Gong, Q.; Zhou, H. Efficacy and safety of probiotics in the treatment of Candida-associated stomatitis. Mycoses 2014, 57, 141–146. [Google Scholar] [CrossRef]
- Miyazima, T.Y.; Ishikawa, K.H.; Mayer, M.; Saad, S.; Nakamae, A. Cheese supplemented with probiotics reduced the Candida levels in denture wearers-RCT. Oral Dis. 2017, 23, 919–925. [Google Scholar] [CrossRef]
- Petti, S.; Tarsitani, G.; D’Arca, A.S. A randomized clinical trial of the effect of yoghurt on the human salivary microflora. Arch. Oral Biol. 2001, 46, 705–712. [Google Scholar] [CrossRef]
- Burton, J.P.; Drummond, B.K.; Chilcott, C.N.; Tagg, J.R.; Thomson, W.M.; Hale, J.D.; Wescombe, P.A. Influence of the probiotic Streptococcus salivarius strain M18 on indices of dental health in children: A randomized double-blind, placebo-controlled trial. J. Med. Microbiol. 2013, 62, 875–884. [Google Scholar] [CrossRef]
- Da Costa, B.R.; Rutjes, A.W.S.; Johnston, B.C.; Reichenbach, S.; Nüesch, E.; Tonia, T.; Gemperli, A.; Guyatt, G.H.; Jüni, P. Methods to convert continuous outcomes into odds ratios of treatment response and numbers needed to treat: Meta-epidemiological study. Int. J. Epidemiol. 2012, 41, 1445–1459. [Google Scholar] [CrossRef]
- Rane, D.J.; Nayakar, R.; Harakuni, S.; Patil, R. To evaluate the effect of probiotics on the prevalence of oral Candida organisms in denture wearers: An in vivo study. Indian J. Health Sci. Biomed. Res. 2018, 11, 136–145. [Google Scholar] [CrossRef]
- Sutula, J.; Coulthwaite, L.A.; Thomas, L.V.; Verran, J. The effect of a commercial probiotic drink containing Lactobacillus casei strain Shirota on oral health in healthy dentate people. Microb. Ecol. Health Dis. 2013, 24. [Google Scholar] [CrossRef]
- Lopez-Jornet, P.; Soler Tornero, C. Is Lactobacillus reuteri administration beneficial to oral candida levels? Int. J. Dermatol. 2018, 57, e5–e7. [Google Scholar] [CrossRef] [PubMed]
- Mendonça, F.H.; Santos, S.S.; Faria Ida, S.; Gonçalves e Silva, C.R.; Jorge, A.O.; Leão, M.V. Effects of probiotic bacteria on Candida presence and IgA anti-Candida in the oral cavity of elderly. Braz. Dent. J. 2012, 23, 534–538. [Google Scholar] [CrossRef]
- Woolson, R.F.; Clarke, W.R. Mcnemar test. In Statistical Methods for the Analysis of Biomedical Data, 2nd ed.; Wiley: Hoboken, NJ, USA, 2011; p. 221. [Google Scholar]
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions; Version 5.1.0.; The Cochrane Collaboration, 2011; Available online: www.handbook.cochrane.org (accessed on 23 December 2018).
- Study Quality Assessment Tools. Available online: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools (accessed on 3 January 2019).
- Sutton, A.J.; Abrams, K.R. Bayesian Methods in Meta-Analysis and Evidence Synthesis. Stat. Methods Med. Res. 2001, 10, 277–303. [Google Scholar] [CrossRef]
- Gelman, A.; Rubin, D.B. Inference from iterative simulation using multiple sequences. Stat. Sci. 1992, 7, 457–511. [Google Scholar] [CrossRef]
- Egger, M.; Davey Smith, G.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef]
- Begg, C.B.; Mazumdar, M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994, 50, 1088–1101. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2012; Available online: http://www.R-project.org/ (accessed on 03 January 2019).
- Lunn, D.; Spiegelhalter, D.; Thomas, A.; Best, N. The BUGS project: Evolution, critique and future directions. Stat. Med. 2009, 28, 3049–3067. [Google Scholar] [CrossRef]
- Rodloff, C.; Koch, D.; Schaumann, R. Epidemiology and antifungal resistance in invasive candidiasis. Eur. J. Med. Res. 2011, 16, 187–195. [Google Scholar] [CrossRef]
- Dartevelle, P.; Ehlinger, C.; Zaet, A.; Boehler, C.; Rabineau, M.; Westermann, B.; Strub, J.M.; Cianferani, S.; Haïkel, Y.; Metz-Boutigue, M.H.; et al. D-Cateslytin: A new antifungal agent for the treatment of oral Candida albicans associated infections. Sci. Rep. 2018, 8, 9235. [Google Scholar] [CrossRef] [PubMed]
- Taylor, R.S. Probiotics to prevent necrotizing enterocolitis: Too cheap and easy? Paediatr. Child. Health 2014, 19, 351–352. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Shinkar, D.M.; Dhake, A.S.; Setty, C.M. Drug delivery from the oral cavity: A focus on mucoadhesive buccal drug delivery systems. PDA J. Pharm. Sci. Technol. 2012, 66, 466–500. [Google Scholar] [CrossRef] [PubMed]
- Shimizu, K.; Yamada, T.; Ogura, H.; Mohri, T.; Kiguchi, T.; Fujimi, S.; Asahara, T.; Yamada, T.; Ojima, M.; Ikeda, M.; et al. Synbiotics modulate gut microbiota and reduce enteritis and ventilator-associated pneumonia in patients with sepsis: A randomized controlled trial. Crit. Care 2018, 27, 239. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury, A.H.; Adiamah, A.; Kushairi, A.; Varadhan, K.K.; Krznaric, Z.; Kulkarni, A.D.; Neal, K.R.; Lobo, D.N. Perioperative Probiotics or Synbiotics in Adults Undergoing Elective Abdominal Surgery: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Ann. Surg. 2019. [Google Scholar] [CrossRef] [PubMed]
| Factors Related to Oral Candidiasis |
|---|
| Iatrogenic factors |
| Antineoplastic agents [12] |
| Broad-spectrum antibiotics [13] |
| Inhaled corticosteroids [14] |
| Substance abuse [15,16] |
| Health conditions |
| Anemia [17] |
| Immunosuppression status [18] |
| Nutritional deficiencies [13] |
| Xerostomia [19] |
| Diseases |
| Cancer [20] |
| Cushing syndrome [13] |
| Diabetes mellitus [21,22] |
| Human immunodeficiency virus (HIV) [23] |
| Other factors |
| Age [17] |
| Denture wearing [20] |
| Pregnancy [24] |
| Smoke [16] |
| Reference | Study Design | Setting | Studied Population | No. of Participants | Intervention | Comparison | Follow-up | Sample Type | Outcome |
|---|---|---|---|---|---|---|---|---|---|
| Burton et al. 2013 [60] | RCT | Schools with dental clinics City: Dunedin Country: New Zealand | Child population, schoolchildren with active caries. Age: 5 to 10 years (mean 8.5 years) | Total: 83; 40 in the probiotic group, 43 in the placebo group | Two lozenges with S. salivarius (each lozenge 3.6 × 109 CFU of strain), two times a day, one in the morning and one at night, for three months | Placebo. Lozenges with identical appearance and taste, without probiotics | 3 months | Saliva samples | OR* 1.427 95% CI (0.667–3.054) |
| Hatakka et al. 2007 [53] | RCT | Homes and sheltered housing units City: Helsinki Country: Finland | Elderly people, aged 70–100 years | Total: 192; 92 in the probiotic group, 100 in the placebo group. | Daily 50 g of Emmental-type probiotic cheese divided into two portions, with Lactococcus lactis and Lactobacillus helveticus as starter cultures and 107 CFU/g of each probiotic strain: L. rhamnosus GG (ATCC 53103), L. rhamnosus LC705, and Propionibacterium freudenreichii ssp. shermanii JS | Daily 50 g of edam type cheese, divided into two portions, with Lactococcus lactis as starter culture without the addition of other probiotic strains | 16 weeks | Saliva samples | OR 0.505 95% CI (0.263–0.970)OR calculated for a cut-off of Candida ≥104 CFU/ml |
| Ishikawa et al. 2015 [54] | RCT | Patients seeking dental treatment (complete denture) at the School of Dentistry, University of São Paulo City: São Paulo Country: Brazil | Denture wearers harboring Candida spp. in the oral cavity with no clinical symptoms, aged (mean) 61.8 ± 8.5 years | Total: 55. 30 in the probiotic group. 25 in the placebo group | 1 capsule/day containing lyophilized cultures (obtainedfrom HardiStrain® – Probiotics) of L. rhamnosus HS111, L. acidophilus HS101, and Bifidobacterium bifidum combined in equal amounts, reaching 108 CFU (3.3 × 107 CFU of each) per capsule | Placebo 1 capsule/day with same characteristics as the probiotic product, but without the probiotic bacteria | 5 weeks | Palatal mucosal samples | OR 0.066 95% CI (0.013–0.338)OR calculated for a cut-off of Candida ≥104 CFU/ml |
| Keller et al. 2018 [55] | RCT | Clinic for oral medicine City: Copenhagen Country: Denmark | Patients attending the Clinic for Oral Medicine, aged median (67) years, with diagnosis of oral lichen planus | Total: 22.9 in the probiotic group, 13 in the placebo group | Pre-treatment: all patients were treated with the current conventional treatment regimens at the Clinic for Oral Medicine, including those who required additional conventional treatment during the 1-year study period Patients diagnosed with oral candidiasis were treated withnystatin, patients without oral candidiasis were treated with steroid, fluocinolone acetonide gel 0.025% Treatment: probiotic lozenges containing two strains of the probiotic bacteria L. reuteri (DSM 17938 and ATCC PTA 5289) dissolved intra-orally three times daily (morning, noon, and evening just before bedtime) for 16 weeks | Pre-treatment: the same of intervention group Treatment: placebo lozenges without probiotic bacteria | 16 weeks | Saliva samples | OR 0.952 95% CI (0.125–7.275)OR calculated with cut-off Candida carriage yes/no |
| Kraft- Bodi et al. 2015 [56] | RCT | Nursing homes. Country: south of Sweden | Elderly people, aged (mean) 88 years | Total: 174; 84 in the probiotic group, 90 in the placebo group | 2 lozenges daily the morning and in the early evening, containing a minimum of 108 live bacteria of each strain of the probiotic bacterium Lactobacillus reuteri (DSM 17938 and ATCC PTA 5289; Prodentis™, Biogaia® AB, Lund, Sweden) | Placebo lozenges without active bacteria | 12 weeks | Saliva samples | OR 0.505 95% CI (0.259–0.984)OR calculated for a cut-off of Candida ≥ 104 CFU/ml |
| Li et al. 2014 [57] | RCT | Department of Oral Medicine, West China College of Stomatology, Sichuan University City: Sichuan Country: China | Patients with clinically and microbiologically proven Candida-associated stomatitis (detection rate of Candida albicans in the saliva >102 CFU mL−1), aged (mean, SD) 64 ± 10.75 years | Total: 65; 34 in the probiotic group, 31 in the control group | Pre-treatment: administration orally of 2% sodium bicarbonate solution and then application of 2% nystatin pasteTreatment: four lozenges containing the mixture of B. longum (5 × 106 CFU in 0.5 g of skim milk powder per tablet), L. bulgaricus (5 × 105 CFU in 0.5 g of skim milk powder per tablet), and S. thermophilus (5 × 105 CFU in 0.5 g of skim milk powder per tablet)The medication was applied three times daily for 4 weeks. | 2% sodium bicarbonate solution and 2% nystatin paste | 4 weeks | Saliva samples | OR 0.176 95% CI (0.044–0.710)OR calculated for a cut-off of Candida ≥102 CFU/mL |
| Lopez-Jornet et al. 2018 [64] | Before–after study | Clınica Odontologica Universitaria Hospital Morales MeseguerCity: Murcia. Country: Spain | Patients, aged (mean) 71.2 years | Total: 27 | Lactobacillus reuteri DSM 17938 (German Culture Collection of Microorganisms) and ATCC PTA 5289 (American Type Culture Collection) (GUM Periobalance®, Sunstar) one tablet per day for 28 days | 28 days | Saliva samples | OR 3.00095 %CI (0.312–28.842)OR calculated with a cut-off of Candida >102 CFU/mL | |
| Mendonça et al. 2012 [65] | Before–after study | City: Taubaté Country: Brazil | Healthy women aged 65 or older who lived in the city of Taubaté, SP, Brazil | Total: 42 | 1 g (content of 1 envelope) of the probiotic Yakult LB® (Lactobacillus casei and Bifidobacterium breve, 2 × 107 to 109 and 5 × 107 to 109 CFU/mL, respectively), 3 times a week, at the same hour, for 30 days | 30 days | Saliva samples | OR 0.400 95% CI (0.078–2.062)OR calculated with a cut-off Candida carriage yes/no | |
| Miyazima et al. 2017 [58] | RCT | School of Dentistry, University of São Paulo City: São Paulo Country: Brazil | Denture-wearing patients seeking for dental treatment (complete denture), aged (mean, SD) 64.4 ±12.07 years | Total: 60; 20 in each group (treatment 1, treatment 2, control) | Treatment 1, T1 group: fresh cheese added with probiotics containing 8 to 9 log CFU∙g−1 of L. acidophilus NCFMTreatment 2, T2 group: fresh cheese added with probiotics containing 8 to 9 log CFU∙g−1 of L. rhamnosus Lr-32 | PlaceboControl group (C group): fresh cheese with no added probiotics | 8 weeks | Mouth-rinse samples | OR 0.464 95% CI (0.155–1.392)OR calculated for a cut-off of Candida ≥103 CFU/mL |
| Petti et al. 2001 [59] | RCT | Country: Italy | Adult volunteers, aged (mean) 28.2 years | Total: 42; 20 in the yoghurt group, 22 in the control group | 125 g of fruit yoghurt twice daily, between breakfast and lunch, and between lunch and dinnerThen, 2 weeks without yogurt intake | 125 g of fruit soybean ice cream twice daily, between breakfast and lunch, and between lunch and dinner Then, 2 weeks without soybean ice cream intake | 16 weeks | Saliva samples | OR 1.167 95% CI (0.335–4.060)OR calculated for a cut-off of Candida between 3.5 and 7.6 × 102 CFU/mL |
| Rane et al. 2018 [62] | Before–after study | Country: India | Healthy complete denture wearers, aged ≥50 years | Total: 60; 20 in group A (age 50–59 years), 20 in group B (age 60–69 years), 20 in group C (age ≥ 70 years) | Once daily, 1 capsule content of probiotic (Probiotic immune®, Zenith nutrition) in the palatal region of the cleaned maxillary denture | 5 weeks | Palatal mucosa samples | OR* group A 0.891 95% CI (0.290–2.736)OR group B 1.323 95% CI (0.431–4.063)OR group C 0.846 95% CI (0.276–2.598) | |
| Sutula et al. 2013 [63] | Before–after study | Manchester Metropolitan University City: Manchester. Country: United Kingdom | Healthy dentate volunteers, aged (mean, SD) 32 ± 11.5 years | Total: 21 | One bottle per day of drink milk Yakult ®, containing a minimum of 6.5 × 109 viable cells of probiotic L. casei strain Shirota, for 4 weeks | 4 weeks | Saliva samples | OR* 4.967 95% CI (1.662–14.843) |
| Type of Meta-Analysis | Meta-Analytic Estimate (OR) (95% CrI) | I2 (95% CrI) |
|---|---|---|
| All 12 studies | 0.71 (0.37–1.32) | 56.3 (6.0–84.4) |
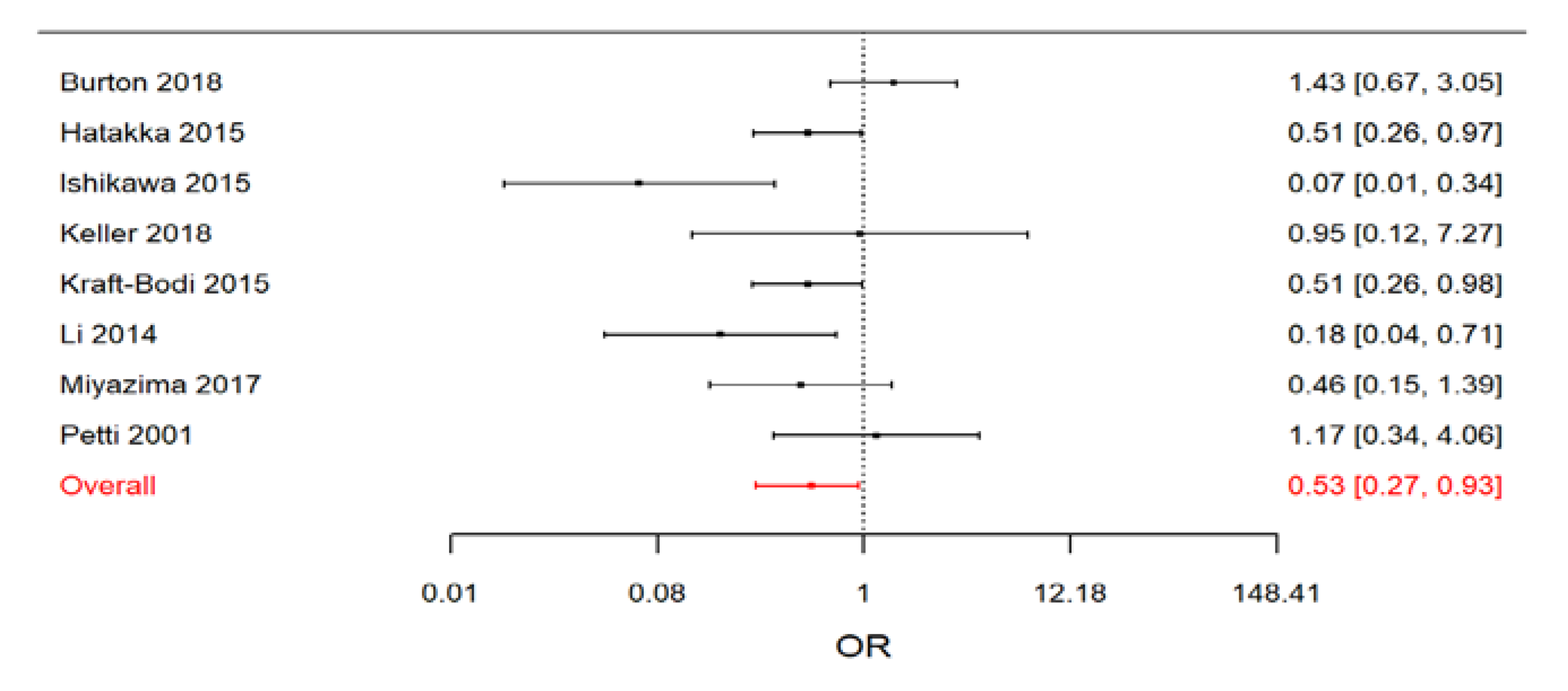
| Only RCTs | 0.53 (0.27–0.93) | 32.2 (0.3–84.0) |
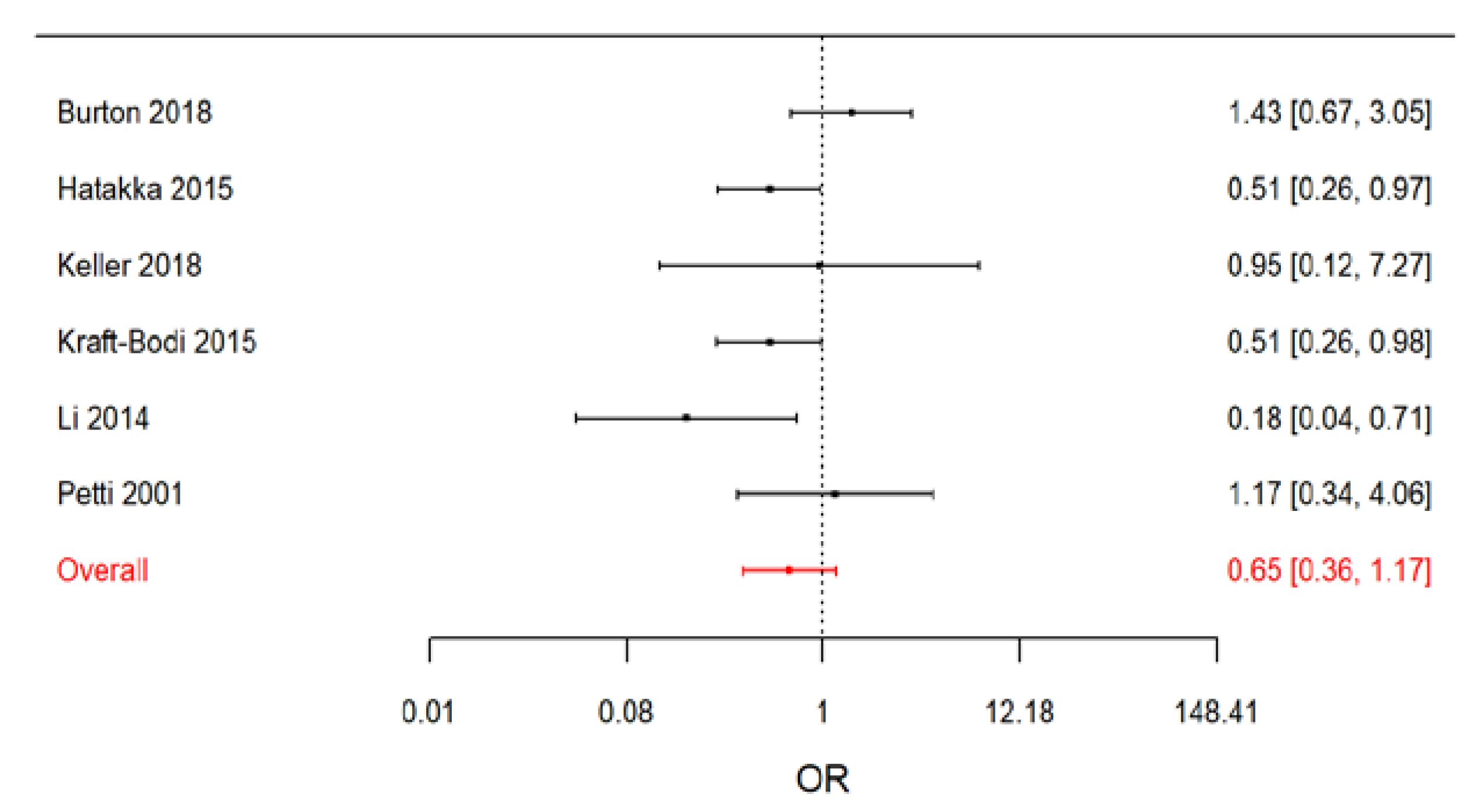
| RCTs with non-denture wearers | 0.65 (0.36–1.17) | 17.6 (0.3–81.8) |
| RCTs with denture wearers 1 | 0.19 (0.03–1.29) | |
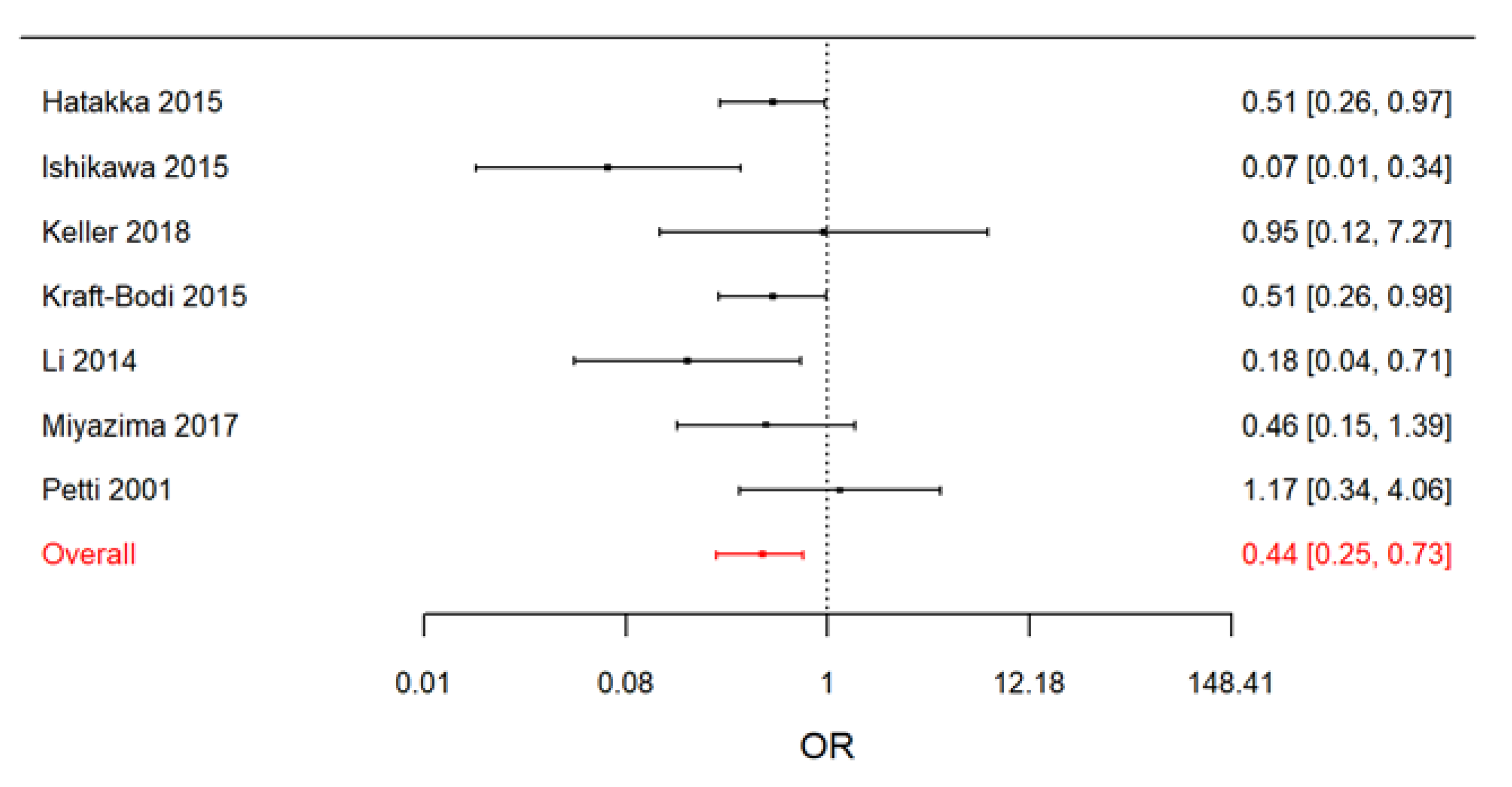
| RCTs with adult patients | 0.44 (0.25–0.73) | 7.0 (0.2–76.2) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mundula, T.; Ricci, F.; Barbetta, B.; Baccini, M.; Amedei, A. Effect of Probiotics on Oral Candidiasis: A Systematic Review and Meta-Analysis. Nutrients 2019, 11, 2449. https://doi.org/10.3390/nu11102449
Mundula T, Ricci F, Barbetta B, Baccini M, Amedei A. Effect of Probiotics on Oral Candidiasis: A Systematic Review and Meta-Analysis. Nutrients. 2019; 11(10):2449. https://doi.org/10.3390/nu11102449
Chicago/Turabian StyleMundula, Tiziana, Federica Ricci, Beatrice Barbetta, Michela Baccini, and Amedeo Amedei. 2019. "Effect of Probiotics on Oral Candidiasis: A Systematic Review and Meta-Analysis" Nutrients 11, no. 10: 2449. https://doi.org/10.3390/nu11102449
APA StyleMundula, T., Ricci, F., Barbetta, B., Baccini, M., & Amedei, A. (2019). Effect of Probiotics on Oral Candidiasis: A Systematic Review and Meta-Analysis. Nutrients, 11(10), 2449. https://doi.org/10.3390/nu11102449







