Changes in Weight and Substrate Oxidation in Overweight Adults Following Isomaltulose Intake During a 12-Week Weight Loss Intervention: A Randomized, Double-Blind, Controlled Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Study Design
2.3. Dietary Intervention
2.4. Data Collection
2.4.1. Anthropometrics and Body Composition
2.4.2. Energy Intake (EI)
2.4.3. Energy Metabolism
2.4.4. Other Parameters
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Anthropometrics and Body Composition
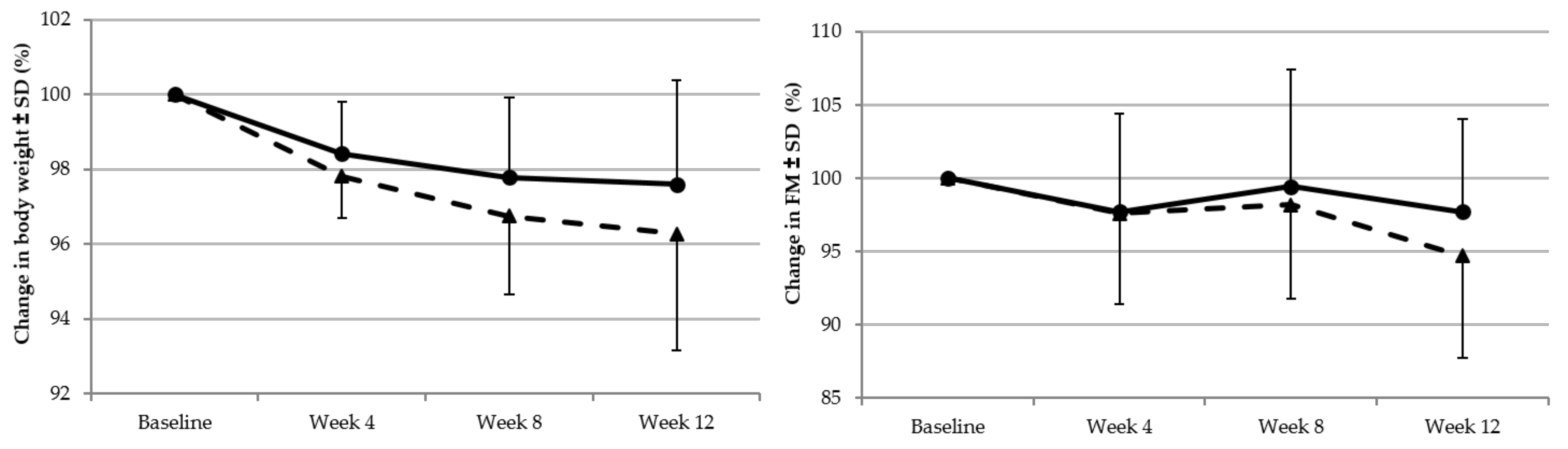
3.2.1. Body Weight, BMI, and Waist Circumference
3.2.2. Fat Mass and Fat Free Mass
3.3. Energy Intake and Metabolism
3.3.1. Energy and Macronutrient Intake
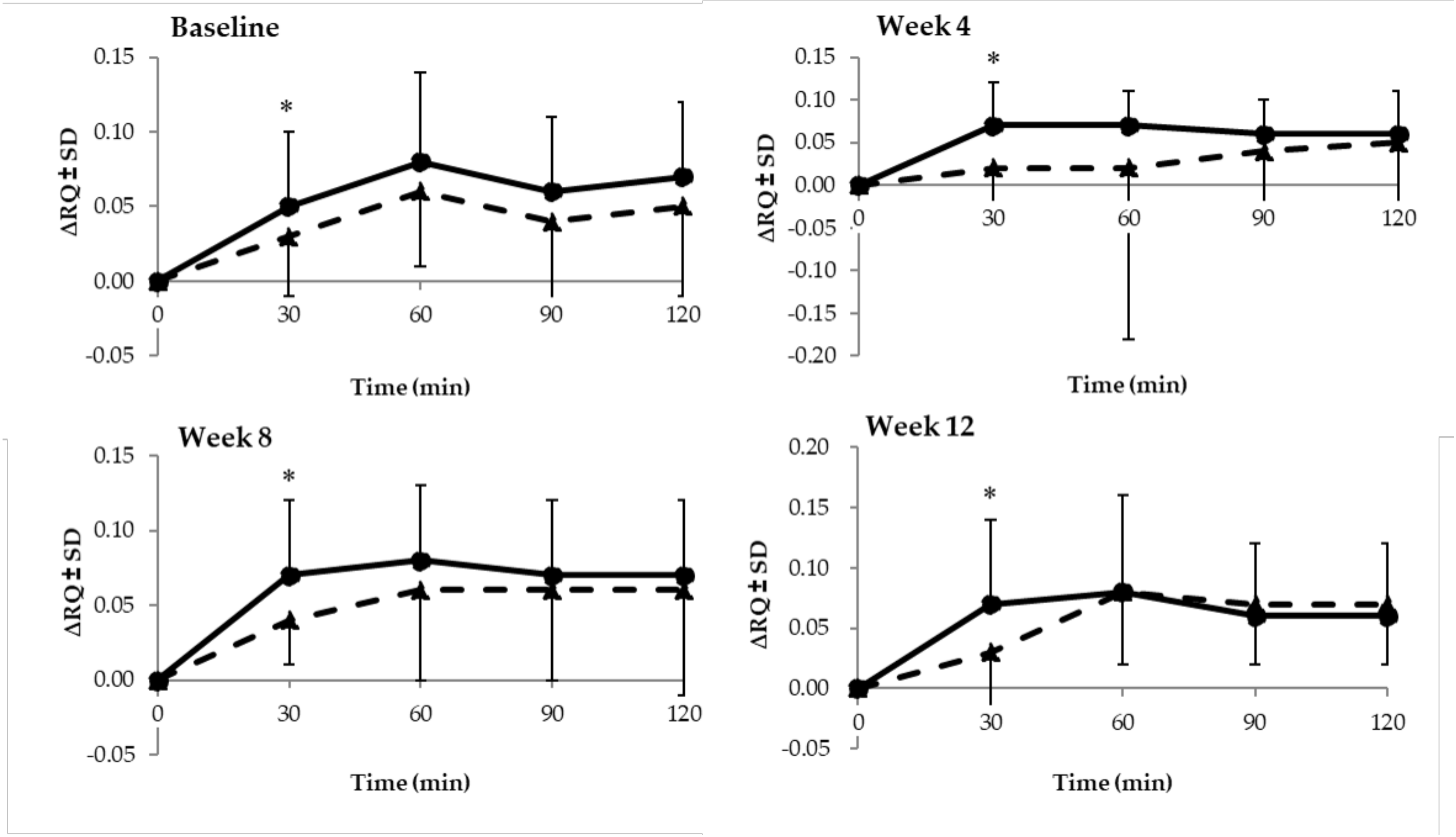
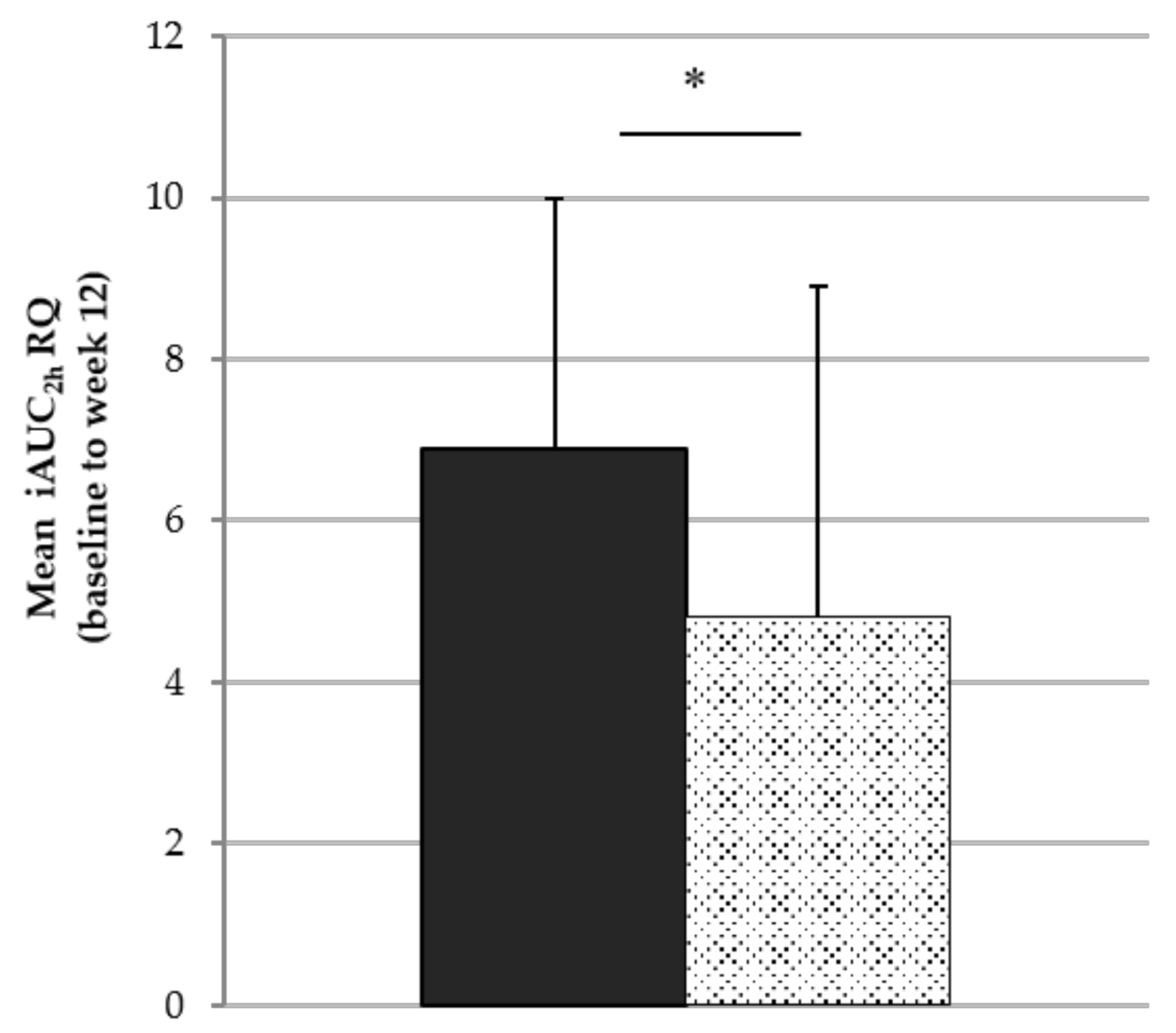
3.3.2. Energy Expenditure and Substrate Oxidation
3.4. Other Parameters and Adverse events
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Hargreaves, M.; Hawley, J.A.; Jeukendrup, A. Pre-exercise carbohydrate and fat ingestion: Effects on metabolism and performance. J. of Spo. Sci. 2007, 22, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Kelley, D.E. Skeletal muscle fat oxidation: timing and flexibility are everything. J. Clin. Investig. 2005, 115, 1699–1702. [Google Scholar] [CrossRef] [PubMed]
- Jeukendrup, A. Modulation of carbohydrate and fat utilization by diet, exercise and environment. Biochem. Soc. Trans. 2003, 31, 1270–1273. [Google Scholar] [CrossRef] [PubMed]
- Nutrition and Athletic Performance. Med. Sci. Sports Exerc. 2009, 41, 709–731. [CrossRef] [PubMed]
- Shah, M.; Garg, A. High-Fat and High-Carbohydrate Diets and Energy Balance. Diabetes Care 1996, 19, 1142–1152. [Google Scholar] [CrossRef]
- Holloway, G.P.; Bonen, A.; Spriet, L.L. Regulation of skeletal muscle mitochondrial fatty acid metabolism in lean and obese individuals. Am. J. Clin. Nutr. 2009, 89, 455–462. [Google Scholar] [CrossRef] [PubMed]
- Wells, G.D.; Noseworthy, M.D.; Hamilton, J.; Tarnopolski, M.; Tein, I. Skeletal muscle metabolic dysfunction in obesity and metabolic syndrome. Can. J. Neurol. Sci. J. Can. Sci. Neurol. 2008, 35, 31–40. [Google Scholar] [CrossRef]
- Ellis, A.C.; Hyatt, T.C.; Hunter, G.R.; Gower, B.A. Respiratory quotient predicts fat mass gain in premenopausal women. Obesity 2010, 18, 2255–2259. [Google Scholar] [CrossRef]
- König, D.; Theis, S.; Kozianowski, G.; Berg, A. Postprandial substrate use in overweight subjects with the metabolic syndrome after isomaltulose (Palatinose™) ingestion. Nutri. 2012, 28, 651–656. [Google Scholar] [CrossRef]
- König, D.; Zdzieblik, D.; Holz, A.; Theis, S.; Gollhofer, A. Substrate Utilization and Cycling Performance Following Palatinose™ Ingestion: A Randomized, Double-Blind. Control. Trial. Nutri 2016, 8, 390. [Google Scholar] [CrossRef]
- Solomon, T.P.J.; Haus, J.M.; Cook, M.A.; Flask, C.A.; Kirwan, J.P. A low-glycemic diet lifestyle intervention improves fat utilization during exercise in older obese humans. Obesity 2013, 21, 2272–2278. [Google Scholar] [CrossRef] [PubMed]
- Henry, C.J.; Kaur, B.; Quek, R.Y.C.; Camps, S.G. A Low Glycaemic Index Diet Incorporating Isomaltulose Is Associated with Lower Glycaemic Response and Variability, and Promotes Fat Oxidation in Asians. Nutrients 2017, 9, 473. [Google Scholar] [CrossRef] [PubMed]
- Stevenson, E.J.; Williams, C.; E Mash, L.; Phillips, B.; Nute, M.L. Influence of high-carbohydrate mixed meals with different glycemic indexes on substrate utilization during subsequent exercise in women1,2. Am. J. Clin. Nutr. 2006, 84, 354–360. [Google Scholar] [CrossRef] [PubMed]
- Sun, M.; Schutz, Y.; Maffeis, C. Substrate metabolism, nutrient balance and obesity development in children and adolescents: a target for intervention? Obes. Rev. 2004, 5, 183–188. [Google Scholar] [CrossRef] [PubMed]
- Van Can, J.G.P.; Ijzerman, T.H.; Van Loon, L.J.C.; Brouns, F.; Blaak, E.E. Reduced glycaemic and insulinaemic responses following trehalose ingestion: implications for postprandial substrate use. Br. J. Nutr. 2009, 102, 1395–1399. [Google Scholar] [CrossRef] [PubMed]
- McKeown, N.M.; Meigs, J.B.; Liu, S.; Saltzman, E.; Wilson, P.W.; Jacques, P.F. Carbohydrate nutrition, insulin resistance, and the prevalence of the metabolic syndrome in the Framingham Offspring Cohort. Diabetes Care 2004, 27, 538–546. [Google Scholar] [CrossRef] [PubMed]
- Lukaczer, D.; DeAnn, J.L.; Lerman, R.H.; Darland, G.; Schiltz, B.; Tripp, M.; Bland, J.S. Effect of a low glycemic index diet with soy protein and phytosterols on CVD risk factors in postmenopausal women. Nutrients 2006, 22, 104–113. [Google Scholar] [CrossRef]
- Elliott, E.J.; Thomas, D. Low glycaemic index, or low glycaemic load, diets for diabetes mellitus. Cochrane Database Syst. Rev. 2009, 2009, 95. [Google Scholar]
- Kahlhöfer, J.; Karschin, J.; Silberhorn-Bühler, H.; Breusing, N.; Bosy-Westphal, A. Effect of low-glycemic-sugar-sweetened beverages on glucose metabolism and macronutrient oxidation in healthy men. Int. J. Obes. 2016, 40, 990–997. [Google Scholar] [CrossRef]
- Thomas, D.; Elliott, E.J.; Baur, L. Low glycaemic index or low glycaemic load diets for overweight and obesity. Cochrane Database Syst. Rev. 2007, 25, 822. [Google Scholar] [CrossRef]
- Bornet, F.R.; Jardy-Gennetier, A.-E.; Jacquet, N.; Stowell, J. Glycaemic response to foods: Impact on satiety and long-term weight regulation. Appetite 2007, 49, 535–553. [Google Scholar] [CrossRef] [PubMed]
- Atkinson, F.S.; Foster-Powell, K.; Brand-Miller, J.C. International Tables of Glycemic Index and Glycemic Load Values: 2008. Diabetes Care 2008, 31, 2281–2283. [Google Scholar] [CrossRef]
- Holub, I.; Gostner, A.; Theis, S.; Nosek, L.; Kudlich, T.; Melcher, R.; Scheppach, W. Novel findings on the metabolic effects of the low glycaemic carbohydrate isomaltulose (Palatinose™). Br. J. Nutr. 2010, 103, 1730–1737. [Google Scholar] [CrossRef] [PubMed]
- Stunkard, A.J.; Messick, S. The three-factor eating questionnaire to measure dietary restraint, disinhibition and hunger. J. Psychosom. Res. 1985, 29, 71–83. [Google Scholar] [CrossRef]
- Food Standards Agency. Eatwell Guide. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/528193/Eatwell_guide_colour.pdf. (accessed on 5 August 2019).
- Gibson, R.S. Principles of Nutritional Assessment, 2nd ed.; Oxford University Press: Oxford, UK, 2005; ISBN 9780195171693. [Google Scholar]
- Weir, J.B.D.V. New methods for calculating metabolic rate with special reference to protein metabolism. J. Physiol. 1949, 109, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Frayn, K.N. Calculation of substrate oxidation rates in vivo from gaseous exchange. J. Appl. Physiol. 1983, 55, 628–634. [Google Scholar] [CrossRef]
- Matthews, J.N.; Altman, D.G.; Campbell, M.J.; Royston, P. Analysis of serial measurements in medical research. BMJ 1990, 300, 230–235. [Google Scholar] [CrossRef]
- Allen, J.C. Sample Size Calculation for Two Independent Groups: A Useful Rule of Thumb. Proc. Singap. Heal. 2011, 20, 138–140. [Google Scholar] [CrossRef]
- Anderson, M.J.; Carey, A.L.; Newman, D.G.; Kriketos, A.D.; Cooney, G.J.; Bruce, C.R.; Bonen, A.; Hawley, J.A. Muscle Oxidative Capacity Is a Better Predictor of Insulin Sensitivity than Lipid Status. J. Clin. Endocrinol. Metab. 2003, 88, 5444–5451. [Google Scholar]
- Goodpaster, B.H.; Katsiaras, A.; Kelley, D.E. Enhanced fat oxidation through physical activity is associated with improvements in insulin sensitivity in obesity. Diabetes 2003, 52, 2191–2197. [Google Scholar] [CrossRef]
- Venables, M.C.; Jeukendrup, A.E. Endurance Training and Obesity. Med. Sci. Sports Exerc. 2008, 40, 495–502. [Google Scholar] [CrossRef] [PubMed]
- Isken, F.; Klaus, S.; Petzke, K.J.; Loddenkemper, C.; Pfeiffer, A.F.H.; O Weickert, M. Impairment of fat oxidation under high- vs. low-glycemic index diet occurs before the development of an obese phenotype. Am. J. Physiol. Metab. 2010, 298, E287–E295. [Google Scholar] [CrossRef] [PubMed]
- Brand-Miller, J.C.; Holst, S.H.; Pawlak, D.B.; McMillan, J. Glycemic index and obesity. American J. of Clini. Nutri. 2002, 76, 281–285. [Google Scholar] [CrossRef]
- Thomas, D.; Brotherhood, J.; Brand, J. Carbohydrate Feeding before Exercise: Effect of Glycemic Index. Int. J. Sports Med. 1991, 12, 180–186. [Google Scholar] [CrossRef] [PubMed]
- Rogge, M.M. The Role of Impaired Mitochondrial Lipid Oxidation in Obesity. Boil. Res. Nurs. 2009, 10, 356–373. [Google Scholar] [CrossRef]
- Ross, R.; Freeman, J.; Hudson, R.; Janssen, I. Abdominal Obesity, Muscle Composition, and Insulin Resistance in Premenopausal Women. J. Clin. Endocrinol. Metab. 2002, 87, 5044–5051. [Google Scholar] [CrossRef] [PubMed]
- Murakami, K.; McCaffrey, T.A.; Livingstone, M.B.E. Associations of dietary glycaemic index and glycaemic load with food and nutrient intake and general and central obesity in British adults. Br. J. Nutr. 2013, 110, 2047–2057. [Google Scholar] [CrossRef]
- Ebbeling, C.B.; Leidig, M.M.; Feldman, H.A.; Lovesky, M.M.; Ludwig, D.S. Effects of a Low–Glycemic Load vs Low-Fat Diet in Obese Young Adults. JAMA 2007, 297, 2092. [Google Scholar] [CrossRef]
- Slabber, M.; Barnard, H.C.; Kuyl, J.M.; Dannhauser, A.; Schall, R. Effects of a low-insulin-response, energy-restricted diet on weight loss and plasma insulin concentrations in hyperinsulinemic obese females. Am. J. Clin. Nutr. 1994, 60, 48–53. [Google Scholar] [CrossRef]
- Pereira, E.V.; Costa, J.D.A.; Alfenas, R.D.C.G. Effect of glycemic index on obesity control. Arch. Endocrinol. Metab. 2015, 59, 245–251. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Hoffmann, G. Long-term effects of low glycemic index/load vs. high glycemic index/load diets on parameters of obesity and obesity-associated risks: A systematic review and meta-analysis. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 699–706. [Google Scholar] [CrossRef] [PubMed]
- Jenkins, D.J.; Wolever, T.M.; Taylor, R.H.; Griffiths, C.; Krzemińska, K.; A Lawrie, J.; Bennett, C.M.; Goff, D.V.; Sarson, D.L.; Bloom, S.R. Slow release dietary carbohydrate improves second meal tolerance. Am. J. Clin. Nutr. 1982, 35, 1339–1346. [Google Scholar] [CrossRef] [PubMed]
- Fletcher, A.J.; Perfield II, J.W.; Thyfault, J.P.; Rector, R.S. The Second Meal Effect and Its Influence on Glycemia. J. Nutri. Disorder Ther. 2012, 02. [Google Scholar] [CrossRef]
- Keyhani-Nejad, F.; Kemper, M.; Schueler, R.; Pivovarova, O.; Rudovich, N.; Pfeiffer, A.F. Effects of Palatinose and Sucrose Intake on Glucose Metabolism and Incretin Secretion in Subjects With Type 2 Diabetes. Diabetes Care 2016, 39, e38–e39. [Google Scholar] [CrossRef] [PubMed]
- Keyhani-Nejad, F.; Irmler, M.; Isken, F.; Wirth, E.K.; Beckers, J.; Birkenfeld, A.L.; Pfeiffer, A.F.H. Nutritional strategy to prevent fatty liver and insulin resistance independent of obesity by reducing glucose-dependent insulinotropic polypeptide responses in mice. Diabetologia 2015, 58, 374–383. [Google Scholar] [CrossRef] [PubMed]
- Pfeiffer, A.F.; Keyhani-Nejad, F. High Glycemic Index Metabolic Damage – a Pivotal Role of GIP and GLP-1. Trends Endocrinol. Metab. 2018, 29, 289–299. [Google Scholar] [CrossRef]
- Holst, J.J. The Physiology of Glucagon-like Peptide 1. Physiol. Rev. 2007, 87, 1409–1439. [Google Scholar] [CrossRef] [PubMed]
- Ball, S.D.; Keller, K.R.; Moyer-Mileur, L.J.; Ding, Y.-W.; Donaldson, D.; Jackson, W.D. Prolongation of satiety after low versus moderately high glycemic index meals in obese adolescents. Pediatrics 2003, 111, 488–494. [Google Scholar] [CrossRef]
- Warren, J.M.; Henry, C.J.K.; Simonite, V. Low Glycemic Index Breakfasts and Reduced Food Intake in Preadolescent Children. Pediatrics 2003, 112, 112. [Google Scholar] [CrossRef]

| Isomaltulose | Sucrose | |||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | Week 4 | Week 8 | Week 12 | Baseline | Week 4 | Week 8 | Week 12 | |
| Females/males (n) | 21/4 (25) | – | – | – | 20/5 (25) | – | – | – |
| Age (yr) | 40.2 ± 12 | – | – | – | 41.2 ± 12 | – | – | – |
| Anthropometrics and body composition | ||||||||
| Weight (kg) | 82.8 ± 13.3 a | 81.0 ± 13.2 b | 80.0 ± 12.4 c | 79.6 ± 12.5 c | 83.2 ± 12.6 a | 81.9 ± 12.2 b | 81.3 ± 11.8 b | 81.0 ± 11.7 b |
| BMI (kg/m2) | 29.7 ± 2.9 a | 29.0 ± 2.9 b | 28.7 ± 2.8 c | 28.6 ± 2.9 c | 29.1 ± 2.5 a | 28.7 ± 2.4 b | 28.5 ± 2.3 b | 28.5 ± 2.3 b |
| WC (cm) | 91.4 ± 10.2 a | 90.1 ± 9.9 a | 87.9 ± 8.8 a | 87.9 ± 7.3 a | 90.7 ± 7.5 a | 89.1 ± 8.1 a | 90.0 ± 6.3 a | 89.1 ± 7.5 a |
| Fat mass (%) | 38.9 ± 5.7 a | 38.0 ± 6.1 a,b | 38.2 ± 6.0 a,b | 37.0 ± 6.9 b | 40.1 ± 6.2 a | 39.3 ± 6.8 a | 39.9 ± 6.5 a | 39.3 ± 6.6 a |
| Fat free mass (%) | 60.9 ± 5.8 a | 61.7 ± 6.6 a,b | 61.8 ± 6.0 a,b | 63.0 ± 6.9 b | 59.9 ± 6.2 a | 61.0 ± 6.9 a | 60.3 ± 6.6 a | 61.0 ± 6.6 a |
| Energy intake and metabolism | ||||||||
| Total EI (kcal/d) | 2223 ± 486 *,a | 1828 ± 397 b | 1719 ± 347 b | 1679 ± 306 b | 1900±372 *,a | 1705 ± 344 a,b | 1583 ± 233 b | 1617 ± 245 b |
| REE (kcal/d) | 1538 ± 318 a | 1526 ± 353 a | 1480 ± 336 a,b | 1460 ± 333 b | 1502 ± 226 a | 1472 ± 223 a | 1467 ± 235 a | 1463 ± 241 a |
| ppEE (kcal/d) | 1781 ± 366 a | 1745 ± 336 a | 1652 ± 456 a | 1690 ± 291 b | 1800 ± 278 a | 1762 ± 233 a | 1749 ± 240 a | 1747 ± 238 a |
| Fasting RQ | 0.81 ± 0.06 a | 0.81 ± 0.06 a | 0.79 ± 0.05 a | 0.80 ± 0.05 a | 0.80 ± 0.06 a | 0.80 ± 0.05 a | 0.79 ± 0.05 a | 0.81 ± 0.06 a |
| ΔRQpp-fasting | 0.04 ± 0.05 a | 0.03 ± 0.10 a | 0.05 ± 0.05 a | 0.06 ± 0.05 a | 0.07 ± 0.05 a | 0.07 ± 0.04 a | 0.07 ± 0.04 a | 0.07 ± 0.03 a |
| iAUC2h RQ | 4.4 ± 4.9 a | 3.1 ± 10 a | 5.6 ± 6.5 a | 6.2 ± 6.5 a | 6.8 ± 7.9 a | 6.9 ± 6.8 a | 7.7 ± 8.2 a | 6.8 ± 6.6 a |
| Total AUC2h CO (kcal) | 64 ± 34 a | 65 ± 30 *,a | 62 ± 23 a | 68 ± 29 a | 74 ± 34 a | 93 ± 57 *,a | 70 ± 31 a | 78 ± 36 a |
| Total AUC2h FO (kcal) | 78 ± 51 a | 77 ± 47 a | 76 ± 40 a | 71 ± 44 a | 75 ± 36 a | 68 ± 31 a | 73 ± 37 a | 62 ± 32 a |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lightowler, H.; Schweitzer, L.; Theis, S.; Henry, C.J. Changes in Weight and Substrate Oxidation in Overweight Adults Following Isomaltulose Intake During a 12-Week Weight Loss Intervention: A Randomized, Double-Blind, Controlled Trial. Nutrients 2019, 11, 2367. https://doi.org/10.3390/nu11102367
Lightowler H, Schweitzer L, Theis S, Henry CJ. Changes in Weight and Substrate Oxidation in Overweight Adults Following Isomaltulose Intake During a 12-Week Weight Loss Intervention: A Randomized, Double-Blind, Controlled Trial. Nutrients. 2019; 11(10):2367. https://doi.org/10.3390/nu11102367
Chicago/Turabian StyleLightowler, Helen, Lisa Schweitzer, Stephan Theis, and Christiani Jeyakumar Henry. 2019. "Changes in Weight and Substrate Oxidation in Overweight Adults Following Isomaltulose Intake During a 12-Week Weight Loss Intervention: A Randomized, Double-Blind, Controlled Trial" Nutrients 11, no. 10: 2367. https://doi.org/10.3390/nu11102367
APA StyleLightowler, H., Schweitzer, L., Theis, S., & Henry, C. J. (2019). Changes in Weight and Substrate Oxidation in Overweight Adults Following Isomaltulose Intake During a 12-Week Weight Loss Intervention: A Randomized, Double-Blind, Controlled Trial. Nutrients, 11(10), 2367. https://doi.org/10.3390/nu11102367





