Food Security of Adolescents in Selected Khat- and Coffee-Growing Areas in the Sidama Zone, Southern Ethiopia
Abstract
1. Introduction
2. Materials and Methods
2.1. Selection of the Study Sites
Description of the Study Sites
2.2. Methods
- (i)
- Worried about having enough food;
- (ii)
- Had to reduce food intake because of shortages of food or money to buy food;
- (iii)
- Had to go without eating because of shortages of food or money to buy food; and
- (iv)
- Had to ask outside the home for food because of shortages of food or money to buy food.
2.3. Statistical Analyses
3. Results
3.1. Descriptive Results
3.2. The Nutritional Status and Food Security of the Adolescents
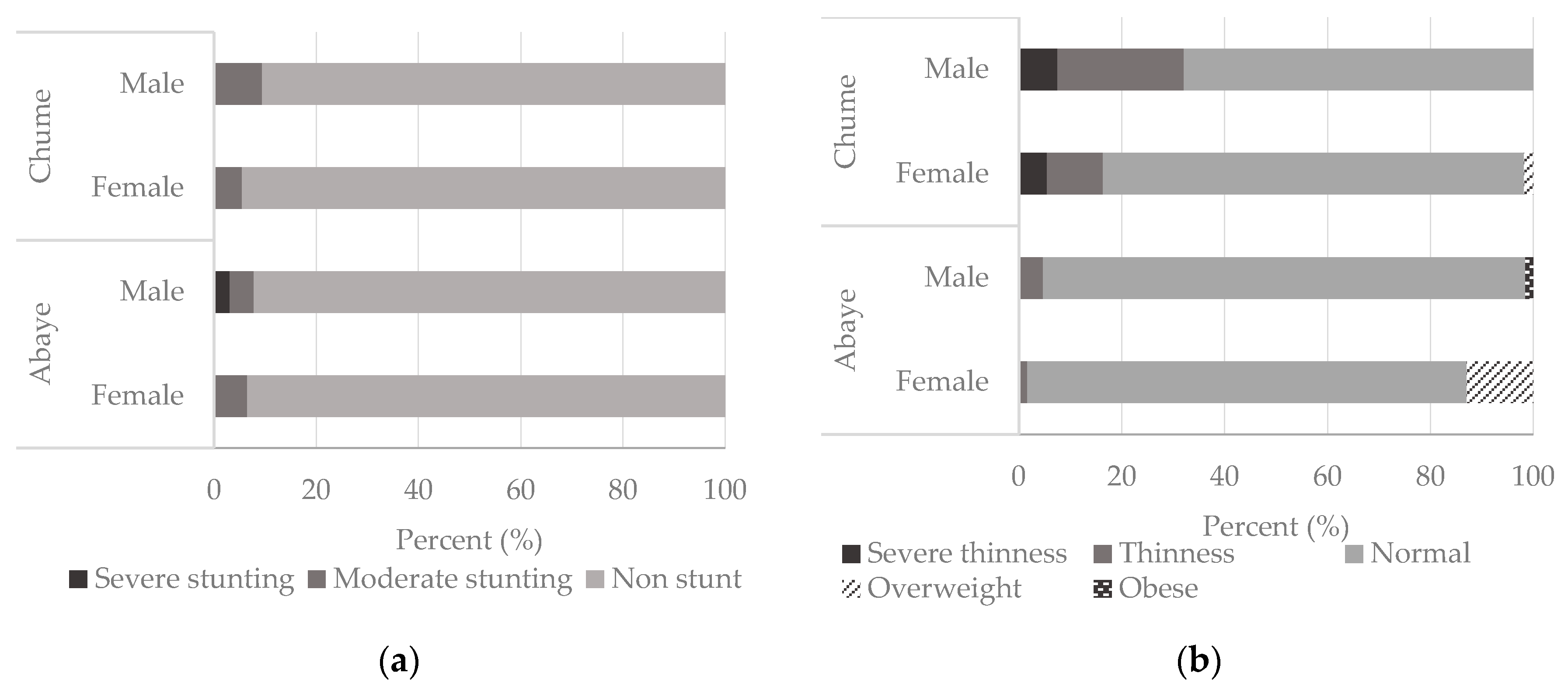
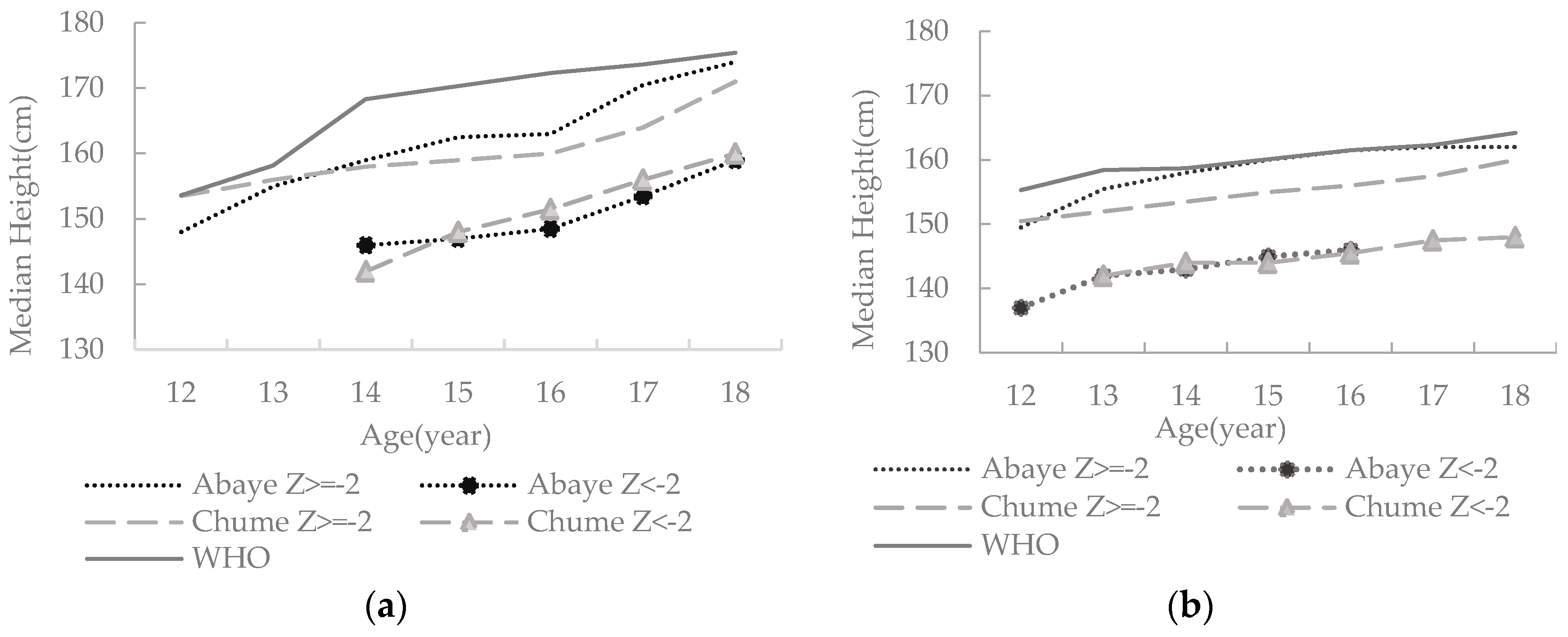
3.2.1. Nutritional Status: Stunting and Thinness
3.2.2. Food Insecurity Experience (FIE)
3.3. Factors Associated with the Stunting, Thinness, and FIE of Adolescents
4. Discussion
4.1. Personal Characteristics
4.2. Socioeconomic and Environmental Factors
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Dick, B.; Ferguson, B.J. Health for the World’s Adolescents: A Second Chance in the Second Decade. J. Adolesc. Health 2015, 56, 3–6. [Google Scholar] [CrossRef] [PubMed]
- The United Nations Children’s Fund (UNICEF). The United Nations Children’s Fund (UNICEF). The State of the World’s Children 2011. In Adolescence an Age of Opportunity; UNICEF: New York, NY, USA, 2011. [Google Scholar]
- Central Statistical Agency (CSA); Inner City Fund (ICF). Ethiopia Demographic and Health Survey 2016; Central Statistical Agency (CSA) and ICF: Addis Ababa, Ethiopia, 2016.
- World Health Organization. Adolescent Nutrition: A Review of the Situation in Selected South-East Asian Countries; WHO: New Delhi, India, 2006. [Google Scholar]
- Mramba, L.; Ngari, M.; Mwangome, M.; Muchai, L.; Bauni, E.; Walker, A.S.; Gibb, D.M.; Fegan, G.; Berkley, J.A. A growth reference for mid upper arm circumference for age among school age children and adolescents, and validation for mortality: Growth curve construction and longitudinal cohort study. BMJ 2017, 358, j3423. [Google Scholar] [CrossRef] [PubMed]
- Melaku, Y.A.; Zello, G.A.; Gill, T.K.; Adams, R.J.; Shi, Z. Prevalence and factors associated with stunting and thinness among adolescent students in Northern Ethiopia: A comparison to World Health Organization standards. Arch. Public Health 2015, 73, 44. [Google Scholar] [CrossRef] [PubMed]
- Largo, R.H. Catch-Up Growth during Adolescence. Horm. Res. 1993, 39, 41–48. [Google Scholar] [CrossRef] [PubMed]
- Gat-Yablonski, G.; Phillip, M. Nutritionally-Induced Catch-Up Growth. Nutrients 2015, 7, 517–551. [Google Scholar] [CrossRef] [PubMed]
- Leenstra, T.; Petersen, L.T.; Kariuki, S.K.; Oloo, A.J.; Kager, P.A.; Kuile, F.O.T. Prevalence and severity of malnutrition and age at menarche; cross-sectional studies in adolescent schoolgirls in western Kenya. Eur. J. Clin. Nutr. 2005, 59, 41–48. [Google Scholar] [CrossRef] [PubMed]
- Gebreyohannes, Y.; Shiferaw, S.; Demtsu, B.; Bugssa, G. Nutritional Status of Adolescents in Selected Government and Private Secondary Schools of Addis Ababa, Ethiopia. Int. J. Nutr. Food Sci. 2014, 3, 504. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Health for the World’s Adolescents: A Second Chance in the Second Decade; WHO Press: Geneva, Switzerland, 2014. [Google Scholar]
- Patton, G.C.; Sawyer, S.M.; Ross, D.A.; Viner, R.M.; Santelli, J.S. From Advocacy to Action in Global Adolescent Health. J. Adolesc. Health 2016, 59, 375–377. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Guideline: Implementing Effective Actions for Improving Adolescent Nutrition; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Pinhas-Hamiel, O.; Reichman, B.; Shina, A.; Derazne, E.; Tzur, D.; Yifrach, D.; Wiser, I.; Afek, A.; Shamis, A.; Tirosh, A.; et al. Sex Differences in the Impact of Thinness, Overweight, Obesity, and Parental Height on Adolescent Height. J. Adolesc. Health 2017, 61, 233–239. [Google Scholar] [CrossRef] [PubMed]
- Evans, E.W.; Lo, C. Adolescents: Nutritional Problems of Adolescents. In Encyclopedia of Human Nutrition; Elsevier: New York, NY, USA, 2013; pp. 14–22. [Google Scholar]
- Abarca-Gómez, L.; Abdeen, Z.A.; Hamid, Z.A.; Abu-Rmeileh, N.M.; Acosta-Cazares, B.; Acuin, C.; Adams, R.J.; Aekplakorn, W.; Afsana, K.; Aguilar-Salinas, C.A.; et al. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 2017, 390, 2627–2642. [Google Scholar] [CrossRef]
- Zenebe, M.; Gebremedhin, S.; Henry, C.J.; Regassa, N. School feeding program has resulted in improved dietary diversity, nutritional status and class attendance of school children. Ital. J. Pediatr. 2018, 44, 16. [Google Scholar] [CrossRef] [PubMed]
- Coll-Black, S.; Gilligan, D.O.; Hoddinott, J.; Kumar, N.; Wiseman, W. 10 Targeting Food Security Interventions in Ethiopia: The Productive Safety Net. In Food and Agriculture in Ethiopia: Progress and Policy Challenges; Dorosh, P.A., Rashid, S., Eds.; University of Pennsylvania Press: Philadelphia, PA, USA, 2012; pp. 280–317. [Google Scholar]
- Regassa, N. Small holder farmers coping strategies to household food insecurity and hunger in Southern Ethiopia. Ethiop. J. Environ. Stud. Manag. 2011, 4. [Google Scholar] [CrossRef]
- Anderson, A.K.D.; Beckerleg, S.; Hailu, D. The Khat Controversy. Stimulating the Debate on Drugs. Soc. Hist. Med. 2008, 21, 189–190. [Google Scholar] [CrossRef]
- The United States Department of Agriculture (USDA). Coffee: World Markets and Trade; USDA: Washington, DC, USA, 2017.
- Tefera, A.; Tefera, T. Ethiopia Coffee Annual Report-GAIN Report Number: ET- 1302; The United States Department of Agriculture (USDA): Addis Ababa, Ethiopia, 2013.
- Cochrane, L.; O’Regan, D. Legal harvest and illegal trade: Trends, challenges, and options in khat production in Ethiopia. Int. J. Drug Policy 2016, 30, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Feyisa, T.H.; Aune, J.B. Khat Expansion in the Ethiopian Highlands. Mt. Res. Dev. 2003, 23, 185–189. [Google Scholar] [CrossRef]
- Dessie, G.; Kinlund, P. Khat Expansion and Forest Decline in Wondo Genet, Ethiopia. Geogr. Ann. Ser. B 2008, 90, 187–203. [Google Scholar] [CrossRef]
- Sahle, M.; Yeshitela, K.; Saito, O. Mapping the supply and demand of Enset crop to improve food security in Southern Ethiopia. Agron. Sustain. Dev. 2018, 38, 7. [Google Scholar] [CrossRef]
- De Onis, M.; Habicht, J.P. Anthropometric reference data for international use: Recommendations from a World Health Organization Expert Committee. Am. J. Clin. Nutr. 1996, 64, 650–658. [Google Scholar] [CrossRef] [PubMed]
- Hadley, C.; Lindstrom, D.; Tessema, F.; Belachew, T. Gender bias in the food insecurity experience of Ethiopian adolescents. Soc. Sci. Med. 2008, 66, 427–438. [Google Scholar] [CrossRef] [PubMed]
- Sidama Zone Culture and Tourism Bureau. Sidama Zone: Location, Area and Administrative Divisions. Unpublished work. 2011. [Google Scholar]
- Assefa, E. Assessment of Production and Marketing System of Goats in Dale District; University of Hawassa: Sidama Zone, Ethiopia, 2007. [Google Scholar]
- Sidama Zone Finance and Economic Development Bureau. Sidama Zone: Administrative Divisions’ Area and Total population. Unpublished work. 2017. [Google Scholar]
- Chume Kebele Agricultural Extension Office. Basic information about the Chume kebele. Unpublished work. 2017. [Google Scholar]
- Abaye Kebele Agricultural Extension Office. Basic information about the Abaye kebele. Unpublished work. 2017.
- Dasgupta, A.; Butt, A.; Saha, T.; Basu, G.; Chattopadhyay, A.; Mukherjee, A. Assessment of malnutrition among adolescents: Can BMI be replaced by MUAC. Indian J. Commun. Med. 2010, 35, 276. [Google Scholar] [CrossRef] [PubMed]
- The World Health Organization (WHO). WHO Child Growth Standards Length/Height-for-Age, Weight-for-Age, Weight-for-Length, Weight-for-Height and Body Mass Index-for-Age Methods and Development; WHO: Geneva, Switzerland, 2006. [Google Scholar]
- Sarkar, S.K.; Midi, H.; Rana, S. Model Selection in Logistic Regression and Performance of its Predictive Ability. Aust. J. Basic Appl. Sci. 2010, 4, 5813–5822. [Google Scholar]
- Wolde, M.; Berhan, Y.; Chala, A. Determinants of underweight, stunting and wasting among schoolchildren. BMC Public Health 2015, 15, 8. [Google Scholar] [CrossRef] [PubMed]
- The World Health Organization (WHO). Global Database on Child Growth and Malnutrition. Available online: http://www.who.int/nutgrowthdb/about/introduction/en/index5.html (accessed on 13 May 2018).
- Al-Shaikh, M.H.; Bashaaib, M.O. Unpredictable pulmonary tuberculosis with Hydatid cyst in adult male. Egypt. J. Chest Dis. Tuberc. 2017, 66, 317–319. [Google Scholar] [CrossRef]
- Bogin, B. Patterns of Human Growth; Cambridge University Press: Cambridge, UK, 1999; Volume 23. [Google Scholar]
- Perola, M. Genetics of Human Stature: Lessons from Genome-Wide Association Studies. Horm. Res. Paediatr. 2011, 76, 10–11. [Google Scholar] [CrossRef] [PubMed]
- Mulugeta, A.; Hagos, F.; Stoecker, B.; Kruseman, G.; Linderhof, V.; Abraha, Z.; Yohannes, M.; Samuel, G.G. Nutritional Status of Adolescent Girls from Rural Communities of Tigray, Northern Ethiopia. Ethiop. J. Health Dev. 2009, 23. [Google Scholar] [CrossRef]
- Roy, S.; Barman, S.; Mondal, N.; Sen, J. Prevalence of Stunting and Thinness Among Adolescent Girls Belonging to the Rajbanshi Population of West Bengal, India. J. Nepal Paediatr. Soc. 2016, 36, 147. [Google Scholar] [CrossRef]
- Haddad, C.N.L.; Peña, C.; Quisumbing, A.S.A. Food Security and Nutrition Implications of Intrahousehold Bias: A Review of Literature; FCND Discussion Paper No. 19; International Food Policy Research Institute: Washington, DC, USA, 1996. [Google Scholar]
- Tessema, M.; Belachew, T.; Ersino, G. Feeding patterns and stunting during early childhood in rural communities of Sidama, South Ethiopia. Pan Afr. Med. J. 2013, 14, 75. [Google Scholar] [PubMed]
- Harris-Fry, H.; Shrestha, N.; Costello, A.; Saville, N.M. Determinants of intra-household food allocation between adults in South Asia–a systematic review. Int. J. Equity Health 2017, 16, 107. [Google Scholar] [CrossRef] [PubMed]
- Dessie, G. Land and Water for Drugs, Cash for Food: Khat Production and Food Security in Ethiopia; I.B. Tauris: London, UK, 2015; Volume 3. [Google Scholar]
- Odenwald, M.; Klein, A.; Warfa, N. Introduction to the special issue: The changing use and misuse of khat (Catha edulis)—Tradition, trade and tragedy. J. Ethnopharmacol. 2010, 132, 537–539. [Google Scholar] [CrossRef] [PubMed]
- Mellisse, B.T.; van de Ven, G.W.J.; Giller, K.E.; Descheemaeker, K. Home garden system dynamics in Southern Ethiopia. Agrofor. Syst. 2017, 1–7. [Google Scholar] [CrossRef]
- Mbow, C.; van Noordwijk, M.; Prabhu, R.; Simons, T. Knowledge gaps and research needs concerning agroforestry’s contribution to Sustainable Development Goals in Africa. Curr. Opin. Environ. Sustain. 2014, 6, 162–170. [Google Scholar] [CrossRef]
- Bezu, S.; Holden, S. Are Rural Youth in Ethiopia Abandoning Agriculture? World Dev. 2014, 64, 259–272. [Google Scholar] [CrossRef]
- Minten, B.; Dereje, M.; Engida, E.; Tamru, S. Tracking the Quality Premium of Certified Coffee: Evidence from Ethiopia. World Dev. 2018, 101, 119–132. [Google Scholar] [CrossRef]
- Fan, S.; Brzeska, J.; Keyzer, M.; Halsema, A. From Subsistence to Profit Transforming Smallholder Farms; International Food Policy Research Institute: Washington, DC, USA, 2013. [Google Scholar]
- Negash, A.; Niehof, A. The significance of enset culture and biodiversity for rural household food and livelihood security in southwestern Ethiopia. Agric. Hum. Values 2004, 21, 61–71. [Google Scholar] [CrossRef]
- Roba, K.; Abdo, M.; Wakayo, T. Nutritional Status and Its Associated Factors among School Adolescent Girls in Adama City, Central Ethiopia. J. Nutr. Food Sci. 2016, 6, 2. [Google Scholar]
- Mohammed, A.Y. Nutritional Status and Associated Risk Factors Among Adolescents Girls in Agarfa High School, Bale Zone, Oromia Region, South East Ethiopia. Int. J. Nutr. Food Sci. 2015, 4, 445. [Google Scholar] [CrossRef]
- Pal, A.; Pari, A.K.; Sinha, A.; Dhara, P.C. Prevalence of undernutrition and associated factors: A cross-sectional study among rural adolescents in West Bengal, India. Int. J. Pediatr. Adolesc. Med. 2017, 4, 9–18. [Google Scholar] [CrossRef]
- Shaikh, R.; Haboubi, G. A comparison of the nutritional status of adolescents from selected schools of South India and UAE: A cross-sectional study. Indian J. Commun. Med. 2009, 34, 108. [Google Scholar] [CrossRef] [PubMed]
- Mark, K.G.-D.S.; Lambert, M.; O’Loughlin, J. Household Income, Food Insecurity and Nutrition in Canadian Youth. Can. J. Public Health. 2012, 102, 94–99. [Google Scholar]
- Assefa, H.; Belachew, T.; Negash, L. Socioeconomic Factors Associated with Underweight and Stunting among Adolescents of Jimma Zone, South West Ethiopia: A Cross-Sectional Study. ISRN Public Health 2013, 2013. [Google Scholar] [CrossRef]
- Demissie, S. Magnitude and Factors Associated with Malnutrition in Children 6–59 Months of Age in Pastoral Community of Dollo Ado District, Somali Region, Ethiopia. Sci. J. Public Health 2013, 1, 175. [Google Scholar] [CrossRef]
- Sandiford, P.; Cassel, J.; Montenegro, M.; Sanchez, G. The Impact of Women’s Literacy on Child Health and its Interaction with Access to Health Services. Popul. Stud. (NY) 1995, 49, 5–17. [Google Scholar] [CrossRef]
- Gezon, L.L. Drug Crops and Food Security: The Effects of Khat on Lives and Livelihoods in Northern Madagascar. Cult. Agric. Food Environ. 2012, 34, 124–135. [Google Scholar] [CrossRef]

| Variable | Area | Sex | N | Min | Max | Median | Mean (SD) | S. Error | d.f | Test Statistics 1 | p-Value |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Age (year) | Abaye | F | 62 | 12.0 | 18.0 | 14.4 | 14.72 (2.05) | 0.26 | |||
| Chume | 55 | 12.0 | 17.8 | 13.9 | 13.90 (1.82) | 0.25 | 1 | 1470 | 0.191 | ||
| Abaye | M | 64 | 12.0 | 18.0 | 14.7 | 14.95 (2.03) | 0.25 | ||||
| Chume | 53 | 12.1 | 18.0 | 14.9 | 15.00 (1.61) | 0.28 | 1 | 1113.5 | 0.001 | ||
| Weight (kg) | Abaye | F | 62 | 30 | 71 | 50.0 | 48.72 (9.41) | 1.21 | |||
| Chume | 55 | 28 | 69 | 43.0 | 42.80 (7.18) | 0.97 | 1 | 981 | 0.000 | ||
| Abaye | M | 64 | 29 | 67 | 48.0 | 46.31 (9.81) | 1.22 | ||||
| Chume | 53 | 31 | 68 | 43.0 | 45.76 (9.16) | 1.26 | 1 | 1644 | 0.776 | ||
| Height (cm) | Abaye | F | 62 | 137 | 173 | 157.5 | 155.95 (7.92) | 1.00 | |||
| Chume | 55 | 143 | 173 | 154.0 | 154.36 (6.59) | 0.89 | 1 | 1432 | 0.136 | ||
| Abaye | M | 64 | 137 | 180 | 158.5 | 157.81 (10.27) | 1.28 | ||||
| Chume | 53 | 144 | 188 | 162.0 | 163.68 (9.41) | 1.29 | 1 | 1165.5 | 0.004 | ||
| HAZ | Abaye | F | 62 | −2.73 | 1.71 | −0.25 | −0.33 (0.91) | 0.12 | |||
| Chume | 55 | −2.73 | 1.52 | −0.91 | −0.82 (0.94) | 0.13 | 1 | 1217.5 | 0.008 ** | ||
| Abaye | M | 64 | −3.46 | 1.64 | −0.37 | −0.55 (1.05) | 0.13 | ||||
| Chume | 53 | −2.63 | 2.24 | −0.53 | −0.50 (1.15) | 0.16 | 1 | 1505.5 | 0.297 | ||
| BMIZ | Abaye | F | 62 | −2.09 | 1.82 | 0.09 | −0.01 (0.85) | 0.11 | |||
| Chume | 55 | −4.07 | 1.01 | −0.77 | −0.96 (1.04) | 0.14 | 1 | 831 | 0.000 ** | ||
| Abaye | M | 64 | −2.29 | 2.67 | −0.41 | −0.43 (0.90) | 0.11 | ||||
| Chume | 53 | −3.32 | 0.04 | −1.43 | −1.60 (0.86) | 0.12 | 1 | 866.5 | 0.000 ** | ||
| Education (school year) | Abaye | F | 62 | 2 | 12 | 5 | 5.94 (2.78) | 0.35 | |||
| Chume | 55 | 2 | 10 | 7 | 6.42 (2.20) | 0.29 | 1 | 1410 | 0.102 | ||
| Abaye | M | 64 | 0 | 10 | 6 | 5.64 (2.22) | 0.28 | ||||
| Chume | 53 | 4 | 10 | 6 | 6.02 (1.69) | 0.23 | 1 | 1577.5 | 0.511 | ||
| Family size (number) | Abaye | F | 62 | 2 | 14 | 7.5 | 7.29 (2.51) | 0.319 | |||
| Chume | 55 | 3 | 9 | 6 | 6.24 (1.41) | 0.191 | 1 | 1159.5 | 0.003 ** | ||
| Abaye | M | 64 | 3 | 15 | 7.5 | 7.33 (2.25) | 0.281 | ||||
| Chume | 53 | 3 | 8 | 6 | 5.94 (1.34) | 0.184 | 1 | 971.5 | 0.000 ** |
| N (%) | Crude OR | (Sig.) | Adjusted OR | (Sig.) | ||
|---|---|---|---|---|---|---|
| Variable | Not Stunted | Stunted | (95% CI) | p-Value | (95% CI) | p-Value |
| Sex | ||||||
| Female | 110 (94.0) | 7 (6.0) | 0.681 (0.250, 1.854) | 0.452 | 0.616 (0.192, 1.971) | 0.414 |
| Male | 107 (91.5) | 10 (8.5) | 1.00 | 1.00 | ||
| Age | ||||||
| 12–14 years | 107 (89.2) | 13 (10.8) | 3.341 (1.056, 10.571) | 0.04* | 3.569 (1.109, 11.485) | 0.033 * |
| 15–18 years | 110 (96.5) | 4 (3.5) | 1.00 | 1.00 | ||
| Education | ||||||
| Up to grade 6 | 89 (93.7) | 6 (6.3) | 0.784 (0.280, 2.199) | 0.644 | 0.364 (0.100, 1.318) | 0.124 |
| Above grade 6 | 128 (92.1) | 11 (7.9) | 1.00 | 1.00 | ||
| Maternal Education | ||||||
| Illiterate @ | 101 (87.8) | 14 (12.2) | 5.360 (1.497, 19.184) | 0.01* | 5.641 (1.560, 20.392) | 0.008 ** |
| Literate | 116 (97.5) | 3 (2.5) | 1.00 | 1.00 | ||
| Area | ||||||
| Abaye | 117 (92.9) | 9 (7.1) | 0.962 (0.358, 2.585) | 0.938 | 0.993 (0.256, 3.855) | 0.992 |
| Chume | 100 (92.6) | 8 (7.8) | 1.00 | 1.00 | ||
| Family size | ||||||
| Over 6 members | 117 (90.7) | 12 (9.3) | 2.051 (0.699, 6.022) | 0.191 | 3.196 (0.954, 10.704) | 0.060 |
| Up to 6 members | 100 (95.2) | 5 (4.8) | 1.00 | 1.00 | ||
| Off farm income | ||||||
| Yes | 67 (89.3) | 8 (10.7) | 1.99 (0.736, 5.382) | 0.175 | 2.337 (0.766, 7.133) | 0.136 |
| No | 150 (94.3) | 9 (5.7) | 1.00 | 1.00 | ||
| Health problem Ф | ||||||
| Yes (in 30 days) | 67 (90.5) | 7 (9.5) | 1.567 (0.572, 4.294) | 0.382 | 2.142 (0.653, 7.022) | 0.209 |
| No (in 30 days) | 150 (93.8) | 10 (6.2) | 1.00 | 1.00 | ||
| Number of meals | ||||||
| <3 meals a day | 87 (89.7) | 10 (10.3) | 2.135 (0.783, 5.822) | 0.139 | 1.664 (1.090, 2.290) | 0.457 |
| ≥3 meals a day | 130 (94.9) | 7 (5.1) | 1.00 | 1.00 | ||
| Animal protein | ||||||
| <3 times a week | 46 (90.2) | 5 (9.8) | 1.549 (0.519, 4.620) | 0.433 | 1.484 (0.420, 5.245) | 0.540 |
| ≥3 times a week | 171 (93.4) | 12 (6.6) | 1.00 | 1.00 | ||
| Family livelihood | ||||||
| Khat | 85 (92.4) | 7 (7.6) | 1.894 (0.472, 7.599) | 0.368 | 1.924 (0.213, 17.353) | 0.852 |
| Other Θ | 63 (90.0) | 7 (10.0) | 2.556 (0.633, 10.311) | 0.187 | 2.266 (0.153, 4.701) | 0.560 |
| Coffee | 69 (95.8) | 3 (4.2) | 1.00 | 1.00 | ||
| N (%) | Crude OR | (Sig.) | Adjusted OR | (Sig.) | ||
|---|---|---|---|---|---|---|
| Variable | Not Thin | Thin | (95% CI) | p-Value | (95% CI) | p-Value |
| Sex | ||||||
| Female | 108 (92.3) | 9 (7.7) | 0.381 (0.166, 0.872) | 0.022 * | 0.386 (0.157, 0.944) | 0.037 * |
| Male | 96 (82.1) | 21 (17.9) | 1.00 | 1.00 | ||
| Age | ||||||
| 12–14 years | 99 (86.8) | 15 (13.2) | 1.061 (0.493, 2.283) | 0.880 | 1.173 (0.439, 3.133) | 0.751 |
| 15–18 years | 105 (87.5) | 15 (12.5) | 1.00 | 1.00 | ||
| Education | ||||||
| Up to grade 6 | 119 (85.6) | 20 (14.4) | 1.429 (0.636, 3.207) | 0.387 | 1.657 (0.607, 4.523) | 0.325 |
| Above grade 6 | 85 (89.5) | 10 (10.5) | 1.00 | 1.00 | ||
| Maternal Education | ||||||
| Illiterate @ | 91 (79.1) | 24 (20.9) | 4.967 (1.948, 12.668) | 0.001 ** | 1.373 (0.401, 4.700) | 0.613 |
| Literate | 113 (95.0) | 6 (5.0) | 1.00 | 1.00 | ||
| Area | ||||||
| Abaye | 122 (96.8) | 4 (3.2) | 0.103 (0.035, 0.307) | 0.000 ** | 0.123 (0.040, 0.375) | 0.000 ** |
| Chume | 82 (75.9) | 26 (24.1) | 1.00 | 1.00 | ||
| Family size | ||||||
| Up to 6 members | 89 (84.8) | 16 (15.2) | 1.477 (0.685,3.186) | 0.320 | 1.394 (0.263, 1.588) | 0.341 |
| Over 6 members | 115 (89.1) | 14 (10.9) | 1.00 | 1.00 | ||
| Off farm income | ||||||
| Yes | 67 (89.3) | 8 (10.7) | 0.744 (0.315, 1.758) | 0.500 | 0.889 (0.264, 2.989) | 0.849 |
| No | 137 (86.2) | 22 (13.8) | 1.00 | 1.00 | ||
| Health problem Ф | ||||||
| Yes (in 30 days) | 64 (86.5) | 10 (13.5) | 1.094 (0.484, 2.470) | 0.829 | 0.883 (0.350, 2.226) | 0.792 |
| No (in 30 days) | 140 (87.5) | 20 (12.5) | 1.00 | 1.00 | ||
| Number of meals | ||||||
| <3 meals a day | 74 (76.3) | 23 (23.7) | 5.772 (2.364, 14.097) | 0.000 ** | 4.164 (1.629, 10.647) | 0.003 ** |
| ≥3 meals a day | 130 (94.9) | 7 (5.1) | 1.00 | 1.00 | ||
| Animal protein | ||||||
| <3 times a week | 43 (84.3) | 8 (15.7) | 1.362 (0. 567, 3.271) | 0.490 | 1.233 (0.405, 3.751) | 0.712 |
| ≥3 times a week | 161 (88.0) | 22 (12.0) | 1.00 | 1.00 | ||
| Family livelihood | ||||||
| Khat | 88 (95.7) | 4 (4.3) | 0.127 (0.041, 0.393) | 0.000 ** | 0.119 (0.035, 0.401) | 0.001 ** |
| Other Θ | 63 (90.0) | 7 (10.0) | 0.310 (0.121, 0.794) | 0.015 * | 0.314 (0.096, 1.029) | 0.056 |
| Coffee | 53 (73.4) | 19 (26.4) | 1.00 | 1.00 | ||
| N (%) | Crude OR | (Sig.) | Adjusted OR | (Sig.) | ||
|---|---|---|---|---|---|---|
| Variable | Food Secure | Food Insecure | (95% CI) | p-Value | (95% CI) | p-Value |
| Sex | ||||||
| Female | 75 (64.1) | 42 (35.9) | 0.834 (0.492, 1.415) | 0.501 | 0.787 (0.445, 1.393) | 0.412 |
| Male | 70 (59.8) | 47 (40.2) | 1.00 | 1.00 | ||
| Age | ||||||
| 12–14 years | 76 (63.3) | 44 (36.7) | 0.888 (0.524, 1.505) | 0.658 | 0.707 (0.368, 1.357) | 0.298 |
| 15–18 years | 69 (60.5) | 45 (39.5) | 1.00 | 1.00 | ||
| Education | ||||||
| Up to grade 6 | 55 (57.9) | 40 (42.1) | 1.336 (0.782, 2.282) | 0.289 | 1.480 (0.766, 2.858) | 0.244 |
| Above grade 6 | 90 (64.7) | 49 (35.3) | 1.00 | 1.00 | ||
| Maternal Education | ||||||
| Illiterate @ | 76 (66.1) | 39 (33.9) | 0.708 (0.417, 1.204) | 0.202 | 0.625 (0.286, 1.365) | 0.239 |
| Literate | 69 (68.0) | 50 (42.0) | 1.00 | 1.00 | ||
| Area | ||||||
| Abaye | 72 (57.1) | 54 (42.9) | 1.564 (0.916, 2.673) | 0.102 | 1.244 (0.466, 3.320) | 0.663 |
| Chume | 73 (67.6) | 35 (32.4) | 1.00 | 1.00 | ||
| Family size | ||||||
| Up to 6 members | 78 (61.5) | 51 (39.5) | 1.153 (0.677, 1.962) | 0.600 | 0.903 (0.498, 1.639) | 0.738 |
| Over 6 members | 67 (63.8) | 38 (36.2) | 1.00 | 1.00 | ||
| Off farm income | ||||||
| Yes | 41 (54.7) | 34 (45.3) | 1.568 (0.896, 2.745) | 0.115 | 1.312 (0.625, 2.756) | 0.473 |
| No | 104 (65.4) | 55 (34.6) | 1.00 | 1.00 | ||
| Health problem Ф | ||||||
| Yes (in 30 days) | 58 (78.4) | 16 (21.6) | 0.329 (0.174, 0.620) | 0.001** | 0.235 (0.115, 0.483) | 0.000 ** |
| No (in 30 days) | 87 (54.4) | 73 (45.6) | 1.00 | 1.00 | ||
| Number of meals | ||||||
| <3 meals a day | 64 (63.9) | 35 (36.1) | 0.868 (0.507, 1.486) | 0.605 | 1.201 (0.564, 2.557) | 0.634 |
| ≥3 meals a day | 83 (60.6) | 54 (39.4) | 1.00 | 1.00 | ||
| Animal protein | ||||||
| <3 times a week | 38 (74.5) | 13 (25.5) | 0.482 (0.240, 0.965) | 0.039 * | 0.651 (0.305, 1.392) | 0.269 |
| ≥3 times a week | 107 (58.5) | 76 (41.5) | 1.00 | 1.00 | ||
| Family livelihood | ||||||
| Khat | 55 (59.8) | 37 (40.2) | 1.634 (0.847, 3.152) | 0.143 | 1.302 (0.439, 3.859) | 0.634 |
| Other Θ | 39 (55.7) | 31 (44.3) | 1.930 (0.965, 3.861) | 0.063 | 1.608 (0.686, 3.768) | 0.275 |
| Coffee | 51 (70.8) | 21 (29.2) | 1.00 | 1.00 | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Juju, D.B.; Sekiyama, M.; Saito, O. Food Security of Adolescents in Selected Khat- and Coffee-Growing Areas in the Sidama Zone, Southern Ethiopia. Nutrients 2018, 10, 980. https://doi.org/10.3390/nu10080980
Juju DB, Sekiyama M, Saito O. Food Security of Adolescents in Selected Khat- and Coffee-Growing Areas in the Sidama Zone, Southern Ethiopia. Nutrients. 2018; 10(8):980. https://doi.org/10.3390/nu10080980
Chicago/Turabian StyleJuju, Denabo Billo, Makiko Sekiyama, and Osamu Saito. 2018. "Food Security of Adolescents in Selected Khat- and Coffee-Growing Areas in the Sidama Zone, Southern Ethiopia" Nutrients 10, no. 8: 980. https://doi.org/10.3390/nu10080980
APA StyleJuju, D. B., Sekiyama, M., & Saito, O. (2018). Food Security of Adolescents in Selected Khat- and Coffee-Growing Areas in the Sidama Zone, Southern Ethiopia. Nutrients, 10(8), 980. https://doi.org/10.3390/nu10080980






