Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls
Abstract
1. Introduction
2. Material and Methods
2.1. Patients, Controls, and Clinical Assessment
2.2. Ethical Publication Statement
2.3. Zinc Measurement
2.4. Statistical Analysis
3. Results
3.1. Cohorts
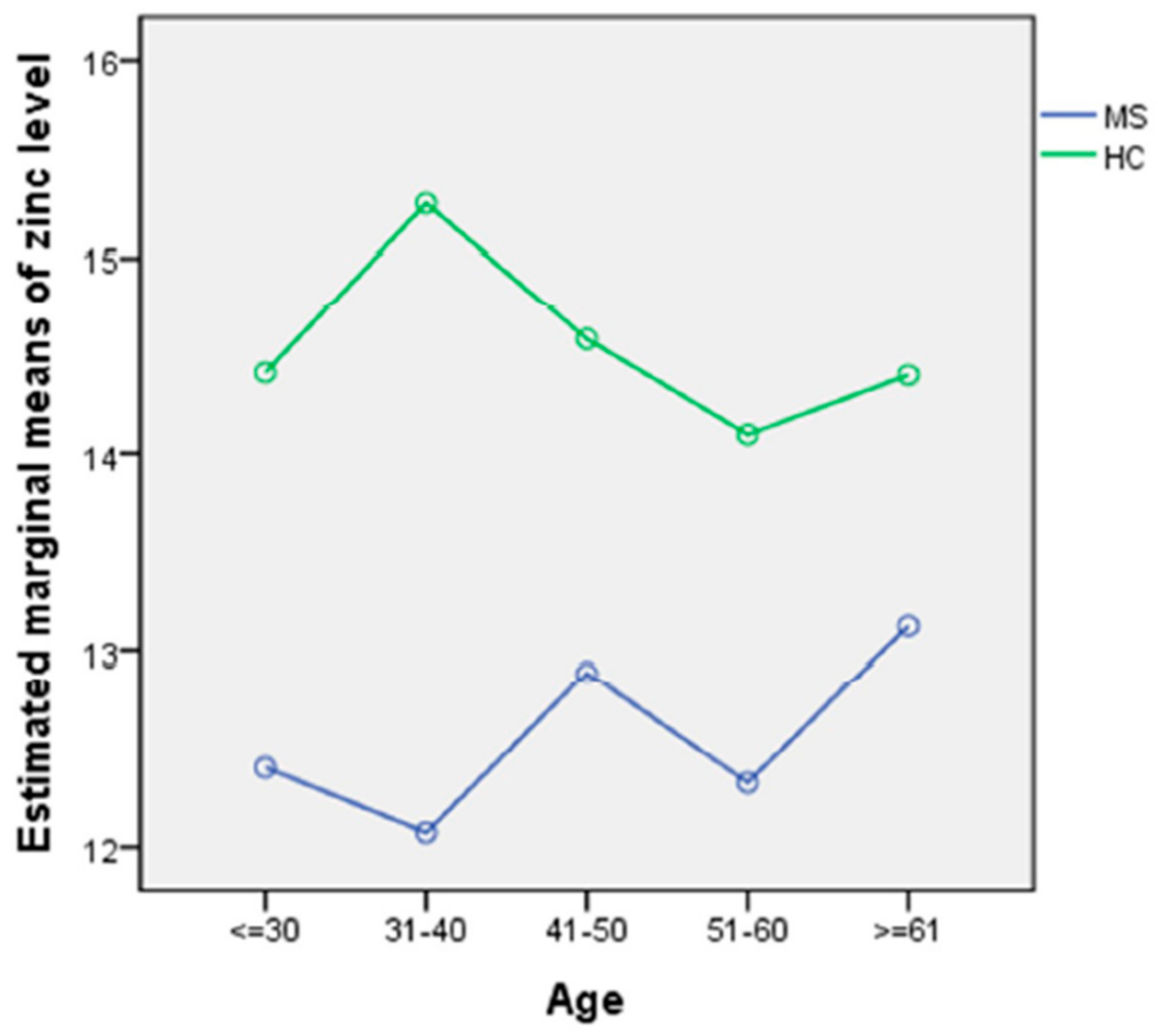
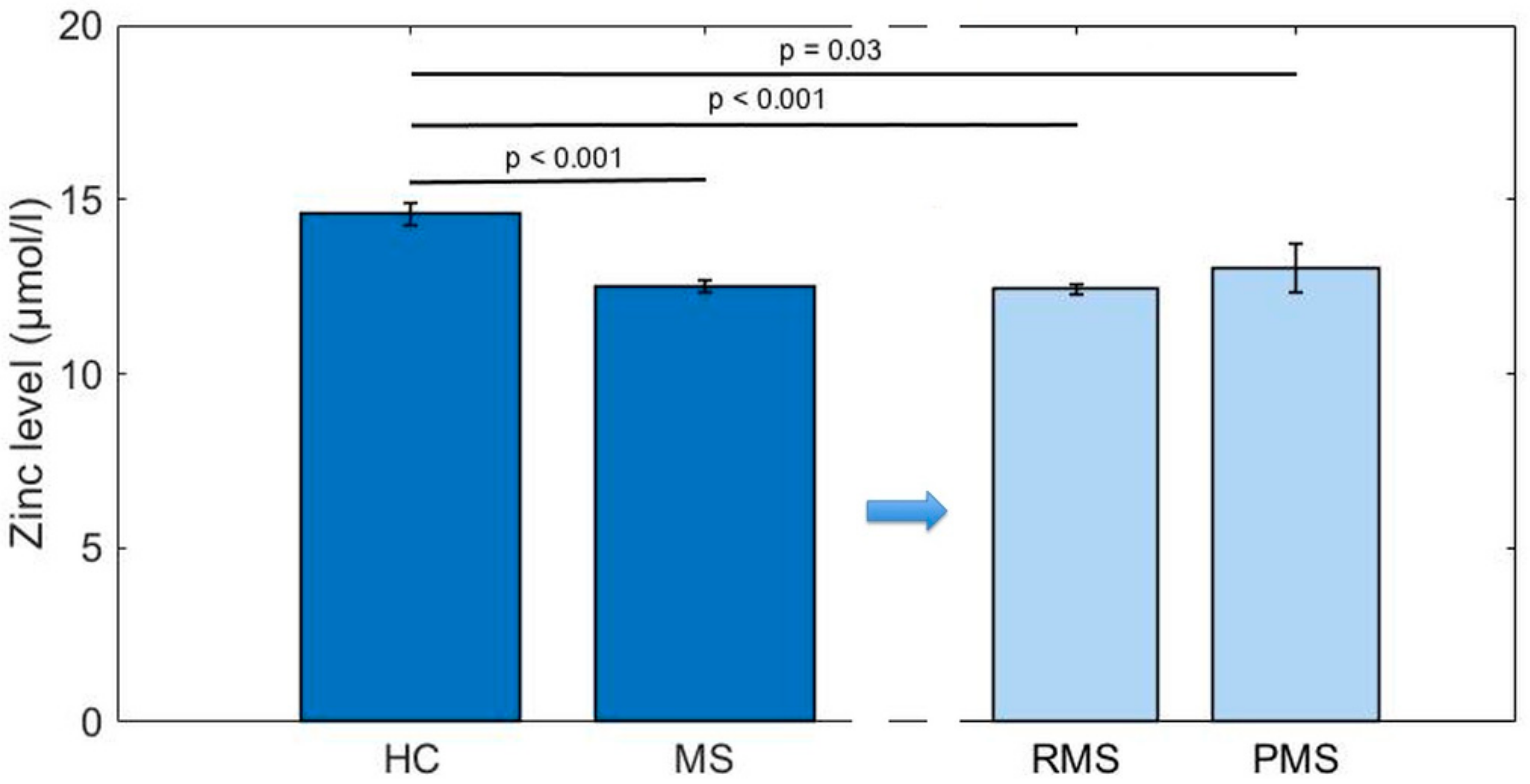
3.2. Serum Zinc Levels
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Weiner, H.L. Multiple sclerosis is an inflammatory T-cell-mediated autoimmune disease. Arch. Neurol. 2004, 61, 1613–1615. [Google Scholar] [CrossRef] [PubMed]
- Riccio, P.; Rossano, R. Nutrition facts in multiple sclerosis. ASN Neuro 2015, 7. [Google Scholar] [CrossRef] [PubMed]
- Maywald, M.; Wessels, I.; Rink, L. Zinc Signals and Immunity. Int. J. Mol. Sci. 2017, 18, 2222. [Google Scholar] [CrossRef] [PubMed]
- Scott, B.J.; Bradwell, A.R. Identification of the serum binding proteins for iron, zinc, cadmium, nickel, and calcium. Clin. Chem. 1983, 29, 629–633. [Google Scholar] [PubMed]
- Vallee, B.L.; Falchuk, K.H. The biochemical basis of zinc physiology. Physiol. Rev. 1993, 73, 79–118. [Google Scholar] [CrossRef] [PubMed]
- Bredholt, M.; Frederiksen, J.L. Zinc in Multiple Sclerosis: A Systematic Review and Meta-Analysis. ASN Neuro 2016, 8. [Google Scholar] [CrossRef] [PubMed]
- Polman, C.H.; Reingold, S.C.; Banwell, B.; Clanet, M.; Cohen, J.A.; Filippi, M.; Fujihara, K.; Havrdova, E.; Hutchinson, M.; Kappos, L.; et al. Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann. Neurol. 2011, 69, 292–302. [Google Scholar] [CrossRef] [PubMed]
- Kurtzke, J.F. Rating neurologic impairment in multiple sclerosis: An expanded disability status scale (EDSS). Neurology 1983, 33, 1444–1452. [Google Scholar] [CrossRef] [PubMed]
- Swardfager, W.; Herrmann, N.; Mazereeuw, G.; Goldberger, K.; Harimoto, T.; Lanctôt, K.L. Zinc in depression: A meta-analysis. Biol. Psychiatry 2013, 74, 872–878. [Google Scholar] [CrossRef] [PubMed]
- Feinstein, A.; Magalhaes, S.; Richard, J.-F.; Audet, B.; Moore, C. The link between multiple sclerosis and depression. Nature reviews. Neurology 2014, 10, 507–517. [Google Scholar] [PubMed]
- Braun, L.A.; Rosenfeldt, F. Pharmaco-nutrient interactions—A systematic review of zinc and antihypertensive therapy. Int. J. Clin. Pract. 2013, 67, 717–725. [Google Scholar] [CrossRef] [PubMed]
- Ranasinghe, P.; Pigera, S.; Galappatthy, P.; Katulanda, P.; Constantine, G.R. Zinc and diabetes mellitus: Understanding molecular mechanisms and clinical implications. DARU J. Pharm. Sci. 2015, 23, 44. [Google Scholar] [CrossRef] [PubMed]
- Foster, M.; Samman, S. Vegetarian diets across the lifecycle: Impact on zinc intake and status. Adv. Food Nutr. Res. 2015, 74, 93–131. [Google Scholar] [PubMed]
- Markowitz, M.E.; Rosen, J.F.; Mizruchi, M. Circadian variations in serum zinc (Zn) concentrations: Correlation with blood ionized calcium, serum total calcium and phosphate in humans. Am. J. Clin. Nutr. 1985, 41, 689–696. [Google Scholar] [CrossRef] [PubMed]
- Forte, G.; Visconti, A.; Santucci, S.; Ghazaryan, A.; Figà-Talamanca, L.; Cannoni, S.; Bocca, B.; Pino, A.; Violante, N.; Alimonti, A.; et al. Quantification of chemical elements in blood of patients affected by multiple sclerosis. Annali Dell'istituto Superiore Sanita 2005, 41, 213–216. [Google Scholar]
- Alimonti, A.; Ristori, G.; Giubilei, F.; Stazi, M.A.; Pino, A.; Visconti, A.; Brescianini, S.; Sepe Monti, M.; Forte, G.; Stanzione, P.; et al. Serum chemical elements and oxidative status in Alzheimer's disease, Parkinson disease and multiple sclerosis. Neurotoxicology 2007, 28, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Kapaki, E.; Segditsa, J.; Papageorgiou, C. Zinc, copper and magnesium concentration in serum and CSF of patients with neurological disorders. Acta Neurol. Scand. 1989, 79, 373–378. [Google Scholar] [CrossRef] [PubMed]
- Smith, D.K.; Feldman, E.B.; Feldman, D.S. Trace element status in multiple sclerosis. Am. J. Clin. Nutr. 1989, 50, 136–140. [Google Scholar] [CrossRef] [PubMed]
- Dore-Duffy, P.; Catalanotto, F.; Donaldson, J.O.; Ostrom, K.M.; Testa, M.A. Zinc in multiple sclerosis. Ann. Neurol. 1983, 14, 450–454. [Google Scholar] [CrossRef] [PubMed]
- Gellein, K.; Skogholt, J.H.; Aaseth, J.; Thoresen, G.B.; Lierhagen, S.; Steinnes, E.; Syversen, T.; Flaten, T.P. Trace elements in cerebrospinal fluid and blood from patients with a rare progressive central and peripheral demyelinating disease. J. Neurol. Sci. 2008, 266, 70–78. [Google Scholar] [CrossRef] [PubMed]
- Giacoppo, S.; Galuppo, M.; Calabrò, R.S.; D’Aleo, G.; Marra, A.; Sessa, E.; Bua, D.G.; Potortì, A.G.; Dugo, G.; Bramanti, P.; et al. Heavy metals and neurodegenerative diseases: An observational study. Biol. Trace Elem. Res. 2014, 161, 151–160. [Google Scholar] [CrossRef] [PubMed]
- Palm, R.; Hallmans, G. Zinc and copper in multiple sclerosis. J. Neurol. Neurosurg. Psychiatry 1982, 45, 691–698. [Google Scholar] [CrossRef] [PubMed]
- Kanesaka, T.; Mori, M.; Hattori, T.; Oki, T.; Kuwabara, S. Serum matrix metalloproteinase-3 levels correlate with disease activity in relapsing-remitting multiple sclerosis. J. Neurol. Neurosurg. Psychiatry 2006, 77, 185–188. [Google Scholar] [CrossRef] [PubMed]
- Rieder, H.P.; Schoettli, G.; Seiler, H. Trace elements in whole blood of multiple sclerosis. Eur. Neurol. 1983, 22, 85–92. [Google Scholar] [CrossRef] [PubMed]
- Prasad, A.S. Effects of zinc deficiency on Th1 and Th2 cytokine shifts. J. Infect. Dis. 2000, 182, S62–S68. [Google Scholar] [CrossRef] [PubMed]
- Kitabayashi, C.; Fukada, T.; Kanamoto, M.; Ohashi, W.; Hojyo, S.; Atsumi, T.; Ueda, N.; Azuma, I.; Hirota, H.; Murakami, M.; et al. Zinc suppresses Th17 development via inhibition of STAT3 activation. Int. Immunol. 2010, 22, 375–386. [Google Scholar] [CrossRef] [PubMed]
- Rostami, A.; Ciric, B. Role of Th17 cells in the pathogenesis of CNS inflammatory demyelination. J. Neurol. Sci. 2013, 333, 76–87. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.-F.; Zhang, S.-X.; Ma, X.-W.; Xue, Y.-L.; Gao, C.; Li, X.-Y. Levels of peripheral Th17 cells and serum Th17-related cytokines in patients with multiple sclerosis: A meta-analysis. Mult. Scler. Relat. Disord. 2017, 18, 20–25. [Google Scholar] [CrossRef] [PubMed]
- Pardo, G.; Jones, D.E. The sequence of disease-modifying therapies in relapsing multiple sclerosis: Safety and immunologic considerations. J. Neurol. 2017, 264, 2351–2374. [Google Scholar] [CrossRef] [PubMed]
- Himoto, T.; Masaki, T. Associations between Zinc Deficiency and Metabolic Abnormalities in Patients with Chronic Liver Disease. Nutrients 2018, 10, 88. [Google Scholar] [CrossRef] [PubMed]
- Fontaine, J.; Nève, J.; Peretz, A.; Capel, P.; Famaey, J.P. Effects of acute and chronic prednisolone treatment on serum zinc levels in rats with adjuvant arthritis. Agents Actions 1991, 33, 247–253. [Google Scholar] [CrossRef] [PubMed]
- Salari, S.; Khomand, P.; Arasteh, M.; Yousefzamani, B.; Hassanzadeh, K. Zinc sulphate: A reasonable choice for depression management in patients with multiple sclerosis: A randomized, double-blind, placebo-controlled clinical trial. Pharmacol. Rep. 2015, 67, 606–609. [Google Scholar] [CrossRef] [PubMed]
- Donangelo, C.M.; King, J.C. Maternal zinc intakes and homeostatic adjustments during pregnancy and lactation. Nutrients 2012, 4, 782–798. [Google Scholar] [CrossRef] [PubMed]
- Park, Y.; Park, J.; Kim, Y.; Baek, H.; Kim, S.H. Association between nutritional status and disease severity using the amyotrophic lateral sclerosis (ALS) functional rating scale in ALS patients. Nutrition 2015, 31, 1362–1367. [Google Scholar] [CrossRef] [PubMed]
- Pouraram, H.; Djazayery, A.; Mohammad, K.; Parsaeian, M.; Abdollahi, Z.; Dorosty Motlagh, A.; Djalali, M.; Khodaverdian, K.; Sotoudeh, G.; Yarparvar, A.; et al. Second National Integrated Micronutrient Survey in Iran: Study Design and Preliminary Findings. Arch. Iran. Med. 2018, 21, 137–144. [Google Scholar] [PubMed]
- Alizadeh, A.; Mehrpour, O.; Nikkhah, K.; Bayat, G.; Espandani, M.; Golzari, A.; Jarahi, L.; Foroughipour, M. Comparison of serum Concentration of Se, Pb, Mg, Cu, Zn, between MS patients and healthy controls. Electron. Physician 2016, 8, 2759–2764. [Google Scholar] [CrossRef] [PubMed]
- Sedighi, B.; Ebrahimi, H.A.; Haghdoost, A.A.; Abotorabi, M. Comparison of serum levels of copper and zinc among multiple sclerosis patients and control group. Iran. J. Neurol. 2013, 12, 125–128. [Google Scholar] [PubMed]
- Monti, M.C.; Guido, D.; Montomoli, C.; Sardu, C.; Sanna, A.; Pretti, S.; Lorefice, L.; Marrosu, M.G.; Valera, P.; Cocco, E. Is Geo-Environmental Exposure a Risk Factor for Multiple Sclerosis? A Population-Based Cross-Sectional Study in South-Western Sardinia. PLoS ONE 2016, 11, e0163313. [Google Scholar] [CrossRef] [PubMed]
- Bonaventura, P.; Lamboux, A.; Albarède, F.; Miossec, P. A Feedback Loop between Inflammation and Zn Uptake. PLoS ONE 2016, 11, e0147146. [Google Scholar] [CrossRef] [PubMed]
- Stoye, D.; Schubert, C.; Goihl, A.; Guttek, K.; Reinhold, A.; Brocke, S.; Grüngreiff, K.; Reinhold, D. Zinc aspartate suppresses T cell activation in vitro and relapsing experimental autoimmune encephalomyelitis in SJL/J mice. Biometals 2012, 25, 529–539. [Google Scholar] [CrossRef] [PubMed]
| Title | HC (n = 50) | MS (n = 151) | RMS (n = 133) | PMS (n = 18) | p-Values | |||
|---|---|---|---|---|---|---|---|---|
| HC vs. MS | HC vs. RMS | HC vs. PMS | RMS vs. PMS | |||||
| Age at zinc measure (years) | 43 [14] (19–82) | 43 [12] (18–80) | 42 [11] (18–76) | 55 [9] (40–80) | 1.0 | 0.5 | 0.001 | <0.001 |
| Female sex, n (%) | 38 (76) | 113 (75) | 95 (71) | 18 (100) | 0.9 | 0.03 | 0.03 | 0.03 |
| Disease duration (years) | - | 10 [8] (0–35) | 9 [8] (0–29) | 13 [11] (0–35) | - | - | - | 0.1 |
| Vegetarian, n (%) | 2 (4) | 8 (5) | 7 (5) | 1 (5) | 0.8 | 0.9 | 0.9 | 0.9 |
| Diabetes, n (%) | 0 (0) | 7 (5) | 6 (5) | 1 (5) | 0.1 | 0.9 | 0.9 | 0.9 |
| Hematocrit | - | 0.42 (0.03) | 0.42 (0.03) | 0.42 (0.02) | - | - | - | 0.7 |
| Median EDSS | - | 3 (0–8) | 2.5 (0–7.5) | 6.0 (2–8) | - | - | - | <0.001 |
| Median relapse, n | - | 2 (0–20) | 2 (0–20) | 1 (0–6) | - | - | - | 0.003 |
| ARR | - | 0.5 (0.5) | 0.5 (0.5) | 0.2 (0.2) | - | - | - | 0.001 |
| Treatment, n (%) | - | 131 (87) | 118 (89) | 13 (72) | - | - | - | 0.05 |
| Depression, n (%) | - | 39 (26) | 34 (26) | 5 (28) | - | - | - | 0.5 |
| Zinc level (µmol/L) | 14.6 (2.1) (9.5–19.3) | 12.5 (2.1) (8.7–24.8) | 12.4 (2.0) (8.7–24.8) | 13.0 (3.0) (8.8–20.3) | <0.001 | <0.001 | 0.03 | 0.8 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pawlitzki, M.; Uebelhör, J.; Sweeney-Reed, C.M.; Stephanik, H.; Hoffmann, J.; Lux, A.; Reinhold, D. Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls. Nutrients 2018, 10, 967. https://doi.org/10.3390/nu10080967
Pawlitzki M, Uebelhör J, Sweeney-Reed CM, Stephanik H, Hoffmann J, Lux A, Reinhold D. Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls. Nutrients. 2018; 10(8):967. https://doi.org/10.3390/nu10080967
Chicago/Turabian StylePawlitzki, Marc, Julia Uebelhör, Catherine M. Sweeney-Reed, Heike Stephanik, Juliane Hoffmann, Anke Lux, and Dirk Reinhold. 2018. "Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls" Nutrients 10, no. 8: 967. https://doi.org/10.3390/nu10080967
APA StylePawlitzki, M., Uebelhör, J., Sweeney-Reed, C. M., Stephanik, H., Hoffmann, J., Lux, A., & Reinhold, D. (2018). Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls. Nutrients, 10(8), 967. https://doi.org/10.3390/nu10080967






