Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome
Abstract
1. Introduction
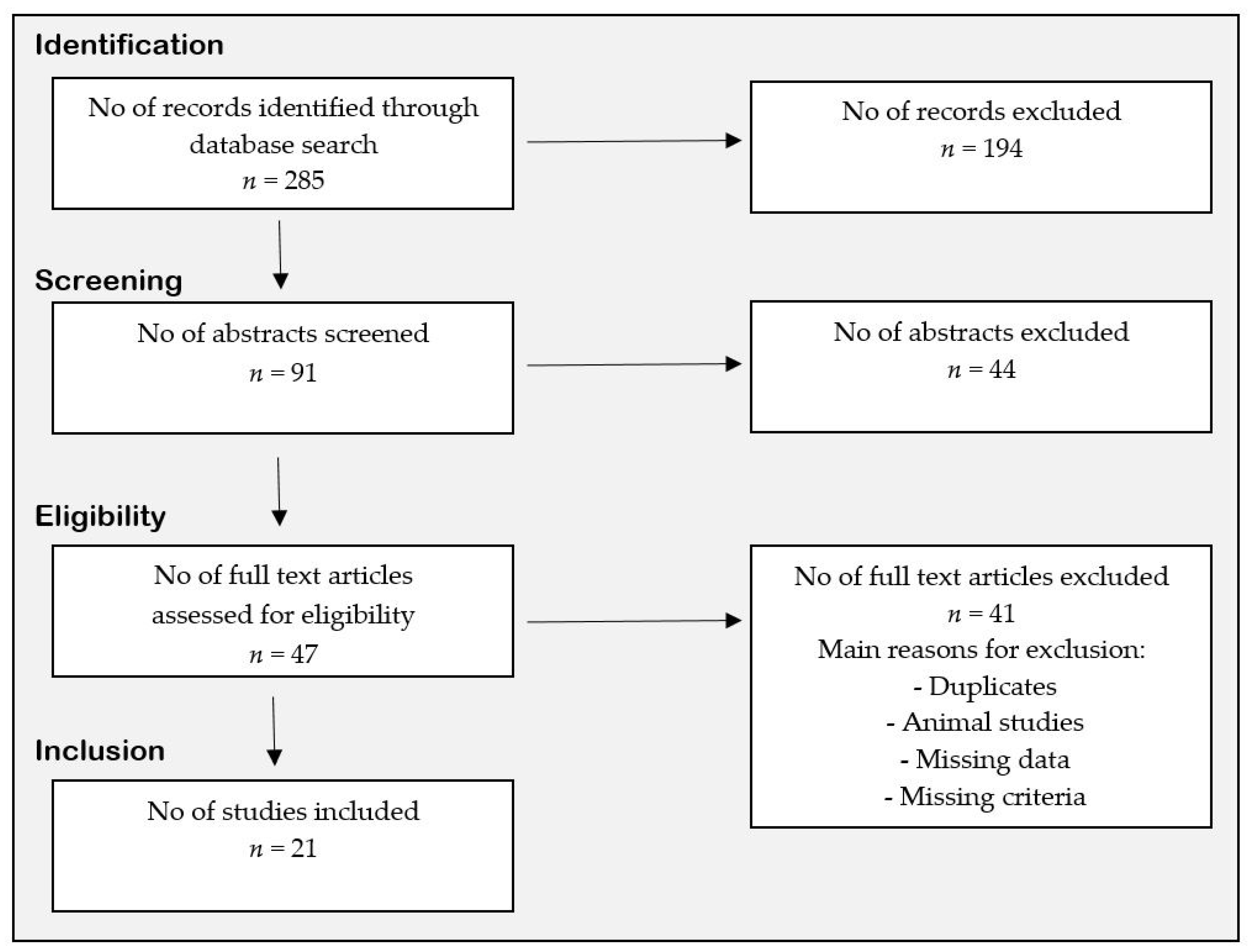
2. Method
3. Results
3.1. Fish Consumption and Metabolic Syndrome
3.2. Fish Consumption and the CVD Risk Factors of Metabolic Syndrome
4. Nutritional Contribution of Fish
4.1. Proteins and Amino Acids
4.2. n-3 Fatty Acids
4.3. Vitamin D
4.4. Iodine and Selenium
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Mendis, S.; Puska, P.; Norrving, B. Global Atlas on Cardiovascular Disease Prevention and Control; World Health Organization: Genevea, Switzerland, 2011. [Google Scholar]
- World Health Organization. Global Status Report on Noncommunicable Diseases 2014; World Health Organization: Genevea, Switzerland, 2011. [Google Scholar]
- Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z. The metabolic syndrome. Lancet 2005, 365, 1415–1428. [Google Scholar] [CrossRef]
- Alberti, K.G.; Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z.; Cleeman, J.I.; Donato, K.A.; Fruchart, J.-C.; James, W.P.T.; Loria, C.M.; Smith, S.C. Harmonizing the metabolic syndrome: A joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009, 120, 1640–1645. [Google Scholar] [PubMed]
- Cameron, A.J.; Boyko, E.J.; Sicree, R.A.; Zimmet, P.Z.; Soderberg, S.; Alberti, K.G.; Tuomilehto, J.; Chitson, P.; Shaw, J.E. Central obesity as a precursor to the metabolic syndrome in the AusDiab study and Mauritius. Obesity 2008, 16, 2707–2716. [Google Scholar] [CrossRef] [PubMed]
- Rask-Madsen, C.; Kahn, C.R. Tissue-specific insulin signaling, metabolic syndrome, and cardiovascular disease. Arterioscler. Thromb. Vasc. Biol. 2012, 32, 2052–2059. [Google Scholar] [CrossRef] [PubMed]
- Lea, T. Immunologiog Immunologiske Teknikker, 3rd ed.; Fagbokforl: Bergen, Norway, 2006. (In Norwegian) [Google Scholar]
- Piepoli, M.F.; Hoes, A.W.; Agewall, S.; Albus, C.; Brotons, C.; Catapano, A.L.; Cooney, M.-T.; Corra, U.; Cosyns, B.; Deaton, C.; et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice. Eur. Heart J. 2016, 37, 2315–2381. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Appel, L.J.; Van Horn, L. Components of a cardioprotective diet: New insights. Circulation 2011, 123, 2870–2891. [Google Scholar] [CrossRef] [PubMed]
- Skåre, J.U.; Brantsæter, A.L.; Frøyland, L.; Hemre, G.-I.; Knutsen, H.K.; Lillegaard, I.T.L.; Torstensen, B. Benefit-Risk Assessment of Fish and Fish Products in the Norwegian Diet—An Update; Norwegian Scientific Committee for Food Safety (VKM): Oslo, Norway, 2014. (In Norwegian) [Google Scholar]
- Potenza, M.V.; Mechanick, J.I. The metabolic syndrome: Definition, global impact, and pathophysiology. Nutr. Clin. Pract. 2009, 24, 560–577. [Google Scholar] [CrossRef] [PubMed]
- Lund, E.K. Health benefits of seafood; is it just the fatty acids? Food Chem. 2013, 140, 413–420. [Google Scholar] [CrossRef] [PubMed]
- Jayedi, A.; Shab-Bidar, S.; Eimeri, S.; Djafarian, K. Fish consumption and risk of all-cause and cardiovascular mortality: A dose-response meta-analysis of prospective observational studies. Public Health Nutr. 2018, 21, 1297–1306. [Google Scholar] [CrossRef] [PubMed]
- Raatz, S.K.; Silverstein, J.T.; Jahns, L.; Picklo, M.J. Issues of fish consumption for cardiovascular disease risk reduction. Nutrients 2013, 5, 1081–1097. [Google Scholar] [CrossRef] [PubMed]
- Panagiotakos, D.B.; Zeimbekis, A.; Boutziouka, V.; Economou, M.; Kourlaba, G.; Toutouzas, P.; Polychronopoulos, E. Long-term fish intake is associated with better lipid profile, arterial blood pressure, and blood glucose levels in elderly people from Mediterranean islands (MEDIS epidemiological study). Med. Sci. Monit. 2007, 13, CR307–CR312. [Google Scholar] [PubMed]
- Strom, M.; Halldorsson, T.I.; Mortensen, E.L.; Torp-Pedersen, C.; Olsen, S.F. Fish, n-3 fatty acids, and cardiovascular diseases in women of reproductive age: A prospective study in a large national cohort. Hypertension 2012, 59, 36–43. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.H.; Zhou, C.H.; Pei, H.J.; Zhou, X.L.; Li, L.H.; Wu, Y.J.; Hui, R.T. Fish consumption and incidence of heart failure: A meta-analysis of prospective cohort studies. Chin. Med. J. 2013, 126, 942–948. [Google Scholar] [PubMed]
- Chowdhury, R.; Stevens, S.; Gorman, D.; Pan, A.; Warnakula, S.; Chowdhury, S.; Ward, H.; Johnson, L.; Crowe, F.; Hu, F.B.; et al. Association between fish consumption, long chain omega 3 fatty acids, and risk of cerebrovascular disease: Systematic review and meta-analysis. BMJ 2012, 345, e6698. [Google Scholar] [CrossRef] [PubMed]
- Heine-Broring, R.C.; Brouwer, I.A.; Proenca, R.V.; van Rooij, F.J.; Hofman, A.; Oudkerk, M.; Witteman, J.C.M.; Geleijnse, J.M. Intake of fish and marine n-3 fatty acids in relation to coronary calcification: The Rotterdam Study. Am. J. Clin. Nutr. 2010, 91, 1317–1323. [Google Scholar] [CrossRef] [PubMed]
- Takata, Y.; Zhang, X.; Li, H.; Gao, Y.T.; Yang, G.; Gao, J.; Cai, H.; Xiang, Y.-B.; Zheng, W.; Shu, X.-O. Fish intake and risks of total and cause-specific mortality in 2 population-based cohort studies of 134,296 men and women. Am. J. Epidemiol. 2013, 178, 46–57. [Google Scholar] [CrossRef] [PubMed]
- Streppel, M.T.; Ocke, M.C.; Boshuizen, H.C.; Kok, F.J.; Kromhout, D. Long-term fish consumption and n-3 fatty acid intake in relation to (sudden) coronary heart disease death: The Zutphen study. Eur. Heart J. 2008, 29, 2024–2030. [Google Scholar] [CrossRef] [PubMed]
- Torris, C.; Molin, M.; Cvancarova Smastuen, M. Fish consumption and its possible preventive role on the development and prevalence of metabolic syndrome—A systematic review. Diabetol. Metab. Syndr. 2014, 6, 112. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Group, P. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. BMJ 2009, 339, b2535. [Google Scholar] [CrossRef] [PubMed]
- Ramel, A.; Jonsdottir, M.T.; Thorsdottir, I. Consumption of cod and weight loss in young overweight and obese adults on an energy reduced diet for 8-weeks. Nutr. Metab. Cardiovasc. Dis. 2009, 19, 690–696. [Google Scholar] [CrossRef] [PubMed]
- Baik, I.; Abbott, R.D.; Curb, J.D.; Shin, C. Intake of fish and n-3 fatty acids and future risk of metabolic syndrome. J. Am. Diet. Assoc. 2010, 110, 1018–1026. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.S.; Xun, P.; Iribarren, C.; Van Horn, L.; Steffen, L.; Daviglus, M.L.; Siscovick, D.; Liu, K.; He, K. Intake of fish and long-chain omega-3 polyunsaturated fatty acids and incidence of metabolic syndrome among American young adults: A 25-year follow-up study. Eur. J. Nutr. 2016, 55, 1707–1716. [Google Scholar] [CrossRef] [PubMed]
- Karlsson, T.; Rosendahl-Riise, H.; Dierkes, J.; Drevon, C.A.; Tell, G.S.; Nygard, O. Associations between fish intake and the metabolic syndrome and its components among middle-aged men and women: The Hordaland Health Study. Food Nutr. Res. 2017, 61, 1347479. [Google Scholar] [CrossRef] [PubMed]
- Kouki, R.; Schwab, U.; Hassinen, M.; Komulainen, P.; Heikkila, H.; Lakka, T.A.; Rauramaa, R. Food consumption, nutrient intake and the risk of having metabolic syndrome: The DR’s EXTRA Study. Eur. J. Clin. Nutr. 2011, 65, 368–377. [Google Scholar] [CrossRef] [PubMed]
- Ruidavets, J.B.; Bongard, V.; Dallongeville, J.; Arveiler, D.; Ducimetiere, P.; Perret, B.; Simon, C.; Amouyel, P.; Ferrières, J. High consumptions of grain, fish, dairy products and combinations of these are associated with a low prevalence of metabolic syndrome. J. Epidemiol. Community Health 2007, 61, 810–817. [Google Scholar] [CrossRef] [PubMed]
- Torris, C.; Molin, M.; Cvancarova, M.S. Lean fish consumption is associated with lower risk of metabolic syndrome: A Norwegian cross sectional study. BMC Public Health 2016, 16, 347. [Google Scholar] [CrossRef] [PubMed]
- Torris, C.; Molin, M.; Cvancarova Smastuen, M. Associations between fish consumption and metabolic syndrome. A large cross-sectional study from the Norwegian Tromso Study: Tromso 4. Diabetol. Metab. Syndr. 2016, 8, 18. [Google Scholar] [CrossRef] [PubMed]
- Zaribaf, F.; Falahi, E.; Barak, F.; Heidari, M.; Keshteli, A.H.; Yazdannik, A.; Esmaillzadeh, A. Fish consumption is inversely associated with the metabolic syndrome. Eur. J. Clin. Nutr. 2014, 68, 474–480. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.S.; Xun, P.; He, K. Fish consumption, long-chain omega-3 polyunsaturated fatty acid intake and risk of metabolic syndrome: A meta-analysis. Nutrients 2015, 7, 2085–2100. [Google Scholar] [CrossRef] [PubMed]
- Lai, Y.H.; Petrone, A.B.; Pankow, J.S.; Arnett, D.K.; North, K.E.; Ellison, R.C.; Hunt, S.C.; Djoussé, L. Association of dietary omega-3 fatty acids with prevalence of metabolic syndrome: The National Heart, Lung, and Blood Institute Family Heart Study. Clin. Nutr. 2013, 32, 966–969. [Google Scholar] [CrossRef] [PubMed]
- Pasalic, D.; Dodig, S.; Corovic, N.; Pizent, A.; Jurasovic, J.; Pavlovic, M. High prevalence of metabolic syndrome in an elderly Croatian population—A multicentre study. Public Health Nutr. 2011, 14, 1650–1657. [Google Scholar] [CrossRef] [PubMed]
- Aadland, E.K.; Lavigne, C.; Graff, I.E.; Eng, O.; Paquette, M.; Holthe, A.; Mellgren, G.; Jacques, H.; Liaset, B. Lean-seafood intake reduces cardiovascular lipid risk factors in healthy subjects: Results from a randomized controlled trial with a crossover design. Am. J. Clin. Nutr. 2015, 102, 582–592. [Google Scholar] [CrossRef] [PubMed]
- Bao, D.Q.; Mori, T.A.; Burke, V.; Puddey, I.B.; Beilin, L.J. Effects of dietary fish and weight reduction on ambulatory blood pressure in overweight hypertensives. Hypertension 1998, 32, 710–717. [Google Scholar] [CrossRef] [PubMed]
- Erkkila, A.T.; Schwab, U.S.; de Mello, V.D.; Lappalainen, T.; Mussalo, H.; Lehto, S.; Kemi, V.; Lamberg-Allardt, C.; Uusitupa, M.I.J. Effects of fatty and lean fish intake on blood pressure in subjects with coronary heart disease using multiple medications. Eur. J. Nutr. 2008, 47, 319–328. [Google Scholar] [CrossRef] [PubMed]
- Hagen, I.V.; Helland, A.; Bratlie, M.; Brokstad, K.A.; Rosenlund, G.; Sveier, H.; Mellgren, G.; Gudbrandsen, O.A. High intake of fatty fish, but not of lean fish, affects serum concentrations of TAG and HDL-cholesterol in healthy, normal-weight adults: A randomised trial. Br. J. Nutr. 2016, 116, 648–657. [Google Scholar] [CrossRef] [PubMed]
- Hallund, J.; Madsen, B.O.; Bugel, S.H.; Jacobsen, C.; Jakobsen, J.; Krarup, H.; Holm, J.; Nielsen, H.H.; Lauritzen, L. The effect of farmed trout on cardiovascular risk markers in healthy men. Br. J. Nutr. 2010, 104, 1528–1536. [Google Scholar] [CrossRef] [PubMed]
- Lara, J.J.; Economou, M.; Wallace, A.M.; Rumley, A.; Lowe, G.; Slater, C.; Caslake, M.; Sattar, N.; Lean, M.E.J. Benefits of salmon eating on traditional and novel vascular risk factors in young, non-obese healthy subjects. Atherosclerosis 2007, 193, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Lindqvist, H.M.; Langkilde, A.M.; Undeland, I.; Sandberg, A.S. Herring (Clupea harengus) intake influences lipoproteins but not inflammatory and oxidation markers in overweight men. Br. J. Nutr. 2009, 101, 383–390. [Google Scholar] [CrossRef] [PubMed]
- Lindqvist, H.; Langkilde, A.M.; Undeland, I.; Radendal, T.; Sandberg, A.S. Herring (Clupea harengus) supplemented diet influences risk factors for CVD in overweight subjects. Eur. J. Clin. Nutr. 2007, 61, 1106–1113. [Google Scholar] [CrossRef] [PubMed]
- Ramel, A.; Martinez, J.A.; Kiely, M.; Bandarra, N.M.; Thorsdottir, I. Moderate consumption of fatty fish reduces diastolic blood pressure in overweight and obese European young adults during energy restriction. Nutrition 2010, 26, 168–174. [Google Scholar] [CrossRef] [PubMed]
- Telle-Hansen, V.H.; Larsen, L.N.; Hostmark, A.T.; Molin, M.; Dahl, L.; Almendingen, K.; Ulven, S.M. Daily intake of cod or salmon for 2 weeks decreases the 18:1n-9/18:0 ratio and serum triacylglycerols in healthy subjects. Lipids 2012, 47, 151–160. [Google Scholar] [CrossRef] [PubMed]
- Thorsdottir, I.; Tomasson, H.; Gunnarsdottir, I.; Gisladottir, E.; Kiely, M.; Parra, M.D.; Bandarra, N.M.; Schaafsma, G.; Martinéz, J.A. Randomized trial of weight-loss-diets for young adults varying in fish and fish oil content. Int. J. Obes. 2007, 31, 1560–1566. [Google Scholar] [CrossRef] [PubMed]
- Vazquez, C.; Botella-Carretero, J.I.; Corella, D.; Fiol, M.; Lage, M.; Lurbe, E.; Richart, C.; Fernández-Real, J.M.; Fuentes, F.; Ordóñez, A.; et al. White fish reduces cardiovascular risk factors in patients with metabolic syndrome: The WISH-CARE study, a multicenter randomized clinical trial. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 328–335. [Google Scholar] [CrossRef] [PubMed]
- Torris, C.; Molin, M.; Smastuen, M.C. Lean Fish Consumption Is Associated with Beneficial Changes in the Metabolic Syndrome Components: A 13-Year Follow-Up Study from the Norwegian Tromso Study. Nutrients 2017, 9, 247. [Google Scholar] [CrossRef] [PubMed]
- Jakobsen, M.U.; Due, K.M.; Dethlefsen, C.; Halkjaer, J.; Holst, C.; Forouhi, N.G.; Tjønneland, A.; Boeing, H.; Buijsse, B.; Palli, D.; et al. Fish consumption does not prevent increase in waist circumference in European women and men. Br. J. Nutr. 2012, 108, 924–931. [Google Scholar] [CrossRef] [PubMed]
- Lankinen, M.; Schwab, U.; Kolehmainen, M.; Paananen, J.; Poutanen, K.; Mykkanen, H.; Seppänen-Laakso, T.; Gylling, H.; Uusitupa, M.; Orešič, M. Whole grain products, fish and bilberries alter glucose and lipid metabolism in a randomized, controlled trial: The Sysdimet study. PLoS ONE 2011, 6, e22646. [Google Scholar] [CrossRef] [PubMed]
- Uusitupa, M.; Hermansen, K.; Savolainen, M.J.; Schwab, U.; Kolehmainen, M.; Brader, L.; Mortensen, L.S.; Cloetens, L.; Johansson-Persson, A.; Önning, G. Effects of an isocaloric healthy Nordic diet on insulin sensitivity, lipid profile and inflammation markers in metabolic syndrome—A randomized study (SYSDIET). J. Intern. Med. 2013, 274, 52–66. [Google Scholar] [CrossRef] [PubMed]
- Norwegian Food Safety Authority; The Norwegian Directorate of Health; University of Oslo. Norwegian Food Composition Database 2016. Available online: www.matvaretabellen.no (accessed on 13 March 2018).
- Gormley, T.; Neumann, T.; Fagan, J.; Brunton, N. Taurine content of raw and processed fish fillets/portions. Eur. Food Res. Technol. 2007, 225, 837–842. [Google Scholar] [CrossRef]
- Dragnes, B.T.; Larsen, R.; Ernstsen, M.H.; Maehre, H.; Elvevoll, E.O. Impact of processing on the taurine content in processed seafood and their corresponding unprocessed raw materials. Int. J. Food Sci. Nutr. 2009, 60, 143–152. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services; U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for Americans, 8th ed.; 2015. Available online: https://health.gov/dietaryguidelines/2015/guidelines/ (accessed on 13 March 2018).
- Brownie, S.; Muggleston, H.; Oliver, C. The 2013 Australian dietary guidelines and recommendations for older Australians. Aust. Fam. Phys. 2015, 44, 311–315. [Google Scholar]
- Wang, S.; Lay, S.; Yu, H.; Shen, S. Dietary Guidelines for Chinese Residents (2016): Comments and comparisons. Biomed. Biotechnol. 2016, 17, 649–656. [Google Scholar] [CrossRef] [PubMed]
- The Norwegian Directorate of Health. Anbefalinger om Kosthold, Ernæring og Fysisk Aktivitet; Helsedirektoratet: Oslo, Norway, 2014. (In Norwegian) [Google Scholar]
- European Food Safety Authority (EFSA). Dietary Reference Values for Nutrients. Summary Report. 2017. Available online: https://www.efsa.europa.eu/sites/default/files/2017_09_DRVs_summary_report.pdf (accessed on 13 March 2018).
- Uhe, A.M.; Collier, G.R.; O’Dea, K. A comparison of the effects of beef, chicken and fish protein on satiety and amino acid profiles in lean male subjects. J. Nutr. 1992, 122, 467–472. [Google Scholar] [CrossRef] [PubMed]
- Borzoei, S.; Neovius, M.; Barkeling, B.; Teixeira-Pinto, A.; Rossner, S. A comparison of effects of fish and beef protein on satiety in normal weight men. Eur. J. Clin. Nutr. 2006, 60, 897–902. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Ellis, V. The acute effects of four protein meals on insulin, glucose, appetite and energy intake in lean men. Br. J. Nutr. 2010, 104, 1241–1248. [Google Scholar] [CrossRef] [PubMed]
- Kritchevsky, D.; Tepper, S.A.; Czarnecki, S.K.; Klurfeld, D.M. Atherogenicity of animal and vegetable protein: Influence of the lysine to arginine ratio. Atherosclerosis 1982, 41, 429–431. [Google Scholar] [CrossRef]
- Hosomi, R.; Fukunaga, K.; Arai, H.; Kanda, S.; Nishiyama, T.; Yoshida, M. Fish protein hydrolysates affect cholesterol metabolism in rats fed non-cholesterol and high-cholesterol diets. J. Med. Food 2012, 15, 299–306. [Google Scholar] [CrossRef] [PubMed]
- Wergedahl, H.; Liaset, B.; Gudbrandsen, O.; Lied, E. Fish Protein Hydrolysate Reduces Plasma Total Cholesterol, Increases the Proportion of HDL Cholesterol, and Lowers Acyl-CoA: Cholesterol Acyltransferase Activity in Liver of Zucker Rats1. J. Nutr. 2004, 134, 1320–1327. [Google Scholar] [CrossRef] [PubMed]
- Drotningsvik, A.; Mjos, S.A.; Pampanin, D.M.; Slizyte, R.; Carvajal, A.; Remman, T.; Høgøy, I.; Gudbrandsen, O.A. Dietary fish protein hydrolysates containing bioactive motifs affect serum and adipose tissue fatty acid compositions, serum lipids, postprandial glucose regulation and growth in obese Zucker fa/fa rats. Br. J. Nutr. 2016, 116, 1336–1345. [Google Scholar] [CrossRef] [PubMed]
- El Khoury, D.; Anderson, G.H. Recent advances in dietary proteins and lipid metabolism. Curr. Opin. Lipidol. 2013, 24, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Ouellet, V.; Marois, J.; Weisnagel, S.J.; Jacques, H. Dietary cod protein improves insulin sensitivity in insulin-resistant men and women: A randomized controlled trial. Diabetes Care 2007, 30, 2816–2821. [Google Scholar] [CrossRef] [PubMed]
- Yamori, Y.; Taguchi, T.; Hamada, A.; Kunimasa, K.; Mori, H.; Mori, M. Taurine in health and diseases: Consistent evidence from experimental and epidemiological studies. J. Biomed. Sci. 2010, 17 (Suppl. 1), S6. [Google Scholar] [CrossRef] [PubMed]
- Imae, M.; Asano, T.; Murakami, S. Potential role of taurine in the prevention of diabetes and metabolic syndrome. Amino Acids 2014, 46, 81–88. [Google Scholar] [CrossRef] [PubMed]
- Murakami, S. Taurine and atherosclerosis. Amino Acids 2014, 46, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Yamori, Y.; Taguchi, T.; Mori, H.; Mori, M. Low cardiovascular risks in the middle aged males and females excreting greater 24-hour urinary taurine and magnesium in 41 WHO-CARDIAC study populations in the world. J. Biomed. Sci. 2010, 17 (Suppl. 1), S21. [Google Scholar] [CrossRef] [PubMed]
- Zhang, M.; Bi, L.F.; Fang, J.H.; Su, X.L.; Da, G.L.; Kuwamori, T.; Kuwamori, T.; Kagamimori, S. Beneficial effects of taurine on serum lipids in overweight or obese non-diabetic subjects. Amino Acids 2004, 26, 267–271. [Google Scholar] [CrossRef] [PubMed]
- Elvevoll, E.O.; Eilertsen, K.E.; Brox, J.; Dragnes, B.T.; Falkenberg, P.; Olsen, J.O.; Kirkhus, B.; Lamglait, A.; Østerud, B. Seafood diets: Hypolipidemic and antiatherogenic effects of taurine and n-3 fatty acids. Atherosclerosis 2008, 200, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Murakami, S. The physiological and pathophysiological roles of taurine in adipose tissue in relation to obesity. Life Sci. 2017, 186, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Rosa, F.; Freitas, E.; Deminice, R.; Jordão, A.; Marchini, J. Oxidative stress and inflammation in obesity after taurine supplementation: A double-blind, placebo-controlled study. Eur. J. Nutr. 2014, 53, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Sun, Q.; Wang, B.; Li, Y.; Sun, F.; Li, P.; Xia, W.; Zhou, X.; Li, Q.; Wang, X.; Chen, J.; et al. Taurine Supplementation Lowers Blood Pressure and Improves Vascular Function in Prehypertension: Randomized, Double-Blind, Placebo-Controlled Study. Hypertension 2016, 67, 541–549. [Google Scholar] [CrossRef] [PubMed]
- Maia, A.R.; Batista, T.M.; Victorio, J.A.; Clerici, S.P.; Delbin, M.A.; Carneiro, E.M.; Davel, A.P. Taurine supplementation reduces blood pressure and prevents endothelial dysfunction and oxidative stress in post-weaning protein-restricted rats. PLoS ONE 2014, 9, e105851. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.J.; Arneja, A.S.; Tappia, P.S.; Dhalla, N.S. The potential health benefits of taurine in cardiovascular disease. Exp. Clin. Cardiol. 2008, 13, 57–65. [Google Scholar] [PubMed]
- Ito, T.; Yoshikawa, N.; Ito, H.; Schaffer, S.W. Impact of taurine depletion on glucose control and insulin secretion in mice. J. Pharmacol. Sci. 2015, 129, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Kris-Etherton, P.M.; Fleming, J.A. Emerging nutrition science on fatty acids and cardiovascular disease: Nutritionists’ perspectives. Adv. Nutr. 2015, 6, 326S–337S. [Google Scholar] [CrossRef] [PubMed]
- Wiktorowska-Owczarek, A.; Berezinska, M.; Nowak, J.Z. PUFAs: Structures, Metabolism and Functions. Adv. Clin. Exp. Med. 2015, 24, 931–941. [Google Scholar] [CrossRef] [PubMed]
- Back, M. Omega-3 fatty acids in atherosclerosis and coronary artery disease. Future Sci. OA 2017, 3, FSO236. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Fernandez, L.; Laiglesia, L.M.; Huerta, A.E.; Martinez, J.A.; Moreno-Aliaga, M.J. Omega-3 fatty acids and adipose tissue function in obesity and metabolic syndrome. Prostaglandins Other Lipid Mediat. 2015, 121 Pt A, 24–41. [Google Scholar] [CrossRef] [PubMed]
- Bang, H.O. Lipid Research in Greenland. Preventive and Therapeutic Consequences. Scand. J. Public Health 1990, 18, 53–57. [Google Scholar] [CrossRef]
- Mori, T.A. Marine OMEGA-3 fatty acids in the prevention of cardiovascular disease. Fitoterapia 2017, 123, 51–58. [Google Scholar] [CrossRef] [PubMed]
- Dunn, S.L.; Siu, W.; Freund, J.; Boutcher, S.H. The effect of a lifestyle intervention on metabolic health in young women. Diabetes Metab. Syndr. Obes. Targets Ther. 2014, 7, 437–444. [Google Scholar] [CrossRef] [PubMed]
- Lee, T.C.; Ivester, P.; Hester, A.G.; Sergeant, S.; Case, L.D.; Morgan, T.; Kouba, E.O.; Chilton, F.H. The impact of polyunsaturated fatty acid-based dietary supplements on disease biomarkers in a metabolic syndrome/diabetes population. Lipids Health Dis. 2014, 13, 196. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, M.H.; Molgaard, C.; Hellgren, L.I.; Lauritzen, L. Effects of fish oil supplementation on markers of the metabolic syndrome. J. Pediatr. 2010, 157, 395–400. [Google Scholar] [CrossRef] [PubMed]
- Aung, T.; Halsey, J.; Kromhout, D.; Gerstein, H.C.; Marchioli, R.; Tavazzi, L.; Geleijnse, J.M.; Rauch, B.; Ness, A.; Galan, P.; et al. Associations of Omega-3 Fatty Acid Supplement Use With Cardiovascular Disease Risks: Meta-analysis of 10 Trials Involving 77 917 Individuals. JAMA Cardiol. 2018, 3, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Tortosa-Caparros, E.; Navas-Carrillo, D.; Marin, F.; Orenes-Pinero, E. Anti-inflammatory effects of omega 3 and omega 6 polyunsaturated fatty acids in cardiovascular disease and metabolic syndrome. Crit. Rev. Food Sci. Nutr. 2017, 57, 3421–3429. [Google Scholar] [CrossRef] [PubMed]
- Mullen, A.; Loscher, C.E.; Roche, H.M. Anti-inflammatory effects of EPA and DHA are dependent upon time and dose-response elements associated with LPS stimulation in THP-1-derived macrophages. J. Nutr. Biochem. 2010, 21, 444–450. [Google Scholar] [CrossRef] [PubMed]
- Romacho, T.; Glosse, P.; Richter, I.; Elsen, M.; Schoemaker, M.H.; van Tol, E.A.; Eckel, J. Nutritional ingredients modulate adipokine secretion and inflammation in human primary adipocytes. Nutrients 2015, 7, 865–886. [Google Scholar] [CrossRef] [PubMed]
- Saravanan, P.; Davidson, N.C.; Schmidt, E.B.; Calder, P.C. Cardiovascular effects of marine omega-3 fatty acids. Lancet 2010, 376, 540–550. [Google Scholar] [CrossRef]
- Visioli, F.; Rise, P.; Barassi, M.C.; Marangoni, F.; Galli, C. Dietary intake of fish vs. formulations leads to higher plasma concentrations of n-3 fatty acids. Lipids 2003, 38, 415–418. [Google Scholar] [CrossRef] [PubMed]
- Ebbesson, S.O.; Tejero, M.E.; Nobmann, E.D.; Lopez-Alvarenga, J.C.; Ebbesson, L.; Romenesko, T.; Carter, E.A.; Resnick, H.E.; Devereux, R.B.; MacCluer, J.W.; et al. Fatty acid consumption and metabolic syndrome components: The GOCADAN study. J. Cardiometab. Syndr. 2007, 2, 244–249. [Google Scholar] [CrossRef] [PubMed]
- Hoe, E.; Nathanielsz, J.; Toh, Z.Q.; Spry, L.; Marimla, R.; Balloch, A.; Mulholland, K.; Licciardi, P.V. Anti-Inflammatory Effects of Vitamin D on Human Immune Cells in the Context of Bacterial Infection. Nutrients 2016, 8, 806. [Google Scholar] [CrossRef] [PubMed]
- Lehmann, U.; Gjessing, H.R.; Hirche, F.; Mueller-Belecke, A.; Gudbrandsen, O.A.; Ueland, P.M.; Mellgren, G.; Lauritzen, L.; Lindqvist, H.; Hansen, A.L.; et al. Efficacy of fish intake on vitamin D status: A meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 2015, 102, 837–847. [Google Scholar] [CrossRef] [PubMed]
- De Roos, B.; Sneddon, A.A.; Sprague, M.; Horgan, G.W.; Brouwer, I.A. The potential impact of compositional changes in farmed fish on its health-giving properties: Is it time to reconsider current dietary recommendations? Public Health Nutr. 2017, 20, 2042–2049. [Google Scholar] [CrossRef] [PubMed]
- Cashman, K.D. Vitamin D: Dietary requirements and food fortification as a means of helping achieve adequate vitamin D status. J. Steroid Biochem. Mol. Biol. 2015, 148, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Cashman, K.D.; Dowling, K.G.; Skrabakova, Z.; Gonzalez-Gross, M.; Valtuena, J.; De Henauw, S.; Moreno, L.; Damsgaard, C.T.; Michaelsen, K.F.; Mølgaard, C.; et al. Vitamin D deficiency in Europe: Pandemic? Am. J. Clin. Nutr. 2016, 103, 1033–1044. [Google Scholar] [CrossRef] [PubMed]
- Conzade, R.; Koenig, W.; Heier, M.; Schneider, A.; Grill, E.; Peters, A.; Thorand, B. Prevalence and Predictors of Subclinical Micronutrient Deficiency in German Older Adults: Results from the Population-Based KORA-Age Study. Nutrients 2017, 9, 1276. [Google Scholar] [CrossRef] [PubMed]
- Forrest, K.Y.; Stuhldreher, W.L. Prevalence and correlates of vitamin D deficiency in US adults. Nutr. Res. 2011, 31, 48–54. [Google Scholar] [CrossRef] [PubMed]
- Schmitt, E.B.; Nahas-Neto, J.; Bueloni-Dias, F.; Poloni, P.F.; Orsatti, C.L.; Petri Nahas, E.A. Vitamin D deficiency is associated with metabolic syndrome in postmenopausal women. Maturitas 2018, 107, 97–102. [Google Scholar] [CrossRef] [PubMed]
- Pan, G.T.; Guo, J.F.; Mei, S.L.; Zhang, M.X.; Hu, Z.Y.; Zhong, C.K.; Zeng, C.Y.; Liu, X.H.; Ma, Q.H.; Li, B.Y.; et al. Vitamin D Deficiency in Relation to the Risk of Metabolic Syndrome in Middle-Aged and Elderly Patients with Type 2 Diabetes Mellitus. J. Nutr. Sci. Vitaminol. 2016, 62, 213–219. [Google Scholar] [CrossRef] [PubMed]
- Elizondo-Montemayor, L.; Castillo, E.C.; Rodriguez-Lopez, C.; Villarreal-Calderon, J.R.; Gomez-Carmona, M.; Tenorio-Martinez, S.; Nieblas, B.; García-Rivas, G. Seasonal Variation in Vitamin D in Association with Age, Inflammatory Cytokines, Anthropometric Parameters, and Lifestyle Factors in Older Adults. Mediat. Inflamm. 2017, 2017, 5719461. [Google Scholar] [CrossRef] [PubMed]
- Ganji, V.; Zhang, X.; Shaikh, N.; Tangpricha, V. Serum 25-hydroxyvitamin D concentrations are associated with prevalence of metabolic syndrome and various cardiometabolic risk factors in US children and adolescents based on assay-adjusted serum 25-hydroxyvitamin D data from NHANES 2001–2006. Am. J. Clin. Nutr. 2011, 94, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Giovinazzo, S.; Alibrandi, A.; Campenni, A.; Trimarchi, F.; Ruggeri, R.M. Correlation of cardio-metabolic parameters with vitamin D status in healthy premenopausal women. J. Endocrinol. Investig. 2017, 40, 1337–1343. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.Y.; Kim, M.K.; Jung, S.; Shin, J.; Choi, B.Y. The cross-sectional relationships of dietary and serum vitamin D with cardiometabolic risk factors: Metabolic components, subclinical atherosclerosis, and arterial stiffness. Nutrition 2016, 32, 1048–1056.e1. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.S.; Hwang, J.H.; Song, M.R. The Association Between Vitamin D Deficiency and Metabolic Syndrome in Korean Adolescents. J. Pediatr. Nurs. 2018, 38, e7–e11. [Google Scholar] [CrossRef] [PubMed]
- Schomburg, L.; Köhrle, J.; Diamond, A.M. On the importance of selenium and iodine metabolism for thyroid hormone biosynthesis and human health. Mol. Nutr. Food Res. 2008, 52, 1235–1246. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization; Food and Agriculture Organization of the United Nations. Vitamin & Mineral Requirements in Human Nutrition; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Reinehr, T. Obesity and thyroid function. Mol. Cell. Endocrinol. 2010, 316, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Brough, L.; Gunn, C.; Weber, J.; Coad, J.; Jin, Y.; Thomson, J.; Mauze, M.; Kruger, M.C. Iodine and Selenium Intakes of Postmenopausal Women in New Zealand. Nutrients 2017, 9, 254. [Google Scholar] [CrossRef] [PubMed]
- Nystrom, H.F.; Brantsaeter, A.L.; Erlund, I.; Gunnarsdottir, I.; Hulthen, L.; Laurberg, P.; Mattisson, I.; Rasmussen, L.B.; Virtanen, S.; Meltzer, H.M. Iodine status in the Nordic countries—Past and present. Food Nutr Res. 2016, 60, 31969. [Google Scholar] [CrossRef] [PubMed]
- Henjum, S.; Lilleengen, A.M.; Aakre, I.; Dudareva, A.; Gjengedal, E.L.F.; Meltzer, H.M.; Brantsæter, A.L. Suboptimal Iodine Concentration in Breastmilk and Inadequate Iodine Intake among Lactating Women in Norway. Nutrients 2017, 9, 643. [Google Scholar] [CrossRef] [PubMed]
- Kirkegaard-Klitbo, D.M.; Perslev, K.; Andersen, S.L.; Perrild, H.; Knudsen, N.; Weber, T.; Rasmussen, L.B.; Laurberg, P. Iodine deficiency in pregnancy is prevalent in vulnerable groups in Denmark. Dan. Med. J. 2016, 63, A5286. [Google Scholar] [PubMed]
- Tam, W.H.; Chan, R.S.; Chan, M.H.; Yuen, L.Y.; Li, L.; Sea, M.M.; Woo, J. Moderate iodine deficiency among pregnant women in Hong Kong: Revisit the problem after two decades. Hong Kong Med. J. 2017, 23, 6. [Google Scholar] [CrossRef] [PubMed]
- Gunnarsdottir, I.; Gustavsdottir, A.G.; Steingrimsdottir, L.; Maage, A.; Johannesson, A.J.; Thorsdottir, I. Iodine status of pregnant women in a population changing from high to lower fish and milk consumption. Public Health Nutr. 2013, 16, 325–329. [Google Scholar] [CrossRef] [PubMed]
- Ayturk, S.; Gursoy, A.; Kut, A.; Anil, C.; Nar, A.; Tutuncu, N.B. Metabolic syndrome and its components are associated with increased thyroid volume and nodule prevalence in a mild-to-moderate iodine-deficient area. Eur. J. Endocrinol. 2009, 161, 599–605. [Google Scholar] [CrossRef] [PubMed]
- Lecube, A.; Zafon, C.; Gromaz, A.; Fort, J.; Caubet, E.; Baena, J.; Tortosa, F. Iodine Deficiency Is Higher in Morbid Obesity in Comparison with Late After Bariatric Surgery and Non-obese Women. Obes. Surg. 2015, 25, 85–89. [Google Scholar] [CrossRef] [PubMed]
- Stoffaneller, R.; Morse, N.L. A review of dietary selenium intake and selenium status in Europe and the Middle East. Nutrients 2015, 7, 1494–1537. [Google Scholar] [CrossRef] [PubMed]
- Alfthan, G.; Eurola, M.; Ekholm, P.; Venalainen, E.R.; Root, T.; Korkalainen, K.; Hartikainen, H.; Salminen, P.; Hietaniemi, V.; Aspila, P.; et al. Effects of nationwide addition of selenium to fertilizers on foods, and animal and human health in Finland: From deficiency to optimal selenium status of the population. J. Trace Elements Med. Biol. 2015, 31, 142–147. [Google Scholar] [CrossRef] [PubMed]
- Olza, J.; Aranceta-Bartrina, J.; Gonzalez-Gross, M.; Ortega, R.M.; Serra-Majem, L.; Varela-Moreiras, G.; Gil, Á. Reported Dietary Intake and Food Sources of Zinc, Selenium, and Vitamins A, E and C in the Spanish Population: Findings from the ANIBES Study. Nutrients 2017, 9, 607. [Google Scholar] [CrossRef] [PubMed]
- Nawrot, T.S.; Staessen, J.A.; Roels, H.A.; Den Hond, E.; Thijs, L.; Fagard, R.H.; Struijker-Boudier, H.A. Blood pressure and blood selenium: A cross-sectional and longitudinal population study. Eur. Heart J. 2007, 28, 628–633. [Google Scholar] [CrossRef] [PubMed]
- Park, K.; Seo, E. Association between Toenail Mercury and Metabolic Syndrome Is Modified by Selenium. Nutrients 2016, 8, 424. [Google Scholar] [CrossRef] [PubMed]
| Measure | Cut Points |
|---|---|
| Waist circumference * | Men: ≥94 cm |
| Women: ≥80 cm | |
| serum-HDL cholesterol | Men: <1.0 mmol/L (40 mg/dL) |
| Women: <1.3 mmol/L (50 mg/dL) | |
| serum-triglyceride | >1.7 mmol/L (150 mg/dL) |
| Systolic blood pressure | ≥130 mm Hg |
| Diastolic blood pressure | ≥85 mm Hg |
| Fasting serum-glucose | ≥5.6 mmol/L (100 mg/dL) |
| Reference | Design | Results |
|---|---|---|
| Ramel et al., 2009 [24] | RCT | No association (8-week intervention, energy restricted * (−30%): 150 g cod 3 times/week, 5 times/week, or no seafood as control) |
| Baik et al., 2010 [25] | 3-years follow-up | Men: Reduced risk of MetS with average daily fish consumption (40–70 g), when compared with less than once a week, OR 0.43 (95% CI 0.23 to 0.83). Women: No associations |
| Kim et al., 2016 [26] | 25-years follow-up | Men and women: Non-fried fish consumption inversely associated with incidence of MetS, age adjusted HR 0.51 (95% CI 0.40 to 0.64) from the highest quintile (≥5 week) |
| Karlsson et al., 2017 [27] | Cross-sectional | Men and women: Total fish intake was inversely associated with MetS, adjusted OR 0.75 (95% CI 0.57 to 0.97). |
| Kouki et al., 2011 [28] | Cross-sectional | Men: Fish consumption (10 g/day) associated with reduced risk of having MetS, OR 0.97 (95% CI 0.94 to 1.00) Women: No associations |
| Lai et al., 2013 [34] | Cross-sectional | No association |
| Pasalic et al 2011 [35] | Cross-sectional | No association |
| Ruidavets et al., 2007 [29] | Cross-sectional | Men: Inverse association between fish consumption and prevalence of MetS, when comparing highest tertile to lowest, OR 0.57 (95% CI 0.38 to 0.86). |
| Tørris et al., 2016 [31] | Cross-sectional | Men and women: Fish consumption was associated with lower risk of MetS in the age group 60–70 years (OR 0.64, 95% CI 0.45 to 0.91), compared to the younger age groups. However, only lean fish consumption was associated with a reduced risk of having MetS, no association for fatty fish consumption. |
| Tørris et al, 2016 [30] | Cross-sectional | Men and women: Fish consumption once a week or more was associated with lower risk of MetS, OR 0.83 (95% CI 0.74 to 0.93), compared to fish consumption less than once a week. Only lean fish was associated with lower risk of having metabolic syndrome, no association for fatty fish consumption. |
| Zaribaf et al., 2014 [32] | Cross-sectional | Women in the highest tertile of fish consumption were less likely to have MetS, compared to those in the lowest tertile, OR 0.35 (95% CI 0.14 to 0.88). |
| Reference/Country | Participants | Intervention | Results |
|---|---|---|---|
| Aadland et al., 2015 [36] Norway | 20 healthy adults (7 men, 13 women) | 4-week, crossover: 1: 60% of proteins lean-seafood 2: No seafood (lean meat and 3.3 g cod liver oil) | Lean fish reduced TG Change −0.17 ± 0.06 mmol/L HDL no association |
| Bao et al., 1998 [37] Australia | 69 overweight nonsmoking men and postmenopausal women, using hypertensive | 16-week, parallel: 1: Fatty fish (3.65 g n-3 FA) & energy restricted (−2MJ/d) 2: Energy restricted (−2MJ/d) 3: Fatty fish (3.65 g n-3 FA) 4: Control | Fatty fish reduced BP SBP −6.0 ± 1.4 mm Hg DBP −3.0 ± 1.4 mm Hg |
| Erkkila et al., 2008 [38] Finland | 33 adults (27 men, 6 women) with coronary heart disease | 8-week, parallel: 1: Fatty fish (4 meals/week) 2: Lean fish (4 meals/week) 3: Control (lean meat) | Lean fish reduced BP SBP −3.5 ± 3.2 mmHg DBP −4.6 ± F 3.6 mmHg |
| Hagen et al. 2016 [39] Norway | 38 healthy adults | 4-week, parallel 1: Lean fish (750 g/w) 2: Fatty fish 3: Control (lean meat) | High intake of fatty fish, but not lean fish reduced TG and increased HDL |
| Hallund et al., 2010 [40] Denmark | 68 healthy men | 8-week, parallel: 1: Trout (marine diet) 2: Trout (vegetable diet) 3: Control (chicken) | No association (BP, TG, HDL, glucose) |
| Lara et al., 2007 [41] UK | 48 healthy adults (16 men) | 4 week: Salmon (4-weeks) followed by no-fish (4-weeks) | Fatty fish reduced TG −0.13 (−0.24 to −0.1) Fatty fish increased HDL 0.09 (0.01 to 0.15) Fatty fish decreased BP SBP −4.6 (−7.1 to −2.0) mmHg DBP −2.9 (−5.0, −0.9) mmHg |
| Lindquist et al., 2009 [42] Sweden | 35 overweight men | 6-week, cross-over 1: Herring 5 day/week 2: Chicken and pork | Fatty fish decreased TG −0.35 mmol/l Fatty fish increased HDL +0.05 mmol/l BP no association |
| Lindquist et al., 2007 [43] Sweden | 15 healthy obese adults | 4-week, cross-over 1: Herring 5 day/week 2: Chicken and pork | Fatty fish increased HDL +0.09 mmol/l TG no association |
| Ramel et al., 2010 [44] Iceland, Spain, Ireland | 324 overweight/obese healthy adults | 8-week, parallel Energy restricted * (−30%): 1: Lean fish (cod) 3 times/week 2: Fatty fish (salmon) 3 × 150 g/week3: Fish oil (DHA/EPA) 4: Control (No seafood) | Fatty fish decreased DBP compared with lean fish, no association with control group |
| Ramel et al., 2009 [24] Iceland | 126 overweight/obese healthy adults | 8-week, parallel Energy restricted * (−30%): 1: 150 g cod 3 times/week 2: 150 g cod 5 times/week 3: Control (no seafood) | Lean fish reduced WC Lean fish 5 t/week −3.4 Lean fish increased BP SBP: Lean fish 5 t/week +5 mmHg DBP: Lean fish 3 t/week +3 mmHg TG no association HDL no association |
| Telle-Hansen et al., 2012 [45] Norway | 30 healthy adults (7 men and 23 women) | 15 days, parallel 1: 150 g cod daily 2: 150 g salmon daily 3: Control (150 g potato daily) | Lean fish decreased TG −0.1 (p < 0.05) HDL no association Fatty fish decreased TG −0.2 (p < 0.05) Fatty fish increased HDL +0.1 (p < 0.05) |
| Thorsdottir et al., 2007 [46] Iceland, Spain, Ireland | 324 overweight/obese healthy adults (138 men and 186 women) | 8-week, parallel: Energy restricted * (−30%): 1: Lean fish (cod) 3 × 150 g/week 2: Fatty fish (salmon) 3 × 150 g/week3: Fish oil (DHA/EPA) 4: Control (no seafood) | Lean fish reduced WC Fatty fish reduced WC Lean fish −5.0 (2.9) (p < 0.05) Fatty fish −5.4 (3.3) (p < 0.05) Fish oil −5.1 (3.1) Control 4.0 (2.4) |
| Vazquez et al., 2014 [47] Spain | 273 patients with metabolic syndrome | 8-week, cross-over: 100 g/day lean fish (Namibia hake) Control: No fish/seafood | Lean fish reduced WC WC: treatment effect p < 0.001 Lean fish reduced DBP DBP: treatment effect p = 0.014 HDL no association TG no association |
| Reference/Country | Participants/Follow-Up Time | Results | |
|---|---|---|---|
| Tørris et al., 2017 [48] Norway | 23,907 adults from the Norwegian Tromsø Study, Tromsø 4 and 6, 13 years | Investigating fish consumption (≥1 ×/week compared to <1 ×/week) and change in MetS components by consumption of fish during the follow-up period, age adjusted | Lean fish decreased WC Men −1.15 (−1.96 to −0.35) Fatty fish increased WC Women 0.97 (0.29 to 1.65) Men 0.60 (0.01 to 1.18) Lean fish reduced TG Women −0.04 (−0.08 to −0.00) Men −0.11 (−0.17 to −0.06) Lean fish increased HDL Women 0.03 (0.01 to 0.05) Men 0.04 (0.02 to 0.05) Fatty fish increased HDL Men 0.02 (0.00 to 0.03) Lean fish decreased BP SBP Men −0.86 (−1.66 to −0.06) DBP Men −0.63 (−1.18 to −0.07) |
| Jakobsen et al., 2012 [49] Europe | 89,432 adults from the European Prospective Investigation into Cancer and Nutrition (EPIC) study 5.5 years Investigating fish consumption and 1-year change in WC | 1-year change in WC | Fatty fish decreased WC Annual WC change 0.01 cm/10 g higher fatty fish consumption per d (95% CI 0.02 to 0.01) Lean fish no association with WC |
| Food Item, Raw | Energy | Fat | n-3 | Taurine | Vitamin D | Selenium | Iodine |
|---|---|---|---|---|---|---|---|
| kJ | g | g | mg | µg | µg | µg | |
| Haddock (Melanogrammus aeglefinus) | 290 | 0.2 | 0.05 | 28 b/57 c | 0.5 | 30 | 320 |
| Pollock (Pollachius pollachius) | 279 | 0.2 | 0.05 | - | 2.2 | 30 | 143 |
| Saithe (Pollachius virens) | 292 | 0.3 | 0.1 | 162 c | 0.8 | 30 | 93 |
| Cod (Gadus morhua) | 343 | 1.1 | 0.26 | 108 a/120 c | 2 | 22 | 119 |
| Cod farmed (Gadus morhua) | 358 | 0.5 | 0.16 | - | 0.7 | 30 | 300 |
| Plaice (Pleuronectes platessa) | 382 | 2.6 | 0.66 | 146 a | 6 | 30 | 14 |
| Trout (Salmo trutta) | 462 | 3.3 | 0.62 | - | 9 | 19 | 19 |
| Mackerel May–June (Scomber scombrus) | 516 | 5.4 | 1.38 | - | 6 | 30 | 50 |
| Trout farmed (Salmo trutta) | 693 | 10 | 2.47 | - | 6.9 | 30 | 5 |
| Salmon wild (Salmo salar) | 760 | 12 | 2.12 | - | 8 | 50 | - |
| Salmon farmed (Salmo salar) | 932 | 16 | 3.63 | 60 a/94 c | 10 | 30 | 12 |
| Mackerel, autumn (Scomber scombrus) | 1214 | 25 | 6.35 | 78 a | 5.4 | 60 | 63 |
| Organization/Diet | Dietary Fish Recommendation |
|---|---|
| Dietary Guidelines for Americans (2015–2020) [55] | Consumption of about 8 ounces (2–3 portions)/week of a variety of seafood (fish and shellfish), which provide an average consumption of 250 mg/day of EPA and DHA |
| Australian Dietary Guidelines 2013 [56] | At least two servings of fish/week |
| Dietary Guidelines for Chinese Residents (2016) [57] | The appropriate weekly intake is set at 280–525 g of fish |
| European Guidelines on cardiovascular disease prevention in clinical practice 2016 [8] | Fish 1–2 times/week, one of which to be fatty fish |
| Norwegian dietary recommendations (2014) [58] | At least 2–3 portions or 300–450 grams of fish weekly, including a minimum of 200 grams of fatty fish |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tørris, C.; Småstuen, M.C.; Molin, M. Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome. Nutrients 2018, 10, 952. https://doi.org/10.3390/nu10070952
Tørris C, Småstuen MC, Molin M. Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome. Nutrients. 2018; 10(7):952. https://doi.org/10.3390/nu10070952
Chicago/Turabian StyleTørris, Christine, Milada Cvancarova Småstuen, and Marianne Molin. 2018. "Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome" Nutrients 10, no. 7: 952. https://doi.org/10.3390/nu10070952
APA StyleTørris, C., Småstuen, M. C., & Molin, M. (2018). Nutrients in Fish and Possible Associations with Cardiovascular Disease Risk Factors in Metabolic Syndrome. Nutrients, 10(7), 952. https://doi.org/10.3390/nu10070952




