Testing the Feasibility and Preliminary Efficacy of an 8-Week Exercise and Compensatory Eating Intervention
Abstract
1. Introduction
2. Materials and Methods
2.1. Participant Recruitment
2.2. Study Design
2.3. Exercise Intervention
2.4. Compensatory Eating Avoidance Program
2.5. Assessment of Feasbility of the Exercise Intervention
2.5.1. CEAP Workshop
2.5.2. Use of Behavior Change Techniques
2.5.3. Open-Ended Feedback and Recommendations
2.6. Assessment of Preliminanary Efficacy of the Intervention
2.6.1. Compensatory Beliefs and Behaviors
2.6.2. Health and Fitness
2.6.3. Snack Intake
2.7. Data Analysis
2.7.1. Recruitment and Baseline Characteristics
2.7.2. Feasibility and Acceptability of the Exercise Intervention
2.7.3. Preliminary Efficacy of the Intervention
3. Results
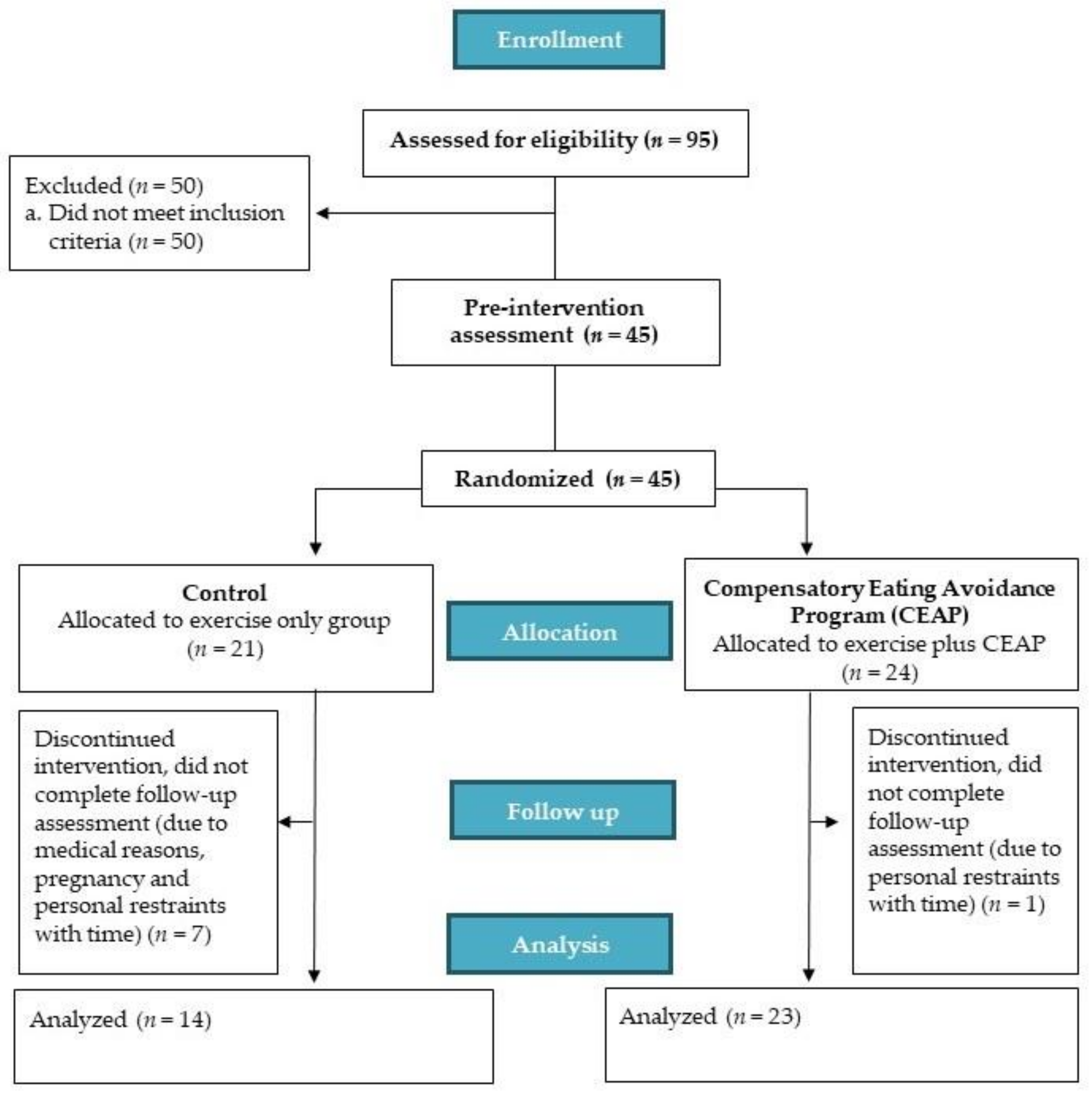
3.1. Recruitement and Baseline Characteristics
3.2. Assessment of Feasbility of the Exercise Intervention
3.2.1. CEAP Workshop
3.2.2. Use of Behavior Change Techniques
3.2.3. Open-Ended Feedback and Recommendations
3.3. Assessment of Preliminary Efficacy of the Intervention
3.3.1. Compensatory Beliefs and Behaviors
3.3.2. Health and Fitness
3.3.3. Snack Intake
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Finlayson, G.; Caudwell, P.; Gibbons, C.; Hopkins, M.; King, N.; Blundell, J. Low fat loss response after medium-term supervised exercise in obese is associated with exercise-induced increase in food reward. J. Obes. 2011, 2011, 658–665. [Google Scholar] [CrossRef] [PubMed]
- King, N.A.; Hopkins, M.; Caudwell, P.; Stubbs, R.J.; Blundell, J.E. Individual variability following 12 weeks of supervised exercise: Identification and characterization of compensation for exercise-induced weight loss. Int. J. Obes. 2008, 32, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D.M.; Bouchard, C.; Church, T.; Slentz, C.; Kraus, W.E.; Redman, L.M.; Martin, C.K.; Silva, A.M.; Vossen, M.; Westerterp, K.; et al. Why do individuals not lose more weight from an exercise intervention at a defined dose? An energy balance analysis. Obes. Rev. 2012, 13, 835–847. [Google Scholar] [CrossRef] [PubMed]
- Fenzl, N.; Bartsch, K.; Koenigstorfer, J. Labeling exercise fat-burning increases post-exercise food consumption in self-imposed exercisers. Appetite 2014, 81, 1–7. [Google Scholar] [CrossRef] [PubMed]
- McCaig, D.C.; Hawkins, L.A.; Rogers, P.J. Licence to eat: Information on energy expended during exercise affects subsequent energy intake. Appetite 2016, 107, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Werle, C.O.C.; Wansink, B.; Payne, C.R. Is it fun or exercise? The framing of physical activity biases subsequent snacking. Mark. Lett. 2015, 26, 691–702. [Google Scholar] [CrossRef]
- Knäuper, B.; Rabiau, M.; Cohen, O.; Patriciu, N. Compensatory health beliefs: Scale development and psychometric properties. Psychol. Health 2004, 19, 607–624. [Google Scholar] [CrossRef]
- Miquelon, P.; Knäuper, B.; Vallerand, R.J. Motivation and goal attainment. The role of compensatory beliefs. Appetite 2012, 58, 608–615. [Google Scholar] [CrossRef] [PubMed]
- West, J.; Guelfi, K.J.; Dimmock, J.A.; Jackson, B. “I deserve a treat”: Exercise motivation as a predictor of post-exercise dietary licensing beliefs and implicit associations toward unhealthy snacks. Psychol. Sport Exerc. 2017, 32, 93–101. [Google Scholar] [CrossRef]
- Moshier, S.J.; Landau, A.J.; Hearon, B.A.; Stein, A.T.; Greathouse, L.; Smits, J.A.J.; Otto, M.W. The development of a novel measure to assess motives for Compensatory Eating in Response to Exercise—The CEMQ. Behav. Med. 2016, 42, 93–104. [Google Scholar] [CrossRef] [PubMed]
- Kivetz, R.; Zheng, Y. Determinants of justification and self-control. J. Exp. Psychol. Gen. 2006, 135, 572–587. [Google Scholar] [CrossRef] [PubMed]
- De Witt Huberts, J.C.; Evers, C.; de Ridder, D.T.D. License to sin: Self-licensing as a mechanism underlying hedonic consumption. Eur. J. Soc. Psychol. 2012, 42, 490–496. [Google Scholar] [CrossRef]
- Michie, S.; Abraham, C.; Whittington, C.; McAteer, J.; Gupta, S. Effective techniques in healthy eating and physical activity interventions: A meta-regression. Health Psychol. 2009, 28, 690–701. [Google Scholar] [CrossRef] [PubMed]
- Dusseldorp, E.; Van Genugten, L.; Van Buuren, S.; Verheijden, M.W.; Van Empelen, P. Combinations of techniques that effectively change health behavior: Evidence from meta-CART analysis. Health Psychol. 2014, 33, 1530–1540. [Google Scholar] [CrossRef] [PubMed]
- De Mestral, C.; Khalatbari-Soltani, S.; Stringhini, S.; Marques-Vidal, P. Fifteen-year trends in the prevalence of barriers to healthy eating in a high-income country. Am. J. Clin. Nutr. 2017, 105, 660–668. [Google Scholar] [CrossRef] [PubMed]
- Armitage, C.J. Evidence that implementation intentions reduce dietary fat intake: A randomized trial. Health Psychol. 2004, 23, 319–323. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Ashford, S.; Sniehotta, F.F.; Dombrowski, S.U.; Bishop, A.; French, D.P. A refined taxonomy of behaviour change techniques to help people change their physical activity and healthy eating behaviours: The CALO-RE taxonomy. Psychol. Health 2011, 26, 1479–1498. [Google Scholar] [CrossRef] [PubMed]
- Olander, E.; Fletcher, H.; Williams, S.; Atkinson, L.; Turner, A.; French, D. What are the most effective techniques in changing obese individuals’ physical activity self-efficacy and behaviour: A systematic review and meta-analysis. Int. J. Behav. Nutr. Phys. Act. 2013, 10, 29. [Google Scholar] [CrossRef] [PubMed]
- Annesi, J.J.; Howton, A.; Johnson, P.H.; Porter, K.J. Pilot testing a cognitive-behavioral protocol on psychosocial predictors of exercise, nutrition, weight, and body satisfaction changes in a college-level health-related fitness course. J. Am. Coll. Health 2015, 63, 268–278. [Google Scholar] [CrossRef] [PubMed]
- Kreausukon, P.; Gellert, P.; Lippke, S.; Schwarzer, R. Planning and self-efficacy can increase fruit and vegetable consumption: A randomized controlled trial. J. Behav. Med. 2012, 35, 443–451. [Google Scholar] [CrossRef] [PubMed]
- Shen, H.; Wang, Y.; Edwards, H. Can a community-based peer-led diabetic self-management programme be effective: 12-week evaluation. J. Clin. Nurs. 2017, 26, 1621–1631. [Google Scholar] [CrossRef] [PubMed]
- Craig, P.; Dieppe, P.; Macintyre, S.; Michie, S.; Nazareth, I.; Petticrew, M. Developing and evaluating complex interventions: The new Medical Research Council guidance. Int. J. Nurs. Stud. 2013, 50, 587–592. [Google Scholar] [CrossRef] [PubMed]
- Lancaster, G.A. Pilot and feasibility studies come of age! Pilot Feasibility Stud. 2015, 1, 1. [Google Scholar] [CrossRef] [PubMed]
- Garber, E.C.; Blissmer, R.B.; Deschenes, A.M.; Franklin, J.B.; Lamonte, C.M.; Lee, P.I.M.; Nieman, P.D.; Swain, P.D. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: Guidance for prescribing exercise. Med. Sci. Sports Exerc. 2011, 43, 1334–1359. [Google Scholar] [CrossRef] [PubMed]
- Borg, A.V.G. Psychophysical bases of perceived exertion. Med. Sci. Sports Exerc. 1982, 14, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Abe, T.; Kawakami, Y.; Sugita, M.; Fukunaga, T. Relationship between training frequency and subcutaneous and visceral fat in women. Med. Sci. Sports Exerc. 1997, 29, 1549–1553. [Google Scholar] [CrossRef] [PubMed]
- Eat For Health Program. Available online: https://www.eatforhealth.gov.au/sites/default/files/files/the_guidelines/n55_australian_dietary_guidelines.pdf (accessed on 14 April 2017).
- Australian Dietary Guidelines. Available online: https://www.nhmrc.gov.au/_files_nhmrc/file/publications/n55_australian_dietary_guidelines1.pdf (accessed on 14 April 2017).
- Doran, G.T. There’s a SMART way to write management’s goals and objectives. Manag. Rev. 1981, 70, 35–36. [Google Scholar]
- Ryan, R.M. Control and information in the intrapersonal sphere: An extension of cognitive evaluation theory. J. Pers. Soc. Psychol. 1982, 43, 450–461. [Google Scholar] [CrossRef]
- Sniehotta, F.; Schwarzer, R.; Scholz, U.; Schuz, B. Action planning and coping planning for long-term lifestyle change: Theory and assessment. Eur. J. Soc. Psychol. 2005, 35, 565–576. [Google Scholar] [CrossRef]
- Godin, G.; Shepherd, R. A simple method to assess exercise behaviour in the community. Can. J. Appl. Sport Sci. 1985, 10, 141–146. [Google Scholar] [PubMed]
- Karlsson, J.; Persson, L.O.; Sjöström, L.; Sullivan, M. Psychometric properties and factor structure of the Three-Factor Eating Questionnaire (TFEQ) in obese men and women. Results from the Swedish Obese Subjects (SOS) study. Int. J. Obes. 2000, 24, 1715–1725. [Google Scholar] [CrossRef]
- Telford, R.; Minikin, B.; Hahn, A.G.; Hooper, L.A. A simple method for the assessment of general fitness: The Tri-level Profile. Aust. J. Sci. Med. Sport 1989, 21, 6–9. [Google Scholar]
- Guelfi, K.J.; Donges, C.E.; Duffield, R. Beneficial effects of 12 weeks of aerobic compared with resistance exercise training on perceived appetite in previously sedentary overweight and obese men. Metabolism 2013, 62, 235–243. [Google Scholar] [CrossRef] [PubMed]
- Markland, D.; Tobin, V. A modification to the behavioural regulation in exercise questionnaire to include an assessment of amotivation. J. Sport Exerc. Psychol. 2004, 26, 191–196. [Google Scholar] [CrossRef]
- Wilson, P.M.; Rodgers, W.M.; Loitz, C.C.; Scime, G. “It’s Who I Am … Really!” The importance of integrated regulation in exercise contexts. J. Appl. Biobehav. Res. 2006, 11, 79–104. [Google Scholar] [CrossRef]
- Little, R.J.A. A test of missing completely at random for multivariate data with missing values. J. Am. Stat. Assoc. 1988, 83, 1198–1202. [Google Scholar] [CrossRef]
- Graham, J.W. Missing data analysis: Making it work in the real world. Annu. Rev. Psychol. 2009, 60, 549–576. [Google Scholar] [CrossRef] [PubMed]
- Gibson, C.; Greene, J.L.; Lowry, B.; Lee, J.; Mount, R.; Alsman, K.; Sullivan, D. Feasibility of a televideo nutrition and physical activity intervention for adult survivors of childhood cancer. J. Acad. Nutr. Diet. 2017, 117, 25. [Google Scholar] [CrossRef]
- Jassil, F.C.; Manning, S.; Lewis, N.; Steinmo, S.; Kingett, H.; Lough, F.; Pucci, A.B.F.; Cheung, W.H.; Finer, N.; Walker, J.; et al. Feasibility and impact of a combined supervised exercise and nutritional-behavioral intervention following bariatric surgery: A pilot study. J. Obes. 2015, 2015, 693829. [Google Scholar] [CrossRef] [PubMed]
- Mackey, E.; Schweitzer, A.; Hurtado, M.E.; Hathway, J.; DiPietro, L.; Lei, K.Y.; Klein, C.J. The feasibility of an e-mail-delivered intervention to improve nutrition and physical activity behaviors in African American college students. J. Am. Coll. Health 2015, 63, 109–117. [Google Scholar] [CrossRef] [PubMed]
- Hsu, Y.-T.; Buckworth, J.; Focht, B.C.; Connell, A.A. Feasibility of a self-determination theory-based exercise intervention promoting healthy at every size with sedentary overweight women: Project CHANGE. Psychol. Sport Exerc. 2013, 14, 283–292. [Google Scholar] [CrossRef]
- Mann, S.; Domone, S.; Wade, M.; Beedie, C. Combining supervised exercise and physical activity counselling might increase retention to GP exercise referral programmes. Med. Sci. Sports Exerc. 2016, 48, 79–80. [Google Scholar] [CrossRef]
- Gillison, F.; Stathi, A.; Reddy, P.; Perry, R.; Taylor, G.; Bennett, P.; Dunbar, J.; Greaves, C. Processes of behavior change and weight loss in a theory-based weight loss intervention program: A test of the process model for lifestyle behavior change. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Elbert, S.P.; Dijkstra, A.; Oenema, A. A mobile phone app intervention targeting fruit and vegetable consumption: The efficacy of textual and auditory tailored health information tested in a randomized controlled trial. J. Med. Internet Res. 2016, 18, 147. [Google Scholar] [CrossRef] [PubMed]
- Mummah, S.; Robinson, T.; Mathur, M.; Farzinkhou, S.; Sutton, S.; Gardner, C. Effect of a mobile app intervention on vegetable consumption in overweight adults: A randomized controlled trial. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 125. [Google Scholar] [CrossRef] [PubMed]
- Turrell, G.; Kavanagh, A.M. Socio-economic pathways to diet: Modelling the association between socio-economic position and food purchasing behaviour. Public Health Nutr. 2006, 9, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Amrein, M.A.; Rackow, P.; Inauen, J.; Radtke, T.; Scholz, U. The role of Compensatory Health Beliefs in eating behavior change: A mixed method study. Appetite 2017, 116, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Kaklamanou, D.; Armitage, C.J.; Jones, C.R. A further look into compensatory health beliefs: A think aloud study. Br. J. Health Psychol. 2013, 18, 139–154. [Google Scholar] [CrossRef] [PubMed]
- Storm, V.; Reinwand, D.; Wienert, J.; Kuhlmann, T.; De Vries, H.; Lippke, S. Brief report: Compensatory health beliefs are negatively associated with intentions for regular fruit and vegetable consumption when self-efficacy is low. J. Health Psychol. 2017, 22, 1094–1100. [Google Scholar] [CrossRef] [PubMed]
- Glock, S.; Müller, B.C.N.; Krolak-Schwerdt, S. Implicit associations and compensatory health beliefs in smokers: Exploring their role for behaviour and their change through warning labels. Br. J. Health Psychol. 2013, 18, 814–826. [Google Scholar] [CrossRef] [PubMed]
- Radtke, T.; Inauen, J.; Rennie, L.; Orbell, S.; Scholz, U. Trait versus state effects of dispositional and situational Compensatory Health Beliefs on high-calorie snack consumption. Zeitschr. Gesundheitspsychol. 2014, 22, 156–164. [Google Scholar] [CrossRef]
- Warde, A.; Yates, L. Understanding eating events: Snacks and meal patterns in Great Britain. Food Cult. Soc. 2017, 20, 15–36. [Google Scholar] [CrossRef]
- Reichenberger, J.; Richard, A.; Smyth, J.M.; Fischer, D.; Pollatos, O.; Blechert, J. It’s craving time: Time of day effects on momentary hunger and food craving in daily life. Nutrition 2018, 55–56, 15–20. [Google Scholar] [CrossRef] [PubMed]
- King, N.A.; Hopkins, M.; Caudwell, P.; Stubbs, R.J.; Blundell, J.E. Beneficial effects of exercise: Shifting the focus from body weight to other markers of health. Br. J. Sports Med. 2009, 43, 924–927. [Google Scholar] [CrossRef] [PubMed]
- Thorogood, A.; Mottillo, S.; Shimony, A.; Filion, K.B.; Joseph, L.; Genest, J.; Pilote, L.; Poirier, P.; Schiffrin, E.L.; Eisenberg, M.J. Isolated aerobic exercise and weight loss: A systematic review and meta-analysis of randomized controlled trials. Am. J. Med. 2011, 124, 747–755. [Google Scholar] [CrossRef] [PubMed]
- Melzer, K.; Renaud, A.; Zurbuchen, S.; Tschopp, C.; Lehmann, J.; Malatesta, D.; Ruch, N.; Schutz, Y.; Kayser, B.; Mäder, U. Alterations in energy balance from an exercise intervention with ad libitum food intake. J. Nutr. Sci. 2016, 5, e7. [Google Scholar] [CrossRef] [PubMed]
- Rocha, J.; Paxman, J.; Dalton, C.; Winter, E.; Broom, D.R. Effects of a 12-week aerobic exercise intervention on eating behaviour, food cravings, and 7-day energy intake and energy expenditure in inactive men. Appl. Physiol. Nutr. Metab. 2016, 41, 1129–1136. [Google Scholar] [CrossRef] [PubMed]
- Obara-Golebiowska, M.; Eufemia Przybylowicz, K. Associations between obesity and diet-related compensatory health beliefs. Iran. J. Public Health 2015, 44, 1156–1157. [Google Scholar] [PubMed]
| Baseline Characteristics | Control (n = 21) | CEAP (n = 24) | p |
|---|---|---|---|
| Age (year) | 30.90 ± 6.96 | 29.58 ± 7.25 | 0.538 |
| Body mass (kg) | 68.15 ± 10.53 | 72.59 ± 13.63 | 0.233 |
| BMI (kg/m2) | 23.79 ± 2.55 | 24.66 ± 3.15 | 0.323 |
| Female | 16 (35.6) | 14 (31.1) | 0.205 |
| SEIFA IRSAD top quintile (n = 44) | 14 (70.0) | 19 (79.2) | 0.484 |
| Leisure time physical activity | 21.93 ± 15.28 | 19.19 ± 14.17 | 0.536 |
| Exercise motivation | 10.42 ± 5.64 | 9.95 ± 4.10 | 0.749 |
| Cognitive restraint of eating | 2.37 ± 0.50 | 2.16 ± 0.40 | 0.136 |
| CEAP Evaluation Items | CEAP Group (n = 23) |
|---|---|
| Post-Workshop | |
| Q1. Overall, the Healthy Lifestyle Workshop was useful in supporting my health objectives. | 3.96 ± 0.83 |
| Q2. The information on exercise and nutrition was useful in supporting my health objectives. | 3.87 ± 0.82 |
| Q3. The information on compensatory health beliefs and licensing was useful in supporting my health objectives. | 4.04 ± 1.07 |
| Q4. The activity on licensing and possible food alternatives was useful in supporting my health objectives. | 3.83 ± 0.94 |
| Q5. The activity on goal setting was useful in supporting my health objectives. | 4.17 ± 0.72 |
| Q6. The activity on identifying possible barriers and coping plans was useful in supporting my health objectives. | 4.26 ± 0.86 |
| Q7. I understood the information that was presented to me during the workshop. | 4.91 ± 0.29 |
| Total mean score | 4.15 ± 0.65 |
| Post-Intervention | |
| “During the 8-week intervention, to what extent did you…” | |
| Q1. Stick to the goals you specified in the Healthy Lifestyle Workshop | 3.57 ± 0.90 |
| Q2. Use the coping plans formulated in the Healthy Lifestyle Workshop | 2.87 ± 1.10 |
| Q3. Enlist social support from others to help you progress toward your health objectives | 3.00 ± 1.04 |
| Q4. Use the self-monitoring diary to monitor your food and drink intake around exercise | 1.86 ± 1.25 |
| Q5. Use cues, reminders, or prompts to aid your progress toward your health objectives | 2.35 ± 1.23 |
| Total mean score | 2.73 ± 0.73 |
| Compensatory Measures | Control (n = 14) | CEAP (n = 22) | ||||
|---|---|---|---|---|---|---|
| Pre-intervention | Post-intervention | Cohen’s d | Pre-intervention | Post-intervention | Cohen’s d | |
| CHB | 2.18 ± 0.91 | 2.21 ± 0.83 | 0.03 | 2.62 ± 1.38 | 2.61 ± 0.98 | 0.01 |
| CEMQ-Q1 | 2 ± 0.78 | 2.07 ± 0.92 | 0.08 | 2.27 ± 0.77 | 1.91 ± 0.87 | 0.44 |
| Health and Fitness Measures | Control (n = 14) | CEAP (n = 23) | Main Effect of Time | ||||
|---|---|---|---|---|---|---|---|
| Pre-intervention | Post-intervention | Cohen’s d | Pre-intervention | Post-intervention | Cohen’s d | p value | |
| Body mass (kg) | 70.23 ± 10.86 | 69.93 ± 11.11 | 0.03 | 72.99 ± 13.79 | 72.64 ± 13.45 | 0.03 | 0.487 |
| BMI | 24.30 ± 2.68 | 24.17 ± 2.49 | 0.05 | 24.68 ± 3.22 | 24.58 ± 3.16 | 0.03 | 0.480 |
| Waist circ. (cm) | 84.3 ± 8.3 | 79.4 ± 7.2 | 0.63 | 81.8 ± 10.2 | 79.4 ± 10.4 | 0.24 | <0.001 |
| Waist: Hip ratio | 0.82 ± 0.06 | 0.79 ± 0.06 | 0.50 | 0.80 ± 0.06 | 0.78 ± 0.06 | 0.33 | <0.001 |
| Body fat (%) | 35.14 ± 6.40 | 34.34 ± 6.22 | 0.13 | 31.81 ± 9.49 | 30.81 ± 9.12 | 0.11 | 0.005 |
| Lean muscle mass (%) | 61.25 ± 6.21 | 62.12 ± 6.08 | 0.14 | 63.42 ± 10.13 | 64.85 ± 9.21 | 0.15 | 0.099 |
| Fasting glucose (mmol/L) | 4.6 ± 0.4 | 4.7 ± 0.6 | 0.21 | 4.6 ± 0.3 | 4.6 ± 0.5 | 0.17 | 0.357 |
| Systolic BP (mmHg) | 115 ± 9 | 110 ± 6 | 0.65 | 115 ± 12 | 110 ± 11 | 0.43 | <0.001 |
| Diastolic BP (mmHg) | 79 ± 6 | 73 ± 5 | 1.09 | 76 ± 7 | 74 ± 8 | 0.27 | 0.001 |
| Cardiovascular fitness (Power output (W)) at 80% HRmax | 130 ± 31 | 146 ± 38 | 0.46 | 144 ± 35 | 159 ± 36 | 0.42 | <0.001 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
West, J.S.; Guelfi, K.J.; Dimmock, J.A.; Jackson, B. Testing the Feasibility and Preliminary Efficacy of an 8-Week Exercise and Compensatory Eating Intervention. Nutrients 2018, 10, 923. https://doi.org/10.3390/nu10070923
West JS, Guelfi KJ, Dimmock JA, Jackson B. Testing the Feasibility and Preliminary Efficacy of an 8-Week Exercise and Compensatory Eating Intervention. Nutrients. 2018; 10(7):923. https://doi.org/10.3390/nu10070923
Chicago/Turabian StyleWest, Jessica S., Kym J. Guelfi, James A. Dimmock, and Ben Jackson. 2018. "Testing the Feasibility and Preliminary Efficacy of an 8-Week Exercise and Compensatory Eating Intervention" Nutrients 10, no. 7: 923. https://doi.org/10.3390/nu10070923
APA StyleWest, J. S., Guelfi, K. J., Dimmock, J. A., & Jackson, B. (2018). Testing the Feasibility and Preliminary Efficacy of an 8-Week Exercise and Compensatory Eating Intervention. Nutrients, 10(7), 923. https://doi.org/10.3390/nu10070923




