Effects of Dietary Intake of Japanese Mushrooms on Visceral Fat Accumulation and Gut Microbiota in Mice
Abstract
1. Introduction
2. Materials and Methods
2.1. Preparation of Mushroom Mixture
2.2. Preparation of the Test Diet
2.3. Animals
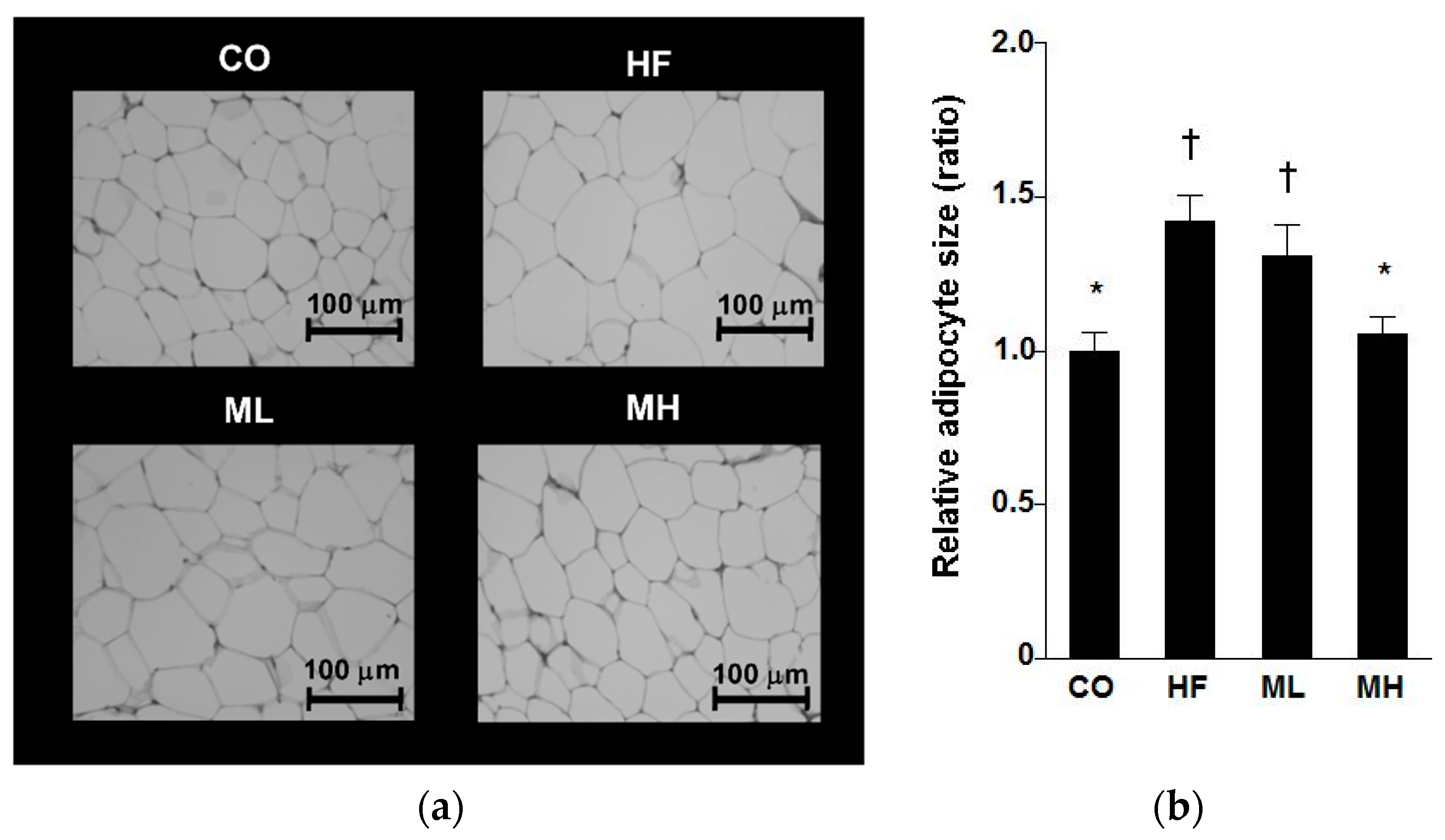
2.4. Histological Analysis
2.5. Biochemical Analyses in Serum and Liver
2.6. mRNA Expression Analysis
2.7. Gut Microbiota Analysis
2.8. Statistical Analysis
3. Results
3.1. Effects of Mushroom Intake on Growth Parameters
3.2. Biochemical Parameters in Serum and Liver
3.3. mRNA Expression in Perinephric Adipose Tissue
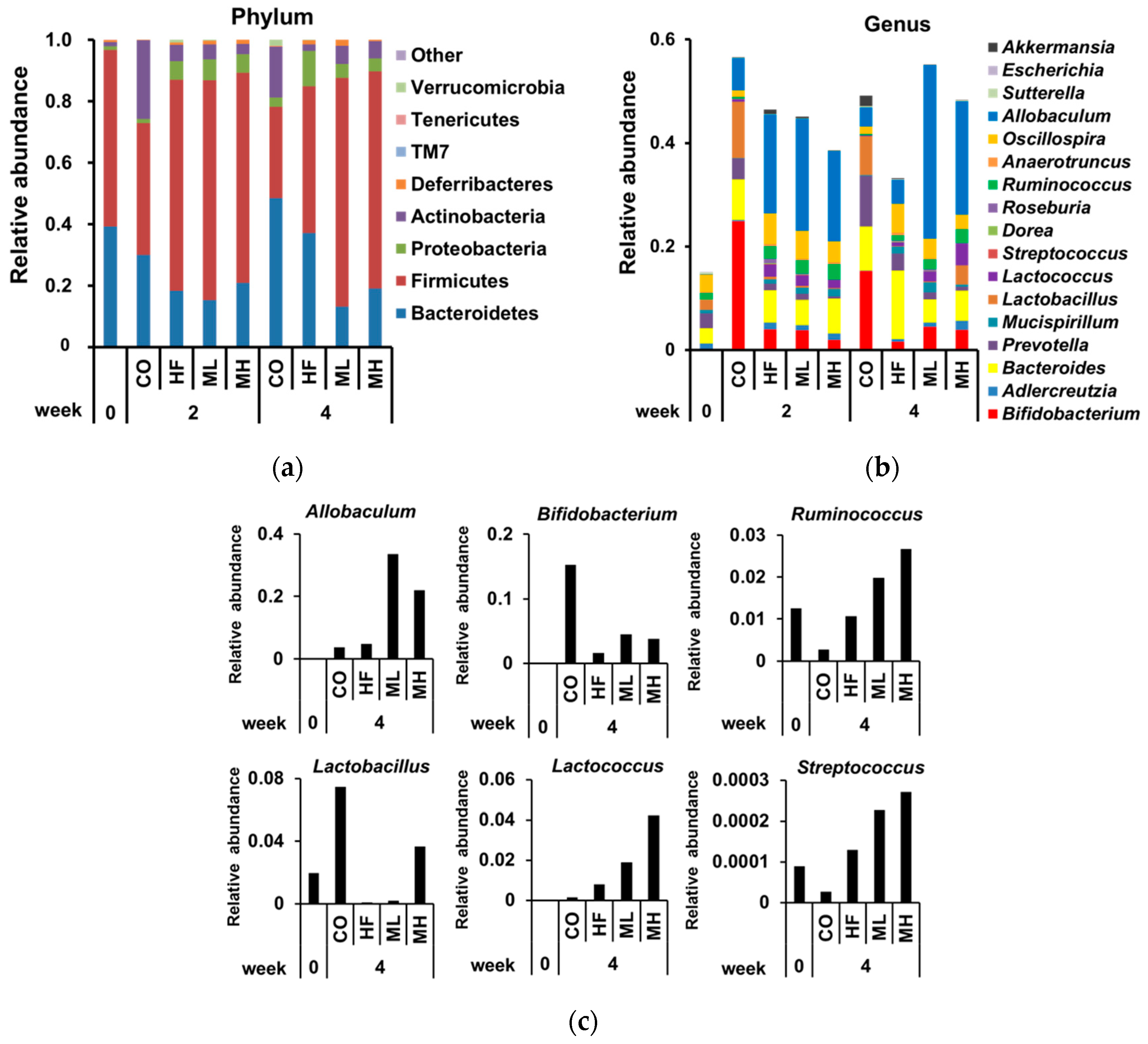
3.4. Effects of Mushroom Intake on Gut Microbiota
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Sugahara, T. Japanese people and mushrooms. J. Cook. Sci. Jpn. 2001, 34, 313–320. (In Japanese) [Google Scholar]
- National Health and Nutrition Survey Report. 2015. Available online: http://www.mhlw.go.jp/bunya/kenkou/eiyou/h27-houkoku.html (accessed on 1 June 2016).
- Valverde, M.E.; Hernández-Pérez, T.; Paredes-López, O. Edible mushrooms: Improving human health and promoting quality life. Int. J. Microbiol. 2015, 2015, 376387. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.; Nie, S. The structure of mushroom polysaccharides and their beneficial role in health. Food Funct. 2015, 6, 3205–3217. [Google Scholar] [CrossRef] [PubMed]
- Survey on Production Forest Products Production Statistics. 2014. Available online: https://www.e-stat.go.jp/stat-search/files?page=1&layout=datalist&lid=000001149816 (accessed on 1 June 2016).
- Mizutani, T.; Inatomi, S.; Inazu, A.; Kawahara, E. Hypolipidemic effect of Pleurotus eryngii extract in fat-loaded mice. J. Nutr. Sci. Vitaminol. 2010, 56, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Handayani, D.; Chen, J.; Meyer, B.J.; Huang, X.-F. Dietary shiitake mushroom (Lentinus edodes) prevents fat deposition and lowers triglyceride in rats fed a high-fat diet. J. Obes. 2011, 2011, 258051. [Google Scholar] [CrossRef] [PubMed]
- Yeh, M.-Y.; Ko, W.-C.; Lin, L.-Y. Hypolipidemic and antioxidant activity of enoki mushrooms (Flammulina velutipes). BioMed Res. Int. 2014, 2014, 352385. [Google Scholar] [CrossRef] [PubMed]
- Iuchi, T.; Hosaka, T.; Shiroishi, M.; Ono, H.; Inukai, K.; Sumita, T.; Sakai, G.; Katayama, S.; Awata, T. Influence of treatment with extracts of Hypsyzigus marmoreus mushroom on body composition during obesity development in kk-ay mice. J. Nutr. Sci. Vitaminol. 2015, 61, 96–100. [Google Scholar] [CrossRef] [PubMed]
- Vetvicka, V.; Vetvickova, J. Immune-enhancing effects of maitake (Grifola frondosa) and shiitake (Lentinula edodes) extracts. Ann. Transl. Med. 2014, 2, 14. [Google Scholar] [PubMed]
- Masuda, Y.; Inoue, H.; Ohta, H.; Miyake, A.; Konishi, M.; Nanba, H. Oral administration of soluble β-glucans extracted from Grifola frondosa induces systemic antitumor immune response and decreases immunosuppression in tumor-bearing mice. Int. J. Cancer 2013, 133, 108–119. [Google Scholar] [CrossRef] [PubMed]
- Mori, K.; Kobayashi, C.; Tomita, T.; Inatomi, S.; Ikeda, M. Antiatherosclerotic effect of the edible mushrooms Pleurotus eryngii (eringi), Grifola frondosa (maitake), and Hypsizygus marmoreus (bunashimeji) in apolipoprotein e-deficient mice. Nutr. Res. 2008, 28, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Hong, L.; Xun, M.; Wutong, W. Anti-diabetic effect of an α-glucan from fruit body of maitake (Grifola frondosa) on kk-ay mice. J. Pharm. Pharmacol. 2007, 59, 575–582. [Google Scholar] [CrossRef] [PubMed]
- Hofbauer, K. Molecular pathways to obesity. Int. J. Obes. Relat. Metab. Disord. 2002, 26, S18. [Google Scholar] [CrossRef] [PubMed]
- Tsuduki, T.; Takeshika, N.; Nakamura, Y.; Nakagawa, K.; Igarashi, M.; Miyazawa, T. DNA microarray analysis of rat liver after ingestion of japanese and american food. J. Jpn. Soc. Nutr. Food Sci. 2008, 61, 255–264. [Google Scholar] [CrossRef]
- Yoneda, M.; Ohuo, H.; Oki, K. Westernization of Lifestyle Causes Obesity-Associated Metabolic Disorders in the Japanese Population. J. Obes. Eat. Disord. 2016, 2, 24. [Google Scholar] [CrossRef][Green Version]
- Kitano, Y.; Honma, T.; Hatakeyama, Y.; Jibu, Y.; Kawakami, Y.; Tsuduki, T.; Nakagawa, K.; Miyazawa, T. Effects of historical differences in components of the japanese diet on the risk of obesity in mice. J. Jpn. Soc. Nutr. Food Sci. 2014, 67, 73–85. [Google Scholar] [CrossRef]
- Egusa, G.; Watanabe, H.; Ohshita, K.; Fujikawa, R.; Yamane, K.; Okubo, M.; Kohno, N. Influence of the extent of westernization of lifestyle on the progression of preclinical atherosclerosis in Japanese subjects. J. Atheroscler. Thromb. 2002, 9, 299–304. [Google Scholar] [CrossRef] [PubMed]
- Enzi, G.; Baritussio, A.; Marchiori, E.; Crepaldi, G. Short-term and long-term clinical evaluation of a non-amphetaminic anorexiant (mazindol) in the treatment of obesity. J. Int. Med. Res. 1976, 4, 305–318. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.G.; Park, C.Y. Anti-obesity drugs: A review about their effects and safety. Diabetes Metab. J. 2012, 36, 13–25. [Google Scholar] [CrossRef] [PubMed]
- Turnbaugh, P.J.; Ley, R.E.; Mahowald, M.A.; Magrini, V.; Mardis, E.R.; Gordon, J.I. An obesity-associated gut microbiome with increased capacity for energy harvest. Nature 2006, 444, 1027. [Google Scholar] [CrossRef] [PubMed]
- Cani, P.D.; Bibiloni, R.; Knauf, C.; Waget, A.; Neyrinck, A.M.; Delzenne, N.M.; Burcelin, R. Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes 2008, 57, 1470–1481. [Google Scholar] [CrossRef] [PubMed]
- Ley, R.E.; Bäckhed, F.; Turnbaugh, P.; Lozupone, C.A.; Knight, R.D.; Gordon, J.I. Obesity alters gut microbial ecology. Proc. Natl. Acad. Sci. USA 2005, 102, 11070–11075. [Google Scholar] [CrossRef] [PubMed]
- Conlon, M.A.; Bird, A.R. The impact of diet and lifestyle on gut microbiota and human health. Nutrients 2014, 7, 17–44. [Google Scholar] [CrossRef] [PubMed]
- Tremaroli, V.; Bäckhed, F. Functional interactions between the gut microbiota and host metabolism. Nature 2012, 489, 242. [Google Scholar] [CrossRef] [PubMed]
- Den Besten, G.; Van Eunen, K.; Groen, A.K.; Venema, K.; Reijngoud, D.-J.; Bakker, B.M. The role of short-chain fatty acids in the interplay between diet, gut microbiota, and host energy metabolism. J. Lipid Res. 2013, 54, 2325–2340. [Google Scholar] [CrossRef] [PubMed]
- Tsai, Y.-T.; Cheng, P.-C.; Pan, T.-M. Anti-obesity effects of gut microbiota are associated with lactic acid bacteria. Appl. Microbiol. Biotechnol. 2014, 98, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Koh, A.; De Vadder, F.; Kovatcheva-Datchary, P.; Bäckhed, F. From dietary fiber to host physiology: Short-chain fatty acids as key bacterial metabolites. Cell 2016, 165, 1332–1345. [Google Scholar] [CrossRef] [PubMed]
- Takasaki, M.; Honma, T.; Yanaka, M.; Sato, K.; Shinohara, N.; Ito, J.; Tanaka, Y.; Tsuduki, T.; Ikeda, I. Continuous intake of a high-fat diet beyond one generation promotes lipid accumulation in liver and white adipose tissue of female mice. J. Nutr. Biochem. 2012, 23, 640–645. [Google Scholar] [CrossRef] [PubMed]
- Tsuduki, T.; Yamamoto, K.; Hatakeyama, Y.; Sakamoto, Y. High dietary fat intake during lactation promotes the development of social stress-induced obesity in the offspring of mice. Nutrients 2015, 7, 5916–5932. [Google Scholar] [CrossRef] [PubMed]
- Rouser, G.; Fleischer, S.; Yamamoto, A. Two dimensional thin layer chromatographic separation of polar lipids and determination of phospholipids by phosphorus analysis of spots. Lipids 1970, 5, 494–496. [Google Scholar] [CrossRef] [PubMed]
- Tsuzuki, T.; Tokuyama, Y.; Igarashi, M.; Miyazawa, T. Tumor growth suppression by α-eleostearic acid, a linolenic acid isomer with a conjugated triene system, via lipid peroxidation. Carcinogenesis 2004, 25, 1417–1425. [Google Scholar] [CrossRef] [PubMed]
- Tsuduki, T.; Kikuchi, I.; Kimura, T.; Nakagawa, K.; Miyazawa, T. Intake of mulberry 1-deoxynojirimycin prevents diet-induced obesity through increases in adiponectin in mice. Food Chem. 2013, 139, 16–23. [Google Scholar] [CrossRef] [PubMed]
- Tsuduki, T.; Yamamoto, K.; Hatakeyama, Y.; Sakamoto, Y. High dietary cholesterol intake during lactation promotes development of fatty liver in offspring of mice. Mol. Nutr. Food Res. 2016, 60, 1110–1117. [Google Scholar] [CrossRef] [PubMed]
- Fukushima, M.; Ohashi, T.; Fujiwara, Y.; Sonoyama, K.; Nakano, M. Cholesterol-lowering effects of maitake (Grifola frondosa) fiber, shiitake (Lentinus edodes) fiber, and enokitake (Flammulina velutipes) fiber in rats. Exp. Biol. Med. 2001, 226, 758–765. [Google Scholar] [CrossRef]
- Caz, V.; Gil-Ramírez, A.; Largo, C.; Tabernero, M.; Santamaría, M.N.; Martin-Hernandez, R.; Marín, F.R.; Reglero, G.; Soler-Rivas, C. Modulation of cholesterol-related gene expression by dietary fiber fractions from edible mushrooms. J. Agric. Food Chem. 2015, 63, 7371–7380. [Google Scholar] [CrossRef] [PubMed]
- Nile, S.H.; Park, S.W. Total, soluble, and insoluble dietary fibre contents of wild growing edible mushrooms. Czech J. Food Sci. 2014, 32, 302–307. [Google Scholar] [CrossRef]
- Kurasawa, S.; Sugahara, T.; Hayashi, J. Proximate and dietary fibre analysis of mushrooms. Nippon Shokuhin Kogyo Gakkaishi 1982, 29, 400–406. [Google Scholar] [CrossRef]
- Manzi, P.; Pizzoferrato, L. Beta-glucans in edible mushrooms. Food Chem. 2000, 68, 315–318. [Google Scholar] [CrossRef]
- Isken, F.; Klaus, S.; Osterhoff, M.; Pfeiffer, A.F.; Weickert, M.O. Effects of long-term soluble vs. Insoluble dietary fiber intake on high-fat diet-induced obesity in C57BL/6J mice. J. Nutr. Biochem. 2010, 21, 278–284. [Google Scholar] [CrossRef] [PubMed]
- Adam, C.L.; Thomson, L.M.; Williams, P.A.; Ross, A.W. Soluble fermentable dietary fibre (pectin) decreases caloric intake, adiposity and lipidaemia in high-fat diet-induced obese rats. PLoS ONE 2015, 10, e0140392. [Google Scholar] [CrossRef] [PubMed]
- Hannan, J.; Ali, L.; Rokeya, B.; Khaleque, J.; Akhter, M.; Flatt, P.; Abdel-Wahab, Y. Soluble dietary fibre fraction of Trigonella foenum-graecum (fenugreek) seed improves glucose homeostasis in animal models of type 1 and type 2 diabetes by delaying carbohydrate digestion and absorption, and enhancing insulin action. Br. J. Nutr. 2007, 97, 514–521. [Google Scholar] [CrossRef] [PubMed]
- Bazzano, L.A. Effects of soluble dietary fiber on low-density lipoprotein cholesterol and coronary heart disease risk. Curr. Atheroscler. Rep. 2008, 10, 473–477. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Jørgensen, H.; Eggum, B.O. The influence of dietary fibre on body composition, visceral organ weight, digestibility and energy balance in rats housed in different thermal environments. Br. J. Nutr. 1995, 73, 687–689. [Google Scholar] [CrossRef] [PubMed]
- Brown, M.S.; Goldstein, J.L. The srebp pathway: Regulation of cholesterol metabolism by proteolysis of a membrane-bound transcription factor. Cell 1997, 89, 331–340. [Google Scholar] [CrossRef]
- Horton, J.D.; Goldstein, J.L.; Brown, M.S. Srebps: Activators of the complete program of cholesterol and fatty acid synthesis in the liver. J. Clin. Investig. 2002, 109, 1125–1131. [Google Scholar] [CrossRef] [PubMed]
- Lee, I.; Kim, J.; Ryoo, I.; Kim, Y.; Choo, S.; Yoo, I.; Min, B.; Na, M.; Hattori, M.; Bae, K. Lanostane triterpenes from Ganoderma lucidum suppress the adipogenesis in 3T3-l1 cells through down-regulation of SREBP-1c. Bioorg. Med. Chem. Lett. 2010, 20, 5577–5581. [Google Scholar] [CrossRef] [PubMed]
- Kanagasabapathy, G.; Malek, S.; Mahmood, A.; Chua, K.; Vikineswary, S.; Kuppusamy, U. Beta-glucan-rich extract from Pleurotus sajor-caju (Fr.) singer prevents obesity and oxidative stress in C57BL/6J mice fed on a high-fat diet. Evid. Based Complement. Altern. Med. 2013, 2013, 185259. [Google Scholar] [CrossRef] [PubMed]
- Asano, L.; Watanabe, M.; Ryoden, Y.; Usuda, K.; Yamaguchi, T.; Khambu, B.; Takashima, M.; Sato, S.; Sakai, J.; Nagasawa, K. Vitamin D metabolite, 25-hydroxyvitamin d, regulates lipid metabolism by inducing degradation of SREBP/SCAP. Cell Chem. Biol. 2017, 24, 207–217. [Google Scholar] [CrossRef] [PubMed]
- Gupte, S.A.; Levine, R.J.; Gupte, R.S.; Young, M.E.; Lionetti, V.; Labinskyy, V.; Floyd, B.C.; Ojaimi, C.; Bellomo, M.; Wolin, M.S. Glucose-6-phosphate dehydrogenase-derived nadph fuels superoxide production in the failing heart. J. Mol. Cell. Cardiol. 2006, 41, 340–349. [Google Scholar] [CrossRef] [PubMed]
- Hecker, P.A.; Lionetti, V.; Ribeiro, R.F.; Rastogi, S.; Brown, B.H.; O’Connell, K.A.; Cox, J.W.; Shekar, K.C.; Gamble, D.; Sabbah, H.N. Glucose 6-phosphate dehydrogenase deficiency increases redox stress and moderately accelerates the development of heart failure. Circ. Heart Fail. 2012, 112, 969576. [Google Scholar] [CrossRef] [PubMed]
- Rosen, E.D.; Spiegelman, B.M. PPARγ: A nuclear regulator of metabolism, differentiation, and cell growth. J. Biol. Chem. 2001, 276, 37731–37734. [Google Scholar] [CrossRef] [PubMed]
- Okuno, A.; Tamemoto, H.; Tobe, K.; Ueki, K.; Mori, Y.; Iwamoto, K.; Umesono, K.; Akanuma, Y.; Fujiwara, T.; Horikoshi, H. Troglitazone increases the number of small adipocytes without the change of white adipose tissue mass in obese zucker rats. J. Clin. Investig. 1998, 101, 1354–1361. [Google Scholar] [CrossRef] [PubMed]
- Whitehead, J.; Richards, A.; Hickman, I.; Macdonald, G.; Prins, J. Adiponectin—A key adipokine in the metabolic syndrome. Diabetes Obes. Metab. 2006, 8, 264–280. [Google Scholar] [CrossRef] [PubMed]
- Trompette, A.; Gollwitzer, E.S.; Yadava, K.; Sichelstiel, A.K.; Sprenger, N.; Ngom-Bru, C.; Blanchard, C.; Junt, T.; Nicod, L.P.; Harris, N.L. Gut microbiota metabolism of dietary fiber influences allergic airway disease and hematopoiesis. Nat. Med. 2014, 20, 159. [Google Scholar] [CrossRef] [PubMed]
- Flint, H.J.; Duncan, S.H.; Scott, K.P.; Louis, P. Links between diet, gut microbiota composition and gut metabolism. Proc. Nutr. Soc. 2015, 74, 13–22. [Google Scholar] [CrossRef] [PubMed]
- Douillard, F.P.; De Vos, W.M. Functional genomics of lactic acid bacteria: From food to health. Microb. Cell Fact. 2014, 13, S8. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Zhao, Y.; Zhang, M.; Pang, X.; Xu, J.; Kang, C.; Li, M.; Zhang, C.; Zhang, Z.; Zhang, Y. Structural changes of gut microbiota during berberine-mediated prevention of obesity and insulin resistance in high-fat diet-fed rats. PLoS ONE 2012, 7, e42529. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, S.; Toh, H.; Hase, K.; Oshima, K.; Nakanishi, Y.; Yoshimura, K.; Tobe, T.; Clarke, J.M.; Topping, D.L.; Suzuki, T. Bifidobacteria can protect from enteropathogenic infection through production of acetate. Nature 2011, 469, 543. [Google Scholar] [CrossRef] [PubMed]
- Xiao, C.; Hsieh, J.; Adeli, K.; Lewis, G.F. Gut-liver interaction in triglyceride-rich lipoprotein metabolism. Am. J. Physiol. Endocrinol. Metab. 2011, 301, E429–E446. [Google Scholar] [CrossRef] [PubMed]
- Zacour, A.C.; Silva, M.E.; Cecon, P.R.; Bambirra, E.A.; Vieira, E.C. Effect of dietary chitin on cholesterol absorption and metabolism in rats. J. Nutr. Sci. Vitaminol. 1992, 38, 609–613. [Google Scholar] [CrossRef] [PubMed]
- Neyrinck, A.M.; Bindels, L.B.; De Backer, F.; Pachikian, B.D.; Cani, P.D.; Delzenne, N.M. Dietary supplementation with chitosan derived from mushrooms changes adipocytokine profile in diet-induced obese mice, a phenomenon linked to its lipid-lowering action. Int. Immunopharmacol. 2009, 9, 767–773. [Google Scholar] [CrossRef] [PubMed]
- Thompson, D.; Karpe, F.; Lafontan, M.; Frayn, K. Physical activity and exercise in the regulation of human adipose tissue physiology. Physiol. Rev. 2012, 92, 157–191. [Google Scholar] [CrossRef] [PubMed]
- Chandra, L.C.; Smith, B.J.; Clarke, S.L.; Marlow, D.; D’Offay, J.M.; Kuvibidila, S.R. Differential effects of shiitake-and white button mushroom-supplemented diets on hepatic steatosis in C57BL/6 mice. Food Chem. Toxicol. 2011, 49, 3074–3080. [Google Scholar] [CrossRef] [PubMed]
- Handayani, D.; Meyer, B.J.; Chen, J.; Brown, S.H.; Mitchell, T.W.; Huang, X.-F. A high-dose shiitake mushroom increases hepatic accumulation of triacylglycerol in rats fed a high-fat diet: Underlying mechanism. Nutrients 2014, 6, 650–662. [Google Scholar] [CrossRef] [PubMed]
- Sugiyama, K.; Yamakawa, A. Dietary eritadenine-induced alteration of molecular species composition of phospholipids in rats. Lipids 1996, 31, 399. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Agellon, L.B.; Allen, T.M.; Umeda, M.; Jewell, L.; Mason, A.; Vance, D.E. The ratio of phosphatidylcholine to phosphatidylethanolamine influences membrane integrity and steatohepatitis. Cell Metab. 2006, 3, 321–331. [Google Scholar] [CrossRef] [PubMed]
- Poudyal, H.; Panchal, S.K.; Ward, L.C.; Brown, L. Effects of ALA, EPA and DHA in high-carbohydrate, high-fat diet-induced metabolic syndrome in rats. J. Nutr. Biochem. 2013, 24, 1041–1052. [Google Scholar] [CrossRef] [PubMed]

| Mushroom | Ratio (%) |
|---|---|
| Flammulina velutipes | 33.0 |
| Hypsizygus marmoreus | 28.2 |
| Lentinusedodes | 17.2 |
| Grifola frondosa | 12.0 |
| Pleurotus eryngii | 9.60 |
| Mushroom Mixture | Mimic Mushroom Mixture | ||
|---|---|---|---|
| (g/100 g) | (g/100 g) | ||
| Protein | 21.6 | Casein | 21.6 |
| Fat | 1.60 | Soybean oil | 1.60 |
| Carbohydrate | 26.2 | Cornstarch | 26.2 |
| Water-soluble dietary fiber | 5.20 | Pectin powder | 5.20 |
| Insoluble dietary fiber | 30.5 | Cellulose powder | 30.5 |
| Other | 14.9 | Cellulose powder | 14.9 |
| (kcal/100 g) | (kcal/100 g) | ||
| Energy | 216 | 216 | |
| CO | HF | ML | MH | |
|---|---|---|---|---|
| Control diet | 100% | 0% | 0% | 0% |
| High-fat diet | 0% | 97% | 97% | 97% |
| Mushroom mixture | 0% | 0% | 0.5% | 3% |
| Mimic mushroom mixture | 0% | 3% | 2.5% | 0% |
| Energy (kcal/100 g) | 391 | 460 | 460 | 460 |
| Genbank ID | Gene Name | Primer Sequence (5′ to 3′) | |
|---|---|---|---|
| NM_009605 | Adipoq | Forward | TGTTCCTCTTAATCCTGCCCA |
| Reverse | CCAACCTGCACAAGTTCCCTT | ||
| NM_007393 | β-actin | Forward | GAAATCGTGCGTGACATCAAAG |
| Reverse | TGTAGTTTCATGGATGCCACAG | ||
| NM_007988 | Fas | Forward | CCTGGATAGCATTCCGAACCTG |
| Reverse | TCACAGCCTGGGGTCATCTTTGC | ||
| NM_008062 | G6pdx | Forward | TGGGTCCACCACTGCCACTTTTG |
| Reverse | ATTGGGCTGCACACGGATGACCA | ||
| NM_001039507 | Hsl | Forward | TTCTCCAAAGCACCTAGCCAA |
| Reverse | TGTGGAAAACTAAGGGCTTGTTG | ||
| M29546 | Me | Forward | GAAAGAGGTGTTTGCCCATGA |
| Reverse | AATTGCAGCAACTCCTATGAGG | ||
| NM_011146 | Pparγ | Forward | TCGCTGATGCACTGCCTATG |
| Reverse | GAGAGGTCCACAGAGCTGATT | ||
| NM_011480 | Srebp-1c | Forward | GGAGACATCGCAAACAAGC |
| Reverse | TGAGGTTCCAAAGCAGACTG | ||
| CO | HF | ML | MH | |
|---|---|---|---|---|
| Body weight (g) | ||||
| Final (g) | 26.6 ± 0.5 | 27.0 ± 0.6 | 28.2 ± 0.5 | 28.0 ± 0.5 |
| Gain (g) | 6.50 ± 0.51 | 7.23 ± 0.74 | 8.32 ± 0.59 | 7.93 ± 0.63 |
| Food intake (g/day) | 3.70 ± 0.22 * | 2.93 ± 0.10 † | 2.88 ± 0.11 † | 2.74 ± 0.09 † |
| Energy intake (kcal/day) | 14.5 ± 0.9 | 13.5 ± 0.5 | 13.3 ± 0.5 | 12.6 ± 0.4 |
| Tissue weight (g/100 g Body weight) | ||||
| Brain | 1.72 ± 0.05 | 1.68 ± 0.03 | 1.69 ± 0.03 | 1.66 ± 0.04 |
| Heart | 0.519 ± 0.018 | 0.490 ± 0.013 | 0.454 ± 0.012 † | 0.458 ± 0.013 † |
| Lung | 1.22 ± 0.15 | 0.941 ± 0.07 | 1.03 ± 0.10 | 0.887 ± 0.10 |
| Liver | 3.96 ± 0.15 | 3.88 ± 0.07 | 3.81 ± 0.06 | 3.68 ± 0.05 |
| Pancreas | 0.703 ± 0.082 | 0.752 ± 0.043 | 0.826 ± 0.045 | 0.742 ± 0.043 |
| Spleen | 0.280 ± 0.022 | 0.290 ± 0.018 | 0.297 ± 0.012 | 0.252 ± 0.016 |
| Kidney | 1.17 ± 0.02 | 1.14 ± 0.01 | 1.16 ± 0.02 | 1.13 ± 0.02 |
| The small intestine | 3.35 ± 0.14 | 2.92 ± 0.20 | 3.01 ± 0.16 | 2.92 ± 0.20 |
| The large intestine | 0.602 ± 0.035 | 0.490 ± 0.035 | 0.645 ± 0.046 * | 0.618 ± 0.045 |
| Lengths of the large intestine (cm) | 7.70 ± 0.20 | 7.30 ± 0.42 | 7.68 ± 0.18 | 8.18 ± 0.19 |
| White adipose tissue | ||||
| Mesenteric | 0.954 ± 0.089 | 1.22 ± 0.09 | 1.12 ± 0.16 | 1.05 ± 0.18 |
| Perinephric | 0.791 ± 0.097 | 0.981 ± 0.084 | 0.717 ± 0.092 | 0.623 ± 0.126 * |
| Epididymal | 1.93 ± 0.13 | 2.63 ± 0.14 | 2.61 ± 0.24 | 2.38 ± 0.29 |
| Total | 3.67 ± 0.28 | 4.83 ± 0.22 | 4.45 ± 0.47 | 4.05 ± 0.59 |
| CO | HF | ML | MH | |
|---|---|---|---|---|
| Serum | ||||
| TC (mmol/L) | 3.51 ± 0.13 * | 4.23 ± 0.14 † | 4.97 ± 0.12 †,* | 4.25 ± 0.17 † |
| TG (mmol/L) | 2.39 ± 0.18 | 2.31 ± 0.10 | 2.35 ± 0.08 | 2.77 ± 0.13 |
| PL (mmol/L) | 17.1 ± 0.4 | 18.6 ± 0.6 | 21.1 ± 0.2 †,* | 19.4 ± 0.5 † |
| TBARS (µmol/L) | 7.37 ± 0.38 * | 5.02 ± 0.28 † | 6.19 ± 0.26 †,* | 5.88 ± 0.08 † |
| Glucose (mmol/L) | 12.0 ± 1.1 | 13.1 ± 1.5 | 12.7 ± 0.5 | 9.94 ± 0.4 |
| Insulin (ng/mL) | 0.0747 ± 0.029 | 0.0777 ± 0.0275 | 0.231 ± 0.087 | 0.0684 ± 0.0223 |
| ALT (IU/L) | 7.20 ± 1.33 | 6.76 ± 0.65 | 7.79 ± 0.43 | 8.14 ± 1.39 |
| AST (IU/L) | 62.4 ± 5.6 | 66.7 ± 3.1 | 56.0 ± 5.1 | 49.6 ± 5.1 |
| IL-6 (pg/mL) | 29.2 ± 8.3 | 23.2 ± 8.9 | 39.6 ± 12.9 | 30.1 ± 8.4 |
| Adiponectin (µg/mL) | 33.6 ± 3.7 | 34.3 ± 3.5 | 32.3 ± 3.3 | 50.4 ± 3.6 †,* |
| Liver | ||||
| TC (mmol/L) | 1.82 ± 0.06 * | 2.17 ± 0.09 † | 2.45 ± 0.06 †,* | 2.15 ± 0.05 † |
| TG (mmol/L) | 30.0 ± 6.84 | 36.9 ± 4.9 | 58.7 ± 7.6 † | 66.2 ± 7.4 †,* |
| PL (mmol/L) | 50.6 ± 2.6 | 50.6 ± 2.0 | 53.8 ± 1.3 | 50.1 ± 0.8 |
| TBARS (µmol/L) | 66.1 ± 2.7 * | 50.7 ± 2.4 † | 59.8 ± 2.7 * | 56.0 ± 2.2 † |
| CO | HF | ML | MH | |
|---|---|---|---|---|
| Fas | 1.00 ± 0.20 | 1.06 ± 0.07 | 0.970 ± 0.117 | 0.782 ± 0.126 |
| Me | 1.00 ± 0.18 * | 0.526 ± 0.055 † | 0.396 ± 0.032 † | 0.617 ± 0.162 |
| G6pdx | 1.00 ± 0.16 | 0.678 ± 0.052 | 1.28 ± 0.22 | 2.27 ± 0.60 †,* |
| Srebp-1c | 1.00 ± 0.14 * | 2.26 ± 0.22 † | 1.70 ± 0.13 † | 1.46 ± 0.28 * |
| Hsl | 1.00 ± 0.20 | 1.05 ± 0.29 | 2.00 ± 0.52 | 3.13 ± 1.27 †,* |
| Pparγ | 1.00 ± 0.79 | 3.91 ± 1.90 | 2.61 ± 1.35 | 6.34 ± 1.61 † |
| Adipoq | 1.00 ± 0.23 | 3.71 ± 0.87 | 4.10 ± 1.48 | 9.31 ± 1.64 †,* |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shimizu, T.; Mori, K.; Ouchi, K.; Kushida, M.; Tsuduki, T. Effects of Dietary Intake of Japanese Mushrooms on Visceral Fat Accumulation and Gut Microbiota in Mice. Nutrients 2018, 10, 610. https://doi.org/10.3390/nu10050610
Shimizu T, Mori K, Ouchi K, Kushida M, Tsuduki T. Effects of Dietary Intake of Japanese Mushrooms on Visceral Fat Accumulation and Gut Microbiota in Mice. Nutrients. 2018; 10(5):610. https://doi.org/10.3390/nu10050610
Chicago/Turabian StyleShimizu, Takamitsu, Koichiro Mori, Kenji Ouchi, Mamoru Kushida, and Tsuyoshi Tsuduki. 2018. "Effects of Dietary Intake of Japanese Mushrooms on Visceral Fat Accumulation and Gut Microbiota in Mice" Nutrients 10, no. 5: 610. https://doi.org/10.3390/nu10050610
APA StyleShimizu, T., Mori, K., Ouchi, K., Kushida, M., & Tsuduki, T. (2018). Effects of Dietary Intake of Japanese Mushrooms on Visceral Fat Accumulation and Gut Microbiota in Mice. Nutrients, 10(5), 610. https://doi.org/10.3390/nu10050610




