Household Food Insecurity as a Predictor of Stunted Children and Overweight/Obese Mothers (SCOWT) in Urban Indonesia
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
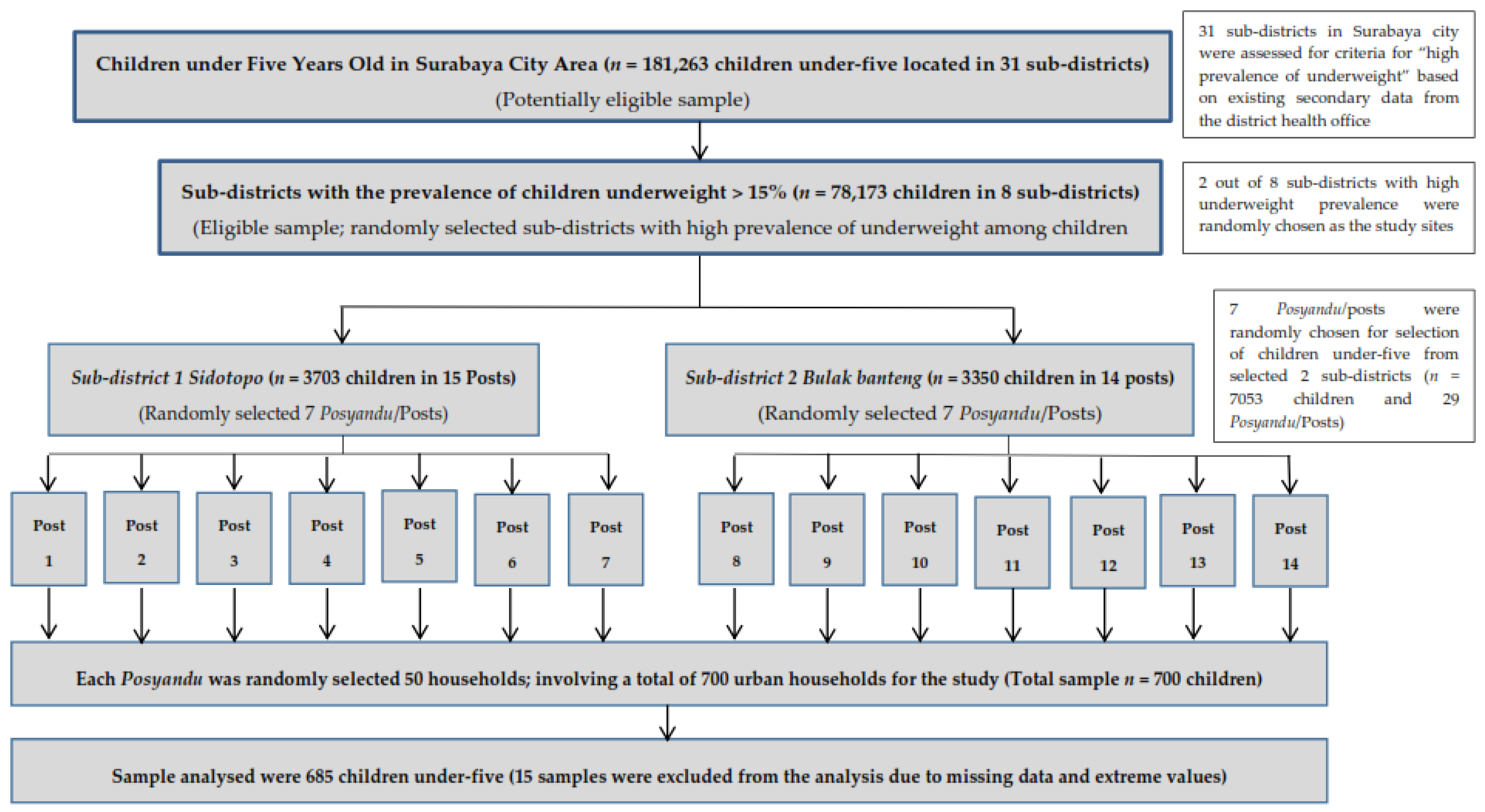
Appendix B
| Variable | Food Security | Mild Insecurity | Moderate Insecurity | Severe Insecurity | Total | p | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | Row % | n | Row % | n | Row % | n | Row % | n | Column % | ||
| Total | 288 | 42.0 | 157 | 22.9 | 105 | 15.3 | 135 | 19.7 | 685 | 100 | |
| Maternal literacy | 0.012 * | ||||||||||
| Illiterate | 17 | 29.8 | 11 | 19.3 | 9 | 15.8 | 20 | 35.1 | 57 | 8.3 | |
| Partially literate | 32 | 34.0 | 20 | 21.3 | 19 | 20.2 | 23 | 24.5 | 94 | 13.7 | |
| Literate | 239 | 44.8 | 126 | 23.6 | 77 | 14.4 | 92 | 17.2 | 534 | 78.0 | |
| Maternal education | <0.001 *** | ||||||||||
| Low (no schooling or elementary school) | 88 | 27.5 | 83 | 25.9 | 54 | 16.9 | 95 | 29.7 | 320 | 46.8 | |
| Medium (junior high school) | 62 | 44.9 | 32 | 23.2 | 27 | 19.6 | 17 | 12.3 | 138 | 20.1 | |
| High (senior high school or college/university) | 138 | 460.8 | 42 | 18.5 | 24 | 10.6 | 23 | 10.1 | 227 | 33.1 | |
| Number of children under 5 years old in the household | 0.046 * | ||||||||||
| 1 child | 260 | 42.1 | 141 | 22.9 | 91 | 14.8 | 125 | 20.3 | 617 | 90.1 | |
| 2 children | 28 | 43.1 | 13 | 20 | 14 | 21.5 | 10 | 15.4 | 65 | 9.5 | |
| Maternal occupation | 0.290 | ||||||||||
| Housewife without maid | 216 | 41.5 | 118 | 22.7 | 86 | 16.5 | 100 | 19.2 | 520 | 75.9 | |
| Housewife with maid | 10 | 38.5 | 5 | 19.2 | 4 | 15.4 | 7 | 26.9 | 26 | 3.8 | |
| Private sector | 23 | 54.8 | 7 | 16.7 | 4 | 9.5 | 8 | 19.1 | 42 | 6.1 | |
| Trade and entrepreneur | 25 | 49.0 | 11 | 21.6 | 5 | 9.8 | 10 | 19.6 | 51 | 7.5 | |
| Labor/miscellaneous services | 11 | 25.6 | 16 | 37.2 | 6 | 14.0 | 10 | 23.3 | 43 | 6.3 | |
| Paternal occupation (n = 650) | <0.001 *** | ||||||||||
| Government officer (including Army/Police) | 56 | 88.9 | 4 | 6.4 | 2 | 3.2 | 1 | 1.6 | 63 | 9.7 | |
| Private sector | 93 | 48.4 | 49 | 25.5 | 24 | 12.5 | 26 | 13.5 | 192 | 29.5 | |
| Trade and entrepreneur | 44 | 39.6 | 26 | 23.4 | 28 | 25.2 | 13 | 11.7 | 111 | 17.1 | |
| Labor | 62 | 31.5 | 53 | 26.9 | 25 | 12.7 | 57 | 28.9 | 197 | 30.3 | |
| Other | 23 | 26.7 | 18 | 20.9 | 22 | 25.6 | 23 | 26.7 | 86 | 13.2 | |
| Household’s monthly income (n = 508) | <0.001 *** | ||||||||||
| Low (≤Indonesian Rupiah (IDR) 1,500,000 or≤$150) | 74 | 28.3 | 71 | 27.1 | 48 | 18.3 | 69 | 26.3 | 262 | 51.6 | |
| Medium (>IDR 1500,000–2,500,000 or >$150–250) | 52 | 42.6 | 22 | 18.0 | 20 | 16.4 | 28 | 23.0 | 122 | 24.0 | |
| High (>IDR 2,500,000 or >$250) | 93 | 75.0 | 19 | 15.3 | 4 | 3.2 | 8 | 6.5 | 124 | 22.4 | |
| Paternal smoking status (n = 683) | 0.045 * | ||||||||||
| Non-smoker | 102 | 50 | 42 | 20.6 | 25 | 12.3 | 35 | 17.2 | 204 | 29.8 | |
| Smoker | 184 | 38.5 | 114 | 23.9 | 80 | 16.7 | 100 | 20.9 | 478 | 69.8 | |
| HFIAS Questions (Due to Lack of Food or Limited Resources to Obtain Food, in the Past Four Weeks Did You or Any Household Member…) | Affirmative Responses | |
|---|---|---|
| n | % | |
| Q1: Worry about food | 353 | 51.5 |
| Q2: Unable to eat preferred foods | 325 | 47.4 |
| Q3: Eat just a few kinds of foods | 249 | 36.4 |
| Q4: Eat foods they really do not want to eat | 243 | 35.5 |
| Q5: Eat small meals a day | 199 | 29.1 |
| Q6: Eat fewer meals in a day | 156 | 22.8 |
| Q7: No food of any kind in the household | 79 | 11.5 |
| Q8: Go to sleep hungry | 104 | 15.2 |
| Q9: Go a whole day and night without eating | 22 | 3.2 |
| Variable | Child Stunting | Maternal Overweight/Obesity | SCOWT | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Crude OR | 95% CI | Adjusted OR | Adjusted 95% CI | Crude OR | 95% CI | Adjusted OR | Adjusted 95% CI | Crude OR | 95% CI | Adjusted OR | Adjusted 95% CI | |
| Child Gender | ||||||||||||
| Male | Ref. | Ref. | Ref. | Ref. | ||||||||
| Female | 0.612 ** | (0.441–0.849) | 1.696 ** | (1.077–2.672) | 1.16 | (0.834–1.614) | 0.74 | (0.515–1.064) | ||||
| Child Age | 0.989 | (0.969–1.009) | 1.014 | (0.993–1.036) | 0 | - | ||||||
| Maternal Age | 0.996 | (0.963–1.031) | 1.026 | (0.99–1.063) | 1.02 | (0.982–1.06) | ||||||
| Maternal literacy | ||||||||||||
| Illiterate | Ref. | Ref. | Ref. | |||||||||
| Partially literate | 0.994 | (0.47–2.105) | 0.897 | (0.395–2.037) | 1.021 | (0.457–2.28) | ||||||
| Literate | 0.702 | (0.374–1.316) | 0.826 | (0.416–1.637) | 0.782 | (0.396–1.547) | ||||||
| Maternal education | ||||||||||||
| Low education | Ref. | Ref. | Ref. | Ref. | ||||||||
| Educated | 0.534 ** | (0.342–0.834) | 0.596 * | (0.372–0.954) | 0.814 | (0.537–1.235) | 0.565 * | (0.34–0.937) | ||||
| Highly educated | 0.58 | (0.213–1.579) | 0.735 | (0.242–2.23) | 0.717 | (0.329–1.565) | 0.849 | (0.294–2.454) | ||||
| Family type | ||||||||||||
| Nuclear family | Ref. | Ref. | Ref. | |||||||||
| Extended family | 0.976 | (0.663–1.435) | 0.901 | (0.613–1.324) | 1.291 | (0.584–1.361) | ||||||
| Number of child at home | ||||||||||||
| 1–2 children | Ref. | Ref. | Ref. | Ref. | ||||||||
| 3–4 children | 1.48 | (0.978–2.238) | 1.75 * | (1.108–2.762) | 1.75 * | (1.108–2.762) | 1.852 ** | (1.184–2.898) | ||||
| >4 children | 1.381 | (0.422–4.525) | 0.473 | (0.15–1.484) | 0.473 | (0.15–1.484) | 1.229 | (0.317–4.766) | ||||
| Number of children under 5 years in household | ||||||||||||
| 1 child | Ref. | Ref. | Ref. | |||||||||
| 2 children | 0.987 | (0.524–1.86) | 0.745 | (0.401–1.384) | 1.015 | (0.504–2.044) | ||||||
| 3 children | 0.877 | (0.054–14.25) | 0.855 | (0.052–13.963) | 1.497 | (0.091–24.713) | ||||||
| Maternal occupation | ||||||||||||
| Housewife without maid | Ref. | Ref. | Ref. | |||||||||
| Housewife with maid | 1.472 | (0.508–4.267) | 2.374 | (0.572–9.859) | 1.935 | (0.653–5.733) | ||||||
| Private sector | 0.435 | (0.158–1.198) | 1.41 | (0.536–3.705) | 0.795 | (0.286–2.212) | ||||||
| Trade and entrepreneur | 0.772 | (0.339–1.756) | 0.734 | (0.334–1.611) | 0.686 | (0.262–1.798) | ||||||
| Labor/miscellaneous | 0.719 | (0.286–1.807) | 1.245 | (0.485–3.193) | 0.817 | (0.294–2.274) | ||||||
| Paternal occupation | ||||||||||||
| Government officer | Ref. | Ref. | Ref. | |||||||||
| Private sector | 4.914 ** | (1.476–16.36) | 0.97 | (0.441–2.135) | 3.963 * | (1.05–14.961) | ||||||
| Trade and entrepreneur | 7.274 *** | (2.099–25.208) | 0.904 | (0.386–2.12) | 4.84 * | (1.23–19.05) | ||||||
| Labor | 7.196*** | (2.14–24.201) | 1.455 | (0.654–3.239) | 5.77 ** | (1.542–21.586) | ||||||
| Other | 11.117 *** | (3.157–39.153) | 0.977 | (0.395–2.414) | 7.436 ** | (1.871–29.549) | ||||||
| Paternal smoking status | ||||||||||||
| Non–smoker | Ref. | Ref. | Ref. | |||||||||
| Smoker | 0.97 | (0.677–1.389) | 1.081 | (0.756–1.546) | 0.973 | (0.652–1.451) | ||||||
| Food insecurity | ||||||||||||
| Food secure | Ref. | Ref. | Ref. | Ref. | Ref. | |||||||
| Mildly food insecure | 1.74 * | (1.043–2.903) | 1.687 | (0.985–2.889) | 1.286 | (0.76–2.176) | 2.647 *** | (1.486–4.712) | 2.798 *** | (1.54–5.083) | ||
| Moderately food insecure | 1.514 | (0.84–2.729) | 1.562 | (0.842–2.897) | 1.174 | (0.646–2.135) | 2.254 * | (1.17–4.342) | 2.53 ** | (1.286–4.98) | ||
| Severely food insecure | 2.182 ** | (1.28–3.717) | 2.005 * | (1.14–3.526) | 1.111 | (0.647–1.91) | 2.057 * | (1.112–3.804) | 2.045 * | (1.087–3.848) | ||
References
- Bhurosy, T.; Jeewon, R. Overweight and obesity epidemic in developing countries: A problem with diet, physical activity, or socioeconomic status? Sci. World J. 2014, 2014, 964236. [Google Scholar] [CrossRef] [PubMed]
- Finucane, M.M.; Stevens, G.A.; Cowan, M.; Lin, J.K.; Paciorek, C.J.; Singh, G.M.; Gutierrez, H.R.; Lu, Y.; Bahalim, A.N.; Farzadfar, F.; et al. National, regional, and global trends in body mass index since 1980: Systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet 2011, 377, 557–567. [Google Scholar] [CrossRef]
- Martorell, R.; Khan, L.K.; Hughes, M.L.; Grummer-Strawn, L.M. Obesity in women from developing countries. Eur. J. Clin. Nutr. 2000, 54, 247–252. [Google Scholar] [CrossRef] [PubMed]
- Riset Kesehatan Dasar Riskesdas 2013. Available online: http://www.depkes.go.id/resources/download/general/Hasil%20Riskesdas%202013.pdf (accessed on 23 March 2018). (In Bahasa Indonesia).
- Bredenkamp, C.; Buisman, L.R.; van de Poel, E. Persistent inequalities in child undernutrition: Evidence from 80 countries, from 1990 to today. Int. J. Epidemiol. 2014, 43, 1328–1335. [Google Scholar] [CrossRef] [PubMed]
- Restrepo-méndez, M.C.; Barros, A.J.D.; Black, R.E.; Victora, C.G. Time trends in socio-economic inequalities in stunting prevalence: Analyses of repeated national surveys. Public Health Nutr. 2015, 18, 2097–2104. [Google Scholar] [CrossRef] [PubMed][Green Version]
- United Nations Children’s Fund. Improving Child Nutrition. The Achievable Imperative for Global Progress. Available online: https://www.unicef.org/gambia/Improving_Child_Nutrition_-_the_achievable_imperative_for_global_progress.pdf (accessed on 23 March 2018).
- World Health Organization. Malnutrition. Fact Sheet Updated 2017. Available online: http://www.who.int/mediacentre/factsheets/malnutrition/en/ (accessed on 23 March 2018).
- Food and Agriculture Organization of the United Nations. The Double Burden of Malnutrition Case Studies from Six Developing Countries. 2006. Available online: http://www.fao.org/tempref/docrep/fao/009/a0442e/a0442e00.pdf (accessed on 23 March 2018).
- Sekiyama, M.; Jiang, H.W.; Gunawan, B.; Dewanti, L.; Honda, R.; Shimizu-Furuzawa, H.; Abdoellah, O.S.; Watanabe, C. Double burden of malnutrition in rural West Java: Household-level analysis for father-child and mother-child pairs and the association with dietary intake. Nutrients 2015, 7, 8376–8391. [Google Scholar] [CrossRef] [PubMed]
- Abegunde, D.O.; Mathers, C.D.; Adam, T.; Ortegon, M.; Strong, K. The burden and costs of chronic diseases in low-income and middle-income countries. Lancet 2015, 370, 1929–1939. [Google Scholar] [CrossRef]
- Delisle, H.; Agueh, V.; Fayomi, B. Partnership research on nutrition transition and chronic diseases in West Africa—Trends, outcomes and impacts. BMC Int. Health Hum. Rights 2011, 11 (Suppl. 2). [Google Scholar] [CrossRef] [PubMed]
- Gartner, A.; El Ati, J.; Traissac, P.; Bour, A.; Berger, J.; Landais, E.; El Hsaini, H.; Ben Rayana, C.; Delpeuch, F. A Double burden of overall or central adiposity and anemia or iron deficiency is prevalent but with little socioeconomic patterning among Moroccan and Tunisian urban women. J. Nutr. 2014, 144, 87–97. [Google Scholar] [CrossRef] [PubMed]
- Dieffenbach, S.; Stein, A.D. Stunted child/overweight mother pairs represent a statistical artifact, not a distinct entity. J. Nutr. 2012, 142, 771–773. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Houser, R.F.; Must, A.; de Fulladolsa, P.P.; Bermudez, O.I. Socioeconomic disparities and the familial coexistence of child stunting and maternal overweight in Guatemala. Econ. Hum. Biol. 2012, 10, 232–241. [Google Scholar] [CrossRef] [PubMed]
- Oddo, V.M.; Rah, J.H.; Semba, R.D.; Sun, K.; Akhter, N.; Sari, M.; de Pee, S.; Moench-pfanner, R.; Bloem, M.; Kraemer, K. Predictors of maternal and child double burden of malnutrition in rural Indonesia and Bangladesh. Am. J. Clin. Nutr. 2012, 95, 951–958. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, B.K.L.; Thi, H.L.; Do, V.A.N.; Thuy, N.T.; Huu, C.N.; Do, T.T.; Deurenberg, P.; Khouw, I. Double burden of undernutrition and overnutrition in Vietnam in 2011: Results of the SEANUTS Study in 0·5–11-year-old children. Br. J. Nutr. 2013, 110, S45–S56. [Google Scholar] [CrossRef] [PubMed]
- Rojroongwasinkul, N.; Kijboonchoo, K.; Wimonpeerapattana, W.; Purttiponthanee, S.; Yamborisut, U.; Boonpraderm, A.; Kunapan, P.; Thasanasuwan, W.; Khouw, I. SEANUTS: The nutritional status and dietary intakes of 0.5–12-year-old Thai children. Br. J. Nutr. 2013, 110, S36–S44. [Google Scholar] [CrossRef] [PubMed]
- Sandjaja, S.; Budiman, B.; Harahap, H.; Ernawati, F.; Soekatri, M.; Widodo, Y.; Sumedi, E.; Rustan, E.; Sofia, G.; Syarief, S.N.; et al. Food consumption and nutritional and biochemical status of 0.5–12-year-old Indonesian children: The SEANUTS Study. Br. J. Nutr. 2013, 110, S11–S20. [Google Scholar] [CrossRef] [PubMed]
- Manyanga, T.; El-Sayed, H.; Doku, D.T.; Randall, J.R. The prevalence of underweight, overweight, obesity and associated risk factors among school-going adolescents in seven African countries. BMC Public Health 2014, 14, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Rosenkranz, R.R.; Dzewaltowski, D.A. Model of the home food environment pertaining to childhood obesity. Nutr. Rev. 2008, 66, 123–140. [Google Scholar] [CrossRef] [PubMed]
- Vaezghasemi, M.; Ohman, A.; Eriksson, M.; Hakimi, M.; Weinehall, L.; Kusnanto, H.; Nawi, N. The effect of gender and social capital on the dual burden of malnutrition: A multilevel study in Indonesia. PLoS ONE 2014, 9. [Google Scholar] [CrossRef] [PubMed]
- Mahmudiono, T. Understanding the increased of child height for age index during the decline coverage of posyandu using intrinsic, extrinsic and macro-environmental factors approach: A literature review. Indones. J. Public Health 2007, 4, 1–7. [Google Scholar]
- Kota Surabaya Dalam Angka 2013. Available online: https://surabayakota.bps.go.id/publication/2013/09/13/b42cb3e2d282ce2db333e862/kota-surabaya-dalam-angka-2013.html (accessed on 7 February 2018). (In Bahasa Indonesia).
- Mei, Z.; Grummer-strawn, L.M. Standard deviation of anthropometric z-scores as a data quality assessment tool using the 2006 WHO growth standards: A cross country analysis. Bull. World Health Organ. 2007, 85, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Coates, J.; Swindale, A.; Bilinsky, P. Household Food Insecurity Access Scale (HFIAS) for Measurement of Food Access: Indicator Guide VERSION 3. 2007. Available online: https://www.fantaproject.org/sites/default/files/resources/HFIAS_ENG_v3_Aug07.pdf (accessed on 23 March 2018).
- WHO Child Growth Standards: Methods and Development. Available online: http://www.who.int/childgrowth/standards/Technical_report.pdf (accessed on 23 March 2018).
- Vaske, J.J. Survey Research and Analysis: Applications in Parks, Recreation and Human Dimensions; Venture Publishing: State College, PA, USA, 2008. [Google Scholar]
- O’Brien, R.M. A Caution regarding rules of thumb for variance inflation factors. Qual. Quant. 2007, 41, 673–690. [Google Scholar] [CrossRef]
- Liao, D.; Valliant, R. Variance inflation factors in the analysis of complex survey data. Surv. Methodol. 2012, 38, 53–62. [Google Scholar]
- Allison, P. When Can You Safely Ignore Multicollinearity? Statistical Horizons. Available online: https://statisticalhorizons.com/multicollinearity (accessed on 5 December 2015).
- Kimani-Murage, E.W.; Schofield, L.; Wekesah, F.; Mohamed, S.; Mberu, B.; Ettarh, R.; Egondi, T.; Kyobutungi, C.; Ezeh, A. Vulnerability to food insecurity in urban slums: Experiences from Nairobi, Kenya. J. Urban Health 2014, 91, 1098–1113. [Google Scholar] [CrossRef] [PubMed]
- Kimani-Murage, E.W.; Muthuri, S.K.; Oti, S.O.; Mutua, M.K.; van de Vijver, S.; Kyobutungi, C. Evidence of a double burden of malnutrition in urban poor settings in Nairobi, Kenya. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- Uauy, R.; Kurpad, A.; Tamo-Debrah, K.; Otoo, G.E.; Aaron, G.A.; Toride, Y.; Ghosh, S. Role of protein and amino acids in infant and young child nutrition: Protein and amino acid needs and relationship with child growth. J. Nutr. Sci. Vitaminol. 2015, 61, S192–S194. [Google Scholar] [CrossRef] [PubMed]
- Felisbino-Mendes, M.S.; Villamor, E.; Velasquez-Melendez, G. Association of maternal and child nutritional status in Brazil: A population based cross-sectional study. PLoS ONE 2014, 9. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, H.S.; Moura, F.A.; Cabral Júnior, C.R.; Florêncio, T.M.M.T.; Vieira, R.C.; de Assunção, M.L. Short stature of mothers from an area endemic for undernutrition is associated with obesity, hypertension and stunted children: A population-based study in the semi-arid region of Alagoas, Northeast Brazil. Br. J. Nutr. 2009, 101, 1239–1245. [Google Scholar] [CrossRef] [PubMed]
- Varela-Silva, M.I.; Azcorra, H.; Dickinson, F.; Bogin, B.; Frisancho, A.R. Influence of maternal stature, pregnancy age, and infant birth weight on growth during childhood in Yucatan, Mexico: A test of the intergenerational effects hypothesis. Am. J. Hum. Biol. 2009, 21, 657–663. [Google Scholar] [CrossRef] [PubMed]
- Widodo, Y. Cakupan Pemberian Asi Eksklusif: Akurasi Dan Interpretasi Data Survei Dan Laporan Program. Gizi Indones. 2011, 34, 101–108, (In Bahasa Indonesia). [Google Scholar]
- López-Olmedo, N.; Hernández-Cordero, S.; Neufeld, L.M.; García-Guerra, A.; Mejía-Rodríguez, F.; Méndez Gómez-Humarán, I. The associations of maternal weight change with breastfeeding, diet and physical activity during the postpartum period. Matern. Child Health J. 2016, 20, 270–280. [Google Scholar] [CrossRef] [PubMed]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mahmudiono, T.; Nindya, T.S.; Andrias, D.R.; Megatsari, H.; Rosenkranz, R.R. Household Food Insecurity as a Predictor of Stunted Children and Overweight/Obese Mothers (SCOWT) in Urban Indonesia. Nutrients 2018, 10, 535. https://doi.org/10.3390/nu10050535
Mahmudiono T, Nindya TS, Andrias DR, Megatsari H, Rosenkranz RR. Household Food Insecurity as a Predictor of Stunted Children and Overweight/Obese Mothers (SCOWT) in Urban Indonesia. Nutrients. 2018; 10(5):535. https://doi.org/10.3390/nu10050535
Chicago/Turabian StyleMahmudiono, Trias, Triska Susila Nindya, Dini Ririn Andrias, Hario Megatsari, and Richard R. Rosenkranz. 2018. "Household Food Insecurity as a Predictor of Stunted Children and Overweight/Obese Mothers (SCOWT) in Urban Indonesia" Nutrients 10, no. 5: 535. https://doi.org/10.3390/nu10050535
APA StyleMahmudiono, T., Nindya, T. S., Andrias, D. R., Megatsari, H., & Rosenkranz, R. R. (2018). Household Food Insecurity as a Predictor of Stunted Children and Overweight/Obese Mothers (SCOWT) in Urban Indonesia. Nutrients, 10(5), 535. https://doi.org/10.3390/nu10050535







