Chinese Medicines in the Treatment of Prostate Cancer: From Formulas to Extracts and Compounds
Abstract
:1. Introduction
2. Chinese Medicine Formulas in the Treatment of Prostate Cancer
3. Chinese Medicine Extracts Inhibit Prostate Cancer
4. Compounds Isolated from Chinese Medicines Inhibit Prostate Cancer
4.1. Compounds Inhibiting the Growth of Prostate Cancer Cells
4.2. Compounds Inhibiting the Proliferation of Prostate Cancer Cells
4.3. Compounds Inhibiting Metastasis of Prostate Cancer Cells
4.4. Summary
5. Perspectives and Outlook
6. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Funding
References
- Attard, G.; Parker, C.; Eeles, R.A.; Eeles, R.A.; Schröder, F.; Tomlins, S.A.; Tannock, I.; Drake, C.G.; de Bono, J.S. Prostate cancer. Lancet 2015, 387, 70–82. [Google Scholar] [CrossRef]
- Ren, S.C.; Chen, R.; Sun, Y.H. Prostate cancer research in China. Asian J. Androl. 2013, 15, 350–353. [Google Scholar] [CrossRef] [PubMed]
- Ling, C.Q.; Yue, X.Q.; Ling, C. Three advantages of using traditional Chinese medicines to prevent and treat tumor. J. Integr. Med. 2014, 12, 331–335. [Google Scholar] [CrossRef]
- Lin, L.Z.; Zhou, D.H.; Zheng, X.T. Effect of traditional Chinese medicines in improving quality of life of patients with non-small cell lung cancer in late stage. Chin. J. Integr. Tradit. West. Med. 2006, 26, 389–393. [Google Scholar]
- Kim, J.; Park, E.J. Cytotoxic anticancer candidates from natural resources. Curr. Med. Chem. Anticancer Agents 2002, 2, 485–537. [Google Scholar] [CrossRef] [PubMed]
- Soignet, S.L.; Frankel, S.R.; Douer, D.; Tallman, M.S.; Kantarjian, H.; Calleja, E.; Stone, R.M.; Kalaycio, M.; Scheinberg, D.A.; Steinherz, P.; et al. United States multicenter study of arsenic trioxide in relapsed acute promyelocytic leukemia. J. Clin. Oncol. 2001, 19, 3852–3860. [Google Scholar] [CrossRef] [PubMed]
- Ghavamzadeh, A.; Alimoghaddam, K.; Rostami, S.; Ghaffari, S.H.; Jahani, M.; Iravani, M.; Mousavi, S.A.; Bahar, B.; Jalili, M. Phase II study of single-agent arsenic trioxide for the front-line therapy of acute promyelocytic leukemia. J. Clin. Oncol. 2011, 29, 2753–2757. [Google Scholar] [CrossRef] [PubMed]
- Jiang, C.M.; Pang, M.R.; Gong, L.Y. Clinical observation on effect of chemotherapy combined with Chinese medicines in treating advanced tumor patients and on immunologic parameters. Chin. J. Integr. Tradit. West. Med. 2001, 21, 885–887. [Google Scholar]
- Yan, G.Y.; Xu, Z.Y.; Deng, H.B.; Wan, Z.Y.; Zhang, L.; Zhu, J.Y. Effects of chemotherapy combined with Chinese herbal medicine Kangliu Zengxiao decoction on tumor markers of patients with advanced non-small-cell lung cancer: A randomized, controlled trial. J. Chin. Integr. Med. 2011, 9, 525–530. [Google Scholar] [CrossRef]
- Tang, Z.Y. Combination of traditional Chinese medicines and western medicine in the treatment of liver cancer. J. Clin. Hepatol. 2011, 27, 449–450. [Google Scholar]
- Shen, F.L.; Jin, J.G.; Cao, F.J. Clinical observation of combination of Chinese medicines combined with chemoradiotherapy in treatment of patients with stage-III non-small-cell lung cancer. Med. J. West China 2014, 26, 445–449. [Google Scholar]
- Kosty, M.P. PC-SPES: Hope or hype? J. Clin. Oncol. 2004, 22, 3657–3659. [Google Scholar] [CrossRef] [PubMed]
- DiPaola, R.S.; Zhang, H.; Lambert, G.H.; Meeker, R.; Licitra, E.; Rafi, M.M.; Zhu, B.T.; Spaulding, H.; Goodin, S.; Toledano, M.B.; et al. Clinical and biologic activity of an estrogenic herbal combination (PC-SPES) in prostate cancer. N. Engl. J. Med. 1998, 339, 785–791. [Google Scholar] [CrossRef] [PubMed]
- Halicka, H.; Ardelt, B.; Juan, G.; Mittelman, A.; Chen, S.; Traganos, F.; Darzynkiewicz, Z. Apoptosis and cell cycle effects induced by extracts of the Chinese herbal preparation PC SPES. Int. J. Oncol. 1997, 11, 437–448. [Google Scholar] [CrossRef] [PubMed]
- Tiwari, R.K.; Geliebter, J.; Garikapaty, V.P.; Yedavelli, S.P.; Chen, S.; Mittelman, A. Anti-tumor effects of PC-SPES, an herbal formulation in prostate cancer. Int. J. Oncol. 1999, 14, 713–719. [Google Scholar] [CrossRef] [PubMed]
- De la Taille, A.; Buttyan, R.; Hayek, O.; Bagiella, E.; Shabsigh, A.; Burchardt, M.; Burchardt, T.; Chopin, D.K.; Katz, A.E. Herbal therapy PC-SPES: In vitro effects and evaluation of its efficacy in 69 patients with prostate cancer. J. Urol. 2000, 164, 1229–1234. [Google Scholar] [CrossRef]
- Kubota, T.; Hisatake, J.; Hisatake, Y.; Said, J.W.; Chen, S.S.; Holden, S.; Taguchi, H.; Koeffler, H.P. PC-SPES: A unique inhibitor of proliferation of prostate cancer cells in vitro and in vivo. Prostate 2000, 42, 163–171. [Google Scholar] [CrossRef]
- Lock, M.; Loblaw, D.A.; Choo, R.; Imrie, K. Disseminated intravascular coagulation and PC-SPES: A case report and literature review. Can. J. Urol. 2001, 8, 1326–1329. [Google Scholar] [PubMed]
- Weinrobe, M.C.; Montgomery, B. Acquired bleeding diathesis in a patient taking PC-SPES. N. Engl. J. Med. 2001, 345, 1213–1214. [Google Scholar] [CrossRef] [PubMed]
- Sovak, M.; Seligson, A.L.; Konas, M.; Hajduch, M.; Dolezal, M.; Machala, M.; Nagourney, R. Herbal composition PC-SPES for management of prostate cancer: Identification of active principles. J. Natl. Cancer Inst. 2002, 94, 1275–1281. [Google Scholar] [CrossRef] [PubMed]
- Olaku, O.; White, J.D. Herbal therapy use by cancer patients: A literature review on case reports. Eur. J. Cancer 2011, 47, 508–514. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.H.; Chen, K.K.; Chiu, J.H. Prevalence, patterns, and costs of Chinese medicines use among prostate cancer patients: A population-based study in Taiwan. Integr. Cancer Ther. 2010, 9, 16–23. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.H.; Chen, K.K.; Chiu, J.H. Trends in Chinese medicines use among prostate cancer patients under national health insurance in Taiwan: 1996–2008. Integr. Cancer Ther. 2011, 10, 317–327. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.H.; Chen, K.K.; Chiu, J.H. Use of Chinese medicines among prostate cancer patients in Taiwan: A retrospective longitudinal cohort study. Int. J. Urol. 2011, 18, 383–386. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.H.; Chen, K.K.; Chiu, J.H. Coprescription of Chinese Herbal Medicine and Western Medications among Prostate Cancer Patients: A Population-Based Study in Taiwan. Evid. Based Complement. Altern. Med. 2012, 2012, 147015. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.M.; Lin, P.H.; Hsu, R.J.; Chang, Y.H.; Cheng, K.C.; Pang, S.T.; Lin, S.K. Complementary traditional Chinese medicines therapy improves survival in patients with metastatic prostate cancer. Medicine 2016, 95, 1–7. [Google Scholar]
- Unlu, A.; Nayir, E.; Kirca, O.; Ozdogan, M. Ganoderma Lucidum (Reishi Mushroom) and cancer. J. BUON 2016, 21, 792–798. [Google Scholar] [PubMed]
- Sliva, D.; Labarrere, C.; Slivova, V.; Sedlak, M.; Lloyd, F.P., Jr.; Ho, N.W. Ganoderma lucidum suppresses motility of highly invasive breast and prostate cancer cells. Biochem. Biophys. Res. Commun. 2002, 298, 603–612. [Google Scholar] [CrossRef]
- Jiang, J.; Slivova, V.; Valachovicova, T.; Sedlak, M.; Lloyd, F.P., Jr.; Ho, N.W. Ganoderma lucidum inhibits proliferation and induces apoptosis in human prostate cancer cells PC-3. Int. J. Oncol. 2004, 24, 1093–1099. [Google Scholar] [CrossRef] [PubMed]
- Stanley, G.; Harvey, K.; Slivova, V.; Jiang, J.; Sliva, D. Ganoderma lucidum suppresses angiogenesis through the inhibition of secretion of VEGF and TGF-β1 from prostate cancer cells. Biochem. Biophys. Res. Commun. 2005, 330, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Guo, H.; Luo, H.; Yuan, H.; Xia, Y.; Shu, P.; Huang, X.; Lu, Y.; Liu, X.; Keller, E.T.; Sun, D.; et al. Litchi seed extracts diminish prostate cancer progression via induction of apoptosis and attenuation of EMT through Akt/GSK-3β signaling. Sci. Rep. 2017, 7, 41656. [Google Scholar] [CrossRef] [PubMed]
- Sunkara, Y.; Robinson, A.; Suresh, B.K.; Naidu, V.G.M.; Vishnuvardhan, M.V.P.S.; Suresh, B.K.; Ramakrishna, S.; Madhavendra, S.S.; Rao, J.M. Anti-inflammatory and cytotoxic activity of chloroform extract of roots of Saussurea lappa Clarke. J. Pharm. Res. 2010, 3, 1775–1778. [Google Scholar]
- Kretschmer, N.; Blunder, M.; Kunert, O.; Kahl, S.; Efferth, T.; Boechzelt, H.; Hao, X.J.; Bauer, R. Activity-Guided Isolation of AntiTumor Compounds from Saussurea lappa Clarke. Sci. Pharm. 2009, 77, 246. [Google Scholar] [CrossRef]
- Kim, E.J.; Hong, J.E.; Lim, S.S.; Kwon, G.T.; Kim, J.; Kim, J.S.; Lee, K.W.; Park, J.H. The hexane extract of Saussurea lappa and its active principle, dehydrocostus lactone, inhibit prostate cancer cell migration. J. Med. Food 2012, 15, 24–32. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.Y.; Wu, J.; Ye, F.; Xue, L.; Jiang, S.; Yi, J.; Zhang, W.; Wei, H.; Sung, M.; Wang, W.; et al. Inhibition of cancer cell proliferation and prostaglandin E2 synthesis by Scutellaria baicalensis. Cancer Res. 2003, 63, 4037–4043. [Google Scholar] [PubMed]
- Kim, E.H.; Shim, B.; Kang, S.; Jeong, G.; Lee, J.S.; Yu, Y.B.; Chun, M. Anti-inflammatory effects of Scutellaria baicalensis extract via suppression of immune modulators and MAP kinase signaling molecules. J. Ethnopharmacol. 2009, 126, 320–331. [Google Scholar] [CrossRef] [PubMed]
- Yoon, S.B.; Lee, Y.J.; Park, S.K.; Kim, H.C.; Bae, H.; Kim, H.M.; Ko, S.G.; Choi, H.Y.; Oh, M.S.; Park, W. Anti-inflammatory effects of Scutellaria baicalensis water extract on LPS-activated RAW 264.7 macrophages. J. Ethnopharmacol. 2009, 125, 286–290. [Google Scholar] [CrossRef] [PubMed]
- Ye, F.; Jiang, S.; Volshonok, H.; Wu, J.; Zhang, D.Y. Molecular mechanism of anti-prostate cancer activity of Scutellaria baicalensis extract. Nutr. Cancer 2007, 57, 100–110. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Ren, B.; Zhang, J.; Liu, L.; Liu, J.; Jiang, G.; Li, M.; Ding, Y.; Li, W. Anti-tumor effect of Scutellaria barbata D. Don extracts on ovarian cancer and its phytochemicals characterisation. J. Ethnopharmacol. 2017, 206, 184–192. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Yang, Y.; Tang, S.; Tang, H.; Yang, G.; Xu, Q.; Wu, J. Anti-tumor effect of polysaccharides from Scutellaria barbata D. Don on the 95-D xenograft model via inhibition of the C-met pathway. J. Pharmacol. Sci. 2014, 125, 255–263. [Google Scholar] [CrossRef] [PubMed]
- Yin, X.; Zhou, J.; Jie, C.; Xing, D.; Zhang, Y. Anticancer activity and mechanism of Scutellaria barbata extract on human lung cancer cell line A549. Life Sci. 2004, 75, 2233–2244. [Google Scholar] [CrossRef] [PubMed]
- Wong, B.Y.; Nguyen, D.L.; Lin, T.; Wong, H.H.; Cavalcante, A.; Greenberg, N.M.; Hausted, R.P.; Zheng, J. Chinese medicinal herb Scutellaria barbata modulates apoptosis and cell survival in murine and human prostate cancer cells and tumor development in TRAMP mice. Eur. J. Cancer Prev. 2009, 18, 331–341. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Ravula, R.; Shi, L.; Song, Y.; Yeung, S.; Liu, M.; Lau, B.; Hao, J.; Wang, J.; Lam, C.W.; et al. Overcoming chemoresistance in prostate cancer with Chinese medicines Tripterygium wilfordii via multiple mechanisms. Oncotarget 2016, 7, 61246–61261. [Google Scholar] [CrossRef] [PubMed]
- Sureshkumar, S.; Sivakumar, T.; Chandrasekar, M.J.N.; Suresh, B. Investigating the Anti-Inflammatory and Analgesic Activity of Leaves of Wedelia chinensis (Osbeck) Merr. In Standard Experimental Animal models. Iran. J. Pharm. Res. 2006, 5, 123–129. [Google Scholar]
- Manjamalai, A.; Shukoor, S.A.; Haridas, A.; Berlin, G. Evaluation of antifungal and anti-inflammatory effect on methanolic extract of Wedelia chinensis leaves. Int. J. Pharm. Biomed. Res. 2011, 2, 446–454. [Google Scholar]
- Manjamalai, A.; Jiflin, G.J.; Grace, V.M.B. Study on the effect of essential oil of Wedelia chinensis (Osbeck) against microbes and inflammation. Asian J. Pharm. Clin. Res. 2012, 5, 155–164. [Google Scholar]
- Tsai, C.H.; Lin, F.M.; Yang, Y.C.; Lee, M.T.; Cha, T.L.; Wu, G.J.; Hsieh, S.C.; Hsiao, P.W. Herbal extract of Wedelia chinensis attenuates androgen receptor activity and orthotopic growth of prostate cancer in nude mice. Clin. Cancer Res. 2009, 15, 5435–5444. [Google Scholar] [CrossRef] [PubMed]
- Chun, J.Y.; Tummala, R.; Nadiminty, N.; Lou, W.; Liu, C.; Yang, J.; Evans, C.P.; Zhou, Q.; Gao, A.C. Andrographolide, an herbal medicine, inhibits interleukin-6 expression and suppresses prostate cancer cell growth. Genes Cancer 2010, 1, 868–876. [Google Scholar] [CrossRef] [PubMed]
- Kan, S.F.; Huang, W.J.; Lin, L.C.; Wang, P.S. Inhibitory effects of evodiamine on the growth of human prostate cancer cell line LNCaP. Int. J. Cancer 2004, 110, 641–651. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Lao, Y.; Zhang, H.; Wang, X.; Tan, H.; Lin, Z.; Xu, H. The natural compound Guttiferone F sensitizes prostate cancer to starvation induced apoptosis via calcium and JNK elevation. BMC Cancer 2015, 15, 254. [Google Scholar] [CrossRef] [PubMed]
- Hahm, E.R.; Singh, S.V. Honokiol causes G0-G1 phase cell cycle arrest in human prostate cancer cells in association with suppression of retinoblastoma protein level/phosphorylation and inhibition of E2F1 transcriptional activity. Mol. Cancer Ther. 2007, 6, 2686–2695. [Google Scholar] [CrossRef] [PubMed]
- Shigemura, K.; Arbiser, J.L.; Sun, S.Y.; Zayzafoon, M.; Johnstone, P.A.; Fujisawa, M.; Gotoh, A.; Weksler, B.; Zhau, H.E.; Chung, L.W. Honokiol, a natural plant product, inhibits the bone metastatic growth of human prostate cancer cells. Cancer 2007, 109, 1279–1289. [Google Scholar] [CrossRef] [PubMed]
- Hahm, E.R.; Sakao, K.; Singh, S.V. Honokiol activates reactive oxygen species-mediated cytoprotective autophagy in human prostate cancer cells. Prostate 2014, 74, 1209–1221. [Google Scholar] [CrossRef] [PubMed]
- Fang, Y.; Yu, Y.; Hou, Q.; Zheng, X.; Zhang, M.; Zhang, D.; Li, J.; Wu, X.R.; Huang, C. The Chinese Herb Isolate Isorhapontigenin Induces Apoptosis in Human Cancer Cells by Down-regulating Overexpression of Antiapoptotic Protein XIAP. J. Biol. Chem. 2012, 287, 35234–35243. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Marín, M.I.; Guerrero, R.F.; García-Parrilla, M.C.; Puertas, B.; Richard, T.; Rodriguez-Werner, M.A.; Winterhalter, P.; Monti, J.P.; Cantos-Villar, E. Isorhapontigenin: A novel bioactive stilbene from wine grapes. Food Chem. 2012, 135, 1353–1359. [Google Scholar] [CrossRef] [PubMed]
- Fang, Y.N.; Liu, G.T. Effect of isorhapontigenin on respiratory burst of rat neutrophils. Phytomedicine 2002, 9, 734–738. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Zhu, Q.; Wu, Z.; Yin, Y.; Kang, D.; Lu, S.; Liu, P. Isorhapontigenin induced cell growth inhibition and apoptosis by targeting EGFR-related pathways in prostate cancer. J. Cell. Physiol. 2018, 233, 1104–1119. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.Z.; Huang, J.; Gong, Z.; Tian, X.Q. A Novel Norlignan and a Novel Phenylpropanoid from Peperomia tetraphylla. Helv. Chim. Acta 2010, 90, 2222–2226. [Google Scholar] [CrossRef]
- Li, Y.; He, N.; Zhai, C. Peperotetraphin inhibits the proliferation of human prostate cancer cells via induction of cell cycle arrest and apoptosis. Med. Oncol. 2015, 32, 468. [Google Scholar] [CrossRef] [PubMed]
- Boots, A.W. Health effects of quercetin: From mechanism to nutraceutical. Eur. J. Pharmacol. 2006, 585, 325–337. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.H.; Szczepanski, M.; Yong, J.L. Role of Bax in quercetin-induced apoptosis in human prostate cancer cells. Biochem. Pharm. 2008, 75, 2345–2355. [Google Scholar] [CrossRef] [PubMed]
- Jung, Y.H.; Heo, J.; Lee, Y.J.; Kwon, T.K.; Kim, Y.H. Quercetin enhances TRAIL-induced apoptosis in prostate cancer cells via increased protein stability of death receptor 5. Life Sci. 2010, 86, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Aalinkeel, R.; Bindukumar, B.; Reynolds, J.L.; Sykes, D.E.; Mahajan, S.D.; Chadha, K.C.; Schwartz, S.A. The Dietary Bioflavonoid, Quercetin, Selectively Induces Apoptosis of Prostate Cancer Cells by Down-Regulating the Expression of Heat Shock Protein 90. Prostate 2008, 68, 1773–1789. [Google Scholar] [CrossRef] [PubMed]
- Vijayababu, M.R.; Kanagaraj, P.; Arunkumar, A.; Ilangovan, R.; Dharmarajan, A.; Arunakaran, J. Quercetin induces p53-independent apoptosis in human prostate cancer cells by modulating Bcl-2-related proteins: A possible mediation by IGFBP-3. Oncol. Res. 2006, 16, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Song, L.; Wang, H.; Xing, N. Quercetin synergizes with 2-methoxyestradiol inhibiting cell growth and inducing apoptosis in human prostate cancer cells. Oncol. Rep. 2013, 30, 357–363. [Google Scholar] [CrossRef] [PubMed]
- Liu, K.C.; Yen, C.Y.; Wu, R.S.; Yang, J.S.; Lu, H.F.; Lu, K.W.; Lo, C.; Chen, H.Y.; Tang, N.Y.; Wu, C.C.; et al. The roles of endoplasmic reticulum stress and mitochondrial apoptotic signaling pathway in quercetin-mediated cell death of human prostate cancer PC-3 cells. Environ. Toxicol. 2014, 29, 428–439. [Google Scholar] [CrossRef] [PubMed]
- Xu, W.; Debeb, B.G.; Lacerda, L.; Li, J.; Woodward, W.A. Tetrandrine, a Compound Common in Chinese Traditional Medicine, Preferentially Kills Breast Cancer Tumor Initiating Cells (TICs) In Vitro. Cancers 2011, 3, 2274–2285. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Kou, B.; Ma, Z.K.; Tang, X.S.; Lv, C.; Ye, M.; Chen, J.Q.; Li, L.; Wang, X.Y.; He, D.L. Tetrandrine suppresses proliferation, induces apoptosis, and inhibits migration and invasion in human prostate cancer cells. Asian J. Androl. 2015, 17, 850–853. [Google Scholar] [PubMed]
- Chen, B.J. Triptolide, a novel immunosuppressive and anti-inflammatory agent purified from a Chinese herb Tripterygium wilfordii Hook F. Leuk. Lymphoma 2001, 42, 253–265. [Google Scholar] [CrossRef] [PubMed]
- Fulda, S. Tumor-necrosis-factor-related apoptosis-inducing ligand (TRAIL). Adv. Exp. Med. Biol. 2014, 818, 167–180. [Google Scholar] [PubMed]
- Thakkar, H. Constitutively active Akt is an important regulator of TRAIL sensitivity in prostate cancer. Oncogene 2001, 20, 6073–6083. [Google Scholar]
- Xiaowen, H.; Yi, S. Triptolide sensitizes TRAIL-induced apoptosis in prostate cancer cells via p53-mediated DR5 up-regulation. Mol. Boil. Rep. 2012, 39, 8763–8770. [Google Scholar] [CrossRef] [PubMed]
- Meng, F.M.; Yang, J.B.; Yang, C.H.; Jiang, Y.; Zhou, Y.F.; Yu, B.; Yang, H. Vitexicarpin induces apoptosis in human prostate carcinoma PC-3 cells through G2/M phase arrest. Asian Pac. J. Cancer Prev. 2012, 13, 6369–6374. [Google Scholar] [CrossRef] [PubMed]
- Cao, H.; Feng, Y.; Chen, L. Repression of MicroRNA-372 by Arsenic Sulphide Inhibits Prostate Cancer Cell Proliferation and Migration through Regulation of large tumour suppressor kinase 2. Basic Clin. Pharmacol. Toxicol. 2017, 120, 256–263. [Google Scholar] [CrossRef] [PubMed]
- Chan, F.L.; Choi, H.L.; Chen, Z.Y.; Chan, P.S.; Huang, Y. Induction of apoptosis in prostate cancer cell lines by a flavonoid, baicalin. Cancer Lett. 2000, 160, 219–228. [Google Scholar] [CrossRef]
- Pang, X.; Yi, Z.; Zhang, J.; Lu, B.; Sung, B.; Qu, W.; Aggarwal, B.B.; Liu, M. Celastrol suppresses angiogenesis-mediated tumor growth through inhibition of AKT/mammalian target of rapamycin pathway. Cancer Res. 2010, 70, 1951–1959. [Google Scholar] [CrossRef] [PubMed]
- Chiang, K.C.; Tsui, K.H.; Chung, L.C.; Yeh, C.; Chen, W.; Chang, P.; Juang, H. Celastrol blocks interleukin-6 gene expression via downregulation of NF-κB in prostate carcinoma cells. PLoS ONE 2014, 9, e93151. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.; Chen, D.; Cui, Q.C.; Yuan, X.; Dou, Q.P. Celastrol, a triterpene extracted from the Chinese “Thunder of God Vine”, is a potent proteasome inhibitor and suppresses human prostate cancer growth in nude mice. Cancer Res 2006, 66, 4758–4765. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.S.; Cao, J.Q.; Zhao, C.; Wang, X.D.; Wu, X.J.; Zhao, Y.Q. Novel dammarane-type triterpenes isolated from hydrolyzate of total Gynostemma pentaphyllum saponins. Bioorg. Med. Chem. Lett. 2015, 25, 3095–3099. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.S.; Zhao, C.; Tang, W.Z.; Wu, X.J.; Zhao, Y.Q. Gypensapogenin H, a novel dammarane-type triterpene induces cell cycle arrest and apoptosis on prostate cancer cells. Steroids 2015, 104, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.H.; Yan, G.H. Anti-allergic effects of scoparone on mast cell-mediated allergy model. Phytomedicine 2009, 16, 1089–1094. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.-K.; Kim, J.-Y.; Kim, H.-J.; Park, K.-G.; Harris, R.A.; Cho, W.J.; Lee, J.-T.; Lee, I.-K. Scoparone exerts anti-tumor activity against DU145 prostate cancer cells via inhibition of STAT3 activity. PLoS ONE 2013, 8, e80391. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Zhang, P.Y.; Guo, J.; Yang, D.; Wang, W.J.; Zheng, M.H.; Ma, Y.C. Effects of triptolide on prostate carcinoma in mouse RM-1 cells. Natl. J. Androl. 2007, 13, 237–241. [Google Scholar]
- Cher, M.L. Mechanisms governing bone metastasis in prostate cancer. Curr. Opin. Urol. 2001, 11, 483–488. [Google Scholar] [CrossRef] [PubMed]
- Msaouel, P.; Pissimissis, N.; Halapas, A.; Koutsilieris, M. Mechanisms of bone metastasis in prostate cancer: Clinical implications. Best practice & research. Clin. Endocrinol. Metab. 2008, 22, 341–355. [Google Scholar]
- Kuchta, K.; Xiang, Y.; Huang, S.; Tang, Y.; Peng, X.; Wang, X.; Zhu, Y.; Li, J.; Xu, J.; Lin, Z.; et al. Celastrol, an active constituent of the TCM plant Tripterygium wilfordii Hook.f., inhibits prostate cancer bone metastasis. Prostate Cancer Prostatic Dis. 2017, 20, 156–164. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Zhang, L.Y.; Chen, W.W.; Kong, F.; Zhang, P.J.; Hu, X.Y.; Zhang, J.Y.; Cui, F.A. Inhibition of the expression of prostate specific antigen by curcumin. Acta Pharm. Sin. 2005, 40, 800–803. [Google Scholar]
- Cao, H.; Yu, H.; Feng, Y.; Chen, L.; Liang, F. Curcumin inhibits prostate cancer by targeting PGK1 in the FOXD3/miR-143 axis. Cancer Chemother. Pharmacol. 2017, 79, 985–994. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Wang, C.; Zhang, Z.; Chen, X.; Jia, Y.; Wang, B.; Kong, T. Curcumin inhibits the survival and metastasis of prostate cancer cells via the Notch-1 signaling pathway. APMIS 2017, 125, 134–140. [Google Scholar] [CrossRef] [PubMed]
- Hu, E.; Wang, D.; Chen, J.; Tao, X. Novel cyclotides from Hedyotis diffusa induce apoptosis and inhibit proliferation and migration of prostate cancer cells. Int. J. Clin. Exp. Med. 2015, 8, 4059–4065. [Google Scholar] [PubMed]
- Lin, T.H.; Tan, T.W.; Tsai, T.H.; Chen, C.C.; Hsieh, T.F.; Lee, S.S.; Liu, H.H.; Chen, W.C.; Tang, C.H. D-pinitol inhibits prostate cancer metastasis through inhibition of αVβ3 integrin by modulating FAK, c-Src and NF-kappaB pathways. Int. J. Mol. Sci. 2013, 14, 9790–9802. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.Y.; Yang, Y.H.; Lin, Y.Y.; Kuan, F.C.; Lin, Y.S.; Lin, W.Y.; Tsai, M.Y.; Yang, J.J.; Cheng, Y.C.; Shu, L.H.; et al. Anti-cancer effect of danshen and dihydroisotanshinone I on prostate cancer: Targeting the crosstalk between macrophages and cancer cells via inhibition of the STAT3/CCL2 signaling pathway. Oncotarget 2017, 8, 40246–40263. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Zheng, L.; Liu, J.; Zhou, Z.; Cao, X.; Lv, X.; Chen, F. Shikonin inhibits prostate cancer cells metastasis by reducing matrix metalloproteinase-2/-9 expression via AKT/mTOR and ROS/ERK1/2 pathways. Int. Immunopharm. 2014, 21, 447–455. [Google Scholar] [CrossRef] [PubMed]
| Scientific Name | Chinese Name | Plant Organs | Extraction Solvents |
|---|---|---|---|
| Ganoderma lucidum (Leyss. ex Fr.) Karst. | Ling Zhi | Spores and unpurified fruiting bodies | No solvent |
| Litchi chinensis Sonn. | Li Zhi | Seed | n-butyl alcohol |
| Saussurea lappa Clarke | Guang Mu Xiang | Root | n-Hexane |
| Scutellaria baicalensis Georgi | Huang Qin | Root | Water |
| Scutellaria barbata D. Don | Ban Zhi Lian | Whole plant | Water |
| Tripterygium wilfordii Hook F. | Lei Gong Teng | Root | EtOH |
| Wedelia chinensis (Osbeck) Merr. | Peng Qi Ju | Whole plant | EtOH |
| General Name | Chemical Structure | Compound Classification | Inhibit prostate Cancer | ||
|---|---|---|---|---|---|
| Gro. | Pro. | Met. | |||
| Andrographolide | 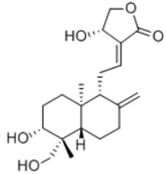 | Diterpenoid lactone | + | ||
| Evodiamine | 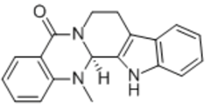 | Alkaloid | + | ||
| Guttiferone F | 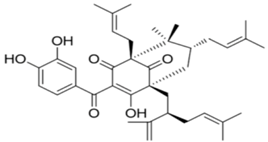 | Prenylated benzophenone derivative | + | ||
| Honokiol | 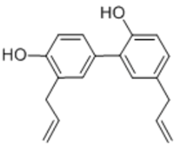 | Aromatic phenol | + | ||
| Isorhapontigenin | 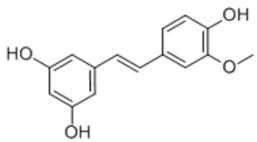 | phytopolyphenol | + | ||
| Peperotetraphin | 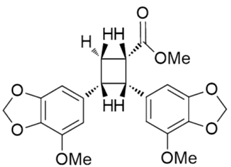 | Norlignan | + | ||
| Quercetin |  | Flavone | + | ||
| Tetrandrine | 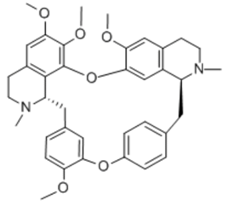 | Alkaloid | + | + | |
| Triptolide |  | Heterocycle | + | + | |
| Vitexicarpin | 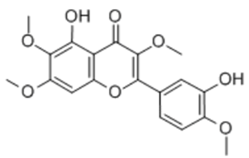 | Flavone | + | ||
| Arsenic sulphide | 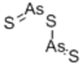 | Metal chalcogenide | + | ||
| Baicalin | 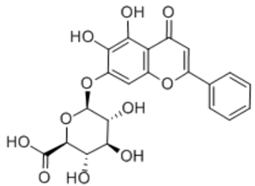 | Flavone glycoside | + | ||
| Celastrol | 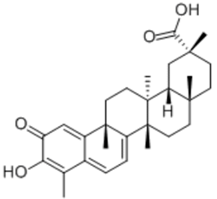 | Pentacyclic triterpenoid | + | + | |
| Gypensapogenin H | 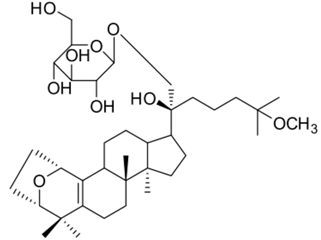 | Triterpene | + | ||
| Scoparone | 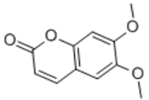 | coumarin | + | ||
| Curcumin | 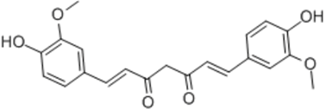 | Diphenyl heptyl hydrocarbon | + | ||
| dihydroisotanshinone I | 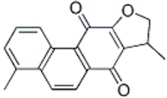 | Phenanthraquinone | + | ||
| D-pinitol | 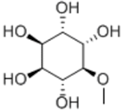 | Alcohol | + | ||
| Shikonin |  | Anthraquinone | + | ||
| Cell Type | Androgen-Dependent Human Prostate Cancer Cell Lines | Androgen-Independent Human Prostate Cancer Cell Lines | HPV-18-Transfected Human Prostate Cancer Cell Line | Mouse Transgenic Prostate Cancer Cell Lines | Mouse Prostate Cancer Cell Lines | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Name | LNCaP | 22Rv1 | PC3 | PC-3M | DU145 | C4-2B | CA-HPV-10 | TRAMP-C1 | TRAMP-C2 | RM-1 | Myc-CaP |
| Ganoderma lucidum (Leyss. ex Fr.) Karst. | + | ||||||||||
| Litchi chinensis Sonn. | + | + | + | + | |||||||
| Saussurea lappa Clarke | + | + | |||||||||
| Scutellaria baicalensis Georgi | + | + | |||||||||
| Scutellaria barbata D. Don | + | + | |||||||||
| Tripterygium wilfordii Hook F. | + | + | |||||||||
| Wedelia chinensis (Osbeck) Merr. | + | + | + | ||||||||
| Andrographolide | + | + | |||||||||
| Evodiamine | + | ||||||||||
| Guttiferone F | + | + | |||||||||
| Honokiol | + | + | + | ||||||||
| Isorhapontigenin | + | + | |||||||||
| Peperotetraphin | + | ||||||||||
| Quercetin | + | + | + | ||||||||
| Tetrandrine | + | + | |||||||||
| Triptolide | + | + | + | ||||||||
| Vitexicarpin | + | ||||||||||
| Arsenic sulphide | + | + | |||||||||
| Baicalin | + | + | + | + | |||||||
| Celastrol | + | ||||||||||
| Gypensapogenin H | + | + | |||||||||
| Scoparone | + | ||||||||||
| Curcumin | + | + | + | ||||||||
| dihydroisotanshinone I | + | + | + | ||||||||
| D-pinitol | + | + | |||||||||
| Shikonin | + | + | |||||||||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, X.; Fang, G.; Pang, Y. Chinese Medicines in the Treatment of Prostate Cancer: From Formulas to Extracts and Compounds. Nutrients 2018, 10, 283. https://doi.org/10.3390/nu10030283
Wang X, Fang G, Pang Y. Chinese Medicines in the Treatment of Prostate Cancer: From Formulas to Extracts and Compounds. Nutrients. 2018; 10(3):283. https://doi.org/10.3390/nu10030283
Chicago/Turabian StyleWang, Xueni, Gang Fang, and Yuzhou Pang. 2018. "Chinese Medicines in the Treatment of Prostate Cancer: From Formulas to Extracts and Compounds" Nutrients 10, no. 3: 283. https://doi.org/10.3390/nu10030283
APA StyleWang, X., Fang, G., & Pang, Y. (2018). Chinese Medicines in the Treatment of Prostate Cancer: From Formulas to Extracts and Compounds. Nutrients, 10(3), 283. https://doi.org/10.3390/nu10030283




