Fatigue as an Extra-Intestinal Manifestation of Celiac Disease: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
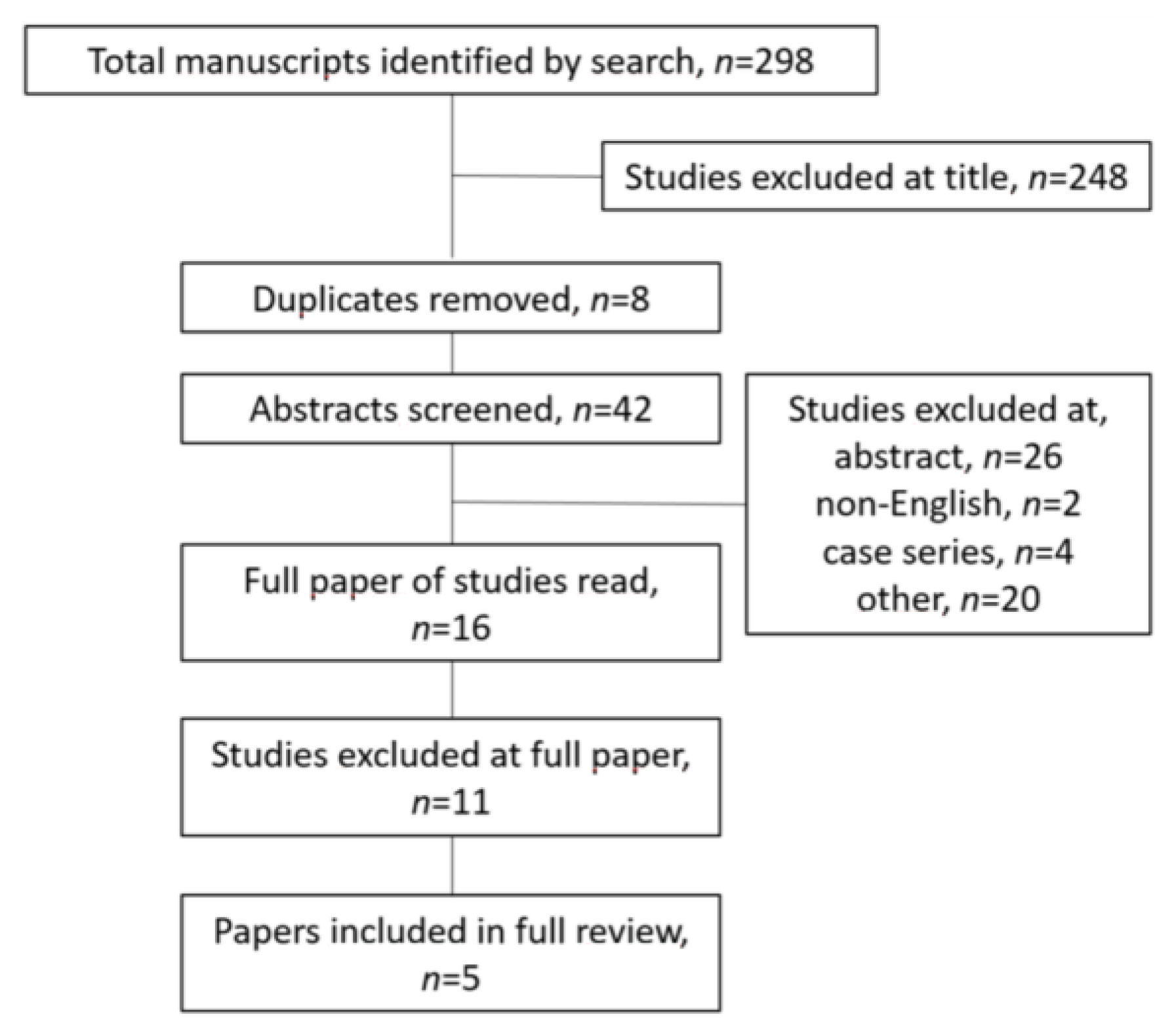
3. Results
3.1. Quality Assessment
3.2. Outline of the Included Papers
3.3. Definition and Measurement of Fatigue
3.4. Prevalence of Fatigue and Its Associations
3.5. Interventions to Alleviate Fatigue
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ludvigsson, J.F.; Leffler, D.A.; Bai, J.C.; Biagi, F.; Fasano, A.; Green, P.H.; Hadjivassiliou, M.; Kaukinen, K.; Kelly, C.P.; Leonard, J.N.; et al. The Oslo definitions for coeliac disease and related terms. Gut 2013, 62, 43–52. [Google Scholar] [CrossRef] [PubMed]
- Ludvigsson, J.F.; Bai, J.C.; Biagi, F.; Card, T.R.; Ciacci, C.; Ciclitira, P.J.; Green, P.H.R.; Hadjivassiliou, M.; Holdoway, A.; van Heel, D.A.; et al. Diagnosis and management of adult coeliac disease: Guidelines from the British Society of Gastroenterology. Gut 2014, 63, 1210–1228. [Google Scholar] [CrossRef] [PubMed]
- Leffler, D.A.; Green, P.H.; Fasano, A. Extraintestinal manifestations of coeliac disease. Nat. Rev. Gastroenterol. Hepatol. 2015, 12, 561–571. [Google Scholar] [CrossRef] [PubMed]
- Lundin, K.E.; Wijmenga, C. Coeliac disease and autoimmune disease-genetic overlap and screening. Nat. Rev. Gastroenterol. Hepatol. 2015, 12, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Hin, H.; Bird, G.; Fisher, P.; Mahy, N.; Jewell, D. Coeliac disease in primary care: Case finding study. BMJ 1999, 318, 164–167. [Google Scholar] [CrossRef] [PubMed]
- Sanders, D.S.; Patel, D.; Stephenson, T.J.; Ward, A.M.; McCloskey, E.V.; Hadjivassiliou, M.; Lobo, A.J. A primary care cross-sectional study of undiagnosed adult coeliac disease. Eur. J. Gastroenterol. Hepatol. 2003, 15, 407–413. [Google Scholar] [CrossRef] [PubMed]
- Jelsness-Jorgensen, L.P.; Bernklev, T.; Henriksen, M.; Torp, R.; Moum, B.A. Chronic fatigue is more prevalent in patients with inflammatory bowel disease than in healthy controls. Inflamm. Bowel Dis. 2011, 17, 1564–1572. [Google Scholar] [CrossRef] [PubMed]
- Van Langenberg, D.R.; Gibson, P.R. Systematic review: Fatigue in inflammatory bowel disease. Aliment. Pharmacol. Ther. 2010, 32, 131–143. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Hauser, W.; Gold, J.; Stein, J.; Caspary, W.F.; Stallmach, A. Health-related quality of life in adult coeliac disease in Germany: Results of a national survey. Eur. J. Gastroenterol. Hepatol. 2006, 18, 747–754. [Google Scholar] [CrossRef] [PubMed]
- Siniscalchi, M.; Iovino, P.; Tortora, R.; Forestiero, S.; Somma, A.; Capuano, L.; Franzese, M.D.; Sabbatini, F.; Ciacci, C. Fatigue in adult coeliac disease. Aliment. Pharmacol. Ther. 2005, 22, 489–494. [Google Scholar] [CrossRef] [PubMed]
- Jorda, F.C.; Lopez Vivancos, J. Fatigue as a determinant of health in patients with celiac disease. J. Clin. Gastroenterol. 2010, 44, 423–427. [Google Scholar] [CrossRef] [PubMed]
- Ciacci, C.; Peluso, G.; Iannoni, E.; Siniscalchi, M.; Iovino, P.; Rispo, A.; Tortora, R.; Bucci, C.; Zingone, F.; Margarucci, S.; et al. l-Carnitine in the treatment of fatigue in adult celiac disease patients: A pilot study. Dig. Liver. Dis. 2007, 39, 922–928. [Google Scholar] [CrossRef] [PubMed]
- Zingone, F.; Siniscalchi, M.; Capone, P.; Tortora, R.; Andreozzi, P.; Capone, E.; Ciacci, C. The quality of sleep in patients with coeliac disease. Aliment. Pharmacol. Ther. 2010, 32, 1031–1036. [Google Scholar] [CrossRef] [PubMed]
- Wessely, S.; Powell, R. Fatigue syndromes: A comparison of chronic “postviral” fatigue with neuromuscular and affective disorders. J. Neurol. Neurosurg. Psychiatr. 1989, 52, 940–948. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for The Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: Mahwah, NJ, USA, 1988. [Google Scholar]
- Zarkadas, M.; Cranney, A.; Case, S.; Molloy, M.; Switzer, C.; Graham, I.D.; Butzner, J.D.; Rashid, M.; Warren, R.E.; Burrows, V. The impact of a gluten-free diet on adults with coeliac disease: Results of a national survey. J. Hum. Nutr. Diet. 2006, 19, 41–49. [Google Scholar] [CrossRef] [PubMed]
- Spijkerman, M.; Tan, I.L.; Kolkman, J.J.; Withoff, S.; Wijmenga, C.; Visschedijk, M.C.; Weersma, R.K. A large variety of clinical features and concomitant disorders in celiac disease—A cohort study in the Netherlands. Dig. Liver Dis. 2016, 48, 499–505. [Google Scholar] [CrossRef] [PubMed]
- Silvester, J.A.; Graff, L.A.; Rigaux, L.; Walker, J.R.; Duerksen, D.R. Symptomatic suspected gluten exposure is common among patients with coeliac disease on a gluten-free diet. Aliment. Pharmacol. Ther. 2016, 44, 612–619. [Google Scholar] [CrossRef] [PubMed]
- Jericho, H.; Sansotta, N.; Guandalini, S. Extraintestinal manifestations of celiac disease: Effectiveness of the gluten-free diet. J. Pediatr. Gastroenterol. Nutr. 2017, 65, 75–79. [Google Scholar] [CrossRef] [PubMed]
- Sansotta, N.; Amirikian, K.; Guandalini, S.; Jericho, H. Celiac disease symptom resolution: Effectiveness of the gluten-free diet. J. Pediatr. Gastroenterol. Nutr. 2018, 66, 48–52. [Google Scholar] [CrossRef] [PubMed]
- Catassi, C.; Kryszak, D.; Louis-Jacques, O.; Duerksen, D.R.; Hill, I.; Crowe, S.E.; Brown, A.R.; Procaccini, N.J.; Wonderly, B.A.; Hartley, P.; et al. Detection of Celiac disease in primary care: A multicenter case-finding study in North America. Am. J. Gastroenterol. 2007, 102, 1454–1460. [Google Scholar] [CrossRef] [PubMed]
- Nurminen, S.; Kivela, L.; Huhtala, H.; Kaukinen, K.; Kurppa, K. Extraintestinal manifestations were common in children with coeliac disease and were more prevalent in patients with more severe clinical and histological presentation. Acta Paediatr. 2018. [Google Scholar] [CrossRef] [PubMed]
- Barratt, S.M.; Leeds, J.S.; Sanders, D.S. Factors influencing the type, timing and severity of symptomatic responses to dietary gluten in patients with biopsy-proven coeliac disease. JGLD 2013, 22, 391–396. [Google Scholar] [PubMed]
- Ford, S.; Howard, R.; Oyebode, J. Psychosocial aspects of coeliac disease: A cross-sectional survey of a UK population. Br. J. Health Psychol. 2012, 17, 743–757. [Google Scholar] [CrossRef] [PubMed]
- Francavilla, R.; Cristofori, F.; Castellaneta, S.; Polloni, C.; Albano, V.; Dellatte, S.; Indrio, F.; Cavallo, L.; Catassi, C. Clinical, serologic, and histologic features of gluten sensitivity in children. J. Pediatr. 2014, 164, 463–467. [Google Scholar] [CrossRef] [PubMed]
- DeLuca, J. Fatigue: As a Window to the Brain, 1st ed.; MIT Press: Cambridge, MA, USA, 2005. [Google Scholar]
- Jelsness-Jorgensen, L.P.; Bernklev, T.; Henriksen, M.; Torp, R.; Moum, B.A. Chronic fatigue is associated with impaired health-related quality of life in inflammatory bowel disease. Aliment. Pharmacol. Ther. 2011, 33, 106–114. [Google Scholar] [CrossRef] [PubMed]
- Frigstad, S.O.; Hoivik, M.L.; Jahnsen, J.; Cvancarova, M.; Grimstad, T.; Berset, I.P.; Huppertz-Hauss, G.; Hovde, Ø.; Bernklev, T.; Moum, B.; et al. Fatigue is not associated with vitamin D deficiency in inflammatory bowel disease patients. WJG 2018, 24, 3293–3301. [Google Scholar] [CrossRef] [PubMed]
- Kotterba, S.; Neusser, T.; Norenberg, C.; Bussfeld, P.; Glaser, T.; Dorner, M.; Schürks, M. Sleep quality, daytime sleepiness, fatigue, and quality of life in patients with multiple sclerosis treated with interferon beta-1b: Results from a prospective observational cohort study. BMC Nephrol. 2018, 18. [Google Scholar] [CrossRef] [PubMed]
- Rupp, I.; Boshuizen, H.C.; Jacobi, C.E.; Dinant, H.J.; van den Bos, G.A.M. Impact of fatigue on health-related quality of life in rheumatoid arthritis. Arthritis Rheum. 2004, 51, 578–585. [Google Scholar] [CrossRef] [PubMed]
- Opheim, R.; Fagermoen, M.S.; Bernklev, T.; Jelsness-Jorgensen, L.P.; Moum, B. Fatigue interference with daily living among patients with inflammatory bowel disease. Qual. Life Res. 2014, 23, 707–717. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J. A power primer. Psychol. Bull. 1992, 112, 155–159. [Google Scholar] [CrossRef] [PubMed]
- Romberg-Camps, M.J.; Bol, Y.; Dagnelie, P.C.; Hesselink-van de Kruijs, M.A.; Kester, A.D.; Engels, L.G.; van Deursen, C.; Hameeteman, W.H.A.; Pierik, M.; Pierik, F.; et al. Fatigue and health-related quality of life in inflammatory bowel disease: Results from a population-based study in the Netherlands: The IBD-South Limburg cohort. Inflamm. Bowel Dis. 2010, 16, 2137–2147. [Google Scholar] [CrossRef] [PubMed]
- Sobrero, A.; Puglisi, F.; Guglielmi, A.; Belvedere, O.; Aprile, G.; Ramello, M.; Grossi, F.A.O.U. San Martino —IST, Istituto Nazionale Ricerca sul Cancro (GENOVA) Fatigue: A main component of anemia symptomatology. Semin. Oncol. 2001, 28, 15–18. [Google Scholar] [CrossRef]
- Bohlius, J.; Tonia, T.; Nuesch, E.; Juni, P.; Fey, M.F.; Egger, M.; Bernhard, J. Effects of erythropoiesis-stimulating agents on fatigue- and anaemia-related symptoms in cancer patients: Systematic review and meta-analyses of published and unpublished data. Br. J. Cancer 2014, 111, 33–45. [Google Scholar] [CrossRef] [PubMed]
- Cella, D.; Kallich, J.; McDermott, A.; Xu, X. The longitudinal relationship of hemoglobin, fatigue and quality of life in anemic cancer patients: Results from five randomized clinical trials. Ann. Oncol. 2004, 15, 979–986. [Google Scholar] [CrossRef] [PubMed]
| Fatigue | Coeliac Disease |
|---|---|
| Fatigue (MeSH) | Coeliac disease |
| Mental fatigue | |
| Chronic fatigue | |
| Tiredness | |
| Exhaustion | |
| Weariness | |
| Vitality | |
| Asthenia | |
| Low energy |
| Study (Ref. No.) | Study Population and Setting | Study Design and Participants | Questionnaires Measuring Fatigue | Strengths and Limitations |
|---|---|---|---|---|
| Häuser et al., 2006 [10] | A subgroup of members (1000/18,355) from the German Coeliac Society (GZG) ≥18 years was invited to participate Every 18th person on the membership list was invited in order to ensure a geographically representative sample Normative data were collected from the handbooks of the SF-36, GBB-24 and HADS-D Exclusion criteria: <18 years of age | Cross-sectional design Available for analyses: n = 446 | SF-36 (Vitality subscale) GBB-24 (Fatigue subscale) | L: Fatigue not specified as aim, merely reported as parts of the questionnaire results L: No definition of fatigue L: Sample consisting of members of a patient society only L: Low response rate S: Normative data for comparison L: Self-reported information on comorbidity L: Single centre study S: Validated instruments used L: Coeliac disease diagnosis self-reported only |
| Siniscalchi et al., 2005 [11] | Caucation adults ≥18 years of age from Campania, Italy, were consecutively recruited from an outpatient clinic Participants divided into two groups (Group 1: Patients on gluten containing diet, Group 2: Patients on gluten-free diet) Control group consisted of volunteers recruited from medical an non-medical hospital staff Exclusion criteria: <18 years of age, lack of informed consent, major psychiatric disease, active thyroid gland disease | Cross-sectional design Coeliac disease: n = 130 Control group: n = 80 | CFS FSS VAS | S: Definition of fatigue. L: Inadequate language L: Groups not comparable due to differences in BMI, Ferritin, Haemoglobin L: No evidence of appropriate matching of groups L: Inadequate statistical control for differences between groups L: Methods used to collect socio-demographic and clinical data is lacking L: Unclear presentation of results L: Procedure for questionnaire handling insufficiently described L: Lack of information about validity and reliability on the study questionnaires, both in Italian and in the target group L: No clear identification and control of potential confounding factors L: Data not presented in line with study aims |
| Jordá et al., 2010 [12] | Patients with celiac disease seen between March 2008 and April 2009 were prospectively invited to participate in the study Included patients stratified in two groups (Group 1: Following gluten-free diet, Group 2: Untreated) | Cross-sectional study n = 51 Group 1: n = 38 Group 2: n = 13 | D-FIS | L: No definition of fatigue. S: Validated fatigue questionnaire used L: Small sample and small subgroups L: Lack of information on recruitment procedure L: Lack of information concerning the collection of socio-demographic and clinical data L: No information on ethical approval L: No information about response rate or number of patients approached for inclusion L: Characteristics differ between groups |
| Ciacci et al., 2007 [13] | Patients with CD screened for inclusion at the Department of Clinical and Experimental Medicine, Federico II University—Naples, Italy6 0 patients randomized following a 30-day gluten-free diet | Randomized, double blind, parallel study n = 60 (l-Carnitine group n = 30, placebo n = 30) | Scott-Huskisson VAS VSA SF-36 (Vitality subscale) | S: Definition of fatigue S: Randomized groups S: Allocation concealment S: Clear definition of coeliac disease L: Large number of participants did not complete study (n = 13 (22%)) L: Single centre L: Lack of calculation of effect size L: No information on validity/reliability of fatigue questionnaires |
| Zingone et al., 2010 [14] | Adult coeliac disease patients consecutively recruited from September 2009 to March 2010 from Frederico II University (Naples, Italy) Participants divided into two groups (Group 1: Coeliac patients at diagnosis on gluten containing diet. Group 2: Coeliac patients at follow up on gluten-free diet) Gender- and age-matched control group Inclusion criteria: Informed consent, 19–60 years Exclusion criteria: Major psychiatric disease, cancer, pregnancy or children blow 3 years of age | Case Control study Group 1: n = 30 Group 2: n = 30 Control group: n = 30 | Fatigue-VAS | L: Fatigue not specified as aim, merely reported as parts of the questionnaire results. L: No definition of fatigue L: No information about response rate or number of patients approached for inclusion L: Large numeric differences in characteristics between coeliac groups L: No control for confounding variables S: Gender- and age-matched controls |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jelsness-Jørgensen, L.-P.; Bernklev, T.; Lundin, K.E.A. Fatigue as an Extra-Intestinal Manifestation of Celiac Disease: A Systematic Review. Nutrients 2018, 10, 1652. https://doi.org/10.3390/nu10111652
Jelsness-Jørgensen L-P, Bernklev T, Lundin KEA. Fatigue as an Extra-Intestinal Manifestation of Celiac Disease: A Systematic Review. Nutrients. 2018; 10(11):1652. https://doi.org/10.3390/nu10111652
Chicago/Turabian StyleJelsness-Jørgensen, Lars-Petter, Tomm Bernklev, and Knut E. A. Lundin. 2018. "Fatigue as an Extra-Intestinal Manifestation of Celiac Disease: A Systematic Review" Nutrients 10, no. 11: 1652. https://doi.org/10.3390/nu10111652
APA StyleJelsness-Jørgensen, L.-P., Bernklev, T., & Lundin, K. E. A. (2018). Fatigue as an Extra-Intestinal Manifestation of Celiac Disease: A Systematic Review. Nutrients, 10(11), 1652. https://doi.org/10.3390/nu10111652






