Bioelectrical Impedance Analysis Results for Estimating Body Composition Are Associated with Glucose Metabolism Following Laparoscopic Sleeve Gastrectomy in Obese Japanese Patients
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects and Protocol
2.2. Biochemical Measurement and Blood Pressure
2.3. Anthropometry and Body Analyses
2.4. Bioelectrical Impedance Analysis
2.5. Statistical Analyses
3. Results
3.1. Basal Clinical Characteristics of Obese Patients and Body Weight Changes after LSG
3.2. Changes in Fat Mass after LSG
3.3. Muscle Mass Changes after LSG
3.4. Time Course Changes in Plasma Metabolic Parameters
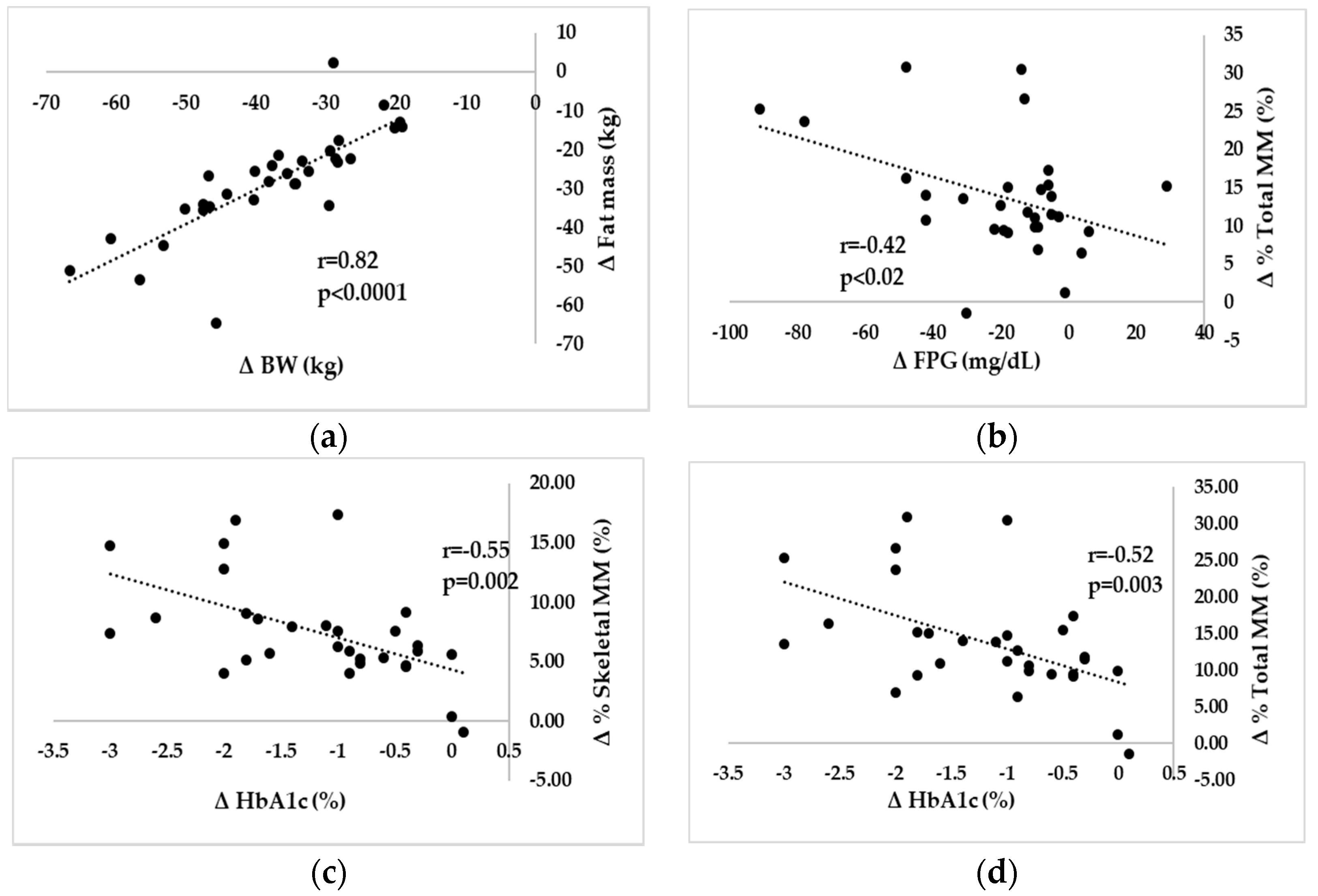
3.5. Correlation between Changes in Body Compositions and Changes in Glycemic Metabolic Parameters 12 Months after LSG
3.6. Relationships among Changes in Body Weight, FPG, and HbA1c
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| LSG | laparoscopic sleeve gastrectomy |
| BW | Body weight |
| BIA | bioelectrical impedance analysis |
| DX | Dual-energy X-ray absorptiometry |
| FM | fat mass |
| MM | muscle mass weight |
| %MM | % muscle mass |
| L/W | the ratio of lower extremity MM to BW |
| U/W | the ratio of upper extremity MM to BW |
| TBWL | total body weight loss |
| EBWL | excessive body weight loss |
| AST | aspartate aminotransferase |
| ALT | alanine transaminase |
| GTP | glutamic pyruvic transaminase |
| BUN | blood urea nitrogen |
| Cr | creatinine |
| LDL | low-density lipoprotein |
| HDL | high-density lipoprotein |
| FPG | fasting plasma glucose |
| HbA1c | Hemoglobin A1c |
References
- Shoar, S.; Mahmoudzadeh, H.; Naderan, M. Long-term outcome of bariatric surgery in morbidly obese adolescents: A systematic review and meta-analysis of 950 patients with a minimum of 3 years follow-up. Obes. Surg. 2017, 27, 3110–3117. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Yi, X.; Li, Q. The effectiveness and safety of sleeve gastrectomy in the obese elderly patients: A systematic review and meta-analysis. Obes. Surg. 2016, 26, 3023–3030. [Google Scholar] [CrossRef] [PubMed]
- Switzer, N.J.; Prasad, S.; Debru, E. Sleeve gastrectomy and type 2 diabetes mellitus: A systematic review of long-term outcomes. Obes. Surg. 2016, 26, 1616–1621. [Google Scholar] [CrossRef] [PubMed]
- Ramírez-Vélez, R.; Correa-Bautista, J.E.; González-Ruíz, K. Predictive validity of the body adiposity index in overweight and obese adults using dual-energy x-ray absorptiometry. Nutrients 2016, 8, 737. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Ambrosi, J.; González-Crespo, I.; Catalán, V. Clinical usefulness of abdominal bioimpedance (ViScan) in the determination of visceral fat and its application in the diagnosis and management of obesity and its comorbidities. Clin. Nutr. 2018, 37, 580–589. [Google Scholar] [CrossRef] [PubMed]
- Umemura, A.; Sasaki, A.; Nitta, H. Effects of changes in adipocyte hormones and visceral adipose tissue and the reduction of obesity-related comorbidities after laparoscopic sleeve gastrectomy in Japanese patients with severe obesity. Endocr. J. 2014, 61, 381–391. [Google Scholar] [CrossRef] [PubMed]
- Widen, E.M.; Strain, G.; King, W.C. Validity of bioelectrical impedance analysis for measuring changes in body water and percent fat after bariatric surgery. Obes. Surg. 2014, 24, 847–854. [Google Scholar] [CrossRef] [PubMed]
- Buffa, R.; Mereu, E.; Comandini, O. Bioelectrical impedance vector analysis (BIVA) for the assessment of two-compartment body composition. Eur. J. Clin. Nutr. 2014, 68, 1234–1240. [Google Scholar] [CrossRef] [PubMed]
- Xiao, J.; Purcell, S.A.; Prado, C.M. Fat mass to fat-free mass ratio reference values from NHANES III using bioelectrical impedance analysis. Clin. Nutr. 2017, 5614, 31353–31355. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, K.I.; Kanazawa, I.; Sugimoto, T. Reduced muscle mass and accumulation of visceral fat are independently associated with increased arterial stiffness in postmenopausal women with type 2 diabetes mellitus. Diabetes Res. Clin. Pract. 2016, 122, 141–147. [Google Scholar] [CrossRef] [PubMed]
- Hamasaki, H.; Kawashima, Y.; Adachi, H. Associations between lower extremity muscle mass and metabolic parameters related to obesity in Obese Japanese patients with type 2 diabetes. Peer. J. 2015, 3, e942. [Google Scholar] [CrossRef] [PubMed]
- Wannamethee, S.G.; Atkins, J.L. Muscle loss and obesity: The health implications of sarcopenia and sarcopenic obesity. Proc. Nutr. Soc. 2015, 74, 405–412. [Google Scholar] [CrossRef] [PubMed]
- Rossi, A.P.; Bianchi, L.; Volpato, S. Dynapenic abdominal obesity as a predictor of worsening disability, hospitalization, and mortality in older adults: Results from the In CHIANTI study. J. Gerontol. Biol. Sci. Med. Sci. 2017, 72, 1098–1104. [Google Scholar] [CrossRef] [PubMed]
- Dixon, J.B.; Bhasker, A.G.; Lambert, G.W. Leg to leg bioelectrical impedance analysis of percentage fat mass in obese patients: Can it tell us more than we already know? Surg. Obes. Relat. Dis. 2016, 12, 1397–1402. [Google Scholar] [CrossRef] [PubMed]
- Anderson, L.J.; Erceg, D.N.; Schroeder, E.T. Utility of multifrequency bioelectrical impedance compared with dual-energy X-ray absorptiometry for assessment of total and regional body composition varies between men and women. Nutr. Res. 2012, 32, 479–485. [Google Scholar] [CrossRef] [PubMed]
- Faria, S.L.; Faria, O.P.; Cardeal, M.D. Validation study of multi-frequency bioelectrical impedance with dual-energy X-ray absorptiometry among obese patients. Obes. Surg. 2014, 24, 1476–1480. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.J.; Madan, A.; Fenton-Lee, D. Does patient compliance with follow-up influence weight loss after gastric bypass surgery? A systematic review and meta-analysis. Obes. Surg. 2014, 24, 647–651. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Yuan, Y.; Qiu, C. A meta-analysis of 2-year effect after surgery: Laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for morbid obesity and diabetes mellitus. Obes. Surg. 2014, 24, 1528–1535. [Google Scholar] [CrossRef] [PubMed]
- Qi, L.; Guo, Y.; Liu, C.Q. Effects of bariatric surgery on glycemic and lipid metabolism, surgical complication and quality of life in adolescents with obesity: A systematic review and meta-analysis. Surg. Obes. Relat. Dis. 2017, 13, 2037–2055. [Google Scholar] [CrossRef] [PubMed]
- Haruta, H.; Kasama, K.; Ohta, M. Long-Term Outcomes of Bariatric and Metabolic Surgery in Japan: Results of a Multi-Institutional Survey. Obes. Surg. 2017, 27, 754–762. [Google Scholar] [CrossRef] [PubMed]
- Seki, Y.; Kasama, K.; Haruta, H. Five-Year-Results of Laparoscopic Sleeve Gastrectomy with Duodenojejunal Bypass for Weight Loss and Type 2 Diabetes Mellitus. Obes. Surg. 2017, 27, 795–801. [Google Scholar] [CrossRef] [PubMed]
- Rayner, J.J.; Banerjee, R.; Francis, J.M. Normalization of visceral fat and complete reversal of cardiovascular remodeling accompany gastric bypass, not banding. J. Am. Coll. Cardiol. 2015, 66, 2569–2570. [Google Scholar] [CrossRef] [PubMed]
- Tewari, N.; Awad, S.; Macdonald, I.A. A comparison of three methods to assess body composition. Nutrition 2018, 47, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Van Caenegem, E.; Wierckx, K.; Taes, Y. Bone mass, bone geometry, and body composition in female-to-male transsexual persons after long-term cross-sex hormonal therapy. J. Clin. Endocrinol. Metab. 2012, 97, 2503–2511. [Google Scholar] [CrossRef] [PubMed]
- Tymitz, K.; Kerlakian, G.; Engel, A. Gender differences in early outcomes following hand-assisted laparoscopic Roux-en-Y gastric bypass surgery: Gender differences in bariatric surgery. Obes. Surg. 2007, 17, 1588–1591. [Google Scholar] [CrossRef] [PubMed]
- Perrone, F.; Bianciardi, E.; Benavoli, D. Gender Influence on Long-Term Weight Loss and Comorbidities after Laparoscopic Sleeve Gastrectomy and Roux-en-Y Gastric Bypass: A Prospective Study with a 5-Year Follow-up. Obes. Surg. 2016, 26, 276–281. [Google Scholar] [CrossRef] [PubMed]
- Ikramuddin, S.; Korner, J.; Lee, W.J. Lifestyle Intervention and Medical Management with vs without Roux-en-Y Gastric Bypass and Control of Hemoglobin A1c, LDL Cholesterol, and Systolic Blood Pressure at 5 Years in the Diabetes Surgery Study. JAMA 2018, 319, 266–278. [Google Scholar] [CrossRef] [PubMed]
- Yang, J. Enhanced skeletal muscle for effective glucose homeostasis. Prog. Mol. Biol. Transl. Sci. 2014, 121, 133–163. [Google Scholar] [PubMed]
| pre-LSG | Three Months | Six Months | Twelve Months | f | F-Value | p-Value | |
|---|---|---|---|---|---|---|---|
| Body weight (kg) | 120.0 ± 25.9 | 91.9 ± 21.3 *** | 85.7 ± 20.8 *** | 82.3 ± 22.2 *** | 3 | 18.4 | <0.001 |
| Total body weight loss (kg) | 28.1 ± 8.7 | 34.3 ± 10.0 † | 37.8 ± 12.1 *††† | 2 | 7.16 | 0.001 | |
| %TBWL | 23.4 ± 5.5 | 28.6 ± 6.0 † | 31.7 ± 8.5 *††† | 2 | 12.3 | <0.001 | |
| %EBWL | 51.9 ± 21.4 | 71.9 ± 24.3 † | 79.6 ± 28.9 *†† | 2 | 5.51 | 0.006 | |
| BMI (kg/m2) | 45.1 ± 9.7 | 34.6 ± 7.9 *** | 32.2 ± 7.7 *** | 30.8 ± 8.1 *** | 3 | 19.1 | <0.001 |
| Systolic blood pressure (mmHg) | 136.1 ± 19.6 | 123.1 ± 18.2 ** | 121.4 ± 20.0 ** | 121.2 ± 16.5 ** | 3 | 4.74 | 0.004 |
| Diastolic blood pressure (mmHg) | 84.8 ± 14.5 | 79.8 ± 12.4 | 77.4 ± 12.3 | 77.1 ± 12.3 | 3 | 2.46 | 0.07 |
| Fasting plasma glucose (mg/dL) | 109.6 ± 21.0 | 91.8 ± 15.7 *** | 89.1 ± 9.9 *** | 91.1 ± 15.8 *** | 3 | 10.8 | <0.001 |
| HbA1c (%) | 6.4 ± 0.9 | 5.3 ± 0.4 *** | 5.3 ± 0.3 *** | 5.3 ± 0.3 *** | 3 | 31.2 | <0.001 |
| Triglycerides (mg/dL) | 163.9 ± 92.0 | 98.8 ± 33.8 *** | 92.0 ± 30.6 *** | 83.8 ± 39.7 *** | 3 | 13.5 | <0.001 |
| HDL cholesterol (mg/dL) | 45.7 ± 8.7 | 47.1 ± 9.6 | 53.8 ± 11.4 **† | 59.1 ± 14.1 ***††† | 3 | 9.45 | <0.001 |
| LDL cholesterol (mg/dL) | 125.2 ± 28.7 | 122.9 ± 32.4 | 125.8 ± 28.0 | 122.9 ± 35.4 | 3 | 0.07 | 0.97 |
| BUN (mg/dL) | 12.5 ± 3.0 | 11.3 ± 4.0 | 12.3 ± 3.7 | 13.6 ± 3.7 | 3 | 2.32 | 0.08 |
| Creatinine (mg/dL) | 0.70 ± 0.21 | 0.69 ± 0.17 | 0.71 ± 0.15 | 0.72 ± 0.17 | 3 | 0.21 | 0.89 |
| AST (IU/L) | 37.7 ± 24.9 | 19.0 ± 5.7 *** | 15.8 ± 3.2 *** | 16.0 ± 4.2 *** | 3 | 20.7 | <0.001 |
| ALT (IU/L) | 55.4 ± 45.1 | 18.4 ± 10.2 *** | 12.8 ± 4.1 *** | 12.9 ± 5.5 *** | 3 | 24.7 | <0.001 |
| GTP (IU/L) | 45.3 ± 34.9 | 20.1 ± 16.4 *** | 17.7 ± 17.2 *** | 16.1 ± 10.1 *** | 3 | 12.9 | <0.001 |
| FM (%) | 48.1 ± 6.9 | 39.9 ± 10.2 *** | 35.9 ± 9.8 *** | 33.4 ± 10.5 ***†† | 3 | 14.8 | < 0.001 |
| FM (kg) | 56.5 ± 19.0 | 37.3 ± 16.3 *** | 31.2 ± 14.8 *** | 28.1 ± 15.3 ***† | 3 | 19.7 | <0.001 |
| Total MM (kg) | 56.7 ± 11.6 | 50.6 ± 10.3 * | 50.6 ± 11.0 * | 50.0 ± 10.7 * | 3 | 2.67 | 0.05 |
| Total MM/BW | 0.49 ± 0.06 | 0.57 ± 0.10 ** | 0.61 ± 0.10 *** | 0.63 ± 0.10 ***†† | 3 | 14.5 | <0.001 |
| Skeletal MM (kg) | 33.4 ± 7.2 | 29.3 ± 6.4 * | 29.2 ± 6.7 * | 29.0 ± 6.7 ** | 3 | 3.18 | 0.03 |
| Skeletal MM/BW | 0.29 ± 0.04 | 0.33 ± 0.06 * | 0.35 ± 0.06 *** | 0.36 ± 0.06 ***† | 3 | 10.9 | <0.001 |
| Upper Skeletal MM/BW | 0.06 ± 0.01 | 0.07 ± 0.01 | 0.07 ± 0.01 ** | 0.07 ± 0.01 ** | 3 | 4.17 | 0.008 |
| Lower Skeletal MM/BW | 0.16 ± 0.02 | 0.19 ± 0.03 *** | 0.20 ± 0.03 *** | 0.21 ± 0.03 ***† | 3 | 15.3 | <0.001 |
| Model | Independent Variables | F Value | p Value |
|---|---|---|---|
| BW | Fat mass (kg) | 59.6 | <0.001 ** |
| FPG | % Total MM (%) | 5.9 | 0.022 * |
| HbA1c | % Skeletal MM (%) | 11.2 | 0.002 ** |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ozeki, Y.; Masaki, T.; Yoshida, Y.; Okamoto, M.; Anai, M.; Gotoh, K.; Endo, Y.; Ohta, M.; Inomata, M.; Shibata, H. Bioelectrical Impedance Analysis Results for Estimating Body Composition Are Associated with Glucose Metabolism Following Laparoscopic Sleeve Gastrectomy in Obese Japanese Patients. Nutrients 2018, 10, 1456. https://doi.org/10.3390/nu10101456
Ozeki Y, Masaki T, Yoshida Y, Okamoto M, Anai M, Gotoh K, Endo Y, Ohta M, Inomata M, Shibata H. Bioelectrical Impedance Analysis Results for Estimating Body Composition Are Associated with Glucose Metabolism Following Laparoscopic Sleeve Gastrectomy in Obese Japanese Patients. Nutrients. 2018; 10(10):1456. https://doi.org/10.3390/nu10101456
Chicago/Turabian StyleOzeki, Yoshinori, Takayuki Masaki, Yuichi Yoshida, Mitsuhiro Okamoto, Manabu Anai, Koro Gotoh, Yuichi Endo, Masayuki Ohta, Masafumi Inomata, and Hirotaka Shibata. 2018. "Bioelectrical Impedance Analysis Results for Estimating Body Composition Are Associated with Glucose Metabolism Following Laparoscopic Sleeve Gastrectomy in Obese Japanese Patients" Nutrients 10, no. 10: 1456. https://doi.org/10.3390/nu10101456
APA StyleOzeki, Y., Masaki, T., Yoshida, Y., Okamoto, M., Anai, M., Gotoh, K., Endo, Y., Ohta, M., Inomata, M., & Shibata, H. (2018). Bioelectrical Impedance Analysis Results for Estimating Body Composition Are Associated with Glucose Metabolism Following Laparoscopic Sleeve Gastrectomy in Obese Japanese Patients. Nutrients, 10(10), 1456. https://doi.org/10.3390/nu10101456





