Impact of the Outbreak of the COVID-19 Pandemic on Formal and Informal Care of Community-Dwelling Older Adults: Cross-National Clustering of Empirical Evidence from 23 Countries
Abstract
:1. Introduction
2. Measures and Methods
2.1. Data Source and Study Sample
2.2. Variables Included in the Analysis
2.3. Cluster Analysis
3. Results
4. Discussion
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Santana, R.; Sousa, J.S.; Soares, P.; Lopes, S.; Boto, P.; Rocha, J.V. The demand for hospital emergency services: Trends during the first month of COVID-19 response. Port. J. Public Health 2020, 38, 30–36. [Google Scholar] [CrossRef]
- Kissler, S.M.; Tedijanto, C.; Lipsitch, M.; Grad, Y. Social distancing strategies for curbing the COVID-19 epidemic. medRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Ashraf, B.N. Economic impact of government interventions during the COVID-19 pandemic: International evidence from financial markets. J. Behav. Exp. Financ. 2020, 27, 100371. [Google Scholar] [CrossRef]
- Tisdell, C.A. Economic, social and political issues raised by the COVID-19 pandemic. Econ. Anal. Policy 2020, 68, 17–28. [Google Scholar] [CrossRef]
- Jantzen, R.; Noisel, N.; Camilleri-Broet, S.; Labbe, C.; de Malliard, T.; Payette, Y.; Broet, P. Epidemiological and socio-economic characteristics of the COVID-19 spring outbreak in Quebec, Canada: A population-based study. medRxiv 2020. [Google Scholar] [CrossRef]
- D’Adamo, H.; Yoshikawa, T.; Ouslander, J.G. Coronavirus disease 2019 in geriatrics and long-term care: The ABCDs of COVID-19. J. Am. Geriatr. Soc. 2020, 68, 912–917. [Google Scholar] [CrossRef]
- Fisman, D.N.; Bogoch, I.; Lapointe-Shaw, L.; McCready, J.; Tuite, A.R. Risk factors associated with mortality among residents with coronavirus disease 2019 (COVID-19) in long-term care facilities in Ontario, Canada. JAMA Netw. Open 2020, 3, e2015957. [Google Scholar] [CrossRef] [PubMed]
- Roxby, A.C.; Greninger, A.L.; Hatfield, K.M.; Lynch, J.B.; Dellit, T.H.; James, A.; Taylor, J.; Page, L.C.; Kimball, A.; Arons, M.; et al. Detection of SARS-CoV-2 Among Residents and Staff Members of an Independent and Assisted Living Community for Older Adults—Seattle, Washington, 2020. MMWR. Morb. Mortal. Wkly. Rep. 2020, 69, 416–418. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cohen, M.A.; Tavares, J. Who are the most at-risk older adults in the COVID-19 era? It’s not just those in nursing homes. J. Aging Soc. Policy 2020, 32, 380–386. [Google Scholar] [CrossRef] [PubMed]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Naylor, M.D.; Hirschman, K.B.; McCauley, K. Meeting the transitional care needs of older adults with COVID-19. J. Aging Soc. Policy 2020, 32, 387–395. [Google Scholar] [CrossRef]
- Eurostat Ageing Europe—Statistics on Population Developments: Statistics Explained (europa.eu) Last Modified on 8 April 2021. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php/Ageing_Europe_-_statistics_on_population_developments (accessed on 28 June 2021).
- Casanova, G.; Tur-Sinai, A.; Lamura, G. Innovating long-term care provision in Mediterranean welfare states: A comparison between Italy and Israel. J. Aging Soc. Policy 2020, 32, 55–82. [Google Scholar] [CrossRef]
- Suanet, B.; Van Groenou, M.B.; Van Tilburg, T.G. Informal and formal home-care use among older adults in Europe: Can cross-national differences be explained by societal context and composition? Ageing Soc. 2012, 32, 491–515. [Google Scholar] [CrossRef]
- Dupraz, J.; Henchoz, Y.; Santos-Eggimann, B. Formal home care use by older adults: Trajectories and determinants in the Lc65+ cohort. BMC Health Serv. Res. 2020, 20, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.Y.Y.; Gobat, N.; Kim, J.H.; A Newnham, E.; Huang, Z.; Hung, H.; Dubois, C.; Hung, K.K.C.; Wong, E.L.Y.; Wong, S.Y.S. Informal home care providers: The forgotten health-care workers during the COVID-19 pandemic. Lancet 2020, 395, 1957–1959. [Google Scholar] [CrossRef]
- Phillips, D.; Paul, G.; Fahy, M.; Dowling-Hetherington, L.; Kroll, T.; Moloney, B.; Duffy, C.; Fealy, G.; Lafferty, A. The invisible workforce during the COVID-19 pandemic: Family carers at the frontline. HRB Open Res. 2020, 3, 24. [Google Scholar] [CrossRef] [PubMed]
- European Commission. The 2021 Ageing Report. Economic & Budgetary Projections for the EU Member States 2019–2070; Institutional Paper 148; Publications Office of the European Union: Luxembourg, 2021; Available online: https://ec.europa.eu/info/publications/2021-ageing-report-economic-and-budgetary-projections-eu-member-states-2019-2070_en (accessed on 28 June 2021).
- Roth, D.L.; Fredman, L.; Haley, W.E. Informal caregiving and its impact on health: A reappraisal from population-based studies. Gerontologist 2015, 55, 309–331. [Google Scholar] [CrossRef] [Green Version]
- Organisation for Economic Co-operation and Development. Care Needed: Improving the Lives of People with Dementia, OECD Health Policy Studies; OECD Publishing: Paris, France, 2018. [Google Scholar]
- Williams, F.; Moghaddam, N.; Ramsden, S.; De Boos, D. Interventions for reducing levels of burden amongst informal carers of persons with dementia in the community. A systematic review and meta-analysis of randomised controlled trials. Aging Ment. Health 2019, 23, 1629–1642. [Google Scholar] [CrossRef]
- van Groenou, M.I.B.; De Boer, A. Providing informal care in a changing society. Eur. J. Ageing 2016, 13, 271–279. [Google Scholar] [CrossRef] [Green Version]
- Hengelaar, A.H.; van Hartingsveldt, M.; Wittenberg, Y.; van Etten-Jamaludin, F.; Kwekkeboom, R.; Satink, T. Exploring the collaboration between formal and informal care from the professional perspective—A thematic synthesis. Health Soc. Care Community 2018, 26, 474–485. [Google Scholar] [CrossRef] [Green Version]
- Phillips, S.S.; Ragas, D.M.; Tom, L.S.; Hajjar, N.; Dong, X.; Simon, M.A. Voices of informal caregivers and community stakeholders: Whether and how to develop an informal caregiver training program. J. Community Health 2016, 41, 550–556. [Google Scholar] [CrossRef] [Green Version]
- Zigante, V. Informal Care in Europe—Exploring Formalisation, Availability and Quality; Publications Office of the European Union: Brussels, Belgium, 2018; ISBN 978-92-79-86583-1. [Google Scholar] [CrossRef]
- Colombo, F.; Frits, T. OECD Health Policy Studies Help Wanted? Providing and Paying for Long-Term Care; Organisation for Economic Co-Operation and Development: Paris, France, 2011.
- Tur-Sinai, A.; Casanova, G.; Lamura, G. Changes in the provision of family care to frail older people in familistic welfare states: Lessons from Israel and Italy. J. Aging Health 2020, 32, 972–986. [Google Scholar] [CrossRef]
- Tur-Sinai, A.; Teti, A.; Rommel, A.; Hlebec, V.; Lamura, G. How many older informal caregivers are there in Europe? Estimates from three European surveys in comparison. Int. J. Environ. Res. Public Health 2020, 17, 9531. [Google Scholar] [CrossRef]
- Vahia, I.V.; Blazer, D.G.; Smith, G.S.; Karp, J.F.; Steffens, D.C.; Forester, B.P.; Reynolds, C.F. COVID-19, mental health and aging: A need for new knowledge to bridge science and service. Am. J. Geriatr. Psychiatry 2020, 28, 695–697. [Google Scholar] [CrossRef] [PubMed]
- Carers, U.K. Caring behind closed doors. In Forgotten Families in the Coronavirus Outbreak; Carers UK: London, UK, 2020. [Google Scholar]
- Walsh, K.; Scharf, T.; Keating, N. Social exclusion of older persons: A scoping review and conceptual framework. Eur. J. Ageing 2017, 14, 81–98. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Torres, S. Social exclusion in old age: Domain-specific contributions to a debate. Int. J. Ageing Later Life 2018, 12, 7–24. [Google Scholar] [CrossRef] [Green Version]
- Madhav, N.; Oppenheim, B.; Gallivan, M.; Mulembakani, P.; Rubin, E.; Wolfe, N. Pandemics: Risks, impacts, and mitigation. In Disease Control Priorities: Improving Health and Reducing Poverty, 3rd ed.; The International Bank for Reconstruction and Development/The World Bank: Washington, DC, USA, 2017. [Google Scholar]
- Sumner, A.; Hoy, C.; Ortiz-Juarez, E. Estimates of the Impact of COVID-19 on Global Poverty; UNU-WIDER: Helsinki, Finland, 2020; pp. 800–809. [Google Scholar]
- Tur-Sinai, A.; Shuldiner, J.; Bentur, N. Sociodemographic inequality in joint-pain medication use among community-dwelling older adults in Israel. Health Soc. Care Community 2019, 27, 1167–1174. [Google Scholar] [CrossRef]
- Katz, R.; Lowenstein, A.; Halperin, D.; Tur-Sinai, A. Generational Solidarity in Europe and Israel. Can. J. Aging 2015, 34, 342–355. [Google Scholar] [CrossRef] [PubMed]
- Tur-Sinai, A.; Soskolne, V. Socioeconomic Status and Health Behaviors as Predictors of Changes in Self-Rated Health among Older Persons in Israel; Health and Social Care in the Community; Wiley: Hoboken, NJ, USA, 2020. [Google Scholar] [CrossRef]
- Carmel, S.; Tur-Sinai, A. Cognitive decline among European retirees: Impact of early retirement, nation-related and personal characteristics: A longitudinal study. Ageing Soc. 2021. [Google Scholar] [CrossRef]
- Scherpenzeel, A.; Axt, K.; Bergmann, M.; Douhou, S.; Oepen, A.; Sand, G.; Schuller, K.; Stuck, S.; Wagner, M.; Borsch-Supan, A. Collecting survey data among the 50+ population during the COVID-19 outbreak: The Survey of Health, Ageing and Retirement in Europe (SHARE). Surv. Res. Methods 2020, 14, 217–221. [Google Scholar]
- Health and Retirement Study (HRS). 2020 HRS COVID-19 Project—Data Description and Usage; HRS: Ann Arbor, MI, USA, 2021. [Google Scholar]
- Esping-Andersen, G. Social Foundations of Postindustrial Economies; OUP Oxford: Oxford, UK, 1999. [Google Scholar]
- Miller, E.A. Protecting and improving the lives of older adults in the COVID-19 era. J. Aging Soc. Policy 2020, 32, 297–309. [Google Scholar] [CrossRef]
- Hoffman, G.J.; Webster, N.J.; Bynum, J.P.W. A framework for aging-friendly services and supports in the age of COVID-19. J. Aging Soc. Policy 2020, 32, 450–459. [Google Scholar] [CrossRef]
- Kim HH, S.; Jung, J.H. Social isolation and psychological distress during the COVID-19 pandemic: A cross-national analysis. Gerontologist 2021, 61, 103–113. [Google Scholar] [CrossRef]

| Country | Cumulative Confirmed COVID-19 Cases per Million People | Cumulative Confirmed COVID-19 Deaths per Million People |
|---|---|---|
| Netherlands | 3311.96 | 360.08 |
| Poland | 1289.13 | 46.40 |
| Germany | 2555.54 | 109.58 |
| Switzerland | 4151.19 | 229.24 |
| France | 3453.66 | 448.68 |
| Luxembourg | 11,193.72 | 188.51 |
| Bulgaria | 1830.19 | 62.60 |
| Lithuania | 786.47 | 23.51 |
| Latvia | 666.42 | 16.96 |
| Slovakia | 442.70 | 5.31 |
| Malta | 2097.21 | 20.38 |
| Belgium | 6139.81 | 850.67 |
| Spain | 6539.80 | 609.52 |
| Denmark | 2493.01 | 106.35 |
| Croatia | 1309.54 | 37.51 |
| Sweden | 7757.10 | 569.05 |
| Finland | 1355.78 | 59.74 |
| Estonia | 1592.87 | 47.49 |
| Cyprus | 1364.31 | 21.69 |
| Italy | 4115.04 | 581.97 |
| Israel | 9044.61 | 72.21 |
| Hungary | 472.45 | 62.01 |
| Greece | 442.70 | 20.15 |
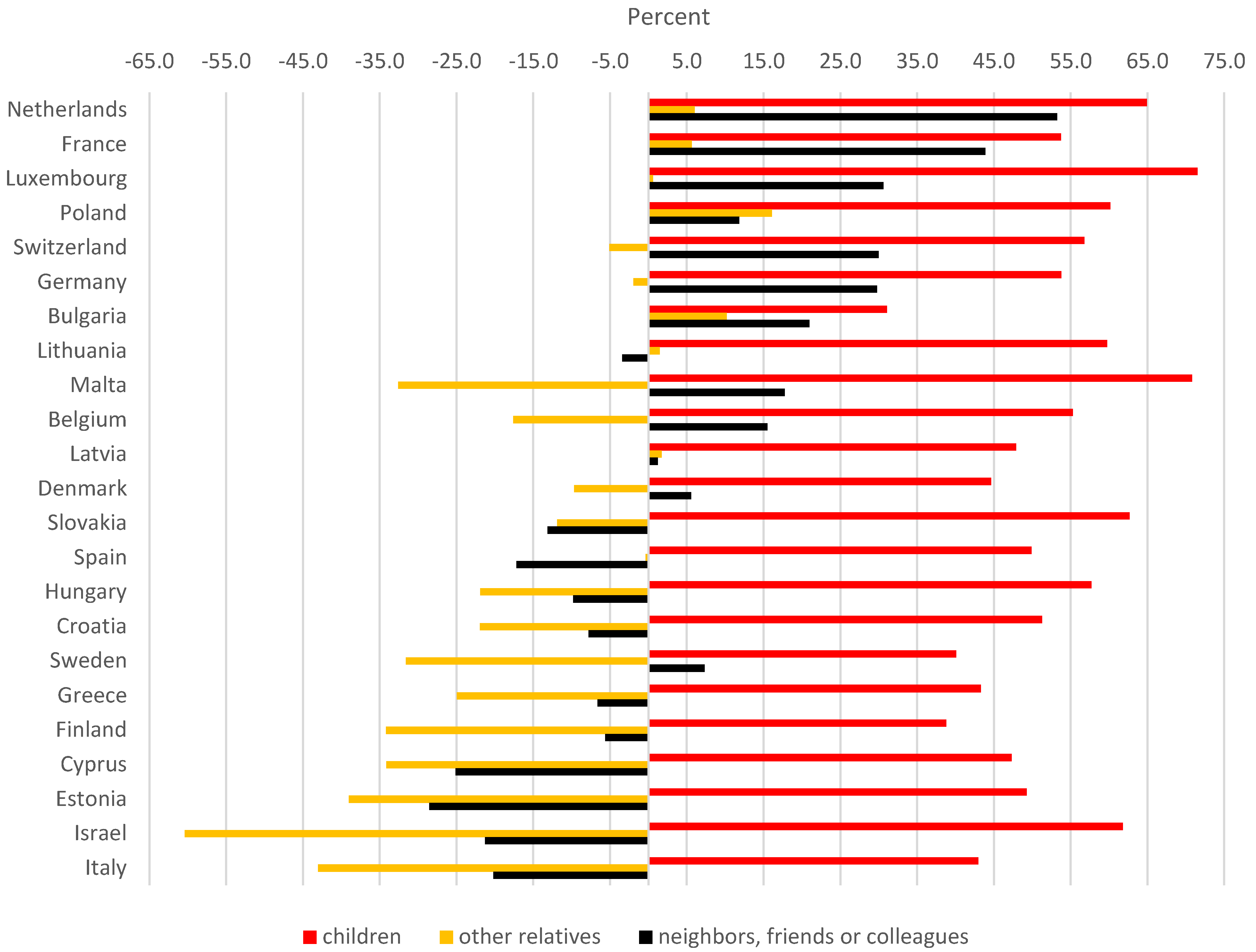
| Cluster | Country | Difference between Those Reporting More and Those Reporting Less Practical Help from… | Change in Informal Care (=Average of Columns “a,” “b” and “c”) | Share of Respondents Reporting More Difficulties in Receiving Home Care | Deviation from Average | |||
| … Children | … Other Relatives | … Non Relatives (Neighbor, etc.) | Informal Care | Home Care | ||||
| a | b | c | d | e | f | g | ||
| 1 | Netherlands | 64.9 | 6.0 | 53.3 | 41.4 | 7.6 | 27.3 | −11.8 |
| 1 | Poland | 60.2 | 16.1 | 11.8 | 29.4 | 2.9 | 15.2 | −16.4 |
| 1 | Germany | 53.8 | −2.0 | 29.8 | 27.2 | 5.1 | 13.0 | −14.2 |
| 1 | Switzerland | 56.8 | −5.1 | 30.0 | 27.2 | 10.5 | 13.1 | −8.8 |
| 2 | France | 53.7 | 5.7 | 43.9 | 34.4 | 29.0 | 20.3 | 9.7 |
| 2 | Luxembourg | 71.5 | 0.6 | 30.6 | 34.2 | 29.2 | 20.1 | 9.9 |
| 3 | Bulgaria | 31.1 | 10.2 | 21.0 | 20.7 | 8.0 | 6.6 | −11.3 |
| 3 | Lithuania | 59.8 | 1.5 | −3.4 | 19.3 | 8.8 | 5.1 | −10.6 |
| 3 | Latvia | 47.9 | 1.7 | 1.2 | 17.0 | 8.2 | 2.8 | −11.1 |
| 3 | Slovakia | 62.7 | −11.9 | −13.1 | 12.6 | 8.7 | −1.6 | −10.7 |
| 4 | Malta | 70.8 | −32.6 | 17.8 | 18.7 | 24.0 | 4.5 | 4.7 |
| 4 | Belgium | 55.3 | −17.6 | 15.5 | 17.7 | 21.0 | 3.6 | 1.6 |
| 4 | Spain | 49.9 | −0.4 | −17.2 | 10.8 | 25.9 | −3.4 | 6.6 |
| 4 | Denmark | 44.6 | −9.7 | 5.5 | 13.5 | 19.7 | −0.6 | 0.3 |
| 5 | Croatia | 51.3 | −22.0 | −7.8 | 7.2 | 15.6 | −7.0 | −3.8 |
| 5 | Sweden | 40.1 | −31.6 | 7.3 | 5.3 | 5.7 | −8.9 | −13.6 |
| 5 | Finland | 38.8 | −34.2 | −5.6 | −0.3 | 8.7 | −14.5 | −10.7 |
| 5 | Estonia | 49.3 | −39.0 | −28.5 | −6.1 | 12.1 | −20.2 | −7.2 |
| 6 | Cyprus | 47.3 | −34.1 | −25.1 | −4.0 | 24.7 | −18.1 | 5.3 |
| 6 | Italy | 43.0 | −43.0 | −20.2 | −6.8 | 28.9 | −20.9 | 9.6 |
| 6 | Israel | 61.8 | −60.4 | −21.3 | −6.6 | 36.4 | −20.8 | 17.0 |
| 7 | Hungary | 57.7 | −21.9 | −9.8 | 8.7 | 56.1 | −5.5 | 36.8 |
| 7 | Greece | 43.3 | −24.9 | −6.6 | 3.9 | 48.0 | −10.2 | 28.6 |
| Average | 52.9 | −15.2 | 4.7 | 14.1 | 19.3 | |||
| Legend: | ||||||||
| First quartile (in relation to the difference between highest and lowest deviation from average) | ||||||||
| Second quartile | ||||||||
| Third quartile | ||||||||
| Fourth quartile | ||||||||
| Change in Home Care Provision * | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1: Fewer Difficulties | 2: Medium | 3: More Difficulties | ||||||||
| Change in informal care * | 1: stronger | Informal Help | Home Care | Informal Help | Home Care | Informal Help | Home Care | |||
| Netherlands | 41 | 8 | France | 34 | 29 | |||||
| Poland | 29 | 3 | ||||||||
| Germany | 27 | 5 | Luxembourg | 34 | 29 | |||||
| Switzerland | 27 | 11 | ||||||||
| 2: medium | Bulgaria | 21 | 8 | Denmark | 14 | 20 | ||||
| Latvia | 17 | 8 | Belgium | 18 | 21 | |||||
| Slovakia | 13 | 9 | Malta | 19 | 24 | |||||
| Lithuania | 19 | 9 | Spain | 11 | 26 | |||||
| 3: weaker | Sweden | 5 | 6 | Cyprus | -4 | 25 | Greece | 4 | 48 | |
| Finland | 0 | 9 | Italy | -7 | 29 | |||||
| Estonia | -6 | 12 | Israel | -7 | 36 | Hungary | 9 | 56 | ||
| Croatia | 7 | 16 | ||||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tur-Sinai, A.; Bentur, N.; Fabbietti, P.; Lamura, G. Impact of the Outbreak of the COVID-19 Pandemic on Formal and Informal Care of Community-Dwelling Older Adults: Cross-National Clustering of Empirical Evidence from 23 Countries. Sustainability 2021, 13, 7277. https://doi.org/10.3390/su13137277
Tur-Sinai A, Bentur N, Fabbietti P, Lamura G. Impact of the Outbreak of the COVID-19 Pandemic on Formal and Informal Care of Community-Dwelling Older Adults: Cross-National Clustering of Empirical Evidence from 23 Countries. Sustainability. 2021; 13(13):7277. https://doi.org/10.3390/su13137277
Chicago/Turabian StyleTur-Sinai, Aviad, Netta Bentur, Paolo Fabbietti, and Giovanni Lamura. 2021. "Impact of the Outbreak of the COVID-19 Pandemic on Formal and Informal Care of Community-Dwelling Older Adults: Cross-National Clustering of Empirical Evidence from 23 Countries" Sustainability 13, no. 13: 7277. https://doi.org/10.3390/su13137277






