Framing the Shades of Sustainability in Health Care: Pitfalls and Perspectives from Western EU Countries
Abstract
1. Introduction
2. Highlighting the Different Shades of Sustainability in Health Care
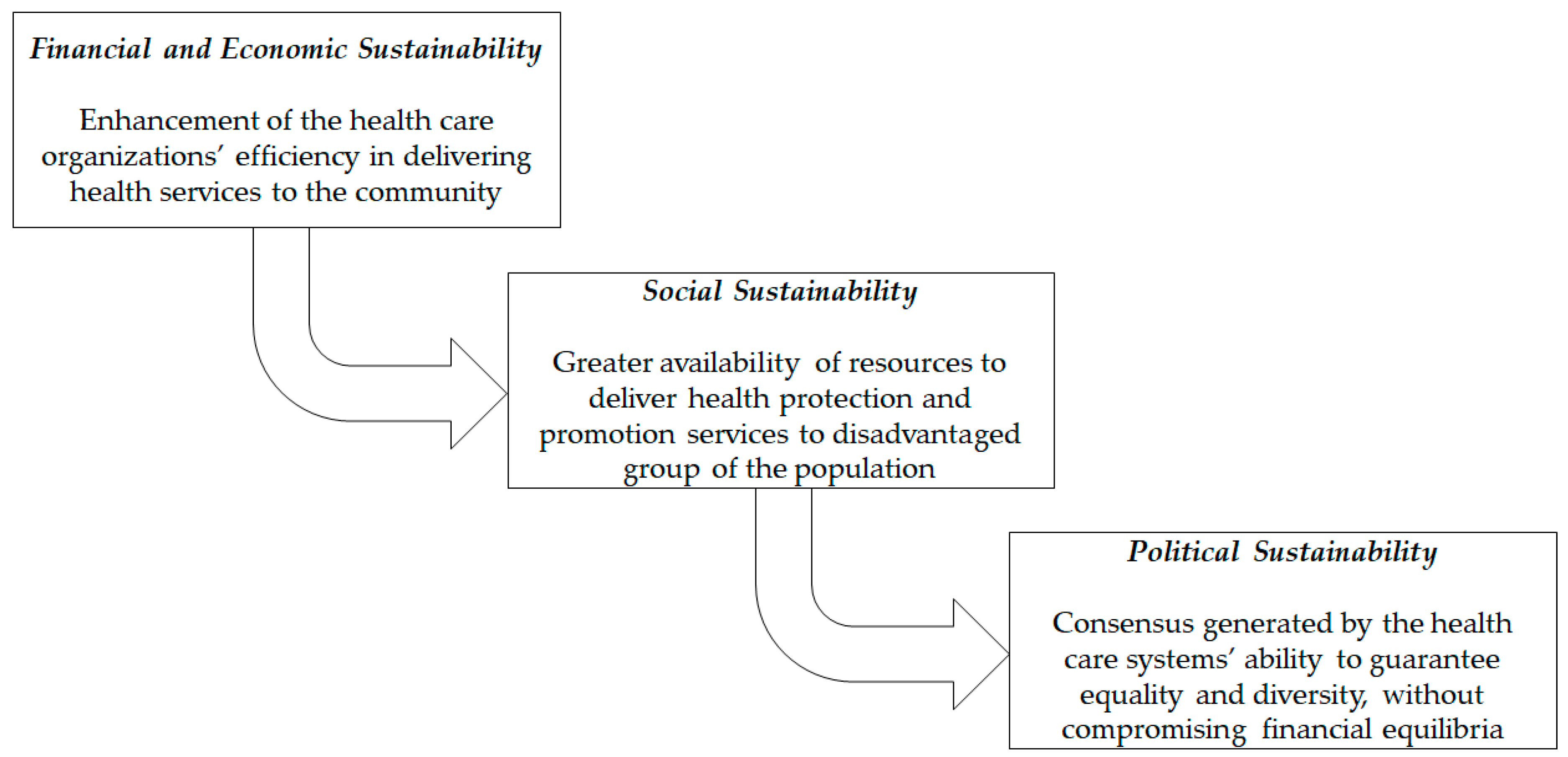
2.1. The Conventional Shade: Financial and Economic Sustainability
2.2. The Hidden Shade: Political Sustainability
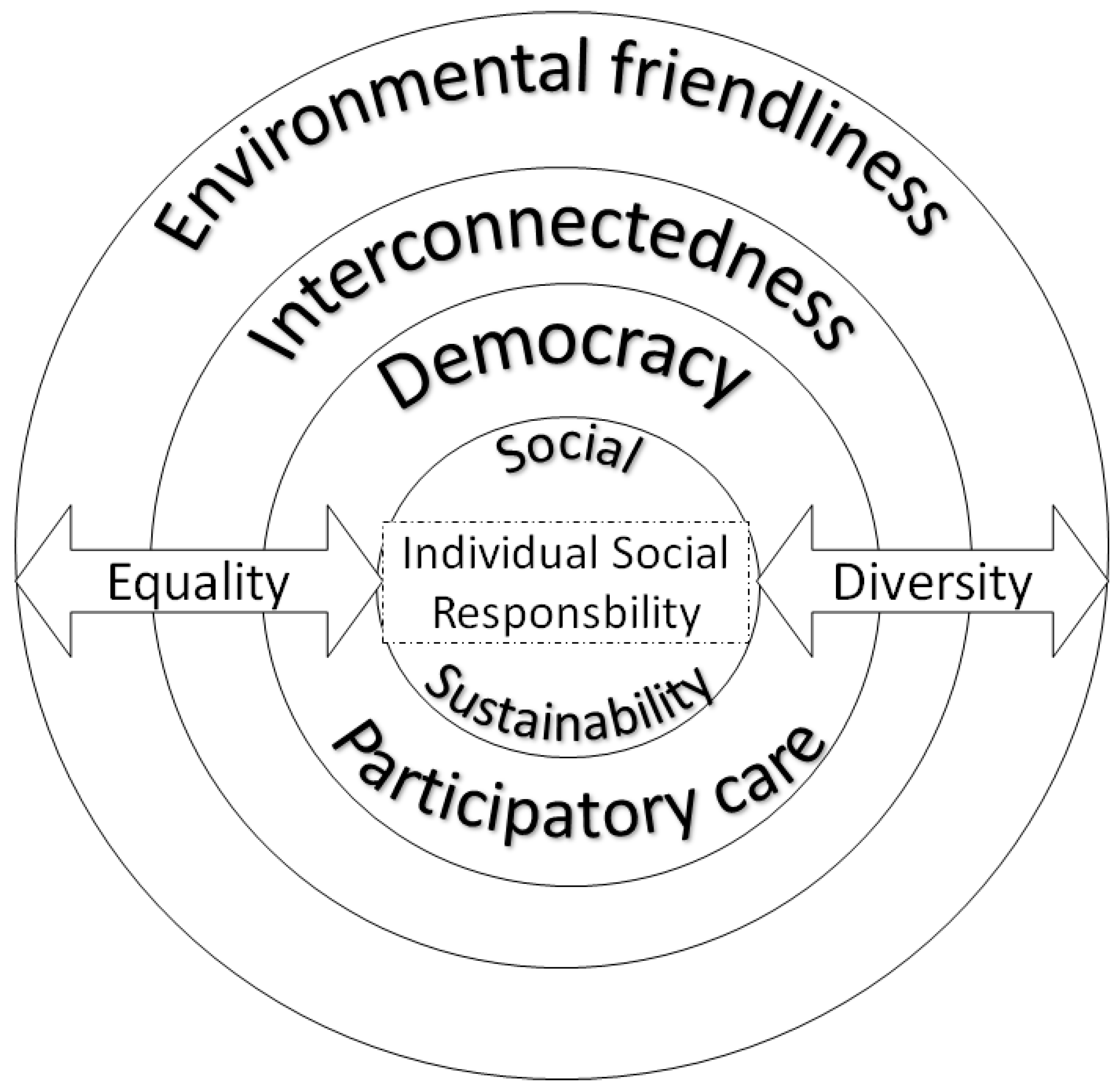
2.3. The Rooted Shade: Social Sustainability
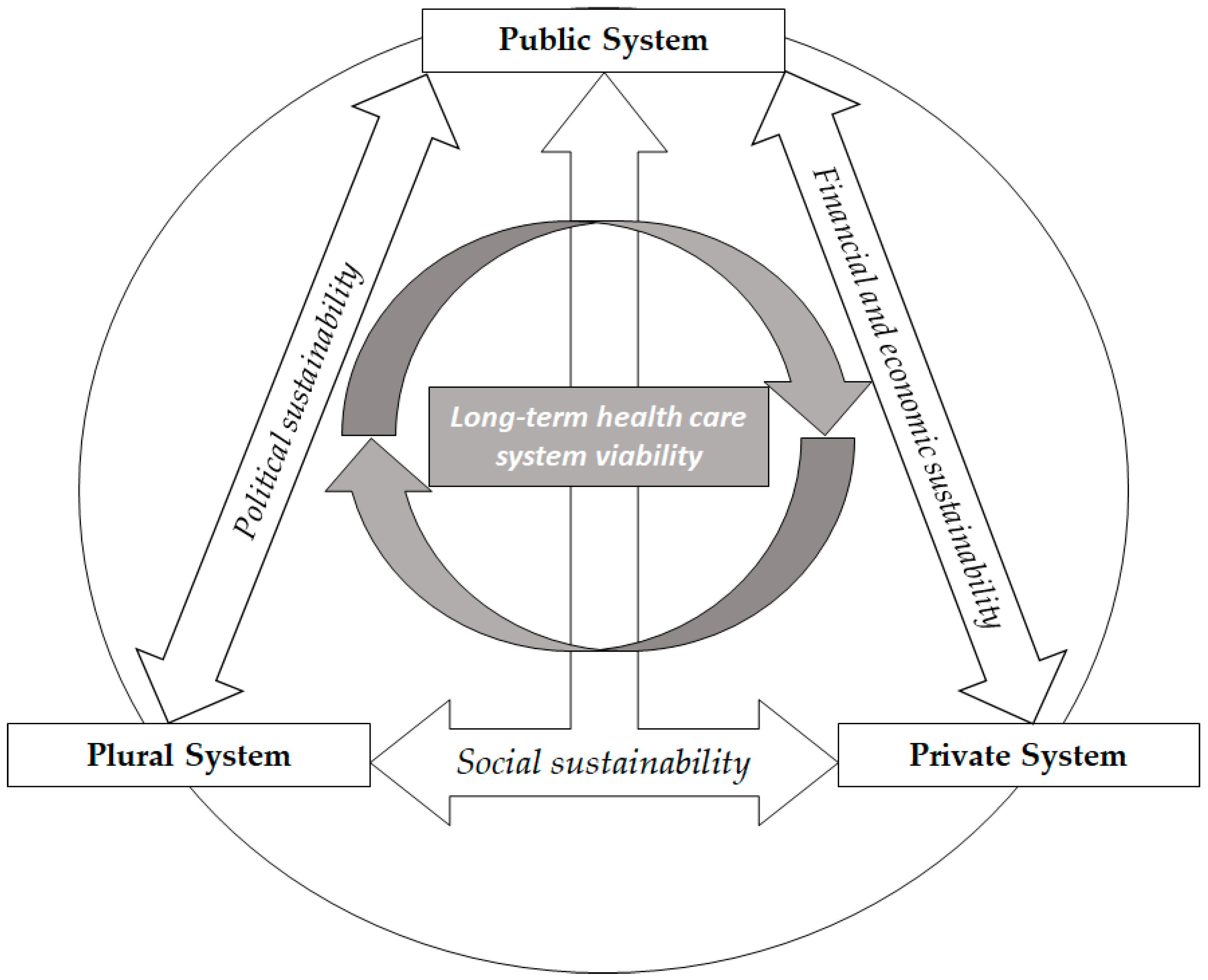
3. Containing the Side Effects of Sustainability
4. A Recipe for Long-Term Sustainability?
5. Concluding Remarks
Author Contributions
Funding
Conflicts of Interest
References
- Guyatt, G.; Yalnizyan, A.; Devereaux, P.J. Solving the public health care sustainability puzzle. Can. Med. Assoc. J. 2002, 167, 36–38. [Google Scholar]
- Immergut, E.M. Health Politics: Interests and Institutions in Western Europe New York; Cambridge University Press: Cambridge, UK, 1992. [Google Scholar]
- Saltman, R.B.; Figueras, J.; Sakellarides, C. Critical Challenges for Health Care Reform. In Europe Maidenhead; Open University Press: London, UK, 1998. [Google Scholar]
- Kus, B. Neoliberalism, Institutional Change and the Welfare State: The Case of Britain and France. Int. J. Comput. Soc. 2006, 47, 488–525. [Google Scholar] [CrossRef]
- Simonet, D. Healthcare reforms and cost reduction strategies in Europe: The cases of Germany, UK, Switzerland, Italy and France. Int. J. Health Care Qual. Assur. 2010, 23, 470–488. [Google Scholar] [CrossRef] [PubMed]
- Pavolini, E.; Guillén, A.M. Health Care Systems in Europe under Austerity; Institutional Reforms and Performance Basingstoke; Palgrave Macmillan: Basingstoke, UK, 2013. [Google Scholar]
- Lennox, L.; Maher, L.; Reed, J. Navigating the sustainability landscape: A systematic review of sustainability approaches in healthcare. Implement. Sci. 2018, 13, 27. [Google Scholar] [CrossRef] [PubMed]
- Chu, K.W.K.; Cheung, L.L.W. Incorporating sustainability in small health-care facilities: An integrated model. Lead Health Serv. 2018, 31, 441–451. [Google Scholar] [CrossRef] [PubMed]
- Guidotti, T.L. Sustainability and health: Notes toward a convergence of agendas. J. Environ. Stud. Sci. 2018, 8, 357–361. [Google Scholar] [CrossRef]
- Rich, C.R.; Singleton, J.K.; Wadhwa, S.S. Sustainability for Healthcare Management: A Leadership Imperative; Routledge: London, UK, 2013. [Google Scholar]
- Boone, T. Organizing for sustainability: Exploratory analysis of the healthcare industry. Int. Ser. Opt. Res. Manag. Sci. 2012, 174, 37–48. [Google Scholar]
- Anåker, A.; Elf, M. Sustainability in nursing: A concept analysis. Scand. J. Caring Sci. 2014, 28, 381–389. [Google Scholar] [CrossRef] [PubMed]
- Buffoli, M.; Capolongo, S.N.M.; Gherardi, G.; Gola, M. Healthcare Sustainability Evaluation Systems. In Improving Sustainability during Hospital Design and Operation. Green Energy and Technology; Capolongo, S., Bottero, M., Buffoli, M., Lettieri, E., Eds.; Springer: Cham, Switzerland, 2015; pp. 23–29. [Google Scholar]
- Hovlid, E.; Bukve, O.; Haug, K.; Aslaksen, A.B.; von Plessen, C. Sustainability of healthcare improvement: What can we learn from learning theory? BMC Health Serv. Res. 2012, 12, 235. [Google Scholar] [CrossRef] [PubMed]
- Buchanan, D.A.; Fitzgerald, L.; Ketley, D. The Sustainability and Spread of Organizational Change: Modernizing Healthcare; Routledge: London, UK, 2007. [Google Scholar]
- Roberts, J.L. Terminology a Glossary of Technical Terms on the Economics and Finance of Health Services; World Health Organization, Regional Office for Europe: Geneva, Switzerland, 1998. [Google Scholar]
- Harris, C.; Green, S.; Elshaug, A.G. Sustainability in Health care by Allocating Resources Effectively (SHARE) 10: Operationalising disinvestment in a conceptual framework for resource allocation. BMC Health Serv. Res. 2017, 17, 632. [Google Scholar] [CrossRef] [PubMed]
- Thomson, S.; Foubister, T.; Figueras, J.; Kutzin, J.; Permanand, G.; Bryndová, L. Addressing Financial Sustainability in Health Systems; World Health Organization, Regional Office for Europe: Copenhagen, Denmark, 2009. [Google Scholar]
- Blank, J.L.T.; Valdmanis, V.G. Technology diffusion in hospitals: A log odds random effects regression model. Int. J. Health Plan. Manag. 2015, 30, 246–259. [Google Scholar] [CrossRef] [PubMed]
- Bigdeli, M.; Shroff, C.Z.G.I.; Ghaffar, A. Health systems research on access to medicines: Unpacking challenges in implementing policies in the face of the epidemiological transition. BMC Glob. Health 2018, 2, 941. [Google Scholar] [CrossRef] [PubMed]
- Van Bokkelen, G.; Morsy, M.; Kobayashi, T.H. Demographic Transition, Health Care Challenges, and the Impact of Emerging International Regulatory Trends with Relevance to Regenerative Medicine. Curr. Stem Cell Rep. 2015, 1, 102–109. [Google Scholar] [CrossRef]
- Zaidi, B.; Morgan, S.P. The Second Demographic Transition Theory: A Review and Appraisal. Annu. Rev. Sociol. 2017, 43, 473–492. [Google Scholar] [CrossRef] [PubMed]
- Porter, M.E. What Is Value in Health Care? N. Eng. J. Med. 2010, 363, 2477–2481. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P.; Starace, F.; Palumbo, R. Health Outcomes and Patient Empowerment. The Case of Health Budgets in Italy. J. Health Manag. 2016, 18, 117–133. [Google Scholar] [CrossRef]
- Palumbo, R.; Manna, R. What if things go wrong in co-producing health services? Exploring the implementation problems of health care co-production. Pol. Soc. 2018, 37, 368–385. [Google Scholar] [CrossRef]
- Picatoste, J.; Ruesga-Benito, S.M.; González-Laxe, F. Economic environment and health care coverage: Analysis of social acceptance of access restrictive policies applied in Spain in the context of economic crisis. J. Clean. Prod. 2018, 172, 3600–3608. [Google Scholar] [CrossRef]
- Berwick, D.M.; Nolan, T.W.; Whittington, J. The Triple Aim: Care, Health, and Cost. Health Aff. 2008, 27, 759–769. [Google Scholar] [CrossRef] [PubMed]
- Maarse, H.; Jeurissen, P.; Ruwaard, D. Concerns over the Financial Sustainability of the Dutch Healthcare System; IFO Institute, Center for Economic Studies: Munich, Germany, 2013.
- Rouse, W.B. Health Care as a Complex Adaptive System: Implications for Design and Management. Bridge 2008, 38, 17–25. [Google Scholar]
- McDaniel, R.R.; Lanham, H.J.; Anderson, R.A. Implications of complex adaptive systems theory for the design of research on health care organizations. Health Care Manag. Rev. 2009, 34, 191–199. [Google Scholar] [CrossRef] [PubMed]
- Rouse, W.B. Managing complexity: Disease control as a complex adaptive system. Inf. Knowl. Syst. Manag. 2000, 2, 143–165. [Google Scholar]
- Kessler, R.; Glasgow, R.E. A Proposal to Speed Translation of Healthcare Research into Practice: Dramatic Change is Needed. Am. J. Prev. Med. 2011, 40, 637–644. [Google Scholar] [CrossRef] [PubMed]
- Waddock, S. The Wicked Problems of Global Sustainability Need Wicked (Good) Leaders and Wicked (Good) Collaborative Solutions. J. Manag. Glob. Sust. 2013, 1, 91–111. [Google Scholar] [CrossRef]
- Raisio, H. Health care reform planners and wicked problems: Is the wickedness of the problems taken seriously or is it even noticed at all? J. Health Organ. Manag. 2009, 23, 477–493. [Google Scholar] [CrossRef] [PubMed]
- Alford, J. Wicked and less wicked problems: A typology and a contingency framework. Pol. Soc. 2017, 36, 397–413. [Google Scholar] [CrossRef]
- Rittel, H.; Webber, M. Dilemmas in a General Theory of Planning. Pol. Sci. 1973, 4, 155–169. [Google Scholar] [CrossRef]
- Blackman, T.; Greene, A.; Hunter, D.J.; McKee, L.; Elliott, E.; Harrington, B.; Marks, L.; Williams, G. Performance Assessment and Wicked Problems: The Case of Health Inequalities. Pub. Pol. Adm. 2006, 21, 66–80. [Google Scholar] [CrossRef]
- Blok, V.; Gremmen, H.G.J.; Wesselink, R. Dealing with the wicked problem of sustainability: The role of individual virtuous competence. Bus. Prof. Ethics J. 2016, 34, 297–327. [Google Scholar] [CrossRef]
- Palumbo, R. Toward a new conceptualization of health care services to inspire public health. Public national health service as a “common pool of resources”. Int. Rev. Public Nonprofit Mark. 2017, 14, 271–287. [Google Scholar] [CrossRef]
- Karanikolos, M.; Mladovsky, P.; Cylus, J.; Thomson, S.; Basu, S.; Stuckler, D.; Mackenbach, J.P.; McKee, M. Financial crisis, austerity, and health in Europe. Lancet 2013, 381, 1323–1331. [Google Scholar] [CrossRef]
- Beard, J.R.; Bloom, D.E. Towards a Comprehensive Public Health Response to Population Ageing. Lancet 2015, 385, 658–661. [Google Scholar] [CrossRef]
- Rosko, M.D. Understanding variations in hospital costs: An economics perspective. Ann. Oper. Res. 1996, 67, 1–21. [Google Scholar] [CrossRef]
- Evans, R.G.; Stoddart, G.L. Producing Health, Consuming Health Care. In Barer M. Why Are Some People Healthy and Others Not? Routledge: New York, NY, USA, 1994; pp. 27–66. [Google Scholar]
- Adinolfi, P.; Florenzano, O.; Palumbo, R. Spending review tra austerity e razionalizzazione: L’Esperienza della Regione Campania. Mecosan 2017, 104. Available online: https://www.francoangeli.it/riviste/sommario.asp?IDRivista=180 (accessed on 25 November 2018).
- Reeves, A.; McKee, M.; Basu, S.; Stuckler, D. The political economy of austerity and healthcare: Cross-national analysis of expenditure changes in 27 European nations 1995–2011. Health Pol. 2014, 115, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Kaminska, M.E.; Wulfgramm, M. Universal or commodified healthcare? Linking out-of-pocket payments to income-related inequalities in unmet health needs in Europe. J. Eur. Soc. Pol. 2018. [CrossRef]
- Luzzard, T.; Hellström, A.; Lifvergren, S. Sustainability in Healthcare Organizations. In Management Innovations for Healthcare Organizations: Adopt, Abandon or Adapt? Örtenblad, A., Löfström, C.A., Sheaff, R., Eds.; Routledge: Abingdon, UK, 2016; pp. 338–358. [Google Scholar]
- Mladovsky, P.; Srivastava, D.; Cylus, J.; Karanikolos, M.; Evetovits, T.; Thomson, S.; McKee, M.; World Health Organization. Health Policy Responses to the Financial Crisis in Europe; World Health Organization, Regional Office for Europe: Copenhagen, Denmark, 2012. [Google Scholar]
- Palumbo, R. Keeping candles lit: The role of concierge medicine in the future of primary care. Health Serv. Manag. Res. 2017, 30, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P. Transparency and Spending Review: A Model for Italian Healthcare. Symphonya 2017, 17, 120–134. [Google Scholar]
- Lim, W.S.; Wong, S.F.; Leong, I.; Choo, P.; Pang, W.S. Forging a Frailty-Ready Healthcare System to Meet Population Ageing. Int. J. Environ. Res. Public Health 2017, 14, 1448. [Google Scholar] [CrossRef] [PubMed]
- Hult, K.J.; Jaffe, S.; Philipson, T.J. How Does Technological Change Affect Quality-Adjusted Prices in Health Care? Systematic Evidence from Thousands of Innovations. Am. J. Health Econ. 2017, 4, 1–21. [Google Scholar] [CrossRef]
- Martin, C.M. Complex adaptive systems approaches in health care—A slow but real emergence? J. Eval. Clin. Pract. 2018, 24, 266–268. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P. Philosophy, medicine and healthcare: Insights from the Italian experience. Health Care Anal. 2014, 22, 223–244. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P. Barriers to reforming healthcare: The Italian case. Health Care Anal. 2014, 22, 36–58. [Google Scholar] [CrossRef] [PubMed]
- Fitzgerald, L.; McDermott, A. Challenging Perspectives on Organizational Change in Health Care; Routledge: London, UK, 2017. [Google Scholar]
- Borgonovi, E.; Compagni, A. Sustaining universal health coverage: The interaction of social, political, and economic sustainability. Value Health 2013, 16, 34–38. [Google Scholar] [CrossRef] [PubMed]
- Dattée, B.; Barlow, J. Multilevel Organizational Adaptation: Scale Invariance in the Scottish Healthcare System. Org. Sci. 2017, 28, 301–319. [Google Scholar] [CrossRef]
- Mountford, N.; Geiger, S. (Re)-Organizing the evolving healthcare market: Collaborative governance in bureaucratic contexts. AOM Proc. 2018, 1. [Google Scholar] [CrossRef]
- Renedo, A.; Marston, C. Spaces for Citizen Involvement in Healthcare: An Ethnographic Study. Sociology 2015, 49, 488–504. [Google Scholar] [CrossRef] [PubMed]
- Mattei, P.; Mitra, M.; Feiler, T. The Politics of ‘Social Accountability’ in England and Germany: Democratic Control and Moral Imperatives. Public Org. Rev. 2018, 18, 399–411. [Google Scholar] [CrossRef]
- Van Gool, K.; Pearson, M. Health, Austerity and Economic Crisis: Assessing the Short-Term Impact in OECD Countries; OECD Health Working Papers, No. 76; OECD Publishing: Paris, France, 2014. [Google Scholar]
- Palumbo, R. Contextualizing co-production of health care: A systematic literature review. Int. J. Pub. Sect. Manag. 2016, 29, 72–90. [Google Scholar] [CrossRef]
- Mattila, M.; Rapeli, L. Just sick of it? Health and political trust in Western Europe. Eur. J. Pol. Res. 2018, 57, 116–134. [Google Scholar] [CrossRef]
- Buffoli, M.; Capolongo, S.; Bottero, M.; Cavagliato, E.; Speranza, S.; Volpatti, L. Sustainable healthcare: How to assess and improve healthcare structures’ sustainability. Ann. Ig 2013, 25, 411–418. [Google Scholar] [PubMed]
- Garcés, J.; Ródenas, F.; Sanjosé, V. Towards a new welfare state: The social sustainability principle and health care strategies. Health Policy 2013, 65, 201–215. [Google Scholar] [CrossRef]
- McKenzie, S. Social Sustainability: Towards Some Definitions; University of South Australia, Hawke Research Institute: Magill, Australia, 2004. [Google Scholar]
- Capolongo, S.; Bottero, M.C.; Lettieri, E.; Buffoli, M.; Bellagarda, A.; Birocchi, M.; Cavagliato, E.; Dervishaj, A.; di Noia, M.; Gherardi, G.; et al. Healthcare Sustainability Challenge. In Improving Sustainability during Hospital Design and Operation. Green Energy and Technology; Capolongo, S., Bottero, M., Buffoli, M., Lettieri, E., Eds.; Springer: Cham, Switzerland, 2015; pp. 1–9. [Google Scholar]
- Beckfield, J.; Olafsdottir, S.; Sosnaud, B. Healthcare Systems in Comparative Perspective: Classification, Convergence, Institutions, Inequalities, and Five Missed Turns. Ann. Rev. Soc. 2013, 39, 127–146. [Google Scholar] [CrossRef] [PubMed]
- Volandes, A.E.; Paasche-Orlow, M.K. Health Literacy, Health Inequality and a Just Healthcare System. Am. J. Bioeth. 2007, 7, 5–10. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, R. Examining the impacts of health literacy on healthcare costs. An evidence synthesis. Health Serv. Manag. Res. 2017, 30, 197–212. [Google Scholar] [CrossRef] [PubMed]
- Henwood, M.; Hudson, B. Lost to the System? The Impact of Fair Access to Care; UK Government Department of Health, Commission for Social Care Inspection: London, UK, 2008.
- Seeleman, C.; Essink-Bot, M.L.; Stronks, K.; Ingleby, D. How should health service organizations respond to diversity? A content analysis of six approaches. BMC Health Serv. Res. 2015, 15, 510. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P.; Adinolfi, R. Rethinking Gender and Health: Some Insights from the Italian Experience. Int. J. Men Health 2013, 12, 42–62. [Google Scholar] [CrossRef]
- Cruz, T.M. Assessing access to care for transgender and gender nonconforming people: A consideration of diversity in combating discrimination. Soc. Sci. Med. 2014, 110, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P. “Bamboccioni” and “Mammoni”? A Familistic Interpretation of Italian Men’s Unhealthy Behaviours. Int. J. Men Health 2013, 12, 63–79. [Google Scholar] [CrossRef]
- Carrasco, C. Beyond Equality: Towards a System of Non-Androcentric Indicators. In Gender and Well-Being in Europe: Historical and Contemporary Perspectives; Harris, B., Gálvez, L., Machado, H., Eds.; Routledge: London, UK, 2016; pp. 185–201. [Google Scholar]
- Bergeson, S.C.; Dean, J.D. A systems approach to patient-centered care. JAMA 2006, 296, 2848–2851. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, R.; Annarumma, C.; Musella, M.; Adinolfi, P. A recipe for excellence in health care: Investigating the relationship between health literacy, self-efficacy, awareness, and health services’ use. Sinergie Ital. J. Manag. 2018, 36. Available online: https://www.sijm.it/journal (accessed on 25 November 2018).
- Palumbo, R.; Annarumma, C.; Adinolfi, P.; Musella, M.; Piscopo, G. The Italian Health Literacy Project: Insights from the assessment of health literacy skills in Italy. Health Policy 2016, 120, 1087–1094. [Google Scholar] [CrossRef] [PubMed]
- Kickbush, I. Health literacy: An essential skill for the twenty-first century. Health Educ. 2008, 108, 101–104. [Google Scholar] [CrossRef]
- Willis, C.D.; Saul, J.E.; Bitz, J.; Pompu, K.; Best, A.; Jackson, B. Improving organizational capacity to address health literacy in public health: A rapid realist review. Public Health 2014, 128, 515–524. [Google Scholar] [CrossRef] [PubMed]
- Weaver, N.L.; Wray, R.J.; Zellin, S.; Gautam, K.J.K. Advancing Organizational Health Literacy in Health Care Organizations Serving High-Needs Populations: A Case Study. J. Health Commun. 2012, 17, 55–66. [Google Scholar] [CrossRef] [PubMed]
- Utley, R. Care and Caring Frameworks. In Frameworks for Advanced Nursing Practice and Research: Philosophies, Theories, Models, and Taxonomies; Utley, R., Henry, K., Smith, L., Eds.; Springer: New York, NY, USA, 2018; pp. 57–70. [Google Scholar]
- Palumbo, R. The Bright Side and the Dark Side of Patient Empowerment: Co-Creation and Co-Destruction of Value in the Healthcare Environment; Springer: Cham, Switzerland, 2017. [Google Scholar]
- Carnero, M.C. Assessment of Environmental Sustainability in Health Care Organizations. Sustainability 2015, 7, 8270–8291. [Google Scholar] [CrossRef]
- Jameton, A.; Pierce, J. Environment and health: 8. Sustainable health care and emerging ethical responsibilities. Can. Med. Assoc. J. 2001, 164, 365–369. [Google Scholar]
- Mohrman, S.A.; Shani, A.B. Organizing for Sustainable Healthcare; Emerald: Bingley, UK, 2012. [Google Scholar]
- Kear, R.; Whiteley, N.; Abercrombie, N. The Authority of the Consumer; Routledge: New York, NY, USA, 2005. [Google Scholar]
- Aujoulat, I.; d’Hoore, W.; Deccache, A. Patient empowerment in theory and practice: Polysemy or cacophony? Patient Educ. Couns. 2007, 66, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, R.; Annarumma, C.; Adinolfi, P.; Musella, M. The missing link to patient engagement in Italy. J. Health Organ Manag. 2016, 30, 1183–1203. [Google Scholar] [CrossRef] [PubMed]
- Bodenheimer, T.; Lorig, K.; Holman, H.; Grumbach, K. Patient Self-management of Chronic Disease in Primary Care. JAMA 2002, 288, 2469–2475. [Google Scholar] [CrossRef] [PubMed]
- Pulvirenti, M.; McMillan, J.; Lawn, S. Empowerment, patient centred care and self-management. Health Expect. 2014, 17, 303–310. [Google Scholar] [CrossRef] [PubMed]
- De Belvis, A.G.; Ferrè, F.; Specchia, M.L.; Valerio, L.; Fattore, G.; Ricciardi, W. The financial crisis in Italy: Implications for the healthcare sector. Health Policy 2012, 106, 10–16. [Google Scholar] [CrossRef] [PubMed]
- Hunter, D.J. The impact of the spending review on health and social care. Brit. Med. J. 2010, 341. [Google Scholar] [CrossRef] [PubMed]
- Kyriopoulos, I.I.; Zavras, D.; Skroumpelos, A.; Mylona, K.; Athanasakis, K.; Kyriopoulos, J. Barriers in access to healthcare services for chronic patients in times of austerity: An empirical approach in Greece. Int. J. Equity Health 2014, 13. [Google Scholar] [CrossRef] [PubMed]
- Legido-Quigley, H.; Otero, L.; la Parra, D.; Alvarez-Dardet, C.; Martin-Moreno, J.M.; McKee, M. Will austerity cuts dismantle the Spanish healthcare system? Br. Med. J. 2013, 346. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Valcarcel, B.G.; Barber, P. Economic Crisis, Austerity Policies, Health and Fairness: Lessons Learned in Spain. Appl. Health Econ. Health Policy 2017, 15, 13–21. [Google Scholar] [CrossRef] [PubMed]
- Majeed, A. Primary care in Europe: Entering the age of austerity. J. Ambul. Care Manag. 2012, 35, 162–166. [Google Scholar] [CrossRef] [PubMed]
- Bailey, D. The Environmental Paradox of the Welfare State: The Dynamics of Sustainability. New Pol. Econ. 2015, 20, 793–811. [Google Scholar] [CrossRef]
- Garrison, L.P.J. Universal Health Coverage—Big Thinking versus Big Data. Value Health 2013, 16, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Grimmeisen, S.; Frisina, L. The Role of the State in the British Healthcare System—Between Marketization and Statism. In The State and Healthcare. Transformations of the State; Rothgang, H., Cacace, M., Frisina, L., Grimmeisen, S., Schmid, A., Wendt, C., Eds.; Palgrave Macmillan: London, UK, 2010; pp. 75–118. [Google Scholar]
- Casamatta, G.; Cremer, H.; Pestieau, P. Political sustainability and the design of social insurance. J. Pub. Econ. 2000, 75, 341–364. [Google Scholar] [CrossRef]
- March, M.; Schroyen, F. Can a Mixed Health Care System Be Desirable on Equity Grounds? Scand. J. Econ. 2005, 107, 1–23. [Google Scholar] [CrossRef]
- Glimmerveen, L.; Ybema, S.; Nies, H. Empowering citizens or mining resources? The contested domain of citizen engagement in professional care services. Soc. Sci. Med. 2018, 203, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Olsen, I.T. Sustainability of Health Care: A Framework for Analysis. Health Policy Plan. 1998, 13, 287–295. [Google Scholar] [CrossRef] [PubMed]
- Borgonovi, E. Healthcare system: Issues of sustainability and economic growth. Int. Rev. Soc. Sci. 2017, 3, 231–248. [Google Scholar]
- Mintzberg, H. Rebalancing Society. Radical Renewal Beyond Left, Right, and Center; Berrett-Koehler: Oakland, CA, USA, 2014. [Google Scholar]
- Compagni, A.; Fosti, G.; Longo, F.; Tozzi, V.; Amatucci, F.; Armeni, P.; Callea, G.; Ciani, O.; Cusumano, N.; Jommi, C.; et al. SSN fast forward. Proposals to make the most effective, equitable and sustainable National Health Service. Mecosan 2016, 24, 101–124. [Google Scholar]
- Maynard, A. The Public-Private Mix for Health: Plus Ça Change, Plus C’est la Même Chose? Radcliffe Publishing: Oxford, UK, 2005. [Google Scholar]
- Maarse, H. The Privatization of Health Care in Europe: An Eight-Country Analysis. J. Health Polit. Policy Law 2006, 31, 981–1014. [Google Scholar] [CrossRef] [PubMed]
- Larson, P. Public and private values at odds: Can private sector values be transplanted into public sector institutions? Pub. Adm. Dev. 1997, 17, 131–139. [Google Scholar] [CrossRef]
- Basu, S.; Andrews, J.; Kishore, S.; Panjabi, R.; Stuckler, D. Comparative Performance of Private and Public Healthcare Systems in Low- and Middle-Income Countries: A Systematic Review. PLoS Med. 2012, 9, e1001244. [Google Scholar] [CrossRef] [PubMed]
- Roehrich, J.K.; Lewis, M.A.; George, G. Are public–private partnerships a healthy option? A systematic literature review. Soc. Sci. Med. 2014, 113, 110–119. [Google Scholar] [CrossRef] [PubMed]
- Akinci, F.; Mollahaliloğlu, S.; Gürsöz, H.; Öğücü, F. Assessment of the Turkish health care system reforms: A stakeholder analysis. Health Policy 2012, 107, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Ramirez, B.J.; West, D.M.; Costell, M. Development of a culture of sustainability in health care organizations. J. Health Organ. Manag. 2013, 27, 665–672. [Google Scholar] [CrossRef] [PubMed]
- Birch, S.; Murphy, G.T.; MacKenzie, A.; Cumming, J. In place of fear: Aligning health care planning with system objectives to achieve financial sustainability. J. Health Serv. Res. Policy 2015, 20, 109–114. [Google Scholar] [CrossRef] [PubMed]
- Adinolfi, P.; Borgonovi, E. The Myths of Health Care. Towards New Models of Leadership and Management in the Healthcare Sector; Springer: Berlin, Germany, 2018. [Google Scholar]
- Towle, A.; Godolphin, W. Patients as educators: Interprofessional learning for patient-centred care. Med. Teach. 2013, 35, 219–225. [Google Scholar] [CrossRef] [PubMed]
- Frow, P.; McColl-Kennedy, J.R.; Payne, A. Co-creation practices: Their role in shaping a health care ecosystem. Ind. Mark. Manag. 2016, 56, 24–39. [Google Scholar] [CrossRef]
| Focus of Interventions | Time Span | Illustrative Examples | Potential Side Effects in Terms of Sustainability |
|---|---|---|---|
| Financial and/or economic sustainability | Short term: balancing of financial/economic inflows and outflows to improve the health care system’s viability | Cuts to health care expenditures, reduction of hospital beds; freeze of staff turnover; spending review; rationalization of health services | Impaired social sustainability due to drawbacks in fair access to health services; negative effects on political sustainability generated by shrinking trust in political institutions |
| Political sustainability | Medium term: consensus maximization across the various stakeholders interested in the appropriate functioning of the health care system | Alignment of potentially conflicting political parties’ interests, such as lower waiting times, increased quality care, and reduction in health-related costs | Direct and indirect negative consequences on the financial and economic equilibria of health care organizations; drawbacks in social sustainability due to lower equity in the access to care |
| Social sustainability | Long term: optimizing the satisfaction of stakeholders’ current interests without compromising the freedom of future generations | Enhancement of equality and diversity in the access to care through increased interconnectedness and greater patients’ participation | Increased health-related costs and deterioration of financial sustainability; mounting conflicts between divergent political parties’ interests |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Borgonovi, E.; Adinolfi, P.; Palumbo, R.; Piscopo, G. Framing the Shades of Sustainability in Health Care: Pitfalls and Perspectives from Western EU Countries. Sustainability 2018, 10, 4439. https://doi.org/10.3390/su10124439
Borgonovi E, Adinolfi P, Palumbo R, Piscopo G. Framing the Shades of Sustainability in Health Care: Pitfalls and Perspectives from Western EU Countries. Sustainability. 2018; 10(12):4439. https://doi.org/10.3390/su10124439
Chicago/Turabian StyleBorgonovi, Elio, Paola Adinolfi, Rocco Palumbo, and Gabriella Piscopo. 2018. "Framing the Shades of Sustainability in Health Care: Pitfalls and Perspectives from Western EU Countries" Sustainability 10, no. 12: 4439. https://doi.org/10.3390/su10124439
APA StyleBorgonovi, E., Adinolfi, P., Palumbo, R., & Piscopo, G. (2018). Framing the Shades of Sustainability in Health Care: Pitfalls and Perspectives from Western EU Countries. Sustainability, 10(12), 4439. https://doi.org/10.3390/su10124439





