Additively Manufactured Commercial Co-Cr Dental Alloys: Comparison of Microstructure and Mechanical Properties
Abstract
:1. Introduction
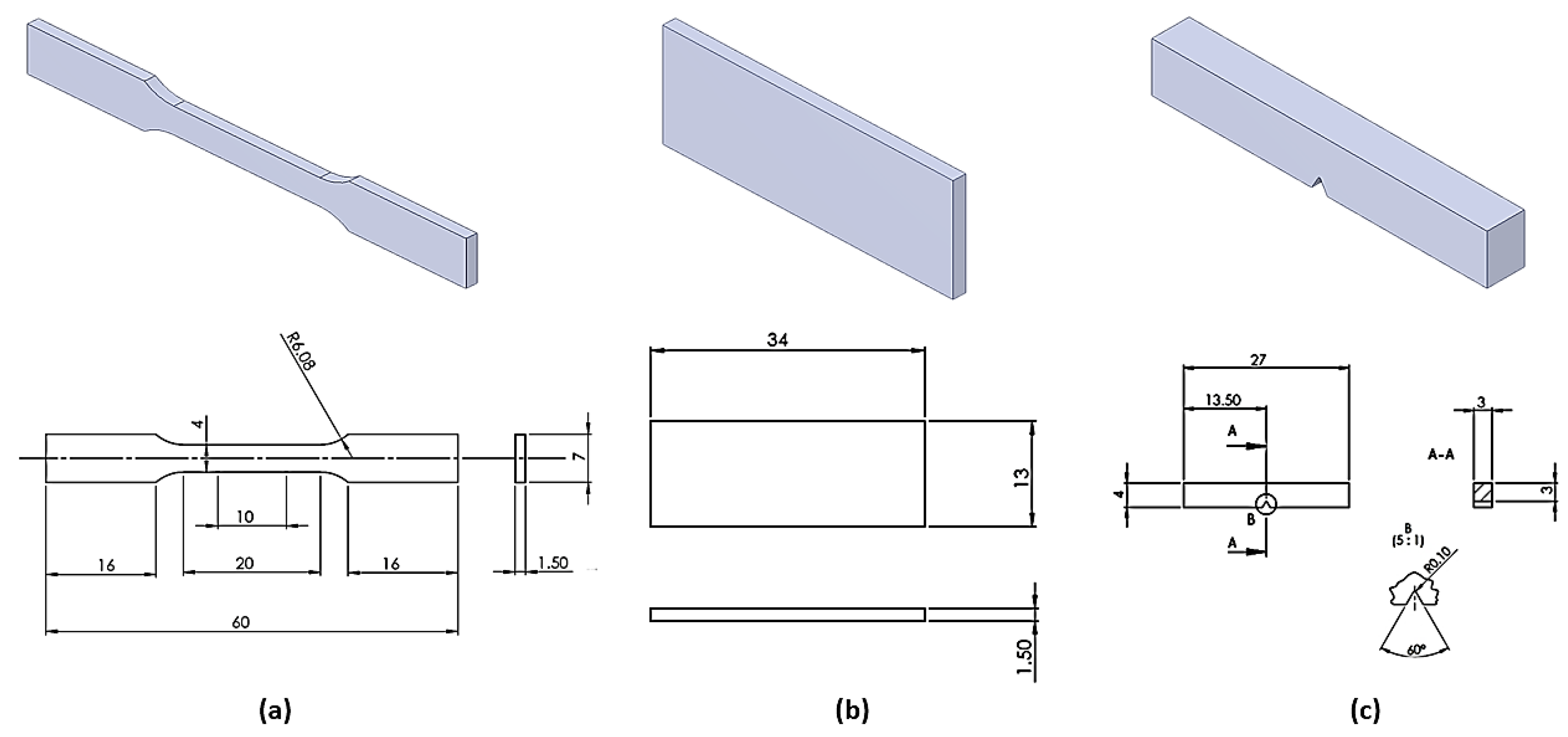
2. Materials and Methods
3. Results
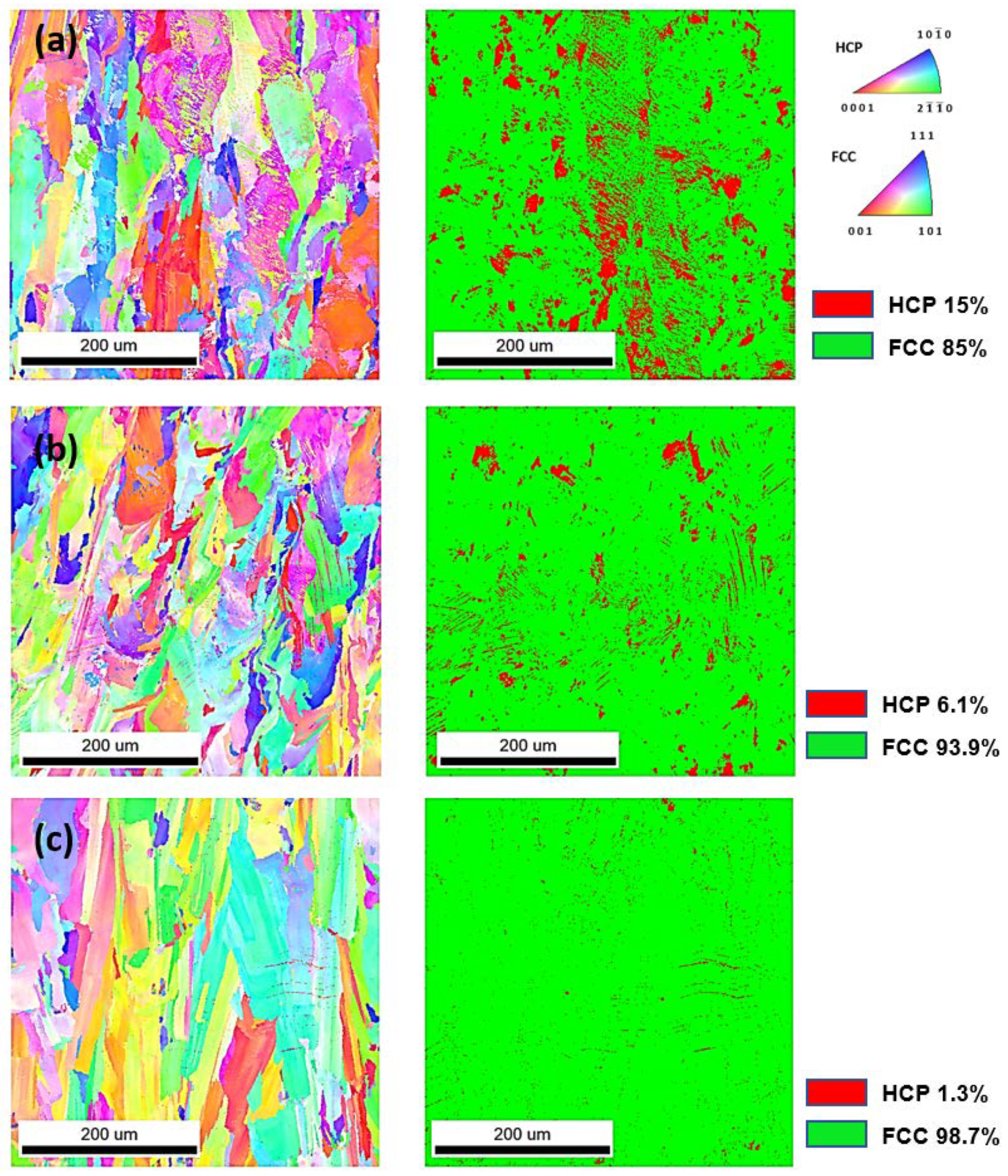
Microstructure Analysis
4. Discussion
5. Conclusions
- The mechanical properties of Co-Cr specimens made on Sysma MySint 100, EOS M100, and 3D Systems DMP Dental 100 are comparable or even better than the mechanical properties of Co-Cr specimens produced by the conventional routes, which are casting and milling (CNC) technologies (except for elongation ε, on Sysma MySint 100 and EOS M100).
- The results of the current study demonstrate that the tested specimens meet at least the type 5 criteria in mechanical properties according to the EN ISO 22674:2016 (Rp0.2 ≥ 500 MPa and ε ≥ 2%), except the Sysma Mysint100 specimens for elongation ε.
- The highest elongation ε (8.1 ± 1.5%), flexural strength RfM (2548 ± 54.3 MPa), and toughness CVN (0.61 ± 0.01 J) have specimens produced by 3D Systems DMP Dental 100 (highest content of Cr (29.1 ± 0.2 wt %) and C (0.015 ± 0.002 wt %) without higher content of W (0.19 ± 0.01 wt %) leads to formatting more Cr23C6 carbides, which determine the higher proportion of γ phase (FCC) and better mechanical properties).
- The highest tensile strength Rm (1370 ± 13.6 MPa), yield strength Rp0.2 (1370 ± 13.6 Mpa), and the microhardness HV0.2 in cross-section (770 ± 80) and longitudinal-section (719 ± 59) have the specimens made on the EOS M100 (the higher HCP (ε phase) amount contributes to higher hardness and mechanical properties such as Rm and Rp0.2 but decreases elongation ε–W (5.6 ± 0.09 wt %) and Mo (5.3 ± 0.08 wt %), leading to formatting Co3W and Co3Mo intermetallic HCP phase).
- Microstructural analyses show the highest HCP amount of 15% (ε phase) in Sysma MySint100 specimens (higher content of C (0.008 ± 0.001 wt %) leads to formatting Cr7C3 (ε phase), MoC, and WC carbides, which leads to decreasing mechanical properties (especially elongation ε), which causes lower mechanical properties compared to the other two AM-produced materials).
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dolgov, N.A.; Ts, D.; Dzh, D.; Pavlova, D.; Simov, M. Mechanical properties of dental CO-CR alloys fabricated via Casting and selective laser melting, Scientific Proceedings Ii International Scientific-Technical Conference “Innovations In Engineering”. Mater. Sci. Non-Equilib. Phase Transform. 2016, 2, 3–7. [Google Scholar]
- Ţălu, Ş.; Stach, S.; Klaić, B.; Čelebić, A. Evaluation of Topographical Co-Cr-Mo Alloy Surface Changes After Various Finishing Treatments. Acta Stomatol. Croat. 2019, 53, 264–273. [Google Scholar] [CrossRef]
- Han, X.; Sawada, T.; Schille, C.; Schweizer, E.; Scheideler, L.; Geis-Gerstorfer, J.; Spintzyk, S. Comparative Analysis of Mechanical Properties and Metal-Ceramic Bond Strength of Co-Cr Dental Alloy Fabricated by Different Manufacturing Processes. Materials 2018, 11, 1801. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gene’va, S. Dentistry—Metallic Materials for Fixed and Removable Restorations and Appliances; EN ISO 22674:2016; European Committee for Standardization: Brussels, Belgium, 2015. [Google Scholar]
- Dikova, T. Properties of Co-Cr Dental Alloys Fabricated Using Additive Technologies. Biomater. Regen. Med. 2018, 141–159. [Google Scholar] [CrossRef] [Green Version]
- Maltar, M.; Miloš, L.; Milardović, S.; Kovačić, I.; Peršić, S.; Juroš, I.; Kranjčić, J. Attitudes of the Students from the School of Dental Medicine in Zagreb towards CAD/CAM. Acta Stomatol. Croat. 2018, 52, 322–329. [Google Scholar] [CrossRef]
- Attar, H.; Calin, M.; Zhang, L.C.; Scudino, S.; Eckert, J. Manufacture by selective laser melting and mechanical behavior of commercially pure titanium. Mater. Sci. Eng. A 2014, 593, 170–177. [Google Scholar] [CrossRef]
- Zhou, Y.; Wei, W.; Yan, J.; Liu, W.; Li, N.; Li, H.; Xu, S. Microstructures and metal-ceramic bond properties of Co-Cr biomedical alloys fabricated by selective laser melting and casting. Mater. Sci. Eng. A 2019, 759, 594–602. [Google Scholar] [CrossRef]
- Tasopoulos, T.; Kouveliotis, G.; Polyzois, G.; Karathanasi, V. Fabrication of a 3D Printing Definitive Obturator Prosthesis: A Clinical Report. Acta Stomatol. Croat. 2017, 51, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Dai, N.; Zhong, Y.; Liu, H.; Yuan, F.; Sun, Y. Digital modeling technology for full dental crown tooth preparation. Comput. Biol. Med. 2016, 71, 190–197. [Google Scholar] [CrossRef]
- Liu, J.; Liu, Y.; Wang, J.; Zuo, X.; Wang, X.; Zhang, Y.; He, H. Dental measurements based on a three-dimensional digital technique: A comparative study on reliability and validity. Arch. Oral Biol. 2021, 124, 105059. [Google Scholar] [CrossRef]
- Peng, M.; Li, C.; Huang, C.; Liang, S. Digital technologies to facilitate minimally invasive rehabilitation of a severely worn dentition: A dental technique. J. Prosthet. Dent. 2020, 126, 167–172. [Google Scholar] [CrossRef] [PubMed]
- Yoon, S.; Jung, H.J.; Knowles, J.C.; Lee, H.H. Digital image correlation in dental materials and related research: A review. Dent. Mater. 2021, 37, 758–771. [Google Scholar] [CrossRef]
- Torabi, K.; Farjood, E.; Hamedani, S. Rapid prototyping technologies and their applications in prosthodontics, Review of Literature. J. Dent. 2015, 16, 1–9. [Google Scholar]
- Ucar, Y.; Akova, T.; Akyil, M.S.; Brantley, W.A. Internal fit evaluation of crowns prepared using a new dental crown fab-rication technique: Laser-sintered Co-Cr crowns. J. Prosthet. Dent. 2009, 102, 253–259. [Google Scholar] [CrossRef]
- Tonelli, L.; Fortunato, A.; Ceschini, L. CoCr alloy processed by Selective Laser Melting (SLM): Effect of Laser Energy Density on microstructure, surface morphology, and hardness. J. Manuf. Process. 2020, 52, 106–119. [Google Scholar] [CrossRef]
- Park, C.; Kee, W.; Lim, H.-P.; Park, S.-W. Combining 3D-printed metal and resin for digitally fabricated dentures: A dental technique. J. Prosthet. Dent. 2019, 123, 389–392. [Google Scholar] [CrossRef] [PubMed]
- Di Fiore, A.; Meneghello, R.; Graiff, L.; Savio, G.; Vigolo, P.; Monaco, C.; Stellini, E. Full arch digital scanning systems performances for implant-supported fixed dental prostheses: A comparative study of 8 intraoral scanners. J. Prosthodont. Res. 2019, 63, 396–403. [Google Scholar] [CrossRef]
- Leeson, D. The digital factory in both the modern dental lab and clinic. Dent. Mater. 2019, 36, 43–52. [Google Scholar] [CrossRef]
- Viderščak, D.; Šolić, S.; Schauperl, Z.; Godec, M.; Ćatić, A.; Črtomir, D.; Paulin, I. The Influence of Machine Type on Microstructure and Mechanical Properties of 3D Printed Commercial Co-Cr Dental Alloy. In Proceedings of the Euro PM2020 Congress & Exhibition/European Powder Metallurgy Association (EPMA), Lisbon, Portugal, 5–7 July 2020. [Google Scholar]
- Koutsoukis, T.; Zinelis, S.; Eliades, G.; Al-Wazzan, K.; Rifaiy, M.A.; Al Jabbari, Y.S. Selective Laser Melting Technique of Co-Cr Dental Alloys: A Review of Structure and Properties and Comparative Analysis with Other Available Techniques. J. Prosthodont. 2015, 24, 303–312. [Google Scholar] [CrossRef] [PubMed]
- Bellefontaine, G. The Corrosion of CoCrMo Alloys for Biomedical Applications. Ph.D. Thesis, School of Metallurgy and Materials, University of Birmingham, Birmingham, UK, January 2010. [Google Scholar]
- Podrrez-Radziszewska, M.; Haimann, K.; Dudzinski, W.; Morawska-Soltysik, M. Characteristic of intermetallic phases in cast dental CoCrMo alloy. Arch. Foundry Eng. 2010, 10, 51–59. [Google Scholar]
- Gupta, P. The Co-Cr-Mo (Cobalt-Chromium-Molybdenum) system. J. Phase Equilibria Diffus. 2005, 26, 87–92. [Google Scholar] [CrossRef]
- Crook, P. Metals Handbook. Nonferrous Alloys and Special-Purpose Materials; Ohio American Society for Metals; ASM International: Materials Park, OH, USA, 1990; 447p. [Google Scholar]
- Wang, J.-H.; Ren, J.; Liu, W.; Wu, X.-Y.; Gao, M.-X.; Bai, P.-K. Effect of Selective Laser Melting Process Parameters on Microstructure and Properties of Co-Cr Alloy. Materials 2018, 11, 1546. [Google Scholar] [CrossRef] [Green Version]
- Takaichi, A.; Suyalatu, T.; Nakamoto, N.; Joko, N.; Nomura, Y.; Tsutsumi, S.; Migita, H.; Doi, S.; Kurosu, A.; Chiba, N.; et al. Microstructures and mechanical properties of Co–29Cr–6Mo alloy fabricated by selective laser melting process for dental applications. Mech. Behav. Biomed. Mater. 2013, 21, 67–76. [Google Scholar] [CrossRef] [PubMed]
- Al Jabbari, Y.S. Physico-mechanical properties and prosthodontic applications of Co-Cr dental alloys: A review of the literature. J. Adv. Prosthodont. 2014, 6, 138–145. [Google Scholar] [CrossRef] [Green Version]
- Ni, J.; Ling, H.; Zhang, S.; Wang, Z.; Peng, Z.; Benyshek, C.; Zan, R.; Miri, A.K.; Li, Z.; Zhang, X.; et al. Three-Dimensional Printing of Metals for Biomedical Applications. Mater. Today Bio 2019, 3, 100024. [Google Scholar] [CrossRef]
- Mergulhão, M.V.; Podestá, C.E.; das Neves, M.D.M. Perspective of Additive Manufacturing Selective Laser Melting in Co-Cr-Mo Alloy in the Consolidation of Dental Prosthesis. Biomater. Regen. Med. 2017, 161–185. [Google Scholar] [CrossRef] [Green Version]
- Zhou, Y.; Li, N.; Yan, J.; Zeng, Q. Comparative analysis of the microstructures and mechanical properties of Co-Cr dental alloys fabricated by different methods. J. Prosthet. Dent. 2018, 120, 617–623. [Google Scholar] [CrossRef] [PubMed]
- Chauhan, M. Microstructural Characterization of Cobalt Chromium (ASTM F75) Cubes Produced by EBM Technique. Master’s Thesis, SE—412 96 Gothenburg, Chalmers University of Technology, Gothenburg, Sweden, 2017. [Google Scholar]
- Konieczny, B.; Szczesio-Wlodarczyk, A.; Sokolowski, J.; Bociong, K. Challenges of Co-Cr Alloy Additive Manufacturing Methods in Dentistry—The Current State of Knowledge (Systematic Review). Materials 2020, 13, 3524. [Google Scholar] [CrossRef] [PubMed]
- Donik, Č.; Kraner, J.; Paulin, I.; Godec, M. Influence of the Energy Density for Selective Laser Melting on the Microstructure and Mechanical Properties of Stainless Steel. Metals 2020, 10, 919. [Google Scholar] [CrossRef]
- Øilo, M.; Nesse, H.; Lundberg, O.J.; Gjerdet, N.R. Mechanical properties of cobalt-chromium 3-unit fixed dental prostheses fabricated by casting, milling, and additive manufacturing. J. Prosthet. Dent. 2018, 120, 156.e1–156.e7. [Google Scholar] [CrossRef]
- Yan, X.; Jiang, R.; Li, W.; Lin, H. Oriented face-centered cubic to hexagonal close-packed martensitic transition, grain morphology, and mechanical properties of Co-Cr alloy fabricated by selective laser melting. J. Prosthet. Dent. 2020. [Google Scholar] [CrossRef] [PubMed]
- Kok, Y.; Tan, X.P.; Wang, P.; Nai, M.L.S.; Loh, N.H.; Liu, E.; Tor, S.B. Anisotropy and heterogeneity of mi-crostructure and mechanical properties in metal additive manufacturing: A critical review. Mater. Des. 2018, 139, 565–586. [Google Scholar] [CrossRef]


| Machine | Co-Cr Powder Type | Powder Chemical Composition (wt %) |
|---|---|---|
| Sysma MySint100 | Wirobond C+ | Co (63.9), Cr (24.7), W (5.4), Mo (5.0), Si (<1.0) |
| EOS M100 | Cobalt Chrome SP2 | Co (63.8), Cr (24.7), Mo (5.1), W (5.4), Si (1), other (<1.0) |
| 3D Systems DMP Dental 100 | Laser Form CoCr (B) | Co (bal.), Cr (28.0–30.0), Mo (5.0–6.0), Si (0.0–1.0), Mn (0.0–1.0), Fe (0.0–0.5), C (0.0–0.02) |
| Type of Mechanical Test | Mechanical Property | Sysma MySint 100 | EOS M100 | 3D Systems DMP Dental 100 | |
|---|---|---|---|---|---|
| Static tensile test | Elongation ε/% | 0.33 ± 0.1 a | 4.90 ± 1.1 b | 8.1 ± 1.5 c | |
| Tensile Strength Rm/MPa | 1112 ± 123.7 a | 1370 ± 13.6 b | 1016 ± 61.7 a | ||
| Yield Strength Rp0.2/MPa | 834 ± 62 a | 1061 ± 21 b | 822 ± 43 a | ||
| 3-point bending test | RfM/MPa | 2059 ± 251.9 a | 2527 ± 92.7 b | 2548 ± 54.3 b | |
| (Impact) Toughness | CVN/J | 0.26 ± 0.02 a | 0.27 ± 0.03 a | 0.61 ± 0.01 b | |
| Microhardness | HV0.2 | Cross-section | 568 ± 27 a | 770 ± 80 b | 513 ± 12 a |
| Longitudinal-section | 554 ± 8 a | 719 ± 59 b | 587 ± 44 a | ||
| Machine | Chemical Composition (wt %) |
|---|---|
| Sysma MySint100 | Co (bal.), Cr (24.6 ± 0.2), W (5.7 ± 0.08), Mo (5.3 ± 0.08), Fe (0.19 ± 0.01), Mn (0.05 ± 0.002), C (0.008 ± 0.001) |
| EOS M100 | Co (bal.), Cr (24.8 ± 0.2), W (5.6 ± 0.09), Mo (5.3 ± 0.08), Fe (0.05 ± 0.003), Mn (< 0.01), C (0.005 ± 0.001) |
| 3D Systems DMP Dental 100 | Co (bal.), Cr (29.1 ± 0.2), W (0.19 ± 0.02), Mo (5.3 ± 0.2), Fe (0.19 ± 0.01), Mn (0.71 ± 0.02), C (0.015 ± 0.002) |
| Property | Milled (CNC) | Cast | SLM | EN ISO 22674:2016 |
|---|---|---|---|---|
| Tensile Strength Rm/MPa | 638 ± 25 [31] 1069 ± 10 [3] | 450 [30] 520 ± 30 [31] 783 ± 32 [3] | 1072 ± 18 [31] 1158 ± 10 [3] 1200 ± 24 [36] | - |
| Yield Strength Rp0.2/MPa | 495 ± 20 [31] 672 ± 4 [3] | 581 ± 16 [3] 655 [37] 658 ± 44 [31] | 783 ± 15 [3] 790 ± 11 [31] 870 ± 26 [35] | ≥500 |
| Elongation ε/% | 10 ± 1 [3] 11.1 ± 1 [31] | 8 [37] 8 ± 0.4 [31] 12 ± 2 [3] | 8.7 ± 1.06 [36] 12.7 ± 1.9 [31] 13 ± 1 [3] | ≥2 |
| 3-point bending test RfM/MPa | - | 1136 ± 1 [30] | 2501 ± 9.7 [30] | - |
| Hardness HV10 | 264 ± 11 [35] 325 ± 18 [31] 353 ± 6 [3] | 270 ± 16 [35] 303 ± 15 [3] 324 ± 27 [31] | 399 ± 24 [3] 466 ± 13 [35] 475 ± 10 [31] | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Viderščak, D.; Schauperl, Z.; Šolić, S.; Ćatić, A.; Godec, M.; Kocijan, A.; Paulin, I.; Donik, Č. Additively Manufactured Commercial Co-Cr Dental Alloys: Comparison of Microstructure and Mechanical Properties. Materials 2021, 14, 7350. https://doi.org/10.3390/ma14237350
Viderščak D, Schauperl Z, Šolić S, Ćatić A, Godec M, Kocijan A, Paulin I, Donik Č. Additively Manufactured Commercial Co-Cr Dental Alloys: Comparison of Microstructure and Mechanical Properties. Materials. 2021; 14(23):7350. https://doi.org/10.3390/ma14237350
Chicago/Turabian StyleViderščak, Dalibor, Zdravko Schauperl, Sanja Šolić, Amir Ćatić, Matjaž Godec, Aleksandra Kocijan, Irena Paulin, and Črtomir Donik. 2021. "Additively Manufactured Commercial Co-Cr Dental Alloys: Comparison of Microstructure and Mechanical Properties" Materials 14, no. 23: 7350. https://doi.org/10.3390/ma14237350
APA StyleViderščak, D., Schauperl, Z., Šolić, S., Ćatić, A., Godec, M., Kocijan, A., Paulin, I., & Donik, Č. (2021). Additively Manufactured Commercial Co-Cr Dental Alloys: Comparison of Microstructure and Mechanical Properties. Materials, 14(23), 7350. https://doi.org/10.3390/ma14237350









