Deterioration of Performance Status during Palliative Radiotherapy Suggests a Significant Short Survival Duration: Indicating the Necessities for Considering Radiotherapy Discontinuation
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethical Statement
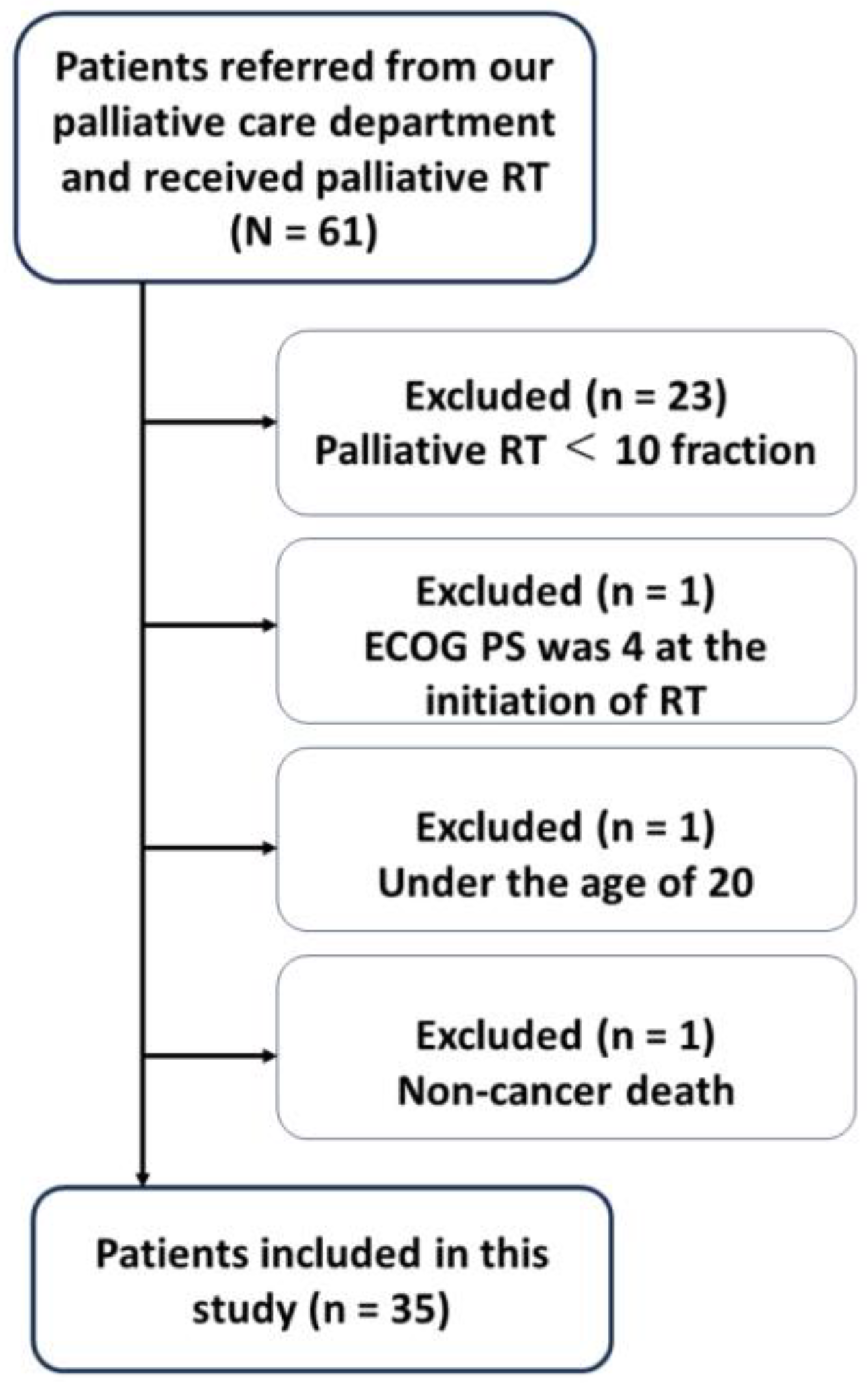
2.2. Patients
2.3. Radiotherapy
2.4. Statistical Analysis
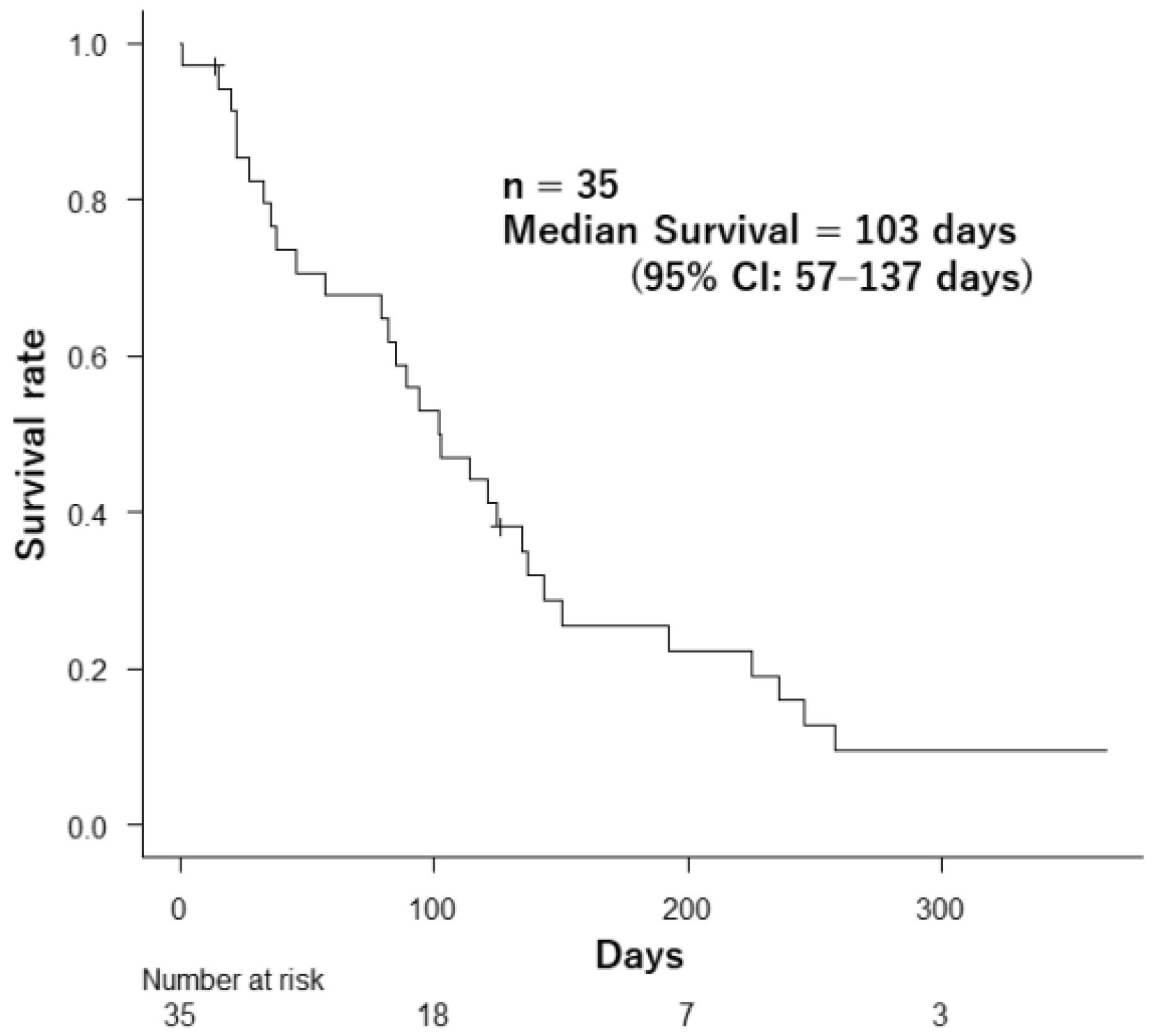
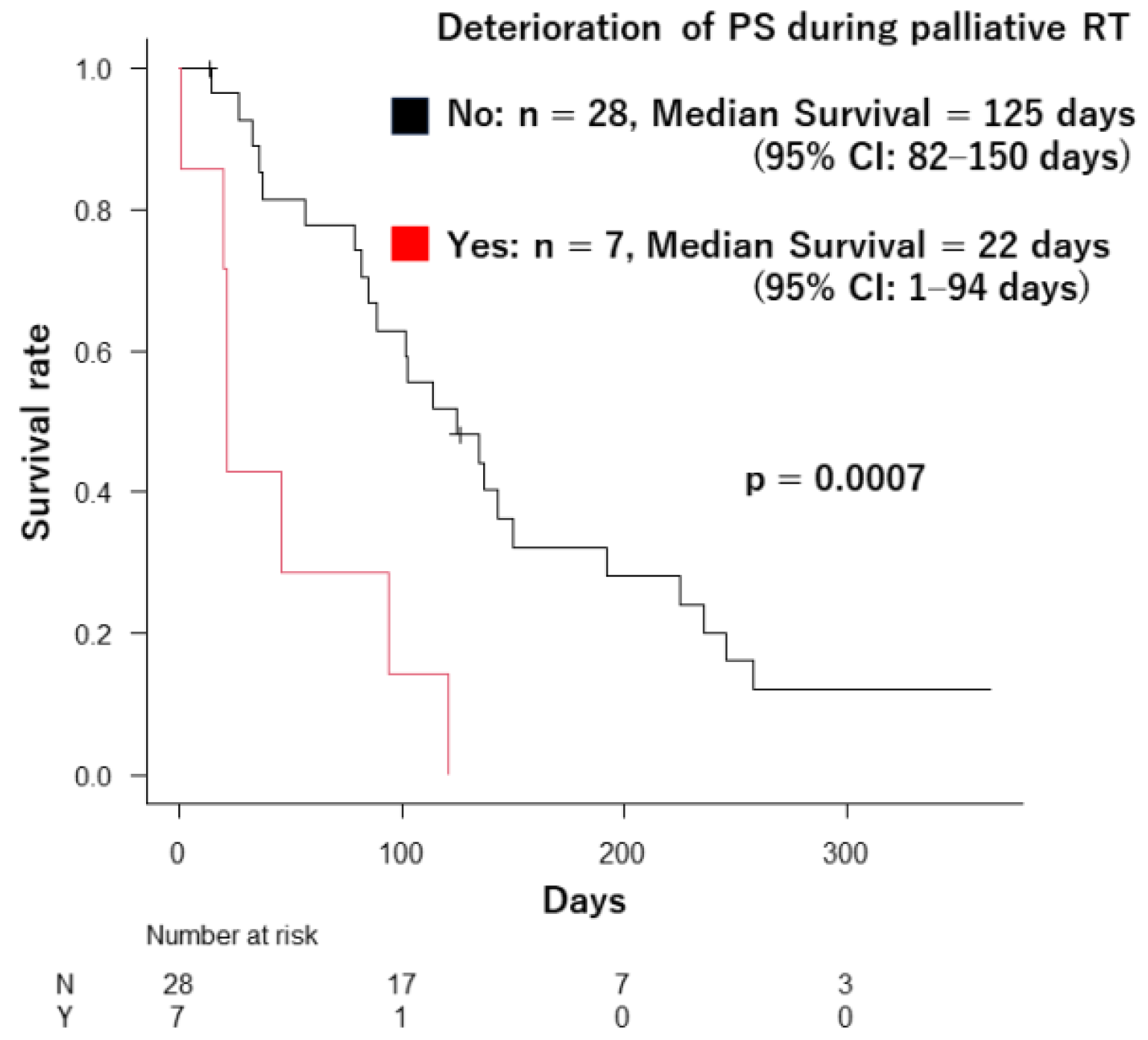
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Fallon, M.; Giusti, R.; Aielli, F.; Hoskin, P.; Rolke, R.; Sharma, M.; Ripamonti, C.I.; ESMO Guidelines Committee. Management of cancer pain in adult patients: ESMO Clinical Practice Guidelines. Ann. Oncol. 2018, 29 (Suppl. S4), iv166–iv191. [Google Scholar] [CrossRef] [PubMed]
- Temel, J.S.; Greer, J.A.; Muzikansky, A.; Gallagher, E.R.; Admane, S.; Jackson, V.A.; Dahlin, C.M.; Blinderman, C.D.; Jacobsen, J.; Pirl, W.F.; et al. Early palliative care for patients with metastatic non-small-cell lung cancer. N. Engl. J. Med. 2010, 363, 733–742. [Google Scholar] [CrossRef] [PubMed]
- Rich, S.E.; Chow, R.; Ramen, S.; Zeng, K.L.; Lutz, S.; Lam, H.; Silva, M.F.; Chow, E. Update of the systematic review of palliative radiation therapy fractionation for bone metastases. Radioether. Oncol. 2018, 126, 547–557. [Google Scholar] [CrossRef] [PubMed]
- Saito, T.; Yamaguchi, K.; Toya, R.; Oya, N. Single- versus multiple-fraction radiation therapy for painful bone metastases: A systematic review and meta-analysis of nonrandomized studies. Adv. Radiat. Oncol. 2019, 4, 706–715. [Google Scholar] [CrossRef]
- Gardner, K.; Laird, B.J.A.; Fallon, M.T.; Sande, T.A. A systematic review examining clinical markers and biomarkers of analgesic response to radiotherapy for cancer-induced bone pain. Crit. Rev. Oncol. Hematol. 2019, 133, 33–44. [Google Scholar] [CrossRef] [PubMed]
- Westhoff, P.G.; de GRaeff, A.; Monninkhof, E.M.; Pomp, J.; Vulpen, M.; Leer, J.W.H.; Marijnen, C.A.M.; Linden, Y.M.; Dutch Bone Metastasis Study Group. Quality of life in relation to pain response to radiation therapy for painful bone metastases. Int. J. Radiat. Oncol. Biol. Phys. 2015, 93, 694–701. [Google Scholar] [CrossRef] [PubMed]
- Lutz, S.T.; Jones, J.; Chow, E. Role of radiation therapy in palliative care of the patient with cancer. J. Clin. Oncol. 2014, 32, 2913–2919. [Google Scholar] [CrossRef] [PubMed]
- Nieder, C.; Tollåli, T.; Haukland, E.; Reigstad, A.; Flatoy, L.R.; Engljahringer, K. Impact of early palliative interventions on the outcomes of care for patients with non-small cell lung cancer. Support. Care Cancer 2016, 24, 4385–4391. [Google Scholar] [CrossRef] [PubMed]
- WHO. Cancer pain relief and palliative care: Reports of a WHO expert committee. World Health Organ. Tech. Rep. Ser. 1990, 804, 1–75. [Google Scholar]
- van Oorschot, B.; Rades, D.; Schulze, W.; Beckmann, G.; Feyer, P. Palliative radiotherapy—New approaches. Semin. Oncol. 2011, 38, 443–449. [Google Scholar] [CrossRef]
- Murphy, J.D.; Nelson, L.M.; Chang, D.T.; Mell, L.K.; Le, Q.T. Patterns of care in palliative radiotherapy: A population-based study. J. Oncol. Pract. 2013, 9, e220–e227. [Google Scholar] [CrossRef] [PubMed]
- van Oorschot, B.; Schuler, M.; Simon, A.; Schleicher, U.; Geinitz, H. Patterns of care and course of symptoms in palliative radiotherapy: A multicenter pilot study analysis. Strahlenther. Onkol. 2011, 187, 461–466. [Google Scholar] [CrossRef] [PubMed]
- Gaspar, L.; Scott, C.; Rotman, M.; Asbell, S.; Phillips, T.; Wasserman, T.; Mckenna, W.G.; Byhardt, R. Recursive partitioning analysis (RPA) of prognostic factors in three radiation oncology group (RTOG). Int. J. Radiat. Oncol. Biol. Phys. 1997, 37, 745–751. [Google Scholar] [CrossRef] [PubMed]
- American Society for Therapeutic Radiology and Oncology. National Quality Forum. NQF #1822 External Beam Radiotherapy for Bone Metastases. Available online: https://www.astro.org/uploadedFiles/_MAIN_SITE/Daily_Practice/Medicare_Incentives/Merit-based_Incentive_Program/Content_Pieces/1822ASTRO.pdf (accessed on 5 December 2023).
- Halla, S.Ó.; Fredrik, K.; Nelson, N.; Gabriella, A.D. Short-course compared to long-course palliative radiotherapy for oesophageal cancer: A single centre observational cohort study. Radiat. Oncol. 2021, 16, 153. [Google Scholar]
- Saito, T.; Kosugi, T.; Nakamura, N.; Wada, H.; Tonari, A.; Ogawa, H.; Matsuhashi, N.; Yamada, K.; Takahashi, T.; Ito, K.; et al. Treatment response after palliative radiotherapy for bleeding gastric cancer: A multicenter prospective observational study (JROSG 17-3). Gastric Cancer 2022, 25, 411–421. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.S.-Y.; Wong, R.; Johnston, M.; Bezjak, A.; Whelan, T.; Cancer Care Ontario Practice Guidelines Initiative Supportive Care Group. Meta-analysis of dose-fractionation radiotherapy trials for the palliation of painful bone metastases. Int. J. Radiat. Oncol. Biol. Phys. 2003, 55, 594–605. [Google Scholar] [CrossRef] [PubMed]
- Rades, D.; Stalpers, L.J.A.; Veninga, T.; Schulte, R.; Hoskin, P.J.; Obralic, N.; Bajrovic, A.; Rudat, V.; Schwarz, R.; Hulshof, M.C.; et al. Evaluation of five radiation schedules and prognostic factors for metastatic spinal cord compression. J. Clin. Oncol. 2005, 23, 3366–3375. [Google Scholar] [CrossRef]
- Hartsell, W.F.; Scott, C.B.; Bruner, D.W.; Scarantino, C.W.; Ivker, R.A.; Mack, R.; Suh, J.H.; Demas, W.F.; Movsas, B.; Petersen, I.A.; et al. Randomized trial of short- versus long-course radiotherapy for palliation of painful bone metastases. J. Natl. Cancer Inst. 2005, 97, 798–804. [Google Scholar] [CrossRef]
- Morita, T.; Tsunoda, J.; Inoue, S.; Chihara, S. The palliative prognostic index: A scoring system for survival prediction of terminally ill cancer patients. Support. Care Cancer 1999, 7, 128–133. [Google Scholar] [CrossRef]
- Katagiri, H.; Okada, R.; Takagi, T.; Takahashi, M.; Harada, H.; Nishimura, T.; Asakura, H.; Ogawa, H. New prognostic factors and scoring system for patients with skeletal metastasis. Cancer Med. 2014, 3, 1359–1367. [Google Scholar] [CrossRef]
- Sperduto, P.W.; Mesko, S.; Li, J.; Cagney, D.; Aizer, A.; Lin, N.U.; Nesbit, E.; Kruser, T.J.; Chan, J.; Braunstein, S.; et al. Survival in patients with brain metastases: Summary report on the updated diagnosis-specific graded prognostic assessment and definition of the eligibility quotient. J. Clin. Oncol. 2020, 38, 3773–3784. [Google Scholar] [CrossRef] [PubMed]
- Chow, E.; Abdolell, M.; Panzarella, T.; Harris, K.; Bezjak, A.; Warde, P.; Tannock, I. Validation of a predictive model for survival in metastatic cancer patients attending an outpatient palliative radiotherapy clinic. Int. J. Radiat. Oncol. Biol. Phys. 2009, 73, 280–287. [Google Scholar] [CrossRef] [PubMed]
- Janssen, S.; Van Oorschot, B.; Käsmann, L.; Schild, S.E.; Rades, D. Validation of a score developed to estimate the 6-month survival of patients treated with palliative local radiotherapy for advanced lung cancer. Anticancer Res. 2017, 37, 2537–2540. [Google Scholar] [CrossRef] [PubMed]
- Rades, D.; Manig, L.; Janssen, S.; Schild, S.E. A survival score for patients assigned to palliative radiotherapy for metastatic bladder cancer. Anticancer Res. 2017, 37, 1481–1484. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Rades, D.; Bolm, L.; Schild, S.E.; Bartscht, T. Survival following palliative external-beam radiotherapy of locally advanced and metastatic liver cancer. Anticancer Res. 2017, 37, 203–206. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nieder, C.; Kämpe, T.A.; Pawinski, A.; Dalhaug, A. Patient-reported symptoms before palliative radiotherapy predict survival differences. Strahlenther. Onkol. 2018, 194, 533–538. [Google Scholar] [CrossRef] [PubMed]
- Zeng, L.; Zhang, L.; Culleton, S.; Jon, F.; Holden, L.; Kwong, J.; Khan, L.; Tsao, M.; Danjoux, C.; Sahgal, A.; et al. Edmonton symptom assessment scale as a prognosticative indicator in patients with advanced cancer. J. Palliat. Med. 2011, 14, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Jones, J.A.; Lutz, S.T.; Chow, E.; Johnstone, P.A. Palliative radiotherapy at the end of life: A critical review. CA Cancer J. Clin. 2014, 64, 296–310. [Google Scholar] [CrossRef] [PubMed]
- Nieder, C.; Angelo, K.; Dalhaug, A.; Pawinski, A.; Haukland, E.; Norum, J. Palliative radiotherapy during the last month of life: Predictability for referring physicians and radiation oncologists. Oncol. Lett. 2015, 10, 3043–3049. [Google Scholar] [CrossRef]
- Guadagnolo, B.A.; Liao, K.P.; Elting, L.; Giordano, S.; Buchholz, T.A.; Shin, Y.C. Use of radiation therapy in the last 30 days of life among a large population-based cohort of elderly patients in the United States. J. Clin. Oncol. 2013, 31, 80–87. [Google Scholar] [CrossRef]
- Franklin, J.B.; Joseph, P.W.; Nicki, D.V. Delivering bad or life-altering news. Am. Fam. Physician 2018, 98, 99–104. [Google Scholar]
- Gebhardt, C.; Gorba, C.; Karin, O.; Vehling, S.; Koch, U.; Mehnert, A. Breaking bad news to cancer patients: Content, communication preferences and psychological distress. Psychother. Psychosom. Med. Psychol. 2017, 67, 312–321. [Google Scholar]
- Reeve, E.; Thompson, W.; Farrell, B. Deprescribing: A narrative review of the evidence and practical recommendations for recognizing opportunities and taking action. Eur. J. Intern. Med. 2017, 38, 3–11. [Google Scholar] [CrossRef] [PubMed]
- Ailabouni, N.J.; Nishtala, P.S.; Mangin, D.; Tordoff, J. Challenges and enablers of deprescribing: A general practitioner perspective. PLoS ONE 2016, 11, e0151066. [Google Scholar] [CrossRef]
- Kuosmanen, L.; Hupil, M.; Ahtiluoto, S.; Haavisto, E. Patient participation in shared decision-making in palliative care—An integrated review. J. Clin. Nurs. 2021, 30, 3415–3428. [Google Scholar] [CrossRef]
- Mulcahy Symmons, S.; Ryan, K.; Aoun, S.M.; Selman, L.E.; Davies, A.N.; Cornally, N.; Lombard, J.; McQuilllan, R.; Guerin, S.; O’Leary, N.; et al. Decision-making in palliative care: Patient and family caregiver concordance and discordance-systematic review and narrative synthesis. BMJ Support. Palliat. Care 2023, 13, 374–385. [Google Scholar] [CrossRef] [PubMed]
- Kanda, Y. Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transpl. 2013, 48, 452–458. [Google Scholar] [CrossRef]
- Bone Pain Trial Working Party. 8 Gy single fraction radiotherapy for the treatment of metastatic skeletal pain: Randomized comparison with a multifraction schedule over 12 months of patient follow-up. Radiother. Oncol. 1999, 52, 111–121. [Google Scholar] [CrossRef]
- Spencer, K.; Parrish, R.; Barton, R.; Henry, A. Palliative radiotherapy. BMJ 2018, 360, k821. [Google Scholar] [CrossRef]
- Kapadia, N.S.; Mamet, R.; Zornosa, C.; Niland, J.C.; D’Amico, T.A.; Hayman, J.A. Radiation therapy at the end of life in patients with incurable non-small cell lung cancer. Cancer 2012, 118, 4339–4345. [Google Scholar] [CrossRef]
| Factor | |
|---|---|
| Age, median (range), years | 74 (48–95) |
| Sex, Female/Male | 19/16 |
| ECOG PS, 1/2/3 | 11/19/5 |
| Primary site | |
| Head and Neck | 6 |
| Lung | 4 |
| Breast/Prostate | 3/1 |
| Esophagus/Stomach/Rectum | 1/1/4 |
| Pancreas/Gallbladder/Kidney | 2/1/1 |
| Uterine/Ovary/Vulva | 5/1/1 |
| Soft tissue sarcoma | 4 |
| Multiple organ metastasis * | |
| Multiple lung metastases | Yes: 15/No: 19 |
| Multiple liver metastases | Yes: 4/No: 30 |
| Multiple bone metastases | Yes: 10/No: 24 |
| Target lesion for Palliative RT | |
| Primary site | 18 |
| Bone metastasis | 12 |
| Lymph node metastasis | 3 |
| Lung metastasis | 2 |
| RT regimen (classified by BED) | |
| <30 Gy/10 fr | 5 |
| 30 Gy/10 fr | 21 |
| >30 Gy/10 fr | 9 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maemoto, H.; Kushi, K.; Owan, I.; Ariga, T.; Heianna, J.; Nishie, A. Deterioration of Performance Status during Palliative Radiotherapy Suggests a Significant Short Survival Duration: Indicating the Necessities for Considering Radiotherapy Discontinuation. Curr. Oncol. 2024, 31, 1752-1761. https://doi.org/10.3390/curroncol31040133
Maemoto H, Kushi K, Owan I, Ariga T, Heianna J, Nishie A. Deterioration of Performance Status during Palliative Radiotherapy Suggests a Significant Short Survival Duration: Indicating the Necessities for Considering Radiotherapy Discontinuation. Current Oncology. 2024; 31(4):1752-1761. https://doi.org/10.3390/curroncol31040133
Chicago/Turabian StyleMaemoto, Hitoshi, Kazuaki Kushi, Isoko Owan, Takuro Ariga, Joichi Heianna, and Akihiro Nishie. 2024. "Deterioration of Performance Status during Palliative Radiotherapy Suggests a Significant Short Survival Duration: Indicating the Necessities for Considering Radiotherapy Discontinuation" Current Oncology 31, no. 4: 1752-1761. https://doi.org/10.3390/curroncol31040133
APA StyleMaemoto, H., Kushi, K., Owan, I., Ariga, T., Heianna, J., & Nishie, A. (2024). Deterioration of Performance Status during Palliative Radiotherapy Suggests a Significant Short Survival Duration: Indicating the Necessities for Considering Radiotherapy Discontinuation. Current Oncology, 31(4), 1752-1761. https://doi.org/10.3390/curroncol31040133





