A Study to Validate the Relevance of Semen F2-Isoprostanes on Human Male Infertility
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patients
2.2. Light Microscopy
2.3. F2-IsoP Determination
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Roberts, L.J., 2nd; Milne, G.L.J. Isoprostanes. J. Lipid. Res. 2009, 50, S219–S223. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Milne, G.L.; Sanchez, S.C.; Musiek, E.S.; Morrow, J.D. Quantification of F2-isoprostanes as a biomarker of oxidative stress. Nat. Protoc. 2007, 2, 221–226. [Google Scholar] [CrossRef] [PubMed]
- Milne, G.L.; Yin, H.; Hardy, K.D.; Davies, S.S.; Roberts, L.J., 2nd. Isoprostane Generation and Function. Chem. Rev. 2011, 111, 5973–5996. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nourooz-Zadeh, J. Key issues in F2-isoprostane analysis. Biochem. Soc. Trans. 2008, 36, 1060–1065. [Google Scholar] [CrossRef]
- Halliwell, B.; Lee, C.Y. Using Isoprostanes as Biomarkers of Oxidative Stress: Some Rarely Considered Issues. Antioxid. Redox Signal. 2010, 13, 145–156. [Google Scholar] [CrossRef] [PubMed]
- van’t Erve, T.J.; Kadiiska, M.B.; London, S.J.; Mason, R.P. Classifying oxidative stress by F2-isoprostane levels across human diseases: A meta-analysis. Redox Biol. 2017, 12, 582–599. [Google Scholar] [CrossRef]
- Milne, G.; Dai, Q.; Roberts, L.J. The isoprostanes—25 years later. Biochim. et Biophys. Acta (BBA) Mol. Cell Biol. Lipids 2014, 1851, 433–445. [Google Scholar] [CrossRef] [Green Version]
- Taber, D.F.; Herr, R.J.; Gleave, D.M. Diastereoselective Synthesis of an Isoprostane: (±)-8-epi-PGF2α Ethyl Ester. J. Org. Chem. 1997, 62, 194–198. [Google Scholar] [CrossRef]
- Takahashi, K.; Nammour, T.M.; Fukunaga, M.; Ebert, J.; Morrow, J.D.; Roberts, L.J.; Hoover, R.L.; Badr, K.F. Glomerular actions of a free radical-generated novel prostaglandin, 8-epi-prostaglandin F2 alpha, in the rat. Evidence for interaction with thromboxane A2 receptors. J. Clin. Investig. 1992, 90, 136–141. [Google Scholar] [CrossRef]
- Comporti, M.; Signorini, C.; Arezzini, B.; Vecchio, D.; Monaco, B.; Gardi, C. F2-isoprostanes are not just markers of oxidative stress. Free Radic. Biol. Med. 2008, 44, 247–256. [Google Scholar] [CrossRef]
- Yura, T.; Fukunaga, M.; Khan, R.; Nassar, G.N.; Badr, K.F.; Montero, A. Free-radical–generated F2-isoprostane stimulates cell proliferation and endothelin-1 expression on endothelial cells. Kidney Int. 1999, 56, 471–478. [Google Scholar] [CrossRef] [Green Version]
- Moretti, E.; Collodel, G.; Salvatici, M.C.; Belmonte, G.; Signorini, C. New insights into sperm with total globozoospermia: Increased fatty acid oxidation and centrin1 alteration. Syst. Biol. Reprod. Med. 2019, 65, 390–399. [Google Scholar] [CrossRef] [PubMed]
- Collodel, G.; Castellini, C.; Iacoponi, F.; Noto, D.; Signorini, C. Cytosolic phospholipase A 2 and F 2 isoprostanes are involved in semen quality and human infertility—A study on leucocytospermia, varicocele and idiopathic infertility. Andrologia 2020, 52, e13465. [Google Scholar] [CrossRef] [PubMed]
- Longini, M.; Moretti, E.; Signorini, C.; Noto, D.; Iacoponi, F.; Collodel, G. Relevance of seminal F2-dihomo-IsoPs, F2-IsoPs and F4-NeuroPs in idiopathic infertility and varicocele. Prostaglandins Other Lipid Mediat. 2020, 149, 106448. [Google Scholar] [CrossRef] [PubMed]
- Collodel, G.; Noto, D.; Signorini, C.; Gambera, L.; Stendardi, A.; Mahmutbegovic, A.; Micheli, L.; Menchiari, A.; Moretti, E. Do Seminal Isoprostanes Have a Role in Assisted Reproduction Outcome? Life 2021, 11, 675. [Google Scholar] [CrossRef]
- World Health Organization. WHO Laboratory Manual for the Examination and Processing of Human Semen, 5th ed.; WHO Press: Geneva, Switzerland, 2010. [Google Scholar]
- Signorini, C.; Moretti, E.; Noto, D.; Mattioli, S.; Castellini, C.; Pascarelli, N.; Durand, T.; Oger, C.; Galano, J.-M.; De Felice, C.; et al. F4-Neuroprostanes: A Role in Sperm Capacitation. Life 2021, 11, 655. [Google Scholar] [CrossRef]
- Agarwal, A.; Rana, M.; Qiu, E.; Albunni, H.; Bui, A.D.; Henkel, R. Role of oxidative stress, infection and inflammation in male infertility. Andrologia 2018, 50, e13126. [Google Scholar] [CrossRef]
- Collodel, G.; Moretti, E.; Longini, M.; Pascarelli, N.A.; Signorini, C. Increased F2-Isoprostane Levels in Semen and Immunolocalization of the 8-Iso Prostaglandin F2α in Spermatozoa from Infertile Patients with Varicocele. Oxid. Med. Cell. Longev. 2018, 2018, 1–9. [Google Scholar] [CrossRef] [Green Version]
- Graille, M.; Wild, P.; Sauvain, J.-J.; Hemmendinger, M.; Guseva Canu, I.; Hopf, N.B. Urinary 8-OHdG as a Biomarker for Oxidative Stress: A Systematic Literature Review and Meta-Analysis. Int. J. Mol. Sci. 2020, 21, 3743. [Google Scholar] [CrossRef]
- Karlis, G.; Kotanidou, A.; Georgiopoulos, G.; Masi, S.; Magkas, N.; Xanthos, T. Usefulness of F2-isoprostanes in early prognostication after cardiac arrest: A topical review of the literature and meta-analysis of preclinical data. Biomarkers 2020, 25, 315–321. [Google Scholar] [CrossRef]
- Ames, P.R.J.; Merashli, M.; Bucci, T.; Nourooz-Zadeh, J. Isoprostane in systemic sclerosis: A systematic review and meta-analysis. Mod. Rheumatol. 2019, 29, 470–475. [Google Scholar] [CrossRef] [PubMed]
- Barati, E.; Nikzad, H.; Karimian, M. Oxidative stress and male infertility: Current knowledge of pathophysiology and role of antioxidant therapy in disease management. Cell. Mol. Life Sci. 2020, 77, 93–113. [Google Scholar] [CrossRef]
- Krzyściak, W.; Papież, M.; Bąk, E.; Morava, E.; Krzyściak, P.; Ligęzka, A.; Gniadek, A.; Vyhouskaya, P.; Janeczko, J. Sperm Antioxidant Biomarkers and Their Correlation with Clinical Condition and Lifestyle with Regard to Male Reproductive Potential. J. Clin. Med. 2020, 9, 1785. [Google Scholar] [CrossRef] [PubMed]
- Pizzino, G.; Irrera, N.; Cucinotta, M.; Pallio, G.; Mannino, F.; Arcoraci, V.; Squadrito, F.; Altavilla, D.; Bitto, A. Oxidative Stress: Harms and Benefits for Human Health. Oxid. Med. Cell. Longev. 2017, 2017, 8416763. [Google Scholar] [CrossRef] [PubMed]
| Vol (mL) | Sperm (106/mL) | Progressive Motility (%) | Rapid Motility (%) | Slow Motility (%) | Normal Morphology (%) | Viability (%) | F2-IsoPs (ng/mL) |
|---|---|---|---|---|---|---|---|
| 4.00 (1.50) | 37.88 (68.98) | 29.00 (21.00) | 18.00 (20.00) | 10.00 (11.00) | 9.00 (9.00) | 70.00 (22.25) | 40.90 (44.64) |
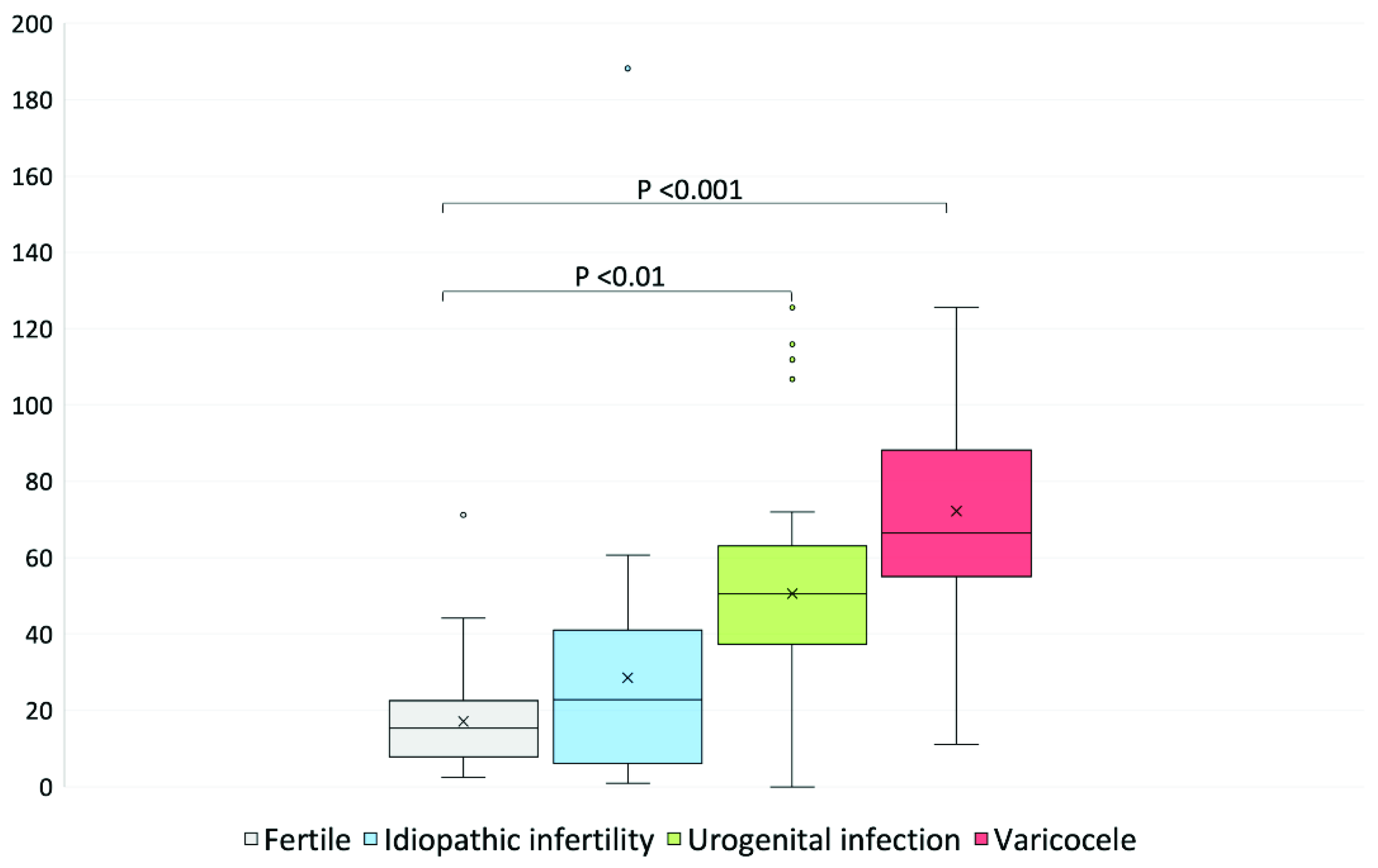
| Variable | Fertile Men (F, n = 45) | Idiopathic Infertility (I, n = 41) | Urogenital Infections (U, n = 52) | Varicocele (V, n = 54) | Statistics |
|---|---|---|---|---|---|
| Vol (mL) | 4.00 (1.30) | 4.00 (1.50) | 3.65 (1.15) | 4.00 (0.98) | |
| Sperm (106/mL) | 110.00 (98.00) | 12.00 (31.90) | 24.50 (47.48) | 38.50 (31.56) | F vs. I, U, V. p < 0.001 I vs. U. p < 0.05 |
| Progressive motility (%) | 51.00 (18.00) | 28.00 (15.00) | 23.00 (12.25) | 24.50 (16.75) | F vs. I, U, V. p < 0.001 |
| Rapid motility (%) | 40.00 (10.00) | 20.00 (13.00) | 12.00 (12.25) | 12.00 (6.75) | F vs. I, U, V. p < 0.001 |
| Slow motility (%) | 12.00 (11.00) | 8.00 (9.00) | 8.00 (8.50) | 12.00 (10.75) | F vs. I. p < 0.05 |
| Normal morphology (%) | 15.00 (7.00) | 7.00 (5.00) | 6.00 (5.00) | 8.00 (5.00) | F vs. I, U, V. p < 0.001 |
| Viability (%) | 85.00 (11.00) | 65.00 (20.00) | 60.00 (24.00) | 65.00 (16.50) | F vs. I, U, V. p < 0.001 |
| F2-IsoPs (ng/mL) | 15.36 (14.41) | 22.80 (31.44) | 52.10 (24.62) | 66.40 (31.91) | F vs. U. p < 0.01 F vs. V. p < 0.001 |
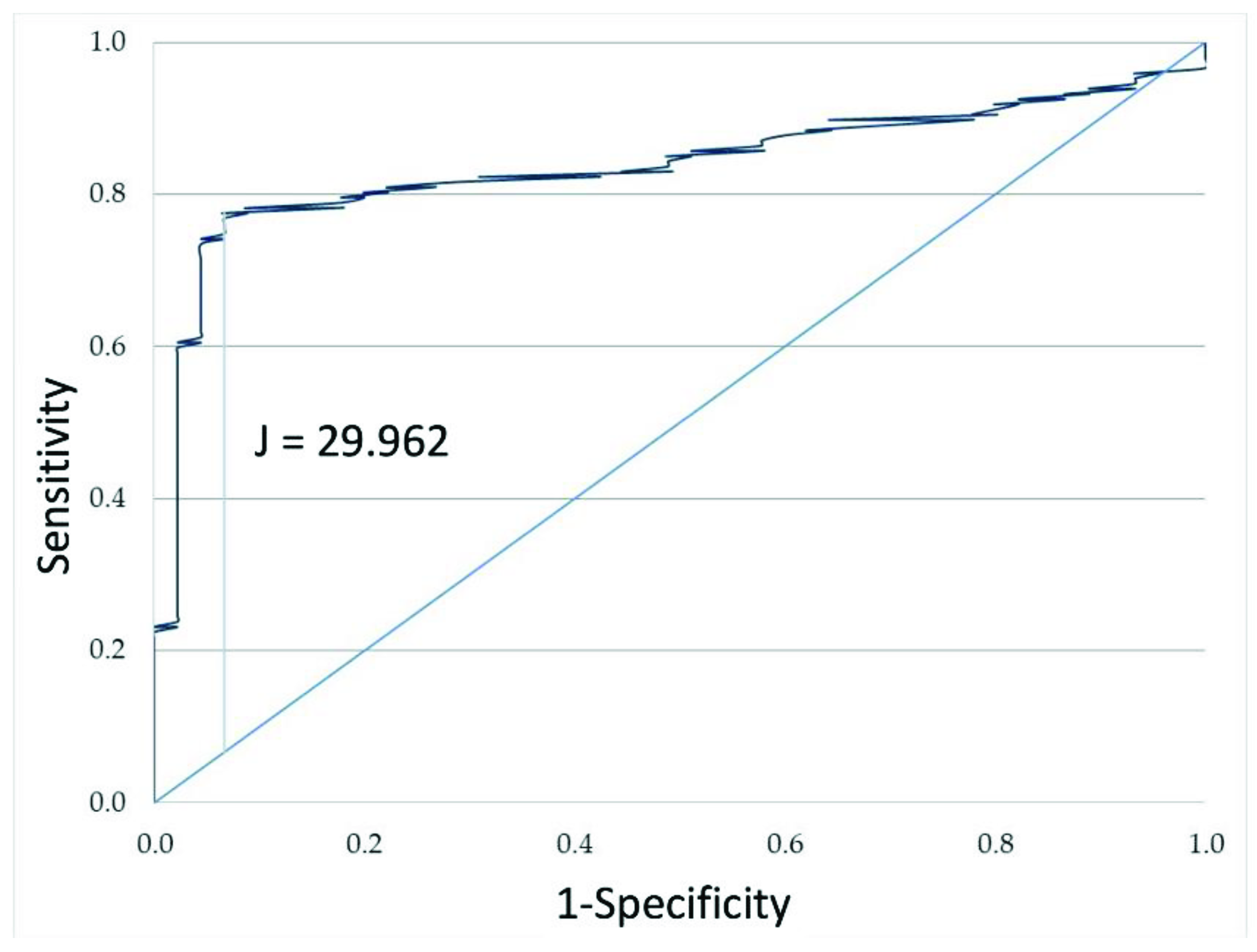
| Variable | Class 1 (<29.96 ng/mL) (n = 78) | Class 2 (>29.96 ng/mL) (n = 114) |
|---|---|---|
| Vol (mL) | 4.00 (1.50) | 4.00 (1.40) |
| Sperm (106/mL) | 56.00 (98.43) | 25.00 (40.00) ** |
| Progressive motility (%) | 40.00 (25.50) | 23.00 (17.00) *** |
| Rapid motility (%) | 32.00 (19.00) | 12.00 (10.00) *** |
| Slow motility (%) | 10.00 (13.00) | 10.00 (10.00) |
| Normal morphology (%) | 12.00 (7.00) | 7.00 (6.00) * |
| Viability (%) | 78.00 (20.00) | 64.00 (20.00) * |
| F2-IsoPs (ng/mL) | 11.20 (14.93) | 59.80 (27.23) *** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moretti, E.; Signorini, C.; Ferretti, F.; Noto, D.; Collodel, G. A Study to Validate the Relevance of Semen F2-Isoprostanes on Human Male Infertility. Int. J. Environ. Res. Public Health 2022, 19, 1642. https://doi.org/10.3390/ijerph19031642
Moretti E, Signorini C, Ferretti F, Noto D, Collodel G. A Study to Validate the Relevance of Semen F2-Isoprostanes on Human Male Infertility. International Journal of Environmental Research and Public Health. 2022; 19(3):1642. https://doi.org/10.3390/ijerph19031642
Chicago/Turabian StyleMoretti, Elena, Cinzia Signorini, Fabio Ferretti, Daria Noto, and Giulia Collodel. 2022. "A Study to Validate the Relevance of Semen F2-Isoprostanes on Human Male Infertility" International Journal of Environmental Research and Public Health 19, no. 3: 1642. https://doi.org/10.3390/ijerph19031642
APA StyleMoretti, E., Signorini, C., Ferretti, F., Noto, D., & Collodel, G. (2022). A Study to Validate the Relevance of Semen F2-Isoprostanes on Human Male Infertility. International Journal of Environmental Research and Public Health, 19(3), 1642. https://doi.org/10.3390/ijerph19031642









