Body Positivity and Self-Compassion on a Publicly Available Behavior Change Weight Management Program
Abstract
1. Introduction
2. Materials and Methods
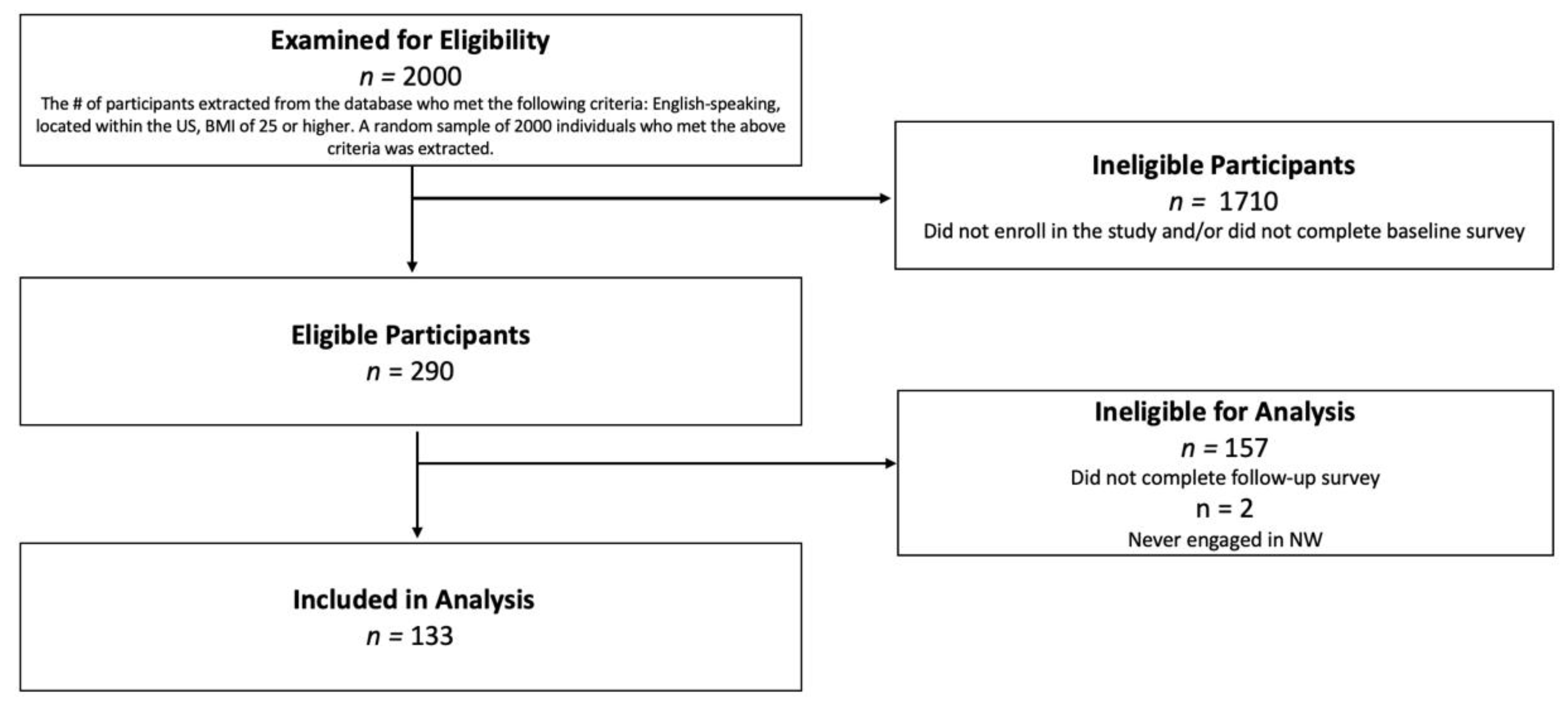
2.1. Participants
2.2. Power and Sample Size Calculation
2.3. Procedure
2.4. Program
2.5. Measures
2.6. Statistical Analysis
3. Results
3.1. Participant Characteristics
3.2. Changes in Outcomes
3.3. Baseline Measures and Engagement
3.4. Changes in Outcomes and Engagement
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Swami, V.; Weis, L.; Barron, D.; Furnham, A. Positive body image is positively associated with hedonic (emotional) and eu-daimonic (psychological and social) well-being in British adults. J. Soc. Psychol. 2018, 158, 541–552. [Google Scholar] [CrossRef] [PubMed]
- Zessin, U.; Dickhäuser, O.; Garbade, S. The relationship between self-compassion and well-being: A meta-analysis. Appl. Psychol. Health Well-Being 2015, 7, 340–364. [Google Scholar] [CrossRef] [PubMed]
- Halliwell, E. Future directions for positive body image research. Body Image 2015, 14, 177–189. [Google Scholar] [CrossRef] [PubMed]
- Biber, D.D.; Ellis, R. The effect of self-compassion on the self-regulation of health behaviors: A systematic review. J. Health Psychol. 2017, 24, 2060–2071. [Google Scholar] [CrossRef] [PubMed]
- Phillips, W.J.; Hine, D.W. Self-compassion, physical health, and health behaviour: A meta-analysis. Health Psychol. Rev. 2019, 15, 113–139. [Google Scholar] [CrossRef]
- Webb, J.B.; Butler-Ajibade, P.; Robinson, S.A. Considering an affect regulation framework for examining the association between body dissatisfaction and positive body image in black older adolescent females: Does body mass index matter? Body Image 2014, 11, 426–437. [Google Scholar] [CrossRef]
- Braun, T.D.; Park, C.L.; Gorin, A. Self-compassion, body image, and disordered eating: A review of the literature. Body Image 2016, 17, 117–131. [Google Scholar] [CrossRef]
- Cox, A.E.; Ullrich-French, S.; Tylka, T.L.; McMahon, A.K. The roles of self-compassion, body surveillance, and body appreciation in predicting intrinsic motivation for physical activity: Cross-sectional associations, and prospective changes within a yoga context. Body Image 2019, 29, 110–117. [Google Scholar] [CrossRef]
- Kelly, A.C.; Stephen, E. A daily diary study of self-compassion, body image, and eating behavior in female college students. Body Image 2016, 17, 152–160. [Google Scholar] [CrossRef]
- Jones, R.A.; Lawlor, E.R.; Birch, J.M.; Patel, M.I.; Werneck, A.O.; Hoare, E.; Griffin, S.J.; van Sluijs, E.M.; Sharp, S.J.; Ahern, A.L. The impact of adult behavioural weight management interventions on mental health: A systematic review and meta-analysis. Obes. Rev. 2020, 22, e13150. [Google Scholar] [CrossRef]
- Chao, H.-L. Body image change in obese and overweight persons enrolled in weight loss intervention programs: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0124036. [Google Scholar] [CrossRef] [PubMed]
- Dionne, M.M.; Yeudall, F. Monitoring of weight in weight loss programs: A double-edged sword? J. Nutr. Educ. Behav. 2005, 37, 315–318. [Google Scholar] [CrossRef]
- Niemeier, H.M.; Leahey, T.; Reed, K.P.; Brown, R.A.; Wing, R.R. An acceptance-based behavioral intervention for weight loss: A pilot study. Behav. Ther. 2012, 43, 427–435. [Google Scholar] [CrossRef]
- Carels, R.A.; Darby, L.A.; Rydin, S.; Douglass, O.M.; Cacciapaglia, H.M.; O’Brien, W.H. The relationship between self-monitoring, outcome expectancies, difficulties with eating and exercise, and physical activity and weight loss treatment outcomes. Ann. Behav. Med. 2005, 30, 182–190. [Google Scholar] [CrossRef]
- Cooper, Z.; Fairburn, C.G. A new cognitive behavioural approach to the treatment of obesity. Behav. Res. Ther. 2001, 39, 499–511. [Google Scholar] [CrossRef]
- Forman, E.M.; Herbert, J.D. New directions in cognitive behavior therapy: Acceptance-based therapies. In General Principles and Empirically Supported Techniques of Cognitive Behavior Therapy; O’Donohue, W.T., Fisher, J.E., Eds.; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2009; pp. 77–101. [Google Scholar]
- Lawlor, E.R.; Islam, N.; Bates, S.; Griffin, S.J.; Hill, A.J.; Hughes, C.A.; Sharp, S.J.; Ahern, A.L. Third-wave cognitive behaviour therapies for weight management: A systematic review and network meta-analysis. Obes. Rev. 2020, 21, e13013. [Google Scholar] [CrossRef]
- Lillis, J.; Kendra, K.E. Acceptance and commitment therapy for weight control: Model, evidence, and future directions. J. Context. Behav. Sci. 2014, 3, 1–7. [Google Scholar] [CrossRef]
- Rahimi-Ardabili, H.; Reynolds, R.C.; Vartanian, L.; McLeod, L.V.D.; Zwar, N. A systematic review of the efficacy of interventions that aim to increase self-compassion on nutrition habits, eating behaviours, body weight and body image. Mindfulness 2017, 9, 388–400. [Google Scholar] [CrossRef]
- Castelnuovo, G.; Pietrabissa, G.; Manzoni, G.M.; Cattivelli, R.; Rossi, A.; Novelli, M.; Varallo, G.; Molinari, E. Cognitive behavioral therapy to aid weight loss in obese patients: Current perspectives. Psychol. Res. Behav. Manag. 2017, 10, 165–173. [Google Scholar] [CrossRef]
- Griffiths, C.; Williamson, H.; Zucchelli, F.; Paraskeva, N.; Moss, T. A systematic review of the effectiveness of acceptance and commitment therapy (ACT) for body image dissatisfaction and weight self-stigma in adults. J. Contemp. Psychother. 2018, 48, 189–204. [Google Scholar] [CrossRef]
- Linardon, J.; Gleeson, J.; Yap, K.; Murphy, K.; Brennan, L. Meta-analysis of the effects of third-wave behavioural interventions on disordered eating and body image concerns: Implications for eating disorder prevention. Cogn. Behav. Ther. 2018, 48, 15–38. [Google Scholar] [CrossRef] [PubMed]
- Yadavaia, J.E.; Hayes, S.C.; Vilardaga, R. Using acceptance and commitment therapy to increase self-compassion: A randomized controlled trial. J. Context. Behav. Sci. 2014, 3, 248–257. [Google Scholar] [CrossRef] [PubMed]
- Barnard, L.K.; Curry, J.F. Self-compassion: Conceptualizations, correlates, and interventions. Rev. Gen. Psychol. 2011, 15, 289–303. [Google Scholar] [CrossRef]
- Comșa, L.; David, O.; David, D. Outcomes and mechanisms of change in cognitive-behavioral interventions for weight loss: A meta-analysis of randomized clinical trials. Behav. Res. Ther. 2020, 132, 103654. [Google Scholar] [CrossRef]
- Palmeira, A.L.; Markland, D.A.; Silva, M.N.; Branco, T.L.; Martins, S.C.; Minderico, C.S.; Vieira, P.N.; Barata, J.T.; Serpa, S.O.; Sardinha, L.B.; et al. Reciprocal effects among changes in weight, body image, and other psychological factors during behavioral obesity treatment: A mediation analysis. Int. J. Behav. Nutr. Phys. Act. 2009, 6, 1–12. [Google Scholar] [CrossRef]
- Swencionis, C.; Wylie-Rosett, J.; Lent, M.R.; Ginsberg, M.; Cimino, C.; Wassertheil-Smoller, S.; Caban, A.; Segal-Isaacson, C.J. Weight change, psychological well-being, and vitality in adults participating in a cognitive–behavioral weight loss program. Health Psychol. 2013, 32, 439. [Google Scholar] [CrossRef]
- Stubbs, J.; Whybrow, S.; Teixeira, P.; Blundell, J.; Lawton, C.; Westenhoefer, J.; Engel, D.; Shepherd, R.; McConnon, Á.; Gilbert, P.; et al. Problems in identifying predictors and correlates of weight loss and maintenance: Implications for weight control therapies based on behaviour change. Obes. Rev. 2011, 12, 688–708. [Google Scholar] [CrossRef]
- Rapoport, L.; Clark, M.; Wardle, J. Evaluation of a modified cognitive–behavioural programme for weight management. Int. J. Obes. 2000, 24, 1726–1737. [Google Scholar] [CrossRef] [PubMed]
- Toro-Ramos, T.; Michaelides, A.; Anton, M.; Karim, Z.; Kang-Oh, L.; Argyrou, C.; Loukaidou, E.; Charitou, M.M.; Sze, W.; Miller, J.D. Mobile delivery of the diabetes prevention program in people with prediabetes: Randomized controlled trial. JMIR mHealth uHealth 2020, 8, e17842. [Google Scholar] [CrossRef]
- DeLuca, L.; Toro-Ramos, T.; Michaelides, A.; Seng, E.; Swencionis, C. Relationship between age and weight loss in noom: Quasi-experimental study. JMIR Diabetes 2020, 5, e18363. [Google Scholar] [CrossRef]
- Michaelides, A.; Major, J.; Pienkosz, E., Jr.; Wood, M.; Kim, Y.; Toro-Ramos, T. Usefulness of a novel mobile diabetes prevention program delivery platform with human coaching: 65-week observational follow-up. JMIR mHealth uHealth 2018, 6, e93. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.; Kim, Y.; Go, Y.; Lee, S.; Na, M.; Lee, Y.; Choi, S.; Choi, H.J. Multidimensional cognitive behavioral therapy for obesity applied by psychologists using a digital platform: Open-label randomized controlled trial. JMIR mHealth uHealth 2020, 8, e14817. [Google Scholar] [CrossRef]
- Luoma, J.B.; Hayes, S.C.; Walser, R.D. Learning ACT: An Acceptance and Commitment Therapy Skills-Training Manual for Therapists; New Harbinger Publications: Oakland, CA, USA, 2007; ISBN 1-57224-498-4. [Google Scholar]
- Linehan, M. DBT Skills Training Manual; Guilford Publications: New York, NY, USA, 2014; ISBN 1-4625-1699-8. [Google Scholar]
- Dobson, D.; Dobson, K.S. Evidence-Based Practice of Cognitive-Behavioral Therapy; Guilford Publications: New York, NY, USA, 2018; ISBN 1-4625-3802-9. [Google Scholar]
- Burke, L.E.; Wang, J.; Sevick, M.A. Self-monitoring in weight loss: A systematic review of the literature. J. Am. Diet. Assoc. 2011, 111, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Khaylis, A.; Yiaslas, T.; Bergstrom, J.; Gore-Felton, C. A review of efficacious technology-based weight-loss interventions: Five key components. Telemed. e-Health 2010, 16, 931–938. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.; Tietsort, C.; Posteher, K.; Michaelides, A.; Toro-Ramos, T. Enabling self-management of a chronic condition through patient-centered coaching: A case of an mHealth diabetes prevention program for older adults. Health Commun. 2019, 35, 1791–1799. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, E.; Yang, Q.; Ho, A.; Behr, H.; May, C.; DeLuca, L.; Michaelides, A. Self-reported nutritional factors are associated with weight loss at 18 months in a self-managed commercial program with food categorization system: Observational study. Nutrients 2021, 13, 1733. [Google Scholar] [CrossRef] [PubMed]
- Tylka, T.L.; Wood-Barcalow, N.L. The body appreciation scale-2: Item refinement and psychometric evaluation. Body Image 2015, 12, 53–67. [Google Scholar] [CrossRef]
- Sandoz, E.K.; Wilson, K.G.; Merwin, R.M.; Kellum, K.K. Assessment of body image flexibility: The body image-acceptance and action questionnaire. J. Context. Behav. Sci. 2013, 2, 39–48. [Google Scholar] [CrossRef]
- Raes, F.; Pommier, E.; Neff, K.D.; Van Gucht, D. Construction and factorial validation of a short form of the self-compassion scale. Clin. Psychol. Psychother. 2010, 18, 250–255. [Google Scholar] [CrossRef]
- Cowdrey, F.A.; Park, R.J. Assessing rumination in eating disorders: Principal component analysis of a minimally modified ruminative response scale. Eat. Behav. 2011, 12, 321–324. [Google Scholar] [CrossRef]
- Holland, B.S.; Copenhaver, M.D. An improved sequentially rejective Bonferroni test procedure. Biometrics 1987, 43, 417. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Elsevier Science: Amsterdam, The Netherlands, 2013; ISBN 9781483276489. [Google Scholar]
- Golden, H.L.; Vosper, J.; Kingston, J.; Ellett, L. The impact of mindfulness-based programmes on self-compassion in nonclinical populations: A systematic review and meta-analysis. Mindfulness 2020, 12, 29–52. [Google Scholar] [CrossRef]
- Stewart, T.M.; Bachand, A.R.; Han, H.; Ryan, D.; Bray, G.A.; Williamson, D.A. Body image changes associated with participation in an intensive lifestyle weight loss intervention. Obesity 2011, 19, 1290–1295. [Google Scholar] [CrossRef] [PubMed]
- Carey, A.; Yang, Q.; DeLuca, L.; Toro-Ramos, T.; Kim, Y.; Michaelides, A. The relationship between weight loss outcomes and engagement in a mobile behavioral change intervention: A retrospective analysis. JMIR mHealth uHealth 2021, 9, e30622. [Google Scholar] [CrossRef] [PubMed]
- Neff, K.D. Self-compassion, self-esteem, and well-being: Self-compassion, self-esteem, and well-being. social and personality. Psychol. Compass 2011, 5, 1–12. [Google Scholar] [CrossRef]
- Germer, C.K.; Neff, K.D. Self-compassion in clinical practice. J. Clin. Psychol. 2013, 69, 856–867. [Google Scholar] [CrossRef]
- Rapoport, O.; Bengel, S.; Möcklinghoff, S.; Neidhardt, E. Self-compassion moderates the influence of procrastination on postponing sporting activity. Personal. Individ. Differ. 2021, 185, 111242. [Google Scholar] [CrossRef]
- Cowdrey, F.A.; Park, R.J. The role of experiential avoidance, rumination and mindfulness in eating disorders. Eat. Behav. 2012, 13, 100–105. [Google Scholar] [CrossRef]
- Smith, K.E.; Mason, T.B.; Lavender, J.M. Rumination and eating disorder psychopathology: A meta-analysis. Clin. Psychol. Rev. 2018, 61, 9–23. [Google Scholar] [CrossRef]
- Klos, L.A.; Esser, V.E.; Kessler, M.M. To weigh or not to weigh: The relationship between self-weighing behavior and body image among adults. Body Image 2012, 9, 551–554. [Google Scholar] [CrossRef]
- Pacanowski, C.R.; Linde, J.A.; Neumarksztainer, D. Self-weighing: Helpful or harmful for psychological well-being? A review of the literature. Curr. Obes. Rep. 2015, 4, 65–72. [Google Scholar] [CrossRef] [PubMed]
- Rodgers, R.F. The role of the “healthy weight” discourse in body image and eating concerns: An extension of sociocultural theory. Eat. Behav. 2016, 22, 194–198. [Google Scholar] [CrossRef] [PubMed]
- Hunger, J.M.; Tomiyama, A.J. A call to shift the public health focus away from weight. Am. J. Public Health 2015, 105, e3. [Google Scholar] [CrossRef]
- McWhorter, K.L. Obesity acceptance: Body positivity and clinical risk factors. In Cardiac Diseases—Novel Aspects of Cardiac Risk, Cardiorenal Pathology and Cardiac Interventions; Gaze, D.C., Kibel, A., Eds.; IntechOpen: London, UK, 2020; ISBN 9781839681622. [Google Scholar]
- Papadopoulos, S.; Brennan, L. Correlates of weight stigma in adults with overweight and obesity: A systematic literature review. Obesity 2015, 23, 1743–1760. [Google Scholar] [CrossRef] [PubMed]
| Outcome | Mean Difference (Week 16—Baseline) | Test Statistic | p-Value | Cohen’s d |
|---|---|---|---|---|
| Body appreciation | +0.22 | t(132) = −5.23 | <0.001 *** | 0.45 |
| Body image flexibility 1 | −2.86 | t(132) = 3.56 | 0.001 *** | 0.31 |
| Total self-compassion | +2.22 | t(132) = −4.04 | <0.001 *** | 0.35 |
| Self-judgment subscale 2 | +0.56 | t(132) = −3.87 | <0.001 *** | 0.34 |
| Common humanity subscale | +0.56 | t(132) = −3.64 | <0.001 *** | 0.31 |
| Mindfulness subscale | +0.39 | t(132) = −2.71 | 0.007 ** | 0.24 |
| Self-kindness subscale | +0.24 | t(132) = −1.66 | 0.10 + | 0.14 |
| Isolation subscale 2 | +0.19 | t(132) = −1.12 | 0.27 | 0.10 |
| Overidentification subscale 2 | +0.29 | t(132) = −1.88 | 0.06 + | 0.16 |
| Total rumination | −0.95 | t(132) = 2.92 | 0.004 ** | 0.25 |
| Brooding subscale | −0.71 | t(132) = 3.11 | 0.002 ** | 0.27 |
| Reflection subscale | −0.24 | t(132) = 1.47 | 0.14 | 0.13 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
McCallum, M.; Ho, A.S.; May, C.N.; Behr, H.; Mitchell, E.S.; Michealides, A. Body Positivity and Self-Compassion on a Publicly Available Behavior Change Weight Management Program. Int. J. Environ. Res. Public Health 2021, 18, 13358. https://doi.org/10.3390/ijerph182413358
McCallum M, Ho AS, May CN, Behr H, Mitchell ES, Michealides A. Body Positivity and Self-Compassion on a Publicly Available Behavior Change Weight Management Program. International Journal of Environmental Research and Public Health. 2021; 18(24):13358. https://doi.org/10.3390/ijerph182413358
Chicago/Turabian StyleMcCallum, Meaghan, Annabell Suh Ho, Christine N. May, Heather Behr, Ellen Siobhan Mitchell, and Andreas Michealides. 2021. "Body Positivity and Self-Compassion on a Publicly Available Behavior Change Weight Management Program" International Journal of Environmental Research and Public Health 18, no. 24: 13358. https://doi.org/10.3390/ijerph182413358
APA StyleMcCallum, M., Ho, A. S., May, C. N., Behr, H., Mitchell, E. S., & Michealides, A. (2021). Body Positivity and Self-Compassion on a Publicly Available Behavior Change Weight Management Program. International Journal of Environmental Research and Public Health, 18(24), 13358. https://doi.org/10.3390/ijerph182413358






