To Vaccinate or Not to Vaccinate—This Is the Question among Swiss University Students
Abstract
1. Introduction
2. Materials and Methods
2.1. Survey Design and Study Design
2.2. Missing Data
2.3. Measures
2.3.1. Outcome: Vaccination Intention
2.3.2. Predictors
2.3.3. Covariates
2.4. Statistical Analyses
3. Results
3.1. Participants’ Characteristics
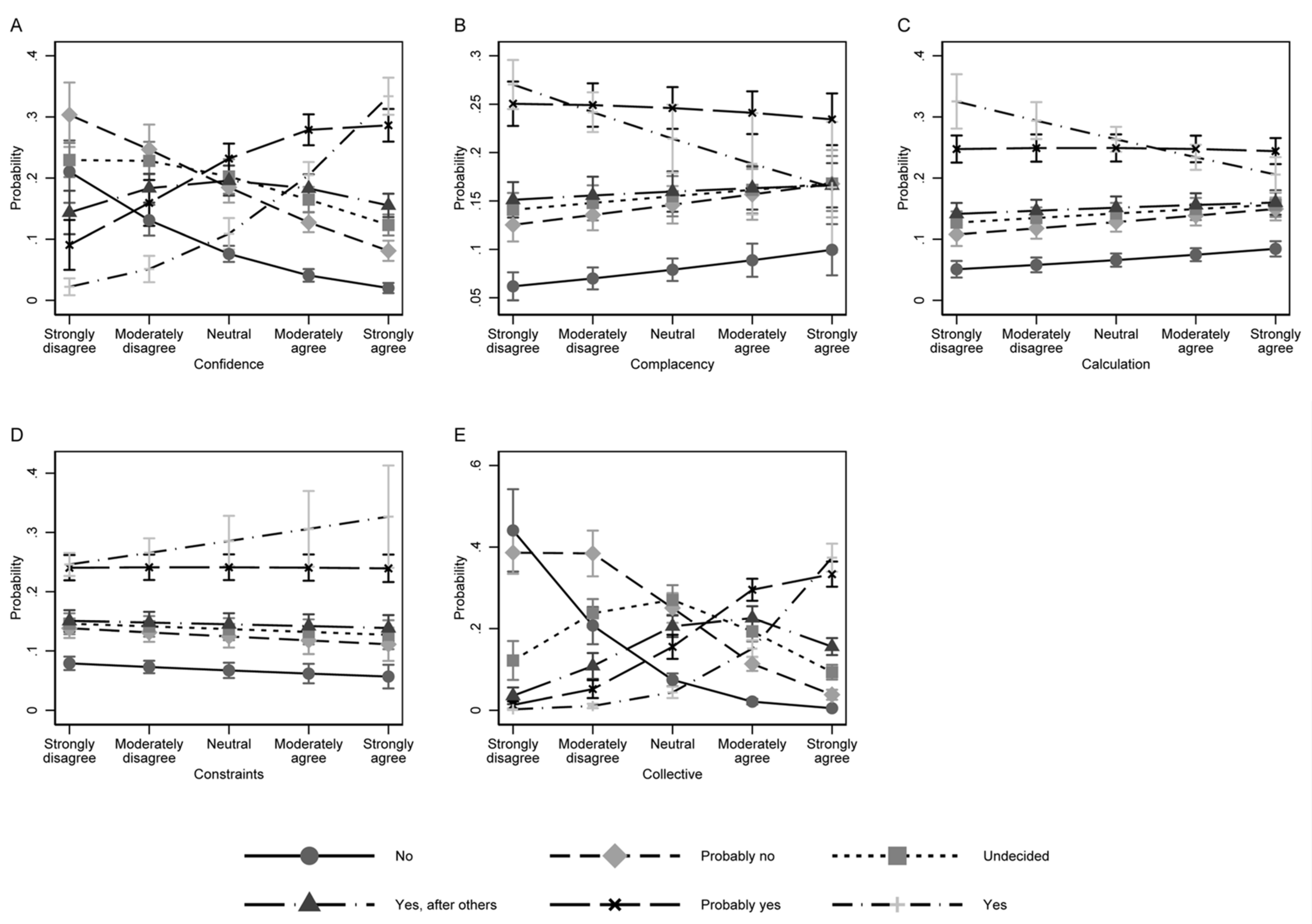
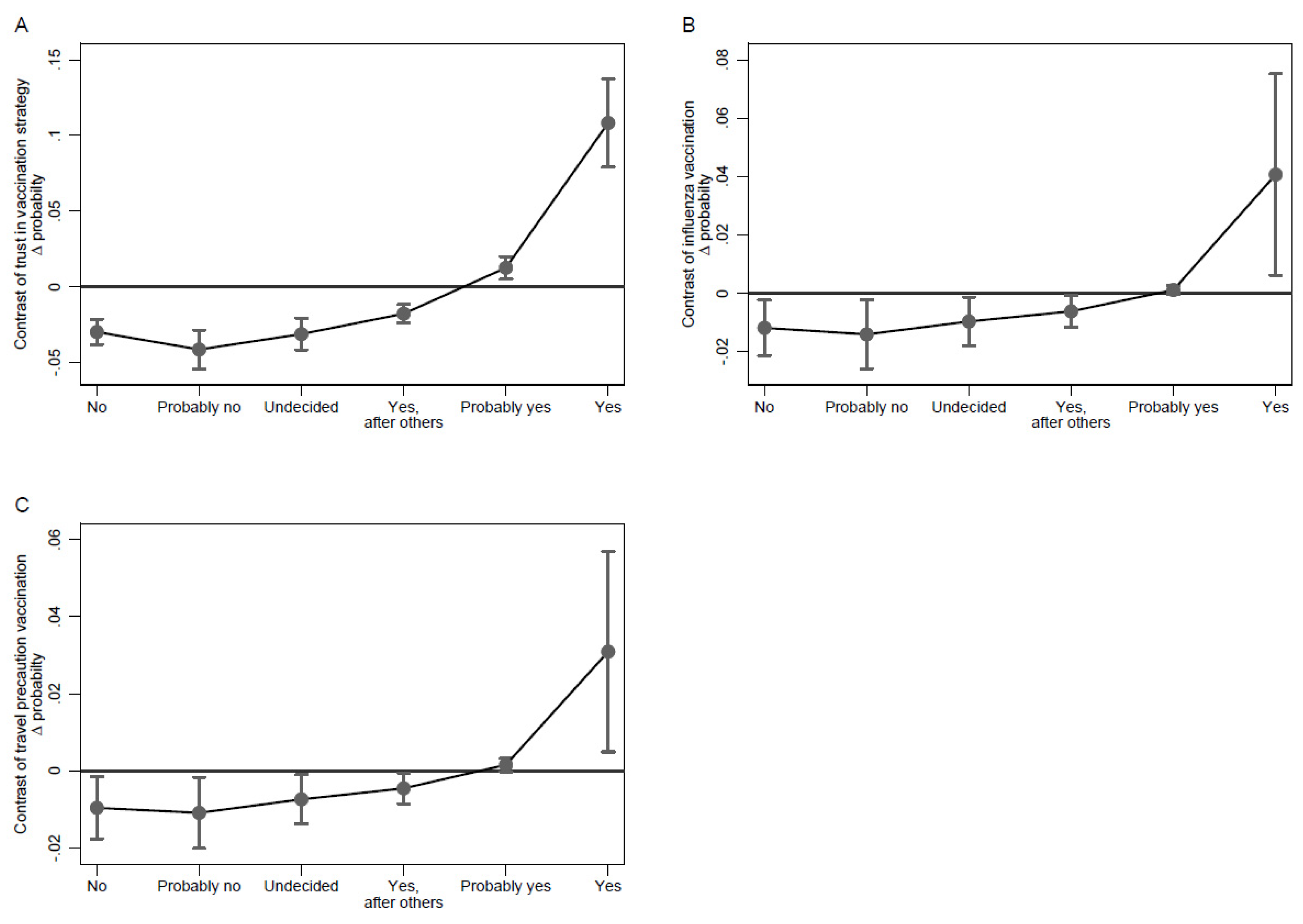
3.2. Factors Associated with COVID-19 Vaccination Intention
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Fischer, A. SARS-CoV-2 Vaccines, Where Do We Stand? Comptes Rendus Biol. 2021, 344, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Abdulla, Z.A.; Al-Bashir, S.M.; Al-Salih, N.S.; Aldamen, A.A.; Abdulazeez, M.Z. A Summary of the SARS-CoV-2 Vaccines and Technologies Available or under Development. Pathogens 2021, 10, 788. [Google Scholar] [CrossRef] [PubMed]
- Fadda, M.; Albanese, E.; Suggs, L.S. When a COVID-19 Vaccine Is Ready, Will We All Be Ready for It? Int. J. Public Health 2020, 65, 711–712. [Google Scholar] [CrossRef]
- MacDonald, N.E. Vaccine Hesitancy: Definition, Scope and Determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- Lane, S.; MacDonald, N.E.; Marti, M.; Dumolard, L. Vaccine Hesitancy around the Globe: Analysis of Three Years of WHO/UNICEF Joint Reporting Form Data-2015–2017. Vaccine 2018, 36, 3861–3867. [Google Scholar] [CrossRef]
- Wiysonge, C.S.; Ndwandwe, D.; Ryan, J.; Jaca, A.; Batouré, O.; Anya, B.-P.M.; Cooper, S. Vaccine Hesitancy in the Era of COVID-19: Could Lessons from the Past Help in Divining the Future? Hum. Vaccines Immunother. 2021. [Google Scholar] [CrossRef]
- Murphy, J.; Vallières, F.; Bentall, R.P.; Shevlin, M.; McBride, O.; Hartman, T.K.; McKay, R.; Bennett, K.; Mason, L.; Gibson-Miller, J.; et al. Psychological Characteristics Associated with COVID-19 Vaccine Hesitancy and Resistance in Ireland and the United Kingdom. Nat. Commun. 2021, 12, 29. [Google Scholar] [CrossRef]
- Sharma, M.; Davis, R.E.; Wilkerson, A.H. COVID-19 Vaccine Acceptance among College Students: A Theory-Based Analysis. Int. J. Environ. Res. Public Health 2021, 18, 4617. [Google Scholar] [CrossRef] [PubMed]
- Lu, H.; Weintz, C.; Pace, J.; Indana, D.; Linka, K.; Kuhl, E. Are College Campuses Superspreaders? A Data-Driven Modeling Study. Comput. Methods Biomech. Biomed. Eng. 2021. [Google Scholar] [CrossRef]
- Sallam, M.; Dababseh, D.; Eid, H.; Hasan, H.; Taim, D.; Al-Mahzoum, K.; Al-Haidar, A.; Yaseen, A.; Ababneh, N.A.; Assaf, A.; et al. Low COVID-19 Vaccine Acceptance Is Correlated with Conspiracy Beliefs among University Students in Jordan. Int. J. Environ. Res. Public Health 2021, 18, 2407. [Google Scholar] [CrossRef] [PubMed]
- Hermann, M. Special Report on COVID-19 Vaccination (Spezialauswertung COVID-19-Impfung: Informationsstand, Einstellungen und Verhalten; Forschungsstelle Sotomo: Bern, Switzerland, 2021. [Google Scholar]
- Afifi, T.O.; Salmon, S.; Taillieu, T.; Stewart-Tufescu, A.; Fortier, J.; Driedger, S.M. Older Adolescents and Young Adults Willingness to Receive the COVID-19 Vaccine: Implications for Informing Public Health Strategies. Vaccine 2021, 39, 3473–3479. [Google Scholar] [CrossRef] [PubMed]
- Studie zur Gesundheit von Studierenden in Zeiten der Corona-Pandemie. Available online: https://www.zhaw.ch/de/gesundheit/forschung/gesundheitswissenschaften/projekte/studierendengesundheit/ (accessed on 19 August 2021).
- Jakobsen, J.C.; Gluud, C.; Wetterslev, J.; Winkel, P. When and How Should Multiple Imputation Be Used for Handling Missing Data in Randomised Clinical Trials—Practical Guide with Flowcharts. BMC Med. Res. Methodol. 2017, 17, 162. [Google Scholar] [CrossRef]
- Corona Immunitas. Available online: https://www.corona-immunitas.ch/ (accessed on 21 July 2021).
- Betsch, C.; Schmid, P.; Heinemeier, D.; Korn, L.; Holtmann, C.; Böhm, R. Beyond Confidence: Development of a Measure Assessing the 5C Psychological Antecedents of Vaccination. PLoS ONE 2018, 13, e0208601. [Google Scholar] [CrossRef] [PubMed]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092. [Google Scholar] [CrossRef]
- Brant, R. Assessing Proportionality in the Proportional Odds Model for Ordinal Logistic Regression. Biometrics 1990, 46, 1171–1178. [Google Scholar] [CrossRef]
- Brandt, E.J.; Rosenberg, J.; Waselewski, M.E.; Amaro, X.; Wasag, J.; Chang, T. National Study of Youth Opinions on Vaccination for COVID-19 in the U.S. J. Adolesc. Health 2021, 68, 869–872. [Google Scholar] [CrossRef]
- Kwok, K.O.; Li, K.-K.; WEI, W.I.; Tang, A.; Wong, S.Y.S.; Lee, S.S. Influenza Vaccine Uptake, COVID-19 Vaccination Intention and Vaccine Hesitancy among Nurses: A Survey. Int. J. Nurs. Stud. 2021, 114, 103854. [Google Scholar] [CrossRef] [PubMed]
- Dorman, C.; Perera, A.; Condon, C.; Chau, C.; Qian, J.; Kalk, K.; DiazDeleon, D. Factors Associated with Willingness to Be Vaccinated against COVID-19 in a Large Convenience Sample. J. Commun. Health 2021. [Google Scholar] [CrossRef]
- OECD. Government at a Glance 2017; Government at a Glance; OECD Publishing: Paris, France, 2017; ISBN 978-92-64-26872-2. [Google Scholar]
- Hermann, M. COVID-19-Präventionsmassnahmen: Informationsstand, Einstellungen und Verhalten—Bericht zur Wirkungsmessung von Ende Oktober 2020 im Auftrag des Bundesamts für Gesundheit BAG; Forschungsstelle Sotomo: Bern, Switzerland, 2020. [Google Scholar]
- Zysset, A.E.; Schlatter, N.; von Wyl, A.; Huber, M.; Volken, T.; Dratva, J. Students’ Experience and Adherence to Containment Measures during COVID-19 in Switzerland. Health Promot. Int. 2021. [Google Scholar] [CrossRef] [PubMed]
- Thaker, J. The Persistence of Vaccine Hesitancy: COVID-19 Vaccination Intention in New Zealand. J. Health Commun. 2021, 26, 104–111. [Google Scholar] [CrossRef]
- Schwarzinger, M.; Watson, V.; Arwidson, P.; Alla, F.; Luchini, S. COVID-19 Vaccine Hesitancy in a Representative Working-Age Population in France: A Survey Experiment Based on Vaccine Characteristics. Lancet Public Health 2021, 6, e210–e221. [Google Scholar] [CrossRef]
- Ruiz, J.B.; Bell, R.A. Predictors of Intention to Vaccinate against COVID-19: Results of a Nationwide Survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef]
- Al-Sanafi, M.; Sallam, M. Psychological Determinants of COVID-19 Vaccine Acceptance among Healthcare Workers in Kuwait: A Cross-Sectional Study Using the 5C and Vaccine Conspiracy Beliefs Scales. Vaccines 2021, 9, 701. [Google Scholar] [CrossRef]
- Kwok, K.O.; Li, K.K.; Tang, A.; Tsoi, M.T.F.; Chan, E.Y.Y.; Tang, J.W.T.; Wong, A.; Wei, W.I.; Wong, S.Y.S. Psychobehavioral Responses and Likelihood of Receiving COVID-19 Vaccines during the Pandemic, Hong Kong. Emerg. Infect. Dis. 2021, 27, 1802–1810. [Google Scholar] [CrossRef] [PubMed]
- Sherman, S.M.; Smith, L.E.; Sim, J.; Amlôt, R.; Cutts, M.; Dasch, H.; Rubin, G.J.; Sevdalis, N. COVID-19 Vaccination Intention in the UK: Results from the COVID-19 Vaccination Acceptability Study (CoVAccS), a Nationally Representative Cross-Sectional Survey. Hum. Vaccines Immunother. 2021, 17, 1612–1621. [Google Scholar] [CrossRef]
- Bhopal, S.S.; Bagaria, J.; Olabi, B.; Bhopal, R. Children and Young People Remain at Low Risk of COVID-19 Mortality. Lancet Child Adolesc. Health 2021, 5, e12–e13. [Google Scholar] [CrossRef]
- Abbott, A.; Askelson, N.; Scherer, A.M.; Afifi, R.A. Critical Reflections on COVID-19 Communication Efforts Targeting Adolescents and Young Adults. J. Adolesc. Health 2020, 67, 159–160. [Google Scholar] [CrossRef] [PubMed]
- Gebhard, C.E.; Sütsch, C.; Bengs, S.; Deforth, M.; Buehler, K.P.; Hamouda, N.; Meisel, A.; Schuepbach, R.A.; Zinkernagel, A.S.; Brugger, S.D.; et al. Sex- and Gender-Specific Risk Factors of Post-COVID-19 Syndrome: A Population-Based Cohort Study in Switzerland. medRxiv 2021. [Google Scholar] [CrossRef]
- Menges, D.; Ballouz, T.; Anagnostopoulos, A.; Aschmann, H.E.; Domenghino, A.; Fehr, J.S.; Puhan, M.A. Burden of Post-COVID-19 Syndrome and Implications for Healthcare Service Planning: A Population-Based Cohort Study. PLoS ONE 2021, 16, e0254523. [Google Scholar] [CrossRef]
- Gangarosa, E.J.; Galazka, A.M.; Wolfe, C.R.; Phillips, L.M.; Gangarosa, R.E.; Miller, E.; Chen, R.T. Impact of Anti-Vaccine Movements on Pertussis Control: The Untold Story. Lancet 1998, 351, 356–361. [Google Scholar] [CrossRef]
- Smith, A.; Yarwood, J.; Salisbury, D.M. Tracking Mothers’ Attitudes to MMR Immunisation 1996–2006. Vaccine 2007, 25, 3996–4002. [Google Scholar] [CrossRef] [PubMed]
- Mason, B.W.; Donnelly, P.D. Impact of a Local Newspaper Campaign on the Uptake of the Measles Mumps and Rubella Vaccine. J. Epidemiol. Commun. Health 2000, 54, 473–474. [Google Scholar] [CrossRef][Green Version]
- Suppli, C.H.; Hansen, N.D.; Rasmussen, M.; Valentiner-Branth, P.; Krause, T.G.; Mølbak, K. Decline in HPV-Vaccination Uptake in Denmark—The Association between HPV-Related Media Coverage and HPV-Vaccination. BMC Public Health 2018, 18, 1360. [Google Scholar] [CrossRef]
- Hansen, N.D.; Mølbak, K.; Cox, I.J.; Lioma, C. Relationship between Media Coverage and Measles-Mumps-Rubella (MMR) Vaccination Uptake in Denmark: Retrospective Study. JMIR Public Health Surveill 2019, 5, e9544. [Google Scholar] [CrossRef] [PubMed]
- Jain, J.; Saurabh, S.; Kumar, P.; Verma, M.K.; Goel, A.D.; Gupta, M.K.; Bhardwaj, P.; Raghav, P.R. COVID-19 Vaccine Hesitancy among Medical Students in India. Epidemiol. Infect. 2021, 149, e132. [Google Scholar] [CrossRef]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J.A. Vaccine Hesitancy. Hum. Vaccines Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef]
- Romer, D.; Jamieson, K.H. Patterns of Media Use, Strength of Belief in COVID-19 Conspiracy Theories, and the Prevention of COVID-19 from March to July 2020 in the United States: Survey Study. J. Med. Internet Res. 2021, 23, e25215. [Google Scholar] [CrossRef] [PubMed]
- Kanyike, A.M.; Olum, R.; Kajjimu, J.; Ojilong, D.; Akech, G.M.; Nassozi, D.R.; Agira, D.; Wamala, N.K.; Asiimwe, A.; Matovu, D.; et al. Acceptance of the Coronavirus Disease-2019 Vaccine among Medical Students in Uganda. Trop. Med. Health 2021, 49, 37. [Google Scholar] [CrossRef]
- Kelly, B.J.; Southwell, B.G.; McCormack, L.A.; Bann, C.M.; MacDonald, P.D.M.; Frasier, A.M.; Bevc, C.A.; Brewer, N.T.; Squiers, L.B. Predictors of Willingness to Get a COVID-19 Vaccine in the U.S. BMC Infect. Dis. 2021, 21, 338. [Google Scholar] [CrossRef]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2020, 9, 16. [Google Scholar] [CrossRef]
- Soares, P.; Rocha, J.V.; Moniz, M.; Gama, A.; Laires, P.A.; Pedro, A.R.; Dias, S.; Leite, A.; Nunes, C. Factors Associated with COVID-19 Vaccine Hesitancy. Vaccines 2021, 9, 300. [Google Scholar] [CrossRef] [PubMed]
- Reiter, P.L.; Pennell, M.L.; Katz, M.L. Acceptability of a COVID-19 Vaccine among Adults in the United States: How Many People Would Get Vaccinated? Vaccine 2020, 38, 6500–6507. [Google Scholar] [CrossRef]
- Fisher, K.A.; Bloomstone, S.J.; Walder, J.; Crawford, S.; Fouayzi, H.; Mazor, K.M. Attitudes toward a Potential SARS-CoV-2 Vaccine: A Survey of U.S. Adults. Ann. Intern. Med. 2020, 173, 964–973. [Google Scholar] [CrossRef] [PubMed]
- Mercadante, A.R.; Law, A.V. Will They, or Won’t They? Examining Patients’ Vaccine Intention for Flu and COVID-19 Using the Health Belief Model. Res. Soc. Adm. Pharm. 2021, 17, 1596–1605. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, J.V.; Wyka, K.; Rauh, L.; Rabin, K.; Ratzan, S.; Gostin, L.O.; Larson, H.J.; El-Mohandes, A. Hesitant or Not? The Association of Age, Gender, and Education with Potential Acceptance of a COVID-19 Vaccine: A Country-Level Analysis. J. Health Commun. 2020, 25, 799–807. [Google Scholar] [CrossRef]
| Variable | Statistics | Women | Men | Total | |||
|---|---|---|---|---|---|---|---|
| Gender | n (%) | 912 | (70.3) | 385 | (29.7) | 1297 | (100.0) |
| Age | Md (IQR) | 24 | (22–27) | 24 | (23–27) | 24 | (22–27) |
| Health professions student *** | n (%) | 279 | (30.6) | 21 | (5.5) | 300 | (23.1) |
| (Very) good health status ** | n (%) | 689 | (75.6) | 263 | (68.3) | 952 | (73.4) |
| Anxiety level | n (%) | ||||||
| Minimal (0–4) | 246 | (27.0) | 109 | (28.3) | 355 | (27.4) | |
| Mild (5–9) | 358 | (39.3) | 149 | (38.7) | 507 | (39.1) | |
| Moderate (10–14) | 211 | (23.1) | 81 | (21.0) | 292 | (22.5) | |
| Severe (15–21) | 97 | (10.6) | 46 | (12.0) | 143 | (11.0) | |
| Trust in vaccination strategy ** | n (%) | 412 | (45.2) | 199 | (51.7) | 611 | (47.1) |
| Previous vaccinations | |||||||
| Seasonal influenza vaccination | n (%) | 193 | (21.2) | 72 | (18.7) | 265 | (20.4) |
| Travel vaccination * | n (%) | 449 | (49.2) | 156 | (40.5) | 605 | (46.7) |
| 5C vaccination antecedents | Mean (SD) | ||||||
| Confidence ** | 3.88 | (0.87) | 4.04 | (0.89) | 3.93 | (0.88) | |
| Complacency * | 1.96 | (0.71) | 2.07 | (0.82) | 1.99 | (0.75) | |
| Constraints | 1.36 | (0.60) | 1.43 | (0.71) | 1.38 | (0.64) | |
| Calculation *** | 3.73 | (0.90) | 3.44 | (1.05) | 3.64 | (0.96) | |
| Collective responsibility | 4.04 | (0.91) | 3.94 | (1.04) | 4.01 | (0.95) | |
| COVID-19 vaccination intention | n (%) | ||||||
| No | 71 | (7.8) | 27 | (7.0) | 98 | (7.6) | |
| Probably no | 126 | (13.8) | 54 | (14.0) | 180 | (13.9) | |
| Undecided | 144 | (15.8) | 43 | (11.2) | 187 | (14.4) | |
| Yes, after others | 136 | (14.9) | 58 | (15.1) | 194 | (15.0) | |
| Probably yes | 226 | (24.8) | 87 | (22.6) | 313 | (24.1) | |
| Yes | 209 | (22.9) | 116 | (30.1) | 325 | (25.1) | |
| Variable | OR | p | 95% CI |
|---|---|---|---|
| Gender (ref = women) | |||
| Men | 1.30 | 0.038 | 1.01–1.66 |
| Age (years) | 1.03 | 0.001 | 1.01–1.05 |
| Health professions student (ref = no) | |||
| Yes | 0.94 | 0.621 | 0.72–1.22 |
| Health status (ref = poor-fair health) | |||
| Very good/good health | 0.74 | 0.026 | 0.57–0.96 |
| Generalized anxiety (ref = minimal (0–4)) | |||
| Mild (5–9) | 0.94 | 0.663 | 0.73–1.23 |
| Moderate (10–14) | 0.97 | 0.854 | 0.71–1.33 |
| Severe (15–21) | 0.73 | 0.136 | 0.48–1.11 |
| Trust in vaccination strategy (ref = no) | |||
| Yes | 2.40 | 0.000 | 1.89–3.05 |
| Seasonal influenza vaccination (ref = no) | |||
| Yes | 1.39 | 0.019 | 1.06–1.83 |
| Travel vaccination (ref = no) | |||
| Yes | 1.29 | 0.020 | 1.04–1.60 |
| 5C vaccination antecedents | |||
| Confidence | 2.52 | 0.000 | 2.09–3.03 |
| Complacency | 0.79 | 0.018 | 0.66–0.96 |
| Constraints | 1.18 | 0.072 | 0.99–1.41 |
| Calculation | 0.79 | 0.000 | 0.70–0.89 |
| Collective responsibility | 4.47 | 0.000 | 3.69–5.40 |
| Cut points | |||
| #1 | 4.13 | 2.89–5.36 | |
| #2 | 6.44 | 5.17–7.71 | |
| #3 | 7.96 | 6.66–9.26 | |
| #4 | 9.23 | 7.91–10.55 | |
| #5 | 11.12 | 9.77–12.48 | |
| Number of observations | 1297 | ||
| Pseudo R-squared | 0.29 | ||
| Likelihood ratio Chi2 (15) | 1308 | ||
| p > Chi2 | 0.000 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dratva, J.; Wagner, A.; Zysset, A.; Volken, T. To Vaccinate or Not to Vaccinate—This Is the Question among Swiss University Students. Int. J. Environ. Res. Public Health 2021, 18, 9210. https://doi.org/10.3390/ijerph18179210
Dratva J, Wagner A, Zysset A, Volken T. To Vaccinate or Not to Vaccinate—This Is the Question among Swiss University Students. International Journal of Environmental Research and Public Health. 2021; 18(17):9210. https://doi.org/10.3390/ijerph18179210
Chicago/Turabian StyleDratva, Julia, Aylin Wagner, Annina Zysset, and Thomas Volken. 2021. "To Vaccinate or Not to Vaccinate—This Is the Question among Swiss University Students" International Journal of Environmental Research and Public Health 18, no. 17: 9210. https://doi.org/10.3390/ijerph18179210
APA StyleDratva, J., Wagner, A., Zysset, A., & Volken, T. (2021). To Vaccinate or Not to Vaccinate—This Is the Question among Swiss University Students. International Journal of Environmental Research and Public Health, 18(17), 9210. https://doi.org/10.3390/ijerph18179210









