A Scoping Review of the Relationship between Running and Mental Health
Abstract
1. Introduction
- (1)
- to provide an overview of what is known regarding the relationship between running and mental health outcomes in all age groups and populations
- (2)
- to highlight current knowledge gaps and research priorities
2. Materials and Methods
2.1. Identify Research Question
2.2. Identify Relevant Outcomes
2.3. Identify Relevant Studies
- Any geographical location
- All years between 1970 and 2019
- Quantitative effects of running on predetermined mental health outcomes
- ○
- Preventive effects (negative)
- ○
- Health promotion effects (positive)
- ○
- Intervention effects
- Any age group or sex
- Human studies
- Designs including primary research (cross-sectional, longitudinal, interventions and natural experiments with pre-post measures with or without non-running comparisons)
- Studies that mentioned walking as well as running were included because it is not possible to differentiate walkers from runners in events such as Parkrun.
- Specialist groups including elite, professional or competitive athletes.
- General physical or aerobic activity, rather than exclusively running
- Qualitative and ethnographic designs
- Systematic and scoping reviews (individual studies from identified reviews were included if relevant)
- Editorials, opinion pieces, magazine/newspaper articles, case reports and papers without primary data
- Focus on secondary mental health within clinical groups with specific physical or mental conditions that is not the condition being treated with running (e.g., effects on depression in patients with cancer)
- Evidence types including guidelines, unpublished and ongoing trials, annual reports, dissertations and conference proceedings
- Animal studies
- Unavailable in English
- Running intervention was part of a wider study where differentiating the individual effect of running was not possible (e.g., combined with weight management).
- Conference abstracts that were not published as full articles
Search Strategy and Databases
2.4. Study Selection
2.5. Charting the Data
- (1)
- Author(s), year of publication and geographical location of study
- (2)
- Mental health conditions examined
- (3)
- Sample size and population details
- (4)
- Study design
- (5)
- Measures used to quantify any change in mental health outcome(s)
- (6)
- Running dose (if applicable) and compliance (if applicable)
- (7)
- Whether running was beneficial and the main findings
2.6. Collating, Summarising and Reporting Results
3. Results
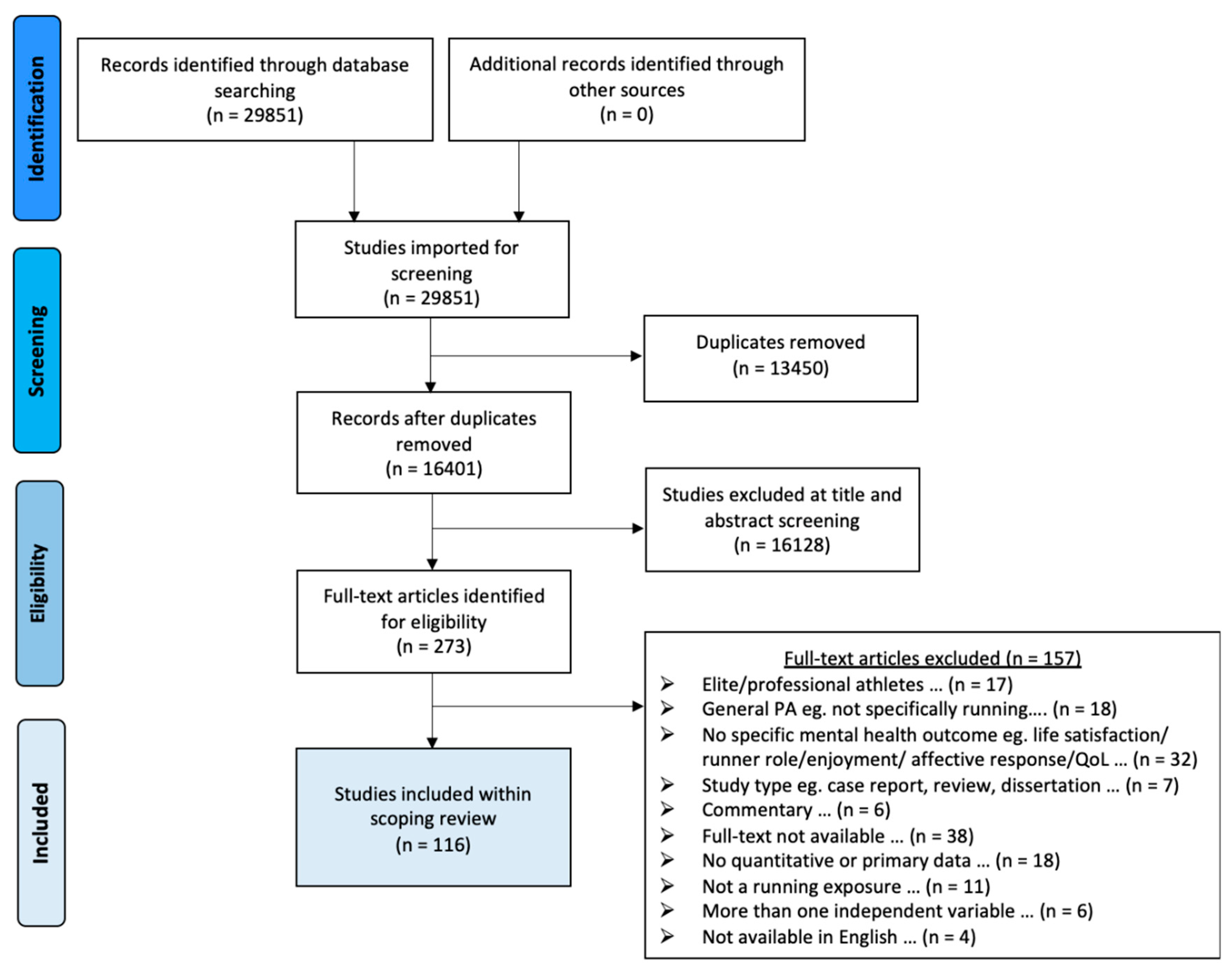
3.1. Included Studies
3.2. Category 1: Cross-Sectional Studies
3.2.1. Runners Versus Non-Running Comparisons
3.2.2. Runners Only
3.2.3. Runners Compared to Individuals with Eating Disorders
3.2.4. Prevented Runners
3.2.5. Runners Compared to Gym Exercisers
3.2.6. Summary of Cross-Sectional Evidence
3.3. Category 2: Acute Bouts of Running
3.3.1. Single Bouts
3.3.2. Double Bouts
3.3.3. Triple Bouts
3.3.4. Summary of Acute Bouts
3.4. Category 3: Longer-Term Interventions
Summary of Longer-Term Interventions
3.5. Summary of Key Findings
3.6. Evidence Gaps
- lack of studies in those aged over 45;
- lack of gender-specific approaches;
- few studies investigating clinical populations; and
- limited diversity in patient demographics.
4. Discussion
4.1. Principal Findings
4.2. Plausible Explanations for Findings
4.3. Comparison to Literature
4.4. Strengths and Limitations
4.5. Implications
4.6. Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Section | Item | PRISMA-ScR CHECKLIST ITEM | Reported on Page Number |
|---|---|---|---|
| Title | |||
| Title | 1 | Identify the report as a scoping review. | 1 |
| Abstract | |||
| Structured summary | 2 | Provide a structured summary that includes (as applicable) background, objectives, eligibility criteria, sources of evidence, charting methods, results and conclusions that relate to the review questions and objectives. | 1 |
| Introduction | |||
| Rationale | 3 | Describe the rationale for the review in the context of what is already known. Explain why the review questions/objectives lend themselves to a scoping review approach. | 1–2 |
| Objectives | 4 | Provide an explicit statement of the questions and objectives being addressed with reference to their key elements (e.g., population or participants, concepts and context) or other relevant key elements used to conceptualize the review questions and/or objectives. | 1–2 |
| Methods | |||
| Protocol and registration | 5 | Indicate whether a review protocol exists; state if and where it can be accessed (e.g., a Web address), and if available, provide registration information, including the registration number. | 2 |
| Eligibility criteria | 6 | Specify characteristics of the sources of evidence used as eligibility criteria (e.g., years considered, language and publication status), and provide a rationale. | 3 |
| Information sources * | 7 | Describe all information sources in the search (e.g., databases with dates of coverage and contact with authors to identify additional sources) as well as the date that the most recent search was executed. | 4 |
| Search | 8 | Present the full electronic search strategy for at least 1 database, including any limits used, such that it could be repeated. | Appendix B |
| Selection of sources of evidence † | 9 | State the process for selecting sources of evidence (i.e., screening and eligibility) included in the scoping review. | 4 |
| Data charting process ‡ | 10 | Describe the methods of charting data from the included sources of evidence (e.g., calibrated forms or forms that have been tested by the team before their use and whether data charting was done independently or in duplicate) and any processes for obtaining and confirming data from investigators. | 4 |
| Data items | 11 | List and define all variables for which data were sought and any assumptions and simplifications made. | 4 |
| Critical appraisal of individual sources of evidence § | 12 | If done, provide a rationale for conducting a critical appraisal of included sources of evidence; describe the methods used and how this information was used in any data synthesis (if appropriate). | N/A |
| Synthesis of results | 13 | Describe the methods of handling and summarizing the data that were charted. | 4 |
| Results | |||
| Selection of sources of evidence | 14 | Give numbers of sources of evidence screened, assessed for eligibility and included in the review, with reasons for exclusions at each stage, ideally using a flow diagram. | 4 |
| Characteristics of sources of evidence | 15 | For each source of evidence, present characteristics for which data were charted and provide the citations. | Table 2, Table 3, Table 4, Table 5 and Table 6 |
| Critical appraisal within sources of evidence | 16 | If done, present data on critical appraisal of included sources of evidence (see item 12). | N/A |
| Results of individual sources of evidence | 17 | For each included source of evidence, present the relevant data that were charted that relate to the review questions and objectives. | Table 2, Table 3, Table 4, Table 5 and Table 6 |
| Synthesis of results | 18 | Summarize and/or present the charting results as they relate to the review questions and objectives. | 5–40 |
| Discussion | |||
| Summary of evidence | 19 | Summarize the main results (including an overview of concepts, themes and types of evidence available), link to the review questions and objectives and consider the relevance to key groups. | 40–41 |
| Limitations | 20 | Discuss the limitations of the scoping review process. | 41 |
| Conclusions | 21 | Provide a general interpretation of the results with respect to the review questions and objectives as well as potential implications and/or next steps. | 42 |
| Funding | |||
| Funding | 22 | Describe sources of funding for the included sources of evidence as well as sources of funding for the scoping review. Describe the role of the funders of the scoping review. | 43 |
Appendix References
- (1)
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32.
- (2)
- Levac, D.; Colquhoun, H; O’Brien, K.K. Scoping studies: Advancing the methodology. Implement Sci. 2010, 5, 69, doi:10.1186/1748-5908-5-69.
- (3)
- Peters, M.D.; Godfrey, C.M.; Khalil, H.; McInerney, P.; Parker, D.; Soares, C.B. Guidance for conducting systematic scoping reviews. Int. J. Evid. Based Healthc. 2015, 13, 141–146, doi:10.1097/XEB.0000000000000050.
- (4)
- Peters, M.D.J.; Godfrey, C.; McInerney, P.; Baldini Soares, C.; Khalil, H.; Parker, D. Scoping reviews. In Joanna Briggs Institute Reviewer’s Manual; Aromataris, E., Munn, Z., Eds.; Joanna Briggs Inst: Adelaide, Australia, 2017.
Appendix B
| Notes for Database | Ovid (Embase) | Ovid (Medline) | Sport DISCUS (Ebscohost) | ProQuest Social Science Journals |
|---|---|---|---|---|
| Ti,ab Searches Title & Abstract | Ti,ab Searches Title & Abstract | AB Searches Abstract | Ab Searches Abstract | |
| Running Search Terms | ||||
| Run*, Jog*, Sprint*, Park-run, Orienteer, Orienteering, Marathon, Marathon-running, Treadmill | ||||
| Mental Health Search Terms | ||||
| Mental Health, Mental illness, Mental state, Emotions, Emotional, Depression, Depressive disorder, depressive therapy, Postnatal depression, Postpartum depression, Seasonal affective disorder, Situational depression, Atypical depression, Persistent depressive disorder, anxiety, loneliness, stress, mood, self-efficacy, sleep, psychological, psychological characteristics, psychology, eating disorder, disordered eating, anorexia, bulimia, exercise, health status disparities, quality of life, motivation, adjustment disorder, sick role. relaxation, lifestyle, exercise therapy, social support | ||||
| NOT search Terms | ||||
| Rodent, mouse, rat, bovine, pig, animal*, horses, mice, ecology, dermatology, epigenetics, gene*, molecule*, cell*, phenotype, drug*, hormone*, food, nutrient*, glucose, imaging, football, tennis, swimming, heart, troponin, cardiology, lung, respiratory, bone, cesarean, newborn, breast-feeding, HIV, cough, rectal, protocol, procedure, surgery, operation, stroke, sacroiliitis, COPD, asthma, Apnoea, angina, allergy, railway, falling | ||||
| Search Syntax | (remember the ‘adj’ function) | (remember the ‘adj’ function) | (remember the ‘adj’ function) | (remember the ‘adj’ function) |
| (((“mental-health” or “mental-illness” or “mental-state” or emotions or emotional or depression or “depressive-disorder” or “depressive-therapy” or “postpartum-depression” or “seasonal-affective-disorder” or “situational-depression” or “atypical-depression” or “persistent-depressive-disorder” or anxiety or loneliness or stress or mood or “self-efficacy” or sleep or psychological or “psychological-characteristics” or psychology or “eating-disorder” or “disordered-eating” or anorexia or Bulimia or exercise or “health-status-disparities” or “quality-of-life” or motivation or “adjustment-disorder” or “sick-role” or relaxation or lifestyle or “exercise-therapy” or “social-support”)) AND (run* or Jog* or sprint* or “park-run” or orienteer or orienteering or marathon or “Marathon-running” or treadmill) NOT (dermatology OR epigenetics OR gene* OR drug* OR surgery OR hormone* OR food OR imaging OR animal* OR football OR tennis OR swimming OR rodent OR mouse OR rat OR pig OR bovine OR phenotype or Heart or cardiology OR lung or bone OR caesarean OR HIV OR troponin OR cough OR protocol OR breast-feeding OR cell* OR sacroiliitis OR rectal or procedure OR COPD or respiratory OR nutrient* OR glucose or newborn OR stroke OR asthma OR operation OR horses OR falling OR railway OR molecule* OR apn?ea OR angina OR allergy OR mice OR ecology)).ab,ti. | (((“mental-health” or “mental-illness” or “mental-state” or emotions or emotional or depression or “depressive-disorder” or “depressive-therapy” or “postpartum-depression” or “seasonal-affective-disorder” or “situational-depression” or “atypical-depression” or “persistent-depressive-disorder” or anxiety or loneliness or stress or mood or “self-efficacy” or sleep or psychological or “psychological-characteristics” or psychology or “eating-disorder” or “disordered-eating” or anorexia or Bulimia or exercise or “health-status-disparities” or “quality-of-life” or motivation or “adjustment-disorder” or “sick-role” or relaxation or lifestyle or “exercise-therapy” or “social-support”) and (run* or Jog* or sprint* or “park-run” or orienteer or orienteering or marathon or “Marathon-running” or treadmill)) not (dermatology or epigenetics or gene* or drug* or surgery or hormone* or food or imaging or animal* or football or tennis or swimming or rodent or mouse or rat or pig or bovine or phenotype or Heart or cardiology or lung or bone or caesarean or HIV or troponin or cough or protocol or breast-feeding or cell* or sacroiliitis or rectal or procedure or COPD or respiratory or nutrient* or glucose or newborn or stroke or asthma or operation or horses or falling or railway or molecule* or apn?ea or angina or allergy or mice or ecology)).ab,ti. | (AB(run* OR jog* OR sprint OR “park run” OR orienteer OR orienteering OR marathon OR “marathon-running” OR treadmill) AND AB(“mental health” OR “mental illness” OR “mental state” OR emotions OR emotional OR depression OR “depressive disorder” OR “depressive therapy” OR “postpartum depression” OR “seasonal affective disorder” OR “situational depression” OR “atypical depression” OR “persistent depressive disorder” OR anxiety OR loneliness OR stress OR mood OR “self-efficacy” OR sleep OR psychological OR “psychological characteristics” OR psychology OR “eating disorder” OR “disordered eating” OR anorexia OR bulimia OR exercise OR “health status disparities” OR “quality-of-life” OR motivation OR “adjustment disorder” OR “sick role” OR relaxation OR lifestyle OR “exercise therapy” OR “social-support”)) NOT (dermatology OR epigenetics OR gene* OR drug* OR surgery OR hormone* OR food OR imaging OR animal* OR football OR tennis OR swimming OR rodent OR mouse OR rat OR pig OR bovine OR phenotype or Heart or cardiology OR lung or bone OR caesarean OR HIV OR troponin OR cough OR protocol OR breast-feeding OR cell* OR sacroiliitis OR rectal or procedure OR COPD or respiratory OR nutrient* OR glucose or newborn OR stroke OR asthma OR operation OR horses OR falling OR railway OR molecule* OR apnoea OR angina OR allergy OR mice OR ecology) | (ab((run* OR jog* OR sprint OR “park run” OR orienteer OR orienteering OR marathon OR “marathon-running” OR treadmill)) AND ab((“mental health” OR “mental illness” OR “mental state” OR emotions OR emotional OR depression OR “depressive disorder” OR “depressive therapy” OR “postpartum depression” OR “seasonal affective disorder” OR “situational depression” OR “atypical depression” OR “persistent depressive disorder” OR anxiety OR loneliness OR stress OR mood OR “self-efficacy” OR sleep OR psychological OR “psychological characteristics” OR psychology OR “eating disorder” OR “disordered eating” OR anorexia OR bulimia OR exercise OR “health status disparities” OR “quality-of-life” OR motivation OR “adjustment disorder” OR “sick role” OR relaxation OR lifestyle OR “exercise therapy” OR “social-support”)) NOT ab((dermatology OR epigenetics OR gene* OR drug* OR surgery OR hormone* OR food OR imaging OR animal* OR football OR tennis OR swimming OR rodent OR mouse OR rat OR pig OR bovine OR phenotype OR Heart OR cardiology OR lung OR bone OR caesarean OR HIV OR troponin OR cough OR protocol OR breast-feeding OR cell* OR sacroiliitis OR rectal OR procedure OR COPD OR respiratory OR nutrient* OR glucose OR newborn OR stroke OR asthma OR operation OR horses OR falling OR railway OR molecule* OR apnoea OR angina OR allergy OR mice OR ecology))) AND (stype.exact(“Scholarly Journals”) AND la.exact(“ENG”)) | |
| Search complete? | Yes | Yes | Yes | Yes |
| Search saved? | Yes | Yes | Yes | Yes |
| Saved under: | Embase RunningMH | Medline RunningMH | Sport Discus Running MH | ProQuest RunningMH |
| Number of hits: | 10,131 Text results (this had a limit of only human studies, as well as a limit for articles and articles in press applied to the search) | 10,154 text results (this had a limit of human studies applied to the search) | 3461 (this had a limit of English studies only, and academic journal only applied to the search) | 5933 (this search was carried out within the sports medicine and education index database and in the social sciences database) |
| Uploaded to Covidence? | Yes | Yes | Yes | Yes |
References
- Whiteford, H.A.; Ferrari, A.J.; Degenhardt, L.; Feigin, V.; Vos, T. The global burden of mental, neurological and substance use disorders: An analysis from the Global Burden of Disease Study 2010. PLoS ONE 2015, 10, e0116820. [Google Scholar] [CrossRef] [PubMed]
- Lopez, A.D.; Murray, C.C.J.L. The global burden of disease, 1990–2020. Nat. Med. 1998, 4, 1241–1243. [Google Scholar] [CrossRef] [PubMed]
- GBD 2017 DALYs and HALE Collaborators. ‘Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet Lond. Engl. 2018, 392, 1859–1922. [Google Scholar] [CrossRef]
- Demyttenaere, K.; Bruffaerts, R.; Posada-Villa, J.; Gasquet, I.; Kovess, V.; Lepine, J.P.; Angermeyer, M.C.; Bernert, S.; De Girolamo, G.; Morosini, P.; et al. Prevalence, severity, and unmet need for treatment of mental disorders in the World Health Organization World Mental Health Surveys. JAMA 2004, 291, 2581–2590. [Google Scholar] [CrossRef] [PubMed]
- Chan, J.S.Y.; Liu, G.; Liang, D.; Deng, K.; Wu, J.; Yan, J.H. Special Issue-Therapeutic Benefits of Physical Activity for Mood: A Systematic Review on the Effects of Exercise Intensity, Duration, and Modality. J. Psychol. 2019, 153, 102–125. [Google Scholar] [CrossRef]
- Richards, J.; Jiang, X.; Kelly, P.; Chau, J.; Bauman, A.; Ding, D. Don’t worry, be happy: Cross-sectional associations between physical activity and happiness in 15 European countries. BMC Public Health 2015, 15, 53. [Google Scholar] [CrossRef]
- Schuch, F.B.; Vancampfort, D.; Richards, J.; Rosenbaum, S.; Ward, P.B.; Stubbs, B. Exercise as a treatment for depression: A meta-analysis adjusting for publication bias. J. Psychiatr. Res. 2016, 77, 42–51. [Google Scholar] [CrossRef]
- Kelly, P.; Williamson, C.; Niven, A.G.; Hunter, R.; Mutrie, N.; Richards, J. Walking on sunshine: Scoping review of the evidence for walking and mental health. Br. J. Sports Med. 2018, 52, 800–806. [Google Scholar] [CrossRef]
- Active Lives. Sport England. Available online: https://www.sportengland.org/know-your-audience/data/active-lives (accessed on 27 September 2020).
- Couch to 5K: Week by Week-NHS’. Available online: https://www.nhs.uk/live-well/exercise/couch-to-5k-week-by-week/ (accessed on 28 November 2019).
- Nonprofit Girls Empowerment Program | Girls on the Run. GOTR. Available online: https://www.girlsontherun.org/ (accessed on 28 November 2019).
- Parkrun Eases the Loneliness of the Long-Distance Runner | British Journal of General Practice’. Available online: https://bjgp.org/content/64/625/408 (accessed on 28 November 2019).
- Sifers, S.K.; Shea, D.N. Evaluations of Girls on the Run/Girls on Track to Enhance Self-Esteem and Well-Being. J. Clin. Sport Psychol. 2013, 7, 77–85. [Google Scholar] [CrossRef]
- Grunseit, A.; Richards, J.; Merom, D. Running on a high: Parkrun and personal well-being. BMC Public Health 2017, 18, 59. [Google Scholar] [CrossRef]
- Parkrun Practice. Available online: https://elearning.rcgp.org.uk/course/view.php?id=723 (accessed on 28 November 2019).
- Patel, V.; Garrison, P.; Mari, J.D.; Minas, H.; Prince, M.; Saxena, S. The Lancet’s Series on Global Mental Health: 1 year on. Lancet 2008, 372, 1354–1357. [Google Scholar] [CrossRef]
- Scoping Studies: Towards a Methodological Framework: International Journal of Social Research Methodology: Vol 8, No 1’. Available online: https://www.tandfonline.com/doi/full/10.1080/1364557032000119616 (accessed on 27 September 2019).
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467. [Google Scholar] [CrossRef]
- American Psychological Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5®); American Psychiatric Pub: Washington, DC, USA, 2013. [Google Scholar]
- Physical Activity Guidelines Advisory Committee Report, 2008 to the Secretary of Health and Human Services: (525442010-001); American Psychological Association: Worcester, MA, USA, 2008. [CrossRef]
- Zulkosky, K. Self-Efficacy: A Concept Analysis. Nurs. Forum (Auckl.) 2009, 44, 93–102. [Google Scholar] [CrossRef]
- Ridner, S.H. Psychological distress: Concept analysis. J. Adv. Nurs. 2004, 45, 536–545. [Google Scholar] [CrossRef] [PubMed]
- Fairburn, C.G.; Brownell, K.D. Eating Disorders and Obesity: A Comprehensive Handbook; Guilford Press: New York, NY, USA, 2005. [Google Scholar]
- Pressman, S.D.; Cohen, S. Does positive affect influence health? Psychol. Bull. 2005, 131, 925–971. [Google Scholar] [CrossRef]
- Goodman, A. Addiction: Definition and implications. Br. J. Addict. 1990, 85, 1403–1408. [Google Scholar] [CrossRef]
- Ryff, C.D. Eudaimonic well-being and health: Mapping consequences of self-realization. In The Best within Us: Positive Psychology Perspectives on Eudaimonia; American Psychological Association: Washington, DC, USA, 2013; pp. 77–98. [Google Scholar]
- Kinch, J.W. A Formalized Theory of the Self-Concept. Am. J. Sociol. 1963, 68, 481–486. [Google Scholar] [CrossRef]
- Lane, A.M.; Terry, P.C. The Nature of Mood: Development of a Conceptual Model with a Focus on Depression. J. Appl. Sport Psychol. 2000, 12, 16–33. [Google Scholar] [CrossRef]
- Wilson, V.E.; Morley, N.C.; Bird, E.I. Mood profiles of marathon runners, joggers and non-exercisers. Percept. Mot. Skills 1980, 50, 117–118. [Google Scholar] [CrossRef]
- Joesting, J. Running and Depression. Percept. Mot. Skills 1981, 52, 442. [Google Scholar] [CrossRef]
- Jorgenson, D.E.; Jorgenson, C.B. Perceived Effects of Running/Jogging: A Social Survey of Three Clubs. Int. Rev. Sport Sociol. 1981, 16, 75–85. [Google Scholar] [CrossRef]
- Valliant, P.M.; Bennie, F.A.; Valiant, J.J. Do marathoners differ from joggers in personality profile: A sports psychology approach. J. Sports Med. Phys. Fit. 1981, 21, 62–67. [Google Scholar]
- Francis, K.T.; Carter, R. Psychological characteristic of joggers. J. Sports Med. Phys. Fit. 1982, 22, 386–391. [Google Scholar]
- Hailey, B.J.; Bailey, L.A. Negative addiction in runners: A quantitative approach. J. Sport Behav. 1982, 5, 150–154. [Google Scholar]
- Callen, K.E. Mental and emotional aspects of long-distance running. Psychosomatics 1983, 24, 133–134. [Google Scholar] [CrossRef]
- Galle, P.C.; Freeman, E.W.; Galle, M.G.; Huggins, G.R.; Sondheimer, S.J. Physiologic and psychologic profiles in a survey of women runners. Fertil. Steril. 1983, 39, 633–639. [Google Scholar] [CrossRef]
- Lobstein, D.D.; Mosbacher, B.J.; Ismail, A.H. Depression as a powerful discriminator between physically active and sedentary middle-aged men. J. Psychosom. Res. 1983, 27, 69–76. [Google Scholar] [CrossRef]
- Rudy, E.B.; Estok, P.J. Intensity of jogging: Its relationship to selected physical and psychosocial variables in women. West. J. Nurs. Res. 1983, 5, 325–336. [Google Scholar] [CrossRef]
- Goldfarb, L.A.; Plante, T.G. Fear of fat in runners: An examination of the connection between anorexia nervosa and distance running. Psychol. Rep. 1984, 55, 296. [Google Scholar] [CrossRef]
- Guyot, G.W.; Fairchild, L.; Nickens, J. Death concerns of runners and nonrunners. J. Sports Med. Phys. Fit. 1984, 24, 139–143. [Google Scholar]
- Rape, R.N. Running and Depression. Percept. Mot. Skills 1987, 64 (Suppl. 3), 1303–1310. [Google Scholar] [CrossRef]
- Weight, L.M.; Noakes, T.D. Is running an analog of anorexia?: A survey of the incidence of eating disorders in female distance runners. Med. Sci. Sports Exerc. 1987, 19, 213–217. [Google Scholar] [CrossRef] [PubMed]
- Chan, C.S.; Grossman, H.Y. Psychological effects of running loss on consistent runners. Percept. Mot. Skills 1988, 66, 875–883. [Google Scholar] [CrossRef] [PubMed]
- Frazier, S.E. Mood state profiles of chronic exercisers with differing abilities. Int. J. Sport Psychol. 1988, 19, 65–71. [Google Scholar]
- Lobstein, D.D.; Ismail, A.H.; Rasmussen, C.L. Beta-endorphin and components of emotionality discriminate between physically active and sedentary men. Biol. Psychiatry 1989, 26, 3–14. [Google Scholar] [CrossRef]
- Lobstein, D.D.; Rasmussen, C.L.; Dunphy, G.E.; Dunphy, M.J. Beta-endorphin and components of depression as powerful discriminators between joggers and sedentary middle-aged men. J. Psychosom. Res. 1989, 33, 293–305. [Google Scholar] [CrossRef]
- Nouri, S.; Beer, J. Relations of moderate physical exercise to scores on hostility, aggression, and aggression, and trait-anxiety. Percept. Mot. Skills 1989, 68 Pt 2, 1191–1194. [Google Scholar] [CrossRef]
- Chan, D.W.; Lai, B. Psychological aspects of long-distance running among Chinese male runners in Hong Kong. Int. J. Psychosom. Off. Publ. Int. Psychosom. Inst. 1990, 37, 30–34. [Google Scholar]
- Chapman, C.L.; de Castro, J.M. Running addiction: Measurement and associated psychological characteristics. J. Sports Med. Phys. Fit. 1990, 30, 283–290. [Google Scholar]
- Guyot, W.G. Psychological and medical factors associated with pain running. J. Sports Med. Phys. Fit. 1991, 31, 452–460. [Google Scholar]
- Maresh, C.M.; Sheckley, B.G.; Allen, G.J.; Camaione, D.N.; Sinatra, S.T. Middle age male distance runners: Physiological and psychological profiles. J. Sports Med. Phys. Fit. 1991, 31, 461–469. [Google Scholar]
- Gleaves, D.H.; Williamson, D.A.; Fuller, R.D. Bulimia nervosa symptomatology and body image disturbance associated with distance running and weight loss. Br. J. Sports Med. 1992, 26, 157–160. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Coen, S.P.; Ogles, B.M. Psychological characteristics of the obligatory runner: A critical examination of the anorexia analogue hypothesis. J. Sport Exerc. Psychol. 1993, 15, 338–354. [Google Scholar] [CrossRef]
- Furst, D.M.; Germone, K. Negative addiction in male and female runners and exercisers. Percept. Mot. Skills 1993, 77, 192–194. [Google Scholar] [CrossRef]
- Masters, K.S.; Ogles, B.M.; Jolton, J.A. The development of an instrument to measure motivation for marathon running: The Motivations of Marathoners Scales (MOMS). Res. Q. Exerc. Sport 1993, 64, 134–143. [Google Scholar] [CrossRef]
- Pierce, E.F.; McGowan, R.W.; Lynn, T.D. Exercise dependence in relation to competitive orientation of runners. J. Sports Med. Phys. Fitness 1993, 33, 189–193. [Google Scholar]
- Klock, S.C.; DeSouza, M.J. Eating disorder characteristics and psychiatric symptomatology of eumenorrheic and amenorrheic runners. Int. J. Eat. Disord. 1995, 17, 161–166. [Google Scholar] [CrossRef]
- Thornton, E.W.; Scott, S.E. Motivation in the committed runner: Correlations between self-report scales and behaviour. Health Promot. Int. 1995, 10, 177–184. [Google Scholar] [CrossRef]
- Powers, P.S.; Schocken, D.D.; Boyd, F.R. Comparison of habitual runners and anorexia nervosa patients. Int. J. Eat. Disord. 1998, 23, 133–143. [Google Scholar] [CrossRef]
- Slay, H.A.; Hayaki, J.; Napolitano, M.A.; Brownell, K.D. Motivations for running and eating attitudes in obligatory versus nonobligatory runners. Int. J. Eat. Disord. 1998, 23, 267–275. [Google Scholar] [CrossRef]
- Ryujin, D.H.; Breaux, C.; Marks, A.D. Symptoms of eating disorders among female distance runners: Can the inconsistencies be unraveled? Women Health 1999, 30, 71–83. [Google Scholar] [CrossRef] [PubMed]
- Leedy, G. Commitment to Distance Running: Coping Mechanisms or Addiction. J. Sport Behav. Mob. Ala 2000, 23, 255–270. [Google Scholar]
- Edwards, S.D.; Ngcobo, H.S.; Edwards, D.J.; Palavar, K. Exploring the relationship between physical activity, psychological well-being and physical self- perception in different exercise groups. South Afr. J. Res. Sport Phys. Educ. Recreat. 2005, 27, 59–74. [Google Scholar] [CrossRef]
- Schnohr, P.; Kristensen, T.S.; Prescott, E.; Scharling, H. Stress and life dissatisfaction are inversely associated with jogging and other types of physical activity in leisure time--The Copenhagen City Heart Study. Scand. J. Med. Sci. Sports 2005, 15, 107–112. [Google Scholar] [CrossRef] [PubMed]
- Strachan, S.M.; Woodgate, J.; Brawley, L.R.; Tse, A. The Relationship of Self-Efficacy and Self-Identity to Long-Term Maintenance of Vigorous Physical Activity. J. Appl. Biobehav. Res. 2005, 10, 98–112. [Google Scholar] [CrossRef]
- Galper, D.I.; Trivedi, M.H.; Barlow, C.E.; Dunn, A.L.; Kampert, J.B. Inverse association between physical inactivity and mental health in men and women. Med. Sci. Sports Exerc. 2006, 38, 173–178. [Google Scholar] [CrossRef]
- Luszczynska, A.; Mazurkiewicz, M.; Ziegelmann, J.P.; Schwarzer, R. Recovery self-efficacy and intention as predictors of running or jogging behavior: A cross-lagged panel analysis over a two-year period. Psychol. Sport Exerc. 2007, 8, 247–260. [Google Scholar] [CrossRef]
- Smith, D.; Wright, C.; Winrow, D. Exercise dependence and social physique anxiety in competitive and non-competitive runners. Int. J. Sport Exerc. Psychol. 2010, 8, 61–69. [Google Scholar] [CrossRef]
- Gapin, J.I.; Petruzzello, S.J. Athletic identity and disordered eating in obligatory and non-obligatory runners. J. Sports Sci. 2011, 29, 1001–1010. [Google Scholar] [CrossRef]
- Wadas, G.; DeBeliso, M. Disordered eating, eating attitudes, and reasons for exercise among male high school cross country runners. Sport J. 2014, 17. Available online: https://www.cabdirect.org/cabdirect/abstract/20153072464 (accessed on 15 July 2020).
- Download Citation of The Relationship between Motivations, Perceived Control, and Mental Toughness Among Marathon Runners. ResearchGate. Available online: https://www.researchgate.net/publication/325793259_The_relationship_between_motivations_perceived_control_and_mental_toughness_among_marathon_runners (accessed on 15 July 2020).
- Lucidi, F.; Pica, G.; Mallia, L.; Castrucci, E.; Manganelli, S.; Bélanger, J.J.; Pierro, A. Running away from stress: How regulatory modes prospectively affect athletes’ stress through passion. Scand. J. Med. Sci. Sports 2016, 26, 703–711. [Google Scholar] [CrossRef] [PubMed]
- Batmyagmar, D.; Kundi, M.; Ponocny-Seliger, E.; Lukas, I.; Lehrner, J.; Haslacher, H.; Winker, R. High intensity endurance training is associated with better quality of life, but not with improved cognitive functions in elderly marathon runners. Sci. Rep. 2019, 9, 4629. [Google Scholar] [CrossRef]
- Cleland, V.; Nash, M.; Sharman, M.J.; Claflin, S. Exploring the Health-Promoting Potential of the “parkrun” Phenomenon: What Factors are Associated With Higher Levels of Participation? Am. J. Health Promot. AJHP 2019, 33, 13–23. [Google Scholar] [CrossRef]
- Lukács, A.; Sasvári, P.; Varga, B.; Mayer, K. Exercise addiction and its related factors in amateur runners. J. Behav. Addict. 2019, 8, 343–349. [Google Scholar]
- Solmon, M.; Stewart, L. Changes in self-efficacy and affect during a 15-week marathon training program. Int. J. Sport Psychol. 2013, 44, 55–68. [Google Scholar]
- Nowlis, D.P.; Greenberg, N. Empirical description of effects of exercise on mood. Percept. Mot. Skills 1979, 49, 1001–1002. [Google Scholar] [CrossRef]
- Wilson, V.E.; Berger, B.G.; Bird, E.I. Effects of running and of an exercise class on anxiety. Percept. Mot. Skills 1981, 53, 472–474. [Google Scholar] [CrossRef]
- Markoff, R.A.; Ryan, P.; Young, T. Endorphins and mood changes in long-distance running. Med. Sci. Sports Exerc. 1982, 14, 11–15. [Google Scholar] [CrossRef] [PubMed]
- Thaxton, L. Physiological and Psychological Effects of Short-term Exercise Addiction on Habitual Runners. J. Sport Exerc. Psychol. 1982, 4, 73–80. [Google Scholar] [CrossRef]
- McGowan, R.W.; Pierce, E.F.; Jordan, D. Mood alterations with a single bout of physical activity. Percept. Mot. Skills 1991, 72 Pt 2, 1203–1209. [Google Scholar] [CrossRef]
- Goode, K.T.; Roth, D.L. Factor Analysis of Cognitions during Running: Association with Mood Change. J. Sport Exerc. Psychol. 1993, 15, 375–389. [Google Scholar] [CrossRef]
- Morris, M.; Salmon, P. Qualitative and quantitative effects of running on mood. J. Sports Med. Phys. Fit. 1994, 34, 284–291. [Google Scholar]
- Rudolph, D.L.; Butki, B.D. Self-efficacy and affective responses to short bouts of exercise. J. Appl. Sport Psychol. 1998, 10, 268–280. [Google Scholar] [CrossRef]
- Cox, R.H.; Thomas, T.R.; Davis, J.E. Positive and negative affect associated with an acute bout of aerobic exercise. J. Exerc. Physiol. Online 2001, 4, 13–20. [Google Scholar]
- O’Halloran, P.D.; Murphy, G.C.; Webster, K.E. Measure of beliefs about improvements in mood associated with exercise. Psychol. Rep. 2002, 90 Pt 1, 834–840. [Google Scholar] [CrossRef]
- Szabo, A. The Acute Effects of Humor and Exercise on Mood and Anxiety. J. Leis. Res. 2003, 35, 152–162. [Google Scholar] [CrossRef]
- O’Halloran, P.D.; Murphy, G.C.; Webster, K. Mood during a 60-minute treadmill run: Timing and type of mood change. Int. J. Sport Psychol. 2004, 35, 309–327. [Google Scholar]
- Robbins, L.B.; Pender, N.J.; Ronis, D.L.; Kazanis, A.S.; Pis, M.B. Physical activity, self-efficacy, and perceived exertion among adolescents. Res. Nurs. Health 2004, 27, 435–446. [Google Scholar] [CrossRef] [PubMed]
- Pretty, J.; Peacock, J.; Sellens, M.; Griffin, M. The mental and physical health outcomes of green exercise. Int. J. Environ. Health Res. 2005, 15, 319–337. [Google Scholar] [CrossRef]
- Hoffman, M.D.; Hoffman, D.R. Exercisers achieve greater acute exercise-induced mood enhancement than nonexercisers. Arch. Phys. Med. Rehabil. 2008, 89, 358–363. [Google Scholar] [CrossRef]
- Kwan, B.M.; Bryan, A.D. Affective response to exercise as a component of exercise motivation: Attitudes, norms, self-efficacy, and temporal stability of intentions. Psychol. Sport Exerc. 2010, 11, 71–79. [Google Scholar] [CrossRef] [PubMed]
- Weinstein, A.A.; Deuster, P.A.; Francis, J.L.; Beadling, C.; Kop, W.J. The Role of Depression in Short-Term Mood and Fatigue Responses to Acute Exercise. Int. J. Behav. Med. 2010, 17, 51–57. [Google Scholar] [CrossRef]
- Anderson, R.J.; Brice, S. The mood-enhancing benefits of exercise: Memory biases augment the effect. Psychol. Sport Exerc. 2011, 12, 79–82. [Google Scholar] [CrossRef]
- Kane, I.; Robertson, R.; Fertman, C.; Nagle, E.; McConnaha, W.; Rabin, B. Self-efficacy and enjoyment of middle school children performing the Progressive Aerobic Cardiovascular Endurance Run (PACER). Percept. Mot. Skills 2013, 117, 470–483. [Google Scholar] [CrossRef]
- Szabo, A.; Abrahám, J. The psychological benefits of recreational running: A field study. Psychol. Health Med. 2013, 18, 251–261. [Google Scholar] [CrossRef]
- McDowell, C.P.; Campbell, M.J.; Herring, M.P. Sex-Related Differences in Mood Responses to Acute Aerobic Exercise. Med. Sci. Sports Exerc. 2016, 48, 1798–1802. [Google Scholar] [CrossRef]
- Rogerson, M.; Brown, D.K.; Sandercock, G.; Wooller, J.-J.; Barton, J. A comparison of four typical green exercise environments and prediction of psychological health outcomes. Perspect. Public Health 2016, 136, 171–180. [Google Scholar] [CrossRef]
- Edwards, M.K.; Rhodes, R.E.; Loprinzi, P.D. A Randomized Control Intervention Investigating the Effects of Acute Exercise on Emotional Regulation. Am. J. Health Behav. 2017, 41, 534–543. [Google Scholar] [CrossRef]
- Wildmann, J.; Krüger, A.; Schmole, M.; Niemann, J.; Matthaei, H. Increase of circulating beta-endorphin-like immunoreactivity correlates with the change in feeling of pleasantness after running. Life Sci. 1986, 38, 997–1003. [Google Scholar] [CrossRef]
- O’Connor, P.J.; Carda, R.D.; Graf, B.K. Anxiety and intense running exercise in the presence and absence of interpersonal competition. Int. J. Sports Med. 1991, 12, 423–426. [Google Scholar] [CrossRef]
- Nabetani, T.; Tokunaga, M. The effect of short-term (10- and 15-min) running at self-selected intensity on mood alteration. J. Physiol. Anthropol. Appl. Hum. Sci. 2001, 20, 231–239. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bodin, M.; Hartig, T. Does the outdoor environment matter for psychological restoration gained through running? Psychol. Sport Exerc. 2003, 4, 141–153. [Google Scholar] [CrossRef]
- Butryn, T.M.; Furst, D.M. The effects of park and urban settings on the moods and cognitive strategies of female runners. J. Sport Behav. 2003, 26, 335–355. [Google Scholar]
- Kerr, J.H.; Fujiyama, H.; Sugano, A.; Okamura, T.; Chang, M.; Onouha, F. Psychological responses to exercising in laboratory and natural environments. Psychol. Sport Exerc. 2006, 7, 345–359. [Google Scholar] [CrossRef]
- Rose, E.A.; Parfitt, G. Exercise experience influences affective and motivational outcomes of prescribed and self-selected intensity exercise. Scand. J. Med. Sci. Sports 2012, 22, 265–277. [Google Scholar] [CrossRef]
- Reed, K.; Wood, C.; Barton, J.; Pretty, J.N.; Cohen, D.; Sandercock, G.R.H. A repeated measures experiment of green exercise to improve self-esteem in UK school children. PLoS ONE 2013, 8, e69176. [Google Scholar] [CrossRef]
- Krotee, M.L. The Effects of Various Physical Activity Situational Settings on the Anxiety Level of Children. J. Sport Behav. Mob. Ala 1980, 3, 158–164. [Google Scholar]
- Harte, J.L.; Eifert, G.H. The effects of running, environment, and attentional focus on athletes’ catecholamine and cortisol levels and mood. Psychophysiology 1995, 32, 49–54. [Google Scholar] [CrossRef]
- Berger, B.; Owen, D.; Motl, R.; Parks, L. Relationship between expectancy of psychological benefits and mood alteration in joggers. Int. J. Sport Psychol. 1998, 29, 1–16. [Google Scholar]
- Markowitz, S.M.; Arent, S.M. The exercise and affect relationship: Evidence for the dual-mode model and a modified opponent process theory. J. Sport Exerc. Psychol. 2010, 32, 711–730. [Google Scholar] [CrossRef]
- Lion, L.S. Psychological effects of jogging: A preliminary study. Percept. Mot. Skills 1978, 47 Pt 2, 1215–1218. [Google Scholar] [CrossRef]
- Blue, F.R. Aerobic running as a treatment for moderate depression. Percept. Mot. Skills 1979, 48, 228. [Google Scholar] [CrossRef] [PubMed]
- Young, R.J. The effect of regular exercise on cognitive functioning and personality. Br. J. Sports Med. 1979, 13, 110–117. [Google Scholar] [CrossRef]
- Blumenthal, J.A.; Williams, R.S.; Needels, T.L.; Wallace, A.G. Psychological changes accompany aerobic exercise in healthy middle-aged adults. Psychosom. Med. 1982, 44, 529–536. [Google Scholar] [CrossRef] [PubMed]
- Trujillo, C.M. The effect of weight training and running exercise intervention programs on the self-esteem of college women. Int. J. Sport Psychol. 1983, 14, 162–173. [Google Scholar]
- Tuckman, B.W.; Hinkle, J.S. An experimental study of the physical and psychological effects of aerobic exercise on schoolchildren. Health Psychol. Off. J. Div. Health Psychol. Am. Psychol. Assoc. 1986, 5, 197–207. [Google Scholar] [CrossRef]
- Doyne, E.J.; Ossip-Klein, D.J.; Bowman, E.D.; Osborn, K.M.; McDougall-Wilson, I.B.; Neimeyer, R.A. Running versus weight lifting in the treatment of depression. J. Consult. Clin. Psychol. 1987, 55, 748–754. [Google Scholar] [CrossRef] [PubMed]
- Fremont, J.; Craighead, L.W. Aerobic exercise and cognitive therapy in the treatment of dysphoric moods. Cogn. Ther. Res. 1987, 11, 241–251. [Google Scholar] [CrossRef]
- Hannaford, C.P.; Harrell, E.H.; Cox, K. Psychophysiological Effects of a Running Program on Depression and Anxiety in a Psychiatric Population. Psychol. Rec. 1988, 38, 37–48. [Google Scholar] [CrossRef]
- Long, B.C.; Haney, C.J. Long-Term Follow-up of Stressed Working Women: A Comparison of Aerobic Exercise and Progressive Relaxation. J. Sport Exerc. Psychol. 1988, 10, 461–470. [Google Scholar] [CrossRef]
- Simons, C.W.; Birkimer, J.C. An exploration of factors predicting the effects of aerobic conditioning on mood state. J. Psychosom. Res. 1988, 32, 63–75. [Google Scholar] [CrossRef]
- Moses, J.; Steptoe, A.; Mathews, A.; Edwards, S. The effects of exercise training on mental well-being in the normal population: A controlled trial. J. Psychosom. Res. 1989, 33, 47–61. [Google Scholar] [CrossRef]
- Ossip-Klein, D.J.; Doyne, E.J.; Bowman, E.D.; Osborn, K.M.; McDougall-Wilson, I.B.; Neimeyer, R.A. Effects of running or weight lifting on self-concept in clinically depressed women. J. Consult. Clin. Psychol. 1989, 57, 158–161. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.; Steinberg, H.; Sykes, E.A.; Salmon, P. Effects of temporary withdrawal from regular running. J. Psychosom. Res. 1990, 34, 493–500. [Google Scholar] [CrossRef]
- Friedman, E.; Berger, B.G. Influence of gender, masculinity, and femininity on the effectiveness of three stress reduction techniques: Jogging, relaxation response, and group interaction. J. Appl. Sport Psychol. 1991, 3, 61–86. [Google Scholar] [CrossRef]
- Williams, T.J.; Krahenbuhl, G.S.; Morgan, D.W. Mood state and running economy in moderately trained male runners. Med. Sci. Sports Exerc. 1991, 23, 727–731. [Google Scholar] [CrossRef]
- Kerr, J.H.; Vlaswinkel, E.H. Self-reported mood and running under natural conditions. Work Stress 1993, 7, 161–177. [Google Scholar] [CrossRef]
- Long, B.C. Aerobic conditioning (jogging) and stress inoculation interventions: An exploratory study of coping. Int. J. Sport Psychol. 1993, 24, 94–109. [Google Scholar]
- Berger, B.G.; Friedman, E. Comparison of Jogging, the Relaxation Response, and Group Interaction for Stress Reduction. J. Sport Exerc. Psychol. 1988, 10, 431–447. [Google Scholar] [CrossRef]
- Berger, B.G.; Owen, D.R. Relation of low and moderate intensity exercise with acute mood change in college joggers. Percept. Mot. Skills 1998, 87, 611–621. [Google Scholar] [CrossRef]
- Szabo, A.; Frenkl, R.; Janek, G.; Kálmán, L.; Lászay, D. Runners’ anxiety and mood on running and non-running days: An in situ daily monitoring study. Psychol. Health Med. 1998, 3, 193–199. [Google Scholar] [CrossRef]
- Broman-Fulks, J.J.; Berman, M.E.; Rabian, B.A.; Webster, M.J. Effects of aerobic exercise on anxiety sensitivity. Behav. Res. Ther. 2004, 42, 125–136. [Google Scholar] [CrossRef]
- Haffmans, P.M.J.; Kleinsman, A.C.M.; van Weelden, C.; Huijbrechts, I.P.A.M.; Hoencamp, E. Comparing running therapy with physiotraining therapy in the treatment of mood disorders. Acta Neuropsychiatr. 2006, 18, 173–176. [Google Scholar] [CrossRef] [PubMed]
- Thornton, E.; Cronholm, P.; McCray, L.; Webner, D. Does Marathon Training Adversely Affect Baseline Anxiety Levels? AMAA J. 2008, 21, 5–9. [Google Scholar]
- Scholz, U.; Nagy, G.; Schüz, B.; Ziegelmann, J.P. The role of motivational and volitional factors for self-regulated running training: Associations on the between- and within- person level. Br. J. Soc. Psychol. 2008, 47 Pt 3, 421–439. [Google Scholar] [CrossRef]
- Kalak, N.; Gerber, M.; Kirov, R.; Mikoteit, T.; Yordanova, J.; Pühse, U. Daily morning running for 3 weeks improved sleep and psychological functioning in healthy adolescents compared with controls. J. Adolesc. Health Off. Publ. Soc. Adolesc. Med. 2012, 51, 615–622. [Google Scholar] [CrossRef]
- Inoue, Y.; Funk, D.; Jordan, J.S. The role of running involvement in creating self-sufficiency for homeless individuals through a community-based running program. J. Sport Manag. 2013, 27, 439–452. [Google Scholar] [CrossRef]
- Doose, M.; Ziegenbein, M.; Hoos, O.; Reim, D.; Stengert, W.; Hoffer, N.; Vogel, C.; Ziert, Y.; Sieberer, M. Self-selected intensity exercise in the treatment of major depression: A pragmatic RCT. Int. J. Psychiatry Clin. Pract. 2015, 19, 266–275. [Google Scholar] [CrossRef]
- von Haaren, B.; Haertel, S.; Stumpp, J.; Hey, S.; Ebner-Priemer, U. Reduced emotional stress reactivity to a real-life academic examination stressor in students participating in a 20-week aerobic exercise training: A randomised controlled trial using Ambulatory Assessment. Psychol. Sport Exerc. 2015, 20, 67–75. [Google Scholar] [CrossRef]
- Kahan, D.; McKenzie, T.L. Physical Activity and Psychological Correlates During an After-School Running Club. Am. J. Health Educ. 2018, 49, 113–123. [Google Scholar] [CrossRef]
- Keating, L.E.; Becker, S.; McCabe, K.; Whattam, J.; Garrick, L.; Sassi, R.B.; Frey, B.N.; McKinnon, M.C. Effects of a 12-week running programme in youth and adults with complex mood disorders. BMJ Open Sport Exerc. Med. 2018, 4, e000314. [Google Scholar] [CrossRef] [PubMed]
- Nezlek, J.B.; Cypryańska, M.; Cypryański, P.; Chlebosz, K.; Jenczylik, K.; Sztachańska, J.; Zalewska, A.M. Within-Person Relationships Between Recreational Running and Psychological Well-Being. J. Sport Exerc. Psychol. 2018, 40, 146–152. [Google Scholar] [CrossRef] [PubMed]
- Kruisdijk, F.; Hopman-Rock, M.; Beekman, A.T.F.; Hendriksen, I. EFFORT-D: Results of a randomised controlled trial testing the EFFect of running therapy on depression. BMC Psychiatry 2019, 19, 170. [Google Scholar] [CrossRef]
- Kruisdijk, F.; Hendriksen, I.; Tak, E.; Beekman, A.-J.; Hopman-Rock, M. EFFORT-D study process evaluation: Challenges in conducting a trial into the effects of running therapy in patients with major depressive disorder. Ann. Gen. Psychiatry 2018, 17, 10. [Google Scholar] [CrossRef]
- Krogh, J.; Nordentoft, M.; Sterne, J.A.C.; Lawlor, D.A. The effect of exercise in clinically depressed adults: Systematic review and meta-analysis of randomized controlled trials. J. Clin. Psychiatry 2011, 72, 529–538. [Google Scholar] [CrossRef]
- Stanton, R.; Reaburn, P. Exercise and the treatment of depression: A review of the exercise program variables. J. Sci. Med. Sport 2014, 17, 177–182. [Google Scholar] [CrossRef]
- Lubans, D.; Richards, J.; Hillman, C.; Faulkner, G.; Beauchamp, M.; Nilsson, M.; Kelly, P.; Smith, J.; Raine, L.; Biddle, S. Physical Activity for Cognitive and Mental Health in Youth: A Systematic Review of Mechanisms. Pediatrics 2016, 138, e20161642. [Google Scholar] [CrossRef]
- Greist, J.H.; Klein, M.H.; Eischens, R.R.; Faris, J.; Gurman, A.S.; Morgan, W.P. Running as treatment for depression. Compr. Psychiatry 1979, 20, 41–54. [Google Scholar] [CrossRef]
- Vezina, M.L.; Ruegger, R.H. THE PSYCHOLOGY OF RUNNING: Implications for nursing and health. Nurs. Forum (Auckl.) 1980, 19, 108–121. [Google Scholar] [CrossRef] [PubMed]
- Hinkle, J.S. Aerobic running behaviour and psychotherapeutics: Implications for sports counseling and psychology. J. Sport Behav. 1992, 15, 263–277. [Google Scholar]
- Weinstein, W.S.; Meyers, A.W. Running as Treatment for Depression: Is It Worth It? J. Sport Exerc. Psychol. 1983, 5, 288–301. [Google Scholar] [CrossRef]
- Katz, J.L. Long-distance running, anorexia nervosa, and bulimia: A report of two cases. Compr. Psychiatry 1986, 27, 74–78. [Google Scholar] [CrossRef]
- Prussin, R.A.; Harvey, P.D. Depression, dietary restraint, and binge eating in female runners. Addict. Behav. 1991, 16, 295–301. [Google Scholar] [CrossRef]
- Yates, A.; Shisslak, C.M.; Allender, J.; Crago, M.; Leehey, K. Comparing obligatory to nonobligatory runners. Psychosomatics 1992, 33, 180–189. [Google Scholar] [CrossRef]
- Pierce, E.F.; Rohaly, K.A.; Fritchley, B. Sex differences on exercise dependence for men and women in a marathon road race. Percept. Mot. Skills 1997, 84 Pt 1, 991–994. [Google Scholar] [CrossRef]
- Yatham, L.N.; Kennedy, S.H.; Parikh, S.V.; Schaffer, A.; Bond, D.J.; Frey, B.N.; Sharma, V.; Goldstein, B.I.; Rej, S.; Beaulieu, S.; et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) 2018 guidelines for the management of patients with bipolar disorder. Bipolar Disord. 2018, 20, 97–170. [Google Scholar] [CrossRef]
- Scott, J.; Pope, M. Nonadherence with mood stabilizers: Prevalence and predictors. J. Clin. Psychiatry 2002, 63, 384–390. [Google Scholar] [CrossRef]
- Keller, M.B.; Lavori, P.W.; Mueller, T.I.; Endicott, J.; Coryell, W.; Hirschfeld, R.M.; Shea, T. Time to recovery, chronicity, and levels of psychopathology in major depression. A 5-year prospective follow-up of 431 subjects. Arch. Gen. Psychiatry 1992, 49, 809–816. [Google Scholar] [CrossRef]
- Kennedy, S.H.; Lam, R.W.; McIntyre, R.S.; Tourjman, S.V.; Bhat, V.; Blier, P.; Hasnain, M.; Jollant, F.; Levitt, A.J.; MacQueen, G.M.; et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) 2016 Clinical Guidelines for the Management of Adults with Major Depressive Disorder: Section 3. Pharmacological Treatments. Can. J. Psychiatry Rev. Can. Psychiatry 2016, 61, 540–560. [Google Scholar] [CrossRef]
- Thomas, J.; Thirlaway, K.; Bowes, N.; Meyers, R. Effects of combining physical activity with psychotherapy on mental health and well-being: A systematic review. J. Affect. Disord. 2020, 265, 475–485. [Google Scholar] [CrossRef]
- Schuch, F.B.; Vancampfort, D.; Rosenbaum, S.; Richards, J.; Ward, P.B.; Veronese, N.; Solmi, M.; Cadore, E.L.; Stubbs, B. Exercise for depression in older adults: A meta-analysis of randomized controlled trials adjusting for publication bias. Rev. Bras. Psiquiatr. 2016, 38, 247–254. [Google Scholar] [CrossRef] [PubMed]
- Children Fit for Life. The Daily Mile. Available online: https://thedailymile.co.uk (accessed on 18 September 2020).
| Outcome | Description |
|---|---|
| Depression | Depression is a mood disorder with prolonged periods of low mood and a lack of interest and/or pleasure in normal activities most of the time. This includes major depressive disorder [19]. |
| Anxiety | Anxiety is characterised by uncomfortable or upsetting thoughts and is usually accompanied by agitation, feelings of tension and activation of the autonomic nervous system. It is important to note the distinction between transient anxiety symptoms (state anxiety), persistent symptoms (trait anxiety) and anxiety disorders: a collection of disabling conditions characterised by excessive, chronic anxiety. Examples of anxiety disorders are specific phobias, social phobia, generalised anxiety disorder, panic disorder, obsessive–compulsive disorder and post-traumatic stress disorder [20]. |
| Self-efficacy | Self-efficacy is a situation-specific form of self-confidence. Self-efficacy beliefs influence how people think, feel, motivate themselves and act [21]. |
| Psychological stress | Psychological stress or distress can be defined as the unique discomforting, emotional state experienced by an individual in response to a specific stressor or demand that results in harm, either temporary or permanent, to that person [22]. |
| Eating pathology | Eating pathology or disorder can be described as persistent disturbance of eating behaviours or behaviours intended to control weight, which significantly impairs physical health or psychosocial functioning. This disturbance should not be secondary to any recognised general medical disorder, e.g., hypothalamic tumour. This definition includes anorexia nervosa and bulimia nervosa [23]. |
| Self-esteem | Self-esteem is the feelings of value and worth that a person has for oneself. It contributes to overall self-concept as a construct of mental health [24]. |
| Addiction | Addiction designates a process whereby a behaviour that can function both to produce pleasure and to provide escape from internal discomfort is employed in a pattern characterized by (1) recurrent failure to control the behaviour (powerlessness) and (2) continuation of the behaviour despite significant negative consequences (unmanageability) [25]. |
| Psychological well-being | Psychological well-being links with autonomy, environmental mastery, personal growth, positive relations with others, purpose in life and self-acceptance. This is often referred to as eudemonic well-being [26]. |
| Self-concept | Self-concept is the organisation of qualities that the individual attributes to themself, which in turn guides or influences the behaviour of that individual [27]. |
| Mood | Mood is a transient state of a set of feelings, usually involving more than one emotion. Seen as a conscious summative recognition of feelings that can vary in intensity and duration [28]. |
| Author | Year | Country | Design | Population | Mental Health Outcome (Measurement) | Study Aim | Main Findings |
|---|---|---|---|---|---|---|---|
| Wilson et al. [29] | (1980) | Canada | Cross-sectional | n = 30, all male; age range 20–45; 10 marathoners, 10 regular joggers and 10 non-exercisers | Mood (Profile of Mood States) | Comparing mood states of marathon runners, regular joggers and non-exercisers | Marathoners and joggers reported less depression (F(2,28) = 7.51, p < 0.003), anger (F = 10.11, p < 0.001) and confusion (F = 12.41, p < 0.001) and more vigour (F = 103.21, p < 0.001) than non-exercisers. Marathoners reported less fatigue (F = 10.26, p < 0.001) and tension (F = 7.51, p < 0.003) than non-exercisers. Marathoners and joggers did not significantly differ on reported fatigue and tension; however, marathoners had significantly less depression, anger and confusion but more vigour than joggers. |
| Joesting [30] | (1981) | USA | Controlled cross-sectional | n = 100 runners; 79 males, mean age 18.36; 21 females, mean age 16.53 | Depression (Depression Adjective Checklist) | Investigating the relationship between running and depression | Significantly (p < 0.01) decreased depression in males and female runners compared to Lubin’s data for nonpsychiatric patients: male and female runners mean depression scores were 4.59 and 4.33, respectively, while the normative nonpsychiatric sample means were 8.02 and 7.32, respectively. |
| Jorgenson et al. [31] | (1981) | USA | Cross-sectional | n = 454 regular runners; 390 males and 64 females; majority aged 30–39 | Emotional well-being (structured questionnaire consisting of 55 items designed by the author) | Investigating the relationship between emotional well-being and running | Of the runners, 92.3% (n = 419) indicated an increase in emotional well-being (p < 0.01) but no report on the scale of improvement. Age and emotional well-being were significantly correlated (gamma value = 0.42, p < 0.001), with the older runner having the greater perception of emotional well-being resulting from running. There was a significant inverse relationship between average hours per week running and emotional well-being (gamma value = −0.43, p < 0.001). |
| Valliant et al. [32] | (1981) | Canada | Cross-sectional | n = 68 male runners; 30 marathon runners, mean age 34.4; 38 recreational runners, mean age 20.6 | Self-sufficiency and personality profiles (a 1-h “Sixteen Personality Factor Questionnaire”) | Comparing self-sufficiency and personality profiles in marathon runners vs. recreational joggers | Marathon runners had a more self-sufficient personality compared to joggers who were less assertive and more conscientious and had controlled personality types: On average, marathoners more reserved (F = 17.07, df = 1,66, p < 0.001), intelligent (F = 12.69, df = 1,66, p < 0.001), tender-minded (F = 11.79, df = 1,66, p < 0.001), imaginative (F = 11.09, df = 1,66, p < 0.005) and self-sufficient (F = 19.84, df = 1,66, p < 0.001) than joggers. Conversely, joggers were more happy-go-lucky (F = 10.05, df = 1,66, p < 0.005), apprehensive (F = 10.51, df = 1,66, p < 0.005) and controlled (F = 7.09, df = 1,66, p < 0.01). |
| Francis et al. [33] | (1982) | USA | Cross-sectional | n = 44 male participants; mean age 32; non-running controls who ran 0 miles weekly (n = 16), 20 miles (n = 10), 30–40 miles (n = 8) and 50–60 miles (n = 10) | Anxiety, depression and hostility (State-Trait Anxiety Inventory and the Multiple Affect Adjective Check List) | Comparing anxiety, depression and hostility in various groups of runners vs. sedentary controls | Compared to sedentary controls, runners had lower anxiety (4.2 vs. 7.2, p < 0.01), depression (8.6 vs. 12.3, p < 0.01) and hostility (4.8 vs. 6.8, p < 0.01). |
| Hailey et al. [34] | (1982) | USA | Cross-sectional | n = 60 male runners; aged 13–60; Those who ran for less than 1 year (n = 12), those who ran for 1–4 years (n = 32) and those who ran for over 4 years (n = 16) | Negative addiction (Negative addiction scale) | Investigating the relationship between running and negative addiction | The more years that a male had been running, the greater the risk of developing negative addiction (F(2,58) = 3.48, p < 0.05). Runners with a running history of <1 year scored a mean of 3.84 (scale of 1–14), those running for 1–4 years scored 5.63 and those running for 4+ years scored 6.38. Addiction scores for runners of 4+ years was greater than the addiction score for runners of <1 year (t(59) = 2.72, p < 0.005). Likewise, the addiction score for runners of between 1–4 years was greater than the score for runners <1 year (t(59) = 2.52, p < 0.01). No statistically significant difference in addiction scores were found between the 1–4-year group and the 4+ year group. |
| Callen [35] | (1983) | USA | Cross-sectional | n = 424 non-professional runners who ran on average more than 28.8 miles per week; 303 males and 121 females; mean age 34 | Mental and emotional aspects (a questionnaire designed by the author) | Investigating mental and emotional aspects associated with long-distance running in non-professional runners, including depression, tension, mood, happiness, self-confidence and self-image | Ninety-six percent of subjects noticed mental/emotional benefits from running, but none reported the size of benefits. Benefits included relief of tension (86% of all respondents, n.s.), improved self-image (77%, n.s.), better mood (66%, p < 0.05), improved self-confidence (64%, n.s.), relieved depression (56%, p < 0.05) and improved happiness (58%, n.s.). However, 25% stated they had experienced emotional problems associated with running, with almost every instance being a problem of depression, anger or frustration associated with not being able to run due to injury, but no details of size or significance were reported. Sixty-nine percent of runners experienced an emotional “high” while running. |
| Galle et al. [36] | (1983) | USA | Controlled cross-sectional | n = 391 female subjects; aged 15 to 50; runners (n = 102), infertility patients (n = 103), fertile subjects (n = 139) and Clomid study patients whose only infertility abnormality was ovulation dysfunction (n = 47) | Anxiety and depression (Hopkins Symptom Checklist-90) | Comparing psychologic profiles including anxiety and depression in runners, infertility patients, fertile subjects and Clomid study patients whose only infertility abnormality was ovulation dysfunction | Emotional distress scores of runners were not significantly different from the fertile control subjects (F = 1.19, ns), but both groups of infertility patients showed greater distress on items in the depression subscale than the runners and fertile control subjects (F = 3.42, p < 0.025). The only significant difference between runners and fertile control subjects was that control subjects had higher hostility (p < 0.05). Regarding just runners, there was significant differences in depression between amenorrhoeic (n = 15) and regular cycling runners (n = 87), with amenorrhoeic runners scoring higher in the depression factor than regular ovulation cycle runners (F = 3.0, p < 0.10). |
| Lobstein et al. [37] | (1983) | USA | Pre-post controlled between subject design | n = 22 medically healthy men; 11 physically active men and 11 sedentary men; aged 40–60 | Depression (Minnesota Multiphasic Personality Inventory) | Assessing the impact of a treadmill run with increasing gradient on depression | Sedentary men were significantly more depressed than men who ran (mean = 61.36 vs. 50.73, respectively, p < 0.01), but both groups were within clinical limits for normal, mentally healthy, middle aged men. |
| Rudy et al. [38] | (1983) | USA | Cross-sectional | n = 319 female regular runners; aged between 16 and 60 | Anxiety and self-esteem (Rosenberg Self-esteem Scale and Zuckerman’s Anxiety Adjective Checklist) | Investigating how levels of anxiety and self-esteem related to intensity of jogging | Female runners jogging with great intensity had significantly less anxiety than lower intensities (x2 = 22.83; p < 0.001). Results indicate that intensity of jogging influences self-esteem but was not significant: 89% of women scored in the range of high self-esteem, and in the open-ended answers, 29% of responses stated that they feel better about themselves, 12% had increased self-confidence and 6% stated a sense of accomplishment. |
| Goldfarb et al. [39] | (1984) | USA | Cross-sectional | n = 200 distance runners; 136 males and 64 females | Anorexia nervosa traits (Goldfarb Fear of Fat scale and Activity Vector Analysis) | Investigating anorexia nervosa traits within distance runners | Runners had a mean score of 2.91 (on a 10-point scale), indicating a low–normal fear of fat, and only 29 (14.5%) participants reported a high fear-of-fat score (score between 6 and 10). Fear-of-fat scores did not correlate significantly with measures of running zealousness: miles run per week (r = −0.04), number of workouts per week (r = 0.09), number of road races (r = 0.05), marathons completed (r = −0.05) or degree of importance placed on running (r = −0.03). Runners who demonstrated the greatest zealousness demonstrated Activity Vector Analysis profiles that clustered around one particular profile (r = 0.64, p < 0.05) indicating assertive, obsessive, perfectionistic and anxious individuals. Results do not support a correlation between running and fear of fat; however, runners most closely resembling “obligatory runners” exhibited traits characteristic of anorexia nervosa patients. |
| -Guyot et al. [40] | (1984) | USA | Controlled cross-sectional | n = 126 participants; 64 runners (44 males and 20 females) vs. 62 non-runners (37 males and 25 females) | Death anxiety (Death Concern Scale) | Comparing death anxiety in runners vs. non-runners | Runners experienced more death thoughts (F(1,122) = 4.49, p < 0.05) but less death anxiety (F(1,122) = 6.35, p < 0.05) than non-runners. |
| Rape [41] | (1987) | USA | Controlled cross-sectional | n = 42 male participants; aged 18–25; 21 runners vs. 21 non-exercisers | Depression (Beck Depression Inventory) | Comparing depression scores in runners vs. non-exercisers | Runners were significantly less depressed (M = 4.38, SD = 3.88) than the non-exercisers (M = 9.55, SD = 5.40) (t40 = 3.55, p < 0.001). Overall results suggest that running reduces depression. |
| Weight et al. [42] | (1987) | South Africa | Controlled cross-sectional | n = 135 female participants consisting of marathon runners (n = 85) vs. cross country runners (n = 25) vs. non-running controls (n = 25); aged 18–56 | Eating attitudes and disorders (Eating Attitudes Test and the Eating Disorder Inventory) | Comparing eating attitudes and disorders in marathon runners vs. cross country runners vs. non-running controls. | No significant differences were found between groups on any of the Eating Attitudes Test scores (mean scores = 8.4, 14.3 and 11.8). Eating Disorder Inventory scores also did not follow a definite pattern (mean scores for marathoners, cross country runners and non-running controls were 24.8, 27.1 and 32.0, respectively), indicating that abnormal eating attitudes and the incidence of anorexia was no more common among competitive female runners than among the general population, with a low incidence of anorexia in the total group (2 out of 135 participants). |
| Chan et al. [43] | (1988) | USA | Cross-sectional | n = 60 runners who ran at least 3× per week for a minimum of a year; 28 males and 32 females; prevented runners n = 30 vs. continuing runners n = 30; aged 15–50. | Depression, self-esteem and mood (Zung depression Scale, Rosenberg Self-esteem Scale and Profile of Mood States) | Comparing depression, self-esteem and mood in prevented runners vs. continuing runners | Prevented runners reported significantly greater overall psychological distress (Wilks’s = 0.63, p < 0.01: X92 = 24.38, p < 0.01), depression (F(1,58) = 11.57, p < 0.01) and overall mood disturbance (F(1,58) = 11.03, p < 0.01) than continuing runners. Prevented runners reported significantly lower self-esteem (F(1,58) = 3.17, p < 0.05), less satisfaction with the way their bodies’ present looks (F(1,58) = 4.17, p < 0.05) and had greater desire to change something about the way their bodies look (F(1,58) = 4.54, p < 0.05) compared to continuing runners. |
| Frazier [44] | (1988) | USA | Post only, nonrandomised long-term observational study | n = 86 regular, distance runners who had all completed a marathon; 68 males with mean age of 33.7 and 18 females with a mean age of 32.2 | Mood (Profile of Mood States) | Investigating the relationship between running and mood in regular distance runners | Results suggest that regular, distance running improves mood in both males and females. Running subjects had lower mean scores on tension, anger, depression, fatigue and confusion and a higher mean of vigour compared to scores for test norms; however, statistical significance was not reported here. The only significant difference between males and females was on the confusion subscale: female mean = 7.8 vs. male = 5.5 (F(1,84) = 5.33, p < 0.05). |
| Lobstein, Ismail et al. [45] | (1989) | USA | Controlled cross-sectional | n = 36 male participants; aged 40–60; runners (n = 21) vs. sedentary controls (n = 15) | Anxiety and depression (Minnesota Multiphasic Personality Inventory and Eysenck Personality Inventory) | Comparing anxiety and depression levels in runners vs. sedentary controls | Overall, running reduced anxiety (mean = 48.95 vs. 61.48 respectively, p < 0.05, standardised canonical coefficient = −1.07) and depression (mean = 50.76 vs. 57.93, respectively, p < 0.05, standardised canonical coefficient = 0.00) compared to being sedentary. |
| Lobstein, Rasmussen et al. [46] | (1989) | USA | Controlled cross-sectional | n = 20 psychologically normal, medically healthy men; aged 40–60; physically active joggers (n = 10) vs. sedentary (n = 10) | Depression and stress (Eysenck Personality Inventory and Minnesota Multiphasic Personality Inventory) | Comparing depression and stress in sedentary men to physically active joggers | The findings suggest that regular jogging increases emotional stability (t = −2.84, p < 0.01) and decreases subjective depression with MMPI subscales of depression and Wiggins depression both being significantly lower in the joggers (t = 3.70, p < 0.01; t = 2.40, p < 0.05; respectively). |
| Nouri et al. [47] | (1989) | USA | Cross-sectional | n = 100 male participants; aged 18–62; non-exercisers (n = 28), drop-out joggers (n = 21), beginning joggers (n = 15), intermediate joggers (n = 16) and 20 advanced joggers (n = 20) | Anxiety and addiction/commitment (State-Trait Anxiety Inventory, Commitment to Running Scale, and The Buss–Dutkee Inventory measuring hostility and aggression) | Investigating the relationship between various levels of jogging vs. non-exercising on anxiety and addiction/commitment | Running reduced anxiety levels compared to physical inactivity (F(4,89) = 4.43, p < 0.01), with advanced joggers scoring significantly lower on trait anxiety than beginner and intermediate joggers (1.42 vs. 1.77 vs. 1.69, respectively, p < 0.01) and commitment to running significantly higher for the joggers than the non-exercisers (F(4,89) = 14.30, p < 0.01). |
| Chan et al. [48] | (1990) | Hong Kong | Cross-sectional | n = 44 male runners of track clubs who ran a mean of 57.2 km per week; mean age 27.8 | Depression, stress, tension and personality profiles (Chinese version of the Personality Research Form) | Investigating the relationship between running and depression, stress, tension and personality profiles | Running increased mood, happiness and outlook, while relieving anger, depression and aggression, but none reported the size of changes or significance; 36.4% of participants reported “improving mental health” as a reason to start running. Emotional benefits from running reported were more self-confident (59.1% of respondents), happier (56.8%), better mood (50.0%), relieved tension (45.5%), better self-image (36.4%), relieved depression (36.4%), more aggression (36.4%), improved outlook (34.1%), more content (31.8%) and better family relationship (15.9%). However, when participants stopped running, 38.6% experienced low mood and 25.0% experienced anxiousness. More experienced runners, compared to less experienced runners, were less aggressive or easily angered (t = 2.92, df = 42, p < 0.01), less guarded or defensive (t = 2.13, df = 42, p < 0.005) and more likely to present themselves favourably (t = 2.68, df = 35, p < 0.05). |
| Chapman et al. [49] | (1990) | USA | Cross-sectional | n = 47 runners; 32 males aged 34–57 and 15 females aged 35 to 59 | Running addiction, psychological characteristics and running (Running Addiction Scale, Commitment to Running Scale, Symptom Checklist (SCL-90-R) and Levenson’s Locus of Control Scale) | Investigating the relationship between running addiction, psychological characteristics and running | Results suggest a sex difference in the relationship between addiction and commitment, in that commitment to running can occur without addiction in females. Running Addiction Scale (RAS) scores correlated strongly for both sexes with self-rated addiction (p < 0.05) and moderately with discomfort (p < 0.05). However, the Commitment to Running Scale (CR) did not significantly correlate with self-rated addiction in females (0.246, ns) while RAS did (0.753, p < 0.05) (z = 2.00, p < 0.05). Running addiction was associated with a high frequency of running (p < 0.05) and longer duration of running (males = p < 0.05; females = ns). The CR score correlated significantly with run frequency for male (0.59, p < 0.05) but not female runners (0.14, ns), while CR and run duration did not correlate significantly for either sex (males = 0.16, females = 0.28, n.s.). Duration of running was associated with mood enhancement, implying that the benefits of running to mood may be obtained without addiction. Males were above the norm for obsessive–compulsive tendencies (SCL-90 score) and significantly higher than for females (p < 0.05), with running addiction associated with male-positive personality characteristics (p < 0.05) but not with mood enhancement. There were no significant correlations with personality traits for females. |
| Guyot [50] | (1991) | USA | Cross-sectional | n = 370 regular long-distance runners; 289 males, mean age 38; 81 females, mean age 35 | Addiction and death anxiety (Dickstein Death Concern Scale and author-created questionnaires for pain running, running motives, risk taking and medical symptoms) | Investigating the relationship between addiction and death anxiety between pain runners and non-pain runners | Of the 370 runners, 56% pushed themselves during running until they felt pain. Compared to non-pain runners, pain runners were more likely to be male, taller (F(1,366) = 11.45, p < 0.05), heavier (F(1,366) = 9.19, p < 0.05) and younger (F(1,366) = 5.75, p < 0.05). Overall, results suggest that runners classified as pain runners experienced significantly more death thoughts (F(1,364) = 5.04, p < 0.05) and death anxiety (F(1,364) = 8.86, p < 0.05) than non-pain runners. |
| Maresh et al. [51] | (1991) | USA | Cross-sectional | n = 29 male distance runners; mean age 40.1 | Psychological characteristics including anxiety, depression and stress (Myers–Briggs Type Indicator Form and Multidimensional Anger-Inventory) | Investigating psychological characteristics including anxiety, depression and stress in distance runners | Results suggest that long-term involvement in running is associated with low levels of self-reported anxiety (m = 2.5 on a 6-point scale), depression (M = 1.8) and stress (m = 2.5). Runners’ personality profiles differed from the normative sample, suggesting that running is associated with more introverted personalities compared to men in the general population. Compared to a normative sample of male control students, runners were less angry overall, less frequently angry, and angry across fewer situations. However, 82% of runners reported withdrawal symptoms when forced to be inactive, with a self-reported addiction average of 4.4 (“moderately” to “very”) on a 6-point scale. |
| Gleaves et al. [52] | (1992) | USA | Controlled cross-sectional | n = 60 female participants; runners (n = 20), bulimia patients (n = 20) and a non-exercising, non-dieting control group (n = 20) | Depression, body image and bulimia nervosa symptomology (Beck’s Depression Inventory, Body Image Assessment Procedure, subscales from the Eating Disorder Inventory, Automatic thoughts Questionnaire and dieting/weight loss questionnaire) | Comparing depression, body image disturbance and bulimia nervosa symptomology in runners, bulimia patients and a non-exercising, non-dieting control group | No differences were found between runners and controls throughout the study. Bulimics had significantly higher depression scores than runners and controls (20.65, 3.30 and 4.80 respectively, F = 56.95, p < 0.0001), but runners and controls did not differ from each other. The same pattern of results was found for the Autonomic Thoughts Questionnaire (F = 45.87, p < 0.0001) and Eating Disorder Inventory (F = 34.95, p < 0.0001), with bulimics scoring higher, but no significant difference was found between runners and controls: ATQ means = 85.40, 41.10 and 41.50, respectively, and EDI means = 12.80, 0.80 and 1.60, respectively. There were significant group effects for all three variables of body image (p < 0.01); again, bulimics differed from runners and controls. |
| Coen et al. [53] | (1993) | USA | Cross-sectional | n = 142 male marathon runners; mean age 44.07; obligatory runners (n = 65) vs. non-obligatory runners (n = 77) | Anxiety, anorexia and self-identity (Obligatory Exercise Questionnaire, State-Trait Personality Inventory and The Ego Identity Scale) | Investigating the relationship between obligatory running vs. non-obligatory running on anxiety, anorexia and self-identity | Compared to the non-obligatory runners, the obligatory group ran significantly more miles per week,0 spent more time running each week (t(140) = 13.19, p < 0.001) and had significantly higher levels of anxiety (18.85 vs. 6.45, respectively, (p < 0.01), suggesting that running represents a successful coping mechanism to reduce anxiety. There was no statistically significant difference in Ego Identity Scale score (p > 0.05), indicating that neither group showed a higher developed sense of identity. |
| Furst et al. [54] | (1993) | USA | Controlled cross-sectional | n = 188 participants, with n = 98 runners: 72 males and 26 females vs. n = 90 gym exercisers: 60 males and 30 females; majority aged 20–29 | Negative addiction (Negative Addiction Scale) | Comparing negative addiction in runners vs. gym exercisers | A significant association was found between years of participation in physical activity and addiction scores (F(5,182) = 6.39, p < 0.01) regardless of the type of activity, with no significant differences in addiction scores between runners and gym exercisers. |
| Masters et al. [55] | (1993) | USA | Cross-sectional | n = 712 participants in a marathon; 601 males and 111 females; aged 16–79 | Self-esteem and psychological coping of runners (Motivation of Marathoners Scales, Sport Orientation Questionnaire, Marlowe–Crowne Social Desirability Scale, Attentional Focusing Questionnaire, and 3 body satisfaction and composition questions) | Investigating self-esteem and psychological coping of marathon runners | Participation in marathon running and training was used as a way to problem solve with self-distraction for psychological coping (r(66) = 0.54, p < 0.001), improving self-esteem (r(66) = 0.31, p < 0.01) and life meaning (r(66) = 0.36, p < 0.01). Marathon runners reporting higher anxiety levels were more likely to endorse psychological motives for marathon running, indicating that their running helps them avoid or dampen negative emotional experiences: psychological coping (r(62) = 0.38, p < 0.01) and self-esteem (r(62) = 0.36, p < 0.01). Women more strongly endorsed weight concern as a reason for involvement in marathons (t(588) = −3.52, p < 0.001). Personal goal achievement and competition were both positively related to training miles per week (r(575) = 0.22, p < 0.001 and r(576) = 0.30, p < 0.001, respectively). |
| Pierce et al. [56] | (1993) | USA | Cross-sectional | n = 89 male runners; n = 33 non-competitive runners vs. n = 24 5-km runners vs. n = 32 marathoner runners | Exercise dependence (negative addiction scale) | Comparing exercise dependence in recreational (non-competitive) runners vs. 5-km runners vs. marathoner runners | Training mileage was significantly correlated with exercise dependence, with marathoners showing significantly higher (p < 0.05) mean exercise dependence scores (3.78) compared to 5K (2.9) and recreational runners (2.16). There was no significant difference in exercise dependence scores found between recreational and 5K runners. |
| Klock et al. [57] | (1995) | USA | Controlled cross-sectional | n = 22 females who were not currently pregnant or taking oral contraceptives; amenorrhoeic runners (n = 7, mean age 28.0), eumenorrheic runners (n = 9, mean age 32.1) and eumenorrheic sedentary women as controls (n = 6, mean age = 27.5) | Depression, anorexia nervosa, excessive exercise and eating disorder (The modified Body Image Questionnaire, the Beck Depression Inventory, the Symptom Checklist-90 and the Eating Disorders Inventory) | Comparing depression, anorexia nervosa, excessive exercise and eating disorders in amenorrhoeic runners, eumenorrheic runners and eumenorrheic sedentary women as controls | No significant differences were found between amenorrhoeic runners, eumenorrheic runners and eumenorrheic sedentary controls on any of the psychological measures; hence, these results do not suggest that there are psychological similarities between obligatory runners and anorexics. However, there was a subgroup of amenorrhoeic runners (3 out of 9) who scored in the clinically depressed range on the BDI, indicating that they were mild to moderately depressed, and who also had the highest scores in their group on the Eating Disorder Inventory measures. |
| Thornton et al. [58] | (1995) | UK | Cross-sectional | n = 40 long-standing, habitual male runners who ran on average 4 times per week with a weekly mileage of 42.5 miles; mean age 38 | Addiction (Rudy and Estok Running Addiction Scale, the Hailey and Bailey Running Addiction Scale, and the Personal Incentives for Exercise questionnaire) | Investigating a relationship between habitual running and addiction | A high level of commitment in runners was found, with 55% classified as moderately committed (scores 13–20) and 22% classified as highly “addicted” (scores +20), but no relationship between years of running and addiction scales was found. This contrasts the significant correlations between both the Estok RAS and frequency of running (rs = 0.38; p < 0.05) and the Bailey RAS and number of runs per week (rs = 0.55; p < 0.01). The correlation between the two addiction scales revealed a strong positive relationship (rs = 0.81; p < 0.001). The primary motivation for running was mastery (mean Personal Incentives for Exercise score of 4.2), followed by competition (3.93), weight regulation (3.9), health benefits (3.89), fitness (3.87) and social recognition (3.01). |
| Powers et al. [59] | (1998) | USA | Controlled cross-sectional | n = 57; habitual male runners (n = 20), habitual female runners (n = 20) and female anorexia nervosa patients (n = 17) | Psychological profiles (Minnesota Multiphasic Personality Inventory, Leyton Obsessional Inventory, Obligate Running Questionnaire, Becks Depression Inventory and three body image tests) | Comparing psychological profiles of habitual male runners, habitual female runners and female anorexia nervosa patients | Significant differences in body image between groups (F = 7.969, p < 0.001) were found, but no significant differences between female groups were found. Anorexics scored higher than either group of runners (p < 0.001) for MMPI subscales of depression, hysteria and psychopathic deviate, while none of the mean scores for either set of runners were considered clinically significant. Anorexics scored higher on the Becks Depression Inventory than both male and female runners (F = 68,645, p < 0.0001, mean scores = 23, 2.4 and 3.45, respectively), but again, there was no significant differences between the runners. While there were suggestive similarities between female runners and anorexics on body image, the overall results found few psychological similarities between anorexia patients and habitual runners, with evidence of significant psychopathology on all psychological measures in the anorexia group, while both groups of runners were consistently in the normal range. |
| Slay et al. [60] | (1998) | USA | Cross-sectional | n = 324 regular runners; 240 males and 84 females; 84 classified as obligatory runners: 63 males and 21 females; ages 15–71 | Eating pathology traits (Eat Attitudes Test, and Obligatory Running and Motivations for Running Questionnaire) | Comparing eating pathology traits between obligatory and non-obligatory runners | Obligatory runners, particularly females, are most at risk of eating pathophysiology, as obligatory runners scored significantly higher on the EAT test, with female obligatory runners having the highest mean EAT score (r = 0.40, p < 0.0002). At low levels of obligatory running, women and men scored similarly on the EAT test (F(1,164) = 2.78, p > 0.05); however, at higher levels of obligatory running, women demonstrated significantly higher EAT scores than men (F(1,164) = 29.50, p < 0.001). |
| Ryujin et al. [61] | (1999) | USA | Controlled cross-sectional | n = 55 female participants; collegiate distance runners (n = 20) vs. non-running undergraduate student controls (n = 35) | Eating disorder symptomology (Eating Disorders Inventory 2) | Comparing eating disorder symptomology in collegiate distance runners to non-running undergraduate student controls | Distance runners showed no enhanced symptomatology of eating disorders; instead, female distance runners exhibited fewer symptoms of eating disorders on all subscales of the Eating Disorder Inventory-2 except Perfectionism: drive for thinness (t(107) = 3.34, p < 0.005), bulimia (t(107) = 2.48, p < 0.05) and body dissatisfaction (t(107) = 4.23, p < 0.001). |
| Leedy [62] | (2000) | USA | Controlled cross-sectional | n = 276 runners with an average of 11.5 years of running experience; 239 men, mean age 37.9; 37 women, mean age 40.5 | Depression and anxiety (Diagnostic and Statistical Manual-IV, and an author-adapted scale based on the Running Addiction Scale) | Comparing depression and anxiety in runners to non-runners | Of the non-runners and runners, 16.2% and 4.6%, respectively, had been diagnosed with an anxiety disorder or prescribed an anxiolytic medication. These participants had significantly higher anxiety trait scores than those without a diagnosis: F(1,274) = 18.87, p < 0.0001; 27% of non-runners and 11.8% of runners reported a diagnosis of depression or were prescribed an antidepressant. These participants had significantly higher measures of depression traits: F(1,274) = 22.46, p < 0.0001. Women’s Stress Relief scores were significantly higher than men’s (F(1,229) = 20.51, p < 0.001). Stress relief scores also varied across race length (F(2,229) = 6.47, p < 0.005), indicating that runners entered in the 5–10K runs had lower scores than those running the half/full marathon. Results indicate that highly committed runners (n = 31) had significantly lower anxiety (F(2,113) = 5.73, p < 0.01) and depression scores (F(2,113) = 8.00, p < 0.001) than recreational runners (n = 46) and non-runners (n = 39). |
| Edwards et al. [63] | (2005) | South Africa | Cross-sectional | n = 277 participants; 94 males and 183 females; mean age 25.2; hockey players (n = 60), runners (n = 40) and health club gym members (n = 69) vs. a control group of non-exercisers (n = 108) | Psychological well-being and physical self-perception (Ryff’s Short Standardized 18-item scale of Objective Psychological Well-being, Fox’s Physical Self-Perception Profile (PSPP) and the Physical Self-Perception Profile) | Comparing psychological well-being and physical self-perception in hockey players, runners and health club gym members vs. a control group of non-exercisers. | All three forms of physical activity were associated with significantly higher (p < 0.01) scores on 11 out of the 15 dimensions of psychological well-being and physical self-perception scales compared to the control group: autonomy (F = 11.3), personal growth (F = 35.4), environmental mastery (F = 9.6), purpose in life (F = 149.2), positive relations with others (F = 81.6), self-acceptance (F = 50.4), sport competence (F = 41.3), conditioning (F = 28.1), sport importance (F = 11.7), conditioning importance (F = 28.1) and body importance (F = 31.0). |
| Schnohr et al. [64] | (2005) | Denmark | Observational cohort study | n = 12,028 participants; 5479 males and 6549 females; aged 20–79 | Stress (An author-created questionnaire) | Comparing stress levels between jogging and various levels of physical (in)activity in leisure time | Those who were vigorously physically active (joggers) had the lowest level of stress compared to those with low activity levels (males, 3.1% vs. 12.8%, respectively; female, 3.3% vs. 19.3%, respectively). With increasing physical activity in leisure time, there was a decrease in level of stress between sedentary persons and joggers (Odds Ratio (OR) = 0.30) and a decrease in life dissatisfaction between sedentary persons and joggers (OR = 0.30). The highest levels of stress and dissatisfaction was seen in sedentary persons who remained inactive at follow-up, while the group that changed from sedentary to active had an adjusted OR < 0.50. |
| Strachan et al. [65] | (2005) | Canada | Prospective longitudinal study | n = 67 regular runners; 32 were male and 35 were female; mean age of 40.6 | Self-efficacy and self-identity (author-created measures of task self-efficacy and self-regulatory efficacy, and a 10-item, validated athletic identity measurement scale) | Investigating the relationship between running and self-efficacy and self-identity | Significant comparisons were made between extreme self-identity groups on social cognitive and behavioural variables (F(5,37) = 4.72, p < 0.002), with those higher in self-identity scoring higher on task self-efficacy (p < 0.001), scheduling self-efficacy (p < 0.03), running more frequently (p < 0.001) and running for longer durations (p < 0.005) than those who scored lowest on self-identity. Both scheduling self-efficacy (R2 change = 0.16, p < 0.001) and barriers to self-efficacy (R2 change = 0.22, p < 0.001) were correlated with self-identity to prospectively predict running frequency (F(2,64) = 9.98, p < 0.001; F(2,63) = 12.89, p < 0.001, respectively). Both task self-efficacy (R2 change = 0.06, p < 0.05) and self-identity (R2 change = 0.06, p < 0.04) were significant predictors of maintenance duration. |
| Galper et al. [66] | (2006) | USA | Retrospective cross-sectional | n = 6728 participants; 5451 males with a mean age of 49.5 and 1277 females with a mean age of 48.1; inactive (n = 1454 men and n = 422 women), insufficiently active (n = 1892 men and n = 443 women), sufficiently active (n = 1396 men and n = 283 women) and highly active (n = 709 men and n = 129 women) | Depression and emotional well-being (Center for Epidemiological Studies Scale for Depression and the General Well-Being Schedule) | Assessing retrospectively if the level of walking/running impacted depression and emotional well-being | Significant inverse association between increased physical activity and reduced depression scores for both men (F(6, 5306) = 20.93, p < 0.0001) and women (F(6, 1247) = 11.80, p < 0.0001) and a positive association between increased physical activity and increased well-being scores in men (F(6, 5306) = 78.65, p < 0.0001) and women (F(6, 1247) = 24.82, p < 0.0001) were found. These effects peaked at 11–19 miles per week (the sufficiently active category). |
| Luszcynska et al. [67] | (2007) | UK | Longitudinal prospective cohort study | n = 139 runners; 111 males and 29 females; mean age of 29.5; strong (n = 72) and weak (n = 66) maintenance self-efficacy, strong (n = 72) and weak (n = 61) recovery self-efficacy, and strong (n = 87) and weak (n = 45) intentions | Self-efficacy and running behaviour (an author-created questionnaire) | Investigating the relationship between self-efficacy and running behaviour with data collected twice with a time gap of 2 years | Participants decreased the frequency of running sessions after 2 years, regardless of baseline intensions or self-efficacy; however, those with stronger recovery in self-efficacy jogged more than those with weaker recovery in self efficacy 2 years later. All participants reduced the number of jogging or running sessions over 2 years (F(1,131) = 43.43, p < 0.001); however, those with strong baseline recovery self-efficacy ran/jogged more often at 2 years than those who had weak recovery self-efficacy at baseline (F(1,131) = 6.12, p < 0.05). Participants reduced the number of running or jogging sessions over the 2 years, regardless of strong or weak intentions at baseline (F(1,130) = 34.55, p < 0.001) or of strong or weak baseline maintenance of self-efficacy (F(1,130) = 42.12, p < 0.001). No effects of maintenance self-efficacy were found. Recovery self-efficacy at T1 predicted recovery self-efficacy (p < 0.05), maintenance self-efficacy (p < 0.05), and jogging or running behaviour (p < 0.05) assessed 2 years later. Overall, social-cognitive variables predicted behaviour, whereas behaviour did not predict social-cognitive variables. |
| Smith et al. [68]. | (2010) | UK | Cross-sectional | n = 93 non-competitive, regular runners; 47 males and 46 females | Exercise dependence, running addiction and social physique anxiety (Exercise Dependence Scale, Running Addiction Scale and Social Physique Anxiety Scale) | Comparing exercise dependence, running addiction and social physique anxiety in male vs. female runners | While a significant proportion of runners displayed symptoms of exercise dependence, results did not find that exercise dependence was linked to social physique anxiety (F(3.179) = 1.21, p > 0.05) or that there was a difference between men and women (p > 0.05 in all cases). There was no significant difference between males and females for running addiction scale (22.64 and 20.91, respectively), social physique anxiety scale (22.30 and 22.61, respectively) or total exercise dependence scale scores (72.56 and 66.86, respectively). |
| Gapin et al. [69] | (2011) | USA | Cross-sectional | n = 179 regular runners; 88 males and 91 females; 91 obligatory and 88 non-obligatory runners | Disordered eating (Eating Disorder Inventory, Athletic Identity Measurement Scale and Obligatory Exercise Questionnaire) | Comparing disordered eating in obligatory and non-obligatory runners. | Obligated running (exercising to maintain identification with the running role) may be associated with pathological eating and training practices, with obligatory runners scoring significantly higher on all of the Eating Disorder Inventory measures (F(1,166) = 9.75, p < 0.002),and the Athletic Identity Measure Scale (F(8,161) = 8.85, p < 0.001). Results also indicated that runners in the obligatory group demonstrated greater concern with dieting, preoccupation with weight and pursuit of thinness. |
| Wadas [70] | (2014) | USA | Cross-sectional | n = 68 male, high school cross country runners; mean age 15.9 | Disordered eating behaviours (questionnaire consisting of The Exercise Motivation Inventory 2, the Eating Attitudes Test 26 and the ATHLETE questionnaire) | Investigating any relationship between male runners with disordered eating behaviours and eating attitudes | Risk factors associated with eating disorders within high school male cross-country runners were found. Factors that had a significant relationship with disordered eating were weight management (r = 0.31, p = 0.011), drive for thinness and performance (r = 0.36, p < 0.05), and feelings about performance/performance perfectionism (r = 0.26, p < 0.05). No significant relationships were found between disordered eating behaviours and personal body feelings (r = 0.19, p = 0.109), feelings about eating (r = 0.18, p = 0.137), and feelings about being an athlete (r = 0.12, p = 0.345); 4.41% (n = 3) of participants scored 20 or higher on the EAT-26, indicating being at risk for disordered eating and displaying symptoms. An additional 13.2% (n = 9) met the cutoff score of 14 for disordered eating behaviours. |
| Samson et al. [71] | (2015) | USA | Cross-sectional | n = 308 marathon runners; 177 males and 191 females; mean age 41 | Self-esteem and psychological coping (Motivation for Marathons Scale, The Perceived control questionnaire and Sport Mental Toughness Questionnaire) | Investigating the relationship between self-esteem and psychological coping with marathon running | Self-esteem was positively associated with perceived control (r = 0.40) (x27 = 47.08, p < 0.001, CFI = 0.85 and RMSEA = 0.14) but negatively associated with mental toughness. There was also a positive relationship between perceived control and psychological coping (r = 0.42) (x28 = 45.65, p < 0.001, CFI = 0.85 and RMSEA = 0.12). Results of the Motivations of Marathoners Scales suggested than females were more likely to run to improve psychological coping (4.8 and 4.42, respectively) and self-esteem (5.22 and 4.62, respectively) than men. |
| Lucidi et al. [72] | (2016) | Italy | Cross-sectional prospective field study | n = 669 runners training for a marathon; 569 males and 100 females; mean age 42.07 | Stress (Perceived Stress Scale, the Passion Scale and The Italian version of the Locomotion and Assessment Scales) | Investigating the relationship between running and stress in runners training for a marathon | Results suggest that running does not directly impact stress (β = −0.01; p = 0.75); however, running increases harmonious passion (β = 0.37; p < 0.001), which in turn reduced athletes’ experience of stress. The indirect effect of running on anticipatory stress perception through harmonious passion was statistically significant (αβ = −0.10; 95% confidence interval: from −0.15 to −0.05). Similarly, the indirect effect of assessment on stress through obsessive passion was statistically significant (αβ = 0.12; 95% confidence interval: from 0.07 to 0.17). Results also indicated a significant direct effect of assessment on the athletes’ experience of stress (β = 0.22; p < 0.001). |
| Batmyagmar et al. [73] | (2019) | Austria | Prospective longitudinal study | n = 99 participants; n = 50 elderly marathon runners, mean age of 66, with 46 men and 4 women vs. n = 49 non-exercising controls, mean age of 66, with 44 men and 5 women | Self-reported health and well-being and quality of life (Short Form Health Survey-36) | Comparing self-reported health and well-being, and quality of life over 4 years in elderly marathon runners to non-exercising controls | Findings suggested that extensive high-intensity endurance exercise is linked with improved subjective health and well-being in elderly persons, with athletes evaluating their health as better than non-athletes in the following categories: general health perception (F = 14.21, p < 0.001), vitality (F = 13.37, p < 0.001), social functioning (F = 11.30, p < 0.001), emotional role functioning (F = 1.42, p < 0.002) and mental health (F = 6.07, p < 0.0016). |
| Cleland et al. [74] | (2019) | Australia | Cross-sectional | 372 participants of “Parkrun” events; mean age 43.8 | Enjoyment, self-efficacy and factors of participation in Parkrun event (author-created questionnaires). | Investigating enjoyment, self-efficacy and factors of participation in Parkrun event participants | Overall results suggested that perceived social benefits (B coefficient = 0.43) and self-efficacy for Parkrun (B coefficient = 0.18) were positively associated with Parkrun participation. Perceived benefits of Parkrun including enjoyment and social factors (B = 0.70) were positively associated with participation, as was overall enjoyment (B = 0.30), self-efficacy for Parkrun (B = 0.46), social support for Parkrun from family (absolute: B = 0.05) and social support from friends (B = 0.04) related to Parkrun. |
| Lukacs et al. [75] | (2019) | Hungary | Cross-sectional | n = 257 amateur runners with at least 2 years of running experience; 131 males and 126 females; mean age 40.49 | Exercise addiction and psychological features (Exercise Dependence Scale; a Cantril ladder for Overall life satisfaction; SCOFF eating disorder questionnaire; the UCLA 3-item Loneliness Scale; Body Image Subscale from Body Investment scale; and the Depression, Anxiety and Stress Scale-21). | Investigating the prevalence of exercise addiction and psychological features in amateur runners, including perceived health, life satisfaction, loneliness, stress, anxiety, depression, body shape and eating disorders | Respondents (137) were characterized as nondependent symptomatic, 97 were nondependent asymptomatic and 23 were at risk of exercise addiction. Results found that five variables significantly predicted the risk of exercise addiction in runners: weekly time spent running, childhood physical activity, lower educational attainment, anxiety and loneliness (ranges of B = 0.47 to 2.06, 95% CI for odds ratio = 1.61 to 7.86, p < 0.001 to p = 0.023). |
| Author | Year | Country | Design | Population | Mental Health Outcome (Measurement) | Study Aim | Main Findings |
|---|---|---|---|---|---|---|---|
| Nowlis et al. [77] | (1979) | Canada | Pre-post non-controlled study | n = 18, experienced joggers; 5 females and 13 males; age range 17 to 55 | Mood and anxiety (Mood Adjective Checklist and State Trait Anxiety Inventory) | Impact of a 12.5-mile jog on mood and anxiety | Significant improvement in measures of pleasantness (2.00 to 2.67, p < 0.01); a significant decrease in trait anxiety (34.81 to 33.31, p < 0.10); a nonsignificant increase in activation; a reduction in state-anxiety; and a reduction of sadness, anxiety, depression and relaxation subscales |
| Wilson et al. [78] | (1981) | Canada | Pre-post controlled study | n = 42; 20 runners, 12 aerobics class exercisers vs. 10 people having lunch; 23 females and 19 males; age range 21 to 28 | Anxiety (State-Trait Anxiety Inventory) | Impact of a solo indoor track run on anxiety | Significant decrease in anxiety post-activity (F(1,39) = 15.63, p < 0.003) |
| Markoff et al. [79] | (1982) | Hawaii | Pre-post non-controlled | n = 15, all had run at least 1 marathon; 11 males and 4 females; aged 23–45 | Mood (Profile of Mood States) | Impact of a 1-h run on mood | Significant reduction in anxiety (t = 2.72, p < 0.01) and a nonsignificant reduction in depression (t = 1.80, n.s.) |
| Thaxton et al. [80] | (1982) | USA | Non-randomised controlled trial | n = 33, regular runners; 24 males and 9 females; mean age 36; 4 groups: outdoor running test (n = 6), pre-test but no running test (n = 9), no pre-test but running test (n = 11), and no pre-test and no running test (n = 7). | Mood (Profile of Mood States) | Impact of 30 min outdoor running on mood | Significant differences in the depression scores between the 30 min outdoor running group and abstaining groups (F(1,29) = 4.8, p < 0.05) but no significant differences between anxiety, vigour and fatigue scores |
| McGowan et al. [81] | (1991) | USA | Non-randomised controlled trial | n = 72, college students; 25 joggers vs. 11 karate vs. 26 weight lifters vs. 10 science lecture class members | Mood (Profile of Mood States) | Impact of 75 min of jogging on an outdoor track on mood | Significant decrease in total mood disturbance from pre- (35.68) to post- (24.16) test (t24 = 2.84, p < 0.009) following 75 min of jogging on a track |
| Goode et al. [82] | (1993) | USA | Pre-post non-controlled | n = 150, regular runners; 104 males, 36 females; mean age 31.7 | Mood (Profile of Mood States) | Impact of own training for running on mood | Significant alterations in all but one (vigor) of the POMS scales, with a significant reduction post-run in tension/anxiety (mean change of −3.1, p < 0.1), depression (mean change of −1.5, p < 0.1), confusion (mean change of −1.1, p < 0.1) and anger (mean change of −1.8, p < 0.1) and a significant increase in fatigue post-run (mean change of +1.8, p < 0.1). |
| Morris et al. [83] | (1994) | UK | Pre-post non-controlled | n = 165, members of a road runners club; 98 males and 67 females; mean age 34 | Mood (author-devised adjective checklist based on POMS) | Impact of a 3 mile “fun-run” on mood | Increase in positive mood (F(1,163) = 68.18, p < 0.001), decrease in negative mood (F(1.163) = 47.62, p < 0.001) and greater improvements in mood in women than in men that was not significant (p > 0.1). |
| Rudolph et al. [84] | (1996) | USA | Randomised non-controlled trial | n = 36, moderately active female university students; n = 12 for 10-, 15- and 20-min interventions; mean age 20.6 | Self-efficacy (Exercise-Efficacy Scale) | Impact of various timings of treadmill running on self-efficacy (10, 15 and 20 min) | Significant increase in mean scores of self-efficacy in all 3 groups, from pre to postexercise (F(1, 33) = 74.57, p < 0.001), and moderate effect sizes in the 15- (ES = 0.36) and 10- (ES = 0.49) minute conditions although the largest effect size (ES) occurred in the 20-min condition (ES = 0.68) |
| Cox et al. [85] | (2001) | USA | Randomised controlled trial | n = 24, physically active male university students; mean age of 28.3 | Psychological affect and well-being (Subjective Exercise Experiences Scale) | Impact of 30 min of treadmill jogging at either 50% or 75% predicted VO2 max on psychological affect and well-being | Significant improvement in psychological well-being following an acute bout of aerobic exercise (p = 0.037, η2p = 0.07) |
| O’Halloran et al. [86] | (2002) | Australia | Pre-post non-controlled | n = 50, regular runners; 25 males and 25 females; mean age 26.6 | Mood (Profile of Mood States and Beliefs Concerning Mood Improvements Associated with Running Scale) | Impact of a 60-min treadmill run on mood | Significant reductions in anxiety (composed-anxious POMS scale = 25.6 to 29.12, p < 0.05, i.e., more composed-less anxious) and depression (elated-depressed POMS scale = 24.56 to 27.10, p < 0.01, i.e., more elated-less depressed) |
| Szabo et al. [87] | (2003) | UK | Pre-post non-controlled time series quasi-experimental | n = 39, sports science university students; 22 males and 17 females; aged 20–23 | Anxiety, positive well-being and psychological distress (Spielberger State Anxiety Inventory and Exercise induced Feeling Inventory) | Impact of 20 min of track running on anxiety and feelings | Significant reduction in state anxiety (F(1.5, 58.3) = 5.32, p < 0.01) and a positive effect on psychological distress and positive well-being |
| O’Halloran et al. [88] | (2004) | Australia | Randomised controlled trial | n = 160 regular runners; 80 did run vs. 80 no running; 80 males and 80 females; aged 18–40 | Mood (Profile of Mood States and Beliefs Concerning Mood Improvements Associated with Running Scale). | Impact of a 60-min treadmill run on mood | Improvements in composure, energy, elation and mental clarity during the run; in the energetic-tired subscale, evident improvements at 25 min (F(1,156) = 10.09, p = 0.002); in the rest, non-evident mood improvements until 40 min of running; and more composure (less anxious) (F(1,156) = 9.47, p = 0.002) and more clear headedness (less confused) (F(1,156) = 5.57, p = 0.02) in runners |
| Robbins et al. [89] | (2004) | USA | Pre-post non-controlled | n = 168, inactive children and adolescents; 86 males and 82 females; mean age 12.6 | Self-esteem using the Walking Efficacy Scale | Impact of a 20-min treadmill run on self-efficacy in children and adolescents | Significant increase in children and adolescents’ self-efficacy postexercise (F(1, 158) = 84.31, p < 0.001) but significantly lower pre-activity self-efficacy in African American girls reported than the other three race-gender groups (F(3,164) = 5.55, p < 0.01) |
| Pretty et al. [90] | (2005) | UK | Randomised controlled trial | n = 100; 45 males and 55 females; mean age 24.6 | Mood and self-esteem (Profile of Mood States and Rosenberg Self-Esteem Questionnaire) | Impact of a 20-min treadmill run with rural vs. urban stimuli on mood and self-esteem | Significant increase in self-esteem (from 19.4 to 18.1 on the Rosenberg Self-Esteem Questionnaire, p < 0.001), with rural and urban pleasant stimuli producing a significantly greater positive effect on self-esteem than exercise alone, while both rural and urban unpleasant scenes reduced the positive effects of exercise on self-esteem |
| Hoffman et al. [91] | (2008) | USA | Pre-post pre-experimental study | n = 32; 16 regular exercisers and 16 non-exercisers; 8 males and 8 females in each group | Mood (Profile of Mood States) | Impact of a 30-min treadmill run on mood | Decreased total mood disturbance in a 30-min treadmill run in both regular exercisers (−16 points, 95% CI = 7–24) and non-exercisers (−9 points, 95% CI = 1–18) but almost double the effect in exercisers. |
| Kwan et al. [92] | (2010) | USA | Pre-post non-controlled | n = 129; 62 males and 67 females; mean age 22 | General affective response (Physical Activity Affect scale) | Impact of a 30-min treadmill run on general affective response | Positive effect of the run on general affective response during exercise (b = 0.52, SE = 0.09, p < 0.0001) and 15 min postexercise (b = 0.73, CI.95 = 0.56, 0.89, t(126) = 8.63, p < 0.0001). |
| Weinstein et al. [93] | (2010) | USA | Pre-post controlled study | n = 30; 15 males and 15 females; 2 with minor depressive disorder, 12 with major depressive disorder and 16 as controls; mean age 39.8 | Mood and depression (Becks depression Inventory scale and Profile of Mood States) | Impact of 25 min of increasing graded treadmill running on mood and depression | Not only improvements in depressed mood immediately following exercise (p = 0.02) of 25 min of increasing graded treadmill running but also increased depressed mood at 30 min postexercise (F(1,27) = 3.98; p = 0.05; ηp2 = 0.13) and significant relation between the severity of depression and increases in depressed mood (r = 0.60, p = 0.001) at 30 min postexercise |
| Anderson et al. [94] | (2011) | UK | Randomised controlled trial 2 × 2 mixed design | n = 40, from various sports clubs; aged 18–25 | Mood (“Incredibly Short Profile of Mood States”) | Impact of a light 10-min outdoor jog on mood | Significant mood enhancement even with a light 10=min jog on a grass playing field (F(1,38) = 24.18, p < 0.001, n2p = 0.39) compared with a 10-min cognitive task |
| Kane et al. [95] | (2013) | USA | Pre-post non-controlled | n = 34 school children; 16 males and 18 females; aged 11–14 | Self-efficacy (Self-efficacy questionnaire adapted for children) | Impact of the running PACER challenge (20 m sprints with increasing pace inside a gymnasium) on self-efficacy in children | Decrease in self-efficacy following participation in the run (from 2.7 to 2.3 following exercise, t = 4.6, p < 0.001, large effect size of d = 0.79) but positive correlation between PACER laps and pre- and post-measures of exercise self-efficacy |
| Szabo et al. [96] | (2013) | Hungary | Pre-post non-controlled | n = 50 recreational runners; 37 males and 13 females mean age 29.02 | States of affect using the Exercise Induced Feeling Inventory | Impact of a 5 km self-paced run along a public running path on states of affect | Significant positive changes in all 4 measures of states of affect following a 5-km self-paced run: revitalisation (F(1,48) = 145.93, p < 0.001, partial n2 = 0.75, ES = 2.0), positive engagement (F(1,48) = 97.11, p < 0.001, partial n2 = 0.67, ES = 1.6), tranquillity (F(1,48) = 85.02, p < 0.001, partial n2 = 0.64, ES = 1.5) and exhaustion (F(1,48) = 32.25, p < 0.001, partial n2 = 0.40, ES = 1.0) |
| McDowell et al. [97] | (2016) | Ireland | Randomised controlled trial | n = 53; 27 males and 26 females; mean age of 21.2 | Mood and anxiety (Profile and Mood States and State-Trait Anxiety Inventory) | Impact of a 30-min treadmill run on mood and anxiety | Significantly improved state anxiety (F1,92 = 12.52, p < 0.001), feelings of depression (F1,86 = 5.05, p < 0.027) and total mood disturbance (F = 36.91, p < 0.001) compared to 30 min of seated quiet rest |
| Rogerson et al. [98] | (2016) | UK | Pre-post non-controlled mixed between-within | n = 331 Parkrun attendees; 180 males and 151 females; mean age 40.8 | Psychological well-being (Questionnaire containing parts of the Profile of Mood States, Rosenberg Self-esteem scale and Perceived Stress Scale) | Impact of a 5-km park run on psychological well-being | Significant (p < 0.001) improvements post-run for self-esteem (7.7% improvement; F(1, 324) = 100.58, η2 = 0.24), stress (18.4% improvement; F(1, 315) = 50.78, η2 p = 0.139) and total mood disturbance (14.2% improvement; F(1, 278) = 22.15, η2p = 0.07) |
| Edwards et al. [99] | (2017) | USA | Randomised controlled trial | n = 27; 8 joggers vs. 9 walkers vs. 10 stretchers; aged 18–35 | Stress and anxiety (Exercise-Induced Feeling Inventory and Affective Circumplex Scale, and the Strait-Trait Anxiety Inventory) | Impact of a 15-min treadmill jog on stress and anxiety | Emotionally protective effect from a 15-min bout of treadmill jogging (n = 8) compared to an equivalent amount of time walking (n = 9) or stretching (n = 10) after exposure to a film clip intended to elicit a negative emotional response, with reduced anxiousness from baseline to post-jog (28.8 to 13.1, p = 0.06) on the State-Trait Anxiety Inventory, and increased anger score from baseline to post-film clip in the stretching group (1.2 to 26.0, p = 0.048) unlike the walking (p = 0.11) and jogging (11.3 to 9.4, p = 0.19) groups |
| Author | Year | Country | Design | Population | Mental health Outcome (Measurement) | Study Aim | Main Findings |
|---|---|---|---|---|---|---|---|
| Krotee [108] | (1980) | USA | Pre-post pre-experimental non-controlled | n = 78, children aged 7–12. | Anxiety (State-Trait Inventory for Children) | Impact of 50-metre group vs. solo run on anxiety | Children’s anxiety levels increased nonsignificantly following a run in either an individual (30.54 to 32.72, n.s.) or a group setting (30.67 to 31.83, n.s.). |
| Wildmann et al. [100] | (1986) | Germany | Pre-post non-controlled | n = 21, male long-distance runners; mean age of 29.8 | Feelings of pleasantness and changes of mood (Eigenschaftsworterliste scale adjective checklist) | Impact of 2 identical 10-km runs (1 week apart) on feelings of pleasantness and change of mood | Higher scores of good mood and feelings of pleasantness were found following the runs (mean increase of the two runs for all subjects was 2.79 from a total of 19 items, but the increase did not reach significance). |
| O’Connor et al. [101] | (1991) | USA | Pre-post non-controlled | n = 17, members of local running clubs; 10 males and 7 females; mean age 25 | Anxiety and body awareness (State-Trait Anxiety Inventory and Body Awareness Scale) | Impact of a 5-mile outdoor group vs. solo run on anxiety | Anxiety levels were reduced following both a group (mean baseline = 34.0 vs. pre-exercise = 42.5 vs. postexercise = 27.5, p < 0.05) and solo run (mean baseline = 34.0 vs. pre-exercise = 40.0 vs. postexercise = 30.0, p < 0.05). |
| Nabetani et al. [102] | (2001) | Japan | Pre-post non-controlled | n = 15, healthy, moderately active male graduate students | Mood (Mood Checklist Short-form 1) | Impact of a 10-min vs. a 15-min treadmill run on mood | Following the 10-min trial, anxiety significantly decreased (ES = 0.61, p < 0.01), whilst there was no significant difference in pleasantness (ES = 0.86) and relaxation (ES = 0.33). Following the 15-min trial, anxiety (ES = 0.51) and pleasantness (ES = 0.62) significantly decreased (p < 0.01), but relaxation (ES = 0.07) had no significant pre-post difference. |
| Bodin et al. [103] | (2003) | Sweden | Pre-post non-controlled within-subjects | n = 12, regular runners. 6 male and 6 female. Mean age of 39.7. | Emotional restoration ie. depression/anxiety (Exercise-Induced Feeling Inventory and the Negative Mood Scale). | Impact of 1 h park vs. urban run on depression and anxiety. | Runners preferred the park to the urban environment and perceived it as more psychologically restorative; there was no statistical difference in results for park vs. urban settings, with running in both settings causing a significant decline in anxiety/depression (F(1,10) = 16.2, p < 0.002, r = 0.78, effect size = 0.30). |
| Butryn et al. [104] | (2003) | USA | Pre-post non-controlled within-subjects | n = 30, non-elite female distance runners; mean age 31 | Mood, feeling states and cognition states (Profile of Mood States, Exercise-Induced Feeling Inventory and Thoughts During Running Scale) | Impact of a 4-mile park vs. urban run on mood | Total mood disturbance scores decreased by 8.97 (p < 0.001), with a similar effect following the urban run: total mood disturbance scores decreased by 9.13 (p < 0.001). |
| Kerr et al. [105] | (2006) | Japan | Pre-post non-controlled | n = 22, recreational runners; mean age 22.7 | Stress and emotions (Tension and Effort Stress Inventory) | Impact of indoor vs. outdoor 5-km run on stress and emotions | Significant pre-post effects irrespective of running condition were found, with an increase in relaxation (F(1, 21) = 5.60, p < 0.05) and excitement (F(1, 21) = 24.65, p < 0.001) and a decrease in anxiety (F(1, 21) = 9.90, p < 0.01). |
| Rose et al. [106] | (2012) | New Zealand | Pre-post controlled | n = 32, all females; 17 sedentary and 15 active; mean age 45 | Self-efficacy (Self-Efficacy for Exercise Scale) | Impact of self-paced vs. prescribed pace 30-min treadmill run on self-efficacy | Higher self-efficacy was observed before the prescribed paced run compared to the self-paced run (F1,28 = 5.81; p < 0.023; n2 = 0.17). |
| Reed et al. [107] | (2013) | UK | Pre-post non-controlled | n = 75, children aged 11 and 12 | Self-esteem (Rosenberg Self Esteem Scale) | Impact of rural vs. urban 1.5-mile run on self-esteem | Significant increase in self-esteem (F(1,74) = 12.2, p < 0.001) was found, but no significant difference between the urban or green exercise condition (F(1,74) = 0.13, p = 0.72) or any significant difference between boys and girls were found. |
| Author | Year | Country | Design | Population | Mental Health Outcome (Measurement) | Study Aim | Main Findings |
|---|---|---|---|---|---|---|---|
| Harte et al. [109] | (1995) | Australia | Pre-post non-randomised controlled-repeated measure design | n = 10, male amateur triathletes or marathon runners with a mean age of 27.1 | Mood (Profile of Mood States) | Impact of a 12-km outdoor run vs. indoor treadmill run with external stimuli vs. an indoor treadmill run with internal stimuli on mood | While the two indoor runs had a positive effect on mood, outdoor running had an even greater benefit to mood with subjects less anxious (F(3,35) = 14.12, p < 0.005), less depressed (F(3,35) = 4.16, p < 0.01), less hostile (F(3,35) = 13.13, p < 0.005), less fatigued (F(3,35) = 15.09, p < 0.005) and more invigorated F(3,35) = 13.01, p < 0.005). |
| Berger, Owen + Motl [110] | (1998) | USA | Pre-post non- controlled study | Study 1: n = 71 college students (32 males and 39 females) with a mean age of 21.39; study 2: n = 68 college students (28 males and 40 females) with a mean age of 22.22 | Mood (Profile of Mood States) | Impact of three 15-min runs of varying intensities (50, 65 or 80% age-adjusted HR max) on mood | Significant overall mood benefits postexercise (F(6.57) = 6.43, p < 0.0001) for all intensities but no significant differences between intensities were found. |
| Markowitz et al. [111] | (2010) | USA | Pre-post controlled trial | n = 28, college-aged students; 14 active vs. 14 sedentary controls; mean age 21 | Anxiety (State-Trait Anxiety Inventory) | Impact of three 20-min treadmill runs of varying intensities (5% below, 5% above and directly at lactate threshold) on anxiety | This was the only triple-bout study with a sedentary control condition. State anxiety improved postexercise at 5% below (effect size = −0.38, p < 0.001) and after exercise at the lactate threshold (effect size = −0.20, p < 0.001), but anxiety increased at 5% above the lactate threshold (effect size = +0.13, p = 0.0030). |
| Author | Year | Country | Design | Population | Mental Health Outcome (Measurement) | Study Aim | Main Findings |
|---|---|---|---|---|---|---|---|
| Lion [112] | (1978) | USA | Randomised controlled trial | n = 6, chronic psychiatric patients; 2 males and 4 females; 3 had the running intervention and 3 were controls; middle aged | Anxiety and body image (State-Trait Anxiety Inventory and Rorschach Inkblot Test for body-boundary image) | Impact of running a mile 3 times per week for 2 months on anxiety and body image in chronic psychiatric patients | Post-test anxiety was significantly reduced in the jogging group vs. control group (t = 3.2, df = 4, p < 0.05). Joggers showed an average drop of 9 points on the STAI (39.3 to 30.3) from pre- to post-test, while controls showed an average rise of 4 points (32.6 to 36.6). No statistical difference was found between groups for post-test body image scores. |
| Blue [113] | (1979) | USA | Pre-post non-controlled | n = 2 former inpatients of a psychiatric hospital; 1 male aged 37 and 1 female aged 32 | Depression (Zung depression scale) | Impact of 3 runs per week for 9 weeks on depression | Following running intervention, both patients’ depression scores reduced from “moderately depressed” to “mildly depressed” (decrease of 18 and 15 points on the Zung Depression Scale). |
| Young [114] | (1979) | USA | Pre-post non-controlled | n = 32 adults; 4 groups: young males (n = 8, mean age 30.13), middle-aged males (n = 8, mean age 53.0), young females (n = 8, mean age 28.25) and middle aged females (n = 8, mean age 50.25) | Anxiety and depression using the Multiple Affect Adjective Checklist | Impact of a 10-week walking/jogging programme consisting of 1 h 3× per week on anxiety and depression | Significant reductions in pre- to post-test anxiety (F(1,28) = 6.01, p < 0.05) were found. Results for anxiety and depression both showed significant age differences in favour of older subjects ((F(1,28) = 5.37, p < 0.05) and (F(1,28) = 5.21, p < 0.05), respectively). However, there was no significant improvement with subject depression scores. |
| Blumenthal et al. [115] | (1982) | USA | Non-randomised controlled cohort | n = 16 healthy adults; 5 males and 11 females; mean age 45.1 | Anxiety and mood (Profile of Mood States and the State-Trait Anxiety Inventory) | Impact of 3 times weekly walking-jogging programme for 10 weeks vs. 10 weeks of sedentary controls on anxiety and mood | The exercise group exhibited less tension (F(1,30) = 4.49, p < 0.04), depression (F(1,15) = 4.82, p < 0.04), fatigue (F(1,30) = 3.88, p < 0.05) and confusion (F(1,15) = 4.40, p < 0.05) but more vigour (F(1,15) = 3.28, p < 0.09) than sedentary controls. No change was observed for either group on the POMS anger subscale. After the 10-week programme, exercisers also exhibited less state anxiety (F(1,26) = 4.15, p < 0.05) and less trait anxiety (F(1,26) = 6.05, p < 0.02). |
| Trujillo [116] | (1983) | USA | Randomised controlled trial | n = 35 female college students; 13 weight trainers, 12 runners and 10 controls | Self-esteem (Tennessee Self-concept Scale and the Bem Sex Role Inventory) | Impact of a 16-week running programme vs. weight training vs. a control on self-esteem | Both the running and weight training groups showed a significant increase in self-esteem from pre- to post-programme (t(11) = 2.11, p < 0.05), while the control group showed a nonsignificant loss in self-esteem (t(9) = 0.55, p > 0.05). |
| Tuckman et al. [117] | (1986) | USA | Randomised non-controlled trial | n = 154 children; aged 9–11 | Psychological affects such as creativity, perceptual function, behaviour and self-concept (Alternate Uses Test, Bender–Gestalt Test, Devereaux Elementary School Behaviour Rating Scale and Piers–Harris Children’s Self-Concept Scale) | Impact of three 30-min runs per week on an outdoor running track for 12 weeks on psychological affects in children (creativity, perceptual function, behaviour and self-concept, compared to 12 weeks of the school’s regular physical education | Running significantly improved creativity of school children compared to regular physical education participants (F ratio = 17.00, p < 0.001) but had no significant effect on classroom behaviour, perceptual functioning or self-concept. |
| Doyne et al. [118] | (1987) | USA | Randomised controlled trial | n = 40 women; all with a diagnosis of minor or major depression; mean age of 28.52 | Depression (Beck’s Depression Inventory, Hamilton Rating Scale for Depression and Depression Adjective Checklists) | Impact of 3 runs per week on an indoor track for 8 weeks on depression in women diagnosed with depression, compared to 8 weeks of weight lifting vs. control | Running statistically and clinically significantly decreased depression scores (F(4,138) = 14.98, p < 0.01) relative to the wait-list control group, with improvements reasonably well maintained at 1 year follow-up. |
| Fremont et al. [119] | (1987) | USA | Randomised non-controlled trial | n = 49; 13 males and 36 females; aged 19–62 | Depression, anxiety and mood state (Beck’s Depression inventory, State-Trait Anxiety Inventory and The Profile of Mood States) | Impact of 3 runs per week for 10 weeks on depression, anxiety and mood vs. 10 weeks of counselling vs. 10 weeks of a combination of running and counselling | Depression, trait anxiety and state anxiety all decreased significantly ((F(4,184) = 50.3, p < 0.0001), (F(1, 46) = 27.1, p < 0.0001), (F(1,46) = 21.9, p < 0.0001), respectively), while mood improved significantly over the 10 weeks (F(18,378) = 4.5, p < 0.001). |
| Hannaford et al. [120] | (1988) | USA | Randomised controlled trial | n = 27 male psychiatric patients with major psychiatric disorders; age range 25–60; 9 runners, 9 in corrective therapy for 8 weeks and 9 waiting list controls | Depression and anxiety (Zung Self Rating Depression Scale and State Trait Anxiety Index) | Impact of three 30-min runs per week for 8 weeks on depression and anxiety in psychiatric patients with major psychiatric disorders | Significant reductions were observed in depression scores (F(2,23) = 3.61, p = 0.043) compared to the waiting list controls, and nonsignificant reductions were observed in anxiety scores (F(2,23) = 1.085, p = 0.354) compared to the waiting list control group. |
| Long et al. [121] | (1988) | Canada | Randomised non-controlled trial | n = 39 chronically stressed, sedentary working women; mean age 40; 18 joggers vs. 21 relaxation intervention | Stress, anxiety and self-efficacy (Trait Anxiety Inventory, Sherer et al.’s Inventory for Self-Efficacy and a modified version of the Ways of Coping Checklist) | Impact of an 8-week running programme consisting of a weekly group session plus twice weekly solo jogs on stress, anxiety and self-efficacy | Runners had significantly less anxiety and greater self-efficacy than baseline; 24% of subjects reached clinically significant improvements at the end of treatment, and 36% reached clinically significant improvements at 14-month follow-up. The jogging group exhibited higher self-efficacy, and the time effect for the pre to the post/follow-up average was significant for both self-efficacy and trait anxiety (F(2, 36) = 15.38, p < 0.001), while total coping scores did not change (F(2, 35) = 2.88, p < 0.07) from pre to post/follow-up. |
| Simons et al. [122] | (1988) | USA | Non-randomised controlled trial | n = 128; 53 experimental subjects (24 male, 30 female, mean age 44.9); 75 control subjects (28 male, 47 female, mean age of 42.0) | Mood (Profile of Mood States, Nowicki–Strickland Internal–External Control Scale for Adults and Marlowe–Crowne Social Desirability Scale) | Impact of two 30 min walk/runs per week for 8 weeks on mood, compared to a weekly 30-min fitness lecture for 8 weeks | Significant improvement in mood pre- to post-test intervention compared to non-treatment controls (F(1,126) = 4.46, p < 0.05) as well as significant improvement in pre- to follow-up mood change scores (F(1,98) = 7.63, p < 0.01) were observed. |
| Moses et al. [123] | (1989) | UK | Randomised controlled trial | n = 75 sedentary adult volunteers; mean age 38.8; four 10-week conditions: high-intensity aerobic walk-jog programme (n = 18); moderate intensity walk-jog programme (n = 19); attention-placebo including strength, mobility and flexibility exercises (n = 18); or waiting list control (n = 20). | Mood and mental well-being (Profile of Mood States and the Hospital Anxiety and Depression Scale) | Impact of varying intensity 10 week walk-jog programmes on mood and mental well-being | Significant reductions in tension/anxiety (F(3,71) = 2.94, p < 0.05) were reported only by subjects in the moderate exercise condition. Significant differences in the confusion subscale were found over time (F(1,71) = 3.70, p < 0.06), with greater decreases in the moderate exercise group than in the high exercise, attention-placebo or waiting list conditions. No significant effects were found on the perceived coping scales, but there was significant improvement on the physical well-being scale in the exercisers (F(3,71) = 3.82, p < 0.01) after 10 weeks, while the waiting list group ratings decreased. At follow-up, only subjects in the moderate exercise condition reported decreased ratings of depression/dejection (F(2,55) = 3.00, p < 0.06) and positive changes that approached significance for the perceived coping assets scale (F(2,55) = 2.56, p < 0.08), but this was not the case for the high exercise or attention-placebo conditions. |
| Ossip-Klein et al. [124] | (1989) | USA | Randomised controlled trial | n = 32 clinically depressed women; mean age 28.52 | Self-concept (Beck Self-Concept Test) | Impact of running on an indoor track 4 times per week for 8 weeks on self-concept in clinically depressed women compared to weight lifting 4 times weekly vs. a delayed treatment (assessment only) control | Self-concept significantly improved in the clinically depressed women compared to controls (F(3,99) = 7.62, p < 0.0001). Self-concept scores were also significantly higher in those in the running condition compared to the wait-list condition at post-treatment (F(2, 33) = 4.69, p < 0.05), with improvements also reasonably well-maintained over time. |
| Morris et al. [125] | (1990) | UK | Pre-post study with randomised comparison | n = 30 male regular runners; mean age 37; 20 participants stopped running for 2 weeks vs. 20 continued running as normal | Anxiety and depression (General Health Questionnaire and short forms of the Zung Anxiety and Zung Depression scales) | Impact of stopping running for 2 weeks on anxiety and depression | Somatic symptoms, anxiety/insomnia and social dysfunction, symptoms of depression (p < 0.05), were all significantly greater in deprived than in continuing runners, and Zung depression (F(1,37) = 22.64, p < 0.001) and anxiety (F(1,37) = 11.51, p < 0.01) scores were significantly higher after the two weeks. Significantly more deprived than non-deprived subjects exceeded the suggested cutoff score for a psychiatric case after both weeks of deprivation (x2 = 5.38 and 4.51, respectively, df = 1, p < 0.05), but there was no statistical difference between groups once the deprived group resumed running. |
| Friedman et al. [126] | (1991) | USA | Randomised controlled trial | n = 387 students; 177 males and 188 females; mean age 20; 84 joggers, 96 relaxation, 100 group interaction and 107 lecture-control | Stress and mood (Profile of Mood States and Bem Sex Role Inventory) | Impact of 12 weeks of jogging on stress and mood | High masculinity male and female joggers reported significantly more mood improvement than those with low masculinity (p < 0.004). All women joggers reported significant reductions in depression after jogging, but those with high psychological masculinity experienced significantly greater reductions than low masculinity joggers (p < 0.04). Femininity had a significant effect on combined POMS scores (F(6,297) = 2.79, p < 0.02), with higher psychological femininity associated with higher tension, depression and fatigue and with lower vigour and confusion scores compared to those low in femininity. There were significant pre-post session × technique interactions for high and low masculinity women (F(18,843.36) = 2.47, p < 0.0007; F(18,843.36) = 2.49, p < 0.0006, respectively). Short-term improvements in POMS scores depended upon masculinity for women joggers and participants in group interaction. |
| Williams et al. [127] | (1991) | USA | Pre-post non-controlled within subject design | n = 10 moderately trained male runners; mean age 25.6 | Mood (Profile of Mood States) | Impact of 4 weeks of treadmill running 5 times per week at set paces reflecting 50, 60 and 70% VO2 max on mood | Regarding within-subject data, an increase in mean VO2 was associated with a significant increase in total mood disturbance (r = 0.88, p < 0.01), while running at a pace with more economical values was associated with more positive mental health profiles. However, when considered as a group, there was no relationship between running efficiency in moderately trained male runners and total mood disturbance. |
| Kerr et al. [128] | (1993) | Holland | Pre-post non-controlled | n = 32 regular exercising university students (18 males and 14 females) aged 18–22 | Mood (Stress-Arousal Checklist and Telic State Measure) | Impact of a weekly 40-min fixed distance run (5 km for females, 6.6 km for males) through a wooded area for 7 weeks on mood | In both males and females, there were significant increases from pre- to post-running intervention in telic state measure felt arousal scores (F(1,16) = 52.37, p = 0.0001 and F(1,12) = 16.16, p = 0.002, respectively), stress-arousal checklist arousal scores (F(1,16) = 15.34, p = 0.001 and F(1,12) = 25.19, p = 0.0001, respectively) and telic state measure preferred arousal scores (F(1,16) = 4.49, p = 0.05 and F(1,12) = 11.82, p = 0.005, respectively). In contrast, telic state measure arousal discrepancy scores decreased significantly for males (F(1,16) = 6.74, p = 0.02) and females (F(1,12) = 11.86, p = 0.005) pre- to post-running. |
| Long [129] | (1993) | Canada | Randomised controlled trial | n = 35; 14 males and 21 females; mean age 35.6; 12 runners, 9 stress inoculation and 14 wait-list control | Anxiety and stress (Cornell Medical Symptom Checklist) | Impact of 3 runs per week for 10 weeks on anxiety and stress | Although the exercise group was more likely to report using exercise to cope with stress, there was no significant differences found between groups on stress or coping classifications. There was also no significant difference in scores of the Cornell Medical Symptom Checklist between the running group and the stress inoculation treatment groups (F < 1; M = 87.4 vs. M = 86.2, respectively). |
| Berger and Friedman [130] | (1998) | USA | Randomised controlled trial | n = 387 undergraduate college students; 117 males and 188 females; mean age 20.0; 84 joggers vs. 96 relaxation response vs. 100 in discussion groups vs. 107 in the control group | Stress and mood (Profile of Mood States) | Impact of three jogs per week for a minimum of 20 min over 12 weeks on stress and mood | Jogging was significantly more effective in reducing stress than the control activity (F(18,280) = 1.79 to 1.85, p < 0.03), and joggers reported larger and more numerous reductions in tension, depression and anger than the control group; however, changes in vigour, fatigue and confusion were sporadic. There were no long-term benefits observed. |
| Berger and Owen [131] | (1998) | USA | Pre-post with comparison | n = 91 college students; n = 67 in weekly walking/jogging (32 males and 35 females) vs. n = 24 in a weekly health science class (9 males and 15 females) | Mood and anxiety (Profile of Mood States and State-Trait Anxiety Inventory) | Impact of twice weekly walking/jogging for 14 weeks on mood and anxiety | No significant interaction between exercise intensity and pre-post mood benefits was observed. Joggers reported significant short-term mood benefits following running regardless of exercise intensities (F(6,56) = 4.87, p < 0.0005). Joggers reported significant pre-post exercise changes on all POMS subscales: tension (F = 15.67, p < 0.0002), depression (F = 15.64, p < 0.0002), anger (F = 12.77, p < 0.0007), vigour (F = 22.29, p < 0.00005), fatigue (F = 20.14, p < 0.00005) and confusion (F = 26.34, p < 0.00005). |
| Szabo et al. [132] | (1998) | UK | Pre-post non-controlled observational cohort study | n = 40 members of an amateur running club; 30 males, mean age 40.5, and 10 females, mean age 37 | Anxiety and mood, i.e., exhaustion, tranquillity, positive engagement and revitalization (Commitment to running scale, Exercise-induced Feeling Inventory and Spielberger State Anxiety Inventory) | Impact of running vs. non-running days on anxiety and mood over 21 consecutive days | Reported differences (effect sizes ranging from 0.07 to 0.56, all p < 0.05) all favour running days over non-running days, concluding that, on running days, runners experienced less anxiety (F(1,38) = 5.22, p < 0.03) and better subscales of mood: exhaustion (F(1,38) = 4.34, p < 0.04), tranquillity (F(1,38) = 5.56, p < 0.02), revitalisation (F(1,38) = 18.32, p < 0.001) and positive engagement (F(1,38) = 11.79, p < 0.001). |
| Broman-Fulks et al. [133] | (2004) | USA | Randomised non-controlled trial | n = 54 participants with elevated anxiety sensitivity scores; 13 males and 41 females; mean age 21.17; 29 high-intensity aerobic exercisers vs. 25 low-intensity aerobic exercisers | Anxiety sensitivity (Anxiety Sensitivity Index, State-trait Anxiety Inventory and Body Sensations Questionnaire) | Impact of six 20-min treadmill sessions of either high/low-intensity aerobic exercise across 2 weeks on anxiety sensitivity in participants with elevated anxiety sensitivity scores | Six 20-min treadmill sessions of both high-intensity and low-intensity running across 2 weeks reduced anxiety sensitivity (F(2,56) = 42.50, p < 0.001, n2 = 0.60; F(2, 48) = 13.72, p < 0.001, n2 = 0.36; respectively). State anxiety also decreased from pre-post high-intensity running (35.10 to 32.03); however, it increased following low-intensity running (42.72 to 42.32), but neither of these effects were significant. |
| Haffmans et al. [134] | (2006) | Holland | Randomised controlled trial | n = 60 psychiatric patients all suffering from a depressive disorder; 19 males and 41 females; mean age 39; 20 runners vs. 21 in physiotherapy training vs. 19 controls | Depression and self-efficacy (Hamilton Rating Scale for Depression, Becks Depression Inventory, Self-Efficacy Scale and Physical Self-Efficacy Scale) | Impact of running therapy for 3 days per week for 12 weeks on depression and self-efficacy in psychiatric patients all suffering from depression | While after 6 weeks of running, self-efficacy was significantly higher (p = 0.03), after the full 12 weeks of running, there was no significant difference in depression (26.7 to 25.5, n.s.) or self-efficacy (46.6 to 49.1, n.s.) scores from baseline. |
| Thornton et al. [135] | (2008) | USA | Repeated measures design | n = 50 runners over age 18 | Anxiety (Beck Anxiety Inventory) | The relationship between anxiety and marathon | Marathon training decreased Beck Anxiety Inventory scores (0.9) initially from baseline pre-training levels compared to 2 months prior to marathon day (0.7; 72% had no change from baseline, 22% were less anxious and 6% were more anxious). However, anxiety scores increased as race day approached: at 1 month prior to race day (1.4; 46% had no change from baseline, 19% were less anxious and 35% were more anxious than baseline) and 1 week prior to race (2.6; 22% had no change from baseline, 14% were less anxious and 64% were more anxious than baseline, respectively). |
| Scholz et al. [136] | (2008) | Switzerland | Pre-post non-controlled non-experimental longitudinal study | n = 30 untrained participants; 4 males and 26 females; mean age 41.2 | Self-efficacy (4-part author-created measurement) | Impact of a 1-year marathon training programme on self-efficacy | The trend between running and self-efficacy had substantial correlation but was not significant. No statically significant differences was observed in the baseline level, trend or fluctuation of self-efficacy between the participants who successfully completed the marathon and those who did not, but the baseline level of self-efficacy was positively associated with the baseline level in running (correlation analyses = 0.27; p < 0.05; 95% CI = 0.00; 0.53) and fluctuation in self-efficacy correlated positively with fluctuation in running (0.39; p < 0.05; 95% CI = 0.03; 0.74). As this was a non-experimental longitudinal study, no causal statements can be drawn. |
| Kalak et al. [137] | (2012) | Switzerland | Randomised controlled trial | n = 51 adolescents; 24 males and 27 females; mean age 18.3; 27 runners vs. 24 controls | Mood and stress (A-a daily mood log, a questionnaire assessing positive and negative comping strategies, and Perceived Stress Scale) | Impact of daily 30-min morning runs on weekdays for 3 weeks (i.e., 3 × 5 runs) on stress and mood | Perceived stress did not differ significantly between running and control groups over time (F(1,49) = 1.71, n2 = 0.034, n.s.), while mood in the morning increased significantly over time in the running group compared with controls (F(5,245) = 16.08, n2 = 0.247, p < 0.05). However, irrespective of group, mood in the evening improved, and there was no significant difference of mood in the evening between groups. |
| Inoue et al. [138] | (2013) | USA | Pre-post non-controlled | n = 148 homeless people; 134 males and 14 females; mean age 29.9 | Self-sufficiency (author-created scale) | Impact of 10 organised runs on self-sufficiency in homeless people | Running involvement had a significant positive correlation with perceived self-sufficiency (r = 0.30, p < 0.01). Results suggested that participants gained higher levels of perceived self-sufficiency as they became more involved with running during the program (F = 3.39, p < 0.01, Adjusted R2 = 0.08), and increases in running involvement were the sole significant predictor of the outcome (β = 0.29, t = 3.57, p < 0.01). |
| Samson et al. [76] | (2013) | USA | Pre-post non-controlled | n = 39 university students who all had running experience; 11 males and 28 females; mean age 20.5 | General affect and self-efficacy (Positive and Negative Affect Scale and author-created measurements for self-efficacy) | Impact of a 15-week marathon training program of 3 group training days per week and one run of 8–20 miles on the weekend on general affect and self-efficacy | Self-efficacy significantly increased over the training programme (F(12,444) = 5.81, p < 0.01), but there was a significant decrease of positive affect over time (F(12,444) = 8.35, p < 0.01) and no significant change was found for negative affect over the programme. |
| Doose et al. [139] | (2015) | Germany | Randomised controlled trial | n = 46 outpatients diagnosed with mild to severe depression; aged 18–65; 30 walker/runner vs. 16 controls | Depression (Hamilton Rating Scale and Beck Depression Inventory) | Impact of group walking/running 3 times per week for 8 weeks on depression | Depression clinically significantly decreased on the Hamilton Rating Scale (Cohen’s d = 1.8; mean change = 8.24; p = <0.0001), and while there were reductions, they were without clinical significance (Cohen’s d = 0.50; mean change = 4.66; p = 0.09) in the Becks Depression Inventory scores. |
| Von Haaren et al. [140] | (2015) | Germany | Randomised controlled trial, within subject design | n = 61 inactive male university students; mean age 21.4 | Stress and mood (a shorten mood scale based on the Multidimensional Mood Questionnaire and a one-item test for perceived control and stress) | Impact of a 20-week running training course on stress and mood during academic examinations, compared to waiting list controls | Significant emotional stress reactivity was observed in both groups during academic assessment episodes; participants in aerobic training showed lower emotional stress reactivity compared with the control participants after the 20-week training programme, with perceived stress of the aerobic group remaining similar during both exam periods (2.27 to 2.24), while it increased further in the control group (2.43 to 2.51). |
| Kahan et al. [141] | (2018) | USA | Pre-post with comparison | n = 11 children; 9 males and 2 females; aged 9 and 10 | Self-esteem and self-efficacy (50-item, author-created questionnaire) | Impact of 20 running sessions alternating between game vs. lap running on self-esteem and self-efficacy in children | Means for self-esteem and task-efficacy were 3.63 and 4.16, respectively, on a 5-point scale, while the mean for task-efficacy was 4.16 on a 5-point scale, and high inherent-interest participants (i.e., higher moderate–vigorous physical activity in the running laps condition) had statistically significant higher scores than low inherent-interest participants on recognition (p = 0.01), ego orientation (p = 0.03) and expectancy beliefs (p = 0.03) subscales. There were no direct comparisons of self-esteem and self-efficacy in game vs. lap running. |
| Keating et al. [142] | (2018) | Canada | Pre-post non-controlled | n = 46 participants with complex mood disorders; 11 males and 35 females; 29 youths (mean age 22.1) and 17 adults (mean age 45.2) | Stress, anxiety and depression (Cohen’s Perceived Stress Scale, Becks Depression Inventory, Becks Anxiety Inventory and Short Form Survey) | Impact of 12 weeks of twice weekly running in a group setting that offers social support supervised by clinical professionals on stress, anxiety and depression | Significant decreases in depression (F(11,201) = 4.5, p < 0.0001), anxiety (F(11,186) = 4.8, p < 0.0001) and stress (F(11,186) = 2.3, p = 0.01) from baseline was observed. Following intervention, mean depression scores decreased by 39% in adults from high to low levels and by 27% in youths from moderate to reduced moderate levels. Younger participant age, younger age at onset of illness and higher perceived levels of friendship with other running group members (ps ≤ 0.04) were associated with lower depression, anxiety and stress scores. Higher attendance was linked with decreasing depression and anxiety (ps ≤ 0.01) scores over time. |
| Nezlek et al. [143] | (2018) | Poland | Pre-post observational cohort study over 3 months with no control | n = 244 recreational runners; 127 males and 117 females; mean age 32.5 | Psychological well-being, self-esteem, self-efficacy and affect (Rosenberg Self-esteem Scale, Satisfaction with Life Scale, and a circumplex model that distinguishes the valence and arousal of affect) | Impact of 3 months of self-prescribed running on psychological well-being, self-esteem, self-efficacy and affect | Positive within-person relationships between how much people ran each week and self-reports of well-being were observed, with well-being significantly higher during weeks when individuals ran more often and further. Self-efficacy was related to distance run but not to frequency. For the km that people ran each week, significant moderation was found for weekly Satisfaction with Life Scale (γ11 = −0.0002, p = 0.013), self-esteem (γ11 = −0.0002, p = 0.015), positive activated affect (γ11 = −0.0003, p < 0.001), positive deactivated affect (γ11 = −0.0008, p < 0.01), negative activated affect (γ11 = 0.0002, p = 0.046) and negative deactivated affect (γ11 = 0.0003, p = 0.01). |
| Kruisdijk et al. [144] | (2019) | Holland | Randomised controlled trial | n = 48 participants with major depressive disorder; mean age 42.6; 25 runner-walkers vs. 23 controls | Depression (Hamilton Depression Scale) | Impact of 6 months of running-walking for one hour twice a week on depression in subjects with major depressive disorder | No significant difference or effect on depression in favour of the intervention group (Cohen’s d < 0.2, F = 0.13, p = 0.73) with only 9 participants (19%) completing the study was found, with low statistical power and lack of follow-up at six and 12 months. |
| Study Type | Number of Studies | Summary of Evidence |
|---|---|---|
| Cross-sectional | 47 studies | Consistent evidence was found for a positive association between mental health and habitual or long-term recreational running compared to non-runners. In contrast, there was evidence that high or extreme levels of running were associated with markers of running ill-health compared to levels of moderate running. |
| Acute: single/double/triple bout | 35 studies | Overall, these studies suggest that acute bouts of running can improve mental health and that the type of running can lead to differential effects. Evidence suggests that acute bouts of treadmill, track, outdoor and social running (2.5–20 km and 10–60 min) all result in improved mental health outcomes. There were few differences between high and low intensities. Studies consistently show that any running improves acute/short-term mood markers but that lack of inactive comparisons limits the strength of evidence. Little variation in the demographics of participants and small sample sizes limit generalizability and precision of findings. |
| Interventions (2 weeks or more) | 34 studies | Overall, running interventions of 2–20 weeks generally show improved markers of a range of mental health outcomes compared to non-running controls, including mental health outcomes in psychiatric and homeless populations. The risk of longer-term running interventions on adverse mental health outcomes remains unclear. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oswald, F.; Campbell, J.; Williamson, C.; Richards, J.; Kelly, P. A Scoping Review of the Relationship between Running and Mental Health. Int. J. Environ. Res. Public Health 2020, 17, 8059. https://doi.org/10.3390/ijerph17218059
Oswald F, Campbell J, Williamson C, Richards J, Kelly P. A Scoping Review of the Relationship between Running and Mental Health. International Journal of Environmental Research and Public Health. 2020; 17(21):8059. https://doi.org/10.3390/ijerph17218059
Chicago/Turabian StyleOswald, Freya, Jennifer Campbell, Chloë Williamson, Justin Richards, and Paul Kelly. 2020. "A Scoping Review of the Relationship between Running and Mental Health" International Journal of Environmental Research and Public Health 17, no. 21: 8059. https://doi.org/10.3390/ijerph17218059
APA StyleOswald, F., Campbell, J., Williamson, C., Richards, J., & Kelly, P. (2020). A Scoping Review of the Relationship between Running and Mental Health. International Journal of Environmental Research and Public Health, 17(21), 8059. https://doi.org/10.3390/ijerph17218059








