Diode versus CO2 Laser Therapy in the Treatment of High Labial Frenulum Attachment: A Pilot Randomized, Double-Blinded Clinical Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Blinded Methodology
2.2. Randomization
2.3. Dimension of Sample and Inclusion Criteria
- Wound healing was clinically evaluated considering the residual amount of fibrin after oral surgery treatment. Unfortunately, there are no evaluative scales about wound healing process, hence according to what is explained in the book (Oral Wound Healing), it has been estimated: score 1 (wound totally covered by fibrin); score 2 (wound partially covered by fibrin); score 3 (complete healing without fibrin) [26].
- Gingival Recession was clinically evaluated through the use of a periodontal probe (P.C.P 15). Only patients with recession class I were considered, and it has been estimated: score 1 (0 to 1 mm of recession) score 2 (2 mm of recession) score 3 (3 mm of recession) [23].
- Clinical attachment loss was clinically evaluated through the use of a periodontal probe (P.C.P 15). Furthermore, for clinical attachment, only patients with stage I and II were considered and it has been estimated: score 1 (0–1 mm of probing); score 2 (2–3 mm of probing); score 3 (4 mm of probing) [24].
- Pain was calculated thought the use of the Numerical Rating Scale (NRS) which evaluation interval is from number 0 to 10.
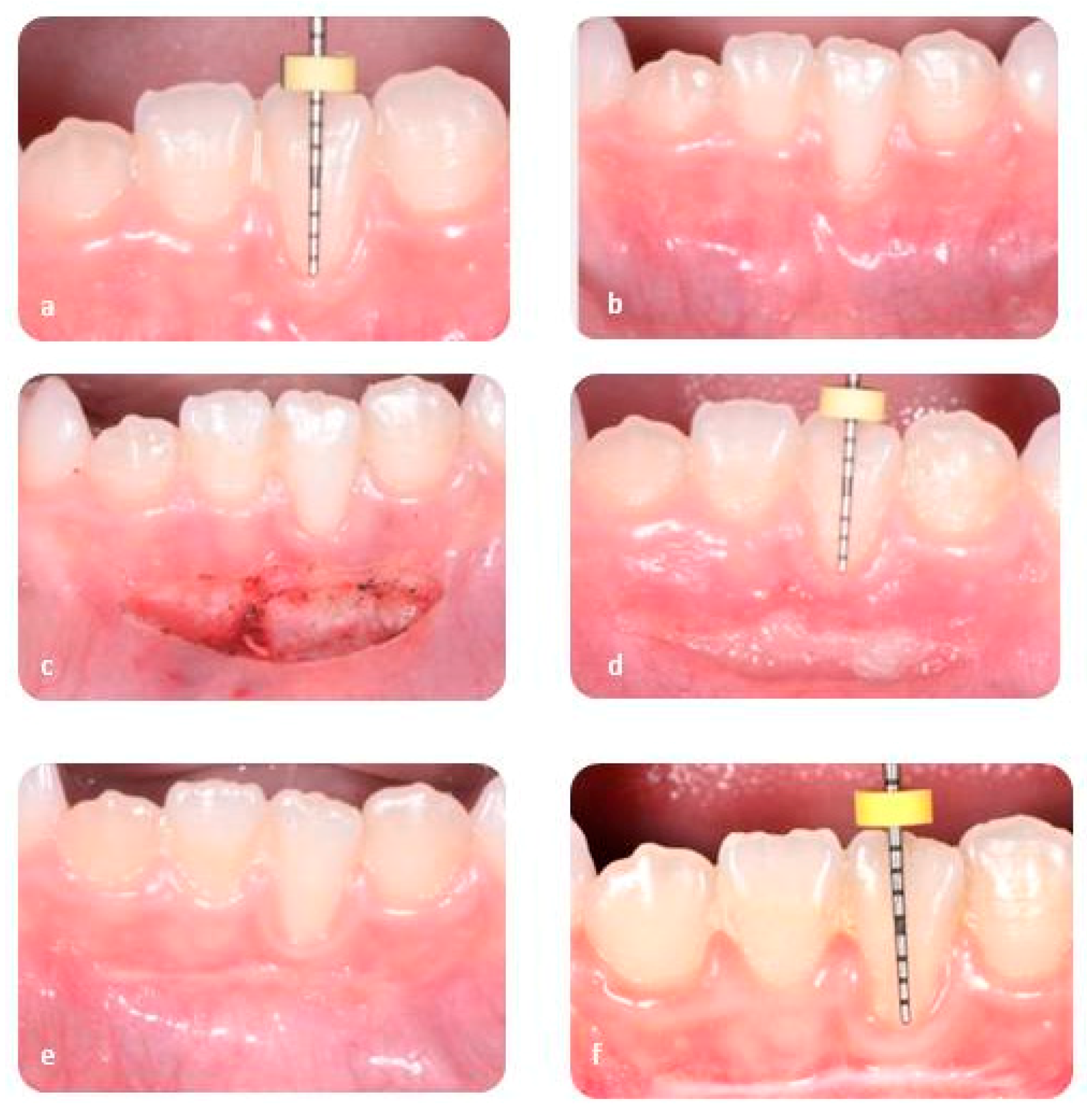
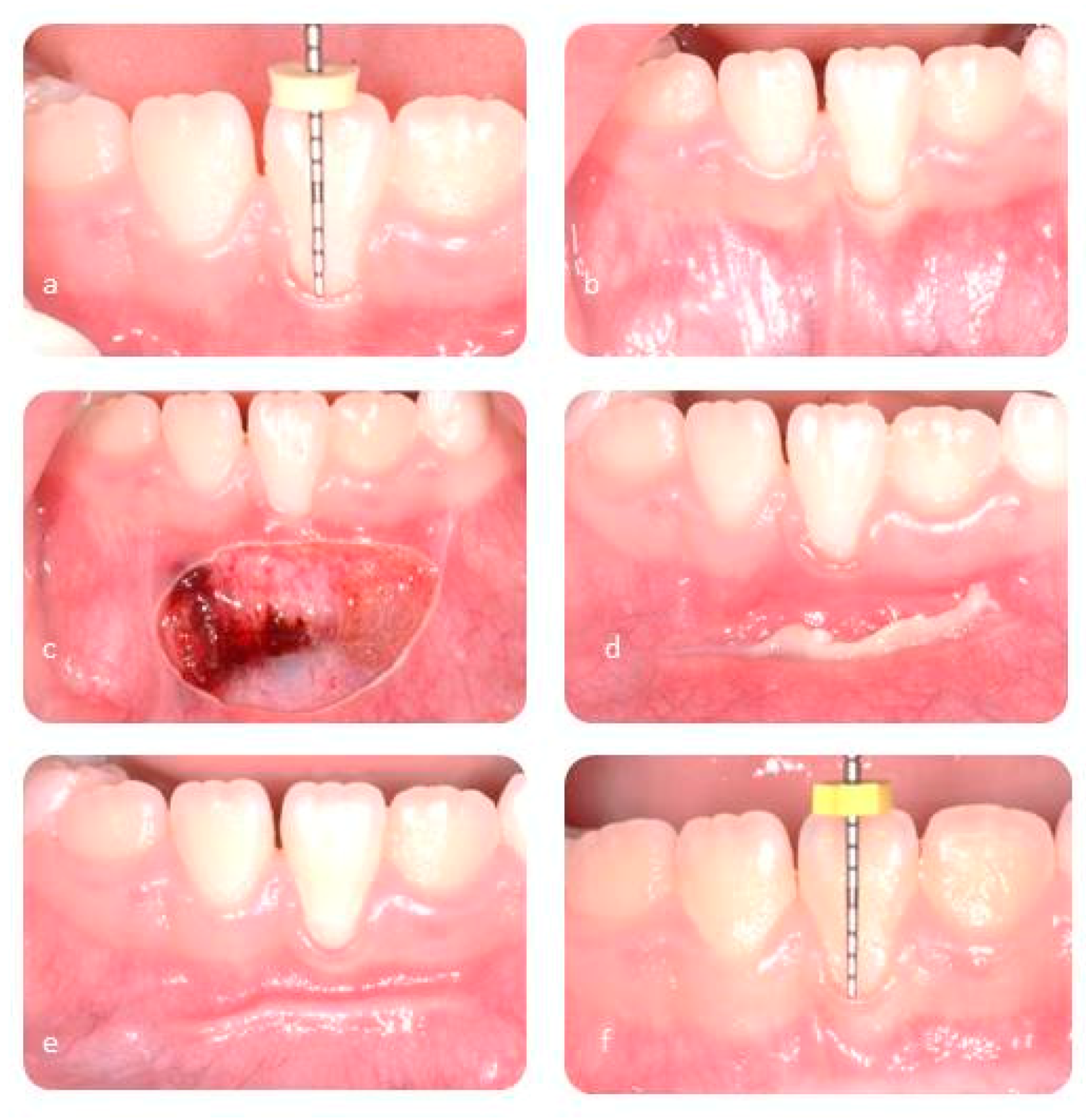
2.4. Surgical Protocol
2.5. Clinical Case
2.6. Statistical Methodology
3. Results
- In the manner of patients’ bleeding. In particular, after six months passed after the treatment, using CO2 caused fewer bleeding cases on average compared to the Diode Laser treatment. Specifically, we observed this impact on female patients more significantly rather than male patients
- In the manner of wound healing there is very strong evidence that after the treatment with the Diode Laser, patients’ wounds showed fast healing with respect to CO2 treatment
- In the manner of gingival recession, there is very strong evidence that the treatment with Diode Laser causes reducing patients’ gingival recession that is, on average, significantly better than the CO2 treatment. In particular, gingival recession of male patients decreases fast compared to female patients with Diode Laser treatment, whereas CO2 treatment has a better outcome on the reduction of gingival recession in female patients rather than male patients.
- In the manner of CAL, it can be said that after six months of the treatment with Diode Laser, the improvement of CAL is statistically significant and firmly reducing the periodontal pocket occurrence, whereas, there is no significant finding related to CAL after CO2 treatment
- Lastly, in the manner of NRS, it can be said that both methods reduce the pain very efficiently, Diode Laser treatment removes the pain faster than CO2 treatment. In fact, during the first fourteen days after the treatment, there was a reduction by 89% of pain in the group where it was used diode laser technique. On the other hand, in the same time rate, the reduction of pain was by 65% in the group where a CO2 laser was used. Notably, it is found that male patients got over the pain with Diode Laser easier than female patients, whilst CO2 treatment helped to remove the pain more effectively on female patients with respect to male patients.
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- McDonald, R.E.; Avery, D.R.; Dean, J.A. Examination of the Mouth and Other Relevant Structures. In McDonald and Avery Dentistry for the Child and Adolescent, 10th ed.; Elsevier: Amsterdam, The Netherlands, 2015; pp. 1–18. ISBN 9780323287456. [Google Scholar]
- Gottsegen, R. Frenum position and vestibule depth in relation to gingival health. Oral. Surg. Oral. Med. Oral. Pathol. 1954, 7, 1069–1078. [Google Scholar] [CrossRef]
- Rajani, E.R.; Biswas, P.P.; Emmatty, R. Prevalence of variations in morphology and attachment of maxillary labial frenum in various skeletal patterns—A cross-sectional study. J. Indian Soc. Periodontol. 2018, 22, 257–262. [Google Scholar] [CrossRef] [PubMed]
- Placek, M.; Skach, M.; Lubor, M. Significance of the Labial Frenum. Attachment in Periodontal Disease in Man. Part 1. Classification and Epidemiology of the Labial Frenum Attachment. J. Periodontol. 1974, 45, 891–894. [Google Scholar]
- Priyanka, M.; Sruthi, R.; Ramakrishnan, T.; Emmadi, P.; Ambalavanan, N. An overview of frenal attachments. J. Indian Soc. Periodontol. 2013, 17, 12–15. [Google Scholar] [CrossRef] [PubMed]
- Mello-Moura, A.C.V.; Cadioli, I.C.; Narras Pires Corrêa, M.S.; Delgado Rodrigues, C.R.M.; De Nardi Fonoff, R. Early Diagnosis and Surgical Treatment of the Lower Labial Frenum in Infancy: A Case Report. J. Clin. Pediatr. Dent. Spring 2008, 32, 181–183. [Google Scholar] [CrossRef]
- Di Stefano, D.A.; Maietti, S. Indicazioni cliniche degli innesti gengivali in pedodonzia. Ital. Oral Surg. 2009, 8, 257–262. [Google Scholar] [CrossRef]
- Song, H.J. Periodontal Considerations for Children. Dent. Clin. N. Am. 2013, 57, 17–37. [Google Scholar] [CrossRef]
- Lindhe, J.; Lang, N.P. Mucogingival Therapy. In Lindhe-Clinical Periodontology and Implant. Dentistry, 6th ed.; Wiley-Blackwell: Hoboken, NJ, USA, 2015; Volume 2, pp. 1000–1100. ISBN 9780470672488. [Google Scholar]
- Jati, A.S.; Furquim, L.Z.; Consolaro, A. Gingival recession: Its causes and types, and the importance of orthodontic treatment. Dental. Press J. Orthod. 2016, 21, 18–29. [Google Scholar] [CrossRef]
- Chan, H.L.; Chun, Y.H.P.; MacEachern, M.; Oates, T.W. Does gingival recession require surgical treatment? Dent. Clin. N. Am. 2015, 59, 981–996. [Google Scholar] [CrossRef]
- Seong, J.; Bartlett, D.; Newcombe, R.G.; Claydon, N.C.A.; Hellin, N.; West, N.X. Prevalence of gingival recession and study of associated related factors in young UK adults. J. Dent. 2018, 76, 58–67. [Google Scholar] [CrossRef]
- Janarthanan, S.; Arun, R.T.; Srinivasan, S.; Kumar, S.S. Frenectomy combined with a laterally displaced pedicle graft. Indian J. Dent. Sci. 2019, 11, 112–115. [Google Scholar] [CrossRef]
- Sobiech, P.; Szerszeń, M.; Wiśniewska, J. Application of Kazanjian’s vestibuloplasty in the prevention of gingival recession in children—A report of two cases. Nowa Stomatol. 2019, 24, 34–39. [Google Scholar]
- Vozza, I.; Mari, D.; Pacifici, E.; Luzzi, V.; Ierardo, G.; Sfasciotti, G.L.; Polimeni, A. Pediatric patients tolerance: A comparative study about using of Er:YAG laser and self-adhesive flowable composite for treatment of primary decayed teeth. Ann. Stomatol. 2016, 7, 24–28. [Google Scholar] [CrossRef]
- Derikvand, N.; Chinipardaz, Z.; Ghasemi, S.; Chiniforush, N. The Versatility of 980 nm Diode Laser in Dentistry: A Case Series. J. Lasers Med. Sci. 2016, 7, 205–208. [Google Scholar] [CrossRef] [PubMed]
- Sfasciotti, G.L.; Zara, F.; Fioravanti, M.; Guaragna, M.; Palaia, G.; Polimeni, A. Frenulectomy with Diode Laser Technology in Pediatric Patients: Quantitative and Qualitative Evaluations. Randomized Double-Blind Clinical Trial. Appl. Sci. 2020, 10, 4114. [Google Scholar] [CrossRef]
- Medeiros, R.J.; Gueiros, L.A.; Silva, I.H.; Carvalho, A.D.A.; Leão, J.C. Labial frenectomy with Nd:YAG laser and conventional surgery: A comparative study. Lasers Med. Sci. 2015, 30, 851–856. [Google Scholar]
- Pié-Sánchez, J.; España-Tost, A.J.; Arnabat-Domínguez, J.; Gay-Escoda, C. Comparative study of upper lip frenectomy with the CO2 laser versus the Er, Cr:YSGG laser. Med. Oral Patol Oral Cir. Bucal 2012, 17, e228–e232. [Google Scholar] [CrossRef]
- Zeinoun, T.; Majzoub, Z.; Khoury, C.; Nammour, S. CO2. Laser-Mediated Apically Positioned Flap in Areas Lacking Keratinized Gingiva. Laser Ther. 2017, 26, 121–127. [Google Scholar] [CrossRef]
- Research Randomizer. Available online: https://www.randomizer.org/ (accessed on 10 September 2020).
- Bartlett, D.; Ganss, C.; Lussi, A. Basic erosive wear examination (BEWE): A new scoring system for scientific and clinical needs. Clin. Oral Investig. 2008, 12, 165–168. [Google Scholar] [CrossRef]
- Miller, P.D. Miller Classification of Marginal Tissue Recession Revisited After 35 Years. Compend. Contin Educ. Dent. 2018, 39, 514–520. [Google Scholar]
- Papapanou, P.N.; Sanz, M.; Buduneli, N.; Dietrich, T.; Feres, M.; Fine, D.H.; Flemmig, T.F.; Garcia, R.; Giannobile, W.V.; Graziani, F.; et al. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Periodontol. 2018, 89, S173–S182. [Google Scholar] [CrossRef]
- Ainamo, J.; Bay, I. Problems and proposals for recording gingivitis and plaque. Int. Dent. J. 1975, 25, 229–235. [Google Scholar] [PubMed]
- Hannu, L. Oral Wound Healing: An Overview. In Oral Wound Healing; John Wiley & Sons, Ltd.: Hoboken, NJ, USA, 2013; ISBN 9781118704509. [Google Scholar]
- Löe, H. The Gingival Index, the Plaque Index and the Retention Index Systems. J. Periodontol. 1967, 38, 610–616. [Google Scholar] [CrossRef]
- Müller, H.P.; Heinecke, A.; Schaller, N.; Eger, T. Masticatory mucosa in subjects with different periodontal phenotypes. J. Clin. Periodontol. 2000, 27, 621–626. [Google Scholar] [CrossRef] [PubMed]
- Protásio, A.C.R.; Galvão, E.L.; Falci, S.G.M. Laser Techniques or Scalpel Incision for Labial Frenectomy: A Meta-analysis. J. Maxillofac. Oral. Surg. 2019, 18, 490–499. [Google Scholar] [CrossRef] [PubMed]
- Calisir, M.; Ege, B. Evaluation of patient perceptions after frenectomy operations: A comparison of neodymium-doped yttrium aluminum garnet laser and conventional techniques in the same patients. Niger. J. Clin. Pract. 2018, 21, 1059–1064. [Google Scholar] [PubMed]
- Sezgin, G.; Ozener, H.O.; Meseli, S.E.; Kuru, L. Evaluation of Patient’s Perceptions, Healing, and Reattachment After Conventional and Diode Laser Frenectomy: A Three-Arm Randomized Clinical Trial. Photobiomodul. Photomed. Laser Surg. 2020, 38, 552–559. [Google Scholar] [CrossRef] [PubMed]
- Uraz, A.; Çetiner, F.D.; Cula, S.; Guler, B.; Oztoprak, S. Patient Perceptions and Clinical Efficacy of Labial Frenectomies Using Diode Laser Versus Conventional Techniques. Stomatol. Oral Maxillofac. Surg. 2018, 119, 182–186. [Google Scholar] [CrossRef]
- Achom, M.; Chopra, R.; Sharma, N. Conventional or Diode laser for frenectomy. Which way to go? Int. J. Sci. Res. 2020, 7, 5. [Google Scholar]
- Yan, J.; Zhang, J.; Zhang, Q.; Zhang, X.; Ji, K. Effectiveness of laser adjunctive therapy for surgical treatment of gingival recession with flap graft techniques: A systematic review and meta-analysis. Lasers Med. Sci. 2018, 33, 899–908. [Google Scholar] [CrossRef]
- Jingarwar, M.; Pathak, A.; Kaur, B.N.; Kalaskar, R. Vestibular Extension Along With Frenectomy in Management of Localized Gingival Recession in Pediatric Patient: A New Innovative Surgical Approach. Int. J. Clin. Pediatr. Dent. 2015, 8, 224–226. [Google Scholar] [PubMed]
- Stylianou, P.; Soldatos, N.; Edmondson, E.K.; Angelov, N.; Weltman, R. Mandibular Labial Frenuloplasty. Early Creeping Attachment Noted After. Case Rep. Dent. 2020, 12, 3130894. [Google Scholar] [CrossRef] [PubMed]
| Periodontal Phenotype | Plaque Index | |||||
|---|---|---|---|---|---|---|
| A1 | A2 | B | 1 | 2 | 3 | |
| CO2 | 1 | 7 | 5 | 10 | 0 | 3 |
| Diode Laser | 1 | 4 | 8 | 8 | 2 | 3 |
| Type | Diode | CO2 |
|---|---|---|
| Name | Raffaello Bio | Smart US20D |
| Wavelength | 980-nm | 10.600 nm |
| Power | 2.5 W | 4.5 W |
| Modality of pulse | Continuous | Super pulse wave |
| Frequency | 1.000 Hz | 80 Hz |
| Medical class/Laser | IIB/IV | IIB/IV |
| Number of sessions | Single surgery session | Single surgery session |
| Production site. | DMT Dental Medical Technology | Deka |
| Bleeding | Wound Healing | Gingival Recession | CAL | NRS | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | SEM | Mean | SD | SEM | Mean | SD | SEM | Mean | SD | SEM | Mean | SD | SEM | ||
| Diode Laser | T0 | 1.15 | 0.55 | 0.15 | 3.00 | 0.00 | 0.00 | 1.69 | 0.63 | 0.17 | 1.46 | 0.66 | 0.18 | 0.00 | 0.00 | 0.00 |
| T1 | 1.62 | 0.65 | 0.18 | 1.69 | 0.48 | 0.13 | 1.62 | 0.51 | 0.14 | 1.46 | 0.66 | 0.18 | 3.62 | 2.96 | 0.82 | |
| T2 | 1.31 | 0.63 | 0.17 | 1.92 | 0.28 | 0.08 | 1.62 | 0.51 | 0.14 | 1.46 | 0.66 | 0.18 | 1.54 | 1.56 | 0.43 | |
| T3 | 1.15 | 0.55 | 0.15 | 2.54 | 0.66 | 0.18 | 1.00 | 0.00 | 0.00 | 1.15 | 0.38 | 0.10 | 0.08 | 0.28 | 0.08 | |
| T4 | 1.15 | 0.55 | 0.15 | 2.77 | 0.60 | 0.17 | 1.00 | 0.00 | 0.00 | 1.08 | 0.28 | 0.08 | 0.00 | 0.00 | 0.00 | |
| N | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | |
| CO2 | T0 | 1.00 | 0.00 | 0.00 | 3.00 | 0.00 | 0.00 | 1.38 | 0.77 | 0.21 | 1.31 | 0.63 | 0.17 | 0.00 | 0.00 | 0.00 |
| T1 | 2.00 | 0.58 | 0.16 | 1.92 | 0.49 | 0.14 | 1.38 | 0.77 | 0.21 | 1.31 | 0.63 | 0.17 | 3.38 | 2.26 | 0.63 | |
| T2 | 1.38 | 0.51 | 0.14 | 1.92 | 0.28 | 0.08 | 1.23 | 0.60 | 0.17 | 1.23 | 0.44 | 0.12 | 1.38 | 1.33 | 0.37 | |
| T3 | 1.00 | 0.00 | 0.00 | 2.23 | 0.93 | 0.26 | 1.08 | 0.49 | 0.14 | 1.23 | 0.44 | 0.12 | 0.23 | 0.83 | 0.23 | |
| T4 | 1.00 | 0.00 | 0.00 | 2.54 | 0.97 | 0.27 | 1.00 | 0.41 | 0.11 | 1.15 | 0.38 | 0.10 | 0.00 | 0.00 | 0.00 | |
| N | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | 13 | |
| Diode Laser | CO2 | ||||||
|---|---|---|---|---|---|---|---|
| t-Test | p-Value | SEM | t-Test | p-Value | SEM | ||
| Bleeding | Female | 2.828 | 0.030 ** | 0.571 | 4.582 | 0.004 ** | 1 |
| Male | 1.581 | 0.175 | 0.333 | 3.873 | 0.012 ** | 1 | |
| Total | 3.207 | 0.008 ** | 0.462 | 6.245 | 0.000 *** | 1.000 | |
| Wound Healing | Female | −3.873 | 0.008 ** | −0.714 | −1.441 | 0.199 | −0.429 |
| Male | −2.236 | 0.076 * | −0.500 | −1 | 0.363 | −0.333 | |
| Total | −4.383 | 0.000 *** | 0.616 | −1.806 | 0.096 * | −0.385 | |
| Gingival Recession | Female | 2.121 | 0.078 * | 0.429 | 2.828 | 0.030 ** | 0.571 |
| Male | 5 | 0.004 *** | 0.833 | 1 | 0.363 | 0.167 | |
| Total | 4.382 | 0.000 *** | 0.615 | 2.739 | 0.018 ** | 0.385 | |
| Periodontal Pocket | Female | 2.827 | 0.031 ** | 0.572 | 1 | 0.356 | 0.143 |
| Male | 1 | 0.363 | 0.167 | 1 | 0.360 | 0.165 | |
| Total | 2.612 | 0.017 ** | 0.384 | 1.477 | 0.165 | 0.154 | |
| NRS | Female | 2.547 | 0.043 ** | 2.857 | 4.831 | 0.002 ** | 3.285 |
| Male | 3.737 | 0.013 ** | 4.5 | 2.976 | 0.031 ** | 3.572 | |
| Total | 4.405 | 0.000 *** | 3.615 | 5.409 | 0.000 *** | 3.385 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sfasciotti, G.L.; Zara, F.; Vozza, I.; Carocci, V.; Ierardo, G.; Polimeni, A. Diode versus CO2 Laser Therapy in the Treatment of High Labial Frenulum Attachment: A Pilot Randomized, Double-Blinded Clinical Trial. Int. J. Environ. Res. Public Health 2020, 17, 7708. https://doi.org/10.3390/ijerph17217708
Sfasciotti GL, Zara F, Vozza I, Carocci V, Ierardo G, Polimeni A. Diode versus CO2 Laser Therapy in the Treatment of High Labial Frenulum Attachment: A Pilot Randomized, Double-Blinded Clinical Trial. International Journal of Environmental Research and Public Health. 2020; 17(21):7708. https://doi.org/10.3390/ijerph17217708
Chicago/Turabian StyleSfasciotti, Gian Luca, Francesca Zara, Iole Vozza, Veronica Carocci, Gaetano Ierardo, and Antonella Polimeni. 2020. "Diode versus CO2 Laser Therapy in the Treatment of High Labial Frenulum Attachment: A Pilot Randomized, Double-Blinded Clinical Trial" International Journal of Environmental Research and Public Health 17, no. 21: 7708. https://doi.org/10.3390/ijerph17217708
APA StyleSfasciotti, G. L., Zara, F., Vozza, I., Carocci, V., Ierardo, G., & Polimeni, A. (2020). Diode versus CO2 Laser Therapy in the Treatment of High Labial Frenulum Attachment: A Pilot Randomized, Double-Blinded Clinical Trial. International Journal of Environmental Research and Public Health, 17(21), 7708. https://doi.org/10.3390/ijerph17217708







