Acute Myocardial Infarction Hospitalizations between Cold and Hot Seasons in an Island across Tropical and Subtropical Climate Zones—A Population-Based Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Study Cases
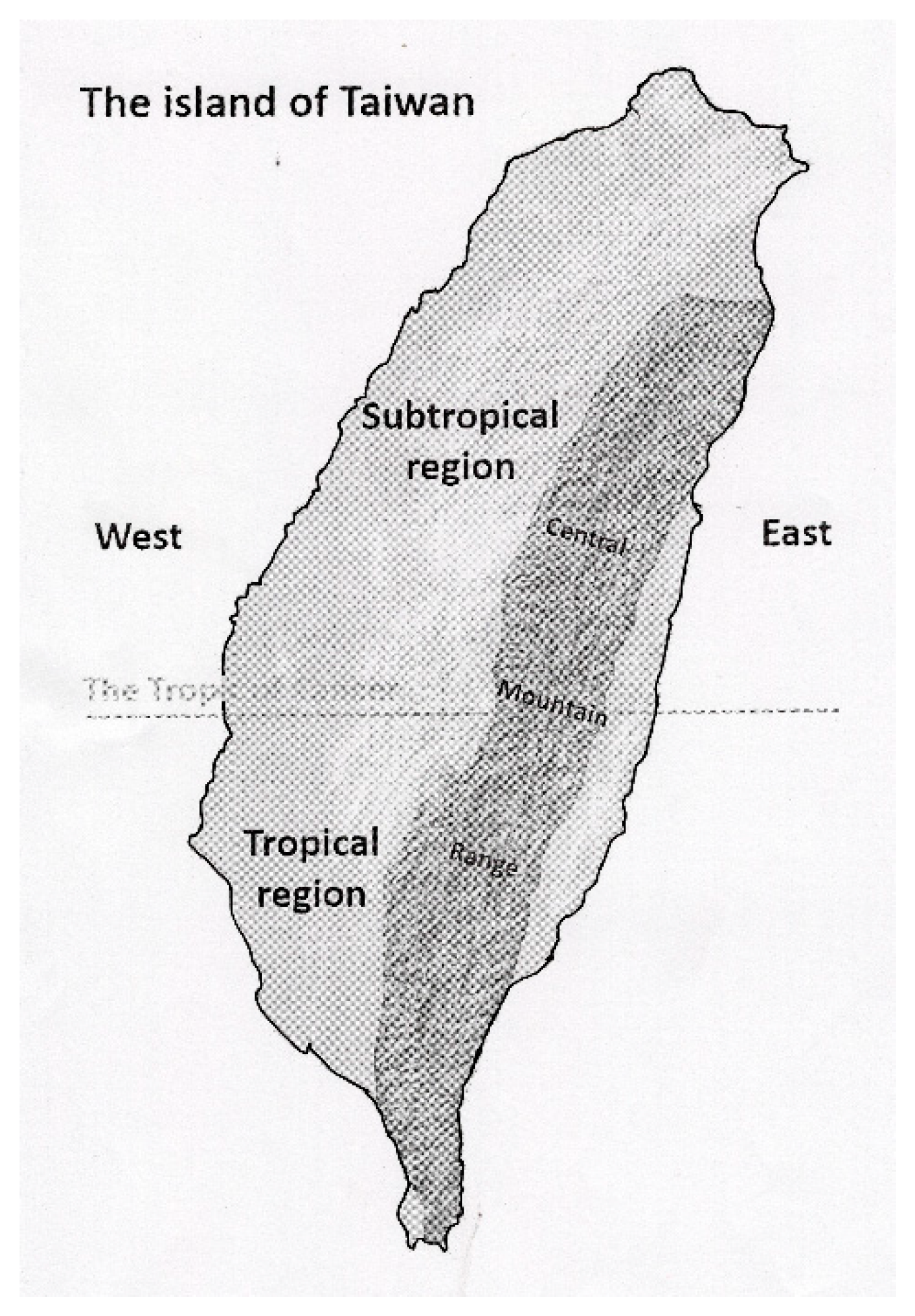
2.3. Weather Data and Season
2.4. Statistical Analysis
3. Results
3.1. Descriptive Statistics
3.2. Comparison of AMI Hospitalizations between Cold and Hot Seasons
3.3. Logistic Regression Model on the Association of the Cold Season with AMI Hospitalizations
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tofler, G.H.; Muller, J.E. Triggering of acute cardiovascular disease and potential preventive strategies. Circulation 2006, 114, 1863–1872. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A.; Guo, Y.; Hashizume, M.; Lavigne, E.; Zanobetti, A.; Schwartz, J.; Tobias, A.; Tong, S.; Rocklov, J.; Forsberg, B.; et al. Mortality risk attributable to high and low ambient temperature: A multicountry observational study. Lancet 2015, 386, 369–375. [Google Scholar] [CrossRef]
- Watts, N.; Amann, M.; Ayeb-Karlsson, S.; Belesova, K.; Bouley, T.; Boykoff, M.; Byass, P.; Cai, W.; Campbell-Lendrum, D.; Chambers, J.; et al. The Lancet Countdown on health and climate change: From 25 years of inaction to a global transformation for public health. Lancet 2018, 391, 581–630. [Google Scholar] [CrossRef]
- Claeys, M.J.; Rajagopalan, S.; Nawrot, T.S.; Brook, R.D. Climate and environmental triggers of acute myocardial infarction. Eur. Heart J. 2017, 38, 955–960. [Google Scholar] [CrossRef] [PubMed]
- Spencer, F.A.; Goldberg, R.J.; Becker, R.C.; Gore, J.M. Seasonal distribution of acute myocardial infarction in the second National Registry of Myocardial Infarction. J. Am. Coll. Cardiol. 1998, 31, 1226–1233. [Google Scholar] [CrossRef]
- Bhaskaran, K.; Hajat, S.; Haines, A.; Herrett, E.; Wilkinson, P.; Smeeth, L. Short term effects of temperature on risk of myocardial infarction in England and Wales: Time series regression analysis of the Myocardial Ischaemia National Audit Project (MINAP) registry. BMJ 2010, 341, c3823. [Google Scholar] [CrossRef]
- Lee, J.H.; Chae, S.C.; Yang, D.H.; Park, H.S.; Cho, Y.; Jun, J.E.; Park, W.H.; Kam, S.; Lee, W.K.; Kim, Y.J.; et al. Influence of weather on daily hospital admissions for acute myocardial infarction (from the Korea Acute Myocardial Infarction Registry). Int. J. Cardiol. 2010, 144, 16–21. [Google Scholar] [CrossRef] [PubMed]
- Vasconcelos, J.; Freire, E.; Almendra, R.; Silva, G.L.; Santana, P. The impact of winter cold weather on acute myocardial infarctions in Portugal. Environ. Pollut. 2013, 183, 14–18. [Google Scholar] [CrossRef]
- Heyer, H.E.; Teng, H.C.; Barris, W. The increased frequency of acute myocardial infarction during summer months in a warm climate; a study of 1386 cases from Dallas, Texas. Am. Heart J. 1953, 45, 741–748. [Google Scholar] [CrossRef]
- Ku, C.S.; Yang, C.Y.; Lee, W.J.; Chiang, H.T.; Liu, C.P.; Lin, S.L. Absence of a seasonal variation in myocardial infarction onset in a region without temperature extremes. Cardiology 1998, 89, 277–282. [Google Scholar] [CrossRef]
- Goggins, W.B.; Chan, E.Y.; Yang, C.Y. Weather, pollution, and acute myocardial infarction in Hong Kong and Taiwan. Int. J. Cardiol. 2013, 168, 243–249. [Google Scholar] [CrossRef]
- Lam, H.C.Y.; Chan, J.C.N.; Luk, A.O.Y.; Chan, E.Y.Y.; Goggins, W.B. Short-term association between ambient temperature and acute myocardial infarction hospitalizations for diabetes mellitus patients: A time series study. PLoS Med. 2018, 15, e1002612. [Google Scholar] [CrossRef]
- Wu, T.Y.; Majeed, A.; Kuo, K.N. An overview of the healthcare system in Taiwan. Lond. J. Prim. Care 2010, 3, 115–119. [Google Scholar] [CrossRef]
- Danet, S.; Richard, F.; Montaye, M.; Beauchant, S.; Lemaire, B.; Graux, C.; Cottel, D.; Marecaux, N.; Amouyel, P. Unhealthy effects of atmospheric temperature and pressure on the occurrence of myocardial infarction and coronary deaths. A 10-year survey: The Lille-World Health Organization MONICA project (Monitoring trends and determinants in cardiovascular disease). Circulation 1999, 100, E1–E7. [Google Scholar] [CrossRef]
- Morabito, M.; Crisci, A.; Grifoni, D.; Orlandini, S.; Cecchi, L.; Bacci, L.; Modesti, P.A.; Gensini, G.F.; Maracchi, G. Winter air-mass-based synoptic climatological approach and hospital admissions for myocardial infarction in Florence, Italy. Environ. Res. 2006, 102, 52–60. [Google Scholar] [CrossRef]
- Enquselassie, F.; Dobson, A.J.; Alexander, H.M.; Steele, P.L. Seasons, temperature and coronary disease. Int. J. Epidemiol. 1993, 22, 632–636. [Google Scholar] [CrossRef]
- Esler, M.D.; Thompson, J.M.; Kaye, D.M.; Turner, A.G.; Jennings, G.L.; Cox, H.S.; Lambert, G.W.; Seals, D.R. Effects of aging on the responsiveness of the human cardiac sympathetic nerves to stressors. Circulation 1995, 91, 351–358. [Google Scholar] [CrossRef]
- Green, R.S.; Basu, R.; Malig, B.; Broadwin, R.; Kim, J.J.; Ostro, B. The effect of temperature on hospital admissions in nine California counties. Int. J. Public Health 2010, 55, 113–121. [Google Scholar] [CrossRef]
- Yang, J.; Yin, P.; Zhou, M.; Ou, C.Q.; Li, M.; Liu, Y.; Gao, J.; Chen, B.; Liu, J.; Bai, L.; et al. The effect of ambient temperature on diabetes mortality in China: A multi-city time series study. Sci. Total Environ. 2016, 543, 75–82. [Google Scholar] [CrossRef]
- Seposo, X.T.; Dang, T.N.; Honda, Y. How Does Ambient Air Temperature Affect Diabetes Mortality in Tropical Cities? Int. J. Environ. Res. Public Health 2017, 14, 385. [Google Scholar] [CrossRef]
- Sun, Z.; Chen, C.; Xu, D.; Li, T. Effects of ambient temperature on myocardial infarction: A systematic review and meta-analysis. Environ. Pollut. 2018, 241, 1106–1114. [Google Scholar] [CrossRef]
- Wolf, K.; Schneider, A.; Breitner, S.; von Klot, S.; Meisinger, C.; Cyrys, J.; Hymer, H.; Wichmann, H.E.; Peters, A. Air temperature and the occurrence of myocardial infarction in Augsburg, Germany. Circulation 2009, 120, 735–742. [Google Scholar] [CrossRef]
- Madrigano, J.; Mittleman, M.A.; Baccarelli, A.; Goldberg, R.; Melly, S.; von Klot, S.; Schwartz, J. Temperature, myocardial infarction, and mortality: Effect modification by individual—And area-level characteristics. Epidemiology 2013, 24, 439–446. [Google Scholar] [CrossRef]
- Yoon, K.H.; Lee, J.H.; Kim, J.W.; Cho, J.H.; Choi, Y.H.; Ko, S.H.; Zimmet, P.; Son, H.Y. Epidemic obesity and type 2 diabetes in Asia. Lancet 2006, 368, 1681–1688. [Google Scholar] [CrossRef]
- Briaud, I.; Harmon, J.S.; Kelpe, C.L.; Segu, V.B.; Poitout, V. Lipotoxicity of the pancreatic beta-cell is associated with glucose-dependent esterification of fatty acids into neutral lipids. Diabetes 2001, 50, 315–321. [Google Scholar] [CrossRef]
- Parhofer, K.G. Interaction between Glucose and Lipid Metabolism: More than Diabetic Dyslipidemia. Diabetes Metab. J. 2015, 39, 353–362. [Google Scholar] [CrossRef]
| Cold Season | Hot Season | |||||
|---|---|---|---|---|---|---|
| Nov | to | Apr | May | to | Oct | |
| Subtropical region | ||||||
| Monthly temperature (Mean ± SD) (°C) | 21.9 ± 0.9 | - | 22.6 ± 1.2 | 25.7 ± 0.9 | - | 25.0 ± 0.9 |
| Seasonal temperature (Mean ± SD) (°C) | 19.2 ± 2.7 | 27.3 ± 1.8 | ||||
| Tropical region | ||||||
| Monthly temperature (Mean ± SD) (°C) | 23.6 ± 1.1 | - | 25.2 ± 0.9 | 27.4 ± 0.6 | - | 26.5 ± 0.8 |
| Seasonal temperature (Mean ± SD) (°C) | 21.5 ± 2.7 | 28.0 ± 1.1 | ||||
| Total | Subtropical Group | Tropical Group | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n = 6897 | % | Mean | ±SD | n = 4604 | % | Mean | ±SD | n = 2293 | % | Mean | ±SD | |
| Gender | ||||||||||||
| Male | 4741 | 68.7 | 3152 | 68.5 | 1589 | 69.3 | ||||||
| Female | 2156 | 31.3 | 1452 | 31.5 | 704 | 30.7 | ||||||
| Age | 66.0 | 14.1 | 66.5 | 13.7 | ||||||||
| Male | 63.9 | 13.9 | 63.6 | 13.9 | 64.4 | 13.8 | ||||||
| Female | 71.3 | 12.8 | 71.3 | 13.0 | 71.3 | 12.2 | ||||||
| <65 years | 3047 | 44.2 | 2065 | 44.9 | 982 | 42.8 | ||||||
| ≥65 years | 3850 | 55.8 | 2539 | 55.1 | 1311 | 57.2 | ||||||
| Comorbidity | ||||||||||||
| Hypertension | 4286 | 62.1 | 2847 | 61.8 | 1439 | 62.8 | ||||||
| DM | 2436 | 35.3 | 1580 | 34.3 | 856 | 37.3 | ||||||
| Dyslipidemia | 1254 | 18.2 | 844 | 18.3 | 410 | 17.9 | ||||||
| Cold–Hot Seasons | Cold Season | Hot Season | OR (95%CI) | p-Value | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Nov | Dec | Jan | Feb | Mar | Apr | May | Jun | Jul | Aug | Sep | Oct | |||
| Total | ||||||||||||||
| No. of AMI Hosp. each month | 576 | 612 | 661 | 620 | 590 | 580 | 567 | 492 | 543 | 572 | 523 | 561 | ||
| No. of AMI Hosp./No. of Overall Hosp. (%) in Total | 3639/242,791 (1.5%) | 3258/249,572 (1.3%) | 1.15 (1.10–1.21) | <0.001 ★ | ||||||||||
| Subtropical group | ||||||||||||||
| No. of AMI Hosp. each month | 374 | 397 | 437 | 408 | 411 | 412 | 373 | 333 | 369 | 375 | 349 | 366 | ||
| No. of AMI Hosp./No. of Overall Hosp. (%) in Total | 2439/171,304 (1.4%) | 2165/176,298 (1.2%) | 1.16 (1.10–1.23) | <0.001 ★ | ||||||||||
| Tropical group | ||||||||||||||
| No. of AMI Hosp. each month | 202 | 215 | 224 | 212 | 179 | 168 | 194 | 159 | 174 | 197 | 174 | 195 | ||
| No. of AMI Hosp./No. of Overall Hosp. (%) in Total | 1200/71,847(1.7%) | 1093/73,274 (1.5%) | 1.15 (1.11–1.19) | 0.040 ★ | ||||||||||
| Total n = 6897 | Subtropical Group n = 4604 | Tropical Group n = 2293 | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value | |
| Age | |||||||||
| <65 years (ref.) | 1539/3047 (50.5) | 1 | 1037/2065 (50.2) | 1 | 502/982 (51.1) | 1 | |||
| ≥65 years | 2100/3850 (54.5) | 1.20 (1.07–1.35) | 0.002 ★ | 1402/2539 (55.2) | 1.28 (1.11–1.48) | 0.001 ★ | 698/1311 (53.2) | 1.06 (0.87–1.30) | 0.165 |
| Gender | |||||||||
| Male (ref.) | 2499/4741 (52.7) | 1 | 1659/3152 (52.6) | 1 | 840/1589 (52.9) | 1 | |||
| Female | 1140/2156 (52.9) | 1.01 (0.84–1.20) | 0.951 | 780/1452 (53.7) | 1.10 (0.88–1.37) | 0.399 | 360/704 (51.1) | 0.80 (0.58–1.10) | 0.165 |
| Age by Gender | 0.93 (0.75–1.16) | 0.527 | 0.84 (0.64–1.10) | 0.202 | 1.17 (0.90–1.72) | 0.427 | |||
| Diabetes mellitus | |||||||||
| No | 2297/4461 (51.5) | 1 | 1570/3024 (51.9) | 1 | 727/1437 (50.6) | 1 | |||
| Yes | 1342/2436 (55.1) | 1.17 (1.05–1.30) | 0.005 ★ | 869/1580 (55.0) | 1.12 (0.98–1.28) | 0.111 | 473/856 (55.3) | 1.25 (1.04–1.51) | 0.018 ★ |
| Hypertension | |||||||||
| No | 1358/2611 (52.0) | 1 | 913/1757 (52.0) | 1 | 445/854 (52.1) | 1 | |||
| Yes | 2281/4286 (53.2) | 0.95 (0.85–1.06) | 0.329 | 1526/2847 (53.6) | 0.97 (0.85–1.11) | 0.674 | 755/1439 (52.5) | 0.94 (0.78–1.14) | 0.522 |
| Dyslipidemia | |||||||||
| No | 2972/5643 (52.7) | 1 | 1988/3760 (52.9) | 1 | 984/1883 (52.3) | 1 | |||
| Yes | 667/1254 (53.2) | 0.97 (0.85–1.10) | 0.584 | 451/844 (53.4) | 0.98 (0.83–1.15) | 0.784 | 216/410 (52.7) | 0.97 (0.77–1.21) | 0.764 |
| ≥65 Years Group | Subtropical Group n = 2539 | Tropical Group n = 1311 | ||||
| N = 3850 | Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value |
| Gender | ||||||
| Male (ref.) | 828/1480 (55.9) | 1 | 430/802 (53.6) | 1 | ||
| Female | 574/1059 (54.2) | 0.93 (0.79–1.09) | 0.346 | 268/509 (52.7) | 0.92 (0.73–1.15) | 0.453 |
| Diabetes mellitus | ||||||
| No | 518/1495 (54.5) | 1 | 382/757 (50.5) | 1 | ||
| Yes | 587/1044 (56.2) | 1.10 (0.93–1.31) | 0.257 | 316/554 (57.0) | 1.32 (1.04–1.67) | 0.022 ★ |
| Hypertension | ||||||
| No | 338/610 (55.4) | 1 | 166/324 (51.2) | 1 | ||
| Yes | 1064/1929 (55.2) | 0.98 (0.81–1.19) | 0.859 | 532/987 (53.9) | 1.04 (0.80–1.35) | 0.781 |
| Dyslipidemia | ||||||
| No | 1118/2017 (55.4) | 1 | 566/1068 (53.0) | 1 | ||
| Yes | 284/522 (54.4) | 0.94 (0.77–1.15) | 0.556 | 132/243 (54.3) | 0.96 (0.72–1.29) | 0.799 |
| <65 Years Group | Subtropical Group n = 2065 | Tropical Group n = 982 | ||||
| N = 3047 | Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value |
| Gender | ||||||
| Male (ref.) | 831/1672 (49.7) | 1 | 410/787 (52.1) | 1 | ||
| Female | 206/393 (52.4) | 1.10 (0.88–1.37) | 0.421 | 92/195 (47.2) | 0.82(0.60–1.14) | 0.236 |
| Diabetes mellitus | ||||||
| No | 755/1529 (49.4) | 1 | 345/680 (50.7) | 1 | ||
| Yes | 282/536 (52.6) | 1.14 (0.91–1.42) | 0.260 | 157/302 (52.0) | 1.16(0.85–1.56) | 0.352 |
| Hypertension | ||||||
| No | 575/1147 (50.1) | 1 | 279/530 (52.6) | 1 | ||
| Yes | 462/918 (50.3) | 0.95 (0.79–1.15) | 0.619 | 223/452 (49.3) | 0.86(0.65–1.13) | 0.274 |
| Dyslipidemia | ||||||
| No | 870/1743 (49.9) | 1 | 418/815 (51.3) | 1 | ||
| Yes | 167/322 (51.9) | 1.04 (0.80–1.35) | 0.767 | 84/167 (50.3) | 0.98(0.69–1.41) | 0.928 |
| DM Group | Subtropical Group n = 1580 | Tropical Group n = 856 | ||||
| n = 2436 | Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value |
| Age | ||||||
| <65 years (ref.) | 282/536 (52.6) | 1 | 157/302 (52.0) | 1 | ||
| ≥65 years | 587/1044 (56.2) | 1.20 (0.92–1.57) | 0.177 | 316/554 (57.0) | 1.10 (0.77–1.58) | 0.605 |
| Gender | ||||||
| Male (ref.) | 497/907 (54.8) | 1 | 270/501 (53.9) | 1 | ||
| Female | 372/673 (55.3) | 1.06 (0.73–1.55) | 0.758 | 203/355 (57.2) | 0.96 (0.58–1.59) | 0.878 |
| Age by Gender | 0.92 (0.59–1.45) | 0.733 | 1.26 (0.69–2.30) | 0.455 | ||
| Hypertension | ||||||
| No | 132/231 (57.1) | 1 | 78/139 (56.1) | 1 | ||
| Yes | 737/1349 (54.6) | 0.88 (0.66–1.18) | 0.402 | 395/717 (55.1) | 0.94 (0.64–1.37) | 0.749 |
| Dyslipidemia | ||||||
| No | 572/1022 (56.0) | 1 | 338/585 (57.8) | 1 | ||
| Yes | 297/558 (53.2) | 0.91 (0.74–1.12) | 0.386 | 135/271 (49.8) | 0.74 (0.55–0.99) | 0.040 ★ |
| Non-DM Group | Subtropical Group n = 3024 | Tropical Group n = 1437 | ||||
| n = 4461 | Event n/N (%) | OR (95%CI) | p-Value | Event n/N (%) | OR (95%CI) | p-Value |
| Age | ||||||
| <65 years (ref.) | 755/1529 (49.4) | 1 | 345/680 (50.7) | 1 | ||
| ≥65 years | 815/1495 (54.5) | 1.31 (1.10–1.56) | 0.002★ | 382/757 (50.5) | 1.07 (0.83–1.37) | 0.610 |
| Gender | ||||||
| Male (ref.) | 1162/2245 (51.8) | 1 | 570/1088 (52.4) | 1 | ||
| Female | 408/779 (52.4) | 1.13 (0.86–1.48) | 0.394 | 157/349 (45.0) | 0.75 (0.49–1.14) | 0.174 |
| Age by Gender | 0.79 (0.56–1.11) | 0.175 | 0.99 (0.59–1.67) | 0.975 | ||
| Hypertension | ||||||
| No | 781/1526 (51.2) | 1 | 349/715 (51.3) | 1 | ||
| Yes | 789/1498 (52.7) | 0.99 (0.85–1.15) | 0.875 | 360/722 (49.9) | 0.91 (0.73–1.14) | 0.409 |
| Dyslipidemia | ||||||
| No | 1416/2738 (51.7) | 1 | 646/1298 (49.8) | 1 | ||
| Yes | 154/286 (53.8) | 1.08 (0.84–1.39) | 0.535 | 81/139 (58.3) | 1.45 (1.01–2.09) | 0.044 ★ |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chu, M.-L.; Shih, C.-Y.; Hsieh, T.-C.; Chen, H.-L.; Lee, C.-W.; Hsieh, J.-C. Acute Myocardial Infarction Hospitalizations between Cold and Hot Seasons in an Island across Tropical and Subtropical Climate Zones—A Population-Based Study. Int. J. Environ. Res. Public Health 2019, 16, 2769. https://doi.org/10.3390/ijerph16152769
Chu M-L, Shih C-Y, Hsieh T-C, Chen H-L, Lee C-W, Hsieh J-C. Acute Myocardial Infarction Hospitalizations between Cold and Hot Seasons in an Island across Tropical and Subtropical Climate Zones—A Population-Based Study. International Journal of Environmental Research and Public Health. 2019; 16(15):2769. https://doi.org/10.3390/ijerph16152769
Chicago/Turabian StyleChu, Min-Liang, Chiao-Yu Shih, Tsung-Cheng Hsieh, Han-Lin Chen, Chih-Wei Lee, and Jen-Che Hsieh. 2019. "Acute Myocardial Infarction Hospitalizations between Cold and Hot Seasons in an Island across Tropical and Subtropical Climate Zones—A Population-Based Study" International Journal of Environmental Research and Public Health 16, no. 15: 2769. https://doi.org/10.3390/ijerph16152769
APA StyleChu, M.-L., Shih, C.-Y., Hsieh, T.-C., Chen, H.-L., Lee, C.-W., & Hsieh, J.-C. (2019). Acute Myocardial Infarction Hospitalizations between Cold and Hot Seasons in an Island across Tropical and Subtropical Climate Zones—A Population-Based Study. International Journal of Environmental Research and Public Health, 16(15), 2769. https://doi.org/10.3390/ijerph16152769




