Adjustment Disorder: Current Developments and Future Directions
Abstract
1. Introduction
2. Diagnostic Criteria
2.1. Commonalities between DSM-5 and ICD-11
2.2. Differences between DSM-5 and ICD-11
2.2.1. Subtypes
2.2.2. Adjustment Disorder as a Subsyndromal Disorder
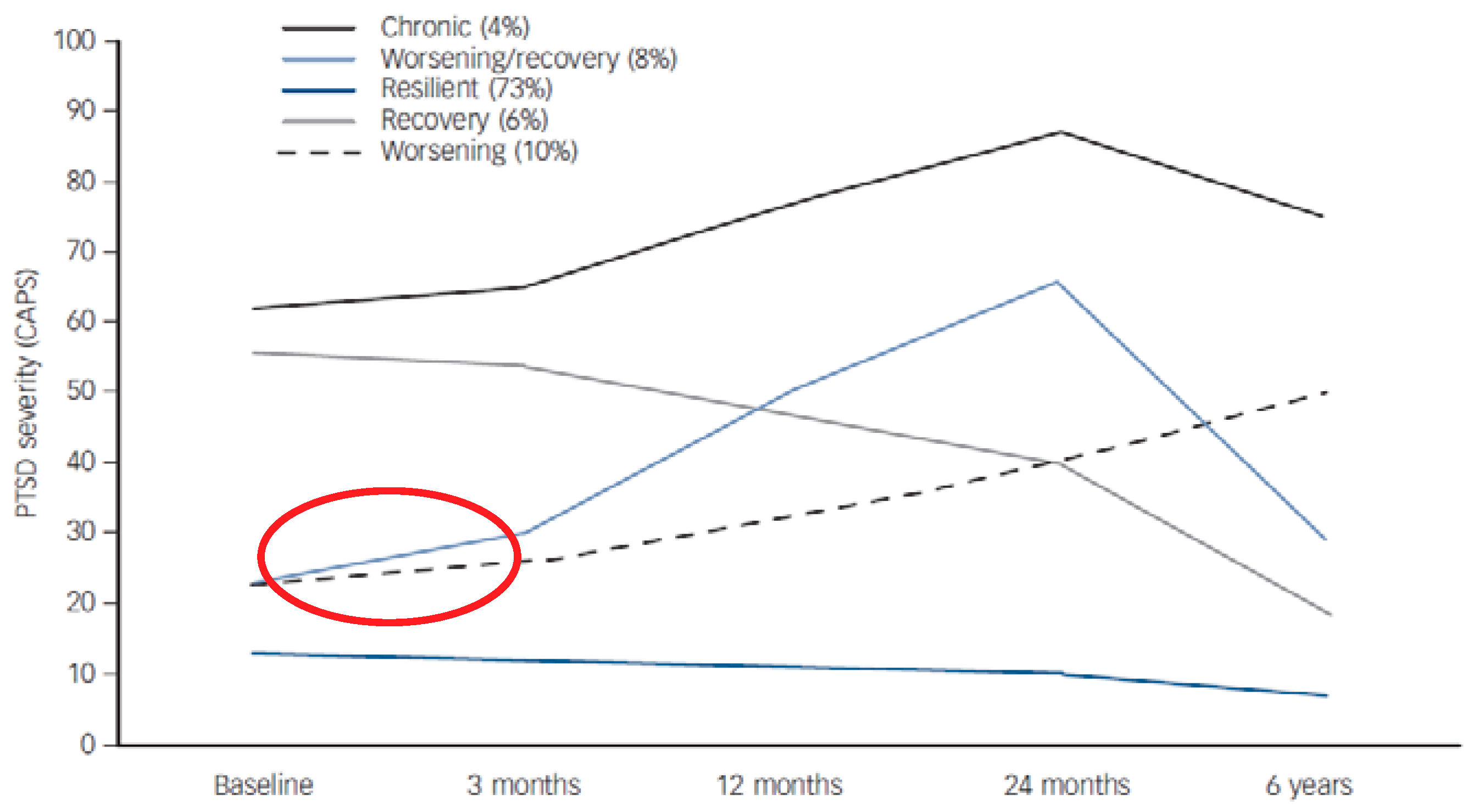
3. Course and Trajectory
4. Assessment
5. Treatment and Intervention
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- American Psychiatric Association. Trauma- and stressor-related disorders. In Diagnostic and Statistical Manual of Mental Disorders (DSM-5®), 5th ed.; American Psychiatric Association Publishing: Washington, DC, USA, 2013. [Google Scholar]
- Einsle, F.; Köllner, V.; Dannemann, S.; Maercker, A. Development and validation of a self-report for the assessment of adjustment disorders. Psychol. Health Med. 2010, 15, 584–595. [Google Scholar] [CrossRef] [PubMed]
- Gradus, J.L. Prevalence and prognosis of stress disorders: A review of the epidemiologic literature. Clin. Epidemiol. 2017, 9, 251. [Google Scholar] [CrossRef] [PubMed]
- Glaesmer, H.; Romppel, M.; Brähler, E.; Hinz, A.; Maercker, A. Adjustment disorder as proposed for ICD-11: Dimensionality and symptom differentiation. Psychiatry Res. 2015, 229, 940–948. [Google Scholar] [CrossRef] [PubMed]
- Perkonigg, A.; Lorenz, L.; Maercker, A. Prevalence and correlates of ICD-11 adjustment disorder: Findings from the Zurich Adjustment Disorder Study. Int. J. Clin. Health Psychol. 2018, 18, 209–217. [Google Scholar] [CrossRef] [PubMed]
- Killikelly, C.; Lorenz, L.; Bauer, S.; Mahat-Shamir, M.; Ben-Ezra, M.; Maercker, A. Prolonged grief disorder: Its co-occurrence with adjustment disorder and post-traumatic stress disorder in a bereaved Israeli general-population sample. J. Affect. Disord. 2019, 249, 307–314. [Google Scholar] [CrossRef]
- Foster, P.; Oxman, T. A descriptive study of adjustment disorder diagnoses in general hospital patients. Ir. J. Psychol. Med. 1994, 11, 153–157. [Google Scholar] [CrossRef]
- Strain, J.J.; Smith, G.C.; Hammer, J.S.; McKenzie, D.P.; Blumenfield, M.; Muskin, P.; Newstadt, G.; Wallack, J.; Wilner, A.; Schleifer, S.S. Adjustment disorder: A multisite study of its utilization and interventions in the consultation-liaison psychiatry setting. Gen. Hosp. Psychiatry 1998, 20, 139–149. [Google Scholar] [CrossRef]
- Sadock, B.J.; Sadock, V.A. Kaplan and Sadock’s Synopsis of Psychiatry: Behavioral Sciences/Clinical Psychiatry; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2015. [Google Scholar]
- Taggart, C.; O’Grady, J.; Stevenson, M.; Hand, E.; Mc Clelland, R.; Kelly, C. Accuracy of diagnosis at routine psychiatric assessment in patients presenting to an accident and emergency department. Gen. Hosp. Psychiatry 2006, 28, 330–335. [Google Scholar] [CrossRef]
- Mitchell, A.J.; Chan, M.; Bhatti, H.; Halton, M.; Grassi, L.; Johansen, C.; Meader, N. Prevalence of depression, anxiety, and adjustment disorder in oncological, haematological, and palliative-care settings: A meta-analysis of 94 interview-based studies. Lancet Oncol. 2011, 12, 160–174. [Google Scholar] [CrossRef]
- Okamura, H.; Watanabe, T.; Narabayashi, M.; Katsumata, N.; Ando, M.; Adachi, I.; Akechi, T.; Uchitomi, Y. Psychological distress following first recurrence of disease in patients with breast cancer: Prevalence and risk factors. Breast Cancer Res. Treat. 2000, 61, 131–137. [Google Scholar] [CrossRef]
- Silverstone, P.H. Prevalence of psychiatric disorders in medical inpatients. J. Nerv. Ment. Dis. 1996, 184, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Strain, J.J.; Friedman, M.J. Considering adjustment disorders as stress response syndromes for DSM-5. Depress. Anxiety 2011, 28, 818–823. [Google Scholar] [CrossRef] [PubMed]
- Bachem, R.; Casey, P. Adjustment disorder: A diagnosis whose time has come. J. Affect. Disord. 2017, 227, 243–253. [Google Scholar] [CrossRef] [PubMed]
- Casey, P. Adjustment disorder: New developments. Curr. Psychiatry Rep. 2014, 16, 451. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, M.L.; Alkemade, N.; Creamer, M.; McFarlane, A.C.; Silove, D.; Bryant, R.A.; Felmingham, K.; Steel, Z.; Forbes, D. A longitudinal study of adjustment disorder after trauma exposure. Am. J. Psychiatry 2016, 173, 1231–1238. [Google Scholar] [CrossRef] [PubMed]
- Baumeister, H.; Maercker, A.; Casey, P. Adjustment disorder with depressed mood. Psychopathology 2009, 42, 139–147. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. World Health Organisation International Statistical Classification of Diseases and Related Health Problems, 11th ed.; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Carta, M.G.; Balestrieri, M.; Murru, A.; Hardoy, M.C. Adjustment Disorder: Epidemiology, diagnosis and treatment. Clin. Prac. Epidemiol. Ment. Health 2009, 5, 15. [Google Scholar] [CrossRef]
- Casey, P.; Bailey, S. Adjustment disorders: The state of the art. World Psychiatry 2011, 10, 11–18. [Google Scholar] [CrossRef]
- Maercker, A.; Brewin, C.R.; Bryant, R.A.; Cloitre, M.; van Ommeren, M.; Jones, L.M.; Humayan, A.; Kagee, A.; Llosa, A.E.; Rousseau, C.; et al. Diagnosis and classification of disorders specifically associated with stress: Proposals for ICD-11. World Psychiatry 2013, 12, 198–206. [Google Scholar] [CrossRef]
- Zelviene, P.; Kazlauskas, E.; Eimontas, J.; Maercker, A. Adjustment disorder: Empirical study of a new diagnostic concept for ICD-11 in the general population in Lithuania. Eur. Psychiatry 2017, 40, 20–25. [Google Scholar] [CrossRef]
- Lorenz, L.; Hyland, P.; Maercker, A.; Ben-Ezra, M. An empirical assessment of adjustment disorder as proposed for ICD-11 in a general population sample of Israel. J. Anxiety Disord. 2018, 54, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, L.; Hyland, P.; Perkonigg, A.; Maercker, A. Is adjustment disorder unidimensional or multidimensional? Implications for ICD-11. Int. J. Methods Psychiatr. Res. 2018, 27, e1591. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, M.L.; Alkemade, N.; Nickerson, A.; Creamer, M.; McFarlane, A.C.; Silove, D.; Bryant, R.A.; Forbes, D. Impact of the diagnostic changes to post-traumatic stress disorder for DSM-5 and the proposed changes to ICD-11. Br. J. Psychiatry 2014, 205, 230–235. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, M.L.; Alkamade, N.; Forbes, D. Is Australia in the post-traumatic stress disorder petri dish? Aust. N. Z. J. Psychiatry 2015, 49, 315–316. [Google Scholar] [CrossRef] [PubMed]
- Kazlauskas, E.; Zelviene, P.; Lorenz, L.; Quero, S.; Maercker, A. A scoping review of ICD-11 adjustment disorder research. Eur. J. Psychotraumtol. 2017, 8, 1421819. [Google Scholar] [CrossRef] [PubMed]
- Bonanno, G.A.; Galea, S.; Bucciarelli, A.; Vlahov, D. Psychological resilience after disaster: New York City in the aftermath of the September 11th terrorist attack. Psychol. Sci. 2006, 17, 181–186. [Google Scholar] [CrossRef] [PubMed]
- Bonanno, G.A.; Mancini, A.D.; Horton, J.L.; Powell, T.M.; LeardMann, C.A.; Boyko, E.J.; Wells, T.S.; Hooper, T.I.; Gackstetter, G.D.; Smith, T.C. Trajectories of trauma symptoms and resilience in deployed US military service members: Prospective cohort study. Br. J. Psychiatry 2012, 200, 317–323. [Google Scholar] [CrossRef]
- Bryant, R.A.; Nickerson, A.; Creamer, M.; O’Donnell, M.; Forbes, D.; Galatzer-Levy, I.; McFarlane, A.C.; Silove, D. Trajectory of post-traumatic stress following traumatic injury: 6-year follow-up. Br. J. Psychiatry 2015, 206, 417–423. [Google Scholar] [CrossRef]
- deRoon-Cassini, T.A.; Mancini, A.D.; Rusch, M.D.; Bonanno, G.A. Psychopathology and resilience following traumatic injury: A latent growth mixture model analysis. Rehabil. Psychol. 2010, 55, 1. [Google Scholar] [CrossRef]
- Fink, D.S.; Lowe, S.; Cohen, G.H.; Sampson, L.A.; Ursano, R.J.; Gifford, R.K.; Fullerton, C.S.; Galea, S. Trajectories of posttraumatic stress symptoms after civilian or deployment traumatic event experiences. Psychol. Trauma 2017, 9, 138. [Google Scholar] [CrossRef]
- Lam, W.W.; Bonanno, G.A.; Mancini, A.D.; Ho, S.; Chan, M.; Hung, W.K.; Or, A.; Fielding, R. Trajectories of psychological distress among Chinese women diagnosed with breast cancer. Psychooncology 2010, 19, 1044–1051. [Google Scholar] [CrossRef] [PubMed]
- Santiago, P.N.; Ursano, R.J.; Gray, C.L.; Pynoos, R.S.; Spiegel, D.; Lewis-Fernandez, R.; Friedman, M.J.; Fullerton, C.S. A systematic review of PTSD prevalence and trajectories in DSM-5 defined trauma exposed populations: Intentional and non-intentional traumatic events. PLoS ONE 2013, 8, e59236. [Google Scholar] [CrossRef] [PubMed]
- Weathers, F.W.; Bovin, M.J.; Lee, D.J.; Sloan, D.M.; Schnurr, P.P.; Kaloupek, D.G.; Keane, T.M.; Marx, B.P. The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5): Development and initial psychometric evaluation in military veterans. Psychol. Assess 2018, 30, 383–395. [Google Scholar] [CrossRef] [PubMed]
- Bryant, R.A.; O’Donnell, M.L.; Creamer, M.; McFarlane, A.C.; Silove, D. A multisite analysis of the fluctuating course of posttraumatic stress disorder. JAMA Psychiatry 2013, 70, 839–846. [Google Scholar] [CrossRef] [PubMed]
- Casey, P.; Jabbar, F.; O’Leary, E.; Doherty, A.M. Suicidal behaviours in adjustment disorder and depressive episode. J. Affect. Disord. 2015, 174, 441–446. [Google Scholar] [CrossRef]
- Greenberg, W.M.; Rosenfeld, D.N.; Ortega, E.A. Adjustment disorder as an admission diagnosis. Am. J. Psychiatry 1995, 152, 459. [Google Scholar] [CrossRef]
- Kryzhanovskaya, L.; Canterbury, R. Suicidal behaviour in patients with adjustment disorders. Crisis 2001, 22, 125–131. [Google Scholar] [CrossRef]
- Lewis, G.; Pelosi, A.J.; Araya, R.; Dunn, G. Measuring psychiatric disorder in the community: A standardized assessment for use by lay interviewers. Psychol. Med. 1992, 22, 465–486. [Google Scholar] [CrossRef]
- Kessler, R.C.; Üstün, T.B. The world mental health (WMH) survey initiative version of the world health organization (WHO) composite international diagnostic interview (CIDI). Int. J. Methods Psychiatr. Res. 2004, 13, 93–121. [Google Scholar] [CrossRef]
- First, M.B. Structured Clinical Interview for the DSM (SCID). In The Encyclopedia of Clinical Psychology; Cautin, R.L., Lilienfeld, S.O., Eds.; American Psychiatric Association Publishing: Philadelphia, PA, USA, 2015; pp. 1–6. [Google Scholar] [CrossRef]
- Sheehan, D.V.; Lecrubier, Y.; Sheehan, K.H.; Amorim, P.; Janavs, J.; Weiller, E.; Hergueta, T.; Baker, R.; Dunbar, G.C. The Mini-International Neuropsychiatric Interview (MINI): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 1998, 59, 22–23. [Google Scholar]
- Maercker, A.; Lorenz, L. Adjustment disorder diagnosis: Improving clinical utility. World J. Biol. Psychiatry 2018, 19, S3–S13. [Google Scholar] [CrossRef] [PubMed]
- Cornelius, L.R.; Brouwer, S.; de Boer, M.R.; Groothoff, J.W.; van der Klink, J.J. Development and validation of the Diagnostic Interview Adjustment Disorder (DIAD). Int. J. Methods Psychiatr. Res. 2014, 23, 192–207. [Google Scholar] [CrossRef] [PubMed]
- Maercker, A.; Einsle, F.; Köllner, V. Adjustment disorders as stress response syndromes: A new diagnostic concept and its exploration in a medical sample. Psychopathology 2007, 40, 135–146. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, L.; Bachem, R.; Maercker, A. The adjustment disorder–new module 20 as a screening instrument: Cluster analysis and cut-off values. Int. J. Occup. Environ. Med. 2016, 7, 215–220. [Google Scholar] [CrossRef] [PubMed]
- Bachem, R.; Perkonigg, A.; Stein, D.J.; Maercker, A. Measuring the ICD-11 adjustment disorder concept: Validity and sensitivity to change of the Adjustment Disorder–New Module questionnaire in a clinical intervention study. Int. J. Methods Psychiatr. Res. 2017, 26, e1545. [Google Scholar] [CrossRef] [PubMed]
- Ben-Ezra, M.; Mahat-Shamir, M.; Lorenz, L.; Lavenda, O.; Maercker, A. Screening of adjustment disorder: Scale based on the ICD-11 and the Adjustment Disorder New Module. J. Psychiatr. Res. 2018, 103, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Kazlauskas, E.; Gegieckaite, G.; Maercker, A.; Eimontas, J.; Zelviene, P. A brief measure of the International Classification of Diseases-11 adjustment disorder: Investigation of psychometric properties in an adult help-seeking sample. Psychopathology 2018, 1–6. [Google Scholar] [CrossRef]
- O’Donnell, M.L.; Metcalf, O.; Watson, L.; Phelps, A.; Varker, T. A Systematic Review of Psychological and Pharmacological Treatments for Adjustment Disorder in Adults. J. Trauma. Stress 2018, 31, 321–331. [Google Scholar] [CrossRef]
- GRADE Working Group. Grading quality of evidence and strength of recommendations. BMJ 2004, 328, 1490. [Google Scholar] [CrossRef]
- Bachem, R.; Maercker, A. Self-help interventions for adjustment disorder problems: A randomized waiting-list controlled study in a sample of burglary victims. Cogn. Behav. Ther. 2016, 45, 397–413. [Google Scholar] [CrossRef]
- Eimontas, J.; Rimsaite, Z.; Gegieckaite, G.; Zelviene, P.; Kazlauskas, E. Internet-based self-help intervention for ICD-11 adjustment disorder: Preliminary findings. Psychiatr. Q. 2018, 89, 451–460. [Google Scholar] [CrossRef] [PubMed]
- Quero, S.; Molés, M.; Campos, D.; Andreu-Mateu, S.; Baños, R.M.; Botella, C. An adaptive virtual reality system for the treatment of adjustment disorder and complicated grief: 1-year follow-up efficacy data. Clin. Psychol. Psychother. 2019, 26, 204–217. [Google Scholar] [CrossRef] [PubMed]
- Singla, D.R.; Kohrt, B.A.; Murray, L.K.; Anand, A.; Chorpita, B.F.; Patel, V. Psychological treatments for the world: Lessons from low-and middle-income countries. Annu. Rev. Clin. Psychol. 2017, 13, 149–181. [Google Scholar] [CrossRef] [PubMed]
- Gibson, K.; Forbes, D.; O’Donnell, M.L. Skills for Life Adjustment and Resilience (SOLAR)–A pilot study in Tuvalu. In Proceedings of the 7th World Congress of Asian Psychiatry, Sydney, Australia, 22 February 2019. [Google Scholar]
- O’Donnell, M.L.; Lau, W.; Fredrickson, J.; Bryant, R.A.; Bisson, J.; Burke, S.; Busuttil, W.; Coghlan, A.; Creamer, M.; Gray, D.; et al. SOLAR: The Skills fOr Life Adjustment and Resilience Program: A brief intervention to promote adjustment following disaster. In Proceedings of the 34th meeting of the International Society for Traumatic Stress Studies, Washington DC, USA, 9 November 2018. [Google Scholar]
| DSM-5 | ICD-11 |
|---|---|
| A. Onset of emotional or behavioural symptoms must occur in response to identifiable stressor, and within 3 months of the stressor. | 1. Presence of an identifiable psychosocial stressor(s). Symptoms emerge within 1 month of the stressor. |
| B. These symptoms are clinically significant, marked by: | 2. Preoccupation related to the stressor or its consequences in the form of at least one of the following: |
| - Distress that is disproportionate to the severity or intensity of the stressor, taking into account contextual and cultural factors. | (a) excessive worry about the stressor (b) recurrent and distressing thoughts about the stressor (c) constant rumination about the implications of the stressor. |
| or | |
| - Significant impairments in social, occupational or other domains of functioning. | 3. Failure to adapt to the stressor that causes significant impairment in personal, family, social, educational, occupational or other important areas of functioning |
| C. The disturbance does not meet the diagnostic criteria for another mental disorder, and is not an exacerbation of a pre-existing disorder. | 4. Symptoms are not of a sufficient specificity or severity to justify diagnosis of another mental or behavioural disorder. |
| D. The symptoms do not represent normal bereavement. | |
| E. Symptoms do not last for more than six additional months after the stressor or its consequences have been resolved. | 5. Symptoms typically resolve within 6 months, unless the stressor persists for a longer duration |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
O’Donnell, M.L.; Agathos, J.A.; Metcalf, O.; Gibson, K.; Lau, W. Adjustment Disorder: Current Developments and Future Directions. Int. J. Environ. Res. Public Health 2019, 16, 2537. https://doi.org/10.3390/ijerph16142537
O’Donnell ML, Agathos JA, Metcalf O, Gibson K, Lau W. Adjustment Disorder: Current Developments and Future Directions. International Journal of Environmental Research and Public Health. 2019; 16(14):2537. https://doi.org/10.3390/ijerph16142537
Chicago/Turabian StyleO’Donnell, Meaghan L., James A. Agathos, Olivia Metcalf, Kari Gibson, and Winnie Lau. 2019. "Adjustment Disorder: Current Developments and Future Directions" International Journal of Environmental Research and Public Health 16, no. 14: 2537. https://doi.org/10.3390/ijerph16142537
APA StyleO’Donnell, M. L., Agathos, J. A., Metcalf, O., Gibson, K., & Lau, W. (2019). Adjustment Disorder: Current Developments and Future Directions. International Journal of Environmental Research and Public Health, 16(14), 2537. https://doi.org/10.3390/ijerph16142537





