The Impact of a Multi-Level Multi-Component Childhood Obesity Prevention Intervention on Healthy Food Availability, Sales, and Purchasing in a Low-Income Urban Area
Abstract
1. Introduction
- (1)
- To evaluate the impact of the BHCK multilevel intervention on sales of promoted foods at the wholesaler level.
- (2)
- To evaluate the impact of BHCK on stocking and sales of promoted foods in corner stores and carryouts.
- (3)
- To assess the impact of BHCK on adult caregiver and child healthy food purchasing.
2. Materials and Methods
2.1. Setting and Study Design
2.2. Measurements
2.2.1. Wholesaler
2.2.2. Corner Stores & Carryouts Stocking and Sales
2.2.3. Child-Caregiver Dyads
2.2.4. Data Collection and Management
2.3. Statistical Analysis
2.3.1. Wholesaler
2.3.2. Corner Stores and Carryouts
2.3.3. Child-Caregiver Dyads
3. Results
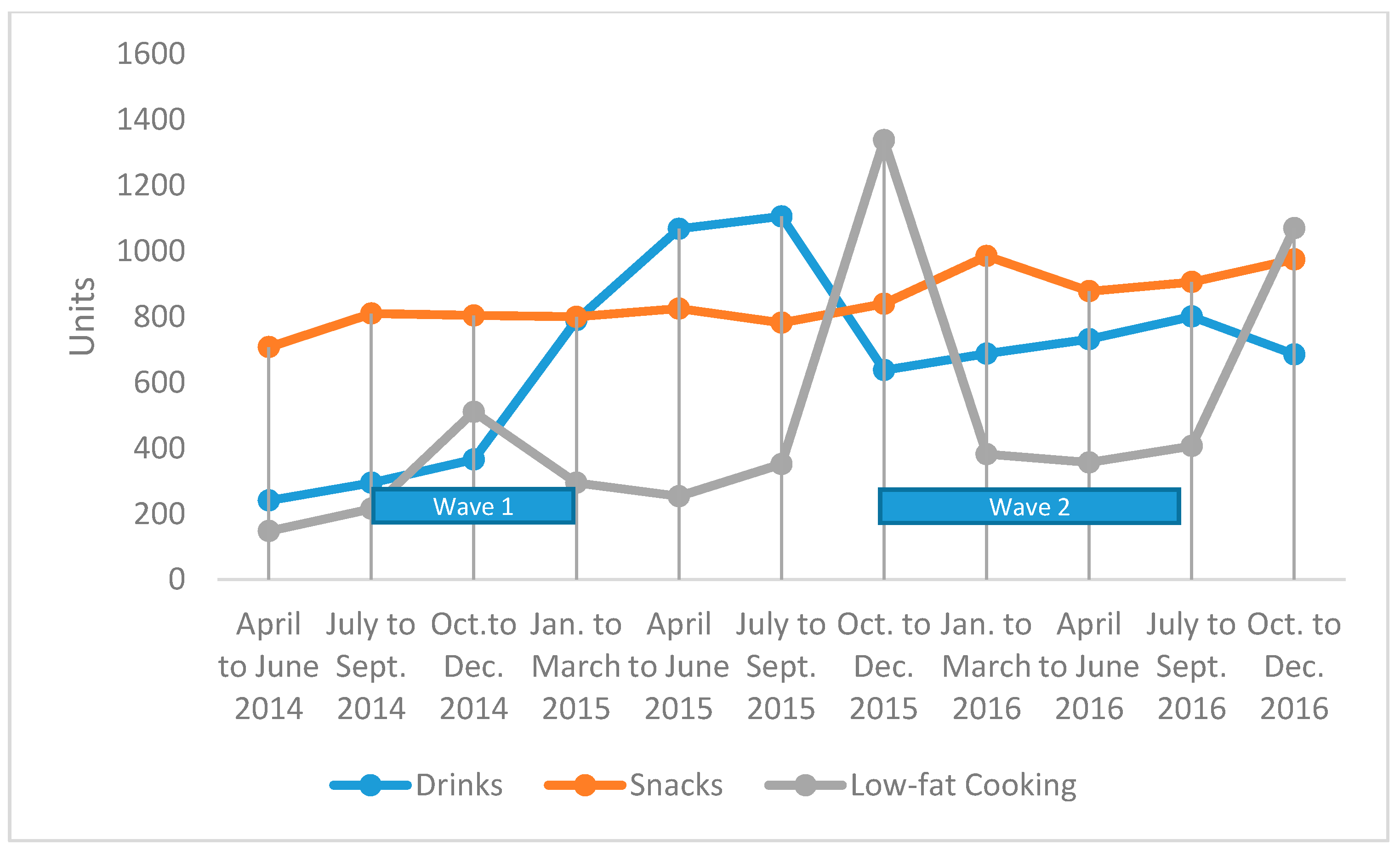
3.1. Impact on Sales of Promoted Foods at the Wholesaler Level
3.2. Impact on Stocking and Sales of Promoted Foods in Corner Stores and Carryouts
3.3. Association between Exposure to BHCK Corner Store and Carryout Intervention and Change in Purchasing of Promoted Foods and Beverages among Adult Caregivers
3.4. Association between Exposure to BHCK Corner Store and Carryout Intervention and Change in Purchasing Promoted Foods and Beverages among Children
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Hurt, R.T.; Kulisek, C.; Buchanan, L.A.; McClave, S.A. The obesity epidemic: Challenges, health initiatives, and implications for gastroenterologists. Gastroenterol. Hepatol. 2010, 6, 780–792. [Google Scholar] [CrossRef] [PubMed]
- Biro, F.M.; Wien, M. Childhood obesity and adult morbidities. Am. J. Clin. Nutr. 2010, 91, 1499S–1505S. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Cai, L.; Wu, Y.; Wilson, R.F.; Weston, C.; Fawole, O.; Bleich, S.N.; Cheskin, L.J.; Showell, N.N.; Lau, B.D.; et al. What childhood obesity prevention programmes work? A systematic review and meta-analysis. Obes. Rev. 2015, 16, 547–565. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Mui, Y.; Adam, A.; Lin, S.; Kharmats, A.; Igusa, T.; Lee, B.Y. Incorporating systems science principles into the development of obesity prevention interventions: Principles, benefits, and challenges. Curr. Obes. Rep. 2015, 4, 174–181. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.T.; Drewnosksi, A.; Kumanyika, S.; Glass, T.A. A systems-oriented multilevel framework for addressing obesity in the 21st century. Prev. Chronic Dis. 2009, 6, A82. [Google Scholar] [PubMed]
- Economos, C.D.; Hyatt, R.R.; Must, A.; Goldberg, J.P.; Kuder, J.; Naumova, E.N.; Collins, J.J.; Nelson, M.E. Shape up somerville two-year results: A community-based environmental change intervention sustains weight reduction in children. Prev. Med. 2013, 57, 322–327. [Google Scholar] [CrossRef] [PubMed]
- Shin, A.; Surkan, P.J.; Coutinho, A.J.; Suratkar, S.R.; Campbell, R.K.; Rowan, M.; Sharma, S.; Dennisuk, L.A.; Karlsen, M.; Gass, A.; et al. Impact of baltimore healthy eating zones: An environmental intervention to improve diet among African American youth. Health Educ. Behav. 2015, 42, 97–105. [Google Scholar] [CrossRef] [PubMed]
- Foster, G.D.; Sherman, S.; Borradaile, K.E.; Grundy, K.M.; vander Veur, S.S.; Nachmani, J.; Karpyn, A.; Kumanyika, S.; Shults, J. A policy-based school intervention to prevent overweight and obesity. Pediatrics 2008, 121, e794–e802. [Google Scholar] [CrossRef] [PubMed]
- Turrell, G.; Blakely, T.; Patterson, C.; Oldenburg, B. A multilevel analysis of socioeconomic (small area) differences in household food purchasing behaviour. J. Epidemiol. Community Health 2004, 58, 208–215. [Google Scholar] [CrossRef] [PubMed]
- Glanz, K.; Sallis, J.F.; Saelens, B.E.; Frank, L.D. Healthy nutrition environments: Concepts and measures. Am. J. Health Promot. 2005, 19, 330–333. [Google Scholar] [CrossRef] [PubMed]
- Sallis, J.F.; Glanz, K. Physical activity and food environments: Solutions to the obesity epidemic. Milbank Q. 2009, 87, 123–154. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Anderson Steeves, E.; Mui, Y.; Kharmats, A.Y.; Hopkins, L.C.; Dennis, D. B’more Healthy Communities for Kids: Design of a multi-level intervention for obesity prevention for low-income African American children. BMC Public Health 2014, 14, 942. [Google Scholar] [CrossRef] [PubMed]
- Buczynski, A.B.; Freishtat, H.; Buzogany, S. Baltimore Food Environment: 2015 Report; The Johns Hopkins Center for a Livable Future: Baltimore, MD, USA, 2015. [Google Scholar]
- Schwendler, T.; Shipley, C.; Budd, N.; Trude, A.; Surkan, P.J.; Anderson Steeves, E.; de Morais Sato, P.; Eckmann, T.; Loh, H.; Gittelsohn, J. Development and implementation: B’more healthy communities for kids store and wholesaler intervention. Health Promot. Pract. 2017, 18, 822–832. [Google Scholar] [CrossRef] [PubMed]
- Dodson, J.L.; Hsiao, Y.-C.; Kasat-Shors, M.; Murray, L.; Nguyen, N.K.; Richards, A.K.; Gittelsohn, J. Formative research for a healthy diet intervention among inner-city adolescents: The importance of family, school and neighborhood environment. Ecol. Food Nutr. 2009, 48, 39–58. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Suratkar, S.; Song, H.; Sacher, S.; Rajan, R.; Rasooly, I.R.; Bednarek, E.; Sharma, S.; Anliker, J.A. Process evaluation of baltimore healthy stores: A pilot health intervention program with supermarkets and corner stores in Baltimore city. Health Promot. Pract. 2010, 11, 723–732. [Google Scholar] [CrossRef] [PubMed]
- Loh, H.; Schwendler, T.; Gittelsohn, J.; Al, E. Implementation evaluation of social media strategies within multi-level B’more Healthy Communities for Kids childhood obesity prevention intervention. Obes. J. 2016. under review. [Google Scholar]
- Sato, P.M.; Steeves, E.A.; Carnell, S.; Cheskin, L.J.; Trude, A.C.; Shipley, C.; Mejía Ruiz, M.J.; Gittelsohn, J. A youth mentor-led nutritional intervention in urban recreation centers: A promising strategy for childhood obesity prevention in low-income neighborhoods. Health Educ. Res. 2016, 31, 195–206. [Google Scholar] [CrossRef] [PubMed]
- Trude, A.; Anderson Steeves, E.; Shipley, C.; Surkan, P.; Sato, P.; Estep, T.; Clanton, S.; Lachenmayr, L.; Gittelsohn, J. A youth-leader program in Baltimore city recreation centers: Lessons learned and applications. Health Promot. Pract. 2017. [Google Scholar] [CrossRef] [PubMed]
- Glanz, K.; Sallis, J.F.; Saelens, B.E.; Frank, L.D. Nutrition environment measures survey in stores (nems-s): Development and evaluation. Am. J. Prev. Med. 2007, 32, 282–289. [Google Scholar] [CrossRef] [PubMed]
- Franco, M.; Diez Roux, A.V.; Glass, T.A.; Caballero, B.; Brancati, F.L. Neighborhood characteristics and availability of healthy foods in Baltimore. Am. J. Prev. Med. 2008, 35, 561–567. [Google Scholar] [CrossRef] [PubMed]
- Song, H.-J.; Gittelsohn, J.; Kim, M.; Suratkar, S.; Sharma, S.; Anliker, J. A corner store intervention in a low-income urban community is associated with increased availability and sales of some healthy foods. Public Health Nutr. 2009, 12, 2060–2067. [Google Scholar] [CrossRef] [PubMed]
- Vedovato, G.M.; Surkan, P.J.; Jones-Smith, J.; Steeves, E.A.; Han, E.; Trude, A.C.; Kharmats, A.Y.; Gittelsohn, J. Food insecurity, overweight and obesity among low-income African-American families in Baltimore city: Associations with food-related perceptions. Public Health Nutr. 2015, 19, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Trude, A.; Kharmats, A.; Hurley, K.; Anderson Steeves, E.; Talegawkar, S.; Gittelsohn, J. Household and individual-level determinants of fruit, vegetable, and fiber intake among low-income urban African American youth. BMC Public Health 2016, 16, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Kim, E.M.; He, S.; Pardilla, M. A food store-based environmental intervention is associated with reduced bmi and improved psychosocial factors and food-related behaviors on the navajo nation. J. Nutr. 2013, 143, 1494–1500. [Google Scholar] [CrossRef] [PubMed]
- Bodor, J.N.; Ulmer, V.M.; Dunaway, L.F.; Farley, T.A.; Rose, D. The rationale behind small food store interventions in low-income urban neighborhoods: Insights from new orleans. J. Nutr. 2010, 140, 1185–1188. [Google Scholar] [CrossRef] [PubMed]
- Dannefer, R.; Williams, D.A.; Baronberg, S.; Silver, L. Healthy bodegas: Increasing and promoting healthy foods at corner stores in New York city. Am. J. Public Health 2012, 102, e27–e31. [Google Scholar] [CrossRef] [PubMed]
- Eisenmann, J.C.; Gentile, D.A.; Welk, G.J.; Callahan, R.; Strickland, S.; Walsh, M.; Walsh, D.A. Switch: Rationale, design, and implementation of a community, school, and family-based intervention to modify behaviors related to childhood obesity. BMC Public Health 2008, 8, 223. [Google Scholar] [CrossRef] [PubMed]
- Gentile, D.A.; Welk, G.; Eisenmann, J.C.; Reimer, R.A.; Walsh, D.A.; Russell, D.W.; Callahan, R.; Walsh, M.; Strickland, S.; Fritz, K. Evaluation of a multiple ecological level child obesity prevention program: Switch what you do, view, and chew. BMC Med. 2009, 7, 49. [Google Scholar] [CrossRef] [PubMed]
- Lee-Kwan, S.H.; Bleich, S.N.; Kim, H.; Colantuoni, E.; Gittelsohn, J. Environmental intervention in carryout restaurants increases sales of healthy menu items in a low-income urban setting. Am. J. Health Promot. 2015, 29, 357–364. [Google Scholar] [CrossRef] [PubMed]
- Lee-Kwan, S.H.; Yong, R.; Bleich, S.N.; Kwan, N.H.; Park, J.H.; Lawrence, R.; Gittelsohn, J. Carry-out restaurant intervention increases purchases of healthy food. J. Hunger Environ. Nutr. 2015, 10, 456–466. [Google Scholar] [CrossRef]
- Song, H.-J.; Gittelsohn, J.; Kim, M.; Suratkar, S.; Sharma, S.; Anliker, J. Korean American storeowners’ perceived barriers and motivators for implementing a corner store-based program. Health Promot. Pract. 2011, 12, 472–482. [Google Scholar] [CrossRef] [PubMed]
- Lawman, H.G.; vander Veur, S.; Mallya, G.; McCoy, T.A.; Wojtanowski, A.; Colby, L.; Sanders, T.A.; Lent, M.R.; Sandoval, B.A.; Sherman, S.; et al. Changes in quantity, spending, and nutritional characteristics of adult, adolescent and child urban corner store purchases after an environmental intervention. Prev. Med. 2015, 74, 81–85. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Dennisuk, L.; Christiansen, K.; Bhimani, R.; Johnson, A.; Alenxander, E.; Lee, M.; Lee, S.; Rowan, M.; Coutinho, A. Development and implementation of Baltimore Healthy Eating Zones: A youth-centered intervention trial to improve the food environment around recreation centers in Baltimore city. Health Educ. Res. 2011, 28, 732–744. [Google Scholar] [CrossRef] [PubMed]
- Gittelsohn, J.; Song, H.-J.; Suratkar, S.; Kumar, M.B.; Henry, E.G.; Sharma, S.; Mattingly, M.; Anliker, J.A. An urban food store intervention positively affects food-related psychosocial variables and food behaviors. Health Educ. Behav. 2010, 37, 390–402. [Google Scholar] [CrossRef] [PubMed]
| Wave | Child-Caregiver Dyad Data Collection | Wave 1 Implementation (14 Zones) | Child-Caregiver Dyad Data Collection (Wave 1 Post and Wave 2 Baseline) | Wave 2 Implementation (14 Zones) | Child-Caregiver Dyad Data Collection | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Phase | Phase 1 Beverages | Phase 2 Snacks | Phase 3 Cooking | Phase 1 Snacks | Phase 2 Cooking | Phase 3 Beverages | Phase 4 Review | |||
| Promoted Products’ Example | 1. Water 2. Sugar free tea mixes 3. Low-sugar fruit drinks | 1. Low-fat yogurt 2. Low-fat popcorn 3. Fresh fruits 4. Fresh vegetables | 1. Low-sugar cereal 2. 100% whole wheat bread 3. Fresh/frozen vegetables | 1. Low-fat yogurt 2. Low-fat popcorn 3. Fresh fruits 4. Fresh vegetables | 1. Low-sugar cereal 2. 100% whole wheat bread 3. Fresh/frozen vegetables | 1. Water 2. Sugar free tea mixes 3. Low-sugar fruit drinks | 1. Low-fat yogurt 2. Fresh/frozen vegetables 3. Small fresh vegetables bags | |||
| Start date | June 2013 | July 2014 | September 2014 | November 2014 | April 2015 | December 2015 | March 2016 | May 2016 | June 2016 | August 2016 |
| End date | June 2014 | August 2014 | October 2014 | February 2015 | November 2015 | February 2016 | April 2016 | June 2016 | July 2016 | January 2017 |
| Baseline Sociodemographic | Intervention | Comparison | ||
|---|---|---|---|---|
| n | Mean (SD) or % | n | Mean (SD) or % | |
| Child’s Characteristics | ||||
| Age 1 | 199 | 11.7 (1.4) | 186 | 11.9 (1.6) |
| Sex (female) 2 | 109 | 54% | 90 | 60% |
| Caregiver’s Characteristics | ||||
| Age 1 | 197 | 39.4 (1.2) | 188 | 40.5 (9.8) |
| Sex (female) 2 | 187 | 94.4% | 170 | 90.4% |
| Race (African American) 2 | 185 | 93.4% | 174 | 93.0% |
| Household’s Characteristics | ||||
| Household Size 1 | 198 | 4.5 (1.5) | 188 | 4.5 (1.6) |
| SNAP 2 | 133 | 70.7% | 141 | 71.2% |
| WIC 2 | 46 | 23.2% | 44 | 23.4% |
| Average Change in Corner Store HFAI by Treatment Group | |||
|---|---|---|---|
| Change in HFAI | Comparison (n = 24) | Intervention (n = 26) | p-Value 1 |
| Mean (±SD) | Mean (±SD) | ||
| Total score | 1.67 (5.35) | 5.65 (4.95) | 0.01 |
| Beverage subscore 2 | 0.17 (1.09) | 0.92 (1.16) | 0.02 |
| Snack subscore 3 | 0 (1.10) | 1.19 (1.81) | 0.01 |
| Cooking subscore 4 | 1.5 (4.35) | 3.54 (3.87) | 0.08 |
| Average Change in Corner Store HFAI by Wave and Treatment Groups | |||
| Total Score | |||
| Wave 1 | 5.56 (4.28) | 7.86 (4.00) | 0.20 |
| Wave 2 | −0.67 (4.59) | 3.08 (4.83) | 0.05 |
| Beverage subscore 2 | |||
| Wave 1 | 0.56 (1.13) | 0.86 (1.03) | 0.52 |
| Wave 2 | −0.07 (1.03) | 1.0 (1.35) | 0.03 |
| Snack subscore 3 | |||
| Wave 1 | 0.77 (0.97) | 1.64 (1.45) | 0.13 |
| Wave 2 | −0.47 (0.92) | 0.67 (2.10) | 0.07 |
| Cooking subscore 4 | |||
| Wave 1 | 4.22 (3.31) | 5.36 (3.65) | 0.46 |
| Wave 2 | −0.13 (4.16) | 1.42 (3.03) | 0.29 |
| Change in Food Purchasing Behavior by Exposure Quartiles | Combined Exposure Score | Corner Store Score | Carryout Score | |||
|---|---|---|---|---|---|---|
| IRR (Robust SE) | 95% CI | IRR (Robust SE) | 95% CI | IRR (Robust SE) | 95% CI | |
| Healthy Food Purchasing 2 | ||||||
| Very LowExposure | Reference | Reference | Reference | |||
| Low Exposure | 1.07 (0.21) | 0.73; 1.58 | 0.97 (0.19) | 0.65; 1.45 | 1.07 (0.21) | 0.89; 1.34 |
| Medium Exposure | 0.71 (0.16) | 0.45; 1.10 | 0.77 (0.17) | 0.50; 1.20 | 0.74 (0.17) | 0.95; 1.43 |
| High Exposure | 0.92 (0.19) | 0.61; 1.37 | 0.99 (0.20) | 0.67; 1.48 | 0.93 (0.19) | 1.00; 1.47 |
| Healthy Food Purchasing 2 among Intervention | ||||||
| Very Low Exposure | Reference | Reference | Reference | |||
| Low Exposure | 0.59 (0.24) | 0.25; 1.33 | 0.54 (0.23) | 0.23; 1.24 | 0.67 (0.27) | 0.30; 1.48 |
| Medium Exposure | 0.54 (0.18) | 0.27; 1.07 | 0.51 (0.18) | 0.24; 1.04 | 0.56 (0.20) | 0.27; 1.12 |
| High Exposure | 0.67 (0.22) | 0.36; 1.27 | 0.80 (0.25) | 0.43; 1.51 | 0.70 (0.23) | 0.37; 1.33 |
| Healthy Food Purchasing 2 among Comparison | ||||||
| Very Low Exposure | Reference | Reference | Reference | |||
| Low Exposure | 1.33 (0.30) | 0.85; 2.07 | 1.25 (0.29) | 0.85; 1.29 | 1.30 (0.30) | 0.82; 2.05 |
| Medium Exposure | 0.87 (0.31) | 0.43; 1.75 | 1.18 (0.32) | 0.56; 1.11 | 0.97 (0.31) | 052; 1.81 |
| High Exposure | 1.17 (0.37) | 0.63; 2.17 | 1.07 (0.36) | 0.32; 1.05 | 1.23 (0.38) | 0.66; 2.27 |
| Change in Food Purchasing Behavior by Exposure Quartiles | Combined Exposure Score | Corner Store Score | Carryout Score | |||
|---|---|---|---|---|---|---|
| IRR (Robust SE) | 95% CI | IRR (Robust SE) | 95% CI | IRR (Robust SE) | 95% CI | |
| Healthy Food Purchasing 2 | ||||||
| Very Low Exposure | Reference | Reference | Reference | |||
| Low Exposure | 1.12 (0.12) | 0.92; 1.40 | 1.15 (0.11) | 0.94; 1.41 | 1.10 (0.11) | 0.89; 1.34 |
| Medium Exposure | 1.23 (0.12) | 1.01; 1.50 | 1.14 (0.12) | 0.94; 1.41 | 1.17 (0.12) | 0.95; 1.43 |
| High Exposure | 1.24 (0.12) | 1.02; 1.52 | 1.22 (0.12) | 1.01; 1.48 | 1.21 (0.12) | 1.00; 1.47 |
| Healthy Food Purchasing 2 among Intervention | ||||||
| Very Low Exposure | Reference | Reference | Reference | |||
| Low Exposure | 2.36 (0.74) | 1.27; 4.38 | 2.15 (0.63) | 1.21; 3.85 | 1.96 (0.57) | 1.10; 3.49 |
| Medium Exposure | 2.72 (0.82) | 1.51; 4.93 | 2.38 (0.67) | 1.37; 4.13 | 2.29 (0.64) | 1.32; 3.95 |
| High Exposure | 2.81 (0.83) | 1.56; 5.04 | 2.51 (0.70) | 1.45; 4.34 | 2.35 (0.64) | 1.37; 4.03 |
| Healthy Food Purchasing 2 among Comparison | ||||||
| Very Low Exposure | Reference | Reference | Reference | |||
| Low Exposure | 0.96 (0.11) | 0.77; 1.21 | 1.05 (0.11) | 0.85; 1.29 | 1.01 (0.11) | 0.81; 1.25 |
| Medium Exposure | 0.92 (0.14) | 0.68; 1.23 | 0.79 (0.14) | 0.56; 1.11 | 0.84 (0.13) | 0.62; 1.15 |
| High Exposure | 0.52 (0.17) | 0.27; 1.01 | 0.58 (0.17) | 0.32; 1.05 | 0.57 (0.18) | 0.30; 1.08 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gittelsohn, J.; Trude, A.C.; Poirier, L.; Ross, A.; Ruggiero, C.; Schwendler, T.; Anderson Steeves, E. The Impact of a Multi-Level Multi-Component Childhood Obesity Prevention Intervention on Healthy Food Availability, Sales, and Purchasing in a Low-Income Urban Area. Int. J. Environ. Res. Public Health 2017, 14, 1371. https://doi.org/10.3390/ijerph14111371
Gittelsohn J, Trude AC, Poirier L, Ross A, Ruggiero C, Schwendler T, Anderson Steeves E. The Impact of a Multi-Level Multi-Component Childhood Obesity Prevention Intervention on Healthy Food Availability, Sales, and Purchasing in a Low-Income Urban Area. International Journal of Environmental Research and Public Health. 2017; 14(11):1371. https://doi.org/10.3390/ijerph14111371
Chicago/Turabian StyleGittelsohn, Joel, Angela C. Trude, Lisa Poirier, Alexandra Ross, Cara Ruggiero, Teresa Schwendler, and Elizabeth Anderson Steeves. 2017. "The Impact of a Multi-Level Multi-Component Childhood Obesity Prevention Intervention on Healthy Food Availability, Sales, and Purchasing in a Low-Income Urban Area" International Journal of Environmental Research and Public Health 14, no. 11: 1371. https://doi.org/10.3390/ijerph14111371
APA StyleGittelsohn, J., Trude, A. C., Poirier, L., Ross, A., Ruggiero, C., Schwendler, T., & Anderson Steeves, E. (2017). The Impact of a Multi-Level Multi-Component Childhood Obesity Prevention Intervention on Healthy Food Availability, Sales, and Purchasing in a Low-Income Urban Area. International Journal of Environmental Research and Public Health, 14(11), 1371. https://doi.org/10.3390/ijerph14111371






