Sclerosing Extramedullary Hematopoietic Tumor (SEHT) Mimicking a Malignant Bile Duct Tumor-Case Report and Literature Review
Abstract
:1. Introduction
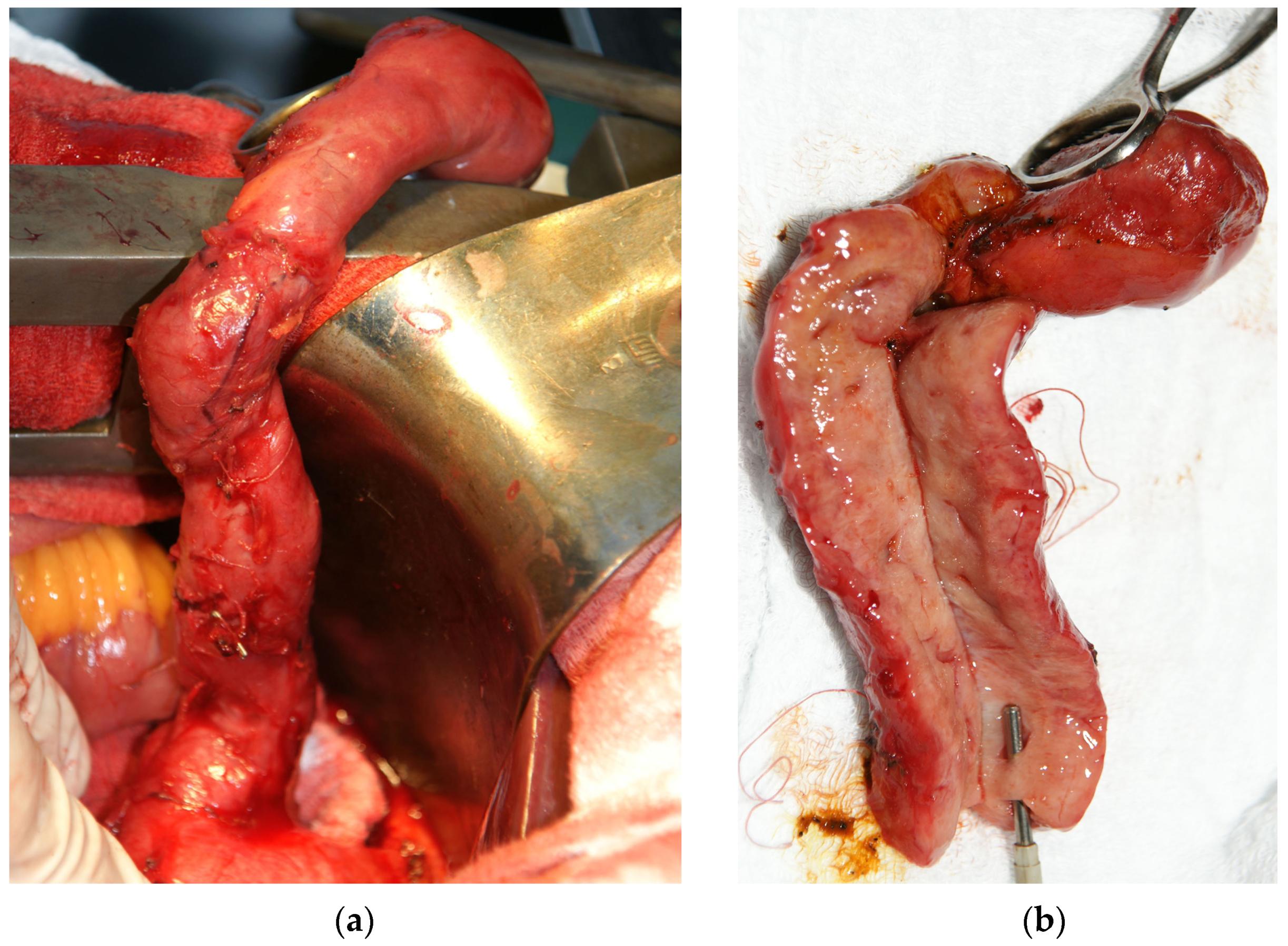
2. Case Presentation
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Beckman, E.N.; Oehrle, J.S. Fibrous hematopoietic tumors arising in agnogenic myeloid metaplasia. Hum. Pathol. 1982, 13, 804–810. [Google Scholar] [CrossRef]
- Yuen, H.K.L.; Mahesh, L.; Tse, R.K.K.; Yau, K.C.; Chan, N.; Lam, D.S.C. Orbital Sclerosing Extramedullary Hematopoietic Tumor. Arch. Ophthalmol. 2005, 123, 689–691. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gu, M.-J. Sclerosing extramedullary hematopoietic tumor presenting as an inguinal mass in a patient with primary myelofibrosis: A diagnostic pitfall. Int. J. Clin. Exp. Pathol. 2015, 8, 3381–3383. [Google Scholar] [PubMed]
- Karaarslan, S.; Nese, N.; Oncel, G.; Ozsan, N.; Akalin, T.; Kaplan, H.; Buyukkececi, F.; Hekimgil, M. Sclerosing Extramedullary Hematopoietic Tumor Mimicking Intra-abdominal Sarcoma. J. Pathol. Transl. Med. 2015, 49, 335–338. [Google Scholar] [CrossRef] [PubMed]
- Deniz, K.; Kahriman, G.; Koçyiğit, I.; Okten, T.; Ünal, A. Sclerosing Extramedullary Hematopoietic Tumor. Turk. J. Hematol. 2017, 35, 209–210. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Castro, E.; Rao, A.; McPhaul, C.M. Sclerosing Extramedullary Hematopoietic Tumor: A Case Report. J. Investig. Med. High Impact Case Rep. 2020, 8. [Google Scholar] [CrossRef] [PubMed]
- Babushok, D.V.; Nelson, E.J.; Morrissette, J.J.D.; Joshi, S.; Palmer, M.B.; Frank, D.; Cambor, C.L.; Hexner, E.O. Myelofibrosis patients can develop extramedullary complications including renal amyloidosis and sclerosing hematopoietic tumor while otherwise meeting traditional measures of ruxolitinib response. Leuk. Lymphoma 2018, 60, 852–855. [Google Scholar] [CrossRef] [PubMed]
- Remstein, E.D.; Kurtin, P.J.; Nascimento, A.G. Sclerosing Extramedullary Hematopoietic Tumor in Chronic Myeloproliferative Disorders. Am. J. Surg. Pathol. 2000, 24, 51. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tefferi, A. Primary myelofibrosis: 2012 update on diagnosis, risk stratification, and management. Am. J. Hematol. 2011, 86, 1017–1026. [Google Scholar] [CrossRef] [PubMed]
- Thiele, J.; Kvasnicka, H.M. Myelofibrosis—What’s in a name? Consensus on definition and EUMNET grading. Pathobiology 2007, 74, 89–96. [Google Scholar] [CrossRef]
- Miranda, R.N.; Khoury, J.D.; Medeiros, L.J. Atlas of Lymph Node Pathology; Springer: New York, NY, USA, 2013. [Google Scholar] [CrossRef]
- Sukov, W.R.; Remstein, E.D.; Nascimento, A.G.; Sethi, S.; Lewin, M. Sclerosing extramedullary hematopoietic tumor: Emphasis on diagnosis by renal biopsy. Ann. Diagn. Pathol. 2009, 13, 127–131. [Google Scholar] [CrossRef]
- Kwon, Y.; Yu, E.; Huh, J.; Lee, S.K.; Ro, J.Y. Sclerosing extramedullary hematopoietic tumor involving lesser omentum and ligamentumteres in liver explant. Ann. Diagn. Pathol. 2004, 8, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Luo, H.; Zheng, Y.; Zou, Z.; Niu, T.; Jia, Y.; Zhu, H.; Liu, T.; Wu, Y.; Chang, H.; et al. Low-dose ruxolitinib shows effective in treating myelofibrosis. Ann. Hematol. 2020, 100, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Hanamornroongruang, S.; Neungton, C.; Warnnissorn, M. Extramedullary Hematopoiesis in the Uterine Cervix Associated with Tissue Repair. Case Rep. Obstet. Gynecol. 2013, 2013, 1–4. [Google Scholar] [CrossRef] [Green Version]
- Leblanc, R.E.; Lester, L.; Kwong, B.; Rieger, K.E. JAK2-positive cutaneous myelofibrosis presenting as sclerosing extramedullary hematopoietic tumors on the scalp: Case presentation and review of the literature. J. Cutan. Pathol. 2015, 42, 858–862. [Google Scholar] [CrossRef] [PubMed]
- Gualco, G.; Ojopi, E.B.; Chioato, L.; Cordeiro, D.L.; Negretti, F.; Bacchi, C.E. Postsplenectomy sclerosing extramedullary hematopoietic tumor with unexpected good clinical evolution: Morphologic, immunohistochemical, and molecular analysis of one case and review of the literature. Appl. Immunohistochem. Mol. Morphol. 2010, 18, 291–295. [Google Scholar] [CrossRef] [PubMed]
- Ghazi, N.G.; Bowman, A.M.; Shields, M.D. Bilateral lacrimal system involvement by sclerosing extramedullary hematopoietic tumor. Ophthalmic Plast. Reconstr. Surg. 2006, 22, 296–298. [Google Scholar] [CrossRef] [PubMed]
- Dupriez, B.; Morel, P.; Demory, J.; Lai, J.; Simon, M.; Plantier, I.; Bauters, F. Prognostic factors in agnogenic myeloid metaplasia: A report on 195 cases with a new scoring system [see comments]. Blood 1996, 88, 1013–1018. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reilly, J.; Brindley, L.; Kay, M.; Fielding, S.; Kennedy, A.; Dolan, G.; Smith, A. Bone marrow and serum connective tissue polypeptides in idiopathic myelofibrosis. Clin. Lab. Haematol. 1995, 17. [Google Scholar] [CrossRef] [PubMed]

| Blood Parameter | Value | Laboratory Range |
|---|---|---|
| WBC 1,2 | 28 × 103/µL 3 → 31.3 × 103/µL → 20.9 × 103/µL → 16.6 × 103/µL → 14.1 × 103/µL → 11.3 × 103/µL | 4–9 × 103/µL |
| Lymphocytes | 14 × 103/µL | 1–3.2 × 103/µL |
| Monocytes | 4.7 × 103/µL | 0.2–0.7 × 103/µL |
| Granulocytes | 9.4 × 103/µL | 2.1–6.7 × 103/µL |
| Erythrocytes | 3.64 × 106/µL | 4–5.50 × 106/µL |
| Hemoglobin | 9.1 g/dL 4 | 11.5–15 g/dL |
| Hematocrit | 28.5% | 35–45% |
| MCV 7 | 78.3 Fl 5 | 80–100 fL |
| MHC 8 | 25 pg 6 | 27–32 pg |
| MCHC 9 | 31.9 g/dL | 32–36 g/dL |
| Platelet count | 273 × 103/µL | 150–400 × 103/µL |
| AST 10 | 40 U/L | 5–34 U/L |
| Primary Antibody | IHC Expression | Clone | Company |
|---|---|---|---|
| CD31 | Positive atypical megakaryocytes | CD31-607 | Novocastra |
| CD61 | Positive atypical megakaryocytes | 2F2 | Novocastra |
| MPO 1 | Positive granulocytic precursors; Negative atypical megakaryocytes; | 59A5 (1:100, pH6) | Novocastra |
| PanCK 2 | Negative | AE1/AE3 | Dako/Agilent Technologies |
| EMA 3 | Negative | E29 | Dako/Agilent Technologies |
| SMA 4 | Negative | 1A4 | Dako/Agilent Technologies |
| Desmin | Negative | D33 | Dako/Agilent Technologies |
| Vimentin | Negative | V9 | Dako/Agilent Technologies |
| ALK 5 | Negative | ALK1 | Dako/Agilent Technologies |
| S100 | Negative | Polyclonal | Novocastra |
| CD3 | Negative | Polyclonal | Cell Marque |
| CD10 | Negative | 56C6 | Dako/Agilent Technologies |
| CD15 | Negative | Carb-3 | Dako/Agilent Technologies |
| CD20 | Negative | L26 | Dako/Agilent Technologies |
| CD30 | Negative | Ber-H2 | Dako/Agilent Technologies |
| CD34 | Negative | QBEnd10 | Novocastra |
| CD68 | Negative | PG-M1 | Dako/Agilent Technologies |
| CD117 | Negative | EP110 | Master Diagnostica |
| Ki-67 | <3% | MIB 1 | Dako/Agilent Technologies |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dema, S.; Lazar, F.; Barna, R.; Dobrescu, A.; Dema, A.L.C.; Popa, O.; Ionita, I.; Taban, S.M. Sclerosing Extramedullary Hematopoietic Tumor (SEHT) Mimicking a Malignant Bile Duct Tumor-Case Report and Literature Review. Medicina 2021, 57, 824. https://doi.org/10.3390/medicina57080824
Dema S, Lazar F, Barna R, Dobrescu A, Dema ALC, Popa O, Ionita I, Taban SM. Sclerosing Extramedullary Hematopoietic Tumor (SEHT) Mimicking a Malignant Bile Duct Tumor-Case Report and Literature Review. Medicina. 2021; 57(8):824. https://doi.org/10.3390/medicina57080824
Chicago/Turabian StyleDema, Sorin, Fulger Lazar, Robert Barna, Amadeus Dobrescu, Alis Liliana Carmen Dema, Oana Popa, Ioana Ionita, and Sorina Maria Taban. 2021. "Sclerosing Extramedullary Hematopoietic Tumor (SEHT) Mimicking a Malignant Bile Duct Tumor-Case Report and Literature Review" Medicina 57, no. 8: 824. https://doi.org/10.3390/medicina57080824
APA StyleDema, S., Lazar, F., Barna, R., Dobrescu, A., Dema, A. L. C., Popa, O., Ionita, I., & Taban, S. M. (2021). Sclerosing Extramedullary Hematopoietic Tumor (SEHT) Mimicking a Malignant Bile Duct Tumor-Case Report and Literature Review. Medicina, 57(8), 824. https://doi.org/10.3390/medicina57080824






