The Existence of Periodontal Disease and Subsequent Ocular Diseases: A Population-Based Cohort Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Source
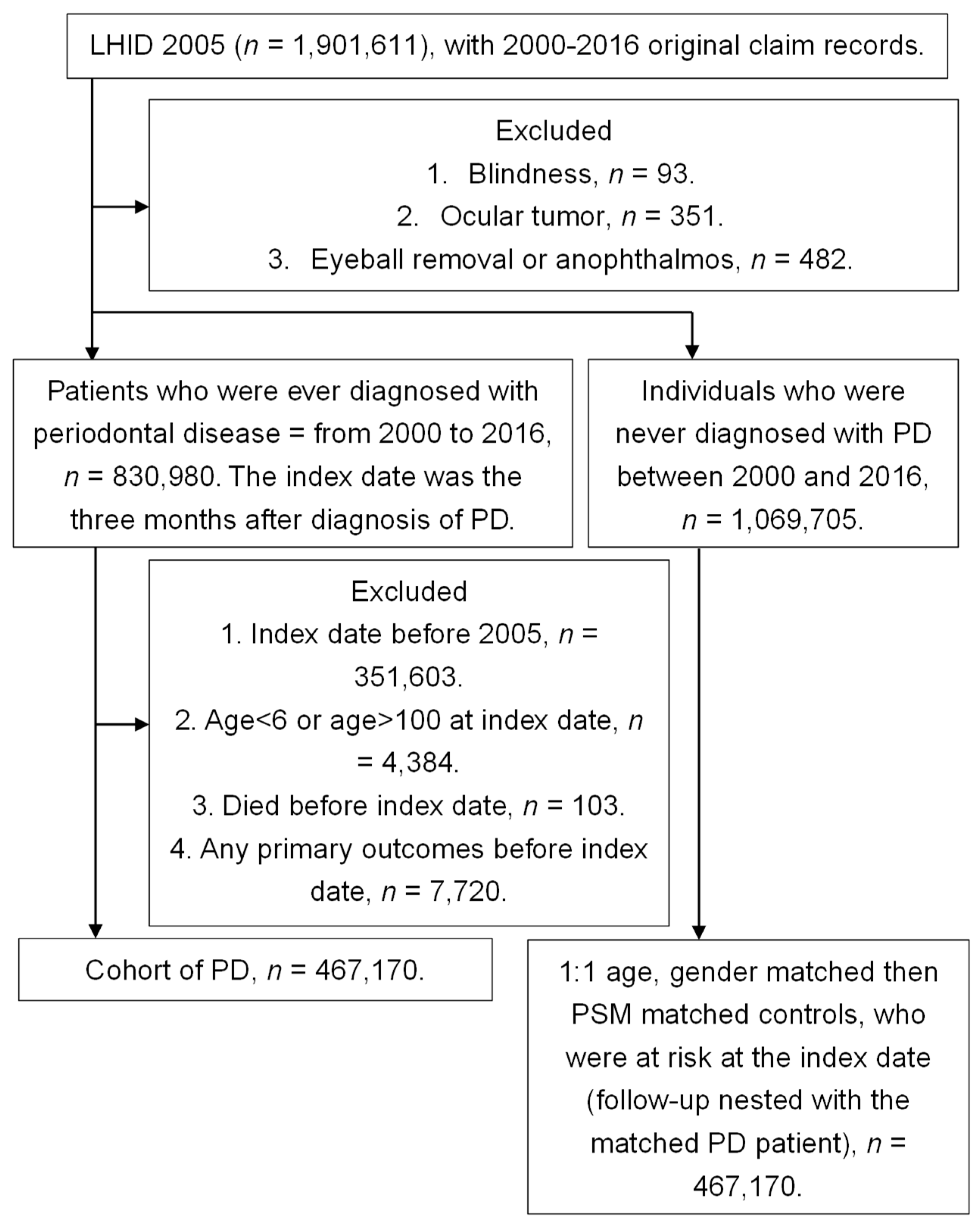
2.2. Subject Selection
2.3. Main Outcome Measurement
2.4. Demographic Variables and Co-Morbidities
2.5. Statistical Analysis
3. Results
3.1. Basic Characteristics of Study Population
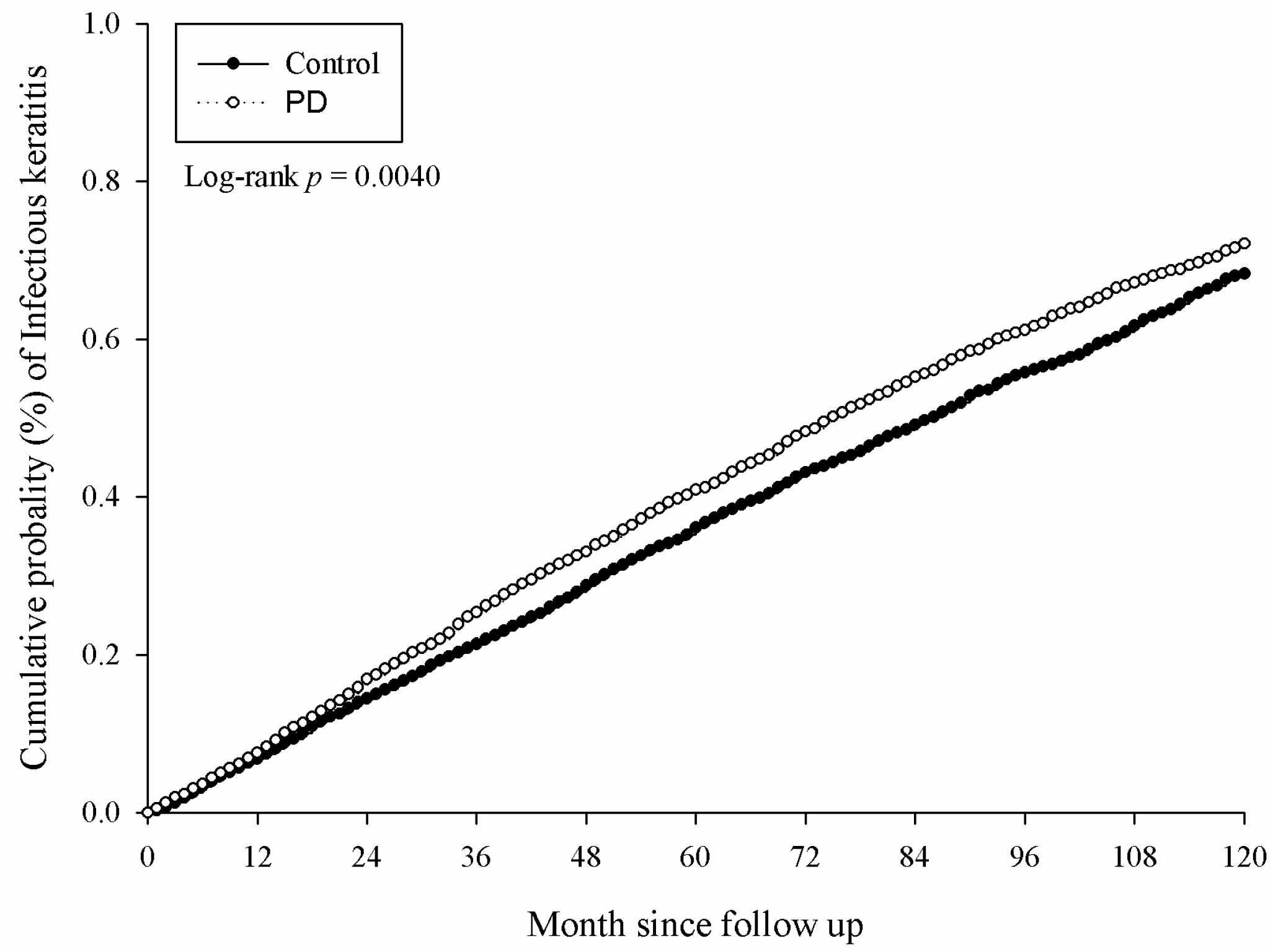
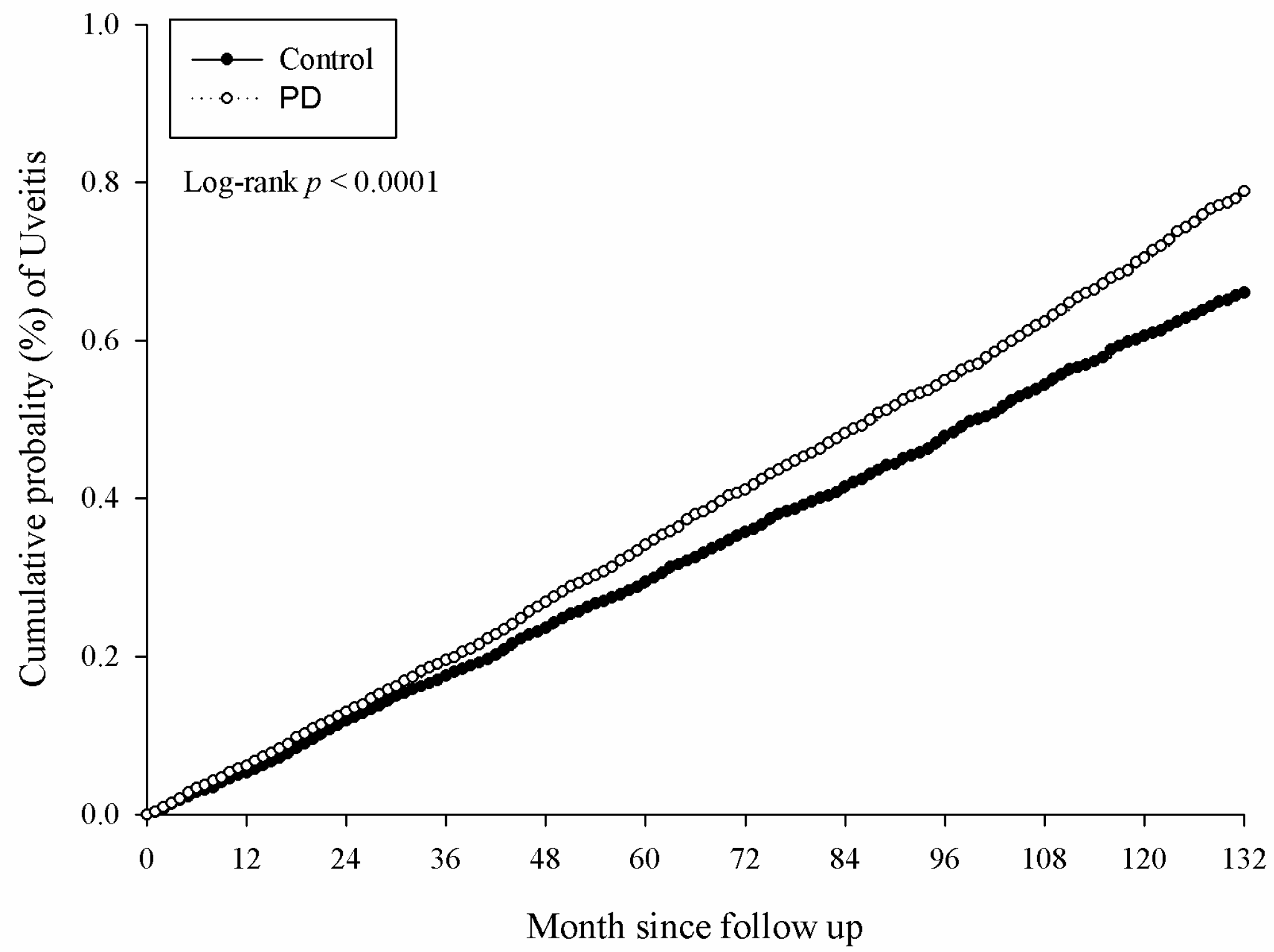
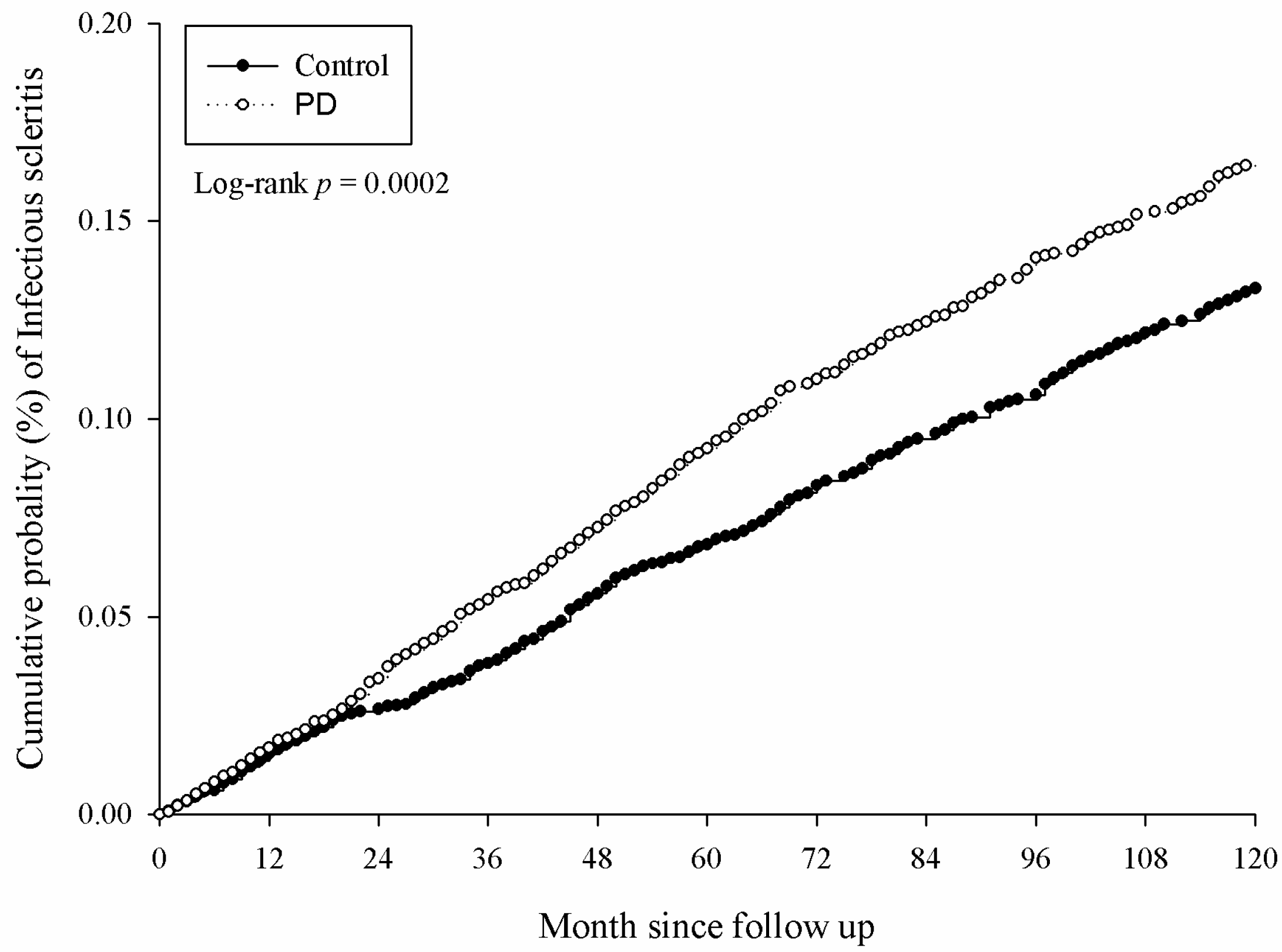
3.2. The Incidence of Ocular Disease in Periodontal Disease
3.3. The Subgroup Analysis for the Development of Ocular Disorders
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Slots, J. Periodontitis: Facts, fallacies and the future. Periodontology 2000 2017, 75, 7–23. [Google Scholar] [CrossRef] [PubMed]
- Coll, P.P.; Lindsay, A.; Meng, J.; Gopalakrishna, A.; Raghavendra, S.; Bysani, P.; O’Brien, D. The prevention of infections in older adults: Oral health. J. Am. Geriatr. Soc. 2019, 68, 411–416. [Google Scholar] [CrossRef]
- Cekici, A.; Kantarci, A.; Hasturk, H.; Van Dyke, T.E. Inflammatory and immune pathways in the pathogenesis of periodontal disease. Periodontology 2000 2014, 64, 57–80. [Google Scholar] [CrossRef] [PubMed]
- Abusleme, L.; Moutsopoulos, N.M. Il-17: Overview and role in oral immunity and microbiome. Oral Dis. 2017, 23, 854–865. [Google Scholar] [CrossRef] [PubMed]
- Debelian, G.J.; Olsen, I.; Tronstad, L. Systemic diseases caused by oral microorganisms. Endod. Dent. Traumatol. 1994, 10, 57–65. [Google Scholar] [CrossRef] [PubMed]
- Ceccarelli, F.; Saccucci, M.; Di Carlo, G.; Lucchetti, R.; Pilloni, A.; Pranno, N.; Luzzi, V.; Valesini, G.; Polimeni, A. Periodontitis and rheumatoid arthritis: The same inflammatory mediators? Mediat. Inflamm. 2019, 2019, 6034546. [Google Scholar] [CrossRef]
- de Molon, R.S.; Rossa, C., Jr.; Thurlings, R.M.; Cirelli, J.A.; Koenders, M.I. Linkage of periodontitis and rheumatoid arthritis: Current evidence and potential biological interactions. Int. J. Mol. Sci. 2019, 20, 4541. [Google Scholar] [CrossRef]
- Munoz Aguilera, E.; Suvan, J.; Buti, J.; Czesnikiewicz-Guzik, M.; Barbosa Ribeiro, A.; Orlandi, M.; Guzik, T.J.; Hingorani, A.D.; Nart, J.; D’Aiuto, F. Periodontitis is associated with hypertension: A systematic review and meta-analysis. Cardiovasc. Res. 2019, 116, 28–39. [Google Scholar] [CrossRef]
- Wisniewska-Spychala, B.; Sokalski, J.; Grajek, S.; Jemielity, M.; Trojnarska, O.; Choroszy-Krol, I.; Sojka, A.; Maksymiuk, T. Dentigenous infectious foci—A risk factor of infective endocarditis. Med. Sci. Monit. 2012, 18, Cr93–Cr104. [Google Scholar] [CrossRef]
- Byun, S.H.; Yoo, D.M.; Lee, J.W.; Choi, H.G. Analyzing the association between hyperuricemia and periodontitis: A cross-sectional study using koges hexa data. Int. J. Environ. Res. Public Health 2020, 17, 4777. [Google Scholar] [CrossRef]
- Pockpa, Z.A.; Struillou, X.; Coulibaly, N.T.; Weber, M.; Soueidan, A.; Badran, Z. Potential relationship between periodontal diseases and eye diseases. Med. Hypotheses 2017, 99, 63–66. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, T.; Nakagawa, H.; Matsuo, N. Endogenous aspergillus endophthalmitis associated with periodontitis. Ophthalmologica 1995, 209, 109–111. [Google Scholar] [CrossRef] [PubMed]
- Guncu, G.N.; Caglayan, F. Resolution of anterior scleritis after periodontal therapy. Eur. J. Dent. 2011, 5, 337–339. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Pedroso, J.F.; Lotfollahi, Z.; Albattarni, G.; Arrruda Schulz, M.; Monteiro, A.; Sehnem, A.L.; Gidlund, M.A.; Figueiredo Neto, A.M.; Jardini, M.A.N. Influence of periodontal disease on cardiovascular markers in diabetes mellitus patients. Sci. Rep. 2019, 9, 16138. [Google Scholar] [CrossRef]
- Darcey, J.; Ashley, M. See you in three months! The rationale for the three monthly periodontal recall interval: A risk based approach. Br. Dent. J. 2011, 211, 379–385. [Google Scholar] [CrossRef]
- Chien, H.W.; Wu, P.H.; Wang, K.; Sun, C.C.; Huang, J.Y.; Yang, S.F.; Chen, H.C.; Lee, C.Y. Increased incidence of glaucoma in sensorineural hearing loss: A population-based cohort study. Int. J. Environ. Res. Public Health 2019, 16, 2907. [Google Scholar] [CrossRef]
- Kononen, E.; Gursoy, M.; Gursoy, U.K. Periodontitis: A multifaceted disease of tooth-supporting tissues. J. Clin. Med. 2019, 8, 1135. [Google Scholar] [CrossRef]
- Flemmig, T.F. Periodontitis. Ann. Periodontol. 1999, 4, 32–38. [Google Scholar] [CrossRef]
- Bartold, P.M.; Van Dyke, T.E. An appraisal of the role of specific bacteria in the initial pathogenesis of periodontitis. J. Clin. Periodontol. 2019, 46, 6–11. [Google Scholar] [CrossRef]
- Slots, J. Focal infection of periodontal origin. Periodontology 2000 2019, 79, 233–235. [Google Scholar] [CrossRef]
- Zhou, R.; Shen, L.; Yang, C.; Wang, L.; Guo, H.; Yang, P.; Song, A. Periodontitis may restrain the mandibular bone healing via disturbing osteogenic and osteoclastic balance. Inflammation 2018, 41, 972–983. [Google Scholar] [CrossRef] [PubMed]
- Arias-Bujanda, N.; Regueira-Iglesias, A.; Balsa-Castro, C.; Nibali, L.; Donos, N.; Tomas, I. Accuracy of single molecular biomarkers in gingival crevicular fluid for the diagnosis of periodontitis: A systematic review and meta-analysis. J. Clin. Periodontol. 2019, 46, 1166–1182. [Google Scholar] [CrossRef] [PubMed]
- Austin, A.; Lietman, T.; Rose-Nussbaumer, J. Update on the management of infectious keratitis. Ophthalmology 2017, 124, 1678–1689. [Google Scholar] [CrossRef] [PubMed]
- Bro, T.; Tallstedt, L. Epidemiology of uveitis in a region of southern sweden. Acta Ophthalmol. 2019, 98, 32–35. [Google Scholar] [CrossRef] [PubMed]
- Guerrero-Wooley, R.L.; Peacock, J.E., Jr. Infectious scleritis: What the id clinician should know. In Open Forum Infectious Diseases; Oxford University Press: New York, NY, USA, 2018; Volume 5, p. ofy140. [Google Scholar]
- Bauer, D.; Kasper, M.; Walscheid, K.; Koch, J.M.; Muther, P.S.; Kirchhof, B.; Heiligenhaus, A.; Heinz, C. Multiplex cytokine analysis of aqueous humor in juvenile idiopathic arthritis-associated anterior uveitis with or without secondary glaucoma. Front. Immunol. 2018, 9, 708. [Google Scholar] [CrossRef] [PubMed]
- Zou, Y.; Zhang, H.; Li, H.; Chen, H.; Song, W.; Wang, Y. Strain-dependent production of interleukin-17/interferon-gamma and matrix remodeling-associated genes in experimental candida albicans keratitis. Mol. Vis. 2012, 18, 1215–1225. [Google Scholar]
- Radomska-Lesniewska, D.M.; Osiecka-Iwan, A.; Hyc, A.; Gozdz, A.; Dabrowska, A.M.; Skopinski, P. Therapeutic potential of curcumin in eye diseases. Cent. Eur. J. Immunol. 2019, 44, 181–189. [Google Scholar] [CrossRef] [PubMed]
- Kaur, A.; Kumar, V.; Singh, S.; Singh, J.; Upadhyay, N.; Datta, S.; Singla, S.; Kumar, V. Toll-like receptor-associated keratitis and strategies for its management. 3 Biotech 2015, 5, 611–619. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Chang, J.H.; McCluskey, P.J.; Wakefield, D. Recent advances in toll-like receptors and anterior uveitis. Clin. Exp. Ophthalmol. 2012, 40, 821–828. [Google Scholar] [CrossRef]
- Song, B.; Zhang, Y.L.; Chen, L.J.; Zhou, T.; Huang, W.K.; Zhou, X.; Shao, L.Q. The role of toll-like receptors in periodontitis. Oral Dis. 2017, 23, 168–180. [Google Scholar] [CrossRef] [PubMed]
- Artifoni, M.; Rothschild, P.R.; Brezin, A.; Guillevin, L.; Puechal, X. Ocular inflammatory diseases associated with rheumatoid arthritis. Nat. Rev. Rheumatol. 2014, 10, 108–116. [Google Scholar] [CrossRef] [PubMed]
- Boillot, A.; Bouchard, P.; Moss, K.; Offenbacher, S.; Czernichow, S. Periodontitis and retinal microcirculation in the atherosclerosis risk in communities study. J. Clin. Periodontol. 2015, 42, 342–349. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Fu, T.; Gu, H.; Jie, Y.; Sun, Z.; Jiang, D.; Yu, J.; Zhu, X.; Xu, J.; Hong, J. Trends in dacryocystitis in china: A strobe-compliant article. Medicine 2018, 97, e11318. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.; Livingstone, I.; Foot, B.; Murgatroyd, H.; MacEwen, C.J. Orbital cellulitis in scotland: Current incidence, aetiology, management and outcomes. Br. J. Ophthalmol. 2014, 98, 1575–1578. [Google Scholar] [CrossRef] [PubMed]
- Soriano, E.S.; Nishi, M. Endophthalmitis: Incidence and prevention. Curr. Opin. Ophthalmol. 2005, 16, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Malihi, M.; Li, X.; Patel, S.; Eck, T.; Chu, D.S.; Zarbin, M.A.; Bhagat, N. Infectious keratitis-associated endophthalmitis: A 14-year study. Retina 2017, 37, 662–666. [Google Scholar] [CrossRef] [PubMed]
- Nentwich, M.M.; Bordon, M.; di Martino, D.S.; Campuzano, A.R.; Torres, W.M.; Laspina, F.; Lichi, S.; Samudio, M.; Farina, N.; Sanabria, R.R.; et al. Clinical and epidemiological characteristics of infectious keratitis in paraguay. Int. Ophthalmol. 2015, 35, 341–346. [Google Scholar] [CrossRef] [PubMed]
- Tsirouki, T.; Dastiridou, A.; Symeonidis, C.; Tounakaki, O.; Brazitikou, I.; Kalogeropoulos, C.; Androudi, S. A focus on the epidemiology of uveitis. Ocul. Immunol. Inflamm. 2018, 26, 2–16. [Google Scholar] [CrossRef]
- Khumaedi, A.I.; Purnamasari, D.; Wijaya, I.P.; Soeroso, Y. The relationship of diabetes, periodontitis and cardiovascular disease. Diabetes Metab. Syndr. 2019, 13, 1675–1678. [Google Scholar] [CrossRef]
- Lamster, I.B.; Asadourian, L.; Del Carmen, T.; Friedman, P.K. The aging mouth: Differentiating normal aging from disease. Periodontology 2000 2016, 72, 96–107. [Google Scholar] [CrossRef]
- Eke, P.I.; Dye, B.A.; Wei, L.; Thornton-Evans, G.O.; Genco, R.J. Prevalence of periodontitis in adults in the united states: 2009 and 2010. J. Dent. Res. 2012, 91, 914–920. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.C.; Su, N.Y.; Huang, J.Y.; Lee, S.S.; Chang, Y.C. Trends in the prevalence of periodontitis in taiwan from 1997 to 2013: A nationwide population-based retrospective study. Medicine 2017, 96, e8585. [Google Scholar] [CrossRef] [PubMed]
- Hawkins, D.M. The problem of overfitting. J. Chem. Inf. Comput. Sci. 2004, 44, 1–12. [Google Scholar] [CrossRef]
- Lee, C.Y.; Chen, H.C.; Lin, H.W.; Huang, J.Y.; Lin, T.L.; Yang, C.H.; Yeh, C.B.; Lin, H.Y.; Yang, S.F. Increased risk of keratopathy after psoriasis: A nationwide population-based study. PLoS ONE 2018, 13, e0201285. [Google Scholar] [CrossRef] [PubMed]
- Nakib, S.; Han, J.; Li, T.; Joshipura, K.; Qureshi, A.A. Periodontal disease and risk of psoriasis among nurses in the united states. Acta Odontol. Scand. 2013, 71, 1423–1429. [Google Scholar] [CrossRef]
| Basic Characteristics | Study | Control | ASD |
|---|---|---|---|
| N (percentage) | 426,594 | 426,594 | |
| Age | 0.044 | ||
| 6–20 | 75,517 (17.70%) | 73,288 (17.18%) | |
| 20–39 | 158,846 (37.24%) | 162,049 (37.99%) | |
| 40–59 | 138,858 (32.55%) | 137,982 (32.35%) | |
| 60–100 | 53,373 (12.51%) | 53,275 (12.49%) | |
| Gender | 0.014 | ||
| Male | 196,352 (46.03%) | 197,345 (46.26%) | |
| Female | 230,242 (53.97%) | 229,249 (53.74%) | |
| Education | 0.050 | ||
| <6 | 168,683 (39.54%) | 168,293 (39.45%) | |
| 6–9 | 69,957 (16.40%) | 68,450 (16.05%) | |
| 9–12 | 150,977 (35.39%) | 155,830 (36.53%) | |
| ≥12 | 36,977 (8.67%) | 34,021 (7.98%) | |
| Marriage status | 0.000 | ||
| Not marriage | 198,894 (46.62%) | 199,868 (46.85%) | |
| Marriage | 188,496 (44.19%) | 187,163 (43.87%) | |
| Divorce | 19,525 (4.58%) | 19,781 (4.64%) | |
| Death of spouse | 19,679 (4.61%) | 19,782 (4.64%) | |
| Co-morbidities | |||
| Hypertension | 43,816 (10.27%) | 44,129 (10.34%) | 0.002 |
| Diabetes mellitus | 20,181 (4.73%) | 20,449 (4.79%) | 0.003 |
| Ischemic heart diseases | 8195 (1.92%) | 8208 (1.92%) | 0.000 |
| Hyperlipidemia | 21,999 (5.16%) | 21,607 (5.07%) | 0.004 |
| Cerebrovascular disease | 6573 (1.54%) | 6693 (1.57%) | 0.002 |
| Upper airway infections | 195,734 (45.88%) | 189,686 (44.47%) | 0.028 |
| Oral soft tissue infections | 4490 (1.05%) | 4486 (1.05%) | 0.000 |
| Facial cellulitis | 256 (0.06%) | 279 (0.07%) | 0.002 |
| Rheumatic diseases | 1574 (0.37%) | 1607 (0.38%) | 0.001 |
| Liver abscess | 53 (0.01%) | 51 (0.01%) | 0.000 |
| Allergic otolaryngologic diseases | 16,831 (3.95%) | 15,742 (3.69%) | 0.013 |
| Hordeolum and chalazion | 3661 (0.86%) | 3467 (0.81%) | 0.005 |
| Ocular Disease | Study | Control | aHR (95% CI) | ||
|---|---|---|---|---|---|
| Person-Months | Event | Person-Months | Event | ||
| Infectious keratitis | 35,964,736 | 2282 | 35,320,440 | 2056 | 1.094 (1.030–1.161) * |
| Endophthalmitis | 36,082,525 | 143 | 35,423,178 | 171 | 0.799 (0.639–1.007) |
| Orbital cellulitis | 36,080,669 | 172 | 35,421,228 | 193 | 0.871 (0.709–1.070) |
| Lacrimal duct infections | 36,082,173 | 151 | 35,425,872 | 130 | 1.101 (0.871–1.393) |
| Uveitis | 35,985,047 | 2119 | 35,341,802 | 1784 | 1.144 (1.074–1.218) * |
| Infectious scleritis | 36,061,675 | 514 | 35,410,360 | 393 | 1.270 (1.114–1.449) * |
| Ocular Disease | Study | Control | aHR (95% CI) | ||
|---|---|---|---|---|---|
| Person-Months | Event | Person-Months | Event | ||
| Age 6–20 | |||||
| Infectious keratitis | 6,234,633 | 582 | 6,071,389 | 492 | 1.148 (1.018–1.294) * |
| Endophthalmitis | 6,266,511 | 4 | 6,096,636 | 4 | 1.003 (0.251–4.013) |
| Orbital cellulitis | 6,264,868 | 29 | 6,095,236 | 31 | 0.922 (0.556–1.530) |
| Lacrimal duct infections | 6,265,912 | 10 | 6,096,682 | 4 | 2.424 (0.760–7.731) |
| Uveitis | 6,259,233 | 143 | 6,091,721 | 116 | 1.204 (0.942–1.538) |
| Infectious scleritis | 6,263,816 | 53 | 6,094,741 | 44 | 1.159 (0.777–1.729) |
| Age 20–39 | |||||
| Infectious keratitis | 13,593,414 | 932 | 13,889,191 | 827 | 1.148 (1.045–1.261) * |
| Endophthalmitis | 13,647,328 | 27 | 13,934,273 | 32 | 0.840 (0.503–1.403) |
| Orbital cellulitis | 13,645,764 | 58 | 13,932,632 | 63 | 0.928 (0.650–1.327) |
| Lacrimal duct infections | 13,647,781 | 23 | 13,935,030 | 22 | 1.044 (0.582–1.875) |
| Uveitis | 13,619,287 | 561 | 13,912,402 | 450 | 1.261 (1.114–1.428) * |
| Infectious scleritis | 13,636,469 | 210 | 13,927,604 | 140 | 1.502 (1.212–1.860) * |
| Age 40–59 | |||||
| Infectious keratitis | 11,982,844 | 528 | 11,575,239 | 474 | 1.085 (0.959–1.229) |
| Endophthalmitis | 12,006,899 | 52 | 11,597,795 | 60 | 0.843 (0.581–1.222) |
| Orbital cellulitis | 12,006,284 | 56 | 11,597,317 | 62 | 0.875 (0.609–1.256) |
| Lacrimal duct infections | 12,007,033 | 42 | 11,598,160 | 51 | 0.796 (0.529–1.198) |
| Uveitis | 11,967,214 | 826 | 11,562,807 | 727 | 1.097 (0.993–1.213) |
| Infectious scleritis | 12,000,242 | 172 | 11,592,897 | 147 | 1.119 (0.898–1.395) |
| Age ≥ 60 | |||||
| Infectious keratitis | 4,153,845 | 240 | 3,784,621 | 263 | 0.851 (0.714–1.014) |
| Endophthalmitis | 4,161,787 | 60 | 3,794,474 | 75 | 0.742 (0.528–1.042) |
| Orbital cellulitis | 4,163,753 | 29 | 3,796,043 | 37 | 0.736 (0.452–1.197) |
| Lacrimal duct infections | 4,161,447 | 76 | 3,796,000 | 53 | 1.308 (0.920–1.859) |
| Uveitis | 4,139,313 | 589 | 3,774,872 | 491 | 1.091 (0.967–1.230) |
| Infectious scleritis | 4,161,148 | 79 | 3,795,118 | 62 | 1.191 (0.853–1.661) |
| Ocular Disease | Study | Control | aHR (95% CI) | ||
|---|---|---|---|---|---|
| Person-Months | Event | Person-Months | Event | ||
| Male | |||||
| Infectious keratitis | 16,434,094 | 872 | 16,154,942 | 773 | 1.108 (1.006–1.221) * |
| Endophthalmitis | 16,477,073 | 71 | 16,189,610 | 89 | 0.762 (0.558–1.041) |
| Orbital cellulitis | 16,477,026 | 72 | 16,189,666 | 94 | 0.748 (0.550–1.017) |
| Lacrimal duct infections | 16,478,613 | 43 | 16,192,664 | 36 | 1.127 (0.723–1.757) |
| Uveitis | 16,425,329 | 1082 | 16,150,987 | 863 | 1.204 (1.101–1.317) * |
| Infectious scleritis | 16,470,040 | 206 | 16,186,651 | 148 | 1.335 (1.081–1.649) * |
| Female | |||||
| Infectious keratitis | 19,530,642 | 1410 | 19,165,498 | 1283 | 1.081 (1.002–1.166) * |
| Endophthalmitis | 19,605,452 | 72 | 19,233,568 | 82 | 0.838 (0.610–1.150) |
| Orbital cellulitis | 19,603,643 | 100 | 19,231,562 | 99 | 0.991 (0.751–1.309) |
| Lacrimal duct infections | 19,603,560 | 108 | 19,233,208 | 94 | 1.093 (0.829–1.441) |
| Uveitis | 19,559,718 | 1037 | 19,190,815 | 921 | 1.087 (0.995–1.188) |
| Infectious scleritis | 19,591,635 | 308 | 19,223,709 | 245 | 1.228 (1.038–1.453) * |
| Event | Study | Control | aHR (95% CI) | ||
|---|---|---|---|---|---|
| Person-Months | Event | Person-Months | Event | ||
| PD interval < 2 years | |||||
| Infectious keratitis | 9,902,485 | 719 | 9852,697 | 618 | 1.159 (1.041–1.291) * |
| Endophthalmitis | 9,910,251 | 43 | 9859,367 | 46 | 0.925 (0.611–1.403) |
| Orbital cellulitis | 9,910,104 | 44 | 9859,010 | 62 | 0.703 (0.478–1.034) |
| Lacrimal duct infections | 9,910,041 | 42 | 9859,397 | 39 | 1.055 (0.682–1.632) |
| Uveitis | 9,904,225 | 557 | 9854,210 | 506 | 1.091 (0.968–1.231) |
| Infectious scleritis | 9,908,949 | 154 | 9858,365 | 113 | 1.345 (1.055–1.714) * |
| PD interval 2–5 years | |||||
| Infectious keratitis | 12,683,048 | 864 | 12,491,050 | 776 | 1.098 (0.996–1.209) |
| Endophthalmitis | 12,718,716 | 42 | 12,521,096 | 63 | 0.642 (0.434–0.949) |
| Orbital cellulitis | 12,718,150 | 74 | 12,520,183 | 77 | 0.940 (0.683–1.294) |
| Lacrimal duct infections | 12,718,699 | 48 | 12,521,654 | 34 | 1.354 (0.872–2.102) |
| Uveitis | 12,691,895 | 768 | 12,497,366 | 629 | 1.184 (1.065–1.315) * |
| Infectious scleritis | 12,712,409 | 213 | 12,517,409 | 150 | 1.386 (1.125–1.708) * |
| PD interval ≥ 5 years | |||||
| Infectious keratitis | 13,379,203 | 728 | 12,976,693 | 705 | 1.005 (0.906–1.114) |
| Endophthalmitis | 13,453,558 | 60 | 13,042,715 | 65 | 0.856 (0.603–1.217) |
| Orbital cellulitis | 13,452,415 | 57 | 13,042,035 | 54 | 1.025 (0.706–1.488) |
| Lacrimal duct infections | 13,453,433 | 62 | 13,044,821 | 57 | 1.004 (0.700–1.440) |
| Uveitis | 13,388,927 | 834 | 12,990,226 | 681 | 1.149 (1.038–1.272) * |
| Infectious scleritis | 13,440,317 | 165 | 13,034,586 | 137 | 1.139 (0.908–1.429) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chau, S.-F.; Lee, C.-Y.; Huang, J.-Y.; Chou, M.-C.; Chen, H.-C.; Yang, S.-F. The Existence of Periodontal Disease and Subsequent Ocular Diseases: A Population-Based Cohort Study. Medicina 2020, 56, 621. https://doi.org/10.3390/medicina56110621
Chau S-F, Lee C-Y, Huang J-Y, Chou M-C, Chen H-C, Yang S-F. The Existence of Periodontal Disease and Subsequent Ocular Diseases: A Population-Based Cohort Study. Medicina. 2020; 56(11):621. https://doi.org/10.3390/medicina56110621
Chicago/Turabian StyleChau, Siu-Fung, Chia-Yi Lee, Jing-Yang Huang, Ming-Chih Chou, Hung-Chi Chen, and Shun-Fa Yang. 2020. "The Existence of Periodontal Disease and Subsequent Ocular Diseases: A Population-Based Cohort Study" Medicina 56, no. 11: 621. https://doi.org/10.3390/medicina56110621
APA StyleChau, S.-F., Lee, C.-Y., Huang, J.-Y., Chou, M.-C., Chen, H.-C., & Yang, S.-F. (2020). The Existence of Periodontal Disease and Subsequent Ocular Diseases: A Population-Based Cohort Study. Medicina, 56(11), 621. https://doi.org/10.3390/medicina56110621






