Nutritional Aspects in Diabetic CKD Patients on Tertiary Care
Abstract
1. Introduction
2. Materials and Methods
2.1. Biochemistry
2.2. Anthropometry
2.3. Resting Energy Expenditure
2.4. Physical Activity and Performance
2.5. Functional Tests
2.6. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Kooman, J.P.; van der Sande, F.M.; Leunissen, K.M. Kidney disease and aging: A reciprocal relation. Exp. Gerontol. 2017, 87, 156–159. [Google Scholar] [CrossRef]
- Lee, S.J.; Son, H.; Shin, S.K. Influence of frailty on health-related quality of life in pre-dialysis patients with chronic kidney disease in Korea: A cross-sectional study. Health Qual. Life Outcomes 2015, 29, 70–76. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, E.; Miller, M.; Yaxley, A.; Isenring, E. Malnutrition in the elderly: A narrative review. Maturitas 2013, 76, 296–302. [Google Scholar] [CrossRef] [PubMed]
- Giglio, J.; Kamimura, M.A.; Lamarca, F.; Rodrigues, J.; Santin, F.; Avesani, C.M. Association of Sarcopenia with Nutritional Parameters, Quality of Life, Hospitalization, and Mortality Rates of Elderly Patients on Hemodialysis. J. Ren. Nutr. 2018, 28, 197–207. [Google Scholar] [CrossRef]
- Obermayr, R.P.; Temml, C.; Knechtelsdorfer, M.; Gutjahr, G.; Kletzmayr, J.; Heiss, S.; Ponholzer, A.; Madersbacher, S.; Oberbauer, R.; Klauser-Braun, R. Predictors of new-onset decline in kidney function in a general middle-European population. Nephrol. Dial. Transplant. 2008, 23, 1265–1273. [Google Scholar] [CrossRef] [PubMed]
- Kramer, H.J.; Saranathan, A.; Luke, A.; Durazo-Arvizu, R.A.; Guichan, C.; Hou, S.; Cooper, R. Increasing body mass index and obesity in the incident ESRD population. J. Am. Soc. Nephrol. 2006, 17, 1453–1459. [Google Scholar] [CrossRef]
- Roshanravan, B.; Robinson-Cohen, C.; Patel, K.V.; Ayers, E.; Littman, A.J.; de Boer, I.H.; Ikizler, T.A.; Himmelfarb, J.; Katzel, L.I.; Kestenbaum, B.; et al. Association between physical performance and all-cause mortality in CKD. J. Am. Soc. Nephrol. 2013, 24, 822–830. [Google Scholar] [CrossRef] [PubMed]
- Bellizzi, V.; Cupisti, A.; Locatelli, F.; Bolasco, P.; Brunori, G.; Cancarini, G.; Caria, S.; De Nicola, L.; Di Iorio, B.R.; Di Micco, L.; et al. “Conservative Treatment of CKD” study group of the Italian Society of Nephrology. Low-protein diets for chronic kidney disease patients: The Italian experience. BMC Nephrol. 2016, 17, 77. [Google Scholar] [CrossRef]
- Tuttle, K.R.; Bakris, G.L.; Bilous, R.W.; Chiang, J.L.; de Boer, I.H.; Goldstein-Fuchs, J.; Hirsch, I.B.; Kalantar-Zadeh, K.; Narva, A.S.; Navaneethan, S.D.; et al. Diabetic kidney disease: A report from an ada consensus conference. Am. J. Kidney Dis. 2014, 64, 510–533. [Google Scholar] [CrossRef]
- Boule, N.G.; Haddad, E.; Kenny, G.P.; Wells, G.A.; Sigal, R.J. Effects of exercise on glycemic control and body mass in type 2 diabetes mellitus: A meta-analysis of controlled clinical trials. JAMA 2001, 286, 1218–1227. [Google Scholar] [CrossRef]
- Hamasaki, H. Daily physical activity and type 2 diabetes: A review. World J. Diabetes 2016, 7, 243–251. [Google Scholar] [CrossRef] [PubMed]
- Delmonico, M.J.; Harris, T.B.; Lee, J.S.; Visser, M.; Nevitt, M.; Kritchevsky, S.B.; Tylavsky, F.A.; Newman, A.B. Health, Aging and Body Composition Study. Alternative definitions of sarcopenia, lower extremity performance, and functional impairment with aging in older men and women. J. Am. Geriatr. Soc. 2007, 55, 769–774. [Google Scholar] [CrossRef] [PubMed]
- Hanatani, S.; Izumiya, Y.; Onoue, Y.; Tanaka, T.; Yamamoto, M.; Ishida, T.; Yamamura, S.; Kimura, Y.; Araki, S.; Arima, Y.; et al. Non-invasive testing for sarcopenia predicts future cardiovascular events in patients with chronic kidney disease. Int. J. Cardiol. 2018, 268, 216–221. [Google Scholar] [CrossRef] [PubMed]
- Kosmadakis, G.C.; Bevington, A.; Smith, A.C.; Clapp, E.L.; Viana, J.L.; Bishop, N.C.; Feehally, J. Physical exercise in patients with severe kidney disease. Nephron Clin. Pract. 2010, 115, c7–c16. [Google Scholar] [CrossRef] [PubMed]
- Moorthi, R.N.; Avin, K.G. Clinical relevance of sarcopenia in chronic kidney disease. Curr. Opin. Nephrol. Hypertens. 2017, 26, 219–228. [Google Scholar] [CrossRef] [PubMed]
- Park, S.W.; Goodpaster, B.H.; Strotmeyer, E.S.; Kuller, L.H.; Broudeau, R.; Kammerer, C.; de Rekeneire, N.; Harris, T.B.; Schwartz, A.V.; Tylavsky, F.A.; et al. Health, Aging, and Body Composition Study. Accelerated loss of skeletal muscle strength in older adults with type 2 diabetes: The health, aging, and body composition study. Diabetes Care 2007, 30, 1507–1512. [Google Scholar] [CrossRef] [PubMed]
- D’Alessandro, C.; Piccoli, G.B.; Calella, P.; Brunori, G.; Pasticci, F.; Egidi, M.F.; Capizzi, I.; Bellizzi, V.; Cupisti, A. “Dietaly”: Practical issues for the nutritional management of CKD patients in Italy. BMC Nephrol. 2016, 17, 102. [Google Scholar] [CrossRef]
- Cupisti, A.; D’Alessandro, C.; Di Iorio, B.; Bottai, A.; Zullo, C.; Giannese, D.; Barsotti, M.; Egidi, M.F. Nutritional support in the tertiary care of patients affected by chronic renal insufficiency: Report of a step-wise, personalized, pragmatic approach. BMC Nephrol. 2016, 17, 124. [Google Scholar] [CrossRef]
- Maroni, B.J.; Steinman, T.I.; Mitch, W.E. A method for estimating nitrogen intake in patients with chronic renal failure. Kidney Int. 1985, 27, 58–65. [Google Scholar] [CrossRef]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.L.; Castro, A.F., 3rd; Feldman, H.I.; Kusek, J.W.; Eggers, P.; Van Lente, F.; Greene, T.; et al. CKD-EPI (Chronic Kidney Disease Epidemiology Collaboration). A New Equation to Estimate Glomerular Filtration Rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef]
- Saragat, B.; Buffa, R.; Mereu, E.; De Rui, M.; Coin, A.; Sergi, G.; Marini, E. Specific bioelectrical impedance vector reference values for assessing body composition in the Italian elderly. Exp. Gerontol. 2014, 50, 52–56. [Google Scholar] [CrossRef] [PubMed]
- Nieman, D.C.; Austin, M.D.; Benezra, L.; Pearce, S.; McInnis, T.; Unick, J.; Gross, S.J. Validation of Cosmed’s FitMate in measuring oxygen consumption and estimating resting metabolic rate. Appalachian State University, Boone, North Carolina, USA. Res. Sports Med. 2006, 14, 89–96. [Google Scholar] [CrossRef]
- Weir, J.B. New methods for calculating metabolic rate with special reference to protein metabolism. Nutrition 1949, 6, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.J.; Rikli, R.E.; Beam, W.C. A 30-s chair-stand test as a measure of lower body strength in community-residing older adults. Res. Q. Exerc. Sport 1999, 70, 113–119. [Google Scholar] [CrossRef] [PubMed]
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS Statement: Guidelines for the Six-Minute Walk Test. Am. J. Respir Crit. Care Med. Vol. 2002, 166, 111–117. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.J.; Rikli, R.E. Measuring functional fitness of older adults. J. Act. Aging 2002, 1, 24–30. [Google Scholar]
- Schlussel, M.M.; Anjos, L.A.D.; Vasconcellos, M.T.L.; Kac, G. Reference values of handgrip dynamometry of healthy adults: A population-based study. Clin. Nutr. 2008, 27, 601–607. [Google Scholar] [CrossRef] [PubMed]
- Bianchi, L.; Volpato, S. Muscle dysfunction in type 2 diabetes: A major threat to patient’s mobility and independence. Acta Diabetol. 2016, 53, 879–889. [Google Scholar] [CrossRef]
- Tsutsui, H.; Kinugawa, S.; Matsushima, S.; Yokota, T. Oxidative stress in cardiac and skeletal muscle dysfunction associated with diabetes mellitus. J. Clin. Biochem. Nutr. 2011, 48, 68–71. [Google Scholar] [CrossRef]
- Hall, J.E.; Henegar, J.R.; Dwyer, T.M.; Liu, J.; Silva, A.A.; Kuo, J.J.; Tallam, L. Is obesity a major cause of chronic kidney disease? Adv. Ren. Replace. Ther. 2004, 11, 41–54. [Google Scholar] [CrossRef]
- Kopple, J.D.; Feroze, U. The effect of obesity on chronic kidney disease. J. Ren. Nutr. 2011, 21, 66–71. [Google Scholar] [CrossRef] [PubMed]
- Piccoli, G.B.; Ventrella, F.; Capizzi, I.; Vigotti, F.N.; Mongilardi, E.; Grassi, G.; Loi, V.; Cabiddu, G.; Avagnina, P.; Versino, E. Low-protein Diets in Diabetic Chronic Kidney Disease (CKD) Patients: Are They Feasible and Worth the Effort? Nutrients 2016, 8, 649. [Google Scholar] [CrossRef] [PubMed]
- Porrini, E.; Ruggenenti, P.; Mogensen, C.E.; Barlovic, D.P.; Praga, M.; Cruzado, J.M.; Hojs, R.; Abbate, M.; de Vries, A.P. ERA-EDTA diabesity working group. Non-proteinuric pathways in loss of renal function in patients with type 2 diabetes. Lancet Diabetes Endocrinol. 2015, 3, 382–391. [Google Scholar] [CrossRef]
- Metti, A.L.; Best, J.R.; Shaaban, C.E.; Ganguli, M.; Rosano, C. Longitudinal changes in physical functionand physical activity in older adults. Age Ageing 2018, 13. [Google Scholar] [CrossRef]
- Dong, L.; Li, J.; Lian, Y.; Tang, Z.X.; Zen, Z.; Yu, P.; Li, Y. Long-Term Intensive Lifestyle Intervention Promotes Improvement of Stage III Diabetic Nephropathy. Med. Sci. Monit. 2019, 25, 3061–3068. [Google Scholar] [CrossRef] [PubMed]
- Hamano, T.; Nakano, C.; Obi, Y.; Fujii, N.; Matsui, I.; Tomida, K.; Mikami, S.; Inoue, K.; Shimomura, A.; Kusunoki, Y.; et al. Fibroblast growth factor 23 and 25-hydroxyvitamin D levels are associated with estimated glomerular filtration rate decline. Kidney Int. Suppl. 2013, 3, 469–475. [Google Scholar] [CrossRef]
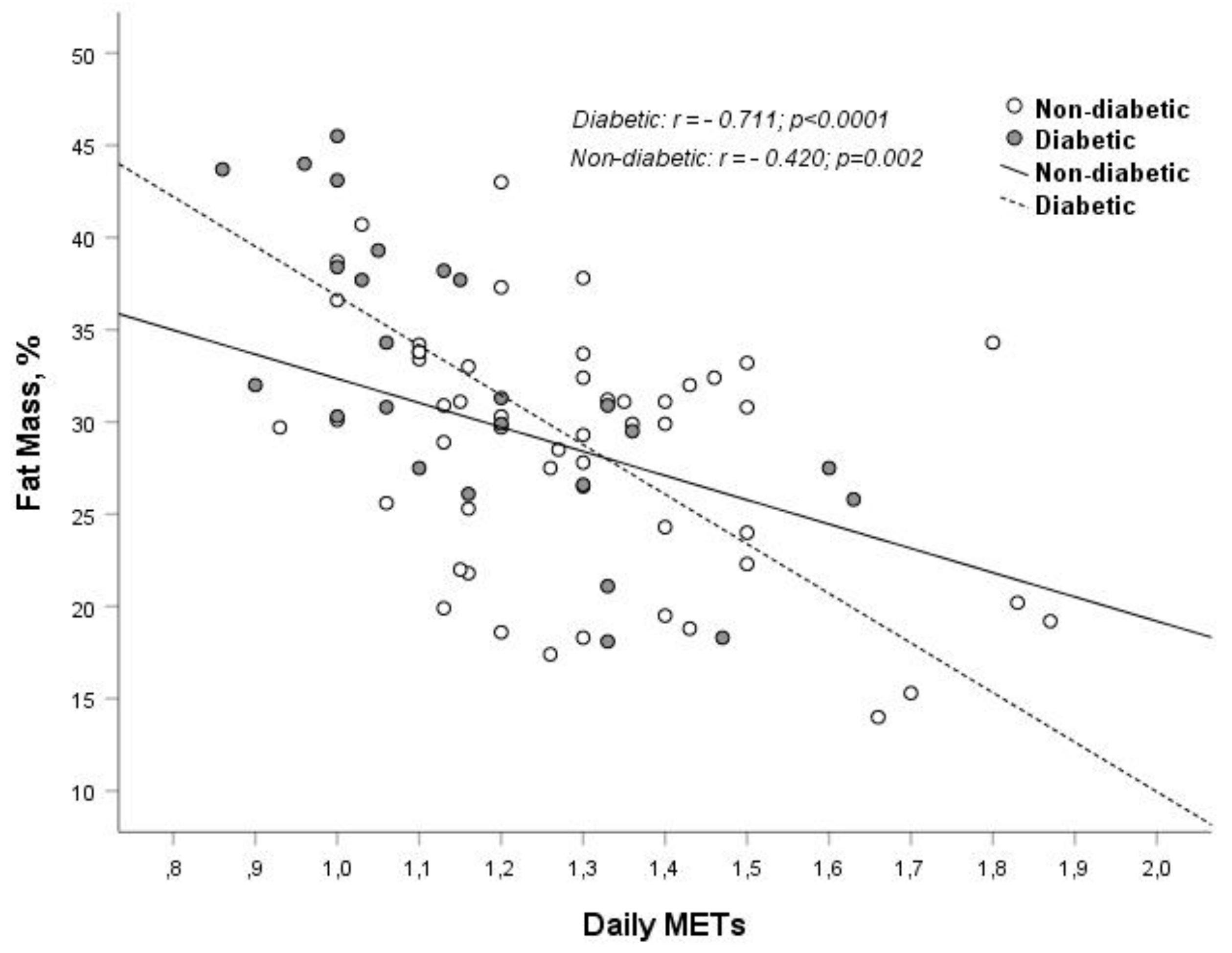
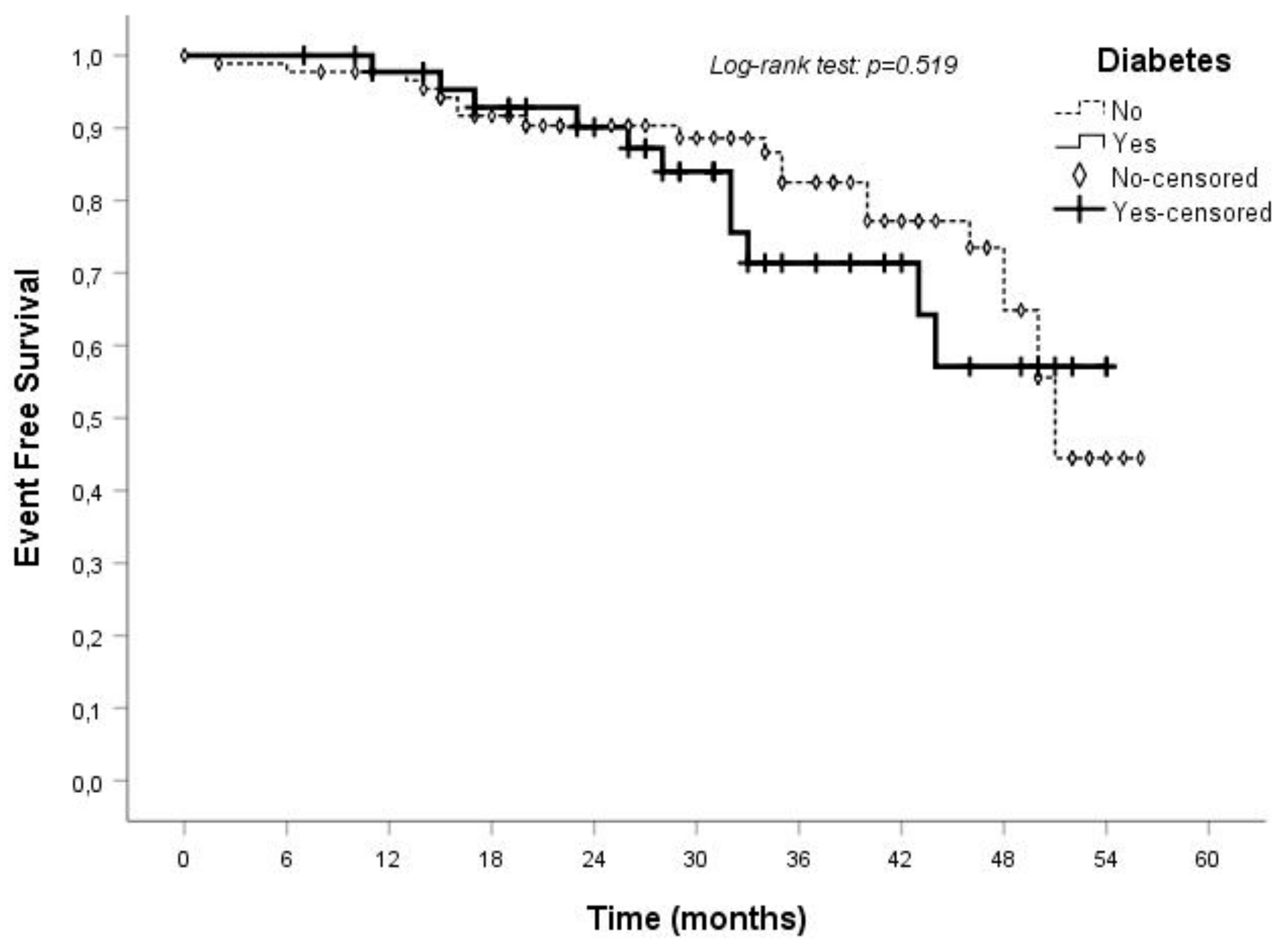
| Diabetic CKD | Nondiabetic CKD | p Value | |
|---|---|---|---|
| Gender, m/f | 40/8 | 80/16 | |
| Age, yrs | 71.5 ± 8.2 | 71.6 ± 9 | 0.875 |
| eGFR, ml/min×1.73 m2 | 29.8 ± 9.1 | 31.3 ± 10.9 | 0.398 |
| BUN, mg/dL | 43 ± 16 | 37.6 ± 12.2 | 0.044 |
| sCreatinine, mg/dL | 2.26 (1.77–2.78) | 2.10 (1.68–2.82) | 0.596 |
| sSodium, mEq/L | 141 (140–142) | 140 (139–142) | 0.843 |
| sPotassium, mEq/L | 4.78 ± 0.52 | 4.70 ± 0.52 | 0.406 |
| sCalcium, mg/dL | 9.33 ± 0.41 | 9.29 ± 0.48 | 0.602 |
| sPhosphate, mg/dL | 3.34 ± 0.63 | 3.33 ± 0.56 | 0.915 |
| Bicarbonate, mEq/L | 25.4 ± 3.7 | 24.7 ± 2.7 | 0.354 |
| sTotal Protein, g/dL | 7.10 ± 0.48 | 7.14 ± 0.47 | 0.614 |
| sAlbumin, g/dL | 4.18 ± 0.45 | 4.16 ± 0.38 | 0.762 |
| Hemoglobin, g/dL | 13.1 ± 1.7 | 13.2 ± 1.6 | 0.743 |
| Hematocrit, % | 38.8 ± 5.8 | 39.7 ± 4.5 | 0.332 |
| 25(OH)VitD, ng/mL | 20.5 ± 10.3 | 22.4 ± 10.9 | 0.398 |
| sCholesterol, mg/dL | 170 ± 38 | 179 ± 39 | 0.197 |
| Diabetic CKD n = 48 | Nondiabetic CKD n = 96 | p Value | |
|---|---|---|---|
| Body weight, kg | 83.1 ± 15 | 76.4 ± 12.3 | 0.0090 |
| BMI, kg/m2 | 29.1 ± 4.64 | 27.2 ± 3.52 | 0.0144 |
| Waist circ., cm | 104.7 ± 11.9 | 99.4 ± 12.4 | 0.0162 |
| MAMC, cm | 26.0 ± 4.2 | 25.3 ± 10 | 0.5581 |
| MAMA, cm2 | 55.4 ± 16.9 | 58.9 ± 86.5 | 0.7030 |
| Phase angle, ° | 5 ± 1 | 4.9 ± 1 | 0.8655 |
| BCMI, kg/m2 | 9.5 ± 1.9 | 9.4 ± 2.9 | 0.8423 |
| FM, % | 31.5 ± 7.4 | 27.8 ± 6.7 | 0.0071 |
| MM, % | 40.1 ± 5.3 | 43.2 ± 5.7 | 0.0324 |
| Average daily Mets | 1.17 ± 0.2 | 1.29 ± 0.2 | 0.0167 |
| Average daily steps | 3580 ± 2471 | 5628 ± 4143 | 0.0080 |
| 6MWT, m | 318 ± 94 | 331 ± 84 | 0.4839 |
| Hand grip, kg | 29.1 ± 7.5 | 26.5 ± 7.9 | 0.0602 |
| REE, kcal/d | 1341 (1231–1531) | 1224 (1150–1468) | 0.012 |
| nPCR, g/kg b.w/d | 0.86 ± 0.22 | 0.81 ± 0.19 | 0.3481 |
| Univariate Analysis | eGFR Adjusted | ||
|---|---|---|---|
| HR (CI 95%) | p Value | p Value | |
| Diabetes, (0) no; (1) yes | 1.26 (0.62–2.57) | 0.691 | 0.414 |
| MAMC, cm | 0.85 (0.78–0.91) | <0.001 | <0.001 |
| Phase angle, ° | 0.67 (0.46–0.98) | 0.041 | 0.025 |
| BCM, kg | 0.95 (0.89–1.01) | 0.125 | 0.184 |
| FFM, kg | 0.99 (0.95–1.02) | 0.475 | 0.963 |
| Urea, mg/dL | 1.03 (1.02–1.04) | <0.001 | 0.088 |
| Phosphate, mg/dL | 3.20 (1.61–6.34) | 0.001 | 0.082 |
| Total cholesterol, mg/dL | 0.98 (0.97–0.99) | 0.001 | <0.001 |
| sAlbumin, g/dL | 0.24 (0.09–0.66) | 0.005 | 0.024 |
| Hemoglobin, g/dL | 0.66 (0.51–0.86) | 0.002 | 0.072 |
| Hematocrit, % | 0.95 (0.90–0.97) | 0.034 | 0.221 |
| nPCR*, g/kg b.w/d | 0.13 (0.01–1.55) | 0.106 | 0.768 |
| 6MWT, m | 0.98 (0.99–1.01) | 0.203 | 0.373 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
D’Alessandro, C.; Barsotti, M.; Cianchi, C.; Mannucci, C.; Morganti, R.; Tassi, S.; Cupisti, A. Nutritional Aspects in Diabetic CKD Patients on Tertiary Care. Medicina 2019, 55, 427. https://doi.org/10.3390/medicina55080427
D’Alessandro C, Barsotti M, Cianchi C, Mannucci C, Morganti R, Tassi S, Cupisti A. Nutritional Aspects in Diabetic CKD Patients on Tertiary Care. Medicina. 2019; 55(8):427. https://doi.org/10.3390/medicina55080427
Chicago/Turabian StyleD’Alessandro, Claudia, Massimiliano Barsotti, Caterina Cianchi, Claudia Mannucci, Riccardo Morganti, Serena Tassi, and Adamasco Cupisti. 2019. "Nutritional Aspects in Diabetic CKD Patients on Tertiary Care" Medicina 55, no. 8: 427. https://doi.org/10.3390/medicina55080427
APA StyleD’Alessandro, C., Barsotti, M., Cianchi, C., Mannucci, C., Morganti, R., Tassi, S., & Cupisti, A. (2019). Nutritional Aspects in Diabetic CKD Patients on Tertiary Care. Medicina, 55(8), 427. https://doi.org/10.3390/medicina55080427





