Can PSMA-Targeting Radiopharmaceuticals Be Useful for Detecting Hepatocellular Carcinoma Using Positron Emission Tomography? An Updated Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol
2.2. Literature Search Strategy and Information Sources
2.3. Eligibility Criteria
2.4. Selection Process
2.5. Data Collection Process and Data Extraction
2.6. Quality Assessment (Risk of Bias Assessment)
2.7. Effect Measures
2.8. Statistical Analysis
2.9. Additional Analyses
3. Results
3.1. Literature Search and Study Selection
3.2. Study Characteristics
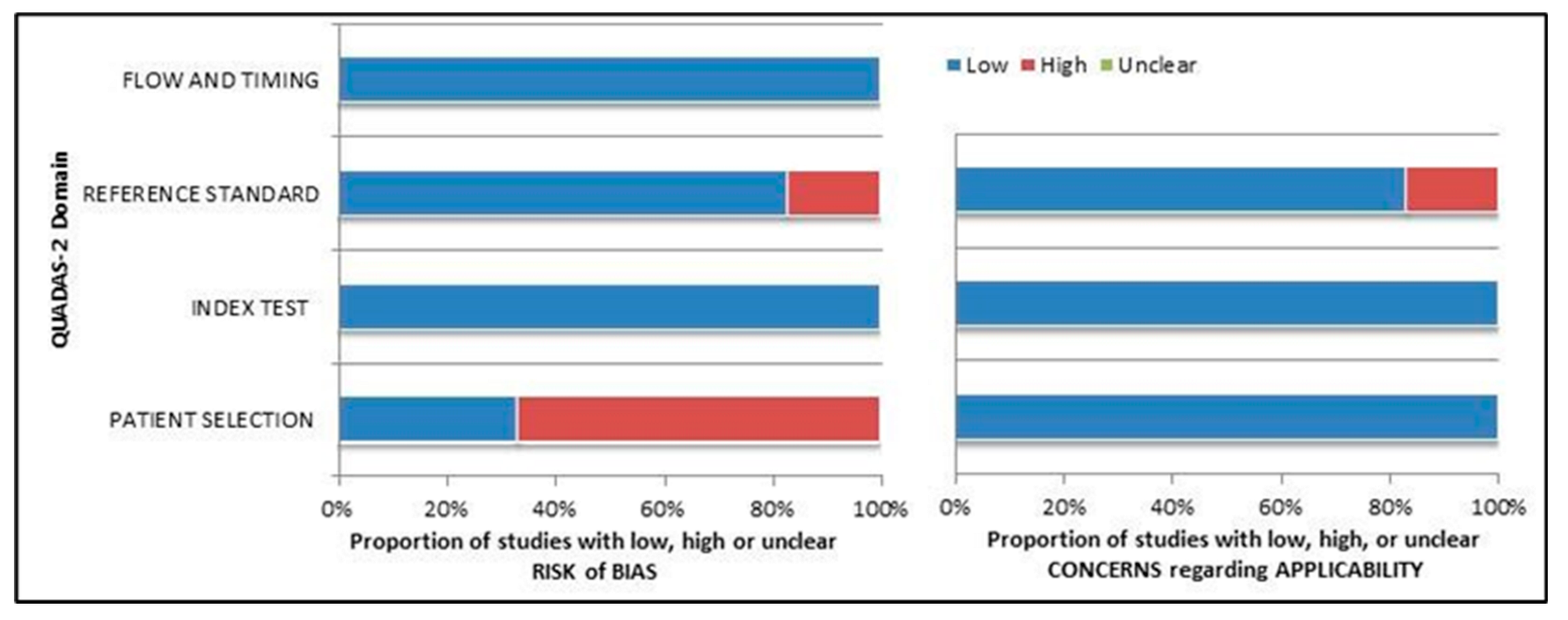
3.3. Risk of Bias and Applicability
3.4. Results of Individual Studies (Qualitative Synthesis)
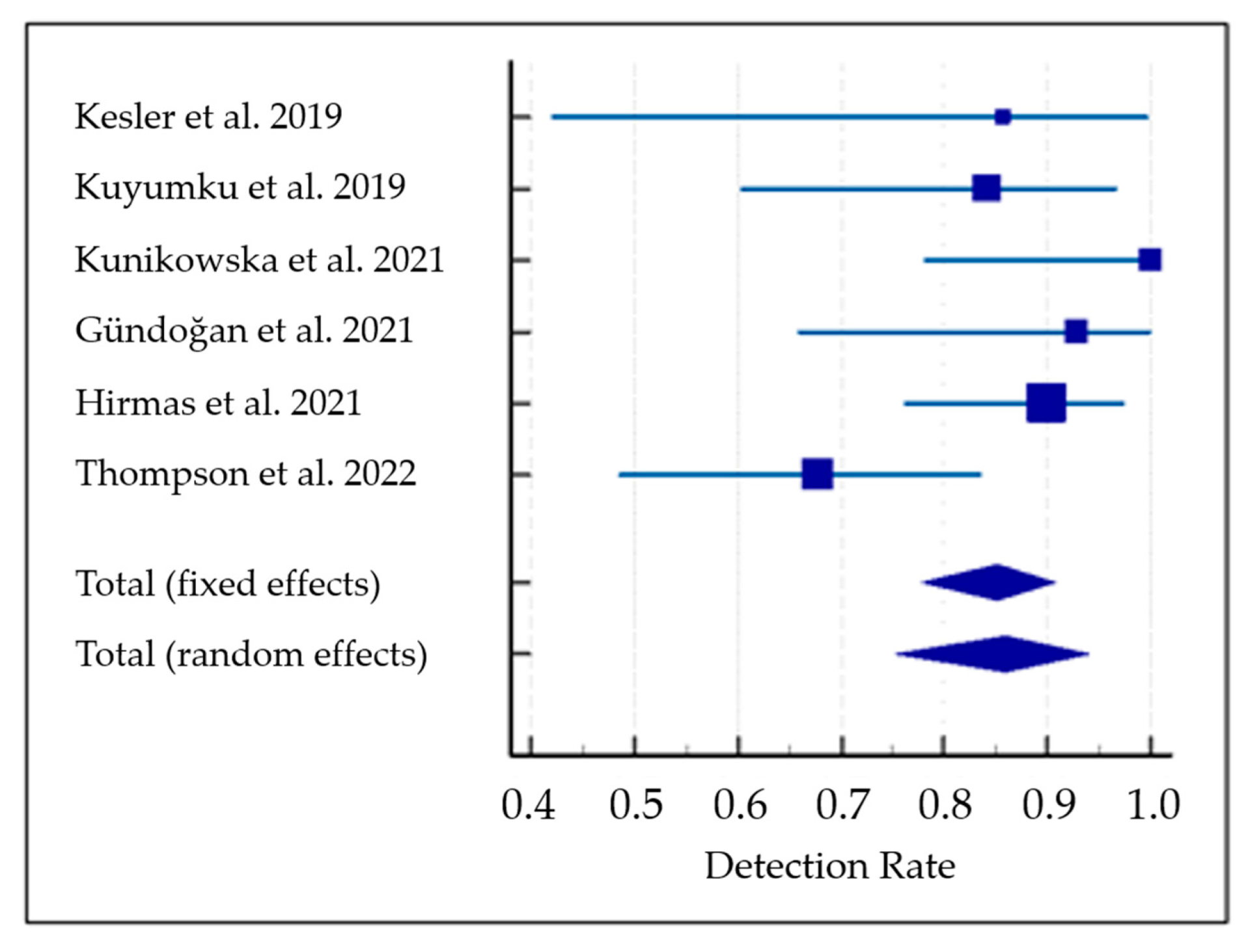
3.5. Meta-Analysis (Quantitative Synthesis)
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Llovet, J.M.; Kelley, R.K.; Villanueva, A.; Singal, A.G.; Pikarsky, E.; Roayaie, S.; Lencioni, R.; Koike, K.; Zucman-Rossi, J.; Finn, R.S. Hepatocellular Carcinoma. Nat. Rev. Dis. Prim. 2021, 7, 6. [Google Scholar] [CrossRef] [PubMed]
- McGlynn, K.A.; Petrick, J.L.; London, W.T. Global Epidemiology of Hepatocellular Carcinoma: An Emphasis on Demographic and Regional Variability. Clin. Liver Dis. 2015, 19, 223–238. [Google Scholar] [CrossRef] [PubMed]
- Rahib, L.; Smith, B.D.; Aizenberg, R.; Rosenzweig, A.B.; Fleshman, J.M.; Matrisian, L.M. Projecting Cancer Incidence and Deaths to 2030: The Unexpected Burden of Thyroid, Liver, and Pancreas Cancers in the United States. Cancer Res. 2014, 74, 2913–2921. [Google Scholar] [CrossRef] [PubMed]
- European Association for the Study of the Liver. Electronic address: Easloffice@easloffice.eu. European Association for the Study of the Liver EASL Clinical Practice Guidelines: Management of Hepatocellular Carcinoma. J. Hepatol. 2018, 69, 182–236. [Google Scholar] [CrossRef]
- Marrero, J.A.; Kulik, L.M.; Sirlin, C.B.; Zhu, A.X.; Finn, R.S.; Abecassis, M.M.; Roberts, L.R.; Heimbach, J.K. Diagnosis, Staging, and Management of Hepatocellular Carcinoma: 2018 Practice Guidance by the American Association for the Study of Liver Diseases. Hepatology 2018, 68, 723–750. [Google Scholar] [CrossRef]
- Schulze, K.; Imbeaud, S.; Letouzé, E.; Alexandrov, L.B.; Calderaro, J.; Rebouissou, S.; Couchy, G.; Meiller, C.; Shinde, J.; Soysouvanh, F.; et al. Exome Sequencing of Hepatocellular Carcinomas Identifies New Mutational Signatures and Potential Therapeutic Targets. Nat. Genet 2015, 47, 505–511. [Google Scholar] [CrossRef]
- Ayuso, C.; Rimola, J.; Vilana, R.; Burrel, M.; Darnell, A.; García-Criado, Á.; Bianchi, L.; Belmonte, E.; Caparroz, C.; Barrufet, M.; et al. Diagnosis and Staging of Hepatocellular Carcinoma (HCC): Current Guidelines. Eur. J. Radiol. 2018, 101, 72–81. [Google Scholar] [CrossRef]
- Kanmaniraja, D.; Dellacerra, G.; Holder, J.; Erlichman, D.; Chernyak, V. Liver Imaging Reporting and Data System (LI-RADS) V2018: Review of the CT/MRI Diagnostic Categories. Can. Assoc. Radiol. J. 2021, 72, 142–149. [Google Scholar] [CrossRef]
- Chou, R.; Cuevas, C.; Fu, R.; Devine, B.; Wasson, N.; Ginsburg, A.; Zakher, B.; Pappas, M.; Graham, E.; Sullivan, S.D. Imaging Techniques for the Diagnosis of Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis. Ann. Intern. Med. 2015, 162, 697–711. [Google Scholar] [CrossRef]
- Lee, Y.J.; Lee, J.M.; Lee, J.S.; Lee, H.Y.; Park, B.H.; Kim, Y.H.; Han, J.K.; Choi, B.I. Hepatocellular Carcinoma: Diagnostic Performance of Multidetector CT and MR Imaging-a Systematic Review and Meta-Analysis. Radiology 2015, 275, 97–109. [Google Scholar] [CrossRef]
- Hanna, R.F.; Miloushev, V.Z.; Tang, A.; Finklestone, L.A.; Brejt, S.Z.; Sandhu, R.S.; Santillan, C.S.; Wolfson, T.; Gamst, A.; Sirlin, C.B. Comparative 13-Year Meta-Analysis of the Sensitivity and Positive Predictive Value of Ultrasound, CT, and MRI for Detecting Hepatocellular Carcinoma. Abdom Radiol. 2016, 41, 71–90. [Google Scholar] [CrossRef] [PubMed]
- Terzi, E.; Iavarone, M.; Pompili, M.; Veronese, L.; Cabibbo, G.; Fraquelli, M.; Riccardi, L.; De Bonis, L.; Sangiovanni, A.; Leoni, S.; et al. Contrast Ultrasound LI-RADS LR-5 Identifies Hepatocellular Carcinoma in Cirrhosis in a Multicenter Restropective Study of 1006 Nodules. J. Hepatol. 2018, 68, 485–492. [Google Scholar] [CrossRef]
- Manini, M.A.; Sangiovanni, A.; Fornari, F.; Piscaglia, F.; Biolato, M.; Fanigliulo, L.; Ravaldi, E.; Grieco, A.; Colombo, M. Study Participants Clinical and Economical Impact of 2010 AASLD Guidelines for the Diagnosis of Hepatocellular Carcinoma. J. Hepatol. 2014, 60, 995–1001. [Google Scholar] [CrossRef] [PubMed]
- Ronot, M.; Clift, A.K.; Vilgrain, V.; Frilling, A. Functional Imaging in Liver Tumours. J. Hepatol. 2016, 65, 1017–1030. [Google Scholar] [CrossRef]
- Bertagna, F.; Bertoli, M.; Bosio, G.; Biasiotto, G.; Sadeghi, R.; Giubbini, R.; Treglia, G. Diagnostic Role of Radiolabelled Choline PET or PET/CT in Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis. Hepatol. Int. 2014, 8, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Ghidaglia, J.; Golse, N.; Pascale, A.; Sebagh, M.; Besson, F.L. 18F-FDG /18F-Choline Dual-Tracer PET Behavior and Tumor Differentiation in HepatoCellular Carcinoma. A Systematic Review. Front. Med. 2022, 9, 924824. [Google Scholar] [CrossRef] [PubMed]
- Sharma, B.; Martin, A.; Zerizer, I. Positron Emission Tomography-Computed Tomography in Liver Imaging. Semin. Ultrasound CT MR 2013, 34, 66–80. [Google Scholar] [CrossRef]
- Signore, G.; Nicod-Lalonde, M.; Prior, J.O.; Bertagna, F.; Muoio, B.; Giovanella, L.; Furlan, C.; Treglia, G. Detection Rate of Radiolabelled Choline PET or PET/CT in Hepatocellular Carcinoma: An Updated Systematic Review and Meta-Analysis. Clin. Transl. Imaging 2019, 7, 237–253. [Google Scholar] [CrossRef]
- Israeli, R.S.; Powell, C.T.; Fair, W.R.; Heston, W.D. Molecular Cloning of a Complementary DNA Encoding a Prostate-Specific Membrane Antigen. Cancer Res. 1993, 53, 227–230. [Google Scholar]
- Horoszewicz, J.S.; Kawinski, E.; Murphy, G.P. Monoclonal Antibodies to a New Antigenic Marker in Epithelial Prostatic Cells and Serum of Prostatic Cancer Patients. Anticancer Res. 1987, 7, 927–935. [Google Scholar]
- Wester, H.-J.; Schottelius, M. PSMA-Targeted Radiopharmaceuticals for Imaging and Therapy. Semin. Nucl. Med. 2019, 49, 302–312. [Google Scholar] [CrossRef]
- Sartor, O.; de Bono, J.; Chi, K.N.; Fizazi, K.; Herrmann, K.; Rahbar, K.; Tagawa, S.T.; Nordquist, L.T.; Vaishampayan, N.; El-Haddad, G.; et al. Lutetium-177-PSMA-617 for Metastatic Castration-Resistant Prostate Cancer. N. Engl. J. Med. 2021, 385, 1091–1103. [Google Scholar] [CrossRef] [PubMed]
- Jadvar, H.; Calais, J.; Fanti, S.; Feng, F.; Greene, K.L.; Gulley, J.L.; Hofman, M.; Koontz, B.F.; Lin, D.W.; Morris, M.J.; et al. Appropriate Use Criteria for Prostate-Specific Membrane Antigen PET Imaging. J. Nucl. Med. 2022, 63, 59–68. [Google Scholar] [CrossRef]
- Sadeghi, R.; Treglia, G. Systematic Reviews and Meta-Analyses of Diagnostic Studies: A Practical Guideline. Clin. Transl. Imaging 2017, 5, 83–87. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef] [PubMed]
- QUADAS-2: A Revised Tool for the Quality Assessment of Diagnostic Accuracy Studies|Annals of Internal Medicine. Available online: https://www.acpjournals.org/doi/10.7326/0003-4819-155-8-201110180-00009 (accessed on 21 August 2022).
- Higgins, J.P.T.; Thompson, S.G. Quantifying Heterogeneity in a Meta-Analysis. Stat. Med. 2002, 21, 1539–1558. [Google Scholar] [CrossRef] [PubMed]
- Kesler, M.; Levine, C.; Hershkovitz, D.; Mishani, E.; Menachem, Y.; Lerman, H.; Zohar, Y.; Shibolet, O.; Even-Sapir, E. 68Ga-PSMA Is a Novel PET-CT Tracer for Imaging of Hepatocellular Carcinoma: A Prospective Pilot Study. J. Nucl. Med. 2019, 60, 185–191. [Google Scholar] [CrossRef]
- Kuyumcu, S.; Has-Simsek, D.; Iliaz, R.; Sanli, Y.; Buyukkaya, F.; Akyuz, F.; Turkmen, C. Evidence of Prostate-Specific Membrane Antigen Expression in Hepatocellular Carcinoma Using 68Ga-PSMA PET/CT. Clin. Nucl. Med. 2019, 44, 702–706. [Google Scholar] [CrossRef]
- Kunikowska, J.; Cieślak, B.; Gierej, B.; Patkowski, W.; Kraj, L.; Kotulski, M.; Zieniewicz, K.; Królicki, L. [68 Ga]Ga-Prostate-Specific Membrane Antigen PET/CT: A Novel Method for Imaging Patients with Hepatocellular Carcinoma. Eur. J. Nucl. Med. Mol. Imaging 2021, 48, 883–892. [Google Scholar] [CrossRef]
- Gündoğan, C.; Ergül, N.; Çakır, M.S.; Kılıçkesmez, Ö.; Gürsu, R.U.; Aksoy, T.; Çermik, T.F. 68Ga-PSMA PET/CT Versus 18F-FDG PET/CT for Imaging of Hepatocellular Carcinoma. Mol. Imaging Radionucl. Ther. 2021, 30, 79–85. [Google Scholar] [CrossRef]
- Hirmas, N.; Leyh, C.; Sraieb, M.; Barbato, F.; Schaarschmidt, B.M.; Umutlu, L.; Nader, M.; Wedemeyer, H.; Ferdinandus, J.; Rischpler, C.; et al. 68Ga-PSMA-11 PET/CT Improves Tumor Detection and Impacts Management in Patients with Hepatocellular Carcinoma. J. Nucl. Med. 2021, 62, 1235–1241. [Google Scholar] [CrossRef] [PubMed]
- Thompson, S.M.; Suman, G.; Torbenson, M.S.; Chen, Z.-M.E.; Jondal, D.E.; Patra, A.; Ehman, E.C.; Andrews, J.C.; Fleming, C.J.; Welch, B.T.; et al. PSMA as a Theranostic Target in Hepatocellular Carcinoma: Immunohistochemistry and 68 Ga-PSMA-11 PET Using Cyclotron-Produced 68 Ga. Hepatol. Commun. 2022, 6, 1172–1185. [Google Scholar] [CrossRef]
- Farolfi, A.; Telo, S.; Castellucci, P.; Morais de Campos, A.L.; Rosado-de-Castro, P.H.; Altino de Almeida, S.; Artigas, C.; Scarlattei, M.; Leal, A.; Deandreis, D.; et al. Lung Uptake Detected by 68Ga-PSMA-11 PET/CT in Prostate Cancer Patients with SARS-CoV-2: A Case Series. Am. J. Nucl. Med. Mol. Imaging 2021, 11, 300–306. [Google Scholar]
- Annunziata, S.; Pizzuto, D.A.; Treglia, G. Diagnostic Performance of PET Imaging Using Different Radiopharmaceuticals in Prostate Cancer According to Published Meta-Analyses. Cancers 2020, 12, 2153. [Google Scholar] [CrossRef]
- Silver, D.A.; Pellicer, I.; Fair, W.R.; Heston, W.D.; Cordon-Cardo, C. Prostate-Specific Membrane Antigen Expression in Normal and Malignant Human Tissues. Clin. Cancer Res. 1997, 3, 81–85. [Google Scholar] [PubMed]
- Rizzo, A.; Dall’Armellina, S.; Pizzuto, D.A.; Perotti, G.; Zagaria, L.; Lanni, V.; Treglia, G.; Racca, M.; Annunziata, S. PSMA Radioligand Uptake as a Biomarker of Neoangiogenesis in Solid Tumours: Diagnostic or Theragnostic Factor? Cancers 2022, 14, 4039. [Google Scholar] [CrossRef]
- Conway, R.E.; Rojas, C.; Alt, J.; Nováková, Z.; Richardson, S.M.; Rodrick, T.C.; Fuentes, J.L.; Richardson, N.H.; Attalla, J.; Stewart, S.; et al. Prostate-Specific Membrane Antigen (PSMA)-Mediated Laminin Proteolysis Generates a pro-Angiogenic Peptide. Angiogenesis 2016, 19, 487–500. [Google Scholar] [CrossRef] [PubMed]
- Muto, J.; Shirabe, K.; Sugimachi, K.; Maehara, Y. Review of Angiogenesis in Hepatocellular Carcinoma. Hepatol. Res. 2015, 45, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.-X.; Zou, S.-J.; Li, D.; Zhou, J.-Y.; Cheng, Z.-T.; Zhao, J.; Zhu, Y.-L.; Kuang, D.; Zhu, X.-H. Prostate-Specific Membrane Antigen Expression in Hepatocellular Carcinoma, Cholangiocarcinoma, and Liver Cirrhosis. World J. Gastroenterol. 2020, 26, 7664–7678. [Google Scholar] [CrossRef]
- Delbeke, D.; Martin, W.H.; Sandler, M.P.; Chapman, W.C.; Wright, J.K.; Pinson, C.W. Evaluation of Benign vs Malignant Hepatic Lesions with Positron Emission Tomography. Arch. Surg. 1998, 133, 510–515; discussion 515–516. [Google Scholar] [CrossRef]
- Böhm, B.; Voth, M.; Geoghegan, J.; Hellfritzsch, H.; Petrovich, A.; Scheele, J.; Gottschild, D. Impact of Positron Emission Tomography on Strategy in Liver Resection for Primary and Secondary Liver Tumors. J. Cancer Res. Clin. Oncol. 2004, 130, 266–272. [Google Scholar] [CrossRef] [PubMed]
- Asman, Y.; Evenson, A.R.; Even-Sapir, E.; Shibolet, O. [18F]Fludeoxyglucose Positron Emission Tomography and Computed Tomography as a Prognostic Tool before Liver Transplantation, Resection, and Loco-Ablative Therapies for Hepatocellular Carcinoma. Liver Transpl. 2015, 21, 572–580. [Google Scholar] [CrossRef] [PubMed]
- Ronca, R.; Benkheil, M.; Mitola, S.; Struyf, S.; Liekens, S. Tumor Angiogenesis Revisited: Regulators and Clinical Implications. Med. Res. Rev. 2017, 37, 1231–1274. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.; Zhu, W.; Du, J.; Yang, C.; Han, B.; Zhou, D.; Huo, L.; Zhuang, J. 11C-Acetate Positron Emission Tomography Is More Precise than 18F-Fluorodeoxyglucose Positron Emission Tomography in Evaluating Tumor Burden and Predicting Disease Risk of Multiple Myeloma. Sci. Rep. 2021, 11, 22188. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Kim, T.-S.; Kang, S.H.; Kim, H.B.; Park, J.-W.; Kim, S.-K. 11C-Acetate and 18F-Fluorodeoxyglucose Positron Emission Tomography/Computed Tomography Dual Imaging for the Prediction of Response and Prognosis after Transarterial Chemoembolization. Medicine 2018, 97, e12311. [Google Scholar] [CrossRef]
- Li, C.-W.; Kuo, Y.C.; Chen, C.-Y.; Kuo, Y.-T.; Chiu, Y.-Y.; She, F.-O.; Liu, G.-C. Quantification of Choline Compounds in Human Hepatic Tumors by Proton MR Spectroscopy at 3 T. Magn. Reson Med. 2005, 53, 770–776. [Google Scholar] [CrossRef]
- Roivainen, A.; Forsback, S.; Grönroos, T.; Lehikoinen, P.; Kähkönen, M.; Sutinen, E.; Minn, H. Blood Metabolism of [Methyl-11C]Choline; Implications for in Vivo Imaging with Positron Emission Tomography. Eur. J. Nucl. Med. 2000, 27, 25–32. [Google Scholar] [CrossRef]
- Podo, F. Tumour Phospholipid Metabolism. NMR Biomed. 1999, 12, 413–439. [Google Scholar] [CrossRef]
- Chen, Y.; Pullambhatla, M.; Foss, C.A.; Byun, Y.; Nimmagadda, S.; Senthamizhchelvan, S.; Sgouros, G.; Mease, R.C.; Pomper, M.G. 2-(3-{1-Carboxy-5-[(6-[18F]Fluoro-Pyridine-3-Carbonyl)-Amino]-Pentyl}-Ureido)-Pentanedioic Acid, [18F]DCFPyL, a PSMA-Based PET Imaging Agent for Prostate Cancer. Clin. Cancer Res. 2011, 17, 7645–7653. [Google Scholar] [CrossRef]
- Cardinale, J.; Schäfer, M.; Benešová, M.; Bauder-Wüst, U.; Leotta, K.; Eder, M.; Neels, O.C.; Haberkorn, U.; Giesel, F.L.; Kopka, K. Preclinical Evaluation of 18F-PSMA-1007, a New Prostate-Specific Membrane Antigen Ligand for Prostate Cancer Imaging. J. Nucl. Med. 2017, 58, 425–431. [Google Scholar] [CrossRef]
- Giesel, F.L.; Hadaschik, B.; Cardinale, J.; Radtke, J.; Vinsensia, M.; Lehnert, W.; Kesch, C.; Tolstov, Y.; Singer, S.; Grabe, N.; et al. F-18 Labelled PSMA-1007: Biodistribution, Radiation Dosimetry and Histopathological Validation of Tumor Lesions in Prostate Cancer Patients. Eur. J. Nucl. Med. Mol. Imaging 2017, 44, 678–688. [Google Scholar] [CrossRef] [PubMed]
- Giesel, F.L.; Will, L.; Lawal, I.; Lengana, T.; Kratochwil, C.; Vorster, M.; Neels, O.; Reyneke, F.; Haberkon, U.; Kopka, K.; et al. Intraindividual Comparison of 18F-PSMA-1007 and 18F-DCFPyL PET/CT in the Prospective Evaluation of Patients with Newly Diagnosed Prostate Carcinoma: A Pilot Study. J. Nucl. Med. 2018, 59, 1076–1080. [Google Scholar] [CrossRef] [PubMed]
- Uijen, M.J.M.; Derks, Y.H.W.; Merkx, R.I.J.; Schilham, M.G.M.; Roosen, J.; Privé, B.M.; van Lith, S.A.M.; van Herpen, C.M.L.; Gotthardt, M.; Heskamp, S.; et al. PSMA Radioligand Therapy for Solid Tumors Other than Prostate Cancer: Background, Opportunities, Challenges, and First Clinical Reports. Eur. J. Nucl. Med. Mol. Imaging 2021, 48, 4350–4368. [Google Scholar] [CrossRef]
- Rizzo, A.; Annunziata, S.; Salvatori, M. Side Effects of Theragnostic Agents Currently Employed in Clinical Practice. Q. J. Nucl. Med. Mol. Imaging 2021, 65, 315–326. [Google Scholar] [CrossRef]
- Dondi, F.; Albano, D.; Cerudelli, E.; Gazzilli, M.; Giubbini, R.; Treglia, G.; Bertagna, F. Radiolabelled PSMA PET/CT or PET/MRI in Hepatocellular Carcinoma (HCC): A Systematic Review. Clin. Transl. Imaging 2020, 8, 461–467. [Google Scholar] [CrossRef]


| Authors [Ref.] | Year | Country | Study Design/Number of Involved Centers | Funding Sources |
|---|---|---|---|---|
| Kesler et al. [28] | 2018 | Israel | Prospective/Monocentric | None declared |
| Kuyumcu et al. [29] | 2019 | Turkey | Prospective/Monocentric | None declared |
| Kunikowska et al. [30] | 2020 | Poland | Prospective/Monocentric | None declared |
| Gündoğan et al. [31] | 2021 | Turkey | Prospective/Monocentric | None declared |
| Hirmas et al. [32] | 2021 | Germany | Retrospective/Monocentric | None declared |
| Thompson et al. [33] | 2022 | USA | Prospective/Monocentric | None declared |
| Authors [Ref.] | Sample Size (No. Patients) | Mean/Median Age (Years) | Gender (Male %) | Clinical Setting (No. Patients) | Child-Pugh (No. Patients—Score) | PSMA Staining | Comparative Imaging |
|---|---|---|---|---|---|---|---|
| Kesler et al. [28] | 7 | Median: 56 | 71% | staging (6) restaging (1) | 3-A 4-B | NVE | [18F]FDG PET/CT; ceCT; MRI |
| Kuyumcu et al. [29] | 19 | Mean: 57.8 | 84% | restaging (19) | n.a. | n.a. | [18F]FDG PET/CT |
| Kunikowska et al. [30] | 15 | Mean 55.6 | 87% | staging (10) restaging (5) | 14-A 1-B | NVE | ceCT; MRI |
| Gündoğan et al. [31] | 14 | Mean: 63.8 | 93% | staging (12) restaging (2) | n.a | n.a. | [18F]FDG PET/CT; MRI |
| Hirmas et al. [32] | 40 | Median: 65 | 85% | staging (27) restaging (13) | 33-A 7-B | n.a. | ceCT |
| Thompson et al. [33] | 31 | Median: 66 | 74% | staging (31) | n.a | NVE | ceCT; MRI |
| Authors [Ref.] | Tracer | Hybrid Imaging | Tomograph | Administered Activity | Uptake Time (Minutes) | Image Analysis |
|---|---|---|---|---|---|---|
| Kesler et al. [28] | [68Ga]Ga-PSMA-11 | PET/CT | Discovery 690 (GE ®) | 148 MBq | n.a | Qualitative and semi- quantitative (SUVmin, SUVmax, TBR) |
| Kuyumcu et al. [29] | [68Ga]Ga-PSMA-11 | PET/CT | Biograph TruePont (Siemens ®) | 2.5 MBq/kg ± 10% | 60 | Qualitative and semi-quantitative (SUVmax, TBR) |
| Kunikowska et al. [30] | [68Ga]Ga-PSMA-11 | PET/CT | Biograph 64 TruePoint (Siemens ®) | 2 MBq/kg | 60 | Qualitative and semi-quantitative (SUVmean, SUVmax, TBR) |
| Gündoğan et al. [31] | [68Ga]Ga-PSMA-11 | PET/CT | mCT 20 ultra HD LSO (Siemens ®) | 2-2.5 MBq/kg | 60 | Qualitative and semi-quantitative (SUVmax, TBR) |
| Hirmas et al. [32] | [68Ga]Ga-PSMA-11 | PET/CT | Biograph 128 mCT; Biograph Vision (Siemens ®) | Median: 112.5 MBq | Median: 78 | Qualitative and semi-quantitative (SUVmax) |
| Thompson et al. [33] | [68Ga]Ga-PSMA-11 | PET/CT; PET/MRI | Biograph Vision 600 (Siemens ®); Signa (GE ®) | 185 MBq ± 10% | 90 ± 15 | Qualitative and semi-quantitative (SUVmean, SUVmax, TBR) |
| Study | Sample Size | Detection Rate (%) | 95% CI | Weight (%) | |
|---|---|---|---|---|---|
| Fixed | Random | ||||
| Kesler et al. [28] | 7 | 85.714 | 42.128 to 99.639 | 6.06 | 10.26 |
| Kuyumku et al. [29] | 19 | 84.211 | 60.422 to 96.617 | 15.15 | 17.05 |
| Kunikowska et al. [30] | 15 | 100.000 | 78.198 to 100.000 | 12.12 | 15.36 |
| Gündoğan et al. [31] | 14 | 92.857 | 66.132 to 99.819 | 11.36 | 14.87 |
| Hirmas et al. [32] | 40 | 90.000 | 76.336 to 97.207 | 31.06 | 22.03 |
| Thompson et al. [33] | 31 | 67.742 | 48.627 to 83.318 | 24.24 | 20.43 |
| Total (fixed effects) | 126 | 85.118 | 77.881 to 90.712 | 100 | 100 |
| Total (random effects) | 126 | 85.942 | 75.262 to 93.970 | 100 | 100 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rizzo, A.; Racca, M.; Albano, D.; Dondi, F.; Bertagna, F.; Annunziata, S.; Treglia, G. Can PSMA-Targeting Radiopharmaceuticals Be Useful for Detecting Hepatocellular Carcinoma Using Positron Emission Tomography? An Updated Systematic Review and Meta-Analysis. Pharmaceuticals 2022, 15, 1368. https://doi.org/10.3390/ph15111368
Rizzo A, Racca M, Albano D, Dondi F, Bertagna F, Annunziata S, Treglia G. Can PSMA-Targeting Radiopharmaceuticals Be Useful for Detecting Hepatocellular Carcinoma Using Positron Emission Tomography? An Updated Systematic Review and Meta-Analysis. Pharmaceuticals. 2022; 15(11):1368. https://doi.org/10.3390/ph15111368
Chicago/Turabian StyleRizzo, Alessio, Manuela Racca, Domenico Albano, Francesco Dondi, Francesco Bertagna, Salvatore Annunziata, and Giorgio Treglia. 2022. "Can PSMA-Targeting Radiopharmaceuticals Be Useful for Detecting Hepatocellular Carcinoma Using Positron Emission Tomography? An Updated Systematic Review and Meta-Analysis" Pharmaceuticals 15, no. 11: 1368. https://doi.org/10.3390/ph15111368
APA StyleRizzo, A., Racca, M., Albano, D., Dondi, F., Bertagna, F., Annunziata, S., & Treglia, G. (2022). Can PSMA-Targeting Radiopharmaceuticals Be Useful for Detecting Hepatocellular Carcinoma Using Positron Emission Tomography? An Updated Systematic Review and Meta-Analysis. Pharmaceuticals, 15(11), 1368. https://doi.org/10.3390/ph15111368







