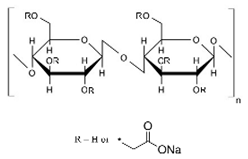
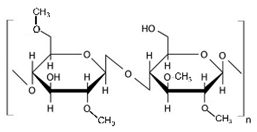
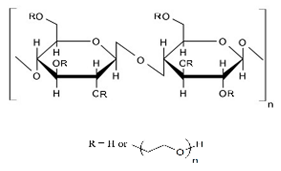
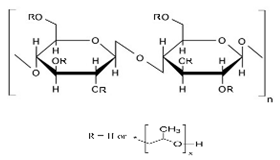
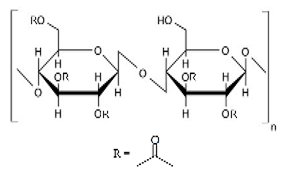
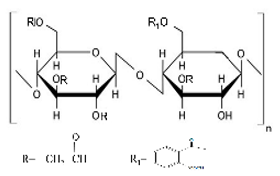
10.1.1. Methylcellulose
Methylcellulose is a water-soluble, non-toxic, tasteless, and odorless cellulose derivative (
Table 2). It exhibits sol-gel phase transition that is temperature-sensitive (LCST polymer) [
131], and the mechanism of gelation is a hydrophobic interaction between the molecules that contain a methoxy substitution [
103]. Various thermo-responsive ocular drug delivery can be made by use of phase transition, and the critical gelling concentration depends on polymer–polymer interactions, polymer–solvent interactions, hydrophilic–lipophilic characters, molecular weight, and the flexibility of a chain. Gelation can be affected by a high concentration of electrolytes, surfactants, sugar, and natural gums; this decreases the polymer hydration and gelation temperature [
126]. As the concentration of the MC increases, the gelation temperature decrease linearly [
132].
Yidan Wei et al. studied the in-situ gel of Betaxolol hydrochloride, which is used as a model drug, poloxamer 407, where methylcellulose was used as the carrier. In this study, a thermosensitive in situ gel was formulated and evaluated. In vitro study shows that incorporation of HPMC 606W (4%) into poloxamer 407 (15%) and PEG 4000 into MC (2%) gives a significant gelation temperature and a sustained release the same as the BH eye drop; the in vivo study also shows the same drug concentration in cornea, iris ciliary, and aqueous humor. The concentration of methylcellulose increases the gelation temperature around 45 °C, because as the concentration increases, the hydrophobic interaction of the MC increases, causing a decrease in the gelation temperature. It is not fit for ocular delivery. PEG is hydrophilic and leads to an increased hydrophobic interaction by acting as a proton acceptor; therefore, in this study, they kept the MC at 2% constant, and for a different proportion of PEG. PEG decreases the extension of MC in water. A large MW PEG (more than 1500) is long enough to decrease the extension of MC, and therefore PEG 1500/4000/6000 (5%) had a gelation temperature of around 34 °C, which is suitable for ocular delivery [
132]. Another study related to MC was done by Xia et al., where needle clogging by microparticles is a challenge for injectable ocular delivery. In this study, hyaluronic acid (HA) and MC were used because they are applicable for ocular injection; this polymer was blended with Sunitinib malate-loaded PLGA microparticles (MPs); this polymer has shear thinning viscous properties, which eases the injection by a fine-gauged needle. HA and MC decreases the burst release and extend the release of the drug from the microparticles. The particles were entrapped in the HA and MC mesh-like network as this polymer has sufficient viscosity for retention of microparticles for a prolonged period. The physical adhesion or attachment to the conjunctiva may also extend the release of drugs [
133]. A similar study was done by Nagai et al.; in this study, an in-situ gel was prepared by assimilating TL-NPs and the methylcellulose (0.5–3%) to get the prolonged residence time of the drug. The drug is more dispersed in the formulation with MC, and diffusion decreases as MC are added. An in vivo study shows the TL quantity increase in lacrimal fluid. An optimal amount of MC (0.5–1.5%) increases the TL in the cornea and conjunctiva, and the anti-inflammatory effect of the drug was seen. As the concentration of MC (3%) is in excess, the anti-inflammatory effect was reduced compared with the TL-NPs formulation of MC (0.5–1.5%). Therefore MC (0.5–1.5%) has a prolonged residence time in the pre-corneal and pre-conjunctival part of TL [
134]. Wafa et al. also studied increasing the residence time of Pilocarpine nitrate drug, an in-situ gel/film-forming system. In this study, they used polyvinyl alcohol (PVA) as a film former, sodium alginate as bio-adhesive, and the effect of CMC, MC, Carbopol, and PVP was studied. All inserts had significant bio-adhesion in the in vitro study, and showed the matrix diffusion kinetics of the formulations [
135].
10.1.2. Hydroxypropyl Methylcellulose
HPMC is also called Hypromellose and it is a white or pale white cellulose used for a different purpose. It is a hydrophilic derivative used in oral and oro-mucosal drug delivery as a controlled release system; it can swell and form a gel, is stable in the pH range of 3–11, and cannot be cleavable by a gastric enzyme [
124,
136]. HPMC, which is produced by a hydroxyl group of cellulose, is partially etherified by a methyl group and a small quantity is substituted by hydroxypropyl groups. This is the most widely used polymer among the different derivatives of cellulose as it is a biodegradable [
137] and biocompatible material [
138,
139], and has transparency and rheological properties [
140] (
Table 3). HPMC is a semi-synthetic dietary fiber of cellulose; it is a carbohydrate containing anhydrous glucose units. It is used as a prolonged release excipient [
139] emulsifier, thickener, stabilizer, and forms a viscous solution [
141] when it come into contact with water or GI fluid [
142]. It is inert to many drugs and is used in capsule form [
143] and has a good encapsulation efficacy and has the option of 3D printing [
144]. It is used widely due to regulatory acceptance, ease of manufacture, and preparation of the control release formulations [
145]. HPMC-based ongoing clinical trials are mentioned in
Table 4 HPMC has negative thermo-sensitivity, it has a lower critical solution temperature (LCST) of 50 °C. Below this temperature, HPMC is soluble in water, and above it is not soluble when gelation takes place. However, on the eye surface, the temperature is less than LCST, and thus has less effect on viscosity [
146,
147]. HPMC K4M and HPMC E4M possess shear thinning properties [
144]. HPMC is produced by various companies and is available in several trademarks such as METHOCEL (Dow Chemical Company, Rochester, NY, United State of America (USA)), BENECEL (Ashland, Rotterdam, The Netherlands), METOLOSE, PHARMACOAT (Shinetsu Chemical Company, Tokyo, Japan), and AFFINISOL (Dupont, Brooklyn, NY, USA) [
124]. This polymer has a sol-gel phase transition that is a temperature-sensitive LCST of the polymer. The gelling concentration of various cellulose derivatives depends on the polymer–solvent interaction, polymer–polymer interaction, molecular weight, the flexibility of the chain, and other characteristics of polymers. Gelation is affected by the presence of a high concentration of electrolytes, sugar, natural gums, and surfactants; this decreases the hydration of the polymer and indirectly by the salting-out process due to the gelation temperature [
126]. The transition temperature of HPMC is 75 to 90%. The gelation temperature can be lower up to 40% by the addition of sodium chloride by lowering the hydroxypropyl molar substitution [
148]. Minitablets, which are used in the eyeball, are made of various polymers, e.g., cellulose derivatives such as HPMC, CMC, and HEC [
94].
HPMC is used for enhancing the bioavailability by increasing the penetration of hydrophobic drug molecules [
149]. Liu et al. examined the ocular delivery of Fk506 loaded nanomicelles in an amino-terminated polyethylene glycol block poly (D, L)-lactic acid and HPMC, which shows enhanced bioavailability and efficacy of FK506 (tacrolimus) for ocular disorder therapy in anti-allograft rejection; the nanomicelles were prepared by solvent evaporation-induced self-assembly in an aqueous medium and have a diameter of 101.4 ± 1.3 nm. These nanomicelles that solubilized the drug were evaluated for their stability, drug loading, encapsulating efficacy, surface tension, and in vitro release of the drug, and results show that the nanomicelles were more suitable for intraocular then the 0.05% suspension drops of the same. In vitro studies show a significantly high quantity of FK506 permeated and an in vivo study shows an increased concentration and prolonged retention of FK506 [
150]. Elkasabgy et al. explored the potential of HPMC as a precipitation inhibitor. The solubility and bioavailability of econazole was increased by preparing an ocular supersaturated self-emulsifying drug delivery system (S-SNEDDS) using various oils, surfactants, and co-surfactants. Globule size, polydispersity index, and irritation potential was tested by using Hen’s Egg Test-Chorioallantoic membrane (HET-CAM). The precipitation inhibitor effects were studied in an in vitro precipitation test of S-SNEDDS, and permeation of econazole was studied in rabbits. The in vitro results show the use of HPMC sustains the S-SNEDDS release by inhibiting econazole precipitation; this shows high Cmax, Tmax, and AUC08, and successful formulation with improving bioavailability [
151]. Nanda et al. also work on the permeation enhancement of mucoadhesive ocular film by the use of HPMC. He worked on the corneal permeation improvement of amlodipine anti-inflammatory drug and the effect of sulpho butyl-ether β cyclodextrin, and tested these on a carrageenan-induced rabbit model. Maximum swelling and higher erosion were seen in the film without cyclodextrin. A big improvement in the drug release and permeation was seen in sulfo butyl ether β-cyclodextrin (SBCD). The in vitro study showed enhanced amlodipine release and ocular permeation was seen in the HPMC complex with cyclodextrin and SBCD, both at a higher level. Results show enhanced permeation of amlodipine-HPMC film with sulpho butyl ether β-cyclodextrin [
152]. Another bioavailability enhancement study was done by Morsi et al.; he studied the availability improvement and prolongation of ketorolac tromethamine for postoperative inflammation. In this, the gelling capacity pluronic 1 F-127 was 20% and pluronic1 F-127 14%/x HPMC K4M (14%). The mucoadhesive strength was increased by the addition of HPMC. The result shows sustained release, enhanced bioavailability, and prolonged residence time of the nano-dispersion of ketorolac tromethamine into the in situ gel for ocular delivery [
153].
HPMC was studied for sustained release of ocular delivery. Wei et al. determined that in in vitro studies of 4% HPMC 606W in 15% P407 solution and 5% PEG4000 in 2% MC solution gives a gelation temperature and a sustained-release effect. In vivo studies showed a higher drug concentration in the cornea, aqueous humor, iris, and ciliary after 4 h to that of commercial BH suspension eye drops with Betaxolol hydrochloride (model drug). In poloxamer 407, methylcellulose is used as the carriers. A two times higher AUC and MRI of the in situ gelling eye drops was found comparable with the commercial product [
132]. Ela et al. studied the HPMC to increase the permeation of an ocular antifungal drug (fluconazole) by using the anti-solvent precipitation non-ionization method. The stabilizers used were HPMC E3, xanthan gum, polyvinyl pyrrolidone K30 (PVP), Pluronic F-127 (PL F 127), Kollicoat IR (KL), and sodium lauryl sulfate (SLS). By using a goat cornea, ex vivo studies were done. The result of the ex vivo study shows improvement in treated fluconazole over untreated fluconazole. Optimization of both treated and untreated fluconazole was studied in rabbits. Particle size and zeta potential vary according to the type and pharmacokinetics parameter of the drug [
154]. A similar study was performed by Gugleva et al., who worked on the thermosensitivity of situ gels for ocular delivery. The polymer used in their study was poloxamer 407 and by combining it with HPMC was made by the cold method and sol-gel transition. Gelling time and capacity were evaluated, and HPMC leads to a reduced phase-transition temperature. The gelation temperature (34 °C), pseudoplastic flow, and very good physical stability were found in doxycycline niosome in an in-situ gel form of 15%
w/
w poloxamer and 1.5%
w/
w HPMC. An in vitro study shows prolonged and sustained release of doxycycline than noisome alone. Results showed a significant therapeutic concentration and a sustained release of the drug [
155]. In another study of an in-situ gelling system, the controlled release of latanoprost by the use of HPMC was studied by Khattab et al. An optimal factorial design was built of 4-factor concentrations of P127, P68, and HPMC, depending on the sol to gel transition temperature, the strength of the gel, and the mucoadhesive properties. The optimal formula showed a sol-gel transition of 34.3 °C, muco-adhesion of 0.06, gel strength of 23.13 g, a flux of 11.4 µg/cm
2/h, even the anti-glaucoma effects rose 2.9fold and there was a reduction in the intraocular pressure (IOP) after 30 min and extended release to 8 h compared to conventional eye drops. This thermosensitive in situ gel of latanoprost is a good alternative to conventional drops [
156].
HPMC was also used for drug recovery and to decrease the degradation of drugs. Terreni et al. studied antimicrobial peptide (hLF 1-11) derived from the N-terminus of lactoferrin, which is chemically, physically, and biologically unstable. In this study, the solid matrices containing mucoadhesive polymers were evaluated for rheology, hydration time, bio-adhesive property, drug content, and in vitro release of the formulation. The HPMC /T2/HA/hLF-11fd shows good drug recovery and chemical degradation was not seen for 6 months. This is a very promising result for pre-corneal delivery of anti-microbial peptides onto the ocular surface [
157]. In another study, Maharana et al. showed that HPMC is used for the tear substitutes for dry eyes; in this study, they used CMC (0.5%), hydroxypropyl-guar, which contain polyethylene glycol 400 or propylene glycol, and HPMC (0.3%). In this, study they divided the patients into three groups: group-1 (CMC), group-2 (PEG/PG), and group-3 (HPMC). The result showed that HPMC and hydroxypropyl-guar containing PEG/PG was better than the CMC but HPMC improved more than PEG/PG [
125].
Table 5 includes the comparison between the free drug and drug with cellulosic polymers and
Table 6 indicates the marketed products of polymers.
Table 3.
Application of HPMC in ocular drug delivery.
Table 3.
Application of HPMC in ocular drug delivery.
| Cellulosic Polymer | Drug Used | Application of Polymer | Effect on Drug Property | Ref |
|---|
| HPMC | Fk506 (tacrolimus) | Improve bioavailability and efficacy, prolonged retention | Reduced surface tension of nanomicelles solution (33.61 ± 0.29 Mn/m) caused easy contact with ocular surface leading to improved retention and enhancing permeation and in-turn bioavailability | [150] |
| Econazole | Increase the solubility and bioavailability | 5 and 10% HPMC 15cp was preserved the supersaturation state of drug loaded SEDDS | [151] |
| Ketorolac tromethamine | Sustain release, enhance bioavailability, and prolonged residence time | Enhanced AUC, Tmax and relative bioavailability that is 2.742 ± 0.11 µgh/mL, 11.57 ± 0.73 h and 250% | [153] |
| Betaxolol hydrochloride | Prolonged release upto 85% in 6 h which is similar to higher concentration of P407 alone | Enhanced in AUC and MRT by 2 times compared to commercial preparation | [132] |
| Fluconazole | Increase the permeation and stabilizer | Nanoparticle contaning drug was stabilized by 0.5 to 1% HPMC | [154] |
| Doxycycline | Prolong and sustain release | Decreased burst release of drug | [155] |
| Latanoprost | Controlled release upto 8 h | Anti-glucoma effect of in situ gel was 2.9 fold greater than eye drop | [156] |
| Antimicrobial peptide (hLF 1-11) | Reduce chemical degradation | Mucoadhesive effect of HPMC improves the peptide interaction with ocular surface thus prevent rapid elimination of formulation | [157] |
| HPMC and CMC | Tear substitutes | OSDI was significantly lower mean in HPMC containing group | [125] |
Table 4.
Clinical trials based on various cellulosic polymers used in ocular drug delivery.
Table 4.
Clinical trials based on various cellulosic polymers used in ocular drug delivery.
| Clinical Trial | Drug Used | Phase | Location of Work | NCT Number | Ref |
|---|
| HPMC 0.3% and sodium hyaluronate 0.18% for ocular surface disease in glaucoma | HPMC and sodium hyaluronate | Not applicable | Bangkok, Thailand | NCT01284439 | [158] |
| Assess the safety and efficacy of CsA ophthalmic gel in subjects with moderate to severe dry eye disease | CsA ophthalmic gel,
Hypromellose eye drop and placebo | 3 | China | NCT04541888 | [159] |
| Effect of topical besifloxacin on ocular surface bacterial microbiota prior to cataract surgery | Besifloxacin, HPMC ophthalmic solution | 1 | Mexico | NCT04542759 | [160] |
| An efficacy and safety study of bimatoprost alone compared with travoprost and timolol in glaucoma or ocular hypertension | Hypromellose (0.3%), Bimatoprost (0.01%), travatan (0.004%), timolol (0.5%) | 4 | Barrie, Ontario, Canada. | NCT01881126 | [161] |
| Efficacy and safety study of bimatoprost alone compared with travoprost and timolol in glaucoma or ocular hypertension | Hypermellose (0.3%), Bimatoprost (0.01%), Travoprost (0.004%), Timolol (0.5%). | 4 | United state | NCT02097719 | [162] |
| Evaluate the safety and efficacy of a new artificial tear for use after LASIK surgery | CMC and glycerin-based artificial tear | Not applicable | United state | NCT00544713 | [163] |
| Safety and efficacy of Alphagan P and Lumigan in subjects previously treated with latanoprost for glaucoma and hypertension | Hypromellose (0.2%), Brimonidine tartrate (0.1%), bimatoprost (0.2%), latanoprost (0.005%). | 4 | United state | NCT01525173 | [164] |
| Efficacy study of ketorolac and HPMC to treat dry eye | Ketorolac and HPMC | 2 | United state | NCT03693183 | [165] |
| The effect of BAK on the blood-aqueous barrier of pseudophakic patients | HPMC and CMC | 4 | Brazil | NCT01280110 | [166] |
| Efficacy, Tolerability, and comfort of Hypromellose eyedrop in patients undergoing LASIK surgery | Pre LASIK Hypromellose (0.3%), post LASIK Hypromellose (0.3%). | 4 | India | NCT00909324 | [167] |
| Assessment of alcon’s ocular image quantification system | Olopatadine HCL, Patanol (0.1%), dextran 70 (0.1%), HPMC (0.3%) | 4 | United state | NCT01282138 | [168] |
| Corneal protection used during cataract surgery | HPEC (2% gel), BSS | Not applicable | China | NCT02363530 | [169] |
| Interval intraocular pressure in intravitreal injection study (IIII) | Hypromellose, travatan, timolol | Not applicable | Hong kong | NCT04868175 | [170] |
Table 5.
Comparison between of Free form of Drug and Drug with Cellulosic Polymers.
Table 5.
Comparison between of Free form of Drug and Drug with Cellulosic Polymers.
| Drug | Cellulosic Polymer Used | Effect of Drug in Free Form | Effect of Drug along with Cellulosic Polymer | Ref |
|---|
| Betaxol HCL | HPMC 606W, MC | No sustain release is seen, AUC and MRT is less and does not have prolonged drug release | Higher drug concentration after 4 h, AUC and MRT of in situ gel was 2 time higher than free drug, have prolonged drug release | [132] |
| Econazole nitrate | HPMC | Econazole under precipitation and have low aqueous solubility | HPMC sustain the supersaturated state by decreasing econazole precipitation, improve aqueous solubility of econazole. | [151] |
| Fluconazole | HPMC | NP is not stable compared to drug along with HPMC, particle size is larger less viscous formulation, permeation and pharmacokinetics parameter is less. | HPMC stabilized the NP formulation, increase polymer concentration reducing the particle size, and increase the viscosity of formulation Fluconazole NP enhance the corneal permeation and improve pharmacokinetics parameters. | [154] |
| Tacrolimus | HPMC | Permeation of drug is less, as it poorly water-soluble drug, therefore have less bioavailability and efficacy | Enhance penetration of hydrophobic drug, improve bioavailability and efficacy of the drug. | [150] |
| Olopatadine HCL | EC | Drug is inefficient because of low bioavailability, | Olopatadine doughnut CL along with EC shows sustained and extended release of drug with limited alteration to optical and swelling property of CL | [171] |
| Timolol maleate and metformin HCL | EC | It had low viscosity their rapid clearance from the eye, intravitreal is only option for delivery of drug to back of the eye so have more side effects and risk of infection and retinal detachment | Oleo-gel prepared from EC provide the viscosity to the formulation and give control or sustain release of drug which reduces the frequency of dosing, release of metformin form gelled emulsion is 1400 h and for timolol it is 2200 h that shows sustained release and drug loading is also increased. | [127] |
| Voriconazole | CMC | Drug have low residence time and bioavailability because of the rapid clearance of drug from the eye | In situ gel improves the residence time and bioavailability of the drug, formulation shows sustain release of drug | [172] |
Table 6.
Marketed products based on cellulosic polymers for eyes.
Table 6.
Marketed products based on cellulosic polymers for eyes.
| Drug | Name of Marketed Products | Dosage Form | Polymer |
|---|
| HPMC | RETAINE HPMC-hypromellose 2910 | Solution/drops | HPMC |
| HPMC | IO Gel (HPMC solution) | Solution | HPMC |
| HPMC | OCCUGEL 2% | Solution | HPMC |
| HPMC | VIBKOOL | Solution | HPMC |
| HPMC | Lubricate | Solution | HPMC |
| HPMC | Eyemist | Eye drops | HPMC |
| HPMC | IRIMIST | Solution | HPMC |
| HPMC | BLINK lubricant | Eye drops | HPMC |
| HPMC | MEDIVISC forte | Eye drops | HPMC |
| HPMC | Tobmat | Eye drops | HPMC |
| Flurbiprofen and HPMC | Flumat | Eye drops | HPMC |
| Sodium CMC | A-CMC | Eye drops | CMC |
| Calcium CMC | CELLU TEARS gel | Eye drops | CMC |
| Naphazoline HCL, Camphor, Menthol and chlorpheniramine maleate | BRISCOOL | Eye drops | CMC |
| Sodium CMC 0.5% | LUBRIZETHIC | Eye Drops | CMC |
10.1.3. Carboxymethyl Cellulose
Carboxymethyl cellulose (CMC) is a biocompatible, biodegradable, non-toxic, and water-soluble ether derivative of cellulose; therefore, it is used for various purposes (
Table 7). CMC is white to cream-colored, odorless, tasteless, free-flowing powder, and sodium CMC is generally called CMC [
173]. It is an anionic, linear anhydrous-glucose polysaccharide, water-soluble, and generally recognized as safe (GRAS) [
174,
175]. By β-1,4-glycosidic bonds the polysaccharide repeating units are connected. CMC differs from cellulose as CMC has anionic carboxymethyl groups (CH
2COOH), which are replaced by the hydrogen atom of a hydroxyl group of cellulose and it was first synthesized in 1918 but the commercial preparation was developed in 1920 in Germany [
176]. Cellulose precursors are corn cob [
177], corn stalk [
178], corn husk [
179], durian rind [
180], maize stalks, pineapple peel [
181], orange peels, sugarcane bagasse [
182], asparagus stalk [
183], and other materials such as waste paper [
184], waste textile [
185], knitted rag [
186], cotton gin waste [
187], waste cotton linter, etc. Apart from pharmaceutical use, it is also used in detergents, food, paper industries, oil drilling mud, and as a hydrogel in delivery systems and so on. There are many patents related to cellulosic polymers (
Table 8). CMC can absorb a large amount of water and swells, and when it swells, the drug diffuses out from the hydrated layer of the swollen mass and shows its effects. Hence, its forms a metallo-polymeric material by chelating with the metal ions [
188].
Neslihan et al. studied the improved residence time and bioavailability of the in situ ocular gel formulation of Voriconazole, used in fungal keratitis treatment. To prepare the thermosensitive in situ ocular gel, poloxamer 407, poloxamer 188, and CMC were used. The formulation prepared by use of this material showed a gelation temperature of 29–34 °C. They were evaluated for sterility, antifungal activity, stability, in vitro drug release, in vivo studies, and ex vivo studies for penetration and permeation. All three formulations showed good sustainability of drug release. This showed a good effect of CMC for increasing the residence time and bioavailability [
172]. Similarly, Hassan et al. studied the enhancement of bioavailability of an in-situ gel of voriconazole for ocular insert loaded with a noisome suspension. In this study, noisome was made with span 40 and span 60 with pluronic L64 and pluronic F127. Then, the noisome was evaluated for entrapment efficacy, poly-dispersity index, mean vesicle size, zeta potential, and in vitro drug release. An in situ gel was made by sodium CMC and sodium alginate and then evaluated for surface morphology, surface pH, water uptake, mucoadhesive properties, and in vitro release; this CMC sustains the release of the drug and prolong its effect [
189]. In another study, sustained release of a drug by the use of CMC was studied by Sarimsakov et al. In this study, he used the soluble antiviral eye films of a polymeric form. The materials used were aqueous-soluble sodium CMC and derivative of sodium CMC that contains a chemically bound natural polyphenol-gossypol with the quantity of polymerization of 630 ± 20 and 0 mole%, where soluble CMC has a degree of substitution of 0.85 ± 2. CelAgrip is the antiviral drug substance, and sodium CMC-CelAgrip showed the prolonged effect of the drug, and the film is transparent and non-irritating [
190]. Another study is about the bioavailability enhancement and prolonging the residence time of beclomethasone dipropionate (BDP), done by Gaballa et al. In this study, glyceryl monooleate (GM) Cubosome was made, and the stabilizer used was poloxamer 407 and Solulan C24. The particle size of Cubosome was 100–278 nm, the EE% was 94%, and they found significant trans-corneal permeability (
p < 0.05). Then, the optimized Cubosome was incorporated into the CMC gel to form a Cubo-gel; this gel shows better rheology, enhance ocular tolerance, and superior anti-inflammatory activity compared to a suspension of BMD. The cumulative % of drug release from the Cubosome and Cubo-gel is 18.7% and 29.7%, showing an 8.64- and 13.6-fold increase in release compared to the control suspension BDP (2.17%). Increasing the concentration of CMC from 0.5 to 1% causes an increase in viscosity and decrease in drug release, leading to a decrease in the cumulative % release and had a prolonged residence time [
191].
Jiang et al. studied CMC combined with Mistletoe for dry eyes in postmenopausal women. Here, one group was given the eye drop whereas another group was given normal saline eye drops. Patients were diagnosed with diastolic pressure, systolic pressure, glutamic-pyruvic transaminase, glutamic oxaloacetic transaminase, and urine creatinine for safety and efficacy of the treatment after eight weeks. Ocular surface, OSDI, tear protein, and tear film functionality were evaluated after two months of treatment; this shows a slight change for normal saline whereas enhancing the effect in CMC combined with the mistletoe eye drop group. The result shows mistletoe combined with CMC improves the symptoms of dry eye [
192]. In another study, Prasad et al. studied the safety and efficacy of CMC (0.5%) and HPMC (0.3%) for dry eyes due to computer vision syndrome. Efficacy parameters checked were the ocular surface disease index (OSDI) score, tear film break-up time, and Schirmer l test score, and the safety were checked in all. OSDI was reduced in both, the tear film breakup time was enhanced in both, and the Schirmer l test was increased in both, showing CMC and HPMC are both effective and safe for dry eye occurrence due to computer vision syndrome (CVS) [
193]. Titiyal et al. studied the function of topical chloroquine as a topical lubricant for dry eye disease. In this study, CMC 0.5% and chloroquine with CMC 0.5% were evaluated for 3 months. Results show the OSDI score was better in chloroquine with CMC than CMC alone; the Nelson’s score for the CMC group was 1.60 ± 0.77 and for chloroquine CMC 0.92 ± 0.69, and Schirmer test and OSDI were better for chloroquine with CMC, showing this is effective for dry eye disease [
194]. A similar study based on treatments of dry eye was studied by Lievens et al.; in his study, he compared two lubricant artificial tear formulations, which have more viscosity. He used CMC 1.0% with glycerin 0.9% that contain an osmo-protectant compared with CMC 1.0%. The CMC with glycerin at 7 days shows significant enhancement in a baseline of OSDI (all patients
p < 0.001, severe
p < 0.001), TBUT (
p < 0.001), and corneal stain (
p = 0.031), and other results are the same I for both formulations. Adverse effects reported were blurred vision. This showed CMC GLY formulations are the same as CMC alone; therefore, they both were better for dry eye disease [
195].
The CMC was combined with hyaluronic acid to get synergistic effects. In one of the studies, Aragona et al. combined the two polymers CMC and HA and compared this with CMC alone to treat dry eye. The primary evaluation parameters OSDI and secondary are TBUT, surface stain, Schirmer test, and visual analog scale scores in dry eye patients. The safety parameters are adverse events, bio-microscopy, and visual acuity. This study shows the OSDI score at 90 days for CMC-HA and CMC are −16.9 ± 17.5 and −16.0 ± 16.1, and the results show CMC-HA was as effective as CMC for dry eye disease. Both formulations have significantly enhanced properties of OSDI, TBUT, and surface stain for a dry eye [
196]. Another study of polymer combination was done by Simmons et al. In this study, they used a water-soluble polymer, which helps to improve the residence time, moisture retention, and mucin binding, and increase the corneal healing. In the study, CMC and HA alone and the combination was prepared and checked for viscosity rheometry, where the viscosity test showed the enhanced shear rate and simulating eye movement. The viscosity of CMC 0.5% and HA 0.1% was 2.5 and 5.7 cp whereas the viscosity of the combined solution was 13.1 cp, which is 60% higher. The results show that the combination of CMC and HA has a synergistic effect in low shear viscosity and high shear viscoelasticity; these data tells us that the CMC–HA combination can be used for dry eye as artificial tears, which has less blurred vision and stickiness when blinking [
197].
In another study, Sodeinde et al. studied the encapsulation efficacy of CMC of vitamin A in an oil phase; he modified the native cellulose to CMC and cellulose acetate by etherification or acetylation and then studied the material for structural crystallinity, morphology, thermal studies, chemical composition, degree of substitution, and acetyl modification. This modification results in decreased structural crystallinity, and an enhanced amorphous nature when scanning in a wide X-ray diffractometry. This shows CMC enhances the stability of a vegetable oil–water emulsion and significant encapsulation of vitamin A [
198]. In another study, Downie et al. studied the nano emulsion artificial tear efficacy by use of CMC and glycerin, flaxseed oil and castor oil, and levocarnitine, erythritol, and trehalose as an osmo-protectant were compared with the artificial tear that contains the same ingredients, except for trehalose and flaxseed oil. A 7-day run-in period of topical CMC (0.5%) was taken, showing both emulsified artificial tears have an improved baseline in the ocular surface disease index (OSDI) score, ocular surface staining, and tear film breakup time (TBUT) [
199].
10.1.4. Ethyl Cellulose
Ethyl cellulose is a linear, non-toxic, non-swellable polysaccharide [
211] derivative of cellulose [
149], it is insoluble in water and soluble in organic solvents, and has great mechanical properties [
212]. It can be produced by Williamson etherification of cellulose and ethyl chloride. It is mainly used for thin-film coating, acts as a binder taste masking agent, and modified release excipient [
213]. It can be modified at the C2 and C6 positions with 2.1–2.6 of the DS range. The reactivity of ethyl cellulose is low for more functionalization because the remaining free hydroxyl groups are present on C2 and C3. Ethyl cellulose has various important properties, such as chemical stability, thermo-plasticity, and avoid alkali and salts degradation, and even low water absorption capacity; therefore, it has application in paints, lacquers, varnishes, and is also used in hair sprays. It has very good solubility in organic solvents that make it a good candidate for various formulations [
214]. Ethyl cellulose is biocompatible and has a self-assembling capacity; therefore, it is widely used in biotechnology [
215].
Obiedallah et al. studied the improved therapeutic effect and decrease in the systemic adverse effect of acetazolamide, formulated as microsponge in situ gel for ocular delivery. Microsponges were prepared by using various proportions of ethyl cellulose. Further, the developed microsponges were incorporated into the Pluronic F-127 (25%) in situ gel and was compared with a free drug gel formulation. Drug and polymer in ratio 2:1 have shown a high entrapment efficiency (82%) with a particle size 10 µm and polydispersity index of 0.22; these results best suited for ocular delivery. [
216]. Zhu et al. studied the controlled release of diclofenac sodium from the developed by contact lenses. However, this system had some disadvantages related to storage stability, drug loading, and limited release duration. To overcome these limitations, the research group embedded an inner layer of contact lenses, which showed pH triggered extended release of the drug. The inner layer was made by a blend film of ethyl cellulose and Eudragit S 100 and the outer layer was made by p HEMA hydrogel. An in vivo study showed sustained release for 24 h in the tear film, which revealed enhanced corneal resistance time; therefore, this embedded inner layer by ethyl cellulose and Eudragit can be used for extended or control release [
217]. A similar study based on controlled release of drugs was done by Maulvi et al. In this study, drug control release was done in contact lenses, but the optical and physical properties of the lenses changed the drug loading. Timolol maleate (TM) was loaded in an ethyl cellulose nanoparticulate-laden ring in a hydrogel contact lens; this hydrogel contributed to the controlled release without altering the characteristics of the contact lenses. Lenses were prepared by dispersing the TM encapsulated ethyl cellulose nanoparticles in acrylate hydrogel. In vitro studies showed sustained release of the drug for 168 h and the drug loading was 150 µg. In vivo studies showed significant enhancement in mean residence time and AUC and also shows the decrease in intraocular pressure for 192 h, which was compared to the eye drops of TM [
218] (
Table 9). Another similar study related to timolol maleate loaded with ocusert was studied by Nair et al. In this study, ocusert was made with sodium alginate (hydrophilic polymer) and ethyl cellulose (hydrophobic polymer), and polyethylene glycol as a plasticizer. The ethyl cellulose concentration used was 1–6%. The formulation was evaluated for drug entrapment efficacy (94–98%) and content uniformity (93.1 ± 0.264–98.0 ± 0.321%), and the in vitro drug release shows (83.42 ± 0.35%) after 12 h and the ex vivo study gave a significant result and a decrease in intraocular pressure was found after 3 days. An increase in the concentration of ethyl cellulose decreased the permeability coefficient of the timolol maleate in the ocular insert. Therefore, for sustained release of drug from the ocusert, a high ratio of ethyl cellulose is needed and this was compared with the marketed eye drops of timolol. Result shows sustained or delayed-release from ocusert through a corneal membrane [
219]. Another study of controlled release of the drug was done by Balzus et al. In this study, dexamethasone-loaded ethyl cellulose, Eudragit RS, and a combination of both EC and Eudragit RS NP was prepared. The formulation was evaluated for drug release, drug penetration, and NP toxicity. The study shows that ethyl cellulose NP (1.4–2.2%), which is larger in size and has a negative zeta potential because of adsorption of the hydroxyl group, has a better loading capacity than Eudragit (0.3–0.7%), which is smaller and have a positive zeta potential because of the quaternary ammonium group in the Eudragit RS surface; this positive charge decreases the NP–NP aggregation and it has a lower viscosity than ethyl cellulose. The polymer combination in a ratio of 1:1 showed a smaller particle size (105 µm), positive charge NP (+37 mV) with drug loading (1.3%). As the drug–polymer ratio was decreased, there was a decrease in the drug release and drug penetration. However, when the Eudragit and ethyl cellulose blend was used, the drug release and drug penetration was increased [
220].
10.1.5. Hydroxyethyl Cellulose
Hydroxyethyl cellulose is a water-soluble cellulose ether; it is produced commercially by a chemical reaction between ethylene oxide and cellulose. Hydroxyethyl has randomly substituted glucopyranose units at positions 2,3,6 by hydroxyethyl groups and the side chain will be mono, di, or trimer. It is a biocompatible, biodegradable, hydrophilic, non-ionic water-soluble, low toxic, and non-immunogenic cellulose derivative [
128] (
Table 10). HEC can be used as a stabilizer, thickener, or coating material, and because of the high aqueous solubility, HEC can be used in various applications that as film-forming materials, in pharmaceuticals, in cosmetics, biotechnology, and in ophthalmic preparations [
221,
222,
223].
France et al. studied the sustained release of dorzolamide (hydrophilic drug) as an anti-glaucomic agent that is an ocular insert that can decrease the dose frequency, low systemic exposure, decrease the adverse effect, and improve patient compliance. They used chitosan and HEC ocular inserts to produce sustained release of the drug. The inserts were tested for effectiveness in a rat model and in vitro release shows that at 3 h, 75% of the drug was released from the inserts, whereas ex vivo studies show that the biodistribution of 99 m Tc dorzolamide is more than 50% 18 h after administration. The thickness of the inserts was 40 to 70 µm. Dorzolamide is dispersed in the polymeric matrix which causes sustained release of dorzolamide. This system is a control–release system that has an advantage over conventional ones, as inserts allow the sustained release of drugs (
Table 6); this leads to a decrease in the dosing frequency and increase in patient compliance [
68].
Mohammadi et al. studied the improvement in the delivery of Ketorolac tromethamine; in this study, they used Eudragit L-100 NPs with ketorolac, which was incorporated into the PVA and hydroxyethyl cellulose (HEC) films. The encapsulation efficacy and physicochemical property and physiochemical parameters, such as % moisture absorption, % moisture loss, thickness, and folding endurance, were evaluated. Results showed a mean particle size (153.8–217 nm) and zeta potential −10.8 to −40.7 mV, and the loading of the drug increases as the quantity of Eudragit and HEC increases, and the thickness of the inserts was 0.072 ± 0.0098 to 0.0865 ± 0.0035 mm. The thickness and folding endurance of the inserts increased with an amount of polymer; therefore, Eudragit NPs loaded with the PVA and HEC is an effective carrier for delivery of the drug. In this study, the inserts were formulated to reduce the frequency of ketorolac and enhance patient compliance [
224]. A similar study to improve the drug delivery was done by Taghe et al. In this study, azithromycin-loaded Eudragit L 100 NPs inserts, which are sustained release and have increased ophthalmic performance, were prepared by use of HEC, HPMC, and a plasticizer such as PVA. The optimized formulation has a particle size of 78.06 ± 2.3 nm, zeta potential around −2.45 ± 0.69 mV, polydispersity index of 0.179 ± 0.007, and EE of 62.167 ± 0.07%. The thickness of AZM-HEC was 0.156 ± 0.008 mm and AZM-HEC was 0.164 ± 0.005 mm, which is suitable for insertion into a cul-de-sac and show no irritation of the eye. The tensile strength and elongation at the break were higher in HEC films compared to HPMC film and the pH was between 6.66 ± 0.05 and 6.83 ± 0.055, which is near to the ocular pH 6–7.6; this shows that these inserts can be applied to the ocular tissue with no irritation [
225]. Allam et al. studied the Betaxolol noisome that is a pH-responsive in situ gel for the prolongation of pre-corneal retention of Betaxolol. Optimal nano-dispersion was incorporated into the pH-responsive in situ gel by use of HEC and Carbopol 934P. The prepared gel was translucent, pseudoplastic, mucoadhesive, and had sustained release. The formulation was evaluated for vesicle size, morphology, size distribution, surface charge, and EE. This formulation had to extend the decrease in intraocular pressure and enhanced relative bioavailability was seen compared to the marketed one. Therefore, niosome may be an effective carrier for the ocular drug delivery [
226]. A similar study of sustaining the release of the drug was done by Destruel et al. In this study, a mucoadhesive and ion active in situ gel of Phenylephrine and Tropicamide was prepared by use of hydroxyethyl cellulose and gellan gum. The suitable property of ocular administration was checked by the physicochemical characteristics and rheological properties such as viscosity, and the gelation ability was checked. A new rheological technique was established to check gel resistance in simulated eye blinking. Fluorescence intensity determined the extended residence time on the surface of the eye compared to the conventional eye drops, which showed an extended-release of the drug from this oxidized hydroxyethyl cellulose hydrogel [
227]. In another study, Pennington et al. studied infectious ocular disease; in this study, povidone-iodine (0.5%) alone or in combination with HEC (1%) was evaluated for its efficacy. Povidone alone is effective for feline herpesvirus type 1, Chlamydia felis, and Mycoplasma felis, whereas povidone with HEC has an additive effect for feline herpesvirus type1 and C. felis. This additive effect may be due to an increase in culture medium viscosity because of the HEC [
228]. A similar study about ocular disease was done by Mckenzie et al. In this study, cysteamine is used to treat corneal crystal deposition. The pre-formulation evaluation of the cysteamine-containing gel was evaluated, and the suitability of the drug was identified by analysis of the rheology, bio-adhesion, dissolution, and stability. Various polymers were checked for the above properties and as a result, the three polymers that suit ocular delivery were hydroxyethyl cellulose, sodium hyaluronate, and carbomer 934. As sodium hyaluronate and HEC are four to five times more viscous, carbomer is the clear solution [
229]. Kang et al. prepared a novel oxidized hydroxyethyl cellulose and allyl co-polymer-based hydrogel. In this study, they used a hydroxyethyl cellulose molecule chain as the biomacromolecule template, from which the Schiff base and mechanical properties were obtained by borate and hydrogen bonds, which have fast recovery with little or no hysteresis and have significant compressive capacity. In oxidized hydroxyethyl cellulose, a hydrogel functionalized allyl spiro-oxazine derivative was applied to endow photo- and pH-sensitive substrates. This hydrogel has a good pH environment adaptability and was found non-toxic in the in vitro test; this oxidized hydroxyethyl cellulose hydrogel had significant use as a safe development, is fashionable, such as for pH-detectable contact lenses [
63].