Is There a Role for the Therapeutic Drug Monitoring of Colistin? An Overview
Abstract
1. Introduction
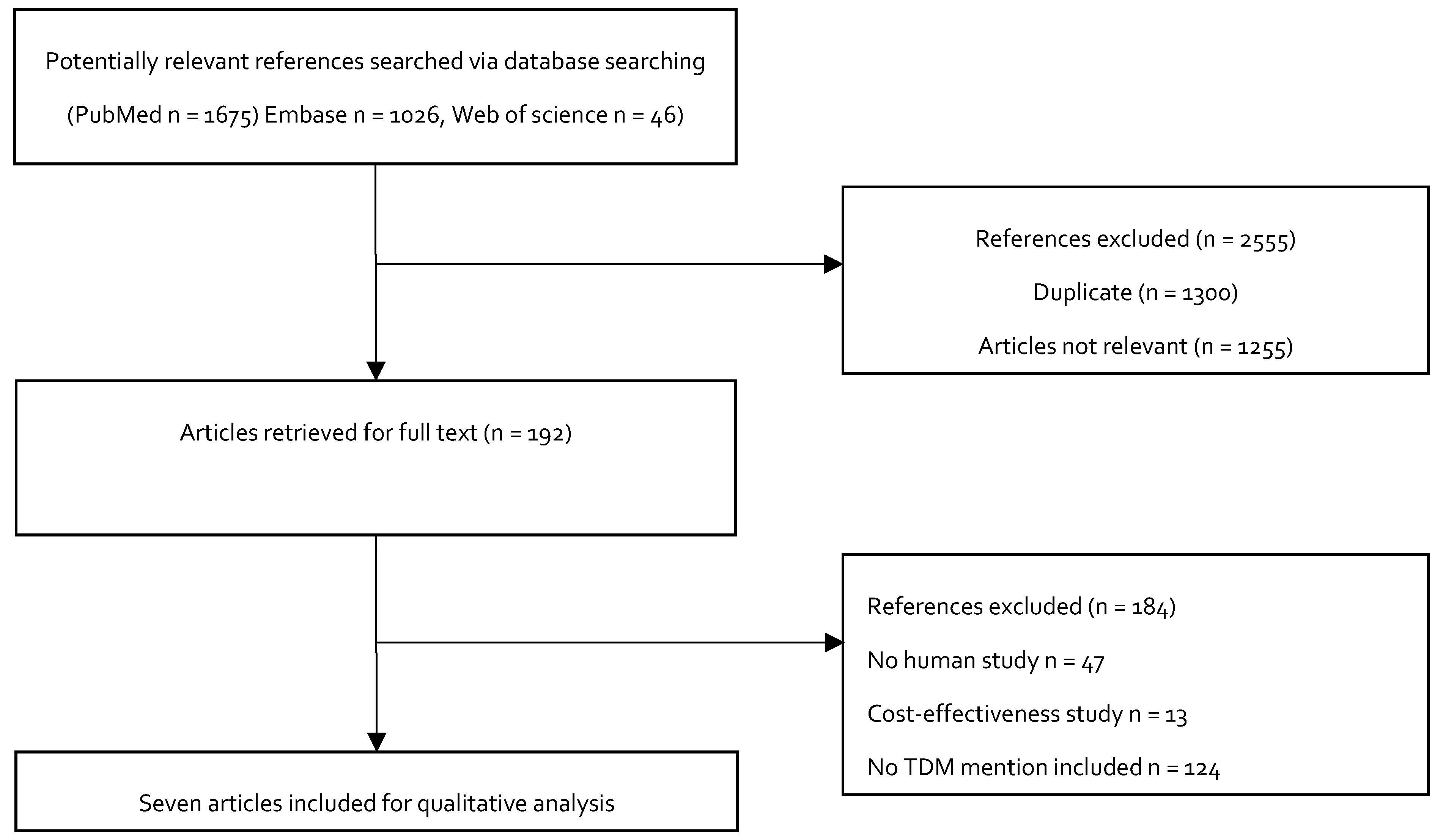
2. Data Sources and Search
3. Study Selection Criteria
4. Data Extraction and Outcomes
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Chan-Tompkins, N.H. Multidrug-resistant gram-negative infections. Bringing back the old. Crit. Care Nurs. Q. 2011, 34, 87–100. [Google Scholar] [CrossRef]
- Falagas, M.E.; Koletsi, P.K.; Bliziotis, I.A. The diversity of definitions of multidrug-resistant (MDR) and pandrug-resistant (PDR) Acinetobacter baumannii and Pseudomonas aeruginosa. J. Med. Microbiol. 2006, 55, 1619–1629. [Google Scholar] [CrossRef]
- Antibiotic Resistance Threats in the United States, 2013; Centres for Disease Control and Prevention, US Department of Health and Human Services: Washington, WA, USA, 2013.
- Ana, C.G.; Rafael, V. Curso Online Interpretación del Antibiograma en la Práctica Clínica. Available online: https://cdn1.redemc.net/campus/wp-content/uploads/2018/03/ATB-01-VignoliGales-Manual-Resistencia-ES-PUB.pdf (accessed on 27 June 2019).
- Creative Commons Attribution 3.0 Unported License; Creative Commons: Boston, MA, USA, 2019; Available online: https://creativecommons.org/licenses/by/3.0/ (accessed on 27 June 2019).
- Servier Medical Art. Available online: https://smart.servier.com/ (accessed on 30 May 2019).
- Azzopardi, E.A.; Ferguson, E.L.; Thomas, D.W. Colistin past and future: A bibliographic analysis. J. Crit. Care 2013, 28, e213–e219. [Google Scholar] [CrossRef]
- Ezadi, F.; Ardebili, A.; Mirnejad, R. Antimicrobial Susceptibility Testing for Polymyxins: Challenges, Issues, and Recommendations. J. Clin. Microbiol. 2019, 57. [Google Scholar] [CrossRef]
- Moraes, M.; Vieira, J.; Vieira, S.; Valbao, S.; Moraes, R.; Pratte-Santos, R. Microbial resistance to colistin in consequence of mutations in the MCR-1 gene of Escherichia coli. MedCrave 2018, 7, 59–63. [Google Scholar]
- Touw, D.J.; Neef, C.; Thomson, A.H.; Vinks, A.A. Cost-effectiveness of therapeutic drug monitoring: A systematic review. Ther. Drug Monit. 2005, 27, 10–17. [Google Scholar] [CrossRef]
- Benedict, R.G.; Langlykke, A.F. Antibiotic activity of Bacillus polymyxa. J. Bacteriol. 1947, 54, 24. [Google Scholar]
- Brink, A.J.; Richards, G.A.; Colombo, G.; Bortolotti, F.; Colombo, P.; Jehl, F. Multicomponent antibiotic substances produced by fermentation: Implications for regulatory authorities, critically ill patients and generics. Int. J. Antimicrob. Agents 2014, 43, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Pastewski, A.A.; Caruso, P.; Parris, A.R.; Dizon, R.; Kopec, R.; Sharma, S.; Mayer, S.; Ghitan, M.; Chapnick, E.K. Parenteral polymyxin B use in patients with multidrug-resistant gram-negative bacteremia and urinary tract infections: A retrospective case series. Ann. Pharm. 2008, 42, 1177–1187. [Google Scholar] [CrossRef] [PubMed]
- Nation, R.L.; Velkov, T.; Li, J. Colistin and polymyxin B: Peas in a pod, or chalk and cheese? Clin. Infect. Dis. 2014, 59, 88–94. [Google Scholar] [CrossRef] [PubMed]
- Gallardo-Godoy, A.; Muldoon, C.; Becker, B.; Elliott, A.G.; Lash, L.H.; Huang, J.X.; Butler, M.S.; Pelingon, R.; Kavanagh, A.M.; Ramu, S.; et al. Activity and Predicted Nephrotoxicity of Synthetic Antibiotics Based on Polymyxin B. J. Med. Chem. 2016, 59, 1068–1077. [Google Scholar] [CrossRef] [PubMed]
- Velkov, T.; Thompson, P.E.; Nation, R.L.; Li, J. Structure—Activity relationships of polymyxin antibiotics. J. Med. Chem. 2010, 53, 1898–1916. [Google Scholar] [CrossRef] [PubMed]
- Performance Standards for Antimicrobial Susceptibility Testing. Twenty-Fourth Informational Supplement. Available online: https://www.academia.edu/25600446/M100-S24_Performance_Standards_for_Antimicrobial_Susceptibility_Testing_Twenty-Fourth_Informational_Supplement_An_informational_supplement_for_global_application_developed_through_the_Clinical_and_Laboratory_Standards_Institute_consensus_process (accessed on 20 May 2019).
- Regenthal, R.; Krueger, M.; Koeppel, C.; Preiss, R. Drug levels: Therapeutic and toxic serum/plasma concentrations of common drugs. J. Clin. Monit. Comput. 1999, 15, 529–544. [Google Scholar] [CrossRef] [PubMed]
- Chepyala, D.; Tsai, I.L.; Sun, H.-Y.; Lin, S.-W.; Kuo, C.-H. Development and validation of a high-performance liquid chromatography-fluorescence detection method for the accurate quantification of colistin in human plasma. J. Chromatogr. B 2015, 980, 48–54. [Google Scholar] [CrossRef]
- Spapen, H.; Jacobs, R.; Van Gorp, V.; Troubleyn, J.; Honore, P.M. Renal and neurological side effects of colistin in critically ill patients. Ann. Intensive Care 2011, 1, 14. [Google Scholar] [CrossRef]
- Kadri, S.S.; Hohmann, S.F.; Orav, E.J.; Bonne, S.L.; Moffa, M.A.; Timpone, J.G.; Strich, J.R.; Palmore, T.; Christopher, K.B.; Varughese, C.; et al. Tracking Colistin-Treated Patients to Monitor the Incidence and Outcome of Carbapenem-Resistant Gram-Negative Infections. Clin. Infect. Dis. 2014, 60, 79–87. [Google Scholar] [CrossRef][Green Version]
- Pacheco, T.; Bustos, R.H.; Gonzalez, D.; Garzon, V.; Garcia, J.C.; Ramirez, D. An Approach to Measuring Colistin Plasma Levels Regarding the Treatment of Multidrug-Resistant Bacterial Infection. Antibiotics 2019, 8, 100. [Google Scholar] [CrossRef]
- World Health Organization. WHO Global Antimicrobial Resistance Surveillance System (GLASS)—The Detection and Reporting of Colistin Resistance. 2018. Available online: https://apps.who.int/iris/bitstream/handle/10665/277175/WHO-WSI-AMR-2018.4-eng.pdf (accessed on 30 September 2019).
- Battikh, H.; Harchay, C.; Dekhili, A.; Khazar, K.; Kechrid, F.; Zribi, M.; Masmoudi, A.; Fendri, C. Clonal Spread of Colistin-Resistant Klebsiella pneumoniae Coproducing KPC and VIM Carbapenemases in Neonates at a Tunisian University Hospital. Microb. Drug Resist. 2017, 23, 468–472. [Google Scholar] [CrossRef]
- Lu, Y.; Feng, Y.; McNally, A.; Zong, Z. The Occurence of Colistin-Resistant Hypervirulent Klebsiellapneumoniae in China. Front. Microbiol. 2018, 9, 2568. [Google Scholar] [CrossRef]
- Moubareck, C.A.; Mouftah, S.F.; Pál, T.; Ghazawi, A.; Halat, D.H.; Nabi, A.; AlSharhan, M.A.; AlDeesi, Z.O.; Peters, C.C.; Celiloglu, H.; et al. Clonal emergence of Klebsiella pneumoniae ST14 co-producing OXA-48-type and NDM carbapenemases with high rate of colistin resistance in Dubai, United Arab Emirates. Int. J. Antimicrob. Agents 2018, 52, 90–95. [Google Scholar] [CrossRef]
- Wang, Q.; Wang, X.; Wang, J.; Ouyang, P.; Jin, C.; Wang, R.; Zhang, Y.; Jin, L.; Chen, H.; Wang, Z.; et al. Phenotypic and Genotypic Characterization of Carbapenem-resistant Enterobacteriaceae: Data From a Longitudinal Large-scale CRE Study in China (2012–2016). Clin. Infect. Dis. 2018, 67, S196–S205. [Google Scholar] [CrossRef] [PubMed]
- Sheck, E.A.; Edelstein, M.V.; Sukhorukova, M.V.; Ivanchik, N.V.; Skleenova, E.Y.; Dekhnich, A.V.; Azizov, I.S.; Kozlov, R.S. Epidemiology and Genetic Diversity of Colistin Nonsusceptible Nosocomial Acinetobacter baumannii Strains from Russia for 2013-2014. Can. J. Infect. Dis. Med. Microbiol. 2017, 2017, 5. [Google Scholar] [CrossRef] [PubMed]
- Giamarellou, H. Epidemiology of infections caused by polymyxin-resistant pathogens. Int. J. Antimicrob. Agents 2016, 48, 614–621. [Google Scholar] [CrossRef] [PubMed]
- Gales, A.C.; Jones, R.N.; Sader, H.S. Contemporary activity of colistin and polymyxin B against a worldwide collection of Gram-negative pathogens: Results from the SENTRY Antimicrobial Surveillance Program (2006–09). J. Antimicrob. Chemother. 2011, 66, 2070–2074. [Google Scholar] [CrossRef] [PubMed]
- Pogue, J.M.; Ortwine, J.K.; Kaye, K.S. Optimal Usage of Colistin: Are We Any Closer? Clin. Infect. Dis. 2015, 61, 1778–1780. [Google Scholar] [CrossRef]
- Kassamali, Z.; Rotschafer, J.C.; Jones, R.N.; Prince, R.A.; Danziger, L.H. Polymyxins: Wisdom does not always come with age. Clin. Infect. Dis. 2013, 57, 877–883. [Google Scholar] [CrossRef]
- Dortet, L.; Bonnin, R.; Jousset, A.; Gauthier, L.; Naas, T. Émergence de la résistance à la colistine chez les entérobactéries : Une brèche dans le dernier rempart contre la pan-résistance! J. AntiInfect. 2016, 18, 139–159. [Google Scholar] [CrossRef]
- Nation, R.L.; Li, J.; Cars, O.; Couet, W.; Dudley, M.N.; Kaye, K.S.; Mouton, J.W.; Paterson, D.L.; Tam, V.H.; Theuretzbacher, U.; et al. Framework for optimisation of the clinical use of colistin and polymyxin B: The Prato polymyxin consensus. Lancet Infect. Dis. 2015, 15, 225–234. [Google Scholar] [CrossRef]
- Tsuji, B.T.; Pogue, J.M.; Zavascki, A.P.; Paul, M.; Daikos, G.L.; Forrest, A.; Giacobbe, D.R.; Viscoli, C.; Giamarellou, H.; Karaiskos, I.; et al. International Consensus Guidelines for the Optimal Use of the Polymyxins: Endorsed by the American College of Clinical Pharmacy (ACCP), European Society of Clinical Microbiology and Infectious Diseases (ESCMID), Infectious Diseases Society of America (IDSA), International Society for Anti-infective Pharmacology (ISAP), Society of Critical Care Medicine (SCCM), and Society of Infectious Diseases Pharmacists (SIDP). Pharmacotherapy 2019, 39, 10–39. [Google Scholar]
- Bode-Boger, S.M.; Schopp, B.; Troger, U.; Martens-Lobenhoffer, J.; Kalousis, K.; Mailander, P. Intravenous colistin in a patient with serious burns and borderline syndrome: The benefits of therapeutic drug monitoring. Int. J. Antimicrob. Agents 2013, 42, 357–360. [Google Scholar] [CrossRef]
- Horcajada, J.P.; Sorli, L.; Luque, S.; Benito, N.; Segura, C.; Campillo, N.; Montero, M.; Esteve, E.; Mirelis, B.; Pomar, V.; et al. Validation of a colistin plasma concentration breakpoint as a predictor of nephrotoxicity in patients treated with colistin methanesulfonate. Int. J. Antimicrob. Agents 2016, 48, 725–727. [Google Scholar] [CrossRef] [PubMed]
- Sorli, L.; Luque, S.; Grau, S.; Berenguer, N.; Segura, C.; Montero, M.M.; Alvarez-Lerma, F.; Knobel, H.; Benito, N.; Horcajada, J.P. Trough colistin plasma level is an independent risk factor for nephrotoxicity: A prospective observational cohort study. BMC Infect. Dis. 2013, 13, 380. [Google Scholar] [CrossRef] [PubMed]
- Tafelski, S.; Wagner, L.; Angermair, S.; Deja, M.; Group, A.B.S. Therapeutic drug monitoring for colistin therapy in severe multi-resistant Acinetobacter intracerebral abscess: A single case study with high-dose colistin and review of literature. SAGE Open Med. Case Rep. 2017, 5, 2050313X17711630. [Google Scholar] [CrossRef]
- Yamada, T.; Ishiguro, N.; Oku, K.; Higuchi, I.; Nakagawa, I.; Noguchi, A.; Yasuda, S.; Fukumoto, T.; Iwasaki, S.; Akizawa, K.; et al. Successful Colistin Treatment of Multidrug-Resistant Pseudomonas aeruginosa Infection Using a Rapid Method for Determination of Colistin in Plasma: Usefulness of Therapeutic Drug Monitoring. Biol. Pharm. Bull. 2015, 38, 1430–1433. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sorli, L.; Luque, S.; Segura, C.; Campillo, N.; Montero, M.; Esteve, E.; Herrera, S.; Benito, N.; Alvarez-Lerma, F.; Grau, S.; et al. Impact of colistin plasma levels on the clinical outcome of patients with infections caused by extremely drug-resistant Pseudomonas aeruginosa. BMC Infect. Dis. 2017, 17, 11. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.J.; Oh, J.; Lee, K.; Yu, K.S.; Chung, J.Y.; Hwang, J.H.; Nam, E.Y.; Kim, H.S.; Kim, M.; Park, J.S.; et al. Pharmacokinetic Characteristics and Limited Sampling Strategies for Therapeutic Drug Monitoring of Colistin in Patients with Multidrug-Resistant Gram-Negative Bacterial Infections. Drug Monit. 2019, 41, 102–106. [Google Scholar] [CrossRef]
- Grant, M.J.; Booth, A. A typology of reviews: An analysis of 14 review types and associated methodologies. Health Inf. Libr. J. 2009, 26, 91–108. [Google Scholar] [CrossRef]
| Ref | Design, Year, Country | Type of Infection | Pathogen and Susceptibility of the Isolate (MDR–XDR) | n | Loading Dose (MU) | Dose (MU/day) | Peak Level (µg/mL) | Trough Level (mg/mL) | Clinical Efficacy | ADR: Nephrotoxicity |
|---|---|---|---|---|---|---|---|---|---|---|
| [36] | Case Report 2013 Germany | Borderline Syndrome | Pseudomonas aeruginosa MDR | 1 | Yes 9 MU | Days 1–6: 9 MU | 0.91 | 0.48 | Inadequate | Non |
| Days 6–9: 18 MU | 1.1 | 0.5 | Adequate | ↓ eGFR | ||||||
| Days 9–21: 9 MU | 7.1 | 4.2 | Adequate | ↓ eGFR CVVHDF | ||||||
| Days 21–28: 6 MU | 0.97 | 0.5 | Inadequate | Multi-organ failure | ||||||
| [37] | Prospective cohort 2011–2015 Spain | Bronchial infections (21), UTI (11) Pneumonia (7) Skin infections (6) Bacteremia (10) | Pseudomonas aeruginosa MDR 59 cases (92.2%) | 64 | Yes 6 MU | 6 | NI | >2.42 (n = 7) <2.42 (n = 57) | NI | >2.42 (mg/mL) Nephrotoxicity more frequent and earlier |
| [38] | Prospective observational 2013 Spain * | Pneumonia 24 Acute bronchitis 23 Urinary tract infection 15 Skin and soft tissue infection and surgical site infection 15 Bacteremia 5 Others 20 | Pseudomonas aeruginosa MDR:89 Acinetobacter baumannii MDR:9 Klebsiella pneumoniae MDR: 1 | 102 | NI | 3 (n = 28) | 0.65 (0.24–1.99) | 0.71 (0.2–2.01) | n = 25 adequate | AKI day 7 = 11 AKI EOT = 21 |
| 6 (n = 42) | 1.13 (0.15–5) | 1.14 (0.11–5) | n = 32 adequate | AKI day 7 = 11 AKI EOT = 21 | ||||||
| 9 (n = 16) | 1.84 (0.5–6.62) | 1.84 (0.45–5.99) | n = 11 adequate | AKI day 7 = 7 AKI EOT = 9 | ||||||
| Others (n = 16) | 1.5 (0.16–3.7) | 1.5 (0.16–3.7) | n = 11 adequate | AKI day 7 = 6 AKI EOT = 11 | ||||||
| [39] | Case Report 2017 Germany | Intracranial infection | Acinetobacter Baumannii MDR | 1 | YES 10 MU | 9MU IV Plus intraventricular 0.5 MU | 4.4 | 1.36 | Adequate | AKI day: 7 |
| [40] | Case Report 2015 Japan | Bacteremia | Pseudomonas aeruginosa MDR | 1 | 2.5 mg/kg | NI | Day 13 = 7.88 | Adequate and microbiological efficacy (>1.36 mg/L) | Day 13: eGFR = 23.8 | |
| [41] | Prospective Cohort 2009–2013 Spain ** | Pneumonia and ITU | Pseudomonas aeruginosa XDR | 91 | NI | 3–9 mg/kg | NI | 1.49 ± 1.4 | Adequate n = 72 | AKI day 7: n = 18 AKI EOT: 33 |
| 2.42 ± 1.49 | Inadequate n = 19 | AKI day 7: n = 12 AKI EOT: 16 | ||||||||
| [42] | Prospective Cohort 2019 Korea ** | Pneumonia and ITU | Acinetobacter Baumannii XDR | 15 | NI | 5 mg/kg | 5.50 ± 2.75 | 2.29 ± 1.15 | Adequate | AKI day 7: n = 4 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Avila, M.-P.; Pacheco, T.; Arias, S.; Bustos, R.-H.; Garcia, J.-C.; Jaimes, D. Is There a Role for the Therapeutic Drug Monitoring of Colistin? An Overview. Pharmaceuticals 2020, 13, 42. https://doi.org/10.3390/ph13030042
Avila M-P, Pacheco T, Arias S, Bustos R-H, Garcia J-C, Jaimes D. Is There a Role for the Therapeutic Drug Monitoring of Colistin? An Overview. Pharmaceuticals. 2020; 13(3):42. https://doi.org/10.3390/ph13030042
Chicago/Turabian StyleAvila, Maria-Paula, Tatiana Pacheco, Sara Arias, Rosa-Helena Bustos, Julio-Cesar Garcia, and Diego Jaimes. 2020. "Is There a Role for the Therapeutic Drug Monitoring of Colistin? An Overview" Pharmaceuticals 13, no. 3: 42. https://doi.org/10.3390/ph13030042
APA StyleAvila, M.-P., Pacheco, T., Arias, S., Bustos, R.-H., Garcia, J.-C., & Jaimes, D. (2020). Is There a Role for the Therapeutic Drug Monitoring of Colistin? An Overview. Pharmaceuticals, 13(3), 42. https://doi.org/10.3390/ph13030042






