Proanthocyanidins: Impact on Gut Microbiota and Intestinal Action Mechanisms in the Prevention and Treatment of Metabolic Syndrome
Abstract
1. Metabolic Syndrome: General Aspects
2. Loss of Intestinal Homeostasis as an Etiological Factor of Metabolic Syndrome and the Importance of Consuming a High-Fat Diet
2.1. Intestinal Dysbiosis and Alterations in the SCFAs Profile Promoted by High-Fat Diets and Associated with Metabolic Syndrome
2.2. Colon Barrier Integrity Disruption Promoted by High-Fat Diets and Associated with Metabolic Syndrome
2.3. Metabolic Endotoxemia Promoted by High-Fat-Diets and Associated with Metabolic Syndrome
3. Metabolic Syndrome Management
4. Proanthocyanidins
4.1. General Aspects
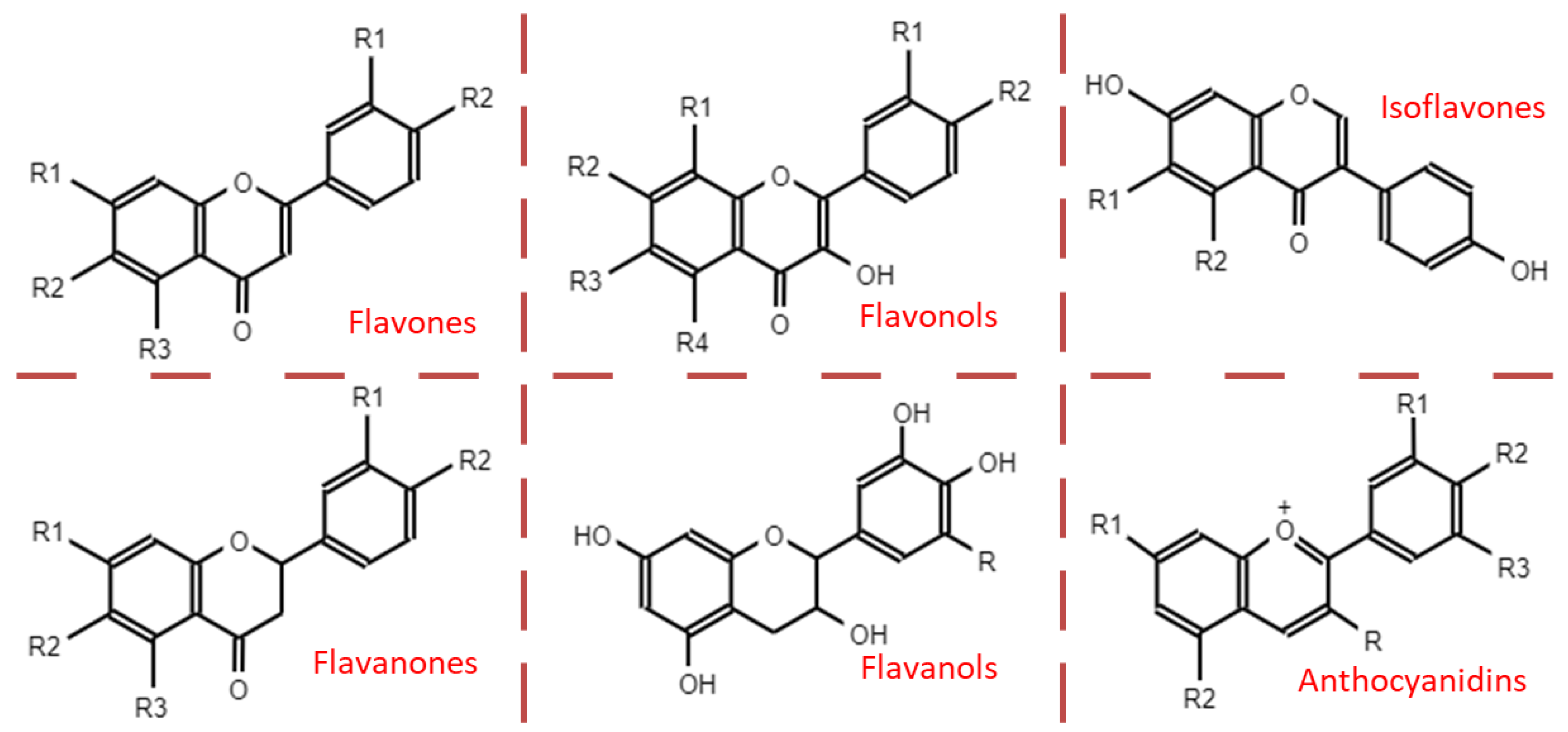
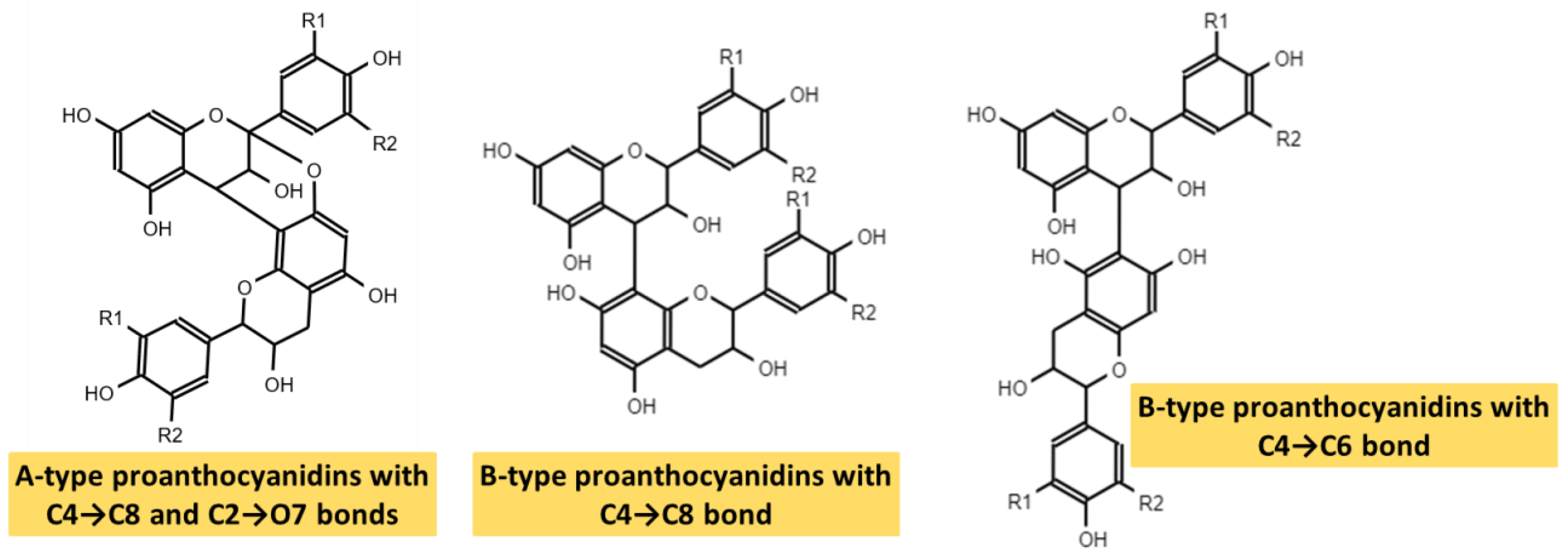
4.2. Structure and Classification
4.3. Absorption, Metabolism, and Excretion of Proanthocyanidins, Biotransformation by the Microbiota
4.4. Bidirectional Relationship of Proanthocyanidins with the Microbiota
5. Gut Microbiota Modulation by Dietary Proanthocyanidins in Metabolic Syndrome
5.1. Results Obtained from Rodent Experiments
5.1.1. Effects of Proanthocyanidins Consumption on Bacteria Considered Beneficial in Metabolic Syndrome
5.1.2. Effects of Proanthocyanidins Consumption on Bacteria Which There Is Ignorance or Controversy in Relation with Metabolic Syndrome
5.1.3. Effects of Proanthocyanidins Consumption on Bacteria Considered Deleterious in Metabolic Syndrome
5.1.4. Relevant Considerations and Recommendations
- Added to the animal model and the diet composition, authors should specify the specific experimental scheme, highlighting when PAs are introduced. This determines the nutritional strategy used, that is, if dietary supplementation is approached as a preventive or treatment of MS. Thus, if PA and MS-inducing diets begin simultaneously, it should be viewed as a prevention model, because the disease is not established when PAs are introduced. However, it should be a treatment strategy if PAs are introduced after the unhealthy diet has been consumed for a reasonable period for MS establishment. It is recommended that MS was confirmed before introducing PA, measuring a recognized variable such as fasting glucose [61,97], to ascertain treatment strategy.
- Most of the preclinical studies use male rodents. It is urgent that females are also included in preclinical studies, because MS-inducing diets have a different impact depending on sex. Furthermore, there are variations in the composition of GM between sex [101] that will determine a modified fermentation of PAs, crucial for their systemic effects. Last, due to the recruiting of men and women, it would be important to predict differences in PAs effects from animal experiments.
- As the type of PAs and the presence of associated compounds could relate to understanding their effects and the differences found in previous studies, it would be helpful for the authors to carefully describe the composition of PA extract used in each experiment.
- It is also recommended to use feces collected directly from the colon at the animal’s slaughter time. Thus, contamination can be avoided as much as possible, and the GM present in the sample will be representative.
- The presence of bacterial taxa strongly associated with the consumption of PAs or MS should be determined. It is increasingly common to perform next-generation sequencing of GM, leading to report a wide variety of changes in bacterial taxa whose role in physiological conditions or their relationship with MS is unknown [65,97,98,99,100,101,102,103,104]. Although this is positive, because it increases the knowledge about the changes in GM promoted by PA consumption in pathological conditions, the dispersion and variety of data makes their analysis difficult; and their poor knowledge complicates the interpretation. Therefore, to have the greatest evidence available, we suggest determining as a priority the abundance of strains ascribed to A. muciniphila, Bifidobacterium, Desulfovibrionaceae, F. prausnitzii, Lactobacillus, Lactococcus, and Roseburia. Furthermore, the abundance of Firmicutes and Bacteroidetes phyla can be measured to obtain the F/B ratio, although their analysis at the phylum level is not conclusive. It is recommended that results about these bacteria can be found in the manuscript, even if they have not changed after PA consumption.
5.2. Results Obtained in Clinical Trials
6. Restoration of Intestinal Epithelial Barrier Integrity by Dietary Proanthocyanidins
6.1. Impact on Mucus and Antimicrobial Peptides’ Production by Dietary Proanthocyanidins
6.2. Restoration of Intestinal Wall Morphology by Dietary Proanthocyanidins
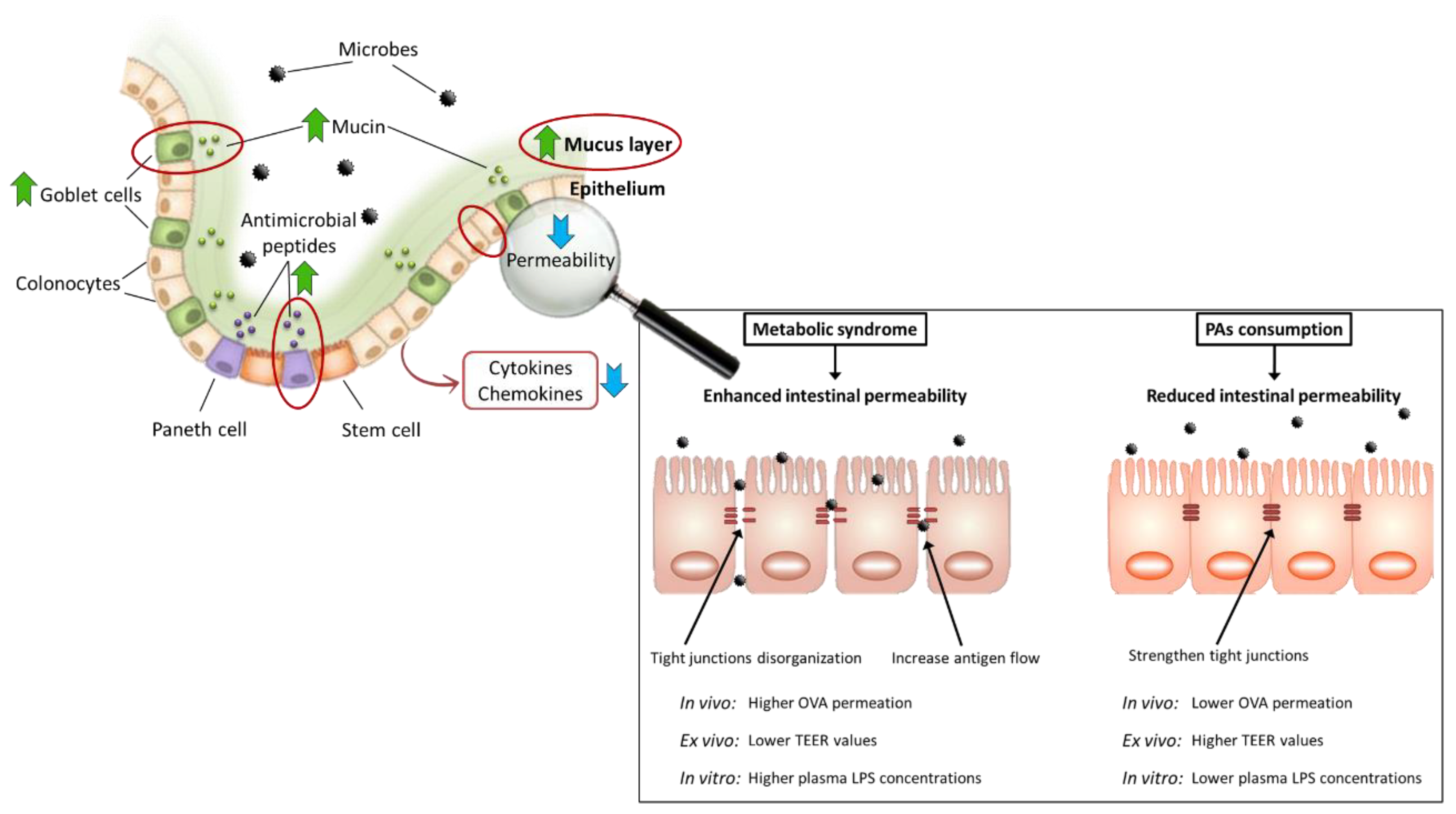
6.3. Improvement of Altered Intestinal Permeability by Dietary Proanthocyanidins
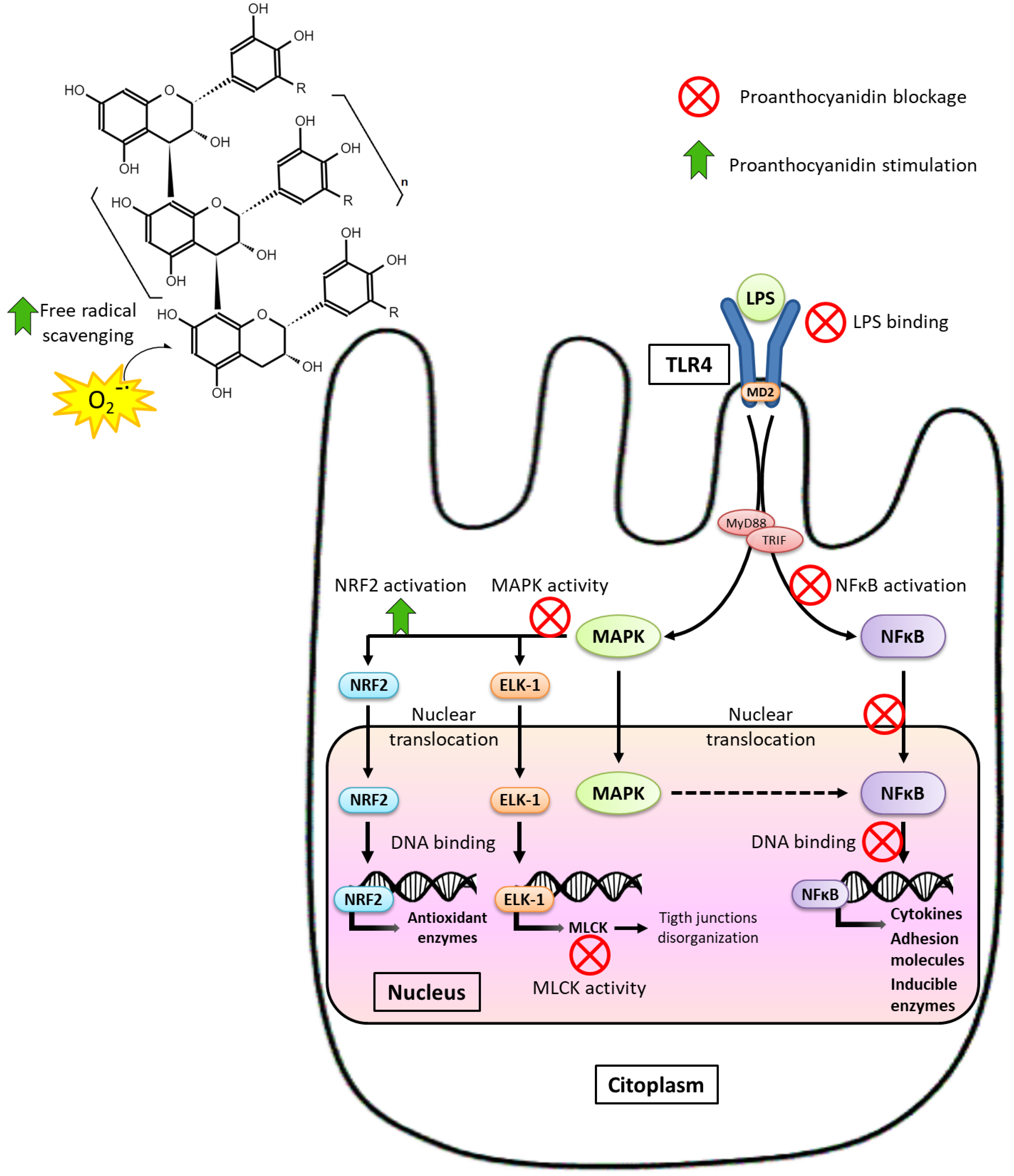
6.4. Improvement of Intestinal Inflammation, Immune Response, and Oxidative Stress by Dietary Proanthocyanidins
- Radical scavenging activity, due to its aromatic structure [107,121]. PAs can prevent free radical-induced oxidative damage and avoid lipid peroxidation, which increases in MS. Again, polymeric PAs can exert this action independently of the degree of fermentation, ensuring positive results in treatment strategies (t > 0).
- Inhibition of the activity of enzymes that cause oxidative stress, such as neutrophil myeloperoxidase (MPO) over-activated in MS [111,112,113]. This enzyme produces large amounts of ROS to cause oxidative damage to invading microorganisms. However, overproduction of ROS over time depletes antioxidant defenses, causes oxidative stress, and has a negative effect on the organism. Ileal MPO activity was decreased by GSPE administration in both preventive [111] and treatment strategies for diet-induced MS, placing these values in the normal range [112,113].
- Inactivation of signaling pathways related to oxidative stress and an increase in the expression of antioxidant enzymes. As indicated above, PAs decrease the transcription of inflammatory enzymes that produce oxidative stress such as COX-2 and iNOS [113,122]. In addition, PAs regulate these signaling pathways toward activation of the transcription factor nuclear factor erythroid-2-related factor 2 (NRF2) [29,107,119,122,123], which favors the transcription of antioxidant enzymes (e.g., catalase, superoxide dismutase, glutathione peroxidase, etc.), thus strengthening the ability of tissue to defend against oxidative stress.
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Alberti, K.G.M.M.; Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z.; Cleeman, J.I.; Donato, K.A.; Fruchart, J.C.; James, W.P.T.; Loria, C.M.; Smith, S.C. Harmonizing the metabolic syndrome. Circulation 2009, 120, 1640–1645. [Google Scholar] [CrossRef]
- McCracken, E.; Monaghan, M.; Sreenivasan, S. Pathophysiology of the metabolic syndrome. Clin. Dermatol. 2018, 36, 14–20. [Google Scholar] [CrossRef]
- Cascio, G.; Schiera, G.; Di Liegro, I. Dietary fatty acids in metabolic syndrome, diabetes and cardiovascular diseases. Curr. Diabetes Rev. 2012, 8, 2–17. [Google Scholar] [CrossRef]
- Vaquero, M.P.; Martínez-Suárez, M.; García-Quismondo, Á.; del Cañizo, F.J.; Sánchez-Muniz, F.J. Diabesity negatively affects transferrin saturation and iron status. The DICARIVA study. Diabetes Res. Clin. Pract. 2021, 172, 108653. [Google Scholar] [CrossRef]
- Macho-González, A.; Garcimartín, A.; López-Oliva, E.; Benedí, J.; Bastida, S.; Sánchez-Muniz, F.J. Papel de las proantocianidinas sobre la microbiota, permeabilidad intestinal e inflamación. In Inmunonutrición. Estilo de Vida, 2nd ed.; Marcos, A., Ed.; Editorial Panamericana: Madrid, Spain, 2020; pp. 245–266. [Google Scholar]
- Alemao, C.A.; Budden, K.F.; Gomez, H.M.; Rehman, S.F.; Marshall, J.E.; Shukla, S.D.; Donovan, C.; Forster, S.C.; Yang, I.A.; Keely, S.; et al. Impact of diet and the bacterial microbiome on the mucous barrier and immune disorders. Allergy 2021, 76, 714–734. [Google Scholar] [CrossRef] [PubMed]
- Amar, J.; Chabo, C.; Waget, A.; Klopp, P.; Vachoux, C.; Bermúdez-Humarán, L.G.; Smirnova, N.; Bergé, M.; Sulpice, T.; Lahtinen, S.; et al. Intestinal mucosal adherence and translocation of commensal bacteria at the early onset of type 2 diabetes: Molecular mechanisms and probiotic treatment. EMBO Mol. Med. 2011, 3, 559–572. [Google Scholar] [CrossRef]
- Statovci, D.; Aguilera, M.; MacSharry, J.; Melgar, S. The impact of western diet and nutrients on the microbiota and immune response at mucosal interfaces. Front. Immunol. 2017, 8, 838. [Google Scholar] [CrossRef] [PubMed]
- Sittipo, P.; Lobionda, S.; Lee, Y.K.; Maynard, C.L. Intestinal microbiota and the immune system in metabolic diseases. J. Microbiol. 2018, 56, 154–162. [Google Scholar] [CrossRef] [PubMed]
- Croci, S.; D’apolito, L.I.; Gasperi, V.; Catani, M.V.; Savini, I. Dietary Strategies for Management of Metabolic Syndrome: Role of Gut Microbiota Metabolites. Nutrients 2021, 13, 1389. [Google Scholar] [CrossRef]
- Nishitsuji, K.; Xiao, J.; Nagatomo, R.; Umemoto, H.; Morimoto, Y.; Akatsu, H.; Inoue, K.; Tsuneyama, K. Analysis of the gut microbiome and plasma short-chain fatty acid profiles in a spontaneous mouse model of metabolic syndrome. Sci. Rep. 2017, 7, 15876. [Google Scholar] [CrossRef]
- Van Hul, M.; Geurts, L.; Plovier, H.; Druart, C.; Everard, A.; Ståhlman, M.; Rhimi, M.; Chira, K.; Teissedre, P.L.; Delzenne, N.M.; et al. Reduced obesity, diabetes, and steatosis upon cinnamon and grape pomace are associated with changes in gut microbiota and markers of gut barrier. Am. J. Physiol. Endocrinol. Metab. 2018, 314, E334–E352. [Google Scholar] [CrossRef] [PubMed]
- Tao, W.; Zhang, Y.; Shen, X.; Cao, Y.; Shi, J.; Ye, X.; Chen, S. Rethinking the mechanism of the health benefits of proanthocyanidins: Absorption, metabolism, and interaction with gut microbiota. Compr. Rev. Food Sci. Food Saf. 2019, 18, 971–985. [Google Scholar] [CrossRef]
- Masumoto, S.; Terao, A.; Yamamoto, Y.; Mukai, T.; Miura, T.; Shoji, T. Non-absorbable apple procyanidins prevent obesity associated with gut microbial and metabolomic changes. Sci. Rep. 2016, 6, 31208. [Google Scholar] [CrossRef] [PubMed]
- Machate, D.J.; Figueiredo, P.S.; Marcelino, G.; Guimarães, R.d.C.A.; Hiane, P.A.; Bogo, D.; Pinheiro, V.A.Z.; de Oliveira, L.C.S.; Pott, A. Fatty acid diets: Regulation of gut microbiota composition and obesity and its related metabolic dysbiosis. Int. J. Mol. Sci. 2020, 21, 4093. [Google Scholar] [CrossRef] [PubMed]
- Chambers, E.S.; Preston, T.; Frost, G.; Morrison, D.J. Role of gut microbiota-generated short-chain fatty acids in metabolic and cardiovascular health. Curr. Nutr. Rep. 2018, 7, 198. [Google Scholar] [CrossRef] [PubMed]
- Cong, J.; Zhou, P.; Zhang, R. Intestinal microbiota-derived short chain fatty acids in host health and disease. Nutrients 2022, 14, 1977. [Google Scholar] [CrossRef]
- Hu, J.; Lin, S.; Zheng, B.; Cheung, P.C.K. Short-chain fatty acids in control of energy metabolism. Crit. Rev. Food Sci. Nutr. 2017, 58, 1243–1249. [Google Scholar] [CrossRef]
- Yao, Y.; Cai, X.; Fei, W.; Ye, Y.; Zhao, M.; Zheng, C. The role of short-chain fatty acids in immunity, inflammation and metabolism. Crit. Rev. Food Sci. Nutr. 2022, 62, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Perry, R.J.; Peng, L.; Barry, N.A.; Cline, G.W.; Zhang, D.; Cardone, R.L.; Petersen, K.F.; Kibbey, R.G.; Goodman, A.L.; Shulman, G.I. Acetate mediates a microbiome–brain–β-cell axis to promote metabolic syndrome. Nature 2016, 534, 213–217. [Google Scholar] [CrossRef]
- Martínez-Cuesta, M.C.; del Campo, R.; Garriga-García, M.; Peláez, C.; Requena, T. Taxonomic characterization and short-chain fatty acids production of the obese microbiota. Front. Cell. Infect. Microbiol. 2021, 11, 598093. [Google Scholar] [CrossRef]
- Kim, K.N.; Yao, Y.; Ju, S.Y. Short chain fatty acids and fecal microbiota abundance in humans with obesity: A systematic review and meta-analysis. Nutrients 2019, 11, 2512. [Google Scholar] [CrossRef] [PubMed]
- Boscaini, S.; Leigh, S.J.; Lavelle, A.; García-Cabrerizo, R.; Lipuma, T.; Clarke, G.; Schellekens, H.; Cryan, J.F. Microbiota and body weight control: Weight watchers within? Mol. Metab. 2022, 57, 101427. [Google Scholar] [CrossRef]
- Ilyés, T.; Silaghi, C.N.; Crăciun, A.M. Diet-related changes of short-chain fatty acids in blood and feces in obesity and metabolic syndrome. Biology 2022, 11, 1556. [Google Scholar] [CrossRef] [PubMed]
- Ashaolu, T.J.; Ashaolu, J.O.; Adeyeye, S.A.O. Fermentation of prebiotics by human colonic microbiota in vitro and short-chain fatty acids production: A critical review. J. Appl. Microbiol. 2021, 130, 677–687. [Google Scholar] [CrossRef] [PubMed]
- Salvo-Romero, E.; Alonso-Cotoner, C.; Pardo-Camacho, C.; Casado-Bedmar, M.; Vicario, M. The intestinal barrier function and its involvement in digestive disease. Rev. Española Enferm. Dig. 2015, 107, 686–696. [Google Scholar] [CrossRef]
- Leech, B.; McIntyre, E.; Steel, A.; Sibbritt, D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int. J. Clin. Pract. 2019, 73, e13385. [Google Scholar] [CrossRef]
- Malesza, I.J.; Malesza, M.; Walkowiak, J.; Mussin, N.; Walkowiak, D.; Aringazina, R.; Bartkowiak-Wieczorek, J.; Mądry, E. High-fat, Western-style diet, systemic inflammation, and gut microbiota: A narrative review. Cells 2021, 10, 3164. [Google Scholar] [CrossRef]
- González-Quilen, C.; Rodríguez-Gallego, E.; Beltrán-Debón, R.; Pinent, M.; Ardévol, A.; Blay, M.T.; Terra, X. Health-promoting properties of proanthocyanidins for intestinal dysfunction. Nutrients 2020, 12, 130. [Google Scholar] [CrossRef]
- Gebrayel, P.; Nicco, C.; Al Khodor, S.; Bilinski, J.; Caselli, E.; Comelli, E.M.; Egert, M.; Giaroni, C.; Karpinski, T.M.; Loniewski, I.; et al. Microbiota medicine: Towards clinical revolution. J. Transl. Med. 2022, 20, 111. [Google Scholar] [CrossRef]
- Jamar, G.; Ribeiro, D.A.; Pisani, L.P. High-fat or high-sugar diets as trigger inflammation in the microbiota-gut-brain axis. Crit. Rev. Food Sci. Nutr. 2021, 61, 836–854. [Google Scholar] [CrossRef]
- André, P.; Laugerette, F.; Féart, C. Metabolic endotoxemia: A potential underlying mechanism of the relationship between dietary fat intake and risk for cognitive impairments in humans? Nutrients 2019, 11, 1887. [Google Scholar] [CrossRef]
- Thomas, M.S.; Blesso, C.N.; Calle, M.C.; Chun, O.K.; Puglisi, M.; Fernandez, M.L. Dietary influences on gut microbiota with a focus on metabolic syndrome. Metab. Syndr. Relat. Disord. 2022, 20, 429–439. [Google Scholar] [CrossRef]
- Aguilar-Salinas, C.A.; Viveros-Ruiz, T. Recent advances in managing/understanding the metabolic syndrome. F1000Research 2019, 8, 370. [Google Scholar] [CrossRef]
- Rask Larsen, J.; Dima, L.; Correll, C.U.; Manu, P. The pharmacological management of metabolic syndrome. Expert Rev. Clin. Pharmacol. 2018, 11, 397–410. [Google Scholar] [CrossRef] [PubMed]
- Mannino, G.; Iovino, P.; Lauria, A.; Genova, T.; Asteggiano, A.; Notarbartolo, M.; Porcu, A.; Serio, G.; Chinigò, G.; Occhipinti, A.; et al. Bioactive triterpenes of Protium heptaphyllum gum resin extract display cholesterol-lowering potential. Int. J. Mol. Sci. 2021, 22, 2664. [Google Scholar] [CrossRef] [PubMed]
- Hosseini, A.; Razavi, B.M.; Banach, M.; Hosseinzadeh, H. Quercetin and metabolic syndrome: A review. Phyther. Res. 2021, 35, 5352–5364. [Google Scholar] [CrossRef]
- Gouveia, H.J.C.B.; Urquiza-Martínez, M.V.; Manhães-de-Castro, R.; Costa-de-Santana, B.J.R.; Villarreal, J.P.; Mercado-Camargo, R.; Torner, L.; de Souza Aquino, J.; Toscano, A.E.; Guzmán-Quevedo, O. Effects of the Treatment with Flavonoids on Metabolic Syndrome Components in Humans: A Systematic Review Focusing on Mechanisms of Action. Int. J. Mol. Sci. 2022, 23, 8344. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Song, X.; Hu, X.; Chen, F.; Ma, C. Health benefits of proanthocyanidins linking with gastrointestinal modulation: An updated review. Food Chem. 2023, 404, 134596. [Google Scholar] [CrossRef] [PubMed]
- Zhu, W.; Oteiza, P.I. Proanthocyanidins at the gastrointestinal tract: Mechanisms involved in their capacity to mitigate obesity-associated metabolic disorders. Crit. Rev. Food Sci. Nutr. 2022, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Wang, J.; Zou, L.; Cao, H.; Ni, X.; Xiao, J. Dietary proanthocyanidins on gastrointestinal health and the interactions with gut microbiota. Crit. Rev. Food Sci. Nutr. 2022, 1–24. [Google Scholar] [CrossRef]
- Kasprzak-Drozd, K.; Oniszczuk, T.; Stasiak, M.; Oniszczuk, A. Beneficial effects of phenolic compounds on gut microbiota and metabolic syndrome. Int. J. Mol. Sci. 2021, 22, 3715. [Google Scholar] [CrossRef] [PubMed]
- Salvadó, M.J.; Casanova, E.; Fernández-Iglesias, A.; Arola, L.; Bladé, C. Roles of proanthocyanidin rich extracts in obesity. Food Funct. 2015, 6, 1053–1071. [Google Scholar] [CrossRef] [PubMed]
- Rasmussen, S.E.; Frederiksen, H.; Krogholm, K.S.; Poulsen, L. Dietary proanthocyanidins: Occurrence, dietary intake, bioavailability, and protection against cardiovascular disease. Mol. Nutr. Food Res. 2005, 49, 159–174. [Google Scholar] [CrossRef] [PubMed]
- Smeriglio, A.; Barreca, D.; Bellocco, E.; Trombetta, D. Proanthocyanidins and hydrolysable tannins: Occurrence, dietary intake and pharmacological effects. Br. J. Pharmacol. 2017, 174, 1244–1262. [Google Scholar] [CrossRef]
- Mannino, G.; Chinigò, G.; Serio, G.; Genova, T.; Gentile, C.; Munaron, L.; Bertea, C.M. Proanthocyanidins and where to find them: A meta-analytic approach to investigate their chemistry, biosynthesis, distribution and effect on human health. Antioxidants 2021, 10, 1229. [Google Scholar] [CrossRef]
- Luca, S.V.; Macovei, I.; Bujor, A.; Miron, A.; Skalicka-Woźniak, K.; Aprotosoaie, A.C.; Trifan, A. Bioactivity of dietary polyphenols: The role of metabolites. Crit. Rev. Food Sci. Nutr. 2019, 60, 626–659. [Google Scholar] [CrossRef]
- Diotallevi, C.; Fava, F.; Gobbetti, M.; Tuohy, K. Healthy dietary patterns to reduce obesity-related metabolic disease: Polyphenol-microbiome interactions unifying health effects across geography. Curr. Opin. Clin. Nutr. Metab. Care 2020, 23, 437–444. [Google Scholar] [CrossRef]
- Constabel, C.P. Molecular controls of proanthocyanidin synthesis and structure: Prospects for genetic engineering in crop plants. J. Agric. Food Chem. 2018, 66, 9882–9888. [Google Scholar] [CrossRef]
- Es-Safi, N.E.; Ghidouche, S.; Ducrot, P.H. Flavonoids: Hemisynthesis, Reactivity, Characterization and Free Radical Scavenging Activity. Molecules 2007, 12, 2228–2258. [Google Scholar] [CrossRef]
- Man, A.W.C.; Zhou, Y.; Xia, N.; Li, H. Involvement of gut microbiota, microbial metabolites and interaction with polyphenol in host immunometabolism. Nutrients 2020, 12, 3054. [Google Scholar] [CrossRef]
- Ou, K.; Gu, L. Absorption and metabolism of proanthocyanidins. J. Funct. Foods 2014, 7, 43–53. [Google Scholar] [CrossRef]
- Marín, L.; Miguélez, E.M.; Villar, C.J.; Lombó, F. Bioavailability of dietary polyphenols and gut microbiota metabolism: Antimicrobial properties. BioMed Res. Int. 2015, 2015, 905215. [Google Scholar] [CrossRef]
- Cejudo, P.S.; Bastida, S.; Macho-González, A.; Sánchez-Muniz, F.J. Functional foods as an alternative to increase the consumption of dietary fiber and proanthocyanidins. Possible effects on the gut microbiota. JONNPR 2020, 5, 1575–1598. [Google Scholar] [CrossRef]
- Choy, Y.Y.; Jaggers, G.K.; Oteiza, P.I.; Waterhouse, A.L. Bioavailability of intact proanthocyanidins in the rat colon after ingestion of grape seed extract. J. Agric. Food Chem. 2013, 61, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Zhao, S.; Wang, J.; Shi, J.; Sun, Y.; Wang, W.; Ning, G.; Hong, J.; Liu, R. Grape seed proanthocyanidin extract ameliorates inflammation and adiposity by modulating gut microbiota in high-fat diet mice. Mol. Nutr. Food Res. 2017, 61, 1601082. [Google Scholar] [CrossRef]
- Koudoufio, M.; Desjardins, Y.; Feldman, F.; Spahis, S.; Delvin, E.; Levy, E. Insight into polyphenol and gut microbiota crosstalk: Are their metabolites the key to understand protective effects against metabolic disorders? Antioxidants 2020, 9, 982. [Google Scholar] [CrossRef] [PubMed]
- Martins Ferreira, Y.A.; Jamar, G.; Estadella, D.; Pisani, L.P. Proanthocyanidins in grape seeds and their role in gut microbiota-white adipose tissue axis. Food Chem. 2023, 404, 134405. [Google Scholar] [CrossRef]
- Anhê, F.F.; Roy, D.; Pilon, G.; Dudonné, S.; Matamoros, S.; Varin, T.V.; Garofalo, C.; Moine, Q.; Desjardins, Y.; Levy, E.; et al. A polyphenol-rich cranberry extract protects from diet-induced obesity, insulin resistance and intestinal inflammation in association with increased Akkermansia spp. population in the gut microbiota of mice. Gut 2015, 64, 872–883. [Google Scholar] [CrossRef]
- Lee, S.; Keirsey, K.I.; Kirkland, R.; Grunewald, Z.I.; Fischer, J.G.; de La Serre, C.B. Blueberry supplementation influences the gut microbiota, inflammation, and insulin resistance in high-fat-diet-fed rats. J. Nutr. 2018, 148, 209–219. [Google Scholar] [CrossRef] [PubMed]
- Macho-González, A.; Garcimartín, A.; Redondo, N.; Cofrades, S.; Bastida, S.; Nova, E.; Benedí, J.; Sánchez-Muniz, F.J.; Marcos, A.; Elvira López-Oliva, M. Carob fruit extract-enriched meat, as preventive and curative treatments, improves gut microbiota and colonic barrier integrity in a late-stage T2DM model. Food Res. Int. 2021, 141, 110124. [Google Scholar] [CrossRef] [PubMed]
- Morissette, A.; Kropp, C.; Songpadith, J.P.; Moreira, R.J.; Costa, J.; Mariné-Casadó, R.; Pilon, G.; Varin, T.V.; Dudonné, S.; Boutekrabt, L.; et al. Blueberry proanthocyanidins and anthocyanins improve metabolic health through a gut microbiota-dependent mechanism in diet-induced obese mice. Am. J. Physiol. Endocrinol. Metab. 2020, 318, E965–E980. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Daza, M.C.; Daoust, L.; Boutkrabt, L.; Pilon, G.; Varin, T.; Dudonné, S.; Levy, É.; Marette, A.; Roy, D.; Desjardins, Y. Wild blueberry proanthocyanidins shape distinct gut microbiota profile and influence glucose homeostasis and intestinal phenotypes in high-fat high-sucrose fed mice. Sci. Rep. 2020, 10, 2217. [Google Scholar] [CrossRef] [PubMed]
- Xiao, Y.; Yang, C.; Xu, H.; Wu, Q.; Zhou, Y.; Zhou, X.; Miao, J. Procyanidin B2 prevents dyslipidemia via modulation of gut microbiome and related metabolites in high-fat diet fed mice. J. Funct. Foods 2020, 75, 104285. [Google Scholar] [CrossRef]
- Zheng, S.; Huang, K.; Zhao, C.; Xu, W.; Sheng, Y.; Luo, Y.; He, X. Procyanidin attenuates weight gain and modifies the gut microbiota in high fat diet induced obese mice. J. Funct. Foods 2018, 49, 362–368. [Google Scholar] [CrossRef]
- Zhu, W.; Lin, K.; Li, K.; Deng, X.; Li, C. Reshaped fecal gut microbiota composition by the intake of high molecular weight persimmon tannin in normal and high-cholesterol diet-fed rats. Food Funct. 2018, 9, 541–551. [Google Scholar] [CrossRef]
- Anhê, F.F.; Nachbar, R.T.; Varin, T.V.; Vilela, V.; Dudonné, S.; Pilon, G.; Fournier, M.; Lecours, M.A.; Desjardins, Y.; Roy, D.; et al. A polyphenol-rich cranberry extract reverses insulin resistance and hepatic steatosis independently of body weight loss. Mol. Metab. 2017, 6, 1563–1573. [Google Scholar] [CrossRef]
- Xu, H.; Zhao, C.; Li, Y.; Liu, R.; Ao, M.; Li, F.; Yao, Y.; Tao, Z.; Yu, L. The ameliorative effect of the Pyracantha fortuneana (Maxim.) H. L. Li extract on intestinal barrier dysfunction through modulating glycolipid digestion and gut microbiota in high fat diet-fed rats. Food Funct. 2019, 10, 6517–6532. [Google Scholar] [CrossRef]
- Hamer, H.M.; Jonkers, D.; Venema, K.; Vanhoutvin, S.; Troost, F.J.; Brummer, R.J. Review article: The role of butyrate on colonic function. Aliment. Pharmacol. Ther. 2008, 27, 104–119. [Google Scholar] [CrossRef]
- Fu, X.; Liu, Z.; Zhu, C.; Mou, H.; Kong, Q. Nondigestible carbohydrates, butyrate, and butyrate-producing bacteria. Crit. Rev. Food Sci. Nutr. 2019, 59 (Suppl. S1), S130–S152. [Google Scholar] [CrossRef]
- Santos-Marcos, J.A.; Perez-Jimenez, F.; Camargo, A. The role of diet and intestinal microbiota in the development of metabolic syndrome. J. Nutr. Biochem. 2019, 70, 1–27. [Google Scholar] [CrossRef]
- Zhang, L.; Carmody, R.N.; Kalariya, H.M.; Duran, R.M.; Moskal, K.; Poulev, A.; Kuhn, P.; Tveter, K.M.; Turnbaugh, P.J.; Raskin, I.; et al. Grape proanthocyanidin-induced intestinal bloom of Akkermansia muciniphila is dependent on its baseline abundance and precedes activation of host genes related to metabolic health. J. Nutr. Biochem. 2018, 56, 142–151. [Google Scholar] [CrossRef]
- Stein, R.R.; Bucci, V.; Toussaint, N.C.; Buffie, C.G.; Rätsch, G.; Pamer, E.G.; Sander, C.; Xavier, J.B. Ecological modeling from time-series inference: Insight into dynamics and stability of intestinal microbiota. PLoS Comput. Biol. 2013, 9, e1003388. [Google Scholar] [CrossRef]
- Festi, D.; Schiumerini, R.; Eusebi, L.H.; Marasco, G.; Taddia, M.; Colecchia, A. Gut microbiota and metabolic syndrome. World J. Gastroenterol. 2014, 20, 16079–16094. [Google Scholar] [CrossRef] [PubMed]
- Louis, P.; Flint, H.J. Formation of propionate and butyrate by the human colonic microbiota. Environ. Microbiol. 2017, 19, 29–41. [Google Scholar] [CrossRef]
- Tarrés, M.C.; Gayol, M.D.C.; Picena, J.C.; Alet, N.; Bottasso, O.; McIntyre, G.; Stanford, C.; Stanford, J. Beneficial effects of immunotherapy with extracts derived from Actinomycetales on rats with spontaneous obesity and diabetes. Immunotherapy 2012, 4, 487–497. [Google Scholar] [CrossRef]
- Dudonné, S.; Varin, T.V.; Forato Anhê, F.; Dubé, P.; Roy, D.; Pilon, G.; Marette, A.; Levy, É.; Jacquot, C.; Urdaci, M.; et al. Modulatory effects of a cranberry extract co-supplementation with Bacillus subtilis CU1 probiotic on phenolic compounds bioavailability and gut microbiota composition in high-fat diet-fed mice. PharmaNutrition 2015, 3, 89–100. [Google Scholar] [CrossRef]
- Litvak, Y.; Byndloss, M.X.; Tsolis, R.M.; Bäumler, A.J. Dysbiotic Proteobacteria expansion: A microbial signature of epithelial dysfunction. Curr. Opin. Microbiol. 2017, 39, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Tilg, H.; Zmora, N.; Adolph, T.E.; Elinav, E. The intestinal microbiota fuelling metabolic inflammation. Nat. Rev. Immunol. 2019, 20, 40–54. [Google Scholar] [CrossRef]
- Bradley, P.H.; Pollard, K.S. Proteobacteria explain significant functional variability in the human gut microbiome. Microbiome 2017, 5, 36. [Google Scholar] [CrossRef]
- Rios-Covian, D.; Salazar, N.; Gueimonde, M.; de los Reyes-Gavilan, C.G. Shaping the metabolism of intestinal Bacteroides population through diet to improve human health. Front. Microbiol. 2017, 8, 376. [Google Scholar] [CrossRef] [PubMed]
- Zafar, H.; Saier, M.H. Gut Bacteroides species in health and disease. Gut Microbes 2021, 13, 1848158. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Li, W.; Wang, C.; Wang, L.; He, T.; Hu, H.; Song, J.; Cui, C.; Qiao, J.; Qing, L.; et al. Enterotype Bacteroides is associated with a high risk in patients with diabetes: A pilot study. J. Diabetes Res. 2020, 2020, 6047145. [Google Scholar] [CrossRef] [PubMed]
- Nash, V.; Ranadheera, C.S.; Georgousopoulou, E.N.; Mellor, D.D.; Panagiotakos, D.B.; McKune, A.J.; Kellett, J.; Naumovski, N. The effects of grape and red wine polyphenols on gut microbiota—A systematic review. Food Res. Int. 2018, 113, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Egshatyan, L.; Kashtanova, D.; Popenko, A.; Tkacheva, O.; Tyakht, A.; Alexeev, D.; Karamnova, N.; Kostryukova, E.; Babenko, V.; Vakhitova, M.; et al. Gut microbiota and diet in patients with different glucose tolerance. Endocr. Connect. 2016, 5, 9. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, K.S.; Bourwis, N.; Dolan, S.; Lang, S.; Spencer, J.; Craft, J.A. Characterisation of gut microbiota of obesity and type 2 diabetes in a rodent model. Biosci. Microbiota Food Health 2021, 40, 74. [Google Scholar] [CrossRef]
- Kashtanova, D.A.; Tkacheva, O.N.; Doudinskaya, E.N.; Strazhesko, I.D.; Kotovskaya, Y.V.; Popenko, A.S.; Tyakht, A.V.; Alexeev, D.G. Gut microbiota in patients with different metabolic statuses: Moscow study. Microorganisms 2018, 6, 98. [Google Scholar] [CrossRef]
- Nadal, I.; Santacruz, A.; Marcos, A.; Warnberg, J.; Garagorri, M.; Moreno, L.A.; Martin-Matillas, M.; Campoy, C.; Martí, A.; Moleres, A.; et al. Shifts in clostridia, bacteroides and immunoglobulin-coating fecal bacteria associated with weight loss in obese adolescents. Int. J. Obes. 2009, 33, 758–767. [Google Scholar] [CrossRef]
- Moorthy, M.; Sundralingam, U.; Palanisamy, U.D. Polyphenols as prebiotics in the management of high-fat diet-induced obesity: A Systematic review of animal studies. Foods 2021, 10, 299. [Google Scholar] [CrossRef]
- Portela-Cidade, J.P.; Borges-Canha, M.; Leite-Moreira, A.F.; Pimentel-Nunes, P. Systematic review of the relation between intestinal microbiota and Toll-like receptors in the metabolic syndrome: What Do we know so far? GE Port. J. Gastroenterol. 2015, 22, 258. [Google Scholar] [CrossRef]
- Shah, V.; Lambeth, S.M.; Carson, T.; Lowe, J.; Ramaraj, T.; Leff, J.W.; Luo, L.; Bell, C.J. Composition diversity and abundance of gut microbiome in prediabetes and type 2 diabetes. J. Diabetes Obes. 2015, 2, 108–114. [Google Scholar] [CrossRef]
- Chang, B.J.; Park, S.U.; Jang, Y.S.; Ko, S.H.; Joo, N.M.; Kim, S.I.; Kim, C.H.; Chang, D.K. Effect of functional yogurt NY-YP901 in improving the trait of metabolic syndrome. Eur. J. Clin. Nutr. 2011, 65, 1250–1255. [Google Scholar] [CrossRef]
- Eslinger, A.J.; Eller, L.K.; Reimer, R.A. Yellow pea fiber improves glycemia and reduces Clostridium leptum in diet-induced obese rats. Nutr. Res. 2014, 34, 714–722. [Google Scholar] [CrossRef]
- Schwiertz, A.; Taras, D.; Schäfer, K.; Beijer, S.; Bos, N.A.; Donus, C.; Hardt, P.D. Microbiota and SCFA in lean and overweight healthy subjects. Obesity 2010, 18, 190–195. [Google Scholar] [CrossRef] [PubMed]
- Rabot, S.; Membrez, M.; Blancher, F.; Berger, B.; Moine, D.; Krause, L.; Bibiloni, R.; Bruneau, A.; Gérard, P.; Siddharth, J.; et al. High fat diet drives obesity regardless the composition of gut microbiota in mice. Sci. Rep. 2016, 6, 32484. [Google Scholar] [CrossRef]
- Zhi, C.; Huang, J.; Wang, J.; Cao, H.; Bai, Y.; Guo, J.; Su, Z. Connection between gut microbiome and the development of obesity. Eur. J. Clin. Microbiol. Infect. Dis. 2019, 38, 1987–1998. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Huang, B.; Wang, L.; Lu, Q.; Liu, R. Peanut skin procyanidins ameliorate insulin resistance via modulation of gut microbiota and gut barrier in type 2 diabetic mice. J. Sci. Food Agric. 2022, 102, 5935–5947. [Google Scholar] [CrossRef]
- Matthies, C.; Evers, S.; Ludwig, W.; Schink, B. Anaerovorax odorimutans gen. nov., sp. nov., a putrescine-fermenting, strictly anaerobic bacterium. Int. J. Syst. Evol. Microbiol. 2000, 50, 1591–1594. [Google Scholar] [CrossRef]
- Duvallet, C.; Gibbons, S.M.; Gurry, T.; Irizarry, R.A.; Alm, E.J. Meta-analysis of gut microbiome studies identifies disease-specific and shared responses. Nat. Commun. 2017, 8, 1784. [Google Scholar] [CrossRef]
- Wu, M.R.; Chou, T.S.; Tzu, T.; Hospital, C.; Huang, C.Y.; Hsiao, J.K. A potential probiotic-Lachnospiraceae NK4A136 group: Evidence from the restoration of the dietary pattern from a high-fat diet. Res. Sq. 2020, preprint. [CrossRef]
- Shi, Y.; Wei, L.; Xing, L.; Wu, S.; Yue, F.; Xia, K.; Zhang, D. Sex difference is a determinant of gut microbes and their metabolites SCFAs/MCFAs in high fat diet fed rats. Curr. Microbiol. 2022, 79, 347. [Google Scholar] [CrossRef] [PubMed]
- Gao, Z.; Wu, H.; Zhang, K.; Hossen, I.; Wang, J.; Wang, C.; Xu, D.; Xiao, J.; Cao, Y. Protective effects of grape seed procyanidin extract on intestinal barrier dysfunction induced by a long-term high-fat diet. J. Funct. Foods 2020, 64, 103663. [Google Scholar] [CrossRef]
- Li, X.; Sui, Y.; Xie, B.; Sun, Z.; Li, S. Diabetes diminishes a typical metabolite of litchi pericarp oligomeric procyanidins (LPOPC) in urine mediated by imbalanced gut microbiota. Food Funct. 2021, 12, 5375–5386. [Google Scholar] [CrossRef] [PubMed]
- Yu, Y.; Chen, P.; Li, X.; Shen, S.; Li, K. Persimmon proanthocyanidins with different degrees of polymerization possess distinct activities in models of high fat diet induced obesity. Nutrients 2022, 14, 3718. [Google Scholar] [CrossRef]
- Ramos-Romero, S.; Martínez-Maqueda, D.; Hereu, M.; Amézqueta, S.; Torres, J.L.; Pérez-Jiménez, J. Modifications of gut microbiota after grape pomace supplementation in subjects at cardiometabolic risk: A randomized cross-over controlled clinical trial. Foods 2020, 9, 1279. [Google Scholar] [CrossRef] [PubMed]
- Rinott, E.; Meir, A.Y.; Tsaban, G.; Zelicha, H.; Kaplan, A.; Knights, D.; Tuohy, K.; Scholz, M.U.; Koren, O.; Stampfer, M.J.; et al. The effects of the Green-Mediterranean diet on cardiometabolic health are linked to gut microbiome modifications: A randomized controlled trial. Genome Med. 2022, 14, 29. [Google Scholar] [CrossRef]
- Andersen-Civil, A.I.S.; Arora, P.; Williams, A.R. Regulation of Enteric Infection and Immunity by Dietary Proanthocyanidins. Front. Immunol. 2021, 12, 165. [Google Scholar] [CrossRef]
- Gulhane, M.; Murray, L.; Lourie, R.; Tong, H.; Sheng, Y.H.; Wang, R.; Kang, A.; Schreiber, V.; Wong, K.Y.; Magor, G.; et al. High fat diets induce colonic epithelial cell stress and inflammation that is reversed by IL-22. Sci. Rep. 2016, 6, 28990. [Google Scholar] [CrossRef]
- Tran, H.Q.; Bretin, A.; Adeshirlarijaney, A.; Yeoh, B.S.; Vijay-Kumar, M.; Zou, J.; Denning, T.L.; Chassaing, B.; Gewirtz, A.T. “Western Diet”-induced adipose inflammation requires a complex gut microbiota. Cell. Mol. Gastroenterol. Hepatol. 2020, 9, 313–333. [Google Scholar] [CrossRef]
- Zou, J.; Chassaing, B.; Singh, V.; Pellizzon, M.; Ricci, M.; Fythe, M.D.; Kumar, M.V.; Gewirtz, A.T. Fiber-mediated nourishment of gut microbiota protects against diet-induced obesity by restoring IL-22-mediated colonic health. Cell Host Microbe 2018, 23, 41–53.E4. [Google Scholar] [CrossRef]
- Gil-Cardoso, K.; Ginés, I.; Pinent, M.; Ardévol, A.; Blay, M.; Terra, X. The co-administration of proanthocyanidins and an obesogenic diet prevents the increase in intestinal permeability and metabolic endotoxemia derived to the diet. J. Nutr. Biochem. 2018, 62, 35–42. [Google Scholar] [CrossRef]
- Gil-Cardoso, K.; Ginés, I.; Pinent, M.; Ardévol, A.; Arola, L.; Blay, M.; Terra, X. Chronic supplementation with dietary proanthocyanidins protects from diet-induced intestinal alterations in obese rats. Mol. Nutr. Food Res. 2017, 61, 1601039. [Google Scholar] [CrossRef]
- González-Quilen, C.; Gil-Cardoso, K.; Ginés, I.; Beltrán-Debón, R.; Pinent, M.; Ardévol, A.; Terra, X.; Blay, M.T. Grape-seed proanthocyanidins are able to reverse intestinal dysfunction and metabolic endotoxemia induced by a cafeteria diet in wistar rats. Nutrients 2019, 11, 979. [Google Scholar] [CrossRef] [PubMed]
- Feldman, F.; Koudoufio, M.; El-Jalbout, R.; Sauvé, M.F.; Ahmarani, L.; Sané, A.T.; Ould-Chikh, N.E.H.; N’Timbane, T.; Patey, N.; Desjardins, Y.; et al. Cranberry proanthocyanidins as a therapeutic strategy to curb metabolic syndrome and fatty liver-associated disorders. Antioxidants 2023, 12, 90. [Google Scholar] [CrossRef] [PubMed]
- Delehanty, J.B.; Johnson, B.J.; Hickey, T.E.; Pons, T.; Ligler, F.S. Binding and neutralization of lipopolysaccharides by plant proanthocyanidins. J. Nat. Prod. 2007, 70, 1718–1724. [Google Scholar] [CrossRef] [PubMed]
- Xing, J.; Li, R.; Li, N.; Zhang, J.; Li, Y.; Gong, P.; Gao, D.; Liu, H.; Zhang, Y. Anti-inflammatory effect of procyanidin B1 on LPS-treated THP1 cells via interaction with the TLR4-MD-2 heterodimer and p38 MAPK and NF-κB signaling. Mol. Cell. Biochem. 2015, 407, 89–95. [Google Scholar] [CrossRef]
- Midttun, H.L.E.; Ramsay, A.; Mueller-Harvey, I.; Williams, A.R. Cocoa procyanidins modulate transcriptional pathways linked to inflammation and metabolism in human dendritic cells. Food Funct. 2018, 9, 2883–2890. [Google Scholar] [CrossRef]
- Williams, A.R.; Klaver, E.J.; Laan, L.C.; Ramsay, A.; Fryganas, C.; Difborg, R.; Kringel, H.; Reed, J.D.; Mueller-Harvey, I.; Skov, S.; et al. Co-operative suppression of inflammatory responses in human dendritic cells by plant proanthocyanidins and products from the parasitic nematode Trichuris suis. Immunology 2017, 150, 328. [Google Scholar] [CrossRef]
- Yang, L.; Xian, D.; Xiong, X.; Lai, R.; Song, J.; Zhong, J. Proanthocyanidins against oxidative stress: From molecular mechanisms to clinical applications. BioMed Res. Int. 2018, 2018, 8584136. [Google Scholar] [CrossRef]
- Liu, T.; Zhang, L.; Joo, D.; Sun, S.C. NF-κB signaling in inflammation. Signal Transduct. Target. Ther. 2017, 2, 17023. [Google Scholar] [CrossRef]
- Bladé, C.; Aragonès, G.; Arola-Arnal, A.; Muguerza, B.; Bravo, F.I.; Salvadó, M.J.; Arola, L.; Suárez, M. Proanthocyanidins in health and disease. BioFactors 2016, 42, 5–12. [Google Scholar] [CrossRef] [PubMed]
- Koudoufio, M.; Feldman, F.; Ahmarani, L.; Delvin, E.; Spahis, S.; Desjardins, Y.; Levy, E. Intestinal protection by proanthocyanidins involves anti-oxidative and anti-inflammatory actions in association with an improvement of insulin sensitivity, lipid and glucose homeostasis. Sci. Rep. 2021, 11, 3878. [Google Scholar] [CrossRef]
- Shuhua, Y.; Lingqi, M.; Yunlong, D.; He, T.; Yao, S.; Peng, L. Proanthocyanidins activate Nrf2/ARE signaling pathway in intestinal epithelial cells by inhibiting the ubiquitinated degradation of Nrf2. BioMed Res. Int. 2022, 2022, 8562795. [Google Scholar] [CrossRef] [PubMed]
- Balkwill, F.; Charles, K.A.; Mantovani, A. Smoldering and polarized inflammation in the initiation and promotion of malignant disease. Cancer Cell 2005, 7, 211–217. [Google Scholar] [CrossRef] [PubMed]
- Zeng, H.; Ishaq, S.L.; Liu, Z.; Bukowski, M.R. Colonic aberrant crypt formation accompanies an increase of opportunistic pathogenic bacteria in C57BL/6 mice fed a high-fat diet. J. Nutr. Biochem. 2018, 54, 18–27. [Google Scholar] [CrossRef] [PubMed]
- Engelbrecht, A.M.; Mattheyse, M.; Ellis, B.; Loos, B.; Thomas, M.; Smith, R.; Peters, S.; Smith, C.; Myburgh, K. Proanthocyanidin from grape seeds inactivates the PI3-kinase/PKB pathway and induces apoptosis in a colon cancer cell line. Cancer Lett. 2007, 258, 144–153. [Google Scholar] [CrossRef]
- Ferguson, P.J.; Kurowska, E.M.; Freeman, D.J.; Chambers, A.F.; Koropatnick, J. In vivo inhibition of growth of human tumor lines by flavonoid fractions from cranberry extract. Nutr. Cancer 2006, 56, 86–94. [Google Scholar] [CrossRef]
- Zhang, C.; Chen, W.; Zhang, X.; Zheng, Y.; Yu, F.; Liu, Y.; Wang, Y. Grape seed proanthocyanidins induce mitochondrial pathway-mediated apoptosis in human colorectal carcinoma cells. Oncol. Lett. 2017, 14, 5853–5860. [Google Scholar] [CrossRef]
- López-Oliva, M.E.; Agis-Torres, Á.; Goñi, I.; Muñoz-Martínez, E. Grape antioxidant dietary fibre reduced apoptosis and induced a pro-reducing shift in the glutathione redox state of the rat proximal colonic mucosa. Br. J. Nutr. 2010, 103, 1110–1117. [Google Scholar] [CrossRef]
- Wan, M.L.Y.; Co, V.A.; El-Nezami, H. Dietary polyphenol impact on gut health and microbiota. Crit. Rev. Food Sci. Nutr. 2020, 61, 690–711. [Google Scholar] [CrossRef]
- Khan, H.; Belwal, T.; Efferth, T.; Farooqi, A.A.; Sanches-Silva, A.; Vacca, R.A.; Nabavi, S.F.; Khan, F.; Prasad Devkota, H.; Barreca, D.; et al. Targeting epigenetics in cancer: Therapeutic potential of flavonoids. Crit. Rev. Food Sci. Nutr. 2021, 61, 1616–1639. [Google Scholar] [CrossRef]
- Banerjee, N.; Kim, H.; Talcott, S.T.; Turner, N.D.; Byrne, D.H.; Mertens-Talcott, S.U. Plum polyphenols inhibit colorectal aberrant crypt foci formation in rats: Potential role of the miR-143/protein kinase B/mammalian target of rapamycin axis. Nutr. Res. 2016, 36, 1105–1113. [Google Scholar] [CrossRef]
- Cheng, Z.; Zheng, L.; Almeida, F.A. Epigenetic reprogramming in metabolic disorders: Nutritional factors and beyond. J. Nutr. Biochem. 2018, 54, 1–10. [Google Scholar] [CrossRef] [PubMed]

| Bacteria | Taxa | Phylum | Effect | Origin and Dose | Experimental Model | PA Introduction | PA Intake Period | Reference |
|---|---|---|---|---|---|---|---|---|
| Akkermansia | Genus | Verrucomicrobia | ↑ | Red cranberry PAs (300 mg/kg) | HFHNCCD mice (65% lipids, 15% proteins and 20% CH) | 1 week before starting the HFHNCCD | 8 weeks | [59] |
| Akkermansia muciniphila | Species | Verrucomicrobia | ↑ | Wild blueberry PAs (200 mg/kg) | HFHNCCD mice (65% lipids, 15% proteins and 20% CH) | Simultaneous beginning with the experimental diet | 8 weeks | [63] |
| Akkermansia muciniphila | Species | Verrucomicrobia | ↑ | Cranberry extract PAs (200 mg/kg) | HFHNCCD mice C57BI/6J (65% lipids, 15% proteins and 20% CH) | 13 weeks after HFHNCCD | 8 weeks | [67] |
| Allobaculum | Genus | Firmicutes | ↑ | Cinnamon (2 g/kg) and grape extract (8.2 g/kg) | HFD mice (60% kcal fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [12] |
| Bacteroidetes | Phylum | Bacteroidetes | ↑ | Cinnamon (2 g/kg) and grape extract (8.2 g/kg) | HFD mice (60% kcal fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [12] |
| Bacteroidetes | Phylum | Bacteroidetes | ↑ | B2 procyanidin (0.2% of diet) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Bifidobacterium | Genus | Actinobacteria | ↑ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Bifidobacteriaceae | Family | Actinobacteria | ↑ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal diet + 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Clostridium XIVa | Cluster | Firmicutes | ↑ | Grape seed extract (300 mg/kg) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Coprobacillus | Genus | Firmicutes | ↑ | Cranberry extract PAs (200 mg/kg) | HFHNCCD mice C57BI/6J (65% lipids, 15% proteins and 20% CH) | 13 weeks after HFHNCCD | 8 weeks | [67] |
| Faecalibacterium praustnitzii | Species | Firmicutes | ↑ | Carob fruit extract (4 g/kg restructured meat) | HFD mice (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Lactobacillales | Order | Firmicutes | ↑ | Blueberry PAs (10% of diet) | HFD mice (45% kcal as fat) | Simultaneous beginning with the experimental diet | 8 weeks | [60] |
| Lactobacillus | Genus | Firmicutes | ↑ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Lactobacillus | Genus | Firmicutes | ↑ | Persimmon tannins (50 or 100 mg/kg) | High-cholesterol Diet Sprague Dawley rats | Simultaneous beginning with the experimental diet | 4 weeks | [66] |
| Lactobacillus | Genus | Firmicutes | ↑ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal diet + 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Roseburia | Genus | Firmicutes | ↑ | Grape seed extract (300 mg/kg) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Roseburia | Genus | Firmicutes | ↑ | Cinnamon (2 g/kg) and grape extract (8.2 g/kg) | HFD mice (60% kcal fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [12] |
| Bacteria | Taxa | Phylum | Effect | Origin and Dose | Experimental Model | PA Introduction | PA Intake Period | Reference |
|---|---|---|---|---|---|---|---|---|
| Actinomycetales | Order | Actinobacteria | ↑ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal diet + 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Adlercreutzia | Genus | Actinobacteria | ↑ | Blueberry powder PAs (160 mg) | HFHNCCD mice (65% fat + 18% sucrose) | Simultaneous beginning with the experimental diet | 12 weeks | [62] |
| Adlercreutzia equolifaciens | Species | Actinobacteria | ↑ | Wild blueberry PAs (200 mg/kg) | HFHNCCD mice (65% lipids, 15% proteins and 20% CH) | Simultaneous beginning with the experimental diet | 8 weeks | [63] |
| Bacteroides | Genus | Bacteroidetes | ↑ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Bacteroides | Genus | Bacteroidetes | ↓ | Grape seed extract (300 mg/Kg/day) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Bacteroides | Genus | Bacteroidetes | ↓ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal die t+ 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Barnesiella | Genus | Bacteroidetes | ↑ | Cranberry extract PAs (200 mg/kg) | HFHNCCD mice C57BI/6J (65% lipids, 15% proteins and 20% CH) | 13 weeks after HFHNCCD | 8 weeks | [67] |
| Bilophila | Genus | Proteobacteria | ↓ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Blautia | Genus | Firmicutes | ↑ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Blautia | Genus | Firmicutes | ↑ | Procyanidin (100 mg/kg) | C57BL/6 mice with HFD (60% kcal from fat) | Simultaneous beginning with the experimental diet | 12 weeks | [65] |
| Blautia | Genus | Firmicutes | ↑ | Grape seed extract (300 mg/Kg/day) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Blautia | Genus | Firmicutes | ↑ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal die t+ 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Blautia coccoides - Eubacterium rectale | Group | Firmicutes | ↓ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Blautia coccoides - Eubacterium rectale | Group | Firmicutes | ↓ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | 3 weeks after HFD | 5 weeks | [61] |
| Clostridium leptum | Group | Firmicutes | ↓ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | Simultaneous beginning with the experimental diet | 8 weeks | [61] |
| Lachnoclostridium | Genus | Firmicutes | ↓ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Lachnospiraceae | Family | Firmicutes | ↓ | Procyanidin (100 mg/kg) | C57BL/6 mice with HFD (60% kcal from fat) | Simultaneous beginning with the experimental diet | 12 weeks | [65] |
| Muribaculum intestinale | Species | Bacteroidetes | ↑ | Blueberry powder PAs (160 mg) | HFHNCCD mice (65% fat + 18% sucrose) | Simultaneous beginning with the experimental diet | 12 weeks | [62] |
| Oscillospira | Genus | Firmicutes | ↓ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal die t+ 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Proteobacteria | Phylum | Proteobacteria | ↑ | Grape seed extract (300 mg/Kg/day) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Proteobacteria | Phylum | Proteobacteria | ↑ | Blueberry PAs (10% of diet) | HFD mice (45% kcal as fat) | Simultaneous beginning with the experimental diet | 8 weeks | [60] |
| Proteobacteria | Phylum | Proteobacteria | ↑ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Proteus | Genus | Proteobacteria | ↓ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Ruminococcus | Genus | Firmicutes | ↓ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal die t+ 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Ruminococcaceae | Family | Firmicutes | ↓ | Procyanidin (100 mg/kg) | C57BL/6 mice with HFD (60% kcal from fat) | Simultaneous beginning with the experimental diet | 12 weeks | [65] |
| Turicibacterales | Order | Firmicutes | ↑ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal diet + 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Bacteria | Taxa | Phylum | Effect | Origin and Dose | Experimental Model | PAs Introduction | PAs Intake Period | Reference |
|---|---|---|---|---|---|---|---|---|
| Desulfovibrio | Genus | Proteobacteria | ↓ | Procyanidin (100 mg/kg) | C57BL/6 mice with HFD (60% kcal from fat) | Simultaneous beginning with the experimental diet | 12 weeks | [65] |
| Desulfovibrionaceae | Family | Proteobacteria | ↓ | Cinnamon (2 g/kg) and grape extract (8.2 g/kg) | HFD mice (60% kcal fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [12] |
| Desulfovibrionaceae | Family | Proteobacteria | ↓ | Pyracantha fortuneana (0.4% of diet) | HFD rats (Normal diet + 12% fat) | 2 weeks after HFD | 8 weeks | [68] |
| Enterobacteriaceae | Family | Proteobacteria | ↓ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | 3 weeks after HFD | 5 weeks | [61] |
| Enterococcus | Genus | Firmicutes | ↓ | Persimmon tannins (50 or 100 mg/kg) | High-cholesterol Diet Sprague-Dawley rats | Simultaneous beginning with the experimental diet | 4 weeks | [66] |
| Enterococcus | Genus | Firmicutes | ↓ | Carob fruit extract (4 g/kg restructured meat) | HFD rats (50% fat, 1.4% cholesterol and 0.2% cholic acid) | 3 weeks after HFD | 5 weeks | [61] |
| Lactococcus | Genus | Firmicutes | ↓ | Grape seed extract (300 mg/Kg/day) | C57BL/6 mice with HFD (60% fat content HFD) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Lactococcus | Genus | Firmicutes | ↓ | Cinnamon (2 g/kg) and grape extract (8.2 g/kg) | HFD mice (60% kcal fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [12] |
| Firmicutes | Phylum | Firmicutes | ↓ | Blueberry PAs (10% of diet) | HFD mice (45% kcal as fat) | Simultaneous beginning with the experimental diet | 8 weeks | [60] |
| Firmicutes | Phylum | Firmicutes | ↓ | Grape seed extract (300 mg/Kg/day) | C57BL/6 mice with HFD (60% fat content) | Simultaneous beginning with the experimental diet | 7 weeks | [56] |
| Firmicutes | Phylum | Firmicutes | ↓ | B2 procyanidin (0.2%) | C57BL/6 mice with HFD (34% fat diet) | Simultaneous beginning with the experimental diet | 8 weeks | [64] |
| Firmicutes | Phylum | Firmicutes | ↓ | Persimmon tannins (50 or 100 mg/kg) | High-cholesterol Diet Sprague-Dawley rats | Simultaneous beginning with the experimental diet | 4 weeks | [66] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Redondo-Castillejo, R.; Garcimartín, A.; Hernández-Martín, M.; López-Oliva, M.E.; Bocanegra, A.; Macho-González, A.; Bastida, S.; Benedí, J.; Sánchez-Muniz, F.J. Proanthocyanidins: Impact on Gut Microbiota and Intestinal Action Mechanisms in the Prevention and Treatment of Metabolic Syndrome. Int. J. Mol. Sci. 2023, 24, 5369. https://doi.org/10.3390/ijms24065369
Redondo-Castillejo R, Garcimartín A, Hernández-Martín M, López-Oliva ME, Bocanegra A, Macho-González A, Bastida S, Benedí J, Sánchez-Muniz FJ. Proanthocyanidins: Impact on Gut Microbiota and Intestinal Action Mechanisms in the Prevention and Treatment of Metabolic Syndrome. International Journal of Molecular Sciences. 2023; 24(6):5369. https://doi.org/10.3390/ijms24065369
Chicago/Turabian StyleRedondo-Castillejo, Rocío, Alba Garcimartín, Marina Hernández-Martín, María Elvira López-Oliva, Aránzazu Bocanegra, Adrián Macho-González, Sara Bastida, Juana Benedí, and Francisco J. Sánchez-Muniz. 2023. "Proanthocyanidins: Impact on Gut Microbiota and Intestinal Action Mechanisms in the Prevention and Treatment of Metabolic Syndrome" International Journal of Molecular Sciences 24, no. 6: 5369. https://doi.org/10.3390/ijms24065369
APA StyleRedondo-Castillejo, R., Garcimartín, A., Hernández-Martín, M., López-Oliva, M. E., Bocanegra, A., Macho-González, A., Bastida, S., Benedí, J., & Sánchez-Muniz, F. J. (2023). Proanthocyanidins: Impact on Gut Microbiota and Intestinal Action Mechanisms in the Prevention and Treatment of Metabolic Syndrome. International Journal of Molecular Sciences, 24(6), 5369. https://doi.org/10.3390/ijms24065369








